Professional Documents
Culture Documents
Autonomic Nervous System Pharmacology Therapeutics Semester IV 2002 Lectures 1and 2
Autonomic Nervous System Pharmacology Therapeutics Semester IV 2002 Lectures 1and 2
Uploaded by
Uma MounaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Autonomic Nervous System Pharmacology Therapeutics Semester IV 2002 Lectures 1and 2
Autonomic Nervous System Pharmacology Therapeutics Semester IV 2002 Lectures 1and 2
Uploaded by
Uma MounaCopyright:
Available Formats
1
Autonomic Nervous System Pharmacology
Therapeutics Semester IV 2002
Lectures 1and 2
John Kefer PH.D.
Introduction
To discuss the pharmacology of the sympathetic and parasympathetic nervous system can be
overwhelming. The number of drugs that influence these systems is immense, and you will be hard
pressed to find drugs that do not either directly or indirectly interact with the SNS/PNS. Therefore, to
discuss this subject in a more focused manner, today we will discuss this subject from a cell surface
receptor-oriented perspective. We will discuss agonists and antagonists of the following receptors:
receptors, receptors and dopamine receptors (sympathetic receptors), and muscarinic (M) receptors
and nicotinic receptors. Again, this subject could become overwhelming, as each organ in the body
expresses these receptors. Sometimes, the same receptor can have different responses for different
organs.
How can this disparity be resolved? Is there a conceptual model to help form a unified picture of what
each of these drugs is doing throughout the body? There is.
Unifying Model: Bear vs. Couch
1. Sympathetic: How will this organ behave when chased by a bear?
2. Parasympathetic: How will behave while sitting on the couch?
Goal of Lecture:
To allow you to build a framework of understanding to properly predict the effects and side effects of
different drugs simply by knowing what receptor they interact with. I feel this is much more effective
than trying to retain lists of seemingly unrelated side effects for all of these drugs.
Receptors and Function of the Eye Fig. 1
1. Ciliary epithelium produces aqueous humor through 1 receptors. This fluid
keeps the anterior chamber of the eye at the proper pressure to
focus light onto the lens and to the retina.
2. Sympathetic activity stimulates the alpha receptors on the iris to
contract longitudinally to pull the iris towards itself,
concentrically opening the sphincter.
3. The ciliary muscle and sphincter are stimulated by parasympathetic neurons
releasing acetylcholine (Ach), binding muscarinic (M) receptors. These muscles
work by:
a) ciliary muscle pulls on the trabecular meshwork to open the canal of schlemm
and drain the fluid.
b) ciliary muscle contracts the entire machinery to accommodate lens by relaxing
its pull on the lens.
c) The sphincter contracts to constrict the pupil.
So under high stress, sympathetics release NE. NE (, ) increases aqueous humor production,
and dilates the pupil.
Once the stress is gone, the parasympathetics constrict the pupil and drain the anterior chamber.
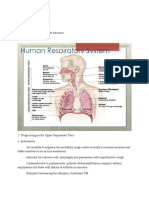
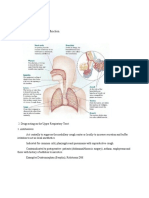
Lungs: Fig. 2
1. Sympathetic activity- 2 receptor stimulation bronchodilates the airways
and
decreases airway secretions.
2. Parasympathetic activity- Ach stimulates M receptors,
bronchoconstrict the airways
and also to increase airway secretions.
In the lungs there are many other receptors and mediators affecting lung
function, but these are not directly involved in the SNS/PNS system.
Heart
1. Sympathetic activity- 1 receptor stimulation increases heart
rate, contractility, AV
nodal conduction and cardiac output.
2. Parasympathetic activity- muscarinic (M) receptor stimulation
decreases SA nodal
firing, decrease AV node conduction
and decrease CO.
Blood Vessels
The blood vessels express , , dopamine (DA), histamine and M receptors.
This system is more complex.
1. Sympathetic- NE (, 1), and epinephrine(1, 2, 1, 2) and dopamine
(DA) are released,
- 1 vasoconstricts vessels, mainly at the arterioles, to increase
pressure/ cut off blood flow to unnecessary organs and shunt it to
organs that need it.
- 2 vasodilates skeletal vessel beds to increase blood flow to
needed muscles. Also lowers vascular resistance overall, and
therefore blood pressure.
- DA- three different mechanisms, concentrationdependent.
a.) Low dose DA- dilates renal artery, increasing kidney
perfusion.
b.) Mid-dose DA- stimulates 2 receptors as well,
resulting in dilation of
skeletal bed BVs to decrease systemic
resistance.
c.) High Dose DA- stimulate 1 receptors and blood
vessels constrict,
resulting in an overall increased
blood pressure.
(At all three doses, low medium or high, the renal artery is
dilated to increase perfusion of the kidney.)
low dose DA = D1, , Medium dose DA = 2, High dose DA =
1
The interplay of these drugs with blood vessels and heart rate will
be discussed below.
GIVery complex, poorly understood.
-
Parasympathetic activity (M) stimulates GI motility, allows
sphincters to open, and increase secretions.
sympathetic activity (, ) slows GI motility, increases
sphincter tone, and decreases GI secretions.
DA receptor activation causes increased GI motility,
stimulates secretion, and decreases sphincter tone.
opioids- also must be considered in the GI function, as opioids
will promptly decrease GI motility, decrease secretions and
increase sphincter tone, inducing constipation.
Bladder-
1. Sympathetic: The receptors prevent bladder contraction by
relaxing the bladder,
and contracting the internal sphincter.
2. Parasympathetic: Muscarinic receptors in the bladder
stimulate bladder contraction
and relax the internal sphincter. (Micturition
Reflex)
Introduction
In the last section, we discussed the receptor-oriented behavior of each
organ system. We will now discuss the drugs of the
sympathetic/parasympathetic nervous system affecting each of these organ
systems, and the resulting side effects of each of these drugs.
Drugs of the Eye
The main disease of the eye (as far as Boards go) and discussed in
pharmacology is glaucoma.
It is a common disease and can result in blindness.
1. Pathophysiology of glaucoma- Increased pressure in the intraocular
space due to increased production and decreased drainage of
aqueous humor.
2. Closed angle vs. open angle glaucoma
Glaucoma is treated with cholinomimetics, -blockers, and epinephrine
Cholinomimetics- The use of these agents is based on their chemistry.
Tertiary amines such as
pilocarpine and physostigmine are uncharged
molecules and therefore pass
easily through membranes. These two drugs have the
same effect on the eye
but through two distinct mechanisms.
a) Pilocarpine: - direct muscarinic agonist
- passes easily through the cornea
- Stimulates M receptors on the ciliary
muscle and the
sphincter muscle of the iris. This helps
open the canal of
Schlemm, and helps fluid reach it.
b) Physostigmine: - cholinesterase inhibitor
- passes easily through the cornea as well
as the blood
brain barrier.
- Increases local Ach by blocking
acetylcholinesterase,
increasing ciliary muscle and sphincter
muscle
contraction.
Pilocarpine vs. Physostigmine: Pilocarpine, based on
its own individual
charge, does not cross the blood-brain-barrier quite as
easily as
physostigmine, so less central nervous system effects with
pilocarpine.
Therefore, pilocarpine is the drug of choice for glaucoma,
and if
a patient does not respond well, physostigmine can also be
tried.
Blockers- Timolol is the blocker of choice for glaucoma.
-blocks 1 and 2 receptors.
-Lack of the anesthetic effect of other blockers,
-Blocks the receptors of the ciliary epithelium, decreasing
synthesis of aqueous
humor w/o anaesthetizing the cornea and causing asensory
trauma.
-Timolol happens to cross the cornea more effectively than
the other
blockers.
Acetazolamide- -diuretic
- blocks carbonic anhydrase activity, no HCO3 can be made.
- Production of aqueous humor requires the presence of HCO3.
- Blocking HCO3 prevents production of aqueous humor.
Antimuscarinics- These are not used for glaucoma, as these agents would
worsen glaucoma.
These agents are used to dilate the eye for eye exams. The
prototype is
atropine, which blocks muscarinic receptors. Others include
homatropine, cyclopentolate and tropicamide. These drugs vary
only in their duration of effect. Atropine lasts > 72 h,
homatropine 24 h, cyclopentolate 10 h, and tropicamide .5- 4 h.
The muscarinic receptor blockade relaxes the ciliary muscle,
causing the lens to relax and "thicken", and also relaxes the iris
sphincter, resulting in cycloplegia, and mydriasis.
Lungs
The two main actions of the drugs affecting the lungs occur by:
1) affecting airway diameter,
2) affecting airway secretions.
The two receptors involved in this control are 2 and M receptors.
1a. Airway diameter- Bronchodilation--Sympathetic activity (EPI,
DA)
- Stimulate 2, with: -epinephrine (1, 2, 1, 2),
- medium dose DA,
- exogenous 2 agonists (albuterol and
other similar drugs),
- Causes bronchial smooth muscle dilation and decreased
secretions in the lungs.
- Withdrawal of these agents or decreased sympathetic activity
causes
bronchiolar relaxation, and increases bronchiolar secretions.
- The antimuscarinic agent ipratropium, a muscarinic
receptor antagonist, is
very effective in blocking muscarinic bronchoconstriction and
increased
secretion.
- It is a quaternary amine, therefore it crosses membranes
poorly and is therefore
excellent for inhalation and targeting to the lungs with
minimal systemic side
effects.
- Epinephrine and Dopamine can be used for emergencies
where increased
ventilation is required, but due to their systemic side effects,
are not used for
long term therapy.
- Norepinephrine has little effect on the lungs because it is
specific for 1.
b. Bronchoconstriction- Muscarinic receptor activity results in
decreased airway
diameter with increased secretions.
Muscarinic drugs are not
used for this action, as there is little
indication for decreasing
the diameter of the airways.
HeartThe activity of the heart is controlled through 1 and M receptors.
- 1 stimulation of the heart increases heart rate, contractility and cardiac
output.
Epinephrine, Norepinephrine, dopamine and isoproterenol all
increase heart activity.
- Muscarinic agonists or cholinesterase antagonists increase Ach,
slowing the heart rate,
decreasing contractility and decreasing AV nodal conduction
velocity through the AV
node.
- There are few agents used in cardiology to stimulate M receptors.
blockers are
employed to slow heart rate instead.
- blockers are covered in the cardiac chapter, and are beyond the
scope of this lecture;
(however, know that atenolol, metoprolol, are both 1 specific,
and therefore the
best blocker for use in asthmatics (good board question). Also,
labetolol and
carvedilol has both and 1 activity, carvedilol is used for CHF
treatment because
decreases afterload (boards). Non-selective blockers can
exacerbate an asthma
attack. )
Baroreceptor Reflex:
Before moving on to the drugs affecting the blood vessels, we must first
engage in a review of the baroreceptor reflex.
Fig 3
Anything that changes arterial pressure, such as an alpha agonist or
high dose
dopamine, causes an automatic decrease in HR by stimulating the
brainstem .nucleus
tractus solitarius to decrease basal sympathetic stimulation of the
heart. The change in
sympathetic activity changes NE release at the SA node, and heart
rate and contractility
are altered accordingly.
- When arterial pressure decreases, the blood vessels signal the NTS to
increase
sympathetic tone, and heart rate goes up to compensate and
maintain organ perfusion.
- When arterialpressure increases, the sympathetic activity is inhibited,
and heart rate and
contractility decrease.
Blood Vessels/ Baroreceptor Reflex
Epinephrine- (1, 2, 1, 2)We have discussed the baroreceptor reflex. How
do drugs with
multiple receptor actions affect the blood pressure and heart
rate? Which receptor
action wins?
1- constricts arterioles and large arteries
2- blocks central nervous system release of norepinephrine
1- increase heart rate
2 dilates skeletal vessel beds
Overall, you see increased HR, increased BP.
Norepinephrine- (1, 1)
1- constricts arterioles and large arteries
1- increase heart rate, contractility
Although 1 increases arterial pressure, baroreceptor reflex
results in a subsequent
decreased HR and 1 vs vagus = vagus wins. Overall see
increased pressure,
decreased heart rate.
Isoproterenol- (1, 2)
- stimulates heart through 1 directly.
- 2 stimulates vasodilation, leading to decrease in BP,
stimulating the
baroreceptor reflex and further stimulating heart rate.
Fig. 4. Know these figures for boards!
Dopamine- (1, 1, 2, D1) All effects are dose-dependent-if give a low dose, only see D1 activity in renal
artery.
10
- medium dose results in skeletal vessel dilation
and increased heart
rate through 1 and the baroreceptor reflex.
- High dose results in increased arterial pressure
via 1.
-1 agonists- Phenylephrine, methoxyamine are specific 1 agonists,
which increase arterial
pressure, stimulating the baroreceptor reflex and decreasing
heart rate.
Non-selective antagonists- To fully understand how these drugs operate
we must remember that 2 receptors mainly affect the central nervous
system. This receptor is on the presynaptic sympathetic vessels in the CNS
and are normally stimulated by NE which has 1 and 2 activities. The 2
receptor inhibits release of norepinephrine from the CNS.
Phenoxybenzamine and Phentolamine are non-selective -blockers,
used to control hypertension and tachycardia associated with
pheochromocytoma.
Prazosin- is an 1 specific antagonist which can be used as a second line
agent for control of
hypertension, and to treat urinary retention (see below).
Because phenoxybenzamine and phentolamine block 1 and 2 receptors,
tachycardia is exacerbated with these drugs and can be problematic.
However, these drugs are used to temporarily control the more dangerous
malignant hypertension associated with pheochromocytoma until surgery
can be performed. These drugs are preferred over prazosin because they
block 1 more effectively. However, the exacerbation of tachycardia makes
the use of these drugs temporary.
Phenoxybenzamine binds 1 irreversibly.
Phentolamine binds 1 reversibly.
Effectiveness and Orthostatic Hypotension?
Muscarinic Agonists- Stimulation of muscarinic receptors on blood vessels
results in vasodilation through the production of nitric oxide. Thus, one side
effect of muscarinic agonists or cholinesterase inhibitors is vasodilation,
potentially leading to orthostatic hypotension.
GI Pharmacology
The GI system expresses /, DA receptors, M receptors, opioid receptors, and 5HT receptors.
11
Sympathomimetic drugs- Drugs acting on //DA receptors down regulate GI activity.
These drugs decrease motility, decrease secretory activity,
increase motility, and increase sphincter tone.
(Antidopaminergic drugs such as the cisapride and metoclopramide are used extensively
in hospital setting as antinauseate and promotility agents.)
Muscarinics- increase blood flow to the gut, increase motility, increase secretions of the
GI tract.
- Bethanechol has been used to stimulate the GI tract and increase
secretions for digestion in diabetic nephropathies, or after surgeries that
decrease vagal function, two conditions that lead to GI paralysis.
Anti-muscarinics- Propantheline, a competitive muscarinic receptor antagonist is used to
relax the smooth muscle of the GI tract, increases sphincter tone and
decreases secretions.
- This drug is used to decrease nervous stomach/irritable bowel
syndrome.
Opioid Agonists- constipation is a common side effect of opioids. Opioid receptors exist
in high density in the GI tract, and directly mediate decreased motility, decreased secretion, and
increased sphincter tone through the enteric nervous system and the central nervous system.
These actions delay passage of the fecal mass and increased absorption of water.
Ondansetron- ondansetron is a 5HT antagonist. Serotonin plays a role in the nausea and
vomiting reflex. Ondansetron blocks GI serotonin receptors, and therefore prevents nausea and
vomiting. Ondansetron is used for serious nausea and vomiting, such as post-op N/V that is
resistant to the more common DA blockers such as cisapride and metoclopramide. Ondansetron
is also used for the intractable nausea and vomiting associated with chemotherapy.
Bladder
There are 2 main receptors for the bladder, and M receptors.
The muscarinic agonist bethanechol is used to stimulate bladder function in nonobstructive disease, such as diabetic neuropathy.
The muscarinic antagonist propantheline is used to stimulate urinary retention in
incontinence.
The - antagonist prazosin and terazosin (longer half-life) can increase
micturition by relaxing the smooth muscle of the internal sphincter, as well as the
smooth muscle of an enlarged and therefore obstructive prostate.
12
Note: The lack of lists of side effects in this lecture is for a purpose. Every side effect of all
of these drugs has been discussed. By knowing how each class of drug interacts with its
receptors in each organ system, you can then correctly predict the side effects of each drug.
This level of understanding is of greater depth than the book chapters provided to you.
With an understanding of how these drugs will affect other organ systems (rather than
memorizing a list of side effects) you will be well served on boards and on the floors next
year.
Questions:
What is the effect of pilocarpine and other direct muscarinic agonists on the
eye? Lungs? Heart? Blood vessels? Glands? Bladder? GI tract?
Answer:
(miosis and accommodation/bronchoconstriction and increased bronchial
secretions/bradycardia and decreased contractility/ vasodilation and
decreased blood pressure/ increased secretions/ increased urination/
increased GI motility)
What is the effect of physostigmine and other cholinesterase inhibitors on
the eye? Lungs? Heart? Blood vessels? Glands? Bladder? GI tract? Skeletal
muscles?
What is the effect of timolol and other blockers on the eye? Lungs? Heart?
Blood vessels? Glands? Bladder? GI tract?
What is the effect of atropine and other antimuscarinics on the eye? Lungs?
Heart? Blood vessels? Glands? Bladder? GI tract? (remember the
mnemonic: Red as a beet (no sweating, so hyperthermia can occur), dry as a
bone, mad as a hatter (due to abnormal nerve conduction in the CNS), blind
as a stone (mydriasis and poor near-sightedness).
What is the effect of albuterol and other 2 agonists on the eye? Lungs?
Heart? Blood vessels? Glands? Bladder? GI tract? (Usually, only blood
pressure and heart effects are discussed-- remember, agonists are
selective, but not perfectly selective and you can get some interaction
between receptor subtypes).
What is the effect of EPI, NE and DA on the eye? Lungs? Heart? Blood
vessels? Glands? Bladder? GI tract? Kidney?
What is the effect of methoxamine, phenylephrine and other agonists on
the eye? Lungs? Heart? Blood vessels? Glands? Bladder? GI tract?
Baroreceptor reflex?
13
What is the effect of non-specific agonists on the eye? Lungs? Heart?
Blood vessels? Glands? Bladder? GI tract? Baroreceptor reflex? What role
does orthostatic hypotension play with these drugs? Name the other drugs
discussed in this lecture which may cause orthostatic hypotension?
What is the effect of agonists on the eye? Lungs? Heart? Blood vessels?
Glands? Bladder? GI tract? Baroreceptor reflex? Orthostatic hypotension?
What is the effect of cisapride and metoclopramide on the blood vessels? GI
tract?
What is the effect of bethanechol and other muscarinic agonists on the eye?
Lungs? Heart? Blood vessels? Glands? Bladder? GI tract?
What is the effect of propantheline and other muscarinic antagonists on the
eye? Lungs? Heart? Blood vessels? Glands? Bladder? GI tract?
You might also like
- Chapter 12 Drugs and The Autonomic Nervous System PDFDocument10 pagesChapter 12 Drugs and The Autonomic Nervous System PDFMaha KhanNo ratings yet
- Medical Pharmacology Ovidius 2014 1st TestDocument19 pagesMedical Pharmacology Ovidius 2014 1st TestWissam DadiNo ratings yet
- Nursing PharmacologyDocument22 pagesNursing PharmacologyDharren Rojan Garvida Agullana100% (2)
- Equine Radiographic AnatomyDocument32 pagesEquine Radiographic AnatomySam Bot100% (2)
- Appeal Letter FfsDocument1 pageAppeal Letter FfsAndrea LaBarberaNo ratings yet
- Q & A - Solo Parent's Welfare Act and Parental LeaveDocument6 pagesQ & A - Solo Parent's Welfare Act and Parental Leaveelvie_arugay100% (1)
- 05 Chapter1Document15 pages05 Chapter1inderpreetNo ratings yet
- A Case Study: Glaceau: Marketing Vitamin WaterDocument34 pagesA Case Study: Glaceau: Marketing Vitamin WaterNikhil VarshneyNo ratings yet
- Autonomic Nervous System Pharmacology Therapeutics Semester IV 2002 Lectures 1and 2Document11 pagesAutonomic Nervous System Pharmacology Therapeutics Semester IV 2002 Lectures 1and 2Rezy KurniaNo ratings yet
- Autonomic Nervous System PharmacologyDocument7 pagesAutonomic Nervous System Pharmacologydonordarah93No ratings yet
- Adrenergic Agonists 1Document90 pagesAdrenergic Agonists 1OMAR NASSERNo ratings yet
- Chapter 2 230327072253 9bf1fc09Document23 pagesChapter 2 230327072253 9bf1fc09parmarkeval1610No ratings yet
- PCOL CHP 4-6 (Situational Analysis)Document2 pagesPCOL CHP 4-6 (Situational Analysis)Sunshine_Bacla_4275No ratings yet
- Adrenergic PharmacologyDocument17 pagesAdrenergic PharmacologyCatNo ratings yet
- Adrenergic Agonists and AntagonistsDocument9 pagesAdrenergic Agonists and Antagonistsstephanienwafor18No ratings yet
- L19 - Adrenergic IVDocument7 pagesL19 - Adrenergic IVyasaira707No ratings yet
- Cholinoceptor AntagonistDocument21 pagesCholinoceptor Antagonistraafat mohammedNo ratings yet
- Pharm QuestionsDocument5 pagesPharm Questionsvaroon525No ratings yet
- Antagonis KolinergikDocument49 pagesAntagonis KolinergikGde Ananda ArmanditaNo ratings yet
- Cholinergic ReceptorsDocument67 pagesCholinergic ReceptorsShynne RPhNo ratings yet
- Cardiovascular Pharmacology PDFDocument20 pagesCardiovascular Pharmacology PDFMelanie PrinceNo ratings yet
- Selfassessment QuestionsPharmBasicsDocument7 pagesSelfassessment QuestionsPharmBasicsTsukikage12No ratings yet
- PHARMACOLOGY of ANS (Synopsis For Students)Document16 pagesPHARMACOLOGY of ANS (Synopsis For Students)JIEHASMARTNo ratings yet
- Assignment On Adrenergic ReceptorDocument13 pagesAssignment On Adrenergic ReceptoryannaingNo ratings yet
- Practical Guidance Introduction of The PracticalDocument4 pagesPractical Guidance Introduction of The PracticalNella Rosyalina DamayantiNo ratings yet
- L17 - Adrenergics IIDocument6 pagesL17 - Adrenergics IIyasaira707No ratings yet
- SympathomimeticsDocument25 pagesSympathomimeticsMirza Shaharyar BaigNo ratings yet
- Al-Bayan University Pharmacy College 3 Stage Pharmacy: 5 Drugs Acting On ANS DR - Khulood SaadoonDocument42 pagesAl-Bayan University Pharmacy College 3 Stage Pharmacy: 5 Drugs Acting On ANS DR - Khulood SaadoonAsdar LeaqerNo ratings yet
- Pharmacology: Drugs Acting On The Autonomic Nervous SystemDocument9 pagesPharmacology: Drugs Acting On The Autonomic Nervous SystemShun Reigh SumilangNo ratings yet
- Inotropic Agents: Submitted ToDocument87 pagesInotropic Agents: Submitted Toraman kumariNo ratings yet
- Pharmacology Table For Cardiovascular LectureDocument10 pagesPharmacology Table For Cardiovascular LecturemuhammadridhwanNo ratings yet
- Neuropathophysiology I Synaptic Transmission and What Can Go WrongDocument12 pagesNeuropathophysiology I Synaptic Transmission and What Can Go Wrongmaestrojedi33No ratings yet
- Soal AnfismanDocument5 pagesSoal AnfismanDike IrvaniNo ratings yet
- Intro To Pharmacology Study GuideDocument93 pagesIntro To Pharmacology Study GuideMichelle Morgan LongstrethNo ratings yet
- ANS Dan FD Gizi 2012Document31 pagesANS Dan FD Gizi 2012indahNo ratings yet
- Autonomic Nervous System PharmacologyDocument97 pagesAutonomic Nervous System PharmacologyKarun Kumar Shingari100% (1)
- Pharmacology Test 1Document39 pagesPharmacology Test 1Niki BolinNo ratings yet
- ANS ReceptorsDocument14 pagesANS ReceptorsAisha AliNo ratings yet
- Activity 2. Drug TargetsDocument3 pagesActivity 2. Drug TargetsKim KraliNo ratings yet
- Jelie Rose BSM 3 Phama Midterm ActivityDocument8 pagesJelie Rose BSM 3 Phama Midterm ActivityJanine VegaNo ratings yet
- Chapter 2 PharmacologyDocument18 pagesChapter 2 Pharmacologynikhilkhatker2020No ratings yet
- First Page PDFDocument1 pageFirst Page PDFferhanmu419No ratings yet
- Ok MarkDocument2 pagesOk MarkJordan KiddNo ratings yet
- Phama Exam.Document14 pagesPhama Exam.muwonge benonNo ratings yet
- Subject: Pharmacology Topic: ANS 2 Lecturer: Maria Luisa D. Delacruz, M.D. Date of Lecture:August 3, 2011 Transcriptionist: Anonymous Pages: 16Document16 pagesSubject: Pharmacology Topic: ANS 2 Lecturer: Maria Luisa D. Delacruz, M.D. Date of Lecture:August 3, 2011 Transcriptionist: Anonymous Pages: 16dtimtimanNo ratings yet
- Drugs Acting On Autonomic Nervous System: Week 13Document12 pagesDrugs Acting On Autonomic Nervous System: Week 13Alee Iz HarNo ratings yet
- Pharmacology: Students Notes/ WorkbookDocument50 pagesPharmacology: Students Notes/ WorkbookPABLO, JACKSON P.No ratings yet
- CristineBSM 3 Phama Midterm ActivityDocument7 pagesCristineBSM 3 Phama Midterm ActivityJanine VegaNo ratings yet
- 08 Autonomic Nervous SystemDocument0 pages08 Autonomic Nervous SystemjuniorebindaNo ratings yet
- HPHY 225 Assignment - FinalDocument5 pagesHPHY 225 Assignment - FinalSylvester MathiasNo ratings yet
- Mechanisms of Anesthetic ActionDocument3 pagesMechanisms of Anesthetic ActionRahma TomuNo ratings yet
- SympathomimeticDocument71 pagesSympathomimeticahmad tariqNo ratings yet
- Total Point Value: 20 Towards The Simbiosys Grade/Homework 2Document6 pagesTotal Point Value: 20 Towards The Simbiosys Grade/Homework 2Katia KovalenkaNo ratings yet
- Lec 16Document3 pagesLec 16Abdullahayad farouqNo ratings yet
- Lec #10 Introduction To CNS Pharmacology: 1. Voltage-GatedDocument13 pagesLec #10 Introduction To CNS Pharmacology: 1. Voltage-GatedAya ShahrouriNo ratings yet
- Camille I BSM 3 Phama Midterm ActivityDocument8 pagesCamille I BSM 3 Phama Midterm ActivityJanine VegaNo ratings yet
- Pharm Assign 3Document7 pagesPharm Assign 3mjamie12345No ratings yet
- 11 Ancylostoma StrongylodDocument61 pages11 Ancylostoma Strongylodmedical.student.messiNo ratings yet
- Pharm Drug ListDocument20 pagesPharm Drug Listsxymd321No ratings yet
- The Cholinergic Antagonists: PharmacologyDocument5 pagesThe Cholinergic Antagonists: PharmacologyDr-Dalya ShakirNo ratings yet
- Tutorial On ANS PharmacologyDocument23 pagesTutorial On ANS PharmacologyRomaine-Ricardo FrancisNo ratings yet
- Type of Neurotransmitter, Synthesis-Activation-Termination and Comparison Between Normal and DisorderDocument9 pagesType of Neurotransmitter, Synthesis-Activation-Termination and Comparison Between Normal and DisorderNehasish SahuNo ratings yet
- Veterinary ImmunologyDocument271 pagesVeterinary ImmunologySam Bot100% (1)
- Equine Anesthesia Course NotesDocument15 pagesEquine Anesthesia Course NotesSam Bot100% (1)
- Veterinary Virology PDFDocument275 pagesVeterinary Virology PDFSam Bot100% (5)
- Brag Sheet Easy Typing From HSMSEDocument6 pagesBrag Sheet Easy Typing From HSMSEmoonshoesgirlNo ratings yet
- 0813 Part B DCHB Sikar PDFDocument296 pages0813 Part B DCHB Sikar PDFMohit JangidNo ratings yet
- OverthinkingDocument9 pagesOverthinkinghabibatullah nur hanifahNo ratings yet
- Aime201704040 M162367Document29 pagesAime201704040 M162367Ziggy GonNo ratings yet
- Abdominal & Urology Surgical Signs: Murphy'S SignDocument2 pagesAbdominal & Urology Surgical Signs: Murphy'S SignAljon AgustinNo ratings yet
- Writing Dentistry Sample Test 1Document5 pagesWriting Dentistry Sample Test 1Eduardo Antonio Comaru GouveiaNo ratings yet
- Dentofacial Effects of Miniscrew-Anchored Maxillary Protraction On Prepubertal Children With Maxillary Deficiency A RCTDocument13 pagesDentofacial Effects of Miniscrew-Anchored Maxillary Protraction On Prepubertal Children With Maxillary Deficiency A RCTtanloonhanNo ratings yet
- リーフレットDocument2 pagesリーフレットFedPort MIntNo ratings yet
- GSIS V. BaulDocument12 pagesGSIS V. BaulWolf DenNo ratings yet
- Annexure-E: List of Programmes For Financial Aid To Education Board Toppers and Specific Educational GroupsDocument5 pagesAnnexure-E: List of Programmes For Financial Aid To Education Board Toppers and Specific Educational GroupsRushikesh ZirpeNo ratings yet
- 4 - CLinical Epidemiology - Diagnostic Tests 1 - NSU Jun 2019Document77 pages4 - CLinical Epidemiology - Diagnostic Tests 1 - NSU Jun 2019jon abedin jonyNo ratings yet
- Omnicell Product Catalog - 2018Document119 pagesOmnicell Product Catalog - 2018Futurista SNo ratings yet
- Front Office MCQDocument15 pagesFront Office MCQNoor TayyabaNo ratings yet
- Playbook HCPSerialization Opt V10Document182 pagesPlaybook HCPSerialization Opt V10Kapil Dev SaggiNo ratings yet
- Periapical LesionsDocument36 pagesPeriapical LesionsGaddafi HamzaNo ratings yet
- Ascaris, Trichuris, Oxyuris, HookwormDocument55 pagesAscaris, Trichuris, Oxyuris, HookwormnurlailiNo ratings yet
- Discussion: Part 1: Nurse's Knowledge Toward MRSADocument1 pageDiscussion: Part 1: Nurse's Knowledge Toward MRSAMustafa KhudhairNo ratings yet
- Disaster Management CycleDocument36 pagesDisaster Management CycleArra Placides100% (1)
- Literature ReviewDocument4 pagesLiterature Reviewapi-548856677No ratings yet
- Oprec Bersinar - Soal Dan PembahasanDocument3 pagesOprec Bersinar - Soal Dan Pembahasansalsabila zahronNo ratings yet
- Chiller Column Beam ErectionDocument6 pagesChiller Column Beam ErectionShrikant SawantNo ratings yet
- Jurnal - KUALITAS PELAYANAN RAWAT INAP RUMAH SAKIT UMUM DAERAHDocument9 pagesJurnal - KUALITAS PELAYANAN RAWAT INAP RUMAH SAKIT UMUM DAERAHPeri HidayatNo ratings yet
- PrematurityDocument11 pagesPrematurityKenneth UbaldeNo ratings yet
- Normal LabourDocument10 pagesNormal LabourikeyoganitabangunNo ratings yet
- Principle of Fish Health ManagementDocument2 pagesPrinciple of Fish Health ManagementMegersaNo ratings yet
- The Problem and Its Scope RationaleDocument7 pagesThe Problem and Its Scope RationaleSimplicio Gadugdug VNo ratings yet