Professional Documents
Culture Documents
What Is Biliary Atresia?
Uploaded by
dhinialfiandariOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
What Is Biliary Atresia?
Uploaded by
dhinialfiandariCopyright:
Available Formats
Biliary Atresia
National Digestive Diseases Information Clearinghouse
What is biliary atresia? Biliary
U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH
atresia is a life-threatening condi- tion in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic ducts, are tubes that carry bile from the liver to the gallbladder for storage and to the small intestine for use in digestion. Bile is a fluid made by the liver that serves two main functions: carrying toxins and waste prod ucts out of the body and helping the body digest fats and absorb the fat-soluble vitamins A, D, E, and K.
With biliary atresia, bile becomes trapped, builds up, and damages the liver. The damage leads to scarring, loss of liver tissue, and cirrhosis. Cirrhosis is a chronic, or long lasting, liver condition caused by scar tissue and cell damage that makes it hard for the liver to remove toxins from the blood. These toxins build up in the blood and the liver slowly deteriorates and malfunctions. Without treatment, the liver eventually fails and the infant needs a liver transplant to stay alive. The two types of biliary atresia are fetal and perinatal. Fetal biliary atresia appears while the baby is in the womb. Perinatal biliary atresia is much more common and does not become evident until 2 to 4 weeks after birth. Some infants, particularly those with the fetal form, also have birth defects in the heart, spleen, or intestines.
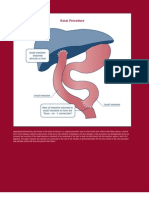
Liver Hepatic ducts
Who is at risk for biliary atresia?
Cystic duct
Gallbladder
Biliary atresia is rare and only affects about one out of every 18,000 infants.1 The disease is more common in females, premature babies, and children of Asian or African American heritage.
Duodenum Common bile duct Pancreatic duct
Pancreas Prevelance of rare diseases: Bibliographicdata. Orphareport Series, Rare Diseases Collection website. www.orpha.net/orphacom/cahiers/docs/GB/Prevalence_ of_rare_diseases_by_decreasing_prevalence_or_cases. pdf. Published November 2011. Accessed March 23,
1
Normal liver and biliary system
2012.
What are the symptoms of biliary atresia?
The first symptom of biliary atresia is jaundicewhen the skin and whites of the eyes turn yellow. Jaundice occurs when the liver does not remove bilirubin, a reddishyellow substance formed when hemoglobin breaks down. Hemoglobin is an iron-rich protein that gives blood its red color. Biliru bin is absorbed by the liver, processed, and released into bile. Blockage of the bile ducts forces bilirubin to build up in the blood. Jaundice can be difficult to detect. Many healthy infants have mild jaundice during the first 1 to 2 weeks of life due to an immature liver. This type of jaundice disappears 2 to 3 weeks after birth, whereas the jaundice of biliary atresia worsens over time. Other common symptoms of biliary atresia include dark urine, from the high levels of bilirubin in the blood spilling over into the urine gray or white stools, from a lack of bilirubin reaching the intestines slow weight gain and growth
What causes biliary atresia?
Biliary atresia likely has multiple causes, though none are yet proven. Biliary atresia is not an inherited disease, meaning it does not pass from parent to child. Therefore, survivors of biliary atresia are not at risk for passing the disorder to their children. Biliary atresia is most likely caused by an event in the womb or around the time of birth. Possible triggers of the event may include one or more of the following: a viral or bacterial infection after birth, such as cytomegalovirus, reovirus, or rotavirus an immune system problem, such as when the immune system attacks the liver or bile ducts for unknown reasons a genetic mutation, which is a perma nent change in a genes structure a problem during liver and bile duct development in the womb exposure to toxic substances
Biliary Atresia t
How is biliary atresia diagnosed?
No single test can definitively diagnose biliary atresia, so a series of tests is needed. All infants who still have jaundice 2 to 3 weeks after birth, or who have gray or white stools after 2 weeks of birth, should be checked for liver damage. 2 Infants with suspected liver damage are usually referred to a pediatric gastroenterologist, a doctor who specializes in childrens digestive diseases pediatric hepatologist, a doctor who specializes in childrens liver diseases pediatric surgeon, a doctor who special izes in operating on childrens livers and bile ducts The health care provider may order some or all of the following tests to diagnose biliary atresia and rule out other causes of liver problems. If biliary atresia is still suspected after testing, the next step is diagnostic surgery for confirmation. Blood test. A blood test involves drawing blood at a health care providers office or commercial facility and sending the sample to a lab for analysis. High levels of bilirubin in the blood can indicate blocked bile ducts.
Abdominal x rays. An x ray is a picture created by using radiation and recorded on film or on a computer. The amount of radia tion used is small. An x ray is performed at a hospital or outpatient center by an x-ray technician, and the images are interpreted by a radiologista doctor who specializes in medical imaging. Anesthesia is not needed, but sedation may be used to keep infants still. The infant will lie on a table during the x ray. The x-ray machine is positioned over the abdominal area. Abdominal x rays are used to check for an enlarged liver and spleen. Ultrasound. Ultrasound uses a device, called a transducer, that bounces safe, painless sound waves off organs to create an image of their structure. The procedure is performed in a health care providers office, outpatient center, or hospital by a specially trained technician, and the images are interpreted a radiologist. Anesthesia is not needed, but sedation may be used to keep the infant still. The images can show whether the liver or bile ducts are enlarged and whether tumors or cysts are blocking the flow of bile. An ultrasound cannot be used to diagnose biliary atresia, but it does help rule out other common causes of jaundice. Liver scans. Liver scans are special x rays that use chemicals to create an image of the liver and bile ducts. Liver scans are performed at a hospital or outpatient facility, usually by a nuclear medicine technician. The infant will usually receive general anesthesia or be sedated before the procedure. Hepatobiliary iminodiacetic acid scanning, a type of liver scan, uses injected radioactive
Hartley JL, Davenport M, Kelly DA. Biliary atresia. Lancet. 2009;374(9702):17041713.
2
dye to trace the path of bile in the body. The test can show if and where bile flow is blocked. Blockage is likely to be caused by biliary atresia. Liver biopsy. A biopsy is a procedure that involves taking a piece of liver tissue for examination with a microscope. The biopsy is performed by a health care provider in a hospital with light sedation and local anesthetic. The health care provider uses imaging techniques such as ultrasound or a computerized tomography scan to guide the biopsy needle into the liver. The liver tissue is examined in a lab by a pathologista doctor who specializes in diagnosing diseases. A liver biopsy can show whether biliary atresia is likely. A biopsy can also help rule out other liver problems, such as hepatitisan irritation of the liver that sometimes causes permanent damage. Diagnostic surgery. During diagnostic surgery, a pediatric surgeon makes an incision, or cut, in the abdomen to directly examine the liver and bile ducts. If the surgeon confirms that biliary atresia is the problem, a Kasai procedure will usually be performed immediately. Diagnostic surgery and the Kasai procedure are performed at a hospital or outpatient facility; the infant will be under general anesthesia during surgery.
How is biliary atresia treated?
Biliary atresia is treated with surgery, called the Kasai procedure, or a liver transplant.
Kasai Procedure
The Kasai procedure, named after the surgeon who invented the operation, is usually the first treatment for biliary atresia. Dur ing a Kasai procedure, the pediatric surgeon removes the infants damaged bile ducts and brings up a loop of intestine to replace them. As a result, bile flows straight to the small intestine. While this operation doesnt cure biliary atresia, it can restore bile flow and correct many problems caused by biliary atresia. Without surgery, infants with biliary atresia are unlikely to live past age 2. This proce dure is most effective in infants younger than 3 months old, because they usually havent yet developed permanent liver damage. Some infants with biliary atresia who undergo a successful Kasai procedure regain good health and no longer have jaundice or major liver problems.
Liver
Gallbladder
Small intestine
The Kasai procedure
Biliary Atresia
If the Kasai procedure is not successful, infants usually need a liver transplant within 1 to 2 years. Even after a successful surgery, most infants with biliary atresia slowly develop cirrhosis over the years and require a liver transplant by adulthood.
What are possible complications after the Kasai procedure?
After the Kasai procedure, some infants continue to have liver problems and, even with the return of bile flow, some infants develop cirrhosis. Possible complications after the Kasai procedure include ascites, bacterial cholangitis, portal hypertension, and pruritus. Ascites. Problems with liver function can cause fluid to build up in the abdomen, called ascites. Ascites can lead to spontane ous bacterial peritonitis, a serious infection that requires immediate medical attention. Ascites usually only lasts a few weeks. If ascites lasts more than 6 weeks, cirrhosis is likely present and the infant will probably need a liver transplant. Bacterial cholangitis. Bacterial cholangitis is an infection of the bile ducts that is treated with bacteria-fighting medications called antibiotics. Portal hypertension. The portal vein carries blood from the stomach, intestines, spleen, gallbladder, and pancreas to the liver. In cirrhosis, scar tissue partially blocks and slows the normal flow of blood, which increases the pressure in the portal vein. This condition is called portal hypertension. Portal hyperten sion can cause gastrointestinal bleeding that may require surgery and an eventual liver transplant.
Liver Transplant
Liver transplantation is the definitive treat ment for biliary atresia, and the survival rate after surgery has increased dramatically in recent years. As a result, most infants with biliary atresia now survive. Progress in transplant surgery has also increased the availability and efficient use of livers for transplantation in children, so almost all infants requiring a transplant can receive one. In years past, the size of the transplanted liver had to match the size of the infants liver. Thus, only livers from recently deceased small children could be trans planted into infants with biliary atresia. New methods now make it possible to transplant a portion of a deceased adults liver into an infant. This type of surgery is called a reduced-size or split-liver transplant. Part of a living adult donors liver can also be used for transplantation. Healthy liver tissue grows quickly; therefore, if an infant receives part of a liver from a living donor, both the donor and the infant can grow complete livers over time.
Infants with fetal biliary atresia are more likely to need a liver transplantand usually soonerthan infants with the more common perinatal form. The extent of damage can also influence how soon an infant will need a liver transplant.
Pruritus. Pruritus is caused by bile buildup in the blood and irritation of nerve endings in the skin. Prescription medication may be recommended for pruritus, including resins that bind bile in the intestines and antihista mines that decrease the skins sensation of itching.
Biliary Atresia
What medical care is needed after a liver transplant?
After a liver transplant, a regimen of medica tions is used to prevent the immune system from rejecting the new liver. Health care providers may also prescribe blood pressure medications and antibiotics, along with special diets and vitamin supplements.
Points to Remember
Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. The first symptom of biliary atre sia is jaundicewhen the skin and whites of the eyes turn yellow. Other symptoms include dark urine, gray or white stools, and slow weight gain and growth. Biliary atresia likely has multiple causes, though none is yet proven. No single test can definitively diagnose biliary atresia, so a series of tests is needed, including a blood test, abdominal x ray, ultrasound, liver scans, liver biopsy, and diagnostic surgery. Initial treatment for biliary atresia is usually the Kasai procedure, an operation where the bile ducts are removed and a loop of intestine is brought up to replace them. The definitive treatment for biliary atresia is liver transplant.
Eating, Diet, and Nutrition
Infants with biliary atresia often have nutri tional deficiencies and require special diets as they grow up. They may need a higher calorie diet, because biliary atresia leads to a faster metabolism. The disease also prevents them from digesting fats and can lead to protein and vitamin deficiencies. Vitamin supplements may be recommended, along with adding medium-chain triglyceride oil to foods, liquids, and infant formula. The oil adds calories and is easier to digest without bile than other types of fats. If an infant or child is too sick to eat, a feeding tube may be recommended to provide high-calorie liquid meals. After a liver transplant, most infants and children can go back to their usual diet. Vitamin supplements may still be needed because the medications used to keep the body from rejecting the new liver can affect calcium and magnesium levels.
After a liver transplant, a regimen of medications is used to prevent the immune system from rejecting the new liver. Health care providers may also prescribe blood pressure medications and antibiotics, along with special diets and vitamin supplements.
Biliary Atresia
Hope through Research
Researchers are studying the possible causes of biliary atresia and new ways to diagnose and treat it. One of the largest research initiatives is the ChiLDREN (the Childhood Liver Disease Research and Education Net work), a consortium of centers funded by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). More infor mation about ChiLDRENs clinical trials, funded under National Institutes of Health clinical trial number NCT00061828, can be found at www.childrennetwork.org. The network comprises 15 liver disease and transplant centers and one data-coordinating center. The centers work together to coordi nate research and share ideas and resources. The network enrolls infants with biliary atresia in a large study to evaluate the best ways of managing the disease and to carry out clinical trials of new and promising treat ments or approaches for diagnosis and moni toring the disease. Biliary atresia is a rare disease; therefore, only a network of centers can identify enough infants with this disease to carry out studies of new therapies. Centers collect blood, tissue, and other samples from infants with biliary atresia so researchers can learn more about biliary atresia and find better treatments. An important goal of ChiLDREN is to help find the causes of biliary atresia and make recommendations for early detection and proper management.
For More Information
American Association for the Study of Liver Diseases 1001 North Fairfax Street, Suite 400 Alexandria, VA 22314 Phone: 7032999766 Fax: 7032999622 Email: aasld@aasld.org Internet: www.aasld.org
American Liver Foundation 39 Broadway, Suite 2700 New York, NY 10006 Phone: 1800GOLIVER (1800 4654837) or 2126681000 Fax: 2124838179 Email: info@liverfoundation.org Internet: www.liverfoundation.org
Childrens Liver Association for Support Services 25379 Wayne Mills Place, Suite 143 Valencia, CA 91355 Phone: 18776798256 or 6612639099 Fax: 6612639099 Email: info@classkids.org Internet: www.classkids.org
Acknowledgments
Publications produced by the Clearinghouse are carefully reviewed by both NIDDK scientists and outside experts. This publication was originally reviewed by ChiLDREN investigators: Ronald Sokol, M.D., University of Colorado/The Childrens Hospital of Denver; Jorge Bezerra, M.D., Cincinnati Childrens Hospital and Medical Center; and Benjamin Shneider, M.D., Mount Sinai Hospital of New York. The original illustration of the Kasai procedure was provided by Julie Porter.
Participants in clinical trials can play a more active role in their own health care, gain access to new research treatments before they are widely available, and help others by contributing to medical research. For information about current studies, visit www.ClinicalTrials.gov.
Biliary Atresia
You may also find additiona l informatio n about this topic by visiting MedlinePlu s at www.medlineplus.gov. This publication may contain informatio n about medications. When prepared , this publication included the most current informatio n available. For updates or for questions about any medications, contact the U.S. Food and Drug Administratio n tollfree at 1888INFOF DA (18884636332) or visit www.fda.gov. Consult your health care provider for more information.
National Digestive Diseases Information Clearinghouse
2 Information Way Bethesda, MD 208923570 Phone: 18008915389 TTY: 18665691162 Fax: 7037384929 Email: nddic@info.niddk.nih.gov Internet: www.digestive.niddk.nih.gov
The National Digestive Diseases Information Clearinghouse (NDDIC) is a service of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). The NIDDK is part of the National Institutes of Health of the U.S. Department of Health and Human Services. Established in 1980, the Clearinghouse provides information about digestive diseases to people with digestive disorders and to their families, health care professionals, and the public. The NDDIC answers inquiries, develops and distributes publications, and works closely with professional and patient organizations and Government agencies to coordinate resources about digestive diseases.
This publication is not copyrighted. The Clearinghouse encourages users of this publication to duplicate and distribute as many copies as desired. This publication is available at www.digestive.niddk.nih.gov.
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
NIH Publication No. 125289 July 2012
The NIDDK prints on recycled paper with bio-based ink.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- 20 Prolonged JaundiceDocument2 pages20 Prolonged JaundiceGiorgi BradNo ratings yet
- Routine Neonatal Care: Neonatology DR - MHD BonowaraDocument75 pagesRoutine Neonatal Care: Neonatology DR - MHD Bonowaraahmed abosamraNo ratings yet
- Neonatal Cholestasis 2Document28 pagesNeonatal Cholestasis 2HafsaJabbarNo ratings yet
- HepatosplenomegalyDocument10 pagesHepatosplenomegalyนายนภนต์ จันทมณีNo ratings yet
- Approach To Hepatomegaly, Splenomegaly and HepatosplenomegalyDocument43 pagesApproach To Hepatomegaly, Splenomegaly and HepatosplenomegalyLee Jun Xiong100% (2)
- 33 34 IV 12 Atresia BiliarisDocument13 pages33 34 IV 12 Atresia BiliarisTasia AmeliaNo ratings yet
- Presentation Utk State Meetng (DR DAUD)Document45 pagesPresentation Utk State Meetng (DR DAUD)Mohd Daud Che YusofNo ratings yet
- Neonatal Jaundice: AuthorsDocument9 pagesNeonatal Jaundice: AuthorsRam Kumar ShresthaNo ratings yet
- Liver, Biliary Tree and Pancreas Pathology Lecture Final by DRDocument94 pagesLiver, Biliary Tree and Pancreas Pathology Lecture Final by DRapi-3700579100% (5)
- 19 Anesthesia For Biliary AtresiaDocument19 pages19 Anesthesia For Biliary AtresiaDwiki Surya PrayogaNo ratings yet
- Pediatric Cholestasis: Epidemiology, Genetics, Diagnosis, and Current ManagementDocument5 pagesPediatric Cholestasis: Epidemiology, Genetics, Diagnosis, and Current ManagementAnnisa SusiloNo ratings yet
- Ni Hms 267898Document20 pagesNi Hms 267898Thesar WaldiNo ratings yet
- Ascending Cholangitis - Pao EditDocument62 pagesAscending Cholangitis - Pao EditSamuel WibowoNo ratings yet
- Article Wjpps 15465140481Document12 pagesArticle Wjpps 15465140481Tech RajaNo ratings yet
- Biliary Atresia Copy LNGDocument10 pagesBiliary Atresia Copy LNGlloraoNo ratings yet
- Extrahepatic Biliary AtresiaDocument3 pagesExtrahepatic Biliary AtresiaTiti Afrianto100% (1)
- The Murmur - October 2014Document9 pagesThe Murmur - October 2014RyanLoveNo ratings yet
- (Hepatoportoenterostomy) : Anna M. Banc-Husu, MDDocument1 page(Hepatoportoenterostomy) : Anna M. Banc-Husu, MDwatimelawatiNo ratings yet
- What Is Biliary Atresia?Document10 pagesWhat Is Biliary Atresia?dhinialfiandariNo ratings yet
- Biliary AtresiaDocument25 pagesBiliary Atresiajulius billiNo ratings yet
- Hepatomegaly in Neonates and Children: Ann D. Wolf, MD, and Joel E. Lavine, MD, PHDDocument10 pagesHepatomegaly in Neonates and Children: Ann D. Wolf, MD, and Joel E. Lavine, MD, PHDmirfanjee89No ratings yet
- Neonatal Hepatitis SyndromeDocument18 pagesNeonatal Hepatitis Syndromeenny_rommyNo ratings yet
- KasaiDocument7 pagesKasaishalukiriNo ratings yet
- Bagan KolestasisDocument1 pageBagan KolestasisSoma SkaNo ratings yet
- Quiz Gastrointestinal Part 2 of 2Document34 pagesQuiz Gastrointestinal Part 2 of 2MedShare100% (1)
- Atresia BilieerDocument9 pagesAtresia BilieerSolo UpdateNo ratings yet
- Biliary Atresia Digestive IVDocument13 pagesBiliary Atresia Digestive IVherdigunantaNo ratings yet
- Hepatomegali in Infant and Children - Pediatrics in Review-2000-Wolf-303-10Document10 pagesHepatomegali in Infant and Children - Pediatrics in Review-2000-Wolf-303-10Reddy LufyanNo ratings yet
- Neonatal Jaundice CME ANisDocument47 pagesNeonatal Jaundice CME ANisAnisNo ratings yet