Professional Documents
Culture Documents
Hypothyroidism AIIMS PDF
Hypothyroidism AIIMS PDF
Uploaded by
abhivnairOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Hypothyroidism AIIMS PDF
Hypothyroidism AIIMS PDF
Uploaded by
abhivnairCopyright:
Available Formats
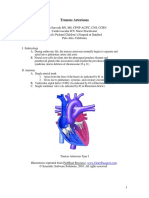
AIIMS- NICU protocols 2010
Congenital Hypothyroidism
Vandana Jain1, Ramesh Agarwal2, Ashok Deorari3, Vinod Paul3
1,2
Assistant Professor, 3Professor
1
Division of Pediatric Endocrinology, 2,3Division of Neonatology,
Department of Pediatrics
All India Institute of Medical Sciences
Ansari Nagar, New Delhi –110029
Address for correspondence:
Dr Ramesh Agarwal
Assistant Professor
Department of Pediatrics
All India Institute of Medical Sciences
Ansari Nagar, New Delhi 110029
Email: aranag@rediffmail.com
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Abstract
Congenital Hypothyroidism (CH) is one of the most common preventable
causes of mental retardation with a worldwide incidence of 1: 3000-4000 live
births. Ideally universal screening at 3-4 days of age should be done for
detecting CH. Abnormal values on screening should be confirmed by a venous
sample (using age appropriate cut-offs). Term as well as preterm infants with
low T4 and elevated TSH should be started on L-thyroxine at a dose of 10-
15µg/ kg/ day as soon as the diagnosis is made. Regular monitoring should be
done to ensure that TSH is suppressed to within normal range and T4 is in the
upper half of normal range. The outcome of CH depends on the time of
initiation of therapy and the dose of L-thyroxine used with the best outcome in
infants started on treatment before 2 weeks of age with a dose > 9.5µg/ kg/
day.
Keywords: congenital hypothyroidism, L-thyroxine, newborn
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Congenital Hypothyroidism (CH) is one of the most common preventable
causes of mental retardation. The worldwide incidence is 1:3000-4000 live
births and the estimated incidence in India is 1:2500-2800 live births. 1 Thyroid
dysgenesis is the commonest cause accounting for 75-80% of all cases of CH.
Embryology and physiology of the thyroid in the fetus – The thyroid
gland originates as a proliferation of endodermal epithelial cells at 3 to 4
weeks of gestation. Synthesis and secretion of thyroxine (T4) and
triiodothyronine (T3) starts from 12 weeks of gestation. Hypothalamic-
pituitary-thyroid (HPT) axis begins to develop in the first trimester and
thyrotropin-releasing hormone (TRH) and thyroid stimulating hormone (TSH)
are also detectable by the end of first trimester. However, the activity of HPT
axis is low with insufficient production of thyroid hormones by the fetus until
about 18-20 weeks of gestation. In the second half of gestation, the T4 and
TSH levels increase progressively. In the first trimester, the fetus is dependent
on transplacental passage of thyroid hormones.
In the hypothyroid fetus, this transplacental passage of maternal thyroid
hormones is critical for neuroprotection throughout the intra-uterine life. The
cord blood T4 concentration at birth in infants who are unable to synthesize T4
is 20-30% of normal. In addition, there is increased conversion of T4 to T3 in
the fetal brain by the activity of type 2 deiodinase, resulting in increased local
availability of the physiologically more important T3. Near normal cognitive
outcome is possible in even the most severely affected infants with CH as long
as postnatal therapy is initiated early in optimum doses and maternal thyroid
function is normal. In contrast, when both maternal and fetal hypothyroidism
are present as in severe iodine deficiency, there is a significant impairment in
neuro-intellectual development despite adequate therapy soon after birth.2
Similarly, maternal subtle or overt hypothyroidism during pregnancy have also
been seen to have an adverse impact on the neuro-intellectual outcome of the
offspring.3
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Neonatal physiology - After birth, the term baby experiences a surge of TSH
as a physiological response to cold environment. The TSH concentration rises
to 60-80 mU/L within 30 to 60 minutes after delivery and falls quickly in the
first 24 hours to about 20 mU/L, followed by a slower decrease to below 10
mU/L after the first postnatal week. The rise in TSH initiates increase of T4 and
free T4 to peak levels of 17 µg/dL and 3.5 ng/dL, respectively at 24 to 36 hours
after birth with a slow decline to adult values over 4-5 weeks. Preterm infants
demonstrate a similar but blunted response due to HPT axis immaturity.
Etiology of CH
CH can be permanent or transient. Thyroid dysgenesis is the commonest cause
of permanent CH affecting 1 in 4000 live births. It is usually sporadic with a 2:1
female to male preponderance. Some of the genes proposed as operative in
dysgenesis have been recently identified as TITF1, TITF2, PAX8 and TSHR.4
(Table I )
Thyroid hormone synthetic defects account for 10-15% of all cases. These are
inherited as autosomal recessive disorders. The defect can lie in iodide
trapping or organification, iodotyrosine coupling or deiodination and
thyroglobulin synthesis or secretion. The commonest of these is a defect in the
thyroid peroxidase (TPO) activity leading to impaired oxidation and
organification of iodide to iodine. These disorders usually result in goitrous
hypothyroidism. Iodine deficiency is responsible for endemic cretinism and
hypothyroidism in some regions of India.
Hypothalamic-pituitary hypothyroidism has an estimated incidence of 1 in
50,000. It may be isolated or associated with deficiency of other pituitary
hormones and present with hypoglycemia and microphallus. Transient
hypothyroidism due to transplacental transfer of TSH binding inhibitory
immunoglobulins (TBII) from mothers with autoimmune thyroid disease is seen
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
in 1: 50,000 births. Their effect wanes off by 3-6 months in the majority but
may last up to 9 months. Exposure to iodine in sick preterm infants (e.g.
application of povidone iodine for skin disinfection (Wolff-Chaikoff effect) or
intake of iodine containing expectorants by pregnant mothers can also induce
transient hypothyroidism.
Transient hypothyroxinema of prematurity refers to low serum concentration of
thyroid hormones in up to 85% of preterm infants in early postnatal life as
compared to term infants. This reflects the underdevelopment of the HPT axis,
which cannot compensate for the loss of maternal thyroid hormone in preterm
infants. The normal levels of fT4 and TSH in preterm infants are presented in
Table 2.5 There has been a concern that transient hypothyroxinemia is
associated with adverse neurodevelopmental outcomes and decreased survival
in affected infants.6
Sick euthyroid syndrome reflects suppression of the pituitary’s response to
TRH, with inappropriately low TSH concentrations in the context of low T3 and
in the more severe cases, low T4 concentrations.
Diagnosis
Newborn screening- Ideally universal screening at 3-4 days of age should be
done for detecting CH. Alternatively cord blood can also be used if screening is
being done only for CH and not other inborn errors of metabolism. Universal
newborn screening is currently being done in many parts of the world including
Western Europe, North America, Japan, Australia, and parts of Eastern Europe,
Asia, South America, and Central America. Three approaches are being used
for screening:
1. Primary TSH, back upT4
2. Primary T4, back up TSH
3. Concomitant T4 and TSH
In the first approach, TSH is measured first. T4 is measured only if TSH is >
20mu/L. This approach is likely to miss central hypothyroidism, thyroid binding
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
globulin deficiency and hypothyroxinema with delayed elevation of TSH. In the
second approach, T4 is checked first and if low TSH is also checked. This is
likely to miss milder/ subclinical cases of CH in which T4 is initially normal with
elevated TSH. Concomitant measurement of T4 and TSH is the most sensitive
approach but incurs a higher cost.7 Screening programs use either percentile
based cut-offs (e.g, T4 below 10th centile or TSH above 90th centile or absolute
cut-offs such as T4 < 6.5 ug/dL and TSH > 20mu/L.
Abnormal values on screening should always be confirmed by a
venous sample (using age appropriate cut-offs given in Table 3 8-10).
Most centers initiate treatment after drawing the infants’ sample if
TSH > 30 mu/L or T4 is low and the decision to continue or withhold
treatment is taken after obtaining the blood report. For intermediate
screening values of TSH, with normal T4 (if available), the treatment
is initiated only after confirmation of diagnosis based on the blood
report. Among infants with proven CH, TSH is > 50 mu/L in 90% and T4 is <
6.5 ug/dL in greater than 75% of cases.
In the absence of universal screening, the newborns with the following
indications should be screened:
1. Family history of CH
2. History of thyroid disease or antithyroid medicine intake in mother
3. Presence of other conditions like Down’s syndrome, trisomy 18,
neural tube defects, congenital heart disease, metabolic disorders,
familial autoimmune disorders and Pierre- Robin syndrome which are
associated with higher prevalence of CH
Thyroid function should be tested in any infant with signs/ symptoms of
hypothyroidism such as postmaturity, macrosomia or wide open posterior
fontanel at birth or prolonged jaundice, constipation, poor feeding, hypotonia,
hoarse cry, umbilical hernia, macroglossia, or dry edematous skin in infancy.
The tests should be performed even in those infants who have a normal
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
newborn screening report as it is not entirely free from pitfalls. The test results
should be compared to the age related norms as presented in Table 3.
Once the diagnosis is established, further investigations to determine the
etiology should be done. A nuclear medicine scan using sodium pertechnate
(99mTc) is especially useful in diagnosing true athyreosis or ectopy as well as
goitrous hypothyroidism due to dyshormonogenesis. However, since the scan
can be done only before initiating treatment, one should not withhold therapy
if it is not possible to get it performed immediately. 11,12
A list of diagnostic
studies useful in infants with congenital hypothyroidism is presented in Table 4
and an algorithmic approach to investigation in Figure 1. ,.
When should we ask for free T4 levels?
In most situations, T4 (total) levels are sufficient for diagnosis of
hypothyroidism and monitoring treatment, but free T4 can be obtained as a
more robust marker of the bioavailable T4, when readily accessible. When
availability or cost is a constraint, estimation of free T4 should be definitely
done in the following situations:8, 13:
1. In premature newborns, T4 (total) values may be low because of
abnormal protein binding or low levels of thyroxine binding globulin
(TBG) due to immaturity of liver function, proteinuria or undernutrition.
Therefore, free T4 values provide a better estimate of true thyroid
function in premature or sick newborns.
2. Free T4 should be asked for in case of finding a low T4 with normal TSH.
If free T4 is normal, it can be a case of congenital partial (prevalence
1:4000-12000 newborns) or complete (prevalence 1:15000 newborns)
TBG deficiency. TBG levels should be evaluated to confirm this but this
test is not available routinely. If free T4 is also low along with low T4
with normal TSH, central hypothyroidism should be suspected.
3. During monitoring for adequacy of treatment, we usually monitor with
T4 (total) level. This assumes a normal TBG level. This can be confirmed
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
by measuring free T4 or TBG levels once at the time of the first post-
treatment T4 measurement.
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Treatment of CH
Term as well as preterm infants with low T4 and elevated TSH should be
started on L-thyroxine as soon as the diagnosis is made. The initial dose of L-
thyroxine should be 10-15µg/ kg/ day with the aim to normalize the T4 level at
the earliest. Those infants with severe hypothyroidism (very low T4, very high
TSH and absence of distal femoral and proximal tibial epiphyses on radiograph
of knee) should be started with the highest dose of 15µg/ kg/ day.14
Monitoring of therapy:
T4 should be kept in the upper half of normal range (10-16 µg/dL) or free T4 in
the 1.4 - 2.3 ng/dl range with the TSH suppressed in the normal range. T4 and
TSH levels should be checked according to the following schedule:
0-6 months: every 6 weeks
6 months-3 years: every 3 months
> 3 years: 6 monthly
T4 and TSH should also be checked 6-8 weeks after any dosage change.
Growth and development of the infant should also be regularly monitored.
It is equally important to avoid over treatment. Adverse effects of over
treatment include premature fusion of cranial sutures, acceleration of skeletal
maturation and problems with temperament and behavior.
Asymptomatic hyperthyrotropinemia: Elevated TSH with normal T4 values are
seen commonly. This hyperthyrotropinemia can be transient or permanent.
Perinatal iodine exposure is the commonest cause of transient elevation in
TSH. Other causes of hyperthyrotropinemia include defects in biological
activity of TSH or TSH receptor, a mild thyroid hormone biosynthesis defect,
subtle developmental defects or a disturbance in the negative feedback control
of TSH. Hyperthyrotropinemia in newborns is usually treated but in the
presence of free T4 levels in upper half of normal range, expectant
management can be followed. In case of starting treatment, a 6 week trial of
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
putting the child off therapy followed by measuring TSH and T4 levels should
be done at 3 years of age.14
Preterm infants with low T4 and normal TSH levels (Transient
hypothyroxinemia of prematurity): Use of levothyroxine in an attempt to
“normalize” levels remains controversial because there is insufficient evidence
that early treatment with thyroid hormone leads to improved outcomes. Larger
studies, especially in the extremely preterm infants are needed to resolve this
issue.15
Transient Hypothyroidism: Infants with presumed transient hypothyroidism due
to maternal goitrogenic drugs need not be treated unless low T4 and elevated
TSH values persist beyond 2 weeks. Therapy can be discontinued after 8-12
weeks. Intake of antithyroid drugs can be continued by the hyperthyroid
mothers during breast feeding because concentration of these drugs is very
low in breast milk. If we have been able to document the presence of TBII in an
infant and are attributing hypothyroidism to maternal autoimmune thyroiditis,
treatment should be started if T4 is low and continued for 3-6 months 8.
However, when TBII estimation is not available it is best to continue treatment
till the age of 3 years and then give a trial off therapy for 6 weeks followed by
retesting of T4 and TSH to determine the need for continuation of therapy.
The management has been summarized in Panel 1.
Outcome: The best outcome occurs with L-thyroxine therapy started by 2
weeks of age at 9.5 µg/kg or more per day, compared with lower doses or later
start of therapy. Residual defects can include impaired visuospatial processing
and selective memory and sensorimotor defects. More than 80% of infants
given replacement therapy before three months of age have an IQ greater than
85 but may show signs of minimal brain damage, including impairment of
arithmetic ability, speech, or fine motor coordination in later life.7 When
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
treatment is started between 3-6 months, the mean IQ is 71 and when delayed
• Abnormal values on screening should always be confirmed by a venous
sample using age appropriate cut-offs.
• Investigations to determine the etiology such as scintigraphy should be
done as soon as the diagnosis is made. If it is not possible, the therapy
should be started without delay.
• The initial dose of L-thyroxine should be 10-15µg/ kg/ day with the aim
to normalize the T4 level at the earliest. T4 should be kept in the upper
half of normal range (10-16 µg/dL) with TSH level suppressed in the
normal range.
• Asymptomatic hyperthyrotropinemia should be treated unless the free
T4 levels are in upper half of normal range.
• When treatment has been started in an infant with suspected transient
hypothyroidism or isolated increase in TSH or borderline values of T4
and TSH, a 6 week trial of putting the child off therapy followed by
measuring TSH and T4 levels should be done at 3 years of age.
to beyond 6 months, the mean IQ drops to 54.16
Panel 1 MANAGEMENT OF CONGENITAL HYPOTHYROIDISM
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
References
1. Desai MP, Upadhye P, Colaco MP, Mehre M, Naik SP, Vaz
FE, Nair N, Thomas M. Neonatal screening for congenital hypothyroidism
using the filter paper thyroxine technique. Indian J Med Res 1994; 100:
36-42.
2. Fisher DA, Klein AH. Thyroid development and disorders of
thyroid function in the newborn. N Engl J Med. 1981; 304:702–712.
3. Haddow JE, Palomaki GR, Allan WC et al. Maternal thyroid
deficiency during pregnancy and subsequent neuro-psychological
development of the child.
4. Macchia P. Recent advances in understanding the
molecular basis of primary congenital hypothyroidism. Mol Med Today
2000;6:36–42
5. Adams LM, Emery JR, Clark SJ, Carlton EI, Nelson JC.
Reference ranges for newer thyroid function tests in premature infants. J
Pediatr 1995;126:122–7.
6. Nikta Forghani, Tandy Aye. Hypothyroxinemia and
prematurity. Neoreviews 2008; 9: e66-71.
7. American Academy of Pediatrics, Rose SR; Section on
Endocrinology and Committee on Genetics, American Thyroid
Association, Brown RS; Public Health Committee, Lawson Wilkins
Pediatric Endocrine Society, Foley T, Kaplowitz PB, Kaye CI,
Sundararajan S, Varma SK. Update of newborn screening and therapy
for congenital hypothyroidism. Pediatrics 2006; 117:2290-303.
8. Fisher DA. Disorders of the thyroid in newborns and infants.
In Sperling MA, ed. Pediatric Endocrinology, 2nd edition. Philadelphia:
Saunders, 2002; 161-86.
9. Soldin OP, Jang M, Guo T, Soldin SJ. Pedistric reference
intervals for free thyroxine and free triiodothyronine. Thyroid 2009; 19:
699-702.
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
10. Fisher DA. Disorders of the thyroid in childhood and
adolescence. In Sperling MA, ed. Pediatric Endocrinology, 2 nd edition.
Philadelphia: Saunders, 2002; 187-210.
11. LaFranchi S. Congenital hypothyroidism: etiologies,
diagnosis and management. Thyroid 1999;9:735-40.
12. Fisher DA. Management of congenital hypothyroidism. J
Clin Endocrinol Metab 1991;72:525-8.
13. Brown RS. The thyroid gland. In Brook CGD, Hindmarsh PC
eds. Clinical Pediatric Endocrinology, 4th edition. London: Blackwell
Science, 2001; 288-320.
14. LaFranchi SH, Austin J. How should we be treating children
with congenital hypothyroidism? J Pediatr Endocrinol Metab 2007;
20:559-78.
15. Postnatal thyroid hormones for preterm infants with
transient hypothyroxinaemia. Cochrane Database Syst Rev. 2007:
CD005945.
16. Klien AH, Meltzer S, Kenny FM. Improved prognosis in
congenital hypothyroidism treated before age three months. J Pediatr
1972;81:912-5.
Table 1 Etiology of CH
1. Permanent hypothyroidism.
b. Thyroid dysgenesis (aplasia, hypoplasia or ectopia)
c. Thyroid hormone biosynthetic defects
d. Iodine deficiency (endemic cretinism)
e. Hypothalamic-pituitary hypothyroidism
2. Transient hypothyroidism.
a. TSH binding inhibitory immunoglobulins
b. Exposure to goitrogens (iodides or antithyroid drugs)
c. Transient hypothyroxinemia of prematurity
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
d. Sick euthyroid syndrome
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Table 2 Reference ranges for serum free T4 (fT4) and TSH in preterm infants
Age in weeks Free T4 (ng/dl) TSH (mu/l)
25-27 06-2.2 0.2-30.3
28-30 0.6-3.4 0.2-20.6
31-33 1.0-3.8 0.7-20.9
34-36 1.2-4.4 1.2-21.6
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Table 3 Reference ranges for T4, fT4 and TSH in term infants
according to age8, 9, 10
Age T4 (μg/dl) fT4 (pg/ml) TSH (μU/ml)
mean (range) mean (SD)/ mean
(range)
range
Cord blood 10.8 (6.6-15) 13.8 (3.5) 10.0 (1-20)
1-3 days 16.5 (11-21.5) * 5.6 (1-10)
4-7 days * 22.3 (3.9) *
1-2 weeks 12.7 (8.2- * 2.3 (0.5-6.5)
17.2)
2-6 weeks 6.5-16.3** 9.0-22.0** 1.7-9.1**
6 weeks to 12 11.1 (5.9-1.3) 13.0-24.0** 2.3(0.5-6.5)
months
*No data available ** data for median/mean not available
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Table 4 Diagnostic studies for evaluation of CH
1. Imaging Studies: will determine location and size
a. Scintigraphy (99mTc or 123 I)
b. Sonography (less sensitive than scintigraphy)
2. Function Studies
a. 123 I uptake
b. Serum thyroglobulin
3. Suspected inborn error of T4 synthesis
a. 123 I uptake and perchlorate discharge
4. Suspected autoimmune thyroid disease
a. Maternal and neonatal serum TBII measurement (not routinely
available)
5. Suspected iodine exposure or deficiency
a. Urinary iodine measurement
6. Ancillary test to determine severity of fetal hypothyroidism
a. Radiograph of knee for skeletal maturation
.
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
Figure 1 Approach to a newborn infant with positive screening test for CH
Positive screening test on filter paper sample
Serum T4/ Free T4, TSH
Normal
Abnormal
Thyroid scan
Normal Absent uptake
Ectopic
Tg Measurement Ultrasound
Normal or Absent Normal gland No thyroid
tissue
TBII measurement* TBII measurement*
Positive Negative Negative Positive
Transient TH synthetic Tg TSH receptor Transient
Thyroid Ectopic
CH defect or synthetic or CH
agenesis thyroid
drug effect defect TH biosynthetic
gland
defect or iodine
blockade
Downloaded from www.newbornwhocc.org
AIIMS- NICU protocols 2010
TBII= TSH binding inhibitory immunoglobulin (*not routinely available)
Tg= thyroglobulin, TH= thyroid hormone
Adapted from Fisher DA. Management of congenital hypothyroidism. J Clin
Endocrinol Metab 1991;72:525-8.13
Downloaded from www.newbornwhocc.org
You might also like
- STUDY GUIDE Pilgrims ProgressDocument68 pagesSTUDY GUIDE Pilgrims Progressl1o2st100% (7)
- GGC BookDocument96 pagesGGC Bookl1o2st100% (1)
- Major & Trace MineralsDocument5 pagesMajor & Trace MineralsRhenier S. IladoNo ratings yet
- Mal Presentations Mal PositionsDocument4 pagesMal Presentations Mal PositionsMelissa Aina Mohd YusofNo ratings yet
- Trace Elements: Reed A Berger MD Visiting Clinical Professor in NutritionDocument47 pagesTrace Elements: Reed A Berger MD Visiting Clinical Professor in NutritionGramoz CubreliNo ratings yet
- 2 Corinthians 12 - Triumphalism, Suffering and Spiritual MaturityDocument26 pages2 Corinthians 12 - Triumphalism, Suffering and Spiritual Maturityl1o2st100% (1)
- Hemophilia ADocument20 pagesHemophilia Adiaharmayukti100% (1)
- VentilatorDocument90 pagesVentilatorthenaloveNo ratings yet
- Trisomy 21-Down Syndrome: Payal DhakappaDocument35 pagesTrisomy 21-Down Syndrome: Payal DhakappaPayal AmarnathNo ratings yet
- Osteomyelitis RadiologyDocument26 pagesOsteomyelitis RadiologySheila Mae CabahugNo ratings yet
- Coagulation DisordersDocument14 pagesCoagulation Disorderssusan_grace123No ratings yet
- Orthopedic Devices DDocument31 pagesOrthopedic Devices Dmakenawairimu30No ratings yet
- Dietary Guidelines For Indians-NINDocument138 pagesDietary Guidelines For Indians-NINsaradhi26No ratings yet
- Hemophilia & Other Hereditary Bleeding Disorders: Djajadiman Gatot Novie Amelia CDocument34 pagesHemophilia & Other Hereditary Bleeding Disorders: Djajadiman Gatot Novie Amelia CpiniNo ratings yet
- Uk PFAPADocument5 pagesUk PFAPAPrerna SehgalNo ratings yet
- Christian or CretinDocument2 pagesChristian or CretinRoberto Fortu100% (1)
- K32 - Pathology of Bone (Dr. Dody)Document60 pagesK32 - Pathology of Bone (Dr. Dody)faris100% (1)
- Hypothyroidism: Darien Liew DaojuinDocument41 pagesHypothyroidism: Darien Liew DaojuinDarien LiewNo ratings yet
- Chronic Otitis Media, Cholesteatoma, and Mastoiditis in AdultsDocument14 pagesChronic Otitis Media, Cholesteatoma, and Mastoiditis in AdultschristineNo ratings yet
- The Final Days of Jesus: 40-Day Devotional Reading GuideDocument5 pagesThe Final Days of Jesus: 40-Day Devotional Reading Guidel1o2stNo ratings yet
- Hum Notebook Nov2005Document142 pagesHum Notebook Nov2005l1o2stNo ratings yet
- 1 RicketsDocument32 pages1 RicketsDarina Ismakaieva100% (1)
- Unit 8: Pain Assessment and ManagementDocument24 pagesUnit 8: Pain Assessment and ManagementMatthew RyanNo ratings yet
- Bladder Extrophy: Medical ManagementDocument8 pagesBladder Extrophy: Medical ManagementChristian James CamaongayNo ratings yet
- A Child With WheezeDocument53 pagesA Child With WheezeCodillia CheongNo ratings yet
- Case Study Congenital HyperthyroidismDocument10 pagesCase Study Congenital HyperthyroidismCamille CaraanNo ratings yet
- Thalassemia: Dr. Deep Shah Under Guidance of Dr. Krutika Ma'Am and Dr. Rahul SirDocument46 pagesThalassemia: Dr. Deep Shah Under Guidance of Dr. Krutika Ma'Am and Dr. Rahul SirDeep ShahNo ratings yet
- Child With Respiratory DysfunctionDocument23 pagesChild With Respiratory DysfunctionmeganNo ratings yet
- Nutritional Deficiency For ClassDocument74 pagesNutritional Deficiency For ClassBelayneh TadesseNo ratings yet
- EPISTAXIS LectureDocument30 pagesEPISTAXIS LectureDhienWhieNo ratings yet
- Congenital HypothyroidismDocument21 pagesCongenital HypothyroidismDanna GarcíaNo ratings yet
- Dietary Guidelines For IndiansDocument92 pagesDietary Guidelines For IndiansbacchanNo ratings yet
- Definition of Operation Performed Tonsillectomy (ton-sih-LEK-tuh-mee) Is The Surgical Removal of The Tonsils, Two Oval-Shaped Pads ofDocument3 pagesDefinition of Operation Performed Tonsillectomy (ton-sih-LEK-tuh-mee) Is The Surgical Removal of The Tonsils, Two Oval-Shaped Pads ofcaligean_827936No ratings yet
- Distinguishing TRALI and TACODocument6 pagesDistinguishing TRALI and TACOl1o2stNo ratings yet
- Filariasis: Causes, Tests, and Treatment OptionsFrom EverandFilariasis: Causes, Tests, and Treatment OptionsRating: 5 out of 5 stars5/5 (2)
- Albendazole in PediatricsDocument38 pagesAlbendazole in PediatricsKishore ChandkiNo ratings yet
- Otitis MediaDocument7 pagesOtitis MediaNorminaKiramAkmadNo ratings yet
- Congenital Hypothyroidism 06.08.2015Document12 pagesCongenital Hypothyroidism 06.08.2015Emily EresumaNo ratings yet
- Congenital Hypothyroidism From MedscapeDocument11 pagesCongenital Hypothyroidism From MedscapeAgustin IskandarNo ratings yet
- Tetralogy of FallotDocument37 pagesTetralogy of Fallottintinlovessu100% (1)
- MeaslesDocument23 pagesMeaslesadwait marhattaNo ratings yet
- Truncus ArteriosusDocument4 pagesTruncus ArteriosuskemalahmadNo ratings yet
- Acute Management of Burns in ChildrenDocument52 pagesAcute Management of Burns in ChildrenJonie Vince SañosaNo ratings yet
- Assessment of A NewbornDocument16 pagesAssessment of A NewbornlouradelNo ratings yet
- What Is Meningitis?Document7 pagesWhat Is Meningitis?laujeroNo ratings yet
- Growth ChartsDocument8 pagesGrowth ChartsMohamedDiabNo ratings yet
- Chronic Otitis MediaDocument24 pagesChronic Otitis Mediaingidzai100% (1)
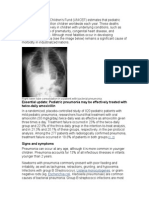
- Essential Update: Pediatric Pneumonia May Be Effectively Treated With Twice-Daily AmoxicillinDocument54 pagesEssential Update: Pediatric Pneumonia May Be Effectively Treated With Twice-Daily AmoxicillinYostesara Maurena SantosaNo ratings yet
- Near DrowningDocument48 pagesNear DrowningS.m. TehseenNo ratings yet
- Chronic Suppurative Otitis MediaDocument16 pagesChronic Suppurative Otitis MediaEmil P. MuhammadNo ratings yet
- Hydrocephalus IDocument52 pagesHydrocephalus IVlad Alexandra50% (2)
- Tetanus RabiesDocument67 pagesTetanus RabiesWaNda GrNo ratings yet
- Otitis Media OtolaryngologyDocument45 pagesOtitis Media OtolaryngologyDr.Sherif Bugnah100% (5)
- Taking History in PaediatricsDocument7 pagesTaking History in PaediatricsNikola IgnjatovicNo ratings yet
- Assessment 2 Vital Signs Normal ValuesDocument4 pagesAssessment 2 Vital Signs Normal Valuesthannikkotte12345No ratings yet
- Approach To Comatose ChildDocument63 pagesApproach To Comatose Childdrmindhacker100% (1)
- Anatomic Disorders of Female Reproductive SystemDocument42 pagesAnatomic Disorders of Female Reproductive SystemNelly AstikaNo ratings yet
- DVT NotesDocument3 pagesDVT NotesTodd EvansNo ratings yet
- PolyhydramniosDocument5 pagesPolyhydramniosPATRICIA SAN PEDRONo ratings yet
- Cervical Incompetence Moh AbdallaDocument46 pagesCervical Incompetence Moh AbdallaDr. mohammed50% (2)
- Tetralogy of FallotDocument33 pagesTetralogy of FallotjeenaejyNo ratings yet
- Tetralogy of Fallot RadiologyDocument13 pagesTetralogy of Fallot RadiologyErlan Anugrah PratamaNo ratings yet
- Ventric Ul Omega LyDocument40 pagesVentric Ul Omega LyErliana FaniNo ratings yet
- NewbornDocument72 pagesNewbornAbdul Ghaffar AbdullahNo ratings yet
- Anatomy of The Female Pelvis: by DR. Zeinab Abotalib, MRCOG Associate Prof. of Obs & Gyn - King Saud UniversityDocument24 pagesAnatomy of The Female Pelvis: by DR. Zeinab Abotalib, MRCOG Associate Prof. of Obs & Gyn - King Saud UniversityThrishia Jade IgotNo ratings yet
- LATHYRISM AND PHOTOSENSiTIZATIONDocument33 pagesLATHYRISM AND PHOTOSENSiTIZATIONSunilNo ratings yet
- Congenital Adrenal Hyperplasia (CAH)Document17 pagesCongenital Adrenal Hyperplasia (CAH)Rastu MaharthaNo ratings yet
- Otalgia (Ear Pain)Document43 pagesOtalgia (Ear Pain)Suzzane MNo ratings yet
- ClubfootDocument5 pagesClubfootcreyannc0% (1)
- Approach To Limping ChildDocument3 pagesApproach To Limping ChildShamen KohNo ratings yet
- Senior Project ProposalDocument12 pagesSenior Project Proposalapi-402826509No ratings yet
- Arthritis, Suppurative Arthritis) : Pyogenic Arthritis (Septic Arthritis, InfectiveDocument4 pagesArthritis, Suppurative Arthritis) : Pyogenic Arthritis (Septic Arthritis, InfectiveRajveerNo ratings yet
- Hemophilia in ChildrenDocument16 pagesHemophilia in ChildrenVinay Sahu100% (1)
- Brucellosis 2Document70 pagesBrucellosis 2Zara IftikharNo ratings yet
- DDH - PFDocument34 pagesDDH - PFAnnisa Oktoviani MursidaNo ratings yet
- Fanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandFanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Critique of Gentry and Wellum'S, Kingdom Through Covenant: A Hermeneutical-Theological ResponseDocument17 pagesA Critique of Gentry and Wellum'S, Kingdom Through Covenant: A Hermeneutical-Theological Responsel1o2stNo ratings yet
- Vancomycin Protocol RQHRDocument15 pagesVancomycin Protocol RQHRl1o2stNo ratings yet
- Edubriefs in CCTC: Svo (Mixed Venous Oxygen Saturation) or Scvo Central Venous Oxygen Saturation)Document3 pagesEdubriefs in CCTC: Svo (Mixed Venous Oxygen Saturation) or Scvo Central Venous Oxygen Saturation)l1o2stNo ratings yet
- Teper, Segal, & Inzlicht - Inside The Mindful Mind (In Press)Document6 pagesTeper, Segal, & Inzlicht - Inside The Mindful Mind (In Press)l1o2st100% (1)
- 10429Document2 pages10429l1o2stNo ratings yet
- Colossians-Personal Notes: 1. Paul's Messengers (4:7-9)Document5 pagesColossians-Personal Notes: 1. Paul's Messengers (4:7-9)l1o2stNo ratings yet
- Creation, AshfordR 2Document9 pagesCreation, AshfordR 2l1o2stNo ratings yet
- Iodine and Iron DeficienciesDocument145 pagesIodine and Iron DeficienciesAtika SugiartoNo ratings yet
- Tura KuDocument104 pagesTura KuFitzgerald BillyNo ratings yet
- Nutrition and Malnutrition Resource UnitDocument22 pagesNutrition and Malnutrition Resource UnitMitch GatdulaNo ratings yet
- Mag Nascent IodineDocument3 pagesMag Nascent IodineNavigator4life100% (1)
- Iodine DeficiencyDocument2 pagesIodine Deficiencymubashir_mm4uNo ratings yet
- 98th Indian SC CongDocument316 pages98th Indian SC CongBuddhadeb BasuNo ratings yet
- Pathology Lab V Diffuse and Multinodular Goiter.Document18 pagesPathology Lab V Diffuse and Multinodular Goiter.Jeffry Chandra TjahayadiNo ratings yet
- WHO NMH NHD EPG 14.5 Eng PDFDocument6 pagesWHO NMH NHD EPG 14.5 Eng PDFsimbawulaNo ratings yet
- Congenital Hypothyroidism - AIIMS ProtocolDocument19 pagesCongenital Hypothyroidism - AIIMS Protocoll1o2stNo ratings yet
- Lecture 5, GoiterDocument56 pagesLecture 5, GoiterAna-Maria TobescuNo ratings yet
- Dwarfism: Needed)Document11 pagesDwarfism: Needed)Annapurna DangetiNo ratings yet
- Nuclear Thyroid - DR Siegel 2017Document414 pagesNuclear Thyroid - DR Siegel 2017AHNo ratings yet
- Disorders of The Thyroid Gland Harrison's Principles of Internal Medicine, 19eDocument21 pagesDisorders of The Thyroid Gland Harrison's Principles of Internal Medicine, 19ePeterNo ratings yet