Professional Documents
Culture Documents
Enfermedades Digestivas
Uploaded by
Stefany GonzalesOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Enfermedades Digestivas
Uploaded by
Stefany GonzalesCopyright:
Available Formats
1130-0108/2004/96/2/138-142
REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS REV ESP ENFERM DIG (Madrid)
Copyright © 2004 ARÁN EDICIONES, S. L. Vol. 96. N.° 2, pp. 138-142, 2004
Recurrent Dieulafoy’s disease with surgical management:
diagnosis by endoscopic ultrasonography
D. Martínez Ares, J. Souto Ruzo, J. Yáñez López, P. Alonso Aguirre, C. Gómez Mata2, L. Valbuena
Ruvira1 and J. L. Vázquez Iglesias
Service of Digestive Diseases, 1Pathology and 2General Surgery. Complejo Hospitalario Universitario Juan Canalejo. A
Coruña, Spain
ABSTRACT accurately known, since misdiagnosis may occur in some
cases (4). Most of these lesions are located in the stomach
Dieulafoy’s disease is an uncommon but potentially significant (1), although they may also appear in other parts of the
cause of gastrointestinal bleeding caused by a large-caliber arterial
vessel in the submucosa, which causes erosion and debilitation of gastrointestinal tract such as the duodenum, jejunum or
the surrounding mucosa and may lead to massive gastrointestinal rectum. Although fairly uncommon, this entity may be
bleeding. Since endoscopy may prove insufficient, echoendos- potentially severe and even have a fatal outcome.
copy may help in the diagnosis of this condition. Echoendoscopy It is also known as “caliber-persistent artery”, and
may also help improve endoscopic management using mechanical
techniques (hemoclips or band ligation) or a combination of ther-
consists of a large caliber artery which protrudes through
mal techniques and injection sclerotherapy, since this allows an the submucosa and contacts the mucosa (5). Minute
accurate localization of the submucosal vessel. ruptures in this usually atrophied mucosa (6) lead to
We present a case illustrating this approach by endoscopic ul- rupture of the vessel and cause subsequent bleeding.
trasonography, and describe the morphological substrate of this This bleeding may be recurrent or single. Diagnosis is
condition.
difficult when no active bleeding is observed, since no
Key words: Dieulafoy’s disease. Endoscopic ultrasonography. apparent lesion in the mucosa can be seen (5). Initial
Surgical management. Endoscopic management. treatment usually consists of endoscopic management:
injection techniques combined with another modality of
endoscopic hemostasis: thermocoagulation or mechani-
cal methods (hemoclipping or band ligation). If the ble-
Martínez Ares D, Souto Ruzo J, Yáñez López J, Alonso Agui- eding cannot be stopped by these techniques, a surgical
rre P, Gómez Mata C, Valbuena Ruvira L, Vázquez Iglesias JL.
Recurrent Dieulafoy’s disease with surgical management: diag- resection of the affected segment is generally indicated.
nosis by endoscopic ultrasonography. Rev Esp Enferm Dig
2004; 96: 138-142.
CASE REPORT
We present the case of a 39-year-old male with a his-
INTRODUCTION tory of two previous hospital admissions 9 and 4 years
before, both for upper gastrointestinal bleeding secon-
Dieulafoy’s disease is an uncommon cause of gas- dary to Dieulafoy’s disease, one of which required sur-
trointestinal bleeding (1), which accounts for approxima- gery. The patient did not report previous alcohol abuse,
tely 1% of all non-variceal upper gastrointestinal bleed- smoking or other unhealthy habits. There was no history
ing episodes (2). Most are cases of peptic ulcer (3). of NSAID or other drugs ingestion.
Nevertheless, the actual incidence of this disease is not The patient presented with anemia and melenic stools
at admission. Biochemistry revealed severe anemia with
a hematocrit of 25% (38-50) and hemoglobin 7.5 g/dl
Recibido: 23-04-03. (13.5-18). An emergency upper endoscopy showed a pro-
Aceptado: 04-09-03.
truding lesion with preserved mucosa at the junction of
Correspondencia: David Martínez Ares. C/ Emilio González López, 11, 7º the body and fundus, and no active bleeding at that time,
B. 15011 A Coruña. e-mail: dmartinezares@sepd.es a picture that apparently corresponded to the Dieulafoy’s
Vol. 96. N.° 2, 2004 RECURRENT DIEULAFOY’S DISEASE WITH SURGICAL MANAGEMENT: 139
DIAGNOSIS BY ENDOSCOPIC ULTRASONOGRAPHY
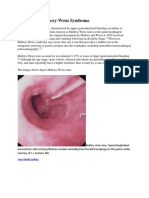
Fig. 1.- An elevated lesion with no active bleeding is identified at the Fig. 2.- Echoendoscopy reveals the presence of an hypoechogenic tu-
junction of the gastric body and fundus, apparently corresponding to a bular structure that corresponds to an arterial vessel with an abnor-
Dieulafoy’s lesion. A minute bleeding spot may be seen at the site of mally large caliber and an ulceration in its apex in contact with the mu-
sclerosant injection. cosa, which suggests the presence of a case of Dieulafoy’s disease.
A nivel de la unión de cuerpo y fundus gástrico se identifica lesión so- La ecoendoscopia muestra una estructura tubular hipoecogénica que
breelevada sin sangrado activo, que parecía corresponder a una lesión corresponde al vaso arterial con calibre anormlamente grande en con-
de Dieulafoy; en la imagen se aprecia un mínimo punto de sangrado tacto con la mucosa, ulcerado en el vértice, sugestiva de enfermedad
que corresponde al lugar de la inyección de sustancia esclerosante. de Dieulafoy.
disease (Fig. 1). Endoscopic ultrasonography revealed form similar to that of gastrointestinal varices (8). When
the presence of a hypoechogenic tubular structure which the diagnosis is difficult to reach, endoscopic ultrasono-
corresponded to an arterial vessel with an abnormally lar- graphy and Doppler imaging may help locate the large-
ge caliber and an ulceration in its apex in contact with the caliber arterial vessel in contact with the mucosa, which
mucosa, which suggested the diagnose of Dieulafoy’s is characteristic of this lesion (9,10). In our case, this is
disease (Fig. 2). An endoscopic sclerotherapy was perfor- illustrated by the images provided by echoendoscopy.
med and two hemoclips were placed on the lesion. Recu- The initial management of Dieulafoy’s disease should
rrent bleeding with hematemesis, rectal bleeding and he- be endoscopic. Hemostasis may be equally achieved by
modynamic instability developed in the days following mechanical and thermal methods, whether these are com-
this treatment, requiring the transfusion of six concentra- bined with injection sclerotherapy or not (1). However,
tes of red blood cells. Surgical management was then de- endoscopic sclerosis cannot be considered the only thera-
cided upon, and consisted of partial gastrectomy. The peutic approach acceptable, since it does not offer the ef-
pathological study revealed the presence of an aberrant ficacy provided by the combination of sclerosis and ther-
dilated submucosal vessel, erosion of the overlying mu- mal methods (2), or by mechanical treatments (11). As
cosa, luminal thrombosis, and areas of peripheral bleed- for mechanical options, both elastic band ligation (12,13)
ing (Fig. 3). The subsequent recovery of the patient was and hemoclipping (11,14) have proven to be safe, effi-
uneventful, and bleeding has not recurred. cient and cost-effective techniques. These techniques
may be combined with Doppler imaging and ultrasono-
graphy in order to better locate the vessel, thus allowing
DISCUSSION better outcomes especially in cases where the lesion is
not apparent (15,16). In our case, endoscopic ultrasono-
The diagnosis of Dieulafoy’s disease is not always graphy confirmed the diagnosis and was of help for the
easy, especially when no active bleeding is observed du- placement of two hemoclips. However, despite an appa-
ring endoscopy. For this reason, repeat examinations may rently correct placement of hemoclips and the perfor-
be required. Norton et al. published in 1999 a series of 90 mance of an endoscopic sclerosing of the lesion, recu-
cases in which a mean of 1.9 explorations were required rrent bleeding developed, and so surgical management
before a diagnosis was reached (7). In our study, the diag- was performed as the definitive solution.
nosis appeared in the form of a nodular lesion with active In conclusion, Dieulafoy’s disease is an uncommon
bleeding, suggestive of Dieulafoy’s lesion. Nevertheless, condition that is sometimes difficult to diagnose. In these
this entity may have a presentation not allowing diagno- cases, endoscopic ultrasonography may be helpful both
sis when there is no active bleeding, or it may have a to reach a diagnosis and perform a more precise endosco-
REV ESP ENFERM DIG 2004; 96(2): 138-142
140 D. MARTÍNEZ ARES ET AL. REV ESP ENFERM DIG (Madrid)
Fig. 3.- A submucosal aneurysmal vessel identified in the surgical specimen. There is erosion of the overlying mucosa, thrombosis of the lumen, and pe-
ripheral bleeding.
En la pieza quirúrgica se identifica una vaso aneurismático submucoso con erosión de la mucosa suprayacente, trombosis de la luz y zonas de hemo-
rragia periférica.
pic approach. Surgical treatment is generally the option 5. Vázquez Iglesias, JL. Alteraciones Vasculares. En: Endoscopia Di-
gestiva Alta. Volumen I. Galcia Editorial, SA, 1992: 228-9.
of choice when endoscopy is unsuccessful and when 6. Owaki T, Kusano C, Ojiro M, Aikou T. Massive bleeding from Dieu-
there is recurrent bleeding. lafoy’s lesion of the small intestine in a child - therapy for the blee-
ding from gastrointestinal tract out of endoscopic observation. Dig
Surg 2002; 19 (4): 321-4.
7. Norton ID, Petersen BT, Sorbi D, Balm RK, Alexander GL, Gostout
REFERENCES CJ. Management and long-term prognosis of Dieulafoy lesion. Gas-
trointest Endosc 1999; 50 (6): 762-7.
1. Mumtaz R, Shaukat M, Ramírez FC. Outcomes of endoscopic treat- 8. Pohle T, Helleberg M, Menzel J, Diallo R, Vestring T, Senninger N,
ment of gastroduodenal Dieulafoy’s lesion with rubber band ligation et al. An extraordinary Dieulafoy’s lesion presenting as varices of the
and thermal/injection therapy. J Clin Gastroenterol 2003; 36 (4): 310- gastric fundus. Gastrointest Endosc 2001; 54 (6): 776-9.
4. 9. Fockens P, Meenan J, van Dullemen HM, Bolwerk CJ, Tytgat GN.
2. Kasapidis P, Georgopoulos P, Delis V, Balatsos V, Konstantinidis A, Dieulafoy’s disease: endosonographic detection and endosono-
Skandalis N. Endoscopic management and long-term follow-up of graphy-guided treatment. Gastrointest Endosc 1996; 44 (4): 437-42.
Dieulafoy’s lesions in the upper GI tract. Gastrointest Endosc 2002; 10. Nesje LB, Skarstein A, Matre K, Myking AO, Odegaard S. Dieula-
55 (4): 527-31. foy’s vascular malformation: role of endoscopic ultrasonography in
3. Palmer KR. Ulcers and nonvariceal bleeding. Endoscopy 2000; 32 therapeutic decision-making. Scand J Gastroenterol 1998; 33 (1):
(2): 118-23. 104-8.
4. Schmulewitz N, Baillie J. Dieulafoy lesions: a review of 6 years of 11. Chung IK, Kim EJ, Lee MS, Kim HS, Park SH, Lee MH, et al. Blee-
experience at a tertiary referral center. Am J Gastroenterol 2001; 96 ding Dieulafoy’s lesions and the choice of endoscopic method: com-
(6): 1688-94. paring the hemostatic efficacy of mechanical and injection methods.
REV ESP ENFERM DIG 2004; 96(2): 138-142
Vol. 96. N.° 2, 2004 ENFERMEDAD DE DIEULAFOY RECIDIVANTE TRATADA QUIRÚRGICAMENTE: 141
DIAGNÓSTICO MEDIANTE ULTRASONOGRAFÍA ENDOSCÓPICA
Gastrointest Endosc 2000; 52 (6): 721-4. Dieulafoy’s lesion with a hemoclip in a newborn infant. Gastrointest
12. Matsui S, Kamisako T, Kudo M, Inoue R. Endoscopic band ligation Endosc 2003; 57 (3): 435-6.
for control of nonvariceal upper GI hemorrhage: comparison with bi- 15. Folvik G, Nesje LB, Berstad A, Odegaard S. Endosonography-guided
polar electrocoagulation. Gastrointest Endosc 2002; 55 (2): 214-8. endoscopic band ligation of Dieulafoy’s malformation: a case report.
13. Nikolaidis N, Zezos P, Giouleme O, Budas K, Marakis G, Parouto- Endoscopy 2001; 33 (7): 636-8.
glou G, et al. Endoscopic band ligation of Dieulafoy-like lesions in 16. Ribeiro A, Vázquez-Sequeiros E, Wiersema MJ. Doppler EUS-gui-
the upper gastrointestinal tract. Endoscopy 2001; 33 (9): 754-60. ded treatment of gastric Dieulafoy’s lesion. Gastrointest Endosc
14. Lee YJ, Oh JM, Park SE, Park JH. Successful treatment of a gastric 2001; 53 (7): 807-9.
Enfermedad de Dieulafoy recidivante tratada quirúrgicamente:
diagnóstico mediante ultrasonografía endoscópica
D. Martínez Ares, J. Souto Ruzo, J. Yáñez López, P. Alonso Aguirre, C. Gómez Mata2, L. Valbuena
Ruvira1 y J. L. Vázquez Iglesias
Servicios de Aparato Digestivo, 1Anatomía Patológica y 2Cirugía General. Complejo Hospitalario Universitario Juan
Canalejo. A Coruña
RESUMEN INTRODUCCIÓN
La enfermedad de Dieulafoy constituye una causa rara pero
potencialmente muy grave de hemorragia digestiva. Se debe a
La enfermedad de Dieulafoy representa una causa
la presencia de un vaso arterial de gran calibre en la submuco- poco frecuente de hemorragia digestiva (1) que repre-
sa, en contacto con una mucosa a la que debilita y erosiona, lo senta aproximadamente el 1% de las hemorragias di-
que puede conducir a un sangrado digestivo de gran magnitud. gestivas altas no varicosas (2), cuyo grupo mayoritario,
El diagnóstico endoscópico no siempre es fácil, siendo la eco- como es bien conocido, lo representa la úlcera péptica
endoscopia una técnica que puede venir a solucionar estas difi-
cultades. Además, dado que permite localizar con gran exacti- (3). No obstante, su incidencia real no es conocida con
tud este vaso submucoso, puede contribuir a aumentar la exactitud ya que algunos casos pueden no ser correcta-
precisión del tratamiento endoscópico mediante métodos me- mente diagnosticados (4). La mayoría de estas lesiones
cánicos (hemoclips o bandas elásticas) o la combinación de suelen localizarse en la cavidad gástrica (1), aunque
métodos térmicos y la inyección de sustancias esclerosantes. pueden aparecer en otras localizaciones del tubo diges-
Presentamos a continuación un caso que ilustra perfecta-
mente esta aplicación de la ultrasonografía endoscópica, defi- tivo como duodeno, yeyuno o incluso el recto. Esta en-
niendo perfectamente el sustrato morfológico de esta entidad. tidad es poco frecuente pero que puede alcanzar eleva-
das cotas de gravedad, e incluso puede tener un
desenlace fatal.
Palabras clave: Enfermedad de Dieulafoy. Ultrasonografía
Se denomina también “persistencia del calibre arte-
endoscópica. Tratamiento quirúrgico. Tratamiento endoscópi- rial”, caracterizándose por la presencia de una arteria de
co. grueso calibre que atraviesa la submucosa, discurriendo
REV ESP ENFERM DIG 2004; 96(2): 138-142
142 D. MARTÍNEZ ARES ET AL. REV ESP ENFERM DIG (Madrid)
en contacto con la mucosa (5). Mínimas roturas de esta DISCUSIÓN
mucosa (6), que generalmente se encuentra atrofiada, fa-
vorece la rotura del vaso y la subsiguiente hemorragia. El diagnóstico de la enfermedad de Dieulafoy no siem-
Estas hemorragias pueden ser únicas o recidivantes. El pre es fácil, especialmente cuando durante la endoscopia
diagnóstico es muy complicado si no se objetiva hemo- no se aprecia sangrado activo, y puede requerirse la repe-
rragia activa, ya que puede no verse una lesión evidente tición de la exploración. Norton y cols. publicaron en
en la mucosa (5). Inicialmente suele realizarse un trata- 1999 una serie de 90 casos en las que se precisaron una
miento endoscópico con esclerosis asociada o no a coa- media de 1,9 exploraciones para alcanzar el diagnóstico
gulación con métodos térmicos o tratamiento mediante (7). En nuestro caso se presentó bajo la forma de una le-
métodos mecánicos (hemoclips o bandas elásticas). sión con cierto aspecto nodular y con sangrado activo,
Cuando no se consigue controlar de este modo la hemo- todo ello muy sugestivo de una lesión de Dieulafoy, pero
rragia o esta recidiva, suele indicarse la cirugía con resec- esta entidad puede presentar un aspecto que le haga pasar
ción del segmento afecto. totalmente despercibido si no hay hemorragia activa o
adoptar un aspecto tan abigarrado que simule el de las va-
rices gástricas (8). Cuando existen dudas para el diagnós-
tico la ultrasonografía endoscópica y el doppler pueden
CASO CLÍNICO ser de gran ayuda para localizar el vaso arterial de gran
calibre en contacto con la mucosa que define esta lesión
Se trata de un varón de 39 años con dos ingresos pre- (9,10); este hecho queda perfectamente ilustrado con las
vios, nueve y cuatro años antes, por HDA secundaria a espectaculares imágenes ofrecidas por la ecoendoscopia
enfermedad de Dieulafoy, uno de los cuales había reque- en el caso que presentamos.
rido intervención quirúrgica. No refería otros antece- El tratamiento inicial de la enfermedad de Dieulafoy
dentes personales de interés, negaba ingesta etílica, taba- debe ser endoscópico. La hemostasia puede lograrse con
quismo u otros hábitos tóxicos. Negaba asimismo similar eficacia con métodos mecánicos y con métodos
consumo de AINE y de cualquier otro fármaco. térmicos combinados o no con la inyección de sustancias
En esta ocasión había consultado por un cuadro de 3 esclerosantes (1). De lo que no existe duda alguna en este
días de evolución caracterizado por un síndrome ané- momento es de que la esclerosis endoscópica como única
mico intenso acompañado de deposiciones de carácter actitud terapéutica no es aceptable, ya que su eficacia es
melénico. La analítica reflejaba una anemia severa con claramente inferior a la combinación de esclerosis y mé-
un hematocrito del 25% (38-50) y una hemoglobina de todos térmicos (2), y de los tratamientos mecánicos (11).
7,5 g/dl (13,5-18). En la endoscopia alta urgente se ob- En relación con estos últimos, tanto la colocación de ban-
jetivó una lesión protuyente con mucosa conservada en das elásticas (12,13), como la colocación de hemoclips
la unión de cuerpo y fundus, sin sangrado activo en ese (11,14), se han mostrado como técnicas seguras, muy efi-
momento y que parecía corresponder a una enfermedad caces y con escasos costes. Estas técnicas pueden apoyar-
de Dieulafoy (Fig. 1). En la ecoendoscopia se describió se en el doppler y en la ultrasonografía endoscópica para
una estructura tubular hipoecogénica, que correspondía la localización del vaso con mayor precisión y de esta
al vaso arterial con calibre anormalmente grande en forma mejorar los resultados, especialmente en los casos
contacto con la mucosa, ulcerado en el vértice, sugesti- en los que la lesión es poco evidente (15,16). En nuestro
va de enfermedad de Dieulafoy (Fig. 2). Se realizó es- caso, la ultrasonografía endoscópica nos confirmó el
cleroterapia endoscópica y fueron colocados dos hemo- diagnóstico y guió la colocación de dos hemoclips. A pe-
clips sobre la lesión. El paciente presentó en los días sar de que su colocación aparentemente fue precisa y de
posteriores una recidiva hemorrágica, con hematemesis que también se había realizado esclerosis endoscópica
y rectorragias, presentando inestabilidad hemodinámi- sobre la lesión, se produjo una recidiva hemorrágica, mo-
ca y requiriendo transfusión de 6 concentrados de he- tivo por el que se optó por la cirugía como solución defi-
matíes. Por este motivo se decidió realizar un trata- nitiva.
miento quirúrgico. La intervención consistió en una En definitiva, la enfermedad de Dieulafoy es una enti-
gastrectomía parcial, y en el estudio anatomopatológi- dad poco frecuente, en la que el diagnóstico no siempre
co se objetivó un vaso aneurismático submucoso con es fácil, y en la que la ultrasonografía endoscópica puede
erosión de la mucosa suprayacente, trombosis de la luz ser útil tanto en el diagnóstico como para guiar una más
y zonas de hemorragia periférica (Fig. 3). La evolución precisa terapéutica endoscópica. Cuando esta fracasa o
posterior del enfermo fue satisfactoria, sin evidencia de existe una recidiva hemorrágica el tratamiento definitivo
recidiva hemorrágica. suele ser el quirúrgico.
REV ESP ENFERM DIG 2004; 96(2): 138-142
You might also like
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Ulkus PeptikDocument26 pagesUlkus PeptikKang MunirNo ratings yet
- Daram2013 Article BenchtopTestingAndComparisonsADocument9 pagesDaram2013 Article BenchtopTestingAndComparisonsAJorge CisnerosNo ratings yet
- GI Bleeding (Text)Document11 pagesGI Bleeding (Text)Hart ElettNo ratings yet
- EN CS 4 DA NL FR DE EL HU IT NO PL PT ES SV: MedicalDocument48 pagesEN CS 4 DA NL FR DE EL HU IT NO PL PT ES SV: MedicalKhushboo WarhadeNo ratings yet
- Overview of MalloryDocument10 pagesOverview of MalloryVivi Maulidatul AzizahNo ratings yet
- Philippine Consensus Statements On The Management of Non-Variceal Upper Gastrointestinal Bleeding 2012Document13 pagesPhilippine Consensus Statements On The Management of Non-Variceal Upper Gastrointestinal Bleeding 2012Danica Nicole Seco Gabon100% (1)
- Mallory Weiss Syndrome PDFDocument10 pagesMallory Weiss Syndrome PDFKarlon Moses Delfin PiniliNo ratings yet
- Endoscopic Skills Training in A Simulated Clinical.8Document6 pagesEndoscopic Skills Training in A Simulated Clinical.8Alberto Kenyo Riofrio PalaciosNo ratings yet
- Hematemesis Melena (Upper Gi Bleeding)Document134 pagesHematemesis Melena (Upper Gi Bleeding)Mardoni Efrijon100% (1)
- Postpyloric Feeding Access in Infants And.4Document7 pagesPostpyloric Feeding Access in Infants And.4Yazmin TorresNo ratings yet
- CME Upper GI BleedDocument46 pagesCME Upper GI Bleedfarah fadzilNo ratings yet