Professional Documents
Culture Documents
Number of Follicles As A Risk Factor For Multiple Pregnancy With IUI Cycles
Uploaded by
NaliniOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Number of Follicles As A Risk Factor For Multiple Pregnancy With IUI Cycles
Uploaded by
NaliniCopyright:
Available Formats
Number of follicles as a risk factor for multiple pregnancy with IUI cycles
Advanced Fertility Center of Chicago Gurnee & Crystal Lake, Illinois Title of article: Relationship of follicle numbers and estradiol levels to multiple implantation in 3,608 intrauterine insemination cycles
Authors: Richard P. Dickey, Steven N. Taylor, Peter Y. Lu, Belinda M. Sartor, Phillip H. Rye, and Roman Pyrzak (from The Fertility Institute of New Orleans, New Orleans, Louisiana, USA, and the Section of Reproductive Endocrinology, Department of Obstetrics and Gynecology, Louisiana State University School of Medicine) Source: Fertility and Sterility, January 2001 (Vol.75) Pages 69-78.
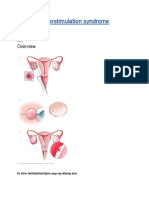
Background on ovarian stimulation for infertility and multiple birth risks:
Multiple pregnancy - particularly triplets and higher - is a very significant problem in the world of infertility treatment. Doctors and patients all want the same thing - successful delivery of a healthy child. However, some of the treatments that we use involve stimulation of the ovaries to make multiple mature eggs - and multiple ovulations. In general, more eggs means more chance for a pregnancy resulting. More eggs also means more risk for multiple pregnancies. In vitro fertilization allows us to control risks for multiple pregnancy by replacing a "reasonable" number of embryos into the uterus. Blastocyst transferallows us even more control than ever before - while maintaining high pregnancy success rates. However, we do not want to do IVF on everyone. We need to be able to maximize chances for pregnancy with ovarian stimulation cycles for intrauterine insemination - while at the same time having very low (preferably zero) rates of triplets and higher order pregnancies.
So how aggressive should we be we be with the ovarian stimulating drugs? How much do pregnancy rates differ according to how many follicles there are? What about effects on multiple pregnancy rates? Should we try to stimulate so that there are 2 eggs per month instead of the 1 that matures in a natural menstrual cycle? Or, should we try to get 3, or more than 3? Does the age of the woman matter much? Does the type of stimulating drug matter? Does the peak estrogen hormone level before ovulation matter?
There have been many studies done over the years that have investigated some of these important issues. Results have varied, and study sizes were often limited. This study looks at these issues again with a very large group of infertile couples.
How this study was done:
The stated objective of the study: To determine the relationship of follicle numbers and estradiol (E2) levels to multiple implantations in human menopausal gonadotropin HMG (injectable gonadotropins) and clomiphene citrate (Clomid, Serophene) cycles. Design of the study: Fifteen-year prospective study. Intervention(s): Ovulation induction with: 1. Clomid, or 2. HMG (injectable meds) 3. Clomid + injectable meds Main Outcome Measure(s): Pregnancy and multiple implantations
3608 cycles were included in this analysis. All women were stimulated with either clomiphene or HMG, or both together in the same cycle. The fresh or frozen sperm had to be at least 30% motility and at least 10 million total sperm before processing, and at least 4 million total motile sperm after processing (to reduce the negative influence of severe male factor cases). Follicles and estradiol hormone levels were measured in the usual fashion of infertility clinics. Data was recorded in a computer database and analyzed with respect to number of follicles of various sizes (on the day of HCG), peak estradiol levels and outcomes of pregnancy, as well as single, twin, and triplet or higher order pregnancy.
Results: Clomiphene citrate cycles - Clomid Of 176 clomiphene pregnancies, 14 (8.0%) twin and three (1.7%) triplet or higher-order implantations. In clomiphene cycles, pregnancy was more closely related to the number of follicles > or = 15 mm than to follicles > or = 18 mm or those > or = 12 mm. Pregnancy was unrelated to estrogen (E2) level, E2 levels per follicle, or patient age. Learn more about Clomid treatment for unexplained infertility Learn more about Clomid treatment for ovulation problems and PCOS
HMG injectable cycles and clomiphene + HMG injectable cycles
HMG is injectable FSH and LH hormone, similar to the brand name drugs Menopur, Bravelle, Follistim and Gonal-F. The 179 HMG pregnancies included 20 (11.2%) twin and 13 (7.2%) triplet or higher-order implantations. Of the 115 clomiphene + HMG pregnancies, 21 (18.3%) were twin and seven (6.1%) were triplet or higher-order implantations. Pregnancy was more closely related to the number of follicles > or = 12 mm than to follicles > or = 15 mm or > or = 18mm. Pregnancy was additionally related to E2 levels, but not to E2 levels per follicle, and was negatively related to age. In these cycles, implantation rates were more closely related to the number of follicles > or = 12mm than to follicles > or = 15 mm or > or = 18mm.
Effect of female age
The effects of female age on the rates of single and multiple pregnancy:
For clomiphene cycles, pregnancy rates per cycle were constant from age < 28 to 41, and then declined dramatically (by 50%) from age 42 to 44. For HMG and clomiphene + HMG cycles, pregnancy rates were twice the rates for CC before age 32, but declined sharply thereafter, and were the same as the pregnancy rates for clomiphene after age 37. The incidence of multiple implantations in clomiphene pregnancies was 15% before age 30 and 8 to 10% after age 30. No triplet implantations occurred after age 33 in clomiphene cycles. The incidence of multiple implantations exceeded 20% before age 35 in HMG pregnancies and before age 39 in clomiphene + HMG pregnancies. No triplet or higher-order births occurred after age 34 in HMG and clomiphene + HMG patients.
In HMG cycles, the number of follicles decreased with age, from 7.3 before age 28 to 3.5 for ages 42 to 43. In clomiphene + HMG cycles, the number of follicles decreased from 5.8 before age 28 to 3.3 for ages 42 to 43. The implantation rates per follicle were identical for all three stimulation regimens and decreased sharply after age 39.
Follicle number
In HMG and clomiphene + HMG cycles for patients less than 35 years of age, the incidence of three or more implantations per cycle (but not of twin implantations) was tripled, while pregnancy rates were not significantly increased, when E2 was over 1000 pg/mL, when six or more follicles were > or = 12mm, and when four or more follicles were > or = 15mm.
Estradiol (E2) level
The percentage of triplet and higher-order implantation rates was increased 5-fold when E2 was over 1000 pg/mL in HMG and clomiphene + HMG cycles (10.4% versus 2.0%). No triplet implantations occurred in the 608 clomiphene cycles in which E2 was measured.
Critical values for triplet and high-order pregnancies
In this study, pregnancy as well as triplet and higher-order implantations (but not twin implantations) were related to the number of follicles that were over 12 mm in clomiphene, HMG, and clomiphene + HMG cycles, and to E2 levels in HMG and clomiphene + HMG cycles. When values were below critical levels of six or more follicles >12mm, four or more follicles >15mm, and E2 levels >1000 in HMG and clomiphene + HMG cycles - and six or more follicles >12mm in CC cycles - triplet and higher-order implantations occurred in less than 1% of cycles and in less than 5% of pregnancies. When values were above these critical levels, triplet and higher-order implantations occurred in 2.8% to 3.2% of cycles and in 12% to 14% of pregnancies. The incidence of three or more implantations was identical in clomiphene and in HMG or clomiphene + HMG cycles when six or more follicles were >12mm. However, six or more follicles of >12mm occurred in only 5% of clomiphene cycles compared to 38% of HMG and 27% of clomiphene + HMG cycles. For patients age 35 and older, pregnancy rates in HMG and clomiphene + HMG cycles were doubled when six or more follicles were > or = 12mm without a significant increase in twin or higher order implantations. In clomiphene cycles, triple implantation occurred in 3.8% of cycles and 15.3% of pregnancies for patients less than 35 years old, when six or more follicles measured >12mm.
Conclusions:
Withholding HCG or IUI in clomiphene, HMG, and clomiphene + HMG cycles when six or more follicles are 12 mm or more in diameter may reduce triplet and higher-order implantations by 67% without significantly reducing pregnancy rates for patients under 35 years of age. For patients age 35 and older, withholding HCG under the same circumstances may decrease pregnancy rates by half without significantly reducing multiple implantations.
Comments about the study (by Dr. Sherbahn):
Triplet and higher-order pregnancies are to be avoided as much as possible. Infertility specialists and patients both should be very careful when considering treatment options, and when deciding whether to proceed with an IUI cycle - or cancel it - when several follicles are present on ultrasound. Studies like this can help us to make the most informed "educated guess" about what to do. This is a good and needed study in our field. Although other studies have investigated similar issues, this study was large and fairly well controlled, as well as prospective (looking at what happens in the future, after the study is designed, rather than looking at patient charts to see what happened in the past). This research confirms and details what we already knew in more general terms - that there is a good correlation between the number of "larger" follicles visible on ultrasound and the risks for multiple pregnancy after ovarian stimulation with clomiphene or with injectable gonadotropins (HMG). This study helps us to better understand the "average risks" involved with stimulation cycles with multiple follicles in the 12 - 20 mm (or larger) range. Women under 35 were at high risk for multiples when there were six or more follicles 12 mm or more in diameter. However, for women over 35, the pregnancy rate was improved when there were six or more follicles in that size range, without significantly increasing the multiple implantation rate. We need to be careful about this. There is not a sudden change in the egg quantity and quality that occurs on a woman's 35th birthday. The changes will be gradual, and the decision-making regarding a "safe" number of follicles should take that into account. No study can ever tell us what will happen in an individual case. The information in this study can help us to regulate the ovarian stimulations in our patients more appropriately. We also need to be willing to cancel cycles that are at high risk for triplets because of development of too many follicles (or convert these cycles to IVF if the patient prefers).
You might also like
- Sem 10 PortfolioDocument14 pagesSem 10 PortfolioNaliniNo ratings yet
- Rectal Prolapse 1Document6 pagesRectal Prolapse 1NaliniNo ratings yet
- (Notes) Bipolar Disorder and Mood StabilizersDocument7 pages(Notes) Bipolar Disorder and Mood StabilizersNaliniNo ratings yet
- Otolaryngology PDA Toronto NotesDocument29 pagesOtolaryngology PDA Toronto NotesNor Aimi Abd Rahman100% (1)
- MCQ PallorDocument4 pagesMCQ PallorNalini50% (2)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- A History of Developments To Improve in Vitro Ferti Lizati OnDocument4 pagesA History of Developments To Improve in Vitro Ferti Lizati OnichaNo ratings yet
- In Vitro FertilizationDocument10 pagesIn Vitro FertilizationMoe AboamNo ratings yet
- AI and ET in Mares 2011Document5 pagesAI and ET in Mares 2011Andy jamesNo ratings yet
- Forty Years of Embryo Transfer in CattleDocument18 pagesForty Years of Embryo Transfer in CattleFodi Beatriz Huarcaya AyhuaNo ratings yet
- Isabr 2008Document169 pagesIsabr 2008Cláudia KiyaNo ratings yet
- Assisted Reproductive TechnologyDocument28 pagesAssisted Reproductive TechnologyftvyvyvNo ratings yet
- Infertility Treatment Options Western Medications and Eastern ProceduresDocument13 pagesInfertility Treatment Options Western Medications and Eastern Proceduresboron32No ratings yet
- Advances and Limitations of in Vitro Embryo Production in Sheep and Goats, Menchaca Et Al., 2016Document7 pagesAdvances and Limitations of in Vitro Embryo Production in Sheep and Goats, Menchaca Et Al., 2016González Mendoza DamielNo ratings yet
- (Libro) The Role of Biotechnology in Improvement of Livestock Animal Health and Biotechnology-Muhammad Abubakar, Ali Saeed, ODocument151 pages(Libro) The Role of Biotechnology in Improvement of Livestock Animal Health and Biotechnology-Muhammad Abubakar, Ali Saeed, OramsesmuseNo ratings yet
- Maxwell, Noyes, Keefe, Berkeley, & Goldman, 2017Document4 pagesMaxwell, Noyes, Keefe, Berkeley, & Goldman, 2017Anonymous 75M6uB3OwNo ratings yet
- InVitroFertilization IVF KP AnalysisDocument14 pagesInVitroFertilization IVF KP AnalysisOvn Murthy100% (1)
- CARTR Plus Upload Specification v1.5.1 - Final BBS Comments 01052022Document139 pagesCARTR Plus Upload Specification v1.5.1 - Final BBS Comments 01052022josephkhouryNo ratings yet
- Infertility PDFDocument12 pagesInfertility PDFdian_c87100% (1)
- Infertility NirwenDocument55 pagesInfertility Nirwenpok yeahNo ratings yet
- Training Manual For EmbryoDocument158 pagesTraining Manual For Embryotolimania2951No ratings yet
- Interventions For Endometriosis-Related Infertility: A Systematic Review and Network Meta-AnalysisDocument11 pagesInterventions For Endometriosis-Related Infertility: A Systematic Review and Network Meta-Analysismuhammad hafidzNo ratings yet
- ESHRE COS Guideline - Final 09102019Document136 pagesESHRE COS Guideline - Final 09102019Raluca HabaNo ratings yet
- Hormones Reproduction: 6.6, Homeostasis andDocument41 pagesHormones Reproduction: 6.6, Homeostasis andSeanLaiNo ratings yet
- ART Rules March, 2022-1 PDFDocument96 pagesART Rules March, 2022-1 PDFsasankNo ratings yet
- Advances Embryo TransferDocument258 pagesAdvances Embryo Transferpasseriforme0% (1)
- Super Ovulation of EwesDocument1 pageSuper Ovulation of EwesgnpobsNo ratings yet
- Immature Oocyte Incidence Contributing Factors and Effects OnDocument7 pagesImmature Oocyte Incidence Contributing Factors and Effects OnTrang Nguyễn NhưNo ratings yet
- Gonadotropins in ARTDocument37 pagesGonadotropins in ARTVarun DhallNo ratings yet
- DR Sohani VermaDocument46 pagesDR Sohani VermaKosygin LeishangthemNo ratings yet
- A New Classification For Female InfertilityDocument125 pagesA New Classification For Female InfertilityIndah Pratiwi100% (1)
- Bo 1994 TheriogenologyDocument16 pagesBo 1994 TheriogenologyGilson Antonio PessoaNo ratings yet
- Artificial InseminationDocument19 pagesArtificial InseminationDonna Lei G. RosarioNo ratings yet
- Gonal F - RFF 75 IU Instruction - For - UseDocument20 pagesGonal F - RFF 75 IU Instruction - For - UseKirubakaranNo ratings yet
- Ovarian Hyperstimulation SyndromeDocument5 pagesOvarian Hyperstimulation SyndromeReni ReniNo ratings yet
- Fertility AssessmentDocument38 pagesFertility AssessmentSkmc InfertilityNo ratings yet