Professional Documents
Culture Documents
Atrial Septal Defect
Uploaded by
almorsOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Atrial Septal Defect
Uploaded by
almorsCopyright:
Available Formats
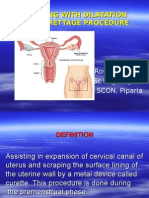
Atrial Septal Defect
Definition
An atrial septal defect is an abnormal opening in the wall separating the left and right upper chambers (atria) of the heart.
Description
During the normal development of the fetal heart, there is an opening in the wall (the septum) separating the left and right upper chambers of the heart. Normally, this opening closes before birth, but if it does not, the child is born with a hole between the left and right atria. This abnormal opening is called an atrial septal defect and causes blood from the left atrium to flow into the right atrium. Different types of atrial septal defects can occur, and they are classified according to where in the separating wall they are found. The most commonly found atrial septal defect occurs in the middle of the atrial septum and accounts for about 70% of all atrial septal defects. Abnormal openings can form in the upper and lower parts of the atrial septum as well.
Causes and symptoms
Abnormal openings in the atrial septum occur during fetal development and are twice as common in females as in males. These abnormalities can go unnoticed if the opening is small, producing no abnormal symptoms. If the defect is big, large amounts of blood flowing from the left to the right atrium will cause the right atrium to swell to hold the extra blood. People born with an atrial septal defect can have no symptoms through their twenties, but by age 40, most people with this condition have symptoms that can include shortness of breath, rapid abnormal beating of the atria (atrial fibrillation), and eventually heart failure.
Diagnosis
Atrial septal defects can be identified by various methods. Abnormal changes in the sound of the heart beats can be heard when a doctor listens to the heart with a stethoscope. In addition, a chest x ray, an electrocardiogram (ECG, an electrical printout of the heartbeats), and an echocardiogram (a test that uses sound waves to form a detailed image of the heart) can also be used to identify this condition. An atrial septal defect can also be diagnosed by using a test called cardiac catheterization. This test involves inserting a very thin tube (catheter) into the heart's chambers to measure the amount of oxygen present in the blood within the heart. If the heart has an opening between the atria, oxygen-rich blood from the left atrium enters the right atrium. Through cardiac catheterization, doctors can detect the higher-than-normal amount of oxygen in the heart's right atrium, right ventricle, and the large blood vessels that carry blood to the lungs, where the blood would normally subsequently get its oxygen.
Treatment
Atrial septal defects often correct themselves without medical treatments by the age of two. If this dose not happen, surgery is done by sewing the hole closed, or by sewing a patch of Dacron material or a piece of the sac that surrounds the heart (the pericardium), over the opening. Some patients can have the defect fixed by having an clam-shaped plug placed over the opening. This plug is a manmade device that is put in place through a catheter inserted into the heart.
Prognosis
Individuals with small defects can live a normal life, but larger defects require surgical correction. Less than 1% of people younger than 45 years of age die from corrective surgery. Five to ten percent of patients can die from the surgery if they are older than 40 and have other heart-related problems. When an atrial septal defect is corrected within the first 20 years of life, there is an excellent chance for the individual to live normally.
Key terms
Cardiac catheterization A test that involves having a tiny tube inserted into the heart through a blood vessel. Dacron A synthetic polyester fiber used to surgically repair damaged sections of heart muscle and blood vessel walls. Echocardiogram A test that uses sound waves to generate an image of the heart, its valves, and chambers.
Resources
Organizations American Heart Association. 7320 Greenville Ave. Dallas, TX 75231. (214) 373-6300. http://www.americanheart.org.
Gale Encyclopedia of Medicine. Copyright 2008 The Gale Group, Inc. All rights reserved.
Atrial Septal Defect (ASD)
What is an atrial septal defect?
Anatomy of the heart, normal
Click Image to Enlarge An atrial septal defect is an opening in the atrial septum, or dividing wall between the two upper chambers of the heart known as the right and left atria. ASD is a congenital (present at birth) heart defect. As the fetus is growing, something occurs to affect heart development during the first eight weeks of pregnancy, resulting in an ASD. Normally, oxygen-poor (blue) blood returns to the right atrium from the body, travels to the right ventricle, then is pumped into the lungs where it receives oxygen. Oxygen-rich (red) blood returns to the left atrium from the lungs, passes into the left ventricle, and then is pumped out to the body through the aorta. An atrial septal defect allows oxygen-rich (red) blood to pass from the left atrium, through the opening in the septum, and then mix with oxygen-poor (blue) blood in the right atrium. Illustration of the anatomy of a heart with an atrial septal defect
Click Image to Enlarge Atrial septal defects occur in 6 percent to 8 percent of all children born with congenital heart disease. For unknown reasons, girls have atrial septal defects twice as often as boys.
What causes an atrial septal defect?
The heart is forming during the first eight weeks of fetal development. It begins as a hollow tube, then partitions within the tube develop that eventually become the septa (or walls) dividing the right side of the heart from the left. Atrial septal defects occur when the partitioning process does not occur completely, leaving an opening in the atrial septum. Some congenital heart defects may have a genetic link, either occurring due to a defect in a gene, a chromosome abnormality, or environmental exposure, causing heart problems to occur more often in certain families. Most atrial septal defects occur sporadically (by chance), with no clear reason for their development.
What are the types of atrial septal defects?
There are four types of atrial septal defects:
ostium secundum atrial septal defect This is the most common atrial septal defect, affecting 80 percent of people with atrial septal defects. It is caused when a part of the atrial septum fails to close completely while the heart is developing. This causes an opening to develop in the center of the wall separating the two atria. ostium primum atrial septal defect This defect is part of the atrioventricular canal defects, and is associated with a split (cleft) in one of the leaflets of the mitral valve. sinus venosus atrial septal defect This defect occurs at the superior vena cava and right atrium junction, in the area where the pulmonary veins enter the heart. As a result, the drainage of one or more of the pulmonary veins may be abnormal in that the pulmonary veins enter the right atrium rather than the left atrium.
coronary sinus atrial septal defect This defect is located within the coronary sinus, which is the structure in the right atrium where all the heart's own veins drain into the right atrium. It is the rarest of all atrial septal defects.
Why is an atrial septal defect a concern?
This heart defect can over time cause lung problems if not repaired. When blood passes through the ASD from the left atrium to the right atrium, a larger volume of blood than normal must be handled by the right side of the heart. This extra blood passes through the pulmonary artery into the lungs, causing higher amounts of blood flow than normal in the vessels in the lungs. A small opening in the atrial septum allows a small amount of blood to pass through from the left atrium to the right atrium. A large opening allows more blood to pass through and mix with the normal blood flow in the right heart.. The lungs are able to cope with this blood flow for a long period of time. In some patients, the extra blood flow eventually raises the blood pressure in the lungs, usually after several decades. This then hardens the blood vessels in the lungs, causing them to be diseased, resulting in irreversible changes in the lungs.
What are the symptoms of an atrial septal defect?
Many children have no symptoms and seem healthy. However, if the ASD is large, permitting a large amount of blood to pass through to the right side of the heart, the right atrium, right ventricle, and lungs will become overworked, and symptoms may be noted. The following are the most common symptoms of atrial septal defect. However, each child may experience symptoms differently. Symptoms may include:
child tires easily when playing fatigue sweating rapid breathing shortness of breath poor growth frequent respiratory infections The symptoms of an atrial septal defect may resemble other medical conditions or heart problems. Always consult your child's physician for a diagnosis.
How is an atrial septal defect diagnosed?
Your child's physician may have heard a heart murmur during a physical examination, and referred your child to a pediatric cardiologist for a diagnosis. A heart murmur is simply a noise caused by the turbulence of blood flowing through the opening from the left side of the heart to the right. A pediatric cardiologist specializes in the diagnosis and medical management of congenital heart defects, as well as heart problems that may develop later in childhood. The cardiologist will perform a physical examination, listening to the heart and lungs, and make other observations that help in the diagnosis. The location within the chest that the murmur is heard best, as well as the loudness and quality of the murmur (harsh, blowing, etc.) will give the cardiologist an initial idea of which heart problem your child may have. Diagnostic testing for congenital heart disease varies by the child's age, clinical condition, and institutional preferences. Some tests that may be recommended include the following:
chest X-ray - a diagnostic test which uses invisible X-ray beams to produce images of internal tissues, bones, and organs onto film. With an ASD, the heart may be enlarged because the right atrium and ventricle have to handle larger amounts of blood flow than normal. Also, there may be changes that take place in the lungs due to extra blood flow that can be seen on an X-ray. electrocardiogram (ECG or EKG) - a test that records the electrical activity of the heart, shows abnormal rhythms (arrhythmias or dysrhythmias), and detects heart muscle stress. echocardiogram (echo) - a procedure that evaluates the structure and function of the heart by using sound waves recorded on an electronic sensor that produce a moving picture of the heart and heart valves. An echo can show the pattern of blood flow through the atrial septal opening, and determine how large the opening is, as well as how much blood is passing through it. cardiac catheterization - a cardiac catheterization is an invasive procedure that gives very detailed information about the structures inside the heart. Under sedation, a small, thin, flexible tube (catheter) is inserted into a blood vessel in the groin, and guided to the inside of the heart. Blood pressure and oxygen measurements are taken in the four chambers of the heart, as well as the pulmonary artery and aorta. Contrast dye is also injected to more clearly visualize the structures inside the heart. Although an echocardiogram often provides enough diagnostic information, device closure of the ASD can be performed at the time of the catheterization.
Treatment for atrial septal defect:
Specific treatment for ASD will be determined by your child's physician based on:
your child's age, overall health, and medical history extent of the disease your child's tolerance for specific medications, procedures, or therapies expectations for the course of the disease your opinion or preference
Secundum atrial septal defects may close spontaneously as a child grows. Once an atrial septal defect is diagnosed, your child's cardiologist will evaluate your child periodically to see whether it is closing on its own. Usually, an ASD will be repaired if it has not closed on its own by the time your child starts school - to prevent lung problems that will develop from long-time exposure to extra blood flow. The decision to close the ASD may also depend on the size of the defect. Individuals who have their atrial septal defects repaired in childhood can prevent problems later in life.
Treatment may include:
medical management Many children have no symptoms, and require no medications. However, some children may need to take medications to help the heart work better, since the right side is under strain from the extra blood passing through the ASD. Medications that may be prescribed include the following:
o o
digoxin - a medication that helps strengthen the heart muscle, enabling it to pump more efficiently. diuretics - the body's water balance can be affected when the heart is not working as well as it could. These medications help the kidneys remove excess fluid from the body.
infection control Children with certain heart defects are at risk for developing an infection of the inner surfaces of the heart known as bacterial endocarditis. It is important that you inform all medical personnel that your child has an ASD so they may determine if the antibiotics are necessary before a procedure. surgical repair Your child's ASD may be repaired surgically in the operating room. The surgical repair is performed under general anesthesia. The defect may be closed with stitches or a special patch. device closure Device closure is frequently performed for secundum ASD, depending on the size of the defect and the weight of the child. During the cardiac catheterization procedure, the child is sedated and a small, thin, flexible tube (catheter) is inserted into a blood vessel in the groin and guided to the inside of the heart. Once the catheter is in the heart, the cardiologist will pass a special device, called a septal occluder, into the open ASD, preventing blood from flowing through it.
Post-procedure care for your child:
device closure procedure When the procedure is complete, the catheter(s) will be withdrawn. Several gauze pads and a large piece of medical tape will be placed on the site where the catheter was inserted to prevent bleeding. In some cases, a small, flat weight or sandbag may be used to help keep pressure on the catheterization site and decrease the chance of bleeding. If blood vessels in the leg were used, your child will be told to keep the leg straight for a few hours after the procedure to minimize the chance of bleeding at the catheterization site. Your child will be taken to a unit in the hospital where he/she will be monitored by nursing staff for several hours after the test. The length of time it takes for your child to wake up after the procedure will depend on the type of medicine given to your child for relaxation prior to the test, and also on your child's reaction to the medication. After the procedure, your child's nurse will monitor the pulses and skin temperature in the leg or arm that was used for the procedure. Your child may be able to go home after a specified period of time, providing he/she does not need further treatment or monitoring. You will receive written instructions regarding care of the catheterization site, bathing, activity restrictions, and any new medications your child may need to take at home.
surgical repair In most cases, children will spend time in the intensive care unit (ICU) for several hours, or overnight, after an ASD repair. During the first several hours after surgery, your child will most likely be drowsy from the anesthesia that was used during the operation, and from medications given to relax him/her and to help with pain. As time goes by, your child will become more alert. While your child is in the ICU, special equipment will be used to help him/her recover, and may include the following:
ventilator - a machine that helps your child breathe while he/she is under anesthesia during the operation. A small, plastic tube is guided into the windpipe and attached to the ventilator, which breathes for your child while he/she is too sleepy to breathe effectively on his/her own. Many children have the ventilator tube removed right after surgery, but some other children will benefit from remaining on the ventilator for a few hours afterwards so they can rest. intravenous (IV) catheters - small, plastic tubes inserted through the skin into blood vessels to provide IV fluids and important medications that help your child recover from the operation. arterial line - a specialized IV placed in the wrist, or other area of the body where a pulse can be felt, that measures blood pressure continuously during surgery and while your child is in the ICU. nasogastric (NG) tube - a small, flexible tube that keeps the stomach drained of acid and gas bubbles that may build up during surgery. urinary catheter - a small, flexible tube that allows urine to drain out of the bladder and accurately measures how much urine the body makes, which helps determine how well the heart is functioning. After surgery, the heart will be a little weaker than it was before, and, therefore, the body may start to hold onto fluid, causing swelling and puffiness. Diuretics may be given to help the kidneys remove excess fluids from the body.
o o o o
o o
chest tube - a drainage tube may be inserted to keep the chest free of blood that would otherwise accumulate after the incision is closed. Bleeding may occur for several hours, or even a few days after surgery. heart monitor - a machine that constantly displays a picture of your child's heart rhythm, and monitors heart rate, arterial blood pressure, and other values.
Your child may need other equipment, not mentioned here, to provide support while in the ICU, or afterwards. The hospital staff will explain all of the necessary equipment to you. Your child will be kept as comfortable as possible with several different medications; some of which relieve pain and some of which relieve anxiety. The staff may also ask for your input as to how best to soothe and comfort your child. After discharge from the ICU, your child will recuperate on another hospital unit for a few days before going home. You will learn how to care for your child at home before your child is discharged. Your child may need to take medications for a while and these will be explained to you. The staff will provide instructions regarding medications, activity limitations, and follow-up appointments before your child is discharged.
Care for your child at home following ASD repair:
Most children feel fairly comfortable when they go home, and have a fair tolerance for activity. Your child may become tired quicker than before the repair, but usually will be allowed to play with supervision, while avoiding blows to the chest that might cause injury to the incision or breastbone. Within a few weeks, your child should be fully recovered and able to participate in normal activity. Pain medications, such as acetaminophen or ibuprofen, may be recommended to keep your child comfortable at home. Your child's physician will discuss pain control before your child is discharged from the hospital.
Long-term outlook after ASD repair:
The majority of children who have had an atrial septal defect repair will live healthy lives. Your child's cardiologist may recommend that your child take antibiotics to prevent bacterial endocarditis for a specific time period after discharge from the hospital. Outcomes also depend on the type of ASD, as well as how early in life the ASD was diagnosed and whether or not it was repaired. With early diagnosis and repair of an ASD, the outcome is generally excellent, and minimal follow-up is necessary. When an ASD is diagnosed later in life, if complications occur after surgical closure, or the ASD is never repaired, the outlook may be worse than normal. There is a risk of developing pulmonary hypertension (high blood pressure in the blood vessels of the lungs) or Eisenmenger's syndrome. These individuals should receive follow-up care at a center that specializes in congenital heart disease. Consult your child's physician regarding the specific outlook for your child.
Topic Home Page | Return to Full List of Topics The information on this Web page is provided for educational purposes. You understand and agree that this information is not intended to be, and should not be used as, a substitute for medical treatment by a health care professional. You agree that Lucile Salter Packard Children's Hospital is not making a diagnosis of your condition or a recommendation about the course of treatment for your particular circumstances through the use of this Web page. You agree to be solely responsible for your use of this Web page and the information contained on this page. Lucile Salter Packard Children's Hospital, its officers, directors, employees, agents, and information providers shall not be liable for any damages you may suffer or cause through your use of this page even if advised of the possibility of such damages.
You might also like
- Atrial Septal DefectDocument3 pagesAtrial Septal Defectmu_crNo ratings yet
- Holter MonitoringDocument19 pagesHolter Monitoringomotola Ayobundle-oyewo MA206100% (1)
- Agency ProjectDocument14 pagesAgency Projectapi-304517936No ratings yet
- Lesson Plan On Preterm CareDocument4 pagesLesson Plan On Preterm CarePabhat KumarNo ratings yet
- D&C Procedure GuideDocument18 pagesD&C Procedure GuideRoselineTiggaNo ratings yet
- Mitral Stenosis Facts, Causes, Symptoms and TreatmentDocument16 pagesMitral Stenosis Facts, Causes, Symptoms and TreatmentAsrafur RahmanNo ratings yet
- Intubation ProcedureDocument5 pagesIntubation ProcedurePurwadi SujalmoNo ratings yet
- Chest PhysiotherapyDocument4 pagesChest Physiotherapyhakky gamyNo ratings yet
- HOLTER MONITORING: A GUIDE TO THE AMBULATORY ECG PROCEDUREDocument21 pagesHOLTER MONITORING: A GUIDE TO THE AMBULATORY ECG PROCEDUREAngel LeeNo ratings yet
- Incentive SpirometryDocument3 pagesIncentive SpirometryNursidar Pascual MukattilNo ratings yet
- Cardiac MonitorDocument5 pagesCardiac MonitorhumbertolgeNo ratings yet
- TOF Patient EducationDocument8 pagesTOF Patient EducationMia MiaNo ratings yet
- 3&4&5-Assessment of Peripheral Vascular SystemDocument43 pages3&4&5-Assessment of Peripheral Vascular SystemKhaled Mohamed AssemNo ratings yet
- Endotracheal IntubationDocument11 pagesEndotracheal Intubationanon_784834955100% (1)
- Chest Physiotherapy - Postural DrainageDocument2 pagesChest Physiotherapy - Postural DrainageMicah MagallanoNo ratings yet
- Administration of Inotropes Evidence Based Nursing PolicyDocument8 pagesAdministration of Inotropes Evidence Based Nursing PolicyRonald ThakorNo ratings yet
- BiopsyDocument5 pagesBiopsypayments8543No ratings yet
- Defibrillator1 200806145633Document28 pagesDefibrillator1 200806145633harpreetNo ratings yet
- PartoghraphDocument60 pagesPartoghraphharley dela cruzNo ratings yet
- WeaningDocument7 pagesWeaningKiran KhasaNo ratings yet
- Holter Monitor: 'Ambulatory Electrocardiography Device''Document22 pagesHolter Monitor: 'Ambulatory Electrocardiography Device''Rachel PeredaNo ratings yet
- IschemicheartdiseaseDocument11 pagesIschemicheartdiseaseZaimon MaulionNo ratings yet
- Performing Chest PhysiotherapyDocument14 pagesPerforming Chest PhysiotherapyDivya Chauhan100% (1)
- 13.format - App-Hand Anthropometry and Grip StrengthDocument6 pages13.format - App-Hand Anthropometry and Grip StrengthImpact JournalsNo ratings yet
- Pregnancy Induced HypertensionDocument4 pagesPregnancy Induced HypertensionMjhay SalvadorNo ratings yet
- Cardiac SurgeryDocument35 pagesCardiac SurgeryxxxNo ratings yet
- Hypoxic-Ischemic Encephalopathy A Review For The ClinicianDocument7 pagesHypoxic-Ischemic Encephalopathy A Review For The ClinicianKaren Carpio100% (1)
- Advanced Cardiac ProcedureDocument9 pagesAdvanced Cardiac ProcedureSachin DwivediNo ratings yet
- Introduction Definition: Types of PacemakersDocument8 pagesIntroduction Definition: Types of PacemakersPrasann RoyNo ratings yet
- A Lumbar PunctureDocument6 pagesA Lumbar PunctureNivinj KennedyNo ratings yet
- A Clinical Evidence and Management of AsthmaDocument19 pagesA Clinical Evidence and Management of Asthmaraajverma1000mNo ratings yet
- Basic Respiratory Mechanics: Ventilation, Diffusion, and Gas ExchangeDocument36 pagesBasic Respiratory Mechanics: Ventilation, Diffusion, and Gas ExchangeRizqi Luqmanul HakimNo ratings yet
- Syllabus Course English For Nursing 1 Year of StudyDocument35 pagesSyllabus Course English For Nursing 1 Year of StudyAna Maria DrăgotescuNo ratings yet
- Checklist For The VS Measurement (TPR and BP) A. Temperature A.1. Axillary Temperature (Digital Thermometer) Done Needs PracticeDocument3 pagesChecklist For The VS Measurement (TPR and BP) A. Temperature A.1. Axillary Temperature (Digital Thermometer) Done Needs PracticeCyrillNo ratings yet
- Difficult AirwayDocument77 pagesDifficult AirwayParvathy R Nair100% (1)
- Thoracic and Lung Assessment: Physical Examination of The Thorax and The LungsDocument16 pagesThoracic and Lung Assessment: Physical Examination of The Thorax and The Lungsshannon c. lewis100% (1)
- Cyanotic Congenital Heart DiseaseDocument6 pagesCyanotic Congenital Heart DiseaseSimran JosanNo ratings yet
- Presentation On EchocardiogramDocument17 pagesPresentation On EchocardiogramSoniya NakkaNo ratings yet
- TRANSPOSITION OF THE GREAT VESSELS PrintDocument8 pagesTRANSPOSITION OF THE GREAT VESSELS PrintAnandhu GNo ratings yet
- LUMBERPUNCTURDocument14 pagesLUMBERPUNCTURRahul VasavaNo ratings yet
- Fetal CirculationDocument13 pagesFetal CirculationPraveen YadavNo ratings yet
- Peripheral Artery Disease: Nikhil Vaishnav M.Sc. (Nursing)Document70 pagesPeripheral Artery Disease: Nikhil Vaishnav M.Sc. (Nursing)Dimpal ChoudharyNo ratings yet
- Development of The HeartDocument19 pagesDevelopment of The HeartYusuf UmarNo ratings yet
- Bells Palsy DorisDocument37 pagesBells Palsy DoristheychemNo ratings yet
- Modes of Mechanical VentilationDocument55 pagesModes of Mechanical VentilationLuis LopezNo ratings yet
- Patent Ductus ArteriosusDocument49 pagesPatent Ductus Arteriosusarchana vermaNo ratings yet
- Cardiopulmonary Cerebral ResuscitationDocument17 pagesCardiopulmonary Cerebral ResuscitationrizalNo ratings yet
- Range of Motion ExercisesDocument13 pagesRange of Motion Exercisesmoira77No ratings yet
- Post Partum Care: Care Within The First 24 HoursDocument4 pagesPost Partum Care: Care Within The First 24 HoursCarrie ANo ratings yet
- Acyanotic Congenital Heart DiseaseDocument48 pagesAcyanotic Congenital Heart DiseasenabillagusrinaNo ratings yet
- SuctioningDocument27 pagesSuctioningMoni Mbumba MelekeNo ratings yet
- Machanical Ventilator Nursing Care PalnDocument13 pagesMachanical Ventilator Nursing Care PalnAnnie Priscilla100% (1)
- Types of Skin Traction PresentationDocument16 pagesTypes of Skin Traction PresentationZerjohn Seniorom100% (1)
- Neonatal Sepsis LectureDocument142 pagesNeonatal Sepsis Lectureokwadha simion0% (1)
- Endotracheal IntubationDocument1 pageEndotracheal IntubationAnusha VergheseNo ratings yet
- Devices Used in ICU: Critical Care NursingDocument95 pagesDevices Used in ICU: Critical Care NursinghendranatjNo ratings yet
- Vital SignDocument4 pagesVital SignGabriel JocsonNo ratings yet
- Hirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Atrial Septal DefectDocument7 pagesAtrial Septal DefectRis Amy AyaNo ratings yet
- About The Heart and Blood Vessels Anatomy and Function of The Heart ValvesDocument4 pagesAbout The Heart and Blood Vessels Anatomy and Function of The Heart ValvesdomlhynNo ratings yet
- The Meaning of The Miraculous MedalDocument3 pagesThe Meaning of The Miraculous MedalalmorsNo ratings yet
- DXN ProductsDocument3 pagesDXN ProductsalmorsNo ratings yet
- CoachingDocument66 pagesCoachingalmorsNo ratings yet
- Positive Discipline in Everyday Teaching - A Primer For Filipino TeachersDocument48 pagesPositive Discipline in Everyday Teaching - A Primer For Filipino Teachersjhunma2000281783% (12)
- Gad AccordDocument4 pagesGad AccordalmorsNo ratings yet
- DXN Philippines Service CentersDocument8 pagesDXN Philippines Service Centersalmors75% (4)
- Classroom Management StrategiesDocument19 pagesClassroom Management Strategiesalmors0% (1)
- Doctrine of in Loco ParentisDocument7 pagesDoctrine of in Loco ParentisalmorsNo ratings yet
- Legal Bases of Prohibiting Corporal PunishmentDocument9 pagesLegal Bases of Prohibiting Corporal PunishmentalmorsNo ratings yet
- Table of PenaltiesDocument2 pagesTable of PenaltiesalmorsNo ratings yet
- Doctrine of in Loco ParentisDocument7 pagesDoctrine of in Loco ParentisalmorsNo ratings yet
- Cot Rpms RubricDocument5 pagesCot Rpms Rubricalmors92% (12)
- What Writers Say About the Power of WordsDocument4 pagesWhat Writers Say About the Power of WordsalmorsNo ratings yet
- Revising Bloom's Taxonomy to Better Reflect CognitionDocument7 pagesRevising Bloom's Taxonomy to Better Reflect CognitionalmorsNo ratings yet
- InsectsDocument2 pagesInsectsalmorsNo ratings yet
- How To Prepare Better Multiple-Choice Test ItemsDocument35 pagesHow To Prepare Better Multiple-Choice Test ItemsnamavayaNo ratings yet
- Test PlanningDocument86 pagesTest PlanningalmorsNo ratings yet
- Blooms TaxonomyDocument1 pageBlooms TaxonomysivaeeinfoNo ratings yet
- Balancing RationsDocument10 pagesBalancing RationsalmorsNo ratings yet
- 07 ChairmansReportDocument3 pages07 ChairmansReportalmorsNo ratings yet
- House RulesDocument1 pageHouse RulesalmorsNo ratings yet
- Business Meeting ScriptDocument4 pagesBusiness Meeting ScriptalmorsNo ratings yet
- Three-Salary Grade LimitationDocument3 pagesThree-Salary Grade LimitationalmorsNo ratings yet
- Academic freedom in the PhilippinesDocument2 pagesAcademic freedom in the PhilippinesalmorsNo ratings yet
- MCQ Dimaampao W Answer KeyDocument25 pagesMCQ Dimaampao W Answer KeyJohn Henry Naga100% (3)
- Fertilizer IdentificationDocument1 pageFertilizer IdentificationalmorsNo ratings yet
- Prayer PostureDocument3 pagesPrayer PosturealmorsNo ratings yet
- 4 Stroke CycleDocument1 page4 Stroke CyclealmorsNo ratings yet
- How To Prepare Better Multiple-Choice Test ItemsDocument35 pagesHow To Prepare Better Multiple-Choice Test ItemsnamavayaNo ratings yet
- Accounting For Merchandising ActivitiesDocument53 pagesAccounting For Merchandising ActivitiesalmorsNo ratings yet
- BS EN 1677-5-2001 - Inc.Document3 pagesBS EN 1677-5-2001 - Inc.Ameer Sadimin SGNo ratings yet
- About Topsøe - and What We DoDocument20 pagesAbout Topsøe - and What We DoAbhishek ChaudharyNo ratings yet
- English A June 2008 p2Document9 pagesEnglish A June 2008 p2LilyNo ratings yet
- Haier's Performance Management in Other CulturesDocument8 pagesHaier's Performance Management in Other CulturesSubhransu SahooNo ratings yet
- Gabriel Nobre de Souza - Groningen Mini-MetropolisDocument9 pagesGabriel Nobre de Souza - Groningen Mini-MetropolisGabrielNobredeSouzaNo ratings yet
- Liugong 938 Wheel Loader Parts ManualDocument20 pagesLiugong 938 Wheel Loader Parts Manualjonathan100% (49)
- 3 - 6consctructing Probability Distributions CG A - 4 - 6 Lesson 2Document24 pages3 - 6consctructing Probability Distributions CG A - 4 - 6 Lesson 2CHARLYN JOY SUMALINOGNo ratings yet
- Solution Manual For Contemporary Project Management 4th EditionDocument15 pagesSolution Manual For Contemporary Project Management 4th EditionDanaAllendzcfa100% (77)
- Introduction To The Philosophy of The Human Person Quarter I - Module 2Document26 pagesIntroduction To The Philosophy of The Human Person Quarter I - Module 2Katrina TulaliNo ratings yet
- Educational Leadership Platform PaperDocument4 pagesEducational Leadership Platform Paperapi-273087939No ratings yet
- MATH6113 - PPT5 - W5 - R0 - Applications of IntegralsDocument58 pagesMATH6113 - PPT5 - W5 - R0 - Applications of IntegralsYudho KusumoNo ratings yet
- Benedict - Ethnic Stereotypes and Colonized Peoples at World's Fairs - Fair RepresentationsDocument16 pagesBenedict - Ethnic Stereotypes and Colonized Peoples at World's Fairs - Fair RepresentationsVeronica UribeNo ratings yet
- Basic Concepts of Citrix XenAppDocument13 pagesBasic Concepts of Citrix XenAppAvinash KumarNo ratings yet
- Technical Bro A4 UK LR NEW v2Document45 pagesTechnical Bro A4 UK LR NEW v2Roxana NegoitaNo ratings yet
- 1F4 Catalog0808Document12 pages1F4 Catalog0808Edwin Ng0% (1)
- Media LiteracyDocument33 pagesMedia LiteracyDo KyungsooNo ratings yet
- SBFP Timeline 2019Document1 pageSBFP Timeline 2019Marlon Berjolano Ere-erNo ratings yet
- 4MB0 02R Que 20160609 PDFDocument32 pages4MB0 02R Que 20160609 PDFakashNo ratings yet
- PEB Requirment by ClientDocument4 pagesPEB Requirment by ClientViraj ModiNo ratings yet
- Why study operating systems and how they workDocument12 pagesWhy study operating systems and how they workMario ManihurukNo ratings yet
- 360 PathwaysDocument4 pages360 PathwaysAlberto StrusbergNo ratings yet
- Cambridge International General Certificate of Secondary EducationDocument16 pagesCambridge International General Certificate of Secondary EducationAdaaan AfzalNo ratings yet
- Event ReportDocument2 pagesEvent Reportakshitdaharwal997No ratings yet
- OB HandoutsDocument16 pagesOB HandoutsericNo ratings yet
- Makerwys - Exe Version 4.891: by Pete Dowson © 2019 InstructionsDocument11 pagesMakerwys - Exe Version 4.891: by Pete Dowson © 2019 InstructionsRafrol RamonNo ratings yet
- Digital Burner Controller: Tbc2800 SeriesDocument4 pagesDigital Burner Controller: Tbc2800 SeriesSUDIP MONDALNo ratings yet
- DelhiDocument40 pagesDelhiRahul DharNo ratings yet
- Amity Online Exam OdlDocument14 pagesAmity Online Exam OdlAbdullah Holif0% (1)
- Laboratory SafetyDocument4 pagesLaboratory SafetyLey DoydoraNo ratings yet
- Johnson 1999Document20 pagesJohnson 1999Linh Hoàng PhươngNo ratings yet