Professional Documents
Culture Documents
Acute Upper Abdominal Pain: Step-By-Step Assessment
Uploaded by
zafar_183250 ratings0% found this document useful (0 votes)
10 views1 pageusmle
Original Title
mcleaod 49
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentusmle
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
10 views1 pageAcute Upper Abdominal Pain: Step-By-Step Assessment
Uploaded by
zafar_18325usmle
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 1
4
Abdominal pain
Acute upper abdominal pain: step-by-step assessment
and look for evidence of complications, e.g.
infection, particularly in patients with persistent organ failure or a systemic inflammatory response.
4
Jaundice?
Organise an urgent abdominal USS for all
patients with acute upper abdominal pain
and jaundice to look for evidence of biliary
obstruction or hepatitis.
Assume biliary sepsis, at least initially, if
the patient is unwell with high fever
rigors or cholestatic jaundice (p. 177); give
IV antibiotics and, if the USS confirms a
dilated CBD, refer immediately to surgery
for biliary decompression.
Assess as described in Chapter 19 if
there are clinical or USS features of acute
hepatitis.
5
Inflammatory response?
At this stage, use the presence or absence of
a systemic inflammatory response (see Box
4.1) to narrow the differential diagnosis.
Arrange prompt abdominal USS to
confirm or exclude acute cholecystitis in
any patient with inflammatory features
accompanied by any of the following:
localised RUQ pain
direct tenderness to palpation in the
RUQ
positive Murphys sign (sudden arrest
of inspiration while taking a deep
breath during palpation of the
gallbladder).
In the absence of acute cholecystitis, the
USS may reveal an alternative cause for the
presentation, e.g. pyelonephritis, hepatitis,
subphrenic collection.
If none of these features is present, consider alternative disorders:
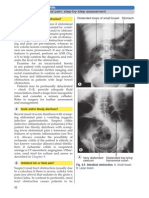
basal pneumonia if there is clinical or
CXR evidence of basal consolidation
(see Figs 12.3 and 12.4, pp. 116 and 117),
especially if accompanied by productive
cough or dyspnoea
gastroenteritis in patients with an acute
vomiting illness and no abdominal
guarding or rigidity (reassess regularly)
36
acute pyelonephritis if urinalysis is
positive for leucocytes/nitrites.
Otherwise, consider USS/CT to exclude
atypical presentations of acute appendicitis/
pancreatitis/cholecystitis, Crohns disease
or other acute inflammatory pathology.
6
Characteristics of biliary colic?
Biliary colic is a common cause of acute
severe upper abdominal pain in patients
who are otherwise well and do not exhi
bit evidence of a systemic inflammatory
response. Abdominal USS can assist the
diagnosis by demonstrating the presence
of gallstones. However, asymptomatic
gallstones are very common and so the
history is critical to making an accurate
diagnosis.
Look for the following suggestive
features:
onset of pain a few hours after a meal
(may waken the patient from sleep)
duration 6 hours followed by complete
resolution of symptoms
the main site is the epigastrium or RUQ
radiation to the back
constant, vague, aching or cramping
discomfort (it is not, strictly speaking,
colicky)
history of previous similar episodes.
Arrange abdominal USS only in patients
with a suggestive history. If the pain has
settled and LFTs are not deranged, USS
may be performed in the outpatient
department.
7
Consider other causes observation/
surgical review if any concern
Systemically well patients with an acute
vomiting illness and recent infectious
contact or ingestion of suspicious foodstuffs
are likely to have gastroenteritis.
Suspect acute gastritis if the patient
reports new-onset gnawing, burning or
vague epigastric discomfort mild tenderness especially if this is associated with
dyspeptic symptoms e.g. nausea, belching,
heartburn, or a history of recent alcohol
excess/NSAID use; consider peptic ulcer
You might also like
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Akut AbdomenDocument38 pagesAkut AbdomenAprianNo ratings yet
- PROBLEM 3 GIT Jeffrey 405170048Document162 pagesPROBLEM 3 GIT Jeffrey 405170048Mohammad Jofa Rachman PNo ratings yet
- Acute Abdominal-Wps OfficeDocument26 pagesAcute Abdominal-Wps OfficeAbhash MishraNo ratings yet
- The Acute AbdomenDocument7 pagesThe Acute AbdomenMarwan M.No ratings yet
- Acute Abdomen: Preseptor: Dr. Liza Nursanty, SPB, Mkes, FinacsDocument39 pagesAcute Abdomen: Preseptor: Dr. Liza Nursanty, SPB, Mkes, FinacsHarum Binar MetrikasantiNo ratings yet
- Acute Abdominal PainDocument5 pagesAcute Abdominal PainLM Mys100% (1)
- Acute AbdomenDocument36 pagesAcute AbdomenAdriani NadhirahNo ratings yet
- Intestinal Perforation Clinical Presentation: HistoryDocument2 pagesIntestinal Perforation Clinical Presentation: HistorypricillyaNo ratings yet
- Acute Abdomen Utk SekarwangiDocument33 pagesAcute Abdomen Utk SekarwangiIca Trianjani SetyaningrumNo ratings yet
- Abdominal PainDocument12 pagesAbdominal PainGeeza Gem VicencioNo ratings yet
- Acute Abdomen, Nyeri Akut AbdomenDocument35 pagesAcute Abdomen, Nyeri Akut AbdomenYanuar Yudha SudrajatNo ratings yet
- Acut e Abdome NDocument58 pagesAcut e Abdome NArchana MoreyNo ratings yet
- HP Nov02 PainDocument6 pagesHP Nov02 PainSampath GoudNo ratings yet
- CHOLECYSTITISDocument5 pagesCHOLECYSTITISRACHELLE ANNE L LUISNo ratings yet
- Acute AbdomenDocument7 pagesAcute AbdomenStanley MwendaNo ratings yet
- Acute Abdomen - Shaking Down The SuspectsDocument11 pagesAcute Abdomen - Shaking Down The SuspectsKeldon15100% (1)
- Acute AbdomenDocument53 pagesAcute AbdomenMahdi DiabNo ratings yet
- Dyspepsia GastritisDocument80 pagesDyspepsia GastritisSoumya Ranjan PandaNo ratings yet
- ACUTE ABDOMEN Low Abdominal PainDocument8 pagesACUTE ABDOMEN Low Abdominal PainSaputra Tri NopiantoNo ratings yet
- Acute AbdomenDocument11 pagesAcute AbdomenRenad AleneziNo ratings yet
- Abdominal Pain PDFDocument6 pagesAbdominal Pain PDFRandy MusashiNo ratings yet
- CardiologyDocument19 pagesCardiologyshadabNo ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Case Study For Diagnosis of DiseaseDocument29 pagesCase Study For Diagnosis of DiseaseFirifan DiribaNo ratings yet
- Acute AbdomenDocument66 pagesAcute AbdomenFahid MalikNo ratings yet
- Acute Appendicitis: History and ExaminationDocument6 pagesAcute Appendicitis: History and ExaminationPraktek Dokter Umum drjosefdrelsyNo ratings yet
- GIS-K-25 Acute Appendicitis Appendiceal Mass / AbscessDocument24 pagesGIS-K-25 Acute Appendicitis Appendiceal Mass / AbscessYasmine Fitrina SiregarNo ratings yet
- Acute Abdomen: The "Black Hole" of MedicineDocument97 pagesAcute Abdomen: The "Black Hole" of Medicineedward iskandarNo ratings yet
- Acute Abdomen - StatPearls - NCBI BookshelfDocument7 pagesAcute Abdomen - StatPearls - NCBI BookshelfAinani TajrianNo ratings yet
- Abdominal Pain - Royal Children HospitalDocument4 pagesAbdominal Pain - Royal Children HospitalMehrdad IraniNo ratings yet
- Necrotizing Enterocolitis ProtocolDocument3 pagesNecrotizing Enterocolitis Protocoleddy riachyNo ratings yet
- L 8 Acute AbdomenDocument53 pagesL 8 Acute Abdomenfdyrrbfb2nNo ratings yet
- PROBLEM 4 GIT Group 11Document118 pagesPROBLEM 4 GIT Group 11Shitta InayahNo ratings yet
- Acute AbdomenDocument24 pagesAcute AbdomenGrace SimmonsNo ratings yet
- Acute Abdomen &peritonitisDocument63 pagesAcute Abdomen &peritonitisSamar Ahmad100% (1)
- Acute Abdomen - StatPearls - NCBI BookshelfDocument6 pagesAcute Abdomen - StatPearls - NCBI Bookshelfimehap033No ratings yet
- Examination of Intestinal Obstruction, Acute Abdomen and Acute Appendicitis - Eugh & BwembyaDocument29 pagesExamination of Intestinal Obstruction, Acute Abdomen and Acute Appendicitis - Eugh & BwembyaForeighn97No ratings yet
- 0 Bxzs HMZydz R5 C Ed OSl B2 TK 9 LWUkDocument10 pages0 Bxzs HMZydz R5 C Ed OSl B2 TK 9 LWUkTricia LlorinNo ratings yet
- Abdominal PainDocument39 pagesAbdominal PainIsma Resti PratiwiNo ratings yet
- Abdominal Distension: Common Causes: - (Five F'S) 1. 2. 3. 4. 5. History of Present Illness 1Document3 pagesAbdominal Distension: Common Causes: - (Five F'S) 1. 2. 3. 4. 5. History of Present Illness 1Maxamed DananNo ratings yet
- History PerformaDocument5 pagesHistory PerformaHariharan NarendranNo ratings yet
- Acute Abdominal Pain: Presented by Dr. Kolahdouzan Thoracic Surgen Alzahra HospitalDocument77 pagesAcute Abdominal Pain: Presented by Dr. Kolahdouzan Thoracic Surgen Alzahra HospitalGraceline Margaretha Marsintauly SianiparNo ratings yet
- Acute AbdomenDocument29 pagesAcute AbdomenUmar AzlanNo ratings yet
- Acute AbdomenDocument54 pagesAcute AbdomenMoses ChatipaNo ratings yet
- SESSION 1 - Acute AbdomenDocument33 pagesSESSION 1 - Acute AbdomenLinux KaikaNo ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Patient With RIF Pain: Differentials & ManagementDocument4 pagesPatient With RIF Pain: Differentials & ManagementgeotrophNo ratings yet
- ABDOMEN Agudo EnfrentamientoDocument22 pagesABDOMEN Agudo Enfrentamientonicositja_vangoh91No ratings yet
- Abdominal Pain: James S Newman, M.D. The University of Texas Medical BranchDocument27 pagesAbdominal Pain: James S Newman, M.D. The University of Texas Medical BranchYudiese YouNo ratings yet
- Presented by Dr. Ayalew ZDocument35 pagesPresented by Dr. Ayalew Zyared getachewNo ratings yet
- 5 Mesenteric IschemiaDocument39 pages5 Mesenteric IschemiaFahd Abdullah Al-refaiNo ratings yet
- Evaluation of Acute AbdomenDocument38 pagesEvaluation of Acute Abdomenأبو عبيدةNo ratings yet
- Abdome AgudoDocument63 pagesAbdome AgudoAnne Caroline De Morais AlvesNo ratings yet
- Abdomen Agudo en Enfermedades No QuirurgicasDocument5 pagesAbdomen Agudo en Enfermedades No QuirurgicasGonzalez ByronNo ratings yet
- Acute Abdomen WebinarDocument64 pagesAcute Abdomen WebinaratinafansifNo ratings yet
- Acute Abdominal Pain: OverviewDocument1 pageAcute Abdominal Pain: Overviewzafar_18325No ratings yet
- Appendicitis CaseDocument8 pagesAppendicitis CaseStarr NewmanNo ratings yet
- Ulcerative Colitis, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandUlcerative Colitis, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- A Simple Guide to Gastritis and Related ConditionsFrom EverandA Simple Guide to Gastritis and Related ConditionsRating: 4.5 out of 5 stars4.5/5 (3)
- PMDCDocument5 pagesPMDCzafar_18325No ratings yet
- The Diagnostic ProcessDocument1 pageThe Diagnostic Processzafar_18325No ratings yet
- Assessment of Common Presenting ProblemsDocument1 pageAssessment of Common Presenting Problemszafar_18325No ratings yet
- Assessing Patients: A Practical Guide: The Clinical ExaminationDocument1 pageAssessing Patients: A Practical Guide: The Clinical Examinationzafar_18325No ratings yet
- The Diagnostic Process: See Further Assessment of Chronic Liver Disease (P. 181) YesDocument1 pageThe Diagnostic Process: See Further Assessment of Chronic Liver Disease (P. 181) Yeszafar_18325No ratings yet
- Mcleaod 38Document1 pageMcleaod 38zafar_18325No ratings yet
- Mcleaod 39Document1 pageMcleaod 39zafar_18325No ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Box 4.1 Indicators of Systemic Inflammation: Differential DiagnosisDocument1 pageBox 4.1 Indicators of Systemic Inflammation: Differential Diagnosiszafar_18325No ratings yet
- Differential Diagnosis: Abdominal PainDocument1 pageDifferential Diagnosis: Abdominal Painzafar_18325No ratings yet
- Mesenteric Ischaemia Renal Tract Disorders: Non-Ulcer DyspepsiaDocument1 pageMesenteric Ischaemia Renal Tract Disorders: Non-Ulcer Dyspepsiazafar_18325No ratings yet
- Acute Abdominal Pain: OverviewDocument1 pageAcute Abdominal Pain: Overviewzafar_18325No ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- General Surgery Paper I TosDocument2 pagesGeneral Surgery Paper I Toszafar_18325No ratings yet
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Medicine MCQDocument9 pagesMedicine MCQemmaazizNo ratings yet
- Acute Upper Abdominal Pain: OverviewDocument1 pageAcute Upper Abdominal Pain: Overviewzafar_18325No ratings yet
- Laurence Hunter Helen Leng Caroline Jones Miles Hitchen Jennifer Rose AntbitsDocument1 pageLaurence Hunter Helen Leng Caroline Jones Miles Hitchen Jennifer Rose Antbitszafar_18325No ratings yet
- Cost Estimate TemplateDocument2 pagesCost Estimate Templatezafar_18325No ratings yet
- 02 EyeanatomyDocument12 pages02 Eyeanatomyzafar_18325No ratings yet
- Screening Tests: Click To Edit Master Subtitle StyleDocument15 pagesScreening Tests: Click To Edit Master Subtitle Stylezafar_18325No ratings yet
- General Spec of Oman June 2010Document2 pagesGeneral Spec of Oman June 2010zafar_18325No ratings yet
- Benign Condition of Biliary ApparatusDocument19 pagesBenign Condition of Biliary ApparatusRiya ShindeNo ratings yet
- Colon Rectum ResectionDocument28 pagesColon Rectum ResectionAnca TomaNo ratings yet
- Journal Homepage: - : IntroductionDocument5 pagesJournal Homepage: - : IntroductionIJAR JOURNALNo ratings yet
- Digestion of FoodDocument25 pagesDigestion of FoodJaymee GonzalesNo ratings yet
- The Liver and Its DisordersDocument41 pagesThe Liver and Its Disordersreuben kwotaNo ratings yet
- NCP For Patient With GastritisDocument1 pageNCP For Patient With GastritisBer Anne33% (3)
- Diarrhea Cmap ScriptDocument5 pagesDiarrhea Cmap ScriptmaryNo ratings yet
- Jeopardy Digestive and Urinary SystemsDocument27 pagesJeopardy Digestive and Urinary Systemsapi-133770097No ratings yet
- Cirrhosis: What Is It? What Causes It and Why CausesDocument3 pagesCirrhosis: What Is It? What Causes It and Why CausesJonathan Q. ArancoNo ratings yet
- Digestive Enzymes: Pancreas What Is The Pancreas?Document4 pagesDigestive Enzymes: Pancreas What Is The Pancreas?Joan ChumbaNo ratings yet
- Visayas Community Medical Center Department of Surgery: Curan, Jan Kleen Ediza, Janseen Tortugo, Andrea MarieDocument43 pagesVisayas Community Medical Center Department of Surgery: Curan, Jan Kleen Ediza, Janseen Tortugo, Andrea MarieJanseen EdizaNo ratings yet
- New Consolidated List of EmpanelmentDocument36 pagesNew Consolidated List of EmpanelmentSHAURYA VERMANo ratings yet
- Gastric Resection: General Surgical and Anesthetic ConsiderationsDocument26 pagesGastric Resection: General Surgical and Anesthetic ConsiderationsBlanchette ChNo ratings yet
- ProbioticsDocument30 pagesProbioticstummalapalli venkateswara rao100% (2)
- 8 Supplements To Repair A Leaky GutDocument9 pages8 Supplements To Repair A Leaky GutalbinutaNo ratings yet
- When The Tummy Gets BusyDocument59 pagesWhen The Tummy Gets BusyChris Reubal BuscayNo ratings yet
- Program Hepato 24 03 2023Document20 pagesProgram Hepato 24 03 2023Loredana BoghezNo ratings yet
- Test Report MeDocument4 pagesTest Report MeMkeen BhaiNo ratings yet
- LIVER PROFILE LFT Test Report Format Example Sample Template Drlogy Lab ReportDocument1 pageLIVER PROFILE LFT Test Report Format Example Sample Template Drlogy Lab ReportM ShafiqNo ratings yet
- Hepatology DR Osama Mahmoud PDFDocument86 pagesHepatology DR Osama Mahmoud PDFRaouf Ra'fat Soliman71% (7)
- Laxatives: Psyllium Mucilloid (Metamucil, Others)Document3 pagesLaxatives: Psyllium Mucilloid (Metamucil, Others)Corrine IvyNo ratings yet
- Diverticulum in Small Bowel With Foreign ObjectDocument7 pagesDiverticulum in Small Bowel With Foreign ObjectFerris BuhlerNo ratings yet
- Activating GNAS and KRAS Mutations in Gastric Foveolar Metaplasia, Gastric Heterotopia, and Adenocarcinoma of The DuodenumDocument8 pagesActivating GNAS and KRAS Mutations in Gastric Foveolar Metaplasia, Gastric Heterotopia, and Adenocarcinoma of The DuodenumNurhadi EffendyNo ratings yet
- Biliary Tract Surgery 2008, Vol.88, Issues 6Document292 pagesBiliary Tract Surgery 2008, Vol.88, Issues 6Barbero JuanNo ratings yet
- Dyspepsia BrochureDocument5 pagesDyspepsia BrochureJns RamNo ratings yet
- VomitingDocument29 pagesVomitinganusrisaranganNo ratings yet
- Final CholelithiasisDocument36 pagesFinal CholelithiasisRalph Pelegrino100% (2)
- Catheterization and EnemaDocument49 pagesCatheterization and EnemakhaimahalenylenNo ratings yet
- Bruno, Gene - Using Betaine Hydrochloride & Digestive Enzymes For Indigestion - Huntington College (2014)Document3 pagesBruno, Gene - Using Betaine Hydrochloride & Digestive Enzymes For Indigestion - Huntington College (2014)pedpixNo ratings yet
- Pathophysiology of Liver Cancer 2Document3 pagesPathophysiology of Liver Cancer 2Charis Paroginog92% (12)