Professional Documents
Culture Documents
Cardionursing 110207023802 Phpapp01 PDF
Cardionursing 110207023802 Phpapp01 PDF
Uploaded by
zhai bambalanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Cardionursing 110207023802 Phpapp01 PDF
Cardionursing 110207023802 Phpapp01 PDF
Uploaded by
zhai bambalanCopyright:
Available Formats
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
MEDICAL AND SURGICAL NURSING
Cardiovascular System
Lecturer: Mark Fredderick R. Abejo RN, MAN
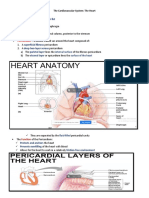
Anatomy and Physiology of the Heart
Cardiovascular system consists of the heart, arteries,
veins & capillaries. The major function are circulation of blood,
delivery of O2 & other nutrients to the tissues of the body &
removal of CO2 & other cellular products metabolism
Pericardium invaginated sac
Visceral attached to the exterior of
myocardium
Parietal attached to the great vessels and
diaphragm
Heart
Papillary Muscle
Arise from the endocardial & myocardial surface of the
ventricles & attach to the chordae tendinae
Chordae Tendinae
Attach to the tricuspid & mitral valves & prevent eversion
during systole
Separated into 2 pumps:
right heart pumps blood through the lungs
left heart pumps blood through the peripheral
organs
Chamber of the Heart
Atria
2 chambers, function as receiving chambers, lies
above the ventricles
Muscular pumping organ that propel blood into the arerial
system & receive blood from the venous system of the body.
Hollow muscular behind the sternum and between the lungs
Located on the middle of mediastinum
Resemble like a close fist
Weighs approximately 300 400 grams
Has heart wall has 3 layers
Endocardium lines the inner chambers of the
heart, valves, chordate tendinae and papillary
muscles.
Myocardium muscular layer, middle layer,
responsible for the major pumping action of the
ventricles.
Epicardium thin covering(mesothelium),
covers the outer surface of the heart
Medical and Surgical Nursing
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
Upper Chamber (connecting or receiving)
Right Atrium: receives systemic venous blood
through the superior vena cava, inferior vena cava &
coronary sinus
Left Atrium: receives oxygenated blood returning to
the heart from the lungs trough the pulmonary veins
Coronary Veins
Coronary sinus main vein of the heart
Great Cardiac vein main tributary of the coronary sinus
Oblique vein remnant of SVC, small unsignificant
Heart Circulation
Ventricles
2 thick-walled chambers; major responsibility for
forcing blood out of the heart; lie below the atria
Lower Chamber (contracting or pumping)
Right Ventricle: contracts & propels deoxygenated
blood into pulmonary circulation via the aorta
during ventricular systole; Right atrium has
decreased pressure which is 60 80 mmHg
Left Ventricle: propels blood into the systemic
circulation via aortaduring ventricular systole; Left
ventricle has increased pressure which is 120 180
mmHg in order to propel blood to the systemic
circulation
Heart Valves
Tricuspid
Pulmonic
Mitral
Aortic
Cardiac Conduction System
Properties of Heart Conduction System
Automaticity
Excitability
Conductivity
Contractility
Coronary artery 1st branch of aorta
Right Coronary
SA nodal Branch supplies SA node
Right marginal Branch supplies the right border
of the heart
AV nodal branch supplies the AV node
Posterior interventricular artery supplies both
ventricles
Left Coronary
Circumflex branch supplies SA node in 40 % of
people
Left marginal supplies the left ventricle
Anterior interventricular branch aka Left anterior
descending(LAD)supplies both ventricles and
interventricular septum
Lateral branch terminates in ant surface of the
heart
Structure of Heart Conduction System
Medical and Surgical Nursing
Nodal tissues
SA Node( Sino-atrial, Keith and Flack)
Primary Pacemaker
Between SVC and RA
Vagal and symphatetic innervation
Sinus Rhythms
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
The Normal Cardiac Cycle
AV Node( Atrioventricular , Kent and Tawara)
At the right atrium
3 zones
AN Zone(atrionodal)
N Zone (nodal)
NH zone (nodal HIS)
General Concepts
Systole - period of chamber contraction
Diastole - period of chamber relaxation
Cardiac cycle - all events of systole and diastole during one
heart flow cycle
Internodal and Interatrial Pathways
Connects SA and AV Node
Ant. Internodal(bachman) tract
Middle Internodal(wenkebach) tract
Posterior internodal(Thorel) tract
Events of Cardiac Cycle
1.
Bundle of His/ Purkinje Fibers
Provides for ventricular conduction system
Fastest conduction among cardiac tissues
Right bundle
Left Bundle
Cardiac Action Potential
Depolarization: electrical activation of a cell caused by
the influx of sodium into the cell while potassium exits
the cell
Repolarization: return of the cell to the resting state
caused by re-entry of potassium into the cell while
sodium exits
Refractory periods:
Effective refractory period: phase in which cells
are incapable of depolarizing
Relative refractory period: phase in which cells
require a stronger-than-normal stimulus to
depolarize
2.
3.
b.
Atrioventricular node (AV node) - impulses pass from
SA via gap junctions in about 40 ms.; impulses are
delayed about 100 ms to allow completion of the
contraction of both atria; located just above tricuspid
valve (between right atrium & ventricle)
c.
Atrioventricular bundle (bundle of His) - in the
interATRIAL septum (connects L and R atria)
d.
L and R bundle of His branches - within the
interVENTRICULAR septum (between L and R
ventricles)
e.
Purkinje fibers - within the lateral walls of both the L and
R ventricles; since left ventricle much larger, Purkinjes
more elaborate here; Purkinje fibers innervate papillary
muscles before ventricle walls so AV can valves prevent
backflow
Medical and Surgical Nursing
ventricles relax, ventricular pressure becomes LOW
semilunar valves close, aorta & pulmonary trunk
backflow
TOTAL CARDIAC CYCLE TIME = 0.8 second
(normal 70 beats/minute)
atrial systole (contraction)
=
ventricular systole (contraction) =
quiescent period (relaxation)
=
0.1 second
0.3 second
0.4 second
Cardiac Output - Blood Pumping of the Heart
General Concepts
Stroke volume: the amount of blood ejected with each
heartbeat
Cardiac output: amount of blood pumped by the
ventricle in liters per minute
Preload: degree of stretch of the cardiac muscle fibers at
the end of diastole
Contractility: ability of the cardiac muscle to shorten in
response to an electrical impulse
Afterload: the resistance to ejection of blood from the
ventricle
Ejection fraction: the percent of end-diastolic volume
ejected with each heartbeat
(from SA through complete heart contraction = 220 ms = 0.22 s)
Sinoatrial node (SA node) "the pacemaker" - has the
fastest autorhythmic rate (70-80 per minute), and sets the
pace for the entire heart; this rhythm is called the sinus
rhythm; located in right atrial wall, just inferior to the
superior vena cava
filled ventricles begin to contract, AV valves
CLOSE
contraction of closed ventricles increases pressure
ventricular ejection phase - blood forced out
semilunar valves open, blood -> aorta & pulmonary
trunk
isovolumetric relaxation: early ventricular diastole
(right atrium)
sinoatrial node (SA)
(right AV valve)
atrioventricular node (AV)
atrioventricular bundle (bundle of His)
right & left bundle of His branches
Purkinje fibers of ventricular walls
a.
the AV valves are open
pressure: LOW in chambers; HIGH in
aorta/pulmonary trunk
aortic/pulmonary semilunar valves CLOSED
blood flows from vena cavas/pulmonary vein INTO
atria
blood flows through AV valves INTO ventricles
(70%)
ventricular systole: blood ejected from heart
Anatomical Sequence of Excitation of the Heart
mid-to-late ventricular diastole: ventricles filled
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
hypernatremia - HIGH Na+ concentration; can
block Na+ transport & muscle contraction
General Variables of Cardiac Output
1. Cardiac Output (CO) - blood amount pumped per minute
CO (ml/min) = HR (beats/min) X SV (ml/beat)
Normal CO = 75 beats/min X 70 ml/beat
= 5.25 L/min
3. Other Factors Effecting Heart Rate (HR)
normal heart rate - fetus 140 - 160 beats/minute
female 72 - 80 beats/minute
male 64 - 72 beats/minute
2. Heart Rate (HR) - cardiac cycles per minute
Normal range is 60-100 beats per minute
Tachycardia is greater than 100 bpm
Bradycardia is less than 60 bpm
Sympathetic system INCREASES HR
Parasympathetic system (Vagus) DECREASES HR
1.
2.
3.
4.
3. Blood pressure - Cardiac output X peripheral resistance
Control is neural (central and peripheral) and
hormonal
Baroreceptors in the carotid and aorta
Hormones- ADH, aldosterone, epinephrine can
increase BP; ANF can decrease BP
5.
Vascular System
Regulation of Stroke Volume (SV)
exercise - lowers resting heart rate (40-60)
heat - increases heart rate significantly
cold - decreases heart rate significantly
tachycardia - HIGHER than normal resting heart rate
(over 100); may lead to fibrillation
bradycardia - LOWER than normal resting heart rate
(below 60); parasympathetic drug side effects; physical
conditioning; sign of pathology in non-healthy patient
Major function of the blood vessels isto supply the tissue
with blood, remove wastes, & carry unoxygenated blood
End diastolic volume (EDV) - total blood collected in
ventricle at end of diastole; determined by length of
diastole and venous pressure (~ 120 ml)
End systolic volume (ESV) - blood left over in ventricle
at end of contraction (not pumped out); determined by
force of ventricle contraction and arterial blood pressure
(~50 ml)
back to the heart
Types of Blood Vessels
Arteries
SV (ml/beat) = EDV (ml/beat) - ESV (ml/beat)
Normal SV
= 120 ml/beat - 50 ml/beat
= 70 ml/beat
Elastic-walled vessels that can stretch during systole &
recoil during diastole; they carry blood away from the
heart & distribute oxygenated blood throughout the body
Frank-Starling Law of the Heart - critical factor for stroke
volume is "degree of stretch of cardiac muscle cells";
more stretch = more contraction force
Arterioles
Small arteries that distribute blood to the capillaries &
increased EDV = more contraction force
slow heart rate = more time to fill
exercise = more venous blood return
function in controlling systemic vascular resistance &
therefore arterial pressure
Capilliaries
The following exchanges occurs in the capilliaries
Regulation of Heart Rate (Autonomic, Chemical, Other)
O2 & CO2
1. Autonomic Regulation of Heart Rate (HR)
Solutes between the blood & tissue
Sympathetic - NOREPINEPHRINE (NE) increases heart
rate (maintains stroke volume which leads to increased
Cardiac Output)
Fluid volume transfer between the plasma &
interstitial space
Venules
Parasympathetic - ACETYLCHOLINE (ACh) decreases
heart rate
Small veins that receive blood from capillaries &
function as collecting channels between the capillaries &
Vagal tone - parasympathetic inhibition of inherent rate
of SA node, allowing normal HR
veins
Veins
Baroreceptors, pressoreceptors - monitor changes in
blood pressure and allow reflex activity with the
autonomic nervous system
Low-pressure vessels with thin small & less muscles than
arteries; most contains valves that prevent retrograde
blood flow; they carry deoxygenated blood back to the
2. Hormonal and Chemical Regulation of Heart Rate (HR)
heart. When the skeletal surrounding veins contract, the
epinephrine - hormone released by adrenal medulla
during stress; increases heart rate
thyroxine - hormone released by thyroid; increases heart
rate in large quantities; amplifies effect of epinephrine
Ca++, K+, and Na+ levels very important;
hyperkalemia - increased K+ level; KCl used to
stop heart on lethal injection
hypokalemia - lower K+ levels; leads to
abnormal heart rate rhythms
hypocalcemia - depresses heart function
hypercalcemia - increases contraction phase
Medical and Surgical Nursing
veins are compressed, promoting movement of blood
back to the heart.
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
Palpation:
Assessment of the Client with Cardiovascular
Disorders
Nursing History
Risk Factors
A. Non Modifiable Risk Factor
Age
Gender
Race
Heredity
Heart Sounds: Stethoscope Listening
B. Modifiable Risk Factor
Stress
Diet
Exercise
Sedentary lifestyle
Cigarette smoking
Alcohol
Hypertension
Hyperlipidemia
DM
Obesity
Type A personality
Contraceptive Pills
Overview of Heart Sounds (lub-du ; lub, dub )
Common Clinical Manifestations of Cardiovascular Disorders
S2 - due to the closure of the semi-lunar (pulmonic/aortic) valves
- timing: diastole
- loudest at the base
a.
b.
c.
d.
e.
f.
g.
h.
i.
j.
k.
lub - closure of AV valves, onset of ventricular systole
dub - closure of semilunar valves, onset of diastole
Tricuspid valve (lub) - RT 5th intercostal, medial
Mitral valve (lub) - LT 5th intercostal, lateral
Aortic semilunar valve (dub) - RT 2nd intercostal
Pulmonary semilunar valve (dub) - LT 2nd intercostals
S1 - due to closure of the AV(mitral/tricuspid) valves
- timing: beginning of systole
- loudest at the apex
Dyspnea
- Exertional
- Orthopnea
- Paroxysmal Noctural Dyspnea
- Cheyne-stokes
Chest Pain
Edema
- Ascites
- Hydrothorax
- Anasarca
Palpitation
Hemoptysis
Fatigue
Syncope and Fainting
Cyanosis
Abdominal Pain
Clubbing of fingers
Jaundice
S3 Ventricular Diastolic Gallop
Mechanism: vibration resulting from resistance to rapid
ventricular filling secondary to poor compliance
Timing: early diastole
Location: Apex (LV) or LLSB (RV)
Pitch: faint and low pitched
S4 - Atrial Diastolic Gallop
Mechanism: vibration resulting from resistance to late
ventricular filling during atrial systole
Timing: late diastole ( before S1)
Location: Apex ( LV) or LLSB (RV)
Pitch: low ( use bell)
Physical Assessment
Inspection:
Skin color
Neck vein distention
Heart Murmurs
Murmur - sounds other than the typical "lub-dub"; typically caused
by disruptions in flow
Respirations
Pulsations
Clubbing
Capillary refill
Medical and Surgical Nursing
Incompetent valve - swishing sound just AFTER the
normal "lub" or "dub"; valve does not completely close,
some regurgitation of blood
Stenotic valve - high pitched swishing sound when blood
should be flowing through valve; narrowing of outlet in
the open state
Pericardial Friction Rub
It is an extra heart sound originating from the pericardial sac
Mechanism: Originates from the pericardial sac as it moves
Timing: with each heartbeat
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
Location: over pericardium. Upright position, leaning
forward
Pitch: high pitched and scratchy. Sounds like sandpaper
being rubbed together
Significance: inflammation, infection, infiltration
2. Coagulation Screening Test
a. Bleeding Time measures the ability to stop bleeding after
small puncture wound
b. Partial Thromboplastin Time (PTT) used to identify
deficiencies of coagulation factors, prothrombin and fibrinogen;
monitors heparin therapy.
Classification of Clients with Diseases of the
Heart ( Functional Capacity )
c. Prothrombin Time (Pro-time) determines activity and
interaction of the Prothrombin group: factors V (preacclerin), VII
(proconvertin), X (Stuart-Power factor), prothrombin and
fibrinogen; used to determine dosages of oral anti-coagulant.
Class I. Patients with cardiac disease but without
resulting limitations of physical activity.
Class II. Patients with cardiac disease resulting to slight
limitation of physical activity
Class III. Patients with cardiac disease resulting in
marked limitation of physical activity. They are
comfortable at rest.
Class IV. Patients with cardiac disease resulting in
inability to carry on any physical activity without
discomfort
Normal Values
Bleeding Time: 2.75-8 min
Partial Thromboplastin Time (PTT): 60 - 70 sec.
Prothrombin Time (PT): 12-14 sec.
3. Erythrocyte sedimentation rate ( ESR)
It is a measurement of the rate at which RBCs settle out
of anticoagulated blood in an hour
It is elevated in infectious heart disorder or myocardial
infarction
Diagnostic Assessment
Purposes:
1. To assist in diagnosing MI
2. To identify abnormalities
3. To assess inflammation
4. To determine baseline value
5. To monitor serum level of medications
6. To assess the effects of medications
Normal Values
Male:
15-20 mm/hr
Female: 20-30 mm/hr
4. CARDIAC Proteins and enzymes
A. Blood Studies
a.
CK- MB ( creatine kinase)
Most cardiac specific enzymes
Accurate indicator of myocardial dammage
Elevates in MI within 4 hours, peaks in 18 hours and
then declines till 3 days
Normal value is 0-7 U/L or males 50-325 mu/ml
Female 50-250 mu/ml
b.
Lactic Dehydrogenase (LDH)
Most sensitive indicator of myocardial damage
Elevates in MI in 24 hours, peaks in 48-72 hours
Return to normal in 10-14 days
Normally LDH1 is greater than LDH2
Lactic Dehydrogenase (LDH)
MI- LDH2 greater than LDH1 (flipped LDH pattern)
Normal value is 70-200 IU/L (100 225 mu/ml)
c.
Myoglobin
Rises within 1-3 hours
Peaks in 4-12 hours
Returns to normal in a day
Not used alone
Muscular and RENAL disease can have elevated
myoglobin
d.
Troponin I and T
Troponin I is usually utilized for MI
Elevates within 3-4 hours, peaks in 4-24 hours and
persists for 7 days to 3 weeks!
Normal value for Troponin I is less than 0.6 ng/mL
REMEMBER to AVOID IM injections before
obtaining blood sample!
Early and late diagnosis can be made!
e.
SERUM LIPIDS
Lipid profile measures the serum cholesterol,
triglycerides and lipoprotein levels
Cholesterol= 200 mg/dL
Triglycerides- 40- 150 mg/dL
LDH- 130 mg/dL
HDL- 30-70- mg/dL
NPO post midnight (usually 12 hours)
1. Complete Blood Count
a. RBC count- # of RBCs/ mm3 of blood, to diagnose anemia and
ploycythemia
b. Hemoglobin- # of grams of hgb/ 100ml of blood; to measure the
oxygen-carrying capacity of the blood
c. Hematocrit expressed in %; measures the volume of RBCs in
proportion to plasma; used also to diagnose anemia and
polycythemia and abnormal hydration states
d. RBC indices- measure RBC size and hemoglobin content
a. MCV (mean corpuscular volume)
b. MCH (mean corpuscular hemoglobin)
c. MCHC (mean corpuscular hemoglobin concentrarion)
e. Platelet count- # of Platelet/ mm3; to diagnose
thrombocytopenia and subsequent bleeding tendencies
f. WBC count- of WBCs/ mm3 of blood; to detect infection or
inflammation
g. WBC Differential count- determines proportion of each WBC
in a sample of 100 WBCs; used to classify leukemias
Normal Values
RBC: Women 4.2-5.4 million/mm3
Men 4.7-6.1 million/mm3
Hgb: Women 12-16 g/dl
Men 13-18 g/dl
Hct : Women 36-42%
Men 42-48%
WBC: 5000-10,000/mm3
Granulocytes
Neutrophils: 55-70%
Eosinophils: 1-4%
Basophils: 0.5-1.0%
Agranulocytes
Lymphocytes: 20-40%
Monocytes: 2-8%
Platelets: 150,000-450,000/mm3
Medical and Surgical Nursing
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
B. Non-Invasive Procedure
1. Cardiac Monitoring / Electrocardiography (ECG)
A non-invasive procedure that evaluates the electrical
activity of the heart
a. Limb Leads
b. Precordial Leads
Deflection Waves of ECG
1. P wave - initial wave, demonstrates the depolarization from SA
Node through both ATRIA; the ATRIA contract about 0.1 s after
start of P Wave.
2. QRS complex - next series of deflections, demonstrates the
depolarization of AV node through both ventricles; the ventricles
contract throughout the period of the QRS complex, with a short
delay after the end of atrial contraction; repolarization of atria also
obscured
3. T Wave - repolarization of the ventricles (0.16 s)
The precordial leads VI V6 are part of the 12 lead EKG.
They are not monitored with the standard limb leads
4. PR (PQ) Interval - time period from beginning of atrial
contraction to beginning of ventricular contraction (0.16 s)
c. 12 lead ECG
5. QT Interval - the time of ventricular contraction (about 0.36 s);
from beginning of ventricular depolarization to end of
repolarization.
2. Holter Monitoring
A non-invasive test in which the client wears a Holter
monitor and an ECG tracing recorded continuously over
a period of 24 hours
Instruct the client to resume normal activities and
maintain a diary of activities and any symptoms that may
develop
ECG Paper
Medical and Surgical Nursing
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
3. Stress Test
A non-invasive test that studies the heart during
activity and detects and evaluates CAD
Exercise test, pharmacologic test and emotional test
Treadmill testing is the most commonly used stress
test
Used to determine CAD, Chest pain causes, drug
effects and dysrhythmias in exercise
Pre-test: consent may be required, adequate rest , eat
a light meal or fast for 4 hours and avoid smoking,
alcohol and caffeine
During the test: secure electrodes to appropriate
location on chest, obtain baseline BP and ECG
tracing, instruct client to exercise as instructed and
report any pain, weakness and SOB, monitor BP and
ECG continuously, record at frequent interval
Post-test: instruct client to notify the physician if
any chest pain, dizziness or shortness of breath .
Instruct client to avoid taking a hot shower for 10-12
hours after the test
C. Invasive Procedure
1. Cardiac Catheterization ( Coronary Angiography /
Arteriography )
Insertion of a catheter into the heart and surrounding
vessels
Is an invasive procedure during which physician
injects dye into coronary arteries and immediately
takes a series of x-ray films to assess the structures
of the arteries
Determines the structure and performance of the
heart valves and surrounding vessels
Used to diagnose CAD, assess coronary atery
patency and determine extent of atherosclerosis
Pretest: Ensure Consent, assess for allergy to
seafood and iodine, NPO, document weight and
height, baseline VS, blood tests and document the
peripheral pulses
Pretest: Fasting for 8-12 hours, teachings,
medications to allay anxiety
Intra-test: inform patient of a fluttery feeling as the
catheter passes through the heart; inform the patient
that a feeling of warmth and metallic taste may
occur when dye is administered
Post-test: Monitor VS and cardiac rhythm
Monitor peripheral pulses, color and warmth and
sensation of the extremity distal to insertion site
Maintain sandbag to the insertion site if required to
maintain pressure
Monitor for bleeding and hematoma formation
4. Pharmacological stress test
Use of dipyridamole
Maximally dilates coronary artery
Side-effect: flushing of face
Pre-test: 4 hours fasting, avoid alcohol, caffeine
Post test: report symptoms of chest pain
5. ECHOCARDIOGRAM
Non-invasive test that studies the structural and
functional changes of the heart with the use of ultrasound
Client Preparation: instruct client to remain still during
the test, secure electrodes for simultaneous ECG tracing,
explain that there will be no pain or electrical shock,
lubricant placed on the skin will be cool.
2. Nuclear Cardiology
Are safe methods of evaluating left ventricular muscle
function and coronary artery blood distribution.
Client Preparation: obtain written consent, explain
procedure, instruct client that fasting may be required for
a short period before the exam, assess for iodine allergy.
Post Procedure: encourage client to drink fluids to
facilitate the excretion of contrast material, assess
venipuncture site for bleeding or hematoma.
Types of Nuclear Cardiology
o Multigated acquisition (MUGA) or cardiac
blood pool scan
Provides information on wall motion
during systole and diastole, cardiac
valves, and EF.
o Single-photon emission computed
tomography (SPECT)
Used to evaluate the myocardium at
risk of infarction and to determine
infarction size.
o Positron emission tomography (PET)
scanning
Uses two isotopes to distinguish
viable and nonviable myocardial
tissue.
6. Phonocardiography
Is a graphic recording of heart sound with simultaneous
ECG.
Medical and Surgical Nursing
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
Perfusion imaging with exercise testing
Determines whether the coronary
blood flow changes with increased
activity.
Used to diagnose CAD, determine
the prognosis in already diagnosed
CAD, assess the physiologic
significance of a known coronary
lesion, and assess the effectiveness of
various therapeutic modalities such
as coronary artery bypass surgery,
percutaneous coronary intervention,
or thrombolytic therapy.
CARDIAC DISORDER
CORONARY ARTERIAL DISEASE
ISCHEMIC HEART DISEASE
D. Hemodynamics Monitoring
1. CVP ( Central Venous Pressure )
Reflects the pressure of the blood in the right atrium.
Engorgement is estimated by the venous column that can
be observed as it rises from an imagined angle at th point
of manubrium ( angle of Louis).
With normal physiologic condition, the jugular venous
column rises no higher than 2-3 cm above the clavicle
with the client in a sitting position at 45 degree angle.
Client Preparation: obtain consent, insertion is under
strict sterile technique, usually at the bedside, explain to
client the sterile drapes may cover the face, assists to
position client flat or slight T-postion as tolerated and
instruct to remain still during the procedure
Nursing Care During Insertion: Monitor and document
HR,BP and ECG during the procedure
Results from the focal narrowing of the large and
medium-sized coronary arteries due to deposition of atheromatous
plaque in the vessel wall
Stages of Development of Coronary Artery Disease
1.
2.
3.
CVP is a measurement of:
- cardiac efficiency
- blood volume
- peripheral resistance
Right ventricular pressure a catheter is passed from a
cutdown in the antecubital, subclavian jugular or basilica
vein to the right atrium and attached to a prescribed
manometer or tranducer.
NORMAL CVP is 2 -8 cm h20 or 2-6 mm Hg
Decrease indicates dec. circulating volume, increase
indicates inc. blood volume or right heart beat failure.
To Measure: patient should be flat with zero point of
manometer at the same level of the RA which
corresponds to the mid-axillary line of the patient or
approx. 5 cm below the sternum.
Fluctuations follow patients respiratory function and will
fall on inspiration and rise on expiration due to changes
in intrapulmonary pressure. Reading should be obtained
at the highest point of fluctuation.
Myocardial Injury: Atherosclerosis
Myocardial Ischemia: Angina Pectoris
Myocardial Necrosis: Myocardial Infarction
I. ATHEROSCLEROSIS
ATHEROSCLEROSIS
ARTERIOSCLEROSIS
Narrowing of artery
Lipid or fat deposits
Tunica intima
Hardening of artery
Calcium and protein
deposits
Tunica media
A. PRESDISPOSING FACTORS
1. Sex: male
2. Race: black
3. Smoking
4. Obesity
5. Hyperlipidemia
6. Sedentary lifestyle
7. Diabetes Mellitus
8. Hypothyroidism
9. Diet: increased saturated fats
10. Type A personality
2. Pulmonary Artery Pressure ( PAP) Monitoring
Appropriate for critically ill clients requiring more
accurate assessments of the left heart pressure
Swan-Ganz Catheter / Pulmonary Artery Catheter is use
B. SIGNS AND SYMPTOMS
1. Chest pain
2. Dyspnea
3. Tachycardia
4. Palpitations
5. Diaphoresis
C. TREATMENT
Percutaneous Transluminal Coronary Angioplasty and
Intravascular Stenting
Mechanical dilation of the coronary vessel wall by
compresing the atheromatous plaque.
It is recommended for clients with single-vessel
coronary artery disease.
Medical and Surgical Nursing
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
Prosthetic intravascular cylindric stent maintain
good luminal geometry after ballon deflation and
withdrawal.
Intravascular stenting is done to prevent restenosis
after PTCA
Nursing Management:
Nitroglycerine is the drug of choice for relief of pain
from acute ischemic attacks
Instruct to avoid over fatigue
Plan regular activity program
For Saphenous Vein Site:
Wear support stocking 4-6 week postop
Apply pressure dressing or sand bag on the site
Keep leg elevated when sitting
3 Complications of CABG
1. Pneumonia: encourage to perform deep breathing,
coughing exercise and use of incentive spirometer
2. Shock
3. Thrombophlebitis
II. ANGINA PECTORIS
Transient paroxysmal chest pain produced by insufficient
blood flow to the myocardium resulting to myocardial
ischemia
Clinical syndrome characterized by paroxysmal chest
pain that is usually relieved by rest or nitroglycerine due
to temporary myocardial ischemia
Types of Angina Pectoris
Coronary Arterial Bypass Graft Surgery
Stable Angina: pain less than 15 minutes, recurrence is less
frequent.
Unstable Angina : pain is more than 15 mins.,but not less
than 30 minutes, recurrence is more frequent and the
intensity of pain increases.
Variant Angina ( Prinzmetals Angina ): Chest pain is on
longer duration and may occur at rest. Result from coronary
vasospasm.
Angina Decubitus: paroxysmal chest pain that occur when
the client sits or stand.
A.
PRESDISPOSING FACTORS
1. Sex: male
2. Race: black
3. Smoking
4. Obesity
5. Hyperlipidemia
6. Sedentary lifestyle
7. Diabetes Mellitus
8. Hypertension
9. CAD: Atherosclerosis
10. Thromboangiitis Obliterans
11. Severe Anemia
12. Aortic Insufficiency: heart valve that fails to open &
close efficiently
13. Hypothyroidism
14. Diet: increased saturated fats
15. Type A personality
B.
PRESIPITATING FACTORS
4 Es of Angina Pectoris
1. Excessive physical exertion: heavy exercises, sexual
activity
2. Exposure to cold environment: vasoconstriction
3. Extreme emotional response: fear, anxiety,
excitement, strong emotions
4. Excessive intake of foods or heavy meal
C.
SIGNS AND SYMPTOMS
1. Levines Sign: initial sign that shows the hand
clutching the chest
2. Chest pain: characterized by sharp stabbing pain
located at sub sterna usually radiates from neck,
back, arms, shoulder and jaw muscles usually
relieved by rest or taking nitroglycerine(NTG)
3. Dyspnea
4. Tachycardia
5. Palpitations
6. Diaphoresis
Greater and lesser saphenous veins are commonly used for
bypass graft procedures
Objectives of CABG
1. Revascularize myocardium
2. To prevent angina
3. Increase survival rate
4. Done to single occluded vessels
5. If there is 2 or more occluded blood vessels CABG is
done
Medical and Surgical Nursing
10
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
D.
E.
F.
DIAGNOSTIC PROCEDURE
1. History taking and physical exam
2. ECG: may reveals ST segment depression & T wave
inversion during chest pain
3. Stress test / treadmill test: reveal abnormal ECG
during exercise
4. Increase serum lipid levels
5. Serum cholesterol & uric acid is increased
C.
MEDICAL MANAGEMENT
1. Drug Therapy: if cholesterol is elevated
Nitrates: Nitroglycerine (NTG)
Beta-adrenergic blocking agent: Propanolol
Calcium-blocking agent: nefedipine
Ace Inhibitor: Enapril
2. Modification of diet & other risk factors
3. Surgery: Coronary artery bypass surgery
4. Percutaneuos Transluminal Coronary Angioplasty
(PTCA)
4.
5.
6.
7.
8.
NURSING INTERVENTIONS
1. Enforce complete bed rest
2. Give prompt pain relievers with nitrates or narcotic
analgesic as ordered
3. Administer medications as ordered:
A.
Nitroglycerine(NTG): when given in small
doses will act as venodilator, but in large doses
will act as vasodilator
Give 1st dose of NTG: sublingual 3-5
minutes
Give 2nd dose of NTG: if pain persist after
giving 1st dose with interval of 3-5
minutes
Give 3rd& last dose of NTG: if pain still
persist at 3-5 minutes interval
9.
NTG Tablets(sublingual)
Keep the drug in a dry place, avoid
moisture and exposure to sunlight as it
may inactivate the drug
Change stock every 6 months
Offer sips of water before giving
sublingual nitrates, dryness of mouth may
inhibit drug absoprtion
Relax for 15 minutes after taking a tablet:
to prevent dizziness
Monitor side effects: orthostatic
hypotension, flushed face. Transient
headache & dizziness: frequent side effect
Instruct the client to rise slowly from
sitting position
Assist or supervise in ambulation
Administer oxygen inhalation
Place client on semi-to high fowlers position
Monitor strictly V/S, I&O, status of
cardiopulmonary fuction & ECG tracing
Provide decrease saturated fats sodium and caffeine
Provide client health teachings and discharge
planning
Avoidance of 4 Es
Prevent complication (myocardial infarction)
Instruct client to take medication before
indulging into physical exertion to achieve the
maximum therapeutic effect of drug
Reduce stress & anxiety: relaxation techniques
& guided imagery
Avoid overexertion & smoking
Avoid extremes of temperature
Dress warmly in cold weather
Participate in regular exercise program
Space exercise periods & allow for rest periods
The importance of follow up care
Instruct the client to notify the physician
immediately if pain occurs & persists despite rest &
medication administration
Death of myocardial cells from inadequate oxygenation,
often caused by sudden complete blockage of a coronary
artery
Characterized by localized formation of necrosis (tissue
destruction) with subsequent healing by scar formation &
fibrosis
Heart attack
Terminal stage of coronary artery disease characterized
by malocclusion, necrosis & scarring.
Types of M.I
Transmural Myocardial Infarction: most dangerous type
characterized by occlusion of both right and left coronary
artery
Subendocardial Myocardial Infarction: characterized by
occlusion of either right or left coronary artery
The Most Critical Period Following Diagnosis of
Myocardial Infarction
6-8 hours because majority of death occurs due to
arrhythmia leading to premature ventricular contractions
(PVC)
Beta-blockers: decreases myocardial oxygen
demand by decreasing heart rate, cardiac output
and BP
Propanolol
Metropolol
Pindolol
Atenolol
Assess PR, withhold if dec.PR
Administer with food ( prevent GI upset )
Medical and Surgical Nursing
Calcium Channel Blockers: relaxes smooth
cardiac muscle, reduces coronary vasospasm
Amlodipine ( norvasc )
Nifedipine ( calcibloc )
Diltiazem ( cardizem )
Assess HR and BP
Adminester 1 hour before meal and 2 hours
after meal ( foods delay absorption )
III. MYOCARDIAL INFARCTION
NTG Nitrol or Transdermal patch
Nitropatch is applied once a day, usually
in the morning.
Avoid placing near hairy areas as it may
decrease drug absorption
Avoid rotating transdermal patches as it
may decrease drug absorption
Avoid placing near microwave ovens or
during defibrillation as it may lead to
burns (most important thing to remember)
B.
Propanolol: not given to COPD cases: it causes
bronchospasm and DM cases: it cause
hypoglycemia
Side Effects: Nausea and vomiting, mental
depression and fatigue
A.
11
PREDISPOSING FACTORS
1. Sex: male
2. Race: black
3. Smoking
4. Obesity
5. CAD: Atherosclerotic
6. Thrombus Formation
7. Genetic Predisposition
8. Hyperlipidemia
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
9.
10.
11.
12.
13.
B.
C.
2.
3.
4.
5.
6.
SIGNS AND SYMPTOMS
1. Chest pain
Excruciating visceral, viselike pain with sudden
onset located at substernal& rarely in
precordial
Usually radiates from neck, back, shoulder,
arms, jaw & abdominal muscles (abdominal
ischemia): severe crushing
Not usually relieved by rest or by
nitroglycerine
2. N/V
3. Dyspnea
4. Increase in blood pressure & pulse, with gradual
drop in blood pressure (initial sign)
5. Hyperthermia: elevated temp
6. Skin: cool, clammy, ashen
7. Mild restlessness & apprehension
8. Occasional findings:
Pericardial friction rub
Split S1& S2
Rales or Crackles upon auscultation
S4 or atrial gallop
7.
8.
9.
10.
11.
12.
13.
DIAGNOSTIC PROCEDURED
1. Cardiac Enzymes
CPK-MB: elevated
Creatinine phosphokinase(CPK):elevated
Heart only, 12 24 hours
Lactic acid dehydrogenase(LDH): is increased
Serum glutamic pyruvate transaminase(SGPT):
is increased
Serum glutamic oxal-acetic
transaminase(SGOT): is increased
2. Troponin Test: is increased
3. ECG tracing reveals
ST segment elevation
T wave inversion
Widening of QRS complexes: indicates that
there is arrhythmia in MI
4.
5.
D.
Sedentary lifestyle
Diabetes Mellitus
Hypothyroidism
Diet: increased saturated fats
Type A personality
14. Provide client health teaching & discharge planning
concerning:
a. Effects of MI healing process & treatment regimen
b. Medication regimen including time name purpose,
schedule, dosage, side effects
c. Dietary restrictions: low Na, low cholesterol,
avoidance of caffeine
d. Encourage client to take 20 30 cc/week of wine,
whisky and brandy:to induce vasodilation
e. Avoidance of modifiable risk factors
f. Prevent Complication
Arrhythmia: caused by premature ventricular
contraction
Cardiogenic shock: late sign is oliguria
Left Congestive Heart Failure
Thrombophlebitis: homans sign
Stroke / CVA
Dresslers Syndrome(Post MI Syndrome):client
is resistant to pharmacological agents:
administer 150,000-450,000 units of
streptokinase as ordered
g. Importance of participation in a progressive activity
program
h. Resumption of ADL particularly sexual intercourse:
is 4-6 weeks post cardiac rehab, post CABG &
instruct to:
Serum Cholesterol & uric acid: are both increased
CBC: increased WBC
NURSING INTERVENTIONS
Goal: Decrease myocardial oxygen demand
1.
Decrease myocardial workload (rest heart)
Establish a patent IV line
Administer narcotic analgesic as ordered: Morphine
Sulfate IV: provide pain relief(given IV because
after an infarction there is poor peripheral perfusion
& because serum enzyme would be affected by IM
injection as ordered)
Side Effects: Respiratory Depression
Antidote: Naloxone (Narcan)
Side Effects of Naloxone Toxicity: is tremors
Medical and Surgical Nursing
Administer oxygen low flow 2-3 L / min: to prevent
respiratory arrest or dyspnea & prevent arrhythmias
Enforce CBR in semi-fowlers position without bathroom
privileges(use bedside commode): to decrease cardiac
workload
Instruct client to avoid forms of valsalva maneuver
Place client on semi fowlers position
Monitor strictly V/S, I&O, ECG tracing & hemodynamic
procedures
Perform complete lung / cardiovascular assessment
Monitor urinary output & report output of less than 30 ml
/ hr: indicates decrease cardiac output
Provide a full liquid diet with gradual increase to soft diet:
low in saturated fats, Na & caffeine
Maintain quiet environment
Administer stool softeners as ordered:to facilitate bowel
evacuation & prevent straining
Relieve anxiety associated with coronary care
unit(CCU)environment
Administer medication as ordered:
a. Vasodilators:Nitroglycirine (NTG), Isosorbide
Dinitrate, Isodil (ISD): sublingual
b. Anti Arrythmic Agents: Lidocaine (Xylocane),
Brithylium
Side Effects: confusion and dizziness
c. Beta-blockers: Propanolol (Inderal)
d. ACE Inhibitors: Captopril (Enalapril)
e. Calcium Antagonist: Nefedipine
f. Thrombolytics / Fibrinolytic Agents: Streptokinase,
Urokinase, Tissue Plasminogen Activating Factor
(TIPAF)
Side Effects:allergic reaction, urticaria, pruritus
Nursing Intervention: Monitor for bleeding
time
g. Anti Coagulant
Heparin
Antidote: Protamine Sulfate
Nursing Intervention: Check for Partial
Thrombin Time (PTT)
Caumadin(Warfarin)
Antidote:Vitamin K
Nursing Intervention: Check for
Prothrombin Time (PT)
h. Anti Platelet: PASA (Aspirin): Anti thrombotic
effect
Side Effects:Tinnitus, Heartburn, Indigestion /
Dyspepsia
Contraindication:Dengue, Peptic Ulcer Disease,
Unknown cause of headache
12
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
i.
j.
k.
Make sex as an appetizer rather than dessert
Instruct client to assume a non weight bearing
position
Client can resume sexual intercourse: if can
climb or use the staircase
Need to report the ff s/sx:
Increased persistent chest pain
Dyspnea
Weakness
Fatigue
Persistent palpitation
Light headedness
Enrollment of client in a cardiac rehabilitation
program
Strict compliance to mediation & importance of
follow up care
Aminophylline to reduce
bronchospasm caused by severe
congestion.
Vasodilators to reduce venous return
Diuretics to decrease circulating
volume
V. PERICARDITIS / DRESSLERS SYNDROME
Is the inflammation of the pericardium which occurs
approximately 1 6 weeks after AMI.
Results as an antigen antibody response. The necrotic
tissues play the role of an antigen, which trigger antibody
formation. Inflammatory process follows.
Constrictive Pericarditis is a condition in which a chronic
inflammatory thickening of the pericardium compresses
the heart so that it is unable to fill normally during
diastole.
IV. CARDIOGENIC SHOCK ( POWER/PUMP FAILURE )
A.
SIGNS AND SYMPTOMS
1. Pain in the anterior chest, aggravated by coughing,
yawning, swallowing, twisting and turning the torso,
relieved by upright, leaning forward position.
2. Pericardial friction rub scratchy, grating or
cracking sound
3. Dyspnea
4. Fever, sweating, chills
5. Joints pains
6. Arrhythmias
B.
NURSING INTERVENTIONS
Is a shock state which result from profound left
ventricular failure usually from massive MI.
It result to low cardiac output, thereby systemic
hypoperfusion.
A.
B.
C.
SIGNS AND SYMPTOMS
1. Decrease systolic BP
2. Oliguria
3. Cold, clammy skin
4. Weak pulse
5. Cyanosis
6. Mental lethargy
7. Confusion
1.
2.
3.
MEDICAL MANAGEMENT
1. Counterpulsation ( mechanical cardiac assistance /
diastolic augmentation )
Involves introduction of the intra aortic
balloon catheter via the femoral artery
Intra Aortic Balloon Pump augments
diastole, resulting in increased perfusion
of the coronary arteries and the
myocardium and a decrease in left
ventricular workload.
The balloon is inflated during diastole, it
is deflated during sytole.
Indications:
Cardiogenic shock
AMI
Unstable Angina
Open heart surgery
4.
5.
VI. CARDIAC TAMPONADE
Also known as pericardial tamponade, is an emergency
condition in which fluid accumulates in the pericardium
(the sac in which the heart is enclosed).
If the fluid significantly elevates the pressure on the heart
it will prevent the heart's ventricles from filling properly.
This in turn leads to a low stroke volume.
The end result is ineffective pumping of blood, shock,
and often death.
NURSING INTERVENTIONS
1.
2.
3.
4.
5.
6.
7.
Perform hemodynamic monitoring
Administer oxygen therapy
Correct hypovolemia. Administer IV fluids as
ordered
Pharmacology:
a. Vasodilators: Nitroglycerine
b. Inotropic agents:Digitalis, Dopamine
c. Diuretics : Furosemide
d. Sodium Bicarbonate, Relieve lactic acidosis
Monitor hourly urine output, LOC and arrhythmias
Provide psychosocial support
Decrease pulmonary edema
a. Auscultate lung fields for crackles and wheezes
b. Note for dyspnea, cough , hemoptysis and
orthopnea
c. Monitor ABG for hypoxia and metabolic
acidosis
d. Place in fowlers position to reduce venous
return
e. Administer during therapy as ordered:
Morphine sulfate to reduce venous
return.
Medical and Surgical Nursing
Elevate head of bed, place pillow on the overbed
table so that the patient can lean on it.
Bed rest
Administer prescribed pharmacotherapy.
a. ASA to suppress inflammatory process
b. Corticosteriods for more severe symptoms
Assist in pericardiocentesis if cardiac tamponade is
present.
Pericardiocentesis is aspiration of blood or fluid
from pericardial sac.
13
A.
PREDISPOSING FACTORS
1. Chest trauma ( blunt or penetrating )
2. Myocardial ruptured
3. Cancer
4. Pericarditis
5. Cardiac surgery ( first 24 48 hours )
6. Thrombolytic therapy
B.
SIGNS AND SYMPTOMS
1. Becks Triad
Hypotension
Jugular venous distension
Muffled heart sound
2. Pulsus paradoxus ( drop of at least 10 mmHg in
arterial BP on inspiration )
3. Tachycardia
4. Breathlessness
5. Decrease in LOC
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
C.
NURSING INTERVENTIONS
3.
1.
2.
4.
5.
3.
4.
5.
6.
Administer oxygen
Elevate head of bed, place pillow on the overbed
table so that the patient can lean on it.
Bed rest
Administer prescribed pharmacotherapy.
c. ASA to suppress inflammatory process
d. Corticosteriods for more severe symptoms
Assist in pericardiocentesis and thoracotomy
Pericardiocentesis is aspiration of blood or fluid
from pericardial sac.
B.
SIGNS AND SYMPTOMS (Venous congestion)
1. Jugular vein distention
2. Pitting edema
3. Ascites
4. Weight gain
5. Hepatosplenomegaly
6. Jaundice
7. Pruritus/ urticaria
8. Esophageal varices
9. Anorexia
10. Generalized body malaise
C.
DIAGNOSTICS
1. CXR cardiomegaly
2. CVP measures pressure in right atrium; N = 410cc H2O
During CVP: trendelenburg to prevent
pulmo embolism and to promote ventricular
filling
Flat on bed post CVP, check CVP readings
Hypovolemia fluid challenge
Hypervolemia diuretics (loop)
3. Echocardiography reveals enlarged heart chamber
Muffled heart sounds cardiomyopathy
Cyanotic heart diseases
TOF tet spells cyanosis with
hypoxemia
Tricuspid valve stenosis
Transposition of aorta
Acyanotic
PDA machine-like murmur
DOC: indomethacin SE: corneal
cloudiness
4. Liver enzymes
SGPT up
SGOT up
D.
NURSING MANAGEMENT
CONGESTIVE HEART FAILURE
Inability of the heart to pump blood towards systemic
circulation
I.
LEFT-SIDED HEART FAILURE
A.
PREDISPOSING FACTORS
1. 90% - Mitral valve stenosis
RHD
Inflammation of mitral valve
Anti-streptolysin O titer (ASO) 300 todd
units
Penicillin, PASA, steroids
Aging
2. MI
3. IHD
4. HPN
5. Aortic valve stenosis
B.
SIGNS AND SYMPTOMS
1. Pulmonary edema/congestion
Dyspnea, PND (awakening at night d/t
difficulty in breathing), 2-3 pillow orthopnea
Productive cough (blood tinged)
Rales/crackles
Bronchial wheezing
Frothy salivation
2. Pulsus alternans (A unique pattern during which the
amplitude of the pulse changes or alternates in size
with a stable heart rhythm.)This is common in
severe left ventricular dysfunction.)
3. Anorexia and general body malaise
4. PMI displaced laterally, cardiomegaly
5. S3 (ventricular gallop)
C.
Goal: increase myocardial contraction increase CO;
Normal CO is 3-6L/min; N stroke volume is 60-70ml/h2o
1.
DIAGNOSTICS
1. CXR cardiomegaly
2. PAP pulmonary arterial pressure
Measures pressure in right ventricle
Reveals cardiac status
3. PCWP pulmonary capillary wedge pressure
Measures end-systolic and end-diastolic
pressure (elevated)
Done through cardiac catheterization (SwanGanz)
4. Echocardiograph reveals enlarged heart chamber
5. ABG analysis reveals elevated PCO2 and decreased
PO2 (respiratory acidosis) hypoxemia and
cyanosis
Tracheostomy for severe respiratory distress and laryngospasm
performed at bedside within 10-15 minutes
CVP reveals fluid status; Normal = 4-10cm H2o; right atrium
PAP cardiac status; left atrium
ALLENS test collateral circulation
Cardiac Tamponade: pulsus paradoxus, muffled heart sounds, HPN
2.
3.
4.
5.
6.
7.
8.
II. RIGHT SIDED HEART FAILURE
A.
PREDISPOSING FACTORS
1. Tricuspid valve stenosis
2. COPD
Medical and Surgical Nursing
Pulmonary embolism (char by chest pain and
dyspnea)
Pulmonic stenosis
Left sided heart failure
14
Administer medications as ordered
Cardiac glycosides
Digoxin (N=.5-1.5, tox=2)
Tox: Anorexia, N&V; A: Digibind
Digitoxin given if (+) ARF; metabolized
in liver and not in kidneys
Loop diuretics
Lasix IV push, mornings
Bronchodilators
Aminophylline (theophylline)
Tachycardia, palpitations
CNS hyperactivity, agitation
Narcotic analgesics
Morphine sulfate induces vasodilation
Vasodilators
NTG and ISDN
Anti-arrhythmic agents
Lidocaine (SE: dizziness and
confusion)
Bretyllium
YOU DONT GIVE BETA-BLOCKERS TO
THESE PATIENTS
Administer O2 inhalation at 3-4 L/minute via NC as
ordered high flow
High fowlers, 2-3 Pillows
Restrict Na and fluids
Monitor strictly VS and IO and Breath Sounds
Weigh pt daily and assess for pitting edema
abdominal girth daily and notify MD
provide meticulous skin care
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
9.
provide a dietary intake which is low in saturated
fats and caffeine
10. Institute bloodless phlebotomy
ROTATING TOURNIQUET
Rotated clockwise every 15 minutes to
promote a decrease in venous return
11. Health teaching and discharge planning
Prevent complications : Arrhythmia, Shock,
Thrombophlebitis, MI, Cor pulmonale RV
hypertrophy
Regular adherence to medications
Diet modifications
Importance of ffup care
B.
RISK FACTORS
1. Family history
2. Age
3. High salt intake
4. Low potassium intake
5. Obesity
6. Excess alcohol consumption
7. Smoking
8. Stress
C.
SIGNS AND SYMPTOMS
1. Headache
2. Epistaxis
3. Dizziness
4. Tinnitus
5. Unsteadiness
6. Blurred vision
7. Depression
8. Nocturia
9. Retinopathy
D.
TREATMENT STRATEGIES
HYPERTENSION
Is an abnormal elevation of Bp, systolic pressure above
140 mmHg and or diastolic pressure above 90mmHg at
least two readings
WHO: BP >160/95 mmHg
AHA:
BP >140/90 mmHg
In hypertension, vasoconstriction vasospasm
increases PVR decrease blood flow to the organ.
Target Organs:
Heart : MI, CHF, Dysrhythmias
Eyes: blurred / impaired vision, retinopathy,
cataract.
Brain: CVA, encephalopathy
Kidneys : renal insufficiency, RF
Peripheral Bloods Vessels aneurysm,
gangrene
Non-pharmacologic therapy
1. Low salt diet.
2. Weight reduction.
3. Exercise.
4. Cessation of smoking.
5. Decreased alcohol consumption.
6. Psychological methods: Relaxation / meditation.
7. Dietary decrease in saturated fat.
Drug therapy
Stepped Care
o Progressive addition of drugs to a regimen,
starting with one, usually a diuretic, and adding,
in a stepwise fashion, a sympatholytic,
vasodilator, and sometimes an ACE inhibitor.
Monotherapy
o Advantageous because of its simplicity, better
patient compliance, and relatively low
incidence of toxicity.
CLASSIFICATION OF BP FOR ADULTS 18 YRS AND
OLDER (PHIL. SOCIETY OF HPN)
Optimal
o <120 mmHg / <80 mmHg
Recheck in 2 years.
Normal
o 120-129 mmHg / 80-84 mmHg
Recheck in 2 years.
High normal
o 130-139 mmHg / 85-89 mmHg
Recheck in 1 year.
Stage 1 (mild) HPN
o 140-159 mmHg / 90-99 mmHg
Confirm in 2 months.
Stage 2 (moderate) HPN
o 160-179 mmHg / 100-109 mmHg
Evaluate within a month.
Stage 3 (severe) HPN
o 180-209 mmHg / 110-119mmHg
Evaluate
within a
week.
Stage 4 (very severe) HPN
o 210 mmHg / >/=120 mmHg Evaluate
A.
CATEGORIES OF
ANTI-HYPERTENSIVE DRUGS
Drugs that alter sodium and water balance Diuretics.
Loop diuretics
Thiazides
Spironolactone and Triamterene
Drugs that alter sympathetic nervous system function
Sympatholytic drugs.
Centrally-acting sympatholytics
Clonidine
Guanabenz
Guanfacine
Methyldopa
Peripherally-acting sympatholytics
Guanadrel
Guanethidine
Reserpine
a-blockers
Doxazosin
Prazosin
b-blockers
Acebutolol
- Labetalol
Atenolol
- Metoprolol
Betaxolol
- Nadolol
Bisoprolol
- Penbutolol
Carteolol
- Pindolol
Carvedilol
- Propranolol
Esmolol
- Timolol
CLASSIFICATION
Essential / Idiophatic / Primary HPN, accounts
for 90 95% of all cases of HPN, cause is
unknown
Secondary HPN, due to known causes ( Renal
failure, Hypertension )
Malignant Hypertension, is severe, rapidly
progressive elevation in BP that causes rapid onset
of end organ complication
Labile HPN, intermittently elevated BP
Resistant HPN, does not respond to usual
treatment
White Coat HPN, elevation of B only during
clinic or hospital visits
Medical and Surgical Nursing
Hypertensive Crisis, situation that requires
immediate blood pressure lowering 240mmHg /
120 mmHg
15
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
Vasodilators
Direct vasodilators
Diazoxide
Minoxidil
Fenoldopam
Calcium channel blockers
Amlodipine
Diltiazem
Felodipine
Isradipine
Manidipine
Lacidipine
Lercanidipine
- Hydralazine
- Nitroprusside
- Nifedipine
- Nimodipine
- Nisoldipine
- Nitrendipine
- Nicardipine
- Verapamil
- Gallopamil
AGENTS THAT BLOCK THE PRODUCTION OR
ACTION OF ANGIOTENSIN
ACE inhibitors
Benazepril
- Moexipril
Captopril
- Quinapril
Enalapril
- Perindopril
Fosinopril
- Ramipril
Lisinopril
- Trandolapril
AT1-receptor blockers
Irbesartan
- Losartan
Telmisartan
- Valsartan
Candesartan
- Eprosartan
Olmesartan
DRUGS FOR HYPERTENSIVE EMERGENCIES OR
CRISES
Trimethaphan
o
1 mg/ml IV infusion; titrate;
instantaneous onset
Sodium nitroprusside
o 5-10 mg/L IV infusion; titrate;
instantaneous onset
Diazoxide
o 300-600 mg Rapid IV push;
instantaneous onset
Nifedipine
o 10-20 mg Sublingual or chewed;
onset within 5-30 min.
Labetalol
o 20-80 mg IV at 10-minute intervals (max.dose:
300mg); immediate onset
MECHANISMS OF DRUG ACTION
PRINCIPLES OF DRUG THERAPY
Monotherapy is generally reserved for mild to moderate
HPN; it has gained popularity because of its simplicity,
fewer side effects, and improved patient compliance.
More severe HPN may require treatment with several
drugs that are selected to minimize adverse effects of
combined regimen.
Treatment is initiated with any of 4 drugs depending on
individual patient: Diuretic, b-blocker, ACEI, and a Cachannel blocker; if BP is inadequately controlled, a 2nddrug is then added.
HPN may co-exist with other disease that may be
aggravated by some of the anti-HPN agents.
Lack of patient compliance is the most common reason
for failure of anti-HPN therapy; it is important to enhance
compliance by carefully selecting a drug regimen that
minimizes adverse effects.
Therapy is directed at preventing disease that may occur
in the future, rather than in relieving present discomfort
of the patient.
Medical and Surgical Nursing
16
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
E.
NURSING INTERVNTIONS
1. Patient Teaching and Counselling
Teaching about HPN and its risk factors
Stress therapy
Low NA and low saturated fat
Avoid stimulants ( caffeine, alcohol, smoking )
Regular pattern of exercise
Weight reduction if obese
2. Teaching about medication
The most common side effects of diuretics are
potassium depletion and orthostatic
hypotension.
The most common side effect of the different
antihypertensive drugs is orthostatic
hypotension.
Take anti hypertensive medications at regular
basis
Assume sitting or lying position for few
minutes
Avoid very warm bath
Avoid prolonged sitting and standing
Avoid alcoholic beverages
Avoid tyramine rich foods ( proteins ) as
follows: ( this may cause hypertensive crisis )
Aged cheese
Liver
Beer
Wine
Chocolate
Pickles
Sausages
Soy sauce
3. Preventing Non-compliance
Inform the client that absence of symptoms
does not indicate control of BP
Advise the client against abrupt withdrawal of
medication, rebound hypertension may occur.
Device ways to facilitate remembering of
taking medications
D.
MEDICAL / SURGICAL MANAGEMENT
1. Hypertensive Medication
2. Surgery if aneurysm is greater than 4 cm
Teflon graft
Dacron graft
Gortex graft
E.
NURSING INTERVENTIONS
1. Monitor the following
VS
Hemodynamic measurements
Urine output
BUN and creatinine
Bowel sounds
Passage of flatus
Peripheral pulses
2. Promoting Fluid Volume
Check dressing for excessive drainage
Assess for abdominal pain or backpain
Assess Hgb and Hct values
PERIPHERAL VASCULAR DISORDERS
ANEURYSM
ARTERIAL ULCERS
It is the localized, irreversible dilatation of an artery
secondary to an alteration in the integrity of its wall.
Most common type is AAA ( abdominal aortic aneurysm )
The most common cause is hypertension
A.
I.
CLASSIFICATIONS
Fusiform Aneurysm , involves outpouching of the
both side of the artery
Saccular Aneurysm , outpouching of only one side
of the artery.
Dissecting Aneurysm, involves separation or tear in
the tunica intima and tunica media
B.
RISK FACTOR
1. Age
2. Tobacco use
3. HPN
4. Atherosclerosis
5. Race
6. Gender
7. Family history
C.
SIGNS AND SYMPTOMS
1.
2.
3.
4.
5.
6.
A.
B.
C.
Pulsating mass over abdomen (AAA)
Presence of the bruit sound
Low back pain
Lower abdominal pain
Flank pain
Shock
Medical and Surgical Nursing
THROMBOANGITIS OBLITERANS ( Buergers Dse. )
acute inflammatory condition affecting the smaller and
medium sized arteries and veins of the lower extremities.
IDIOPATHIC
17
PREDISPOSING FACTORS
1. High risk group men 30 years old above
2. Chronic smoking
SIGNS AND SYMPTOMS Consistent to all arterial
diseases
1. Intermittent claudication leg pain upon strenuous
walking r/t temporary ischemia
2. Cold sensitivity and skin color changes
White/pallor bluish/cyanosis red/rubor
(+) especially post smoking
3. Decreased peripheral pulses volume particularly in
dorsalis pedis and posterior tibial
4. Trophic changes
5. Ulceration
6. Gangrene formation
DIAGNOSTICS
1. Oscillometry reveals a decrease in peripheral
pulse volume
2. Doppler UTZ decrease in blood flow to affected
extremity
3. Angiography site and extent of malocclusion
Abejo
Lecture Notes on Cardiovascular System
Prepared By: Mark Fredderick R Abejo R.N, MAN
D.
II.
NURSING MANAGEMENT
1. Encourage slow progressive physical activity
Walking 3-4x/day
Out of bed 3-4x/day
2. Medications as ordered
Analgesics
Vasodilators
Anticoagulants
3. Instruct patient to avoid smoking and exposure to
cold environment
4. Institute foot care management
Avoid barefoot walking
Straight nails
Lanolin cream for feet
(-) constricting clothes
5. Assist in surgery: BKA
A.
PREDISPOSING FACTORS
1. Hereditary
2. Congenital weakness of veins
3. Thrombophlebitis
4. Cardiac diseases
5. Pregnancy
6. Obesity
7. Prolonged immobility prolonged standing and
sitting
B.
SIGNS AND SYMPTOMS
1. Pain after prolonged standing
2. Dilated tortuous skin veins which are warm to touch
3. Heaviness in the legs
C.
DIAGNOSTICS
1. Venography
2. Trendelenburgs test reveals that veins distend
quickly < 35 seconds incompetent valves
D.
NURSING MANAGEMENT (consistent to all venous
ulcers)
1. Elevate legs above heart level increased venous
return (2-3 pillow elevation)
2. Measure circumference of leg to determine swelling
3. Anti-embolic stocking, full support panty hose
4. Medications as ordered analgesics
5. Assist in surgery
Vein stripping and ligation (more effective, no
recurrence)
Sclerotherapy
For spider-web varicosities
Cold solution injection
SE: thrombosis
REYNAULDS DISEASE characterized by acute episodes
of arterial spasms involving the digits of hands and fingers
II. THROMBOPHLEBITIS / DEEP VEIN THROMBOSIS
(DVT)
A.
B.
C.
D.
PREDISPOSING FACTORS
1. High risk group women 40 years old up
2. Smoking
3. Collagen diseases
SLE
RA
4. Direct hand trauma
Piano playing
Excessive typing (tsk tsk! Lagot!)
Carpal tunnel syndrome
Operating chainsaw (nyek!)
Writing (tsk tsk, kaya dapat may module eh!
Grr!)
SIGNS AND SYMPTOMS
1. Intermittent claudication
2. Cold sensitivity and skin color changes
White/pallor bluish/cyanosis red/rubor
(+) especially post smoking
3. Trophic changes
4. Ulceration
5. Gangrene formation
DIAGNOSTICS
1. Oscillometry reveals a decrease in peripheral
pulse volume
2. Angiography site and extent of malocclusion
NURSING MANAGEMENT
1. Administer medications as ordered
Analgesics
Vasodilators
2. Encourage pt to wear gloves
3. Instruct: avoid smoking and exposure to cold
environment
VENOUS ULCERS
I.
A.
PREDISPOSING FACTORS
1. Smoking
2. Obesity
3. Prolonged use of OCPs
4. Chronic anemia
5. Diet high in saturated fats
6. DM
7. CHF
8. MI
9. Post-cannulation (insertion of various catheters)
10. Post-surgical operation
11. Sedentary lifestyle
B.
SIGNS AND SYMPTOMS
1. Pain at the affected extremity
2. Presence of cyanosis
3. Dilated tortuous veins
4. (+) HOMANS pain on calf on dorsiflexion
C.
DIAGNOSTICS
1. Venography
2. Doppler UTZ
3. Angiography
D.
NURSING MANAGEMENT
1. Elevate the legs above heart level
2. Apply warm moist pack to relieve lymphatic
congestion
3. Measure circumference of leg muscles to determine
if it is swollen
4. Anti-embolic stockings
5. Administer medications as ordered
Analgesics
Anticoagulants heparin
6. Prevent complications
Pulmonary embolism
VARICOSE VEINS abnormal dilation of the veins of the
lower extremities d/t incompetent valves leading to increased
venous pooling and venostasis decreased venous return
Medical and Surgical Nursing
18
Abejo
You might also like
- Fluid and Electrolytes Study GuideDocument16 pagesFluid and Electrolytes Study GuideDianaNursing96% (28)
- Cardiovascular Physiology Concepts Klabu PDFDocument257 pagesCardiovascular Physiology Concepts Klabu PDFJer100% (5)
- Lehnes Pharmacotherapeutics For Advanced Practice Providers Ebook PDFDocument39 pagesLehnes Pharmacotherapeutics For Advanced Practice Providers Ebook PDFmarilyn.llamas494100% (39)
- Fundamentals of NursingDocument8 pagesFundamentals of NursingFreeNursingNotes92% (13)
- Test Bank CardioDocument16 pagesTest Bank CardioLudwigJayBarayuga86% (7)
- ECG Review Packet-1Document23 pagesECG Review Packet-1Tori RolandNo ratings yet
- Endocrine NursingDocument2 pagesEndocrine NursingUnclePorkchop94% (34)
- Handout Medical-Surgical Nursing Fluid and ElectrolyteDocument13 pagesHandout Medical-Surgical Nursing Fluid and ElectrolytePaul Christian P. Santos, RN100% (10)
- Med-Surg Nusing BulletsDocument65 pagesMed-Surg Nusing BulletsHarley C. Tan100% (1)
- Cardiovascular SystemDocument10 pagesCardiovascular Systemsurviving nursing school100% (2)
- Cardiac Drugs Study Guide CourseDocument19 pagesCardiac Drugs Study Guide CourseAmanda Brittain100% (6)
- Cardiac DrugsDocument5 pagesCardiac Drugseric100% (17)
- Respiratory Nursing #1Document19 pagesRespiratory Nursing #1shenric16100% (12)
- Genito UrinarysystemDocument7 pagesGenito Urinarysystemshenric16No ratings yet
- Fluid and ElectrolytesDocument13 pagesFluid and ElectrolytesHenry Philip93% (15)
- Gastrointestinal NursingDocument8 pagesGastrointestinal Nursingohsnapitslei90% (10)
- Mus Culo SkeletalDocument16 pagesMus Culo Skeletalshenric16100% (2)
- Medical Surgical Nursing 64 PagsDocument64 pagesMedical Surgical Nursing 64 Pagstanya nNo ratings yet
- Shock Comparison ChartDocument2 pagesShock Comparison Chartlinnaete88% (8)
- Cardiac Notes NursingDocument16 pagesCardiac Notes NursingYemaya8494% (17)
- MK Combined PDFDocument93 pagesMK Combined PDFAnkit ChoudharyNo ratings yet
- Medsurg Cardio Ana&PhysioDocument6 pagesMedsurg Cardio Ana&Physiorabsibala80% (10)
- Respiratory DisordersDocument15 pagesRespiratory Disordersmnlstr100% (5)
- Medicationpart1 110202192115 Phpapp02Document10 pagesMedicationpart1 110202192115 Phpapp02Jessamine Rochelle Reyes Esberto100% (1)
- Chapter (10) : Assessment of Cardiovascular SystemDocument10 pagesChapter (10) : Assessment of Cardiovascular SystemSandra GabasNo ratings yet
- Handout 5 CardioVascular System Overview PDFDocument7 pagesHandout 5 CardioVascular System Overview PDFGrape JuiceNo ratings yet
- Cardiac DrugsDocument10 pagesCardiac Drugssurviving nursing school100% (4)
- The GastroDocument25 pagesThe Gastroangel_maui100% (7)
- Anatomy & Physiology Cardiac SystemDocument1 pageAnatomy & Physiology Cardiac SystemTori RolandNo ratings yet
- Cardiovascular SystemDocument10 pagesCardiovascular Systemtheglobalnursing75% (4)
- 05 Cardiovascular System PhysiologyDocument34 pages05 Cardiovascular System PhysiologyKaye Alyssa EnriquezNo ratings yet
- Cardiovascular System Acronyms and MnemonicsDocument18 pagesCardiovascular System Acronyms and Mnemonicsdecsag06No ratings yet
- Med Surg Study GuideDocument98 pagesMed Surg Study Guideprogramgrabber100% (23)
- Head To Toe AssessmentDocument9 pagesHead To Toe AssessmentTori Roland0% (1)
- 313 - Disorders of Renal and Urinary SystemsDocument8 pages313 - Disorders of Renal and Urinary SystemsChrissy Mendoza100% (2)
- HematologyDocument10 pagesHematologyFranzes R. Herrera100% (4)
- Nursing Pharmacology Perfusion Study GuideDocument9 pagesNursing Pharmacology Perfusion Study GuideChelsea SmithNo ratings yet
- Endocrine NursingDocument2 pagesEndocrine Nursingsurviving nursing school100% (2)
- Chapter 14 Fluid and Electrolytes ChartsDocument7 pagesChapter 14 Fluid and Electrolytes ChartsBNA_RN100% (3)
- Cardiac MedsDocument7 pagesCardiac MedsMary Fair DelcidNo ratings yet
- Resp Lecture NotesDocument18 pagesResp Lecture Notessurviving nursing schoolNo ratings yet
- CARDIOLOGYDocument15 pagesCARDIOLOGYPatty RomeroNo ratings yet
- Medical Surgical Nursing Cardio Vascular System ClassDocument15 pagesMedical Surgical Nursing Cardio Vascular System Classvallal100% (2)
- Endocrine Disorders (Study Notes)Document11 pagesEndocrine Disorders (Study Notes)Danelle Harrison, RN90% (10)
- Med Surg: GI - Gastrointestinal: PathophysiologyDocument1 pageMed Surg: GI - Gastrointestinal: PathophysiologyTori RolandNo ratings yet
- Cardiovascular DrugsDocument6 pagesCardiovascular Drugslhayes123488% (16)
- Neuro Study GuideDocument7 pagesNeuro Study GuideNursingSchoolNotes100% (2)
- Musculoskeletal Note1Document34 pagesMusculoskeletal Note1FreeNursingNotes100% (4)
- Cardiac AssessmentDocument7 pagesCardiac AssessmentBryan Mae H. Degorio75% (4)
- 8 Heart Failure - Notes-DONE - PrintedDocument9 pages8 Heart Failure - Notes-DONE - PrintedKristin SmithNo ratings yet
- Heart Blocks: "The Heart Block Poem"Document18 pagesHeart Blocks: "The Heart Block Poem"Bijay Kumar Mahato100% (1)
- Adult III Cardiac Study GuideDocument15 pagesAdult III Cardiac Study GuideNursingSchoolNotes100% (6)
- 60 Item Exam On Cardiovascular DisordersDocument9 pages60 Item Exam On Cardiovascular DisordersAijem RyanNo ratings yet
- Cardiovascular I: CAD: Coronary Artery Disease (Most Common in US) Risk FactorsDocument4 pagesCardiovascular I: CAD: Coronary Artery Disease (Most Common in US) Risk FactorsJessica100% (1)
- Cardiac DrugsDocument4 pagesCardiac DrugsIbrahem Al100% (2)
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideFrom EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideNo ratings yet
- Cardionursing 110207023802 Phpapp01Document18 pagesCardionursing 110207023802 Phpapp01arvinnnnNo ratings yet
- Heart Anatomy: LocationDocument45 pagesHeart Anatomy: LocationZaira100% (1)
- Cardiac Anatomy and Physiology: Iris Ken R. Rico, OTRPDocument90 pagesCardiac Anatomy and Physiology: Iris Ken R. Rico, OTRPAndra HijratulNo ratings yet
- Cardiovascular System BSN 1Document16 pagesCardiovascular System BSN 1Arianne Jen GenotivaNo ratings yet
- NPTE CArdio NotesDocument27 pagesNPTE CArdio NotesAubrey Vale SagunNo ratings yet
- Health Assessment Conceptual OverviewDocument80 pagesHealth Assessment Conceptual OverviewLudwigJayBarayugaNo ratings yet
- Circulatory System DiseasesDocument4 pagesCirculatory System DiseasesLudwigJayBarayugaNo ratings yet
- Bullets Paediaterics ReviewDocument3 pagesBullets Paediaterics ReviewRavneetKalkatNo ratings yet
- Therapeutic CommunicationDocument13 pagesTherapeutic CommunicationLudwigJayBarayugaNo ratings yet
- Therapeutic CommunicationDocument13 pagesTherapeutic CommunicationLudwigJayBarayugaNo ratings yet
- Peripheral Cardiovascular SystemDocument9 pagesPeripheral Cardiovascular SystemLudwigJayBarayugaNo ratings yet
- Fluid and Electrolyte Balance, Nutrition and Metabolism and EndocrineDocument12 pagesFluid and Electrolyte Balance, Nutrition and Metabolism and EndocrineLudwigJayBarayugaNo ratings yet
- Training For The Female Athlete Children and Special PopulationDocument25 pagesTraining For The Female Athlete Children and Special PopulationAqsa ZaheerNo ratings yet
- 3 Preanestesic EvaluaciónDocument15 pages3 Preanestesic EvaluaciónManu BGNo ratings yet
- Cardiac Enzymes FinalDocument3 pagesCardiac Enzymes FinalRumelle ReyesNo ratings yet
- Kremil S Drug StudyDocument1 pageKremil S Drug StudyDivine LavaNo ratings yet
- RECOVER Guidelines CompressedDocument28 pagesRECOVER Guidelines Compressedkkfyc2020No ratings yet
- Physical Exam Final Written Exam Study Guide 2Document51 pagesPhysical Exam Final Written Exam Study Guide 2pelly3190100% (2)
- Treatment of Acute AppendicitisDocument17 pagesTreatment of Acute Appendicitiszamir90No ratings yet
- Quarter 1 Science 9 (Weeks 1-2) /50Document2 pagesQuarter 1 Science 9 (Weeks 1-2) /50MarkNo ratings yet
- Situs Colli: Tri Indah Winarni Dept of Anatomy Faculty of Medicine Diponegoro UniversityDocument51 pagesSitus Colli: Tri Indah Winarni Dept of Anatomy Faculty of Medicine Diponegoro UniversityLailatuz ZakiyahNo ratings yet
- Philippine Integrated Nurse Licensure ExaminationDocument96 pagesPhilippine Integrated Nurse Licensure Examinationmhiersalyn mirulNo ratings yet
- ST Segment ElevationsDocument114 pagesST Segment ElevationsMuruganandham RNo ratings yet
- Cardiovascular PhysiologyDocument42 pagesCardiovascular PhysiologyancillaagraynNo ratings yet
- CardiomyopathiesDocument13 pagesCardiomyopathiesNinna Isabel VictorioNo ratings yet
- The Top 20 Drugs by Worldwide Sales in 2020 - Fierce PharmaDocument50 pagesThe Top 20 Drugs by Worldwide Sales in 2020 - Fierce PharmaBonnie DebbarmaNo ratings yet
- How To Monitor Cardiovascular Function in Critical Illness in Resource-Limited SettingsDocument8 pagesHow To Monitor Cardiovascular Function in Critical Illness in Resource-Limited SettingsHendra DarmawanNo ratings yet
- DS (Calcium + Vit. D)Document6 pagesDS (Calcium + Vit. D)Mary April MendezNo ratings yet
- Anticoagulants DaniellewelschmeyerDocument30 pagesAnticoagulants Daniellewelschmeyersumanth gowdaNo ratings yet
- Anatomy of The Kidney and UreterDocument6 pagesAnatomy of The Kidney and UreterMario Ivan De la Cruz LaraNo ratings yet
- Indication For Arterial Blood Gas AnalysisDocument10 pagesIndication For Arterial Blood Gas AnalysisRohini RaiNo ratings yet
- Intracranial ArteriesDocument98 pagesIntracranial ArteriesAgnesthesiaNo ratings yet
- Level 2. How Do Cigarettes Affect The Body - Krishna SudhirDocument3 pagesLevel 2. How Do Cigarettes Affect The Body - Krishna SudhirELIBERTO FIGUEROA OMENo ratings yet
- Hematologic Disorders Intensive For Brilliant Post Test Answer KeyDocument4 pagesHematologic Disorders Intensive For Brilliant Post Test Answer Keymarlou agananNo ratings yet
- CVD NCD Risk Assessment FormDocument2 pagesCVD NCD Risk Assessment Formsmoothp3akNo ratings yet
- Mrcs Part A Essential Revision Notes Boo K 1Document22 pagesMrcs Part A Essential Revision Notes Boo K 1Fath Elrahman MohammedNo ratings yet
- Chest X-RayDocument39 pagesChest X-Rayendah cahya sufianyNo ratings yet
- Drug StudyDocument79 pagesDrug StudyShea Janson MercurioNo ratings yet
- Strokeaha 120 033033Document7 pagesStrokeaha 120 033033AudryaNo ratings yet