Professional Documents
Culture Documents
Upper Airway Obstruction: Critical Care Pearls
Upper Airway Obstruction: Critical Care Pearls
Uploaded by
Dodo Saputera DamianOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Upper Airway Obstruction: Critical Care Pearls
Upper Airway Obstruction: Critical Care Pearls
Uploaded by
Dodo Saputera DamianCopyright:
Available Formats
Ch37 7/10/08 9:47 AM Page 388
37
Upper Airway Obstruction
Jose C. Yataco, MD
Atul C. Mehta, MD
Critical Care Pearls
Upper airway obstruction (UAO) is a life-threatening emergency that requires prompt
diagnosis and treatment.
Severe UAO can be surprisingly asymptomatic at rest if it develops gradually. Sudden
clinical deterioration is unpredictable.
Patients with possible UAO must never be sedated until the airway is secured. Minimal
sedation may precipitate acute respiratory failure.
Achievement of airway patency in total airway obstruction and reestablishment of ventilatory airflow is the first and foremost goal of the treating physicians.
Critical care physicians must be aware that pharmacologic interventions (epinephrine,
steroids, and heliox) provide temporary support but cannot significantly improve
mechanical UAO.
Bronchoscopy constitutes the most accurate diagnostic tool and frequently provides the
best way to correct UAO.
Cricothyroidotomy is the surgical intervention of choice to reestablish airflow when
medical interventions have failed.
pper airway obstruction (UAO) is one of
the most serious emergencies faced by
critical care physicians. Early diagnosis followed by restoration of airflow is essential to
prevent cardiac arrest or irreversible brain
damage that occurs within minutes of complete airway obstruction (1,2).
Although a long list of causes may be
responsible for acute UAO, management must
begin almost immediately after recognition of
the problem. If there is an actual or potential
obstruction sufficient to cause ventilatory or
oxygenation impairment, an intervention to
secure the airway is indicated by whatever
388
method appropriate at the time. No single
method is suitable in all instances; selection
depends on the assessment of the circumstances (1-3). The timing of the intervention,
medical, or surgical, is determined based on
the condition of the patient. In practice, an
elective procedure before acute decompensation is always preferable.
Etiology and Pathogenesis
For purposes of this chapter, upper airway
is considered to represent the conducting
Ch37 7/10/08 9:47 AM Page 389
Upper Airway Obstruction
passages extending from the nose or mouth
to the main carina (Figure 37-1).
UAO may be functional or anatomic and
may develop acutely or subacutely. Relapsing
polychondritis constitutes a good example of
functional UAO caused by lack of a firm cartilaginous structure to support the tracheal
wall. Squamous cell carcinoma of the larynx
represents an anatomic example of UAO.
Narrowing of the upper respiratory tract
has an exponential effect on airflow because
389
linear airflow is a function of the fourth
power of the radius (2-4). Although UAO
occurs at any level of the upper respiratory
tract, laryngeal obstruction has a particular
importance because the larynx is the narrowest portion of the upper airway. The narrowest portion of the larynx is at the glottis in
adults and the subglottis in infants (5).
Some infections such as parapharyngeal
or retropharyngeal abscesses and Ludwig
angina (mixed infection of floor of the
Palatine tonsil
Tongue
Oral pharynx
Retropharyngeal space
Root of tongue
Geniohyoid muscle
Mylohyoid muscle
Submandibular
space
Vallecula
Epiglottis
Hypophyarynx
Vocal cord
Thyroid cartilage
Larynx
Cricoid cartilage
Trachea
Sternum
Figure 37-1 Anatomy of the upper airway. (Adapted from Aboussouan L, Stoller JK. Diagnosis
and management of upper airway obstruction. Clin Chest Med. 1994;15:35-53; with permission.)
Ch37 7/10/08 9:47 AM Page 390
390
Systemic Disorders
mouth) can be associated with severe soft tissue swelling causing UAO.
The differential diagnosis of UAO is wide
and varies by age group and by clinical setting. Table 37-1 summarizes the most common causes of airway obstruction. Figures
37-2 and 37-3 show examples of benign and
malignant causes of UAO.
Clinical Signs and Symptoms
In a conscious patient, signs and symptoms of
UAO include marked respiratory distress,
altered voice, dysphagia, odynophagia, the
hand-to-the-throat choking sign, stridor, facial
swelling, prominence of neck veins, absence of
air entry into the chest, and tachycardia. In an
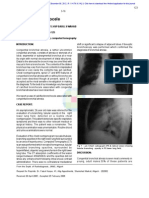
Figure 37-2 Tracheal amyloidosis causing
narrowing of the distal trachea.
Table 37-1 Differential Diagnosis of Upper
Airway Obstruction According to Etiology
Traumatic causes
Laryngeal stenosis
Airway burn
Acute laryngeal injury
Facial trauma (mandibular or maxillary fractures)
Hemorrhage
Infections
Suppurative parotitis
Retropharyngeal abscess
Tonsillar hypertrophy
Ludwigs angina
Epiglottitis
Laryngitis
Laryngotracheobronchitis (croup)
Diphtheria
Iatrogenic causes
Tracheal stenosis post-tracheostomy
Tracheal stenosis post-intubation
Mucous ball from transtracheal catheter
Foreign bodies
Vocal cord paralysis
Tumors
Laryngeal tumors (benign or malignant)
Laryngeal papillomatosis
Tracheal stenosis (caused by intrinsic or
extrinsic tumors)
Angioedema
Anaphylactic reactions
C1 inhibitor deficiency
Angiotensin-converting enzyme inhibitors
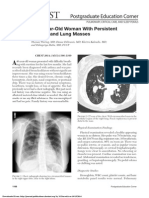
Figure 37-3 Extrinsic compression of the
trachea caused by intrathoracic malignancy.
unconscious or sedated patient, the first sign of
airway obstruction may be inability to ventilate
with a bag-valve mask after an attempt to open
the airway with a jaw-thrust maneuver. After a
few minutes of complete airway obstruction,
asphyxiation progresses to cyanosis, bradycardia, hypotension, and irreversible cardiovascular collapse (1-3).
Occasionally, UAO can develop slowly and is
confused with reactive airway disease. However,
Ch37 7/10/08 9:47 AM Page 391
Upper Airway Obstruction
the obstructive noise or stridor is thought to be
a specific for UAO. Stridor is heard during the
entire respiratory cycle but typically intensifies
during inspiration and is usually more prominent above the neck. The presence of stridor
indicates severe airway obstruction (airway passage <5 mm) but unfortunately does not help to
specify its nature or location (4).
Investigations
The most important diagnostic tool if UAO is
suspected is a quick history and physical
examination. Many times, management of a
patient with UAO must start simultaneously
with the diagnostic process. It is useful to
separate patients with potential UAO into
those with severe symptoms and impending
respiratory failure and those with a more
indolent course and less severe symptoms. It
is important to understand that airway resistance varies inversely with the fourth power of
the radius at the point of UAO, and that small
changes in the underlying pathology may
dramatically worsen respiratory airflow.
Plain Chest and Neck Radiographs
Plain neck and chest films may be useful as
screening tests by identifying tracheal deviation, extrinsic compression, or radiopaque
foreign bodies. Lateral neck radiographs
are considered insensitive and may result
in unnecessary delay in securing the airway
(1,4).
Computed Tomography
Computed tomography (CT) can be important in investigating UAO in the stable
patient or in the unstable patient with an
already secured airway. High-resolution CT
of neck and chest can help identify intrinsic
and extrinsic tumors, vascular structures,
and foreign bodies. It can also provide information on the degree and extension of airway
compromise in UAO (1,4). However, the risks
and benefits of transporting such a patient to
391
the radiology suite for scanning need to be
carefully considered.
Spirometry
Spirometry can be used in the patient with
gradual and mild symptoms of UAO. It is relatively insensitive and has no role in the management of a patient with acute respiratory
distress (3,4). Analysis of the flow-volume
loops may be helpful suggesting the location
and functional severity of the obstruction
(Figure 37-4 A-D).
Bronchoscopy
Rigid or flexible bronchoscopy with direct
visualization is the most effective tool in
establishing diagnosis and frequently provides the best way to correct UAO. The rigid
bronchoscope can be used in the emergency
setting to secure the airway by carefully passing it through the stenotic segment.
Flexible bronchoscopy can be used to establish the diagnosis as well deliver treatment
including laser therapy, photoresection, electrocautery electrosurgery, balloon bronchoplasty,
and tracheal stenting once the airway has been
secured and the patient stabilized (2,3). It is
important to have a secured airway or the
immediate means to have one because flexible
bronchoscopy can worsen UAO to a critical level.
Management
Establishing a secure and patent airway is the
most important goal in the resuscitation of a
patient with acute UAO. A quick evaluation
considering age group, history, physical
examination, and clinical circumstances helps
determine the site and cause of obstruction,
the severity of the obstruction, and the need
to establish an airway urgently.
In the outpatient setting the most common
cause of UAO is obstruction of the larynx with
a foreign body. Heimlich maneuver is recommended for relief of the airway obstruction in
adults and children one to eight years of age. A
Ch37 7/10/08 9:47 AM Page 392
392
Systemic Disorders
10
10
Expiration
Airflow, L/ S
Airflow, L/ S
Expiration
Inspiration
10
10
100
Inspiration
Lung volume, % VC
10
100
Lung volume, % VC
10
Expiration
5
Airflow, L/ S
Airflow, L/ S
Expiration
Inspiration
Inspiration
10
10
100
Lung volume, % VC
100
Lung volume, % VC
Figure 37-4 Flow-volume curves in upper airway obstruction. (A) indicates the normal contour of
the inspiratory and expiratory curves; (B) With variable intrathoracic obstruction (e.g.,
tracheomalacia within the thorax), obstruction is marked during exhalation with marked truncation
of the expiratory curve; (C) With variable extrathoracic obstruction (e.g., collapse of tracheal cartilage in the neck following trauma), obstruction is more marked during inspiration; (D) Finally, with
fixed obstructions (e.g., tracheal stenosis), both the inspiratory and expiratory curves are markedly
truncated. (Adapted from Hall JB, Schmidt GA, Wood LD, eds. Principles of Critical Care. New York:
McGraw-Hill; 1992; with permission.)
subdiaphragmatic abdominal thrust can force
air from the lungs; this may be sufficient to
create an artificial cough and expel a foreign
body from the airway. Repeat abdominal
thrusts may be needed to clear the airway.
Several medical and surgical approaches
are available in the management of UAO
including oropharyngeal airways, endotra-
cheal intubation (transnasally or orally),
tracheotomy, cricothyroidotomy, fiberoptic
intubation, racemic epinephrine, corticosteroids, heliumoxygen mixtures, laser therapy, bronchoscopic dilation, and airway
stenting (Table 37-2). The selection of the
intervention will depend on the cause of UAO
and the urgency to obtain a secure airway.
Ch37 7/10/08 9:47 AM Page 393
Upper Airway Obstruction
Table 37-2 Interventions in Upper Airway
Obstruction
Medical Interventions
Heimlich maneuver (suspected foreign body
aspiration)
Oropharyngeal airways
Endotracheal intubation (transnasally or orally)
Racemic epinephrine
Corticosteroids
Heliumoxygen mixture
Surgical or Bronchoscopic Interventions
Fiberoptic intubation
Cricothyroidotomy
Tracheostomy
Laser/electrocautery/balloon dilation
Airway stenting
Racemic Epinephrine
Racemic epinephrine is usually used in circumstances when the patient with a partial
UAO is still conscious and able to ventilate,
and vasoconstriction is desired to decrease
mucosal edema.
Racemic epinephrine administered by
means of a nebulizer has been proven to be
effective in treating croup (laryngotracheobronchitis) in the pediatric population
decreasing morbidity, mortality, and hospital
stay (6). Conversely, racemic epinephrine is
not effective in the treatment of epiglottitis
and may be deleterious (7).
Racemic epinephrine also is used to treat
postextubation laryngeal edema, which has
been reported to occur from 2.3% to 6.9% (8).
The typical case is that of a patient, breathing
easily for the first two or three hours, followed
by the gradual progression of dyspnea,
inspiratory stridor, and increased work of
breathing. In this situation repeat racemic
epinephrine treatments can be used as a temporary measure until the acute swelling and
inflammation subsides. These patients should
remain in the intensive care unit under careful observation until it is confirmed that the
UAO has resolved or greatly improved.
Corticosteroids
Corticosteroids have been used to treat UAO
because of their potential beneficial effect in
393
reducing airway edema. Randomized trials
have confirmed the usefulness of corticosteroids in the treatment of croup with
decreases in the need for intubation and
hospital stay (9). However the treatment of
epiglottitis with steroids is controversial and
often contraindicated (5).
Experimental studies in animals have
shown that corticosteroids given at the time
of extubation decrease capillary dilatation
and permeability as well as edema formation
and inflammatory cells infiltration. The preventive use of steroids for postextubation
laryngeal edema is until now widely accepted.
However, a placebo controlled, double-blind,
multicenter study showed that dexamethasone does not prevent laryngeal edema after
tracheal extubation, regardless of intubation
duration (8-10).
Heliox
Heliox, a heliumoxygen gas mixture, is
effective in reducing the work of breathing by
decreasing airway resistance to turbulent
flow in the density-dependent pressure drop
across the airway obstruction. Heliox has
been used in several conditions including
postextubation laryngeal edema, tracheal
stenosis or extrinsic compression, status
asthmaticus, and angioedema (11,12).
To be effective, the heliumoxygen ratio
must be at least 70:30. Unfortunately, most
patients with UAO also have lung disease with
varying degrees of hypoxemia preventing the
use of heliox at effective concentrations.
Although the work of breathing and dyspnea
improves to some degree with the use of
heliox, the mechanical obstruction is still in
place. The use of heliox in patients with
severe UAO should only be used to provide
temporary support pending definitive diagnosis and management.
Endotracheal Intubation
In most cases of UAO, the patency of the
upper airway can be reestablished with endotracheal intubation after rapid assessment of
the patients airway anatomy. Evaluation of
Ch37 7/10/08 9:47 AM Page 394
394
Systemic Disorders
mouth opening (>40 mm), dentition, cervical
spine mobility (flexion-extension), thyromental distance (normal is >3 finger breadths)
and the function of the temporomandibular
joints are key to subsequent success and
avoidance of complications (13,14).
Orotracheal intubation under direct visualization with a laryngoscope is the most
commonly used route for emergency intubations. In patients with distorted airway
anatomy or suspected cervical spine injury,
fiberoptic bronchoscopy can be used to guide
the intubation. The endotracheal tube is positioned over a bronchoscope; the operator
introduces the fiberoptic bronchoscope into
the patients mouth or nose and advances it
through the vocal cords into the trachea. The
endotracheal tube is then advanced over the
bronchoscope.
A prompt and successful intubation in a
patient with UAO allows restoration of adequate ventilation and oxygenation and the
performance of further diagnostic and therapeutic procedures.
roidotomy be converted to formal tracheotomy if longer than 72 hours of use is
anticipated.
Tracheostomy is probably the last option
available to establish an airway in acute UAO.
Laryngeal trauma is a relative contraindication to cricothyroidotomy and laryngotracheal intubation; it is the only indication for
emergency tracheostomy. This procedure is
time-consuming and requires expertize and
attention to detail. Comparison of emergent
versus elective tracheotomy reveals a twofold
complication rate in the former because of
the time spent on isolating the trachea as a
result of commonly occurring bleeding (13,15).
Cricothyroidotomy has a higher success
rate than tracheostomy; it also has better
patient neurologic outcome based primarily
on less time required for the procedure (11).
Overall, patients requiring an emergency
surgical airway have a relatively high mortality (15).
Surgical Interventions
Carbon dioxide or neodymium:yttrium-aluminum-garnet (Nd:YAG) laser therapy can be
used to treat intraluminal tracheobronchial
lesions once the UAO has been stabilized with
a secure airway. Although the onset of airway
compromise is usually gradual, some patients
remain asymptomatic despite airways that
are only two to three millimeter in diameter.
These patients only develop dyspnea on exercise or when complete blockage results from
mucus, bleeding, or inflammation with
swelling. Laser therapy can be used to excise
tracheal webs, to treat benign obstructive
lesions, or as palliative therapy for malignant
tracheobronchial lesions.
Overall, emergency laryngotracheal intubation is effective in approximately 97% of
cases (13). Thus, a surgical airway is needed
in only 3% of such emergencies. The need for
an immediate surgical airway must be evaluated considering the potential difficulties
associated with emergency intubation. In
cases of UAO the surgical airway is considered emergently in cases of laryngotracheal
trauma, foreign body lodged in the pharyngolaryngeal area, or severe anatomic deformity
caused by trauma.
When surgical airway management is
required, cricothyroidotomy is the procedure
of choice in the emergency setting; it is faster
(average 30 sec), simpler, and more likely to
be successful than tracheotomy. Intraluminal
diameter of the trachea is narrowest at the
level of the cricoid; there is concern that prolonged use of a cricothyroidotomy may cause
subglottic injury and lead to subglottic narrowing. It is recommended that cricothy-
Laser Therapy
Tracheal Stenting
Tracheal stents placed using either rigid or
flexible bronchoscopy can be helpful to maintain a patent airway in patients with tracheal
obstruction caused by benign or malignant
conditions. Airway resection and reconstruction provide the definitive correction, but
Ch37 7/10/08 9:47 AM Page 395
Upper Airway Obstruction
many patients have unresectable disease. For
these patients, therapeutic bronchoscopy
provides rapid palliation that can be lifesaving and improve quality of life. Benign
lesions can be managed with dilation, with or
without laser resection. Malignant lesions
often require core out of the tumor with a
rigid bronchoscope followed by laser, photodynamic therapy, brachytherapy, cryotherapy,
or electrocautery. Airway stents are a valuable
adjunct to these techniques and can provide
prolonged palliation from an unresectable
recalcitrant benign stenosis or rapidly recurrent endoluminal tumor.
Neither silicone nor the available metal
stents conform to all the ideal characteristics
desired for an endobronchial stent. The silicone stent has the advantages of being easily
repositioned or removed, causing minimal
granulation, and being inexpensive. Its disadvantages are the need for rigid bronchoscopy
and general anesthesia, reduced inner diameter, and the potential for being dislodged or
distorted (16,17). The expandable metal stent
has the advantages of being easily delivered
with flexible bronchoscopy, having minimal
migration, and conforming well to the
anatomy of the airway. The major disadvantage is that it is permanent and can cause significant granulation tissue within the stent
(17). Because of the intrinsic problems associated with airway stents, regardless of type,
it is important to remember that these
patients require lifelong management and
are at risk for development of stent obstruction or migration. In one series, 41% of
patients required additional endoscopic
interventions to maintain airway patency. In
patients with benign disease and normal life
expectancy (e.g., relapsing polychondritis) a
much higher percentage of patients require
further interventions (16,17).
Complications
Pulmonary Edema
Postobstructive pulmonary edema is the sudden onset of edema following UAO without
evidence of any other underlying cardiopul-
395
monary condition (18-20). There are two
types of postobstructive pulmonary edema.
Type I follows a sudden, severe airway
obstruction such as postextubation laryngospasm, epiglottitis, croup, strangulation,
choking, and hanging. Type I is associated
with any cause of acute UAO. Type II pulmonary edema develops after surgical relief
of long-term UAO. Reported causes include
tonsillectomy and removal of upper airway
tumors. Postobstructive pulmonary edema
usually occurs within one hour of a precipitating event but it has reported to occur up to
six hours later. The exact pathogenesis is
unclear but the current theory is that young
patients are able to generate extremely high
negative intrathoracic pressure, which
increases venous return, decreases cardiac
output, and causes fluid transudation into
the alveolar space. The cause of type II postobstructive pulmonary edema is less clear,
but it appears that the obstructing lesion
produces a modest level of positive endexpiratory pressure (PEEP) and increases
end-expiratory lung volume. The sudden
removal of this PEEP may then lead to interstitial fluid transudation and pulmonary
edema (20).
The treatment of postobstructive pulmonary edema is supportive with supplemental oxygen, intubation, and application of low
levels of PEEP (5 cm H2O). The role of diuretics in this setting is unclear. Most patients
respond promptly to appropriate treatment
and have full recovery.
Summary
Upper airway obstruction is a potentially fatal
emergency faced by critical care physicians. It
can be caused by myriad conditions that will
require a particular treatment after appropriate diagnosis. Regardless of the specific cause,
the patient with UAO must be carefully monitored in the ICU for impending respiratory
failure. A secure and patent airway should be
established if clinical deterioration is seen.
Pharmacologic interventions have limited
Ch37 7/10/08 9:47 AM Page 396
396
Systemic Disorders
Stridor suggestive of
UAO
Quick history and physical
examination
Impending respiratory failure
Urgent establishment of
patent airway
Is ET intubation
possible?
Yes
Direct or fiberoptic
intubation
No
Crycothyroidotomy vs
Tracheotomy
Gradual onset and mild
symptoms
Selection of appropriate ancillary
studies:
Bronchoscopy
CT upper airway
Spirometry
Figure 37-5 Algorithm for management of upper airway obstruction. (CT = computed tomography;
ET = endotracheal; UAO = upper airway obstruction.)
usefulness in the setting of acute mechanical
UAO. The critical care physician must be competent in the full range of airway access procedures. Overall, patients requiring an
emergency surgical airway have a poor neurological outcome and higher mortality. Figure
37-5 gives an algorithmic approach to management of UAO.
REFERENCES
1. Jacobson S. Upper airway obstruction. Emerg
Med Clin North Am. 1989;7:205-17.
2. Khosh MM, Lebovics RS. Upper airway obstruction. In: Parrillo JE, Dellinger RP, eds. Critical
Care Medecine. St. Louis: Mosby; 2001:808-25.
3. King EG, Sheehan GJ, McDonell TJ. Upper airway obstruction. In: Hall JB, Schmidt GA,
Wood LD, eds. Principles of Critical Care. New
York: McGraw-Hill; 1992:1710-8.
4. Aboussouan L, Stoller JK. Diagnosis and management of upper airway obstruction. Clin
Chest Med. 94119;5:35-53.
5. Dickison AE. The normal and abnormal pediatric airway. Recognition and management of
obstruction. Clin Chest Med. 87819;5:83-96.
6. Quan L. Diagnosis and treatment of croup. Am
Fam Physician. 92419;6:747-55.
7. Kissoon N, Mitchell I. Adverse effects of
racemic epinephrine in epiglottitis. Pediatr
Emerg Care. 85119;143-4.
8. Darmon JY, Rauss A, Dreyffus D, et al. Evaluation
of risk factors for laryngeal edema after tracheal
extubation in adults and its prevention by dexamethasone. Anesthesiology. 1992;77:245-51.
9. Kairys SW, Olmstead EM, OConnor GT.
Steroid treatment of laryngotracheitis: a metaanalysis of the evidence from randomized trials. Pediatrics. 1989;83:683-93.
10. McCulloch TM, Bishop MJ. Complications of
translaryngeal intubation. Clin Chest Med.
1991;12:507-21.
11. Boorstein JM, Boorstein SM, Humphries GN,
et al. Using heliumoxygen mixtures in the
emergency management of acute upper airway
obstruction. Ann Emerg Med. 1989;18:688-90.
12. Curtis JL, Mahlmeister M, Fink JB, et al.
Heliumoxygen gas therapy. Chest. 1986;90:
455-7.
Ch37 7/10/08 9:47 AM Page 397
Upper Airway Obstruction
13. Feller-Kopman D. Acute complications of artificial airways. Clin Chest Med. 2003;24:445-55.
14. Steinert R, Lullwitz E. Failed intubation with
case reports. HNO. 1987;35:439-42.
15. Goldberg J, Levy PS, Morkovin V, Goldberg JB.
Mortality from traumatic injuries: a casecontrol study using data from the national
hospital discharge survey. Med Care. 1983;21:
692-704.
16. Wood DE, Liu YH, Vallieres E, et al. Airway
stenting for malignant and benign tracheobronchial stenosis. Ann Thorac Surg. 2003;76:
167-74.
397
17. Saad CP, Murthy S, Krizmanich G, Mehta AC.
Self-expandable metallic airway stents and
flexible bronchoscopy: long term outcome
analysis. Chest. 2003;124:1993-9.
18. Kanter RK, Waichko I. Pulmonary edema
associated with upper airway obstruction. Am
J Dis Child. 1984;138:356.
19. Wilms D, Shure D. Pulmonary edema due to
upper airway obstruction in adults. Chest.
88919;4:1090-2.
20. Van Kooy MA, Gargiulo RF. Postobstructive
pulmonary edema. Am Fam Physician.2000;
62:401-4.
You might also like
- Pneumothorax, Tension and TraumaticDocument29 pagesPneumothorax, Tension and TraumaticicaNo ratings yet
- Primary Survey KGD LBM 1Document9 pagesPrimary Survey KGD LBM 1Nur Azizah PermatasariNo ratings yet
- Airway ObstructionDocument7 pagesAirway ObstructionnesredeNo ratings yet
- Predictores de Intubacion DificilDocument12 pagesPredictores de Intubacion DificilNoema AmorochoNo ratings yet
- Pneumothorax: An Update: ReviewDocument5 pagesPneumothorax: An Update: ReviewAby SuryaNo ratings yet
- Diaphragmatic Eventration: Shawn S. Groth,, Rafael S. AndradeDocument9 pagesDiaphragmatic Eventration: Shawn S. Groth,, Rafael S. AndradeFranciscoJ.ReynaSepúlvedaNo ratings yet
- Blunt Thoracic TraumaDocument3 pagesBlunt Thoracic TraumaNetta LionoraNo ratings yet
- Pneumothorax, Tension and TraumaticDocument24 pagesPneumothorax, Tension and TraumaticSatria WibawaNo ratings yet
- TRAUMA Pulmones, Traquea y EsofagoDocument14 pagesTRAUMA Pulmones, Traquea y EsofagosantigarayNo ratings yet
- Tracheal StenosisDocument4 pagesTracheal StenosisJessica MarianoNo ratings yet
- 6 Lethal DeathsDocument4 pages6 Lethal Deathslina_m354No ratings yet
- Journal of Thoracic ImagingDocument11 pagesJournal of Thoracic Imagingestues2No ratings yet
- Congenital Lobar EmphysemaDocument3 pagesCongenital Lobar Emphysemamadimadi11No ratings yet
- Jurnal 2Document0 pagesJurnal 2Seftiana SaftariNo ratings yet
- Airway and Ventilatory ManagementDocument8 pagesAirway and Ventilatory ManagementAshen DissanayakaNo ratings yet
- 145 One Lung VentilationDocument6 pages145 One Lung VentilationEyad AbdeljawadNo ratings yet
- Pulmonary Trauma Emergency Department Evaluation and ManagementDocument23 pagesPulmonary Trauma Emergency Department Evaluation and ManagementPq PrissNo ratings yet
- Pediatrics StridorDocument13 pagesPediatrics StridorEmaNo ratings yet
- Airway and Anesthetic Management of The Traumatized PatientDocument126 pagesAirway and Anesthetic Management of The Traumatized PatientdanocprexoidNo ratings yet
- Laryngeal: Obstruction Relieved by PantingDocument3 pagesLaryngeal: Obstruction Relieved by PantingIndah D. RahmahNo ratings yet
- Smith 2001Document19 pagesSmith 2001PaulHerreraNo ratings yet
- Tracheostomy in IcuDocument45 pagesTracheostomy in IcuCarmen IulianaNo ratings yet
- Home - Clinical - Management - News - Products - Protocols/Guidelines - Research - Buyer's Guide - Expert Insight - ArchivesDocument8 pagesHome - Clinical - Management - News - Products - Protocols/Guidelines - Research - Buyer's Guide - Expert Insight - ArchivesDuvvuri SankarNo ratings yet
- MDCT Evaluation of Foreign Bodies and Liquid Aspiration Pneumonia in AdultsDocument9 pagesMDCT Evaluation of Foreign Bodies and Liquid Aspiration Pneumonia in AdultsHafidz ZuhairNo ratings yet
- Tracheostomy in Icu: Who Should Do It ? The Surgeon or The Anesthesiologist ?Document45 pagesTracheostomy in Icu: Who Should Do It ? The Surgeon or The Anesthesiologist ?Cristina PironNo ratings yet
- Transl MedicineDocument3 pagesTransl MedicineAlina KachurNo ratings yet
- HematopneumothoraxDocument13 pagesHematopneumothoraxtri_budi_20No ratings yet
- Ultrasound A CL 2021Document17 pagesUltrasound A CL 2021Alejandra SanchezNo ratings yet
- Effects of Laryngeal Cancer On VoiceDocument10 pagesEffects of Laryngeal Cancer On VoiceSanNo ratings yet
- Thoracic TraumaDocument24 pagesThoracic TraumaOmar MohammedNo ratings yet
- Asthma and Lung MassDocument4 pagesAsthma and Lung MassAzmachamberAzmacareNo ratings yet
- Pulmonary Atelectasis: A Pathogenic Perioperative EntityDocument18 pagesPulmonary Atelectasis: A Pathogenic Perioperative Entityハルァン ファ烏山No ratings yet
- Surgicaloptionsforthe Treatmentofobstructive Sleepapnea: Jon-Erik C. Holty,, Christian GuilleminaultDocument37 pagesSurgicaloptionsforthe Treatmentofobstructive Sleepapnea: Jon-Erik C. Holty,, Christian GuilleminaultJuan Pablo Mejia BarbosaNo ratings yet
- Rapid Diagnosis and Treatment of A Pleural Effusion in A 24-Year-Old ManDocument4 pagesRapid Diagnosis and Treatment of A Pleural Effusion in A 24-Year-Old ManJonathan EdbertNo ratings yet
- Atelectasis: Go ToDocument10 pagesAtelectasis: Go Tosuci triana putriNo ratings yet
- Pulmonary Function TestDocument7 pagesPulmonary Function TestGhada HusseinNo ratings yet
- Occurs Most Often In:: Muscular DystrophyDocument4 pagesOccurs Most Often In:: Muscular DystrophyJiezl Abellano AfinidadNo ratings yet
- Truma Slide 4 Chest TrumaDocument38 pagesTruma Slide 4 Chest TrumaadnanreshunNo ratings yet
- Pulmonary Aspergillosis Imaging: Practice EssentialsDocument9 pagesPulmonary Aspergillosis Imaging: Practice EssentialsPutri PrameswariNo ratings yet
- ICU Imaging: Joshua R. Hill, MD, Peder E. Horner, MD, Steven L. Primack, MDDocument18 pagesICU Imaging: Joshua R. Hill, MD, Peder E. Horner, MD, Steven L. Primack, MDJackee_BlackNo ratings yet
- Apneea de SomnDocument37 pagesApneea de SomnAlbert GheorgheNo ratings yet
- Surgical Therapy For Necrotizing Pneumonia and Lung Gangrene PDFDocument6 pagesSurgical Therapy For Necrotizing Pneumonia and Lung Gangrene PDFmichael24kNo ratings yet
- Accuracy of The Physical Examination in Evaluating Pleural EffusionDocument7 pagesAccuracy of The Physical Examination in Evaluating Pleural EffusionTeresa MontesNo ratings yet
- 4.pneumothorax Imaging - Practice Essentials, Radiography, Computed TomographyDocument11 pages4.pneumothorax Imaging - Practice Essentials, Radiography, Computed TomographyAchmadRizaNo ratings yet
- 241 TracheostomyDocument12 pages241 Tracheostomyalbert hutagalungNo ratings yet
- PnemotoraksDocument4 pagesPnemotoraksGung Citra PratikaNo ratings yet
- TX CuelloDocument16 pagesTX CuelloStephany RodriguezNo ratings yet
- Airway ComplicationsDocument19 pagesAirway ComplicationsAinil MardiahNo ratings yet
- Congenital Malformations, TrakeaDocument3 pagesCongenital Malformations, TrakeaAntonia DinaNo ratings yet
- Traumatic Diaphragmatic Hernia: Key Words: Trauma, Diaphragm, HerniaDocument3 pagesTraumatic Diaphragmatic Hernia: Key Words: Trauma, Diaphragm, HerniaRangga Duo RamadanNo ratings yet
- A Case of Anterior Tracheal Rupture Following Trivial TraumaDocument5 pagesA Case of Anterior Tracheal Rupture Following Trivial TraumaBhavesh PatadiyaNo ratings yet
- Ent Throat 1Document58 pagesEnt Throat 1ميمونه عبدالرحيم مصطفىNo ratings yet
- Chest TraumaDocument28 pagesChest TraumaGitaAmeliaTurnipNo ratings yet
- 53 47 PBDocument7 pages53 47 PBpinaNo ratings yet
- Pulmonary Imaging: Xie Xin Li Department of Nuclear Medicine, First Affiliated Hospital, Zhengzhou UniversityDocument38 pagesPulmonary Imaging: Xie Xin Li Department of Nuclear Medicine, First Affiliated Hospital, Zhengzhou Universityapi-19916399No ratings yet
- A Case of Acquired Tracheal Diverticulum Presenting With Globus PharyngeusDocument3 pagesA Case of Acquired Tracheal Diverticulum Presenting With Globus PharyngeusFranspolNo ratings yet
- Essentials in Lung TransplantationFrom EverandEssentials in Lung TransplantationAllan R. GlanvilleNo ratings yet