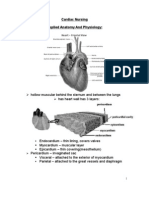
Professional Documents
Culture Documents
ICU Procedures
Uploaded by
vovaatanasov100%(1)100% found this document useful (1 vote)
668 views100 pagesThis document discusses the evolution of arterial pressure monitoring from its early beginnings in the 1700s to modern techniques. Some key points:
- Direct arterial pressure measurement was first performed on a human amputee in 1856 but was impeded until heparin was discovered in 1917.
- In the 1940s-50s, the introduction of plastic tubing and strain gauge transducers allowed for more frequent clinical use of direct intraarterial pressure monitoring.
- In the 1950s-60s, the expansion of cardiovascular surgery drove the need for continuous direct blood pressure monitoring during non-pulsatile cardiopulmonary bypass.
- Modern arterial pressure monitoring utilizes plastic catheters connected to
Original Description:
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses the evolution of arterial pressure monitoring from its early beginnings in the 1700s to modern techniques. Some key points:
- Direct arterial pressure measurement was first performed on a human amputee in 1856 but was impeded until heparin was discovered in 1917.
- In the 1940s-50s, the introduction of plastic tubing and strain gauge transducers allowed for more frequent clinical use of direct intraarterial pressure monitoring.
- In the 1950s-60s, the expansion of cardiovascular surgery drove the need for continuous direct blood pressure monitoring during non-pulsatile cardiopulmonary bypass.
- Modern arterial pressure monitoring utilizes plastic catheters connected to
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
100%(1)100% found this document useful (1 vote)
668 views100 pagesICU Procedures
Uploaded by
vovaatanasovThis document discusses the evolution of arterial pressure monitoring from its early beginnings in the 1700s to modern techniques. Some key points:
- Direct arterial pressure measurement was first performed on a human amputee in 1856 but was impeded until heparin was discovered in 1917.
- In the 1940s-50s, the introduction of plastic tubing and strain gauge transducers allowed for more frequent clinical use of direct intraarterial pressure monitoring.
- In the 1950s-60s, the expansion of cardiovascular surgery drove the need for continuous direct blood pressure monitoring during non-pulsatile cardiopulmonary bypass.
- Modern arterial pressure monitoring utilizes plastic catheters connected to
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 100
When you can measure what you are speaking about,
ane expres it in number, you know something about i
but when you cannot measure it, when you cannot express it
in numbers, your knowledge is of 2 meager and unsatisfactory kind
it may be the beginning of lnowledge, but you have scarcely
in your thoughts, advanced to the state of sine
William Thompion, Lond Kein
Isee907
Invasive Montrorinc
AND ITS.
ComPLICATIONS
IN THE
Intensive Care Unir
ARNOLD SLADEN, M.D.
Profesor of Anesthesiology aed Critical Care Medicine,
Asocate Profesor of Surgery,
Univesity of Pitsburgh School of Medicine;
Director, Surgical Intensive Care Unit
Montene Hospital
Pisburgh, Pensyvania
With 205 illastrations
Tur C. V. Mossy Company
St Louis # Bahimore + Philadelphia * Toronto 1990
seers
EPEC TOE r rere errr eres Cleese site)
CONTENTS
cure,
1
EVOLUTION OF MONITORING, 1
Diagnosis in the early seventeenth century, 1
Edocation ofthe seventeenth-century physician, 3
Leaders in. mor
toring from the late seventeenth century, 7
Evolution ofthe intensive care units, 36
ARTERIAL PRESSURE MONITORING, 47
Auterial cannulation, 47
Arterial pressure monitoring, 49
Arterial catheters and plumbing, 52
Site selection, 53
4
Preparation for arterial cannulatio
Anatomy of radial and uln
palmar
anteties and superficial and deep
5, 56
Radial or ulnar artery cannulation, 61
Complications of radial and ulnar artery catheterization, 67
Femoral artery, 78
Femoral artery cannulation, 79
Complications of femoral artery catheterization, 85
Auillay artery, 86
Axillary artery cannulation, 57
Complications of axillary artery cannulation, 93
Brachial artery cannulation, 94
Arterial blood sampling (arterial phlebotomy), 4
cuvrrer
3
CENTRAL VENOUS CATHETERIZATION, 99
Indications for central venous catheterization, 101
Subelavian vein, 102
Internal jugular vein, 103
Cannulation, 105,
Complications of central venous catheterization, 114
4
PULMONARY ARTERY CATHETERIZATION, 125
Indications for pulmonary artery catheter Re
Pulmonary artery catheter, 129
te selection, 131
Pulmonary artery catheterization, 132
Complications of pulmonary artery catheterization, 161
Frequeney of complications, 161
Complications at insertion sites, 162
Errors and artifacts, 163
Knotting, entanglement, and embolic fragments, 166
Arhythmias, 168
Intracardia lesions, 172
Perforation of the pulmonary artery, 178
TTheombus formation, 180
Pheumonectomy, 183,
Other complications, 183
Lack of corelation between PAWP and left ventricular end
diastolic volume post coronary bypass procedures, 184
I
S222IIIIDIZIQIIIITTITIT TEE eit
contents wii
corre
5
INFECTION-COMPLICATING INTRAVASCULAR
DEVICES, 191
Identification of intravascular catheter-related infections, 193,
CCatheterelated infections, 193,
Mechanical equipment and infection, 197
compre
6
INTRACRANIAL PRESSURE MONITORIN'
Indications for ICP monitoring, 200
Complications of ICP monitoring, 211
cuarreR
7
URINARY BLADDER CATHETERIZATION,
Indications for urinary eatheteization, 215
Infection and complications of urinary catheterization, 216,
Prevention of infection, 217
a
‘THE ROLE OF INVASIVE MONITORING,
zu
CHAPTER
1
EVOLUTION OF MONITORING
Monitoring had is genesis inthe late seventeenth century, when
science became independent of philosophy, when precise measure-
‘ment and exact methodology became as important tothe physician
as empiricism had been. In the last three centuries scientific know
cedge and understanding of the frailty and complesty of the hu-
rman body has inereased steadily and unbounded, Consequently,
‘monitoring techniques have been advanced and refined. However,
what advancements have been made toward beter patient:
physician communication? Has the advent of sophisticated moni
toring equipment and the data derived from it inthe intensive care
tunit (ICU) produced physicians who look only at waveforms and
rmumbers, are remote from the bedside, and ignore the patient”
DIAGNOSIS IN ‘THE EARLY
SEVENTEENTH CENTURY
‘Three centuries ago, the early seventeenth-century physician at
tended his patient primarily by listening to his narrative and then
prescribing therapy." Diagnosis was made by allowing the patent to
fully describe his symptoms, when necessary supplemented by in
{errogative remarks of the physician. This remains the typical
method of obtaining a medical history, even in the twentieth cen-
tury. From the history the seventeenth-centry physician would se
lect specific point as indicators of current ot even pas illnes. The
physician became skilled in studying the patient's overall physical,
appearance and behavior pattern, and it was unusual for any phys:
ical contact to take place between physician and patient
46 INVASIVE MONITORING AND ms COM
51. Lasen HCA: A preliminary reprt on the 1952 epidemic of pions
clits in Copenhagen with special reference tothe treatment of acute
respiratory mnslcency, Lancet 137, 1953,
Itven Bs Anaesthetists viewpoint ofthe treatment of respiratory com.
pliations in poliomyelitis daring the epidemic in Copenhagen, 1952.
Poe R'Sec Med 14:72, 1954
53, Fainky HB: The Toronto Genctal Hospital piratory unit, Anaesthe-
sia 16.267, 1961
54, Holmudahl MH: The esptatory cae unit, Anethesiology 23559,
1962
55, Sar P et al The intensive care unit, Anaesthesia 16275, 1961
56, Waklund PE: Intensive care nits: design, locaton, stafing ancillary
atas, equipment, Anesthesiology 31:122, 1969.
Shoemaker WC, Een DH, and Rosen AL: Development and goal
‘of trauma apd shock research center, Mt Sinai } Med 35451, 1968,
58. Brown KWG et al: Coronary unit an inlensvecarecente for acute
rvocardal infarction, Lancet 2349, 1963
tein A-and Scheiner ME The eadotachoscope, Anesthesia
2, 1952.
(60, Safar P and Grenvik A: Crcal care medicine: onganizing and safing
intensive care units, Chest
INNA
CHAPTER
2
ARTERIAL PRESSURE
MONITORING.
ARTERIAL CANNULATION
Although the direct invasive technique for measuring arterial
blood pressure was used on a animal ay ealy as 1733, it was not
‘until 1856 that it was used on a human being. The technique was
teed by a French physician named Fuivte, who cannulated the leg
antery ofan amputee."
“Many factors have impeded the progres of diet invasive mea:
surement, but the discovery of heparin in 1917 greatly facilitated
the technique, whieh wsed a metal needle, a heparinized saline
‘ridge, and a mercury oF aneroid manometer." In 1947 the stain
gauge ransdcer was introduced‘ The transducer functions on the
basis that stretch force applied toa wite changes both length and
‘ros Sectional area and in turn electrical resistance. Using four
‘utes to form a Wheattone bridge, one ean calibrate changes in
‘output voltage to represent pressures applied to the transduce’ dh
aphragm. The strain gauge tansducet and introduction of paste
tubing allowed direct inteaatesal pressure measurement to be uscd
more requenty in clinical practice, Peterson, Deipps, and Risman,
working sn the Hanson Depurtment of Surgical Research atthe
University of Pennsylvania School of Medicine, disked both the
id metal needle and the need to proces the photographic paper
of the atrial tracing before the data could be analyzed—a tet
spective clinical evaluation.” To overcome these hurdles they de-
signed and made intaarteval plastic cannulae, which they used in
conjunction with an amplificr and ink recorder. This provided a
4 INVASIVE MONITORING AND TS GoMRLICATIONS
dynamic, visible, and perm:
ng of the arterial pulse
contour. ‘The catheters were made by heating polyvinyl resin tubing
and drawing itout to the desived length and diameter, ‘The cathe
ters were cut to size and, until requited, left to soak in Zephiran
Chloride solution. Even at that time Peterson and Dripps were
concemed with end pressure, turbulence, and capacity. They were
aware that pressure monitoring conduits were under damped sys
tems of natural frequeney that could produce overshoot of pressure
measurement. ‘The pressure ttacings reproduced from their text
clearly demonstrate in clinical situations the effects of hemorshage
and failure to contol the hemorrhage (Figure 2-1)
In 1961, Barr fist described the percutaneous puncture of the
radial artery with a Teflon catheter that could be used for contin
‘ous monitoring and arterial blood sampling." ‘The thrust for direct
blood pressure monitoring came with the rapid expansion of eatdion
vascular surgery in the 1950s and 19606. Previously used classic
noninvasive techniques were useless during the nonpubatile low of
Blond being replaced-stll Bleeding
FIGURE 2.1. Brachial atery tracings frm a 55-year-old male undergoing
pneumonectomy for bronchogenic carcinoma, 1157: Peicadiar
‘pened. 1201: Masive hemorshage fom lung hil. 12.2%: Tal of 3000
rl of blocd given by syringe. 1250 Hemonhage continued, heat
slopped. and presure decreased to 23 mm Hg. from Peteran LH
Dripps RD and Risman GC: A method fr mconding the arterial presune
pulse and Blood prsur in man, Am Hert 137.771, 1949)
NNR
ARTERIAL PRESSURE MONITORING ”
cardiopulmonary bypass. Continuous intaarteril pressure moni-
toring became indispensable,
ARTERIAL PRESSURE MONITORING
Its essential to be aware at the outset that there isa lack of eor-
relation between the acquired data of arterial pressure measured by
the inditeet classic method and by the direct invasive method, since
the two techniques do not measure the same functions. Indirect
blood pressure measurements depend on blood flow and are deter:
‘mined by using an inflatable cuff and either a stethoscope or Dop
pler system, ‘The return of blood flow in the artery as the cull is
deflated indicates systole, and subsequent changes in sound indi-
cate diastole. An intraarterial catheter measures presses ditcely
‘One technique measures flow; the other measures pressure. There-
fore it is not surprising that direct measurements of systolic and di-
astolic pressures corteate rather poorly with indirect measure-
rents, Bruner and co-workers, using the most extensive review to
date, coupled with their own clinica studies, conclude that auscul-
tatory systolic pressure is usually lower than direct, but there are
‘numerous instances in which Riva-Rocei readings are 20 mun Hg
for more higher than direct readings.” Similanly, indirect diastolic
pressure is lower than direct, but because of the narrow range of
diastolic pressures, the differences are less than those that occur in
systole. One would expect direct pressure measurement to be sim
ple and yield correct values. A variety of complex and complicating
factors interfere with the determination of true values, producing
terrors and therefore inherent complications in both primary mea-
‘surements and subsequent therapy,
‘To display arterial blood pressure on a monitor digitally, one re-
‘quires, in addition to the monitor, an indwelling arterial catheter,
tubing containing a heparinized solution, a transducer and stop:
cock’). Each of these, because oftheir ox natural frequency and
damping effects, changes what the monitor finally records from
within the intraarteral system, The natural fequency refers to how
rapidly the system oscillaes, and the damping coefficient refers to
Thow quickly the system comes to rest. The underdamped catheter
transducer system overestimates the systolic prssute, frequently by
as much as 15 to 30 mim Hg,
A presure transducer consists of a chamber with a stiff, low
‘compliance, pressure-snsing diaphragm capable of bending and
creating a small volume change in response to an applied pressure
50 INVASIVE MONITORING AND IS COMRUICATIONS
change. ‘The mechanical movement then is converted into an elee-
trical signal by changing the resistance in a Wheatstone bridge
This apparatus is very sensitive and will provide false values if dam.
aged. Recently developed silicon erystals have redced the errors
inherent inthe older wite transducers, which were easily subject to
damage, The transducer dome should be stall, made of tratspar-
‘ent material to disclose air bubbles, and designed for easy removal
The transducer requires an orifice to which a stopcock can be at
tached. Its at this site, opaque and invisible, that air bubbles ac
cumulate, Periodically, transducers should be calibrated directly
with a mereury manometer, From the transducer the electrical sig
nal enters the preamplifier and amplifier, where the transducers
cean be zeroed and calibrated. Finally, the signal is displayed on a
cathode ray tube or sercen. Resonance in the Auidicssstem, which
consists of tab
1g and its fluid content, results in the production of
autifets. These artifcts are filtered out in the electronic hardware
to give an acceptable systole contour. Because of the use of high
frequency filtering in pressure monitors, diferences may become
apparent between direct prestre measiements, and indivect or
marked differences in systole pressures can be observed if a patent
is moved from one monitor to another with high-frequency filers
of diferent physical characteristics,
‘The system is calibrated when filled with « heparinized solution
fiom a pressurized bag. As the solution enters the flow chamber
and is depressurized, air bubbles accumulate—a major source of
pressure measurement errors, ‘These bubbles become sequestered in
the transducer dome, in the connecting tubing, or within the
‘opaque stopcock; they depres oscillation and in turn overdampen
the sytem. Another cause of etror is overpresurizing the transdue-
cers with ud either while the system is being set up or during cal:
ibration. Depressurizing by leakage from the system results in a
progressive downward drift of the shape ofthe waveform, which in
tum is reflected by inaccurate recordings and subsequent misman-
agement,
Finally the transducer has to be leveled, Arterial pressure is ef
cerenced, usally tothe left ventricle, and itis to this position the
transducer must be leveled and with the stopeock open (atmo-
spheric pressure). Failure to have a comrect zero reference point will
provide useless data, A transducer set too low will record pressures
that ate too high. A transducer set too high will dacument pressures
that are too low. Incorrect leveling may not be catastrophic in the
cae of arterial pressure, but it will result in significant diserepan
RMN
ARTERINL PRESSURE MONTTORING SI
cies when low-pressure sstems such as pulmonary artery presures
are involved, With correct setup and balancing ofthe monitor and
transducer, inherent errors may sill occur because of the inertia
and fition of the uid in the tubing and elasticity of the tubing
Using high-compliance tubing reals in lowering ofthe fequent
response of the sstem, distortion of the presure waveform and
‘overshoot ofthe sstolie pressure. It is possible to overcome this
robles by using noncompliant pressure conneetng tubing
Bedford has demoratrated thatthe aerial puise-pressure wave-
fons changes progresvely fom the ascending ast to peripheral
sites (Figure 22)" Wis believed that these changes in areal wave
fore, particularly the systolic component, account forthe difer-
ceces between diet and initcet arterial pressures measured a the
Sane site and diferences in dinect pressures bericen diferent sts
“The systolic presre in the aorta i ar lower than the systolic pres-
sure inthe radial artery. Indeed, the aortic pressure represents the
tive aferlod against which the heat works. As the pube-pressure
‘wave moves dtl, at about 10 meters per second, the ial up-
stroke becomes steeper and the systolic maximum becomes progres-
Sutcoven
mn
ait
FIGURE 2-2. Arterial alee presure waveform tracings demonstating pro
sresive changes fom the ascending aot tothe femoral artery
sively peaked. As the waveform becomes narrower, the systolic and
pulse pressures increase and the diastolic and mean pressures de
crease. ‘The major modifying factors in the systolic component of
the pule-pressure waveforms are wave reflections from the periph
cry. As the pulse-pressure wave hits the arterioles, much of itis re-
Acted backwards, These reflected waves alter the tue value of the
pulse-pressure wave in the peripheral pulses. Because of is proxim=
ity to the peripheral arterioles, the radial artery will indicate a
higher dicect systolic pressure than that measured indirectly at the
brachial artery. It should be noted that if the lumen of an arterial
catheter becomes occluded, the reflected waveform is initiated at
the occlusion point
(Other factors that alter the configuration of the pulse-pressure
waveform include a dectease in elastic tissue and an increase in
muscle tise as the arterial tree progresses distally as well as the
narrowing of the artery that amplifies the pulse wave. The develop
‘ment of arteriosclerosis and the loss of elasticity with age accounts,
for the decrease in both ditect and indirect systolic pressure mea
surements at distal sites.
ARTERIAL CATHETERS AND PLUMBING
The Cournand needle was used for intraatterial cannulation in
the physiologic laboratory and cardiac catheterization suite and
later introduced into other clinical areas. It consisted of a metal
needle with two wings a right angles tothe long axis ofthe needle
and adjacent to the hub, and an inner metal stylet, Subsequently,
with the development of plastics, the plastic catheter placed over a
metal needle has become a common} used tool for access into pe-
ripheral narow arteries such a the radial. Larger vésels, for exam-
ple, the femoral, are usually cannulated by using the Seldinger
guide wire technique, ‘The technique consists of intially inserting a
thin-walled, narrow needle into the vessel. When acces is gained,
a flexible smooth-tipped wite i fed through the needle, which is,
then withdrawn, An introducer or larger bore catheter then can be
threaded over the wire into the artery. A Seldinger-ype sytem has
been designed for radial artery cannulation
Arterial catheters have been manufactured from polypropylene,
polyvinyl chloride, and Teflon. Fach has its own characteristics
with respect to stiffness, kinking, and thrombus formation, The
‘most commonly used catheter at this time, though, is manufac-
tured from ‘Teflon. To have optimum frequency response with
PEPER ERPECEIEIEETEEerrrITTrreeeee
ARTTRIAL PRESSURE MONITORING 3
iminimam distortion of the pulespesure wave, itis best to use
‘wide bore catheter. However, small bore catheters are efficient be-
Cause although they have some high-Fequeney response, their
dmsping ceticients ae high. The sal eather dampens the un-
derdamped catheter-estension tube system, resulting in less ringing
or hypetesonance in response t0 repetitive pulse waveforms, The
result that stole pessre is measured more accurately
Extension tubing promot ringing or bypetesonance, which ne
cases with the length ofthe tubing. Indeed, the ation of 5 Feet
fof tubing will provide a systolic pressure 16% greater than that of
brachial arterial presire. Hence, every attempt should be made to
reduce the connecting tubing t the minimum.
‘Air bubbles inthe plumbing system are the greats source of er
tor in measuring direct atrial presure. Large bubbles darnpen the
pulsepresite wave; small bubbles produce ringing or hypereso-
france: The addition of 0.05 to D.25 ml of arin an arterial pressure
Tine will augment sstlie pressure fom 150 o 190 mm Hg. Dias
tole and electronic mean remain unchanged. It is impossible 10
prevent the formation of air bubbles. When fluid moves fom the
High-pressure heparin flow hag to the low-pressure hyalie system,
air bubbles alway ill accumulate. Stet and frequent attention 1
‘eteting alteration in Frequeney response and damping is essential
fd should be of major concern to the ICU physician and nurse.
‘One should seatch for ar bubbles and remove them prompl
SITE SELECTION
Any sup sey cn be xa for lial we, The
wood ariel uated al, ag, ne ps
dis, and, in children, the temporal artery. In our surgical ICU the
Se ee maa ped oscar doy Th ow,
aerate bach and the oul ate these
ce oaphatans mel tik po.
cere ee dine eae han fe ae he el
SO rotamer we, lose
a cil hc ga tation dead
en reas te ther coats palog, shen
Set ee es ieee been
Te ee ee etal he ous ce
Senay taeda bed ine inane
wen tc aniited el cettztan wl be osha
ree Pein Sabah igh oregon ta sno
You might also like
- Critical Care NoteDocument10 pagesCritical Care NoteHanis Rozib99% (69)
- CCRN CardiacDocument39 pagesCCRN CardiacMike100% (5)
- EKG/ECG Interpretation Made Easy: A Practical Approach to Passing the ECG/EKG Portion of NCLEXFrom EverandEKG/ECG Interpretation Made Easy: A Practical Approach to Passing the ECG/EKG Portion of NCLEXRating: 5 out of 5 stars5/5 (2)
- Ccu Survival GuideDocument10 pagesCcu Survival Guideomegasauron0gmailcom100% (1)
- ICU GuidelinesDocument111 pagesICU GuidelinesIchal fais100% (2)
- The Intensive Care Unit at The Mid Yorkshire Hospitals NHS TrustDocument164 pagesThe Intensive Care Unit at The Mid Yorkshire Hospitals NHS TrustRajiv Srinivasa71% (7)
- Critical Care Nursing Certification: Springhouse Review ForDocument384 pagesCritical Care Nursing Certification: Springhouse Review ForNrhildaNo ratings yet
- FLASH CardsDocument3 pagesFLASH Cardsclarheena100% (2)
- Icu Nursing BrainDocument2 pagesIcu Nursing Brainapi-282417591100% (2)
- The Intensive Care Unit MaualDocument356 pagesThe Intensive Care Unit MaualMariefel Villanueva AlejagaNo ratings yet
- Critical Care NursingDocument26 pagesCritical Care NursingBarbie Sarabia100% (2)
- Icu GuidebookDocument43 pagesIcu Guidebookdrimran570100% (5)
- Hemodynamic Management Pocket Card PDFDocument8 pagesHemodynamic Management Pocket Card PDFjenn1722No ratings yet
- CCRN Review Part 1: "Never Let What You Cannot Do Interfere With What You Can Do"Document160 pagesCCRN Review Part 1: "Never Let What You Cannot Do Interfere With What You Can Do"Paolo VegaNo ratings yet
- CCRN-PCCN Review GastrointestinalDocument23 pagesCCRN-PCCN Review GastrointestinalGiovanni MictilNo ratings yet
- CCRN PulmonaryDocument107 pagesCCRN PulmonaryCzarina Charmaine Diwa100% (4)
- Icu Nurse Crash CourseDocument3 pagesIcu Nurse Crash CourseSERA B.100% (2)
- Icu NotesDocument47 pagesIcu NotesChryst Louise SaavedraNo ratings yet
- CCRNDocument17 pagesCCRNNílo Stárn100% (1)
- ICU Procedure HandoutsDocument26 pagesICU Procedure HandoutsDadi Veen100% (2)
- Starting Out - New in The ICUDocument30 pagesStarting Out - New in The ICUashdmb217100% (1)
- Haemodynamic Monitoring & Manipulation: an easy learning guideFrom EverandHaemodynamic Monitoring & Manipulation: an easy learning guideNo ratings yet
- Critical Care Reviews Book 2017Document356 pagesCritical Care Reviews Book 2017Herbert Baquerizo VargasNo ratings yet
- Nursing Practice Skills: Adult Intensive Care Unit PatientsDocument10 pagesNursing Practice Skills: Adult Intensive Care Unit PatientsMona Doria67% (3)
- Critical Care NursingDocument11 pagesCritical Care Nursingveinslasher100% (3)
- Mastering ICU Nursing: A Quick Reference Guide, Interview Q&A, and TerminologyFrom EverandMastering ICU Nursing: A Quick Reference Guide, Interview Q&A, and TerminologyNo ratings yet
- ICU Drips: Stephanie Sanderson, RN, MSN, CNS, CCNS, CCRN Medical Cardiac ICU-UNMHDocument32 pagesICU Drips: Stephanie Sanderson, RN, MSN, CNS, CCNS, CCRN Medical Cardiac ICU-UNMHNicole Adkins100% (1)
- Suggest Fluid Responsiveness: Pulse Pressure Variation (PPV) Cardiac Arrest UtilityDocument1 pageSuggest Fluid Responsiveness: Pulse Pressure Variation (PPV) Cardiac Arrest Utilityabobader2100% (1)
- Critical Care NursingDocument159 pagesCritical Care NursingJoy Jarin50% (2)
- Drugs in ICUDocument83 pagesDrugs in ICUJennifer DixonNo ratings yet
- Hemodynamic Rounds: Interpretation of Cardiac Pathophysiology from Pressure Waveform AnalysisFrom EverandHemodynamic Rounds: Interpretation of Cardiac Pathophysiology from Pressure Waveform AnalysisNo ratings yet
- Cardiac NursingDocument26 pagesCardiac Nursingjgcriste95% (20)
- Alfred Hosp ICU-orientation-manualDocument85 pagesAlfred Hosp ICU-orientation-manualdragon66No ratings yet
- Critical Care Nursing Manuall IDocument90 pagesCritical Care Nursing Manuall ILesley Gonzalez75% (4)
- Acute Critical Care Nursing HandoutDocument17 pagesAcute Critical Care Nursing HandoutJulie May100% (6)
- ICU Registered Nurse Resume Brick RedDocument2 pagesICU Registered Nurse Resume Brick RedAngelNo ratings yet
- Critical Care NursingDocument159 pagesCritical Care Nursinggretchen marie80% (5)
- AeonDocument4 pagesAeonsancsa_74No ratings yet
- Transcutaneous Cardiac PacingDocument8 pagesTranscutaneous Cardiac PacingistiNo ratings yet
- Icu Head To Toe AssessmentDocument3 pagesIcu Head To Toe Assessmentmsbunnilee100% (2)
- Critical Care NursingDocument1 pageCritical Care NursingMelissa David0% (1)
- CCRN Sample QuestionsDocument5 pagesCCRN Sample Questionsgwapdose50% (2)
- ICU ManagementDocument26 pagesICU Managementvamshidh100% (2)
- 8-Hemodynamic Monitoring: Central Venous Pressure (CVP)Document6 pages8-Hemodynamic Monitoring: Central Venous Pressure (CVP)AsmaaYL100% (1)
- Akshaya Vanam: Indian SandalwoodDocument52 pagesAkshaya Vanam: Indian Sandalwoodprasadgss100% (4)
- Astm D974-97Document7 pagesAstm D974-97QcHeNo ratings yet
- Inverse Curve Trip Time Calculation: Enter Values in White CellDocument3 pagesInverse Curve Trip Time Calculation: Enter Values in White CellVijay FxNo ratings yet
- 409 Pope, B. and Maillie, S. CCRN-PCCN Review Multisystem and Q and ADocument21 pages409 Pope, B. and Maillie, S. CCRN-PCCN Review Multisystem and Q and Agliftan100% (2)
- 65 ActsDocument178 pages65 ActsComprachosNo ratings yet
- Cardiac Study Guide PDFDocument11 pagesCardiac Study Guide PDF281175100% (1)
- Manual IcuDocument217 pagesManual IcuEmil Zatopek100% (3)
- 209 Pope, B. CCRN-PCCN-CMC Review Cardiac Part 1Document14 pages209 Pope, B. CCRN-PCCN-CMC Review Cardiac Part 1peanant100% (1)
- ICU Orientation ManualDocument107 pagesICU Orientation Manualhery100% (2)
- Icu Survival Guide: SUNY Upstate Medical UniversityDocument36 pagesIcu Survival Guide: SUNY Upstate Medical UniversitySAUMOJIT MAJUMDERNo ratings yet
- Textbook of Therapeutic Cortical StimulationDocument465 pagesTextbook of Therapeutic Cortical Stimulationvovaatanasov100% (2)
- Thermobaric Effects Formed by Aluminum Foils Enveloping Cylindrical ChargesDocument10 pagesThermobaric Effects Formed by Aluminum Foils Enveloping Cylindrical ChargesAnonymous QFUEsUAnNo ratings yet
- Ward-based Critical Care: a guide for health professionalsFrom EverandWard-based Critical Care: a guide for health professionalsRating: 4 out of 5 stars4/5 (5)
- Wet Chemical Pre E PresentationDocument310 pagesWet Chemical Pre E PresentationEdwardAlexanderGarciaNo ratings yet
- The Western and Eastern Concepts of SelfDocument3 pagesThe Western and Eastern Concepts of SelfTakumi Shawn Hinata100% (3)
- Basic Mechanical Ventilation 2014Document62 pagesBasic Mechanical Ventilation 2014dragon66No ratings yet
- Arterial Lines Mark Hammerschmidt, RN FromDocument9 pagesArterial Lines Mark Hammerschmidt, RN FromMark Hammerschmidt100% (3)
- Marxism and The Oppression of Women Lise VogelDocument259 pagesMarxism and The Oppression of Women Lise VogelMoises SaavedraNo ratings yet
- Arterial LinesDocument13 pagesArterial LinesberhanubedassaNo ratings yet
- CRRTprotocol ICU - Hemo ModifiedDocument3 pagesCRRTprotocol ICU - Hemo Modifiedtimie_reyesNo ratings yet
- Shock Study GuideDocument8 pagesShock Study GuideMadameb1No ratings yet
- Onyebuchi Mudalue Coverletter Revisited 1Document1 pageOnyebuchi Mudalue Coverletter Revisited 1api-314643569No ratings yet
- Anatomy of The Callosomarginal Artery Applications To Microsurgery and Endovascular SurgeryDocument9 pagesAnatomy of The Callosomarginal Artery Applications To Microsurgery and Endovascular SurgeryvovaatanasovNo ratings yet
- Alterations in VO2max and The VO2 Plateau With Manipulation of Sampling IntervalDocument8 pagesAlterations in VO2max and The VO2 Plateau With Manipulation of Sampling IntervalvovaatanasovNo ratings yet
- Radio 8 10Document68 pagesRadio 8 10vovaatanasovNo ratings yet
- Aerofax Minigraph 01 - Lockheed SR 71 BlackbirdDocument20 pagesAerofax Minigraph 01 - Lockheed SR 71 Blackbirdvovaatanasov100% (3)
- Lesson Notes Lecture 14Document5 pagesLesson Notes Lecture 14Quantum SaudiNo ratings yet
- Rezhna Hassan FarajDocument2 pagesRezhna Hassan FarajchristoptNo ratings yet
- Mono 108Document438 pagesMono 108pasaricaNo ratings yet
- Solids Separation Study Guide: Wisconsin Department of Natural Resources Wastewater Operator CertificationDocument44 pagesSolids Separation Study Guide: Wisconsin Department of Natural Resources Wastewater Operator CertificationkharismaaakNo ratings yet
- Curso VII Lectura 2. New Rural Social MovementsDocument12 pagesCurso VII Lectura 2. New Rural Social MovementsFausto Inzunza100% (1)
- Ield Methods: A Typical Field Mapping Camp in The 1950sDocument4 pagesIeld Methods: A Typical Field Mapping Camp in The 1950sshivam soniNo ratings yet
- Onitsuka Tiger PDFDocument67 pagesOnitsuka Tiger PDFAhmad Bilal MawardiNo ratings yet
- CFD Analysis of Flow Through Compressor CascadeDocument10 pagesCFD Analysis of Flow Through Compressor CascadeKhalid KhalilNo ratings yet
- Proknow VersionDocument21 pagesProknow Versionapi-392523563No ratings yet
- Curriculum VitaeDocument7 pagesCurriculum VitaeRossy Del ValleNo ratings yet
- Activity - Alien DNA - CompleteDocument36 pagesActivity - Alien DNA - CompleteJennifer ShawkiNo ratings yet
- T 1246784488 17108574 Street Lighting Control Based On LonWorks Power Line CommunicationDocument3 pagesT 1246784488 17108574 Street Lighting Control Based On LonWorks Power Line CommunicationsryogaaNo ratings yet
- Syllabus (402050B) Finite Element Analysis (Elective IV)Document3 pagesSyllabus (402050B) Finite Element Analysis (Elective IV)shekhusatavNo ratings yet
- Science: The Menstrual CycleDocument4 pagesScience: The Menstrual CycleLena Beth Tapawan YapNo ratings yet
- Benefits of OTN in Transport SDNDocument9 pagesBenefits of OTN in Transport SDNGhallab AlsadehNo ratings yet
- Unemployment in IndiaDocument9 pagesUnemployment in IndiaKhushiNo ratings yet
- Outerstellar Self-Impose RulesDocument1 pageOuterstellar Self-Impose RulesIffu The war GodNo ratings yet
- HACH LANGE Amino Acid F Reagent Powder (2353255)Document6 pagesHACH LANGE Amino Acid F Reagent Powder (2353255)kerem__22No ratings yet
- SVR Neuro Quote 2 PROvidoDocument3 pagesSVR Neuro Quote 2 PROvidoChejarla Naveen KumarNo ratings yet
- WL4000Document1 pageWL4000Laser PowerNo ratings yet
- The Latent Phase of LaborDocument8 pagesThe Latent Phase of LaborLoisana Meztli Figueroa PreciadoNo ratings yet