Professional Documents
Culture Documents
Entropion 2
Uploaded by
Casey CameronOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Entropion 2
Uploaded by
Casey CameronCopyright:
Available Formats
Original Article-Surgery
www.cmj.ac.kr
Clinical Effect of a Mixed Solution of Sodium Hyaluronate and
Sodium Carboxymethylcellulose During the Transconjunctival
Approach for Orbital Wall Reconstruction
Byung Wan Kang, Hyo Seok Lee, Han Jin Oh and Kyung Chul Yoon*
Department of Ophthalmology, Research Institute of Medical Sciences, Chonnam National University Medical School and Hospital,
Gwangju, Korea
This study aimed to evaluate the anti-adhesive effect of a mixed solution of sodium hya
luronate and sodium carboxymethylcellulose (HACMC, Guardix-sol ) during the
transconjunctival approach to orbital wall reconstruction. Eighty-seven patients who
underwent orbital wall reconstruction by the transconjunctival approach were enrolled
in this prospective study. We applied HACMC between the orbicularis oculi muscle and
the orbital septum after surgery in 47 patients and did not use it in 40 patients. Lower
lid retraction and marginal reflex distance 2 (MRD2) were measured to analyze the degree of postoperative adhesion at 1 week and 1, 3, and 6 months. The degree of MRD2
showed clinically significant differences at postoperative 1 week and 1 month between
the HACMC and control groups (p0.05). Lower lid ectropion developed in two patients
(5.0%) in the control group but did not occur in the HACMC group. In orbital wall reconstruction by the transconjunctival approach, the HACMC mixture solution is effective for preventing adhesion and lower lid ectropion during the early postoperative
period.
Key Words: Eyelid retraction; Eyelids; Orbital fractures
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial
License (http://creativecommons.org/licenses/by-nc/3.0) which permits unrestricted non-commercial use,
distribution, and reproduction in any medium, provided the original work is properly cited.
Corresponding Author:
Kyung Chul Yoon
Department of Ophthalmology,
Medical School & Research Institute of
Medical Sciences, Chonnam National
University, 8 Hak-dong, Dong-gu,
Gwangju 501-757, Korea
TEL: +82-62-220-6741
FAX: +82-62-227-1642
E-mail: kcyoon@jnu.ac.kr
to prevent adhesion and are absorbed by the surrounding
tissue after the wound healing process. In addition, such
agents do not require an additional removal process after
application because the absorption of the adhesive material into the body is harmless. In ophthalmologic surgery, anti-adhesives have been used in strabismus surgery to prevent adhesion between the extraocular muscles and sclera
as well as in dacryocystorhinostomy to prevent adhesion
at the rhinostomy site.6-9 In addition, a mixture of sodium
hyaluronate (HA) and carboxymethylcellulose (CMC), also
known as Seprafilm (Genzyme Corp., Cambridge, MA,
USA), has been used in orbital wall reconstruction.10
In the present study, we evaluated the clinical anti-adhesive effects of HACMC, a mixture of HA and CMC, by applying it between the orbicularis oculi muscle and orbital septum during a transconjunctival surgical procedure for orbital wall fracture.
INTRODUCTION
Orbital wall reconstruction by the transconjunctival approach involves reduction of the protruded tissue from the
fracture site and insertion of a prosthesis to recover both
the functional and anatomical roles of the orbital wall.1
Diplopia, enophthalmos, ocular deviation, lower lid retraction, infra-orbital nerve damage, occlusion of the lacrimal passage, dacryocystitis, pupil dilation, and lymph
edema are well-known complications that can occur after
orbital wall reconstruction. Among these, lower lid retraction can result in severe problems associated with
cosmesis and tear film function and is known to be caused
by contracture between the orbicularis oculi muscle and orbital septum.2
Recently, many studies have been performed on the use
of various anti-adhesive agents after orbital wall reconstruction by the transconjunctival approach.3-5 Anti-adhesive agents form a physical barrier around the surgical area
http://dx.doi.org/10.4068/cmj.2012.48.2.123
Chonnam Medical Journal, 2012
Article History:
received 13 July, 2012
revised 24 July, 2012
accepted 24 July, 2012
123
Chonnam Med J 2012;48:123-127
Anti-adhesive Effect of HACMC
MATERIALS AND METHODS
A prospective study was performed on 87 eyes of 87 patients who visited our hospital, underwent orbital wall reconstruction by the transconjunctival approach, and were
followed up for at least 6 months from July 2009 to August
2010. No patients had a history of surgery, damages, or abnormality of the lower lid. Anti-adhesive solution was applied between the orbicularis oculi muscle and orbital septum in 47 eyes of 47 patients (the HACMC group), whereas
no anti-adhesive solution was administered to the other 40
eyes of 40 patients (the control group) during the operation.
The anti-adhesive solution, Guardix-sol (Hanmi Pharm
Co., Seoul, Korea), is a colorless clear liquid that uses a 1:1
mixture ratio of HA and CMC. External ocular muscle
movement, forced duction, diplopia, and Hertel exophthalmometer test were evaluated along with routine ophthalmologic examinations. In addition, computed tomography scanning was performed to determine the size and
location of the orbital wall fracture and the involvement of
orbital soft tissues.
Surgery was performed through the transconjunctival
approach under general anesthesia by a single surgeon
(K.C.Y.). The lower lid was retracted downward and an incision was made on the conjunctiva along the border of the
tarsal plate by unipolar electrocautery. The orbicularis
oculi muscle was removed from the orbital septum, and a
DesMarres retractor was used to retract the lower lid and
orbicularis muscle downward. A malleable retractor was
inserted behind the orbital septum to expose the periosteum of the inferior orbital border. A #15 Bard-Parker
knife was used to make an incision on the periosteum, and
a rugine was used to expose the fracture site. Then, the
malleable retractor, suction tip, and rugine were used to
repair the muscles and soft tissues. The damage site was
measured, and Medpor (Stryker, Newnan, GA, USA) was
inserted on the fracture site after applying anti-bacterial
solution. The periosteum was sutured with 5-0 Vicryl sutures, and Guardix-sol was applied between the orbicu-
laris oculi muscle and the orbital septum. Finally, the conjunctiva was sutured with 6-0 Vicryl sutures.
To prevent lower lid retraction, a traction suture was applied to the lower lid to pull it upward. The suture was removed 3 days after the surgery, and dexamethasone was
injected intravenously after the surgery to reduce edema,
which was tapered over 3 days. Ofloxacin (Ocuflox, Samil,
Seoul, Korea) and 0.1% fluorometholone (Ocumetholone,
Samil, Seoul, Korea) eyedrops were applied three times a
day.
Follow-up examination was performed at 1 week and 1,
3, and 6 months after surgery. Ocular movement was classified into five grades as follows: grade 0, no ocular movement impairment; grade 1, 75% of ocular movement compared with the other eye; grade 2, 50-75% of ocular movement compared with the other eye; grade 3, 25-50% of ocular movement compared with the other eye; grade 4, less
than 25% of ocular movement compared with the other
eye.11,12 Diplopia was also classified into five grades as follows: grade 0, no diplopia; grade 1, diplopia above 60 degrees; grade 2, diplopia above 45 degrees; grade 3, diplopia
above 30 degrees; grade 4, diplopia on central gaze. Lower
lid retraction was followed up during the period by using
marginal reflex distance2 (MRD2) for quantitative analysis.
Lower lid retraction was defined as the sclera shown over
the lower lid or MRD2 over 6 mm. The decision of 6 mm was
based on the average MRD2 value of 4.60.7 mm in the
Korean population.13 Because MRD2 was not measured before the surgery owing to edema and bleeding, it was measured only after the surgery and during the follow-up period.
Lower lid ectropion was defined as visible retraction of the
lid margin.
Chi-square test and independent t-test using SPSS version 17.0 (SPSS Inc., Chicago, IL, USA) were performed to
compare the results between groups. p values less than
0.05 were considered statistically significant.
TABLE 1. Demographics and characteristics of patients who underwent orbital wall reconstruction with transconjunctival approach
Number of patients
Age (years)
Sex (M/F)
Site of fracture (no.)
Medial wall
Inferior wall
Both
Size of fracture (no.)
Small (25%)
Medium (25-75%)
Large (75%)
Interval between injury and surgery (days)
HACMC* group
Control group
p value
47
28.8714.26
36/11
40
28.0510.85
32/8
0.936
0.783
10
22
15
8
17
15
0.673
0.541
0.951
4
13
30
15.378.01
2
13
25
12.767.57
0.87
0.963
0.782
0.472
*HACMC: the mixed solution of sodium hyaluronate and sodium carboxymethylcellulose (Guardix-sol ).
124
Byung Wan Kang, et al
RESULTS
In the HACMC group, 36 of 47 patients were male and
11 were female, and the mean patients age was 28.87
14.26 years. In the control group, 32 of 40 patients were
male and 8 were female, and the mean age was 28.0510.85
years. The average time between initial damage and surgery was 15.378.01 days in the HACMC group and
12.767.57 days in the control group. The distribution of
fracture location and size is demonstrated in Table 1. There
were no significant differences in gender, age, fracture location, fracture size, or period between initial fracture and
surgery between the two groups (p0.05).
There were no significant differences in diplopia, enophthalmos, or ocular movement impairment between the two
groups at 1 week and 1, 3, and 6 months after surgery.
MRD2 values for quantitative analysis of lower lid retraction were 4.530.55 mm at 1 week, 4.480.75 mm at
1 month, 4.680.83 mm at 3 months, and 4.730.86 mm at
6 months in the HACMC group. The respective values were
5.190.95 mm (p=0.04), 4.980.84 mm (p=0.04), 4.900.83
mm (p=0.78), and 4.860.81 mm (p=0.73) in the control
group. MRD2 values were significantly lower in the HACMC
group than in the control group at postoperative 1 week and
1 month (Fig. 1). Two patients showed lower lid ectropion
(5.0%) in the control group from 1 month after surgery,
which persisted until 6 months. However, no patients
showed lower lid ectropion in the HACMC group (p=0.08).
DISCUSSION
Transconjunctival, subtarsal, and subciliary approaches
are the major approach methods for orbital fracture surgery. Because the transconjunctival approach does not involve making an incision on the skin, lower lid ectropion
and edema occur less frequently. The transconjunctival approach is also commonly being used for its advantage of a
wide surgical view by performing canthotomy during the
surgery.14
Diplopia, enophthalmos, ocular deviation, infraorbital
nerve damage, occlusion of the lacrimal passage, dacryocystitis, pupil dilation, lymph edema, and lower lid retraction are well-known complications that occur after orbital wall fracture surgery. Lower lid ectropion or lower lid
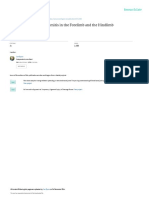
FIG. 1. Comparison of the amount of enophthalmos (A), limitation of motion (B), diplopia (C) and marginal reflex distance2 (D) between
the HACMC and control groups. *Significant at p0.05 compared with control group. HACMC: the mixed solution of sodium hyaluronate
and sodium carboxymethylcellulose (Guardix-sol).
125
Anti-adhesive Effect of HACMC
retraction is caused by contracture around the orbital septum and orbicularis oculi muscle. Also, it may occur after
combined sutures between the periosteum and orbital
septum. It also occurs when the lower lid is sutured on a
lower position than its original position after canthotomy.
Traction suture of the lower lid to pull it upward helps to
prevent lower lid complications. Also, steroid injection and
lower lid massages may be applied on the lesion after lower
lid retraction and ectropion occur.2
Compared with subciliary and subtarsal approaches, for
which the risk of lower lid ectropion exists owing to adhesion between the conjunctiva and fat as well as damage to
the orbicularis oculi muscles, the transconjunctival approach has a lower risk for lower lid complications because
only part of the inferior tarsal muscle and capsulopalpebral
fascia are involved.15 According to Mullins et al.16 in 2,086
patients who underwent orbital fracture repair, lower lid
ectropion developed in 4.7%, lower lid entropion in 0.5%,
lower lid edema in 1.1%, and hypertrophic scarring in 0.6%.
In the subciliary approach group, 14.0% of patients showed
lower lid ectropion, whereas only 1.5% of patients showed
lower lid ectropion in the transconjunctival approach
group. In the lower lid transdermal approach group, 1.5%
showed lower lid entropion, whereas 0.7% of patients
showed lower lid entropion in the transconjunctival approach group. Novelli et al.17 reported that 4 cases (7.1%)
out of 56 patients who underwent orbital fracture repair
showed complications after the surgery. Two patients (3.6%)
showed lower lid entropion and two patients (3.6%) showed
trichiasis.
Adhesion after surgery causes the damage site to release
vasoactive factors and causes accumulation of inflammatory cells, which thereby results in the formation of collagen-rich vessels and infiltration of fibroblasts, macrophages, and giant cells. The tissues are replaced with angiogranular tissues and the adhesion becomes permanent.18 These facts suggest that HACMC can be used to create a physical barrier to prevent the adhesion process. HA
is an anionic polysaccharide that is composed of D-glucuronic acid and N-acetyl-D-glucosamine. It has high viscosity
and elasticity that prevent adhesion by preventing fibrosis
of the tissue when sprayed on the tissue.19 However, HA
is limited as a physical barrier because the physiological
half-life of HA is only 1 to 3 days and it is easily decomposed
by hyaluronidase. On the other hand, CMC uses cellulose
from plants and is not easily disintegrated within the body.
Because of its ability to maintain a physical barrier within
the body tissues, a mixture of the two ingredients allows adequate prevention of postoperative adhesion.20,21 Several
reports have indicated that the use of HACMC solution
(Guardix-sol) in strabismus surgery can prevent adhesion after the surgery.6,8 The use of HACMC solution
(Guardix-sol) during dacryocystorhinostomy was reported
to effectively reduce occlusion and adhesion of the rhinostomy site.9 Furthermore, the use of Seprafilm, a film
structure of HACMC, significantly reduced the occurrence
of adhesion between the conjunctiva, periosteum, and mus126
cles after surgery and reduced the occurrence of adhesion
and ocular movement disorder after orbital fracture repair
surgery.7,10 However, Seprafilm was difficult to manipulate and reposition once it contacted the tissue.7 In contrast, Guardix-sol, a mixture solution of HA and CMC, is
easy to handle and does not cause problems such as displacement and distortion after injection in an area that requires flexibility and movability.8
To our knowledge, no study has been performed on the
use of anti-adhesives during wound repair of orbital wall
reconstruction. In the present study, we used Guardix-sol
during orbital wall reconstruction by the transconjunctival
approach to evaluate the anti-adhesive effects of the solution after the surgery. There were no significant differences in enophthalmos, ocular movement impairment, or
diplopia between the HACMC and control groups. No lower
lid ectropion was found in the HACMC group, whereas 2
cases of lower lid ectropion (5.0%) were found in the control
group after the first month. Although there were no statistically significant differences in MRD2 values between
the two groups between 3 and 6 months after the operation,
MRD2 values were significantly lower in the HACMC group
than in the control group at postoperative 1 week and 1
month. This may have been due to the anti-adhesive effect
of HACMC, which can form a temporary physical barrier
and hence decrease adhesion during the early postoperative period.8 The limitations of this study include a small
sample size and limited follow-up period.
In conclusion, HACMC can be used as a supplementary
agent during orbital wall reconstruction by the transconjunctival approach to reduce early postoperative
adhesion. The use of HACMC seems to reduce the complications related to eyelids such as lower lid ectropion when
contracture around the orbicularis oculi muscle and orbital
septum is expected.
REFERENCES
1. Rhee JS, Lynch J, Loehrl TA. Intranasal endoscopy-assisted repair of medial orbital wall fractures. Arch Facial Plast Surg 2000;
2:269-73.
2. Westfall CT, Shore JW, Nunery WR, Hawes MJ, Yaremchuk MJ.
Operative complications of the transconjunctival inferior fornix
approach. Ophthalmology 1991;98:1525-8.
3. Beck DE, Cohen Z, Fleshman JW, Kaufman HS, van Goor H, Wolff
BG; Adhesion Study Group Steering Committee. A prospective,
randomized, multicenter, controlled study of the safety of Seprafilm adhesion barrier in abdominopelvic surgery of the intestine.
Dis Colon Rectum 2003;46:1310-9.
4. Kelekci S, Uygur D, Yilmaz B, Sut N, Yesildaglar N. Comparison
of human amniotic membrane and hyaluronate/carboxymethylcellulose membrane for prevention of adhesion formation in rats.
Arch Gynecol Obstet 2007;276:355-9.
5. Naito Y, Shin'oka T, Hibino N, Matsumura G, Kurosawa H. A novel method to reduce pericardial adhesion: a combination technique with hyaluronic acid biocompatible membrane. J Thorac
Cardiovasc Surg 2008;135:850-6.
Byung Wan Kang, et al
6. Yaacobi Y, Hamed LM, Kaul KS, Fanous MM. Reduction of postoperative adhesions secondary to strabismus surgery in rabbits.
Ophthalmic Surg 1992;23:123-8.
7. Ozkan SB, Kir E, Culhaci N, Dayanir V. The effect of Seprafilm
on adhesions in strabismus surgery-an experimental study. J
AAPOS 2004;8:46-9.
8. Kwon SW, Seo YW, Cho YA. Antiadhesive effect of the mixed solution of hyaluronate and sodium carboxymethylcellulose after
evaluation of surgical techniques and materials for reconstruction.
J Craniofac Surg 2010;21:1033-7.
15. Baumann A, Ewers R. Use of the preseptal transconjunctival approach in orbit reconstruction surgery. J Oral Maxillofac Surg
2001;59:287-91.
16. Mullins JB, Holds JB, Branham GH, Thomas JR. Complications
of the transconjunctival approach. A review of 400 cases. Arch
Otolaryngol Head Neck Surg 1997;123:385-8.
strabismus surgery. J Korean Ophthalmol Soc 2009;50:145-50.
17. Novelli G, Ferrari L, Sozzi D, Mazzoleni F, Bozzetti A. Transcon-
9. Park JW, Park HY, Yoon KC. Clinical effect of the mixed solution
junctival approach in orbital traumatology: a review of 56 cases.
of sodium hyaluronate and sodium carboxymethylcellulose after
endonasal dacryocystorhinostomy. J Korean Ophthalmol Soc
2010;51:795-801.
10. Taban M, Nakra T, Mancini R, Douglas RS, Goldberg RA. Orbital
wall fracture repair using Seprafilm. Ophthal Plast Reconstr
Surg 2009;25:211-4.
11. Bansagi ZC, Meyer DR. Internal orbital fractures in the pediatric
age group: characterization and management. Ophthalmology
2000;107:829-36.
12. Yang HW, Bae JH, Lee HC. The postoperative recovery of ocular
motility in pediatric blow-out fracture. J Korean Ophthalmol Soc
2003;44:259-64.
J Craniomaxillofac Surg 2011;39:266-70.
18. Hellebrekers BW, Trimbos-Kemper TC, Trimbos JB, Emeis JJ,
Kooistra T. Use of fibrinolytic agents in the prevention of postoperative adhesion formation. Fertil Steril 2000;74:203-12.
19. Kimmelman CP, Edelstein DR, Cheng HJ. Sepragel sinus
(hylan B) as a postsurgical dressing for endoscopic sinus surgery.
Otolaryngol Head Neck Surg 2001;125:603-8.
20. Gago LA, Saed GM, Chauhan S, Elhammady EF, Diamond MP.
Seprafilm (modified hyaluronic acid and carboxymethylcellulose) acts as a physical barrier. Fertil Steril 2003;80:612-6.
21. Oncel M, Remzi FH, Senagore AJ, Connor JT, Fazio VW. Comparison of a novel liquid (Adcon-P) and a sodium hyaluronate and car-
13. Moon CS, Moon SH, Jang JW. Topographic anatomic difference
boxymethylcellulose membrane (Seprafilm) in postsurgical ad-
of the eyelid according to age in Korean. J Korean Ophthalmol Soc
hesion formation in a murine model. Dis Colon Rectum 2003;46:
2003;44:1865-71.
187-91.
14. Nowinski D, Messo E, Hedlund A. Treatment of orbital fractures:
127
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Intussusception Among Japanese Children: An Epidemiologic Study Using An Administrative DatabaseDocument6 pagesIntussusception Among Japanese Children: An Epidemiologic Study Using An Administrative DatabaseCasey CameronNo ratings yet
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- 720109Document10 pages720109Casey CameronNo ratings yet
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- GlaukomDocument4 pagesGlaukomCasey CameronNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Entropion PDFDocument4 pagesEntropion PDFCasey CameronNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- 720109Document10 pages720109Casey CameronNo ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Drug Induced GlaukomDocument7 pagesDrug Induced GlaukomCasey CameronNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- 720109Document10 pages720109Casey CameronNo ratings yet
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Entropion PDFDocument4 pagesEntropion PDFCasey CameronNo ratings yet
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Summary of Bali SDG WorkshopDocument26 pagesSummary of Bali SDG WorkshopCasey CameronNo ratings yet
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- Health in The Sustainable Development Goals: Ready For A Paradigm Shift?Document8 pagesHealth in The Sustainable Development Goals: Ready For A Paradigm Shift?Casey CameronNo ratings yet
- A Human Rights Approach To Data Disaggregation To Leave No One BehindDocument4 pagesA Human Rights Approach To Data Disaggregation To Leave No One BehindCasey CameronNo ratings yet
- JNC 7 Report Guidelines for High Blood PressureDocument52 pagesJNC 7 Report Guidelines for High Blood PressurepatriciajesikaNo ratings yet
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Guide to Recovery at SeaDocument21 pagesGuide to Recovery at SeaRihardsNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- GL-PHYS-7 Total Knee ReplacementDocument8 pagesGL-PHYS-7 Total Knee Replacementandrei_costeaNo ratings yet
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hds HDSX UL Burner Manual, 9-14Document56 pagesHds HDSX UL Burner Manual, 9-14kosmc123No ratings yet
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Snapping Knee Caused by The Gracilis Tendon: A Case Report With An Anatomical StudyDocument5 pagesSnapping Knee Caused by The Gracilis Tendon: A Case Report With An Anatomical StudyDavid BertossiNo ratings yet
- RICHARD F. BAXTER-Pocket Guide To Musculoskeletal AssessmentDocument104 pagesRICHARD F. BAXTER-Pocket Guide To Musculoskeletal Assessmentmaitre1959100% (4)
- Toolbox Talk - Manual HandlingDocument1 pageToolbox Talk - Manual HandlingKashif ImranNo ratings yet
- Anatomy State Exam1Document12 pagesAnatomy State Exam1Manisanthosh KumarNo ratings yet
- HDPE Pipe Installation GuideDocument48 pagesHDPE Pipe Installation GuideAkhil Syamkumar86% (7)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Redefining Hand Protection: Protective Industrial Products, IncDocument12 pagesRedefining Hand Protection: Protective Industrial Products, InceffendiNo ratings yet
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- Walcott, Niecko Ortago V Clayton, Lloyd and Crooks, Jasmine - Jamaican Case On NegligenceDocument16 pagesWalcott, Niecko Ortago V Clayton, Lloyd and Crooks, Jasmine - Jamaican Case On NegligenceKhome' WoodNo ratings yet
- 5 6228562040810636286sjDocument202 pages5 6228562040810636286sjvenkatNo ratings yet
- Muscle IdentificationDocument7 pagesMuscle Identificationhakdog hakdogNo ratings yet
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- DAMS CBT 15 Oct 2017 1Document121 pagesDAMS CBT 15 Oct 2017 1ReekBhattacharya100% (1)
- CavernCrawl 2.0Document26 pagesCavernCrawl 2.0Chris T.No ratings yet
- Are Employers Responsible For Employees' Negligence?Document7 pagesAre Employers Responsible For Employees' Negligence?Jason ItkinNo ratings yet
- Hydrotherap Y: Anna Ria R. Balaladia, PTRPDocument20 pagesHydrotherap Y: Anna Ria R. Balaladia, PTRPFloriza de LeonNo ratings yet
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Take The Ice by Bell A Marie 117 CompleteDocument644 pagesTake The Ice by Bell A Marie 117 CompleteDyan Angelica67% (3)
- Esd Esd9b5.0st5g 5v 1a Sod923 RohsDocument4 pagesEsd Esd9b5.0st5g 5v 1a Sod923 RohsBLUEE009No ratings yet
- Eliseo Araneta vs. CADocument2 pagesEliseo Araneta vs. CAJnacitaNo ratings yet
- Chapter 3Document12 pagesChapter 3Deolita BadiangNo ratings yet
- Cooling Burn WuondsDocument6 pagesCooling Burn Wuondsapi-3801331No ratings yet
- English Vocabulary TestDocument6 pagesEnglish Vocabulary TestBasil AngelisNo ratings yet
- Cranial Nerve: Dr. Dian Prasetyo Wibisono, M.SCDocument49 pagesCranial Nerve: Dr. Dian Prasetyo Wibisono, M.SCgeneNo ratings yet
- Proximal Suspensory Desmitis in The Forelimb and TDocument7 pagesProximal Suspensory Desmitis in The Forelimb and TSam LoretNo ratings yet
- 10 Guitar ErgonomicsDocument5 pages10 Guitar ErgonomicsMayara FlossNo ratings yet
- Pediatric Medical DevicesDocument25 pagesPediatric Medical DevicesDuck Mann-ConsulNo ratings yet
- Introduction To Ergonomics: 10-Hour General Industry Outreach TrainingDocument57 pagesIntroduction To Ergonomics: 10-Hour General Industry Outreach TrainingMau MendietaNo ratings yet
- Steel Erection 1Document154 pagesSteel Erection 1Ranjit KumarNo ratings yet
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Shimano Brake System PDFDocument1 pageShimano Brake System PDFJose Luis GutierrezNo ratings yet
- Damage Control Management in The Polytra PDFDocument462 pagesDamage Control Management in The Polytra PDFFlipNo ratings yet