Professional Documents
Culture Documents
Digital Dental Photography. Part 8: Intra-Oral Set-Ups: I. Ahmad
Uploaded by
bkprosthoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Digital Dental Photography. Part 8: Intra-Oral Set-Ups: I. Ahmad
Uploaded by
bkprosthoCopyright:
Available Formats
Digital dental photography.
IN BRIEF
Once an understanding of the basic set-
Part 8: intra-oral set-ups ups is gained, intra-oral photography can
PRACTICE
be expedited in a few minutes.
Cross-infection control during a
photographic session is mandatory.
I. Ahmad1 As well as taking stock dental images,
one can concentrate on specific points of
interest and analyse them later.
Intra-oral photography is also an
excellent method of communication with
the patient, ceramist and specialist.
The majority of pictures taken in the dental surgery are intra-oral and this article looks at the practicalities involved in full-
arch, quadrant occlusal, lingual (or palatal) and lateral views, as well as magnified images, oral mucosa, enamel texture,
dentine strata and shade analysis for artificial restorations. Additionally, the issue of cross-infection control is considered.
The majority of pictures taken in the den-
tal surgery are intra-oral, which includes
the following:
1. Full arch frontal and occlusal
2. Quadrant occlusal, lingual
(or palatal) and lateral
3. Magnification images for detailed
analysis of teeth or soft tissues
4. Oral mucosa
5. Enamel texture, cracks
and dentine strata
6. Translucency: incisal and
interproximal
7. Shade analysis for
artificial restorations
8. Posterior teeth.
Fig. 1 Photographic equipment should be wrapped with disposable cellophane covers
FUNDAMENTALS OF DIGITAL
DENTAL PHOTOGRAPHY CROSS INFECTION CONTROL rhodium coating. Finally, all intra-oral
1. Digital dental photography: an overview Unlike other forms of photography, dental photographic reflector and backdrop cards
2. Purposes and uses photography requires strict adherence to should be discarded after use.
3. Principles of digital photography cross-infection control measures. Routine
4. Choosing a camera and accessories cross-infection measures carried out for GENERAL GUIDELINES
5. Lighting dental procedures are also applicable for Most intra-oral images necessitate using
6. Camera settings dental photography. It is recommended cheek retractors and/or intra-oral pho-
7. Extra-oral set-ups that a specific zone be reserved for pho- tographic mirrors. The following general
8. Intra-oral set-ups tographic equipment and accessories. All guidelines are applicable for all types of
9. Post-image capture processing photographic equipment, including the intra-oral photography. The first step is
10. Printing, publishing and presentations camera, lens, tripod (if used) and cable asking the patient to wear safety glasses.
releases should be draped with disposable Unless stains or bio-film are being docu-
1
General Dental Practitioner, The Ridgeway Dental
cellophane covers, similar to that used for mented, the teeth should be flossed and
Surgery, 173 The Ridgeway, North Harrow, chair headrests (Fig. 1). Cheek retractors polished with prophylaxis paste to remove
Middlesex, HA2 7DF
Correspondence to: Irfan Ahmad
can either be autoclaved or cold sterilised, food debris, plaque and stains which mask
Email: iahmadbds@aol.com depending on the manufacturers instruc- intrinsic tooth shade and texture. In order
www.IrfanAhmadTRDS.co.uk
tions. Intra-oral mirrors should be cleaned to facilitate placement of cheek retractors,
Refereed Paper with cotton gauze soaked in a mild sur- petroleum jelly is copiously applied to the
Accepted 15 November 2008
DOI: 10.1038/sj.bdj.2009.715
face disinfectant, not surgical spirit, which lips, taking care not to smear the teeth.
British Dental Journal 2009; 207: 151157 causes smears or irreparable damage of the This lubrication also prevents chapping
BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009 151
PRACTICE
Alternatively the dental nurse can stand
behind the patient to hold two unilat-
eral cheek retractors for full arch images,
but this occupies the nurse who may be
required for subsequent stages of the
photographing procedure. After placing
the cheek retractors, the patient is given
tissues to wipe excess salivary flow. The
teeth and gingivae are gently dried with
a warm stream of air without desiccating
the teeth. Other adjuncts to ensure a dry
environment are saliva ejectors and cotton
wool rolls, discretely placed so that they
are not visible in the photograph.
As mentioned in Part 4,1 it is highly
advisable to mount the camera and flashes
Fig. 2 Patient with bilateral cheek retractors onto a tripod. A tripod not only serves as
for photographing the oral cavity Fig. 5 A maxillary tooth will appear shorter a solid platform, but also frees the opera-
if the patients chin is pointing upwards or
the camera axis is inferior to the maxillary tors hand to concentrate on taking the
arch. This is a useful set-up for illuminating photograph, reduces fatigue, and prevents
and capturing crown margins potential accidents such as inadvertently
bumping into surgery equipment. To
ensure that a picture is correctly orien-
tated, the camera axis and patients head
should be parallel in the horizontal, verti-
cal and sagittal planes. Misalignment of
the horizontal plane can convey incorrect
assumptions, for example a slanted incisal
plane, which is especially critical if anterior
crowns are being planned. In the superior-
inferior plane, incorrect alignment results
Fig. 6 Note the clearly visible crown margins in pseudo-shortening or lengthening of
of the left lateral incisor in this picture
taken using the set-up described in Figure 5 teeth in the inciso-gingival perspective, for
compared to Figure 7, when the patient is example the maxillary teeth appear longer
looking directly into the camera (set-up if the patients chin is pointing downwards
Fig. 3 A maxillary tooth will appear longer described in Figure 8)
or the camera axis is superior to the maxil-
if the patients chin is pointing downwards
or the camera axis is superior to the lary arch. However, this is a useful set-up
maxillary arch, but this is a useful set-up for for photographing the mandibular ante-
photographing mandibular anterior teeth rior teeth (Figs 3-4). Conversely, shorter
teeth are recorded if the chin is pointing
upwards or the camera axis is inferior to
the maxillary arch. This type of set-up is
very useful for illuminating and capturing
crown margins (Figs 5-7). While an incor-
rect horizontal plane is readily corrected in
photo-editing software, an incorrect tooth
Fig. 7 When the patient is looking directly perspective (superior-inferior plane) is dif-
into the camera the crown margins of the ficult or almost impossible to rectify with-
Fig. 4 Mandibular anterior teeth photographed left lateral incisor are not clearly discernible out introducing further distortions. This is
using the set-up described in Figure 3 (compare with Figure 6)
particularly significant for magnification
or detailed views.
of the lips while they and the cheeks are available on the market and it is useful to Some clinicians prefer to delegate den-
displaced by the retractors. have a selection to hand to cater for dif- tal photography to another member of the
The choice of cheek retractor is a per- ferent eventualities. For full arch images dental team, for example a nurse, hygienist
sonal preference, and also depends on the the bilateral variety is preferred, while or dental technician. While this obviously
extent of mouth opening of the patient the unilateral retractor is more suitable saves time, especially in a busy prac-
(Fig. 2). Many sizes and varieties are for photographing individual quadrants. tice, the resultant images may not yield
152 BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009
PRACTICE
the anticipated information. Ideally, it is
the clinicians duty to take photographs
since he or she knows what to concen-
trate on. Asking someone else to take
stock, predefined views of each patient
may not reveal clinically relevant infor-
mation. For example, stock images may
not record oral lesions of a patient who
complains of symptoms of oral pathol-
ogy, or document mamelons in a natural
tooth in order that the ceramist can mimic
this in a crown on an adjacent tooth. On
the other hand, standardised views are
indispensable for assessing occlusal rela-
tionships or tooth movement during ortho-
dontic treatment. Furthermore, to achieve
photographically acceptable results, Fig. 8 Full arch frontal set-up Fig. 10 Full maxillary arch occlusal set-up
training and experience in dental pho-
tography is a prerequisite. To summarise,
each patient has different photographic
requirements depending on the proposed
treatment, and therefore the ideal person
to make this judgement is the clinician,
who is also probably more experienced in
dental photography.
The following sections describe the set-
ups necessary for photographing the dif-
Fig. 9 Full arch frontal image Fig. 11 Full maxillary arch occlusal image
ferent types of dental views.
FULL-ARCH mirrors present a potential hazard and it is
Two types of full arch images are required, essential to avoid undue pressure on the soft
frontal and occlusal. tissues or hard tissues to prevent inadvertent
breakage or shattering, with obvious con-
Full arch: frontal view (Figs 8-9) sequences. The set-up is identical to that
1. Ask the patient to bite in centric described previously for full arch pictures,
occlusion with the following differences:
2. Frame picture with as many teeth as 1. Select an appropriate sized occlusal
possible in the composition, ideally mirror depending on the extent of
including the second molars, while mouth opening, and place gently in
ensuring that cheek retractors and the mouth. For the maxillary arch,
cotton wool rolls are not visible place mirror downwards, and for
3. Use the canines as the point of focus mandibular arch upwards, respectively
for ensuring maximum depth of 2. Request the patient to breathe through
field. The point of focus will depend their nose if possible and ask the
on the shape of the upper and lower dental assistant to constantly blow
arches, and if all teeth are not in warm dry air onto the mirror to
Fig. 12 Full mandibular arch occlusal set-up
focus, change the point of focus either prevent condensation
anterior or posterior to the canines 3. Focus onto the reflected image of the
4. Take pictures in various mandibular teeth on the mirror surface, framing as
positions as desired, including many teeth as possible. If mirror edges
centric occlusion, protrusive and or actual teeth are in the frame these
lateral excursions. can be subsequently cropped during
the image processing stage
Full arch: occlusal view 4. Using mirrors means that light
(Figs 10-13) intensity is diminished because it
Occlusal and lateral views require using has to travel a greater distance by
Fig. 13 Full mandibular arch occlusal image
intra-oral photographic mirrors. Intra-orally, being reflected off the mirror surface
BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009 153
PRACTICE
before it reaches and illuminates the
teeth. To compensate for the reduced
illumination, either increase the light
intensity or use a wider aperture, say
f16, to ensure correct exposure.
QUADRANT VIEWS: OCCLUSAL,
LINGUAL AND BUCCAL
The quadrant views record occlusal, lingual
(or palatal) and buccal (lateral) surfaces of
the teeth in an individual quadrant. The
procedure is identical to taking full arch
occlusal pictures, but the only difference
is that narrower lateral mirrors are substi-
tuted for the wider full arch occlusal mir-
rors to concentrate on a specific quadrant
or area. Also, unilateral cheek retractors are Fig. 14 Quadrant occlusal set-up Fig. 18 Quadrant palatal set-up
better suited to photographing quadrants
since they are less cumbersome than the
bilateral variety. As for all images using
mirrors, moisture control is essential and a
warm stream of air prevents condensation
on the mirror surface (Figs 14-15).
Both lingual and buccal images also
require narrower photographic mirrors. For
buccal images, the patient is asked to close Fig. 15 Quadrant occlusal image
their mouth so that the buccinator mus- Fig. 19 Quadrant palatal image
cles are relaxed, allowing room to place
the mirror into the cheeks. Once again,
unilateral cheek retractors may be less
cumbersome than larger bilateral types.
Images can be taken with the teeth fully
occluded or slightly parted to concentrate
on either the maxillary or mandibular
teeth (Figs 16-17).
For palatal images of the maxillary teeth,
the patient is asked to open the mouth and
tilt the head backwards while the mirror is
positioned to reflect the palatal aspects of
the teeth. For improved access, a supine
position is favoured for these types of
images (Figs 18-19).
Lingual surfaces of mandibular teeth
present two unique problems. Firstly, Fig. 16 Quadrant buccal set-up
the sublingual salivary gland openings Fig. 20 Quadrant lingual set-up
present a challenge for moisture control,
and secondly, the proximity of the tongue
causes difficulty for correct positioning of
a mirror. In addition, excessive pressure
may elicit a gagging reflex. Therefore for
these types of views, time, practice and
patience are necessary to achieve satisfac-
tory results (Figs 20-21).
MAGNIFICATION VIEWS
If only particular parts of the oral mucosa
Fig. 17 Quadrant buccal image Fig. 21 Quadrant lingual image
or teeth are of interest, it is best to compose
154 BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009
PRACTICE
the picture concentrating on the desired recommended for safety reasons as well as
areas. As a general rule, excess magnifica- those of limited access. For maximum com-
tion is detrimental to image quality. This is fort and depending on the site of the lesion,
because most macro lenses are incapable of the patient can either be seated or placed in
resolving beyond a 1:1 magnification, and the supine position. If not contra-indicated,
while it is possible to magnify objects to administration of topical or injectible local
greater than life size using various attach- anaesthesia helps alleviate pain and expe-
ments such as extension tubes and bel- dite the photographic session. When com-
lows, the result is a deterioration of image posing the picture, ensure that a healthy
quality. If a magnification greater than 1:1 area beyond or encircling the lesion is vis- Fig. 22 1:1 magnification image
is required it is better to enlarge the image, ible for comparison between healthy and
again within limits, using photo-editing diseased or pathologically altered tissue.
software. This is one of the reasons to start Also, to assess the size of a lesion, placing a
with a high quality image that is capable of periodontal probe or millimetre scale adja-
enlargement without loss of detail. cent to the pathology is helpful. The inten-
The major factor to consider when tak- sity of the photographic light needs to be
ing magnification views is that the depth increased to illuminate poorly lit posterior
of field is substantially reduced, sometimes regions. Finally, colour is important when
as small as 2 mm. This means that fewer photographing soft tissues, as changes from
teeth or parts of teeth are sharply focused, the norm often indicate present or previ-
Fig. 23 1:1 magnification image
not forgetting that the depth of field is in ous pathology. Therefore, calibrating with
front as well as behind the point of focus.
Therefore, to ensure maximum depth of
field it is advantageous to focus on a mid-
point. While framing of a picture is not
critical since the image can be cropped
afterwards, incorrect focusing is difficult
to rectify in photo-editing software. A cer-
tain degree of sharpening can be applied,
but if an image is captured out of focus
it will remain and appear out of focus no
matter the amount of manipulation. A tri-
pod is invaluable for precise focusing and
accurate framing. With a 1:1 magnification
and assuming normal tooth alignment, the
ideal point of focus is the distal aspect of
the maxillary central incisors for maximum
depth of field, which can also be verified
by using the depth of field preview but-
ton. Finally, if no indication is given on the
macro lens regarding the degree of mag-
nification, an easy method for ensuring a
1:1 magnification is when four maxillary Fig. 24 Set-up to capture dentine strata or enamel cracks. A silver reflector is placed on the
contra-lateral side of the flash to bounce light back onto the teeth
incisors occupy the entire viewfinder of a
35 mm DSLR camera (Figs 22-23).
ORAL MUCOSA
Photographing the oral mucosa and gingi-
vae is similar to photographing teeth but
requires minor modifications in technique.
Firstly, disease is painful and therefore
extra care is necessary to avoid trauma
when placing retractors and mirrors if the
tissues are inflamed. Mirrors are essential
if pathological lesions are located in the Fig. 25 Image taken with bilateral flashes Fig. 26 The same image as Figure 25, but
deep recesses of the oral cavity. However, showing the specular reflections that obscure photographed with the set-up described in
dentine strata and enamel cracks Figure 24, which reveals enamel cracks
if trismus is present mirrors are not
BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009 155
PRACTICE
an 18% grey card is advisable for precise
colour rendition.
TEXTURE, DENTINE LAYER
AND ENAMEL CRACKS
Pictures that reveal texture, dentine strata,
enamel cracks and perikymata are invalu-
able for a ceramist for visualising and
subsequently mimicking these characteri-
sations in artificial prostheses. The stand- Fig. 27 Dentine strata and enamel cracks are Fig. 31 A cursory shade analysis is carried
clearly discernible using the set-up described out pre-operatively before bleaching
ard lighting for intra-oral images, ie two in Figure 24
bilateral flashes mounted on either side of
the camera, is the ideal configuration for
capturing texture and lustre by specular
reflection off the enamel surface. However,
specular reflection masks the underlying
dentine colour and characterisations as
well as subtleties such as enamel cracks.
To visualise the latter, a silver or white card
is used to cover one of the bilateral lights,
acting as a reflector to bounce muted light Fig. 32 The patient in Figure 28 two weeks
after bleaching
from the opposite flash onto the teeth with-
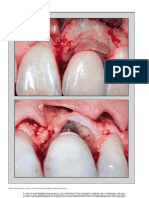
out specular reflection. This set-up reveals Fig. 28 The crown on the right central
incisor is devoid of the fracture line that is
the underlying dentine strata or intra- clearly visible in the enamel of the natural
enamel nuances (Figs 24-27). For this type left central incisor
of image, continuous light sources (LED or
dental operatory lights) are advantageous
because the reflector can be angled until
the desired structures, for example den-
tine layer or perikymata, are visible in the
viewfinder before taking the picture. Fig. 33 A detailed shade analysis is
performed pre-operatively with a single shade
Failure to clearly visualise and cap-
tab placed adjacent to a natural tooth
ture cracks or other characterisations
can result in artificial prostheses that
do not mimic adjacent natural teeth. In
Figure 28, the crown on the right central
incisor is devoid of an enamel crack, which
is clearly discernible on the natural left
central incisor.
TRANSLUCENCY
INCISAL AND INTERPROXIMAL
Enamel translucency is usually located at Fig. 34 A detailed shade analysis performed
Fig. 29 A black card is placed behind the after tooth preparation with a single shade
the incisal edges, cusps and interproximal teeth to highlight enamel translucency tab placed adjacent to the prepared tooth
regions of a tooth. The ability to map the
extent, degree and shape of translucencies
and mamelons is invaluable for communi-
cation between the clinician and ceramist
when fabricating artificial restorations.
The technique is as follows. A black card,
appropriately cut to size, is placed behind
the teeth to obscure the oral cavity and a
1:1 magnification is chosen to concentrate
on the desired teeth (Figs 29-30). Since
black is an optical contrast to the white Fig. 30 Enamel translucency is clearly visible Fig. 35 A detailed shade analysis performed
teeth, the cameras automatic metering in this image taken with the set-up described at the try-in stage using a single shade tab
in Figure 29 placed adjacent to the ceramic crown
may compensate by overexposing the
156 BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009
PRACTICE
image by or 1 f-stop. This will diminish
the visibility of translucency and it may
be necessary to override the metering by
underexposing to obtain correct exposure.
As for recording texture and lustre, a con-
tinuous lighting source is helpful to visu-
alise translucent areas by angling the light
until the translucent areas or mamelon dis-
tribution are visible in the viewfinder.
Fig. 36 A custom shade tab photographed Fig. 37 The same shade tab as in Figure 36,
SHADE ANALYSIS with electronic flash with a colour photographed in natural daylight with a colour
temperature of 5,500 K appears to match the temperature of 6,500 K, now has a higher
Absolute tooth shade comparisons are surrounding dentition value compared to the surrounding dentition
impossible with photography alone and must
be considered in combination with ocular
or instrumental analysis. However, relative
shade analysis is feasible with photography
and is a useful guide for the dental ceramist
for assessing the progress and extent of
bleaching relative to a shade guide.
Photographs for shade are taken using a
standard bilateral flash lighting set-up. As
for the oral mucosa, calibration with a grey
card is essential. The teeth should be moist
and not unduly desiccated, especially if
using a rubber dam, which causes inac-
curate shade assessment. While moisture
control is still necessary, saliva should be
encouraged to flow over the teeth, simu- Fig. 38 Inlay preparation in mandibular right Fig. 39 Cemented inlay in mandibular right
first molar first molar
lating a natural oral environment. The
patient is asked to hold the entire shade
guide for a cursory analysis, or to hold difficult photographs should be taken or a quadrant, unilateral cheek retrac-
individual tabs adjacent to the concerned with illumination of different colour tem- tors and narrow occlusal mirrors are the
teeth. Shade analysis with shade guides is peratures. This helps to avoid metamer- ideal choice. A rubber dam is an excellent
useful for assessing the extent of bleaching ism and facilities the matching procedure method of isolation, preventing condensa-
(Figs 31-32). For a more precise shade com- (Figs 36-37). tion on the mirrors as well as safeguarding
parison, a shade tab can be placed adjacent against ingestion or inhalation of dental
to a tooth that requires a crown. Ideally, POSTERIOR TEETH instruments. These types of dental images
shade analysis should be performed pre- Photographing posterior teeth is challeng- are ideal for using ring flash illumination,
operatively, after tooth preparation and at ing because of limited access and poor illu- which is intense, uniform and allows ease
the try-in stage, especially if the treatment mination, especially with restricted mouth of manipulation in limited access areas. As
objective is to whiten or brighten the shade opening or excess salivation. The set-up is previously mentioned, a slight overexpo-
of the definitive restorations (Figs 33-35). identical to that for photographing quad- sure may be necessary to compensate for
If the shade of a natural tooth does not rant occlusal images, described above. light being reflected off the mirror surface
match those in a standard shade guide it Therefore, a supine position is preferred, to illuminate the teeth (Figs 38-39).
may be necessary to fabricate a custom allowing better manipulation of intra-
1. Ahmad I. Digital dental photography. Part 4:
shade tab. As with conventional shade oral mirrors and ease of access for saliva Choosing a camera and accessories. Br Dent J 2009;
tabs, if the shade matching is proving ejectors. For photographing a few teeth 206: 575-581.
BRITISH DENTAL JOURNAL VOLUME 207 NO. 4 AUG 22 2009 157
You might also like
- The Swing Lock Denture Its Use in Conventional Removable Partial Denture Prosthodontics PDFDocument3 pagesThe Swing Lock Denture Its Use in Conventional Removable Partial Denture Prosthodontics PDFscott_c_kane100% (1)
- Esthetic Oral Rehabilitation with Veneers: A Guide to Treatment Preparation and Clinical ConceptsFrom EverandEsthetic Oral Rehabilitation with Veneers: A Guide to Treatment Preparation and Clinical ConceptsRichard D. TrushkowskyNo ratings yet
- Previsualization A Useful System For Truly Informed Consent To EstheticDocument11 pagesPrevisualization A Useful System For Truly Informed Consent To EstheticEvelina HaddadienNo ratings yet
- Digital Dental Photography Part 1Document5 pagesDigital Dental Photography Part 1Andreea StaicuNo ratings yet
- Oral Surgery - Forcep TechniqueDocument5 pagesOral Surgery - Forcep TechniqueSGNo ratings yet
- Practice: Interdisciplinary Management of Hypodontia: Oral SurgeryDocument5 pagesPractice: Interdisciplinary Management of Hypodontia: Oral SurgeryJawad TariqNo ratings yet
- Feature We Need To Know in Dentistry While Taking Photography For IntraoralDocument3 pagesFeature We Need To Know in Dentistry While Taking Photography For IntraoralInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Ijcmr 2634Document4 pagesIjcmr 2634Akanksha MahajanNo ratings yet
- Telescopic Dentures: An Overlooked TechnologyDocument3 pagesTelescopic Dentures: An Overlooked TechnologyarchanglsNo ratings yet
- Post Insertion Complaints in Complete Dentures - A Never Ending SagaDocument8 pagesPost Insertion Complaints in Complete Dentures - A Never Ending SagaKrupali JainNo ratings yet
- Treatment Planning of The Edentulous Mandible PDFDocument9 pagesTreatment Planning of The Edentulous Mandible PDFHugoMoralesTecnicoDentalNo ratings yet
- ARTICULO 2. Selection of TeethDocument8 pagesARTICULO 2. Selection of Teethnaty yepesNo ratings yet
- The International Journal of Periodontics & Restorative DentistryDocument8 pagesThe International Journal of Periodontics & Restorative DentistryjonvargasNo ratings yet
- Gingival Retraction Techniques: A Review: DentistryDocument9 pagesGingival Retraction Techniques: A Review: DentistrySahana RangarajanNo ratings yet
- The State of Fixed Prosthodontic Impressions: Room For ImprovementDocument4 pagesThe State of Fixed Prosthodontic Impressions: Room For ImprovementErika MuñozNo ratings yet
- Serial Extraction: 20 Years of Follow-UpDocument7 pagesSerial Extraction: 20 Years of Follow-UpDr HuanNo ratings yet
- Presurgical NAM - 2 CazuriDocument8 pagesPresurgical NAM - 2 CazuriDiana PredaNo ratings yet
- Immediate Dental Implant 1Document13 pagesImmediate Dental Implant 1alkhalijia dentalNo ratings yet
- Dental Implant Systems: User ManualDocument8 pagesDental Implant Systems: User ManualPhoebe DavidNo ratings yet
- Vinyl Polysiloxane Impression Material in Removable Prosthodontics Part 1: Edentulous ImpressionsDocument9 pagesVinyl Polysiloxane Impression Material in Removable Prosthodontics Part 1: Edentulous ImpressionsLuis Salvador Martinez Estrada0% (1)
- Radiographic Diagnosis of Root Resorption in Relation To OrthodonticsDocument7 pagesRadiographic Diagnosis of Root Resorption in Relation To OrthodonticsnomanNo ratings yet
- Eview: Retentive Aids in Maxillofacial Prosthodontics - A ReviewDocument5 pagesEview: Retentive Aids in Maxillofacial Prosthodontics - A ReviewjoephinNo ratings yet
- Maxillofacial Prosthesis &materialsDocument7 pagesMaxillofacial Prosthesis &materialsطبطب صالحNo ratings yet
- ART4Document6 pagesART4Madalina MihailaNo ratings yet
- 1 s2.0 S1938973608001062 MainDocument17 pages1 s2.0 S1938973608001062 MainWilliam CorderoNo ratings yet
- Reestablishing Esthetics With Extracted Teeth On A Mandibular Anterior Edentulous Area A Case ReportDocument3 pagesReestablishing Esthetics With Extracted Teeth On A Mandibular Anterior Edentulous Area A Case ReportMuhasbirNo ratings yet
- Dentistry 101Document21 pagesDentistry 101ziad khanNo ratings yet
- Pulpectomy of Deciduous TeethDocument9 pagesPulpectomy of Deciduous TeethSausan HazimahNo ratings yet
- Prosthodontic Rehabilitation of Cleft Lip and Palate With Presurgical Nasoalveolar MoldingDocument3 pagesProsthodontic Rehabilitation of Cleft Lip and Palate With Presurgical Nasoalveolar MoldingVasantha RajanNo ratings yet
- Intraoral Radiography: Positioning and Radiation Protection: 4 CE CreditsDocument11 pagesIntraoral Radiography: Positioning and Radiation Protection: 4 CE Creditsდიმიტრი კოლოტაურიNo ratings yet
- Diagnostic Records (Dr. Ahmed)Document7 pagesDiagnostic Records (Dr. Ahmed)Mohammed JaberNo ratings yet
- CHAPTER 13 - Preparation of The Mouth For R - 2011 - McCracken S Removable Parti PDFDocument20 pagesCHAPTER 13 - Preparation of The Mouth For R - 2011 - McCracken S Removable Parti PDFFlorin Razvan CurcăNo ratings yet
- Internet-Based Prevention: Monitoring ToothbrushingDocument3 pagesInternet-Based Prevention: Monitoring ToothbrushingoanaNo ratings yet
- Prosthetic Options For Implant-Supported Overdentures - October 2015 - Inside DentistryDocument4 pagesProsthetic Options For Implant-Supported Overdentures - October 2015 - Inside Dentistrymaithilieaggarwalmds2124No ratings yet
- Immediate Complete Denture ImpressionsDocument12 pagesImmediate Complete Denture ImpressionsToDownload81No ratings yet
- Ejed 15 3 Staehler p288Document18 pagesEjed 15 3 Staehler p288snkidNo ratings yet
- Impressions in Implant Dentistry: S. Bhakta, J. Vere, I. Calder and R. PatelDocument7 pagesImpressions in Implant Dentistry: S. Bhakta, J. Vere, I. Calder and R. Pateleswar1105820% (1)
- Operative Lecture 1Document10 pagesOperative Lecture 1khalid khalidNo ratings yet
- (IJPRD) GLUCKMAN 2017 - Partial Extraction Therapies Part 2 PDFDocument11 pages(IJPRD) GLUCKMAN 2017 - Partial Extraction Therapies Part 2 PDFFelipeGuzanskyMilaneziNo ratings yet
- Surgical Forcep Techniques PDFDocument4 pagesSurgical Forcep Techniques PDFSyifaa AndrianiNo ratings yet
- Surgical Forcep TechniquesDocument4 pagesSurgical Forcep TechniquesSyifaa AndrianiNo ratings yet
- Identification of Complete Denture Problems: A Summary: ProstheticsDocument7 pagesIdentification of Complete Denture Problems: A Summary: ProstheticsFaheemuddin MuhammadNo ratings yet
- Implant Rehabilitation in The Edentulous Jaw: The "All-On-4" Immediate Function ConceptDocument8 pagesImplant Rehabilitation in The Edentulous Jaw: The "All-On-4" Immediate Function ConceptAnonymous i7fNNiRqh2No ratings yet
- Complete Dentures - Part 2Document7 pagesComplete Dentures - Part 2Lee MulderNo ratings yet
- Ement of Hollow Cheeks With Undetachable Hollow Cheek Plumper: A Case PDFDocument6 pagesEment of Hollow Cheeks With Undetachable Hollow Cheek Plumper: A Case PDFAnita PrastiwiNo ratings yet
- Post Insertion Problems For Complete Denture and Their ManagementDocument8 pagesPost Insertion Problems For Complete Denture and Their ManagementTaha AlaamryNo ratings yet
- A Standardized Approach To Extra-Oral and Intra-Oral Digital PhotographyDocument17 pagesA Standardized Approach To Extra-Oral and Intra-Oral Digital PhotographyCarolina AssisNo ratings yet
- Guidelines For Immediate ImplanttDocument11 pagesGuidelines For Immediate ImplanttAhmed BadrNo ratings yet
- 23 2 157 159 PDFDocument4 pages23 2 157 159 PDFWulanNo ratings yet
- #1 Rationale ImplantDocument5 pages#1 Rationale Implantsohaib197No ratings yet
- BDJ Toothwear 2Document10 pagesBDJ Toothwear 2sdgoihNo ratings yet
- Incisor Alignment With The Inman Aligner: C S W & WDocument13 pagesIncisor Alignment With The Inman Aligner: C S W & WShaghayegh SahraNo ratings yet
- MANUAL FOR OPERATIVE DENTISTRY - Xa - Yimg.com (PDFDrive)Document169 pagesMANUAL FOR OPERATIVE DENTISTRY - Xa - Yimg.com (PDFDrive)cvpk prasannaNo ratings yet
- Mouth Preparation - PDF 161301Document127 pagesMouth Preparation - PDF 161301S ل DentistNo ratings yet
- DOH Equip Oral Maxillofacial Form ASC OMS LTO TRDocument7 pagesDOH Equip Oral Maxillofacial Form ASC OMS LTO TRal gulNo ratings yet
- Preventing The Negative Sequelae of Tooth Extraction: DirectionsDocument2 pagesPreventing The Negative Sequelae of Tooth Extraction: DirectionsrizkiNo ratings yet
- Capelli 2012Document15 pagesCapelli 2012medNo ratings yet
- Hollow Maxillary DentureDocument5 pagesHollow Maxillary DentureDeasireeNo ratings yet
- Orthodontically Induced Inflammatory Root ResorptionDocument15 pagesOrthodontically Induced Inflammatory Root ResorptionmutansNo ratings yet
- Understanding Problems and Failures in TSFDP: Peer Review StatusDocument7 pagesUnderstanding Problems and Failures in TSFDP: Peer Review StatusbkprosthoNo ratings yet
- Infection Control Procedures in Commercial Dental Laboratories in JordanDocument5 pagesInfection Control Procedures in Commercial Dental Laboratories in JordanbkprosthoNo ratings yet
- 1801cei Bernie Web PDFDocument10 pages1801cei Bernie Web PDFbkprosthoNo ratings yet
- Jced 10 E75Document6 pagesJced 10 E75bkprosthoNo ratings yet
- Infection PreventionDocument48 pagesInfection PreventionbkprosthoNo ratings yet
- Alzheimer's Disease and Oral CareDocument5 pagesAlzheimer's Disease and Oral CarebkprosthoNo ratings yet
- Jaw Relation Records For Fixed ProsthodonticsDocument16 pagesJaw Relation Records For Fixed ProsthodonticsbkprosthoNo ratings yet
- Digital Dental Photography. Part 7: Extra-Oral Set-Ups: I. AhmadDocument8 pagesDigital Dental Photography. Part 7: Extra-Oral Set-Ups: I. AhmadbkprosthoNo ratings yet
- Choosing and Using Permanent Lu Ting CementsDocument8 pagesChoosing and Using Permanent Lu Ting CementsbkprosthoNo ratings yet
- Classification of Removable Partial DentureDocument17 pagesClassification of Removable Partial Denturebkprostho100% (1)
- DR Haroon Rashid Baloch Assistant Professor Department of ProsthodonticsDocument52 pagesDR Haroon Rashid Baloch Assistant Professor Department of ProsthodonticsbkprosthoNo ratings yet
- Endodontic Working WidthDocument13 pagesEndodontic Working WidthbkprosthoNo ratings yet
- Safeguarding Children in Dentistry: 2. Do Paediatric Dentists Neglect Child Dental Neglect?Document6 pagesSafeguarding Children in Dentistry: 2. Do Paediatric Dentists Neglect Child Dental Neglect?bkprosthoNo ratings yet
- An Alternative Technique Mandibular Advancement Prosthesis FabricationDocument5 pagesAn Alternative Technique Mandibular Advancement Prosthesis FabricationbkprosthoNo ratings yet
- IckDocument6 pagesIckbkprosthoNo ratings yet
- Introduction To Complete DenturesDocument65 pagesIntroduction To Complete DenturesbkprosthoNo ratings yet
- Intra Orbital ImplantDocument7 pagesIntra Orbital ImplantbkprosthoNo ratings yet
- Felton 2016 Journal of ProsthodonticsDocument16 pagesFelton 2016 Journal of Prosthodonticsbkprostho100% (1)
- Dent Update 2008 35 636-641 PDFDocument5 pagesDent Update 2008 35 636-641 PDFbkprosthoNo ratings yet
- Ddrive Transmission ReportDocument43 pagesDdrive Transmission Reportelah150% (2)
- A-ZKD-13 (ZKD-59 (A) ) : Mechanical ParameterDocument1 pageA-ZKD-13 (ZKD-59 (A) ) : Mechanical Parameterwissam zaatuorNo ratings yet
- Zhou 2019 IOP Conf. Ser. Earth Environ. Sci. 252 032144Document11 pagesZhou 2019 IOP Conf. Ser. Earth Environ. Sci. 252 032144Dante FilhoNo ratings yet
- Iec TR 62343-6-8-2011Document14 pagesIec TR 62343-6-8-2011Amer AmeryNo ratings yet
- Institute of Metallurgy and Materials Engineering Faculty of Chemical and Materials Engineering University of The Punjab LahoreDocument10 pagesInstitute of Metallurgy and Materials Engineering Faculty of Chemical and Materials Engineering University of The Punjab LahoreMUmairQrNo ratings yet
- Driver DST-4812 For 7.2 KG CMDocument5 pagesDriver DST-4812 For 7.2 KG CMWWW.150775.BUGME.PWNo ratings yet
- MS 005 For DUCT FABRICATION - INSULATION & INSTALLATION REV-1Document21 pagesMS 005 For DUCT FABRICATION - INSULATION & INSTALLATION REV-1vusal huseynli100% (2)
- Digital Logic DesignDocument38 pagesDigital Logic DesignAri BaderNo ratings yet
- Tsang Mui Millennium School 2019-2020 English Worksheet: Fill in The Blanks With The Correct Form of The VerbsDocument46 pagesTsang Mui Millennium School 2019-2020 English Worksheet: Fill in The Blanks With The Correct Form of The VerbscocoyipNo ratings yet
- Anil Singh Rathore: Career HighlightsDocument4 pagesAnil Singh Rathore: Career HighlightsHRD CORP CONSULTANCYNo ratings yet
- Vanilla Farming: The Way Forward: July 2019Document6 pagesVanilla Farming: The Way Forward: July 2019mituNo ratings yet
- Phase-Locked Loop Independent Second-Order Generalized Integrator For Single-Phase Grid SynchronizationDocument9 pagesPhase-Locked Loop Independent Second-Order Generalized Integrator For Single-Phase Grid SynchronizationGracella AudreyNo ratings yet
- SCM 025-108 M2Document8 pagesSCM 025-108 M2kazdanoNo ratings yet
- 4th Six Weeks RecoveryDocument8 pages4th Six Weeks RecoveryAshley HighNo ratings yet
- Atlantis Is Discovered - Atlantis in Middle Danubian Depression (Pannonian Basin) A New Location of Atlantis IslandDocument31 pagesAtlantis Is Discovered - Atlantis in Middle Danubian Depression (Pannonian Basin) A New Location of Atlantis Islandpaulct2004721260% (10)
- Elements or Appurtenances of The Stilling BasinsDocument21 pagesElements or Appurtenances of The Stilling BasinsAhmad PshtiwanNo ratings yet
- Safety Data Sheet: Section 1. Identification Jotun Essence Easy CleanDocument11 pagesSafety Data Sheet: Section 1. Identification Jotun Essence Easy CleanHồng PhongNo ratings yet
- Sorsogon State College Engineering & ArchitectureDocument11 pagesSorsogon State College Engineering & ArchitectureArianne Mae De Vera GallonNo ratings yet
- L15 - Parallel Magnetic CircuitsDocument6 pagesL15 - Parallel Magnetic CircuitsParikshit MishraNo ratings yet
- Computer From ScratchDocument6 pagesComputer From ScratchPaul NavedaNo ratings yet
- Module IiDocument5 pagesModule IiFahmi PrayogiNo ratings yet
- Orona Fault CodesDocument19 pagesOrona Fault CodesDanushka Bandara100% (1)
- Greyhound Free Patt.Document14 pagesGreyhound Free Patt.claire_garlandNo ratings yet
- Case Study Mental HealthDocument12 pagesCase Study Mental Healthapi-603895785No ratings yet
- Flap Designs For Flap Advancement During Implant Therapy A Systematic Review 2016 PDFDocument8 pagesFlap Designs For Flap Advancement During Implant Therapy A Systematic Review 2016 PDFRohit ShahNo ratings yet
- L23 - Axial Flow CompressorDocument17 pagesL23 - Axial Flow CompressorRohan GuptaNo ratings yet
- EPP V6 - V7 - ETS - Removal Switch - Sensor Reactivation V12Document15 pagesEPP V6 - V7 - ETS - Removal Switch - Sensor Reactivation V12Rabin TinkariNo ratings yet
- 510 1453 1 PB Tiang ReklameDocument6 pages510 1453 1 PB Tiang ReklameGunaedy UtomoNo ratings yet
- Practice Exam 3 KEY (Solutions)Document13 pagesPractice Exam 3 KEY (Solutions)joseNo ratings yet
- Management Science - Lecture 2Document9 pagesManagement Science - Lecture 2Nicole SallanNo ratings yet
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 4.5 out of 5 stars4.5/5 (82)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (32)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (3)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (4)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (254)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- To Explain the World: The Discovery of Modern ScienceFrom EverandTo Explain the World: The Discovery of Modern ScienceRating: 3.5 out of 5 stars3.5/5 (51)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (46)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (60)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4.5 out of 5 stars4.5/5 (6)
- How to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingFrom EverandHow to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingRating: 1 out of 5 stars1/5 (1)