Professional Documents
Culture Documents
LENTIGO
Uploaded by
NisaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
LENTIGO
Uploaded by
NisaCopyright:
Available Formats
pediatric dermatology
Series Editor: Camila K. Janniger, MD, Newark, New Jersey
Lentigo
Jason F. Okulicz, MD, Newark, New Jersey
Robert A. Schwartz, MD, MPH, Newark, New Jersey
Sergiusz Jzwiak, MD, PhD, Warsaw, Poland
A lentigo is a small pigmented macule with a sharply
circumscribed border. There are multiple clinical
and etiologic forms. Lentigines are often initially
identified shortly after birth, although they may
appear later in childhood. Certain varieties are
associated with systemic abnormalities. Histologic
findings include epidermal hyperplasia with
increased pigmentation of the basal layer.
Lentigo is derived from the Latin word lens meaning lentil.1 Pigmentation varies from homogeneous
to variegated and from brown to black. Lentigines
may evolve slowly over a number of years, or they
may be eruptive, appearing in a short period. They
can be either solitary or multiple, occurring
anywhere on the body depending on the type of
lentigo.2 Certain varieties have associated systemic
manifestations. The clinical distinction of a lentigo,
as opposed to other melanocytic lesions such as
melanocytic nevi or melanoma, is of major significance because of its role as a marker for UV damage
or systemic syndromes.3
Epidemiology
Lentigines are commonly found in people around the
world. Lentigo simplex is the most common form of
lentigo, but its frequency has yet to be determined.4
A study conducted by Alper and Holmes5 revealed
multiple lentigines in 18.5% of 492 black newborns
and in 0.04% of 2682 white newborns. However, histologic confirmation of these lesions was lacking.
Clinical Manifestations
The clinical presentation of lentigines varies depending on their type. Various forms of lentigines
appear in children and are described as follows.
Drs. Okulicz and Schwartz are from the Department of
Dermatology, New Jersey Medical School, Newark. Dr. Jzwiak is
from the Department of Child Neurology, The Childrens Memorial
Health Institute, Warsaw, Poland.
Reprints: Robert A. Schwartz, MD, MPH, Department of
Dermatology, New Jersey Medical School, 185 S Orange Ave,
Newark, NJ 07103-2714.
Lentigo SimplexLentigo simplex, also referred to
as simple or juvenile lentigo, is the most common
form of lentigo. The lentigines are similar in appearance to solar lentigines or liver spots, but they lack
the predilection for sun exposed areas of the body.
Additionally, simple lentigines usually appear initially
in childhood, as opposed to solar lentigines, which
appear in adulthood.6,7 Simple lentigines are round to
oval, asymptomatic macules measuring 3 to 15 mm
in diameter.8 The margins are either jagged or smooth,
and the color ranges from brown to black with even
distribution of pigmentation. Lesions occur anywhere
on the body and are generally few.2
Lentigines ProfusaLentigines profusa, or generalized lentigines, is characterized by numerous
lentigines without signs of associated abnormalities
or triggering factors. The clinical appearance is similar to ephelides, but the distribution is widespread.2
The areas most commonly involved include the
trunk, extremities, palms, genitalia, and mucosal
surfaces such as the conjunctiva, but the buccal
mucosa and soles may be spared. The macules are
dark brown to black and vary in size from 1 mm to
2 cm in diameter.9 Cutaneous manifestations of
lentigines profusa are similar to those of LEOPARD,
LAMB, and NAME syndromes10,11; however, a
notable exception is the lack of physical anomalies
and defects associated with these syndromes.
Agminated LentiginesAgminated lentigines, also
known as segmental, unilateral, or partial unilateral
lentigines, are characterized by numerous lentigines
geographically confined to a particular body
segment.12 The distribution frequently occurs in a
dermatomal pattern. Less commonly, they can be
distributed in midline clusters or a checkerboard
pattern, either unilaterally or bilaterally. The lesions
may be noted at birth, although onset usually occurs
in early childhood.4 Clinically, they appear as dark
circumscribed macules on normal background skin.
This distinguishes agminated lentigines from segmental nevi in which the background skin is hyperpigmented.2 Agminated lentigines are associated
with numerous diseases.4
VOLUME 67, MAY 2001 367
PEDIATRIC DERMATOLOGY
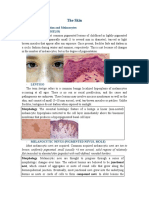
A 13-year-old girl with xeroderma pigmentosum.
Xeroderma PigmentosumXeroderma pigmentosum (Figure) is a condition whose abnormalities stem
from an inability of cells to repair DNA damage
induced by UV light and certain chemicals. Xeroderma pigmentosum is inherited in an autosomal
recessive fashion. Clinically, patients develop
progressive pigmentary changes and skin atrophy.
Subsequent neoplastic changes occur in the skin,
often in childhood.13 Malignancies most commonly
associated with xeroderma pigmentosum are squamous and basal cell carcinomas. However, other
neoplasms such as melanoma also may occur.14 All of
these neoplasms occur on sun exposed areas, particularly the head, neck, and face. The diagnosis of
xeroderma pigmentosum is often delayed until the
skin exhibits some evidence of solar damage. It is
essential for children to avoid sun exposure whenever possible to prevent the acceleration of skin
changes that lead to the formation of skin cancers.13
Peutz-Jeghers SyndromePeutz-Jeghers syndrome
is an autosomal dominant condition with a high
degree of penetrance. The syndrome is characterized
by gastrointestinal polyps and pigmented macules.
The polyps are benign hamartomas of the entire
bowel, with jejunal involvement most characteristic.15,16 The polyps result in recurrent abdominal pain
and perirectal bleeding. Initially, patients are seen in
early childhood with bleeding or signs of intussusception. The lentigines are brown to black to blue
macules varying from 1 to 12 mm in diameter15,16 and
may be present at birth or appear during early childhood. They characteristically involve the lips, mouth,
and buccal mucous membranes, with scattered lesions
around the nose and face. Lesions also may appear on
both the palmar and volar surfaces of the fingers and
toes. There is a characteristic absence on the flexor
368 CUTIS
and extensor surfaces of the rest of the body.16 Some
macules may fade with age, but buccal mucosal macules persist throughout the patients life.15,16 There
appears to be no correlation between the extent of
melanosis and the extent of polyposis. After childhood, most women with Peutz-Jeghers syndrome
develop unusual sex cord tumors, which tend to be
small, bilateral, multifocal, and asymptomatic. These
women also have an increased risk of developing
unilateral or bilateral breast cancer. 15 In addition,
Sertoli cell tumors also have been noted to occur in
men with the condition.
LEOPARD SyndromeLEOPARD syndrome, or
multiple lentigines syndrome, is a condition associated with lentigines, electrocardiographic conduction
defects, ocular hypertelorism, pulmonary stenosis,
abnormal genitalia, retardation of growth, and deafness.16,17 This complex dysmorphogenetic disorder is
autosomal dominant with variable penetrance.10,11
Diagnosis may be difficult because most patients
exhibit only 3 to 5 of the characteristic criteria.
Lentigines are the most typical and one of the most
frequent features.11 Lentigines are present at birth, and
their numbers continue to increase until puberty.
Numerous macules occur on the neck and trunk but
also erupt on the genitalia, scalp, palms, and soles.10,11,18
There is typically some sparing of the face. In some
cases, lentigines may be limited to one side of the
body.17,18 If lentigines are absent, a diagnosis of
LEOPARD syndrome can be made if a patient has an
immediate relative with the disorder and has features
in at least 3 other categories.11,16
Lentigines/Myxoma Syndromes
The following syndromes are associated with lentigines
and myxomas, which can be cardiac, mucocutaneous,
or both.
LAMB SyndromeLAMB syndrome is associated
with lentigines, atrial myxomas, mucocutaneous myxomas, and blue nevi.16 The lentigines are brown and
can be as large as 1 cm in diameter. They are commonly found on the face, lips, sclera, and vulva. The
mucocutaneous myxomas appear on various sites of
the body as papules or dermal nodules and most commonly occur on the tongue, oral mucosa, genitalia,
breasts, and shoulders. Cardiac myxomas occur most
often in adulthood but can, on rare occasions, occur
in childhood. They are usually atrial myxomas, which
can cause valvate obstructions and embolic episodes.19
NAME SyndromeNAME syndrome, a possible
variant of LAMB syndrome, is a combination of
nevi, atrial myxomas, myxoid neurofibromas, and
ephelides.20,21 Lentigines arise as flat, pigmented,
pale to dark brown macules that often begin at birth
and are accentuated in the summer months. The
PEDIATRIC DERMATOLOGY
most common areas affected include the neck,
trunk, and thighs; however, the palms and soles also
may be affected.20
Carney SyndromeCarney syndrome is characterized by cardiac, cutaneous, and mammary myxomatous masses, as well as lentigines, blue nevi,
testicular tumors, and endocrine disorders.22,23 Organ
involvement is often multicentric and bilateral in
young patients.23 Cutaneous myxomas are most
prevalent on the eyelids but also can be found on
the nipples, face, scalp, ears, oral mucosa, neck,
trunk, limbs, and perineum. Single or multiple cardiac myxomas often lead to fibrosis or calcification.
There are 2 types of pigmented macules, namely
blue nevi and lentigines. Lentigines are usually 0.2
to 2 mm in diameter with irregularly shaped jagged
margins. Their color ranges from brown to black,
and distribution is widespread throughout the body,
often coalescing to form large brown patches.
Lentigines are most commonly located on the face,
ears, eyelids, and vermilion borders of the lips. Less
commonly, they occur on the conjunctiva, extremities, vulva, and glans penis. Buccal macules are
rare in contrast to Peutz-Jeghers syndrome.15,22
Endocrine involvement varies but includes calcifying, pigmented, neuroectodermal tumors; pituitary
adenomas with acromegaly and gigantism; and
adrenocortical disease leading to Cushing syndrome. Testicular tumors include Sertoli cell,
Leydig cell, and adrenal rest tumors. Mammary
involvement features gynecomastia and myxomatous enlargement of the stroma.22
ridges associated with marked hyperpigmentation of
the basal layer.19 NAME syndrome is characterized by
lentigines with increased pigmentation of both the
basal and spinous epidermal layers.20,21 Carney syndrome lentigines exhibit hyperpigmentation of the
basal layer and melanocytic hyperplasia, with or without rete ridge elongation.22
Histology
Lentigo simplex exhibits a slight to moderate
elongation of the rete ridges with melanocyte
proliferation in the basal layer, increased melanin in
both melanocytes and basal keratinocytes, and the
presence of melanophages in the upper dermis.1,6
Both lentigines profusa and agminated lentigines are
similar in appearance.4,9,12
Xeroderma pigmentosum lentigines show hyperkeratosis with epidermal atrophy. A few rete ridges
also may be elongated. The basal cell layer contains
increased pigment with a variable number of
melanocytes, and the upper dermis may contain
chronic inflammatory cells.13 Peutz-Jeghers syndrome lentigines have marked hyperpigmentation of
the basal layer but do not always display increased
melanocytes.15,16 LEOPARD syndrome lentigines
exhibit increased pigment content of the epidermis
and increased melanocytes containing melanosomes
that are distributed either singly or in the form
of micronests.10,11
LAMB syndrome lentigines show elongated rete
REFERENCES
Differential Diagnosis
Lentigines may have to be differentiated from other
pigmented lesions such as ephelides, flat seborrheic
keratosis, actinic keratosis, melanocytic nevi, lentigo
maligna, and melanoma. These lesions not only may
appear similar clinically but also may require skillful
distinction histologically.
Treatment
Isolated lentigines can be treated with simple
cryosurgery, which is often successful because
melanocytes are susceptible to freezing with the use
of liquid nitrogen. Destruction of melanocytes is
known to occur at temperatures of 4C to 7C,
while squamous cells resist injury even at 20C.24
The use of lasers has been shown to be effective
in the treatment of lentigines. The frequency-doubled
Q-switched Nd:YAG laser, the 532-nm diodepumped vanadate laser, and the HGM K1 krypton
laser have all been employed with success.25,26
Noninvasive agents such as topical creams also
have been used. After several months of application,
the combination of tretinoin cream and hydroquinone cream have shown to lighten lentigines.7,27
1. The American Heritage Dictionary of the English Language.
2nd college ed. Boston, Mass; Houghton Mifflin Co;
1982;724.
2. Ber Rahman S, Bhawan J. Lentigo. Int J Dermatol. 1996;
35:229-239.
3. Rhodes AR, Melski JW, Sober AJ. Increased intraepidermal melanocyte frequency and size in dysplastic
melanocytic nevi and cutaneous melanoma: a comparative
quantitative study of dysplastic melanocytic nevi, superficial spreading melanoma, nevocellular nevi, and solar
lentigines. J Invest Dermatol. 1983;80:452-459.
4. Micali G, Nasca MR, Innocenzi D. Agminated lentiginosis:
case report and review of the literature. Pediatr Dermatol.
1994;11:241-245.
5. Alper JC, Holmes LB. The incidence and significance of
birthmarks in a cohort of 4,641 newborns. Pediatr Dermatol. 1983;1:58-68.
6. Mehregan AH. Lentigo senilis and its evolutions. J Invest
Dermatol. 1975;65:429-433.
7. Beacham BE. Solar-induced epidermal tumors in the elderly. Am Fam Physician. 1990;42:153-160.
VOLUME 67, MAY 2001 369
PEDIATRIC DERMATOLOGY
8. Buchner A, Hansen LS. Melanotic macule of the oral mucosa: a clinicopathologic study of 105 cases. Oral Surg Oral
Med Oral Pathol. 1979;48:244-249.
9. Uhle P, Norvell SS Jr. Generalized lentiginosis. J Am Acad
Dermatol. 1988;18:444-447.
10. Jozwiak S, Schwartz RA, Janniger CK. LEOPARD syndrome (cardiocutaneous lentiginosis syndrome). Cutis.
1996;57:208-214.
11. Jozwiak S, Schwartz RA, Janniger CK. Familial occurrence
of the LEOPARD syndrome. Int J Dermatol. 1998;37:48-51.
12. Pique E, Aguilar A, Farina MC. Partial unilateral lentiginosis: report of seven cases and review of the literature. Clin
Exp Dermatol. 1995;20:319-322.
13. Leibowitz E, Janniger CK, Schwartz RA. Xeroderma pigmentosum. Cutis. 1997;60:75-77,81-84.
14. Tsao H. Update on familial cancer syndromes and the skin.
J Am Acad Dermatol. 2000;42:939-969.
15. Finan MC, Ray MK. Gastrointestinal polyposis syndromes.
Dermatol Clin. 1989;7:419-434.
16. Lucky AW. Pigmentary abnormalities in genetic disorders.
Dermatol Clin. 1988;6:193-203.
17. Voron DA, Hatfield HH, Kalkhoff RK. Multiple lentigines
syndrome. Case report and review of the literature. Am J
Med. 1976;60:447-456.
18. Bhawan J, Purtilo DT, Riordan JA. Giant and granular
melanosomes in Leopard syndrome: an ultrastructural
study. J Cutan Pathol. 1976;3:207-216.
19. Rhodes AR, Silverman RA, Harrist TJ. Mucocutaneous
370 CUTIS
20.
21.
22.
23.
24.
25.
26.
27.
lentigines, cardiomucocutaneous myxomas, and multiple
blue nevi: the LAMB syndrome. J Am Acad Dermatol.
1984;10:72-82.
Atherton DJ, Pitcher DW, Wells RS. A syndrome of various cutaneous pigmented lesions, myxoid neurofibromata
and atrial myxoma: the NAME syndrome. Br J Dermatol.
1980;103:421-429.
Rees JR, Ross FG, Keen G. Lentiginosis and left atrial myxoma. Br Heart J. 1973;35:874-876.
Carney JA, Gordon H, Carpenter PC. The complex of myxomas, spotty pigmentation, and endocrine overactivity.
Medicine (Baltimore). 1985;64:270-283.
Martin-Reay DG, Shattuck MC, Guthrie FW Jr. Psammomatous melanotic schwannoma: an additional component
of Carneys complex. report of a case. Am J Clin Pathol.
1991;95:484-489.
Leroy D, Dompmartin A, Dubreuil A. Cryotherapy of
PUVA lentigines. Br J Dermatol. 1996;135:988-990.
Chan HH, Fung WK, Ying SY. An in vivo trial comparing
the use of different types of 532 nm Nd:YAG lasers in the
treatment of facial lentigines in Oriental patients. Dermatol Surg. 2000;26:743-749.
Todd MM, Rallis TM, Gerwels JW. A comparison of 3 lasers
and liquid nitrogen in the treatment of solar lentigines: a
randomized, controlled, comparative trial. Arch Dermatol.
2000;136:841-846.
Roenigk HH Jr. Treatment of the aging face. Dermatol Clin.
1995;13:245-261.
You might also like
- Conducting Effective Meetings WorkBookDocument36 pagesConducting Effective Meetings WorkBookCheri HoNo ratings yet
- Down SyndromeDocument4 pagesDown SyndromeninaersNo ratings yet
- Toacs 6Document159 pagesToacs 6Mobin Ur Rehman Khan100% (2)
- Birthmarks Identificationandmx201205ryanDocument4 pagesBirthmarks Identificationandmx201205ryanDanielcc LeeNo ratings yet
- MnemonicS in OphthaDocument22 pagesMnemonicS in Ophthaabuahmed&janaNo ratings yet
- 3 - Cellular Respiration NotesDocument22 pages3 - Cellular Respiration Notesapi-375285021No ratings yet
- Tomorrow Is WaitingDocument8 pagesTomorrow Is WaitingsrplsmskNo ratings yet
- Newborn Physical AssessmentDocument7 pagesNewborn Physical AssessmentFady Jehad Zaben100% (1)
- Vascular Anomalies PresentationDocument45 pagesVascular Anomalies PresentationMhinory OctNo ratings yet
- MRCPCH - Important Skin DiseasesDocument42 pagesMRCPCH - Important Skin DiseasesarjumandNo ratings yet
- Sys-Am-14 Designing An 'Iaq Ready' Air Handler SystemDocument71 pagesSys-Am-14 Designing An 'Iaq Ready' Air Handler SystemtpqnhatNo ratings yet
- Pics MCQSDocument22 pagesPics MCQStania100% (1)
- Erythema MultiformeDocument29 pagesErythema MultiformeSurabhi Sharma100% (1)
- Cleft Lip and Palate New ApproachDocument115 pagesCleft Lip and Palate New ApproachsoorajNo ratings yet
- Cisco Wireless LAN Controller - Configuration Guide PDFDocument696 pagesCisco Wireless LAN Controller - Configuration Guide PDFMiguel MazaNo ratings yet
- LentigoDocument15 pagesLentigoaditya ratna utariNo ratings yet
- Disorders of Pigmentation: John C. Mavropoulos and Bernard A. CohenDocument21 pagesDisorders of Pigmentation: John C. Mavropoulos and Bernard A. Cohendeby sepangNo ratings yet
- Painfulorallesions: Istvan A. HargitaiDocument13 pagesPainfulorallesions: Istvan A. HargitaiAlejandro Ln CNo ratings yet
- Sporothrix and M LepraeDocument6 pagesSporothrix and M LepraeVictor Juris AnonuevoNo ratings yet
- Vesicubullous Diseases & Mucocutaneous DisordersDocument23 pagesVesicubullous Diseases & Mucocutaneous Disordersshahlaraib001No ratings yet
- Ilovepdf MergedDocument22 pagesIlovepdf MergedSRO oONo ratings yet
- Genodermatosis: The IchthyosisDocument4 pagesGenodermatosis: The IchthyosisOman ArifNo ratings yet
- Linear LesionsDocument39 pagesLinear LesionsRegina CzerniawskaNo ratings yet
- Subcutaneous Granuloma Annulare (Pseudorheumatoid Nodule) - , F 38, Ankles.Document13 pagesSubcutaneous Granuloma Annulare (Pseudorheumatoid Nodule) - , F 38, Ankles.Deba P SarmaNo ratings yet
- Bahan Nevus LinearDocument23 pagesBahan Nevus LinearDwi Akbarini AwiNo ratings yet
- Levy 2012Document20 pagesLevy 2012Anonymous ujOv31SNo ratings yet
- Leg, Arm, and Chest Papules: ERM ASEDocument9 pagesLeg, Arm, and Chest Papules: ERM ASEdeenutz93No ratings yet
- Trisomy 21 SyndromeDocument12 pagesTrisomy 21 SyndromeJoan Vinata WinonaNo ratings yet
- Childhood Granulomatous Periorificial DermatitisDocument4 pagesChildhood Granulomatous Periorificial DermatitisNiaUlfaAngreiniTambunanNo ratings yet
- Gejala LeukokoriaDocument37 pagesGejala LeukokoriaAnonymous mFKwUNNo ratings yet
- DBST Dlja INO Studentov (PDF - Io)Document6 pagesDBST Dlja INO Studentov (PDF - Io)eidNo ratings yet
- Pediatric Tumors of The Eye and OrbitDocument60 pagesPediatric Tumors of The Eye and OrbitDMdewiNo ratings yet
- The of Squint: ManagementDocument6 pagesThe of Squint: ManagementAndi AlfianaNo ratings yet
- Skin PigmentatDocument110 pagesSkin Pigmentatsteven saputra0% (1)
- Diagnosis and Management of Down Syndrome: Guest Editor: Bhim S. PandhiDocument8 pagesDiagnosis and Management of Down Syndrome: Guest Editor: Bhim S. PandhiRidwan Balatif - Co-AsstNo ratings yet
- Oral Pathology I Final ReviewDocument373 pagesOral Pathology I Final ReviewAlex ChangNo ratings yet
- Oral Cavity Genetic Disorders Affecting The Oral Mucosa and LipsDocument17 pagesOral Cavity Genetic Disorders Affecting The Oral Mucosa and LipsLakshya J BasumataryNo ratings yet
- Lichen Planus: Skin Mucous Membranes, Nails Hair. Shiny, PapularDocument54 pagesLichen Planus: Skin Mucous Membranes, Nails Hair. Shiny, PapularWorku KifleNo ratings yet
- Oral Lichen PlanusDocument10 pagesOral Lichen PlanusChander KantaNo ratings yet
- 6 - Disorders of MelanocytesDocument5 pages6 - Disorders of MelanocytesAbdul FatahNo ratings yet
- Localized Scleroderma: Clinical Spectrum and Therapeutic UpdateDocument12 pagesLocalized Scleroderma: Clinical Spectrum and Therapeutic UpdateMati AjaNo ratings yet
- 80-Article Text-153-1-10-20161118Document4 pages80-Article Text-153-1-10-20161118Rania SalwanabilaNo ratings yet
- LEUKOKORIADocument3 pagesLEUKOKORIAFahlevie EpinNo ratings yet
- Edward Syndrome: Continuing Education ActivityDocument14 pagesEdward Syndrome: Continuing Education ActivitylalaaNo ratings yet
- Nursing Care Plan For Down SyndromeDocument20 pagesNursing Care Plan For Down SyndromeMuhammad Jefri LukmanNo ratings yet
- Developmental Anamolies of Soft Tissues of Oral CavityDocument73 pagesDevelopmental Anamolies of Soft Tissues of Oral Cavityvellingiriramesh53040% (1)
- Leprosy ManualDocument12 pagesLeprosy ManualArumNo ratings yet
- Chromosomal DisorderDocument23 pagesChromosomal DisorderUmair RizwanNo ratings yet
- MedscapeDocument12 pagesMedscapeRissa WatlolyNo ratings yet
- Print Jurnal 3Document7 pagesPrint Jurnal 3Amalia GrahaniNo ratings yet
- Leprosy ManualDocument16 pagesLeprosy ManualMikee Laceda NamquiNo ratings yet
- Vascular Skin LesionsDocument39 pagesVascular Skin LesionsApril Mae Magos LabradorNo ratings yet
- Oral Pathology: Hyperplasia of Oral MucosaDocument7 pagesOral Pathology: Hyperplasia of Oral Mucosaعلي صادق جعفرNo ratings yet
- NRG 204 - Genetics and TestingDocument2 pagesNRG 204 - Genetics and TestingkeishyaaacarlosNo ratings yet
- You May Find Useful Some of My Pathology Notes. Markos Greece. You May Find Useful Some of My Pathology Notes. Markos Greece. (10557)Document3 pagesYou May Find Useful Some of My Pathology Notes. Markos Greece. You May Find Useful Some of My Pathology Notes. Markos Greece. (10557)Shawn Gaurav JhaNo ratings yet
- Thea Brigette Vergara: Name: Date SubmittedDocument9 pagesThea Brigette Vergara: Name: Date SubmittedMj YuNo ratings yet
- Only Café Au Lait Macule Variant of Neurofibromatosis Without Neurofibroma: A Rare Case ReportDocument2 pagesOnly Café Au Lait Macule Variant of Neurofibromatosis Without Neurofibroma: A Rare Case ReportHowthul AlamNo ratings yet
- Robinson HC CT105003132Document5 pagesRobinson HC CT105003132Francesca BizzocoNo ratings yet
- 494 PDFDocument6 pages494 PDFranz ibonkNo ratings yet
- Vascular Anomalies in Pediatrics 2012 Surgical Clinics of North AmericaDocument32 pagesVascular Anomalies in Pediatrics 2012 Surgical Clinics of North AmericaAntonio TovarNo ratings yet
- Seborrheic KeratosisDocument12 pagesSeborrheic KeratosisMaiza MujadillahNo ratings yet
- Tuberous Sclerosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandTuberous Sclerosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- 8993060532-6991517762a Rod Handling System For CT20: Spare Parts ListDocument164 pages8993060532-6991517762a Rod Handling System For CT20: Spare Parts ListErick Ticona FalconNo ratings yet
- Course Outline BRM AbasynDocument4 pagesCourse Outline BRM Abasynsadeeq sahilNo ratings yet
- Guard Rail Cataloge PDFDocument28 pagesGuard Rail Cataloge PDFreza acbariNo ratings yet
- Examination of Foot and Ankle JointDocument58 pagesExamination of Foot and Ankle JointSantosh KumarNo ratings yet
- Kecamatan Sooko Dalam Angka 2022Document152 pagesKecamatan Sooko Dalam Angka 2022alexanNo ratings yet
- Methods of Determining Thermal Efficiency in Spray Drying ProcessDocument3 pagesMethods of Determining Thermal Efficiency in Spray Drying ProcessDfunz WilphenNo ratings yet
- Practice UA3 Spring 2023Document15 pagesPractice UA3 Spring 2023moyin idowuNo ratings yet
- NCQC Answer Paper-1Document4 pagesNCQC Answer Paper-1Shyamal KumarNo ratings yet
- If ClauseDocument13 pagesIf Clausemadeleine mmdNo ratings yet
- Ethnography Discussion QuestionsDocument2 pagesEthnography Discussion Questionsapi-235718856100% (1)
- Minimum Drag Velocity ExplainedDocument4 pagesMinimum Drag Velocity ExplainedpersesutiNo ratings yet
- C C C !" # # $C% & #'C%Document12 pagesC C C !" # # $C% & #'C%Sneha ShahNo ratings yet
- International Financial Regulation Seminar QuestionsDocument2 pagesInternational Financial Regulation Seminar QuestionsNicu BotnariNo ratings yet
- Workshop On Previewing - CECARDocument12 pagesWorkshop On Previewing - CECARestefaany tejada100% (2)
- Statistical Physics Phy632-Tutorial: Sharifah Hafizah Binti Syed Ab AzizDocument26 pagesStatistical Physics Phy632-Tutorial: Sharifah Hafizah Binti Syed Ab AzizSharifahHafizahAl-jufNo ratings yet
- Research Paper On Employee BenefitsDocument7 pagesResearch Paper On Employee Benefitskrqovxbnd100% (1)
- TKT Module 1 Task Type 4 Introduction To Odd One Out Tasks PDFDocument9 pagesTKT Module 1 Task Type 4 Introduction To Odd One Out Tasks PDFRachel Maria RibeiroNo ratings yet
- Momento de Inercia GD2 PDFDocument9 pagesMomento de Inercia GD2 PDFDavid Delgado RendónNo ratings yet
- Lecture-8: Identification of The Suspect: Attributing Cyber Conduct To A PersonDocument22 pagesLecture-8: Identification of The Suspect: Attributing Cyber Conduct To A Personreputation.com.ngNo ratings yet
- Jawab Semua Soalan Dalam Bahagian IniDocument23 pagesJawab Semua Soalan Dalam Bahagian Inisusan6No ratings yet
- ICMA2011 DigestDocument160 pagesICMA2011 DigestPREEDAIENGINEERINGNo ratings yet
- Z370 AORUS Gaming 3: User's ManualDocument48 pagesZ370 AORUS Gaming 3: User's ManualAtrocitus RedNo ratings yet
- ModelsDocument6 pagesModelsUJJWALNo ratings yet
- DX11 Effects in Metro 2033Document47 pagesDX11 Effects in Metro 2033test23No ratings yet
- Military-Grade Counter-Drone System: Protect Your Airspace From Drone AttacksDocument8 pagesMilitary-Grade Counter-Drone System: Protect Your Airspace From Drone Attackscroffle.inNo ratings yet