Professional Documents
Culture Documents
Ol 5 4 1250 PDF
Uploaded by
Nisa DinanaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ol 5 4 1250 PDF
Uploaded by
Nisa DinanaCopyright:
Available Formats
ONCOLOGY LETTERS 5: 1250-1252, 2013
1250
Acute liver failure associated with diffuse
liver infiltration by metastatic breast
carcinoma: A case report
SUCHANAN HANAMORNROONGRUANG and NAPAKORN SANGCHAY
Department of Pathology, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok 10700, Thailand
Received September 24, 2012; Accepted December 11, 2012
DOI: 10.3892/ol.2013.1165
Abstract. Diffuse parenchymal metastasis is an unusual
pattern of liver metastasis that is capable of causing liver
failure. In the present study, the authors describe malignant
infiltration of the liver by primary breast carcinoma in an
autopsy of a 49-year-old female who had a rapid onset of
liver failure and died after three weeks. Ultrasonography and
computed tomography (CT) scans of the abdomen, as well as
macroscopic examination, failed to detect liver metastasis;
while microscopic examination revealed diffuse tumor cells
with a loss of E-cadherin expression infiltrating into the liver
parenchyma. The prognosis of liver failure associated with
malignant infiltration is extremely poor; the survival time
of patients is extremely low. Liver biopsy may be the most
efficient technique for confirming the diagnosis during the
patient's life.
Introduction
Although the liver is a common target for metastasis, acute
or fulminant liver failure due to metastasis is a rare occurrence(17). Diffuse parenchymal metastasis is a rare pattern
of liver metastasis that is correlated with hepatic failure and
an extremely poor prognosis(18). Unlike the usual patterns
of liver metastasis, radiological studies are typically not able
to detect this type of pattern(1,35,7). Therefore, metastasis is
frequently diagnosed by autopsy(3). In the present study, the
authors describe a case of acute liver failure correlated with
diffuse liver infiltration by metastatic carcinoma in a 49-yearold female with a history of breast cancer.
Correspondence
to: Dr Suchanan Hanamornroongruang,
Department of Pathology, Faculty of Medicine, Siriraj Hospital,
Mahidol University, 2 Prannok Road, Bangkoknoi, Bangkok 10700,
Thailand
E-mail: suchananice@hotmail.com
Key words: diffuse parenchymal metastasis, acute liver failure,
hepatic infiltration, liver metastasis, metastatic breast cancer
Case report
Clinical summary. A 49-year-old Thai female was admitted to
hospital due to a high grade fever, jaundice and abdominal pain
in the right upper quadrant. Four weeks prior to admission, the
patient suffered from malaise, anorexia and weight loss. An
initial investigation revealed that the patient had anemia (Hct,
23%) and abnormal liver function test results (total bilirubin,
75.24mol/l; direct bilirubin, 34.2mol/l; AST, 250U/l;
ALT, 63U/l; ALP, 198U/l). The patient received treatment
for chronic cholecystitis and hepatitis; however, the symptoms
progressed and the patient developed thrombocytopenia and
coagulopathy. The liver function test results also worsened
(peak values: total bilirubin, 890.91mol/l; direct bilirubin,
598.5mol/l; AST, 1152U/l; ALT, 114U/l; ALP, 845U/l;
GGT, 727U/l), while both ultrasonography and computed
tomography (CT) scans of the abdomen were not able to detect
any specific hepatic lesions. No evidence of viral hepatitis or
any identifiable source of infection was observed. The patient's
condition deteriorated further; hepatic encephalopathy developed and the patient died within the third week following
the onset of acute hepatic failure. The patient had a history
of breast carcinoma stageI and had been treated by modified
radical mastectomy (MRM), and had remained diseasefree
for 10years following treatment.
Pathological findings. The gross appearance of the liver
revealed that the patient had hepatomegaly (2,150gm). The
liver capsule was smooth, the cut surfaces of which showed
non-homogeneous dark brown and yellow tissue and no massforming lesions (Fig.1A). An ill-defined yellowbrown nodule
(4cm in diameter) was observed at the pancreas, and multiple
small yellowbrown nodules were found at the pleural surface
and parenchyma of both lungs. Other abnormal gross findings
included splenomegaly and pulmonary congestion. A previous
surgical scar from the MRM was detected without any abnormality in both breasts or axillary regions.
Microscopic examination revealed diffuse infiltration of
the liver parenchyma by pleomorphic cells with some glandular formation (Fig.1B). Extensive necrosis of hepatocytes
was noted. The tumor cells were positive for CK7, ER and PR,
while negative for CK20 and TTF-1. These results support the
diagnosis of primary breast carcinoma.
HANAMORNROONGRUANG and SANGCHAY: A RARE METASTATIC PATTERN CAUSES LIVER FAILURE
1251
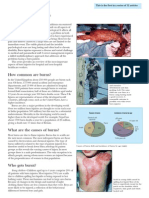
Figure 1. (A) Image of the unfixed liver revealed hepatomegaly without gross metastasis. (B) Microscopic examination of the liver revealed diffuse infiltration
by pleomorphic cells with some glandular formation. (C) Immunohistochemical staining for E-cadherin expression in the metastatic nodule in the lung was
strongly positive, (D) that of metastatic tumor cells in the liver was negative (arrow).
Metastatic tumor infiltration was also detected in the
spleen and both adrenal glands. Sections from nodules in the
pancreas and the lungs demonstrated metastatic carcinoma. In
addition, microscopic foci of metastasis were observed in the
uterine cervix, appendix, bone marrow, thyroid and intrathoracic lymph nodes. No evidence of carcinoma was identified
in the breast tissue samples. Additional abnormal histological
findings included pulmonary congestion with edema and focal
hemorrhage, myocardial hypertrophy, acute tubular necrosis of
both kidneys and hypoxicischemic changes in the brain tissue.
Immunohistochemical staining for E-cadherin was also
performed. Notably, tumor cells in the lung nodule strongly
expressed E-cadherin (Fig.1C), while tumor cells in the liver
did not (Fig.1D).
Discussion
With the exception of the lymph nodes, the liver is considered
to be the most frequent site of metastasis (911). In breast
cancer, the liver is also one of the major metastatic targets along
with the lungs and bone(1,9,12). The most common pattern of
liver metastasis is the formation of discrete multiple nodules
followed by a single nodule, while diffuse tumor invasion into
the liver parenchyma or diffuse parenchymal metastasis is less
common(3,4,12). Hematological malignancies are recognized
to be the most common cause of diffuse parenchymal metastasis(1,3,4). This metastatic pattern has also been identified
in many primary neoplasms, including breast, lung, stomach,
colon, pancreatic, nasopharynx, urothelial, uterine and malignant melanoma(3,4,7,8).
Acute liver failure rarely occurs in typical liver metastasis,
although abnormal liver enzymes may be detected(3,4,7),
whilst this condition is more common in diffuse parenchymal
metastasis(1,7). This complication is speculated to be caused
by extensive hepatocellular necrosis resulting from pressure
atrophy and interference of the vascular supply(4,68,13).
Radiological studies including ultrasonography, CT and MRI
scans are usually not able to identify diffuse parenchymal
metastasis(1,35,7), thus increasing the difficulty in the diagnosis. Radiological findings resembling cirrhosis have also been
reported(1,7,14). To confirm the diagnosis, histological examination is necessary and a liver biopsy may be useful(3,5,7).
The prognosis of acute liver failure secondary to malignant infiltration is extremely poor; the majority of patients
do not survive shortly after the onset of liver failure(14,7,8).
According to a review by Allison etal, concerning 21 reported
cases of acute liver failure due to metastatic breast carcinoma,
18cases died within three days to two months(7). Non-specific
prodromal symptoms, such as malaise, weight loss, right upper
quadrant abdominal pain and fever, are always observed to be
present at least two to four weeks prior to the onset of liver
failure(3,4).
The underlying mechanism of diffuse parenchymal
metastasis remains unknown. Allison etal proposed a loss of
cell surface adhesional molecule expression; the three cases
in their study described as diffuse intrasinusoidal hepatic
metastasis did not express both E-cadherin and CD44, which
are glycoproteins involved in cell-cell and cell-extracellular
matrix adhesion(7). In the present case, a difference in
E-cadherin expression in the two different areas of metastasis
was observed; the tumor cells in the metastatic nodule in the
lung stained positive for E-cadherin, while the infiltrating
tumor cells in the liver stained negative. These findings
support the hypothesis that a loss of cell surface adhesional
molecule expression is involved in facilitating diffuse parenchymal metastais.
1252
ONCOLOGY LETTERS 5: 1250-1252, 2013
In conclusion, although malignant infiltration of the liver
is rare, it ought to be considered as a differential diagnosis in
patients with acute hepatic failure. Liver biopsy may be the
most effective technique to confirm the diagnosis during the
patient's life.
Acknowledgements
The authors would like to thank Dr ChayaweeMuangchan
from the Department of Medicine, Siriraj Hospital, Mahidol
University, for providing the clinical information.
References
1. Nazario HE, Lepe R and Trotter JF: Metastatic breast cancer
presenting as acute liver failure. Gastroenterol Hepatol 7: 6566,
2011.
2. Begin LR, Boucher D and Lamoureux E: Diffuse hepatic
intravascular carcinomatous embolization resulting in fatal
liver failure: a clinicopathologic study of 4 cases. Pathol Res
Pract197: 433-440, 2001.
3. Rowbotham D, Wendon J and Williams R: Acute liver failure
secondary to hepatic infiltration: a single centre experience of
18cases. Gut 42: 576-580, 1998.
4. Athanasakis E, Mouloudi E, Prinianakis G, Kostaki M, TzardiM
and Georgopoulos D: Metastatic liver disease and fulminant
hepatic failure: presentation of a case and review of the literature.
Eur J Gastroenterol Hepatol 15: 1235-1240, 2003.
5. Alexopoulou A, Koskinas J, Deutsch M, DelladetsimaJ,
Kountouras D and Dourakis SP: Acute liver failure as the initial
manifestation of hepatic infiltration by a solid tumor: report of
5cases and review of the literature. Tumori 92: 354-357, 2006.
6. Schneider R and Cohen A: Fulminant hepatic failure complicating metastatic breast carcinoma. South Med J 77: 84-86, 1984.
7. Allison KH, Fligner CL and Parks WT: Radiographically occult,
diffuse intrasinusoidal hepatic metastases from primary breast
carcinomas: a clinicopathologic study of 3 autopsy cases. Arch
Pathol Lab Med 128: 1418-1423, 2004.
8. Barreales M, Casis B, Senz Lpez S and Solis HerruzoJA:
Fulminant hepatic failure caused by metastatic liver disease. Rev
Esp Enferm Dig 99: 245-247, 2007 (In Spanish).
9. Disibio G and French SW: Metastatic patterns of cancers: results
from a large autopsy study. Arch Pathol Lab Med 132: 931939,
2008.
10. Centeno BA: Pathology of liver metastases. Cancer Control 13:
1326, 2006.
11. Mitchell ML, Filippone MD and Wozniak TF: Metastatic
carcinomatous cirrhosis and hepatic hemosiderosis in a patient
heterozygous for the H63D genotype. Arch Pathol Lab Med 125:
10841087, 2001.
12. Wyld L, Gutteridge E, Pinder SE, etal: Prognostic factors
for patients with hepatic metastases from breast cancer. Br J
Cancer89: 284-290, 2003.
13. Burnett RA: Cor pulmonale due to tumour embolism derived
from intrasinusoidal metastatic liver carcinoma. J Clin Pathol28:
457-464, 1975.
14. Nascimento AB, Mitchell DG, Rubin R and WeaverE: Diffuse
desmoplastic breast carcinoma metastases to the liver simulating
cirrhosis at MR imaging: report of two cases. Radiology 221:
117121, 2001.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Jadwal Driver Ambulance Puskesmas Kedungwuni IDocument2 pagesJadwal Driver Ambulance Puskesmas Kedungwuni INisa DinanaNo ratings yet
- Handi Prabowo Master LabelDocument1 pageHandi Prabowo Master LabelNisa DinanaNo ratings yet
- Jadwal APRILDocument2 pagesJadwal APRILNisa DinanaNo ratings yet
- Offline Posbindu Kranji MAR 2018Document28 pagesOffline Posbindu Kranji MAR 2018Nisa DinanaNo ratings yet
- Journal of Pediatric Sciences PDFDocument5 pagesJournal of Pediatric Sciences PDFNisa DinanaNo ratings yet
- Lap Bul 2016Document174 pagesLap Bul 2016Nisa DinanaNo ratings yet
- Offline Posbindu Kranji Jan 2018Document28 pagesOffline Posbindu Kranji Jan 2018Nisa DinanaNo ratings yet
- Jadwal Driver Ambulance Puskesmas Kedungwuni IDocument2 pagesJadwal Driver Ambulance Puskesmas Kedungwuni INisa DinanaNo ratings yet
- Question 18 To 21 Refer To The Following ConversationDocument7 pagesQuestion 18 To 21 Refer To The Following ConversationNisa DinanaNo ratings yet
- Hepatomegaly Multiple: and Liver LesionsDocument2 pagesHepatomegaly Multiple: and Liver LesionsNisa DinanaNo ratings yet
- Show TextDocument4 pagesShow TextNisa DinanaNo ratings yet
- ABC of BurnsDocument37 pagesABC of Burnsiraklisd100% (2)
- Journal of Pediatric Sciences PDFDocument5 pagesJournal of Pediatric Sciences PDFNisa DinanaNo ratings yet
- Mitosis and MeiosisDocument32 pagesMitosis and Meiosisapi-238421605100% (2)
- Human Amyloid Imaging 2015 Book DraftDocument151 pagesHuman Amyloid Imaging 2015 Book DraftWorldEventsForumNo ratings yet
- Inheritance of Sex and Sex-Linked or Influenced Traits - StudentDocument21 pagesInheritance of Sex and Sex-Linked or Influenced Traits - StudentNoob Gamer0% (1)
- Bioc Module 2 Lab ReportDocument11 pagesBioc Module 2 Lab ReportMimi BoisterNo ratings yet
- Type IV Hypersensitivity - WikipediaDocument3 pagesType IV Hypersensitivity - WikipediaLokesh BakshiNo ratings yet
- Upadacitinib AR SELECT NEXT TrialDocument10 pagesUpadacitinib AR SELECT NEXT TrialMr. LNo ratings yet
- Mother Touch in Periodontal Therapy: Chorion MembraneDocument7 pagesMother Touch in Periodontal Therapy: Chorion MembraneInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Purves Neuroscience Website Questions CH 8 AnswersDocument4 pagesPurves Neuroscience Website Questions CH 8 AnswersPK3214598750% (2)
- Simina Maria Boca, PH.D.: EducationDocument13 pagesSimina Maria Boca, PH.D.: EducationRohit AroraNo ratings yet
- VPA & Glia &TLR Deckmann-2018-Autism-ADocument15 pagesVPA & Glia &TLR Deckmann-2018-Autism-AAhmed NagehNo ratings yet
- Pharmacology Lecture 6th WeekDocument55 pagesPharmacology Lecture 6th WeekDayledaniel SorvetoNo ratings yet
- Five Day Diet AnalysisDocument4 pagesFive Day Diet AnalysisphyreflyNo ratings yet
- L96 - Patna Lab 2 (Home Visit) : Patientreportscsuperpanel - SP - General - Template01 - SC (Version: 7)Document3 pagesL96 - Patna Lab 2 (Home Visit) : Patientreportscsuperpanel - SP - General - Template01 - SC (Version: 7)Rohit Gautam DwivediNo ratings yet
- Melanoma-Skin-Cancer FinalDocument48 pagesMelanoma-Skin-Cancer FinalJeanessa Delantar QuilisadioNo ratings yet
- M 8 StsDocument6 pagesM 8 StsGerald Noveda RomanNo ratings yet
- A Comprehensive Review of Global Efforts on COVID-19 Vaccine DevelopmentDocument22 pagesA Comprehensive Review of Global Efforts on COVID-19 Vaccine DevelopmentBeverly EstoqueNo ratings yet
- Virus TableDocument3 pagesVirus TableFrozenManNo ratings yet
- Comprehensive Guide to E@J StandardsDocument46 pagesComprehensive Guide to E@J StandardsEdson LimaNo ratings yet
- Gene DuplicationDocument413 pagesGene Duplicationdjwa163No ratings yet
- Blood Gas Analysis ExplainedDocument28 pagesBlood Gas Analysis ExplainedanojNo ratings yet
- Cholelithiasis and Choledocholithiasis Infos ..Document5 pagesCholelithiasis and Choledocholithiasis Infos ..Franzia Izandra Alkuino MojicaNo ratings yet
- Biology Half Yearly 12Document14 pagesBiology Half Yearly 12Tarun MonNo ratings yet
- G8 B-Thall Chromatogram Interpretation Guide1Document58 pagesG8 B-Thall Chromatogram Interpretation Guide1Kwok Hoi ShanNo ratings yet
- Chapter 2 (Teacher)Document19 pagesChapter 2 (Teacher)ajakazNo ratings yet
- GeneticsDocument35 pagesGeneticsSmithNo ratings yet
- NephronDocument5 pagesNephronrdeguzma100% (1)
- DifcoBBLManual 2ndedDocument700 pagesDifcoBBLManual 2ndedEl CapitanNo ratings yet
- Jessica Hughes AP Biology LabDocument8 pagesJessica Hughes AP Biology LabJessica HughesNo ratings yet
- Eucerin - Nobel Prize Revolutionises Skin Care - Cells' Water Channels Specifically StimulatedDocument2 pagesEucerin - Nobel Prize Revolutionises Skin Care - Cells' Water Channels Specifically StimulatedFelpnilNo ratings yet
- Pathophysiology Respiratory SystemDocument63 pagesPathophysiology Respiratory SystemAli Basha QudahNo ratings yet