Professional Documents
Culture Documents
Nasopharyngeal Cancer
Uploaded by
mynoidanh19Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Nasopharyngeal Cancer
Uploaded by
mynoidanh19Copyright:
Available Formats
NASOPHARYNGEAL
CARCINOMA (NPC)
Identitas Pasien
Nama: Ibu TH
Umur: 48 tahun
Pekerjaan: -
Pendidikan: -
Tanggal Periksa: Poli THT RSUDSH
Purworejo, 5 Desember 2013
Anamnesis
Keluhan Utama:
Pasien kontrol ke Poli RSUDSH tanggal 5
desember 2013 karena post biopsy 2 minggu
sebelum periksa.
Saat ini terdapat benjolan pada leher sebelah
kanan ukuran 4x3x3 cm pada leher, keras,
tidak mobile.
Riwayat Penyakit Sekarang
Pasien dilakukan biopsy 2 minggu sebelum
periksa
Saat ini hanya terdapat keluhan benjolan pada
leher. Sesak (-), dysphagia (-).
Sebelum biopsi OS merasakan sering pilek,
cairan jernih, terkadang berdarah, terutama pada
hidung kanan. Bersin (-), nasolalia (+), rhinalgia (-
), foetor (+), hyposmia (+)
Os juga terkadang merasakan berdenging pada
telinga. Otorrhea (-/-), deafness (-/-), otalgia (-/-),
itching (-/-)
Tidak ada keluhan penurunan berat badan,
pengelihatan ganda, nyeri kepala, sulit
menelan, kelumpuhan bahu, sulit bicara,
serak, sesak, batuk darah.
RPD: Riwayat penyakit serupa (-), riwayat
pengobatan (+: obat warung),
RPK: Riwayat keganasan keluarga (-),
keluhan serupa (-)
Riwayat Alergi: (-)
Pemeriksaan Fisik
Keadaan Umum: Compos Mentis
Vital Sign: Tensi: 100/70 RR:
20x/m
Nadi: 74x/m Suhu: 36.7 C
Kepala: Conjunctiva anemis (-/-), Ikterik (-/-)
Leher: Terdapat benjolan 4x3x3 cm pada Lnn
Coli Dextra, keras, tidak mobile, batas tidak
tegas
Paru: Tidak dilakukan
Jantung: Tidak dilakukan
Anggota gerak: Tidak dilakukan
No Pemeriksaa
n Telinga
Telinga Kanan Telinga Kiri
1 Tragus Nyeri Tekan (-),
Edema (-)
Nyeri Tekan (-), Edema (-)
2 Daun
Telinga
Bentuk dan ukuran
dbn, hematoma (-),
nyeri tarik (-)
Bentuk dan ukuran dbn,
hematoma (-), nyeri tarik (-)
3 Liang
Telinga
Serumen (-),
Hiperemis (-), furunkel
(-), Edema (-),
otorrhea (-)
Serumen (-), Hiperemis (-),
furunkel (-), Edema (-), otorrhea (-)
4 Membran
Timpani
Retraksi (-), Bulging (-
), hiperemis (-),
edema (-), perforasi (-
), cone of light (+)
Retraksi (-), Bulging (-), hiperemis
(-), edema (-), perforasi (-), cone
of light (+)
Pemeriksaan hidung
Pemeriksaan hidung Hidung Kanan Hidung Kiri
Hidung Luar Bentuk normal,
hiperemis (-). Nyeri
tekan (-), deformitas (-)
Bentuk normal,
hiperemis (-). Nyeri
tekan (-), deformitas (-)
Rhinoskopi anterior
Vestibulum nasi Normal, ulkus (-) Normal, ulkus (-)
Cavum nasi Bentuk normal, mukosa
pucat (-), hiperemis (-)
Bentuk normal, mukosa
pucat (-), hiperemis (-)
Meatus nasi media Mukosa hiperemis,
sekret (+), bening,
massa (-)
Mukosa hiperemis,
sekret (+), bening,
massa (-)
Konka nasi inferior Edema (-), mukosa
hiperemis (-)
Edema (-), mukosa
hiperemis (-)
Septum nasi Deviasi (-), perdarahan
(-), ulkus (-)
Deviasi (-), perdarahan
(-), ulkus (-)
Pemeriksaan Tenggorokan
Bibir Mukosa bibir basah, pucat
Mulut Mukosa mulut basah berwarna merah
muda
Lidah Permukaan lidah pink, saat dijulurkan
simetris
Gigi Karies (+), tambalan (-)
Uvula Simetris
Palatum Mole Simetris, massa (-), bercak putih (-)
Faring Hiperemis (-)
Tonsila Palatina Hipertrofi (-)
Nasopharynx
Dinding Belakang
Choanae
Muara Tuba eustachii Tidak diperiksa
Adenoid
Tumor
Laryngopharynx
Dinding Belakang
Parapharynx Tidak diperiksa
Larynx
Epiglotis
Aritenoid
Plica Vocalis
Gerakan Plica vocalis Tidak diperiksa
Tumor
Subglotis
Trachea
Pemeriksaan Penunjang
Pemeriksaan Pathology Anatomy
Makroskopik:
Kiri: Jaringan pecah belah sebanyak 0.5 cc berwarna
coklat kehitaman, semua cetak (A)
Kanan: Jaringan pecah belah sebanyak 0.5 cc
berwarna coklat kehitaman, semua cetak (B)
Mikroskopik
A dan B kedua sediaan menunjukkan jaringan
nasofaring dengan diantara haringan limfoid
ditemukan sarang kecil karsinoma sel skuamosa
tanpa keratinisasi
Kesimpulan
Nasofaring: Non Keratinizing Carcinoma (WHO tipe II)
Diagnosis
Non Keratinizing Carcinoma of Nasopharynx
Plan
Rujuk RSUP dr Sardjito
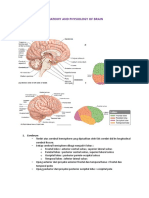
Anatomy
Anatomy
Anatomy
Foramen
lacerum
Foramen
spinosum
Foramen
ovale
Foramen
rotundum
CT anatomy
A nasopharyngeal carcinoma (NPC) is the
most common primary malignancy of the
nasopharynx.
It is of squamous cell origin and some types of
which are strongly associated with Epstein
Barr virus (EBV).
Epidemiology
Nasopharyngeal carcinomas account for
approximately 70% of all primary malignancies
of the nasopharynx.
Although it is rare in western populations, it is
one of the most common malignancies
encountered in Asia, especially China.
Department of Radiotherapy,
PGIMER, Chandigarh
Incidence
Incidence: Sex
Etiology
Normal Epithelium
Low Grade Dysplasia
High Grade Dysplasia
Invasive Carcinoma
Metastatic Carcinoma
P53 Mutation
Gain Chromosome 12
Deletion 11 and 13
Deletion of Chromosomes 3p and 9p
Inactivation of Chromosome p14, 15 and 16
EBV infection
Risk
Environmental
Viruses
EBV- well documented viral fingerprints in tumor
cells and also anti-EBV serologies with WHO
type II and III NPC
HPV - possible factor in WHO type I lesions
Nitrosamines - salted fish
Others - polycyclic hydrocarbons, chronic
nasal infection, poor hygiene, poor ventilation
Clinical Manifestation
Clinical presentation, and often only when the
tumor has grown significantly in size and has
invaded adjacent structures.
Actual presentation is often delayed until more
sinister signs are evident including nodal
masses in the neck (most common), cranial
nerve palsies, tinnitus, headache or even
diplopia and proptosis.
Cervical adenopathy 60%
Epistaxis & Nasorespiratory symptoms
Audiological symptoms 30%
Neurological symptoms 20%
Cervical adenopathy
NPC has a tendency for early lymphatic
spread.
Retropharyngeal node of Rouviere is the
first echelon node.
Commonest first palpable node is the J.D.
node and the apical node under
sternomastoid muscle.
Epistaxis & Nasal symptoms
Commonly seen in advanced NPCs.
Complete nasal obstruction is a late
presentation.
Ozaena occurs as a result of tumour
necrosis.
Tinnitus & Aural symptoms
Serous otitis media is common
Acute otitis media
Aural block
Tinnitus
Nerve palsies
All cranial nerves can be affected
Frequently involved are iv, v, vi, ix, & x.
Nerves ix & x are invariably involved together.
Nerves of the ocular muscles are the next
commonly affected.
Pain & Headache
This is an ominous symptom
Severe pain is hallmark of terminal disease.
Signifies tumour erosion into skull base.
If accompanied by trismus,the disease is
very advanced and has extended into
pterygopalatine fossa.
Metastasis
Tumors arising from fossa of Rosenmuller
frequently extend to paranasopharyngeal space,
then along trigeminal nerve
Often metastasizes to regional nodes; common
presentation is unilateral cervical
lymphadenopathy; 25% have bilateral nodal
metastases
May have distant metastases to bones
After radiation therapy, risk of 0.4% of subsequent
carcinoma in nasal cavity of nasopharynx;
differentiate from recurrence based on > 5 year
delay, different histology, EBV negative
Local Spread
Nasal cavity & PNS
Orbital invasion
Base of Skull, Clivus
Sphenoid sinus
Cavernous Sinus
Lateral Parapharyngeal space
Middle ear cavity
Oropharynx (tonsillar pillars)
C1 vertebrae
Nodal Spread
Cranial Nerve involvement
0
5
10
15
20
25
30
35
40
45
50
I II III IV V VI VII VIII IX X XI XII
Lederman et al Leung et al
Diagnosis
Diagnosis is usually achieved with endoscopic
guided biopsy. A minority of patients have
submucosal disease, with normal appearing
overlying mucosa. MRI is then essential in
guiding biopsy.
blind biopsies, particularly in fossa of
Rosenmuller, can also be done(70% sensitive)
Nasopharyngeal biopsy
Methods:
1. Transnasal
a. Blind
b. Post. Mirror rhinoscopy
c. Endoscopy rigid and flexible
2. Transoral
a. Yankauer speculum
b. Rigid endoscopy
Laboratory: IgG against early EBV antigen is
suggestive, but has 30% false positives; IgA
against viral capsid antigen has 9-18% false
positives
Immunology
EB virus antigens
a. Viral capsid antigen (VCA)
b. Early antigen (EA)
c. Nuclear antigen
Serological markers
IgA and IgG to viral capsid antigen
IgA and IgG to early antigen
Antibody to nuclear antigen
Antibody dependent cellular cytotoxic
antibodies.
Radiographic features
Imaging is crucial in delineating the extent of
local tumor extension, as well as detecting
nodal metastases which are present in the
vast majority of patients at the time of
diagnosis (75-90%).
Unfortunately imaging in isolation is not only
unable to distinguish between the various
types of nasopharyngeal carcinoma, but also
unable to distinguish NPCs from other primary
malignancies of the nasopharynx.
CT Findings
Mildly enhancing off-midline nasopharyngeal
mass
Metastatic nodes often large, necrosis
Retropharyngeal nodes often subtle on imaging
as appears isodense to muscle
Bone CT: May show destruction of clival cortex
or pterygoid plates
MR Findings
T1WI
Asymmetric mass, hypo- to isointense to muscle
Sensitive for infiltration of parapharyngeal fat
Marrow involvement results in low T1 signal
T2WI
Moderate hyperintensity of NPC compared to muscle
Obstructed middle ear secretions markedly hyperintense
T1WI C+ FS
Best illustrates infiltration of deep face, intracranial, and
cavernous sinus disease
Coronal images aid in this evaluation
Mild homogeneous tumor enhancement
(Left) Axial T7WI MR shows isointense right lateral pharyngeal recess NPCa (arrow).
Note low signal in pterygoid plates (open arrow) & right clivus (curved arrow) due to
bony tumor invasion.
(Right) Axial T2WI MR reveals low signal intensity mass in lateral pharyngeal recess,
invading prevertebral muscles (arrow), right pterygoid plates & parapharyngeal space
(open arrow). CurVE'd arrow: RPS node.
(Left) Axial T7 C+ MR shows a large, invasive right NPCa. Tumor has invaded
prevertebral muscles (arrow), nasopharyngeal carotid space (open arrow) and
parapharyngeal space
(curved arrow).
(Right) Coronal T7 C+ MR in same patient reveals NPCa has destroyed large area of
skull base bone (arrows) surrounding the foramen ovale. Opposite normal foramen ovale
has V3 traversing it (open arrow).
(Left) Axial T2WI MR demonstrates a small, minimally invasive NPCa (arrow). Despite
its small size, nodal metastatic tumor is already visible in the contralateral lateral
retropharyngeal node (open arrow).
(Right) Coronal T7 C+ MR in a patient with NPCa reveals bulky bilateral cervical
adenopathy
(arrows). Notice that a smaller, right lateral retropharyngeal node can also be seen
near skull base (open arrow).
Nuclear Medicine Findings
PET/CT
Markedly FDG-avid tumor, nodes, and
metastases
If small primary, can miss with thick slices due to
brain FDG uptake
Need thin collimation, review in coronal plane
MR still necessary for skull base & intracranial
disease
Imaging Recommendations
Best imaging tool
MR is recommended by AJCC for staging
Most sensitive for skull base and intracranial tumor
spread
More sensitive than clinical exam/US/CT for detection
of retropharyngeal nodes
CECT is alternative choice
PET/CT often obtained if N2/3 disease at staging
or recurrent tumor
Staging
Several staging systems are in use:
Complex anatomy and spread patterns
Lack of international consensus:
Separate Chinese, Hong Kong and American staging
systems
Systems available:
Fletcher (1967)
Hos staging (1978)
IUAC (1988)
Huaqing staging (1994)
AJCC (revised in 2010)
AJCC Nasopharynx Staging
(2010)
Tumor Stage (T) Nodal Stage (N)
T1: Confined to nasopharynx or
extension to oropharynx or nasal
cavity
N1: 1 unilateral metastasis 6 cm
&/or unilateral/bilateral
retropharyngeal nodes 6 cm
T2: Extension to parapharyngeal fat N2: Bilateral nodal metastases 6
cm
T3: Clivus or paranasal sinus
invasion
N3a: Nodal metastases > 6 cm
T4: Intracranial spread, cranial
nerve, orbit, hypopharynx, masticator
space
N3b: Nodal metastasis to
supraclavicular fossa
Distant Metastasis (M) NOTE: This nodal staging is unique
to NPC
M0: No distant metastasis, M1:
Distant metastasis
AJCC
Some authors consider carcinomas to be of two types:
Keratinizing
Non keratinizing
Others consider carcinomas to be of 4 types:
Keratinizing Squamous
Non Keratinizing Squamous
Lymphoepithelioma
Undifferentiated carcinomas
Pathology
Nasopharyngeal carcinomas are divided into
three types (WHO)
type I - keratinizing squamous cell carcinoma
type II - non-keratinizing squamous cell
carcinoma (aka lymphoepithelioma)
type III - undifferentiated carcinoma
All three types express cytokeratin, and types
II and III have incorporation of the EBV into
their genome, and circulating IgA antibodies to
EBV in peripheral blood.
Keratinizing squamous cell carcinoma of
nasopharynx
Also called WHO type 1
Minority of nasopharyngeal carcinomas
Often EBV negative, older age group
5 year survival is close to 0%
Treatment: dont respond to radiotherapy, but tend to
remain localized
Micro: squamous differentiation with intercellular
bridges or keratinization in most of tumor; rarely
adenoid or acantholytic forms that mimic
adenocarcinoma
Nonkeratinizing nasopharyngeal carcinoma-
differentiated
Also called WHO type 2
Rare in childhood
5 year survival 35-50%
Treatment: variably radiosensitive, may metastasize to
regional lymph nodes
Micro: cells lack squamous differentiation but have variable
levels of maturation; cells are stratified with well defined cell
margins that interdigitate in a pavement stone pattern; no
mucin or glandular differentiation; variable chronic
inflammatory cells
Positive stains: CK5/CK6, CK8, CK13, CK14, CK19
Negative stains: CK4, CK7
Nonkeratinizing nasopharyngeal carcinoma-undifferentiated
Also called WHO type 3
Very rare in US, common in Taiwan and China (EBV endemic areas)
Often called lymphoepithelioma, although lymphocytes are not neoplastic
and some cases lack lymphocytes
Bimodal age distribution (teens, 50+); in Taiwan, median age is 58 years
(range 36-75 years); 2/3 male
5 year survival after radiation therapy alone is based on stage--confined to
nasopharynx (stage I): 50-60%; cervical node involvement (stage II): 20-
30%; invasion of surrounding structures (stage III): 5-30%
Survival does not vary based on Regaud or Schminke patterns below
Tends to metastasize to regional lymph nodes
Treatment: supervoltage radiotherapy and cis-platinum based
chemotherapy (70-90% 5 year survival overall)
Micro: syncytial arrangement of relatively uniform cells with indistinct cell
margins; cells have vesicular nuclei and prominent nucleoli; may have
spindle cells and scattered effete (worn out) cells with shrunken,
hyperchromatic nuclei that are more variable than sinonasal
undifferentiated carcinoma; usually (but not always) non-neoplastic
lymphocytic infiltrate (often T cells) with plasma cells, eosinophils and
macrophages; patterns below may be mixed; no necrosis
Nasopharyngeal nonkeratinizing carcinoma, differentiated type. This carcinoma is
characterized by the presence of interconnecting cords of neoplastic cells. B, at
higher magnification the cellular infiltrate of the nasopharyngeal nonkeratinizing
carcinoma, differentiated type shows the absence of keratinization
Most cases in childhood and adolescence are type 3, with a
few type 2 cases.
Type 2 and 3 are associated with elevated Epstein-Barr virus
titers, but type 1 is not
Types 2 and 3 may be accompanied by an inflammatory
infiltrate of lymphocytes, plasma cells, and eosinophils, which
are abundant, giving rise to the term lymphoepithelioma.
Two histological patterns may occur:
Regaud type, with a well-defined collection of epithelial cells
surrounded by lymphocytes and connective tissue, and
Schmincke type, in which the tumor cells are distributed
diffusely and intermingle with the inflammatory cells. Both
patterns may be present in the same tumor.
Endemic NPC
Known to occur in China, Hong Kong, South Eastern Asia,
Greenland
Associated with EBV virus infection
Present a decade younger.
Associated with undifferentiated carcinoma ( WHO II and III)
Associated with more advanced disease at presentation
Nodal stage also more advanced and more frequently involved.
Both chemo and radio sensitive
Histologically more vascularized (Better Rx response)
Greater % of cell in the growth fraction.
Better loco regional control and survival than sporadic variants.
Several markers for predicting biological behavior
D/D
Adenoidal Benign Lymphoid Hyperplasia
Children and teens typically have large adenoids
Reactive hypertrophy seen in HIV patients
Symmetric enlargement without infiltration of
adjacent tissues
Nasopharyngeal Non-Hodgkin Lymphoma
Midline symmetric mass, deep infiltration to
prevertebral muscles
In clivus, tends to expand rather than infiltrate
Nasopharyngeal Minor Salivary Gland
Malignancy
Uncommon primary tumor
May be small primary with extensive infiltration
Associated nodal metastases uncommon
Pituitary Macroadenoma
Large sella mass extending through sphenoid to
nasopharynx
Expansion of sella is key imaging finding
Pharyngeal Mucosal Space Sarcoma
Rare; more common differential in children
Submucosal, aggressive mass
Treatment
Treatment for stage I NPC
Patients with stage I disease should be treated
with RT alone.
IMRT alone is effective at treating over 90% of
patients with stage I NPC
Treatment for stage II NPC
the outcomes in patients with stage II disease
have been reported to be less favorable
The Society of Clinical Oncology terminology,
the European Head and Neck Society
European Society for Medical Oncology
European Society for Radiotherapy and
Oncology Clinical Practice Guidelines also
considered CCRT for stage II NPC as level I
evidence with a grade B recommendation
Treatment for stages IIIIVb NPC
Role of exclusive concurrent
chemoradiotherapy
The current standard of care for locoregionally
advanced (AJCC stages IIIIVb) NPC is
cisplatin-based CCRT
31% improvement in 3-year OS compared to
RT alone using concurrent RT and high-dose
cisplatin followed by adjuvant cisplatin and
fluorouracil
they were accompanied by severe toxicity,
including mucositis and bone marrow
suppression.
the dose of cisplatin during the concurrent
phase of CCRT had a significant impact on
locoregional control, while additional adjuvant
chemotherapy with a fluorouracil-containing
combination contributed to improved distant
control
No other regimens have been reported to be
as effective as cisplatin and fluorouracil for
treating NPC in an adjuvant setting
The NCCN guidelines currently include
induction + CCRT as an option (category 3).
Adjuvant chemotherapy is poorly tolerated,
and compliance is limited because patients
suffer substantial toxicities from CCRT
Compared with adjuvant chemotherapy,
induction chemotherapy appears to be better
tolerated, even with more aggressive
regimens.
Treatment for stage IVc NPC
Patients who present with distant metastasis
(stage IVc disease) might account for
approximately 10% of all NPC cases in the
endemic area of NPC
in a study of 125 patients with stage IVc NPC,
Yeh et al found improved 1-year OS in patients
receiving RT alone versus chemotherapy
alone or versus no treatment (48% vs 36% vs
25%, respectively), despite using conventional
RT
In light of the poor prognosis in stage IVc NPC,
treatment has conventionally been palliative in
nature.
It is reasonable to assume that a combination
of chemotherapy and RT might have potential
survival benefits for selected patients with
stage IVc NPC
Treatment for reccurent NPC
about 10% of patients still develop recurrent
disease either in the neck or at the primary site
The options include brachytherapy, external
RT, stereotactic
radiosurgery, nasopharyngectomy, and microwave
coagulation therapy, either alone or in different
combinations
Salvage nasopharyngectomy carried out for 246
selected patients showed a 5-year local control of
disease of 74% and the 5-year disease-free
survival was 56%
Endoscopic nasopharyngectomy is a choice
for recurrent NPC with central roof or floor
lesions with minimal lateral extension.
Hua et al reported the long-term treatment
outcome of 151 recurrent NPC patients treated
with salvage IMRT. The 5-year local control
rate and OS for restage I, II, III, and IV were
80.0%, 85.0%, 80.0%, 78.7% and 71.4%,
62.9%, 35.5%, 30.2%
When the recurrent disease is only in the neck
lymph nodes, salvage surgery is the optimal
treatment method. Radical neck dissection is
currently an accepted surgical management
for recurrent nodal disease in patients with
NPC, with well-proven efficacy and safety
Novel systemic therapy
Epidermal growth-factor receptor (EGFR) and
vascular endothelial growth-factor receptor
(VEGFR) targeted therapies have been
clinically studied in NPC patients.
Cetuximab is a chimeric anti-EGFR
immunoglobulin G
1
monoclonal antibody, the
first EGFR inhibitor that is clinically tested to
treat NPC
A phase II study by Ma et al recently evaluated
the feasibility of adding cetuximab to current
cisplatin and IMRT in locoregionally advanced
NPC
Several phase I and II studies that have
generated EBV-Specific Cytotoxic T Cells for
posttransplant lymphoproliferative disorders have
shown potential efficacies against NPC
Autologous EBV-transformed B-lymphoblastoid
cell line (LCL) reactivated T cells were generated
in vitro and used to treat advanced cases of NPC.
Smith et al recently reported the effectiveness of
a phase I study involvingadenoviral-based EBV
vaccine (referred to as AdE1-LMPpoly)-stimulated
T-cell immunotherapy for EBV-associated
recurrent and metastatic NPC.
Irradiation with protons instead of the currently
used photons generally results in a
significantly lower physical dose in the
coirradiated healthy tissues, due to its superior
beam properties
Dose response
Significant dose response relationship exists.
Several series demonstrate that an increased-
dose leads to better survival
Doses of 90 Gy delivered by boost increase the
local control and the distant metastasis free rate
significantly over doses > 70 Gy
Price however paid in increased morbidity
Local recurrence rate reduced with the use of
larger fields (Field size more than 250 cm
2
associated with a doubling of local control as
compared to field size of 100 cm
2
)
Dose-response
0%
10%
20%
30%
40%
50%
60%
70%
80%
90%
100%
50 - 60 Gy 60 - 67.5 Gy > 67.5 Gy
T1
T2
T3
T4
Doses used
Radical radiotherapy:
60 66 Gy in 2 Gy per fraction over 6 6 weeks
Higher dose can be given with more conformal techniques:
ICBT
IMRT
3 DCRT
In our patients with poor nutrition, advanced disease and
absence of individualized care split course radiotherapy is an
alternative
35 Gy in 15 #
25 30 Gy in 10 15 # after 2-3 weeks
Palliative radiotherapy:
30 Gy / 10#
20 Gy / 5#
800 -1000 cGy single fraction
Treatment
Surgical management
Mainly diagnostic - Biopsy
consider clinic bx if cooperative patient
must obtain large biopsy
clinically normal NP - OR for panendo and bx
Surgical treatment
primary lesion
regional failure with local control
ETD
Treatment
Surgical management
Primary lesion
consider for residual or recurrent disease
approaches
infratemporal fossa
transparotid temporal bone approach
transmaxillary
transmandibular
transpalatal
Prognostic factors
Most important stage.
Parapharyngeal extension is associated with a poorer prognosis.
A Chinese series found that 4
th
cranial nerve involvement poor
prognosis.
Nodal disease status:
Bilateral cervical lymphadenopathy
Supraclavicular lymphadenopathy
Lymph node fixity
Lymphoepithelioma histology: better prognosis
Undifferentiated histology: better prognosis
Molecular markers:
Ki -67 over expression
P 53
E cadherin expression
JCO 2006 Dec.1
EBV and NPC prognosis
Key facts
Terminology
Nasopharyngeal carcinoma (NPC)
Mucosal tumor of lateral pharyngeal recess (fossa
of Rosenmller), strongly associated with EBV
infection
Imaging
MR best demonstrates parapharyngeal fat, skull
base infiltration, & intracranial tumor
Nodal disease in 90% at presentation:
Retropharyngeal, levels II & V most common
Metastatic nodes often large necrosis
Clinical Issues
Peak incidence: 40-60 years
Pediatric NPC rare; most often undifferentiated
NK
Bloody nasal discharge or epistaxis
50-70% present with mass from metastatic nodes
Nitrosamines - salted fish
Serous otitis from eustachian tube obstruction
Nonkeratinizing NPC has 5-year survival ~ 75%
Keratinizing NPC has 5-year survival 20-40%
BSCC generally poor prognosis
Top Differential Diagnoses
Adenoidal benign lymphoid hyperplasia
Nasopharyngeal non-Hodgkin lymphoma
Nasopharyngeal minor salivary gland malignancy
Pituitary macroadenoma
Pathology
25% keratinizing NPC (previously type I)
Nonkeratinizing NPC (NK NPC)
Strongly associated with EBV
15% differentiated (previously type II)
60% undifferentiated (previously type III)
Rarely basaloid squamous cell carcinoma
You might also like
- Anatomi OtakDocument14 pagesAnatomi Otakaditz50% (2)
- Buku Rancangan Pengajaran (BRP)Document19 pagesBuku Rancangan Pengajaran (BRP)AnnissanvlNo ratings yet
- Radiographic Positioning Facial BoneDocument51 pagesRadiographic Positioning Facial BoneFatma MahechiNo ratings yet
- CA PenisDocument54 pagesCA PenisCemel Mayla AfifyNo ratings yet
- Kuliah Soft Tissue DrpriDocument55 pagesKuliah Soft Tissue Drpriputra imanullahNo ratings yet
- DETEKSI GALACTIN-3Document6 pagesDETEKSI GALACTIN-3Nurjannah Muhdi100% (1)
- MAKSILLECTOMY REVIEWDocument20 pagesMAKSILLECTOMY REVIEWIgnatius Aldo WinardiNo ratings yet
- FRAKTUR MAKSILOFASIALDocument13 pagesFRAKTUR MAKSILOFASIALGina Irene IshakNo ratings yet
- Referat Tumor MediastinumDocument24 pagesReferat Tumor MediastinumFahmi HidayatiNo ratings yet
- Knee DislocationDocument9 pagesKnee DislocationniaasetaNo ratings yet
- Dena - TUMOR MALIGNA Melanoma MalignaDocument34 pagesDena - TUMOR MALIGNA Melanoma MalignabulanNo ratings yet
- Massa MediastinumDocument19 pagesMassa MediastinumOchien Ama Ajah YochieNo ratings yet
- Tyroid UhDocument10 pagesTyroid UhIinayati Nur IndhtanNo ratings yet
- PENGOBATAN AENDocument6 pagesPENGOBATAN AENMohd Faie RamliNo ratings yet
- Congenital HydrocephalusDocument12 pagesCongenital HydrocephalusRMRNo ratings yet
- PleurodesisDocument59 pagesPleurodesisErika Putting RozitaNo ratings yet
- Deep Vein Thrombosis (DVT)Document2 pagesDeep Vein Thrombosis (DVT)icigajahNo ratings yet
- CT Scan Kepala & Vertebrae - Nanda Melsi - Kel. 15 2019Document31 pagesCT Scan Kepala & Vertebrae - Nanda Melsi - Kel. 15 2019Elda LizmaNo ratings yet
- Sap NHLDocument12 pagesSap NHLervina fahnulmaharaniNo ratings yet
- Template Bacaan MriDocument9 pagesTemplate Bacaan MriRidho Frihadananta WardhanaNo ratings yet
- Presentasi Hasil Akhir PrabudiDocument68 pagesPresentasi Hasil Akhir PrabudiPrabudi DurazakNo ratings yet
- BLS Dan ACLS (Firman)Document22 pagesBLS Dan ACLS (Firman)floraNo ratings yet
- Tumor Otak. Indah (Recovered)Document21 pagesTumor Otak. Indah (Recovered)indahNo ratings yet
- CT AbdomenDocument50 pagesCT AbdomenFitria Ummu HabibahNo ratings yet
- DR Budi Setiawan - Emergency OncologyDocument24 pagesDR Budi Setiawan - Emergency OncologyPriza RazunipNo ratings yet
- SOP Cervical Open MouthDocument2 pagesSOP Cervical Open MouthMohammad Rozaq IlmiNo ratings yet
- Myiasis Hidung FixDocument17 pagesMyiasis Hidung FixdhinialfiandariNo ratings yet
- MEDIASTINUMDocument7 pagesMEDIASTINUMMia AndikaNo ratings yet
- Salt TriageDocument8 pagesSalt TriageemrithadellaNo ratings yet
- Materi Belajar CT ScanDocument42 pagesMateri Belajar CT ScanRetno AptriwinasihNo ratings yet
- TNBC-KANKERDocument4 pagesTNBC-KANKERganesha translatesNo ratings yet
- Atypical Facial PainDocument8 pagesAtypical Facial Painsalsabila ikhdaNo ratings yet
- Review of Small-Bowel Obstruction: The Diagnosis and When To WorryDocument33 pagesReview of Small-Bowel Obstruction: The Diagnosis and When To WorrySandra MignonNo ratings yet
- PPK Tindakan Rekonstruksi ACLDocument2 pagesPPK Tindakan Rekonstruksi ACLsitihajarNo ratings yet
- NB KarakteristikDocument8 pagesNB KarakteristikLeni YustikaNo ratings yet
- Analisis Masalah Post CraniotomyDocument7 pagesAnalisis Masalah Post CraniotomymistkanurNo ratings yet
- PPK THT Banyaaakk FixDocument134 pagesPPK THT Banyaaakk FixIsti RizkyNo ratings yet
- Panduan Praktik Klinik Rs NHDocument25 pagesPanduan Praktik Klinik Rs NHMuhamad Lucky N. PrameswaraNo ratings yet
- Pemeriksaan PayudaraDocument9 pagesPemeriksaan PayudaraDanny SanjayaNo ratings yet
- SOAL OSCE Bedah SarafDocument10 pagesSOAL OSCE Bedah SarafTri PutraNo ratings yet
- Batu Saluran KemihDocument42 pagesBatu Saluran KemihRizki Khoirun HafidahNo ratings yet
- NeuroradiologiDocument136 pagesNeuroradiologiNadya Aprilianti100% (1)
- NEOPLASMA RADIODIAGNOSTIKDocument133 pagesNEOPLASMA RADIODIAGNOSTIKFiqri Novian100% (1)
- Airway Management RevisiDocument100 pagesAirway Management RevisiFahmi Nur ZamanNo ratings yet
- Radioterapi - KNFDocument28 pagesRadioterapi - KNFParamitha AdriyatiNo ratings yet
- Otot Dan InervasiDocument19 pagesOtot Dan InervasiElliNo ratings yet
- AmyloidosisDocument27 pagesAmyloidosisYoanneveline TanakNo ratings yet
- 1 - 22 - 250Teknik-Pemeriksaan Radiologi Untuk Deteksi PDFDocument4 pages1 - 22 - 250Teknik-Pemeriksaan Radiologi Untuk Deteksi PDFChe CastroNo ratings yet
- AMPUTASI EKSTREMITAS BAWAHDocument52 pagesAMPUTASI EKSTREMITAS BAWAHMuhammad RezaNo ratings yet
- PDT-RBAc Menginduksi Kematian Sel HeLaDocument7 pagesPDT-RBAc Menginduksi Kematian Sel HeLanikkitaihsanNo ratings yet
- Hub Dokter-PasienDocument87 pagesHub Dokter-PasienDita AngelinaNo ratings yet
- Hip DislocationDocument21 pagesHip DislocationgabriellafelisaNo ratings yet
- KNF-16Document25 pagesKNF-16ZulfiqarMuchsinNo ratings yet
- KNF perlu diketahui dokter umumDocument34 pagesKNF perlu diketahui dokter umumYusnida RahmawatiNo ratings yet
- Karsinoma Nasofaring RefratDocument16 pagesKarsinoma Nasofaring RefratMonaliekaNo ratings yet
- Lapsus CA NasofaringDocument34 pagesLapsus CA NasofaringEmma RahmadaniaNo ratings yet
- LBM 4 THT-KLDocument30 pagesLBM 4 THT-KLMasludi S SopriyadiNo ratings yet
- Dr. Bastu Edo, SP - THT-KLDocument51 pagesDr. Bastu Edo, SP - THT-KLedohermendy_32666011No ratings yet
- Preskas THTDocument14 pagesPreskas THTAlindina AnjaniNo ratings yet
- Laporan Kasus CA LaringDocument19 pagesLaporan Kasus CA LaringWyendae CliquersNo ratings yet
- Laporan Kasus Herpes ZosterDocument8 pagesLaporan Kasus Herpes ZosterSonny WijanarkoNo ratings yet
- Refleksi Kasus TonsilitisDocument46 pagesRefleksi Kasus TonsilitisSonny WijanarkoNo ratings yet
- Facial Nerve ParalysisDocument18 pagesFacial Nerve ParalysisSonny WijanarkoNo ratings yet
- ChronicsuppurativeotitismediaDocument30 pagesChronicsuppurativeotitismediaSonny WijanarkoNo ratings yet
- Laporan Kasus Herpes ZosterDocument8 pagesLaporan Kasus Herpes ZosterSonny WijanarkoNo ratings yet
- Refleksi Kasus ChromoblastomycosisDocument4 pagesRefleksi Kasus ChromoblastomycosisSonny WijanarkoNo ratings yet
- Laporan Kasus Herpes ZosterDocument8 pagesLaporan Kasus Herpes ZosterSonny WijanarkoNo ratings yet
- Diskusi Seleksi PaDocument2 pagesDiskusi Seleksi PaSonny WijanarkoNo ratings yet