Professional Documents
Culture Documents
Patella - Reduction & Fixation - Sleeve... e Fixation - A1 - AO Surgery Reference
Uploaded by
Luis Miguel Martins0 ratings0% found this document useful (0 votes)
11 views4 pagespatologia patelar. redução e fixação no caso de sleeve.
Original Title
Patella - Reduction & Fixation - Sleeve...e Fixation - A1 - AO Surgery Reference
Copyright
© © All Rights Reserved
Available Formats
PDF or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentpatologia patelar. redução e fixação no caso de sleeve.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF or read online from Scribd
0 ratings0% found this document useful (0 votes)
11 views4 pagesPatella - Reduction & Fixation - Sleeve... e Fixation - A1 - AO Surgery Reference
Uploaded by
Luis Miguel Martinspatologia patelar. redução e fixação no caso de sleeve.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF or read online from Scribd
You are on page 1of 4
AOR ce
Online reference in clinical life
Le
Executive Editor:
Chris Colton
Authors: Florian
Gebhard, Phil
Kregor, Chris Oliver
Patella 34-a1
ORIF
Search
Isearch.
Q
Shortcuts
All Preparations
All Approaches
All Reductions &
Fixations
Open reduction; sleeve fracture
fixation
1 Principtes
Surgical anatomy
The patella is the
largest sesamoid bone
in the human body. It
is located within the
extensor apparatus of
the knee, Anatomical
features include the proximal articular body, with an
extraarticular anterior surface and a posterior
articular surface, and the extraarticular distal pole.
The rectus femoris and vastus intermedius muscles
insert at the superior pole of the body and the vastus
medialis and vastus lateralis muscles on either side.
The patellar tendon originates from the inferior pole
and inserts into the tibial tuberosity. The articular
surface has the thickest layer of cartilage in the body,
up to 5 mm, reflecting the very high resultant loads
across the patello-femoral joint, rendering it
susceptible to chondromalacia and degenerative joint
disease.
History and examination
Patellar fractures comprise about 1% of all fractures
and are mostly caused by direct trauma to the front
of the knee, for example, a direct fall, or a blow onto
the flexed knee.
Bony avulsions of the adjacent tendons, or pure
ruptures of the quadriceps and patellar tendons, are
caused by indirect forces.
Typical signs are swelling, tenderness and limited, or
lost, function of the extensor mechanism.
Preservation of active knee extension does not rule
out a patellar fracture if the auxiliary extensors of the
knee - the medial and lateral parapatellar retinacula -
are intact.
If displacement is significant, it is possible to palpate
a defect between the fragments, if present. The
hemarthrosis is usually obvious. The examination
must include assessment of the soft tissues, so as
not to confuse with an injury to the prepatellar bursa,
or to omit grading the injury if the fracture is open.
In addition to the
standard x-rays of the
knee in two planes, a
tangential (“skyline”)
view of the patella is
useful. In the AP view,
the patella normally projects into the midline of the
femoral sulcus. Its lower pole is located just above a
line drawn across the distal profile of the femoral
condyles. In the lateral view the proximal tibia must
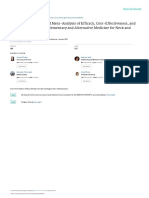
Insall Salvati Ratio
B/A=1
1 2
be visible to exclude a bone avulsion of the patellar
tendon from the tibial tuberosity. A rupture of the
patellar tendon, or an abnormal position of the patella
like patella alta (high-riding patella), or patella baja
(shortening of the tendon), can be recognized with
the help of the Insall-Salvati method. This is the
relationship between the length of the patella (B) and
of the patellar tendon (A) on the lateral x-ray, r=B/A.
This ratio is normally r= 1. A ratio r < 0.8 suggests a
high-riding patella (patella alta), or patellar tendon
rupture.
The third important x-ray projection is the 30°
tangential view, which is obtainable in 45° knee
flexion. If a longitudinal, or osteochondral fracture, is
suspected, the 30° tangential view is a helpful
diagnostic adjunct.
Special imaging is helpful in certain cases, such as
stress fractures, in elderly patients with osteopenia
and hemarthrosis, and also in cases of patellar
nonunion, or malunion.
Computed tomography is recommended only for the
evaluation of articular incongruity in cases of
nonunion, malunion and patello-femoral alignment
disorders,
Scintigraphic examination (or MRI) can be helpful in
the diagnosis of stress fractures; a leukocyte scan
can reveal signs of osteomyelitis.
MRI can be helpful to diagnose cartilage defects and
lesions.
Tendon ruptures and
patellar dislocation
must be ruled out.
Isolated rupture of the
quadriceps, or patellar,
tendon must be
excluded by clinical
evaluation (palpation) and ultrasound scan (or MRI).
Dislocation, most commonly occurring to the lateral
side, may result in osteochondral shear fractures with
lesions of the medial margin of the patella, and
occasionally impaction fractures of the lateral lip of
the patellar groove of the femur.
X-ray by courtesy of Spital Davos, Switzerland, Dr C
Ryf and Dr A Leumann.
2 Reduction and fixation
Reduc!
n techniques and tools
The knee joint and fracture lines must be irrigated
and cleared of blood clots and small debris to allow
exact reconstruction.
‘An image intensifier should always be available so
that the final result can be checked in the AP and
lateral planes.
Patellar tendon avulsion
Occasionally, the patellar tendon is avulsed from the
lower pole of the patella, together with a thin shell, or
“sleeve”, of bone as
illustrated
This may be very
subtle on x-rays as
the sleeve remaining
within the avulsed
tendon is thin and is
often not apparent on over-penetrated images, whilst
at the same time, the lower pole of the patella may
have a virtually normal profile. A clue may be found
by detection of a patella alta (as appreciated by the
Insall-Salvati index).
Fixation of avulsion
Insert a partially
threaded cannulated
screw, with a washer,
as a lag screw.
Neutralization of
bending forces
As implant pull-out, or
failure, is virtually
inevitable, the bending
distraction forces must
be neutralized by
additional patellotibial cerclage wiring.
Repair any tears of the lateral and medial patellar
retinacula with sutures.
GH) 0
a
v1.0 2008-12-03
You might also like
- 4 - 2020 - Acup para Reab Pós-Avc Trat Neglet Unilateral - Sist Rev + Meta AnalDocument9 pages4 - 2020 - Acup para Reab Pós-Avc Trat Neglet Unilateral - Sist Rev + Meta AnalLuis Miguel MartinsNo ratings yet
- 2013 - Melhores Práticas - Prev + Trat Pós-Concussão em Pediatria - AdolescentesDocument6 pages2013 - Melhores Práticas - Prev + Trat Pós-Concussão em Pediatria - AdolescentesLuis Miguel MartinsNo ratings yet
- 2013 - Descanso Pós-Concussão - Questão... A Melhor Abordagem... Questão - Recomendações para Returno Atividade Pós-Concussão em Atletas, Civis, Miliares AtivoDocument10 pages2013 - Descanso Pós-Concussão - Questão... A Melhor Abordagem... Questão - Recomendações para Returno Atividade Pós-Concussão em Atletas, Civis, Miliares AtivoLuis Miguel MartinsNo ratings yet
- 2013 - Tratamento Com Exercícios para Sindrome Pós-Concussão - Alt Sintomas - Figiologia - Ativação Funcional MRiDocument9 pages2013 - Tratamento Com Exercícios para Sindrome Pós-Concussão - Alt Sintomas - Figiologia - Ativação Funcional MRiLuis Miguel MartinsNo ratings yet
- 2013 - Conceitos Na Abordagem Da Concussão No Desporto - Abordagem MultidisciplinarDocument9 pages2013 - Conceitos Na Abordagem Da Concussão No Desporto - Abordagem MultidisciplinarLuis Miguel MartinsNo ratings yet
- 2 - Correção 2017 - Acup para Tratamento Da Espasticidade Pós-Avc - Sist Rev + Meta AnáliseDocument1 page2 - Correção 2017 - Acup para Tratamento Da Espasticidade Pós-Avc - Sist Rev + Meta AnáliseLuis Miguel MartinsNo ratings yet
- Custo Efetividade de Técnicas MTC Cervicalgia Ou LombalgiaDocument62 pagesCusto Efetividade de Técnicas MTC Cervicalgia Ou LombalgiaLuis Miguel MartinsNo ratings yet
- 2012 - Ref.a Adapatada para ... Concussion-Treatment-Recovery-Guide Return To Learn - Return To Work ... GuidelinesDocument2 pages2012 - Ref.a Adapatada para ... Concussion-Treatment-Recovery-Guide Return To Learn - Return To Work ... GuidelinesLuis Miguel MartinsNo ratings yet
- Review ArticleDocument8 pagesReview ArticleLuis Miguel MartinsNo ratings yet
- AACVPR Guidelines For AACVPR Guidelines For Pulmonary Rehabilitation Programs (4 Edition)Document37 pagesAACVPR Guidelines For AACVPR Guidelines For Pulmonary Rehabilitation Programs (4 Edition)Jeffery SamuelNo ratings yet
- Ecam2015 870398Document12 pagesEcam2015 870398YUTRILIANo ratings yet
- 1 - 2017 - Tuina para Prob Musculo-Esqueléticos - Rev SistDocument22 pages1 - 2017 - Tuina para Prob Musculo-Esqueléticos - Rev SistLuis Miguel MartinsNo ratings yet
- Tidal Volumes For Ventilated Patients Should Be Determined at The Endotracheal TubeDocument4 pagesTidal Volumes For Ventilated Patients Should Be Determined at The Endotracheal TubeLuis Miguel MartinsNo ratings yet
- Gonzalez2003 Article AirLeaksDuringMechanicalVentilDocument7 pagesGonzalez2003 Article AirLeaksDuringMechanicalVentilLuis Miguel MartinsNo ratings yet
- The Role of Interdisciplinary Teams in Physical and Rehabilitation MedicineDocument6 pagesThe Role of Interdisciplinary Teams in Physical and Rehabilitation MedicineLakshmi PrasannaNo ratings yet
- Otago Strength and Balance Training Exercise Programme: An Information Guide For PatientsDocument28 pagesOtago Strength and Balance Training Exercise Programme: An Information Guide For PatientsMeenakshiputraeashwarprasad MacherlaNo ratings yet
- Evidence For Prescribing PA As Therapy in 26 Different Chronic Diseases PDFDocument72 pagesEvidence For Prescribing PA As Therapy in 26 Different Chronic Diseases PDFKike TostadoNo ratings yet
- 2013 - KOREA SUL - ACUP (Com Injec. Sc. Veneno Abelha em Acup - PTS.) - R. - Dor Pós-AVCDocument4 pages2013 - KOREA SUL - ACUP (Com Injec. Sc. Veneno Abelha em Acup - PTS.) - R. - Dor Pós-AVCLuis Miguel MartinsNo ratings yet
- 2003 - Reab Post TKA - TKRDocument4 pages2003 - Reab Post TKA - TKRLuis Miguel MartinsNo ratings yet
- Energetics of Table Tennis and Table Tennis Specific Exerc TestingDocument21 pagesEnergetics of Table Tennis and Table Tennis Specific Exerc TestingLuis Miguel MartinsNo ratings yet
- Atlas de AnaomiaDocument496 pagesAtlas de AnaomiaLuis Miguel MartinsNo ratings yet
- 2018 - Défice de Vit D Nas # Femur PDFDocument5 pages2018 - Défice de Vit D Nas # Femur PDFLuis Miguel MartinsNo ratings yet
- Patella Fracture Post-Op Rehab ProtocolDocument1 pagePatella Fracture Post-Op Rehab ProtocolErlin IrawatiNo ratings yet
- Asian Journal of Sports MedicineDocument9 pagesAsian Journal of Sports MedicineLuis Miguel MartinsNo ratings yet
- 2015 - R. CIR % REAB # Patelar SleeveDocument2 pages2015 - R. CIR % REAB # Patelar SleeveLuis Miguel MartinsNo ratings yet
- 2015 - Lesoes Traumáticas Joelho PediátricoDocument23 pages2015 - Lesoes Traumáticas Joelho PediátricoLuis Miguel MartinsNo ratings yet
- 2014 - # Sleever PatelarDocument4 pages2014 - # Sleever PatelarLuis Miguel MartinsNo ratings yet
- 2014 - # Patelar (Classificação, Etiologia, Evolução, Tratamento) .Document10 pages2014 - # Patelar (Classificação, Etiologia, Evolução, Tratamento) .Luis Miguel MartinsNo ratings yet
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)