Professional Documents
Culture Documents
2011 Lown Forum 3
Uploaded by
Lown Cardiovascular Research FoundationCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2011 Lown Forum 3
Uploaded by
Lown Cardiovascular Research FoundationCopyright:
Available Formats
Lown Forum
Although sometimes dicult to understand or talk about, end-oflife care should be discussed with family when the time comes.
T HE
2011
NUMBER
LOWN CARDIOVASCULAR RESEARCH FOUNDATION
Mahlers Ninth
Fred Mamuya, MD, PhD
A family conversation
Edith Davis, who was 91 and suering from congestive heart failure, did not want to spend her last days in a hospital. Her family reects on their experience with hospice and the importance of discussing end-of-life care. (Patient prole, page 4) accepting or voicing the truth that despite our best eorts, death may ultimately prevail. I suspect that many patients hope that we, as physicians, will tell them when further eorts are most likely futile. While most physicians can recognize when a patient is going to lose the battle, we are not good at guessing when he/she is going to die. One of the few quibbles I have with current hospice rules is having to certify that my patient has six months to live, before he/she can be enrolled in hospice. It is my hope that this requirement will ultimately be waived, since many patients cannot be so neatly categorized. My rst patient who enrolled in hospice ended up living for over a year, with a relatively good quality of life until the very end, and I received regular letters asking if we should continue to have the patient enrolled in hospice! I later found out that this was not so unusual, and that paradoxically many patients who enroll in hospice care end up living longer than expected.
At the Lown Center, we meet four times a year to review the lives and care of all of our patients who have passed away. This past February, while preparing for our quarterly mortality conference, I discovered that about 20% of these patients had died while under the care of hospice. Since I was unaware of the existence of a death-panel at our center, it seemed reasonable to spend time exploring endof-life care in this issue of the Forum. Once upon a time, most of us were born in our homes, and died in our homes. Times have changed, and perhaps due to the progress of modern medicine, we are now almost always born in a hospital and die in one too. Yet in all my years of practicing clinical medicine, I have not encountered a patient who would prefer to die in a hospital, let alone in an intensive care unit. As a society, why are we so ill equipped at dealing with one of the absolute certainties in life? I believe how we choose to die is the nal frontier of personalized medicine. When it comes to end-of-life decisions, having a choice is of paramount importance for each individual. Since we are all going to die at some point, I suspect people would prefer to have a choice regarding end-of-life care and the trade-os we are willing to make at the end.
Myths regarding hospice
Contrary to popular beliefs and fears, hospice care does not mean cessation of care. Instead, the focus and priority of hospice care is on the quality of life, and not the prolongation of life. Hospice tries to help patients have the fullest possible life without pain, while maintaining mental alertness for as long as possible so that the patient has the opportunity to reect on life, put aairs in order, say goodbye to friends, and spend time with loved ones without being a burden to the family in the process. The opportunity to have closure is also immensely benecial to families, and it has been shown that caregivers of patients who die in hospice are less likely to experience a major depression in the subsequent six months.
The physicians role
Why, then, are clinicians hesitant to initiate this conversation? Many case reports in medical literature have shown patients who have had unexpected responses to therapy, and outlived their projected demise for many years. Thus, any discussion about dying is usually fraught with peril for the clinician, lest it be interpreted as reluctance to ght or prematurely giving up on a patient. When faced with a dying patient, it is natural for physicians to oer hope, and we usually have trouble
Focus on relationships
The relationship between patients and their families is central to this conversation. Patients are often willing to
continued on page 4
INSIDE
2 3 4
Presidents message Meet the Lown sta: Pdraig Carolan ProCor: Louise Lown Heart Hero Award Mahlers Ninth (cont.) Patient prole: A family conversation
5 6 7 8
Development in action How can I stick to a weight-loss routine? Lown Scholars: Solutions 7500 miles away
NewsBeat
Exercising as you grow older
LOW N
FO RUM
PRESIDENTS MESSAgE
MEET THE LOWN CENTER STAFF
Less is more
Vikas Saini, MD
Less is more. Architect Mies van der Rohe coined the phrase in 1959, referring to a simpler aesthetic that serves a buildings purpose more eectively than an elaborate design. What does less is more mean for health care and the Lown Foundation? Surgery and other risky invasive procedures are the last resort, and less invasive treatments dietary, exercise, medication often do more for the patient. This approach has always been our hallmark, and its been the Foundations role to advance that model of care.
Pdraig Carolan
As the research assistant for the Lown Foundation, Pdraig Carolan is working on two second opinion research projects designed to study the Lown Centers model of care. Sometimes patients come to the Lown Center looking for a second opinion regarding coronary bypass grafting or angioplasty, Pdraig explains. Starting with patients who came to the Lown Center in 1992 for a second opinion, were looking to see what their original advice was, what advice they received at the Lown Center, and how they subsequently fared. The other second opinion project involves patients who came to the Lown Center between 2007 and 2011. By using our practice management software, we can identify the second opinion patients and then review their charts to gather data. We hope to answer some of the same questions that we have with the 1992 patient set, but with data that reect more recent changes in both surgical procedures and medical management. Prior to the second opinion research, Pdraig worked on the Lown Centers Home Care Pilot Study. One set of patients had regularly scheduled faceto-face conversations with their cardiologist over the internet. The other set of patients had regularly scheduled phone calls with their cardiologist. We wanted to see if there was any benet when a patient talks to his/her doctor face-to-face compared to over the telephone. Originally from Dublin, Pdraig moved to Massachusetts at the age of eight. He graduated from University of Notre Dame with a degree in psychology, and has worked at the Lown Foundation for three and a half years. Pdraig lives in Brighton with his wife Carrie, a history teacher at BC High School, and in his spare time, he enjoys camping and hiking. I feel I am making an important contribution to the advancement of cardiovascular health, Pdraig says of his work at the Lown Foundation.
Why have a less is more approach? For one, its better for patients. And it saves money.
After years of being a voice in the wilderness, we now have many allies who recognize the severity of the issue. Unfortunately, the message still isnt widespread. So the Lown Foundation, partnering with the New America Foundation and the Institute of Medicine, is organizing a conference on avoidable care for spring 2012. Policymakers, payers, providers, and patients must recognize the need to remedy the avoidable care problem, including overutilization of routine services, defensive medicine, and inappropriate care. In a New York Times editorial, cardiologist Rita Redberg - who is on the organizing committee for our conference - highlights the problem of avoidable care with several examples: Clinical trials have shown that cardiac stents are no more eective than drugs or lifestyle changes in preventing heart attacks or deathSome studies have shown that stents provide short-term relief of chest pain, but up to 30% of patients receiving stents have no chest pain to begin with, and thus derive no more benet than from equally eective and less expensive medicines. A recent study found that one-fth of all implantable cardiac debrillators were placed in patients who will not benet from them. Medicare pays anyway, at a cost of $50,000 to $100,000 per device implantation. Our conference will be the rst in a series of meetings seeking to catalyze a deep shift in medical culture and education necessary for developing a new ethic around unnecessary care. generating public support to focus national attention on the problem requires leadership. Our goal is to contribute to the long-term eort to transform the culture of health care in the US from one where patients and providers focus on volume and quantity of services to one centered on value and quality.
Reading the Forum online
Did you know you can read the Lown Forum online? To read it on our website or to have a copy emailed to you, please visit www.lownfoundation.org or email info@lownfoundation.org.
LOW N
FO RUM
PROCOR
Educating children to prevent RHD
Benn grover & Jocelyn Sterling The Kenyan-Heart National Foundation receives the 2011 Louise Lown Heart Hero Award
The Kenyan-Heart National Foundations (KHNF) rheumatic heart disease (RHD) prevention program recently received the globally recognized Louise Lown Heart Hero Award from ProCor and the Lown Foundation. Through local initiatives and outreach eorts, the KHNF successfully educates thousands of children on RHD prevention. Virtually unheard of in Europe and the US, RHD is a major cause of death in the developing world. Although current estimates say around 15 million people worldwide have RHD (80% are in the developing world), recent research suggests that it is more likely to be between 62 million and 78 million people and that 1.4 million people die each year because of it. In Kenya alone, there are over 200,000 new cases of RHD each year, and it is the most common cardiovascular disease among children and young people. RHD is caused by strep throat, which can be easily treated. It costs around US$1 to treat one case of strep throat with penicillin; however many people are unaware that they should seek treatment for strep throat. As a result, untreated strep throat leads to rheumatic fever, which leads to RHD requiring open heart surgery that costs thousands of dollars.
only having an impact on the prevention of RHD, but also on the spread of other diseases, said Vibeke Hjortdal from Aarhus University Hospital in Denmark. The KHNFs Kitchen gardens program encourages schools to create fruit and vegetable gardens to help serve healthy foods to schoolchildren this program has reached 60-70% of the public schools in Nairobi. Additionally, the KHNF has organized over 150 KenyanHeart Clubs, which provide opportunities for children to learn about heart health and educate their communities through poems, skits, and dance. The 2010 Heart Clubs Day, which is an annual event that brings together all 150 clubs to compete in activities and showcase their prevention eorts, had 5000 schoolchildren participate.
The strength of the project is its focus on a relatively unknown preventable disease and the organization of local civil society around this issue, said Nicolai Houe, from PACT.
The prevention message does not stop at children. I believe children are very good advocates. Even though they are the ones at risk, they are not shy and once they know something it is very dicult for them to keep quiet. They are great messengers; they have a strong ability to inuence others, like their parents, said Elizabeth gatumia, Executive Director of the KHNF. In addition to using schoolchildren as heart health advocates, the KHNF targets adults with their education programs. In 2011 alone, the KHNF has trained around 1000 adults, 500 teachers, and 300 faith-based leaders on NCD prevention.
Plans for the future
Their RHD prevention program works. Now the goal is to expand to communities all across Kenya. Nairobi has been our area of operation so far, but we hope to Teaching children about RHD expand. People have heard about our success in dierent communities, and they are interested in being trained on RHD and NCD prevention. We know we are making a dierence, said Ms. gatumia. The annual Louise Lown Heart Hero Award recognizes innovative, preventive approaches to cardiovascular health in developing countries. The award was established in 2007 by Dr. Bernard Lown, an internationally-renowned cardiologist and Nobel Peace Prize recipient, to honor his wife, Louise, and her lifelong commitment to the wellbeing of others as a social worker, activist, and writer. For more information about the KHNF or the Louise Lown Heart Hero Award, visit www.procor.org.
This was a dicult selection process. All of the applicants were very deserving of recognition and accolade, but the KHNFs RHD prevention program epitomizes a successful, reproducible project that has had and will have signicant impact, said Dr. Brian Bilchik, member of the Louise Lown Heart Hero Award review team.
By targeting the most vulnerable population children and adolescents the KHNF aims to prevent RHD before it starts. The KHNF educates schoolchildren on recognizing the symptoms of strep throat and on practicing simple but key prevention measures such as washing ones hands and covering ones mouth while sneezing or coughing. To date, the KHNF has educated nearly 11,000 schoolchildren on RHD prevention. The program focuses on information about the disease and the importance of good hygiene for prevention and the early diagnosis for treatment. The program is not
LOW N
FO RUM and fears of patients and their loved ones. Rather than just telling a patient about the disease process or survival rates, the discussion should be driven by an understanding of the entire patient The most needed skills were not taught in a medical school classroom when I was in training. Time spent with a patient, honesty about the nality of a disease process, empathy, and above all conveying that one is not abandoning the patient are among the most important elements in conversations regarding end-of-life care. Recently, I was listening to my son play Mahlers Ninth Symphony with a local youth orchestra. Sitting in the audience, I recalled some of the opening lines from an essay by Lewis Thomas on listening to Mahlers Ninth in the age of weapons of mass destruction. There was a time, not long ago, when what I heard, especially in the nal movement, was an open acknowledgement of death and at the same time a quiet celebration of the tranquility connected to the process. I took this music as a metaphor for reassurance, conrming my own strong hunch that the dying of every living creature, the most natural of all experiences, has to be a peaceful experience. It is my hope this article will initiate conversations that reassure patients that their end-of life care will be wellplanned and personalized.
(continued from page 1)
Mahlers Ninth
Fred Mamuya, MD, PhD
undergo therapies they do not want if they think their loved ones want them to do it. Unfortunately, it is not unusual to have competing desires between patients and their families, and this situation can be made worse if the patient is unable to fully participate in the discussion. On such occasions, family members may disagree on priorities and goals of care, which could lead to additional stress. It is common to have family across the country, and occasionally the globe. Fortunately new technologies that allow for video-conferencing may be helpful in enabling those necessary conversations among family members across long distances.
Engaging in a dialogue
End-of-life care should be discussed with every patient, and written advance directives should be considered a crucial part of every patients medical record. It is important to have these discussions with patients while they are still capable of being active participants, and here at the Lown Center, time spent with patients and their families remains sacrosanct. One conversation is rarely sucient, and usually multiple conversations spread over time are required to fully understand the needs, worries,
PATIENT PROFILE
A family conversation
Edith Davis, who was 91 and suering from congestive heart failure, did not want to spend her last days in a hospital. Her son, Andrew, knew she needed extensive assistance with her daily life but was unsure what options were available. To be honest, I dont think hospice ever crossed my mind. It was only after Dr. Mamuya discussed hospice that we realized there was a service other than the hospital that could assist us. On a routine visit to the Lown Center, Andrews wife, gayle, wanted an honest assessment of Ediths health and pulled Dr. Mamuya aside to ask questions. Instead of having a private talk with just me in the hallway, Dr. Mamuya waited until after Ediths checkup to have a conversation with both of us in his oce. Dr. Mamuya made sure to include Edith in the conversation. He asked her opinion and answered her questions, making it a family discussion. Everyone in the family agreed hospice was the best option because Ediths quality of life was their biggest concern. Her quality of life was hospices biggest concern as well. Hospice helped us in so many ways emotionally by
taking some of the stress away, as well as in a more direct way by answering questions and providing services. Eventually, hospice also took over Ediths increasingly complex medications. Hospice also took time to ask us how we were feeling throughout the process. They still call from time to time to ask how we are doing, said Andrew. I always thought of hospice as a service used during the last week of life, gayle said, but it ended up being a support more than anything. It never felt terminal. Communication between all members of the family was key in the smooth transition to hospice for the Davis family, and the initial discussion with Dr. Mamuya allowed for the process to occur quickly and without doubt of its necessity. The Davis realize every situation is dierent, but ultimately, believe hospice is an important service people should consider. Having the conversation with family about end of life care is key, gayle said. Everybody, whether patients, children, or parents, has to come to grips with reality, and once you do that, you see hospice as a tremendous resource, Andrew said.
LOW N
FO RUM
DEVELOPMENT
Fundraising in action
On July 27th, 2011, Lown Foundation friends from Southern Massachusetts and Rhode Island gathered at the elegant Wamsutta Club in New Bedford to learn more about the Foundations current activities. Hosted by Kenneth and gwen Sullivan, the event featured Dr. Blatt highlighting the importance of continuing Dr. Lowns legacy of patient-centered care. Dr. Saini also reminded guests that their support furthers Foundation activities such as outcomes research and our upcoming conference on avoidable care.
Donor Prole
Carol and Norton Foxman have been Dr. Charles Blatts patients at the Lown Center for ten years, and donors to the Lown Foundation for nearly as long. We recently sat down for a conversation with the Foxmans about their involvement with the Foundation. How did you come to be patients at the Lown Center? Carol: My mother had heart disease. We knew people in our hometown who came here and said such wonderful things. Were very health-conscious, always looking for new ways to stay healthy, and we were interested in the preventive philosophy practiced by the Lown group. Norton: My father and brother both have atrial brillation. We were looking for a practice where the physicians care about the whole patient. Tell us about your support for the Foundation. Carol: We have supported a lot of organizations involved with cancer research, including two university chairs. We wanted to do something Norton and Carol Foxman similar for cardiology, especially because of the prevalence of heart disease. We honor our parents through giving. Norton: We were extremely impressed by Jack Bogles testimonial at the Lown gala in 2008. He spoke so movingly about his experiences with the care he received at the Lown Center, as did several others. What aspects of the Foundations work are you especially interested in? Norton: I am very interested in your outcomes research. I understand lots of people come to the Lown Center for second opinions, and that you have good results that you want to document. The planned conference on avoidable care next spring is also of great interest. What would you say to someone who was considering a donation to the Lown Foundation? Norton: Anyone who wants to support heart research will be making a good, charitable investment here.
New Bedford hosts, Ken and Gwen Sullivan
Dorothy and Alfred Costa, Edward and Jacquellen Sullivan
Lown gala
When: Spring 2012 Where: Mandarin Oriental Hotel What: For more information or to get involved with planning the gala, contact Andi Brown, Director of Development, at arbrown1@partners.org or 617-7321318, ext. 3350
Iris and Harold Katzman, Elia Giusti
LOW N
FO RUM On that particular visit to my oce, I reiterated that in time, burdening his cardiovascular system with excessive weight load is likely to inict serious damage to his heart and general well-being. He had to make a change! Dr. Ravids worried face burned into my mind that day. But he didnt resort to threats he spoke with an understanding that he could do only so much to stop my certain fall from the cli of a life well lived and enjoyed. I left the oce knowing I was sentenced to a self-imposed troubled future because I still ate like I was a teenager. With this new found determination, RJ started eating well and exercising. Just a month after adjusting my diet, I could walk without the shortness of breath that once terried me. After two months, the old belts and pants came out from the back of the closet. I could t into my old suits and dress shirts again. By the third month, the belly ab became a past memory. I looked ten years younger. The diet was simple unlimited fruits, salmon, plates of cherry tomatoes, and egg whites. The choice was easy. Thanks to those moments in the doctors oce, my life changed and I once again could breathe, smell the air, and feel proud of my decision to follow the best advice a doctor ever gave a patient. You can talk the talk, but you need motivation and commitment to stay the course and reap the fruits of your eorts.
QUESTION FROM A PATIENT
I know I need to lose weight, but sometimes it feels like a lost cause. How can I encourage myself to stick to a weight-loss routine?
Shmuel Ravid, MD, MPH
Being overweight is very common among patients with heart conditions. Losing weight is extremely benecial in improving cardiovascular health such as hypertension, diabetes, and heart failure. Nevertheless, we struggle to lose weight. So I was pleasantly surprised to see that my patient RJ recently lost 40 pounds after failing to do so for many years despite my urging. I asked him to describe what was dierent this time that inspired his resilient commitment and how he was able to achieve this tremendous accomplishment. My most recent visit to the Lown Center made me understand that I was trading years of health for the taste of pasta, pizza, Chinese food, bread, and the like, RJ explains. Every walk I took was an eort, every distance was the enemy I was headed upon a course that would injure my heart.
Finding solutions 7500 miles away
A Lown Scholars perspective on the cardiovascular disease epidemic in Tanzania
Dr. Njelekela & Lown physicians
The Lown Scholars program brings together health professionals from developing countries to the Harvard School of Public Health to learn cardiovascular disease prevention and conduct research relevant to their home country. As a Lown Scholar, Dr. Marina Njelekela has a unique perspective on the burden of cardiovascular disease in her home country, Tanzania, as well as how it can be prevented. Compared to the United States, the infrastructure to address cardiovascular disease in Tanzania is not well developed, explains Dr. Njelekela. In Tanzania people are rst diagnosed when they have a stroke they dont recognize their risk factors before they have a stroke and so the diagnosis comes too late and they have complications that are very dicult to manage.
By studying the relationship between cardiovascular disease and the types of food children eat, Dr. Njelekela found that it is not just health infrastructure that is causing problems. Were starting to see an increase in fast food restaurants, rened rice, vegetable oils all of which are foreign to the traditional Tanzanian diet People dont know what they should eat, how much physical activity they should do on a regular basis, or if they are at risk or already have a disease. However, Dr. Njelekela believes that successful prevention eorts to reduce cardiovascular disease are within reach. We can tie cardiovascular disease prevention with HIV/AIDS and use resources to address both. We need integrated clinics clinics that address both HIV/AIDS and cardiovascular disease. Currently, when someone goes to an HIV/AIDS clinic they may not get screened for cardiovascular risk factors. But even if they are living because of anti-retroviral treatment, they should not be dying from cardiovascular disease. Dr. Njelekela remains optimistic. I think the future will be brighter, but it will take time. It took seven years for the Tanzanian government to understand they need a strategy for noncommunicable diseases. But now we have a focus and funding for prevention.
LOW N
FO RUM
LOWN CARDIOVASCULAR CENTER
Thank you for your support
The Lown Cardiovascular Research Foundation promotes cardiac care that advocates prevention over costly, invasive treatments and restores the relationship between doctor and patient. Your financial support allows us to continue our work and carry our heart health message to local, national, and global audiences. We greatly appreciate any donation you are able to make. You can donate online at our website (www.lownfoundation.org) or mail your donation to 21 Longwood Avenue, Brookline, MA 02446. Please make checks payable to the Lown Cardiovascular Research Foundation. For more information about supporting the Foundation, please contact Andi Brown, Director of Development at arbrown1@partners.org or 617-732-1318 (x3350).
NewsBeat
The Lown Foundation welcomed two ProCor interns during the summer 2011. Heidi Chase studied art and social action at george Mason University and received a Masters in Public Interns, Heidi and Jocelyn Health from Boston University. She has worked as an educator, community artist, and public health consultant with programs designed to inuence behavior, initiate conversation, and promote change. Jocelyn Sterling is a graduate student in the Health Communication program at Emerson College. She cohosts and produces a health-focused program at Emersons talk radio station. Jocelyn previously worked as a marketing intern at Horizon West Healthcare in California. She has a Communication Studies and Journalism degree from the University of Portland. Dr. Tom Graboys was recently interviewed by Dr. Peter Rabins for the spring 2011 issue of the Johns Hopkins Bulletins: Memory Disorders. To read the interview please visit: www.tomgraboys.com. On June 4, 2011, Dr. Vikas Saini and Dr. Fred Mamuya spoke at the second annual health expo, VivaFest, in Hyannis, MA, on the topics of healthy aging and heart disease prevention and screening athletes for cardiac health. The event drew an estimated 1200 people and featured speaker workshops, an indoor farmers market, healthy lunch sampling, and yoga and taichi sessions. Dr. Bernard Lown was featured in the Spring/Summer 2011 Harvard Public Health Review. To read the article please visit: http://tiny.cc/83v90. Dr. Vikas Saini addressed the Belmont Council on Aging community on August 4, 2011. The topic of his talk was Second Opinions and Overtreatment. Dr. Sara Russell received the second annual Bernard Lown Award for Excellence in Teaching at Brigham and Womens Hospital. A graduate of Tufts and Columbia Universities, Dr. Russell is the Surgical Director of Cutaneous Oncology and Melanoma at the Dana Farber and is involved in various teaching and mentorship activities with third and fourth year medical students. On August 11, 2011, Dr. Vikas Saini was interviewed by Maryann Napoli, the Associate Director of the Center for Medical Consumers in New York City. Dr. Saini discussed his opinion of the new cholesterol-lowering drug, Lovaza. The interview can be found on the Center for Medical Consumers website: http://tiny.cc/w48kd
Educational opportunities
Interested in hosting a lecture on a heart health topic by one of our physicians at your worksite or community organization? Please contact us at info@lownfoundation.org or 617-732-1318 (x3355).
New patient appointments available
New patient appointments are currently available. If you would like to make an appointment with one of the Lown group cardiologists, please call 617-732-1318 and select option 1.
Board of Directors
Nassib Chamoun Chairman of the Board Vikas Saini, MD President Bernard Lown, MD Chairman Emeritus Thomas B. graboys, MD President Emeritus Patricia Aslanis Charles M. Blatt, MD Joseph Brain, SD Janet Johnson Bullard J. Breckenridge Eagle Carole Anne McLeod C. Bruce Metzler Barbara H. Roberts, MD Ronald Shaich Robert F. Weis
CONTACT US
Lown Cardiovascular Research Foundation
21 Longwood Avenue Brookline, MA 02446 USA (617) 732-1318 info@lownfoundation.org www.lownfoundation.org www.lowncenter.org www.procor.org
Lown Cardiovascular Group
Brian Z. Bilchik, MD Charles M. Blatt, MD Wilfred Mamuya, MD, PhD Shmuel Ravid, MD, MPH Vikas Saini, MD
Lown Forum Editorial Sta
Andi Brown Jessica gottsegen Benn grover Claudia Kenney Jocelyn Sterling
Advisory Board
Martha Crowninshield Herbert Engelhardt Edward Finkelstein William E. Ford Renee gelman, MD Barbara greenberg Milton Lown John R. Monsky Jerey I. Sussman David L. Weltman
2011 Lown Foundation Printed on recycled paper with soybased ink.
Lown Cardiovascular Research Foundation 21 Longwood Avenue Brookline, Massachusetts 02446-5239
Nonprofit Org. US Postage PAID Boston, MA Permit No. 53936
LOW N
FO RUM
I encourage you to introduce an exercise regimen to your daily activities starting modestly and progressively adding more exercise to your routine. For example, beginning with 10 minutes before breakfast and again before lunch allows you to initiate a routine in a painless fashion adding minutes to each series over time and eventually exercising for a goal of 30 minutes daily. Older people have plenty of age-appropriate exercises that can help them live healthier lives. The key is nding the exercise routine that ts you and then sticking to it.
Exercising as you grow older
Charles M. Blatt, MD
It is not uncommon to nd grandparents urging their grandchildren to break loose from their computers or video games. get outdoors and into the fresh air. Exercise, walk, cycle, jog, swim, throw a ball! Indeed, the importance of regular exercise on both ends of the age spectrum cannot be overstated. Fortunately, young people have many opportunities to engage in exercise at some point as they go through school. Older people may nd more impediments in the path to a routine and satisfying exercise. But as dicult as it may be to nd an acceptable routine, it is even more important to nd one that is easy to stick with and follow. As we age, we tend to live more sedentary lives - fewer trips up and down the stairs, fewer dashes out to see friends, walking instead of running, slower rather than faster in almost every realm of activity. This makes it more important to adopt a practical and easy-to-follow routine that ts your bodys limitations. For example, someone with a knee or hip problem cannot rely on walking outside or on a treadmill for exercise. Instead, try using a stationary bicycle or doing an aerobic stretching activity in a heated swimming pool. Many health clubs oer discounts for older members. Another example is to do arm and leg raising activities while sitting in a chair. Many of these exercises can be augmented by using one or two pound weights attached to the ankles or wrists. However, before starting an exercise regimen, you should consult with your doctor to make sure the routine is right for you.
Some exercise resources for older people
Signicant calories can be burned and substantial muscle and bone strengthening accomplished with simple, low cost routines followed daily at home. Here are a couple of examples: Livestrongs Exercise tips for senior citizens encourages people to consult a doctor rst, see a personal trainer, start slowly, get proper shoes, work out with friends, and stretch before exercising. For more information, visit http://tiny.cc/chwub. The National Institute on Aging details four dierent types of exercise that will provide maximum benet to you: endurance, strength, balance, and exibility. For more information, visit http://tiny.cc/hvdqg. Helpguides Senior Exercise and Fitness Tips debunks common myths about elderly exercise, explains the whole-body benets of exercise, and gives tips for starting safely, building exercise routines, and for wheel-chair bound individuals. For more information, visit http://tiny.cc/e0141.
You might also like
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5795)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- FOCUS PDCA Template DR ArjatyDocument119 pagesFOCUS PDCA Template DR ArjatyJose MillerNo ratings yet
- Acute PsychosisDocument8 pagesAcute PsychosisAnonymous EtiONEG7No ratings yet
- Useful Links For Patients and CaregiversDocument17 pagesUseful Links For Patients and CaregiversChip HuntNo ratings yet
- MCQ AnaesthesiaDocument15 pagesMCQ AnaesthesiaProf-Ashraf Emara100% (2)
- EpispadiasDocument9 pagesEpispadiassheranadhilaNo ratings yet
- Daily Newspaper - 2015 - 11 - 09 - 000000Document54 pagesDaily Newspaper - 2015 - 11 - 09 - 000000Anonymous QRT4uuQNo ratings yet
- CadDocument16 pagesCadrachel_galangNo ratings yet
- Fulminant Hepatic FailureDocument33 pagesFulminant Hepatic FailureRojan CardinalNo ratings yet
- Viva Questions AllDocument18 pagesViva Questions AllFiaz medicoNo ratings yet
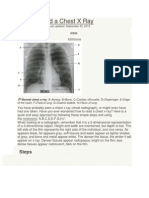
- How To Read A Chest X RayDocument20 pagesHow To Read A Chest X RayJasvin Sidhu100% (1)
- Development of EMG Sensor For Transfemoral Amputation (Knee Flexor and Knee Extensor)Document5 pagesDevelopment of EMG Sensor For Transfemoral Amputation (Knee Flexor and Knee Extensor)seventhsensegroupNo ratings yet
- ArticleDocument9 pagesArticlernvisNo ratings yet
- Instruction For Author ClimactericDocument9 pagesInstruction For Author ClimactericAndi BintangNo ratings yet
- An Approach To Fever Throught Boger BoenninghausenDocument10 pagesAn Approach To Fever Throught Boger BoenninghausenHomoeopathic Pulse100% (2)
- Antenatal SteroidsDocument30 pagesAntenatal Steroidskhadzx100% (2)
- Cardiac Monitoring PDFDocument7 pagesCardiac Monitoring PDFDelia LopNo ratings yet
- Antepartum Haemorrhage - Placenta Previa, Abruption 2Document78 pagesAntepartum Haemorrhage - Placenta Previa, Abruption 2Sivakumar Kathuu KarthikeyanNo ratings yet
- 13 Aseptic TechniqueDocument6 pages13 Aseptic TechniqueaironmaeNo ratings yet
- Cardiovascular Physiology Case 9Document50 pagesCardiovascular Physiology Case 9Kim AcostaNo ratings yet
- Neurological Physiotherapy AssessmentDocument7 pagesNeurological Physiotherapy Assessmentramesh babuNo ratings yet
- Preanalytical ErrorsSDocument4 pagesPreanalytical ErrorsSARIF AHAMMED P100% (1)
- Procedure Checklist With Rating Form Donning and Removing Sterile GlovesDocument4 pagesProcedure Checklist With Rating Form Donning and Removing Sterile GlovesRachel VillanuevaNo ratings yet
- Mechanics of Circular Breathing in Wind MusiciansDocument8 pagesMechanics of Circular Breathing in Wind MusiciansjwmmdNo ratings yet
- Drug ClassificationDocument18 pagesDrug ClassificationAlex CasillaNo ratings yet
- Agencies WebsitesDocument4 pagesAgencies WebsitesWWMTNo ratings yet
- Sample Policy: Reporting Test Results: Philosophy and PurposeDocument8 pagesSample Policy: Reporting Test Results: Philosophy and PurposeDarren CariñoNo ratings yet
- Gastritis PPTDocument86 pagesGastritis PPTWayan Hery75% (4)
- Protocol - Aminoglycoside DosingDocument5 pagesProtocol - Aminoglycoside DosingThomasNo ratings yet
- Rhino-FESS Carny Procedure-Guide en 42042Document64 pagesRhino-FESS Carny Procedure-Guide en 42042Rijal SaputroNo ratings yet
- Navodaya College of Nursing Raichur: Proforma For Registration of Subjects For DissertationDocument23 pagesNavodaya College of Nursing Raichur: Proforma For Registration of Subjects For Dissertationphibina2672No ratings yet