Professional Documents
Culture Documents
Pubid-848078832 1010 PDF
Uploaded by
Cocosul Cocosului CocosaruluiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pubid-848078832 1010 PDF
Uploaded by
Cocosul Cocosului CocosaruluiCopyright:
Available Formats
Infectious Diseases of the Brain and Meninges 83
Table 2.22 Meningitic syndromes
Syndrome Cell count Protein Glucose
Acute bacterial 100 1000, Elevated Low or very low
meningitis mainly polynuclear
Acute viral 100, more mono- Normal or mildly Normal or mildly
meningitis than polynuclear elevated low
Chronic meningitis 100, mainly Elevated or mark- Low or very low
mononuclear edly elevated
stricted to the diagnostic evaluation Bacterial Infections
of radiologically identified abnormal-
ities in the brain. Thus, a biopsy can | Acute Bacterial Meningitis
provide histologic differentiation of (795)
tumors and inflammatory changes, Most cases of bacterial meningitis
which is important for the planning arise by hematogenous spread of a
of further treatment. When a biopsy bacterial infection affecting the upper
is performed, tissue specimens respiratory tract. Less commonly,
should be taken not only for histolog- they are caused by direct extension of
ical examination, but also for culture, pathogenic bacteria from purulent
whenever a bacterial, mycotic, or my- collections in the head, or else patho-
cobacterial infection is a diagnostic gens are directly inoculated into the
possibility. intracranial cavity by traumatic brain
injury, or iatrogenically by punctures
| Neuroimaging Studies and shunt operations.
CT and MRI often provide critical di- The most common pathogens are:
agnostic information about infections > in the newborn: Escherichia coli,
of the central nervous system. MRI, in Group B streptococci;
particular, is indispensable for the di- > in children: Haemophilus influen-
agnosis of abscess and encephalitis zae, pneumococci, and meningo-
(p. 93). Inflammatory changes are of- cocci;
ten visible only after the administra- > in adults: pneumococci and menin-
tion of contrast. Contrast-enhanced gococci.
scans are therefore recommended
whenever a CNS infection is sus- The risk of meningococcal infection
pected. increases in complement disorders or
Angiography may be of assistance in properdin deficiency, while that of
the diagnosis of vasculitis. Mycotic pneumococcal meningitis increases
aneurysms are sometimes visible after splenectomy. Klebsiella, E. coli,
only on an angiogram. and Pseudomonas aeruginosa are the
most common pathogens affecting
aged persons, alcoholics, and persons
who have suffered traumatic brain in-
juries or undergone neurosurgical
procedures; Listeria monocytogenes
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
84 2 Diseases Mainly Affecting the Brain and its Coverings
may also cause meningitis at any age. Diagnosis
Fewer than 1 % of cases of meningitis Examination of the cerebrospinal
involve multiple pathogens. Endemic fluid is critical for diagnosis (Ta-
and epidemic meningitis are a major ble 2.22). If clinical signs of intracra-
public health problem in underdevel- nial hypertension are present (brady-
oped countries and are usually cardia, hypertension, papilledema),
caused by H. influenzae, meningo- an intracranial mass lesion should be
cocci, and pneumococci. ruled out by CT or MRI prior to lum-
bar puncture. The cerebrospinal fluid
Pathological Anatomy is turbid and contains 1,00010,000
A granulocytic infiltration of the me- cells per microliter, and occasionally
ninges and subarachnoid space is ob- more. There is a predominantly gran-
served. This may lead to disturbances ulocytic pleocytosis. The cerebrospi-
of cerebrospinal fluid flow (hydro- nal fluid pressure and protein con-
cephalus), vasospasm, arterial and centration are practically always ele-
venous thrombosis with consequent vated, and the glucose concentration
infarction, infection of the brain tis- low. Gram staining reveals the bacte-
sue (encephalitis, cerebritis, brain ab- rial pathogen in 6090 % of cases. Ce-
scess), cerebral edema, and intracra- rebrospinal fluid cultures are positive
nial hypertension. in ca. 75 % of cases, and blood cultures
in 5075 %. Blood culture should be
Clinical Features performed in all cases, as it may be
The classic clinical triad of meningitis positive even if the cerebrospinal
consists of: fluid culture is negative. Partially
> headache, treated bacterial meningitis and liste-
> fever, and rial meningitis may be associated
> meningism (nuchal rigidity). with fewer than 1000 cells per micro-
liter in the cerebrospinal fluid and
Headache may be extremely intense should not be confused with viral
and diffuse, commonly bioccipital. meningitis.
Back pain, myalgia, photophobia, Neuroimaging studies such as CT and
nausea, and vomiting are further MRI are generally not required for di-
symptoms. As many as 40 % of pa- agnosis, but they are helpful should
tients have epileptic seizures, and complications arise. They are normal
1020 % have cranial nerve deficits. in the early stage of bacterial menin-
Such patients are usually somnolent gitis, but later show compression of
or comatose and manifest a charac- the sulci and cisterns. Meningeal en-
teristic combination of hypertension hancement may be seen on MRI, and
and bradycardia. Papilledema may be more rarely on CT (Fig. 2.15). (760).
present. Fever and meningism may Bony defects of the base of the skull
be only mild in children, the elderly, that may be of pathogenetic signifi-
and immune-suppressed patients, in cance are usually seen in the bone
whom headache and vomiting are the window of a fine-section CT scan.
major manifestations of disease.
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
Infectious Diseases of the Brain and Meninges 85
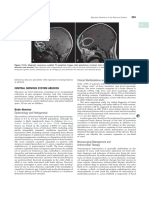
Fig. 2.15a, b Chronic meningitis.
The patient is a 49-year-old woman. The pathogenic organism could not be identified. a
Coronal T1-weighted MRI with contrast. b Axial T1-weighted MRI with contrast. Note the
abnormal contrast enhancement in the meninges.
Fig. 2.16a, b Acute bacterial meningitis.
The patient is a 10-year-old boy. a Coronal T1-weighted MRI with contrast demonstrates
sphenoid sinusitis (arrows) spreading in the epidural space under the left temporal lobe
and causing meningitis by direct extension with involvement of the temporal lobe (arrow-
heads). b T1-weighted MRI with contrast in a coronal section posterior to a shows a prob-
able epidural empyema over the left temporal lobe (arrowheads). There is also extensive
signal change in the left thalamus, probably due to an arterial infarction as a complication
of meningitis.
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
86 2 Diseases Mainly Affecting the Brain and its Coverings
Prognosis Treatment
The prognosis of acute bacterial men- (Fig. 2.17) (777a)
ingitis depends on: If a lumbar puncture cannot be per-
> the pathogenic organism, formed immediately because of
> the severity of the infection, clinical signs of intracranial hyper-
> concomitant illnesses, tension, blind parenteral antimi-
> the state of the immune system, crobial treatment should be initi-
and ated at once, as a few minutes may
> the type of treatment and time at make the difference between life and
which it is instituted. death. If the pathogenic organism is
unknown, the antimicrobial treat-
Mortality is highest in the newborn ment is chosen empirically (Ta-
(over 50 %). Meningitis accompanied ble 2.23). It can then be modified in
by meningococcal sepsis also confers accordance with the findings of the
a high mortality, because it is fre- cerebrospinal fluid and blood cul-
quently complicated by bilateral ad- tures, including sensitivity and re-
renal hemorrhage and subsequent sistance testing.
circulatory collapse (Waterhouse- The duration of treatment is based
Friderichsen syndrome). The mortal- on the findings of serial clinical ex-
ity of other forms of meningitis is ap- amination and cerebrospinal fluid
proximately 20 % (1014). Surviving analysis. Some general recommen-
patients often suffer from permanent dations are:
sequelae including deafness, malre- > for meningococci and H. influen-
sorptive hydrocephalus, epilepsy, and zae, 710 days;
intellectual deficits, particularly in > for pneumococci, 1014 days;
children. > for Listeria and Gram-negative
aerobes, 3 weeks.
Steroids (dexamethasone 0.4 mg/kg
every 12 hours in the first 2 days of
treatment) favorably affect the
course of the inflammatory process
in children and probably also in
adults, and should be given in addi-
tion to antimicrobial agents (560,
831).
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
Infectious Diseases of the Brain and Meninges 87
Suspicion of meningitis
Papilledema or focal
Yes neurologic deficits No
Blood cultures Positive Positive Blood cultures
Immediate empirical Specific Lumbar puncture
antibiotic treatment antibiotic treatment
CT or MRI Positive Immediate empirical
antibiotic treatment
Diagnosis confirmed
Gram stain,
antigen tests, cultures
Meningitis confirmed, or
normal; no evidence of Lumbar puncture
intracranial hypertension
Other diagnosis found
Diagnosis
Other specific therapy Other diagnosis not confirmed
Fig. 2.17 Management flowchart for meningitis.
The essential element of treatment is immediate institution of antimicrobial therapy, at
first empirical and then tailored to the specific pathogen identified by culture.
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
All rights reserved. Usage subject to terms and conditions of license.
Mumenthaler, Neurology 2004 Thieme
Table 2.23 Antimicrobial therapy of bacterial meningitis (824, 831, 836)
88
Patient group Most likely organism Agent(s) of first choice1 Alternatives
2
Newborn Group B streptococci, E. coli, Ampicillin and cefotaxime Ampicillin and aminoglycoside
2
Listeria monocytogenes
Diseases Mainly Affecting the Brain and its Coverings
Infants 13 months Same and H. influenzae, menin- Ampicillin and ceftriaxone or Chloramphenicol and aminogly-
gococci, pneumococci cefotaxime coside
Infants G 3 months, toddlers H. influenzae, meningococci, Ceftriaxone or cefotaxime Chloramphenicol and ampicillin
pneumococci
Children and adults Pneumococci, meningococci, Ceftriaxone or cefotaxime and Chloramphenicol and ampicillin,
Listeria monocytogenes ampicillin or penicillin G vancomycin if penicillin-
resistant
Adults G 60 years, alcoholics, Pneumococci, E. coli, Haemophi- Vancomycin and ceftriaxone2 Chloramphenicol and
patients with systemic lus influenzae, Listeria monocyto- and rifampicin trimethoprim-sulfamethoxazole
disease genes, Pseudomonas aeruginosa,
anaerobes3
Traumatic brain injury, Staphylococcus aureus, E. coli, Vancomycin and ceftriaxone
neurosurgical procedures Pseudomonas aeruginosa,4
pneumococci
Cerebrospinal fluid leak Pneumococci Cefotaxime or ceftriaxone
1 Unless otherwise specified, these recommendations are applicable to the most likely pathogens affecting the group of patients in ques-
tion. If the responsible pathogen is known, the treatment should be correspondingly tailored. Dosages may be found in drug compendia.
2 Or other (third-generation) cephalosporin.
3 Chloramphenicol or metronidazole.
4 Add gentamicin.
Infectious Diseases of the Brain and Meninges 89
Prevention ache, meningism, asymmetrical cra-
The administration of Haemophilus nial nerve deficits, and ischemic
vaccine to infants confers 90 % protec- stroke. Coma is a bad prognostic sign.
tion against this type of meningitis. For miliary tuberculosis, see p. 91.
Inoculation against the meningococ-
cus is recommended for travelers to Diagnosis
endemic areas. After exposure to Cerebrospinal fluid examination re-
Haemophilus or meningococcus, anti- veals a picture of chronic meningeal
microbial prophylaxis is recom- inflammation with at first granulo-
mended (10 mg/kg in children or cytic and then monocytic pleocytosis
600 mg in adults, b.i.d. for 2 days). of 100500 cells, elevated protein
concentration, and low glucose con-
| Tuberculous Meningitis (1051) centration. The diagnosis is con-
Mycobacterium tuberculosis causes a firmed by the demonstration of acid-
chronic bacterial infection character- fast bacilli by the Ziehl-Neelsen
ized by granuloma formation. The method or with auramine
lung is usually affected. The menin- rhodamine staining, either in the
ges may become involved during the fresh cerebrospinal fluid sample or
primary infection in children, or years after 46 weeks of culture.
afterward in adults. Meningitis comes
about by reactivation of clinically si-
lent granulomas and secondary de-
posits in the subarachnoid space,
even in the absence of simultaneous
pulmonary tuberculosis. HIV-positive
persons are at particularly high risk of
infection both by M. tuberculosis and
by atypical mycobacteria.
Pathological Anatomy
An exudative basilar meningitis and
vasculitis is found, particularly in the
vicinity of the anterior and middle ce-
rebral arteries. Meningeal involve-
ment and vasculitis may lead to cra-
nial nerve deficits and to cerebral in-
farction. Hydrocephalus is commonly
seen.
Clinical Features
Over the course of several days or, Fig. 2.18 Tuberculous meningitis.
more rarely, weeks, these patients ex- This contrast-enhanced T1-weighted MR
image reveals enhancement of the in-
hibit progressive symptoms and signs
flamed meninges at the basal cisterns and
including subfebrile temperature, anterior to the brainstem. The asymmetri-
fatigue, depression, personality cal extension of inflammation along the
changes, and (sometimes) confusion. course of the middle cerebral artery is also
One-third of patients develop head- typical.
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
90 2 Diseases Mainly Affecting the Brain and its Coverings
In addition to the cerebrospinal fluid, Prognosis
the sputum, gastric juice, and urine Tuberculous meningitis is fatal if un-
should be examined and cultured for treated, curable without sequelae if
acid-fast bacilli. Contrast-enhanced treated in time. The diagnosis should
CT and MRI reveal meningeal involve- be made, and treatment initiated,
ment at the skull base and along the before the onset of cranial nerve defi-
course of the middle cerebral artery cits or of impaired consciousness.
(151) (Fig. 2.18). Thus: when tuberculous meningitis is
strongly suspected, obtain fluid sam-
Differential Diagnosis ples for culture and then begin antitu-
bercular therapy immediately.
The differential diagnosis includes all
types of chronic lymphocytic menin-
goencephalitis (see below). | Meningoencephalitis
| Listeriosis (957, 959, 695b)
Treatment Listeria are aerobic or facultatively
anaerobic bacilli that are usually in-
The treatment consists of a combi- gested orally in food. They preferen-
nation of four tuberculostatic medi- tially infect the newborn, diabetics,
cations: rifampicin, isoniazid, pyra- alcoholics, and aged or immune-
zinamide, and ethambutol. At the suppressed persons. The clinical pic-
same time, steroids and vitamin B6 ture is generally that of a typical bac-
should be given. The latter pre- terial meningitis, but the cerebrospi-
vents the pyridoxine deficiency nal fluid cell count may be so low as
that may otherwise result from to arouse suspicion of viral meningi-
long-term use of isoniazid. tis. Listeria also causes encephalitis,
This therapy should be continued often with brainstem manifestations,
until the results of culture are as well as meningoencephalitis
available. If culture is positive for and cerebral or spinal abscesses
tubercle bacilli, a combination of (Fig. 2.19).
three medications is given for a fur-
ther 2 months, and then two medi- Treatment
cations for 810 months more.
Once the culture results are nega- The antimicrobial agents of first
tive and the cerebrospinal fluid pic- choice are ampicillin and penicillin
ture has renormalized, treatment G. An alternative is trimethoprim/
may be discontinued. sulfamethoxazole. Cephalosporins
If the patient fails to improve on do not eliminate Listeria.
this regimen, other etiologies of
chronic meningitis should be
| Brucella Meningitis (127)
sought, and, even if cultures for M.
Brucellosis is transmitted in milk or
tuberculosis are negative, it is pru-
other animal products and usually
dent to continue the tuberculo-
presents nonspecifically with fever,
static therapy. The currently used
arthralgias and myalgias, though it
tuberculostatic agents have only
causes localized disease in some
minor side effects even in long-
cases, and its manifestations are
term use.
sometimes restricted to the central
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
Infectious Diseases of the Brain and Meninges 91
Fig. 2.19 Listeria meningoencephalitis.
A 45-year-old woman with multiple cranial nerve deficits and left ataxia.
a The FLAIR sequence reveals a plate-like signal abnormality in the brainstem and left cer-
ebellar hemisphere.
b The T1-weighted image shows several foci of contrast enhancement.
nervous system. These usually consist
of subacute or chronic meningitis,
more rarely meningoencephalitis,
myeloradiculitis or neuritis.
Twenty to 500 cells are found in the
cerebrospinal fluid. The diagnosis is
confirmed by the demonstration of
specific antibodies in the CSF.
Treatment
The treatment consists of doxycy-
cline and rifampicin for 4 months,
with surveillance of the cerebrospi-
nal fluid.
Fig. 2.20 Miliary tuberculosis.
| Meningoencephalitis in Miliary
A 28-year-old woman with miliary tubercu-
Tuberculosis losis. Cerebrospinal fluid examination re-
In miliary tuberculosis, hematoge- vealed a mild monocytic pleocytosis, a
markedly elevated protein concentration,
nous spread of tubercle bacilli leads
and a low glucose concentration. The MRI
to the formation of millet-seed-sized reveals multiple pinhead-sized foci of con-
granulomas throughout the body. The trast enhancement in the brain paren-
clinical manifestations are not spe- chyma and mild contrast enhancement of
cific to this disease but rather reflect the meninges as well.
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
92 2 Diseases Mainly Affecting the Brain and its Coverings
the predominantly involved organ(s). rysms, or any combination of these
Symptoms and signs may include fe- entities.
ver, night sweats, anorexia, general-
ized weakness and fatigue, hepato- Clinical Features
splenomegaly, lymphadenopathy,
The symptoms and signs depend on
and (if the brain is affected) headache
the pathological processes occurring
and progressive impairment of con-
in each individual case. Embolic
sciousness. Miliary tuberculosis
events are prominent in 20 % of cases,
usually affects the brain parenchyma
encephalitis due to multiple micro-
more than the meninges. The cere-
emboli and microabscesses in 10 %,
brospinal fluid findings are the same
hemorrhage due to mycotic aneu-
as for tuberculous meningitis, except
rysms in 5 %, and meningitis in 5 %.
that pleocytosis is usually only
Emboli produce focal manifestations,
mild. MRI reveals multiple pinhead-
while the other types of lesion cause
sized, contrast-enhancing nodules
a diffuse encephalopathy with behav-
(Fig. 2.20).
ioral and cognitive disturbances, im-
For diagnosis and treatment, see Tu-
pairment of consciousness, focal or
berculous meningitis, above (p. 90).
generalized seizures, and sometimes
headache and meningism. Important
| Focal Embolic Encephalitis diagnostic clues include subfebrile or
(148, 315, 819) (in acute endocarditis) septic temper-
Neurological symptoms and signs de- ature, a feeling of severe illness and
velop in at least one-third of patients prostration, anemia, splenomegaly,
with infectious endocarditis and may subungual, palmar and retinal pete-
be the presenting manifestations of chiae, and heart murmur.
the disease.
Streptococcus is the most common Diagnosis
pathogen, followed by staphylococ-
The complete blood count reveals
cus and Gram-negative bacilli. Cen-
acute inflammation, and the erythro-
tral nervous manifestations arise by
cyte sedimentation rate and C-
several different pathogenetic mecha-
reactive protein are elevated. The re-
nisms:
sponsible organism can usually be
> occlusion of cerebral arteries by
demonstrated by blood culture, and
septic and thrombotic emboli aris-
endocarditis by transesophageal echo-
ing from heart valve vegetations;
cardiography (212). The cerebrospinal
> infection of the meninges, brain
fluid may be sterile, purulent or hem-
parenchyma, or vascular walls by
orrhagic, depending on the nature of
septic emboli or by bacteremia;
CNS involvement (772).
> toxic and probably also immune-
MRI is particularly useful for the
mediated injury.
demonstration of embolic and infec-
tious processes affecting the central
Pathological Anatomy nervous system. Angiography is the
There may be bland or hemorrhagic most reliable way to demonstrate
cerebral infarcts, intracerebral, sub- mycotic aneurysms, but need not be
arachnoid or subdural hemorrhage, performed routinely in every patient
meningitis, abscesses, mycotic aneu- (819).
Mumenthaler, Neurology 2004 Thieme
All rights reserved. Usage subject to terms and conditions of license.
You might also like
- Exploring-Grays-Anatomy Coloring Book PDFDocument129 pagesExploring-Grays-Anatomy Coloring Book PDFCocosul Cocosului CocosaruluiNo ratings yet
- Course Title Course Code Course Description Prerequisites Course Credit Placement Program OutcomeDocument10 pagesCourse Title Course Code Course Description Prerequisites Course Credit Placement Program OutcomeNur Sanaani100% (1)
- Meningitis: Review ArticleDocument19 pagesMeningitis: Review ArticleYo Me100% (1)
- Handbook of AnesthesiologyDocument176 pagesHandbook of AnesthesiologyarmelzahfauziNo ratings yet
- Infectious Diseases Pharmacotherapy: Lesson 5 Central Nervous System InfectionDocument63 pagesInfectious Diseases Pharmacotherapy: Lesson 5 Central Nervous System Infectionbest batiNo ratings yet
- Bacterial Meningitis: Etiology and PathophysiologyDocument9 pagesBacterial Meningitis: Etiology and PathophysiologyIndra Dwi VerawatiNo ratings yet
- AbcesoDocument2 pagesAbcesoRocio LedesmaNo ratings yet
- Imaging of Intracranial InfectionsDocument12 pagesImaging of Intracranial Infectionsrafael rocha novaesNo ratings yet
- Infections Diseases of The Central Nervous System: Chapter VI - J. RuscalledaDocument11 pagesInfections Diseases of The Central Nervous System: Chapter VI - J. RuscalledaArif BudimanNo ratings yet
- Invasive Cryptococcal Meningitis Presenting As A Skull Base Mass in An Immunocompetent Host: A Case ReportDocument5 pagesInvasive Cryptococcal Meningitis Presenting As A Skull Base Mass in An Immunocompetent Host: A Case ReportAsep RiswandiNo ratings yet
- Infections of The Central Nervous System Audio (Autosaved)Document72 pagesInfections of The Central Nervous System Audio (Autosaved)hnm mnhNo ratings yet
- Neurological Infections: Gerard Gabriel P. Reotutar, RM, RN, MANDocument33 pagesNeurological Infections: Gerard Gabriel P. Reotutar, RM, RN, MANJeremiash Noblesala Dela CruzNo ratings yet
- BffsDocument60 pagesBffsdrewantaNo ratings yet
- Meningitis - StatPearls - NCBI BookshelfDocument13 pagesMeningitis - StatPearls - NCBI Bookshelfaslan tonapaNo ratings yet
- K - 18 Infection of The CNS (Neurologi)Document137 pagesK - 18 Infection of The CNS (Neurologi)Vera AristaNo ratings yet
- Intracranial Infection - Prof SunartiniDocument12 pagesIntracranial Infection - Prof SunartiniFranciscus BuwanaNo ratings yet
- Central Nervous System Pathology: Presented byDocument70 pagesCentral Nervous System Pathology: Presented byNicholasNo ratings yet
- 2 Brain AbscessDocument25 pages2 Brain AbscessKaif KhanNo ratings yet
- Treatment: Tensive Care Unit Is Often NecessaryDocument12 pagesTreatment: Tensive Care Unit Is Often NecessaryCocosul Cocosului CocosaruluiNo ratings yet
- Neuroinfections Presentation Diagnosis and Treatment of Meningitis and EncephalitisDocument10 pagesNeuroinfections Presentation Diagnosis and Treatment of Meningitis and EncephalitisZarick SaenzNo ratings yet
- AbsesDocument2 pagesAbsesnacenkNo ratings yet
- Bacterial Infections of The Central Nervous System: Paul A. Lapenna, Do Karen L. Roos, MDDocument9 pagesBacterial Infections of The Central Nervous System: Paul A. Lapenna, Do Karen L. Roos, MDOver HidalgoNo ratings yet
- Community Acuired Bactarial MeningitisDocument16 pagesCommunity Acuired Bactarial Meningitisidno1008No ratings yet
- Varicella-Zoster Virus Infections of The Nervous System: Clinical and Pathologic CorrelatesDocument11 pagesVaricella-Zoster Virus Infections of The Nervous System: Clinical and Pathologic CorrelatesarisastraNo ratings yet
- PyomeningitisDocument54 pagesPyomeningitisRiya BagdiNo ratings yet
- Meningitis MedscapeDocument73 pagesMeningitis MedscapeBujangNo ratings yet
- Pathology of The Central Nervous SystemDocument78 pagesPathology of The Central Nervous Systemعلي عليNo ratings yet
- Brain Tuberculomas, Tubercular Meningitis, and Post-Tubercular Hydrocephalus in ChildrenDocument5 pagesBrain Tuberculomas, Tubercular Meningitis, and Post-Tubercular Hydrocephalus in ChildrenDave VentraNo ratings yet
- CNSinfectionsDocument79 pagesCNSinfectionsMatusala BafaNo ratings yet
- Approach To The Patient With Suspected Infection of SNCDocument12 pagesApproach To The Patient With Suspected Infection of SNCJosé Miguel FerreiraNo ratings yet
- Modul 1 CNS InfectionsDocument150 pagesModul 1 CNS InfectionsAndrada-Georgiana NacuNo ratings yet
- Pyogenic and TB Meningitis - FinalDocument65 pagesPyogenic and TB Meningitis - FinalKishor K AdhikariNo ratings yet
- Managing Meningoencephalitis in Indian ICU: Neurocritical CareDocument5 pagesManaging Meningoencephalitis in Indian ICU: Neurocritical CareerikafebriyanarNo ratings yet
- Central Nervous System Infections: Gonzalo B. Roman JR.,MD.,FPSPDocument72 pagesCentral Nervous System Infections: Gonzalo B. Roman JR.,MD.,FPSPBenjamin PrabhuNo ratings yet
- Meningitis &encephalitisDocument9 pagesMeningitis &encephalitisSnIP StandredNo ratings yet
- Acute Bacterial MeningitiDocument31 pagesAcute Bacterial MeningitiHesbon MomanyiNo ratings yet
- Problem 3.01 Nervous System Study Guide 3Document2 pagesProblem 3.01 Nervous System Study Guide 3Monish NaiduNo ratings yet
- DasdasDocument4 pagesDasdasAbdurauf SawadjaanNo ratings yet
- Acute Neurological InfectionsDocument6 pagesAcute Neurological Infectionsramon.camara.03No ratings yet
- Meningitis and Dementia: Dr. Lubna DwerijDocument52 pagesMeningitis and Dementia: Dr. Lubna DwerijNoor MajaliNo ratings yet
- PR Dr. AriadneDocument8 pagesPR Dr. AriadneSofia KusumadewiNo ratings yet
- Bacterial Brain Abscess: Journal ReadingDocument22 pagesBacterial Brain Abscess: Journal ReadingdinarNo ratings yet
- Infections of The Central Nervous System08Document47 pagesInfections of The Central Nervous System08Annisa SasaNo ratings yet
- CNS InfectionDocument17 pagesCNS InfectionEdward PuteraNo ratings yet
- AcuteDocument11 pagesAcutenunu ahmedNo ratings yet
- Meningitis - Practice Essentials, Background, PathophysiologyDocument26 pagesMeningitis - Practice Essentials, Background, PathophysiologydilaNo ratings yet
- Brain AbscessDocument2 pagesBrain AbscessIan RomanNo ratings yet
- Research Paper On Bacterial MeningitisDocument8 pagesResearch Paper On Bacterial Meningitisvvgnzdbkf100% (1)
- Acute Bacterial MeningitisDocument15 pagesAcute Bacterial MeningitisOana StefanNo ratings yet
- Diagnosis and Treatment of Viral Encephalitis: ReviewDocument10 pagesDiagnosis and Treatment of Viral Encephalitis: ReviewnataliaNo ratings yet
- Definition-: Neisseria Meningitidis Invading The Subarachnoid Space of The BrainDocument12 pagesDefinition-: Neisseria Meningitidis Invading The Subarachnoid Space of The BrainAmit MartinNo ratings yet
- Chronic MeningitisDocument7 pagesChronic Meningitisneurojuancarfab100% (1)
- Absceso CerebralDocument8 pagesAbsceso Cerebralgiseladelarosa2006No ratings yet
- Exposicion FinishDocument13 pagesExposicion FinishFernanda ChNo ratings yet
- Manejo Meningitis Art 2022 IngDocument5 pagesManejo Meningitis Art 2022 Ingroman rodriguezNo ratings yet
- Meningitis, AAFPDocument8 pagesMeningitis, AAFPCarlos Danilo Noroña CNo ratings yet
- Meningitis PresentationDocument41 pagesMeningitis PresentationO'Mark AndrewsNo ratings yet
- Meningitis BakteriDocument11 pagesMeningitis BakteriSiq Febri SmnjtkNo ratings yet
- Acutebacterialmeningitis: Current Review and Treatment UpdateDocument11 pagesAcutebacterialmeningitis: Current Review and Treatment UpdateWidya Niendy PrameswariiNo ratings yet
- 12 Cns Infection 2 LecturesDocument18 pages12 Cns Infection 2 LecturesZain AlAbideen AlTaeeNo ratings yet
- Bacterial MeningitisDocument40 pagesBacterial MeningitisDinesh ReddyNo ratings yet
- Neurobiology of Brain Disorders: Biological Basis of Neurological and Psychiatric DisordersFrom EverandNeurobiology of Brain Disorders: Biological Basis of Neurological and Psychiatric DisordersNo ratings yet
- Noac GuidelinesDocument40 pagesNoac GuidelinesCocosul Cocosului CocosaruluiNo ratings yet
- Cardiovascular Complications of The Guillain-Barré Syndrome.Document4 pagesCardiovascular Complications of The Guillain-Barré Syndrome.Cocosul Cocosului CocosaruluiNo ratings yet
- Cardiovascular Dysfunction in Multiple SclerosisDocument7 pagesCardiovascular Dysfunction in Multiple SclerosisCocosul Cocosului CocosaruluiNo ratings yet
- Cardiovascular Autonomic Dysfunction in Parkinson's DiseaseDocument7 pagesCardiovascular Autonomic Dysfunction in Parkinson's DiseaseCocosul Cocosului CocosaruluiNo ratings yet
- Surviving Sepsis Campaign 2016 Guidelines Presentation FinalDocument60 pagesSurviving Sepsis Campaign 2016 Guidelines Presentation FinalCocosul Cocosului CocosaruluiNo ratings yet
- Cardiomyopathy in Motor Neuron DiseasesDocument4 pagesCardiomyopathy in Motor Neuron DiseasesCocosul Cocosului CocosaruluiNo ratings yet
- Curs GeriatrieDocument4 pagesCurs GeriatrieCocosul Cocosului CocosaruluiNo ratings yet
- Examinarea Clinica Neurologica - Geraint FullerDocument222 pagesExaminarea Clinica Neurologica - Geraint FullerCocosul Cocosului CocosaruluiNo ratings yet
- Pubid-848078832 1009 PDFDocument8 pagesPubid-848078832 1009 PDFCocosul Cocosului CocosaruluiNo ratings yet
- Mild Traumatic Brain Injury (Concussion) : DefinitionDocument9 pagesMild Traumatic Brain Injury (Concussion) : DefinitionCocosul Cocosului CocosaruluiNo ratings yet
- Chirila I M.D., Baciu M M.D., Rosu O M.D., Blesneag Av M.D. PHD, Muresan DF M.D. PHDDocument1 pageChirila I M.D., Baciu M M.D., Rosu O M.D., Blesneag Av M.D. PHD, Muresan DF M.D. PHDCocosul Cocosului CocosaruluiNo ratings yet
- Treatment: Tensive Care Unit Is Often NecessaryDocument12 pagesTreatment: Tensive Care Unit Is Often NecessaryCocosul Cocosului CocosaruluiNo ratings yet
- Heart Disease Thesis StatementDocument6 pagesHeart Disease Thesis StatementHelpWithPaperCanada100% (2)
- Jurnal Artritis RematoidDocument9 pagesJurnal Artritis Rematoiddwi restuNo ratings yet
- Lumbar SpondylosisDocument26 pagesLumbar SpondylosisBanni Aprilita PratiwiNo ratings yet
- 1st Assessment Health 6 3rd QuarterDocument2 pages1st Assessment Health 6 3rd QuarterJesusa Franco DizonNo ratings yet
- Neurocritical Care in The General Intensive Care UnitDocument17 pagesNeurocritical Care in The General Intensive Care UnitdanielNo ratings yet
- Psychotic Symptoms As A Continuum Between Normality and PathologyDocument12 pagesPsychotic Symptoms As A Continuum Between Normality and PathologyOana OrosNo ratings yet
- .Au Files Dysbiosis ScoreDocument2 pages.Au Files Dysbiosis ScorekenetmartinNo ratings yet
- TetanusDocument25 pagesTetanusTariq KanharNo ratings yet
- Imaging of Ventricular Septal Defect - Rizki Yuda PurnomoDocument18 pagesImaging of Ventricular Septal Defect - Rizki Yuda PurnomoRizkiYudaPurnomoNo ratings yet
- Orthopedic NursingDocument150 pagesOrthopedic NursingCyrhille Paner100% (2)
- Department of Education: Republic of The PhilippinesDocument1 pageDepartment of Education: Republic of The PhilippinesJen FerrerNo ratings yet
- RA - Heat StresssDocument5 pagesRA - Heat Stresssradeep0% (1)
- COVID-19 Fact Sheet K 12 Exposure and Quarantine Flow ChartDocument1 pageCOVID-19 Fact Sheet K 12 Exposure and Quarantine Flow ChartWSYX/WTTENo ratings yet
- Reflections On Medical Law and Ethics in IndiaDocument2 pagesReflections On Medical Law and Ethics in IndiaJose John17No ratings yet
- ICEID 2018 Program BookDocument286 pagesICEID 2018 Program BookMedia Penelitian Dan Pengembangan KesehatanNo ratings yet
- Dry NeedlingDocument8 pagesDry NeedlingDrVandana Phyworld100% (2)
- Laboratory Test Report: Test Name Result Sars-Cov-2 (RDRP Gene)Document1 pageLaboratory Test Report: Test Name Result Sars-Cov-2 (RDRP Gene)srinathNo ratings yet
- Meniere's Disease & OtosclerosisDocument44 pagesMeniere's Disease & OtosclerosisNadzirah Ahmad JailaniNo ratings yet
- Disorders of Cardiac RhythmDocument66 pagesDisorders of Cardiac RhythmslyfoxkittyNo ratings yet
- Schwannoma - Radiology Reference ArticleDocument16 pagesSchwannoma - Radiology Reference ArticleMagda CabralesNo ratings yet
- Stoelting's Anesthesia and Co-Existing Disease 7th EditionDocument740 pagesStoelting's Anesthesia and Co-Existing Disease 7th EditionninataniaaaNo ratings yet
- Abdominoplasty in The Obese Patient: Risk Versus Reward: Garden City, N.YDocument6 pagesAbdominoplasty in The Obese Patient: Risk Versus Reward: Garden City, N.YМаратNo ratings yet
- Jurnal Internasional Fraktur LumbalDocument8 pagesJurnal Internasional Fraktur LumbalBella FebriantiNo ratings yet
- J Neurol Neurosurg Psychiatry 2008 Jankovic 368 76Document9 pagesJ Neurol Neurosurg Psychiatry 2008 Jankovic 368 76Noven da LopezNo ratings yet
- GERD Diagnosis and Management 2013Document21 pagesGERD Diagnosis and Management 2013vhinrichNo ratings yet
- CopdDocument11 pagesCopdpkm bungamasNo ratings yet
- BarredojuliannenutritionquestionevidenceassignmentDocument5 pagesBarredojuliannenutritionquestionevidenceassignmentapi-639582054No ratings yet
- Case Presentation On Respiratory Track InfectionDocument22 pagesCase Presentation On Respiratory Track InfectionNewtan DebNo ratings yet