Professional Documents
Culture Documents
Interventions For Kidney Disease in HSP
Interventions For Kidney Disease in HSP
Uploaded by
Gavin TexeirraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Interventions For Kidney Disease in HSP
Interventions For Kidney Disease in HSP
Uploaded by
Gavin TexeirraCopyright:
Available Formats
Interventions for preventing and treating kidney disease in
Henoch-Schnlein Purpura (HSP) (Review)
Chartapisak W, Opastirakul S, Hodson EM, Willis NS, Craig JC
This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library
2010, Issue 4
http://www.thecochranelibrary.com
Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
T A B L E O F C O N T E N T S
1 HEADER . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
1 ABSTRACT . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
2 PLAIN LANGUAGE SUMMARY . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
2 SUMMARY OF FINDINGS FOR THE MAIN COMPARISON . . . . . . . . . . . . . . . . . . .
6 BACKGROUND . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
6 OBJECTIVES . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
6 METHODS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
8 RESULTS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
Figure 1. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 10
Figure 2. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 12
Figure 3. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 13
14 ADDITIONAL SUMMARY OF FINDINGS . . . . . . . . . . . . . . . . . . . . . . . . . .
21 DISCUSSION . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
23 AUTHORS CONCLUSIONS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
23 ACKNOWLEDGEMENTS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
24 REFERENCES . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
26 CHARACTERISTICS OF STUDIES . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
44 DATA AND ANALYSES . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
Analysis 1.1. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 1 Persistent kidney disease at any time after treatment. . . . . . . . . . . . . . 46
Analysis 1.2. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 2 Number of children with continuing kidney disease at different time points. . . . . . 47
Analysis 1.3. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 3 Continuing kidney disease at different time points (study with high risk of bias excluded). 48
Analysis 1.4. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 4 Number of children with kidney disease in rst month/with kidney disease at follow-up. . 50
Analysis 1.5. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 5 Number developing severe kidney disease. . . . . . . . . . . . . . . . . . 50
Analysis 1.6. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 6 Duration of kidney disease. . . . . . . . . . . . . . . . . . . . . . . 51
Analysis 1.7. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease, Outcome 7 Gastrointestinal complications requiring hospital admission. . . . . . . . . . . . 51
Analysis 2.1. Comparison 2 Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with supportive
therapy for prevention of persistent kidney disease, Outcome 1 Kidney disease at any time. . . . . . . . 52
Analysis 2.2. Comparison 2 Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with supportive
therapy for prevention of persistent kidney disease, Outcome 2 Kidney disease at any time. . . . . . . . 52
Analysis 3.1. Comparison 3 Heparin compared with placebo for prevention of persistent kidney disease, Outcome 1 Any
kidney disease at 3 months after onset or relapse. . . . . . . . . . . . . . . . . . . . . . . 53
Analysis 3.2. Comparison 3 Heparin compared with placebo for prevention of persistent kidney disease, Outcome 2 Type
of kidney disease at 3 months or more after onset or relapse. . . . . . . . . . . . . . . . . . . 53
Analysis 3.3. Comparison 3 Heparin compared with placebo for prevention of persistent kidney disease, Outcome 3 Time
to development of kidney disease. . . . . . . . . . . . . . . . . . . . . . . . . . . . 54
Analysis 4.1. Comparison 4 Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease,
Outcome 1 Persistent kidney disease. . . . . . . . . . . . . . . . . . . . . . . . . . . 54
Analysis 4.2. Comparison 4 Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease,
Outcome 2 Persistent severe kidney disease. . . . . . . . . . . . . . . . . . . . . . . . 55
Analysis 4.3. Comparison 4 Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease,
Outcome 3 ESKD. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 55
Analysis 5.1. Comparison 5 Cyclosporin compared with methylprednisolone for treatment of severe kidney disease,
Outcome 1 Number without remission at 3 months. . . . . . . . . . . . . . . . . . . . . 56
i Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 5.2. Comparison 5 Cyclosporin compared with methylprednisolone for treatment of severe kidney disease,
Outcome 2 Number without remission at last follow-up. . . . . . . . . . . . . . . . . . . . 56
56 APPENDICES . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
60 WHATS NEW . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
60 HISTORY . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
60 CONTRIBUTIONS OF AUTHORS . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
61 DECLARATIONS OF INTEREST . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
61 DIFFERENCES BETWEEN PROTOCOL AND REVIEW . . . . . . . . . . . . . . . . . . . . .
61 INDEX TERMS . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
ii Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
[Intervention Review]
Interventions for preventing and treating kidney disease in
Henoch-Schnlein Purpura (HSP)
Wattana Chartapisak
2
, Sauwalak Opastirakul
2
, Elisabeth M Hodson
1
, Narelle S Willis
3
, Jonathan C Craig
4
1
a) Centre for Kidney Research, The Childrens Hospital at Westmead, b) School of Public Health, The University of Sydney, Westmead,
Australia.
2
Department of Pediatrics, Chiang Mai University, Chiang Mai, Thailand.
3
Cochrane Renal Group, Centre for Kidney
Research, The Childrens Hospital at Westmead, Westmead, Australia.
4
(a) Cochrane Renal Group, Centre for Kidney Research, The
Childrens Hospital at Westmead, (b) School of Public Health, The University of Sydney, Westmead, Australia
Contact address: Elisabeth M Hodson, a) Centre for Kidney Research, The Childrens Hospital at Westmead, b) School of Public
Health, The University of Sydney, Locked Bag 4001, Westmead, NSW, 2145, Australia. Elisah@chw.edu.au.
Editorial group: Cochrane Renal Group.
Publication status and date: Edited (no change to conclusions), published in Issue 4, 2010.
Review content assessed as up-to-date: 26 November 2008.
Citation: Chartapisak W, Opastirakul S, Hodson EM, Willis NS, Craig JC. Interventions for preventing and treating kidney dis-
ease in Henoch-Schnlein Purpura (HSP). Cochrane Database of Systematic Reviews 2009, Issue 3. Art. No.: CD005128. DOI:
10.1002/14651858.CD005128.pub2.
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
A B S T R A C T
Background
To determine the benets and harms of therapies used to prevent or treat kidney disease in Henoch-Schnlein Purpura (HSP).
Objectives
To evaluate the benets and harms of different agents (used singularly or in combination) compared with placebo or no treatment or
another agent for the prevention or treatment of kidney disease in patients with HSP.
Search strategy
Randomised controlled trials (RCTs) and quasi-RCTs were identied fromthe Cochrane Renal Groups specialised register, the Cochrane
Central Register of Controlled Trials (CENTRAL), MEDLINE and EMBASE using optimally sensitive search strategies combined
with search terms for HSP.
Selection criteria
RCTs comparing any intervention used to prevent or treat kidney disease in HSP compared with placebo, no treatment or other agents
were included.
Data collection and analysis
Three authors independently assessed trial quality and extracted data from each study. Statistical analyses were performed using the
random effects model and the results were expressed as risk ratio (RR) for dichotomous outcomes and mean difference (MD) for
continuous outcomes with 95% condence intervals (CI).
1 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Main results
Ten studies (1230 children) were identied. There was no signicant difference in the risk of persistent kidney disease at six months
(3 studies, 379 children: RR 0.51, 95% CI 0.24 to 1.11) and 12 months (3 studies, 498 children: RR 1.02, 95% CI 0.40 to 2.62) in
children given prednisone for 14 to 28 days at presentation of HSP compared with placebo or supportive treatment. In children with
severe kidney disease, there was no signicant difference in the risk of persistent kidney disease with cyclophosphamide compared with
supportive treatment (1 study, 56 children: RR 1.07, 95% CI 0.65 to 1.78) and with cyclosporin compared with methylprednisolone
(1 study, 19 children: RR 0.39, 95% CI 0.14 to 1.06).
Authors conclusions
Data from RCTs for any intervention used in improve kidney outcomes in children with HSP are very sparse except for short-term
prednisone. There was no evidence of benet of prednisone in preventing serious long-term kidney disease in HSP.
P L A I N L A N G U A G E S U M M A R Y
Interventions to prevent or treat serious kidney disease in patients with Henoch-Schnlein Purpura
Henoch-Schnlein Purpura (HSP) causes inammation of small blood vessels in children and affects approximately 20/100,000
children annually. Symptoms and signs include a purpuric skin rash (which comprises small spots and larger bruises), abdominal pain,
gastrointestinal bleeding, joint pain and swelling, facial swelling and evidence of kidney disease with blood and protein in the urine.
Kidney disease occurs in about one third of children with HSP. In the majority this is mild (small amounts of blood in the urine
only) and resolves completely but a few children have persistent kidney disease that can progress to kidney failure. Treatments with
medications that suppress the immune system (prednisone) and treatments to prevent blood clotting (aspirin, heparin) have been
administered to children at diagnosis to prevent serious kidney disease. Also treatments which suppress the immune system(prednisone,
methylprednisolone, cyclophosphamide and cyclosporin) have been used in an attempt to treat serious kidney disease in HSP and
prevent progression to kidney failure.
This review identied ve studies (789 children) which compared prednisone tablets given for 14-28 days with placebo tablets or
no specic treatment for the prevention of serious kidney disease at 6-12 months after onset of HSP. No signicant reduction in the
frequency of serious kidney disease was demonstrated. Two studies (138 children) showed no benet of aspirin and dipyridamole
(antiplatelet agents) to prevent serious kidney disease. One study (228 children) suggested that heparin given by injection could reduce
the risk for serious kidney disease but this treatment has the potential side effect of severe bleeding so its administration is not justied
when only one third of children develop kidney disease and in most this is not serious and resolves completely.
In children with serious kidney disease, one study (56 children) showed that cyclophosphamide was no more effective than supportive
treatment in preventing kidney failure. A second study (19 children) found no difference in benet between cyclosporin and methyl-
prednisolone/prednisone but numbers were too small to exclude a benet completely.
Most studies did not provide data on side effects of the treatments given.
There are few data from randomised studies examining interventions used to prevent or treat serious kidney disease in HSP except for
short-term prednisone to prevent kidney disease. There was no evidence of benet of prednisone compared with placebo or no specic
therapy in preventing serious kidney disease in HSP.
2 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
S U M M A R Y O F F I N D I N G S F O R T H E M A I N C O M P A R I S O N [Explanation]
Prednisone versus placebo/supportive treatment for preventing persistent kidney disease in Henoch-Schonlein Purpura (HSP)
Patient or population: patients with HSP
Settings: secondary and tertiary paediatric and paediatric nephrology services
Intervention: prednisone versus placebo/supportive treatment
Outcomes Illustrative comparative risks* (95% CI) Relative effect
(95% CI)
No of Participants
(studies)
Quality of the evidence
(GRADE)
Comments
Assumed risk Corresponding risk
Control prednisone
versus placebo/support-
ive treatment
Persistent kidney dis-
ease at any time after
treatment
(follow-up: 6-12 months
1
)
Medium risk population RR 0.73
(0.43 to 1.24)
789
(5)
moderate
2
105 per 1000 77 per 1000
(45 to 130)
Number of children with
continuing kidney dis-
ease at different time
points - Three months
(follow-up: 6-12 months)
Medium risk population RR 0.82
(0.45 to 1.5)
636
(4)
moderate
2
156 per 1000 128 per 1000
(70 to 234)
Number of children with
continuing kidney dis-
ease at different time
points - Six months
(follow-up: 6-12 months)
Medium risk population RR 0.51
(0.24 to 1.11)
379
(3)
moderate
2
53 per 1000 27 per 1000
(13 to 59)
3
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
Number of children with
continuing kidney dis-
ease at different time
points - Twelve months
(follow-up: 6-12 months)
Medium risk population RR 1.02
(0.4 to 2.62)
498
(3)
moderate
2
103 per 1000 105 per 1000
(41 to 270)
Continuing kidney dis-
ease at different time
points, study with high
risk of bias excluded -
Three months
(follow-up: 6-12 months)
Medium risk population RR 0.95
(0.66 to 1.36)
468
(3)
moderate
3
207 per 1000 197 per 1000
(137 to 282)
Continuing kidney dis-
ease at different time
points, study with high
risk of bias excluded -
Twelve months
(follow-up: 6-12 months)
Medium risk population RR 1.28
(0.7 to 2.32)
330
(2)
moderate
3
104 per 1000 133 per 1000
(73 to 241)
Number developing se-
vere kidney disease
(follow-up: 6-12 months)
Medium risk population RR 1.92
(0.57 to 6.5)
461
(2)
low
4,5
21 per 1000 40 per 1000
(12 to 136)
*The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the
assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
CI: Confidence interval; RR: Risk ratio;
GRADE Working Group grades of evidance
High quality: Further research is very unlikely to change our confidence in the estimate of effect.
Moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate.
Low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate.
Very low quality: We are very uncertain about the estimate.
1
Islek 1999 did not specify duration of follow-up
2
Mollica 1992 (with inadequate allocation concealment and no blinding) showed benefit of prednisone 4
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
3
Wide confidence intervals related to small numbers in studies
4
Ronkainen 2006 did not provide definition of serious disease
5
Small numbers of events
xxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxx
5
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
B A C K G R O U N D
Henoch-Schnlein Purpura (HSP) is a primary small vessel vas-
culitis. It is the most common systemic vasculitis in children
though adults may also be affected. The annual incidence of
HSP in children varies between 13.5 and 20/100,000 (Gardner-
Medwin 2002; Steward 1988). The incidence is highest inchildren
aged four to six years (70.3/100,000 children) (Gardner-Medwin
2002). This immunologically-mediated vasculitis involves vari-
ous organ systems including skin, kidney, muscle, joints, gut and
brain. Clinical manifestations include purpuric skin lesions, ab-
dominal pain, gastrointestinal bleeding, arthropathy and kidney
disease (Saulsbury 1999). The international Consensus Confer-
ence on Nomenclature of Systemic Vasculitides has characterised
this syndrome as a vasculitis with IgA dominant immune de-
posits affecting small vessels and typically involving skin, gut, and
glomeruli and associated with arthralgias and arthritis (Jennette
1994).
Glomerulonephritis (GN) is one of the major complications of
HSP. Clinically, kidney involvement is manifested by microscopic
or macroscopic haematuria, proteinuria, nephrotic syndrome and
reduced kidney function. In a systematic reviewof studies (Narchi
2005) of unselected patients, kidney involvement occurred in34%
of children; 80%had isolated haematuria and/or proteinuria while
20% had acute nephritic syndrome or nephrotic syndrome. Kid-
ney disease, if it did occur, developed early - by four weeks in
85% and by six months in nearly all children. Persistent kidney
disease (hypertension, reduced function, nephrotic or nephritic
syndrome) occurred in 1.8% of children overall but the incidence
varied with the severity of the kidney disease at presentation. It
occurred in 5% of children with isolated haematuria and/or pro-
teinuria but in 20% who had acute nephritic syndrome and/or
nephrotic syndrome in the acute phase. In one series of 100 con-
secutive patients, kidney disease occurred in 40 children. Of these
33 (83%) had microscopic haematuria alone and seven (17%)
had macroscopic haematuria. Twenty ve (63%) patients also had
proteinuria and three (7.5%) had nephrotic syndrome (Saulsbury
1999).
In general, the prognosis for long-term kidney function in HSP is
excellent in children with microscopic or macroscopic haematuria
alone. However patients with nephrotic syndrome and reduced
kidney function frequently show a progressive course to end-stage
kidney disease (ESKD). In a study of 78 children with HSP and
kidney involvement presenting to two paediatric nephrology ser-
vices, 44% of children presenting with acute nephritic syndrome
and/or nephrotic syndrome compared with 13% presenting with
haematuria and/or proteinuria had hypertension or impaired kid-
ney function at a mean follow-up of 23.4 years (Goldstein 1992).
Corticosteroid therapy is commonly used in the acute phase of
HSP, particularly for abdominal pain. Controversy remains as to
whether corticosteroids can prevent the development of kidney
involvement and/or reduce its severity in HSP. One systematic re-
view concluded that early corticosteroid therapy may reduce the
risk of developing persistent kidney disease (Weiss 2007). How-
ever two other systematic reviews concluded that the benet of
corticosteroids in preventing persistent kidney disease remained
unproven (Wyatt 2001; Zaffanello 2007). Similarly there remains
considerable uncertainty about the efcacy of therapies to prevent
progression to chronic or ESKD in children with HSP-associated
acute nephritis or nephrotic syndrome. Corticosteroid therapy,
azathioprine, cyclophosphamide, cyclosporine, antiplatelet ther-
apy, anticoagulants and plasmapheresis have been used in such
patients (Bergstein 1998; Flynn 2001; Foster 2000; Iijima 1998;
Niaudet 1998; Ronkainen 2003; Shenoy 2007). Although multi-
ple treatment modalities has been used for treat GN in HSP, there
is no consensus on the efcacy of various therapies. The aims of
this systematic review were to determine the benets and harms
of different interventions used to prevent or treat persistent kid-
ney disease in HSP. The scope was deliberately broad because ran-
domised controlled trials (RCTs) in HSP are few, and variability
in the spectrum of kidney disease included in the relevant studies
was very likely.
O B J E C T I V E S
To evaluate the benets and harms of different agents (used sin-
gularly or in combination) compared with placebo, no treatment
or a single agent for:
The prevention of severe kidney disease in patients with
HSP without kidney disease at presentation.
The prevention of severe kidney disease in patients with
HSP and mild kidney disease (microscopic haematuria, mild
proteinuria) at presentation.
The treatment of established severe kidney disease
(macroscopic haematuria, proteinuria, nephritic syndrome,
nephrotic syndrome with or without acute kidney failure) in
HSP.
The prevention of recurrent episodes of HSP associated
kidney disease.
M E T H O D S
Criteria for considering studies for this review
Types of studies
All RCTs and quasi-RCTS (RCTs in which allocation to treat-
ment was obtained by alternation, use of alternate medical records,
date of birth or other predictable methods) looking at the benets
6 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
and harms of different therapeutic modalities for the prevention
or treatment of kidney disease in HSP. If crossover studies were
identied, the rst period of randomised crossover studies were to
be included.
Types of participants
Inclusion criteria
Patients of any age with HSP with or without kidney disease mani-
festations (microscopic haematuria, macroscopic haematuria, pro-
teinuria, nephrotic syndrome, acute nephritic syndrome, reduced
function, acute kidney failure).
Exclusion criteria
Patients with other forms of primary or secondary GNsuch as IgA
nephropathy, mesangiocapillary GN, membranous GN, systemic
lupus erythematosus, rapidly progressive GN not associated with
HSP, other systemic vasculitides.
Types of interventions
1. Immunosuppressive agents including corticosteroids,
alkylating agents, azathioprine, mycophenolate, cyclosporin.
2. Anticoagulants and antiplatelet agents including warfarin,
dipyridamole, aspirin, heparin.
3. Angiotensin-converting enzyme inhibitors (ACEi) and
angiotensin-receptor blockers (ARB).
4. Fish oil.
5. Immunoglobulin G, plasma exchange, antibody therapy.
6. Dapsone.
7. The above agents used individually or in combination will
be studied.
8. Different durations of the same interventions.
Types of outcome measures
1. ESKD (including dialysis and transplantation).
2. Signicant increase in serum creatinine (SCr) as dened by
the trialists.
3. Signicant reduction in glomerular ltration rate (GFR) as
dened by the trialists.
4. Hypertension due to HSP associated kidney disease.
5. Development, persistence or worsening of proteinuria as
dened by the trialists.
6. Nephrotic syndrome, nephritic syndrome, acute kidney
insufciency.
7. Patient mortality.
8. Biopsy result including percent of crescent formation,
chronicity index, sclerosis, brosis.
9. Quality of life.
10. Complications of therapy e.g. infection, bleeding,
neutropenia, hypertension
Search methods for identication of studies
Electronic searches
1. The Cochrane Renal Groups specialised register and the
Cochrane Central Register of Controlled Trials (CENTRAL) in
The Cochrane Library, (Issue 4, 2008). CENTRAL and the Renal
Groups specialised register contain the handsearched results of
conference proceedings from general and speciality meetings.
This is an ongoing activity across the Cochrane Collaboration
and is both retrospective and prospective (http://
www.cochrane.us/masterlist.asp). Therefore we were not
specically search conference proceedings. Please refer to The
Cochrane Renal Groups Module in The Cochrane Library for the
most up-to-date list of conference proceedings (Renal Group
2009).
2. MEDLINE (from 1966) using the optimally sensitive
strategy developed for the Cochrane Collaboration for the
identication of RCTs (Lefebvre 2008) with a specic search
strategy developed with input from the Cochrane Renal Groups
Trial Search Co-ordinator.
3. EMBASE (from 1980) using a search strategy adapted from
that developed for the Cochrane Collaboration for the
identication of RCTs (Lefebvre 2008) together with a specic
search strategy developed with input from the Cochrane Renal
Groups Trial Search Co-ordinator.
See Appendix 1 for search terms used.
Searching other resources
Reference lists of nephrology textbooks, review articles and
relevant studies were also searched.
Data collection and analysis
Selection of studies
The search strategy described was used to obtain titles and ab-
stracts of studies that might be relevant to the review. The titles
and abstracts were screened independently by two authors, who
discarded studies that were not applicable. However studies and
reviews that might have included relevant data or information on
studies were retained initially. Three authors independently as-
sessed retrieved abstracts and, if necessary the full text, of these
studies to determine which studies satised the inclusion criteria.
Quality assessment was undertaken by two authors.
7 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Data extraction and management
Data extraction was carried out by three authors independently
using standard data extraction forms. No studies reported in non-
English language journals were identied. No duplicate publica-
tions were identied. Further information from the original au-
thor was requested by writtencorrespondence to four authors from
whomadditional trial information was obtained fromtwo authors
(Dudley 2007; Ronkainen 2006a). Disagreements were resolved
by discussion.
Assessment of risk of bias in included studies
The following items will be assessed using the risk of bias assess-
ment tool (Higgins 2008) (see Appendix 2).
Was there adequate sequence generation?
Was allocation adequately concealed?
Was knowledge of the allocated interventions adequately
prevented during the study?
Were incomplete outcome data adequately addressed?
Are reports of the study free of suggestion of selective
outcome reporting?
Was the study apparently free of other problems that could
put it at a risk of bias?
Measures of treatment effect
For dichotomous outcomes (any kidney disease) results were ex-
pressed as risk ratio (RR) with 95% CIs. For continuous out-
comes (duration of haematuria or proteinuria), the mean differ-
ence (MD) with 95% CIs was calculated. Data were pooled us-
ing the random effects model but the xed effect model was also
analysed to ensure robustness of the model chosen. Adverse effects
were inadequately reported so could not be tabulated.
Assessment of heterogeneity
Heterogeneity was analysed using a chi squared test onN-1 degrees
of freedom, with an alpha of 0.05 used for statistical signicance
and with the I test (Higgins 2003). I values of 25%, 50% and
75% correspond to low, medium and high levels of heterogeneity.
Assessment of reporting biases
Insufcient studies on any intervention were available to assess
reporting bias using funnel plots.
Subgroup analysis and investigation of heterogeneity
We hypothesised that certain between-study differences in partic-
ipants (severity of kidney disease, kidney pathology, age), inter-
ventions (agent, dose and duration of treatment) and study qual-
ity might explain any observed heterogeneity of treatment effects.
Examination of these possible between-study differences by sub-
group analysis was attempted but was limited by insufcient study
data.
R E S U L T S
Description of studies
See: Characteristics of includedstudies; Characteristics of excluded
studies.
Twelve studies were identied fromthe literature search. Two stud-
ies were excluded because neither could be conrmed to be RCTs
(Jin 2003; Yu 2001). One study (Yoshimoto 1987a; Yoshimoto
1987b) compared two different interventions with the control in-
tervention and was treated as two studies, thus effectively data
on 1230 children from 11 studies were included. Seven studies
were identied by full text review to be RCTs from 907 stud-
ies obtained from the electronic search (Huber 2004; Islek 1999;
Ronkainen 2006a; Ronkainen 2006b; Tarshish 2004; Yanyan
2001; Yoshimoto 1987a; Yoshimoto 1987b). Two studies were
identied from reference lists of review articles (Mollica 1992;
Peratoner 1990). The tenth study was identied fromthe National
Research Register, National Health Service, United Kingdom and
further information on study methodology and results was ob-
tained directly from the trialists and from a published abstract
(Dudley 2007). Four studies were available in abstract form only
(Islek 1999; Ronkainen 2006b; Yanyan 2001;Yoshimoto 1987a;
Yoshimoto 1987b). All included studies were published inEnglish.
Five studies (789 children) examined the effects of short-duration
corticosteroids (14 to 28 days) on preventing persistent HSP as-
sociated kidney disease at 6 to 12 months after presentation in
comparison with placebo (Dudley 2007; Huber 2004; Ronkainen
2006a) or supportive treatment (Islek 1999; Mollica 1992). Three
studies included children with kidney disease at randomisation
(Dudley 2007; Huber 2004; Ronkainen 2006a). Children consid-
ered to have established HSP associated kidney disease (protein-
uria exceeding 300 mg/L or haematuria exceeding 10 red cells/
high power eld) were excluded from Ronkainen 2006a while
Dudley 2007 and Huber 2004 included children with any degree
of kidney disease at randomisation. Islek 1999 and Mollica 1992
only included children with no haematuria or proteinuria at pre-
sentation.
Peratoner 1990, Yoshimoto 1987a and Yoshimoto 1987b (138
children) evaluated antiplatelet agents (dipyridamole, cyprohep-
tadine and salicylates) in comparison with supportive treatment
and Yanyan 2001 (228 children) compared heparin with placebo.
Peratoner 1990 providedoutcome data separately for childrenwith
and without kidney disease at presentation while the other studies
only included children without kidney disease at randomisation.
Two studies examined the treatment of severe HSP associated
kidney disease (nephrotic range proteinuria, International Study
of Kidney Disease in Children grade III-IV changes on biopsy);
Tarshish 2004 (56 children) compared cyclophosphamide with no
specic treatment and Ronkainen 2006b (19 children) compared
cyclosporin with methylprednisolone.
8 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
No studies examining other immunosuppressive agents (azathio-
prine, mycophenolate), warfarin, ACEi or ARB, sh oil, im-
munoglobulin G, plasma exchange, antibody therapy or dapsone
were identied.
Outcomes were assessed at regular intervals up to six to 12
months in ve studies (Dudley 2007; Huber 2004; Mollica 1992;
Peratoner 1990; Ronkainen 2006a). Two studies reported the out-
comes at the end of the study without providing detailed infor-
mation of the duration of the study (Ronkainen 2006b; Tarshish
2004). The remaining studies did not specify the timing of the
outcome assessment. Denitions for signicant haematuria were
provided in ve studies (Huber 2004; Mollica 1992; Peratoner
1990; Ronkainen 2006a; Tarshish 2004). Dudley 2007 regarded
any degree of haematuria on dipstick as signicant and the other
studies did not report a denition of haematuria. Denitions for
signicant proteinuria using protein/creatinine ratio, timed urine
specimens or dipstick results were specied in six studies (Dudley
2007; Huber 2004; Mollica 1992; Ronkainen 2006a; Ronkainen
2006b; Tarshish 2004). The remaining studies did not provide
a denition of signicant proteinuria. See Table 1: Denition of
kidney disease used in outcome assessment.
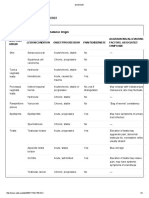
Table 1. Denition of kidney disease used in outcome assessment
Study Timing of outcome Haematuria Proteinuria Blood pressure Kidney function
Dudley 2007 1, 3 and 12 months Any level ondipstick P:Cr > 20 mg/
mmol
Dipstick for
protein
ND ND
Huber 2004 1, 3, 6 and 12
months
5 RBC/HPF or
RBC casts
> 300 mg/L on dip-
stick
> 90th percentile for
age and sex
Elevated Cr
Islek 1999 Unclear ND ND ND ND
Mollica 1992 1, 3, 6 and 12
months
10 RBC/HPF 4 mg/m/h > 2 SD above nor-
mal
Cr 0.8 mg/dL/
mm
Peratoner 1990 During initial 12
months
> 5 RBC/mm ND ND Reduced GFR
Ronkainen 2006a 1, 3 and 6 months > 5 RBC/HPF > 200 mg/L or uri-
nary albumin > 30
mg/L
ND ND
Ronkainen 2006b Unclear ND Remission: P:Cr <
200 mg/mmol or
daily urine protein <
40 mg/m/d
ND ND
Tarshish 2004 Mean follow-up to 7
years
Addis Count
>30,000RBC/h/m
or 1+ on dipstick
3 cells/HPF or >
2 RBC/mm
> 4 mg/h/m
or 2+ or more by
dipstick.
Heavy
proteinuria > 40
mg/h/m
ND GFR < 80 mL/
min/1.73 m
ESKD
Yanyan 2001 Unclear ND ND ND ND
Yoshimoto 1987a Unclear ND ND ND ND
9 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Table 1. Denition of kidney disease used in outcome assessment (Continued)
Yoshimoto 1987b Unclear ND ND ND ND
Cr - creatinine; ESKD - end-stage kidney disease; GFR - glomerular ltration rate; HPF - high power eld; ND - not dened; P:Cr -
protein/creatinine ratio; RBC - red blood cell
Among the eight studies evaluating interventions to prevent per-
sistent HSP associated kidney disease, Dudley 2007 used urinary
protein/creatinine ratio as the primary end point while in the re-
maining studies the primary end point of kidney disease was de-
ned by a composite of haematuria and proteinuria. In the two
studies evaluating interventions for severe HSP associated kidney
disease, the primary end point was dened by composite of pro-
teinuria and reduced kidney function(Ronkainen 2006b; Tarshish
2004).
Risk of bias in included studies
Figure 1 describes the graphical representation of the risk of bias
assessment for all studies.
Figure 1. Methodological quality graph: review authors judgements about each methodological quality
item presented as percentages across all included studies.
Allocation
Three studies (Dudley 2007; Huber 2004; Ronkainen 2006a) re-
ported a satisfactory sequence generation while the method of ran-
domisation was not reported in the remaining studies. Four stud-
ies (Dudley 2007; Huber 2004; Ronkainen 2006a; Tarshish 2004)
reported adequate allocation concealment and one reported inad-
equate allocation concealment (Mollica 1992). In the remaining
studies allocation concealment was unclear.
10 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Blinding
Blinding of participants and investigators occurred in three stud-
ies (Dudley 2007; Huber 2004; Ronkainen 2006a). In one study
participants in both treatment groups received intravenous medi-
cations but it was not clear whether the investigators were blinded
(Yanyan 2001). Blinding of outcome assessors was reported in
three studies (Dudley 2007; Huber 2004; Ronkainen 2006a).
Blinding was not reported in the remaining studies and the out-
come measure of urinalysis reported by participants or investiga-
tors is a subjective outcome measure and could be inuenced by
lack of blinding.
Incomplete outcome data
Reported outcome data was considered satisfactory with a lowrisk
of bias in three studies (Dudley 2007; Huber 2004; Ronkainen
2006a). In Mollica 1992, reporting of outcome data was consid-
ered incomplete and likely to increase risk of bias. In the remain-
ing studies insufcient information was provided to determine
whether all patients entering the study were included in the anal-
ysis so the risk of bias was unclear.
Selective reporting
Reporting appeared to include all important kidney outcomes in
six studies (Dudley 2007; Huber 2004; Mollica 1992; Peratoner
1990; Tarshish 2004; Yanyan 2001). In the remaining studies it
was unclear whether important kidney outcomes (nephrotic syn-
drome, reduced kidney function) had not occurred or had not
been reported.
Other potential sources of bias
Three studies appeared free of other problems that could put it
at risk of bias (Dudley 2007; Huber 2004; Ronkainen 2006a). In
the remaining studies there was insufcient information provided
to determine if there were other potential sources of bias.
Effects of interventions
See: Summary of ndings for the main comparison Prednisone
summary of ndings; Summary of ndings 2 Antiplatelet
summary of ndings; Summary of ndings 3 Heparin summary
of ndings; Summary of ndings 4 Cyclophosphamide summary
of ndings; Summary of ndings 5 Cyclosporin summary of
ndings
Prevention of persistent kidney disease
Prednisone compared with placebo/supportive treatment
In children newly diagnosed with HSP and without signicant
kidney disease, there was no signicant difference in the risk of
any kidney disease following prednisone treatment compared with
placebo or supportive treatment (Analysis 1.1 (5 studies, 789 chil-
dren): RR 0.73, 95% CI 0.43 to 1.24).
Four (Dudley 2007; Huber 2004; Mollica 1992; Ronkainen
2006a) of the ve studies, which evaluated prednisone therapy,
reported outcomes at different time points up to one year. The
fth study did not report the time at which the end point was as-
sessed (Islek 1999). There was no signicant difference in the risk
of development or persistence of kidney disease at one (RR 0.80,
95% CI 0.34 to 1.88), three (RR 0.82, 95% CI 0.45 to 1.50),
six (RR 0.51, 95% CI 0.24 to 1.11) and 12 months (RR 1.02,
95% CI 0.40 to 2.62) with prednisone compared with placebo
or no specic treatment (Analysis 1.2; Figure 2). There was sub-
stantial variability in study outcomes at all time points, except at
six months, which was largely due to one study (Mollica 1992).
This study, which had inadequate allocation concealment and was
therefore at high risk of bias, showed a large benet of prednisone
in contrast to the other three studies. Exclusion of this study elimi-
nated the heterogeneity except at one month (Analysis 1.3; Figure
3).
11 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Figure 2. Forest plot of comparison: 1 Prevention of persistent kidney disease - prednisone compared with
placebo/supportive treatment, outcome: 1.2 Number of children with continuing kidney disease at different
time points.
12 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Figure 3. Forest plot of comparison: 1 Prevention of persistent kidney disease - prednisone compared with
placebo/supportive treatment, outcome: 1.3 Continuing kidney disease at different time points - study with
high risk of bias excluded.
In Ronkainen 2006a post hoc subgroup analysis of 71 children
with kidney disease at or within one month of randomisation
found that kidney disease was signicantly less common at six
months after prednisone therapy compared with placebo (Analysis
1.4.3: RR 0.45, 95% CI 0.21 to 0.98).
Two studies (Dudley 2007; Ronkainen 2006a) reported the
number of children, who developed severe kidney disease with
nephrotic range proteinuria, hypertensionor reduced kidney func-
tion. Again there was no signicant difference in the risk of se-
vere kidney disease between children treated with prednisone or
placebo (Analysis 1.5: RR 1.92, 95% CI 0.57 to 6.50).
Islek 1999 assessed the duration of haematuria and proteinuria
and found no signicant difference in the duration of haematuria
(120 children; MD -1.00, 95% CI -10.26 to 8.26) or proteinuria
(MD -1.60, 95% CI -15.62 to 12.42) (Analysis 1.6). However
condence intervals were very wide.
The risk of gastrointestinal involvement requiring hospital ad-
mission was not signicantly different between prednisone and
placebo (Analysis 1.7 (2 studies, 211 patients): RR 0.58, 95% CI
0.24 to 1.42). In Huber 2004, two children in the placebo group
required surgery for intussusception and were withdrawn fromthe
study. Based on patient diary records in Ronkainen 2006a, chil-
dren on prednisone had a signicantly lower pain severity score for
abdominal or joint pain and had signicantly shorter durations of
abdominal pain but not joint pain compared with placebo.
No adverse effects of prednisone were reported in Huber 2004
and Ronkainen 2006a. In Ronkainen 2006a, children receiving
prednisone had a 1 kg greater increase in weight and 4 mm Hg
increase in diastolic blood pressure during treatment. One child
13 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
had behavioural problems and one had infection, which were con-
sidered related to prednisone therapy in Dudley 2007 while one
child developed abdominal pain related to therapy in the placebo
group. Adverse effects were not reported in Islek 1999 or Mollica
1992.
Dipyridamole, cyproheptadine, salicylates versus supportive
treatment
In children treated with antiplatelet agents (dipyridamole with/
without cyproheptadine, salicylates) or no specic therapies, there
was no signicant difference in the risk of kidney disease occurring
or persisting at any time during follow-up in children without
kidney disease at entry (Analysis 2.1.1 (2 studies, 101 children):
RR 1.16, 95% CI 0.46 to 2.95) or in children with kidney disease
at entry (Analysis 2.1.2 (1 study, 19 children; RR 0.92, 95% CI
0.23 to 3.72).
Ina single small study, there was nosignicant difference inthe risk
of kidney disease with aspirin compared with no specic therapy
(Analysis 2.2 (1 study, 18 children): RR 0.14, 95% CI 0.01 to
2.42). Duration of follow-up was not reported. Adverse effects
were not reported in these studies.
Heparin compared with placebo
A single study found that kidney disease overall (Analysis 3.1:
RR 0.27, 95% CI 0.14 to 0.55), haematuria (Analysis 3.2.1: RR
0.15, 95% CI 0.03 to 0.67) and proteinuria (Analysis 3.2.2: RR
0.37, 95% CI 0.15 to 0.91) was signicantly less common in
children treated with heparin compared with placebo injections
at three months or more after the onset or relapse of HSP. The
risk for nephrotic syndrome did not differ signicantly between
groups but event numbers were small resulting in wide condence
intervals (Analysis 3.2.3: RR 0.31, 95% CI 0.03 to 2.89). The
development of kidney disease was signicantly delayed in the
heparin treated group compared with placebo (Analysis 3.3: MD
47.3 days, 95% CI 34.24 to 60.36). No child developed severe
bleeding.
Treatment of severe kidney disease
Cyclophosphamide compared with supportive treatment
In a single study of 56 children (Tarshish 2004) with signicant
HSP associated kidney disease (proteinuria, reduced kidney func-
tion, crescents and/or segmental lesions on kidney biopsy) treated
within three months of onset of HSP, there was no signicant
difference in the risk for persistent kidney disease of any severity
(Analysis 4.1: RR 1.07, 95% CI 0.65 to 1.78), severe kidney dis-
ease (heavy proteinuria, reduced GFR, ESKD) (Analysis 4.2: RR
0.88, 95% CI 0.37 to 2.09) or ESKD (Analysis 4.3: RR 0.75,
95% CI 0.18 to 3.05) during follow-up between patients treated
with cyclophosphamide and those given supportive therapy. Ad-
verse effects of cyclophosphamide were not reported.
Cyclosporin compared with methylprednisolone
In a single study (Ronkainen 2006b) involving children with se-
vere kidney disease, all of 10 children treated with cyclosporin
compared with 3/9 treated with methylprednisolone were in re-
mission by three months but the difference was not signicant
(Analysis 5.1: RR 0.08, 95% CI 0.01 to 1.31) due to small pa-
tient numbers. At nal follow-up 7/10 children compared with 2/
9 treated with methylprednisolone were in remission. The differ-
ence was not signicant (Analysis 5.2: RR 0.39, 95% CI 0.14 to
1.06). Adverse effects were not reported.
Other outcomes
In most studies the severity of haematuria and proteinuria, the
degree of kidney dysfunction and the presence of hypertension
were not specied. Dudley 2007 provided informationonprotein/
creatinine ratios and Tarshish 2004 provided separate information
on ESKD.
14 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
A D D I T I O N A L S U M M A R Y O F F I N D I N G S [Explanation]
Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) versus supportive therapy for preventing persistent kidney disease in Henoch-Schonlein Purpura (HSP)
Patient or population: patients with HSP
Settings: secondary and tertiary paediatric and paediatric nephrology services
Intervention: antiplatelet agents (dipyridamole, cyproheptadine, salicylates) versus supportive therapy
Outcomes Illustrative comparative risks* (95% CI) Relative effect
(95% CI)
No of Participants
(studies)
Quality of the evidence
(GRADE)
Comments
Assumed risk Corresponding risk
Control antiplatelet
agents (dipyridamole,
cyproheptadine, salicy-
lates) versus supportive
therapy
Kidney disease at any
time - Dipyridamole +/
- cyproheptadine in chil-
dren without kidney dis-
ease at entry
(follow-up: 12 months
1
)
Medium risk population RR 1.16
(0.46 to 2.95)
101
(2)
low
2,3
210 per 1000 244 per 1000
(97 to 620)
Kidney disease at any
time - Dipyridamole +/
- cyproheptadine in chil-
dren with kidney disease
at entry
(follow-up: 12 months)
Medium risk population RR 0.92
(0.23 to 3.72)
19
(1)
low
2,3
333 per 1000 306 per 1000
(77 to 1239)
Kidney disease at any
time - Aspirin compared
with supportive treat-
ment
Medium risk population RR 0.14
(0.01 to 2.42)
18
(1)
low
2,3
1
5
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
333 per 1000 47 per 1000
(3 to 806)
*The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the
assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
CI: Confidence interval; RR: Risk ratio;
GRADE Working Group grades of evidance
High quality: Further research is very unlikely to change our confidence in the estimate of effect.
Moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate.
Low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate.
Very low quality: We are very uncertain about the estimate.
1
Yoshimoto 1987 did not specify duration of follow-up
2
Small studies with unclear allocation concealment and no blinding
3
Wide confidence intervals
1
6
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
Heparin versus placebo for preventing persistent kidney disease in Henoch-Schonlein Purpura (HSP)
Patient or population: patients with HSP
Settings: tertiary paediatric service
Intervention: heparin versus placebo
Outcomes Illustrative comparative risks* (95% CI) Relative effect
(95% CI)
No of Participants
(studies)
Quality of the evidence
(GRADE)
Comments
Assumed risk Corresponding risk
Control heparin versus placebo
Type of kidney disease at
3 months or more after
onset or relapse
Medium risk population RR 0.15
(0.03 to 0.67)
684
(1)
low
1
110 per 1000 17 per 1000
(3 to 74)
*The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the
assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
CI: Confidence interval; RR: Risk ratio;
GRADE Working Group grades of evidance
High quality: Further research is very unlikely to change our confidence in the estimate of effect.
Moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate.
Low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate.
Very low quality: We are very uncertain about the estimate.
1
Unclear allocation concealment, blinding and duration of follow-up
1
7
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
Cyclophosphamide versus supportive treatment for treating severe kidney disease in Henoch-Schonlein Purpura (HSP)
Patient or population: patients with HSP
Settings: tertiary paediatric nephrology services
Intervention: cyclophosphamide versus supportive treatment
Outcomes Illustrative comparative risks* (95% CI) Relative effect
(95% CI)
No of Participants
(studies)
Quality of the evidence
(GRADE)
Comments
Assumed risk Corresponding risk
Control cyclophosphamide ver-
sus supportive treat-
ment
Persistent kidney dis-
ease
(follow-up: mean 4-7
years
1
)
Medium risk population RR 1.07
(0.65 to 1.78)
56
(1)
moderate
2
300 per 1000 321 per 1000
(195 to 534)
Persistent severe kidney
disease
(follow-up: mean 4-7
years
1
)
Medium risk population RR 0.88
(0.37 to 2.09)
56
(1)
moderate
2
300 per 1000 264 per 1000
(111 to 627)
*The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the
assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
CI: Confidence interval; RR: Risk ratio;
GRADE Working Group grades of evidance
High quality: Further research is very unlikely to change our confidence in the estimate of effect.
Moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate.
Low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate.
Very low quality: We are very uncertain about the estimate.
1
Mean duration of follow-up varied according to end-point and ranged between 4 and 7 years
1
8
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
2
Unclear allocation concealment and duration of follow-up. No blinding.
xxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxxx
1
9
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
Cyclosporin versus methylprednisolone for treating severe kidney disease in Henoch-Schonlein Purpura (HSP)
Patient or population: patients with HSP
Settings: tertiary paediatric nephrology service
Intervention: cyclosporin versus methylprednisolone
Outcomes Illustrative comparative risks* (95% CI) Relative effect
(95% CI)
No of Participants
(studies)
Quality of the evidence
(GRADE)
Comments
Assumed risk Corresponding risk
Control cyclosporin versus
methylprednisolone
Number without remis-
sion at last follow-up
(follow-up: mean 2.9
years)
Medium risk population RR 0.39
(0.14 to 1.06)
19
(1)
low
1,2
300 per 1000 117 per 1000
(42 to 318)
*The basis for the assumed risk (e.g. the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% confidence interval) is based on the
assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
CI: Confidence interval; RR: Risk ratio;
GRADE Working Group grades of evidance
High quality: Further research is very unlikely to change our confidence in the estimate of effect.
Moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate.
Low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate.
Very low quality: We are very uncertain about the estimate.
1
Unclear allocation concealment and no blinding
2
Small number of patients in study
2
0
I
n
t
e
r
v
e
n
t
i
o
n
s
f
o
r
p
r
e
v
e
n
t
i
n
g
a
n
d
t
r
e
a
t
i
n
g
k
i
d
n
e
y
d
i
s
e
a
s
e
i
n
H
e
n
o
c
h
-
S
c
h
n
l
e
i
n
P
u
r
p
u
r
a
(
H
S
P
)
(
R
e
v
i
e
w
)
C
o
p
y
r
i
g
h
t
2
0
1
0
T
h
e
C
o
c
h
r
a
n
e
C
o
l
l
a
b
o
r
a
t
i
o
n
.
P
u
b
l
i
s
h
e
d
b
y
J
o
h
n
W
i
l
e
y
&
S
o
n
s
,
L
t
d
.
D I S C U S S I O N
Summary of main results
We identied 10 RCTs of which eight examined the efcacy of
therapies to prevent persistent kidney disease in HSP and two
examined therapies to treat established severe kidney disease.
Prevention of persistent kidney disease - prednisone
Five studies including three well designedplacebocontrolledRCTs
examined the use of prednisone to prevent persistent kidney dis-
ease. Overall no signicant difference in the number of chil-
dren with persistent kidney disease was identied among chil-
dren treated for 14 to 28 days with prednisone at presentation
of HSP compared with placebo or no specic therapy. Based
on the absolute risk of kidney disease seen in the control group
of 105/1000 children, the corresponding risk of kidney disease
in prednisone treated patients did not differ signicantly at 77/
1000 children (95% CI 45 to 130) Summary of ndings for the
main comparison. Data at specied time points after presenta-
tion (Figure 2) revealed no signicant difference in the number of
children with persistent kidney disease at one, three, six and 12
months. Sensitivity analysis, in which the study with a high risk
of bias was excluded, removed heterogeneity between studies and
tended to make the summary result less favourable towards cor-
ticosteroids (Figure 3). Because of the wide condence intervals
resulting in imprecision of results and heterogeneity, the overall
quality of evidence (GRADE) was considered moderate.
Only two studies assessed the use of prednisone in patients with se-
vere kidney disease and identied no evidence of benet. Because
of small numbers of events resulting in wide condence intervals
and inadequate denition of severe disease, there remains uncer-
tainty as to the efcacy of prednisone in preventing severe HSP
associated kidney disease and the quality of evidence (GRADE)
was considered low.
The lack of signicant differences between prednisone and
placebo/supportive therapy in the numbers with kidney disease
at one, three and six months suggests that prednisone did not re-
sult in more rapid resolution of kidney disease overall. However
Ronkainen 2006a presented a post hoc analysis of 71 children,
who had kidney disease at or within one month of presentation.
Prednisone therapy for 28 days signicantly reduced the number
of children with persistent kidney disease at six months. The study
was not stratied before randomisation for the presence or ab-
sence of kidney disease and the sample size was small so the results
can only be considered as hypothesis-generating. The study only
provided outcome data to six months after randomisation so it
is unclear whether prednisone treatment reduced the number of
patients with persistent HSP associated kidney disease overall or
promoted more rapid resolution of kidney disease compared with
placebo. In addition, children considered to have established kid-
ney disease at randomisation were not included in this study. In
the other two well designed studies (Dudley 2007; Huber 2004)
of prednisone therapy, children with any severity of kidney disease
at presentation were potentially included and a meta-analysis of
these studies showed no signicant difference in the risk for per-
sistent HSP associated kidney disease at 12 months.
Two studies found no signicant difference in the number of
children with abdominal complications of HSP (Huber 2004;
Ronkainen 2006a). However Ronkainen 2006a) reported that the
severity and duration of abdominal pain as well as the duration
of joint pain were signicantly less severe in children treated with
prednisone.
Prevention of persistent kidney disease -
dipyridamole, cyproheptadine, salicylates and heparin
No signicant benet of antiplatelet agents was demonstrated in
two small studies suggesting that these agents have no role in pre-
venting kidney disease inHSP. The studies enrolled small numbers
of patients with few events leading to imprecision of results. They
demonstrated unclear allocation concealment and no blinding so
the quality of evidence (GRADE) was considered low (Summary
of ndings 2).
Yanyan 2001, available inabstract only, demonstrated that heparin
reduced the number of children with kidney disease. However no
details on study methodology were available. Heparin or placebo
were administered to children at onset of disease and at relapse and
it was not possible to determine how many children in each group
received more than one period of treatment. Because of these un-
certainties of study design, the quality of evidence (GRADE) was
considered low (Summary of ndings 3). Though bleeding was
not reported in this study, the use of such a potentially danger-
ous therapy is not justied when only about a third of children
with HSP develop kidney disease and less than 2% develop severe
kidney disease (nephrotic syndrome, nephritic syndrome, kidney
failure) (Narchi 2005).
Treatment of severe kidney disease -
cyclophosphamide and cyclosporin
Children with signicant proteinuria, macroscopic haematuria,
nephrotic syndrome, reduced kidney function are more likely to
progress to ESKD so that treatment has been largely directed to-
wards these children. However only two studies, which examined
the treatment of severe established kidney disease in HSP, were
identied. In children with HSP and nephrotic range proteinuria,
Tarshish 2004 reported no signicant benet of cyclophospha-
mide alone compared with no specic therapy. Because of defects
in study design (unclear allocation concealment, lack of blind-
ing and unclear duration of follow-up), the quality of evidence
(GRADE) was considered to be moderate (Summary of ndings
4).
Ronkainen 2006b suggested that cyclosporin may be more effec-
tive than methylprednisolone and prednisone in inducing remis-
sion in children with HSP and nephrotic range proteinuria, but
21 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
numbers were too small to achieve statistical signicance. Because
of small patient numbers resulting in wide condence intervals,
unclear allocation concealment and lack of blinding, the quality
of the evidence (GRADE) was considered to be low (Summary of
ndings 5).
Overall completeness and applicability of
evidence
Corticosteroids are commonly administered for abdominal pain
in HSP but opinions differ as to whether they are indicated to pre-
vent the development of persistent kidney disease. We identied
ve studies involving 789 children which examined the efcacy
of short course prednisone in the prevention of persistent kidney
disease. In meta-analysis of these studies, no signicant benet
of prednisone was identied. However there remains considerable
residual imprecision in the results as indicated by wide condence
intervals. For example compared with the number with persistent
kidney disease at one year in the control group (103/1000 chil-
dren), the number treated with prednisone with persistent kid-
ney disease was 105/1000 children (RR 1.02). However the wide
condence intervals (41 to 270) indicate that prednisone could
reduce the number of children with kidney disease to 41/1000
or increase it to 270/1000 children (Summary of ndings for the
main comparison). In addition, the potential signicance for long
term kidney function of residual urinary abnormalities could not
be assessed in 3/4 studies, which reported the end point as the
presence of haematuria and/or proteinuria without measuring the
degree of proteinuria by protein/creatinine ratio or 24 hour uri-
nary protein excretion.
Immunosuppressive agents are commonly used in an attempt to
treat established severe kidney disease in HSP with observational
studies suggesting benet of methylprednisolone (Niaudet 1993)
azathioprine (Bergstein 1998), cyclophosphamide (Flynn 2001;
Iijima 1998; Tanaka 2003) and cyclosporin (Ronkainen 2003).
Two studies were identied which evaluated therapies for estab-
lished severe kidney disease. No benet of cyclophosphamide was
identied (Tarshish 2004). The study comparing cyclosporin with
methylprednisolone was too small to establish whether or not cy-
closporin was more effective (Ronkainen 2006b).
No studies examining intravenous methylprednisolone alone or
in combination with other medications or of azathioprine, my-
cophenolate, immunoglobulin or plasma exchange were identi-
ed. No studies examining sh oil, ACEi or ARB or dapsone were
identied. No studies which included adults with HSP or which
specically addressed whether therapy reduced the risk of recur-
rent episodes of HSP were identied.
Quality of the evidence
Two of the ve included studies evaluating prednisone were at a
high risk of bias with unclear or inadequate allocation conceal-
ment, no blinding and unclear duration of follow-up. Studies with
a high risk of bias (inadequate or unclear allocation concealment,
no blinding of participants, investigators or outcome assessors)
are associated with an increased likelihood of results favouring the
study intervention (Schulz 1995; Wood 2008). Exclusion of stud-
ies with a high risk of bias removed heterogeneity between stud-
ies without altering the overall result reinforcing the strength of
the evidence suggesting that prednisone does not prevent serious
kidney disease in children with HSP. However the overall quality
of evidence was considered moderate because of residual impreci-
sion.
Three studies assessed the efcacy of antiplatelet agents or heparin
to prevent kidney disease. All studies were at a high risk of bias so
the quality of the evidence was low.
Two studies assessed the efcacy of immunosuppressive agents
(cyclophosphamide, cyclosporin) to treat serious kidney disease.
Both studies were small and at risk of bias limiting the applicability
of the results to patient management.
Potential biases in the review process
We identied ten studies of which ve were available in abstract
form only although some additional information was obtained
from study authors of two studies. Incomplete reporting of these
studies may result in incomplete information being included in
this systematic review. Further publications of two studies (Dudley
2007; Ronkainen 2006b) could lead to additional information
available for this review or for changes to the information in this
review. Since the protocol was published, the literature search has
been run several times up to November 2008 making it unlikely
that any studies have been missed. However 40% of study reports
in the Cochrane Renal Groups specialised trials register have been
identied by handsearching of conference proceedings so it re-
mains possible that further studies of therapy to prevent or treat
serious kidney disease in HSP will be identied as conference pro-
ceedings from different congresses are searched.
Agreements and disagreements with other
studies or reviews
Three systematic reviews have previously assessed the effects of
corticosteroid therapy to prevent or alter the course of kidney dis-
ease in HSP (Weiss 2007; Wyatt 2001; Zaffanello 2007). All three
included data from RCTs and observational studies. Conclusions
based on non-randomised study designs are more likely to be bi-
ased towards a benet of treatment (Chalmers 1983). Two reviews
determined that it remained unclear whether corticosteroid ther-
apy prevented or altered the course of HSP associated kidney dis-
ease (Wyatt 2001; Zaffanello 2007). The third review concluded
22 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
that corticosteroids decreased the likelihood of developing per-
sistent kidney disease but did not prevent kidney disease (Weiss
2007). This conclusion was based on a meta-analysis of the ad
hoc subgroup of children with kidney abnormalities within one
month of presentation from Ronkainen 2006a combined with
data from two other studies (Huber 2004; Mollica 1992). The
inclusion in this Cochrane review of the most recent large study
(Dudley 2007) which showed no benet of corticosteroid therapy
increases the evidence base from RCTs to support the conclusion
that corticosteroids do not appear to alter the course of kidney
disease in HSP. One reviewalso evaluated immunosuppressive and
other therapies in HSP (Zaffanello 2007). It concluded based on
observational studies that cyclophosphamide was of value in treat-
ing HSP associated kidney disease. The single study evaluating cy-
clophosphamide in the Cochrane review did not show any benet
of cyclophosphamide (Tarshish 2004).
A U T H O R S C O N C L U S I O N S
Implications for practice
Prevention of kidney disease in HSP
No evidence of benet has been identied from RCTs for
the use of prednisone to prevent serious kidney disease in
children with HSP. The quality of the evidence is moderate
suggesting that further research could have an important impact
on our condence in the estimate of effect and could change the
estimate of effect.
Small studies examining antiplatelet agents have not
demonstrated any benet in preventing serious kidney disease
but the quality of evidence is low.
In a single study heparin reduced the risk for kidney disease
but the quality of evidence is low and the use of such a
potentially harmful treatment cannot be justied when only a
third of children with HSP develop kidney disease and most
resolve spontaneously.
Treatment of serious kidney disease in HSP
No evidence of benet has been found for treatment with
cyclophosphamide treatment in children with HSP and severe
kidney disease. The quality of evidence is moderate.
It remains unclear whether cyclosporin is more effective
than methylprednisolone in children with HSP and severe
kidney disease and further studies with longer follow-up are
required. The quality of the evidence is low.
Implications for research
Prevention of serious kidney disease
A further adequately powered RCT of short term
prednisone therapy compared with placebo should be considered
in children, who have or develop kidney disease with HSP or
have risk factors for developing kidney disease including older
age (Shin 2006), severe abdominal pain (Ronkainen 2006a; Shin
2006), persistent (Ronkainen 2006a; Shin 2006) or recurrent
purpura (Shin 2006) with clearly dened end points for kidney
function (GFR), proteinuria (protein/creatinine ratios or timed
urine collections), microscopic and macroscopic haematuria and
hypertension. However recruitment to a placebo controlled RCT
may be difcult since Ronkainen 2006a has demonstrated that
short-course prednisone signicantly reduces the severity and
duration of abdominal pain in children with HSP making it
unlikely that clinicians will be prepared to withhold prednisone
from children with severe HSP-associated abdominal pain.
Treatment of serious kidney disease in HSP
Adequately powered well designed RCTs with at least ve
year follow-up periods are particularly needed in children with
HSP-associated nephritic syndrome and/or nephrotic syndrome.
A multicentre RCT comparing, for example, a six month
course of corticosteroids with short duration corticosteroids (28
days) in children with moderately severe kidney disease (acute
nephritic syndrome or nephrotic syndrome with normal kidney
function, mesangial proliferative GN and < 50% crescents or
sclerosing lesions on biopsy) should be considered.
Based on the data from Ronkainen 2006b comparing
cyclosporin and methylprednisolone, a multicentre RCT should
be set up to compare cyclosporin (with or without prednisone)
with methylprednisolone/prednisone in treating children with
HSP and severe kidney disease (50% or more crescents or
sclerosing lesions on biopsy with or without reduced kidney
function). Clinicians are likely to be reluctant to enter children
with HSP and crescentic GN involving more than 50% of
glomeruli into RCTs with a placebo arm even though currently
no therapy has been shown to be effective in an RCT in such
children.
A C K N O W L E D G E M E N T S
We thank Dr Dudley, Dr Smith and Dr Tizard for
additional information on their RCT. We thank Dr Ronkainen
and Dr Nuutinen for additional information on their RCTs.
23 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
We would like to thank Drs Michael Dillon, Matti
Nuutinen and Lesley Rees for their editorial advice during the
preparation of this review
This work has been presented in part at the 42
nd
Annual
Scientic Meeting of the Australian and New Zealand Society of
Nephrology (Melbourne 2006).
R E F E R E N C E S
References to studies included in this review
Dudley 2007 {published and unpublished data}
Dudley J, Smith G, Llewellyn-Edwards A, Tizard EJ. Randomised
placebo controlled trial to assess the role of early prednisolone on
the development and progression of Henoch-Schonlein Purpura
Nephritis [abstract]. Pediatric Nephrology 2007;22:1457.
Smith G. Randomised, double-blind, placebo controlled study to
determine whether steroids reduce the development of nephropathy
in Henoch-Schonlein purpura. National Research Register, UK
[https://portal.nihr.ac.uk/Proles/NRR.aspx?PublicationID=
M0048086115] 2002. [CENTRAL: CN00449954]
Huber 2004 {published data only}
Huber AM, King J, McLaine P, Klassen T, Pothos M. A
randomized, placebo-controlled trial of prednisolone in early
Henoch Schonlein purpura [ISRCTN85109383]. BMC Medicine
2004; Vol. 2, issue 7. [DOI: 10.1186/1741-7015-2-7]
Islek 1999 {published data only}
Islek I, Sezer T, Totan M, Cakir M, Kucukoduk S. The effect of
prolactic prednisolon therapy on renal involvement in henoch
schoenlein vasculitis. XXXVI Congress of the European Renal
Association European Dialysis & Transplant Association; 1999 Sep
5-8; Madrid (Spain). 1999:103. [CENTRAL: CN00484464]
Mollica 1992 {published data only}
Mollica F, Li VS, Garozzo R, Russo G. Effectiveness of early
prednisone treatment in preventing the development of
nephropathy in anaphylactoid purpura. European Journal of
Pediatrics 1992;151(2):1404. [MEDLINE: 1343079]
Peratoner 1990 {published data only}
Peratoner L, Longo F, Lepore L, Freschi P. Prophylaxis and
therapy of glomerulonephritis in the course of anaphylactoid
purpura. The results of a polycentric clinical trial. Acta Paediatrica
Scandinavica 1990;79(10):9767. [MEDLINE: 2264475]
Ronkainen 2006a {published and unpublished data}
Ronkainen J, Koskimies O, Ala-Houhala M, Antkainen M,
Merenmies J, Rajantie J, et al.Early prednisone therapy in Henoch-
Schonlein purpura: a randomized double-blind, placebo-controlled
trial. Journal of Pediatrics 2006;149(2):2417. [MEDLINE:
16887443]
Ronkainen 2006b {published and unpublished data}
Ronkainen J, Ala-Houhala M, Antkainen M, Jahnukainen T,
Koskimies O, Merenmies J, et al.Cyclosporine A (CyA) versus MP
pulses (MP) in the treatment of severe Henoch-Schonlein Nephritis
(HSN) [abstract]. Pediatric Nephrology 2006;21(10):1531.
Tarshish 2004 {published data only}
Tarshish P, Bernstein J, Edelmann CM Jr. Henoch-Schonlein
purpura nephritis: course of disease and efcacy of
cyclophosphamide. Pediatric Nephrology 2004;19(1):516.
[MEDLINE: 14634864]
Yanyan 2001 {published data only}
Yanyan H, Hongmei S, Lihua S, Min W. Preventive value of
heparin on the occurrence of nephropathy in Henoch-Schoenlein
Purpura: a randomized controlled clinical trial [abstract]. 23rd
International Congress of Paediatrics; 2001 Sep 9-14; Beijing
(China). 2001. [CENTRAL: CN00462028]
Yoshimoto 1987a {published data only}
Yoshimoto M, Ito H, Shindo S, Yamashita F. Evaluation of the
preventive role of dipyridamoleant aspirin against renal
complication in Schonlein-Henoch purpura [abstract]. Pediatric
Nephrology 1987;1(1):C47. [CENTRAL: CN00445875]
Yoshimoto 1987b {published data only}
Yoshimoto M, Ito H, Shindo S, Yamashita F. Evaluation of the
preventive role of dipyridamole and aspirin against renal
complication in Schonlein-Henoch purpura [abstract]. Pediatric
Nephrology 1987;1:C47. [CENTRAL: CN00445875]
References to studies excluded from this review
Jin 2003 {published data only}
Jin ZD, Wang SC, Sun YQ, et al.Effect of Danshao granule on
serum superoxide dismutase activity and malonyldialdehyde
content in children with Henoch-Schonlein purpura nephritis.
Zhongguo Zhongxiyi Jiehe Zqzhi [Chinese Journal of Integrated
Traditional & Western Medicine] 2003;23(12):9057.
Yu 2001 {published data only}
Yu YH. Treatment of purpuric nephritis in children with
Tripterygium Wilfordii Polyglucoside and Radix Salviae
Miltiorrhizae [abstract]. Pediatric Nephrology 2001;16:C78.
Additional references
Bergstein 1998
Bergstein J, Leiser J, Andreoli SP. Response of crescentic Henoch-
Schoenlein purpura nephritis to corticosteroid and azathioprine
therapy. Clinical Nephrology 1998;49(1):914. [MEDLINE:
9491279]
Chalmers 1983
Chalmers TC, Celano P, Sacks HS, Smith H. Bias in treatment
assignment in controlled clinical trials. New England Journal of
Medicine 1983;309(22):135861. [MEDLINE: 6633598]
24 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Flynn 2001
Flynn JT, Smoyer WE, Bunchman TE, Kershaw DB, Sedman AB.
Treatment of Henoch-Schonlein Purpura glomerulonephritis in
children with high-dose corticosteroids plus oral
cyclophosphamide. American Journal of Nephrology 2001;18(4):
34750. [MEDLINE: 11359020]
Foster 2000
Foster BJ, Bernard C, Drummond KN, Sharma AK. Effective
therapy for severe Henoch-Schonlein purpura nephritis with
prednisone and azathioprine: a clinical and histopathologic study.
Journal of Pediatrics 2000;136(3):3705. [MEDLINE: 10700695]
Gardner-Medwin 2002
Garner-Medwin JM, Dolezalova P, Cummins C, Southwood TR.
Incidence of Henoch-Schonlein purpura, Kawasaki disease, and
rare vasculitides in children of different ethnic origins. Lancet 2002;
360(9341):1197202. [MEDLINE: 12401245]
Goldstein 1992
Goldstein AR, White RHW, Akuse R, Chantler C. Long term
follow up of childhood Henoch Schonlein nephritis. Lancet 1992;
339(8788):2802. [MEDLINE: 1346291]
Higgins 2003
Higgins JPT, Thompson SG, Deeks JJ, Altman DG. Measuring
inconsistency in meta-analyses. BMJ 2003;327(7414):55760.
[MEDLINE: 12958120]
Higgins 2008
Higgins JPT, Green S (editors). Cochrane Handbook for
Systematic Reviews of Interventions Version 5.0.0 [updated
February 2008]. The Cochrane Collaboration, 2008. Available
from www.cochrane-handbook.org.
Iijima 1998
Iijima R, Ito-Kariya S, Nakamura H, Yoshikowa N. Multiple
combined therapy for severe Henoch Schonlein nephritis in
children. Pediatric Nephrology 1998;12(3):2448. [MEDLINE:
9630047]
Jennette 1994
Jennette JC, Falk RJ, Andrassy K, Bacon PA, Churg J, Gross W, et
al.Nomenclature of systemic vasculitides. Proposal of an
international consensus conference. Arthritis & Rheumatism 1994;
37(2):18792. [MEDLINE: 8129773]
Lefebvre 2008
Lefebvre C, Manheimer E, Glanville J. Chapter 6: Searching for
studies. In: Higgins JPT, Green S (editors). Cochrane Handbook
for Systematic Reviews of Interventions Version 5.0.0 (updated
February 2008). The Cochrane Collaboration, 2008. Available
from www.cochrane-handbook.org.
Narchi 2005
Narchi H. Risk of long term renal impairment and duration of
follow up recommended for Henoch-Schonlein purpura with
normal or minimal urinary ndings: a systematic review. Archives of
Disease in Childhood 2005;90(9):91620. [MEDLINE: 15871983]
Niaudet 1993
Niaudet P, Murcia I, Beauls H, Broyer M, Habib R. Primary IgA
nephropathies in children: prognosis and treatment. Advances in
Nephrology From the Necker Hospital 1993;2:12140. [MEDLINE:
8427055]
Niaudet 1998
Niaudet P, Habib R. Methylprednisolone pulse therapy in the
treatment of severe forms of Schonlein-Henoch purpura nephritis.
Pediatric Nephrology 1998;12(3):23843. [MEDLINE: 9630046]
Renal Group 2009
Willis NS, Mitchell R, Higgins GY, Webster AC, Craig JC.
Cochrane Renal Group. About The Cochrane Collaboration
(Cochrane Review Groups (CRGs)) 2009, Issue 1. Art. No.:
RENAL (accessed March 2009).
Ronkainen 2003
Ronkainen J, Ala- Houhala M, Huttunen NP, Jahnukainen T,
Koskimies O, Ormala T, et al.Outcome of Henoch-Schoenlein
nephritis with nephrotic-range proteinuria. Clinical Nephrology
2003;60(2):804. [MEDLINE: 12940608]
Saulsbury 1999
Saulsbury FT. Henoch-Schonlein Purpura in children. Report of
100 patients and review of the literature. Medicine 1999;78(6):
395409. [MEDLINE: 10575422]
Schulz 1995
Schulz KF. Chalmers I. Hayes RJ. Altman DG. Empirical evidence
of bias. Dimensions of methodological quality associated with
estimates of treatment effects in controlled trials. JAMA 1995;273
(5):40812. [MEDLINE: 7823387]
Shenoy 2007
Shenoy M, Ognjanovic MV, Coulthard MG. Treating severe
Henoch-Schonlein and IgA nephritis with plasmapheresis alone.
Pediatric Nephrology 2007;22(8):116771. [MEDLINE:
17530298]
Shin 2006
Shin JI, Park JM, Shin YH, Hwang DH, Kim JH, Lee JS.
Predictive factors for nephritis, relapse, and signicant proteinuria
in childhood Henoch-Schonlein purpura. Scandinavian Journal of
Rheumatology 2006;35(1):5660. [MEDLINE: 16467044]
Steward 1988
Steward M, Savage JM, Bell B, McCord B. Long term renal
prognosis of Henoch-Schonlein purpura in an unselected
childhood population. European Journal of Pediatrics 1998;147(2):
1135. [MEDLINE: 3366130]
Tanaka 2003
Tanaka H, Suzuki K, Nakahata T, Ito E, Waga S. Early treatment
with oral immunosuppressants in severe proteinuric purpura
nephritis. Pediatric Nephrology 2003;18(4):34750. [MEDLINE:
12700960]
Weiss 2007
Weiss PF, Feinstein JA, Luan X, Burnham JM, Feudtner C. Effects
of corticosteroid on Henoch-Schonlein purpura: a systematic
review. Pediatrics 2007;120(5):107987. [MEDLINE: 17974746]
Wood 2008
Wood L, Egger M, Gluud LL, Schulz KF, Juni P, Altman DG, et
al.Empirical evidence of bias in treatment effect estimates in
controlled trials with different interventions and outcomes: meta-
epidemiological study. BMJ 2008;336(7644):6015. [MEDLINE:
18316340]
25 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Wyatt 2001
Wyatt RJ, Hogg RJ. Evidence-based assessment of treatment
options for children with IgA nephropathies. Pediatric Nephrology
2001;16(2):15667. [: 11261686]
Zaffanello 2007
Zaffanello M, Brugnara M, Franchini M. Therapy for children with
henoch-schonlein purpura nephritis: a systematic review.
Thescienticworldjournal 2007;7:2030. [MEDLINE: 17221139]
References to other published versions of this review
Chartapisak 2005
Chartapisak W, Opastirakul S, Hodson EM, Willis NS, Craig JC.
Interventions for preventing and treating renal disease in Henoch-
Schnlein Purpura (HSP). Cochrane Database of Systematic Reviews
2005, Issue 1. [DOI: 10.1002/14651858.CD005128]
Chartapisak 2008
Chartapisak W, Opastirakul O, Willis NS, Craig JC, Hodson EM.
Prevention and treatment of renal disease in Henoch-Schnlein
Purpura: a systematic review. Archives of Disease in Childhood 2008;
94(2):1327. [MEDLINE: 18701559]
Indicates the major publication for the study
26 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
C H A R A C T E R I S T I C S O F S T U D I E S
Characteristics of included studies [ordered by study ID]
Dudley 2007
Methods Country: UK
Setting/Design: 25 Paediatric departments in secondary/tertiary hospital/parallel group
design
Time frame: Jan 2001 to Jan 2005
Follow-up period: One year
Loss to follow-up: 16 from treatment arm, 6 from placebo arm
Participants Inclusion criteria
Children < 18 years enrolled/randomised within 7 days of onset of HSP rash
HSP dened as: palpable purpura with arthritis, kidney disease, gut involvement
Kidney disease dened as: P:Cr > 20 mg/mmol; positive dipstick for blood or
protein
Patients with haematuria and/or proteinuria at study entry were included; 50/140
had proteinuria in treatment group and 43/140 had proteinuria in placebo group.
Treatment group
Number: 181 entered; 145 analysed (16 lost to follow-up, 20 no specimen at 12
months)
Age: 6.34 (median); range 1 to 15.7 years
Sex (M/F): 93/88
Control group
Number: 172; 145 analysed (6 lost to follow-up, 21 no specimen at 12 months)
Age: 6.12 (median); range 0.5 to 13.9 years
Sex (M/F): 100/72
Exclusion criteria
Already on steroids or immunosuppressives, pre-existing kidney disease,
hypertension, immunodeciency, systemic infection, contraindications to steroids.
Interventions Treatment group
Prednisolone 2 mg/kg/d orally for 7 days (max dose 80 mg); 1mg/kg/d for 7 days
Control group
Placebo given in same regimen
Co-interventions
Additional treatment for gut or kidney disease as steroids (4 prednisolone; 9 placebo);
ACEi or ARBs (2 prednisolone; 3 placebo); other antihypertensives (3 prednisolone; 0
placebo)
Outcomes P:Cr > 20 mg/mmol at 12 months
Haematuria/proteinuria on dipstick at 4 and 12 weeks
Gastrointestinal involvement, joint involvement, rash at 4 and 12 weeks
BP at 4 weeks, 12 weeks and 12 months
Need for additional therapy
Adverse effects
27 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Dudley 2007 (Continued)
Notes Exclusions post randomisation but pre-intervention
10 in treatment group; 15 in placebo discontinued treatment but included
in nal analysis.
20 in treatment group and 21 in placebo group did not have end of study
urine P:Cr measurement so nal analysis involved 290/353 children (82%)
20 in treatment group and 21 in placebo group did not have end of study
urine P:Cr measurement so nal analysis involved 290/353 children (82%)
Stop or end point/s: None
Additional data requested from authors: Draft manuscript provided by authors
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Yes Computer generated random number se-
quence
Allocation concealment? Yes Plain sealed envelopes opened by research
pharmacist
Blinding?
All outcomes
Yes Trial medications (active and placebo) sup-
plied by same company. Identical bot-
tles for active and placebo medications
coded centrally with trial numbers. Pa-
tients, parents, paediatricians, investigators
were blinded to assignment.
Incomplete outcome data addressed?
All outcomes
Yes Lost to follow-up: 16 in prednisone group
and 6 in placebo group
Discontinuedtreatment but analysedinap-
propriate treatment groups: 10 in pred-
nisone group and 15 in placebo group
Twelve month missing data for P:Cr in 20
patients in prednisolone group and 21 pa-
tients in placebo group. These patients ex-
cluded from analysis.
Free of selective reporting? Yes Primary outcome pre-specied as P:Cr in
National Research Register of NHS in UK.
Informationalsoprovidedondipstick anal-
ysis of haematuria and proteinuria. Mean
systolic and diastolic BP levels only pro-
vided and no information provided on kid-
ney function but these were not specied
as outcomes.
Free of other bias? Yes Appears to be free of other biases
28 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Huber 2004
Methods Country: Canada
Setting/Design: Emergency department in tertiary hospital/parallel group design
Time frame: Sep 1996 to Jan 2000
Follow-up period: One year
Loss to follow-up: Three were withdrawn from placebo arm due to complications
(intussusception 2, severe rash 1)
Participants Inclusion criteria
Children 2 to 15 years within 7 days of onset of HSP
HSP dened as: palpable purpura and 1 or more of arthritis, kidney disease or gut
involvement
Kidney disease dened as: haematuria 5 or more RBC/HPF or RBC casts,
proteinuria 0.3g/L or more, hypertension 90th percentile for age/sex or above.
Study included 4 children in prednisone group and 2 in placebo group with
kidney disease at study entry.
Treatment group
Number: 21
Age: 5 (2 to 11) years
Sex (M/F): 13/8
Control group
Number: 19
Age: 6.1(3 to 15) years
Sex (M/F): 7/12
Exclusion criteria
Known underlying systemic vasculitis, steroids in previous month, underlying
kidney, gastrointestinal or immunodeciency illness, active infection, a life threatening
complication of HSP.
Interventions Treatment group
Prednisolone 2 mg/kg orally daily for 7 days; reducing dose over 7 days
Control group
Placebo given in same regimen
Co-interventions: NS
Outcomes New or persistent kidney disease at one year
Gastrointestinal involvement
Notes Exclusions post randomisation but pre-intervention: None
Stop or end point/s: None
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Yes Computer generated sequence of random
numbers.
29 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Huber 2004 (Continued)
Allocation concealment? Yes Plain sealed numbered envelopes opened
at subject randomisation by research phar-
macist. Individuals directly involved in the
study had no access to these envelopes.
Blinding?
All outcomes
Yes Prednisone and placebo groups received
identical number of pills and followed the
same schedule.
Prednisone and placebo tablets placed in
opaque tasteless gelatin capsules.
Incomplete outcome data addressed?
All outcomes
Yes One subject enrolled declined randomisa-
tion.
Three children withdrawn from the
placebo group but included in the analysis.
Free of selective reporting? Yes Reported that children with persistent kid-
ney disease had haematuria and/or protein-
uria and did not have hypertension or kid-
ney insufciency.
Free of other bias? Yes The study appears to be free of other
sources of bias
Islek 1999
Methods Country: Turkey
Setting/Design: University paediatric clinic/parallel group design
Time frame: Sep 1996 to Jan 2000
Duration of follow-up: Unclear
Participants Inclusion criteria
Children aged 9.2 2.7 years with HSP without haematuria/proteinuria on
admission.
Sex (M/F): 69/48
Dened as non-thrombocytopenic purpura, arthritis and arthralgia, abdominal
pain, gastrointestinal haemorrhage.
Treatment group
Number: 70
Age: NS
Sex (M/F): NS
Control group
Number: 50
Age: NS
Sex (M/F): NS
Exclusion criteria
Kidney disease
30 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Islek 1999 (Continued)
Interventions Treatment group
Prednisolone 1mg/kg/d for 10 days; tapered over 1 week and withdrawn
Control group
No treatment
Co-interventions: NS
Outcomes Haematuria and/or proteinuria: No denitions provided
Notes Exclusions post randomisation but pre-intervention: NS
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Unclear No information provided
Blinding?
All outcomes
No Noplacebotablets administeredinthe con-
trol group. No information provided on
whether outcome assessors were blinded.
Incomplete outcome data addressed?
All outcomes
Unclear Unclear whether all eligible patients en-
tered and completed the trial and whether
there was any missing data. All reported pa-
tients appeared to have completed study.
Free of selective reporting? Unclear Only outcomes reported were haematuria
and proteinuria. No reports separately of
more severe kidney disease (acute nephritic
syndrome, nephrotic syndrome, hyperten-
sion).
Free of other bias? Unclear Insufcient information available to deter-
mine
31 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Mollica 1992
Methods Country: Italy
Setting/Design: University hospital, RCT/parallel group design
Time frame: Oct 1978 to Sep 1987
Follow-up period: 24 to 36 months
Loss to follow-up: Unclear, 19 (10.2%) excluded for insufcient or inadequate follow-
up
Participants Inclusion criteria
Unselected children with HSP without kidney disease at study entry
Treatment group
Number: 84
Age: NS
Sex (M/F): NS
Control group
Number: 84
Age: NS
Sex (M/F): NS
Exclusion criteria
34 children with haematuria and/or proteinuria on initial presentation were
excluded
Interventions Treatment group
Prednisolone 1 mg/ kg orally for 2 week
Control group
No treatment
Co-interventions: NS
Outcomes Number of patients who develop HSP kidney disease with 2 or more of:
proteinuria 4 mg/m/h
haematuria > 10 RBC/HPF
BP 2 SD above normal for age
BUN 54 mg/dL
Cr 0.8 mg/dL/m
Notes Exclusions post randomisation but pre-intervention: None reported
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? No Each patient on entry to the trial was alter-
natively assigned to one of the two treat-
ment groups
32 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Mollica 1992 (Continued)
Blinding?
All outcomes
No Control group did not receive placebo
medications. No information provided on
whether outcome assessors were blinded.
Incomplete outcome data addressed?
All outcomes
No 19 patients excluded because of insufcient
or inadequate follow-up.
Free of selective reporting? Yes Information on the numbers with pro-
teinuria, haematuria, hypertension and re-
duced kidney function provided.
Free of other bias? Unclear Insufcient information provided
Peratoner 1990
Methods Country: Italy
Setting/Design: Multicentre RCT in paediatric centre/parallel group design
Time frame: NS
Follow-up period: One year
Loss to follow-up: None
Participants Inclusion criteria
Children aged 2 to 14 year old with HSP
Treatment group
Number: 60 (13 had kidney disease at entry)
Age: NS
Sex (M/F): NS
Control group
Number: 41 (6 had kidney disease at entry)
Age: NS
Sex (M/F): NS
Exclusion criteria: NS
Interventions Treatment group
Dipyridamole 4 mg/kg/d orally in 3 doses; cyproheptadine 0.5 mg/kg/d orally in
3 doses and salicylates 10 mg/kg/d orally in one dose for 8 weeks.
Control group
No treatment
Co-interventions
Anti-pyretics, antibiotics
Outcomes Kidney disease during 1 year of follow-up, assessed using the following scoring
system;
haematuria > 5 RBC/mm (score 0-2)
cylindruria (0-1)
hypertension (0-1)
reduced CrCl (0-2).
33 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Peratoner 1990 (Continued)
Notes Exclusions post randomisation but pre-intervention: None reported
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Unclear No information provided
Blinding?
All outcomes
No No placebo given to control group. No in-
formation provided about outcome asses-
sors. Urinalysis is a potentially a subjective
outcome.
Incomplete outcome data addressed?
All outcomes
Unclear Unclear whether all entered patients com-
pleted trial and were included in the results
Free of selective reporting? Yes Information on type of residual kidney dis-
ease provided in text
Free of other bias? Unclear Insufcient information provided
Ronkainen 2006a
Methods Country: Finland
Setting/Design: University and district hospitals/parallel group design
Time frame: 1999 to 2005
Follow-up period: Six months
Loss to follow-up: 3%
Participants Inclusion criteria
Clinical diagnosis of newly diagnosed HSP (purpura, petechiae gut/joint pain)
176 entered study, 16 in each group had haematuria, proteinuria or both at study
entry
Treatment group
Number: 87 entered; 84 evaluated
Age: Mean 6.8 years (2.0 to 15.2)
Sex (M/F): 49/35
Duration of disease at entry: 4.7 days (0 to 28)
Control group
Number: 89 entered; 87 evaluated
Age: Mean 7.3 years (1.7 to 15.6)
Sex (M/F): 44/43
Duration of disease at entry: 6.4 days (0 to 63)
34 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Ronkainen 2006a (Continued)
Exclusion criteria
Established kidney disease (haematuria > 10 RBC/HPF or proteinuria > 300 mg/
L on initial presentation)
Thrombocytopenia
Systemic vasculitis
Prednisone contraindicated
Interventions Treatment group
Prednisolone 1 mg/kg/d orally for 14 days; 0.5 mg/kg/d for 7 days; 0.5 mg/kg on
alternate days for 7 days.
Control group
Placebo tablets
Co-interventions
Paracetamol for pain
Outcomes Haematuria: urinary > 5 RBC/HPF at 1, 3, 6 months
Proteinuria: urinary protein > 200 mg/L or albumin > 30 mg/L at 1, 3, 6 months
Severity and duration of abdominal pain during rst month
Severity and duration of joint pain during rst month
Adverse effects
weight
BP
Notes Exclusions post randomisation but pre-intervention: Three excluded from
prednisone group and 2 from placebo group after randomisation.
Stop or end point/s: NS
Additional data requested fromauthors: Information on number providing data
for symptom scores and on proportions with kidney disease at 1, 3, 6 months obtained
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Yes Block randomisation scheme with block
size of 6.
Allocation concealment? Yes Observers and subjects were unaware
of randomisation scheme. Pharmia Ltd
packed drugs, labelled containers, per-
formed randomisation and retained key to
randomisation till end of study.
Blinding?
All outcomes
Yes Prednisone (5 mg tablets) and placebo were
similar in size and supplied in lots of 200
tablets in similar containers marked with
sequential numbers.
35 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Ronkainen 2006a (Continued)
Incomplete outcome data addressed?
All outcomes
Yes Three (2 dropped out; 1 protocol vio-
lation) excluded from prednisone group.
Two (both dropped out) excluded from
placebo group. These unlikely to inuence
nal results.
Free of selective reporting? Unclear Kidney data presented as numbers with
kidney symptoms at time points as propor-
tion of all patients with kidney disease in
acute phase but data as proportion of all
treated patients could be dened. No in-
formation provided on severity of kidney
disease (degree of proteinuria, kidney func-
tion). Data on BP, abdominal pain score
and joint pain score provided as mean and
range but these were not primary outcomes
for this review.
Free of other bias? Yes Appears to be free of other biases
Ronkainen 2006b
Methods Country: Finland
Setting/Design: University hospitals/parallel group design
Time frame: 2000 to 2007
Duration of study: Unclear
Follow-up period: 2.9 years (1.1 to 5.6)
Loss to follow-up: None
Participants Inclusion criteria
Kidney biopsy diagnosis of crescentic HSP associated kidney disease of ISKDC
grade III or IV or grade II with nephrotic syndrome
Number: 19
Age: 2 to 18 years (mean 9.2 years)
Sex (M/F): 13/6
Treatment group
Number: 10
Age: NS
Sex (M/F): NS
Duration of disease at entry: NS
Control group
Number: 9
Age: NS
Sex (M/F): NS
Duration of disease at entry: NS
Exclusion criteria
Medication known to interact with cyclosporin.
36 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Ronkainen 2006b (Continued)
Interventions Treatment group
Cyclosporin 5 mg/kg/d for 12 months
Control group
Methylprednisolone: 30 mg/kg IV x 3 in 1 week; Prednisone 30 mg/m/d x 1
month and tapered over 3 months
Co-interventions
ACEi
Outcomes Remission (P:Cr < 200 or urine protein < 40 mg/m/h) at 3 months
Remission at last follow-up
Notes Exclusions post randomisation but pre-intervention: Non reported
Stop or end point/s: NS
Additional data requested from authors: Information to conrm RCT
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Unclear No information provided
Blinding?
All outcomes
No Open label study comparing an orally ad-
ministered agent with an intravenously ad-
ministered agent
Incomplete outcome data addressed?
All outcomes
Unclear No SDs provided with means of urinary
proteinand SCr at last follow-up. Duration
of study not dened.
Free of selective reporting? Unclear No information provided
Free of other bias? Unclear Insufcient information provided
Tarshish 2004
Methods Country: Europe, USA, Canada
Setting/Design: Multicentre tertiary/parallel group design
Time frame: 1973 to 1980
Duration of study: Unclear
Follow-up period: 6.93 (SD 3.32) years in patients who recovered; 6.57 (SD 4.1) years
in group with persistent abnormalities; 3.71 (SD 2.14) years in patients progressing to
ESKD
Loss to follow-up: None
37 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Tarshish 2004 (Continued)
Participants Inclusion criteria
HSP: Purpura plus urticaria with one or more of the following:
joint pain and swelling, kidney disease, abdominal pain and intestinal
bleeding
Age: 12 weeks to 16 years
Estimated GFR > 35 mL/min/1.73 m
Proteinuria > 40 mg/m/h for > 1 month
Histopathology: Crescents/segmental lesions (ISKDC classication)
Treatment group
Number: 28
Age: NS
Sex (M/F): NS
Control group
Number: 28
Age: NS
Sex (M/F): NS
Exclusion criteria
HSP present > 3 months
Prior use of immunosuppressive or cytotoxic therapy other than steroids
Concurrent or pre-existing kidney disease
Interventions Treatment group
Cyclophosphamide 90 mg/m/d orally for 42 days.
Control group
No therapy
Co-interventions
Diet modication, ion exchange resins, vitamins, diuretics
Outcomes Total number of patients with any persistent kidney disease
Number with severe kidney disease (decreased GFR, severe proteinuria, ESKD)
Number of patients with ESKD
Notes Exclusions post randomisation but pre-intervention: None
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Yes Random allocation at central ofce
Blinding?
All outcomes
No No placebo therapy used. While most out-
come measures were laboratory measure-
ments and unlikely to be inuenced by lack
of blinding, end points in some children
38 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Tarshish 2004 (Continued)
were judged on dipstick protein urinaly-
ses, which could have be either doctor or
patient reported. No information provided
on how many children had outcome as-
sessed on urinalysis. No information pro-
vided on outcome assessors.
Incomplete outcome data addressed?
All outcomes
Unclear Duration of follow-up variable and unclear
whether all patients completed follow-up
Free of selective reporting? Yes Data onpersistent abnormalities, severe ab-
normalities and ESKD provided though
detailed information on GFR and urinary
protein excretion at follow-up not pro-
vided.
Free of other bias? Unclear Insufcient information provided on study
design
Yanyan 2001
Methods Country: China
Setting/Design: University hospital/parallel group design
Duration of study: NS
Follow-up period: More than 3 months
Loss to follow-up: Unclear
Participants Inclusion criteria
Children at onset or relapse of HSP but presumed to be without kidney disease
Treatment group
Number: 119
Age: NS
Sex (M/F): NS
Control group
Number: 109
Age: NS
Sex: NS
Exclusion criteria: NS
Interventions Treatment group
Sodium heparin about 120-150 IU/kg/d IV for 5 days or calcium heparin 10 IU/
kg/d for 10 days IM given at onset or relapse of HSP
Control group
Placebo injection only
Co-interventions
Vitamin C, vitamin P
39 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Yanyan 2001 (Continued)
Outcomes Total number of children with kidney disease after 3 months or more (not dened)
Number with haematuria and proteinuria after 3 months or more
Number with nephrotic syndrome after 3 months or more
Time to development of kidney disease
Bleeding
Notes Exclusions post randomisation but pre-intervention: None
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Unclear No information provided
Blinding?
All outcomes
Unclear Control group given IVvehicle but unclear
whether investigators aware of which pa-
tients received heparin or vehicle.
Incomplete outcome data addressed?
All outcomes
Unclear No information provided although all pa-
tients appeared to have been followed. No
information on duration of study. Limited
information on adverse effects provided.
Free of selective reporting? Yes Information provided on numbers with
haematuria alone, haematuria and protein-
uria and haematuria with nephrotic syn-
drome.
Free of other bias? Unclear Insufcient information provided.
Unclear as to whether same patient could
enter the trial twice (at onset or at recur-
rence).
Yoshimoto 1987a
Methods Country: Japan
Setting/Design: Emergency department in tertiary hospital/parallel group design
Time frame: Oct 1984 to Sep 1985
Duration of study: NS
Duration of follow-up: NS
Loss to follow-up: NS
40 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Yoshimoto 1987a (Continued)
Participants Inclusion criteria
Children admitted with HSP without kidney disease
Age: 3 to 10 years
Sex (M/F): 13/15
Treatment group 1 (aspirin)
Number: 9
Age: NS
Sex (M/F): NS
Control group
Number: 9
Age: NS
Sex (M/F): NS
Exclusion criteria
Known underlying systemic vasculitis, steroids in previous month, underlying
kidney, gastrointestinal or immunodeciency illness, active infection, a life threatening
complication of HSP.
Interventions Treatment group 1
Aspirin 5 mg/kg/d for 5 weeks
Control group
Vitamin pills for 5 weeks
Co-interventions: NS
Outcomes Number of patient who has kidney disease (not dened); time of involvement not
specied
Notes Exclusions post randomisation but pre-intervention: None
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Unclear No information provided
Blinding?
All outcomes
No Control group received vitamin pills. Out-
come measures not dened.
Incomplete outcome data addressed?
All outcomes
Unclear Criteria for kidney disease not dened
Free of selective reporting? Unclear No information provided
Free of other bias? Unclear Insufcient information available
41 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Yoshimoto 1987b
Methods Country: Japan
Setting/Design: Emergency department in tertiary hospital/parallel group design
Time frame: Oct 1984 to Sep 1985
Duration of study: NS
Duration of follow-up: NS
Loss to follow-up: NS
Participants Inclusion criteria
Children admitted with HSP without kidney disease
Age: 3 to 10 years
Sex (M/F): 13/15
Treatment group 2 (Dipyridamole)
Number: 10
Age: NS
Sex (M/F): NS
Control group
Number: 9
Age: NS
Sex (M/F): NS
Exclusion criteria
Known underlying systemic vasculitis, steroids in previous month, underlying
kidney, gastrointestinal or immunodeciency illness, active infection, a life threatening
complication of HSP.
Interventions Treatment group 2
Dipyridamole 5 mg/kg/d for 5 weeks
Control group
Vitamin pills for 5 weeks
Co-interventions: NS
Outcomes Number of patient who has kidney disease (not dened); time of involvement not
specied
Notes Exclusions post randomisation but pre-intervention: None
Stop or end point/s: NS
Additional data requested from authors: None
Risk of bias
Item Authors judgement Description
Adequate sequence generation? Unclear No information provided
Allocation concealment? Unclear No information provided
Blinding?
All outcomes
No Control group received vitamin pills. Out-
come measures not dened.
42 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Yoshimoto 1987b (Continued)
Incomplete outcome data addressed?
All outcomes
Unclear Criteria for kidney disease not dened
Free of selective reporting? Unclear No information provided
Free of other bias? Unclear Insufcient information available
ACEi - angiotensin converting enzyme inhibitor; ARB - angiotensin receptor blocker; BP - blood pressure; BUN - blood urea nitrogen;
Cr - creatinine; CrCl - creatinine clearance; ESKD - end-stage kidney disease; HPF - high power eld; HSP - Henoch Schnlein
Purpura; NS - not stated; P:Cr - protein/creatinine ratio; RBC - red blood cells; SCr - serum creatinine; SD - standard deviation
Characteristics of excluded studies [ordered by study ID]
Study Reason for exclusion
Jin 2003 Unclear whether study is RCT
Yu 2001 Unclear whether study is RCT
43 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
D A T A A N D A N A L Y S E S
Comparison 1. Prednisone compared with placebo/supportive treatment for prevention of persistent kidney
disease
Outcome or subgroup title
No. of
studies
No. of
participants
Statistical method Effect size
1 Persistent kidney disease at any
time after treatment
5 789 Risk Ratio (M-H, Random, 95% CI) 0.73 [0.43, 1.24]
2 Number of children with
continuing kidney disease at
different time points
4 Risk Ratio (M-H, Random, 95% CI) Subtotals only
2.1 One month 4 631 Risk Ratio (M-H, Random, 95% CI) 0.80 [0.34, 1.88]
2.2 Three months 4 636 Risk Ratio (M-H, Random, 95% CI) 0.82 [0.45, 1.50]
2.3 Six months 3 379 Risk Ratio (M-H, Random, 95% CI) 0.51 [0.24, 1.11]
2.4 Twelve months 3 498 Risk Ratio (M-H, Random, 95% CI) 1.02 [0.40, 2.62]
3 Continuing kidney disease at
different time points (study
with high risk of bias excluded)
3 Risk Ratio (M-H, Random, 95% CI) Subtotals only
3.1 One month 3 463 Risk Ratio (M-H, Random, 95% CI) 1.02 [0.53, 1.98]
3.2 Three months 3 468 Risk Ratio (M-H, Random, 95% CI) 0.95 [0.66, 1.36]
3.3 Six months 2 211 Risk Ratio (M-H, Random, 95% CI) 0.59 [0.23, 1.50]
3.4 Twelve months 2 330 Risk Ratio (M-H, Random, 95% CI) 1.28 [0.70, 2.32]
4 Number of children with kidney
disease in rst month/with
kidney disease at follow-up
1 Risk Ratio (M-H, Random, 95% CI) Totals not selected
4.1 One month 1 Risk Ratio (M-H, Random, 95% CI) Not estimable
4.2 Three months 1 Risk Ratio (M-H, Random, 95% CI) Not estimable
4.3 Six months 1 Risk Ratio (M-H, Random, 95% CI) Not estimable
4.4 Twelve months 0 Risk Ratio (M-H, Random, 95% CI) Not estimable
5 Number developing severe
kidney disease
2 461 Risk Ratio (M-H, Random, 95% CI) 1.92 [0.57, 6.50]
6 Duration of kidney disease 1 Mean Difference (IV, Random, 95% CI) Totals not selected
6.1 Haematuria 1 Mean Difference (IV, Random, 95% CI) Not estimable
6.2 Proteinuria 1 Mean Difference (IV, Random, 95% CI) Not estimable
7 Gastrointestinal complications
requiring hospital admission
2 211 Risk Ratio (M-H, Random, 95% CI) 0.58 [0.24, 1.42]
44 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Comparison 2. Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with supportive therapy
for prevention of persistent kidney disease
Outcome or subgroup title
No. of
studies
No. of
participants
Statistical method Effect size
1 Kidney disease at any time 2 Risk Ratio (M-H, Random, 95% CI) Subtotals only
1.1 Dipyridamole
cyproheptadine in children
without kidney disease at entry
2 101 Risk Ratio (M-H, Random, 95% CI) 1.16 [0.46, 2.95]
1.2 Dipyridamole
cyproheptadine in children
with kidney disease at entry
1 19 Risk Ratio (M-H, Random, 95% CI) 0.92 [0.23, 3.72]
2 Kidney disease at any time 1 Risk Ratio (M-H, Random, 95% CI) Totals not selected
2.1 Aspirin compared with
supportive treatment
1 Risk Ratio (M-H, Random, 95% CI) Not estimable
Comparison 3. Heparin compared with placebo for prevention of persistent kidney disease
Outcome or subgroup title
No. of
studies
No. of
participants
Statistical method Effect size
1 Any kidney disease at 3 months
after onset or relapse
1 Risk Ratio (M-H, Random, 95% CI) Totals not selected
2 Type of kidney disease at 3
months or more after onset or
relapse
1 Risk Ratio (M-H, Random, 95% CI) Totals not selected
2.1 Haematuria 1 Risk Ratio (M-H, Random, 95% CI) Not estimable
2.2 Proteinuria 1 Risk Ratio (M-H, Random, 95% CI) Not estimable
2.3 Nephrotic syndrome 1 Risk Ratio (M-H, Random, 95% CI) Not estimable
3 Time to development of kidney
disease
1 Mean Difference (IV, Random, 95% CI) Subtotals only
Comparison 4. Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease
Outcome or subgroup title
No. of
studies
No. of
participants
Statistical method Effect size
1 Persistent kidney disease 1 Risk Ratio (M-H, Random, 95% CI) Subtotals only
2 Persistent severe kidney disease 1 Risk Ratio (M-H, Random, 95% CI) Subtotals only
3 ESKD 1 Risk Ratio (M-H, Random, 95% CI) Subtotals only
45 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Comparison 5. Cyclosporin compared with methylprednisolone for treatment of severe kidney disease
Outcome or subgroup title
No. of
studies
No. of
participants
Statistical method Effect size
1 Number without remission at 3
months
1 Risk Ratio (M-H, Random, 95% CI) Subtotals only
2 Number without remission at
last follow-up
1 Risk Ratio (M-H, Random, 95% CI) Subtotals only
Analysis 1.1. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 1 Persistent kidney disease at any time after treatment.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 1 Persistent kidney disease at any time after treatment
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Dudley 2007 19/145 15/145 31.3 % 1.27 [ 0.67, 2.39 ]
Huber 2004 3/21 2/19 8.4 % 1.36 [ 0.25, 7.27 ]
Islek 1999 15/70 18/50 33.9 % 0.60 [ 0.33, 1.06 ]
Mollica 1992 0/84 4/84 3.1 % 0.11 [ 0.01, 2.03 ]
Ronkainen 2006a 7/84 15/87 23.2 % 0.48 [ 0.21, 1.13 ]
Total (95% CI) 404 385 100.0 % 0.73 [ 0.43, 1.24 ]
Total events: 44 (Prednisone), 54 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.13; Chi
2
= 6.40, df = 4 (P = 0.17); I
2
=37%
Test for overall effect: Z = 1.16 (P = 0.24)
0.005 0.1 1 10 200
Prednisone Placebo/supportive
46 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 1.2. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 2 Number of children with continuing kidney disease at different time
points.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 2 Number of children with continuing kidney disease at different time points
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
1 One month
Mollica 1992 0/84 10/84 4.3 % 0.05 [ 0.00, 0.80 ]
Huber 2004 3/21 3/19 13.3 % 0.90 [ 0.21, 3.96 ]
Ronkainen 2006a 14/84 22/87 38.2 % 0.66 [ 0.36, 1.20 ]
Dudley 2007 34/125 22/127 44.2 % 1.57 [ 0.98, 2.53 ]
Subtotal (95% CI) 314 317 100.0 % 0.80 [ 0.34, 1.88 ]
Total events: 51 (Prednisone), 57 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.45; Chi
2
= 10.37, df = 3 (P = 0.02); I
2
=71%
Test for overall effect: Z = 0.52 (P = 0.60)
2 Three months
Mollica 1992 0/84 6/84 4.4 % 0.08 [ 0.00, 1.34 ]
Huber 2004 3/21 2/19 11.4 % 1.36 [ 0.25, 7.27 ]
Ronkainen 2006a 11/84 18/87 35.9 % 0.63 [ 0.32, 1.26 ]
Dudley 2007 30/123 30/134 48.2 % 1.09 [ 0.70, 1.70 ]
Subtotal (95% CI) 312 324 100.0 % 0.82 [ 0.45, 1.50 ]
Total events: 44 (Prednisone), 56 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.14; Chi
2
= 5.01, df = 3 (P = 0.17); I
2
=40%
Test for overall effect: Z = 0.64 (P = 0.53)
3 Six months
Mollica 1992 0/84 3/84 10.5 % 0.14 [ 0.01, 2.72 ]
Huber 2004 2/21 1/19 16.2 % 1.81 [ 0.18, 18.39 ]
Ronkainen 2006a 7/84 15/87 73.3 % 0.48 [ 0.21, 1.13 ]
Subtotal (95% CI) 189 190 100.0 % 0.51 [ 0.24, 1.11 ]
Total events: 9 (Prednisone), 19 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.0; Chi
2
= 1.89, df = 2 (P = 0.39); I
2
=0.0%
Test for overall effect: Z = 1.70 (P = 0.089)
4 Twelve months
Mollica 1992 0/84 4/84 8.0 % 0.11 [ 0.01, 2.03 ]
Huber 2004 3/21 2/19 21.1 % 1.36 [ 0.25, 7.27 ]
0.002 0.1 1 10 500
Prednisone Placebo/supportive
(Continued . . . )
47 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
(. . . Continued)
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Dudley 2007 19/145 15/145 71.0 % 1.27 [ 0.67, 2.39 ]
Subtotal (95% CI) 250 248 100.0 % 1.02 [ 0.40, 2.62 ]
Total events: 22 (Prednisone), 21 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.24; Chi
2
= 2.75, df = 2 (P = 0.25); I
2
=27%
Test for overall effect: Z = 0.05 (P = 0.96)
0.002 0.1 1 10 500
Prednisone Placebo/supportive
Analysis 1.3. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 3 Continuing kidney disease at different time points (study with high risk
of bias excluded).
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 3 Continuing kidney disease at different time points (study with high risk of bias excluded)
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
1 One month
Dudley 2007 34/125 22/127 53.2 % 1.57 [ 0.98, 2.53 ]
Huber 2004 3/21 3/19 8.2 % 0.90 [ 0.21, 3.96 ]
Ronkainen 2006a 14/84 22/87 38.7 % 0.66 [ 0.36, 1.20 ]
Subtotal (95% CI) 230 233 100.0 % 1.02 [ 0.53, 1.98 ]
Total events: 51 (Prednisone), 47 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.19; Chi
2
= 5.02, df = 2 (P = 0.08); I
2
=60%
Test for overall effect: Z = 0.07 (P = 0.95)
2 Three months
Dudley 2007 30/123 30/134 60.7 % 1.09 [ 0.70, 1.70 ]
Huber 2004 3/21 2/19 6.6 % 1.36 [ 0.25, 7.27 ]
Ronkainen 2006a 11/84 18/87 32.7 % 0.63 [ 0.32, 1.26 ]
Subtotal (95% CI) 228 240 100.0 % 0.95 [ 0.66, 1.36 ]
Total events: 44 (Prednisone), 50 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.0; Chi
2
= 1.88, df = 2 (P = 0.39); I
2
=0.0%
0.05 0.2 1 5 20
Prednisone Placebo
(Continued . . . )
48 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
(. . . Continued)
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Test for overall effect: Z = 0.30 (P = 0.76)
3 Six months
Huber 2004 2/21 1/19 13.3 % 1.81 [ 0.18, 18.39 ]
Ronkainen 2006a 7/84 15/87 86.7 % 0.48 [ 0.21, 1.13 ]
Subtotal (95% CI) 105 106 100.0 % 0.59 [ 0.23, 1.50 ]
Total events: 9 (Prednisone), 16 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.08; Chi
2
= 1.10, df = 1 (P = 0.29); I
2
=9%
Test for overall effect: Z = 1.11 (P = 0.27)
4 Twelve months
Dudley 2007 19/145 15/145 84.7 % 1.27 [ 0.67, 2.39 ]
Huber 2004 3/21 2/19 15.3 % 1.36 [ 0.25, 7.27 ]
Subtotal (95% CI) 166 164 100.0 % 1.28 [ 0.70, 2.32 ]
Total events: 22 (Prednisone), 17 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.0; Chi
2
= 0.01, df = 1 (P = 0.94); I
2
=0.0%
Test for overall effect: Z = 0.81 (P = 0.42)
0.05 0.2 1 5 20
Prednisone Placebo
49 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 1.4. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 4 Number of children with kidney disease in rst month/with kidney
disease at follow-up.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 4 Number of children with kidney disease in rst month/with kidney disease at follow-up
Study or subgroup Prednisone Placebo/supportive Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
1 One month
Ronkainen 2006a 14/36 22/35 0.62 [ 0.38, 1.00 ]
2 Three months
Ronkainen 2006a 11/36 18/35 0.59 [ 0.33, 1.07 ]
3 Six months
Ronkainen 2006a 7/36 15/35 0.45 [ 0.21, 0.98 ]
4 Twelve months
0.2 0.5 1 2 5
Prednisone Placebo
Analysis 1.5. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 5 Number developing severe kidney disease.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 5 Number developing severe kidney disease
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Dudley 2007 4/145 1/145 31.2 % 4.00 [ 0.45, 35.36 ]
Ronkainen 2006a 4/84 3/87 68.8 % 1.38 [ 0.32, 5.99 ]
Total (95% CI) 229 232 100.0 % 1.92 [ 0.57, 6.50 ]
Total events: 8 (Prednisone), 4 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.0; Chi
2
= 0.64, df = 1 (P = 0.42); I
2
=0.0%
Test for overall effect: Z = 1.05 (P = 0.29)
0.02 0.1 1 10 50
Prednisone Placebo
50 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 1.6. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 6 Duration of kidney disease.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 6 Duration of kidney disease
Study or subgroup Prednisone Placebo/supportive Mean Difference Mean Difference
N Mean(SD) N Mean(SD) IV,Random,95% CI IV,Random,95% CI
1 Haematuria
Islek 1999 15 12.2 (15.9) 18 13.2 (9.9) -1.00 [ -10.26, 8.26 ]
2 Proteinuria
Islek 1999 15 9 (15.06) 18 10.6 (25.46) -1.60 [ -15.62, 12.42 ]
-20 -10 0 10 20
Prednisone Supportive
Analysis 1.7. Comparison 1 Prednisone compared with placebo/supportive treatment for prevention of
persistent kidney disease, Outcome 7 Gastrointestinal complications requiring hospital admission.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 1 Prednisone compared with placebo/supportive treatment for prevention of persistent kidney disease
Outcome: 7 Gastrointestinal complications requiring hospital admission
Study or subgroup Prednisone Placebo/supportive Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Huber 2004 2/21 3/19 28.2 % 0.60 [ 0.11, 3.23 ]
Ronkainen 2006a 5/84 9/87 71.8 % 0.58 [ 0.20, 1.65 ]
Total (95% CI) 105 106 100.0 % 0.58 [ 0.24, 1.42 ]
Total events: 7 (Prednisone), 12 (Placebo/supportive)
Heterogeneity: Tau
2
= 0.0; Chi
2
= 0.00, df = 1 (P = 0.96); I
2
=0.0%
Test for overall effect: Z = 1.19 (P = 0.24)
0.1 0.2 0.5 1 2 5 10
Prednisone Placebo
51 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 2.1. Comparison 2 Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with
supportive therapy for prevention of persistent kidney disease, Outcome 1 Kidney disease at any time.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 2 Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with supportive therapy for prevention of persistent kidney disease
Outcome: 1 Kidney disease at any time
Study or subgroup Treatment No specic treatment Risk Ratio Weight Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
1 Dipyridamole cyproheptadine in children without kidney disease at entry
Peratoner 1990 6/47 3/35 50.3 % 1.49 [ 0.40, 5.55 ]
Yoshimoto 1987b 3/10 3/9 49.7 % 0.90 [ 0.24, 3.38 ]
Subtotal (95% CI) 57 44 100.0 % 1.16 [ 0.46, 2.95 ]
Total events: 9 (Treatment), 6 (No specic treatment)
Heterogeneity: Tau
2
= 0.0; Chi
2
= 0.29, df = 1 (P = 0.59); I
2
=0.0%
Test for overall effect: Z = 0.31 (P = 0.76)
2 Dipyridamole cyproheptadine in children with kidney disease at entry
Peratoner 1990 4/13 2/6 100.0 % 0.92 [ 0.23, 3.72 ]
Subtotal (95% CI) 13 6 100.0 % 0.92 [ 0.23, 3.72 ]
Total events: 4 (Treatment), 2 (No specic treatment)
Heterogeneity: not applicable
Test for overall effect: Z = 0.11 (P = 0.91)
0.1 0.2 0.5 1 2 5 10
Treatment No specic treatment
Analysis 2.2. Comparison 2 Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with
supportive therapy for prevention of persistent kidney disease, Outcome 2 Kidney disease at any time.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 2 Antiplatelet agents (dipyridamole, cyproheptadine, salicylates) compared with supportive therapy for prevention of persistent kidney disease
Outcome: 2 Kidney disease at any time
Study or subgroup Treatment No specic treatment Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
1 Aspirin compared with supportive treatment
Yoshimoto 1987a 0/9 3/9 0.14 [ 0.01, 2.42 ]
0.005 0.1 1 10 200
Treatment No specic treatment
52 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 3.1. Comparison 3 Heparin compared with placebo for prevention of persistent kidney disease,
Outcome 1 Any kidney disease at 3 months after onset or relapse.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 3 Heparin compared with placebo for prevention of persistent kidney disease
Outcome: 1 Any kidney disease at 3 months after onset or relapse
Study or subgroup Heparin Placebo Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Yanyan 2001 9/119 30/109 0.27 [ 0.14, 0.55 ]
0.1 0.2 0.5 1 2 5 10
Heparin No treatment
Analysis 3.2. Comparison 3 Heparin compared with placebo for prevention of persistent kidney disease,
Outcome 2 Type of kidney disease at 3 months or more after onset or relapse.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 3 Heparin compared with placebo for prevention of persistent kidney disease
Outcome: 2 Type of kidney disease at 3 months or more after onset or relapse
Study or subgroup Heparin Placebo Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
1 Haematuria
Yanyan 2001 2/119 12/109 0.15 [ 0.03, 0.67 ]
2 Proteinuria
Yanyan 2001 6/119 15/109 0.37 [ 0.15, 0.91 ]
3 Nephrotic syndrome
Yanyan 2001 1/119 3/109 0.31 [ 0.03, 2.89 ]
0.01 0.1 1 10 100
Heparin No treatment
53 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 3.3. Comparison 3 Heparin compared with placebo for prevention of persistent kidney disease,
Outcome 3 Time to development of kidney disease.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 3 Heparin compared with placebo for prevention of persistent kidney disease
Outcome: 3 Time to development of kidney disease
Study or subgroup Heparin Placebo Mean Difference Mean Difference
N Mean(SD) N Mean(SD) IV,Random,95% CI IV,Random,95% CI
Yanyan 2001 119 81.8 (64.5) 109 34.5 (32.1) 47.30 [ 34.24, 60.36 ]
-100 -50 0 50 100
Heparin Placebo
Analysis 4.1. Comparison 4 Cyclophosphamide compared with supportive treatment for treatment of
severe kidney disease, Outcome 1 Persistent kidney disease.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 4 Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease
Outcome: 1 Persistent kidney disease
Study or subgroup Cyclophosphamide No specic treatment Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Tarshish 2004 15/28 14/28 1.07 [ 0.65, 1.78 ]
0.5 0.7 1 1.5 2
Cyclophosphamide No treatment
54 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 4.2. Comparison 4 Cyclophosphamide compared with supportive treatment for treatment of
severe kidney disease, Outcome 2 Persistent severe kidney disease.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 4 Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease
Outcome: 2 Persistent severe kidney disease
Study or subgroup Cyclophosphamide No specic treatment Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Tarshish 2004 7/28 8/28 0.88 [ 0.37, 2.09 ]
0.2 0.5 1 2 5
Cyclophosphamide No treatment
Analysis 4.3. Comparison 4 Cyclophosphamide compared with supportive treatment for treatment of
severe kidney disease, Outcome 3 ESKD.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 4 Cyclophosphamide compared with supportive treatment for treatment of severe kidney disease
Outcome: 3 ESKD
Study or subgroup Cyclophosphamide No specic treatment Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Tarshish 2004 3/28 4/28 0.75 [ 0.18, 3.05 ]
0.1 0.2 0.5 1 2 5 10
Cyclophosphamide No treatment
55 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Analysis 5.1. Comparison 5 Cyclosporin compared with methylprednisolone for treatment of severe kidney
disease, Outcome 1 Number without remission at 3 months.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 5 Cyclosporin compared with methylprednisolone for treatment of severe kidney disease
Outcome: 1 Number without remission at 3 months
Study or subgroup Cyclosporin Methylprednisolone Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Ronkainen 2006b 0/10 5/9 0.08 [ 0.01, 1.31 ]
0.005 0.1 1 10 200
Cyclosporin Methylprednisolone
Analysis 5.2. Comparison 5 Cyclosporin compared with methylprednisolone for treatment of severe kidney
disease, Outcome 2 Number without remission at last follow-up.
Review: Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP)
Comparison: 5 Cyclosporin compared with methylprednisolone for treatment of severe kidney disease
Outcome: 2 Number without remission at last follow-up
Study or subgroup Cyclosporin Methylprednisolone Risk Ratio Risk Ratio
n/N n/N M-H,Random,95% CI M-H,Random,95% CI
Ronkainen 2006b 3/10 7/9 0.39 [ 0.14, 1.06 ]
0.1 0.2 0.5 1 2 5 10
Cyclosporin Methylprednisolone
56 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
A P P E N D I C E S
Appendix 1. Electronic search strategies
Database Search terms
CENTRAL 1. MeSH descriptor Purpura, Schoenlein-Henoch, this term only
2. henoch next scho*nlein next purpura:ti,ab,kw
3. allergic next purpura:ti,ab,kw
4. anaphylactoid next purpura:ti,ab,kw
5. henoch next purpura:ti,ab,kw
6. nonthrombocytop*enic next purpura:ti,ab,kw
7. non next thrombocytop*enic next purpura:ti,ab,kw
8. leukocytoclastic next vasculitis:ti,ab,kw
9. peliosis next rheumatica:ti,ab,kw
10. purpura next rheumatica:ti,ab,kw
11. rheumatoid next purpura:ti,ab,kw
12. scho*nlein next disease:ti,ab,k
13. (#1 OR #2 OR #3 OR #4 OR #5 OR #6 OR #7 OR #8 OR #9 OR #10 OR #11 OR #12)
MEDLINE 1. Purpura, Schoenlein-Henoch/
2. henoch scho?nlein purpura.tw.
3. scho?nlein henoch purpura.tw.
4. allergic purpura.tw.
5. anaphylactoid purpura.tw.
6. henoch purpura.tw.
7. (nonthrombocytop?enic purpura or non thrombocytop?enic purpura).tw.
8. leukocytoclastic vasculitis.tw.
9. peliosis rheumatica.tw.
10. purpura rheumatica.tw.
11. rheumatoid purpura.tw.
12. scho?nlein disease.tw.
13. or/1-12
EMBASE 1. Anaphylactoid Purpura/
2. henoch scho?nlein.tw.
3. scho?nlein henoch.tw.
4. allergic purpura.tw.
5. anaphylactoid purpura.tw.
6. henoch purpura.tw.
7. nonthrombocytop?enic purpura.tw.
8. non thrombocytop?enic purpura.tw.
9. leukocytoclastic purpura.tw.
10. leukocytoclastic vasculitis.tw.
11. peliosis rheumatica.tw.
12. purpura rheumatica.tw.
13. rheumatoid purpura.tw.
14. scho?nlein disease.tw.
15. or/1-14
57 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Appendix 2. Risk of bias assessment tool
Potential source of bias Assessment criteria
Was there adequate sequence generation? Yes (low risk of bias): Random number table; computer random
number generator; coin tossing; shufing cards or envelopes;
throwing dice; drawing of lots; minimization (minimization may
be implemented without a randomelement, and this is considered
to be equivalent to being random).
No (high risk of bias): Sequence generated by odd or even date of
birth; date (or day) of admission; sequence generated by hospital
or clinic record number; allocation by judgement of the clinician;
by preference of the participant; basedonthe results of a laboratory
test or a series of tests; by availability of the intervention.
Unclear: Insufcient information about the sequence generation
process to permit judgement.
Was allocation adequately concealed? Yes (low risk of bias): Randomisation method described that would
not allow investigator/participant to know or inuence interven-
tiongroupbefore eligible participant enteredinthe study (e.g. cen-
tral allocation, including telephone, web-based, and pharmacy-
controlled, randomisation; sequentially numbered drug contain-
ers of identical appearance; sequentially numbered, opaque, sealed
envelopes).
No (high risk of bias): Using an open random allocation schedule
(e.g. a list of random numbers); assignment envelopes were used
without appropriate safeguards (e.g. if envelopes were unsealed or
non-opaque or not sequentially numbered); alternation or rota-
tion; date of birth; case record number; any other explicitly un-
concealed procedure.
Unclear: Randomisation stated but no information on method
used is available.
Was knowledge of the allocated interventions adequately pre-
vented during the study?
Yes (low risk of bias): No blinding, but the review authors judge
that the outcome and the outcome measurement are not likely
to be inuenced by lack of blinding; blinding of participants and
key study personnel ensured, and unlikely that the blinding could
have been broken; either participants or some key study personnel
were not blinded, but outcome assessment was blinded and the
non-blinding of others unlikely to introduce bias.
No (high risk of bias): No blinding or incomplete blinding, and the
outcome or outcome measurement is likely to be inuenced by
lack of blinding; blinding of key study participants and personnel
attempted, but likely that the blinding could have been broken;
either participants or some key study personnel were not blinded,
58 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
(Continued)
and the non-blinding of others likely to introduce bias.
Unclear: Insufcient information to permit judgement of Yes or
No
Were incomplete outcome data adequately addressed? Yes (low risk of bias): No missing outcome data; reasons for missing
outcome data unlikely to be related to true outcome (for survival
data, censoring unlikely to be introducing bias); missing outcome
data balanced in numbers across intervention groups, with similar
reasons for missing data across groups; for dichotomous outcome
data, the proportionof missing outcomes compared with observed
event risk not enough to have a clinically relevant impact on the
intervention effect estimate; for continuous outcome data, plau-
sible effect size (difference in means or standardized difference in
means) among missing outcomes not enough to have a clinically
relevant impact on observed effect size; missing data have been
imputed using appropriate methods.
No (high risk of bias): Reason for missing outcome data likely to
be related to true outcome, with either imbalance in numbers or
reasons for missing data across intervention groups; for dichoto-
mous outcome data, the proportion of missing outcomes com-
pared with observed event risk enough to induce clinically relevant
bias in intervention effect estimate; for continuous outcome data,
plausible effect size (difference in means or standardized differ-
ence in means) among missing outcomes enough to induce clini-
cally relevant bias in observed effect size; as-treated analysis done
with substantial departure of the intervention received from that
assigned at randomisation; potentially inappropriate application
of simple imputation.
Unclear: Insufcient information to permit judgement of Yes or
No.
Are reports of the study free of suggestion of selective outcome
reporting?
Yes (low risk of bias): The study protocol is available and all of the
studys pre-specied (primary and secondary) outcomes that are of
interest in the review have been reported in the pre-specied way;
the study protocol is not available but it is clear that the published
reports include all expected outcomes, including those that were
pre-specied (convincing text of this nature may be uncommon).
No (high risk of bias): Not all of the studys pre-specied primary
outcomes have been reported; one or more primary outcomes
is reported using measurements, analysis methods or subsets of
the data (e.g. subscales) that were not pre-specied; one or more
reported primary outcomes were not pre-specied (unless clear
justication for their reporting is provided, such as an unexpected
adverse effect); one or more outcomes of interest in the review are
reported incompletely so that they cannot be entered in a meta-
59 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
(Continued)
analysis; the study report fails to include results for a key outcome
that would be expected to have been reported for such a study.
Unclear: Insufcient information to permit judgement of Yes or
No.
Was the study apparently free of other problems that could
put it at a risk of bias?
Yes (low risk of bias): The study appears to be free of other sources
of bias.
No (high risk of bias): Had a potential source of bias related to
the specic study design used; stopped early due to some data-de-
pendent process (including a formal-stopping rule); had extreme
baseline imbalance; has been claimed to have been fraudulent; had
some other problem.
Unclear: Insufcient information to permit judgement of Yes or
No.
W H A T S N E W
Last assessed as up-to-date: 26 November 2008.
Date Event Description
18 March 2010 Amended Contact details updated.
H I S T O R Y
Protocol rst published: Issue 1, 2005
Review rst published: Issue 3, 2009
Date Event Description
16 June 2008 Amended Converted to new review format.
60 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
C O N T R I B U T I O N S O F A U T H O R S
Wattana Chartapisak: Study selection, quality appraisal, data extraction, data analysis, writing protocol, writing review.
Sauwalak Opastirakul: Study selection, quality appraisal, data extraction, writing protocol
Elisabeth Hodson: Study selection, quality appraisal, data extraction, data analysis, writing protocol, writing review.
Narelle Willis: Reviewing protocol and review, data analysis
Jonathan Craig: Writing review, disagreement resolution
D E C L A R A T I O N S O F I N T E R E S T
None known
D I F F E R E N C E S B E T W E E N P R O T O C O L A N D R E V I E W
New methodology for assessing the risk of bias - replaces assessment of quality.
I N D E X T E R M S
Medical Subject Headings (MeSH)
Adrenal Cortex Hormones [therapeutic use]; Cyclophosphamide [therapeutic use]; Immunosuppressive Agents [therapeutic use];
Kidney Diseases [etiology; prevention & control;
therapy]; Platelet Aggregation Inhibitors [therapeutic use]; Purpura, Schoenlein-
Henoch [
complications]; Randomized Controlled Trials as Topic
MeSH check words
Child; Child, Preschool; Humans
61 Interventions for preventing and treating kidney disease in Henoch-Schnlein Purpura (HSP) (Review)
Copyright 2010 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
You might also like
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5813)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Rosh ReviewDocument125 pagesRosh ReviewPrince Du100% (2)
- 0115 Seizures and SEDocument28 pages0115 Seizures and SEGavin TexeirraNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The HusiaDocument144 pagesThe HusiaGavin Texeirra100% (4)
- Primer On Nephrology 2022Document1,713 pagesPrimer On Nephrology 2022Maievp53100% (1)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- OSCE in Pediatrics, 2011Document267 pagesOSCE in Pediatrics, 2011floare de colt0% (1)
- ATLS Case ScenarioDocument13 pagesATLS Case ScenarioGavin Texeirra97% (39)
- Ventriculoperitoneal Shunt Complications in Children An Evidence-Based Approach To Emergency Department Management PDFDocument24 pagesVentriculoperitoneal Shunt Complications in Children An Evidence-Based Approach To Emergency Department Management PDFGavin TexeirraNo ratings yet
- Patho 4Document59 pagesPatho 4Anum SohaibNo ratings yet
- Nephrotic Syndrome What Is Nephrotic Syndrome? CauseDocument10 pagesNephrotic Syndrome What Is Nephrotic Syndrome? CauseThuganamix50% (2)
- Congenital Nephrotic SyndromeDocument44 pagesCongenital Nephrotic Syndromeaad81kolrenmed50% (2)
- HESI Exam PracticeDocument33 pagesHESI Exam PracticeJean AustenNo ratings yet
- Pediatrics MCQs - DR Ranjan Singh - Part 1Document10 pagesPediatrics MCQs - DR Ranjan Singh - Part 1k sagarNo ratings yet
- Conversion PDFDocument2 pagesConversion PDFGavin TexeirraNo ratings yet
- 0315 DVTDocument28 pages0315 DVTGavin TexeirraNo ratings yet
- Pedia Ward...Document11 pagesPedia Ward...Ella Ramirez MedinaNo ratings yet
- Sindroma Nefrotik Vs NefritikDocument23 pagesSindroma Nefrotik Vs NefritikBobby Fildian Siswanto100% (3)
- Home Epley HandoutsDocument4 pagesHome Epley HandoutsGavin Texeirra100% (1)
- Scrotal Masses EvaluationDocument2 pagesScrotal Masses EvaluationGavin TexeirraNo ratings yet
- Pulmonary EmbolismDocument9 pagesPulmonary EmbolismGavin Texeirra100% (1)
- Endometriosis With Hemorrhagic AscitiesDocument5 pagesEndometriosis With Hemorrhagic AscitiesGavin TexeirraNo ratings yet
- Alcohol Screening QuestionnaireDocument2 pagesAlcohol Screening QuestionnaireGavin TexeirraNo ratings yet
- MRX Software Version 7 Instructions For UseDocument326 pagesMRX Software Version 7 Instructions For UseGavin TexeirraNo ratings yet
- BPPVDocument2 pagesBPPVGavin TexeirraNo ratings yet
- Artigo 16Document8 pagesArtigo 16Gavin TexeirraNo ratings yet
- Philips Heartstart MRXDocument17 pagesPhilips Heartstart MRXGavin TexeirraNo ratings yet
- Pacemaker Data Collection From DeviceDocument6 pagesPacemaker Data Collection From DeviceGavin TexeirraNo ratings yet
- Last Look Nephrology & Rheumatology (Medicine Must Know)Document43 pagesLast Look Nephrology & Rheumatology (Medicine Must Know)rohankananiNo ratings yet
- NullDocument61 pagesNullSreehari BaijuNo ratings yet
- Renal, Urinary Systems - ElectrolytesDocument692 pagesRenal, Urinary Systems - ElectrolytesRoshan MevadaNo ratings yet
- Nephrotic SyndromeDocument31 pagesNephrotic Syndromedrhananfathy100% (1)
- Nephrotic Syndrome PresentationDocument39 pagesNephrotic Syndrome PresentationEzekiel moraraNo ratings yet
- TOP in Clinical Pedutrics PDFDocument227 pagesTOP in Clinical Pedutrics PDFSoad ShedeedNo ratings yet
- 58 Iajps58122019 PDFDocument4 pages58 Iajps58122019 PDFiajpsNo ratings yet
- Case Study 5 - DESOASIDODocument2 pagesCase Study 5 - DESOASIDOEDDREI PAULLYNNE DESOASIDONo ratings yet
- Renal Pathology - 012) Nephrotic Syndrome (Notes)Document10 pagesRenal Pathology - 012) Nephrotic Syndrome (Notes)hasanatiya41No ratings yet
- Efficacy of Rituximab Vs Tacrolimus in Pediatric Corticosteroid-Dependent Nephrotic Syndrome A Randomized Clinical TrialDocument16 pagesEfficacy of Rituximab Vs Tacrolimus in Pediatric Corticosteroid-Dependent Nephrotic Syndrome A Randomized Clinical Trialalicia keyNo ratings yet
- Nephrotic Syndrome in Children: The Indian Journal of Medical Research August 2005Document17 pagesNephrotic Syndrome in Children: The Indian Journal of Medical Research August 2005Hosne araNo ratings yet
- Mortality and Morbidity Conference: Service Census January 2019Document63 pagesMortality and Morbidity Conference: Service Census January 2019AnneCanapiNo ratings yet
- Nephrotic SyndromeDocument20 pagesNephrotic Syndromeami5687No ratings yet
- 1 s2.0 S0140673623010516 MainDocument16 pages1 s2.0 S0140673623010516 MainJOY INDRA GRACENo ratings yet
- Proteinuria in Adults - A Diagnostic Approach - American Family PhysicianDocument7 pagesProteinuria in Adults - A Diagnostic Approach - American Family PhysicianDr Sumant SharmaNo ratings yet
- Infeksi Parasitik Pada Sistem Ginjal Dan Saluran Kemih Dr. ErwinDocument39 pagesInfeksi Parasitik Pada Sistem Ginjal Dan Saluran Kemih Dr. ErwinDaud ParluhutanNo ratings yet
- Nephrotic SyndromeDocument17 pagesNephrotic Syndromevishnu0% (1)
- Panduan Intermediate CycleDocument17 pagesPanduan Intermediate CyclemuhammadridhwanNo ratings yet
- 1 Childhood Nephrotic Syndrome - Diagnosis and ManagementDocument52 pages1 Childhood Nephrotic Syndrome - Diagnosis and ManagementNilupul Niwantha100% (1)
- 16.nephrotic SyndromeDocument115 pages16.nephrotic SyndromeRhomizal MazaliNo ratings yet