Professional Documents
Culture Documents
CAMAF Benefit Brochure 2014
Uploaded by
0796105632Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CAMAF Benefit Brochure 2014
Uploaded by
0796105632Copyright:
Available Formats
HOSPITAL ACCOMMODATION INCLUDING CONFINEMENTS, SUBJECT TO PRE-AUTHORISATION ATTENDING DOCTORS AND SPECIALISTS CONSULTATIONS MEDICAL AND SURGICAL PROCEDURES
INCLUDING CONFINEMENTS AUXILIARY HEALTHCARE IN HOSPITAL (EG. PHYSIOTHERAPY AND PSYCHOTHERAPY) BLOOD TRANSFUSIONS (IN AND OUT OF HOSPITAL) RADIOLOGY IN HOSPITAL ADVANCED SCANS SUBJECT TO PRE-AUTHORISATION PATHOLOGY IN HOSPITAL INTERNAL PROSTHESIS SUBJECT TO PRE-AUTHORISATION HOME NURSING UP TO 21 DAYS, SUBJECT TO PREAUTHORISATION STEP DOWN APPROVED FACILITIES
100% of Negotiated Rate in general ward and specialised units. Private ward for confinements (subject to availability) Up to 300% CBT 100% of Scheme Rate
100% of Negotiated Rate in general ward and specialised units Up to 300% CBT 100% of Scheme Rate
100% of Negotiated Rate in general ward and specialised units Up to 300% CBT 100% of Scheme Rate
100% of Negotiated Rate in general ward and specialised units Up to 200% CBT 100% of Scheme Rate
100% of Negotiated Rate in general ward and specialised units Up to 100% CBT 100% CBT
100% DSP tariff as per protocols
Up to 100% CBT 100% CBT 100% CBT Physiotherapy limited to R 8 700 per family 100% of cost 100% CBT 100% CBT limited to R 26 000 per family in or out of hospital 100% CBT 100% of cost limited to R 26 000 per family 100% CBT (in lieu of hospitalisation only)
100% CBT 100% of cost 100% CBT 100% CBT 100% Negotiated Rate 100% of cost 100% CBT
100% CBT 100% of cost 100% CBT 100% CBT 100% Negotiated Rate 100% of cost 100% CBT
100% CBT 100% of cost 100% CBT 100% CBT 100% Negotiated Rate 100% of cost 100% CBT
100% CBT 100% of cost 100% CBT 100% CBT 100% Negotiated Rate 100% of cost 100% CBT
100% CBT 100% of cost 100% CBT 100% CBT limited to R 23 600 per beneficiary - in or out of hospital 100% CBT 100% of cost 100% CBT
ONLY, UP TO 90 DAYS
SUBJECT TO PRE-AUTHORISATION MEDICATION IN HOSPITAL TTO MEDICATION UP TO ONE WEEKS SUPPLY INFERTILITY TREATMENT SUBSTANCE ABUSE CHRONIC PMB CDL MEDICATION AND TREATMENT - SUBJECT TO PREAUTHORISATION AND PROTOCOLS REFER TO CHRONIC DISEASE LIST
100% Negotiated Rate 100% SEP plus dispensing fee 100% SEP plus dispensing fee Treatment limited to R 58 400 per family PMB applied to hospital based treatment and limited to one rehabilitation treatment per beneficiary per year, subject to pre-authorisation and limited to 21 days 100% SEP plus a dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
100% Negotiated Rate 100% SEP plus dispensing fee 100% SEP plus dispensing fee Treatment limited to R 40 900 per family PMB applied to hospital based treatment and limited to one rehabilitation treatment per beneficiary per year, subject to pre-authorisation and limited to 21 days 100% SEP plus a dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
100% Negotiated Rate 100% SEP plus dispensing fee 100% SEP plus dispensing fee No benefit PMB applied to hospital based treatment and limited to one rehabilitation treatment per beneficiary per year, subject to pre-authorisation and limited to 21 days 100% SEP plus a dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
100% Negotiated Rate 100% SEP plus dispensing fee 100% SEP plus dispensing fee No benefit PMB applied to hospital based treatment and limited to one rehabilitation treatment per beneficiary per year, subject to pre-authorisation and limited to 21 days 100% SEP plus a dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
100% Negotiated Rate 100% SEP plus dispensing fee 100% SEP plus dispensing fee No benefit PMB applied to hospital based treatment and limited to one rehabilitation treatment per beneficiary per year, subject to pre-authorisation and limited to 21 days 100% SEP plus a dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
100% DSP Tariff 100% SEP plus dispensing fee 100% SEP plus dispensing fee No benefit PMB applied to hospital based treatment and limited to one rehabilitation treatment per beneficiary per year, subject to pre-authorisation and limited to 21 days 100% SEP plus a dispensing fee, subject to MMAP and based on a formulary and DSP (Consultations and procedures - at cost) Medication - SEP plus dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
PMB DTP TREATMENT OUT OF HOSPITAL TREATMENT SUBJECT TO REGISTRATION OF CONDITION AND PRE-AUTHORISATION
Medication - SEP plus dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
Medication - SEP plus dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
Medication - SEP plus dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
Medication - SEP plus dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
Medication - SEP plus dispensing fee, subject to RP and DSP. (Consultations and procedures - at cost)
CAMAF LIFESTYLE PROGRAMME
PER ADULT BENEFICIARY ONE GP CONSULTATION ONLY ICD 10 CODE SPECIFIC TO GENERAL CHECK UP ONLY ONE SPECIALIST CONSULTATION *ICD 10 CODE SPECIFIC TO GENERAL CHECK UP ONLY. GYNAECOLOGISTS, UROLOGISTS, OR SPECIALIST PHYSICIANS FOR BENEFICIARIES OVER 16 YEARS. PAEDIATRICIAN FOR BENEFICIARIES UNDER 16 YEARS. PSYCHOTHERAPY SUBJECT TO REGISTRATION ON EMOTIONAL WELLNESS PROGRAMME DIETICIAN CONSULTATION ONE DENTISTRY CONSULTATION GENERAL CHECK UP ONLY ECG (PERFORMED BY GP OR SPECIALIST PHYSICIAN) *ICD 10 CODE SPECIFIC TO GENERAL CHECK UP ONLY
*Refer to website for relevant ICD 10 codes
100% of Negotiated Rate in general ward and specialised units 100% CBT per beneficiary 100% CBT per beneficiary
100% of Negotiated Rate in general ward and specialised units 100% CBT per beneficiary
100% of Negotiated Rate in general ward and specialised units Subject to Medical Savings Account
100% of Negotiated Rate in general ward and specialised units 80% CBT per beneficiary
100% DSP tariff as per protocols Refer to GP, Specialist and Dentist under Other Benefits
100% CBT per beneficiary
100% CBT per beneficiary
100% CBT per beneficiary
Subject to Medical Savings Account
80% CBT per beneficiary
Refer to GP, Specialist and Dentist under Other Benefits
100% CBT limited to R 8 100 per beneficiary One per beneficiary per annum 100% CBT 100% CBT per beneficiary
100% CBT limited to R 8 100 per beneficiary One per beneficiary per annum 100% CBT 100% CBT per beneficiary
100% CBT limited to R 8 100 per beneficiary No Benefit 100% CBT per beneficiary
100% CBT limited to R 8 100 per beneficiary Subject to Medical Savings Account Subject to Medical Savings Account
80% CBT limited to R 7 000 per beneficiary No Benefit 80% CBT per beneficiary
100% CBT for PMB DTP conditions, in or out of hospital No Benefit Refer to GP, Specialist and Dentist under Other Benefits
100% CBT per adult beneficiary
100% CBT per adult beneficiary
100% CBT per adult beneficiary
Subject to Medical Savings Account
80% CBT per adult beneficiary
Refer to GP, Specialist and Dentist under Other Benefits
ONE CONSULTATION AT AN OPTOMETRIST METABOLIC SCREENING FOR NEW BORN BABIES IMMUNISATION (COST OF IMMUNISATION ONLY) CERVICAL CANCER VACCINE (COST OF VACCINE ONLY) SCREENING SCANS SUCH AS BONE DENSITOMETRY AND MAMMOGRAMS AT PROVIDERS WHO ARE NOT RADIOLOGISTS
100% Optical Assistant Rates 100% Negotiated Rate per new born baby SEP plus a dispensing fee, limited to R 3 520 per beneficiary Females between 9 and 16 years of age (SEP plus dispensing fee) 100% of CBT limited to R 1 500 per beneficiary
100% Optical Assistant Rates 100% Negotiated Rate per new born baby SEP plus a dispensing fee, limited to: Adults R 1 750 - Child R 2 920 Females between 9 and 16 years of age (SEP plus dispensing fee) 100% of CBT limited to R 1 200 per beneficiary
100% Optical Assistant Rates 100% Negotiated Rate per new born baby SEP plus a dispensing fee, limited to R 1 170 per beneficiary Females between 9 and 16 years of age (SEP plus dispensing fee) No Benefit
Subject to Medical Savings Account Subject to Medical Savings Account SEP plus a dispensing fee, limited to R 1 170 per beneficiary. Females between 9 and 16 years of age (SEP plus dispensing fee) Subject to Medical Savings Account
Refer to spectacle and lenses benefits 80% Negotiated Rate per new born baby SEP plus a dispensing fee, subject to MMAP, limited to R 1 170 per beneficiary Females between 9 and 16 years of age (SEP plus dispensing fee) No Benefit
Refer to spectacle and lenses benefits No Benefit SEP plus a dispensing fee, subject to MMAP, limited to R 1 170 per beneficiary Females between 9 and 16 years of age (SEP plus dispensing fee) No Benefit
BASIC AND ADVANCED RADIOLOGY OUT OF HOSPITAL
MUST BE PERFORMED BY A REGISTERED RADIOLOGIST, ON REFERRAL FROM MEDICAL PRACTITIONER ONLY. ADVANCED SCANS SUBJECT TO PRE-AUTHORISATION
100% CBT
100% CBT
100% CBT
Subject to Medical Savings Account
100% CBT limited to R 3 030 per beneficiary
Basic Radiology - as per protocols (including Mammograms for females of 40+) Referrals by DSP or specialist, 100% CBT limited to R 3 030 per beneficiary
PATHOLOGY OUT OF HOSPITAL
PERFORMED BY A REGISTERED PATHOLOGIST AND REFERRED BY A MEDICAL PRACTITIONER
100% Negotiated Rate
100% Negotiated Rate
100% Negotiated Rate
Subject to Medical Savings Account
100% CBT limited to R 4 440 per beneficiary
Basic Pathology - as per protocols referred by DSP or specialist, 100% CBT, limited to R 4 810 per beneficiary
POST-HOSPITALISATION CONSULTATIONS AND TREATMENT UP TO 90 DAYS MEDICATION FOR ADDITIONAL CHRONIC CONDITIONS (SUBJECT TO PRE-AUTHORISATION) REFER TO ADDITIONAL CHRONIC CONDITIONS LIST EXTERNAL APPLIANCES IN AND OUT OF HOSPITAL PURCHASE, HIRE AND MAINTENANCE HEARING AIDS - 1 CLAIM PER 3 YEAR CYCLE FOR OVER 16 YEARS OF AGE YOUNGER THAN 16 YEARS OF AGE - 18 MONTH CYCLE WHEELCHAIRS - 3 YEAR CYCLE INSULIN PUMPS, SUBJECT TO PRE-AUTHORISATION - 4 YEAR CYCLE NETCARE 911 EMERGENCY SERVICES
300% CBT for attending practitioners 100% CBT for auxiliary services 100% SEP plus a dispensing fee, subject to RP and DSP Consultations 100% CBT 100% of cost subject to the overall limit of R 58 400 per beneficiary and subject to the following sub-limits: Hearing Aids: Wheelchairs for Quadriplegics: Standard Wheelchairs: Insulin Pumps: Other external appliances: Baby Apnoea monitors: Breast pumps: R 58 400 R R R R R R 58 400 35 000 35 000 11 700 1 800 3 000
300% CBT for attending practitioners 100% CBT for auxiliary services 100% SEP plus a dispensing fee, subject to RP and DSP Consultations 100% CBT 100% of cost subject to the overall limit of R 46 700 per beneficiary and subject to the following sub-limits: Hearing Aids: Wheelchairs for Quadriplegics: Standard Wheelchairs: Insulin Pumps: Other external appliances: Baby Apnoea monitors: Breast pumps: R 46 700 R 46 700 R 29 800 R 30 400 R 9 950 R 1 800 R 3 000
300% CBT for attending practitioners 100% CBT for auxiliary services 100% SEP plus a dispensing fee, subject to RP and DSP Consultations 100% CBT 100% of cost subject to the overall limit of R 26 900 per beneficiary and subject to the following sub-limits: Hearing Aids: Wheelchairs for Quadriplegics: Standard Wheelchairs: Insulin Pumps: Other external appliances: Baby Apnoea monitors: Breast pumps: R 23 300 R 23 300 R 16 400 R 26 900 R 5 850 R 1 800 R 3 000
Subject to Medical Savings Account
No Benefit
No Benefit
Subject to Medical Savings Account
No Benefit except for Depression
No Benefit
Subject to Medical Savings Account
100% of cost in hospital and 80% of cost out of hospital with an overall limit of R 11 800 per beneficiary and subject to the following sub-limits: Baby Apnoea monitors: Breast pumps: R 1 600 R 2 700
100% of cost limited of R 4 500 per beneficiary and subject to DSP referral and subject to the following sub-limits: Baby Apnoea monitors: Breast pumps: R 1 600 R 2 700
Unlimited Subject to Netcare 911 authorisation
Unlimited Subject to Netcare 911 authorisation
Unlimited Subject to Netcare 911 authorisation
Unlimited Subject to Netcare 911 authorisation
Unlimited Subject to Netcare 911 authorisation
Unlimited Subject to Netcare 911
DAY TO DAY BENEFITS BENEFITS BELOW ARE SUBJECT TO THE OVERALL ANNUAL LIMIT GPS, SPECIALISTS AND DENTISTS CONSULTATIONS, PROCEDURES AND RADIOLOGY PERFORMED BY THESE PRACTITIONERS; BASIC DENTISTRY ACUTE MEDICATION INCLUDING INJECTIONS AND MATERIALS NON-DSP VISITS TO DOCTORS ROOMS CASUALTY AND OUT PATIENT TREATMENT AT A HOSPITAL ALL MEDICATIONS WILL BE PAID OUT OF ACUTE MEDICATION BENEFIT HOME NURSING AUXILIARY HEALTH AUDIOLOGY, CHIROPRACTORS, DIETICIANS, HOMOEOPATHS, OCCUPATIONAL THERAPY, PHYSIOTHERAPISTS, PODIATRY AND SPEECH THERAPY
Annual Overall Limits Adult R 22 100 Child R 14 200
Annual Overall Limits Adult R 8 650 Child R 6 050
No Benefit
Limited to funds available in the beneficiarys Medical Savings Account
Annual overall limit: Beneficiary specific limits: (a) Medicines R 2 160 (b) Advanced Dentistry R 4 670 (c) Other R 2 160 80% CBT Subject to limit (c) General practitioner consultations: 10 per beneficiary through a DSP Specialist consultations: 100% CBT limited to R 6 870 per family, only on referral from your network GP Basic dentistry: 100% Scheme Tariff at network provider only 100% SEP plus a dispensing fee for basic formulary and 80% SEP plus dispensing fee for extended formulary, both subject to MMAP One non-network visit per beneficiary or two per family, 20% co-payment AND One casualty visit (facility fee, consumed meds and materials). Limited to R 1 120 No Benefit Occupational therapy and physiotherapy only 100% CBT limited to R 1 870 per beneficiary on referral from DSP only
80% CBT
80% CBT
No Benefit
Subject to Medical Savings Account
80% SEP plus a dispensing fee
80% SEP plus a dispensing fee
No Benefit
Subject to Medical Savings Account
80% SEP plus a dispensing fee, subject to MMAP. Subject to limit (a) Not applicable Medication: 80% SEP plus a dispensing fee subject to limit (a) Treatment: 80% CBT subject to limit (c) 80% CBT subject to limit (c)
Not applicable
Not applicable
Not applicable
Not applicable
80% CBT
80% CBT
No Benefit
Subject to Medical Savings Account
80% CBT up to 21 days
80% CBT up to 21 days
No Benefit
Subject to Medical Savings Account
80% CBT
80% CBT
No Benefit
Subject to Medical Savings Account
80% CBT subject to sub-limit R 1 180 Subject to limit (c)
BENEFIT SPECIFIC LIMITS
ADVANCED DENTISTRY CROWNS, BRIDGES, ORTHODONTICS, DENTURES 80% CBT limited to: Mo R 11 700 M1 R 17 500 M2+ R 21 000 Subject to Annual Benefits 80% SEP plus a dispensing fee, limited to R 2 920 per beneficiary 80% CBT limited to R 8 750 per eye 80% CBT limited to: Mo R 8 650 M1 R 12 500 M2+ R 16 900 Subject to Annual Benefits 80% SEP plus a dispensing fee, limited to R 1 290 per beneficiary 80% CBT limited to R 3 250 per eye No Benefit Subject to Medical Savings Account 50% CBT Subject to limit (b) excluding dental implants 80% SEP plus a dispensing fee, subject to MMAP, limited to R 1 240 per beneficiary. Subject to limit (a) No Benefit 100% of CBT at network provider only, limited to R 2 690 per beneficiary 80% SEP plus a dispensing fee, subject to MMAP, limited to R760 per beneficiary No Benefit
OVER THE COUNTER MEDICATION LASER K NO APPROVAL FOR SURGERY WHERE SPECTACLES OBTAINED IN PREVIOUS 12 MONTHS ANTE-NATAL FOETAL SCANS PER PREGNANCY ANTE-NATAL CLASSES SUBJECT TO ENROLMENT ON THE MOTHER-TO-BE PROGRAMME
No Benefit
Subject to Medical Savings Account
No Benefit
Subject to Medical Savings Account
6 Scans at 80% CBT 80% CBT limited to R 1 750 per pregnancy Consultation: See Preventative Wellness Add ons R 930 Single vision R 1 170 OR Bifocal R 2 340 OR Varifocal R 3 520 AND Frames R 4 650 OR Contact lenses R 5 850 Lenses, frames etc 80% Optical Assistant Rates
4 Scans at 80% CBT 80% CBT limited to R 1 290 per pregnancy Consultation: See Preventative Wellness Add ons R 760 Single vision R 760 OR Bifocal R 2 060 OR Varifocal R 3 160 AND Frames R 2 110 OR Contact lenses R 2 920 Lenses, frames etc 80% Optical Assistant Rates
No Benefit No Benefit
Subject to Medical Savings Account Subject to Medical Savings Account
3 scans at 80% CBT. Subject to limit(c) 80% CBT subject to sub-limit R 770 Subject to limit (c)
3 scans at 80% CBT No Benefit
SPECTACLES AND LENSES FROM OPTOMETRIST ONLY ANNUAL BENEFIT, UNLESS OTHERWISE STATED
Consultation: Part of Preventative Wellness
Subject to Medical Savings Account
Monthly Risk Contribution Adult Child R 3 349 R 1 894
Monthly Risk Contribution Adult Child R 2 218 R 1 321
Total Monthly Contribution Adult Child R 1 433 R 777
Monthly Risk Contribution Principal R 1 108 Adult R 881 R 535 Child NEW Monthly MSA Contribution Principal R R Adult Child R 369 294 178
Income Category R 0 - R 3 470 Adult Child R 3 471 - R 6 770 Adult Child
Income Category R 0 - R 16 890 Principal Adult 1st Child (rest are free) R 16 891 - 27 800 Principal Adult Child R 27 801 + Principal Adult Child
Monthly MSA Contribution Adult Child R R 434 207
Monthly MSA Contribution Adult Child R R 283 184
R R R R
321 179 632 376
R 1 008 R 851 R 454
Total Monthly Contribution Adult Child R 3 783 R 2 101
Total Monthly Contribution Adult Child R 2 501 R 1 505
Total Monthly Contribution Principal R 1 477 Adult R 1 175 Child R 713
R 6 771 - R 13 080 R 1 002 Adult Child R 583 R 13 081 - R 18 530 Adult R 1 498 R 860 Child R 18 531+ Adult Child R 1 866 R 1 201
R 1 339 R 1 046 R 697 R 1 783 R 1 452 R 914
Addisons Disease Asthma* Bipolar Mood Disorder* Bronchiectasis* Cardiac Failure Cardiomyopathy Chronic Obstructive Pulmonary Disorder (COPD)* Chronic Renal Disease Coronary Artery Disease Crohns Disease Diabetes Insipidus Diabetes Mellitus Type 1* Diabetes Mellitus Type 2* Dysrhythmia Epilepsy Glaucoma Haemophilia A & B HIV/AIDS* Hyperlipidaemia Hypertension Hypothyroidism Multiple Sclerosis Parkinsons Disease Rheumatoid Arthritis Schizophrenia* Systemic Lupus Erythematosus Ulcerative Colitis
ADHD (Alliance only) Agranulocytosis Allergic Rhinitis Alzheimers Disease Anaemias: Aplastic, Haemolytic, Sickle Cell Ankylosing Spondylitis Benign Prostatic Hypertrophy Chronic Granulomatous Disease Coagulation Disorders Congenital Heart Malformations Cystic Fibrosis Deep Vein Thrombosis Depression* (includes First Choice and Essential Plus) Eczema Endometriosis Gastro-Oesophageal Reflux Disease (GORD) Gauchers Disease Gout Prophylaxis Hormone Replacement Therapy Hyperparathyroidism Hyperthyroidism Menires Disease Migraine Prophylaxis Muscular Dystrophy Myasthenia Gravis Narcolepsy Organ Transplant Osteoarthritis Osteoporosis Plegia: Hemi, Para & Quad Polycystic Ovarian Syndrome Psoriasis
ADULT CBT
Refers to the member and dependants who are 22 or older at any time in the year of cover. CAMAF Base Tariff - the maximum rate paid by the Scheme to providers of healthcare services, based on 2009 RPL (Medical Aid) rates, increased annually by CPI. Tariff differs per type of service provider and % paid on different options. Chronic Disease List - the list of PMBs includes 27 common chronic conditions called CDLs. Schemes must provide cover for the diagnosis, treatment and care of these conditions. Members must register their conditions to qualify for benefits. Schemes can provide protocols in terms of the range (RP and Formularies) and delivery of medication (DSPs). Condition Medicine List - once a patients chronic condition has been registered, a patient will have access to the CML. This is a list of drugs, appropriate for the condition, that do not require authorisation. This is maintained by the Scheme and differs per Option. Reference pricing may still apply. Refers to a dependant who is younger than an adult, as defined above. Fee negotiated by the Scheme with Network pharmacies and added to SEP. The network of service providers contracted to provide healthcare services to members, eg. Diabetes programme (CDE), HIV programme (LifeSense) PPN for optical benefits on First Choice and Network Choice, Pharmacy networks for all chronic medications and Netcare hospital group for Network Choice hospital admissions. The Regulations to the Medical Schemes Act in Annexure A provide a list of conditions identified as Prescribed Minimum Benefits. The List is in the form of Diagnosis Treatment Pairs (DTPs). A DTP links a specific diagnosis to a treatment/procedure and therefore broadly indicates how each of the 270 PMB conditions should be treated. These treatment pairs cover serious and acute medical problems that include the cost of diagnosis, treatment and care of these conditions. Stands for International Classification of Diseases and Related Health Problems (10th revision). It is a coding system developed by the World Health Organisation (WHO) that translates the written description of medical and health information into standard codes, e.g. Jo3.9 is an ICD-10 code for acute tonsillitis (unspecified) and G40.9 denotes epilepsy (unspecified). These codes are used to inform medical schemes about what conditions their members were treated for so that claims can be paid from the correct benefit. A savings account that accrues monthly but the annualised amount of savings is available immediately and can be used for: top up on cost of service charged by a doctor extension when an overall benefit has been exceeded exclusion from benefits payment of day to day claims on Essential Plus option Newborn screening whereby rare disorders are detected by a blood test done 48 - 72 hours after birth. Maximum Medical Aid Price - is a reference price model and determines the maximum medical scheme price that medical schemes will reimburse for an interchangeable multi-source pharmaceutical product (generic) on the relevant option. MMAP applies to all options for chronic medication. This is the rate, negotiated by the scheme with the service provider/group of service providers, eg. hospitals and pathologists. Prescribed Minimum Benefits - as set out in the Medical Schemes Act, 1998. Medical schemes have to cover the costs related to the diagnosis, treatment and care of: Any emergency medical condition A limited set of 270 medical conditions (Defined in DTPs) 27 chronic conditions defined in the CDL These costs may not be paid from the members savings benefit and cost saving measures can be used by way of utilising DSPs, Reference Pricing and Formularies. A member must obtain prior approval for an intended admission to hospital. Failure to pre-authorise could result in wholly or partly disallowing the claim or imposing a penalty of 20% of related accounts up to a maximum of R 2 500. Emergency treatment is not subject to Pre-authorisation but members should notify the Scheme as soon as possible after the event. Means a set of guidelines in relation to diagnostic testing and management of specific conditions and includes, but is not limited to, clinical practice guidelines, standard treatment guidelines and disease management guidelines. Those funds allocated to the overall pool of funds for the payment of all claims other than those paid from the Medical Savings Account. Reference Pricing is the maximum price for which the Scheme will be liable for specific medicine or classes of medicine, listed on the Schemes Condition Medicine List (CML). The reference price varies per option and where a drug is above the reference price it is indicated that a co-payment will apply. This includes MMAP. Total cost to company prior to deductions. The maximum rate paid by the scheme to providers of healthcare services, based on SAMA (Private) rates, increased annually by CPI. Tariff differs per type of service provider and % paid on different options. Single Exit Price - nationally applied pricing for medication as determined by the Department of Health and the pharmaceutical manufacturers. To Take Out - medication supplied by the hospital for use after the date of discharge from hospital - limited to a 7 day supply.
CDL
CML/ FORMULARY CHILD DISPENSING FEES DSP
DTP
ICD 10 CODE
MEDICAL SAVINGS ACCOUNT
METABOLIC SCREENING MMAP NEGOTIATED RATE
PMB
Oncology* (PMB DTP) consult website for further details
Restrictive Lung Disease Thalassaemia Transient Ischaemic Attack / Stroke Tuberculosis
PRE-AUTHORISATION
*Subject to registration on relevant Wellness Programme
Valvular Heart Disease
*Subject to registration on relevant Wellness Programme
PROTOCOL RISK CONTRIBUTIONS
CAMAF Client Relations* E-mail Fax Reception Hospital Pre-authorisations Hospital Pre-authorisations Fax Hospital Pre-authorisations E-mail Hospital Pre-authorisations Online Website Membership Fax Post Claims to: CAMAF LIFESTYLE PROGRAMME Telephone E-mail CANCER WELLNESS PROGRAMME Telephone CARDIAC SUPPORT LINE Telephone Emergency Contact Number General Enquires Website CHRONIC CONDITION AUTHORISATION Telephone for: Doctors and Pharamacists only / SwiftAuth Members Fax E-mail EMOTIONAL WELLNESS PROGRAMME Telephone Fax E-mail Telephone 24 Hour Call Centre E-mail MOTHER-TO-BE PROGRAMME Telephone NETCARE 911 Emergency Number Telephone Fax Namibia PMB DTP AUTHORISATION Fax E-mail 011 707 8866 pmbdtp@camaf.co.za 082 911 011 254 1911 011 254 1950 09264 61 230 612 0860 100 544 0860 100 544 011 707 8747 emotionalwellness@camaf.co.za 0861 700 600 0860 506 080 camaf@lifesense.co.za 0800 200 300 0861 700 600 Option3 011 707 8622 clinicalrisk@camaf.co.za 0860 100 544 082 456 7844 011 712 6000 www.cdecentr.co.za CENTRE FOR DIABETES AND ENDOCRINOLOGY (CDE) DISEASE MANAGEMENT PROGRAMME 0860 100 544 0860 200 911 lifestyle@camaf.co.za 0860 100 545 custserv@camaf.co.za 0861 113 676 0861 700 600 0860 100 544 011 706 9946 preauth@camaf.co.za www.camaf.co.za www.camaf.co.za 011 707 8735 PO Box 2964, Randburg, 2125 SEP TTO RP SALARY SCHEME RATE
RESPIRATORY PROGRAMME Telephone Fax E-mail STRESSLINE Telephone Fax E-mail General Enquires Fax E-mail Website PPN CALL CENTRE Telephone Post Claims To Website 0860 103 529 PO Box 12450, Centrahil, 6006 www.ppn.co.za 0861 700 600 011 707 8747 emotionalwellness@camaf.co.za 0860 REALITY (732 5489) 021 700 8750 info@reality.co.za www.reality.co.za 0861 700 600 011 707 8622 clinicalrisk@camaf.co.za
REALITY (LOYALTY PROGRAMME)
FOR FIRST CHOICE AND NETWORK CHOICE MEMBERS ONLY
HYPERTENSION AND CHOLESTEROL PROGRAMME LIFESENSE (HIV DISEASE MANAGEMENT PROGRAMME)
You might also like
- NetworX Brochure 2011Document2 pagesNetworX Brochure 2011elletjiesNo ratings yet
- b4b65f86-a937-4920-a8c0-59d848e4de75 - CopyDocument14 pagesb4b65f86-a937-4920-a8c0-59d848e4de75 - CopyassmexellenceNo ratings yet
- ITPPL HMO - IntellicareDocument7 pagesITPPL HMO - IntellicarejsevillaonlineNo ratings yet
- Blue-Cross-Premier-Platinum-Extra-Dental-Vision CareerDocument8 pagesBlue-Cross-Premier-Platinum-Extra-Dental-Vision Careerapi-248930594No ratings yet
- Barbados NemCare Individuals Health InsuranceDocument3 pagesBarbados NemCare Individuals Health InsuranceKammieNo ratings yet
- Plan Comparison 2013Document6 pagesPlan Comparison 2013Amnika JagarnathNo ratings yet
- Momentum - Option Benefits 2017-2018Document28 pagesMomentum - Option Benefits 2017-2018Irzelindo JoaquimNo ratings yet
- SCRC - One PagerDocument1 pageSCRC - One Pagermpjegan90No ratings yet
- Senior Citizen Red Carpet - Snap Shot of The Features & Benefits - SHAHLIP1910V031819 - Launched On 10th JAN2019Document2 pagesSenior Citizen Red Carpet - Snap Shot of The Features & Benefits - SHAHLIP1910V031819 - Launched On 10th JAN2019Ganesh UnNo ratings yet
- Bajaj Allianz Silver HealthDocument18 pagesBajaj Allianz Silver Healthvijay.pandey373No ratings yet
- Senior Citizens Red Carpet Health Insurance Policy PDFDocument8 pagesSenior Citizens Red Carpet Health Insurance Policy PDFrohit22221No ratings yet
- TransAmerica Cancer PlanDocument10 pagesTransAmerica Cancer PlanpreparebenefitsNo ratings yet
- HMO Coverage DetailsDocument5 pagesHMO Coverage DetailsKriszel Torreliza100% (1)
- Daman Select Gold InclusionsDocument2 pagesDaman Select Gold InclusionsmukeshsinghtomarNo ratings yet
- Phil Health Subic Forum BenefitsPkgDocument34 pagesPhil Health Subic Forum BenefitsPkgChielo RosalNo ratings yet
- University of Missouri Kansas City International SBC 500499912071900371 FINAL 2Document7 pagesUniversity of Missouri Kansas City International SBC 500499912071900371 FINAL 2maheshm_erpNo ratings yet
- CLICO Group Health and Life Coverage 1Document12 pagesCLICO Group Health and Life Coverage 1buckianNo ratings yet
- Bs Wellbeing OneDocument4 pagesBs Wellbeing OneShrenik MehtaNo ratings yet
- HmoDocument35 pagesHmoDiorVelasquezNo ratings yet
- Hmo PPT Part 1 and 2Document31 pagesHmo PPT Part 1 and 2DiorVelasquez100% (1)
- Lewermark Health Insurance Copay Plan For Delta State UniversityDocument3 pagesLewermark Health Insurance Copay Plan For Delta State Universityroby sorianoNo ratings yet
- Draft Policy IP Medical Reimbursement As Per CGHS RatesDocument2 pagesDraft Policy IP Medical Reimbursement As Per CGHS RatesHghbsjsnNo ratings yet
- FHO Prospectus PDFDocument20 pagesFHO Prospectus PDFVidhyaRIyengarNo ratings yet
- Revised SCRC One Pager (1) - Converted-Converted - 231107 - 125444Document1 pageRevised SCRC One Pager (1) - Converted-Converted - 231107 - 125444Vageesh VedamoorthyNo ratings yet
- CC Student 1-Pager 2024Document2 pagesCC Student 1-Pager 2024Cleopas ChigambaNo ratings yet
- Star Senior Citizen Red Carpet Health Insurance Plan (10 Jan-19)Document1 pageStar Senior Citizen Red Carpet Health Insurance Plan (10 Jan-19)Harsh VardhanNo ratings yet
- Regional Office, Bhubaneswar: FOR Group Mediclaim Policy FOR Employees OF Psus Under Govt. of OdishaDocument14 pagesRegional Office, Bhubaneswar: FOR Group Mediclaim Policy FOR Employees OF Psus Under Govt. of Odishasohalsingh1No ratings yet
- TCS EX Policy - FY2025 - Policy ConditionsDocument4 pagesTCS EX Policy - FY2025 - Policy ConditionsAkash AgarwalNo ratings yet
- Diabetes Safe Insurance PolicyDocument11 pagesDiabetes Safe Insurance PolicyJyothika JayashriNo ratings yet
- Schedule of Benefits (Core Silver Without Dental)Document5 pagesSchedule of Benefits (Core Silver Without Dental)Nael SwedanNo ratings yet
- Alaga Ka Program by Philhealth: Philhealth Benefits and PacksgesDocument31 pagesAlaga Ka Program by Philhealth: Philhealth Benefits and Packsgesrhu minaNo ratings yet
- Budget Hospital and Super Extras Cover: Question? Need Advice? Consultants Available To HelpDocument11 pagesBudget Hospital and Super Extras Cover: Question? Need Advice? Consultants Available To HelpMaik SpaikNo ratings yet
- Prospectus New India Premier Mediclaim Wef 01 04 2021Document24 pagesProspectus New India Premier Mediclaim Wef 01 04 2021JayashreeNo ratings yet
- Us Apple Plus Ppo Feb2019 en 1Document3 pagesUs Apple Plus Ppo Feb2019 en 1Lucas Coleta AlmeidaNo ratings yet
- Blue Royale 0 65 BrochureDocument12 pagesBlue Royale 0 65 BrochureAna Patricia SanchezNo ratings yet
- Blue Cross Select BronzeDocument6 pagesBlue Cross Select Bronzeapi-285960909No ratings yet
- Benefits HighlightsDocument1 pageBenefits HighlightsRobert AvramescuNo ratings yet
- Star Family Health Optima 2020 PDFDocument1 pageStar Family Health Optima 2020 PDFRajat GuptaNo ratings yet
- Prospectus New India Premier Mediclaim Wef 01 04 2021Document24 pagesProspectus New India Premier Mediclaim Wef 01 04 2021Sayed KhajaNo ratings yet
- Anthem Classic PPO 250-20-20Document4 pagesAnthem Classic PPO 250-20-20PhilippNo ratings yet
- CignaTTK ProHealth Vs Religare CareDocument9 pagesCignaTTK ProHealth Vs Religare Caremaakabhawan26No ratings yet
- Senior Care Plan (: For Ages 61-100 Yrs Old)Document7 pagesSenior Care Plan (: For Ages 61-100 Yrs Old)Clarissa RefugioNo ratings yet
- Kaiser International HMODocument7 pagesKaiser International HMOStefNo ratings yet
- SENIOR Care Eff June 15 2019Document7 pagesSENIOR Care Eff June 15 2019Nico Angelo CopoNo ratings yet
- Gold 500/90: ( ) For Prior Authorization in Network (You Pay) Out-of-Network (You Pay)Document2 pagesGold 500/90: ( ) For Prior Authorization in Network (You Pay) Out-of-Network (You Pay)rcdasariNo ratings yet
- Management Science Associates SpdsDocument64 pagesManagement Science Associates SpdsAshwinNo ratings yet
- Standard Schedule of Benefits - Market Street LTD 2022Document2 pagesStandard Schedule of Benefits - Market Street LTD 2022mariojesus8807No ratings yet
- 20190329011144blue Royale Brochure Full - 2019-03 (March 12)Document12 pages20190329011144blue Royale Brochure Full - 2019-03 (March 12)Al Polen Jr SingcayNo ratings yet
- Benefit Summary: Your BenefitsDocument14 pagesBenefit Summary: Your BenefitsmadhusoftechNo ratings yet
- CIEE Insurance CoverageDocument2 pagesCIEE Insurance CoverageMiguelNo ratings yet
- Snic - Payless Tob 2021Document6 pagesSnic - Payless Tob 2021DIVYAS11No ratings yet
- Family Health Optima Insurance PlanDocument16 pagesFamily Health Optima Insurance Planujjal deyNo ratings yet
- CignaTTK ProHealth Vs ICICI Lombard CHIDocument9 pagesCignaTTK ProHealth Vs ICICI Lombard CHImaakabhawan26No ratings yet
- General IEC 01162015Document36 pagesGeneral IEC 01162015Suzette BalucanagNo ratings yet
- 20210326092901select Brochure Full - 01 April 2021Document12 pages20210326092901select Brochure Full - 01 April 2021iqbal_anggaraNo ratings yet
- Individual Medical Policy For Employees - Emed: Table of BenefitsDocument6 pagesIndividual Medical Policy For Employees - Emed: Table of Benefitsrahul sNo ratings yet
- TOB Ad NationalDocument8 pagesTOB Ad Nationalmuhdm7771No ratings yet
- Good Clinical Practice GuideFrom EverandGood Clinical Practice GuideRating: 5 out of 5 stars5/5 (1)
- Value Vs Growth Stock in Emerging Market-SubmittedDocument72 pagesValue Vs Growth Stock in Emerging Market-Submitted0796105632No ratings yet
- Laurence Connors - Bollinger Bands Trading Strategies That WorkDocument39 pagesLaurence Connors - Bollinger Bands Trading Strategies That Worksamgans91% (11)
- Laurence Connors - ConnorsRSIDocument43 pagesLaurence Connors - ConnorsRSIJoséRamón100% (1)
- Gretl User's Guide: Gnu Regression, Econometrics and Time-SeriesDocument235 pagesGretl User's Guide: Gnu Regression, Econometrics and Time-Series0796105632No ratings yet
- Laurence Connors - Bollinger Bands Trading Strategies That WorkDocument39 pagesLaurence Connors - Bollinger Bands Trading Strategies That Worksamgans91% (11)
- New Reading 360Document2 pagesNew Reading 36007961056320% (3)
- Satrix ETF Form 2 Additional Investments (Lump Sums Only) Aug 2013 - Listing DocumentsDocument5 pagesSatrix ETF Form 2 Additional Investments (Lump Sums Only) Aug 2013 - Listing Documents0796105632No ratings yet
- Topic - EnglishDocument16 pagesTopic - English0796105632No ratings yet
- Chapter5 SolutionsDocument12 pagesChapter5 Solutions0796105632100% (1)
- Chapter6 SolutionsDocument8 pagesChapter6 Solutions0796105632No ratings yet
- Home Buyers Guide Standard BankDocument32 pagesHome Buyers Guide Standard Bank0796105632No ratings yet
- B Com Honours - Investment Management - BrochureDocument8 pagesB Com Honours - Investment Management - Brochure0796105632No ratings yet
- Fear Greed Hope RegretDocument3 pagesFear Greed Hope Regret0796105632No ratings yet
- Your Name & Surname: Personal InfoDocument2 pagesYour Name & Surname: Personal Info0796105632No ratings yet
- House 1Document18 pagesHouse 10796105632No ratings yet
- WHO - HQ - Reports G2 PROD EXT TBCountryProfileDocument1 pageWHO - HQ - Reports G2 PROD EXT TBCountryProfileAngelo Santos EstrellaNo ratings yet
- NCP AppendicitisDocument8 pagesNCP AppendicitisAaron_Kim_Vela_4636No ratings yet
- HEALTH 8 3rdquarterDocument2 pagesHEALTH 8 3rdquarterMarc Angelo L. SebastianNo ratings yet
- 35 - Eposter - Subhenjit Ray.Document1 page35 - Eposter - Subhenjit Ray.Subhenjit RoyNo ratings yet
- Dengue OutlineDocument6 pagesDengue OutlineLouie George NeriNo ratings yet
- Vertigo and Balance TX ArticleDocument7 pagesVertigo and Balance TX Articleapi-262531856No ratings yet
- ACTIVATE-Butea SuperbaDocument22 pagesACTIVATE-Butea Superbaowenangela100% (1)
- Caring For Children Receiving Chemotherapy, Antimicrobial Therapy and Long-Term Insulin TherapyDocument34 pagesCaring For Children Receiving Chemotherapy, Antimicrobial Therapy and Long-Term Insulin TherapyRubinaNo ratings yet
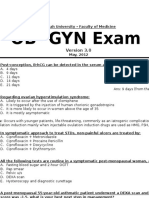
- OB-GYN - MCQ - 2012 - 5th-Year - Mu - TahDocument16 pagesOB-GYN - MCQ - 2012 - 5th-Year - Mu - TahHalah100% (1)
- Electrolyte Disturbances Causes and ManagementDocument19 pagesElectrolyte Disturbances Causes and Managementsuci triana putriNo ratings yet
- 2018 Urinary Tract Infections in ChildrenDocument12 pages2018 Urinary Tract Infections in ChildrenYudit Arenita100% (1)
- Dr. Gyan P. SinghDocument4 pagesDr. Gyan P. SinghMohammed AL-TuhamiNo ratings yet
- NCP 1activity Intolerance N C P BY BHERU LALDocument1 pageNCP 1activity Intolerance N C P BY BHERU LALBheru LalNo ratings yet
- Novel Coronavirus Vocabulary - 2020 03 PDFDocument5 pagesNovel Coronavirus Vocabulary - 2020 03 PDFLena MustafaNo ratings yet
- Navle NotesDocument32 pagesNavle NotesRyan Fortier94% (18)
- Foreign Body AspirationDocument4 pagesForeign Body AspirationpriscaNo ratings yet
- Palliative CareDocument7 pagesPalliative CareTiyara Safitri II100% (1)
- Working With Addicted PopulationsDocument9 pagesWorking With Addicted PopulationsWhimsical BrunetteNo ratings yet
- Medrobotics Receives FDA Clearance For ColorectalDocument2 pagesMedrobotics Receives FDA Clearance For ColorectalmedtechyNo ratings yet
- Medications Commonly Prescribed After A Stroke - GoodRxDocument11 pagesMedications Commonly Prescribed After A Stroke - GoodRxAnonymous EAPbx6No ratings yet
- Broqueza, Jonnel Regoris: Philippine Children's Medical CenterDocument1 pageBroqueza, Jonnel Regoris: Philippine Children's Medical CenterRica RegorisNo ratings yet
- Acute Epididymoorchitis and Torsion of Testis: Seminar 6Document37 pagesAcute Epididymoorchitis and Torsion of Testis: Seminar 6Kumutha MalarNo ratings yet
- Chapter 5neonatal Seizures and Neonatal SyndromesDocument10 pagesChapter 5neonatal Seizures and Neonatal SyndromesArista RiskaNo ratings yet
- NCPDocument2 pagesNCPNiño LuceroNo ratings yet
- Pfizer Vaccine Explainer Version 2Document9 pagesPfizer Vaccine Explainer Version 2nqosa neidscqNo ratings yet
- So My Cat Has Chronic Kidney DiseaseDocument2 pagesSo My Cat Has Chronic Kidney DiseaseNur Alisya Hasnul HadiNo ratings yet
- Are Patients Admitted To Emergency Departments With Regular Supraventricular Tachycardia (SVT) Treated AppropriatelyDocument3 pagesAre Patients Admitted To Emergency Departments With Regular Supraventricular Tachycardia (SVT) Treated AppropriatelyGading AuroraNo ratings yet
- MCQ Final 2014Document19 pagesMCQ Final 2014JohnSon100% (1)
- Knowledge, Attitude and Practice (Kap) Study OnDocument52 pagesKnowledge, Attitude and Practice (Kap) Study OnQazi Muhammad IqbalNo ratings yet
- Artículo de Trabeculectomía.Document13 pagesArtículo de Trabeculectomía.Dore OrtizNo ratings yet