Professional Documents
Culture Documents
49 6 6
Uploaded by
Myrtle Setiawan0 ratings0% found this document useful (0 votes)
1 views7 pages49-6-6
Original Title
49-6-6
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document49-6-6
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
1 views7 pages49 6 6
Uploaded by
Myrtle Setiawan49-6-6
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 7
Paediatrica Indonesiana
VOLUME 49 NUMBER 6 November 2OO9
Original Article
342 Paediatr Indones, Vol. 49, No. 6, November 2009
Incidence and characteristics of antituberculosis drug-
induced hepatotoxicity in children: a preliminary study
Bina Akura, Hanifah Oswari, Bambang Supriyatno, Najib Advani
From the Department of Child Health, Medical School, University of
lndonesia, Cipto Man,unkusumo Hospital, Jakarta, lndonesia
Reprint request to: Bina Akura, MD, Department of Child Health,
Medical School, Universitv of lndonesia, Cipto Man,unkusumo Hospital,
Jl. Salemba 6, Jakarta 1O13O, lndonesia. 1el. 62-21-39O7712. lax. 62-21-
39O7713. l-mail: bnaakr72_vahoo.co.id
1
uberculosis (1B) is a disease known for
vears. New cases of 1B are increasin, and
most of them are in developing countries.
Demo,raphic data shows that tuberculosis in
children is 5 to 6' from total tuberculosis cases.
1
ln 19o9,
World Health r,anization (WH) predicted that everv
vear there were 1.3 thousand new cases of 1B in children
and 15O,OOO cases under 15 vears old died.
Antituberculosis dru,s such as rifampicin (RMP),
isoniazid (lNH), pvrazinamide (PzA), ethambutol
(lMB), and streptomvcin ,ive ,ood efficacv but also
many adverse effects.
1-2
Antituberculosis dru,-induced
hepatotoxicitv is one of the adverse effects which
causes increase of transaminases, bilirubin, icterus,
anorexia, nausea, and vomiting.
1-3
WH toxicitv
classification standards
4
categorize hepatotoxicity
into mild hepatotoxicity if aspartat aminotransferase
(AS1) and/or alanin aminotransferase (Al1) increase
3 to 5 times from upper normal limits (121-2OO U/l),
moderate hepatotoxicitv if transaminases increase 5
to 1O times from upper normal limits (2O1-1OO U/l),
severe hepatotoxicity if transaminases increase to
>1O times from upper normal limits (>1OO U/l).
Abstract
Background Antituberculosis dru,s show ,ood efficacv but have
adverse effects including hepatotoxicity.
Objective 1o find the incidence and characteristics of
antituberculosis hepatotoxicitv in children durin, the first 2
weeks of therapv.
Methods A cohort studv was performed in Cipto Man,unkusumo,
Persahabatan, and 1an,eran, Hospitals from Au,ust 2OOo
toMarch 2OO9. 1he dia,nosis of tuberculosis (1B) based on
1B scorin, svstem. laboratorv tests were performed includin,
transaminase enzymes, bilirubin, G-O1, albumin, ureum, and
creatinine before and after 2 weeks of treatment. Patients were
monitored durin, the first 2 weeks of therapv. lnformed consent
obtained from the parents.
Results Six of o1 subjects had hepatotoxicitv reaction. Most of
the patients were 1 to 5 vears old (65') and well nourished (5O').
lxtrapulmonarv tuberculosis found in 67' of cases. 1hirtv-three
percents of patients received four a,ents. 1hirtv-three percents of
cases received 1 a,ents combined with other hepatotoxic dru,s.
Six subjects had hepatotoxicitv (1 hepatitis, 2 mixed case, and
3 asvmptomatic). 1wo of 5O children (1') with pulmonarv 1B
and 1 out of 31 (13') children with extrapulmonarv 1B had
hepatotoxicitv reaction. Antituberculosis dru, doses were similar
between the hepatotoxicitv ,roup and control.
Conclusions lncidence of antituberculosis hepatotoxicitv in the
first 2 weeks of therapv was 7', consisted of hepatitis (1 cases),
mixed (2 cases), and asvmptomatic (3 cases). 1here was no
difference in sex as well as in nutritional state distribution found in
cases with hepatotoxicitv. [Paediatr Indones. 2009;49:342-8].
Keyword: antituberculosis, hepatotoxicity, incidence,
characteristics
Bina Akura et al : Antituberculosis dru,s induced-hepatotoxicitv in children
Paediatr Indones, Vol. 49, No. 6, November 2009 343
Studv in Japan showed transient elevation of
hepatocellular enzvmes in 1O' subjects with isoniazid
and rifampicin and in 1 to 2 ' subjects had to be
stopped due to fulminant hepatitis.
5
Hepatotoxicity
usually occurs in the first month of therapy and mostly
happens in the first 2 weeks.
6,7
Concomitant therapy
with isoniazid and rifampicin can cause hepatotoxicitv
in less than 1O dav.
8
Chang et al
9
found that
antituberculosis dru,-induced hepatitis occured in O.3
to 11.1 weeks mostlv in 1.1 weeks. Mahmood K et al
1O
found 19.76' hepatotoxicitv due to antituberculosis.
Most of the subjects (61') suffered from hepatotoxiciv
in 2 weeks after startin, therapv with mild and
moderate transaminases elevation. Schaberg et al
11
found that median interval of hepatotoxicitv between
antituberculosis dru,s was not different, isoniazid was
16.5 (95' Cl 7 to 17) davs, rifampicin is 17.5 (95'
Cl 11 to 33) davs, and pvrazinamide was 1o.5 (95'
Cl 17 to 29) davs.
Many studies investigated clinical parameters
associated with susceptibilitv to hepatotoxicitv due to
antituberculosis drugs, but mainly in adult subjects.
1-
5,12-1o
ln contrast, little is known about the risk factors
of hepatotoxicity due to antituberculosis therapy
in children.
5
1herefore it is a necessicitv to identifv
incidence and characteristics of hepatotoxicity during
antituberculosis therapv in children. 1his studv
intended to find the incidence and characteristics
of antituberculosis dru, induced-hepatotoxicitv in
children.
Methods
1his was a cohort studv carried out in Cipto
Man,unkusumo, Persahabatan and 1an,eran,
Hospitals from Au,ust 2OOo to March 2OO9. 1he
dia,nosis of 1B based on 1B scorin, svstem. Sample
size was calculated usin, the formula for estimatin,
sin,le population proportion19 with A~O.O5,
estimated prevalence of 3O', and accuracv of 1O'
revealing minimum sample size of 89 children.
Subjects were selected from outpatient clinic and in-
patient ward with inclusions criteria: a,e from O to 1o
vear old, dia,nosed 1B and received antituberculosis
dru,s. Children with chronic liver diseases, kidnev
diseases, chronic diarrhea, gastritis, metabolic diseases,
HlV infection, historv of familial liver diseases, low
adherence to antituberculosis drugs therapy and
disapproval of studv were excluded.
Laboratory tests performed before and after
2 weeks of treatment to measure transaminase
enzvmes (AS1, Al1), bilirubin, G-O1 (,amma-
,lutamvl transferase), albumin, ureum, and creatinin.
Patients were monitored durin, the first 2 weeks
of therapv. Patients were classified into those who
received 3 antituberculosis agents consisted of
isoniazid, rifampicin, and pyrazinamide and those
who received 1 antituberculosis a,ents consisted of
isoniazid, rifampicin, pvrazinamide and ethambutol/
streptomycin.
Hepatotoxicitv was cate,orized into asvmptomatic,
hepatitis, cholestasis or mixed case (hepatitis-
cholestasis).
2O
Hepatitis was defined if there was
transaminases elevation ~ 5 times upper normal limit
or ~ 3 times upper normal limit with svmptoms of
icteric, anorexia, nausea, vomiting, fever, abdominal
pain and hepatomegaly.
1,1
Cholestasis was defined if
there was direct bilirubin elevation > 1 m,/dl for total
bilirubin < 5 m,/dl or if total bilirubin > 5 m,/dl,
direct bilirubin was > 2O' of total bilirubin.21 Mixed
case was defined if the patient had svmptoms and si,ns
of hepatitis and cholestasis.
4
Asvmptomatic case was
defined if the patient had transaminases elevation ~ 3
and < 5 times upper normal limit without svmptoms.
4
lnformed consent was obtained from the parents. 1he
studv was approved bv the lthical Committee, lacultv
of Medicine, Universitv of lndonesia. Studv results
were processed usin, the SPSS version 15 pro,ram and
presented in textual and tabular forms.
Results
Durin, the studv period there were o9 subjects
collected. 1hree subjects did not fulfill the inclusion
criteria. ne patient died durin, two weeks therapv
due to tuberculous menin,itis. lour subjects were
excluded due to poor adherence to antituberculosis
therapv. At the end of the studv period, onlv o1
subjects could be analyzed. Most of the subjects
had pulmonarv 1B (62') and 3o' subjects had
extrapulmonarv 1B. liftv-four percents subjects with
pulmonarv 1B were female, but male dominated in
extrapulmonarv 1B cases with comparison of male :
female was 2:1. Most of the subjects (55') were 5 to
Bina Akura et al : Antituberculosis dru,s induced-hepatotoxicitv in children
344 Paediatr Indones, Vol. 49, No. 6, November 2009
1o vear old and 59' were malnourished. Most of the
subjects (33') were Sundanese, 2O' Javanese, and
the others (Batak, Betawi, other ethnic) were in small
proportion. Majoritv of the subjects (77') came from
a low social economic status. (Table 1)
1here were six from o1 subjects who suffered
from hepatotoxocitv, with equal number of male and
female patients. 1here were 1/6 patients a,ed 1-5 vears
and 3/6 patients had ,ood nutritional status (Table 2).
Clinical characteristics of these subjects in two weeks
of monitoring are presented in Table 3.
Amon, the pulmonarv 1B subjects, there were
1 mixed case and 1 asvmptomatic case, while amon,
the extrapulmonarv 1B subjects there were 1 hepatitis,
1 mixed case, and 2 asvmptomatic cases. 1here were
2 of 5O subjects (1') with pulmonarv 1B and 1
of 31 subjects (13')with extrapulmonarv 1B had
hepatotoxicitv. (1able 1) 1here was no difference in
the antituberculosis dru, dose between subjects with
hepatotoxicitv and those without. (Table 5)
No difference was found in sex nor in nutritional
status distribution in subjects with hepatotoxicitv
but in those without hepatotoxicitv male (52') and
malnourished (67') were predominant. Both subjects
with and without hepatotoxicitv had normal albumin
level (67' vs o1'). Most of hepatotoxicitv subjects
(1/6) had extrapulmonarv 1B and 61' subjects without
hepatotoxicitv had pulmonarv 1B. (Table 6)
Table 2. Demographic characteristics in subjects with hepatotoxicity
(n=6)
Characteristics Hepatotoxicity
n
Sex
Male
Female
Age
<1 years
1-5 years
5-18 years
Nutritional status
Overweight
Good
Mild
Severe
3
3
1
4
1
0
3
1
2
Table 3. Clinical characteristics of patient with hepatotoxicity
Age Sex Symptoms Disease extent Therapy
Concomitant
hep drugs
Hepatotoxicity
3 yr
2 yr
2 yr
4 yr
7 yr
10 mth
M
M
F
M
F
F
Fever, vomiting, nausea,
malaise
Anorexia, nausea,
vomiting
Fever, malaise, anoreksia,
icteric, hepatomegaly
No symptoms
No symptoms
No symptoms
Meningeal TB
Spondilitis TB
Pulm TB
Meningeal TB
Coxitis TB
Pulm TB
4 drugs
4 drugs
3 drugs
4 drugs
4 drugs
3 drugs
Phenytoin
Cotrimoxazole,
paracetamol
-
-
-
Paracetamol
Hepatitis
Mixed
Mixed
Asymptomatic
Asymptomatic
Asymptomatic
M= male, F= female, extra TB = extrapulmonary TB, Pulm TB= Pulmonary TB, yr= years, mth= month, d= days, hep drugs= others
hepatotoxicity drugs
Table 1. Demographic characteristics of subjects (n=81)
Characteristics
Pulmonary Extrapulmonary
Total (%)
n (%) n
Number
Sex
Male
Female
Age (years)
<1
1-5
5-18
Nutritional status
Severe
Mild
Good
Overweight
Ethnic/Race
Sundanese
Javanese
Betawi
Batak
Others**
Mixed***
Social-economic
Low
Middle
High
50
23
27
6
17
27
4
35
10
1
15
10
8
6
4
7
35
15
0
(62)
(46)
(54)
(12)
(34)
(54)
(8)
(70)
(20)
(2)
(30)
(20)
(16)
(12)
(8)
(14)
(70)
(30)
31
19
12
1
12
18
1
13
16
1
12
6
4
1
5
3
27
4
0
81
42
39
7
29
45
5
48
26
2
27
16
12
7
9
10
62
19
0
(100)
(52)
(48)
(9)
(36)
(55)
(6)
(59)
(32)
(3)
(33)
(20)
(15)
(9)
(11)
(12)
(77)
(23)
**Others = Bangka, Dayak, Madura, Menado, Melayu, Minahasa,
Padang, Palembang. ***Mixed = Batak-Makasar, Betawi-Javanese,
Betawi-Sundanese, Cirebon-Betawi, Javanese-Batak, Javanese-
Betawi, Javanese-Palembang, Javanese-Sundanese, Sundanese-
Flores
Bina Akura et al : Antituberculosis dru,s induced-hepatotoxicitv in children
Paediatr Indones, Vol. 49, No. 6, November 2009 345
Discussion
1his was a preliminarv studv usin, cohort desi,n due
to ethical reason for not giving antituberculosis drug
in normal children. limitation of this studv was no
statistical analysis performed due to small subjects
with hepatotoxicitv. 1his studv could not show which
antituberculosis agents as the cause of hepatotoxicity
because durin, the first 2 weeks of therapv, all subjects
received 3 or 4 drugs.
Most of the subjects were male (52') with a,e
ran,e of 5-1o vears (55'). Re,ardin, sex distribution,
1sa,aropoulou-Stin,a et al
22
and hkawa et al.
5
found
that hepatotoxicitv incidence was not correlated with
sex.
ln this studv, most of the subjects with hepato-
toxicitv was 1 to 5 vear old (67'). hkawa et al
5
found
that all children with hepatotoxicitv was under 5 vears
(mean a,e 2.31.5 vear old) and predominantlv male
(oo') compared to control onlv 15 ' male. 'Brien
et al
23
found that most of the subjects were from 1
to 1 vears (19'). 1sa,aropoulou-Stin,a et al
22
found
mean a,e of subjects was 1.5 vears (1 months-11
vears). Risk of complication increases in voun,er a,e
(O to 1 vears old).
21
Most of our subjects were malnourished (59').
Decrease of bodv wei,ht mav be due to 1B infection.
ln this studv, ethnicitv of the subjects consisted of
Sundanese, Javanese, Batak, Betawi and others.
'Brien et al
23
found 1B infection in 1o' black
race and 1O' white race. Most of our subjects came
from low social economic status, where 1B was still
endemic.
Most of our subjects with hepatotoxicitv had
,ood nutritional status (5O'). Studv of Mahmood et
al
1O
found that most of the subjects with hepatotoxicitv
was malnourished (91'), lernandez-Villar et al
4
found
2o.6' malnourished children with hepatotoxicitv, but
hkawa et al
5
did not find malnourished subjects with
hepatotoxicitv. 1his condition mavbe due to difference
in population study.
ln this studv, there were 6 of o1 patients with
hepatotoxicitv, consisted of 3 asvmptomatic, 1
Table 6. Charateristics subjects with and without hepatotoxicity
Variable With
hepatotoxicity
n=6
Without
hepatotoxicity
n=75 (%)
Sex
Male
Female
Age (years)
0-5
5-18
Nutritional status
Malnourished
Good
Albumin level
Low
Normal
Diseases extent
Extrapulmonary TB
Pulmonary TB
Therapy
3 drugs
4 drugs
3 drugs + OH
4 drugs +OH
3
3
5
1
3
3
2
4
4
2
1
2
1
2
39 (52)
36 (48)
31 (41)
44 (59)
50 (67)
25 (33)
12 (16)
63 (84)
27 (36)
48 (64)
39 (52)
18 (24)
11 (15)
7 (9)
OH= other hepatotoxic drugs
Table 5. Mean dose of antituberculous agents among subjects
with hepatotoxicity and without hepatotoxicity
Agents
With hepatotoxicity
(mg/kg/day) *
Without hepatotoxicity
(mg/kg/day) *
INH
RMP
PZA
EMB
9.07 (2.2)
13.85 (2.7)
23.97 (4.1)
19.42 (3.8)
8.08 (2.2)
13.33 (6.9)
23.26 (7.2)
18.51 (5.6)
INH= isoniazid, RMP= rifampicin, PZA= pyrazinamide,
EMB= ethambutol
* Mean (SD)
Table 4. Mean titer of transaminase, bilirubin, and G-GT in subjects with hepatotoxicity and without
hepatotoxicity
With hepatotoxicity* Without hepatotoxicity*
Before Week II Before Week II
SGOT/AST (U/L)
SGPT/ALT (U/L)
Total bilirubin (mg/dL)
Direct bilirubin (mg/dL)
Indirect bilirubin (mg/dL)
63.33 (29.1)
40.33 (13.8)
0.55 (0.3)
0.30 (0.2)
0.25 (0.2)
220.16 (88.1)
220.66 (100.3)
2.36 (0.3)
1.36 (2.2)
0.99 (1.4)
52.10 (57.1)
33.10 (32.5)
0.49 (0.3)
0.19 (0.2)
0.30 (0.2)
41.20 (19.4)
28.89 (19.1)
0.47 (0.2)
0.20 (0.2)
0.26 (0.1)
* Mean (SD)
Bina Akura et al : Antituberculosis dru,s induced-hepatotoxicitv in children
346 Paediatr Indones, Vol. 49, No. 6, November 2009
hepatitis and 2 mixed cases. hkawa et al
5
found
that o of 99 children with 1B had hepatotoxicitv.
'Brien et al
23
found 16 cases with hepatotoxicitv of
o71 children with 1B. 1sa,aropoulou-Stin,a et al
22
found hepatotoxicitv in 36 from 11 children with 1B
and 15 of them had hepatitis. 1his studv was different
from 1sa,aropoulou-Stin,a due to different dru, dose
,iven to the subjects. 1he dose ,iven in the previous
studv was 15-2O m,/k,/dav for isoniazid and 15 m,/
k,/dav for rifampicin. Ramachandran et al
25
found
incidence of hepatitis in 5O' patients with isoniazid
dose 2O m,/k,/dav and 2O' cases with isoniazid dose
of 12 m,/k,/dav. Palusci et al
26
found hepatitis in 3.5'
children given isoniazid. Meta analysis by Steele et
al
27
showed that hepatitis was found in 6.9' children
given isoniazid and rifampicin.
Svmptoms in subjects with hepatotoxicitv were
fever, malaise, anorexia, nausea, vomiting, icterus, and
hepatomegaly. Shakya et al
2
also found similar results.
Black et al
11
found gastrointestinal manifestation
in 55' cases and viral infection svndrome in 35'
cases.
ln this studv, most of the subjects with hepato-
toxicitv was under 5 vear old (o3') and 5 to 1o vear
old (17'). Meanwhile, most of the subjects without
hepatotoxicitv was from 5 to 1o vear old (59'). A
studv in Japan showed that o' of hepatotoxicitv
was under 5 vear old.
5
Logistic regression analysis
showed that a,e and pvrazinamide were si,nificantlv
related to the risk of severe hepatotoxicitv (P<O.O5).
1sa,aropoulou-Stin,a et al
22
also found mean age of
hepatitis after antituberculosis therapv was 1.5 vears
old (1O'). 'Brien et al
23
did not find any correlation
between a,e and hepatotoxicitv.
Albumin level was normal in 67' subjects
with hepatotoxicitv and o1' subjects without
hepatotoxicitv. hkawa et al
5
found albumin levels
were normal in control subjects (1.1O.3 ,/dl) and
subjects without hepatotoxicitv (1.3O.1 ,/dl).
Mahmood et al
1O
found that 27.1' patients with
hepatotoxicitv had albumin <3.5 ,/dl. Patients
with hvpoalbuminemia had two times hi,her risks
of havin, hepatotoxicitv. ln malnutrition, ,lutation
store is depleted causing someone more vulnerable
of having hepatotoxicity. Malnourished subjects also
have slower dru, metabolisms.
2
ln this studv, most of the subjects with
hepatotoxicitv had extrapulmonarv 1B (67'),
contrarv to subjects without hepatotoxicitv.
hkawa et al
5
found that 1 of o patients with
hepatotoxicitv had extrapulmonarv 1B and showed
si,nificant relation (P<O.O5). Shakva et al
2
found
that the severitv of the disease was the risk factor
of havin, hepatotoxicitv. 'Brien et al
23
found that
extrapulmonarv 1B (milliarv 1B and menin,itis
1B) had risk of havin, hepatotoxicitv 3 times
hi,her than pulmonarv diseases (6.9' vs 1.9').
Rahajoe et al
2o
found hepatitis in 6 of 22 (27.3')
subjects of menin,itis 1B who received isoniazid,
rifampicin, and streptomvcin. ln severe 1B cases,
there are micro lesions of tubercle in the liver. Liver
damage in this case may be due to the tuberculin
effect or tubercle product that is release in the liver
after antituberculosis therapy. Hepatotoxicity in
subjects with extrapulmonarv 1B mavbe due to other
concomitant hepatotoxic drugs.
29
ln this studv, most of our subjects with
hepatotoxicity received 4 antituberculosis drugs
(33') and 1 antituberculosis dru,s with other
concomitant hepatotoxic dru,s (33'). Subjects
without hepato toxi citv received 3 antituberculosis
dru,s (52'). Steele et al
27
found that incidence of
hepatitis was 6.9' in children receivin, isoniazid
and rifampicin and 1.O' in 177 children receivin,
multiple isoniazid a,ents without rifampicin.
Schaberg et al
11
found that other concomitant
hepatotoxic dru,s was not correlated si,nificantlv
with severe adverse effect includin, hepatotoxicitv
from standard antituberculosis therapv (P~O.oO,
R: 1.1, 95' Cl O.1 to 2.o). ln this studv, the cause
of hepatotoxicitv could not be determined whether
due to antituberculosis agents or other concomitant
hepatotoxic dru,s. 1his was due to the small number
of subjects receiving other concomitant hepatotoxic
drugs, therefore statistical analysis could not be
performed. Other concomitant hepatotoxic drugs
that were ,iven to the subjects with hepatotoxicitv
were acetaminophen, phenvtoin, and cotrimoxazole.
Acetaminophen can cause hepatocellular damage,
while phenvtoin and cotrimoxazole can cause mixed
case.
ln conclusion we found that the incidence of
antituberculosis hepatotoxicitv in the first 2 weeks
of therapv was 7.1'. No difference in sex as well as
in nutritional status distribution found in cases with
hepatotoxicity.
Bina Akura et al : Antituberculosis dru,s induced-hepatotoxicitv in children
Paediatr Indones, Vol. 49, No. 6, November 2009 347
References
1. Rahajoe NN, Basir DR, Makmuri, Kartasasmita CB. Pedoman
nasional tuberkulosis anak. 2nd ed. Jakarta: UKK Respirolo,i
PP lDAl, 2OO7, p.3-7, 17-59.
2. Shakva R, Rao BS, Shrestha B. lncidence of hepatotoxicitv
due to antitubercular medicines and assessment of risk
factors. Ann Pharmacother. 2OO1,3o:1O71-9.
3. Navarro VJ, Senior JR. Dru,-related hepatotoxicitv. N ln,l
J Med. 2OO6,351:731-9.
1. lernandez-Villar A, Sopena B, lernandez-Villar J, Vazquez-
Oallardo R, Ulloa l, leiro V, et al. 1he influence of risk
factors on the severitv of anti-tuberculosis dru,-induced
hepatotoxicitv. lnt J 1uberc lun, Dis. 2OO1,o:1199-
15O5.
5. hkawa K, Hashi,uchi M, hno K, Kiuchi C, 1akahashi
S, Kondo S, et al. Risk factors for antituberculosis
chemotherapv-induced hepatotoxicitv in Japanese pediatric
subjects. Clin Pharmacol 1her. 2OO2,72:22O-6.
6. Corrigan D, Paton J. Hepatic enzyme abnormalities in
children on triple therapy for tuberculosis. Pediatr Pulmonol.
1999,27:37-12.
7. Durand l, Jebrak O, Pessavre D, lournier M, Bernuau J.
Hepatotoxicity of antitubercular treatments: rationale for
monitorin, liver status. Dru, Saf. 1996,15:391-1O5.
o. 1hompson NP, Caplin Ml, Hamilton Ml, Oillespie SH,
Clarke SW, Burrou,hs AK, et al. Antituberculosis medication
and the liver: dangers and recommendations in management.
lur Respir J. 1995,o:13o1-o.
9. Chan, KC, leun, CC, Yew WW, 1am CM. Standard
anti-tuberculosis treatment and hepatotoxicitv: do dosin,
schedules matter' lur Respir J. 2OO7,29:317-51.
1O. Mahmood K, Hussain A, Jairamani Kl, 1alib A, Abbasi B,
Salkeen S. Hepatotoxicitv with antituberculosis dru,s: the
risks factors. Pak J Med Sci. 2OO7,23:33-o.
11. Schaber, 1, Rebhan K, lode H. Risk factors for side-effects of
isoniazid, rifampin and pyrazinamide in subjects hospitalized
for pulmonarv tuberculosis. lur Respir J. 1996,9:2O26-3O.
12. Un,o JR, Jones D, Ashkin D, Hollender lS, Bernstein
D, Albanese AP, et al. Antituberculosis dru,-induced
hepatotoxicitv. Am J Respir Crit Care Med. 199o, 157:
1o71-6.
13. Dossin,, Wilcke J1, Ask,aard DS, Nvbo B. liver injurv durin,
antituberculosis treatment: an 11-vear studv. |Abstract].
1uber lun, Dis. 1996,77:335-1O.
11. Black M, Mitchell JR, zimmerman HJ, lshak KO, lpler OR.
lsoniazid-associated hepatitis in 111 patients. |Abstract].
Oastroenterol. 1975,69:2o9-3O2.
15. Pande JN, Sin,h SP, Khilnani OC, Khilnani S, 1andon RK.
Risks factors for hepatotoxicity from antituberculosis drugs:
a case-control studv. 1horax. 1996,51:132-6.
16. Sin,h J, Arora A, Oar, PK, 1hakur VS, Pande JN, 1andon
RK. Antituberculosis treatment-induced hepatotoxicitv: role
of predictive factors. J Post,rad Med. 1995,71:359-62.
17. Smink l, Hoek v, Rin,ers J, Altena RV, Arend SM. Risk
factors of acute hepatic failure during antituberculosis
treatment: two cases and literature reviews. Neth J Med.
2OO6,61: 377-o1.
1o. Hwan, SJ, Wu JC, lee CN, Yen lS, lu Cl, lin 1P, et
al. A prospective clinical studv of isoniazid-rifampisin-
pvrazinamide-induced liver injurv in area endemic for
hepatitis B. |Abstract]. J Oastroenterol Hepatol. 1997,12:o7-
91.
19. Madivono B, Moeslichan S, Sastroasmoro S, Budiman l,
Purwanto SH. Perkiraan besar sampel. ln: Sastroasmoro S,
lsmael S, editors. Dasar - dasar metodolo,i penelitian. 2
nd
ed. Jakarta: Sa,un, Seto, 2OO2, p. 259-2o6.
2O. swari H. Penvakit hati akibat obat (PHA) pada anak.
Proceedin, of 2
nd
Pediatric Gastroenterology National
Con,ress, 2OO3 Julv 3-5, Bandun,.
21. swari H. Kolestasis: atresia bilier dan sindrom hepatitis
neonatal. ln: Hadine,oro SR, Prawitasari 1, lndvarni B,
Kadim M, Sjakti HA, editors. Dia,nosis dan tata laksana
penyakit anak dengan gejala kuning. Proceeding of
Continuing Medical Education, Department of Child Health,
Universitv of lndonesia, 2OO7 Nov 12-13, Jakarta. Jakarta:
Department of Child Health, Universitv of lndonesia, 2OO7,
p. 12-51.
22. 1sa,aropoulou-stin,a H, Mataki-emmanouilidou 1, Karida-
kavalioti S, Manios S. Hepatotoxic reactions in children with
severe tuberculosis treated with isoniazid-rifampin. Pediatr
lnfect Dis. 19o5,1:27O-3.
23. 'Brien RJ, lon, MW, Cross lS, lvle MA, Snider Dl.
Hepatotoxicity from isoniazid and rifampin among children
treated for tuberculosis. Pediatrics. 19o3,72:191-9.
21. World Health r,anization. Ouidance for national
tuberculosis programmes on the management of tuberculosis
in children |homepa,e on internet]. c2OO6. Available from:
http://www.who.int/child_adolescent_health/documents/
htm_tb_2OO6_371/en/index.html
25. Ramachandran P. Chemotherapv of tuberculosis menin,itis
with isoniazid plus rifampicin-interim findin,s in a trial in
children. lndian J 1uberc. 1979,27:51-7.
26. Palusci VJ, 'Hare D, lawrence RM. Hepatotoxicitv and
transaminase measurement during isoniazid chemoprophilaxis
in children. Pediatr lnfect Dis J. 1995,11:111-o.
Bina Akura et al : Antituberculosis dru,s induced-hepatotoxicitv in children
348 Paediatr Indones, Vol. 49, No. 6, November 2009
27. Steele MA, Burk Rl, DesPrez RM. 1oxic hepatitis with isoniazid
and rifampin: a meta-analvsis. Chest. 1991,99:165-71.
2o. Rahajoe NN, Rahajoe N, Boediman l, Said M, lazuardi S.
1he treatment of tuberculous menin,itis in children with
a combination of isoniazid, rifampisin and streptomvcin-
preliminarv report. 1ubercle. 1979,6O:215-5O.
29. 1eleman MD, Chee CBl, larnest A, Wan, Y1. Hepatotoxicitv
of tuberculosis chemotherapy under general programme
conditions in Sin,apore. lnt J 1uberc lun, Dis. 2OO2,o:699-
7O5.
You might also like
- Divya Thesis Final (30th Jan)Document26 pagesDivya Thesis Final (30th Jan)smalaparaNo ratings yet
- RajaniDocument8 pagesRajaniArnette Castro de GuzmanNo ratings yet
- TB AnakDocument6 pagesTB AnakHerlin Ajeng NurrahmaNo ratings yet
- Typhoid Fever With Acute Pancreatitis in A Five-Year-Old ChildDocument2 pagesTyphoid Fever With Acute Pancreatitis in A Five-Year-Old Childnurma alkindiNo ratings yet
- Pulmonary Tuberculosis Remains an Important Complication in Nephrotic ChildrenDocument5 pagesPulmonary Tuberculosis Remains an Important Complication in Nephrotic ChildrenMaghfirah RahimaNo ratings yet
- Ileal-lymphoid-nodular hyperplasia, non-specific colitis, and pervasive developmental disorder in childrenDocument11 pagesIleal-lymphoid-nodular hyperplasia, non-specific colitis, and pervasive developmental disorder in childrenEmmanuelLeidiNo ratings yet
- A Retrospective Study of Korean Adults With Food Allergy: Differences in Phenotypes and CausesDocument6 pagesA Retrospective Study of Korean Adults With Food Allergy: Differences in Phenotypes and CausesAngga Aryo LukmantoNo ratings yet
- Infection and Immunoglobulin Levels in Sudanese Children With Severe Protein-Energy MalnutritionDocument11 pagesInfection and Immunoglobulin Levels in Sudanese Children With Severe Protein-Energy MalnutritionNurfadhilahNo ratings yet
- Oral Esomeprazole in Japanese Pediatric Patients With Gastric Acid-Related Disease: Safety, Efficacy, and PharmacokineticsDocument9 pagesOral Esomeprazole in Japanese Pediatric Patients With Gastric Acid-Related Disease: Safety, Efficacy, and Pharmacokineticsdesak indryNo ratings yet
- Pulmonary Tuberculosis As A Differential Diagnosis of PneumoniaDocument18 pagesPulmonary Tuberculosis As A Differential Diagnosis of PneumoniaKadek AyuNo ratings yet
- A New Approach To The Prophylaxis of Cyclic Vomiting TopiramateDocument5 pagesA New Approach To The Prophylaxis of Cyclic Vomiting TopiramateVianNo ratings yet
- Dyspepsia Journal PediatricDocument11 pagesDyspepsia Journal PediatricFatt ZakiNo ratings yet
- FK concetration is increase in children with celic d....Document6 pagesFK concetration is increase in children with celic d....Nejc KovačNo ratings yet
- 5 SudharshanDocument5 pages5 SudharshaneditorijmrhsNo ratings yet
- The Safety of Acetaminophen and Ibuprofen Among Children Younger Than Two Years OldDocument7 pagesThe Safety of Acetaminophen and Ibuprofen Among Children Younger Than Two Years OldsastiraNo ratings yet
- Changes in Fecal Microbiota and Metabolomics in A Child With JIA Responding To Two Treatment Periods With Exclusive Enteral NutritionDocument6 pagesChanges in Fecal Microbiota and Metabolomics in A Child With JIA Responding To Two Treatment Periods With Exclusive Enteral Nutritiondoc0814No ratings yet
- Jurnal Anak TBDocument8 pagesJurnal Anak TBGintar Isnu WardoyoNo ratings yet
- 611-Main Article Text (Blinded Article File) - 1200-1!10!20171212Document4 pages611-Main Article Text (Blinded Article File) - 1200-1!10!20171212Ramot Tribaya Recardo PardedeNo ratings yet
- Circulating Interleukin-6 and Tumor Necrosis Factor Receptor-1 Predict Resistance To Therapy of Typhoidal SalmonellosisDocument5 pagesCirculating Interleukin-6 and Tumor Necrosis Factor Receptor-1 Predict Resistance To Therapy of Typhoidal SalmonellosisAndri YansyahNo ratings yet
- 282 F 4 e 2 Edaf 124 A 0Document12 pages282 F 4 e 2 Edaf 124 A 0Mazin AlmaziniNo ratings yet
- Oka 5Document4 pagesOka 5Nina lucia Paulino AngelesNo ratings yet
- Single Dose of Fosfomycin Trometamol Versus Five Days Norfloxacin in The Treatment of Lower Uncomplicated Urinary Tract InfectionsDocument5 pagesSingle Dose of Fosfomycin Trometamol Versus Five Days Norfloxacin in The Treatment of Lower Uncomplicated Urinary Tract InfectionsIOSRjournalNo ratings yet
- Primary Care Autism Prevention Through Environmental AwarenessDocument11 pagesPrimary Care Autism Prevention Through Environmental AwarenessratzzuscaNo ratings yet
- International Reports: Incidence of Hepatotoxicity Due To Antitubercular Medicines and Assessment of Risk FactorsDocument6 pagesInternational Reports: Incidence of Hepatotoxicity Due To Antitubercular Medicines and Assessment of Risk FactorsWelki VernandoNo ratings yet
- PK of anti-TB drugs in Malawian children reconsidering role of ethambutolDocument6 pagesPK of anti-TB drugs in Malawian children reconsidering role of ethambutolIsmi Azisa Chaeria SaputriNo ratings yet
- Infection Status of Hospitalized Diarrheal Patients With Gastrointestinal Protozoa, Bacteria, and Viruses in The Republic of KoreaDocument9 pagesInfection Status of Hospitalized Diarrheal Patients With Gastrointestinal Protozoa, Bacteria, and Viruses in The Republic of KoreaMelia Kusuma WardaniNo ratings yet
- Controlled Trial Lansoprazole For Children With Poorly Controlled Asthma: A RandomizedDocument4 pagesControlled Trial Lansoprazole For Children With Poorly Controlled Asthma: A RandomizedJames HollandNo ratings yet
- Cefoperazone Sulbactam en RNDocument4 pagesCefoperazone Sulbactam en RNchieneralbaNo ratings yet
- Comparison of Two Different Antibiotic Regimens For The Prophylaxisis of Cases With Preterm Premature Rupture of Membranes: A Randomized Clinical TrialDocument5 pagesComparison of Two Different Antibiotic Regimens For The Prophylaxisis of Cases With Preterm Premature Rupture of Membranes: A Randomized Clinical TrialVindee VictoryNo ratings yet
- Etm 05 04 1129Document4 pagesEtm 05 04 1129Muhammad Rizky Anugrah PratamaNo ratings yet
- Probiotics in The Prevention of Eczema A Randomised Controlled Trial 2014 Archives of Disease in ChildhoodDocument7 pagesProbiotics in The Prevention of Eczema A Randomised Controlled Trial 2014 Archives of Disease in ChildhoodThiago TartariNo ratings yet
- Platelet Activating FactorDocument8 pagesPlatelet Activating FactorayesayeziaNo ratings yet
- Stuppy 2010 Blastocystis in Ibs Eradication With NitazoxanideDocument1 pageStuppy 2010 Blastocystis in Ibs Eradication With NitazoxanideNikola StojsicNo ratings yet
- Reading Journal ALYADocument14 pagesReading Journal ALYAAlya AnnisaNo ratings yet
- 1471 230X 7 9 PDFDocument5 pages1471 230X 7 9 PDFivanhariachandraNo ratings yet
- Absceso Hepático NeonatalDocument6 pagesAbsceso Hepático NeonatalNabila Peña ZapataNo ratings yet
- 2 TB HipoalbuminDocument9 pages2 TB HipoalbuminfaisalNo ratings yet
- Lower Vitamin D Levels Are Associated With Increased Risk of Early-Onset Neonatal Sepsis in Term InfantsDocument7 pagesLower Vitamin D Levels Are Associated With Increased Risk of Early-Onset Neonatal Sepsis in Term InfantsMohamed Abo SeifNo ratings yet
- Sii ArtículoDocument5 pagesSii ArtículoMonserrat Garduño FonsecaNo ratings yet
- Pediatric Theophylline StudyDocument1 pagePediatric Theophylline StudyElaine M. GeorgeNo ratings yet
- Original Article: Clinical and Laboratory Features of Typhoid Fever in ChildhoodDocument6 pagesOriginal Article: Clinical and Laboratory Features of Typhoid Fever in ChildhoodRidha Surya NugrahaNo ratings yet
- Two Cases of Recurrent ADIH in ChildrenDocument6 pagesTwo Cases of Recurrent ADIH in ChildrenTry Ahmad MirzaNo ratings yet
- Tele The Ruthr AbotuDocument5 pagesTele The Ruthr AbotukhanjanNo ratings yet
- Lactobacillus Reuteri Helicobacter PyloriDocument8 pagesLactobacillus Reuteri Helicobacter PyloriSrisailan KrishnamurthyNo ratings yet
- Krisnisubandiyah Lab/Smf Ilmu Kesehatan Anak FK Unibraw/Rsu Dr. Saiful Anwar MalangDocument11 pagesKrisnisubandiyah Lab/Smf Ilmu Kesehatan Anak FK Unibraw/Rsu Dr. Saiful Anwar MalangfaisalprasetioNo ratings yet
- Risk Factors For Laryngopharyngeal Reflu PDFDocument6 pagesRisk Factors For Laryngopharyngeal Reflu PDFrio yusfiNo ratings yet
- Antimicrobial TutoringDocument3 pagesAntimicrobial TutoringmahapNo ratings yet
- JURNAL READINGnejmoa1007174Document11 pagesJURNAL READINGnejmoa1007174Sukma WinahyuNo ratings yet
- Epidemiological Study of Clinical and Laboratory Profiles of Patients Woth ALL at DR SoetomoDocument5 pagesEpidemiological Study of Clinical and Laboratory Profiles of Patients Woth ALL at DR SoetomoJulia Intan Permata SariNo ratings yet
- Food allergy and asthma characteristics in childrenDocument1 pageFood allergy and asthma characteristics in childrenOlga ArsicNo ratings yet
- Case Report: Acute Hepatitis E in A Pediatric Traveler Presenting With Features of Autoimmune Hepatitis: A Diagnostic and Therapeutic ChallengeDocument4 pagesCase Report: Acute Hepatitis E in A Pediatric Traveler Presenting With Features of Autoimmune Hepatitis: A Diagnostic and Therapeutic Challengeanjingbasah 24No ratings yet
- Digest: Predictors of Failure of Pneumatic Dilatation in AchalasiaDocument3 pagesDigest: Predictors of Failure of Pneumatic Dilatation in AchalasiaDian Eka PermataNo ratings yet
- Paediatric Appendicitis Scoring: A Useful Guide To Diagnose Acute Appendicitis in ChildrenDocument6 pagesPaediatric Appendicitis Scoring: A Useful Guide To Diagnose Acute Appendicitis in ChildrenFebrian Naranggi Aradia PutraNo ratings yet
- Jurnal Reading SjsDocument24 pagesJurnal Reading SjsAnggita Dewi RahmasariNo ratings yet
- 10 1089@cap 2016 0178Document2 pages10 1089@cap 2016 0178Maria Helena Pedraza MNo ratings yet
- Risk Factors and Pattern of Changes in Liver Enzymes Among The Patients With Anti-Tuberculosis Drug-Induced HepatitisDocument3 pagesRisk Factors and Pattern of Changes in Liver Enzymes Among The Patients With Anti-Tuberculosis Drug-Induced HepatitisnazarNo ratings yet
- Impact of Glutathione S-Transferase M1 and T1 On Anti-Tuberculosis Drug-Induced Hepatotoxicity in Chinese Pediatric PatientsDocument11 pagesImpact of Glutathione S-Transferase M1 and T1 On Anti-Tuberculosis Drug-Induced Hepatotoxicity in Chinese Pediatric PatientsLuis JaramilloNo ratings yet
- Mycotoxin Effects On AnimalsDocument4 pagesMycotoxin Effects On AnimalsYusraNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 5: GastrointestinalFrom EverandComplementary and Alternative Medical Lab Testing Part 5: GastrointestinalNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 2: RespiratoryFrom EverandComplementary and Alternative Medical Lab Testing Part 2: RespiratoryNo ratings yet
- 2015 Chinese Government Scholarship-University Postgraduate Study P Rogram (CGS-UPSP)Document1 page2015 Chinese Government Scholarship-University Postgraduate Study P Rogram (CGS-UPSP)Myrtle SetiawanNo ratings yet
- Important:: UploadDocument1 pageImportant:: UploadMyrtle SetiawanNo ratings yet
- TUST Agency Number Is 10057Document1 pageTUST Agency Number Is 10057Myrtle SetiawanNo ratings yet
- Apply for Chinese Government Scholarship at NUST by April 10Document2 pagesApply for Chinese Government Scholarship at NUST by April 10Myrtle SetiawanNo ratings yet
- XDDDDocument1 pageXDDDMyrtle SetiawanNo ratings yet
- The Procedures For Applying For Chinese Government Scholarship at TUSTDocument2 pagesThe Procedures For Applying For Chinese Government Scholarship at TUSTMyrtle SetiawanNo ratings yet
- Application Submit Deadline: Please Mail All The Original Application Documents To Our OfficeDocument1 pageApplication Submit Deadline: Please Mail All The Original Application Documents To Our OfficeMyrtle SetiawanNo ratings yet
- The Procedures For Applying For Chinese Government Scholarship at TustDocument3 pagesThe Procedures For Applying For Chinese Government Scholarship at TustMyrtle SetiawanNo ratings yet
- Online Application: Second Step: ClickDocument1 pageOnline Application: Second Step: ClickMyrtle SetiawanNo ratings yet
- Please Go To Website From - Please Print Out This Application Form, Filling The Forms in DuplicateDocument1 pagePlease Go To Website From - Please Print Out This Application Form, Filling The Forms in DuplicateMyrtle SetiawanNo ratings yet
- 2015 Chinese Government Scholarship-University Postgraduate Study P Rogram (CGS-UPSP)Document1 page2015 Chinese Government Scholarship-University Postgraduate Study P Rogram (CGS-UPSP)Myrtle SetiawanNo ratings yet
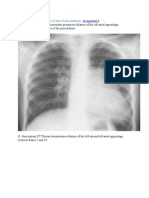
- A. PA Chest Radiograph Demonstrates Prominent Dilation of The Left Atrial Appendage Secondary To Partial Absence of The PericardiumDocument1 pageA. PA Chest Radiograph Demonstrates Prominent Dilation of The Left Atrial Appendage Secondary To Partial Absence of The PericardiumMyrtle SetiawanNo ratings yet
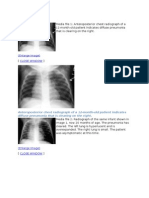
- Radiograph of The Same Infant Shown in Image 1Document1 pageRadiograph of The Same Infant Shown in Image 1Myrtle SetiawanNo ratings yet
- XDDDDocument1 pageXDDDMyrtle SetiawanNo ratings yet
- 7d-2. Congenital Absence of PericardiumDocument2 pages7d-2. Congenital Absence of PericardiumMyrtle SetiawanNo ratings yet
- Complications of Cesarean DeliveryDocument7 pagesComplications of Cesarean DeliverykijokobodroNo ratings yet
- (Enlarge Image) Close WindowDocument1 page(Enlarge Image) Close WindowMyrtle SetiawanNo ratings yet
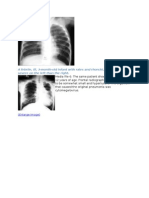
- Same Child Shown in Image 3Document1 pageSame Child Shown in Image 3Myrtle SetiawanNo ratings yet
- Vitamins C & E PregnancyDocument10 pagesVitamins C & E PregnancySri AsmawatiNo ratings yet
- RadiogramDocument1 pageRadiogramMyrtle SetiawanNo ratings yet
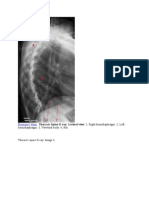
- Previous Next: - Hemidiaphragm. 3, Vertebral Body. 4, RibDocument1 pagePrevious Next: - Hemidiaphragm. 3, Vertebral Body. 4, RibMyrtle SetiawanNo ratings yet
- Febrile Infant With Left Lung Pneumonia Later Develops Lung ChangesDocument1 pageFebrile Infant With Left Lung Pneumonia Later Develops Lung ChangesMyrtle SetiawanNo ratings yet
- Thoracic Spine X-ray AP View AnatomyDocument1 pageThoracic Spine X-ray AP View AnatomyMyrtle SetiawanNo ratings yet
- QL Fqn6qlmpDocument6 pagesQL Fqn6qlmpMyrtle SetiawanNo ratings yet
- Thoracic Spine X-RayDocument1 pageThoracic Spine X-RayMyrtle SetiawanNo ratings yet
- Reliability of Laparoscopic Compared With.11Document7 pagesReliability of Laparoscopic Compared With.11Myrtle SetiawanNo ratings yet
- Chest X-Ray: AP ProjectionDocument1 pageChest X-Ray: AP ProjectionMyrtle SetiawanNo ratings yet
- Nej Mo A 0907736Document13 pagesNej Mo A 0907736Myrtle SetiawanNo ratings yet
- Timing of Copper Intrauterine Device Insertion.18Document6 pagesTiming of Copper Intrauterine Device Insertion.18Myrtle SetiawanNo ratings yet
- Health of Children Born To Mothers Who Had Preeclampsia: A Population-Based Cohort StudyDocument10 pagesHealth of Children Born To Mothers Who Had Preeclampsia: A Population-Based Cohort StudyAdhitya Pratama SutisnaNo ratings yet
- Summary of Infectious DiseasesDocument407 pagesSummary of Infectious DiseasesMh HmNo ratings yet
- Anti-TB Drug RegimensDocument8 pagesAnti-TB Drug Regimensbo gum parkNo ratings yet
- 02 - LEC DOH Programs For Communicable - Non-Communicable DiseasesDocument21 pages02 - LEC DOH Programs For Communicable - Non-Communicable DiseasesJAN CAMILLE LENONNo ratings yet
- Pharmacology Antimycobacterial DrugsDocument9 pagesPharmacology Antimycobacterial Drugsroyce charlieNo ratings yet
- O/dr - Ririn FK UnilaDocument29 pagesO/dr - Ririn FK UnilaNyimas Annissa Mutiara Andini100% (1)
- Bds Third Professional Examination 2007 General Medicine (Seqs) Model PaperDocument15 pagesBds Third Professional Examination 2007 General Medicine (Seqs) Model PaperDania RiazNo ratings yet
- Formularium 2009Document190 pagesFormularium 2009Astri DesmayantiNo ratings yet
- MDR TB Made EasyDocument58 pagesMDR TB Made EasyNezly IderusNo ratings yet
- Soal PAS Bahasa Inggris Kelas 9 K13 Semester 1Document8 pagesSoal PAS Bahasa Inggris Kelas 9 K13 Semester 1Imran Hamid0% (1)
- Akurit 4 TBDocument14 pagesAkurit 4 TBNicolloNo ratings yet
- Tuberculosis (TB) : National Antibiotic GuidelinesDocument12 pagesTuberculosis (TB) : National Antibiotic GuidelinesJun JimenezNo ratings yet
- Communicable Disease NursingDocument41 pagesCommunicable Disease NursingBJ DUQUESA100% (2)
- Principles of Management of MDR-TBDocument22 pagesPrinciples of Management of MDR-TBGeorge VergheseNo ratings yet
- A3 24pt 9BN0 - 01 Question Paper PDFDocument69 pagesA3 24pt 9BN0 - 01 Question Paper PDFAhmed SadhanNo ratings yet
- Mycobacterium Tuberculosis and Antibiotic Resistant A Rememerging Disease and Public Health ProblemDocument37 pagesMycobacterium Tuberculosis and Antibiotic Resistant A Rememerging Disease and Public Health ProblemVincent Samuel Valentine76% (21)
- ERS Handbook-Self-Assessment in Respiratory Medicine, 2e (Sep 1, 2015) - (1849840784) - (European Respiratory Society) .PDF (Konrad E. Bloch, Thomas Brack, Anita K. Simonds)Document560 pagesERS Handbook-Self-Assessment in Respiratory Medicine, 2e (Sep 1, 2015) - (1849840784) - (European Respiratory Society) .PDF (Konrad E. Bloch, Thomas Brack, Anita K. Simonds)Shop Upmed100% (1)
- Anti-TB Drugs MCQ QuizDocument27 pagesAnti-TB Drugs MCQ QuizYashwant ChauhanNo ratings yet
- PTB Case-StudyDocument64 pagesPTB Case-StudyBeverly DatuNo ratings yet
- Second Sempre Finals PHC EXAM K2Document4 pagesSecond Sempre Finals PHC EXAM K2yabaeveNo ratings yet
- Pharmacotherapy of Tuberculosis Treatment SchemesDocument31 pagesPharmacotherapy of Tuberculosis Treatment SchemesjabirNo ratings yet
- Pneumonia & TB NCLEX Practice Questions Med SurgDocument20 pagesPneumonia & TB NCLEX Practice Questions Med SurgKirsten ChavezNo ratings yet
- TB Treatment in Liver Disease PatientsDocument2 pagesTB Treatment in Liver Disease Patientsmoipone makakoleNo ratings yet
- Tuberculosis in Pregnancy UptodateDocument14 pagesTuberculosis in Pregnancy UptodateRahmanu ReztaputraNo ratings yet
- Script Video About TBCDocument2 pagesScript Video About TBCMithaprnmsrNo ratings yet
- Tuberculous meningitis: many questions, too few answersDocument11 pagesTuberculous meningitis: many questions, too few answersGustavo MartinezNo ratings yet
- Gastroenterology: Case Discussion: Pharmacological PerspectiveDocument21 pagesGastroenterology: Case Discussion: Pharmacological PerspectivePanini PatankarNo ratings yet
- Pharmacy MCQSDocument132 pagesPharmacy MCQSomair zafar100% (6)
- Common Pulmonary Diseases: Emmanuel R. Kasilag, MD, FPCP, FPCCPDocument74 pagesCommon Pulmonary Diseases: Emmanuel R. Kasilag, MD, FPCP, FPCCPDivine Grace FernandezNo ratings yet
- LPD - Myrin P Forte (Pakistan)Document17 pagesLPD - Myrin P Forte (Pakistan)Azeem Abbas0% (1)
- Tuberculosis 01Document70 pagesTuberculosis 01kurutalaNo ratings yet