Professional Documents
Culture Documents
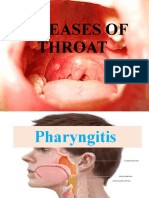
Acute Pharyngitis and Tonsillitis Guide
Uploaded by
william_Satyanegara0 ratings0% found this document useful (0 votes)
9 views56 pagesRespirologi
Original Title
Pemicu 3 (Anak)
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentRespirologi
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views56 pagesAcute Pharyngitis and Tonsillitis Guide
Uploaded by
william_SatyanegaraRespirologi
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 56
Pemicu 3 (Anak)
William Gilbert Satyanegara
Acute Pharyngitis
• Pharyngitis refers to inflammation of the pharynx, including
erythema, edema, exudates, or an enanthem (ulcers, vesicles)
• related to environmental exposures
• Acute infections of the upper respiratory tract account for a
substantial number of visits to pediatricians and many feature sore
throat as a symptom or evidence of pharyngitis on physical
examination
Infection Etiologies
Infection Etiologies –Virus–
• Herpes simplex virus infection;
• Gingivostomatitis and ulcerating vesicles throughout the anterior
pharynx and on the lips are seen in primary oral.
• High fever and difficulty taking oral fluids are common. This infection
can last for 14 days
• Enteroviruses;
• Discrete papulovesicular lesions or ulcerations in the posterior
oropharynx, severe throat pain, and fever are characteristic of
herpangina
Infection Etiologies –Virus–
• Hand-foot-mouth disease;
• Vesicles or ulcers throughout the oropharynx, vesicles on the palms and soles,
and sometimes on the trunk and extremities.
• Coxsackie a16 is the most common agent, but enterovirus 71 and coxsackie a6
can also cause this syndrome
• Adenoviruses cause pharyngitis. When there is conccurrent conjunctivitis the
syndrome is called pharyngoconjunctival fever.
• The pharyngitis tends to resolve within 7 days but conjunctivitis may persist for
up to 14 day
• Outbreaks of a unique clinical illness caused by adenovirus types 3, 7, 2, 4, 7a,
11, and1 4, called pharyngoconjunctival fever
Infection Etiologies –Virus–
• Measles Intense, diffuse pharyngeal erythema and Koplik spots,
the pathognomonic enanthem
• Epstain-Barr virus Splenomegaly or hepatomegaly
• infectious mononucleosis adolescent with exudative tonsillitis
• Primary infection with HIV;
• acute retroviral syndrome, with non-exudative pharyngitis, fever,
maculopapular rash, arthralgia, myalgia, adenopathy, and often a
maculopapular rash.
Infection Etiologies – Bacteria –
• Group C and Group G streptococcus and A. haemolyticum pharyngitis
have been diagnosed most commonly in adolescents and adults.
• F. necrophorum has been suggested to be a fairly common cause of
pharyngitis in older adolescents and adults (15-30 yr old)
• F. necrophorum pharyngitis is associated with development of
Lemierre syndrome, internal jugular vein septic thrombophlebitis.
• symptoms may persist, neck pain and swelling develop, and the
patient appears toxic
Infection Etiologies – Bacteria –
• Gonococcal pharyngeal infections are usually asymptomatic but can
cause acute pharyngitis with fever and cervical lymphadenitis.
• Corynebacterium diphtheria;
• Physical findings are bull neck (extreme neck swelling) and a gray
pharyngeal pseudomembrane that can cause respiratory obstruction.
• M. Pneumoniae and C. Pneumoniae are may also have same sign and
symptom like C.Diphtheria. Severe or persistent cough subsequent to
pharyngitis may be the clue to infection with one of these organisms
Infection Etiologies – Group A
Streptococcus –
• quite common among children 5-15 yr old.
• incubation period of 2-5 days, pharyngeal infection rapid onset of
significant sore throat and fever.
• The pharynx is red, the tonsils are enlarged and often covered with a
white, grayish, or yellow exudate that may be blood-tinged.
• There may be petechiae or “doughnut” lesions on the soft palate and
posterior pharynx and the uvula may be red and swollen
• strawberry tongue / white strawberry tongue
Infection Etiologies – Group A
Streptococcus –
• Enlarged and tender anterior cervical lymph nodes.
• Ear pain is a frequent complaint but the tympanic membranes are
usually normal.
• Patients with gas that produce exotoxin a, b, or c may demonstrate
the fine red, papula rash of scarlet fever.
• Begins on the face and then becomes generalized.
• Rash blanches with pressure and it may be more intense in skin
creases, especially in the antecubital fossae, axillae, and inguinal
creases (pastia’s lines or pastia’s sign)
Clinical Manifestation
• Infection begins with the typical signs and symptoms of pharyngitis
such as sore throat, dysphagia, and fever, usually in an older child who
often has a history of recurrent tonsillitis
• Systemic symptoms such as malaise, poor appetite, and chills appear
early, and mild dehydration may develop.
• The child has a toxic appearance, and trismus almost always occurs.
Characteristic signs are a muffl ed (hot potato) voice, trismus, and
major leucocytosis.
Diagnosis
• Diagnosis ditegakkan berdasakan gejala klinis, pemeriksaan fisis dan
pemeriksaan laboratorium
• Pemeriksaan baku emas pemeriksaan kultur dari apusan tenggorok
• Untuk mendeteksi Streptococcus Gorup A Rapid Antigen Detection
Tests
• Test Serologi baik dilakukan bila curiga terdapat infeksi EBV
• WBC Count paling baik dilakukan untuk infeksi CMV (terdapat
limfositosis dengan gambaran atypical lymphocyte)
Criteria McIsaac
• McIsaac Score ≥ 4 is associated
with positive laboratory test for
GAS in less than 70% of children
with pharyngitis.
Treatment
• Symptomatic therapy;
• Oral antipyretic/analgesic agent (acetaminophen or ibuprofen)
fever and sore throat pain
• Systemic corticosteroids evidence of upper airway compromise
due to mononucleosis
• Corticosteroid connot be recommended for treatment of most
pediatric pharyngitis.
Antibiotic Therapy
Recurrent pharyngitis
• Reinfection with the same M type if type-specific antibody has not
developed
• Poor compliance with oral antibiotic therapy
• Macrolide resistance if a macrolide was used for treatment
• Infection with a new M type.
• Treatment with intramuscular benzathine penicillin eliminates
nonadherence to therapy
Complication and Prognosis
• Bacterial middle ear infections and bacterial sinusitis
• Complications of GAS pharyngitis include
• Local suppurative complications, such as parapharyngeal abscess
• Nonsuppurative illnesses;
• ARF (Acute Rheumatic Fever)
• APSGN (Acute Post Streptococcal Glomerulonephritis)
• Poststreptococcal reactive arthritis
• PANDAS (Pediatrics Autoimmune Neuropsychiatric Disorders Associated With S.
Pyogenes)
• CANS (childhood acute neuropsychiatric symptoms).
Tonsilitis
• Acute Infection
• Most episodes of acute pharyngotonsillitis are caused by viruses
• Group A β-hemolytic streptococcus (GABHS) is the most common
cause of bacterial infection in the pharynx.
• Chronic Infection chronically infected by multiple microbes;
• β-lactamase– producing organisms
• aerobic species H. Inffluenzae
• anaerobic species Peprosteptococcus, Prevotella, Fusobacterium
Clinical Manifestation – Acute
Infection –
• Symptoms of GABHS infection include;
• Odynophagia, dry throat, malaise, fever and chills, dysphagia, referred
otalgia, headache, muscular aches, and enlarged cervical nodes.
• Signs include;
• Dry tongue, erythematous enlarged tonsils, tonsillar or pharyngeal
exudate, palatine petechiae, and enlargement and tenderness of the
jugulodigastric lymph nodes
Clinical Manifestation – Chronic
Infection –
• halitosis, chronic sore throats, foreign-body sensation, or a history of
expelling foul-tasting and foul-smelling cheesy lump.
• Examination reveals tonsils of a range of sizes which often they
contain copious debris within the crypts.
Clinical Manifestation – Airway
Obstruction–
• Daytime symptoms chronic mouth breathing, nasal obstruction,
hyponasal speech, hyposmia, decreased appetite, poor school
performance, and, rarely, symptoms of right-sided heart failure.
• Nighttime symptoms loud snoring, choking, gasping, frank apnea,
restless sleep, abnormal sleep positions, somnambulism, night
terrors, diaphoresis, enuresis, and sleep talking
Treatment – Medical Management –
Tonsillectomy
Acute Infectious Laryngitis
• Viruses cause most cases; diphtheria is an exception but is extremely
rare in industrialized countries.
• onset is usually characterized by an upper respiratory tract infection
during which sore throat, cough, and hoarseness.
• Hoarseness and loss of voice may be out of proportion to systemic signs
and symptoms.
• Epinephrine (1 : 1,000 dilution in dosage of 0.01 ml/kg to a maximum of
0.5 ml/dose) administered intramuscularly.
• Corticosteroids are often required (1-2 mg/ kg/24 hr of prednisone for
3-5 days)
Acute Epiglottitis
• Characterized by an acute rapidly progressive and potentially
fulminating course of high fever, sore throat, dyspnea, and rapidly
progressing respiratory obstruction.
• Drooling is usually present and the neck is hyperextended in an
attempt to maintain the airway.
• The child may assume the tripod position, sitting upright and leaning
forward with the chin up and mouth open while bracing on the arms.
Infection Etiologies
• H. Influenzae most common
• Other S. aureus, S. pnemoniae, C. albicans, virus, trauma
Acute Epiglottitis
• The diagnosis requires visualization
under controlled circumstances of a
large, cherry red, swollen epiglottis by
laryngoscopy.
• Classic radiographs of a child who has
epiglottitis show the thumb sign
Treatment
• All patients should receive oxygen route unless the mask causes
excessive agitation.
• Establishing an airway by endotracheal or nasotracheal intubation or,
less often, by tracheostomy is indicated in patients with epiglottitis.
• Cultures of blood, epiglottic surface, and, in selected cases,
cerebrospinal fluid should be collected after
• Cefotaxime, ceftriaxone, or meropenem should be given parenterally,
pending culture and susceptibility reports, because 10-40% of H.
influenzae type b cases are resistant to ampicillinr the airway is
stabilized
Retropharyngeal Abscess Lateral
Pharyngeal (Parapharyngeal)
Abscess
• Occurs most commonly in children younger than 3-4 yr of age
• Clinical manifestations of retropharyngeal abscess are nonspecific and
include fever, irritability, decreased oral intake, and drooling.
• Neck stiffness, torticollis, and refusal to move the neck may also be
present.
• Muffled voice, stridor, respiratory distress, or even obstructive sleep
apnea.
Retropharyngeal Abscess Lateral
Pharyngeal (Parapharyngeal)
Abscess
• Physical examination can reveal bulging of the posterior pharyngeal
wall, although this is present in
• Cervical lymphadenopathy may also be present.
• Lateral pharyngeal abscess commonly presents as fever, dysphagia,
and a prominent bulge of the lateral pharyngeal wall, sometimes with
medial displacement of the tonsil.
Infection Etiologies
• Retropharyngeal and lateral pharyngeal infections usual pathogens
include;
• group A streptococcus
• Staphylococcus aureus
• S. aureus MRSA
• Other pathogens: Haemophilus influenzae, Klebsiella, and
Mycobacterium avium-intracellulare
Differential Diagnosis
• Acute epiglottitis
• Foreign body aspiration
• neck mobility
• meningitis
Diagnosis
• Incision and drainage and culture of an abscessed node provides the
definitive diagnosis
• CT can be useful in identifying the presence of a retropharyngeal,
lateral pharyngeal, or parapharyngeal abscess
Treatment
• Intravenous antibiotics with or without surgical drainage.
• Third-generation cephalosporin combined with ampicillin-sulbactam
or clindamycin to provide anaerobic coverage is effective.
• Drainage is necessary in the patient with respiratory distress or failure
to improve with intravenous antibiotic treatment
Complications
• Significant Upper Airway Obstruction
• Rupture Leading To Aspiration Pneumonia
• Extension To The Mediastinum
• Thrombophlebitis Of The Internal Jugular Vein
• Erosion Of The Carotid Artery Sheath
Croup (Laryngotracheobronchitis)
• Viruses typically cause croup, the most common form of acute upper
respiratory obstruction.
• Most patients have an upper respiratory tract infection with some
combination of rhinorrhea, pharyngitis, mild cough, and low-grade
fever for 1-3 days before the signs and symptoms of upper airway
obstruction become apparent.
• The characteristic “barking” cough, hoarseness, and inspiratory stridor
• Symptoms are characteristically worse at night and often recur with
decreasing intensity for several days and resolve completely within a
week
Croup (Laryngotracheobronchitis)
• Child may prefer to sit up in bed or be held upright
• Physical examination can reveal a hoarse voice, coryza, normal to
moderately inflamed pharynx, and a slightly increased respiratory rate
• Nasal flaring, suprasternal, infrasternal, and intercostal retractions
• Continuous stridor.
• The child who is hypoxic, cyanotic, pale, or obtunded needs
immediate airway management.
Diphtheria
• Diphtheria is an acute toxic infection caused by corynebacterium
species, typically corynebacterium diphtheria.
• Corynebacteria are aerobic, nonencapsulated, non–spore-forming,
mostly nonmotile, pleomorphic, gram-positive bacilli.
• Cystine-tellurite blood agar or tinsdale agar
• Spread is primarily by airborne respiratory droplets, direct contact
with respiratory secretions of symptomatic individuals, or exudate
from infected skin lesions
Pathogenesis
• C. diphtheria exotoxin, which inhibits protein synthesis and causes
local tissue necrosis.
• 1st few days of respiratory tract infection (usually in the pharynx), a
dense necrotic coagulum of organisms, epithelial cells, fibrin,
leukocytes, and erythrocytes forms, advances, and becomes a gray-
brown, leather-like adherent pseudomembrane (Diphthera is Greek
for leather).
• Paralysis of the palate and hypopharynx is an early local effect of
diphtheritic toxin
Clinical Manifestation (Respiratory
Tract)
• After incubation period of 2-4 days, local signs and symptoms of
inflammation develop.
• Infection of the anterior nares is more common among infants and
causes serosanguineous, purulent, erosive rhinitis with membrane
formation.
• Shallow ulceration of the external nares and upper lip is characteristic
• Unilateral or bilateral tonsillar membrane formation, which can extend
to involve the uvula, soft palate, posterior oropharynx, hypopharynx, or
glottic areas
• Enlarged lymph nodes can cause a bull-neck appearance
Diagnosis
• History
• Immunization
• Sign and symptoms
• Specimens for culture should be obtained from the nose and throat
and any other mucocutaneous lesion
Complications
• Toxic Cardiomyopathy
• Toxic Neuropathy
Treatment
• Antitoxin;
• Equine antitoxin intravenous administration of antitoxin is
preferred
• Before intravenous administration of antitoxin, tests for sensitivity to
horse serum should be performed according to instructions provided
with the material
Treatment – Antitoxin –
• Suggested dose ranges are:
• Pharyngeal or laryngeal disease of 2 days’ duration or less, 20 000 to
40 000 U
• Nasopharyngeal lesions, 40 000 to 60 000 U;
• Extensive disease of 3 or more days’ duration or diffuse swelling of
the neck, 80 000 to 120 000 U
Treatment – Antimicrobial Therapy –
• Erythromycin PO for 14 days
• Aqueous penicillin G administered intravenously for 14 day or,
• penicillin G procaine administered intramuscularly for 14 days
• Prevention Immunization
Jadwal Imunisasi
You might also like
- Ent Infection: Ridha Wahyutomo, SP - MK Clinical Microbiologist-Infection PreventionistDocument28 pagesEnt Infection: Ridha Wahyutomo, SP - MK Clinical Microbiologist-Infection PreventionistAnonymous 1GSeSV0No ratings yet
- Pedi Respir... DR - BrukDocument81 pagesPedi Respir... DR - BrukMatusala BafaNo ratings yet
- 4 - Pharyngitis BronchitisDocument31 pages4 - Pharyngitis BronchitisAishwaryaNo ratings yet
- 10 PharngitisDocument26 pages10 PharngitisCabdiNo ratings yet
- UPPER Respiratory Tract InfectionsDocument14 pagesUPPER Respiratory Tract InfectionsYousif Ahmed DANo ratings yet
- Diseases of Throat: Pharyngitis, Tonsillitis and AdenoiditisDocument39 pagesDiseases of Throat: Pharyngitis, Tonsillitis and Adenoiditismaria jacobNo ratings yet
- Upper Respıratory Tract InfectıonsDocument68 pagesUpper Respıratory Tract InfectıonsMekdes ZewdeNo ratings yet
- Infeksi Saluran Pernafasan Atas Blok 17 PSPDDocument48 pagesInfeksi Saluran Pernafasan Atas Blok 17 PSPDFahmiNo ratings yet
- Throat DisorderDocument46 pagesThroat DisorderKpj KpjNo ratings yet
- Unit V: Conti Upper Respiratory Tract Infection: PharyngitisDocument17 pagesUnit V: Conti Upper Respiratory Tract Infection: PharyngitisshaistaNo ratings yet
- Pediatric Nasopharyngeal Mass: Causes and ManagementDocument79 pagesPediatric Nasopharyngeal Mass: Causes and ManagementShahnawazNo ratings yet
- URTIDocument41 pagesURTIGetaneh LiknawNo ratings yet
- URTI (DR Hemin Khalid)Document21 pagesURTI (DR Hemin Khalid)Darawan MirzaNo ratings yet
- Acute Tonsillitis: Zhong Shixun PH.DDocument43 pagesAcute Tonsillitis: Zhong Shixun PH.DEINSTEIN2DNo ratings yet
- Pneumonia WW ReportDocument29 pagesPneumonia WW ReportAradhanaRamchandaniNo ratings yet
- AdenotonsilitisDocument42 pagesAdenotonsilitisELIA RICHARDNo ratings yet
- Pharyngitis Diagnosis and TreatmentDocument27 pagesPharyngitis Diagnosis and TreatmentSubhada GosaviNo ratings yet
- Felső Légúti FertőzésekDocument20 pagesFelső Légúti FertőzésekKondász Antal Gábor MedNo ratings yet
- Benign Diseases of LarynxDocument76 pagesBenign Diseases of Larynxranjeet kumar lalNo ratings yet
- عرض تقديميDocument19 pagesعرض تقديميJust muhannad AlharbiNo ratings yet
- Respi Patho 1Document111 pagesRespi Patho 1Quolette ConstanteNo ratings yet
- Respiratory Immun AllergyDocument125 pagesRespiratory Immun Allergyhasanatiya41No ratings yet
- Angina (Streptococcal Diphtheria, Herpes, Mononucleosis) - MumpsDocument83 pagesAngina (Streptococcal Diphtheria, Herpes, Mononucleosis) - MumpsBeni KelnerNo ratings yet
- Upper Respiratory Tract Infections.: DR Abdelmoniem Saeed MohammedDocument47 pagesUpper Respiratory Tract Infections.: DR Abdelmoniem Saeed MohammedYousef Al-AmeenNo ratings yet
- Adenotonsillitis NewDocument100 pagesAdenotonsillitis NewDrravikumar Bhandari100% (1)
- Non-Infectious Respiratory ProblemDocument66 pagesNon-Infectious Respiratory ProblemSven OrdanzaNo ratings yet
- File 18584Document12 pagesFile 18584Mohammed MuthanaNo ratings yet
- Acute Air Way Emergencies: Adisu B, MDDocument45 pagesAcute Air Way Emergencies: Adisu B, MDMelkamu TulbakeNo ratings yet
- Upper Respiratory AlterationDocument34 pagesUpper Respiratory AlterationJulia ManaloNo ratings yet
- ARIs CME2Document50 pagesARIs CME2JunaidahMubarakAliNo ratings yet
- Caring for a Child with Respiratory DisordersDocument62 pagesCaring for a Child with Respiratory DisordersErica Veluz LuyunNo ratings yet
- Otitis MediaDocument42 pagesOtitis MediaUchyIntamNo ratings yet
- 4 MumpsDocument18 pages4 MumpsAyu PratiwiNo ratings yet
- 5 Sore ThroatDocument45 pages5 Sore ThroatNurul Wandasari SNo ratings yet
- Pharyngitis, Tonsilitis, LaryngitisDocument62 pagesPharyngitis, Tonsilitis, Laryngitispashiem88No ratings yet
- PharyngitisDocument10 pagesPharyngitisGd SuarantaNo ratings yet
- Presenter: clerk 2 蘇雋淋 Date: 2022/03/11Document39 pagesPresenter: clerk 2 蘇雋淋 Date: 2022/03/11s0501120醫學系No ratings yet
- Pediatric NotesDocument61 pagesPediatric NotesMatusala BafaNo ratings yet
- Respiratory and Nosocomial InfectionsDocument70 pagesRespiratory and Nosocomial InfectionsCezar Alexander GuevaraNo ratings yet
- Respiratory Tract Infection PDFDocument64 pagesRespiratory Tract Infection PDFMaretah TaufahNo ratings yet
- Upper Airway Obstruction Causes and TreatmentsDocument15 pagesUpper Airway Obstruction Causes and TreatmentsPhilippe Ceasar C. BascoNo ratings yet
- Open Infections 2Document76 pagesOpen Infections 2Jehad AlzubairNo ratings yet
- Diseases of The Oropharynx & NasopharynxDocument38 pagesDiseases of The Oropharynx & Nasopharynxalmazmulu76No ratings yet
- Pharyngitis: Dr.M.KarimiDocument60 pagesPharyngitis: Dr.M.KarimiJessa AdenigNo ratings yet
- Pharyngitis: Departemen T.H.T.K.L Fakultas Kedokteran Universitas PadjadjaranDocument64 pagesPharyngitis: Departemen T.H.T.K.L Fakultas Kedokteran Universitas PadjadjaranEtusCelloNo ratings yet
- Diseases of Upper Respiratory System (URTI) : DR Sarwar Hussain, Assistant Professor Department of Pediatrics, NBUDocument36 pagesDiseases of Upper Respiratory System (URTI) : DR Sarwar Hussain, Assistant Professor Department of Pediatrics, NBUخالد مطرNo ratings yet
- Id 1 Ent Infections 2022Document33 pagesId 1 Ent Infections 2022白羽マイリフNo ratings yet
- 4 MumpsDocument18 pages4 MumpsNamira Caroline ErchoNo ratings yet
- Respi SDG Cluster3Document45 pagesRespi SDG Cluster3faye kimNo ratings yet
- Anatomi Tenggorokan Dan Penerapan Klinisnya: Dr. Adi Arianto, M. BiomedDocument39 pagesAnatomi Tenggorokan Dan Penerapan Klinisnya: Dr. Adi Arianto, M. BiomedAl AdinNo ratings yet
- สำเนา pharyngitisDocument47 pagesสำเนา pharyngitisThanawat SimaNo ratings yet
- URT PathologiesDocument58 pagesURT PathologiesFira'ol GabayoNo ratings yet
- Pedia Pulmo 2 10.18.16Document73 pagesPedia Pulmo 2 10.18.16Medisina101No ratings yet
- 14 Respiratory InfectionsDocument16 pages14 Respiratory InfectionsEsteban PrietoNo ratings yet
- Enteroviral InfectionsDocument32 pagesEnteroviral InfectionsTarik PlojovicNo ratings yet
- Adenotonsillar Diseases DrbugnahDocument37 pagesAdenotonsillar Diseases DrbugnahDr.Sherif Bugnah100% (8)
- Presentation URTI& LRTI - G1Document134 pagesPresentation URTI& LRTI - G1Aniq Zahran MasomNo ratings yet
- Respiratory Tract: Elijah Quiaño Miguel Quilit 1-NU01Document59 pagesRespiratory Tract: Elijah Quiaño Miguel Quilit 1-NU01im. EliasNo ratings yet
- Alvin M. Hernandez, RN, RM, MSN, Man Faculty, School of NursingDocument37 pagesAlvin M. Hernandez, RN, RM, MSN, Man Faculty, School of NursingkathnlscNo ratings yet
- High Consumption of Commercial Food Products Among Children Less Than 24 Months of Age and Product Promotion in Kathmandu Valley Nepal PDFDocument16 pagesHigh Consumption of Commercial Food Products Among Children Less Than 24 Months of Age and Product Promotion in Kathmandu Valley Nepal PDFwilliam_SatyanegaraNo ratings yet
- Adult: PO Pain 15-60 MG 4 Hrly. Max: 360 Mg/day. Cough SuppressantDocument13 pagesAdult: PO Pain 15-60 MG 4 Hrly. Max: 360 Mg/day. Cough Suppressantwilliam_SatyanegaraNo ratings yet
- Suh UuuuDocument1 pageSuh Uuuuwilliam_SatyanegaraNo ratings yet
- Chapter 13Document40 pagesChapter 13william_SatyanegaraNo ratings yet
- Part 7 Pyeloroplasty: Quick and BloodlessDocument31 pagesPart 7 Pyeloroplasty: Quick and BloodlessAnonymous MmiBnqnDyNo ratings yet
- Factors Affecting The Activity of Health Caders in The Discovery of Tuberculosis Cases in Kelurahan Sonorejo SukoharjoDocument7 pagesFactors Affecting The Activity of Health Caders in The Discovery of Tuberculosis Cases in Kelurahan Sonorejo SukoharjoIntan AyuNo ratings yet
- Nose Examination:: INSPECTION - ExternalDocument1 pageNose Examination:: INSPECTION - ExternalMark ColganNo ratings yet
- Othello Essay FinalDocument5 pagesOthello Essay Finalapi-244470959No ratings yet
- Inguinal HerniaDocument19 pagesInguinal HerniaAyu W. AnggreniNo ratings yet
- Enoxaparin FDADocument40 pagesEnoxaparin FDAImam Nur Alif Khusnudin100% (2)
- Peroneus Longus Tendon Rupture Case ReportDocument14 pagesPeroneus Longus Tendon Rupture Case ReportAlgivar DaudNo ratings yet
- Mh-Somatic Symptom Disorders - 2Document9 pagesMh-Somatic Symptom Disorders - 2martinNo ratings yet
- Indonesia Healthcare Outlook Nov 16 PDFDocument106 pagesIndonesia Healthcare Outlook Nov 16 PDFAnggunPramudaWardhaniSNo ratings yet
- First AidDocument4 pagesFirst Aidrebz100% (1)
- Drug MenuDocument17 pagesDrug MenukathlynmangasiNo ratings yet
- Post-Op Care and ComplicationsDocument52 pagesPost-Op Care and ComplicationsAbebayehu AyeleNo ratings yet
- Brescia-COVID Respiratory Severity Scale (BCRSS) AlgorithmDocument2 pagesBrescia-COVID Respiratory Severity Scale (BCRSS) AlgorithmAhraxazel Galicia ReynaNo ratings yet
- Introduction to Essay WritingDocument20 pagesIntroduction to Essay WritingTaiyaki Đậu ĐỏNo ratings yet
- Treasures of VijayakarDocument116 pagesTreasures of Vijayakarsurya100% (1)
- Genetic Disorder Brochure ProjectDocument1 pageGenetic Disorder Brochure ProjectErika ContrerasNo ratings yet
- Central Machinery Model 93212 Manual in EnglishDocument37 pagesCentral Machinery Model 93212 Manual in EnglishNoel0% (1)
- Rabies Health TalkDocument10 pagesRabies Health TalkAmit Ranjan100% (1)
- Porcelain Fused To Metal (PFM) Crowns and Caries in Adjacent TeetDocument5 pagesPorcelain Fused To Metal (PFM) Crowns and Caries in Adjacent Teetbaiq rengganis dewiNo ratings yet
- The Rules of The Cancer Patient Diet and Dr. Hammer GNMDocument71 pagesThe Rules of The Cancer Patient Diet and Dr. Hammer GNMshivapuja100% (1)
- QuestionsDocument19 pagesQuestionsFatma AlbakoushNo ratings yet
- Universidad de Zamboanga CPT GuideDocument17 pagesUniversidad de Zamboanga CPT GuideShanayra Ismael JayajiNo ratings yet
- Lipaglyn Product MonographDocument64 pagesLipaglyn Product Monographanurag3069No ratings yet
- Community health nursing standards guide practiceDocument6 pagesCommunity health nursing standards guide practicegreggy_rebel17100% (2)
- Care for Patients with Fluid and Electrolyte ImbalancesDocument10 pagesCare for Patients with Fluid and Electrolyte ImbalancesAbigail LonoganNo ratings yet
- Guillain Barre SyndromeDocument8 pagesGuillain Barre SyndromeStephanie AureliaNo ratings yet
- DobutamineDocument21 pagesDobutamineahsanraja123No ratings yet
- Tryptic Soy Agar (Tryptone Soya Agar, TSA, CASO Agar, Soybean Casein Digest Agar)Document2 pagesTryptic Soy Agar (Tryptone Soya Agar, TSA, CASO Agar, Soybean Casein Digest Agar)vincent secondNo ratings yet
- Ibn SinaDocument2 pagesIbn SinaWaris Husain0% (1)
- Unani IntroductionDocument37 pagesUnani Introductionhabib_VNo ratings yet