Professional Documents
Culture Documents
Sediment Urinar
Uploaded by
George CîciuOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Sediment Urinar
Uploaded by
George CîciuCopyright:
Available Formats
CLS 1521 AND CLS 1531
URINALYSIS (Part 2)
Objectives with narrative and illustrations.
All objectives are cognitive, unless identified as being psychomotor. he student,
at the end of each instructional component, whether in the classroom or lab, is
responsible for meeting the objectives. All student that achieves a cumulative
score of !"# or better on all problem sets, case studies, major e$ams, %ui&&es,
and library assignments are deemed to have met the objectives of this course.
2-94 DESCRIBE THE TYPES OF PROTEINS FOUND IN URINE.
'rine contains very little protein, up to ()" mg in a 2* hour period. Over the
course of 2* hours, urine will contain from (." to ()." mg of protein+d,. Proteins
that are found in the glomerular filtrate have a molecular weight of -",""" or
less. ,arger proteins are non.filterable. One estimate states that a given urine
specimen will contain about /*# albumin and 00# globulins. Other resources
state that albumin is a true small molecular weight protein and will be the
dominate protein in urine. he urinary tract produces three proteins of interest1
(() amm.2orsfall protein, (2) uro3inase (a fibrinolytic en&yme), and (/)
secretory 4gA (immunoglobulin of the renal tubular epithelial cells). Other
proteins reported are from the prostate, seminal vesicles, and vagina.
2-95 DISCUSS THE CLINICAL SIGNIFICANCE OF PROTEIN FOUND
IN URINE.
Protein testing of urine is important because it tends to be denotative of renal
disease. he fact that a test is positive does not mean the patient has a renal
disorder but that additional testing is necessary. A positive protein test of a
random urine specimen is more significant than a first morning specimen. he
presence of protein in urine is 3nown as proteinuria. he major reasons for
pathologic proteinuria are1 (() damage to the glomerular membranes, (2) tubular
disorders characteri&ed by altered tubular reabsorption mechanisms, and (/)
increases in the serum levels of low.molecular weight proteins, which gives rise to
several types of proteinuria1 overflow, renal, glomerular, tubular, post.renal, and
orthostatic. he amount of protein loss that can occur in the urine varies from
".() grams to 2"." grams per day. 4n most cases of proteinuria, protein loss does
not e$ceed *." grams per day.
2-96 DSCUSS ORTHOSTATIC PROTEINURIA.
Also 3nown as functional or postural proteinuria, it is a non.pathogenic condition
associated with the upright position and disappearing when the hori&ontal or
supine position is assumed. he daily protein loss usually does not e$ceed (."
gm+d,, but has been reported at (.) gm+d,. his is a disorder of young adults. o
diagnose this disorder, collect a urine specimen immediately after rising. his
will be negative for protein. 5ollect a second specimen / or * hours after rising.
his will be positive. Patients should be monitored every si$ months and re.
evaluated. his may be due to blood pressure phenomenon in the renal vein when
in the upright position.
2-97 DISCUSS OVERFLOW PROTEINURIA.
Overflow proteinuria (also called 6pre.renal6 or 6overload6 proteinuria) is the
conse%uence of increased amounts of low.molecular weight plasma proteins
passing through the glomerular membranes into the urine. his phenomenon can
be the result of a number of conditions1 (() hemolytic transfusion reaction
episode, (2) muscle trauma that causes myoglobin to also appear in the urine,
and (/) acute.phase reactant proteins due to surgery, myocardial infarctions, or
bacterial septicemia.
Note: Acute-phase reactat prote!s are: he"o#$o%!& C-react!'e
prote!& (1-at!tr)ps!& *!%r!o#e& a+ hapto#$o%!, -hese are
or"a$$) occurr!# prote!s, .ther prote!s are a%or"a$& $o/-
"o$ecu$ar /e!#ht prote!s *ro" $!#ht-cha! +!seases 0e1a"p$e: "u$t!p$e
")e$o"a2,
2-93 DISCUSS GLOMERULAR PROTEINURIA.
his is the most common and serious of the proteinuria7s. 8ost of the protein
found in this disorder is albumin and usually referred to as 6albuminuria6. here
is an increase in glomerular permeability due to injurious effects upon the
glomerular capillaries. 5auses for such injuries includes (() immune comple$es
resultant of multi.systemic diseases as 6systemic lupus erythematosus6 or 6sic3le
cell anemia69 (2) primary glomerular disease, as 6minimal change disease6 or
6focal glomerulosclerosis69 (/) infectious diseases, as 6hepatitis6, malaria, or
bacterial endocarditis69 (*) drug injury, as seen with penicillin, lithium, or
chloramphenicol9 ()) pre.eclampsia9 and (0) transplant rejection. :lomerular
proteinuria can be progressive and if progressive, the amount of protein loss
increases, with losses up to *." gm+day possible. 4f the loss of protein (albumin)
;2." gm+day, then the patient may e$perience edema. his disorder can progress
and develop into nephrotic syndrome or if the glomeruli are destroyed, then renal
failure and proteinuria ceases.
4f the loss of protein is <(." gm+day and is due to a disturbance in the glomerular
apparatus, with no evidence of renal disease, then this condition is designated as
6functional proteinuria6. Also called 6benign proteinuria6, this condition is
thought to be caused by blood flow changes in the glomerulus or slight changes in
permeability. his type of protein loss is seen in pyre$ia, e$posure to cold, heavy
physical activity or e$ercise, congestive heart failure, emotional stress,
hypertension, and atherosclerosis. his type of proteinuria usually resolves itself
over time with care and treatment.
2-99 EXPLAIN WHAT IS MEANT BY SELECTIVE PROTEINURIA.
=elective proteinuria is associated with glomerular proteinuria. 4f the disease is
6non.progressive6 and the si&e of protein molecules being lost are correlated to
the si&e and number of lesions in the glomerulus, then glomerular proteinuria is
designated as 6selective proteinuria6. 4f severe proteinuria is present, with all
3inds of si&es of protein molecules, then the proteinuria is designated as 6non.
selective6.
2-144 DISCUSS TUBULAR PROTEINURIA.
>esults when the normal tubular protein reabsorptive functions are impaired.
=mall molecular weight proteins will appear in the urine. ?$amples of the more
common small proteins that are lost are1
(() @2.microglobulin A8B C ((,0""D,
(2) lyso&yme A8B C (*,)""D,
(/) E2.microglobulin A8B C 2!,""",
(*) E(.acid glycoprotein A8B C *","""D,
()) retinol binding protein A2(,"""D.
he protein loss per day is < 2.) grams. 5ommon causes of tubular proteinuria
include1
(() lupus erythematosus,
(2) galactosemia,
(/) heavy metal poisoning (mercury, cadmium, or lead),
(*) antibiotics (penicillin, sulfonamides, or cephalosporins),
()) muscle trauma,
(0) transfusion reaction,
(!) renal tuberculosis.
his type of proteinuria can be diagnosed by identifying the presence of lyso&yme
or @2.microglobulin. 4f this proteinuria is designated as the acute type, it is
usually reversible with treatment. Acute tubular proteinuria may be seen in acute
pancreatitis or burns. here is a chronic tubular proteinuria. 4ts prognosis is
more serious and may not clear up with treatment. his form of proteinuria is
seen in Fanconi7s syndrome, chronic pyelonephritis, or sarcoidosis.
2-141 DISCUSS POST-RENAL PROTEINURIA.
A disorder that is associated with inflammation in any part of the urinary tract
other than the 3idney. his can result for tissue injury due infections, trauma, or
tumors that allow proteins to 6lea36 into the urinary tract. A diagnostic feature of
this proteinuria is the presence of 6pus6 cells and+or malignant cells in the urine
specimen. >ed blood cells are not a reliable indicator of this type of proteinuria.
2-142 DISCUSS THE IMPORTANCE OF TESTING FOR
MICROALBUMINURIA.
he use of the term 6microalbuminuria6 implies a proteinuria that is not detected
with the usual screening tests used in the urinalysis lab. A patient is designated as
having 6microalbuminuria6 when tests can detect /" to /"" mg of albumin over a
2* hour period in at least two of three specimens over a si$ month period. he
value of detecting this disorder is its correlation to diabetes mellitus. 4f renal
complications are 6silent6 and 6insidious6, being brought on by the presence of
glucose in the urine, the detection of microalbuminuria provides the physician a
clue to implement corrective treatment and better stabili&e the diabetic patient.
Failure to intervene will often lead to diabetic neuropathy.
2-143 BRIEFLY DISCUSS TESTING METHODS FOR
MICROALBUMINURIA.
=ensitive testing methods include en&yme immunoassay, radioimmunoassay, and
fluorescent techni%ue. here are two commercial sensitive screening methods
available.
a. A tablet method (available from Ames) that can detect *." to G." mg
albumin per d,. 'rine and water are placed on top of the tablet and
observed for the appearance of a blue.green color. A color chart is provided
for semi.%uantification.
b. An immunochemical strip reagent test (available from Hoehringer.
8annhein) can detect (." to 2." mg albumin per d,. An antibody.en&yme
conjugate is used to produce a red color. A color chart is provided for
semi.%uantification.
2-144 DESCRIBE BENCE-JONES PROTEINS AND EXPLAIN WHY
IT APPEARS IN THE URINE.
Hence.Iones protein is a low.molecular weight (8B is < **,"""),
immunoglobulin para.protein (either a 3appa or lambda monoclonal light.chain
type) that is abnormally produced in patients with multiple myeloma, primary
amyloidosis, lymphoreticular neoplasms, or macroglobulinemia disorder. his
protein is readily filtered from the glomerular capillaries and possesses uni%ue
solubility properties.
2-145 DESCRIBE AND/OR PERFORM THE CLASSICAL HEAT
SCREENING TEST FOR BENCE-JONES PROTEINS.
Hegin with clear urine (centrifuging or filtering if necessary) and transfer ) to ("
m,s to a large test tube. 2eat in a water bath to a temperature up to 0"
o
5 and
observe for turbidity. 4f Hence.Iones (HI) proteins are present, flocculation will
occur between *"
o
5 and 0"
o
5. 5ontinue heating, bringing the bath to boiling
temperature. he flocculated HI protein will disappear and the urine will be clear.
(JO?1 4f flocculation is still present, there may be other interfering proteins and
the sample should be filtered hot.) Allow the hot, but clear urine specimen to
cool. Observe the behavior as the temperature cools to 0"
o
5. HI proteins will re.
flocculate between *"
o
5 and 0"
o
5. ?lectrophoresis is the best testing method for
detecting HI proteins.
2-146 DISCUSS THE REAGENT STRIP TEST REACTION FOR
PROTEIN.
he reagent strip test employs a indicator dye (tetrabromphenol blue or
/7,/6,)7,)6.tetrachlorophenol./,*,),0.tetrabromosulfonphthalein) in an acidic
buffer to maintain a constant p2 of appro$imately /.". ?ither dye at this p2
value is yellow in color. Albumin is the principle protein measured by the strip,
the globulins and non.albumin proteins have little or no influence. he strip will
not detect HI proteins. Albumin is a hydrogen ion acceptor and will remove
hydrogen ions from the indicator dye causing it to change from yellow to blue.
green. he intensity of the color change is proportional to the amount of protein
in the urine specimen. his testing procedure is sensitive enough to detect ) . ("
mg protein per d,. his testing principle is referred to as 6the protein error of
indicator6. his means that at a certain p2, one color appears with protein
present, but a different color if protein is absent. est readings are reported out
as1 negative, trace (< /" mg+d,), (K (/" mg+d,), 2K (("" mg+d,), /K (/""
mg+d,), and *K (2""" mg+d,).
2-147 LIST CAUSES FOR FALSE-POSITIVE AND FALSE-NEGATIVE
RESULTS WITH PROTEIN REAGENT STRIP TESTING.
5a$se-pos!t!'es1 (() an elevated p2 (L-.") will override the buffer system...
urine specimen should be re.adjusted to !." and retested, (2) %uaternary
ammonium compounds, (/) detergents, and (*) over wetting of the pad (which
leaches out the buffer salts).
5a$se-e#at!'es1 (() elevated specific gravity due to increases 6salts6 may
override the buffer system and cause a lowering of the reading, (2) globulins and
non.albumin proteins present and albumin is absent, (/) polyuria Adilutes out the
protein is non.detectable levelsD,
2-143 DISCUSS AND/OR PERFORM THE KINGSBURY-CLARK
SULFOSALICYLIC ACID SEMI-QUANTITATIVE TURBIDITY
METHOD.
=ulfosalicylic acid (==A) is a wea3 acid, capable of precipitating protein in urine.
his procedure re%uires the addition of /." m,s of /."# ==A to (." m, of clear
urine. he sample is mi$ed and allowed to 6sit6 for five minutes. here are
variations of this procedure and regardless of which procedure used, the final
concentration of urine and ==A will be about () mg of ==A+m, of total solution.
he patient7s sample can be graded on a scale of negative (up to !.) mg+d,), trace
(M2" mg+d,), (K (/" to ("" mg+d,), 2K (("" to 2)" mg+d,), /K (2"" to *)"
mg+d,), and *K (; *)" mg+d,). 5ommercial standards are available that range
from (" mg+d, to ("" mg+d,. his is not a sensitive test, re%uiring 2" mg
protein+d, or higher (regardless of the type of protein present). N.-6: I* the p7
!s 83,4& a+9ust the p7 to 5,4 a+ procee+ /!th the SSA "etho+,
2-149 LIST CAUSES OF FALSE-POSITIVE AND FALSE-NEGATIVE
RESULTS FOR THE SSA PROCEDUR?.
5a$se-pos!t!'es1 (() 4odine based $.ray contrast media, (2) plasma volume
e$panders, (/) intravenous albumin, (*) antibiotics Asulfiso$a&ole or :antrisin,
penicillin, cephalosporinsD, ()) tolbutamide and its metabolites.
5a$se-e#at!'es1 (() highly al3aline urine Ap2 LG."D, (2) elevated specific
gravity due to high salt concentrations.
2-114 COMPARE AND APPRAISE TEST RESULTS BETWEEN SSA
AND THE REAGENT STRIP.
Test Strip SSA Probable
cause
Positive Positive Proteinuria
Jegative Jegative Jo proteinuria
(K Jegative Proteinuria, but li3ely not pathogenic
Jegative Positive 8ay be a false positive or Hence.Iones
protein. 5onfirm with appropriate
tests.
2-111 LIST WHICH TESTS CAN BE CORRELATED WITH THE TESTS FOR
PROTEIN.
A(D Hlood, A2D leu3ocytes, A/D nitrites, and A*D microscopic.
7IS-.RICAL IN-6R6S-
ests for protein in the past have usually been non.specific, failing to
differentiate between the types of protein present. hat is not the case in
todayNs laboratory. he reagent strip test detects albumin and
electrophoresis technology can differentiate between albumins and types of
globulins. ?arlier testing procedure employed use of heat and an acid
(usually acetic acid). he urine specimen was heated in the upper portion of
a test tube and a drop or two of //# acetic acid was added. 4f phosphates
were present, a cloudiness could be initially observed. Addition of acetic acid
with heating dissipated the phosphates. 4f protein was present, then a white
cloudiness remained in the OhotP portion of the tube. ?arly testing was
refined by using saturated Ja5l to prevent precipitation of mucin. Acetic
acid was added to dissolve the phosphates and carbonates. he application
of heat to the upper tube of acidified urine would precipitate the protein
which would be observed as a white cloud. his test with Ja5l and acetic
acid was the PurdyNs heat test. he 2eller test was developed, a layering of
concentrated nitric acid on the top of a test tube of urine would produce a
white ring of precipitate at the interface. A modification of the 2ellerNs test
occurred with 8g=O* was incorporated as part of the reagent. he
procedure of layering the reagent and urine specimen remained the same
and a white ring of precipitate constituted a positive test. 8odifications
followed with trichloroacetic acid and sulfosalicylic acid. he Qingsbury.
5lar3 procedure then developed using sulfosalicylic acid.
2-112 DISCUSS THE IMPORTANCE OF TESTING FOR BILIRUBIN
IN URINE.
Hilirubin is a normal brea3down product of hemoglobin metabolism. his
degradation process re%uires that bilirubin be conjugated in the liver. 4f clinically
significant levels of bilirubin are detected in the urine, then further clinical
investigation is recommended to detect hepatitis, cirrhosis, gallbladder disease,
and cancer. 4n healthy individuals, trace amounts of bilirubin may be found in
urine, but routine testing methods do not detect these clinically insignificant
levels.
2-113 WRITE OR DESCRIBE A BRIEF OVERVIEW OF THE
CATABOLISM OF HEMOGLOBIN TO UROBILINOGEN.
he life span of an erythrocyte is about (2" days. Bhen the >H5 begins to
brea3down, it is removed from circulation by the reticuloendothelial system and
hemoglobin liberated. he hemoglobin molecule is bro3en into heme and
globulin. 2eme is converted to a protoporphyrin compound and the heme ring is
opened to form verdoglobin (choleglobin), 4ron is split away and a linear, non.
conjugated, tetrapyrrole called biliverdin is formed. A reduction reaction converts
biliverdin to bilirubin, an insoluble, yellow pigmented compound. At this stage,
bilirubin is a yellow molecule, non.conjugated and alcohol soluble (which cannot
be e$creted by the 3idneys). As bilirubin is released into circulation it
spontaneously conjugates with albumin. 4n the liver, bilirubin is conjugated with
glucuronic acid, forming a water soluble, bilirubin diglucuronide or bilirubin
monoglucuronide. 4f this conjugated bilirubin re.enters blood circulation, it is
e$creted at the 3idney. 8ost conjugated bilirubin is secreted into the bile system,
where it is temporarily stored in the gallbladder and released into the duodenum.
4n the small intestine, bilirubin is reduced to stercobilinogen, mesobilinogen, and
urobilinogen by bacterial activity. 5ollectively these three colorless, water soluble,
tetrapyrroles are called urobilinogen. hese three OurobilinogensP are o$idi&ed
and e$creted in the final form as stercobilin, mesobilin, and urobilin. he 6bilins6
are orange.brown pigments and contribute to the color of the stool. =ome of the
6urobilinogens6 are reabsorbed (about 2"#) into the blood, returned to the liver.
Appro$imately )# is re.e$creted in the bile and the remainder e$creted in the
3idney as 6urobilinogen6. 6'robilinogen6 is o$idi&ed to urobilin, stercobilin, and
mesobilin (forming part of the urine pigments).
2-114 EXPLAIN WHY CONJUGATED AND NON-CONJUGATED
BILIRUBIN IS CLINICALLY SIGNIFICANT IN URINE TESTING.
Rependent upon the disorder, the presence or absence of conjugated and non.
conjugated bilirubin are clues to successful diagnosis. Hilirubin is normally
e$creted in urine, but in amounts that escape detection by routine screening
methods. 5onjugated bilirubin will appear in the urine only if the integrity of the
bile duct or hepatocytes have been compromised.
A. 4f the bile duct is occluded, conjugated bilirubin cannot pass into the small
intestine and 6urobilinogens6 are not formed. A build up of conjugated
bilirubin means that increased amounts will escape into blood circulation
and be e$creted by the 3idney in significant amounts. =ince conjugated
bilirubin is not passing into the intestine, 6urobilinogens6 are absent and are
not being reabsorbed. A strip test positive for bilirubin and negative for
urobilinogen is suggestive of a bile duct obstruction.
H. 4f the integrity of the liver has been compromised, it does not function as
efficiently. 5onjugated bilirubin is being transferred by the liver into the bile
duct, but at a slower rate, allowing this bilirubin to build.up and some will
pass into the peripheral blood. 5onjugated bilirubin is readily e$creted by
the 3idney7s. he 6urobilinogens6 that are formed and reabsorbed are not as
efficiently recovered and returned to the bile. Peripheral blood levels of the
6urobilinogens6 are increased, resulting in more being e$creted by the
3idney7s. A strip test positive for bilirubin will also be positive for
urobilinogen, supportive of some type of liver cell dysfunction (as in hepatitis
or cirrhosis).
5. 4f a patient e$periences a transfusion reaction or a hemolytic disease crisis,
numerous >H57s will hemoly&e, releasing increased amounts of hemoglobin
in the blood. 4n the degradation of 2emoglobin, large amounts of bilirubin
are formed, overwhelming the ability of the body to rapidly conjugate it. he
e$cess unconjugated bilirubin is absorbed into the tissues giving a jaundice
appearance to the s3in, sclera, body fluids, and tissues. 'nconjugated
bilirubin cannot be e$creted by the 3idneys. he liver is functioning normally
and the conjugated bilirubin is entering the intestines in larger %uantities.
his means that more 6urobilinogens6 are being reabsorbed. his in turn
means that the 3idney7s will e$crete larger %uantities. he strip test will be
negative for bilirubin, but positive for urobilinogen.
2-115 EXPLAIN CHEMICAL REACTION OF THE REAGENT STRIP
TEST FOR BILIRUBIN.
he testing strategy is based upon the dia&o reaction. he dia&o reaction is
dependent upon presence of a dia&o group (CJK or CJ.). 4n this testing
procedure, the pads contain a dia&onium salt (2,*.dichloroanailine dia&onium
salt or 2,0.dichloroben&ene.dia&onium.tetrafluoroborate). he dia&onium
reagent is stabili&ed by acidic buffers. Bhen the reagent reacts with bilirubin, an
a&odye (a&obilirubin) is formed that produces colors ranging from tan, to light
brown, or pin3 or purple. A commercial color chart is used to measure the
reaction. >esults are reported as negative, (K (small), 2K (moderate), and /K
(large). he reagent strip test can detect as little as ".* mg urinary bilirubin+d,.
2-116 DISCUSS AND/OR PERFORM THE ICTOTEST PROCEDURE.
he 4ctotest is a tablet test that uses the same strategy as the reagent strip test,
but is about four times more sensitive, detecting concentrations bilirubin as low
as ".") mg+d,. he tablets use p.nitroben&ene.dia&onium.p.toluenesulfonate as
the dia&onium salt. en drops of urine are placed on the absorbent mat to 6trap6
and concentrate the bilirubin in the fibers. he tablet is placed in the center of the
moistened spot and a drop of water added. 4f the drop spills over the edge of the
tablet and flows on the mat, a second drop may not be re%uired. A second drop of
water is added to the first drop to cause the water+solution to overflow. he
drop(s) of water leach the reagents out of the tablet to form a reactive solution.
he test is read after 0" seconds. A blue or purple color produced on the mat is a
positive test. Any other color is considered to be negative.
2-117 LIST CAUSES FOR FALSE-POSITIVE AND FALSE-NEGATIVE
RESULTS IN BILIRUBIN TESTING.
5a$se-pos!t!'es1 (() urine pigments, (2) ,odine, (/) indican, (*) 8edications as
chlorproma&ine, phena&opyridine, or etho$a&ene. (Jote1 5olors from other
chemicals may interfere with test interpretation if bilirubin is also present.)
5a$se-e#at!'es1 (() urine e$posed to light, (2) urine e$posed to air, (/) elevated
levels of ascorbic acid (bloc3s dia&o reaction), (*) elevated nitrate levels (bloc3s
dia&o reaction).
N.-6: -he Ictotest te+s to %e *ree *ro" "ost !ter*er!# su%staces
s!ce the %!$!ru%! !s co$$ecte+ o the sur*ace o* the "at a+ the other
co"poets o* the ur!e are /ashe+ to/ar+ the ceter o* the "at,
2-113 DISCUSS THE FOAM TEST.
'rine that contains bilirubin ta3es on a dar3 yellow or amber color. 4f the urine is
sha3en and the foam observed, the foam ta3es on the color of the urine. his test
is not reliable since medications can cause the foam to be colored.
2-119 LIST WHICH TEST CAN BE CORRELATED WITH THE
BILIRUBIN TEST.
'robilinogen
2-124 DESCRIBE THREE CHARACTERISTICS OF THE TWO FORMS
OF BILIRUBIN.
FREE BILIRUBIN CONJUGATED BILIRUBIN
A(D non.polar (water insoluble) polar (water soluble
A2D not e$creted in urine e$creted in urine
A/D does not stain tissue stains tissue
7!stor!ca$ Iterest
here are three types of test conducted for bilirubin over the decades. One
type re%uired blending yellow bilirubin with a dye as methylene blue and
measuring the dye dilution. A second method employed o$idation
techni%ues, and the third method was coupling bilirubin to a reagent to
produce a brightly colored chromogen (called dia&oti&ation). he
dia&oti&ation method was found to be the most reliable. One of the earlier
tests for urine bilirubin was the :melin test. his re%uired precipitation of
the bile pigments with a ("# solution barium chloride in 2" m,s of urine.
he solution was filtered and the filter paper spread on a dry filter paper.
A drop of yellow nitric acid as added to the center of the filter paper. 4f
bilirubin was present, a display of colors occurred with green on the
periphery, followed by blue, violet, red, and yellow (in this order to the
center). 4f the green color display was absent, then the reaction was
negative for bilirubin. he dye dilution method re%uired adding drops of
".2# methylene blue to a first morning specimen. 4n a normal urine, the
first drop or two would turn the urine green then on the third or fourth
drop the urine would turn blue. 4f bilirubin was present, the urine would
hold green longer, re%uiring more than four drops of dye. Four drops or
less of methylene blue would be reported as negative, whereas ) or more
drops would be a positive test.
2-121 DISCUSS THE IMPORTANCE OF UROBILINOGEN TESTING.
'robilinogen is a bile pigment, a product of heme degradation. 4t is formed in the
intestines by the reduction reactions of bacteria on bilirubin. 'robilinogen is
normally present in the urine in concentrations < 2.) mg+d,. 'robilinogen
testing is basically limited to screening tests that help detect early liver disease
and hemolytic disease (including transfusion reactions). here is little value in
performing %uantitative tests on urobilinogen since there are better and more
specific liver function tests.
2-122 DISCUSS THE REAGENT STRIP TEST FOR UROBILINOGEN.
he reagent strip test was originally developed using the ?hrlich7s test concept.
?hrlich7s reagent is p.dimethylaminoben&aldehyhde (RAH) and is employed in
the test pad with an acidic buffer. 4n the presence of urobilinogen, the pad turns
from a light pin3 to a dar3 pin3 color. p.dimethylaminoben&aldehyde is non.
selective and will react with a number of substances, termed as 6?hrlich.
reactive6. Another chemical, *.metho$yben&ene.dia&onium.tetrafluoroborate
(8R), is used in other reagent test strips and had been found to be more
specific, with fewer false positives. A positive reaction will produce pin3 to red
color. 4f ?hrlich.reactive substances is present in the urine sample, they will
interfere with the RAH reaction, producing a falsely elevated value. ?hrlich.
reactive substances generally are non.reactive with the 8R reaction. he
reagent strip test should not be used to determine the absence of urobilinogen
(seen in bile duct obstruction).
2-123 LIST CAUSES FOR FALSE-POSITIVES AND FALSE-
NEGATIVES IN UROBILINOGEN TESTING WITH -
DIMETHYLAMINOBEN!ALDEHYDE "EHRLICH#S REAGENT$.
5a$se :os!t!'es1 (() porphobilinogen, (2) indican, (/) bilirubin, (*) indole, ())
sulfonamides, (0) p.aminosalicylic acid, (!) methyldopa, (G) procaine, (-) ).
hydro$y.indole acetic acid, ((") chlorproma&ine.
N.-6: -he presece o* 012 phea;op)r!+!u"& 022 a;o+)es <r!%o=a'!&
!tro*urato!& a+ etho1a;ee2& a+ 032 re+ %eets ca "as> the
uro%!$!o#e pa+ /!th a re++!sh co$or& caus!# a *a$se pos!t!'e,
5a$se-e#at!'es1 (() formaldehyde, (2) improper storage, and (/) high nitrite
levels.
2-124 BRIEFLY DESCRIBE HOW THE LABORATORY MAY TEST
FOR THE ABSENCE OF UROBILINOGEN.
=ince testing urine cannot validate the absence of urobilinogen, fecal testing will
verify the absence or presence of urobilinogen. 5hemical testing for bilirubin will
be helpful
2-125 LIST DISORDERS IN WHICH UROBILINOGEN MAY BE
ELEVATED OR ABSENT.
?levated in (() hemolytic anemia, (2) cardiac infarction, (/) sic3le cell anemia, (*)
pernicious anemia, ()) cirrhosis of the liver, and (0) hepatitis.
Absent in (() cholestasis (bile duct obstruction), (2) starvation, (/) hepatitis with
cholestasis, (*) fibrosis.
2-126 EXPLAIN THE CLINICAL SIGNIFICANCE OF
PORPHOBILINOGENS.
Porphobilinogens are the precursors of porphyrins which are intermediates in the
biosynthesis of hemoglobin. he basic structure of the porphobilinogens is a
pyrrole ring and four pyrrole rings will be combined to form a linear molecule
which has the capability to undergo cycli&ation and form uroporphyrinogen
which will undergo a series of reactions to form protoporphyrin 4S, which can
chelate iron. Bhen iron is incorporated into the porphyrin molecule, it is called
heme. >efer to the following illustration.
4ntermediates in the =ynthesis of 2eme.
he porphobilinogens can spontaneously o$idi&e and if this occurs, then the
o$idi&ed porphobilinogen (biologically non.functional) must be e$creted. 4f there
is an en&yme defect in any of the reaction se%uences between glycine K succinyl.
5oA to protoporphyrinogen, this bloc3 in the synthesis pathway will cause a
deficit in some of the metabolites and an accumulation of others. here are
conse%uences to the accruing of porphobilinogens, which includes accumulation
in certain tissues and a to$ic effect upon nerves. =i$ type of porphyria7s have been
described1 acute intermittent porphyria, congenital erythropoietic porphyria,
porphyria cutanea tarda, hereditary coproporphyria, variegate porphyria, and
protoporphyria. For e$ample, if the en&yme 6uroporphyrinogen cosynthetase6 is
defective, the condition 6Acute intermittent porphyria6 will diagnosed. T.
aminolevulinic acid (A,A) and porphobilinogen (PH:) accumulates in the blood
stream and because of their low renal threshold, they will %uic3ly appear in the
urine. 4t is the PH: that is detected since screening procedures do not detect
A,A. One other point... hemoglobin acts as en&yme inhibitor in porphyrin
synthesis. 4f an en&yme is defective in the metabolic pathway, hemoglobin
production is reduced and its rate controlling effect lost which allows for the
abnormal accumulation of the porphyrins.
2-127 EXPLAIN THE DIFFERENCE BETWEEN ACQUIRED AND
HEREDITARY PORPHYRIAS.
Hereditary porphyria is due to a defective en&yme or the inability of the
tissues to produce sufficient amounts of the en&yme. here are two general types
of hereditary porphyrias1 erythropoietic, in which the effects are e$pressed in the
hemopoietic tissues. he other type is found in the liver as en&yme defects.
Acquired porphyrias are the result of an e$ternal influence upon the liver
parenchyma cells. ?$amples of e$ternal influences are (() antibiotics Apenicillin
or sulfonamidesD, (2) alcohol, (/) stilbestrol, (*) lead poisoning or other heavy
metals, ()) diabetes mellitus, (0) sedatives, (!) hypnotics, and the disease
syphilis.
2-123 DESCRIBE AND/OR PERFORM THE HOESCH TEST.
his is a simple semi%uantitative procedure in which 2./ m,s of modified
?hrlich7s reagent is added a large test tube. wo drops of fresh urine is layered
onto the reagent. A red (or deep pin3) color will form at the interface of the layers
and indicates the presence of porphobilinogen. he modified ?hrlich7s (or
2oesch) reagent consists of 2." gms of p.dimethylaminoben&aldehyde in 0."
8olar 25,.
2-129 EXPLAIN WHY THE HOESCH TEST IS A GOOD SCREENING
TEST FOR PORPHOBILINOGEN.
he 2oesch test is insensitive to urobilinogen, re%uiring L2" mg+d, to produce a
positive reaction. 4t is sensitive to porphobilinogen producing an instant color if
present and can detect levels as low as 2." mg+d,. Although the color produced is
in proportion to the amount of porphobilinogen present, it is not used as a
%uantitative test.
2-134 DESCRIBE AND/OR PERFORM THE WATSON-SCHWART!
DIFFERENTIATION TEST.
?%ual volumes (2.) m,s. each) of fresh urine and ?hrlich7s reagent are mi$ed in a
large test tube. )." m,s of saturated sodium acetate is added and the tube mi$ed
well. 4f urobilinogen, porphobilinogen, or other ?hrlich.reactive substances are
present, the solution will develop a pin3 to cherry.red color. 4f there is no color
the test is negative. 4f the color is present add the test solution to ) m,s of
chloroform in a separatory flas3 and mi$ well. he solution will separate into two
layers, a top a%ueous layer and a bottom chloroform layer. 4f there is color in the
a%ueous later, with the chloroform layer clear, then porphobilinogen or other
?hrlich.reactive substances are present. 4f the color is in the chloroform layer,
then urobilinogen is present. A second e$traction step is re%uired if the color is in
the a%ueous layer. ransfer the a%ueous layer to a second separatory funnel and
add )." m,s of butanol, mi$ing well. 4f the color remains in the a%ueous layer,
then porphobilinogen is present. 4f the color transfers to the butanol layer, then
urobilinogen or other ?hrlich.reactive substances are present. his test is more
sensitive, detecting as little as ".0 mg of porphobilinogen+d,. he results should
be reported as (() positive or negative for urobilinogen, (2) positive for
porphobilinogen, or (/) positive for both porphobilinogen and urobilinogen.
JO?1 'robilinogen is soluble in both chloroform and butanol. Porphobilinogen
is not soluble in either chloroform or butanol. :enerally ?hrlich.reactive
substances are soluble in butanol, but not chloroform.
2-131 LIST A MINIMUM OF ELEVEN EHRLICH-REACTIVE
SUBSTANCES.
(() porphobilinogen, (2) indican, (/) bilirubin, (*) indole, ()) sulfonamides, (0) p.
aminosalicylic acid, (!) methyldopa or Aldomet, (G) procaine, (-) ).hydro$y.
indole acetic acid, ((") chlorproma&ine, ((() urobilinogen
N.-6: -he presece o* 012 phea;op)r!+!u"& 022 a;o+)es
<r!%o=a'!& !tro*urato!& a+ etho1a;ee2& a+ 032 re+ %eets
ca "as> the tests *or porpho%!$!o#e %) !"part!# a re++!sh
co$or a+ cause +!?cu$t) ! !terpretat!o,
2-132 EXPLAIN THE IMPORTANCE OF UROBILIN IN URINE
TESTING.
4t has little if any importance. 4t is not found in fresh urine. 4t is the end product
of urobilinogen o$idation by air, light, or bacteria. he addition of ,ugol7s iodine
to a urine specimen will o$idi&e the urobilinogen to urobilin. he only reason to
perform a urobilin test would be to confirm the absence of urobilinogen and there
are other methods that are easier and user friendly.
2-133 DISTINGUISH BETWEEN THE TERMS %HEMATURIA% &'(
%HEMOGLOBINURIA%.
Hoth terms imply the presence of blood in the urine. 2ematuria means that intact
erythrocytes are present. 2emoglobinuria implies that erythrocytes are
hemoly&ed or absent and only hemoglobin is present.
2-134 EXPLAIN THE IMPORTANCE OF TESTING FOR BLOOD IN
URINE.
he presence of blood (>H5 and+or hemoglobin) is clinically significant.
?valuation is important to determine if the problem is pathological or non.
pathological. Hlood can enter the urinary tract at any point in the urinary system.
4f the urine is transparent and red, then this would strongly suggestive of
hemoglobinuria. 2emoglobinuria may be the result of intravascular hemolysis
because of a transfusion reaction or hemolytic anemia. Other causes of this
problem are burns, e$hausting and intense physical activity, parasite infections,
poisoning, pro$imal nocturnal hemoglobinuria, pro$imal cold hemoglobinuria,
and trauma. 4f hemoglobin is crossing the glomerulus, renal tubular cells will
reabsorb some of the hemoglobin, cataboli&e it to hemosiderin and ferritin, and
e$crete it a few days later into the urine. >enal tubular epithelial cells containing
hemosiderin can be observed in the urine sediment as.well.as hemosiderin
granules. he use of Prussian blue stain will confirm the presence of
hemosiderin. rue hemoglobinuria is an uncommon occurrence. 8ost
hemoglobin in the urine is the conse%uence of hemolysis.
2ematuria is characteri&ed by a cloudy, smo3ey colored urine. 8ajor causes of
hematuria are trauma, pyelonephritis, e$hausting and intense physical activity,
anticoagulants, malaria, appendicitis, leu3emia, thrombocytopenia, hemophilia,
3idney stones, tumors, catheteri&ation, glomerulonephritis, cystitis, acute febrile
episodes, and e$posure to to$ic chemicals. he presence of >H57s in urine may be
an indicator of early renal disease and re%uires medical follow.up. he presence
of a few (very few) >H57s in urine is generally considered to be normal. I* R@CAs
are preset& $oo> *or R@C casts,
2-135 DISCUSS HOW MYOGLOBIN APPEARS IN URINE AND ITS
SIGNIFICANCE.
8yoglobin is a small hemoprotein (8B C (!,""") that is rapidly cleared from
blood and e$creted in the urine. 4t is the result of muscle tissue trauma due to
surgery, injury crushes, to$ic action of ethanol or drug addiction, muscle tissue,
electric shoc3, muscle disease, sna3e venoms, and idiopathic paro$ysmal
myoglobinuria. 8yoglobin is readily reabsorbed by the pro$imal tubular cells.
8yoglobin has the potential to damage the 3idneys. 4t presence in urine is
pathological and should be %uic3ly identified.
2-136 DESCRIBE HOW MYOGLOBIN CAN BE IDENTIFIED AND
CONFIRMED.
A simple screening techni%ue re%uires that )." m,s of centrifuged urine (neutral
p2) be placed in a test tube and add 2.G grams of ammonium sulfate, then mi$
well. Allow the specimen to sit for five minutes. Filter and test the filtrate with a
chemical test for blood. 4f the test is positive, then myoglobin is presumed to be
present. he principle of this test lies in the fact that hemoglobin is precipitated
out in an G"# ammonium sulfate solution. he best methods for identifying
myoglobin is protein electrophoresis. Other reliable test procedures are
radioimmunoassay, absorption spectrophotometry, and immunodiffusion.
2-137 DISCUSS THE REAGENT STRIP TEST FOR BLOOD.
he hemoglobin molecule can brea3 down the pero$ide molecule and the test was
developed to ta3e advantage of this pero$idase activity. 8anufacturers use a
pero$ide (cumene hydropero$ide or 2,).dimethyl.2,).dihydropero$yhe$ane) and
the pseudopero$idase activity of hemoglobin reduces the 6pero$ide6, which in
turn o$idi&es, that is releases o$ygen to convert the reduced chromogen
(tetramethylben&idine), with no color to an o$idi&ed chromogen with a blue color.
he test is sensitive, detecting as few as ) >H57s+U, (M "."() mg hemoglobin+d,)
urine.
2-133 WHEN GIVEN DATA) DIFFERENTIATE BETWEEN
ERYTHROCYTES) HEMOGLOBIN) AND MYOGLOBIN IN URINE.
he following table of information will illustrate the parameters to differentiate
the differences.
Descr!ptor 7e"o#$o%! B)o#$o%!
R@CCs
>eagent strip test positive positive positive
Appearance of urine clear+red clear smo3ey+cloudy
Appearance of plasma pin3+red normal normal
>H57s in urine sediment " to few " to few present
=erum creatine 3inase (5Q) elevated (V) elevated (W) normal
=erum haptoglobin decreased normal normal
=erum lactate dehydrogenase (,R) elevated elevated normal
=erum ,R.( and ,R.2 elevated normal normal
=erum ,R.* and ,R.) normal elevated normal
(V) will be X (" times the upper reference limit.
(W) will be L *" times the upper reference limit.
'pper reference limit for serum 5Q in men C (/" 4'+, and for women C (()
4'+,.
'pper reference limit for serum ,R for adults range from *" to -" 4'+,
139 LIST A MINIMUM OF TEN SUBSTANCES THAT INTERFERE
WITH THE REAGENT TEST STRIP FOR BLOOD) CAUSING FALSE-
POSITIVES AND FALSE-NEGATIVES.
5a$se-pos!t!'es1 (() myoglobin, (2) o$idi&ing detergents, (/) leu3ocyte esterase,
(*) menstrual contamination, ()) hemorrhage contamination, (0) bleach, (!)
microbial pero$idases.
5a$se-e#at!'es1 (() ascorbic acid (note1 iodate is being included in reagent pad
to remove ascorbic acid so that it now re%uires mar3edly elevated levels to
interfere), (2) elevated specific gravity, (/) elevated protein levels, (*) nitrite (L("
mg+d,), ()) captopril, (0) formaldehyde, (!) vegetable pero$idase.
2-144 IDENTIFY WHAT OTHER PARAMETERS IN URINALYSIS
TESTING THAT THE BLOOD TEST CAN BE CORRELATER O.
A(D 8icroscopic sediment and A2D protein testing.
2-141 EXPLAIN THE IMPORTANCE OF TESTING FOR NITRITES
IN URINE.
Jitrites are not normally detected in the urine of healthy individuals. his test
provides a %uic3 and convenient method of screening for urinary tract infections
('4). One value that is inherent in this test is that a '4 may be asymptomatic
or the patient may be complaining of vague symptoms that would not alert an
physician to order a urine culture and sensitivity test. A word of caution.... this
test depends upon the infecting bacteria to be nitrate reducers (have the en&yme
6nitrate reductase) and not all bacteria that can cause a '4 have the nitrate
reducing en&yme .
'rine in the bladder is normally a sterile environment and sterility is supported
by the fre%uent flushing of urine from the bladder. 8ost infections are assumed
to begin in the bladder and may be resultant of infre%uent urination (oliguria),
6malfunction6 of the bladder, or some other problem. 4f a bladder infection
(cystitis) occurs, then it is possible for the infection to spread to other part of the
urinary system. 4nfections that are not detected can lead to renal tissue damage.
esting for nitrites can be a means for assessing the effectiveness of antibiotic
therapy9 the presence of a '4 (cystitis, urethritis, ureteritis, pyelonephritis, or
glomerulonephritis)9 monitoring patients at high ris3 for a '49 and screening
urine specimens for '4.
2-142 EXPLAIN THE CHEMICAL BASIS OF THE STRIP TEST FOR
NITRITES.
his test is a modified :riess reaction ((G!-) and depends upon the presence of
nitrites in the urine. he test pad contains an aromatic amine (p.arsanilic acid or
sulfanilamide) and buffers to maintain an acidic environment for the reaction to
occur. Jitrite and the aromatic amine will chemically interact (called
6dia&oti&ation6) to form an intermediate, a 6dia&onium salt6. he dia&onium salt
would then react with another chemical in the pad, a chromogen A/.hydro$y.
(,2,/,*.tetrahydorben&.(h).%uinolinD and the end product would a pin3 6a&odye6
molecule. he pin3 color (without regard to intensity) is interpreted as positive.
=ee the reaction se%uence in the following illustration.
Aromatic AmineYJ2
2
K Jitrite (JO
2
) ....; Aromatic Amine K
K
JCJ K
chromogen ......; Aromatic AmineYJCJ . chromogen (a pin3 A&o.dye)
his test pad is 6standardi&ed6 to be insensitive to the presence of < ("","""
microorganism+m, in order to eliminate false positive test results. 4f this test is
positive, then there are ; ("",""" microorganisms+m,. Any shade of pin3
represents a clinically significant number of microorganisms. his test will not
wor3 if there are no dietary nitrates in the diet of the patient. Fresh urine
specimens (in particular a first morning specimen) should always be used when
testing for nitrites.
2-143 LIST A MINIMUM OF EIGHT THINGS THAT CAN CAUSE A
FALSE-POSITIVE OR FALSE- NEGATIVE NITRITE TEST.
5a$se-pos!t!'e1 A(D presence of colored medications (pyridium), A2D
contaminating bacteria in a stool that has stood too long or improper collection,
or A/D storage of reagent strip test in an open container.
5a$se-e#at!'e1 A(D lac3 of dietary nitrate, A2D antibiotic therapy, A/D ascorbic
acid at concentrations of 2) mg+d, or greater, A*D high urinary urobilinogen, A)D
a urine p2 < 0.", A0D a urine specimen that did not stay in the bladder a
sufficient amount of time, or A!D or bacteria that do not reduce nitrate.
2-144 IDENTIFY WHAT OTHER PARAMETERS IN URINALYSIS
TESTING THAT THE NITRITE TEST CAN BE CORRELATED TO.
A(D 8icroscopic and A2D leu3ocyte esterase.
2-145 EXPLAIN THE ADVANTAGES OF TESTING FOR THE
PRESENCE OF THE EN!YME LEUKOCYTE ESTERASE.
his is a screening strategy for detecting the presence of a urinary tract infection.
he en&yme 6leu3ocyte esterase6 is produced in the granules of neutrophils and
by monocytes. he presence of this en&yme in the urine is an indicator of a
significant number of leu3ocytes. 4n an inflammatory reaction, white blood cells
increase in number and many will 6lyse6 or are otherwise destroyed in urine. he
microscopic e$amination has been the standard for detecting the BH5 activity
associated with inflammation. he leu3ocyte esterase test will detect the presence
of BH57s without their having to undergo lysis.
2-146 DISCUSS THE SIGNIFICANCE OF WBC*S IN URINE.
he urine of a healthy adult male will contain from &ero to 2 or / BH57s+high
power field (hpf) in a urine specimen that has been concentrated from (" to (2
m,s to ".) to (." m,s of urine. his will be X (" BH57s+U,. Adult female urine
will contain from &ero to five BH57s+hpf. Jormal values for children are similar
to that of the adult female. 4f the number of BH57s in a urine specimen (" to
()+hpf, this is suspicious of a '4 and should be investigated. 4f the count is L
2"+hpf, this is suggestive of a '4.
2-147 EXPLAIN THE BASIS OF THE REAGENT STRIP TEST FOR
LEUKOCYTE ESTERASE AND HOW THE STRIP TEST IS
EVALUATED.
he test uses an en&ymatic reaction principle that employs the dia&o principle as
in the nitrite and bilirubin test. he test pad contain an organic ester
(indo$ylcarbonic acid ester or pyrrole amino acid ester) embedded with a
dia&onium salt. 4f the urine specimen contains the leu3ocyte esterase en&yme, the
organic ester will be cleaved an intermediate that will react with the dia&onium
salt to produce a colored 6a&odye6, which can be measured with standardi&ed
color chart. he intensity of the color will correlate to the amount of leu3ocyte
esterase present in the urine specimen. he test result is reported as negative,
trace, (K (small), 2K (moderate), and /K (large). ?$amine the following reaction
scheme to understand the en&ymatic principle.
?ster K leukocyte esterase ....; AintermediateD K JCJ
K
.Ria&onium
salt (in an acidic buffer) .....; AintermediateDYJCJ.Ria&onium salt
(purple a&o dye)
2-143 IDENTIFY WHAT OTHER PARAMETERS IN URINALYSIS
TESTING THAT THE LEUKOCYTE ESTERASE TEST CAN BE
CORRELATED TO.
A(D 8icroscopic, A2D protein, and A/D nitrate.
2-149 LIST A MINIMUM OF TEN THINGS THAT WILL CAUSE A
FALSE-POSITIVE OR FALSE-NEGATIVE TEST RESULT ON THE
LEUKOCYTE ESTERASE TEST OR OTHERWISE OBSCURE THE
INTERPRETATION OF THE TEST.
5a$se-pos!t!'es1 (() formaldehyde, (2) o$idi&ing agents in the specimen, (/)
urine specimens containing vaginal discharges, (*) any medication that can color
the pad a violet color in an acid environment
5a$se-e#at!'es1 (() ascorbic acid Ahigh levelsD, (2) L )"" mg albumin+d,, (/)
L/." gm glucose+d,, (*) elevated specific gravity, ()) cephalosporin antibiotics,
(0) o$alic acid, (!) gentamycin, (G) tetracycline
N.-6: I* the ur!e has stro# )e$$o/ p!#"etat!o& the test pa+ "a)
ta>e o a #ree co$or, -h!s shou$+ %e !terprete+ as pos!t!'e,
2-154 COMPARE THE PRINCIPLE OF THE REAGENT STRIP TEST
FOR SPECIFIC GRAVITY TO THAT OF THE REFRACTOMETER.
he reagent strip test is based on a chemical principle that measures the change
in the dissociation constant of a polyelectrolyte. his method does not measure
the true solute content, only those solutes that are ionic (pertaining to charged
molecules). 4f the strip test techni%ue is used as the means of evaluating the
specific gravity over time, then this method will provide clinical data regarding
the concentrating and diluting ability of the 3idney. >efer to Objectives W)) and
W)-.
2-151 LIST A MINIMUM OF FIVE THINGS THAT WILL CAUSE AN
INCREASE OR DECREASE IN THE REAGENT STRIP SPECIFIC
GRAVITY TEST RESULTS OR OTHERWISE OBSCURE THE
INTERPRETATION OF THE TEST.
Icrease1 A(D urea ((." gm+d,), A2D a ("" mg+d, protein reading may increase
=: by .""), A/D organic acids (lactic acid, acetoacetic acid, etc), A*D 3etone bodies.
Decrease1 A(D urine p2 of 0.) lowers =:, therefore add ."") to reading
2-152 DESCRIBE THE EFFECTS OF ASCORBIC ACID ON THE
STRIP REAGENT TEST PROCEDURE.
Ascorbic acid (vitamin 5) is a molecule suggestive of the glucose molecule. 4t is
not synthesi&ed in the human and certain other animals because of a deficiency of
,.gulonolactone o$idase, therefore must be included in the diet. Ascorbic acid is
a reducing agent, able to donate a hydrogen ion to acceptable recipient molecules.
For this reason, it is capable of interfering with one of the reactants in the reagent
strip test pads as follows1
A(D Hilirubin contains dia&onium salts which can be reduced causing a
false.negative reaction.
A2D Hlood contains a pseudopero$ide that can be reduced causing a
false.negative reaction.
A/D :lucose contains a pseudopero$ide that can be reduced causing a
false.negative reaction.
A*D Jitrate contains a dia&onium salt that can be reduced causing a
false negative reaction.
Ascorbic acid, when it donates its hydrogen ions to appropriate molecules, is
reduced to dehydroascorbic acid, which can further degrade to o$alate (o$alic
acid). he average diet contains sufficient ascorbic acid for good health and the
individual will e$crete less that ) mg+d, ascorbic acid in the urine. here is some
research that indicates that as much as /G mg+d, may be e$creted on an average.
hese levels are clinically insignificant and cause no problems in reagent strip
test technology. 4f an individual supplement their diet with increased vitamin 5,
then there is a potential ris3 that one or more of the above urine tests will be
altered. 8anufacturers of reagent test strips add a substance that will bloc3
ascorbic acid reaction and allow an accurate test result. =tudies have indicated
that individuals may e$crete up to *"" mg of ascorbic acid in ("" m,s of urine.
=uch levels may interfere with strip testing. 4t may be difficult to detect the
interference of ascorbic acid in urine. here are a few clues that will help. For
e$ample, if you report a urine specimen with >H5Ns in the urine but the strip test
pad for blood is negative, then you might have cause to suspect ascorbic acid is
present. he simplest method might be to 3eep reagent strip tests for ascorbic
acid as part of the lab inventory and if problems arise with urine testing, then the
urine can tested for the presence of ascorbic acid.
2-153 EXPLAIN WHAT HAPPENS WHEN +,) -, ./ 0, ACETIC
ACID IS ADDED TO URINE SEDIMENT.
he nucleus of BH57s are accentuated and >H57s undergo lysis.
2-154 DESCRIBE THE QC STEPS FOR PERFORMING A
MICROSCOPIC EXAMINATION THAT MEETS QUALITY CONTROL
STANDARDS.
A(D 'se fresh urine. 4f unable to perform within one hour of voiding, refrigerate
for up to three hours.
A2D 5entrifuge a standard %uantity. 'se either (", (2, or () m,s.
A/D 'se conical centrifuge tubes
A*D 5entrifuge, using the same centrifuge, rotor, centrifuge speed and force,
and time.
A)D Recant urine the same way+same techni%ue, leaving a residual of ".) to
(." m,s urine to resuspend the sediment and always be consistent in the
amount of residual urine remaining.
A0D 4f sediment is to be stained, always add the stain to the sediment in the
tube, not the slide.
A!D ransfer the sediment to the slide the same way, using the same type of
transfer pipette to deliver the same si&e drop. Ro JO invert the tube to
transfer sediment.
AGD 4f using a cover glass, use the same si&e cover glass since a larger or
smaller si&e will affect the way sediment distributes under the cover glass.
A-D He consistent in the way that the microscopic evaluation is performed.
A("D ?$amine the sediment under low power first to detect the presence or
absence of casts.
A((D 'se the *)S objective to identify sediment
A(2D ?$amine the same number of objective fields. en fields are acceptable,
but 2" is preferable.
A(/D 'se the same terminology for reporting out sediment.
A(*D 5hec3 microscopic findings with physical and chemical results to assure
accuracy of report.
2-155 STATE EIGHT FACTS THAT RELATE TO SOURCES OF ERROR
IN THE EXAMINATION OF URINE SEDIMENT
A(D 'sing dirty slides ma3es accurate differentiation of urine sediment difficult.
A2D >efrigerating urine will cause the urine specimen to become turbid which
will ma3e the microscopic e$amination more difficult. Jote1 'p to ("
percent of urines are turbid or cloudy at the time of voiding.
A/D 4f dilute acetic acid is used to dissolve amorphous phosphates, then any
erythrocytes in the urine specimen will be hemoly&ed.
A*D here are a number of loo3.a.li3es that may be found in urine. Oil
droplets, yeast, certain crystals, and even bubbles have been confused
with erythrocytes by ine$perienced laboratorians.
A)D 'sing a sediment stain will facilitate recognition of formed elements in
the urine.
A0D 'rine that has stood at room temperature for two or more hours will not
be reliable as some of the constitutents in the urine will have disintegrated
or disappeared.
A!D 4f urine contains myoglobin, it will yield a positive blood test and no
erythrocytes will be seen.
AGD 4f a patient ta3es mega.doses of ascorbic acid, then there may be a
suppressive effect upon the blood, nitrate, bilirubin, and glucose reagent
test pads causing a false.negative test result.
2-156 LIST THE CORRECT PROCEDURE FOR REPORTING
URINARY SEDIMENT AND/OR WHEN GIVEN DATA) CORRECTLY
COMPLETE A URINALYSIS REPORT.
>eport should be filled out according to the following parameters.
A(D >H57s, BH57s, renal tubular epithelial cells, transitional epithelial cells,
crystals, and parasites are reported as 6none seen6 or 6W+hpf6.
A2D 5asts and s%uamous epithelial cells are reported as 6none seen6 or 6W+lpf6.
A/D Hacteria, yeast, mucus, fat droplets, spermato&oa, and amorphous crystals
are reported as 6none seen6, Z (trace), (K (few), 2K (moderate),
/K (many), *K (J5+too numerous to count).
A*D >eport casts, crystals, and epithelial cells as to their type.
A)D Artifacts, as a rule, are not reported. 4f you see undigested animal or plant
cells or fibers, this should be investigated to rule out if the urine is actually
stool water, poor hygiene habits. or a vesicosigmoid fistula.
2-157 LIST FOURTEEN ARTIFACTS AND STATE HOW THEY
APPEAR IN THE URINE.
A(D plant cells1 via fecal contamination or vesicosigmoid fistula
A2D starch1 body power from patient or laboratorian gloves
A/D talc1 body powder from patient
A*D pollen1 air contamination
A)D muscle fibers1 via fecal contamination or vesicosigmoid fistula
A0D cotton fibers1 sifting from patient7s clothing during urine collection.
A!D synthetic fibers1 sifting from patient7s clothing during urine collection.
AGD hair1 from the patient7s body.
A-D paper fibers1 during urine collection or wiping urine container.
A("D oil droplets1 body lotion, catheter lubricants.
A((D wood fibers1 wooden applicator stic3s.
A(2D plastic shards1 usually sloughing off from centrifuge tube.
A(/D glass chips1 from the cover slip or glass slide due to scratching.
A(*D air bubbles1 appear when transferring the specimen to the slide.
61a"!e the *o$$o/!# !$$ustrat!os *or e1a"p$es o* art!*acts:
2-153 LIST THE EXPECTED STAINED COLOR WHEN THE
FOLLOWING TEN FORMED ELEMENTS ARE STAINED WITH
STERNHEIMER-MALBIN "S-M$ STAIN.
A(D mucus1 pale pin3 or a pale blue
A2D erythrocytes1 neutral p2 C pin3 to purple, al3aline p2 C purple, acid
p2 C do not stain. >H5 may not stain well with =8 stain.
A/D leu3ocytes1 nucleus C purple, cytoplasm C purple granules.
A*D bacteria1 motile (alive) C not stained, non.motile (dead) C purple
A)D >?51 nucleus C dar3 purple, cytoplasm C light shade of purple.
A0D transitional cells1 nucleus C dar3 purple, cytoplasm C light shade of
purple.
A!D s%uamous epithelial cells1 nucleus C purple, cytoplasm C light shade
of purple.
AGD 6rich61 Trichoo!as "a#i!alis, when alive, has a light greenish
appearance with =.8 stain.
A-D hyaline cast1 pale pin3 or pale blue matri$, similar to mucus.
A("D wa$y cast1 pale pin3 or pale blue, similar to the hyaline cast.
N.-6: "ost casts /!th !c$us!os /!$$ +e"ostrate a s!"!$ar sta!!#
react!o ! the "atr!1, -he !c$us!o "a) or "a) ot sta!, See a)
re*erece te1t or )our te1t %oo>,
N.-6: Co$or percept!o 'ar!es a"o# techs, Ce$$s !+et!De+ as
ta>!# o a purp$e co$or "a) appear %$ue to aother tech,
2-159 WHEN GIVEN DATA) THE NUMBER OF FORMED ELEMENTS
IN A VOLUME OF URINE CAN BE CALCULATED.
he following information and e$ample demonstrates how this can be
accomplished.
A(D Retermine the area of the objective being used for the calculation. For the
low power ((") objective, you may use an area of 2.)*) mm
2
. For the high
power (*)) objective, use an area C ".(-0 mm
2
.
A2D Retermine the number of low.power or high.power fields possible on the
cover glass being used for the microscopic e$amination.
a. he Qova slide area is circular and M/2 mm
2
b. An 22 mm () 22 mm s%uare cover glass M*G* mm
2
c. Other e$amples of cover glass si&es are (G mm (S) (G mm and 22 mm
() *" mm.
d. o calculate the number of fields, divide the area of the coverslip by
the area of the objective. ?$ample1 for a high power objective and a
22 mm () 22 mm cover glass, divide *G* mm
2
by ".(-0 mm
2
. he
answer is 2,*0- high.power fields.
A/D he volume of sediment that is viewed under the objective is re%uired. For
the Qova slide, the volume under the *) objective is ".""0 U,. he
disposable glass slide and coverslip create a problem in reproductivity.
?ven under the best of techni%ues, consistent and e$act standardi&ation is
not possible. 4deally for a 22 mm () 22 mm, e$actly 2" U, of resuspended
sediment concentrate should be placed on a glass slide and the coverslip
placed over it. his means that ".""G U, of sediment is being viewed
under the *) objective. 4f a (G mm () (G mm cover glass is used then
"."(2 U, is being viewed by the (" objective.
A*D Retermine the concentration factor. 4n most labs, (2 m,s of urine is
concentrated down to (." m,s by first centrifuging (2 m,s of urine and
removing (( m,s of supernatant, then resuspending the sediment in the
remaining (." m,s. For this e$ercise, the concentration factor the volume
of urine concentrated, will be (2 m,s and Ls is dropped and only the
number (2 is used.
A)D 'se the following formula to calculate the number of fields viewed per m,.
his step may be called the 6field conversion factor6.
W possible fields W of fields viewed per
........................... C ..........................
total vol. of sediment viewed ( m, urine tested
(in m,s) [ 5onc. factor
A0D o set up problem, use 22 mm (S) 22 mm cover glass data.
2 ,*0- A*)D fields of view 2,*0-
.............................. C ........ C (",2GG hpf+m, of urine
"."2" m,s () (2 ".2*
A!D o find the number of formed elements+m, urine, determine the average
number of formed elements observed in 2" fields of view. For e$ample1 if
you determine that there is an average of * BH57s+hpf, then calculate as
follows1
Formula1
W formed elements+hpf () 6field conversion factor6 C W formed elements
per m, urine.
* BH57s+hpf () (",2GG+hpf C *(,()2 BH57s+m, urine.
2-164 DEFINE A SUPRAVITAL STAIN AND LIST TWO SUCH
STAINS) DISADVANTAGES) HOW THEY WORK) AND/OR
DEMONSTRATE HOW TO PROPERLY STAIN URINE SEDIMENT.
A supravital stain will stain living tissue by perfusing through the cell and
distinguishing cell components. 4t provides more detailed images of leu3ocytes,
epithelial cells, and casts. he =ternheimer.8albin stain and the ".)# toluidine
stain are good stains for urine sediment. =8 stain has a tendency to precipitate in
strongly al3aline urine. 4f you see crystals in urine to which =8 stain has been
added, such crystals will be brown or purple stellate crystals.
2-161 DESCRIBE HOW THE LABORATORY CAN DEMONSTRATE
FAT/LIPIDS IN URINE.
he polari&ing microscope provides an e$cellent way to demonstrate lipids. 4t
provides greater contrast of urinary sediment and the presence of cholesterol
lipids are characteri&ed by the presence of the 8altese cross. Jeutral fats do not
produce the cross phenomenon. ,ipid stains (=udan 444, =udan 4\, and Oil >ed *
are used by labs to stain the neutral fats+triglyceride lipids. Polari&ed light or
lipid stains may be used to demonstrate the presence of free fat globules, oval fat
bodies, and fatty casts.
2-162 EXPLAIN WHY A LABORATORY WOULD USE GRAM STAIN
TO STAIN URINE SEDIMENT.
:ram stain is used in microbiology to differentiate bacteria into gram positive or
gram negative groups. he gram stain in urinalysis would be for this purpose.
2-163 EXPLAIN THE PURPOSE OF HANSEL#S STAIN AND WHEN A
LAB WOULD USE SUCH A STAIN.
2ansel7s stain (as is 2in3leman7s stain and 8anner7s stain) is used for the
staining of eosinophils. ?osinophils will appear in the urine in response to
hypersensitivity reactions. 4f the hypersensitivity is associated with the 3idney,
there may be an adverse reaction to a drug. he presence of increased numbers of
eosinophils is a good indicator that hypersensitive condition is present. Failure
to treat hypersensitivity may result in renal damage.
2-164 EXPLAIN THE PURPOSE OF PRUSSIAN BLUE STAIN.
his stain colors free hemosiderin in urine or that bound in epithelial cells.
Prussian blue actually binds with the iron molecule in the form of hemosiderin to
produce a distinctive blue color.
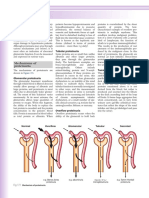
2-165 DESCRIBE AND/OR ILLUSTRATE ERYTHROCYTES IN
HYPOTONIC) ISOTONIC) AND HYPERTONIC URINE SPECIMENS.
he normal >H5 is a round, biconcave dis3 that appears refractile in urine. he
cell will have a colorless or yellow tinge in unstained urine. 4t diameter will be
about ! U. 4f viewed from the side it will ta3e on an hour glass appearance and
when viewing from the top, there will be a central area of pallor. >H57s are
osmotically sensitive. 4n hypotonic urine, water will be absorbed into the >H5
(causing it to swell) until it lysis. 4n isotonic urine, the osmotic forces are e%ual
and the >H5 will retain it normal configuration. 4n hypertonic urine, the osmotic
forces will cause fluid to diffuse from the >H5, leaving the cell to shrin3 and
wrin3le. his cell is called a 6crenated cell6. =ee the following illustration.
2-166 IDENTIFY FOUR ERYTHROCYTE %LOOK-A-LIKES% AND
HOW TO DISTINGUISH THEM.
A(D ]east cells1 Hoth oval and round form are noted. here is variation in si&e
and are characteri&ed by 6budding6. ]east cells are resistant to acetic
acid lysis.
A2D Oil droplets1 8ay be uniform in appearance, but will vary significantly in
si&e. Jeutral lipids will stain with lipid stains.
A/D Air Hubbles1 Bill be variable in si&e and demonstrate dar3 ring
phenomenon.
A*D 5alcium O$alate1 he monohydrate form of calcium o$alate may contain
oval+round forms. Other (dihydrate) calcium o$alate forms are present
and easily eliminates this as a 6loo3.a.li3e).
2-167 DESCRIBE DYSMORPHIC RBC#S AND EXPLAIN THEIR
APPEARANCE IN URINE.
Rysmorphic erythrocytes are irregular >H57s with distorted appearances. heir
appearance has been reported as bi&arre and conse%uently their presence may go
unreported. hese cells will contain variable amounts of hemoglobin which may
be randomly distributed contributing to the appearance of the erythrocyte. he
dysmorphic >H5 is associated with glomerulonephritis. he >H5 will traverse
the length of the nephron, subjected to the osmotic and physical forces, which
produces the dysmorphism. 4n the microscopic, loo3 for irregular cell
membranes, ring.li3e forms, blebs, target cells, buds, and other strange
configurations. =ee the following illustration.
2-163 DESCRIBE WHAT OTHER TEST PARAMETERS THE
MICROSCOPIC CAN BE CORRELATED TO WHEN RBC#S ARE
REPORTED IN THE SEDIMENT.
A(D Appearance1 should to ha&y to cloudy. 4f <*"" >H5+m,, the urine
specimen will be clear.
A2D 5olor1 loo3 for pin3 to red to smo3ey coloration.
A/D =ediment button1 presence of a red button.
A*D >eagent strip test1
a. blood pad will be positive.
b. protein pad may be positive. 4f bleeding from glomerulus, albumin
is being lost from glomerular capillaries.
2-169 DESCRIBE THE APPEARANCE OF RBC#S FROM NON-
GLOMERULAR BLEEDING.
2emoglobin is homogeneously (evenly) distributed. he cells are normal in
appearance and crenated contours may be observed. >efer to the illustration in
,earning Objective 2.(0).
2-174 DISCUSS THE CLINICAL SIGNIFICANCE OF
ERYTHROCYTES IN URINE.
heir presence if pathological if greater than ) >H5+hpf. Jormal values are 2
>H5+hpf which is e%uivalent to X (2 >H5+U,. 4f patient is catheteri&ed or
e$periencing menses, then >H57s in urine are not significant. Pathological
implications may be any of the following1 () bacterial infection, (!) presence of
stones, (") tumors, (#) trauma, or ($) to$ic reactions to drugs+medications. he
increased presence of >H57s in urine is called hematuria.
2-171 DESCRIBE THE TYPE OF LEUKOCYTES AND OTHER
PHAGOCYTES THAT MAY BE FOUND IN URINE.
A(D Jeutrophils1 he most common BH5 encountered. his cell contains a
multi.lobed nucleus, is similar in si&e to a renal tubular epithelial cell
(>?5), and ranges in si&e from (" to (* U8. hese cells produce the
en&yme esterase that cleaves the ester 4n the reagent strip test pad.
hey are increased in all inflammatory responses. >eport these cells as
BH57s or pus cells.
A2D ,ymphocytes1 Are seen in urine specimens and should be reported as
small, mononuclear cells.probably lymphocytes. hey do not produce
esterase and will not affect the reagent strip pad if present in large
numbers. ,arge numbers are reported in viral infections and acute
glomerulonephritis.
NOTE
4f it is necessary to perform a cytodiagnositc differential,
prepare a smear from the urine sediment and stain with
Bright7s stain. BH57s should not be reported out as to type in a
routine urinalysis.
A/D 8onocytes1 hese are similar in si&e to >?57s and are easily confused with
them. hese cells can attain diameters up to *" U8 and are easily identified
if differentially stained. >eport their presence as large, mononuclear cells.
probably monocytes.
A*D ?osinophils1 hese cells are difficult to distinguish from neutrophils. 'nless
differentiated with Bright7s stain, report these cells as you would
neutrophils. ?osinophils are increased in acute interstitial nephritis,
allergies, and acute allograph rejection.
A)D 8acrophages1 Also called histocytes, these cells range usually ranges from
/" to *" U8, but may attain diameters of ("" U8. he nucleus may be
round, irregular, or 3idney shaped. here is an abundance of cytoplasm and
vacuoles are present. Bhen seen in urine, they are in most cases, spherical.
>eporting these cells as macrophages.
2-172 DISCUSS THE NEUTROPHIL AS THE TYPICAL WBC IN
URINE.
his cell should be referred to as a white blood cell, leu3ocyte, or pus cell. 4n a
fresh urine specimen, neutrophils will display neutrophil features and may
e$hibit ameboid movement. 4f nuclear features are important to discern, add a
drop of dilute acetic acid (X/#).
As neutrophils 6age6, disintegration %uic3ly set in and the cell becomes
increasingly granular in appearance. he nuclei will fuse and the cell appear as a
mononuclear cell. Bhen this occurs, it is easily confused with a renal tubular
epithelial cell (>?5). Hlebs may appear on the inner cell membrane, the detach
from the cell and float free. As the cells continue disintegrate, filaments form and
e$tend outward from the membrane surface. Bhen this occurs the cell membrane
brea3s down and the cell ruptures. Jote the following illustration.
4n dilute urine, at room temperature, the BH5 will swell to form spheres, then
lysis occurs. Bithin 2./ hours, up to )"# of the BH57s will have lysed. Ruring the
time that the BH5 is in its swollen state, cytoplasmic granules e$hibit Hrownian
movement and are refractive. Bhen this occurs, the cell is called a 6glitter cell6.
=uch cells have no clinical+pathological significance. Bhen stained with
=ternheimer.8albin stain, the 6glitter cell6 will appear pale blue. :litter cells are
usually seen in urines with a specific gravity less than (."(-. =ee above illustraton.
Old6 leu3ocytes tend to be smaller in si&e, nuclear features are more indistinct,
increased granulation, and in differing states of disintegration. 6Fresh6
leu3ocytes appear larger, distinct nuclear features, abundant cytoplasmic
granules, and absence of disintegration.
N.-6: A or"a$ a+ hea$th) ur!e +oes ot Eshe+E $eu>oc)tes,
2-173 COMPARE AND CORRELATE THE URINE MICROSCOPIC
FINDINGS OF LEUKOCYTES TO PHYSICAL AND CHEMICAL
PARAMETERS.
A(D Appearance will be ha&y to cloudy if L*"" BH5+mm/.
A2D Odor may be strong, pungent, or foul.
A/D A grey button will appear in the bottom of the centrifuge tube in pyuria.
A*D 5lumping will be a characteristic feature in pyuria.
A)D ,eu3ocyte esterase test C positive ( BH5 L("","""+mm
/
)
A0D Jitrite test C positive (if infective bacteria is a nitrate reducer).
A!D Hlood test C positive (if lesions are present due to infection).
AGD 4f there are many BH5Ns present, loo3 for BH5 casts.
2-174 DESCRIBE THE SQUAMOUS EPITHELIAL CELL OBSERVED
IN URINE.
his is the most fre%uently found epithelial cell in urine and has the least clinical
significance. 4t is derived from the vagina, prepuce of uncircumcised men, and
urethra. he s%uamous cell is characteri&ed by an abundance of cytoplasm and a
small eccentric nucleus (which is about the si&e of a >H5). he edges of the cell
can roll and fold, causing the cell to present in a variety of configurations. he
cytoplasm may appear finely granular and also have a few large granules
scattered throughout it. 4t diameter ranges from *" to 0" U8. As the cell
deteriorates, granulation becomes more prevalent. 4t is easy to identify and
should be enumerated with ("S objective. 4f large numbers of s%uamous cells are
noted in a urine specimen from a female, this is an indicator of vaginal
contamination. Jormal amounts of sloughing will be characteri&ed by X0
cells+lpf. Bhen e$amining the s%uamous cell, the cell for any aberrant features in
the cytoplasm, cell, or nucleus. 5omparing the cytoplasm and nuclear ratios will
help to identify the s%uamous cell, being L (2 to (. Jote the following illustration.
2-175 DESCRIBE THE TRANSITIONAL EPITHELIAL CELL
OBSERVED IN URINE.
Also called urothelial or bladder cells, these cells originate from the bladder,
urethra of males, ureters, renal pelvis, and the major and minor calyces. he si&e
is variable dependent upon which later the cell sloughed from. 5ells from the
outer, superficial layer will be larger and flatter, with a diameter ranging from /"
to *" U8, whereas cells from the inner, intermediate layers are smaller and
plumper have a diameter of 2" to /" U8. ransitional cells from the bladder may
be larger and closely resemble s%uamous cells. >eview the following illustrations.
o recogni&e the transitional cell9
A(D loo3 for larger cytoplasmic granules that tend to accumulate around the
nucleus. his is called nuclear distribution.
A2D increased number of inclusions are the rule.
A/D loo3 for distinct peripheral borders on the cytoplasm and nucleus.
A*D shape variations are as follows1
A)D he nucleus will be eccentric, round or oval, and about the si&e of a small
BH5.
A0D 4t is not abnormal to find cells with two nuclei.
A!D they have the tendency to absorb water and this will alter their appearance.
AGD there will be about 0 to ! times more cytoplasmic area than nuclear area.
2-176 DISCUSS THE CLINICAL SIGNIFICANCE OF TRANSITIONAL
CELLS.
'sually there are no clinical significance. 4n urinary tract infections ('4)
increased numbers are sometimes encountered. 4f an increased number of
transitional cells are noted, ta3e time to review the morphology of the cells. 4f
abnormal morphology is noted, the specimen should be referred to a pathologist
for cytologic review. 4f the cell originates from the trigone of the bladder or the
renal pelvis, there will often be a tail.li3e e$tension. hese cells are called caudate
cells and are not diagnostic of anything. >efer to the previous learning objective
(2.(!))
2-177 DESCRIBE A %DECOY% CELL AND ITS SIGNIFICANCE.
he 6decoy6 cell is a transitional cell that is thought to be infected with polyoma
virus. his cell is so called because it displays uni%ue staining phenomenon in
=ternheimer.8albin stain. he cytoplasm stains red and the nucleus is irregular,
very large, vacuolated, and has dense peripheral chromatin. 4t is called a pseudo.
malignant cell. ?$amine the following illustration.
2-173 DESCRIBE %MULTI-NUCLEATED GIANT% CELLS AND THEIR
SIGNIFICANCE.
his is a cell generally thought to be derived from the superficial layers of the
renal pelvis and ureters. 4t is characteri&ed with a vacuolated cytoplasm, multi.
nucleated (with up to ( "" nuclei reported), nucleoli present, and diameters up to
/"" U8. 5ell shapes vary from round to polygonal. he cells are observed in
heavy metal poisoning, inflammation, and trauma. hey have been reported in
normal urine (voided and catheteri&ed). ?$amine the following illustrations.
2-179 DESCRIBE %HISTOCYTES% AND THEIR SIGNIFICANCE.
A large phagocytic cell that is usually seen in inflammatory conditions
(glomerulopathy) . he cell is larger than BH57s with a foamy appearing
cytoplasm containing distinct vacuoles. he cytoplasmic borders are often poorly
defined. he round to bean.shaped nucleus is eccentrically placed in the cell. 4t is
not unusual to observe multinucleated histocytes. >efer to the following
illustrations.
2-134 DESCRIBE %CLUE CELLS% AND THEIR SIGNIFICANCE.
5lue cells are s%uamous epithelial cells of vaginal origin. hey are uni%ue in that
they are coated with the coccobacilli ($ar%!erella "a#i!alis). heir presence is
an indicator of a vaginal infection. ,oo3 for s%uamous cells that have a granular
appearance with shaggy borders. Hacteria may be lightly or densely 6crusted6
across the s%uamous cells and will even e$tend across the cytoplasmic margins.
He cautious because some s%uamous cells will contain irregular 3eratohyaline
granules which ma3es them a 6clue cell loo3.a.li3e6. =ee the following
illustration1
2-131 DESCRIBE AN UMBRELLA% CELL AND ITS SIGNIFICANCE.
'mbrella cells are best observed with =ternheimer.8albin stain. ,oo3 for
concave cells with foamy cytoplasm. hese are multi.nucleated, sloughed.off
disintegrating cells from the renal pelvis, ureters, and bladder. 4t is the largest of
the transitional cells and it is clinically insignificant. ?$amine the following
illustration1
2-132 DESCRIBE RENAL TUBULAR EPITHELIAL CELLS "RTEC$.
he >?5 is the most significant of the epithelial cells. hey can originate from
any part of the nephron and collecting duct. 8ost >?57s appear in urine
sediment as a conse%uence of natural process of cell replacement. hese cells can
be differentiated by si&e and shape. =ince it is difficult to differentiate these cells
into pro$imal, distal, and collecting duct types, most laboratories, these cells are
nor differentiated into their three categories, but simply referred to as >?57s. o
differentiate, slides should be made from the sediment and stained with Bright7s
stain or other good cellular stain. Actually there is no real clinical advantage in
urinary screening procedures to categori&e into different types. =ince some
laboratories do differentiate between >?57s, they will be reviewed in this course.
>?57s are significant only if their numbers are significantly increased. Hased on
the studies of :. H. =chumann, if L() >?57s are observed per high power field,
this is a strong indication for renal pathology. he specimen should then be re.
evaluated according to lab policy.
:eneral morphology describes this cell as being round to oblong in shape with a
si&e that is about (^ to two or three times larger than leu3ocytes. Riameters will
be as up to 2) U8. A dense, round, often eccentric nucleus is typical. he
cytoplasm is granular. hese cells are not prone to absorb water therefore do not
swell and change shapes as do transitional cells. hey tend to retain their original
shape. =ee Figures () and (0.
>efer to the following illustrations1
2-133 DESCRIBE AND/OR DIFFERENTIATE BETWEEN PROXIMAL
CONVOLUTED TUBULE CELLS) DISTAL CONVOLUTED TUBULES
CELLS) AND COLLECTING DUCT CELL=.
:ro1!"a$ co'o$ute+ tu%u$e ce$$s. hese are elongated or oval and polyhedral
in shape with a granular cytoplasm. he nucleus tends to be eccentric, dense, and
small. Riameters range from 2" to 0" U8. 8ultinucleated forms are not unusual
nor abnormal. One side of the cell is usually (but not always) flattened. hey are
reported to be elongated in form and when unstained, may appear to resemble a
small granular cast.
D!sta$ co'o$ute+ tu%u$e ce$$s. hey resemble the pro$imal convoluted
tubule cell, but tend to be smaller. Riameters range from (* to 2) U8.
NOTE
he renal tubular cell that is most li3ely to be observed in the urine
sediment are those that originate from the convoluted tubule and smaller
collecting ducts.
5ollecting tubule cells. hese cells are either columnar, cuboidal or polygonal9
but never round. o identify this cell, loo3 for straight sides and corners. his cell
is characteri&ed by a single, large nucleus that may occupy as much as 2+/ of the
cytoplasm. he smaller of the collecting tubule cells range from (2 to 2" U8 and
become larger as and more columnar as the tubule approaches its minor caly$.
Jote the following illustration1
2-134 DISCUSS THE CLINICAL SIGNIFICANCE OF THE RENAL
EPITHELIAL CELLS WHEN OBSERVED IN INCREASE NUMBERS.
4ncreased in to$ic renal tubular damage due to heavy metal poisons (lead,
mercury, etc.), drugs (cytoto$ins), graft rejection, pyelonephritis (sepsis),
nephrosclerosis, trauma, shoc3, ischemic necrosis, or any renal disorder
characteri&ed by heavy proteinuria.
2-135 DESCRIBE THE COURSE OF ACTION WHEN COLUMNAR
TUBULAR CELLS ARE PRESENT AND A RENAL PATHOLOGY MAY
BE SUSPECT.
?valuate the microscopic sediment for the presence of >H57s, granular casts,
>?5 casts, and wa$y casts. >etest for protein using the sulfosalicylic acid
procedure if the strip test is negative.
2-136 DESCRIBE AND EXPLAIN THE SIGNIFICANCE OF OVAL FAT
BODIES.
Oval fat bodies (OFH) are renal tubular cells that contain lipids (refer to the
following illustration). hese cells are formed when the intracellular lipids
degenerate and coalesce into lipid globules. 4f lipids appear in the glomerular
filtrate due to glomerular dysfunction and plasma lea3age, they will be readily
absorbed by the renal tubular cells. ,ipids, as the coalesce in the >?57s, will
form variable si&e droplets and demonstrate high refractile properties. hey are
more easily recogni&ed with the brightfield microscope than the phase
microscope. 'nder low power, they will resemble brownish spheres. he phase
microscope provides a positive identification if the fat globules (with cholesterol
and cholesterol esters present) demonstrates the maltose cross effect. 4f the fat
globules contains only neutral fats, then verification must be by a fat stain (=udan
444 or Oil >ed *). he presence of OFH are pathologically significant and are to be
reported out in numbers per high power field. heir presence may suggest any of
the following1 (() trauma with release of bone marrow fat, (2) lipid storage
disease (Fabry7s disease, :aucher7s disease, Jiemann.Pic3 disease, etc.), (/)
to$emia of pregnancy, (*) diabetes mellitus, ()) pyelonephritis, (0) polycystic
3idney disease, (!) nephrotic syndrome, and (G) congestive heart failure. Bhen
you observe OFH in urine sediment, evaluate the sediment for free floating fat
globules. Also loo3 for casts and re.chec3 the protein test (which should be
positive).
NOTE
4n lipid storage diseases, fat.filled histocytes and macrophages may be
observed. hey are easily confused with OFH, but are distinguished by
their larger si&e. (>efer to the following illustration).
2-137 DISCUSS THE SIGNIFICANCE OF FINDING INCLUSION
BODIES IN RENAL TUBULAR EPITHELIAL CELLS.
>enal tubular epithelial cells that contain inclusion bodies are difficult to see and
are easily missed unless the sediment is stained. 8ost inclusions are the result of
a viral infection, usually the herpes or rubella (:erman measles). Other
inclusions may be the result of heavy metal poisoning. An infection with
cytomegalovirus (a herpes virus) causes inclusions in the nucleus.
2-133 DESCRIBE CASTS AND HOW THEY ARE FORMED.
5asts are elements of solidified protein that may or may not contain inclusions
that are found in both normal and abnormal urine. he distal convoluted tubules
and collecting tubules secrete a muco.protein (amm.2orsfall protein) that
appears first in the form of fibrils. hese fibrils stic3 to the lumen walls and as
more protein fibrils are secreted, an interweaving occurs and the cast ta3es
forms. 5ast formation is augmented if plasma proteins are present, solutes are
increased, the p2 is acidic, and filtrate flow through the lumen is slow. 5asts are
formed in the tubules and conform to the shape and structure of the tubule. he
cast can undergo changes in the tubule and undergo transitional changes. 5asts
have parallel sides but tend to be thic3er in the middle and more slender toward
the ends. 5asts can be long, short, thin, thic3, convoluted, curved, or straight. he
cast can be fragile (easily bro3en) or resilient (resistant to brea3ing).
2-139 EXPLAIN HOW H) SOLUTE CONCENTRATION) AND
URINARY STASIS IN THE NEPHRON CONTRIBUTE TO CAST
FORMATION.
(() An acidic environment contributes to solute and protein precipitation,
which favors cast formation. his occurs most often in the distal and
collecting tubules.
(2) =olute concentration.... favors crystal precipitation and protein
precipitation.
(/) 'rinary stasis... usually occurs for some type of pathological disease or
obstruction or congenital abnormality. =tasis facilitates accumulation and
concentration of substances that contribute to cast formation. he
presence of plasma proteins (albumin and+or globulins), hemoglobin, or
myoglobin enhances cast formation.
2-194 DISCUSS THE CLASSIFICATION OF CASTS.
5asts are classified according to their matri$ and the 6stuff6 (inclusions) observed
in the matri$. 4nclusions includes1 bacteria, leu3ocytes, erythrocytes, renal
tubular epithelial cells, lipids, granules, hemosiderin, and crystals. 5asts may be
classified as follows1
(a) 2omogeneous+non.inclusion1 hyaline, wa$y.
(b) 4nclusion+cellular1 leu3ocytes, erythrocytes, renal tubular epithelial cells,
bacteria.
(c) 4nclusion+non.cellular1 lipids, granules, hemosiderin, crystals.
(d) Pigmented1 bilirubin, hemoglobin, myoglobin, drug pigments.
N.12& A!other cate#ory o' casts are the (roa% casts. These casts are
e)tra*lar#e a!% ca! (e classi'ie% as i%e!ti'ie% i! +a, throu#h +%,.
2-191 DESCRIBE %FALSE% CASTS AND HOW TO RECOGNI!E
THEM.
his is a phenomenon that occurs during an 6al3aline tide6 which facilitates the
precipitation of amorphous phosphates. he precipitate tends to form in slender,
cylindrical appearing arrangements. o differentiate from true casts, loo3 for the
absence of a protein matri$ border. A true cast will present a hyaline.li3e matri$.
?$amine the surround area. 4f this is a pseudo.cast, there will also be
indiscriminate masses of precipitate scattered about. False.casts can also include
aggregates of groups of bacteria, cells, or crystals. >emember to be a true cast, the
cells or OwhateverP must be embedded in a mucoprotein matri$.
2-192 DISTINGUISH BETWEEN %NARROW% AND %BROAD% CASTS
AND BRIEFLY EXPLAIN THE SIGNIFICANCE OF THEIR
APPEARANCE IN URINE SEDIMENT.
8ost casts tend to have a diameter that similar, however the length may vary.
Jarrow casts usually form during an inflammatory process in which the tubules
are swollen, causing the lumen to be more narrow. 8ost casts reported out as
narrow casts are hyaline and the prognosis is less serious. Hroad casts are formed
in dilated renal tubules or the collecting tubules. hese are the more pathological
of the casts and indicate a severe renal problem. Hroad casts tend to form in
chronic renal disorders or obstruction which produces stasis. 8ost broad casts
that are reported are the wa$y type. Hroad casts are also called 6renal failure6
casts.
2-193 DISCUSS THE HYALINE CAST) HOW TO RECOGNI!E IT)
AND ITS CLINICAL SIGNIFICANCE.
his is the most commonly observed cast and has the least clinical significance. 4t
consists of a congealed mass of amm.2orsfall protein and may contain no or a
few inclusions. he refractive inde$ is low and may be easily overloo3ed if in low
numbers. hese casts tend have rounded ends and present with a variety of si&es
and shapes. =taining with =ternheimer.8albin stains enhances their
visuali&ation. hey ta3e on a pin3 coloration and borders are more distinct.
Jumbers are increased during severe e$ercise, dehydration, heat e$posure, and
stress. hey are also observed to accompany the pathological casts during a
variety of renal disease, congestive heart failure, and febrile illnesses. Jormal
values reported by most laboratories are ".2+lpf. Bhen identifying the hyaline
cast, do not confuse it with mucus threads. 4t is not uncommon see these casts
containing very fine granules, in which case, they are still reported out as hyaline
casts. >efer to the following illustrations.
2-194 DESCRIBE CYLINDEROIDS.
5ylinderoids are hyaline casts, e$cept that one end (as the rule) will be tapering
or serpentine in appearance. 5ylinderoids are to be reported out as hyaline casts.
>efer to the illustration of hyaline casts in previous learning objective.
2-195 DISCUSS THE STABILITY AND SOLUBILITY OF CASTS.
he amm.2orsfall protein matri$ is stable in a acidic urine with an elevated
specific gravity (L(."("). he cast matri$ is soluble in water and the solubility
increases as the p2 increases. 4f the 3idney7s fail to concentrate the urine and
hold an acidic p2, casts may not form. 5asts tend to be fragile, brea3ing easily.
5asts tend to disintegrate in urine that sits out at room temperature over a period
of time.
2-196 DISCUSS THE RBC CAST AND IT CLINICAL SIGNIFICANCE.
he presence of these casts are always pathological. hese casts form when the
>H5 becomes trapped in the amm.2orsfall protein matri$ in a random manner,
not in rows or columns. 4f there is glomerular damage with bleeding, the plasma
proteins and fibrinogen will contribute to the formation of the cast7s matri$.
hese casts form whenever any disorder damages the glomerulus, nephron, or
parenchyma tissue of the 3idney. hese casts are very fragile and urine should be
fresh and carefully handled to increase the success of finding these casts. =ince
this cast is not stable, the >H57s will %uic3ly deteriorate and the cast becomes
unrecogni&able as a >H5 cast. 4t is then referred to as a blood cast. As
erythrocytes lyse in the cast, the cast ta3es on a more homogeneous appearance
with little color variation. >H5 casts are refractile and have a color ranging from
yellow to red.brown. ,oo3 for intact and clearly identifiable erythrocytes. Jote
the margin of the cast, the edge of the hyaline matri$ should be seen about the
cast. 4f you see 2 or / >H57s in a cast, it is acceptable to call it a >H5 cast. 4f >H5
casts are present in the sediment, e$amine the 6neighborhood6, free erythrocytes
should also be present which helps in the identification of the >H5 cast. >H5
casts are observed in (() glomerulonephritis, (2) Begner7s granulomatosis, (/)
polyarthritis, (*) sic3le cell anemia, ()) sub.acute bacterial endocarditis, (0)
systemic lupus erythematosus, (!) renal infarction, and (G) after strenuous
physical e$ertion. >H5 casts should be reported as number you see per lpf. A rare
>H5 cast may be observed in normal urine. Bhen >H5 casts are observed in
urine sediment, it is probable that the blood values for uric acid, blood urea
nitrogen (H'J), and creatinine will be increased. 4f >H5 casts are present, the
strip reagent test pads should be positive for blood and possibly protein. >efer to
the following illustrations of erythrocyte casts.
N.-6
>H5 and hemoglobin casts at one time were thought to represent
different disorders and should be differentiated in the report. his
is no longer true and the >H5 cast, blood cast, or hemoglobin cast
may be reported out as a >H5 cast.
2-197 DISCUSS THE WBC CAST AND ITS CLINICAL
SIGNIFICANCE.
he presence of leu3ocyte casts indicate the presence of a renal inflammation or
infection. =pecific disorders are (() pyelonephritis, (2) post streptococcal acute
glomerulonephritis, (/) nephrotic syndrome, (*) systemic lupus erythematosus,
and ()) polyarteritis nodosa. hese casts should be reported as number per lpf.
=ynonyms are leu3ocyte cast or pus cast. A positive leu3ocytes strip test and
protein help verify the presence of these casts. 4f a bacterial infection is present,
the nitrate test should be positive. =taining the sediment helps to visuali&e the
nuclear detail in the leu3ocytes in the cast. he consensus among laboratorians is
that casts with leu3ocytes scattered throughout the cast matri$ seldom occurs. 4t
is thought that the BH57s adhere to the outside of a hyaline cast to form a BH5
cast by means of it proteinaceous fibrils. BH57s attach to the cast matri$ in a
random manner and do nor form rows or columns. 4f BH5 casts are present, it
might be appropriate to recommend a culture and sensitivity. 5aution1 do not
confuse BH5 casts with >?5 casts. >efer to the following e$amples of BH5
casts.
2-193 DISCUSS THE RTEC CAST AND ITS CLINICAL
SIGNIFICANCE.
>enal tubular epithelial casts (>?5) are formed when >?57s are damaged and
sloughed into the lumen of the nephron. hese cells can be incorporated into the
matri$ of the cast or they can adhere to the surface of the hyaline matri$. =ince
>?57s slough, they are li3ely to do so in sheets, and in the cast will appear as
rows and lines. >enal tubular casts are found in viral diseases (cytomegalovirus
or hepatitis), nephroto$ins (heavy metals, salicylate to$icity),
glomerulonephropathies, lipoid necrosis, and renal parenchymal disease. he
>?5 disintegrates rapidly which may result in the laboratorian miscalling the
cast as a granular cast. hese casts have been confused with BH5 casts. >eport
>?5 casts as number per lpf. Jote the following e$amples of >?5 casts.
2-199 DISCUSS THE HEMOGLOBIN CAST) HOW TO DISTINGUISH
IT) AND ITS CLINICAL SIGNIFICANCE.
2emoglobin casts have the same clinical significance as >H5 casts and appear in
urine under the same causes. =ee Objective W(G-. 4t is generally conceded that
hemoglobin casts are formed by the brea3down of >H5 casts. he three
additional conditions that contribute to hemoglobin cast formation are
transfusion reactions, 5lostridium bacteremia, and hemolytic anemia.
2emoglobin casts should not be confused with pigmented casts (=ee Objective
W2")). An e$amination of the 6neighborhood6 helps to distinguish pigmented
casts. he pigment that stains the cast also stains the cells and other elements
around the cast. =taining the sediment with Puchtler method (Huffalo blac3
stain) causes hemoglobin casts to turn dar3 blue and >alph7s method (a nuclear
fast red stain) will turn hemoglobin casts brown. 4f the reagent test pad for blood
is positive and >H5Ns are observed in the sediment, loo3 for hemoglobin and >H5
casts.
>evised for spring 2""0
You might also like
- Complementary and Alternative Medical Lab Testing Part 6: Liver and GallbladderFrom EverandComplementary and Alternative Medical Lab Testing Part 6: Liver and GallbladderNo ratings yet
- Physiology for General Surgical Sciences Examination (GSSE)From EverandPhysiology for General Surgical Sciences Examination (GSSE)S. Ali MirjaliliNo ratings yet
- Proteinuria in Adults - A Diagnostic Approach - AAFPDocument12 pagesProteinuria in Adults - A Diagnostic Approach - AAFPXeric CedoNo ratings yet
- Proteinuria in Adults and Diagnostic ApproachDocument9 pagesProteinuria in Adults and Diagnostic ApproachCindy JANo ratings yet
- Primary Care Approach To ProteinuriaDocument6 pagesPrimary Care Approach To Proteinuriadanny17phNo ratings yet
- Bence JonesDocument5 pagesBence JonesChristian Eduard de Dios100% (1)
- Protein Uri ADocument2 pagesProtein Uri AAmelia PebriantiNo ratings yet
- Primary Care Approach To Proteinuria: Amir Said Alizadeh Naderi, MD, and Robert F. Reilly, MDDocument6 pagesPrimary Care Approach To Proteinuria: Amir Said Alizadeh Naderi, MD, and Robert F. Reilly, MDDarian AngNo ratings yet
- DR SajadiyehDocument152 pagesDR SajadiyehTeodora JoghiuNo ratings yet
- Nitrogen BalanceDocument16 pagesNitrogen BalanceAli MajidNo ratings yet
- Protein Precipitation As A Possible Important Pitfall in The Clinical Chemistry Analysis of Blood Samples Containing Monoclonal ImmunoglobulinsDocument11 pagesProtein Precipitation As A Possible Important Pitfall in The Clinical Chemistry Analysis of Blood Samples Containing Monoclonal ImmunoglobulinsramazankocabasNo ratings yet
- Useful TestsDocument3 pagesUseful TestsLiamNo ratings yet
- Proteinuria en Perros y GatosDocument16 pagesProteinuria en Perros y GatosKaren PMNo ratings yet
- ProteinuriaDocument12 pagesProteinuriaSaraswati Wulandari HartonoNo ratings yet
- Workup For ProteinuriaDocument17 pagesWorkup For ProteinuriaSantiago ChávezNo ratings yet
- CC CC C C C!"#C $!$%: C$!$C c!"7 ":"!CDocument45 pagesCC CC C C C!"#C $!$%: C$!$C c!"7 ":"!CMukhtar JamacNo ratings yet
- Measurement of Glucose Homeostasis in VivoDocument10 pagesMeasurement of Glucose Homeostasis in Vivo19400668No ratings yet
- P2.07 - SG8Document8 pagesP2.07 - SG8DeirdreNo ratings yet
- Case 2Document4 pagesCase 2Kim Ruiz100% (1)
- Hipoglikemia Pada Seorang Penderita Malaria: PartsDocument4 pagesHipoglikemia Pada Seorang Penderita Malaria: PartsBoy HaqiNo ratings yet
- Concise Review For Primary-Care Physicians: Evaluation of ProteinuriaDocument5 pagesConcise Review For Primary-Care Physicians: Evaluation of ProteinuriaRomadhona KhoiriNo ratings yet
- Approach: A. How The Kidney Handle The Proteins?Document9 pagesApproach: A. How The Kidney Handle The Proteins?Rashed ShatnawiNo ratings yet
- Proteinuria BasicMechanismsPathophys PDFDocument147 pagesProteinuria BasicMechanismsPathophys PDFLedira Dara IsmiNo ratings yet
- A2M ProteinuriaDocument12 pagesA2M ProteinuriaElsiana LaurenciaNo ratings yet
- Judith Blaine (Eds.) - Proteinuria - Basic Mechanisms, Pathophysiology and Clinical Relevance-Springer International Publishing (2016)Document147 pagesJudith Blaine (Eds.) - Proteinuria - Basic Mechanisms, Pathophysiology and Clinical Relevance-Springer International Publishing (2016)Rubén Casas BenítezNo ratings yet
- Buletin DBDDocument8 pagesBuletin DBDLedira Dara IsmiNo ratings yet
- Chemical TestsDocument51 pagesChemical TestsNicole Jane RobesNo ratings yet
- Screening For Diabetic Nephropathy: Take Your Blinkers Off: Ahmed Eid, Shafiq Yusuff, Marie-France KongDocument2 pagesScreening For Diabetic Nephropathy: Take Your Blinkers Off: Ahmed Eid, Shafiq Yusuff, Marie-France KongRaodatul IstiharohNo ratings yet
- 2 Tietz 2012 Kidney Function TestsDocument39 pages2 Tietz 2012 Kidney Function TestsIvana BajunovicNo ratings yet
- Proteinuria - WikipediaDocument43 pagesProteinuria - WikipediaJamesNo ratings yet
- Figure 61-2 Approach To The Patient With HematuriaDocument3 pagesFigure 61-2 Approach To The Patient With HematuriaGood Luck sumsNo ratings yet
- Bence Jones ProteinDocument7 pagesBence Jones ProteinRahman HermansyahNo ratings yet
- Session TwoDocument8 pagesSession TwoBenard apiriNo ratings yet
- Viswanathan2011 PDFDocument6 pagesViswanathan2011 PDFRennilia NitaNo ratings yet
- TestyDocument21 pagesTestyNa ClNo ratings yet
- CLINICAL MICROSCOPY UrinalysisDocument131 pagesCLINICAL MICROSCOPY UrinalysisEng CirroNo ratings yet
- Hematological and Metabolical Aspects From Laboratory MediDocument109 pagesHematological and Metabolical Aspects From Laboratory MediNadirNo ratings yet
- Biochem2 Practical1Document5 pagesBiochem2 Practical1puhranee nathanNo ratings yet
- REVIEW 2023 AUBF Basics On Chemical Tests For UrineDocument84 pagesREVIEW 2023 AUBF Basics On Chemical Tests For UrineJheshari VinaNo ratings yet
- 2002 Kelly 660 7Document9 pages2002 Kelly 660 7Luthie SinghNo ratings yet
- Pediatric Nephrotic Nephritic SyndromesDocument18 pagesPediatric Nephrotic Nephritic SyndromesBryan AtasNo ratings yet
- Lecture 1 ProteinsDocument24 pagesLecture 1 ProteinsMaria Amelia MercaNo ratings yet
- Urine Dipstick Testing + Common Renal Problem 2012Document52 pagesUrine Dipstick Testing + Common Renal Problem 2012Ainul ArinaNo ratings yet
- Primary Care Approach To Proteinuria: Amir Said Alizadeh Naderi, MD, and Robert F. Reilly, MDDocument6 pagesPrimary Care Approach To Proteinuria: Amir Said Alizadeh Naderi, MD, and Robert F. Reilly, MDraviibtNo ratings yet
- Chemical Examination of Urine (Part 1)Document19 pagesChemical Examination of Urine (Part 1)Christine CalumaNo ratings yet
- General Description of Glomerular Syndromes: Isolated ProteinuriaDocument2 pagesGeneral Description of Glomerular Syndromes: Isolated ProteinuriaMovie Scene BankNo ratings yet
- Endocrine Function of Pancreas: 1) Insulin) Hypoglycaemic Factor)Document10 pagesEndocrine Function of Pancreas: 1) Insulin) Hypoglycaemic Factor)mahmoud ayyadNo ratings yet
- All Clinical PathologyDocument100 pagesAll Clinical Pathologyمروة خليل حسن حسينNo ratings yet
- CLINICAL MICROSCOPY (Urinalysis)Document131 pagesCLINICAL MICROSCOPY (Urinalysis)Roderick95% (19)
- Urine Analysis and BiuretDocument30 pagesUrine Analysis and BiuretTom Anthony TonguiaNo ratings yet
- Clinical ChemistryDocument12 pagesClinical ChemistryClark Lopez100% (1)
- Case Presentation and Review of LiteratureDocument65 pagesCase Presentation and Review of LiteratureShrey BhatlaNo ratings yet
- The Patophysiology of Elevated Vit B12Document11 pagesThe Patophysiology of Elevated Vit B12Prasetya Ismail PermadiNo ratings yet
- 1 Glomerular DiseasesDocument127 pages1 Glomerular DiseasesCoy NuñezNo ratings yet
- Wikipedia: 3.1.-Una Patologia On Està Implicada. Modificació Estructural I Funcional (100 Paraules) (Jose)Document4 pagesWikipedia: 3.1.-Una Patologia On Està Implicada. Modificació Estructural I Funcional (100 Paraules) (Jose)jcasanovas1995No ratings yet
- ElectrophoresisDocument27 pagesElectrophoresisAdnan Al-aniNo ratings yet
- Aldesleukin For Injection RX Only: DescriptionDocument16 pagesAldesleukin For Injection RX Only: Descriptionapi-26302710No ratings yet
- Evaluation of Fresh Frozen Plasma Administration in Dogs With Pancreatitis: 77 Cases (1995 2005)Document6 pagesEvaluation of Fresh Frozen Plasma Administration in Dogs With Pancreatitis: 77 Cases (1995 2005)soledadDC329No ratings yet
- Proteinuria in Diabetic Kidney Disease: A Mechanistic ViewpointDocument15 pagesProteinuria in Diabetic Kidney Disease: A Mechanistic ViewpointangelramonrNo ratings yet
- Peptide and Protein DeliveryFrom EverandPeptide and Protein DeliveryChris Van Der WalleRating: 2 out of 5 stars2/5 (1)
- Dr. Ralph Moss Interview: Medical Writer, Author, and FilmmakerDocument27 pagesDr. Ralph Moss Interview: Medical Writer, Author, and FilmmakerRosa AlvarezNo ratings yet
- TranscriptionDocument23 pagesTranscriptionNikhil PularruNo ratings yet
- NRC Guidelines GujrathDocument68 pagesNRC Guidelines GujrathNirajkumar KondekarNo ratings yet
- Andre Tan UPDATED M3 Surgical NotesDocument285 pagesAndre Tan UPDATED M3 Surgical Noteskenyandoctor2880% (5)
- Aberdeenvaricoseveinsquestionnaire PDFDocument4 pagesAberdeenvaricoseveinsquestionnaire PDFdesyislamiatiNo ratings yet
- Nursing Care Plan: Holy Name University College of Health Sciences Department of Nursing Tagbilaran City, BoholDocument4 pagesNursing Care Plan: Holy Name University College of Health Sciences Department of Nursing Tagbilaran City, BoholAllison CrookeNo ratings yet
- Reverse TsaDocument4 pagesReverse Tsaprwill00No ratings yet
- Pulmonary Function TestDocument7 pagesPulmonary Function TestGhada HusseinNo ratings yet
- Health Crisis Slams Disney, But More Bloodletting Ahead: For Personal, Non-Commercial Use OnlyDocument30 pagesHealth Crisis Slams Disney, But More Bloodletting Ahead: For Personal, Non-Commercial Use OnlyMiguel DiazNo ratings yet
- Quarter 4 Week 1 Technical Terms in ResearchDocument7 pagesQuarter 4 Week 1 Technical Terms in Researchsugarnicolas00No ratings yet
- Bipolar Disorder Journal Reading (International Journal Research of Pharmacy)Document19 pagesBipolar Disorder Journal Reading (International Journal Research of Pharmacy)Imron RosyadiNo ratings yet
- 0226.OPWDD Letter From MembersDocument2 pages0226.OPWDD Letter From MembersZacharyEJWilliamsNo ratings yet
- Volunteer Report FinalDocument11 pagesVolunteer Report FinalBeenish JehangirNo ratings yet
- IM-Module B Summarized Notes (IBD)Document69 pagesIM-Module B Summarized Notes (IBD)DeepbluexNo ratings yet
- Msds PG LyondellDocument9 pagesMsds PG LyondellGia Minh Tieu TuNo ratings yet
- MNT-Dislipidemia-Unja 20022019 PDFDocument48 pagesMNT-Dislipidemia-Unja 20022019 PDFAnonymous o3Q3QXENo ratings yet
- Xii Class Practical FileDocument12 pagesXii Class Practical FileBhavik Verma100% (1)
- Obstetrics & GynecologyDocument10 pagesObstetrics & GynecologyRaul DoctoNo ratings yet
- Lesch-Nyhan SyndromeDocument4 pagesLesch-Nyhan Syndromeapi-209017848No ratings yet
- Acne Herbal TreatmentDocument7 pagesAcne Herbal TreatmentPriyanka Bundhoo100% (1)
- RITM LeprosyDocument3 pagesRITM LeprosyDanielle Vince CapunoNo ratings yet
- Liver CancerDocument16 pagesLiver CancerMark James MelendresNo ratings yet
- Drugs With Important Actions On Blood RevisiDocument23 pagesDrugs With Important Actions On Blood RevisiRudi AgustiraNo ratings yet
- Seizure: Eugen Trinka, Reetta KälviäinenDocument9 pagesSeizure: Eugen Trinka, Reetta KälviäinenAaron Nureña JaraNo ratings yet
- Cardiac CycleDocument3 pagesCardiac CycleNorazlina MnNo ratings yet
- Sabutamol SalbutamolDocument2 pagesSabutamol SalbutamolAnanda Felton FalconNo ratings yet
- Bacteria Vs Viruses and DiseasesDocument38 pagesBacteria Vs Viruses and DiseasesNha HoangNo ratings yet
- Atrium Symposium LINC 2012 Dr. GoverdeDocument45 pagesAtrium Symposium LINC 2012 Dr. GoverdegodefroyciosiNo ratings yet
- Using Master Tung's Gallbladder Points For Diseases of The Head and NeckDocument2 pagesUsing Master Tung's Gallbladder Points For Diseases of The Head and NeckTrần Hồ Thạnh Phú100% (1)
- Slide IBSDocument34 pagesSlide IBSRamadhian Galih PratamaNo ratings yet