Professional Documents
Culture Documents
American Family Physician
Uploaded by
Mahardika PutraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
American Family Physician
Uploaded by
Mahardika PutraCopyright:
Available Formats
November 30, 2009 Recommendations for primary care clinicians regarding the diagnosis
and treatment of nephrotic syndrome in adults are reviewed in the November 15 issue of the
American Family Physician.
"In nephrotic syndrome, a variety of disorders cause proteinuria, often resulting in marked
edema and hypoalbuminemia," write Charles Kodner, MD, from the University of Louisville
School of Medicine in Louisville, Kentucky. "Hyperlipidemia is a common associated
finding. Family physicians may encounter persons with nephrotic syndrome from primary
(idiopathic) renal disease or a number of secondary causes, and should initiate appropriate
diagnostic workup and medical management pending specialist consultation."
Nephrotic syndrome may be classified as primary (or idiopathic) renal disease, or it may be
secondary to various causes. The most common primary causes in adults are focal segmental
glomerulosclerosis and membranous nephropathy.
Focal segmental glomerulosclerosis accounts for approximately one third of cases of primary
nephrotic syndrome and for approximately 3.3% of new cases of end-stage renal disease, and
it is the leading cause of idiopathic nephrotic syndrome in adults. It is characterized by
sclerosis and hyalinosis of segments of less than 50% of all glomeruli on electron
microscopic studies. Clinical features may include hypertension, renal insufficiency, and
hematuria.
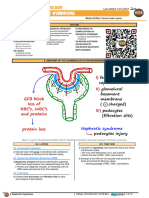
In membranous nephropathy, electron microscopic study reveals thickening of the glomerular
basement membrane, and immunofluorescent staining shows immunoglobulin G and C3
deposits. This form of nephrotic syndrome, which also accounts for approximately one third
of cases of primary nephrotic syndrome, is most often diagnosed at ages 30 to 50 years.
Patients may have microscopic hematuria, and roughly one quarter have systemic lupus
erythematosus, hepatitis B, malignant disease, drug-induced nephrotic syndrome, or other
underlying systemic disease.
Another form of primary nephrotic syndrome is minimal-change disease, which together with
immunoglobulin A nephropathy is responsible for approximately one quarter of cases of
idiopathic nephrotic syndrome. It is diagnosed from normal-appearing glomeruli on renal
biopsy microscopic examination with effacement of foot processes on electron microscopic
studies. After upper respiratory tract infection or immunization, relatively mild or benign
cases of minimal-change disease may develop.
Secondary causes of nephrotic syndrome include diabetes mellitus, which is the most
common secondary cause. Other causes are systemic lupus erythematosus, hepatitis B or C,
use of nonsteroidal anti-inflammatory drugs, minimal-change disease, amyloidosis, multiple
myeloma, HIV, or preeclampsia.
Typical presenting features of nephrotic syndrome are marked edema, proteinuria,
hypoalbuminemia, and usually hyperlipidemia.
Possible complications of nephrotic syndrome are venous thromboembolism. Although acute
renal failure and serious bacterial infection may occur, they are much less common.
To date, there are no established guidelines regarding diagnostic evaluation of patients with
nephrotic syndrome. To diagnose specific disorders, blood tests should be used selectively,
but a broad-ranging or unguided workup is not recommended. Imaging studies are seldom
necessary. In some cases, however, renal biopsy may help confirm an underlying disease or
identify idiopathic disease that has a greater probability of responding to corticosteroids.
Professional organizations have also not yet issued recommendations for treatment of
nephrotic syndrome. Most patients should be treated with fluid and sodium restriction, oral or
intravenous diuretics, and angiotensin-converting enzyme inhibitors.
"Diuretics are the mainstay of medical management; however, there is no evidence to guide
drug selection or dosage," Dr. Kodner writes. "Based on expert opinion, diuresis should aim
for a target weight loss of 1 to 2 lb (0.5 to 1 kg) per day to avoid acute renal failure or
electrolyte disorders. Loop diuretics, such as furosemide (Lasix) or bumetanide, are most
commonly used."
In persons with nephrotic syndrome, angiotensin-converting enzyme inhibitors have been
shown to decrease proteinuria and lower the risk for progression to renal disease.
Although corticosteroid treatment may benefit some adults with nephrotic syndrome,
research evidence supporting this therapy is limited. At present, intravenous albumin,
prophylactic antibiotics, and prophylactic anticoagulation are not advised.
Key Recommendations
Key clinical recommendations for practice, and their accompanying level of evidence rating,
are as follows:
To evaluate the extent of proteinuria, persons with nephrotic syndrome should
undergo measurement of random urine protein-to-creatinine ratio (level of evidence,
C).
Although renal biopsy may help guide diagnosis and management in selected patients,
it is not recommended for all persons with nephrotic syndrome (level of evidence, C).
Most persons with nephrotic syndrome should be treated with sodium and fluid
restriction and high-dose diuretic therapy (level of evidence, C).
Most persons with nephrotic syndrome should be treated with angiotensin-converting
enzyme inhibitors (level of evidence, C).
Despite the lack of evidence that corticosteroid treatment has any proven therapeutic
benefit for nephrotic syndrome, some physicians recommend it for persons who are
refractory to conservative management (level of evidence, C).
"In most cases, family physicians should consult specialists in renal medicine about the need
for renal biopsy in individual patients," Dr. Kodner concludes.
"There are no clinical guidelines and few high-quality studies on the management of
nephrotic syndrome in adults. Recommendations are based primarily on early case series,
other observational studies, and expert opinion."
Dr. Kodner has disclosed no relevant financial relationships.
Laurie Barclay, MD
November 30, 2009
http://www.medscape.com/viewarticle/713110 16/6/2015
You might also like
- Management of Patients With Nephrotic Syndrome: Sophie de Seigneux, Pierre-Yves MartinDocument7 pagesManagement of Patients With Nephrotic Syndrome: Sophie de Seigneux, Pierre-Yves MartinGarit Hapsari KiranaNo ratings yet
- Nephrotic SyndromeDocument8 pagesNephrotic SyndromeKanmani AniNo ratings yet
- Diagnosis and Management of Nephrotic Syndrome in PDFDocument15 pagesDiagnosis and Management of Nephrotic Syndrome in PDFMichael PutrantoNo ratings yet
- Nephroticsyndrome: Seth Anthony Politano,, Gates B. Colbert,, Nida HamiduzzamanDocument17 pagesNephroticsyndrome: Seth Anthony Politano,, Gates B. Colbert,, Nida HamiduzzamanERICKNo ratings yet
- Overview of Heavy Proteinuria and The Nephrotic Syndrome - UpToDateDocument37 pagesOverview of Heavy Proteinuria and The Nephrotic Syndrome - UpToDateAdrian MoranNo ratings yet
- Nephrotic Syndrome-1Document21 pagesNephrotic Syndrome-1Wondimu EliasNo ratings yet
- AAFP Marzo 2016 Sindrome NefroticoDocument7 pagesAAFP Marzo 2016 Sindrome NefroticoAntonio MoncadaNo ratings yet
- Wa0011.Document180 pagesWa0011.Mohamed AbdelmoniemNo ratings yet
- Overview of Heavy Proteinuria and The Nephrotic Syndrome - UpToDateDocument34 pagesOverview of Heavy Proteinuria and The Nephrotic Syndrome - UpToDatechristian47No ratings yet
- Lecture Note On Renal Diseases For Medical Students - Nephrotic SyndromeDocument8 pagesLecture Note On Renal Diseases For Medical Students - Nephrotic SyndromeEsayas KebedeNo ratings yet
- SX Nefrotico 2014Document10 pagesSX Nefrotico 2014Nancy MoranchelNo ratings yet
- Nephrotic SyndromeDocument12 pagesNephrotic SyndromePutra Fatkhul Rizqi QoroidNo ratings yet
- Glomerular Disorders - Part I & Part II (ARI NOTES)Document144 pagesGlomerular Disorders - Part I & Part II (ARI NOTES)Laiba FatimaNo ratings yet
- Nephrotic Syndrome - Armando HasudunganDocument18 pagesNephrotic Syndrome - Armando HasudunganzahraaNo ratings yet
- Nephritis LupusDocument8 pagesNephritis LupusDioNo ratings yet
- GlomerulonephritisDocument46 pagesGlomerulonephritisvanessaNo ratings yet
- Lupus NephritisDocument3 pagesLupus NephritissobanNo ratings yet
- Emergent Management of Acute Glomerulonephritis - Overview, Emergency Department Care, ConsultationsDocument4 pagesEmergent Management of Acute Glomerulonephritis - Overview, Emergency Department Care, ConsultationsHafiz Maulana AhmadNo ratings yet
- Seminar On Nephrotic Syndrome: Medical Surgical NursingDocument15 pagesSeminar On Nephrotic Syndrome: Medical Surgical NursingGargi MP100% (1)
- Nephrotic Syndrome: Signs and SymptomsDocument7 pagesNephrotic Syndrome: Signs and SymptomsErika ManubayNo ratings yet
- IntroductionDocument4 pagesIntroductionCristina L. JaysonNo ratings yet
- Nephrotic Syndrome: BackgroundDocument25 pagesNephrotic Syndrome: BackgroundsDamnNo ratings yet
- Chronic Kidney DiseaseDocument54 pagesChronic Kidney DiseaseJosh Matthew RosalesNo ratings yet
- SNDocument7 pagesSNArdy Syahabuddin GofarNo ratings yet
- Nephrotic Syndrome Msn-3Document12 pagesNephrotic Syndrome Msn-3Bibi Renu100% (3)
- Lupus NephritisDocument29 pagesLupus NephritisMuhammad Julpian0% (1)
- Trad2 SolvedDocument4 pagesTrad2 SolvedIrina StoicaNo ratings yet
- Kidney DiseasesDocument22 pagesKidney Diseasesphoto copyhemnNo ratings yet
- 77 FullDocument6 pages77 FullRizkaNNatsirNo ratings yet
- ABC Acute Renal FailureDocument5 pagesABC Acute Renal FailureAngela CristinoNo ratings yet
- DN 8TH Sem Project FinalDocument30 pagesDN 8TH Sem Project FinalBhoj RajNo ratings yet
- Nephrotic SyndromeDocument29 pagesNephrotic SyndromeMusthafa Afif WardhanaNo ratings yet
- Universidad Privada San Juan Bautista: Escuela de Medicina HumanaDocument6 pagesUniversidad Privada San Juan Bautista: Escuela de Medicina HumanaKarolLeylaNo ratings yet
- The Treatment and Prognosis of Nephrotic Syndrome in The ElderlyDocument5 pagesThe Treatment and Prognosis of Nephrotic Syndrome in The ElderlysulemanbankerNo ratings yet
- Glomerulopatías PrimariasDocument8 pagesGlomerulopatías PrimariasGSENo ratings yet
- Nephrotic Syndrome in Children-LectureDocument52 pagesNephrotic Syndrome in Children-LectureLubinda SitaliNo ratings yet
- NEPHRITISDocument37 pagesNEPHRITISJay RathvaNo ratings yet
- A Case Report On Adult Onset of Nephrotic Syndrome: Research ArticleDocument2 pagesA Case Report On Adult Onset of Nephrotic Syndrome: Research ArticleTTNo ratings yet
- Sindrom NefrotikDocument22 pagesSindrom NefrotikGyta Apriati100% (1)
- Nephrology Notes 2015Document81 pagesNephrology Notes 2015Mahmoud Hussien100% (1)
- Diabetic NephropathyDocument5 pagesDiabetic NephropathyZiedTriki100% (1)
- Medicina 55 00365Document21 pagesMedicina 55 00365Sundas EjazNo ratings yet
- Azotemia - StatPearls - NCBI BookshelfDocument1 pageAzotemia - StatPearls - NCBI Bookshelfmellinda anastasyaNo ratings yet
- GlomerulonephritisDocument4 pagesGlomerulonephritisEmilene ZaragozaNo ratings yet
- Nephrotic Syndrome ComplicationsDocument16 pagesNephrotic Syndrome ComplicationsBeatri AyuzaNo ratings yet
- Case Study yDocument23 pagesCase Study yRaidis PangilinanNo ratings yet
- Eko 3 - Nephrotic Syndrome With PolycythemiaDocument10 pagesEko 3 - Nephrotic Syndrome With PolycythemiaAndri Baftahul KhairiNo ratings yet
- LP Sindrom NefrotikDocument10 pagesLP Sindrom Nefrotikvictor zhefaNo ratings yet
- Paediatric Nephrotic SyndromeDocument44 pagesPaediatric Nephrotic SyndromeAlvin OmondiNo ratings yet
- What Causes Glomerular DiseaseDocument5 pagesWhat Causes Glomerular DiseaseAswin AgusNo ratings yet
- Ni Hms 933167Document30 pagesNi Hms 933167sung rae rimNo ratings yet
- Epidemiology and Classification of Diabetic Neuropathy - UpToDateDocument11 pagesEpidemiology and Classification of Diabetic Neuropathy - UpToDatehochanh199xNo ratings yet
- Evaluation of Chronic Renal Disease, A Staged ApproachDocument8 pagesEvaluation of Chronic Renal Disease, A Staged Approachtaner_soysurenNo ratings yet
- Glomerulonefritis Primaria Medicine 2015Document6 pagesGlomerulonefritis Primaria Medicine 2015Francisco Rebollar GarduñoNo ratings yet
- Lupus NephritisDocument33 pagesLupus NephritisNi MoNo ratings yet
- Drug Induced NephrotoxicityDocument13 pagesDrug Induced NephrotoxicityAgnes BastonNo ratings yet
- Protein Uri ADocument13 pagesProtein Uri ARahma Cita HalidaNo ratings yet
- Pediatric NephroticDocument45 pagesPediatric NephroticMuhammad BilalNo ratings yet
- Jajan Tricks - Google SearchDocument1 pageJajan Tricks - Google SearchMahardika PutraNo ratings yet
- ScribdDocument1 pageScribdMahardika PutraNo ratings yet
- ScribdDocument1 pageScribdMahardika PutraNo ratings yet
- Vish ItnrDocument2 pagesVish ItnrMahardika PutraNo ratings yet
- PutriDocument1 pagePutriMahardika PutraNo ratings yet
- Presentation 1Document1 pagePresentation 1Mahardika PutraNo ratings yet
- Hep Education 101Document20 pagesHep Education 101Mahardika PutraNo ratings yet
- Booking Reference (PNR) : Passenger Type Passenger Name E-Ticket Number FF Number Special Request Meal PreferenceDocument1 pageBooking Reference (PNR) : Passenger Type Passenger Name E-Ticket Number FF Number Special Request Meal PreferenceMahardika PutraNo ratings yet
- Daftar Pustaka FixDocument1 pageDaftar Pustaka FixMahardika PutraNo ratings yet
- Longitudinal Course and Outcome of Chronic Insomnia in Hong Kong Chinese Children: A 5-Year Follow-Up Study of A Community-Based CohortDocument8 pagesLongitudinal Course and Outcome of Chronic Insomnia in Hong Kong Chinese Children: A 5-Year Follow-Up Study of A Community-Based CohortMahardika PutraNo ratings yet
- Nephrotic Syndrome Children PDFDocument11 pagesNephrotic Syndrome Children PDFesdl86No ratings yet
- KDIGO GD Membranous NephropathyDocument1 pageKDIGO GD Membranous NephropathyF AudreyNo ratings yet
- Nephrotic Syndrome Treatment & Management - Approach Considerations, Acute NephroDocument5 pagesNephrotic Syndrome Treatment & Management - Approach Considerations, Acute NephroErvirson Jair Cañon AbrilNo ratings yet
- Kidney Biopsy Finding of The Glomeruli - SUN 2019Document78 pagesKidney Biopsy Finding of The Glomeruli - SUN 2019Galih AryyagunawanNo ratings yet
- Nephrotic Syndrome-1Document21 pagesNephrotic Syndrome-1Wondimu EliasNo ratings yet
- KDIGO 2021 Glomerular Diseases GuidelineDocument276 pagesKDIGO 2021 Glomerular Diseases GuidelineAmbulatório Dieta Cetogênica HUBNo ratings yet
- Ponticelli Treatment V 1.1 11.2019 WebDocument12 pagesPonticelli Treatment V 1.1 11.2019 WebDiddi SkittlessNo ratings yet
- Nephrotic and Nephritic Syndrome - 2008Document65 pagesNephrotic and Nephritic Syndrome - 2008rikasusanti101001201No ratings yet
- Enfermedad GlomerularDocument23 pagesEnfermedad GlomerularAlejandro beuses morrNo ratings yet
- Renal Notes Step 2ckDocument34 pagesRenal Notes Step 2cksamreen100% (1)
- Etiology, Clinical Manifestations, and Diagnosis of Nephrotic Syndrome in Children - UpToDateDocument18 pagesEtiology, Clinical Manifestations, and Diagnosis of Nephrotic Syndrome in Children - UpToDateAngga Julyananda PradanaNo ratings yet
- Renal Pathology - 012) Nephrotic Syndrome (Notes)Document10 pagesRenal Pathology - 012) Nephrotic Syndrome (Notes)hasanatiya41No ratings yet
- Nephrology TestDocument112 pagesNephrology TestRapid Medicine50% (2)
- Treatment of Idiopathic Nephrotic Syndrome in Children - UpToDateDocument31 pagesTreatment of Idiopathic Nephrotic Syndrome in Children - UpToDateChetra ColaNo ratings yet
- AUBF Group 1 Chapter 8Document12 pagesAUBF Group 1 Chapter 8Gerald John PazNo ratings yet
- Glomerular Disease - Evaluation and Differential Diagnosis in Adults - UpToDateDocument23 pagesGlomerular Disease - Evaluation and Differential Diagnosis in Adults - UpToDateRaiya MallickNo ratings yet
- Nbme Form 7 AnswersDocument34 pagesNbme Form 7 AnswersMary Choo Spencer100% (3)
- Renal System and Its Disorders: Key PointsDocument19 pagesRenal System and Its Disorders: Key PointsskNo ratings yet
- Nephrotic Nephritic SyndromeDocument15 pagesNephrotic Nephritic Syndromeshefalika mandremNo ratings yet
- MCQDocument40 pagesMCQLuthie Singh100% (2)
- Management of Membranous Nephropathy After Mentor: Claire Trivin-Avillach and Laurence H. Beck JRDocument3 pagesManagement of Membranous Nephropathy After Mentor: Claire Trivin-Avillach and Laurence H. Beck JRCarolina CastroNo ratings yet
- NEPHSAP - Renal Pathology CasesDocument152 pagesNEPHSAP - Renal Pathology CasesMarwan Abu Sneineh67% (3)
- DK IKA 1 - Ogie RevDocument193 pagesDK IKA 1 - Ogie RevhariogieNo ratings yet
- Steroid Resistant Nephrotic SyndromeDocument72 pagesSteroid Resistant Nephrotic SyndromeMonika Angra100% (1)
- อ.บัญชา Glomerular - disease - handoutพี่ดาวDocument142 pagesอ.บัญชา Glomerular - disease - handoutพี่ดาวNitaan TangsritrakulNo ratings yet
- Nephrotic SyndromeDocument23 pagesNephrotic SyndromeamlymarsNo ratings yet
- Congenital Nephrotic SyndromeDocument44 pagesCongenital Nephrotic Syndromeaad81kolrenmed50% (2)
- Overview of Heavy Proteinuria and The Nephrotic Syndrome - UpToDateDocument34 pagesOverview of Heavy Proteinuria and The Nephrotic Syndrome - UpToDatechristian47No ratings yet
- Nephrotic Syndrome in Adults: Acute Medicine 2018 17 (1) : 36-43 36Document8 pagesNephrotic Syndrome in Adults: Acute Medicine 2018 17 (1) : 36-43 36Deddy TriwijayaNo ratings yet
- KDIGO 2012 GN Guideline EnglishDocument143 pagesKDIGO 2012 GN Guideline EnglishSelena GajićNo ratings yet