Professional Documents
Culture Documents
Genito Urinarysystem 120311072940 Phpapp02 PDF
Genito Urinarysystem 120311072940 Phpapp02 PDF
Uploaded by
zhai bambalanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Genito Urinarysystem 120311072940 Phpapp02 PDF
Genito Urinarysystem 120311072940 Phpapp02 PDF
Uploaded by
zhai bambalanCopyright:
Available Formats
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
B.
C.
D.
E.
MEDICAL AND SURGICAL NURSING
Genito-Urinary Tract Disorder
Lecturer: Mark Fredderick R. Abejo RN,MAN
________________________________________________
Structure
1. Renal pelvis
2. Renal colic
3. Renal medulla
Nephron glomerulus
Functions
1. Urine formation
2. Regulates BP
Urine Formation (Normal GFR: 125 ml of blood is
filtered in the glomerulus per minute)
1. Filtration
2. Tubular Reabsorption 124 ml of ultrafiltrates are
reabsorbed back into the blood
3. Tubular Secretion 1 ml excreted in the urine; of
total cardiac output is received by kidneys
II. Ureters 20-30 mm long serves as a passageway of urine
OVERVIEW OF THE STRUCTURE AND FUNCTION OF
THE GENITO-URINARY TRACT
-
Promotes excretion of nitrogenous waste products
Maintain fluid electrolytes and acid-base balance
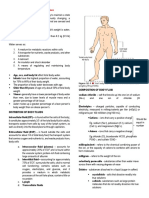
III. Bladder
A. Located behind the symphysis pubis
B. Made up of muscular and elastic tissues distensible
reservoir of urine
C. Max: 1, 200 -1,800 ml of urine
D. Initiates urination: 250-500 cc ml
E. Normal urine:
1. amber, aromatic, turbid/clear, pH 4-8
2. spec gravity: 1.015-1.030
3. WBC, CHON none
4. (-) E. coli
5. mucus threads few
6. (-) amorphous urates
IV. Urethra
A. Serves as a passageway for urine, vaginal/seminal fluids
B. Length
1. F: 3-5 cm or 1-1/2 inches
2. M: 20 cm or 8 inches
C. Catheter
1. Pedia: 8-10 fr
2. F: 12-14 fr
3. M: 16-18 fr
URINARY TRACT INFECTIONS
I.
I.
MS
Kidneys
A. Location a pair of bean shaped organs located
retroperitoneally (behind peritoneum) on either side of
the verbral column
CYSTITIS inflammation of bladder caused by bacterial
infection
A.
PREDISPOSING FACTORS
1. High risk: women
2. Microbial Invasion (E. Coli)
3. Increased estrogen levels, estrogen therapy
4. Sexual intercourse
Abejo
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
5.
6.
7.
8.
B.
S/SX
1. Urinary frequency and urgency
2. Flank pain
3. Fever, chills, anorexia, generalized body malaise
4. Dysuria burning upon urination
5. Hematuria
C.
DX
1. Urine culture and sensitivity
(+) E. Coli 90%
2. Urinalysis
Increased WBC
Increased CHON
Increased pus cells
D.
NSG MGMT
1. Forced fluids (2-3 L/d)
2. Provide warm sitz bath to promote comfort
3. Provide acid-ash diet: cranberries, grape juice,
plums
4.
5.
6.
MS
Urinary retention
Incontinence
Urinary obstruction
Poor perineal hygiene
Monitor for gross hematuria, color, odor of urine
Administer meds as ordered
Systemic antibiotics
Penicillins
Cephalosporins
(SE:
nephrotoxicity,
hepatotoxicity)
Tetracycline
(staining
of
teeth,
photosensitivity)
Sulfonamides
Co-trimoxazole (Bactrim)
Gantricin
Sulfisoxazole
Urinary antiseptics
Nitrofurantoin (Macrodantin)
Furadantoin
Urinary analgesics
Pyridium decreases pain, promotes
relaxation of sphincter
Discharge teaching
Importance of hydration
7.
Void after sexual intercourse
Instruct female client to:
Proper perineal hygiene
Front to back cleaning
Avoid tissue use
Bubble bath
(-) talcum powder, perfume
Prevent complications
Pyelonephritis
II. PYELONEPHRITIS acute or chronic inflammation of
renal pelvis leading to tubular destruction, intestinal abscesses
and renal failure
A.
PREDISPOSING FACTORS
1. Microbial invasion
E. coli
Streptococcus
2. Urinary retention/ stagnation
3. pregnancy
4. DM
5. Exposure to renal toxins/ use of nephrotoxic agents
6. Obesity
B.
S/SX
1. Acute Pyelonephritis
Urinary frequency and urgency
Costovertebral angle pain and tenderness
Fevers and chills, anorexia, general body
malaise
Burning upon urination
Dysuria, nocturia, hematuria
2. Chronic Pyelonephritis
Fatigue and/or weakness
Weight loss
Polyuria
Polydypsia
HPN
C.
DIAGNOSTICS
1. Urine CS: (+) cultured microorganisms (E.coli and
strep)
2. Urinalysis: elevated WBC, CHON, pus cells
3. Cystoscopic exam: (+) urinary obstruction
Abejo
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
D.
4.
5.
6.
NURSING MANAGEMENT
1. Provide CBR especially during acute attack
2. Forced fluids
3. Provide an acid ash in the diet
4. Provide warm sitz bath for comfort
5. Administer medications as ordered
Nitrofurantoin
SE: GIT irritation, give with food,
peripheral neuropathy, hemolytic anemia
(initial sx: fever), discoloration of teeth
Urinary analgesics
Pyridium
6. prevent complications
renal failure
7.
8.
III. NEPHROLITHIASIS/UROLITHIASIS formation of
stones elsewhere in the urinary tract
9.
Strain all urine using gauze pad
Warm sitz bath for comfort
Meds as ordered
Narcotic analgesics morphine
Allopurinol (zyloprim)
Provide dietary intake:
If (+) to ca stones: acid ash
If (+) to oxalate stones: alkaline ash (milk,
tea, vegetables)
If (+) to uric acid: avoid purine rich food
like anchovies, legumes, organ meat, nuts
Assist
Litholapoxy surgical removal of 2/3 stone
Nephrectomy removal of kidney
stagnation
Lithotripsy extracorporeal shockwave
No incision, early discharge
Too costly
Stones can recur
Post-op: strain urine
Prevent complications renal failure
IV. ACUTE RENAL FAILURE (ARF) sudden inability of the
kidneys to excrete nitrogenous waste products, leads to
azotemia
A.
MS
A.
TYPES OF STONES
1. calcium
2. oxalate
3. uric acid
B.
PREDISPOSING FACTORS
1. diet high in calcium and oxalate
2. hereditary (like gout)
3. hyperparathyroidism (Hypercalcemia)
4. obesity
5. sedentary lifestyle
C.
S/SX
1. Renal colic
2. Cool, moist skin
3. Burning upon urination
4. Dysuria, Nocturia
5. Hematuria
D.
DIAGNOSTICS
1. Urinalysis (+) RBC, WBC, Pus cells
2. KUB: reveal site or location of stones
3. Stone analysis: reveals composition of stone
4. Cystoscopic exam: urinary obstruction
5. IVP: reveals obstruction
E.
NURSING MANAGEMENT
1. Forced fluids to prevent further crystallization
2. Alternate warm and cold compress
3. Administer isotonic fluids as ordered
PREDISPOSING FACTORS
1. Pre-renal : involves decrease in GFR
(n=125ml/hr)
Hemorrhage
Shock
Chronic diarrhea (dehydration)
CHF
Hypotension
Septicemia
2. Intrarenal involves renal pathology
Pyelonephritis
DM
AGN
Acute tubular necrosis: common SE posthemolytic BT
3. Post-renal (+) mechanical obstruction
BPH
Nephro/urolithiasis
Tumor
Urinary strictures
Abejo
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
B.
STAGES
1.
2.
3.
V.
Oliguric phase passage of urine (1-2 weeks)
UO: <400 ml/cc
Hyperkalemia
Hypernatremia
Hyperphosphatemia
HYPOCALCEMIA
Hypermagnesemia
Metabolic acidosis
Elevated BUN, Crea
Diuretic Phase (2-3 weeks)
Increased passage of urine
Hyperkalemia
Hyponatremia
Metabolic acidosis
Convalescent phase (3-12 months)
Improvement in passage of urine
Characterized by complete diuresis
CHRONIC RENAL FAILURE (CRF) irreversible loss of
kidney function
A.
PREDISPOSING FACTORS
1. DM and HPN (common causes)
2. Recurrent pyelonephritis
3. Exposure to renal toxins
4. Tumor
B.
STAGES
1. Diminished renal reserve volume asymptomatic,
normal BUN and CREA
2. Renal insufficiency
3. End-stage renal disease (ESRD) presence of
oliguria, azotemia
C.
S/SX
1. Uro
Azotemia (elevated BUN and crea)
Oliguria
Nocturia
Hematuria
Dysuria
2. Neuro
Lethargy
Headache
Disorientation (initial sign of disequilibrium
syndrome) and confusion, restlessness
Memory impairment
Decreased LOC
3. Respi
Depressed or diminished cough reflex
Kussmauls respirations
4. Hema
Anemia
Leukopenia
Bleeding tendencies (thrombocytopenia)
All blood cells decreased
Increased susceptibility to infection
5. CV changes
Pulmo HPN
CHF
Pericarditis
6. GIT distress
7.
8.
9.
D.
NURSING MANAGEMENT
1. Enforce CBR
2. Admin oxygen inhalation as ordered
3. High CHO diet low CHON, fats, High vit and
minerals
4. Provide meticulous skin care
Wash with warm water
Soap irritates and dries skin
5. Meds as ordered
anti-HPN agents
Hydralazine (appresoline)
SE: orthostatic hypotension
NaHCO3
Kayexelate enema
Hematinics
Antibiotics
Supplementary vitamins and minerals
Phosphate binders
Calcium gluconate
6.
MS
Anorexia
N&V
Diarrhea and/or constipation
Stomatitis
Uremic breath
Integumentary
Pruritus
Uremic frost
Metabolic/Electrolyte imbalance
Hyperkalemia
Hyperphosphatemia
Metabolic acidosis
Endo
Gynecomastia
Hyperthyroidism
Assist in hemodialysis
Secure consent and explain procedure to client
Maintain strict aseptic technique
Obtain baseline data before and q30 during
procedure
VS
Wt
Blood exams secure all pre-procedure
I/O
Abejo
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
MS
Have client void pre-procedure
Inform pt about bleeding (blood is heparinized)
Monitor for signs of complications
(BEDSSH)
Bleeding
Embolism
DISEQUILIBRIUM SYNDROME
results from rapid loss of nitrogenous
waste products particularly UREA from
the brain
HPN
Disorientation initial sign
Nausea and vomiting
anorexia
Headache
Paresthesia, peripheral
Numbness
Septicemia
Shock
Hepatitis
Avoid BP taking, phlebotomy, IV meds at the
site of fistula, blood extraction to prevent
compression
Maintain patency of shunt/fistula:
Palpate for thrills, auscultate for bruits
Instruct that minimal bleeding is expected
since blood is heparinized
Avoid use vasodilators, sedatives, and
tranquilizers to prevent hypotension unless
ordered
Prepare at bedside bulldog clips to prevent
embolism
Auscultate for bruits and palpate for thrills
(if (+) patent)
PERITONEAL DIALYSIS
7.
Most
common
complication
is
PERITONITIS and shock
First sign: cloudy dialysate return
Most
common
dialysate:
INFERSOL
Infusion time: 10-20 minutes
Dwelling time: 30-45 minutes
What determines effectiveness of dialysis?
Weight of patient
Assist
in
surgical
TRANSPLANTATION
procedure:
KIDNEY
Meds: steroids, immunosuppressants,
lymphocyte globulin
Feared complication: rejection, characterized
by
hypertension,
headache,
dizziness,
decreased CBC
2 TYPES OF REJECTION
Acute 6 to 10 months
Chronic 5-10 years
1. Oliguria
2. Disorientation
3. Decreased LOC
Abejo
anti
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
MS
Abejo
Medical and Surgical Nursing
Genito-Urinary Tract
Prepared by: Mark Fredderick R. Abejo RN,MAN
MS
Abejo
You might also like
- 100 Item Comprehensive Exam With Answers and RationaleDocument21 pages100 Item Comprehensive Exam With Answers and RationaleAijem Ryan93% (15)
- Gastrointestinal DiseasesDocument11 pagesGastrointestinal DiseasesFreeNursingNotes100% (1)
- Fundamentals of NursingDocument8 pagesFundamentals of NursingFreeNursingNotes92% (13)
- Endocrine NursingDocument2 pagesEndocrine NursingUnclePorkchop94% (34)
- Med-Surg Nusing BulletsDocument65 pagesMed-Surg Nusing BulletsHarley C. Tan100% (1)
- Handout Medical-Surgical Nursing Fluid and ElectrolyteDocument13 pagesHandout Medical-Surgical Nursing Fluid and ElectrolytePaul Christian P. Santos, RN100% (10)
- Nclex Cheat SheetDocument9 pagesNclex Cheat Sheetsophia onuNo ratings yet
- DRRM MoaDocument3 pagesDRRM MoaErnan Baldomero67% (3)
- D&D 3.5 Forgotten Realms - Waterdeep MapDocument1 pageD&D 3.5 Forgotten Realms - Waterdeep MapMarcel Morton100% (5)
- Gastrointestinal NursingDocument8 pagesGastrointestinal Nursingohsnapitslei90% (10)
- Respiratory Nursing #1Document19 pagesRespiratory Nursing #1shenric16100% (12)
- Mus Culo SkeletalDocument16 pagesMus Culo Skeletalshenric16100% (2)
- Gastrointestinal DisordersDocument12 pagesGastrointestinal Disorderssophia yemane100% (4)
- Unit 8 Med Surg Study Guide NursingDocument5 pagesUnit 8 Med Surg Study Guide Nursingatl_nurse_student100% (7)
- Fluid and ElectrolytesDocument13 pagesFluid and ElectrolytesHenry Philip93% (15)
- GI NursingDocument14 pagesGI NursingKarl Bayonito100% (5)
- Electrolyte ChartDocument2 pagesElectrolyte ChartJenny Varghese100% (4)
- Fluids & ElectrolytesDocument15 pagesFluids & Electrolytesarvinnnn100% (2)
- Medical Surgical Nursing 64 PagsDocument64 pagesMedical Surgical Nursing 64 Pagstanya nNo ratings yet
- Professional Adjustment Leadership Management and ResearchDocument10 pagesProfessional Adjustment Leadership Management and Researchshenric16100% (1)
- Fundamentals of NursingDocument31 pagesFundamentals of NursingAngelica Soriano93% (14)
- Community Health Nursing Practice Questions With RationalesDocument15 pagesCommunity Health Nursing Practice Questions With RationalesFelice Lamzon Labrador100% (2)
- Community Health Nursing Practice Questions With RationalesDocument15 pagesCommunity Health Nursing Practice Questions With RationalesFelice Lamzon Labrador100% (2)
- CE Fundamentals Book-Volume 2Document50 pagesCE Fundamentals Book-Volume 2sinpackNo ratings yet
- Cardio, Respi, GastroDocument11 pagesCardio, Respi, Gastrojeshema100% (1)
- Fluid and Electrolytes for Nursing StudentsFrom EverandFluid and Electrolytes for Nursing StudentsRating: 5 out of 5 stars5/5 (12)
- Cardionursing 110207023802 Phpapp01Document18 pagesCardionursing 110207023802 Phpapp01LudwigJayBarayuga100% (5)
- Medsurg Cardio Ana&PhysioDocument6 pagesMedsurg Cardio Ana&Physiorabsibala80% (10)
- Medicationpart1 110202192115 Phpapp02Document10 pagesMedicationpart1 110202192115 Phpapp02Jessamine Rochelle Reyes Esberto100% (1)
- Respiratory DisordersDocument15 pagesRespiratory Disordersmnlstr100% (5)
- The GastroDocument25 pagesThe Gastroangel_maui100% (7)
- Endocrine NursingDocument2 pagesEndocrine Nursingsurviving nursing school100% (2)
- Physiologic Changes of Aging: System AlterationDocument1 pagePhysiologic Changes of Aging: System Alterationshenric16100% (1)
- HematologyDocument10 pagesHematologyFranzes R. Herrera100% (4)
- Musculoskeletal Note1Document34 pagesMusculoskeletal Note1FreeNursingNotes100% (4)
- Male Reproductive System and DiseasesDocument10 pagesMale Reproductive System and DiseasesMadan Kumar100% (2)
- Chapter 14 Fluid and Electrolytes ChartsDocument7 pagesChapter 14 Fluid and Electrolytes ChartsBNA_RN100% (3)
- Intestinal DisordersDocument11 pagesIntestinal DisordersJessica0% (1)
- Medical Surgical Nursing Review Notes 30pgsDocument32 pagesMedical Surgical Nursing Review Notes 30pgsNormala Macabuntal SaripadaNo ratings yet
- Mnemonics For NursesDocument52 pagesMnemonics For Nursessweetpearl27100% (3)
- Gastrointestinal Nclex Questions Part 2Document11 pagesGastrointestinal Nclex Questions Part 2Manilyn Delos Reyes Patlunag100% (1)
- Gastro Intestinal SystemDocument9 pagesGastro Intestinal SystemJe Lyn100% (1)
- Endocrine Disorders and DrugsDocument149 pagesEndocrine Disorders and DrugsJaypee Fabros Edra100% (1)
- Fluid, Electrolyte, and Acid-Base BalanceDocument8 pagesFluid, Electrolyte, and Acid-Base BalanceJo Marchianne PigarNo ratings yet
- COPD Concept MapDocument1 pageCOPD Concept MapSherree HayesNo ratings yet
- Medical Surgical NursingDocument59 pagesMedical Surgical NursingAhmari Zamora Julkarnain100% (8)
- Endocrine Disorders (Study Notes)Document11 pagesEndocrine Disorders (Study Notes)Danelle Harrison, RN90% (10)
- Acute Cardiac AlterationsDocument38 pagesAcute Cardiac AlterationsJoyce SiosonNo ratings yet
- Maternity NursingDocument41 pagesMaternity Nursingbajaoc100% (1)
- Positioning ClientsDocument2 pagesPositioning ClientsROBERT C. REÑA, BSN, RN, MAN (ue)100% (13)
- Tips On NURSING LICENSURE EXAMDocument4 pagesTips On NURSING LICENSURE EXAMFernando Maglunob Lastrollo Jr.94% (17)
- 313 - Disorders of Renal and Urinary SystemsDocument8 pages313 - Disorders of Renal and Urinary SystemsChrissy Mendoza100% (2)
- Resp Lecture NotesDocument18 pagesResp Lecture Notessurviving nursing schoolNo ratings yet
- Blood Disorders AnemiaDocument6 pagesBlood Disorders AnemiaFreeNursingNotesNo ratings yet
- Jarvis 6th Ed - Chapter 21Document6 pagesJarvis 6th Ed - Chapter 21edoble100% (4)
- Quick Nursing Student Notes 2Document1 pageQuick Nursing Student Notes 2Frank KimNo ratings yet
- Medical Surgical NursingDocument59 pagesMedical Surgical NursingChey Dianne Seriña100% (11)
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideFrom EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideNo ratings yet
- Medical and Surgical NursingDocument4 pagesMedical and Surgical NursingCrystal Ann Monsale TadiamonNo ratings yet
- Vanguardia's Online Review Program: Genito-Urinary TractDocument8 pagesVanguardia's Online Review Program: Genito-Urinary TractBobet ReñaNo ratings yet
- Genito Urinary SystemDocument106 pagesGenito Urinary Systemnursereview88% (8)
- Gastrointestinal SystemDocument8 pagesGastrointestinal Systemtheglobalnursing100% (1)
- Alteration in Urinary System - ppt22222Document117 pagesAlteration in Urinary System - ppt22222yen1988No ratings yet
- Disorders of Urinary System Urinary CalculiDocument5 pagesDisorders of Urinary System Urinary CalculiFreeNursingNotes100% (3)
- Urology NotesDocument8 pagesUrology NotesCzarinah Bacuado67% (3)
- Uhc Irr DraftDocument107 pagesUhc Irr Draftshenric16No ratings yet
- Fhsis Annual 2018Document496 pagesFhsis Annual 2018shenric16No ratings yet
- Maternity Nursing ReviewDocument37 pagesMaternity Nursing Reviewshenric16No ratings yet
- Nursing Board Exam Test Drill 3Document2 pagesNursing Board Exam Test Drill 3Kira100% (15)
- Evidence Based Nursing PracticeDocument21 pagesEvidence Based Nursing Practiceshenric16No ratings yet
- Evidence Based Nursing PracticeDocument21 pagesEvidence Based Nursing Practiceshenric16No ratings yet
- Cognitive DisordersDocument2 pagesCognitive DisordersSherrizah Alexis Naag NavaNo ratings yet
- Anti Psychotic DrugsDocument2 pagesAnti Psychotic DrugsJohn Corpuz100% (1)
- Health Teaching PDFDocument1 pageHealth Teaching PDFshenric16No ratings yet
- Maternal Ob NotesDocument37 pagesMaternal Ob Notesshenric16No ratings yet
- Patient Positioning in The Operating RoomDocument33 pagesPatient Positioning in The Operating Roomshenric16No ratings yet
- Palmer Complete Edited Royal PentagonDocument26 pagesPalmer Complete Edited Royal Pentagonshenric16100% (1)
- Nle - July 2011Document12 pagesNle - July 2011shenric16100% (1)
- Community Health NursingDocument49 pagesCommunity Health Nursingshenric16No ratings yet
- Reviewer For NleDocument14 pagesReviewer For Nleshenric16No ratings yet
- Course Audit Professional AdjustmentDocument9 pagesCourse Audit Professional Adjustmentshenric16No ratings yet
- Community Health NursingDocument49 pagesCommunity Health Nursingshenric16No ratings yet
- Final Outline Psychiatric NursingDocument52 pagesFinal Outline Psychiatric Nursingshenric16100% (1)
- Maternal and Child Health Nursing: KeepsDocument32 pagesMaternal and Child Health Nursing: Keepsshenric16No ratings yet
- Pediatric Nursing Edison O Dangkeo RNDocument59 pagesPediatric Nursing Edison O Dangkeo RNshenric16100% (1)
- Medicationpart1 110202192115 Phpapp02Document10 pagesMedicationpart1 110202192115 Phpapp02Jessamine Rochelle Reyes Esberto100% (1)
- Maternal Ob NotesDocument37 pagesMaternal Ob Notesshenric16No ratings yet
- Ms Penta NotesDocument84 pagesMs Penta Notesshenric16No ratings yet
- Gerard Gerrone and The Case of The Missing Pearl NecklaceDocument2 pagesGerard Gerrone and The Case of The Missing Pearl NecklaceAnonymous wFmQJhYNo ratings yet
- Back Exercises: Hamstring StretchDocument5 pagesBack Exercises: Hamstring StretchsreeeeeNo ratings yet
- MAG9811 Hardware Description (V100R006C00 - 01) (PDF) - ENDocument62 pagesMAG9811 Hardware Description (V100R006C00 - 01) (PDF) - ENHibiki KwoaHui0% (1)
- Proportion and Scale Material Proportions: The Brown Bauhaus STUDIO ARCHITECTURE 16Document9 pagesProportion and Scale Material Proportions: The Brown Bauhaus STUDIO ARCHITECTURE 16Claro III TabuzoNo ratings yet
- High Pressure PumpsDocument9 pagesHigh Pressure PumpsAhmed AwwadNo ratings yet
- Labsheet 1 (Int)Document3 pagesLabsheet 1 (Int)mail meNo ratings yet
- Ijird,+16 +MAR16019Document4 pagesIjird,+16 +MAR16019abhay OdedraNo ratings yet
- Siemens 7SK85 V7.90 Motor PTT User Manual ENUDocument6 pagesSiemens 7SK85 V7.90 Motor PTT User Manual ENURaúlEmirGutiérrezLópezNo ratings yet
- Asymptotics Sheet 3Document2 pagesAsymptotics Sheet 3ReginaldRemoNo ratings yet
- Unit 1: Remote Sensing: Syllabus: Definition and Scope, History and Development of Remote Sensing TechnologyDocument12 pagesUnit 1: Remote Sensing: Syllabus: Definition and Scope, History and Development of Remote Sensing TechnologyGMC GamingNo ratings yet
- Spiral Rope Chain - Beading Techniques - Fusion BeadsDocument5 pagesSpiral Rope Chain - Beading Techniques - Fusion BeadsShawn BrownNo ratings yet
- (AC-S04) Week 04 - Pre-Task - Quiz - Weekly Quiz - INGLES IV (10962)Document4 pages(AC-S04) Week 04 - Pre-Task - Quiz - Weekly Quiz - INGLES IV (10962)Elio Mamani TiconaNo ratings yet
- Of Surviving. Some AreDocument3 pagesOf Surviving. Some AreSinh Vạn VũNo ratings yet
- Slim Borehole ScannerDocument2 pagesSlim Borehole ScannerPangestu WibisonoNo ratings yet
- DNV-RP-F203 Riser Interference April 2009Document22 pagesDNV-RP-F203 Riser Interference April 2009TroyNo ratings yet
- Cement Industry: Technical Eia Guidance ManualDocument185 pagesCement Industry: Technical Eia Guidance ManualMas'ud Al-Hyderi100% (1)
- Press Kit BuyamiaDocument3 pagesPress Kit BuyamiaadiwiragunaNo ratings yet
- Impression Techniques in RPDDocument82 pagesImpression Techniques in RPDpramodaniNo ratings yet
- SM 42LG6000 42LG6100 PDFDocument27 pagesSM 42LG6000 42LG6100 PDFeraser2410No ratings yet
- El Capitan - Yosemite National Park - Trekking SketchesDocument1 pageEl Capitan - Yosemite National Park - Trekking Sketchesbruhbruhington101No ratings yet
- DR - Cheung - Dr. Hui - Study Club For 19 ClassDocument1 pageDR - Cheung - Dr. Hui - Study Club For 19 ClassycyNo ratings yet
- CHNN312 FinalDocument26 pagesCHNN312 FinalVALERIANO TRISHANo ratings yet
- Bamusalim Services Limited: Company Profile Civil Works DepartmentDocument14 pagesBamusalim Services Limited: Company Profile Civil Works Departmentkwoshaba pidsonNo ratings yet
- Madler Katalog41 - EN PDFDocument836 pagesMadler Katalog41 - EN PDFMiroslavDjordjevicNo ratings yet
- Majstrovic Electricity-Transmission-And-Distribution Power Oman 2020Document113 pagesMajstrovic Electricity-Transmission-And-Distribution Power Oman 2020Abdul HaseebNo ratings yet
- Surface Combat Ship (SCS)Document6 pagesSurface Combat Ship (SCS)João FródrsonNo ratings yet