Professional Documents
Culture Documents
DX Thorax
Uploaded by
dwi adinda0 ratings0% found this document useful (0 votes)
6 views2 pagesOriginal Title
DX Thorax.docx
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
6 views2 pagesDX Thorax
Uploaded by
dwi adindaCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 2
1.
Assessment and Diagnosis
Pneumothorax is assessed and diagnosed with the following:
Thoracic CT: Studies show that CT is more sensitive than x-ray in detecting
thoracic injuries, lung contusion, hemothorax, and pneumothorax. Early CT may
influence therapeutic management.
Chest x-ray: Reveals air and/or fluid accumulation in the pleural space; may
show shift of mediastinal structures (heart).
ABGs: Variable depending on degree of compromised lung function, altered
breathing mechanics, and ability to compensate. Paco2 occasionally elevated.
Pao2 may be normal or decreased; oxygen saturation usually decreased.
Thoracentesis: Presence of blood/serosanguineous fluid indicates hemothorax.
Hb: May be decreased, indicating blood loss.
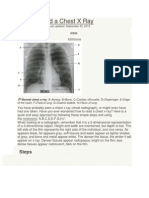
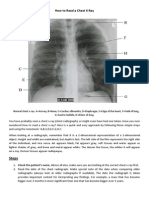
2. Chest radiograph assessment using ABCDEFGHI
ABCD can be used to guide a systematic interpretation of chest x-rays.
Assessment of quality / Airway
The quality of the image can be assessed using the mnemonic PIER:
position: is this a supine AP file? PA? Lateral?
inspiration: count the posterior ribs. You should see 10 to 11 ribs with a
good inspiratory effect
exposure: well-exposed films have good lung detail and an outline of the
spinal column
rotation: the space between the medial clavicle and the margin of the
adjacent vertebrae should be roughly equal to each other; look for
indwelling lines or objects
Bones and soft tissues]
Scan the bones for symmetry, fractures, osteoporosis, and lesions. Evaluate the
soft tissues for foreign bodies, swelling, and subcutaneous air.
Cardiac
Evaluate the heart size: the heart should be <50% of the chest diameter on PA
films and <60% on AP films. Check for the heart shape, calcifications, and
prosthetic valves.
Diaphragm
Check the hemidiaphragms for position (the right is commonly slightly higher
than the left due to the liver) and shape (may be flattened bilaterally in chronic
asthma or emphysema, or unilaterally in case of tension pneumothorax or foreign
body aspiration). Look below the diaphragm for free gas.
You might also like
- Chest X-Ray Interpretation A Structured Approach Radiology OSCEDocument1 pageChest X-Ray Interpretation A Structured Approach Radiology OSCEValentina SepúlvedaNo ratings yet
- How To Read A Chest X RayDocument20 pagesHow To Read A Chest X RayJasvin Sidhu100% (1)
- Chest X-Ray InterpretationDocument67 pagesChest X-Ray Interpretationabhirajkale95% (20)
- Chest X-Ray ReviewDocument145 pagesChest X-Ray ReviewHamid ShaalanNo ratings yet
- How To Read A Chest X RayDocument11 pagesHow To Read A Chest X RayHilmia Fahma100% (2)
- Chest X-Ray CXR InterpretationDocument13 pagesChest X-Ray CXR InterpretationduncanNo ratings yet
- Chest X RayDocument61 pagesChest X RayP Vinod Kumar100% (1)
- Emergency UltrasoundDocument32 pagesEmergency UltrasoundChoga ArlandoNo ratings yet
- Interpretation Chest X RayDocument127 pagesInterpretation Chest X RayVimal NishadNo ratings yet
- Basics of Chest X-RayDocument44 pagesBasics of Chest X-RayMelissa Aina Mohd YusofNo ratings yet
- Chest X-ray Interpretation for Radiographers, Nurses and Allied Health ProfessionalsFrom EverandChest X-ray Interpretation for Radiographers, Nurses and Allied Health ProfessionalsNo ratings yet
- Chest X-RayDocument101 pagesChest X-RayYuke04No ratings yet
- Basic Chest X-Ray Interpretation (5minutes Talk) : DR - Alemayehu (ECCM R1)Document35 pagesBasic Chest X-Ray Interpretation (5minutes Talk) : DR - Alemayehu (ECCM R1)Alex beharuNo ratings yet
- Chest X - Ray InterpretationDocument147 pagesChest X - Ray InterpretationFcsieka FcseikaNo ratings yet
- Interpreting The Chest Radio Graph Friendly)Document9 pagesInterpreting The Chest Radio Graph Friendly)Vagner BorgesNo ratings yet
- Basics of Chest X-RayDocument44 pagesBasics of Chest X-RayvmamikonNo ratings yet
- Chest RadiographyDocument65 pagesChest RadiographyMunish Dogra100% (1)
- Diagnostic Imaging - 8 - Radiological Pathology - Lung Pathologies and Radiology in Specific Cases - Prof - Dr.i̇smet TAMERDocument35 pagesDiagnostic Imaging - 8 - Radiological Pathology - Lung Pathologies and Radiology in Specific Cases - Prof - Dr.i̇smet TAMERAly MssreNo ratings yet
- (RADIO 250) LEC 06 Chest RadiologyDocument10 pages(RADIO 250) LEC 06 Chest Radiologyjmhinos4833No ratings yet
- Plain Chest X RayDocument154 pagesPlain Chest X RaySamuel Gamadey100% (3)
- Two-Dimensional and M-Mode Echocardiography for the Small Animal PractitionerFrom EverandTwo-Dimensional and M-Mode Echocardiography for the Small Animal PractitionerRating: 5 out of 5 stars5/5 (1)
- Interpretasi Foto DadaDocument137 pagesInterpretasi Foto DadaRofi Irman100% (1)
- Cara Baca Foto ThoraxDocument23 pagesCara Baca Foto ThoraxNofilia Citra CandraNo ratings yet
- Chest Radiograph Assessment Using ABCDEFGHIDocument2 pagesChest Radiograph Assessment Using ABCDEFGHIHector SerranoNo ratings yet
- CXR Pnemonic ABCDEFGHIDocument2 pagesCXR Pnemonic ABCDEFGHIAngela PuspitaNo ratings yet
- CXR Interpretation WriteupDocument32 pagesCXR Interpretation WriteupArhanNo ratings yet
- Chest X-Ray (CXR) Interpretation 2Document30 pagesChest X-Ray (CXR) Interpretation 2NaveedNo ratings yet
- Radiological Investigation of Chest. The Radiological Semiotics of The Chest PathologyDocument169 pagesRadiological Investigation of Chest. The Radiological Semiotics of The Chest PathologyВладимир КурпаянидиNo ratings yet
- Chest Xray BasicsDocument47 pagesChest Xray BasicsPartha GanesanNo ratings yet
- Chest X-Ray: Confirm DetailsDocument14 pagesChest X-Ray: Confirm DetailsNosheen HafeezNo ratings yet
- Thoracic Imaging Radiographic BasicsDocument130 pagesThoracic Imaging Radiographic BasicsIsak ShatikaNo ratings yet
- Radiography of The Thorax: BY Abubakar ADocument70 pagesRadiography of The Thorax: BY Abubakar AJameeluh TijjanyNo ratings yet
- ABC ChestDocument4 pagesABC ChestSintounNo ratings yet
- Chest X RayDocument24 pagesChest X RayAman SurahmanNo ratings yet
- 2 1 Diseases of The Respiratory System Radiological Pathology DRDocument43 pages2 1 Diseases of The Respiratory System Radiological Pathology DRNatnael GetahunNo ratings yet
- ANA 412 Respiratory System ImagingDocument48 pagesANA 412 Respiratory System Imagingconqueror12345678No ratings yet
- Chest X-Ray GuideDocument26 pagesChest X-Ray GuideRizky Ayu WirdaningsiNo ratings yet
- How To Read A Chest X-RayDocument3 pagesHow To Read A Chest X-RayKristina KostadinovskaNo ratings yet
- Juanico, Clareen Mae (Assignment)Document3 pagesJuanico, Clareen Mae (Assignment)Clareen JuanicoNo ratings yet
- How To Read Chest X-RayDocument4 pagesHow To Read Chest X-RaydrrajkumarsoniNo ratings yet
- Basic Chest Imaging and Heart FailureDocument57 pagesBasic Chest Imaging and Heart FailureKiaa auliaNo ratings yet
- Chest Xray PDFDocument8 pagesChest Xray PDFOvi SharmaNo ratings yet
- How To Read X-RayDocument8 pagesHow To Read X-RayPeterson Wachira HscNo ratings yet
- Chest AssessmentDocument5 pagesChest Assessmentرحاب المريNo ratings yet
- Dr. Yash Kumar Achantani MBBS, MD (Radio-Diagnosis)Document24 pagesDr. Yash Kumar Achantani MBBS, MD (Radio-Diagnosis)Mayuri DhanushwarNo ratings yet
- Emad Efat Chest CT BestDocument260 pagesEmad Efat Chest CT Bestdr Mohit TaylorNo ratings yet
- Chest X Ray - zp162335Document48 pagesChest X Ray - zp162335Kushmakar VarshneyNo ratings yet
- Imaging - Lecture 2 (Chest Radiography)Document8 pagesImaging - Lecture 2 (Chest Radiography)Adham MohamedNo ratings yet
- Chest Introduction: Technical AdequacyDocument28 pagesChest Introduction: Technical AdequacyAnshul JainNo ratings yet
- X RayDocument18 pagesX RayAbdul Ghaffar AbdullahNo ratings yet
- DX Imaging 1 MT and FinalDocument24 pagesDX Imaging 1 MT and FinalRaymondNo ratings yet
- Reading A Chest X-RayDocument2 pagesReading A Chest X-RaySabrinaAyuPutriNo ratings yet
- How To Read CXR EditedDocument66 pagesHow To Read CXR EditedSurgicalgownNo ratings yet
- Normal Chest RadiographDocument108 pagesNormal Chest RadiographVenu Madhav100% (1)
- CXR Interpretation Checklist ShortDocument1 pageCXR Interpretation Checklist ShortKatalinNo ratings yet
- Respirasi As Agust 2017Document37 pagesRespirasi As Agust 2017Rizki KurniawanNo ratings yet
- RESPIRASI AS Agust 2017 PDFDocument37 pagesRESPIRASI AS Agust 2017 PDFThika AlfredoNo ratings yet
- Immediate Life Support for healthcare Practitioners: A Step-By-Step GuideFrom EverandImmediate Life Support for healthcare Practitioners: A Step-By-Step GuideNo ratings yet
- Proposedas A Task Subjects Basic Science NursingDocument20 pagesProposedas A Task Subjects Basic Science Nursingdwi adindaNo ratings yet
- WOC CaseDocument4 pagesWOC Casedwi adindaNo ratings yet
- Nursing of Urinary System: Answer Case StudyDocument6 pagesNursing of Urinary System: Answer Case Studydwi adindaNo ratings yet
- Therapy Reflexology: 1.1. DefinitionDocument10 pagesTherapy Reflexology: 1.1. Definitiondwi adindaNo ratings yet
- Amniotic Fluid Embolism (Etiology and Pathophysiology)Document2 pagesAmniotic Fluid Embolism (Etiology and Pathophysiology)dwi adindaNo ratings yet
- WOC - Nephrotic SyndromeDocument4 pagesWOC - Nephrotic Syndromedwi adindaNo ratings yet
- WOC of Premature Ruptuid of MembraneDocument2 pagesWOC of Premature Ruptuid of Membranedwi adindaNo ratings yet