Professional Documents
Culture Documents
A Rare Complication of Acute Appendicitis: Superior Mesenteric Vein Thrombosis
Uploaded by
Esha Putriningtyas SetiawanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
A Rare Complication of Acute Appendicitis: Superior Mesenteric Vein Thrombosis
Uploaded by
Esha Putriningtyas SetiawanCopyright:
Available Formats
CASE REPORT
A Rare Complication of Acute Appendicitis:
Superior Mesenteric Vein Thrombosis
Hendra Koncoro*, Rafael Eddy Setijoso*, Maisie ME Johan**
*Department of Internal Medicine, Sint Carolus Hospital, Jakarta
**Department of Radiology, Sint Carolus Hospital, Jakarta
Corresponding author:
Hendra Koncoro. Department of Internal Medicine, Sint Carolus Hospital. Jl. Salemba Raya No. 41 Jakarta Indonesia.
Phone/facsimile: +62-21-3904441. E-mail:hendra_koncoro@yahoo.com.
ABSTRACT
Superior mesenteric vein (SMV) thrombosis caused by acute appendicitis is quite rare nowadays. These
conditions occurs secondary to infection in the region drained by the portal venous system. In this case, we report
a successfully treated case of SMV thrombosis and liver abscess associated with appendicitis with antibiotics
and anticoagulant.Early diagnosis and prompt treatment are basic to a favorable clinical course.
Keywords: superior mesenteric vein thrombosis, pyogenic liver abscess, appendicitis
ABSTRAK
Trombosis vena mesenterika superior yang disebabkan oleh apendisitis akut sangatlah jarang dewasa ini.
Kondisi ini terjadi karena infeksi di daerah yang didrainase oleh sistem vena portal. Dalam kasus ini, kami
melaporkan suatu kasus trombosis vena mesenterika superior dan abses hati yang disebabkan oleh apendisitis
dengan menggunakan antibiotika dan antikoagulan. Diagnosis dini dan terapi segera merupakan dasar terhadap
perbaikan keadaan klinis.
Kata kunci: trombosis vena mesenterika superior, abses hati piogenik, apendisitis
INTRODUCTION
pyogenic liver abscess is often missed due to its non-
Acute appendicitis is the commonest surgical specific clinical presentation, such as abdominal pain,
emergency in adult. In United States, there were fever, chills, fatigue, nausea, and vomiting. Caution
250,000 cases annually.1 If untreated, acute appendicitis need to be taken because mortality rate in SMV
can have complications such as abscess formation, thrombosis and pyogenic liver abscess associated with
perforation and peritonitis.2 intra-abdominal infection can reach 25-50%.2,3
Traditional complications such as abscess or Rare complications in acute appendicitis were
peritonitis are relatively easy to detect while rare scarcely found. Therefore clinicians need to increase
complications such as mesenteric vein thrombosis awareness to decrease mortality. The aim of presenting
and pyogenic liver abscess are more difficult to this case is to discuss the management of this rare
recognize. Superior mesenteric vein (SMV) thrombosis complication of appendicitis.
and pyogenic liver abscess caused by appendicitis is
very rare now, owing to improved antibiotic therapy.
However, the diagnosis of SMV thrombosis and
204 The Indonesian Journal of Gastroenterology, Hepatology and Digestive Endoscopy
A Rare Complication of Acute Appendicitis: Superior Mesenteric Vein Thrombosis
CASE ILUSTRATION Abnormal multiple focal densities located in the liver
were multiple, pyogenic liver abscess. Appendix was
A 17-year-old man presented to the St. Carolus
retrocaecal, swelling with periappendiceal haziness
hospital emergency department with a 3-day history of
suggestive of appendicitis. A small amount of abnormal
fever, chills, right lower quadrant abdominal pain and
fluid was seen around the liver, right paracolic gutter
jaundice. He was previously healthy until one week
and in the pelvis. On the basis of the microbiological
prior to presentation. It was initially a dull central lower
data, treatment was done with ceftriaxone 3 g IV q
abdominal pain that developed into a sharp intense
24 hours and metronidazole 500 mg IV q 8 hours. On
pain associated with rigors. Nausea accompanied
the 7th hospital day, the patients condition continued
his complaints. The patient was previously went
to improve and he was discharged 2 weeks later.
to surgery clinic six months ago with right lower
After 14 days from treatment with ceftriaxone and
quadrant abdominal pain and has been diagnosed with
metronidazole, his bilirubin level was lowered to
appendicitis and advised to be done appendectomy,
total bilirubin 4.90 mg/dL, direct bilirubin 3.43 mg/
however he refused. The patient is a student and denied
dL). Further treatment was not needed. We decided to
any recent travel or sick contacts. He had neither
treat the appendicitis conservatively with antibiotics
alcohol intake nor smokes.
and SMV thrombosis with therapeutic dose of heparin
On examination, his blood pressure was 138/70
after discussion with a haematologist. After two weeks
mmHg with a pulse rate of 100/min. He had a
of antibiotic therapy, the patient showed improvement
temperature of 38.1 0C, with an oxygen saturation of
in clinical and biochemical signs. This patient was
99% on air. Eyes were icteric. The abdomen was soft
planned to done interval appendectomy, however
but there was evidence of a hepatomegaly. Maximum
after careful treatment which showed improvement,
tenderness was elicited in the right upper quadrant of
he denied further appendectomy and discharged home.
the abdomen. The spleen were non-palpable. Bowel
sounds were slightly increased and minimal lower
quadrant tenderness was presented. Peripheral white
blood cell count was 22,750/mm3 (segmen neutrophil
88.7%). Hematocrit was 37.6% and platelet count was
85,000/mm3. Other values were AST 38 IU/L, ALT
52 IU/L, gamma-GT 160 u/L, alkaline phosphatase
202 IU/L, total bilirubin 9.90 mg/dL, direct bilirubin
8.70 mg/dL, protein 5.20 g/dL, albumin 2.04 g/dL,
INR was 1.12, and d-dimer 4650 ng/mL. Abdominal
ultrasonography revealed hepatomegaly with multiple
hypoechoicheterogen masses with largest mass was
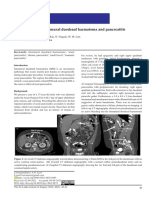
45 x 35 x 46 mm, suggestive of abscess and minimal Figure 2. A contrast-enhanced CT scan confirmed the portal
vein thrombosis and also demonstrated superior mesenteric
sludge in gall bladder. The pancreas and kidneys vein thrombosis. Abnormal multiple focal densities located in
appeared normal (Figure 1). the liver were multiple, pyogenic liver abscess
DISCUSSION
Appendicitis is one of the most common surgical
diagnosis.Appendicitis usually complicated as
perforation, peritonitis and abscess formation. Some
reports stated that appendicitis can result in portal
Figure. 1. Ultrasonography revealed multiple hypoechoicheterogen vein thrombosis.3 Inflammed thrombosis of the portal
masses, suggestive of liver abscess
vein is called pylephlebitis. Pylephlebitis occurs as
Streptococcus agalactiae was grown from blood a result of an abdominal infection draining into the
culture. Since intra-abdominal septic foci were portal venous system.1 The thrombus began from the
suspected, abdominopelvic computerized tomography small veins of the affected area to larger veins, leading
(CT) scan was taken. A contrast-enhanced CT scan to septic thrombophlebitis of the mesenteric vein and,
revealed a thrombus within portal vein that extended eventually, of the portal vein. Swelling of the intestine
throughout superior mesenteric vein (Figure 2). and ischemia may occur due to SMV thrombosis which
Volume 17, Number 3, December 2016 205
Hendra Koncoro, Rafael Eddy Setijoso, Maisie ME Johan
lead to high morbidity and mortality.4 SMV thrombosis intra-abdominal infection, CT scanning may be the
caused by appendicitis itself is not common, with most reasonable initial choice for imaging, given its
incidence rate of 0.4% before 1950 and became proven ability to detect not only thrombi but infection
extremely rare afterwards due to adequate antibiotic foci as well. CT-scan also less operator dependent
use. However, when occurred the mortality rate compared to ultrasonography. Thus, CT scan is the
become 80% in the past and has decreased to 30-50% most reliable initial diagnostic choice. Early phase
nowadays.5 of this intraabdominal infection, hepatic infection are
Pathogenesis of SMV thrombosis are microscopic which coalesce to form macroabscess.8
thrombophlebitis resulting in thrombosis and can be On the basis of treatments, it appears that empirical
explained as follows:hypercoagulability state occurred antibiotic therapy for a patient with suspected SMV
due to abscesses in the mesoappendix; thrombi are thrombosis should include broad coverage for gram-
formed locally. Bacteria infiltrate into the SMV, negative bacilli and agents active against anaerobes,
cause inflammation such as portal vein phlebitis, and coverage for aerobic Streptococcus species.
and induce thrombus formation. Bacteria spread into Patients with demonstrated macroscopic liver abscess
tissues around the veins, cause periphlebitis along the complicating SMV thrombosis should probably
vessels, and as inflammation extends into the vascular receive at least 6 weeks of antibiotic therapy, with or
lumens, coagulation cascade is promoted, leading without drainage.1,8 In our case, ceftriaxone (3 g/ day)
to thrombus formation.6 Coagulation was facilitated and metronidazole (1.5 g/day) was performed for 2
via its surface and capsular components. The surface weeks and resulted in complete resolution of hepatic
component accelerates fibrin cross-linking and the lesions. Further appendectomy was planned, however
capsular polysaccharides initiate the clotting cascade due to condition improvement, he denied any surgical
by activating macrophages.1 procedure.
It is difficult to establish diagnosis only from The role of anticoagulation in the treatment of
clinical findings.The symptoms of SMV thrombosis SMV thrombosis is controversial. Several reports
are non-specific. High suspicion should be assumed in recommended using anticoagulation therapy to
patients who present with abdominal pain, fever, and reduce recurrence rate and mortality rate.9 No formal
signs of sepsis, as well as leukocytosis and elevated study of anticoagulation in SMV thrombosis has ever
liver enzymes. Other clinical features are as follows: been done.10 Despite such evidence that heparin may
fatigue, malaise, chills, nausea, vomiting, diarrhea, not be critical for the survival of patients with SMV
and weight loss. Hepatomegaly and jaundice are other thrombosis, the possibility exists that anticoagulation
clinical findings usually seen. SMV thrombosis can be might benefit some patients by decreasing the chance
diagnosed via abdominal ultrasonography showing of septic embolization to the liver from infected portal
a thrombus in the portal vein.4 An abdominal CT- thrombi and pulmonary emboli. In our patient, a
scan is less operator-dependent and is more widely previously healthy patient presented with nonspecific
used because of its ability to detect other sources of syptoms and fever. Streptococcus agalactiae was
infection in the abdomen. CT imaging can diagnose grown from blood, which clearly suggested an intra-
this complication at an early stage.7 abdominal origin. Infection was most likely caused
In our case, appendicitis was the cause of SMV by appendicitis, confirmed by abdominal CT, which
thrombosis. Diagnosis of SMV thrombosis are made by seeding to the mesenteric vein and liver. Septic
clinical signs and symptoms, laboratory examination, conditions were improved with early initiation of
blood culture and imaging modalities. Clinical broad-spectrum antibiotics. Surgical intervention were
signs and symptoms are fever, right upper quadrant denied due to improvement of condition.8
pain, jaundice and hepatomegaly. Pylephlebitis can
be caused by ascending Escherichia coli, Proteus
REFERENCES
mirabilis, Klebsiella pneumonia, Enterobacter
species, Pseudomonas species and gram-positive cocci 1. Wong K, Weisman DS, Patrice KA. Pylephlebitis: a rare
complication of an intraabdominal infection. J Community
(Staphylococcus aureus, Streptococcus species).8 In Hosp Intern Med Perspect 2013:3:10.342.
our case, Streptococcus agalactiae was grown from 2. Longworth S, Han J. Pyogenic liver abscess. Clin Liver Dis
blood. 2015;6:51-4.
Modern imaging techniques provide supportive 3. Bakti N, Hussain A, El-Hasani S. A rare complication of acute
appendicitis: superior mesenteric vein thrombosis. Int J Surg
diagnostic evidence. In the setting of probable
Case Rep 2011;2:250-52.
206 The Indonesian Journal of Gastroenterology, Hepatology and Digestive Endoscopy
A Rare Complication of Acute Appendicitis: Superior Mesenteric Vein Thrombosis
4. Ponziani FR, Zocco MA, Campanale C, Rinninella E, Tortora
A, Di Maurizio L, et al. Portal vein thrombosis: insight
into physiopathology, diagnosis, and treatment. World J
Gastroenterol 2010:16:143-55.
5. Lee KW, Choi YI. Superior mesenteric vein thrombosis
accompanied with severe appendicitis. Korean J Hepatobiliary
Pancreat Surg 2014;18:101-3.
6. Takehara K, Miyano S, Machida M, Kitabatake T, Fujisawa
M, Kojima K. Superior mesenteric vein thrombosis as a
complication of acute appendicitis: report of a case. Clin J
Gastroenterol 2013;6:269-73.
7. Balthazar EJ, Gollapudi P. Septic thrombophlebitis of the
mesenteric and portal veins: CT imaging. J Comput Assist
Tomogr 2000:24:755-60.
8. Lim HE, Cheong HJ, Woo HJ, Kim WJ, Kim MJ, Lee CH, et
al. Pylephlebitis associated with appendicitis. Korean J Intern
Med 1999;14:73-6.
9. Pinto S, Lerner T, Lingamaneni G, Richards K. Superior
mesenteric vein thrombosis as a complication of cecal
diverticulitis: a case report. Int J Surg Case Rep 2016;25:71-4.
10. Chawla YK, Bodh V. Portal vein thrombosis. J Clin Exp
Hepatol 2015;5:22-40.
Volume 17, Number 3, December 2016 207
You might also like
- M.a.G.I.C! For Minds - Terence WattsDocument317 pagesM.a.G.I.C! For Minds - Terence Wattsiuyrtew100% (4)
- Beat CancerDocument114 pagesBeat CancerGeorge Dragoi100% (8)
- White Crane Medicine's Qi GongDocument5 pagesWhite Crane Medicine's Qi GongtansoeiNo ratings yet
- K.26 Acute AbdomenDocument45 pagesK.26 Acute Abdomenlidz_margaretNo ratings yet
- Progressive Muscle RelaxationDocument16 pagesProgressive Muscle RelaxationFaith DawnNo ratings yet
- Magneto Therapy NotesDocument5 pagesMagneto Therapy NotesMadan Kumar100% (2)
- The Origins of Rebirthing Style Breathwork by Peter Mark AdamsDocument5 pagesThe Origins of Rebirthing Style Breathwork by Peter Mark AdamsPeter Mark Adams100% (2)
- Flexor Tendon Injuries. Hand Clinics. 2005Document152 pagesFlexor Tendon Injuries. Hand Clinics. 2005k2rojo100% (2)
- ALSANGEDY BULLETS For PACES Ankylosing Spondylitis 2nd EditionDocument2 pagesALSANGEDY BULLETS For PACES Ankylosing Spondylitis 2nd EditionGhulamMemonNo ratings yet
- Nutrition and Students Academic PerformanceDocument10 pagesNutrition and Students Academic Performanceapi-222239614No ratings yet
- ToxicologyDocument31 pagesToxicologyEri QuevedoNo ratings yet
- Relationship Between The Five Element Points and Some Major Physiological SystemsDocument4 pagesRelationship Between The Five Element Points and Some Major Physiological SystemsNilton Benfatti100% (1)
- Radicular Cavity PreparationDocument64 pagesRadicular Cavity PreparationAndrea LawNo ratings yet
- Role of Nurses in Drug Administration and Preventing Medication ErrorsDocument35 pagesRole of Nurses in Drug Administration and Preventing Medication Errorsneil garcia100% (2)
- The Movement Continuum Theory of Physical Therapy-2Document2 pagesThe Movement Continuum Theory of Physical Therapy-2Ingela Sjölin100% (2)
- Residents' Clinic: 22-Year-Old Man With Abdominal Pain and RashDocument4 pagesResidents' Clinic: 22-Year-Old Man With Abdominal Pain and RashAkhtar AliNo ratings yet
- Scrotal Abscess As The First Symptom of Fatal Necrotizing PancreatitisDocument4 pagesScrotal Abscess As The First Symptom of Fatal Necrotizing PancreatitisTeja Laksana NukanaNo ratings yet
- Renal Tubular & Interstitial Disease GuideDocument94 pagesRenal Tubular & Interstitial Disease GuideCoy NuñezNo ratings yet
- Hemosuccus Pancreaticus: A Mysterious Cause of Gastrointestinal BleedingDocument6 pagesHemosuccus Pancreaticus: A Mysterious Cause of Gastrointestinal BleedingSINAN SHAWKATNo ratings yet
- Case Report: Peritonitis in Patients With Scrub TyphusDocument3 pagesCase Report: Peritonitis in Patients With Scrub TyphusJasleen KaurNo ratings yet
- Anil Degaonkar, Nikhil Bhamare, Mandar Tilak Arterio-Enteric Fistula A Case ReportDocument6 pagesAnil Degaonkar, Nikhil Bhamare, Mandar Tilak Arterio-Enteric Fistula A Case ReportDr. Krishna N. SharmaNo ratings yet
- 556-Article Text-2974-1-10-20220615Document5 pages556-Article Text-2974-1-10-20220615Hans WinardiNo ratings yet
- Journal of Pharmaceutical and Scientific Innovation: Case StudyDocument3 pagesJournal of Pharmaceutical and Scientific Innovation: Case StudyDinoCsbrowNo ratings yet
- Appendicitis and Peritonitis GuideDocument35 pagesAppendicitis and Peritonitis GuideRose Anne AbivaNo ratings yet
- Acute Appendicitis in A Patient With Systemic Lupus ErythematosusDocument4 pagesAcute Appendicitis in A Patient With Systemic Lupus ErythematosusJessicaNo ratings yet
- 1 s2.0 S2210261223004741 MainDocument5 pages1 s2.0 S2210261223004741 MainDevita SanangkaNo ratings yet
- Chauke NJ 201908564 NUTRITIONAL SCREENINGDocument7 pagesChauke NJ 201908564 NUTRITIONAL SCREENINGRulani PrinceNo ratings yet
- Bruce J BarnonDocument7 pagesBruce J Barnonnasywa rahmatullailyNo ratings yet
- Poliadenitis NodosaDocument5 pagesPoliadenitis NodosaRicardo Uzcategui ArreguiNo ratings yet
- Intestinal ObstructionDocument13 pagesIntestinal Obstructionsantosh kumarNo ratings yet
- Case 1Document4 pagesCase 1Irsanti SasmitaNo ratings yet
- Simson 2017Document3 pagesSimson 20172cpw9fbnpxNo ratings yet
- Penanganan Terkini Bayi PrematurDocument44 pagesPenanganan Terkini Bayi PrematuryudhagpNo ratings yet
- Subsidence of Hypertension in A Patient With GiantDocument4 pagesSubsidence of Hypertension in A Patient With GiantSinbijeo GinNo ratings yet
- Diagnosis and Treatment of Acute AppendicitisDocument5 pagesDiagnosis and Treatment of Acute AppendicitisIrani RamahdaniNo ratings yet
- Recurrent Pancreatitis Caused by Groove PancreatitisDocument7 pagesRecurrent Pancreatitis Caused by Groove PancreatitisroxxanaNo ratings yet
- 1 s2.0 S0929644112000057 MainDocument4 pages1 s2.0 S0929644112000057 MainAisahNo ratings yet
- Acute Surgical Abdomen: Unexpected Medical CauseDocument6 pagesAcute Surgical Abdomen: Unexpected Medical CauseIJAR JOURNALNo ratings yet
- Gastroduodenal Artery Pseudoaneurysm and Aberrant Right Hepatic ArteryDocument3 pagesGastroduodenal Artery Pseudoaneurysm and Aberrant Right Hepatic ArteryGordana PuzovicNo ratings yet
- Case Report: Strangulated Obturator Hernia: A Case Report With Literature ReviewDocument4 pagesCase Report: Strangulated Obturator Hernia: A Case Report With Literature ReviewNi Nyoman SidiasihNo ratings yet
- International Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. AwasthiDocument3 pagesInternational Journal of Infectious Diseases: Anshuman Pandey, Shakeel Masood, Namrata P. Awasthijohanna monsalveNo ratings yet
- Hantavirus Rare Case With Both Renal and Pulmonary-Poster PDFDocument1 pageHantavirus Rare Case With Both Renal and Pulmonary-Poster PDFKeti JanevskaNo ratings yet
- Module 17 Content Nursing Care Management of Adult Clients With Inflammatory Conditions of The Gastrointestinal System Appendicitis and PeritonitisDocument7 pagesModule 17 Content Nursing Care Management of Adult Clients With Inflammatory Conditions of The Gastrointestinal System Appendicitis and PeritonitisVicente, Mary Angeline E.No ratings yet
- Colo-uterineFistulaaRareComplicationofDiverticularDiseasDocument8 pagesColo-uterineFistulaaRareComplicationofDiverticularDiseasRandy SaputraNo ratings yet
- Laparoscopic Cholecystectomy After Conservative Su - 2024 - International JournaDocument4 pagesLaparoscopic Cholecystectomy After Conservative Su - 2024 - International JournaRonald QuezadaNo ratings yet
- 19Document3 pages19Elizabeth ToapantaNo ratings yet
- Peptic Ulcer Disease Complications ExplainedDocument40 pagesPeptic Ulcer Disease Complications ExplainedMr FuckNo ratings yet
- Etiology: Acute AppendicitisDocument3 pagesEtiology: Acute AppendicitisWenna Grace OdtujanNo ratings yet
- Referat AppendicitisDocument28 pagesReferat AppendicitisFerio Joelian ChandraNo ratings yet
- Colonoscopy Is Mandatory AfterDocument3 pagesColonoscopy Is Mandatory AfterLaurice BarronNo ratings yet
- 8874 33333 1 PBDocument3 pages8874 33333 1 PBRanga PereraNo ratings yet
- 2 Semester 1 Major Patho AnatoDocument49 pages2 Semester 1 Major Patho AnatoManushi HenadeeraNo ratings yet
- 1 s2.0 S2210261221012268 MainDocument4 pages1 s2.0 S2210261221012268 Mainzenatihanen123No ratings yet
- Jurnal Bedah 2Document5 pagesJurnal Bedah 2nafamaulidinaNo ratings yet
- Primitive Mesenteric Clamp Syndrome: Unusual Cause of Upper Gastrointestinal ObstructionDocument5 pagesPrimitive Mesenteric Clamp Syndrome: Unusual Cause of Upper Gastrointestinal ObstructionIJAR JOURNALNo ratings yet
- CabdukadirDocument44 pagesCabdukadirAxmed CumarNo ratings yet
- 81-Texto Del Artículo-1437-1-10-20210903Document3 pages81-Texto Del Artículo-1437-1-10-20210903suelly-majorNo ratings yet
- A Rare and Fatal Case of Nasogastric Tube.492Document1 pageA Rare and Fatal Case of Nasogastric Tube.492Stefania Szeibert-KerekesNo ratings yet
- Surgery Organized TotesDocument31 pagesSurgery Organized Totesquestionbank oneNo ratings yet
- General care of the peritonitis patientDocument7 pagesGeneral care of the peritonitis patientRadenJeremySoeriawidjajaNo ratings yet
- Pneumatosis Cystoides Intestinalis: Report of Two Cases: M. Turan, M. S En, R. EgılmezDocument3 pagesPneumatosis Cystoides Intestinalis: Report of Two Cases: M. Turan, M. S En, R. EgılmezzixdiddyNo ratings yet
- In-Depth Review: Nonocclusive Mesenteric Ischemia: A Lethal Complication in Peritoneal Dialysis PatientsDocument6 pagesIn-Depth Review: Nonocclusive Mesenteric Ischemia: A Lethal Complication in Peritoneal Dialysis PatientsFernandoNo ratings yet
- Acute Mesenteric Ischemia in COVID19 Patient - NAT FixedDocument10 pagesAcute Mesenteric Ischemia in COVID19 Patient - NAT FixedAde Tan RezaNo ratings yet
- 260-Article Text-875-1-10-20220728Document4 pages260-Article Text-875-1-10-20220728hasan andrianNo ratings yet
- A Rare Case Report of Spontaneous Resolution of Hepatic Portal Venous Gas Associated With Cocaineinduced Intestinal IschDocument3 pagesA Rare Case Report of Spontaneous Resolution of Hepatic Portal Venous Gas Associated With Cocaineinduced Intestinal IschShiva PNo ratings yet
- Acute Appendicitis Diagnosis and TreatmentDocument3 pagesAcute Appendicitis Diagnosis and TreatmentMavi HayalNo ratings yet
- Peritoneal Encapsulation: A Rare Cause of Small Bowel ObstructionDocument3 pagesPeritoneal Encapsulation: A Rare Cause of Small Bowel ObstructionNatalindah Jokiem Woecandra T. D.No ratings yet
- An Unusual Cause of Acute Abdomend Gas-Forming Liver Abscess Due To Salmonella EnteritidisDocument4 pagesAn Unusual Cause of Acute Abdomend Gas-Forming Liver Abscess Due To Salmonella EnteritidisMenda JangWooyoung SooyoungsterNo ratings yet
- Acute Abdominal Pain Following EsophagogastroduodeDocument2 pagesAcute Abdominal Pain Following Esophagogastroduodeniluh suwasantiNo ratings yet
- Sub Diaphragmatic Abscess Leading To Empyema Thoracis in A Case of Perforated Appendix A Rare Case ReportDocument4 pagesSub Diaphragmatic Abscess Leading To Empyema Thoracis in A Case of Perforated Appendix A Rare Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Spontaneous Rupture of Pyonephrosis Leading To PyoperitoneumDocument3 pagesSpontaneous Rupture of Pyonephrosis Leading To PyoperitoneumsamiNo ratings yet
- Recurrent Infected Mesenteric Cyst Rare Surgical CauseDocument2 pagesRecurrent Infected Mesenteric Cyst Rare Surgical CauseMotivational SpeechNo ratings yet
- Signs, Symptoms and Treatment of AppendicitisDocument14 pagesSigns, Symptoms and Treatment of AppendicitisMary Joy BunuanNo ratings yet
- (Indo 5) Skripsi TTG Protein Dan Kecerdasan Punya Anak UmsDocument11 pages(Indo 5) Skripsi TTG Protein Dan Kecerdasan Punya Anak UmsEsha Putriningtyas SetiawanNo ratings yet
- (Inggris 2) Hubungan Protein Daging Dengan KognitifDocument9 pages(Inggris 2) Hubungan Protein Daging Dengan KognitifEsha Putriningtyas SetiawanNo ratings yet
- Name: Baby. Mrs. Su (AGE: 5 Hours No MR: 01159530Document8 pagesName: Baby. Mrs. Su (AGE: 5 Hours No MR: 01159530Esha Putriningtyas SetiawanNo ratings yet
- Pediatric Acute AppendicitisDocument10 pagesPediatric Acute AppendicitisEsha Putriningtyas SetiawanNo ratings yet
- E4 Full PDFDocument11 pagesE4 Full PDFEsha Putriningtyas SetiawanNo ratings yet
- E4 Full PDFDocument11 pagesE4 Full PDFEsha Putriningtyas SetiawanNo ratings yet
- Your Purchased License Authentication CodeDocument1 pageYour Purchased License Authentication CodeEsha Putriningtyas SetiawanNo ratings yet
- SAF 19 JanuariDocument19 pagesSAF 19 JanuariEsha Putriningtyas SetiawanNo ratings yet
- FR Maxilla Radius Patella EnglishDocument17 pagesFR Maxilla Radius Patella EnglishEsha Putriningtyas SetiawanNo ratings yet
- PG App Perforasi EnglishDocument17 pagesPG App Perforasi EnglishEsha Putriningtyas SetiawanNo ratings yet
- Chest TubeDocument15 pagesChest TubeEsha Putriningtyas SetiawanNo ratings yet
- Low Back Pain: Implementing NICE GuidanceDocument19 pagesLow Back Pain: Implementing NICE GuidanceEsha Putriningtyas SetiawanNo ratings yet
- Pancreatitis: Causes, Symptoms, and TreatmentDocument5 pagesPancreatitis: Causes, Symptoms, and TreatmentSanthu Su100% (2)
- Orthopaedic Connection: Hip DislocationDocument2 pagesOrthopaedic Connection: Hip DislocationTeuku FennyNo ratings yet
- Peritoneal DialysisDocument5 pagesPeritoneal DialysisLisette TupasNo ratings yet
- Schizoaffective With Bipolar DisordersDocument14 pagesSchizoaffective With Bipolar DisordersNaomi MasudaNo ratings yet
- Orofacial Granulomatosis: Causes, Symptoms and TreatmentDocument4 pagesOrofacial Granulomatosis: Causes, Symptoms and TreatmentdevaaNo ratings yet
- Michelle Phan Anorexia Nervosa FinalDocument12 pagesMichelle Phan Anorexia Nervosa Finalapi-298517408No ratings yet
- Suspension Therapy by Rahul Vapms CopDocument20 pagesSuspension Therapy by Rahul Vapms Copvenkata ramakrishnaiahNo ratings yet
- April Raytana EspejoDocument4 pagesApril Raytana EspejoPreng MirrorNo ratings yet
- Formulation and Evaluation of An Injectable Soluti PDFDocument7 pagesFormulation and Evaluation of An Injectable Soluti PDFdhirazhrNo ratings yet
- Vaginal CancerDocument41 pagesVaginal Cancercb_cristianNo ratings yet
- Bomba TranscriptDocument11 pagesBomba Transcriptapi-411111134No ratings yet
- Ce Booklet Fall 14Document28 pagesCe Booklet Fall 14api-279863771No ratings yet
- Drug Dosage Calculation Formulas and Practice ExercisesDocument15 pagesDrug Dosage Calculation Formulas and Practice ExercisesIhtesham Ul Haq100% (1)
- Cognitive & Behavioral Therapy: (Clinical Psychology)Document3 pagesCognitive & Behavioral Therapy: (Clinical Psychology)Nowella Kryzel PelayoNo ratings yet
- UPH - OR Instrument Lists Sample PDFDocument43 pagesUPH - OR Instrument Lists Sample PDFFlorencia WirawanNo ratings yet
- Dissociative Identity Disorder Research OverviewDocument7 pagesDissociative Identity Disorder Research Overviewthom_evans_2No ratings yet
- 2001 Self-Assessment Examination For Residents (Sae-R) Multiple-Choice Questions Booklet Abridged VersionDocument23 pages2001 Self-Assessment Examination For Residents (Sae-R) Multiple-Choice Questions Booklet Abridged VersionSoumabho DasNo ratings yet