Professional Documents
Culture Documents
Arrhythmias
Uploaded by
José Miguel SeguroOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Arrhythmias
Uploaded by
José Miguel SeguroCopyright:
Available Formats
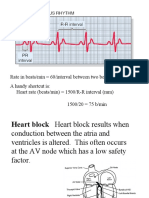
Rate in beats/min = 60/interval between two beats in seconds A handy shortcut is: Heart rate (beats/min) = 1500/R-R interval
(mm) 1500/20 = 75 b/min
Heart block Heart block results when conduction between the atria and ventricles is altered. This often occurs at the AV node which has a low safety factor.
First degree - prolonged PR interval only. The normal PR interval is 0.12 to 0.21 seconds. A PR interval >0.21 would be classified as first degree block. Usually this block is above His bundle
Second degree - some P waves are not followed by QRS. Often has a regular sequence, i.e., 2:1 or 3:2. The first number is the number of P waves present and the second is the number of QRSs. What is this?
Mobitz I (Wenckebach) the PR progressively lengthens with one P wave for every QRS until a beat is dropped. Usually the block is above His bundle. This is common in coronary patients and is caused by increased vagal tone and usually eventually disappears with no problems
Mobitz II the PR is constant but with occasional dropped beats. This is a more serious arrhythmia because the injury is probably in fast conducting tissue below the His bundle which is not under vagal control.
This is unambiguously Mobitz II It is a dangerous arrhythmia because the heart may suddenly start beating very slowly or even stop.
Complete heart block. Since there is no conduction down the AV node pathway atria and ventricles beat regularly but at different rates.
Slow ventricular rate Usually treated with pacemaker May be temporary or intermittent. Can be induced by drugs that cause increased vagotonia
WPW: Normally conducting cardiac muscle bridges the gap between atria and ventricles. The accessory pathway activates the ventricle before normal activation via the AV node.
The PR interval is <0.12 sec Delta waves are usually present
Can get retrograde conduction causing reentry and a tachyarrhythmia. If accessory pathway has short antegrade refractory period, can allow the ventricle to beat too fast with atrial fibrillation
Fig 3
Sinus Tachycardia >100b/min 1. Normal P waves
Normal sinus rhythm
2. Normal or shortened PR interval 3. QRS and T vectors are normal 4. ST segments are normal
Sinus tachycardia
5. RR interval short <15mm 1500/100 = 15
Sinus bradycardia
Fig 3
Sinus Bradycardia <60b/min
Normal sinus rhythm
1. P waves are present and all are followed by a QRS 2. Normal and constant PR interval 3. QRS and T vectors are normal
Sinus tachycardia
4. ST segments are normal 5. RR interval long >25mm 1500/60 = 25
Sinus bradycardia
Premature ventricular contraction (PVC) 1. Arises from ectopic focus in ventricles 2. Early QRS not preceded by a P wave (see fig 4) 3. Will have an unusual QRS shape a) odd vector b) prolonged QRS duration
Premature ventricular contraction (PVC) 1. Arises from ectopic focus in ventricles 2. Early QRS not preceded by a P wave (see fig 4) 3. Will have an unusual QRS shape a) odd vector b) prolonged QRS duration 4. A compensatory pause
Multifocal PVCs. Two separate foci are originating PVCs Irritable ventricle IF all PVC are identical it is from one ectopic site (Unifocal).
Premature atrial contraction (PAC) 1. Arises from an ectopic focus in the atria. 2. Will have an identifiable P wave but the shape of the P wave may be altered 3. May have a normal QRS 4. May have a compensatory pause
The compensatory pause is lacking because the SA node was reset. The rhythm has been shifted.
The QRS may be altered if some of the ventricle is still in its refractory period.
Atrial fibrillation 1. Irregularly irregular 2. No P waves
The AV node keeps the ventricular rate low May be treated with drugs to depress AV conduction and slow the ventricular rhythm: Beta blockers, calcium channel blockers
Common: will occur in about 1/3 of the population Not a serious arrhythmia unless in WPW
Electrical reentry can cause fibrillations and tachycardias.
Ventricular tachycardia (Fig 9) 1. Regularly occurring rhythm originating from a regular ventricular ectopic focus. 2. QRS morphology is usually like a PVC
Because the cardiac output is very low it usually produces myocardial ischemia and often progresses to ventricular fibrillation
Ventricular fibrillation (VF) 1. Thought to be a reentrant excitation of the ventricles; premature impulse may arise during vulnerable period 2. Irregular baseline with no identifiable waves
3. No cardiac output. Usually the cause of "sudden death" 4. May be the result of ischemia, lightning strike, electrocution, chest trauma, or drugs 5. Requires CPR and electrical difibrillation. Patients do not spontaneously recover.
Extended phase two cause long QT syndrome.
12 blocks
Q-T interval is ratedependent and is an index of the duration of phase 2 in the ventricular AP 12 x 40 = 480 ms
Long QT syndrome Prolonged duration of phase 2 causes an early afterdepolarization. That can trigger an early action potential causing a reentrant tachycardia Patients may experience attacks of VT with torsades de pointes - a waxing and waning of the QRS morphology (as if circling around a point).
3. Long QT is induced by some drugs and can be due to genetic abnormalities in some potassium and calcium channels. At present 5 separate genetic defects have been identified which cause long QT
14 STEPS TO ASSURE A SUCCESSFUL READING AND UNDERSTANDING OF AN UNKNOWN ECG 1. Is the ventricular rhythm regular? 2. Are there P waves? 3. Is the atrial rhythm regular? 4. Is there one P wave for each QRS? 5. What are the atrial and ventricular rates? 6. What is the P-R interval? 7. Is the P-R interval constant? 8. Are there extra or premature beats? 9. What is the QRS duration? 10. Does the QRS morphology indicate presence of a conduction defect? 11. What is the mean electrical QRS axis? 12. What is the mean electrical P wave axis? 13. Is there S-T segment deviation? 14. Are there pathologic Q waves?
Fig 12 a summary of heart blocks.
Fig 13 a summary of other arrhythmias.
You might also like
- Rate in Beats/min 60/interval Between Two Beats in Seconds A Handy Shortcut Is: Heart Rate (Beats/min) 1500/R-R Interval (MM) 1500/20 75 B/minDocument37 pagesRate in Beats/min 60/interval Between Two Beats in Seconds A Handy Shortcut Is: Heart Rate (Beats/min) 1500/R-R Interval (MM) 1500/20 75 B/minLuis AlayoNo ratings yet
- ECG NormalDocument9 pagesECG NormalDya AndryanNo ratings yet
- Interpret ECG Rhythms & Manage ArrhythmiasDocument6 pagesInterpret ECG Rhythms & Manage Arrhythmiasjh_ajjNo ratings yet
- Ipd Kuliah Ekg Blok KegawatdaruratanDocument118 pagesIpd Kuliah Ekg Blok Kegawatdaruratansiti solikhaNo ratings yet
- Clinical Teaching Ecg InterpretationDocument25 pagesClinical Teaching Ecg InterpretationAnusha VergheseNo ratings yet
- EkggDocument44 pagesEkggLedy ErvitaNo ratings yet
- Electrocardiograph Y: Dr. Fatimah Eliana, SPPD, Kemd, FinasimDocument118 pagesElectrocardiograph Y: Dr. Fatimah Eliana, SPPD, Kemd, FinasimTommy WidjayaNo ratings yet
- P Wave With A Broad ( 0.04 Sec or 1 Small Square) and Deeply Negative ( 1 MM) Terminal Part in V1 P Wave Duration 0.12 Sec in Leads I and / or IIDocument9 pagesP Wave With A Broad ( 0.04 Sec or 1 Small Square) and Deeply Negative ( 1 MM) Terminal Part in V1 P Wave Duration 0.12 Sec in Leads I and / or IIpisbolsagogulamanNo ratings yet
- Abnomalites of ECGDocument81 pagesAbnomalites of ECGgrreddy8364320No ratings yet
- ? Ecg ?Document60 pages? Ecg ?Nurul SyafiqahNo ratings yet
- Prof. Maila Claire A. Lichauco, RN, MANDocument86 pagesProf. Maila Claire A. Lichauco, RN, MANCedie GomezNo ratings yet
- Kamis 10 September 2015 - IPD 2 - Kuliah-Ekg-Blok-KegawatdaruratanDocument118 pagesKamis 10 September 2015 - IPD 2 - Kuliah-Ekg-Blok-KegawatdaruratanIrfanArifZulfikarNo ratings yet
- ECG ReadingDocument11 pagesECG ReadingSuresh Shrestha100% (1)
- Ventricular FibrilationDocument22 pagesVentricular FibrilationCalvin Martin LeeNo ratings yet
- Definition ECGDocument8 pagesDefinition ECGMelody BoadoNo ratings yet
- I.Sinus Rhythms and Sinus ArrhythmiasDocument64 pagesI.Sinus Rhythms and Sinus ArrhythmiashirschmedNo ratings yet
- ECG InterpretationDocument11 pagesECG InterpretationAndrea AndradaNo ratings yet
- 1st, 2nd, 3rd Degree AV BLockDocument8 pages1st, 2nd, 3rd Degree AV BLockladydreamer_92No ratings yet
- ECG-Arrhythmias: Tiang Soon WeeDocument63 pagesECG-Arrhythmias: Tiang Soon WeeasdasdasdasNo ratings yet
- ECG Approach by DR SSSDocument51 pagesECG Approach by DR SSSAritro DasguptaNo ratings yet
- ECG Dysrhthmias IIIDocument31 pagesECG Dysrhthmias IIIAmani KayedNo ratings yet
- Atrio Ventricular Blockage - FinalDocument14 pagesAtrio Ventricular Blockage - Finalclear mindNo ratings yet
- NCM 103 (LEC) : Electrocardiogram (ECG) ElectrocardiogramDocument10 pagesNCM 103 (LEC) : Electrocardiogram (ECG) ElectrocardiogramJohn Protacio50% (2)
- Workshop Pit IV THN 2017Document57 pagesWorkshop Pit IV THN 2017anettepardedeNo ratings yet
- KRIZELDocument13 pagesKRIZELKrizel Adina TanNo ratings yet
- Ecg RhythmsDocument9 pagesEcg RhythmsNoreena PrincessNo ratings yet
- How To Read An ECGDocument15 pagesHow To Read An ECGcharlyn206No ratings yet
- Dysrhytmia NotesDocument11 pagesDysrhytmia NoteshannahhwolfNo ratings yet
- Cardiology Notes USMLE Step CKDocument135 pagesCardiology Notes USMLE Step CKArianna BetancourtNo ratings yet
- ECG - Complete Heart BlockDocument2 pagesECG - Complete Heart BlockCsilla DobrescuNo ratings yet
- Arrhythmia Diagnosis and ManagementDocument44 pagesArrhythmia Diagnosis and ManagementanwarNo ratings yet
- Ecg Rhythms: Normal Sinus RhythmDocument10 pagesEcg Rhythms: Normal Sinus RhythmJethJayme100% (1)
- ECG Interpretation SkillsDocument46 pagesECG Interpretation SkillsSumeet TripathiNo ratings yet
- How To Read An ECGDocument15 pagesHow To Read An ECGSarah RonquilloNo ratings yet
- Broad Complex Tachycardia-LatestDocument96 pagesBroad Complex Tachycardia-LatestEsayas KebedeNo ratings yet
- How To Read An ECGDocument24 pagesHow To Read An ECGredroseeeeeeNo ratings yet
- Normal Sinus RhythmDocument8 pagesNormal Sinus RhythmRosalyn YuNo ratings yet
- RhythmDocument8 pagesRhythmparkmickyboo100% (1)
- Defibrillation vs Cardioversion: Key DifferencesDocument3 pagesDefibrillation vs Cardioversion: Key DifferencesStephy SojanNo ratings yet
- 5 - Ventricular Tachyarrhythmias DoneDocument79 pages5 - Ventricular Tachyarrhythmias Doneclaimstudent3515No ratings yet
- How To Read An ECG: Confirm DetailsDocument15 pagesHow To Read An ECG: Confirm DetailsRinothja RajaratnamNo ratings yet
- Principles of ECGDocument11 pagesPrinciples of ECGDeinielle Magdangal RomeroNo ratings yet
- Normal Sinus RhythmDocument13 pagesNormal Sinus RhythmJackson Yovin ChellyadhasNo ratings yet
- 16-Handout - ECG Interpretation (Study This)Document38 pages16-Handout - ECG Interpretation (Study This)Sa GhNo ratings yet
- Kuliah EKG Blok Kegawatdaruratan September 2018Document122 pagesKuliah EKG Blok Kegawatdaruratan September 2018khanzaisdiharanaNo ratings yet
- 3881 - Prosedur Pendaftaran Internship Per November 2016Document57 pages3881 - Prosedur Pendaftaran Internship Per November 2016Munawir_Syam91No ratings yet
- Ekg NetDocument15 pagesEkg NetDewi AyuNo ratings yet
- Kuliah EKG II Unswagati 2016Document77 pagesKuliah EKG II Unswagati 2016iikNo ratings yet
- How To Read An ECGDocument21 pagesHow To Read An ECGSlychenkoNo ratings yet
- First Degree Atrioventricular BlockDocument3 pagesFirst Degree Atrioventricular BlockShreyas WalvekarNo ratings yet
- 1.4. Kuliah KBK S03 - Mekanisme Peny Jantung Iskemik - UNSRAT 28 Sept 2020Document40 pages1.4. Kuliah KBK S03 - Mekanisme Peny Jantung Iskemik - UNSRAT 28 Sept 2020FAUZAN ILHAM PRATAMANo ratings yet
- ECG and ArrhythmiasDocument25 pagesECG and ArrhythmiasRashed ShatnawiNo ratings yet
- A Simplified ECG GuideDocument4 pagesA Simplified ECG GuidecherryNo ratings yet
- ArrhythmiaDocument25 pagesArrhythmiad_94No ratings yet
- Pediatrics ECG by DR Ali Bel KheirDocument9 pagesPediatrics ECG by DR Ali Bel KheirFerasNo ratings yet
- Supplementary Material 4.3 Cardiac Rhythm Disorders-2Document14 pagesSupplementary Material 4.3 Cardiac Rhythm Disorders-2Andrea Love PalomoNo ratings yet
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookFrom EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookNo ratings yet
- 12 Lead ECG Color Codes 1 - 04Document62 pages12 Lead ECG Color Codes 1 - 04ChrisieNo ratings yet
- Electrocardiography - Wikipedia, The Free EncyclopediaDocument18 pagesElectrocardiography - Wikipedia, The Free Encyclopediapayments8543No ratings yet
- FLUKE ProSim 8 User Manual 3Document30 pagesFLUKE ProSim 8 User Manual 3Zurab SanikidzeNo ratings yet
- Ele&Arr&Com&Rev&Das&Zip&1 STDocument492 pagesEle&Arr&Com&Rev&Das&Zip&1 STeuinpersoana100% (2)
- Apical Hypertrophic Cardiomyopathy (AHC) : Robert Buttner Mike CadoganDocument36 pagesApical Hypertrophic Cardiomyopathy (AHC) : Robert Buttner Mike CadoganDeliberate self harmNo ratings yet
- Biomedical Signal Processing ChaptersDocument3 pagesBiomedical Signal Processing ChaptersDeepak GowdaNo ratings yet
- ... & More: ECG ChallengeDocument2 pages... & More: ECG ChallengehameunjungNo ratings yet
- 2010 Ieee Titb OreskoDocument7 pages2010 Ieee Titb OreskoPedro ContrerasNo ratings yet
- Understanding Basics of EKG: by Alula A. (R III)Document37 pagesUnderstanding Basics of EKG: by Alula A. (R III)sky nutsNo ratings yet
- 3183 HeartVue CardioDM 06 User's ManualDocument84 pages3183 HeartVue CardioDM 06 User's ManualGP RSUINo ratings yet
- ECG Learning PackageDocument19 pagesECG Learning Packagearulsidd74No ratings yet
- Dr. Anas Yasin - MDDocument58 pagesDr. Anas Yasin - MDMahfouzNo ratings yet
- Prototype Low-Cost Portable Electrocardiogram (ECG) Based On Arduino-Uno With Bluetooth FeatureDocument9 pagesPrototype Low-Cost Portable Electrocardiogram (ECG) Based On Arduino-Uno With Bluetooth FeatureInformatica hpjcNo ratings yet
- Eet312 Module IDocument107 pagesEet312 Module IAnandu DipukumarNo ratings yet
- Matlab Implementation of Pan Tompkins ECG QRS Detector.: 1 BackgroundDocument3 pagesMatlab Implementation of Pan Tompkins ECG QRS Detector.: 1 BackgroundRabah AmidiNo ratings yet
- Ecg MonitoringDocument26 pagesEcg Monitoringclaire yowsNo ratings yet
- ECG Interpretation Guide for Pathologic RhythmsDocument108 pagesECG Interpretation Guide for Pathologic RhythmsVisan Andreea Mihaela RamonaNo ratings yet
- Schiller MT101 MT200 User ManualDocument96 pagesSchiller MT101 MT200 User ManualelcongograndeNo ratings yet
- EKG Crash Course NuRsing 390 SMC - 4Document57 pagesEKG Crash Course NuRsing 390 SMC - 4m1k0e100% (2)
- Recognizing Normal ECGDocument50 pagesRecognizing Normal ECGJosiephine Bucalon100% (2)
- Basic EKG Interpretation Exam AnswersDocument3 pagesBasic EKG Interpretation Exam AnswerstwdroppointNo ratings yet
- FastingDocument21 pagesFastingtpau6272100% (1)
- Sugiyono, S.Kep., Ners., M.KepDocument48 pagesSugiyono, S.Kep., Ners., M.KepHervin RamadhaniNo ratings yet
- Sinus ArrhythmiaDocument6 pagesSinus ArrhythmiaVincent Maralit MaterialNo ratings yet
- Day 3 - EKGDocument115 pagesDay 3 - EKGchristian murtaniNo ratings yet
- RH RV TutorialDocument97 pagesRH RV TutorialTavpritesh SethiNo ratings yet
- Test Bank For Respiratory Disease A Case Study Approach To Patient Care 3rd Edition by WilkinsDocument10 pagesTest Bank For Respiratory Disease A Case Study Approach To Patient Care 3rd Edition by Wilkinsa498226706No ratings yet
- Rigel Uni Sim Lite DatasheetDocument5 pagesRigel Uni Sim Lite Datasheetmailalexmd.vrn.ruNo ratings yet
- Ecg Utah EduDocument87 pagesEcg Utah EduMos Viorel DanutNo ratings yet
- Serial Comparison Algorithm ReferenceDocument28 pagesSerial Comparison Algorithm ReferenceHoàng Anh NguyễnNo ratings yet