Professional Documents
Culture Documents
Treatment of High-Flow Arteriovenous Malformations
Uploaded by
nurminsyahOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Treatment of High-Flow Arteriovenous Malformations
Uploaded by
nurminsyahCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/51564584
Treatment of high-flow arteriovenous malformations (AVMs) of the head and
neck with embolization and surgical resection
Article in Annali italiani di chirurgia · July 2011
Source: PubMed
CITATIONS READS
12 623
5 authors, including:
Valentino Valentini Giorgio Pompa
Sapienza University of Rome Sapienza University of Rome
101 PUBLICATIONS 821 CITATIONS 108 PUBLICATIONS 711 CITATIONS
SEE PROFILE SEE PROFILE
Stefano Di Carlo Luciano Bresadola
Sapienza University of Rome Sapienza University of Rome
50 PUBLICATIONS 367 CITATIONS 20 PUBLICATIONS 144 CITATIONS
SEE PROFILE SEE PROFILE
All content following this page was uploaded by Giorgio Pompa on 12 February 2014.
The user has requested enhancement of the downloaded file.
LEADING ARTICLE
Treatment of high-flow arteriovenous
malformations (AVMs) of the head
Ann. Ital. Chir., 2011 82: 253-259
and neck with embolization
and surgical resection
Valentina Pompa*, Valentino Valentini**, Giorgio Pompa**, Stefano Di Carlo**,
Luciano Bresadola*
*Dept of Radiological Sciences, Sapienza University of Rome, Rome, Italy
**Dept of Odontostomatological and Maxillofacial Sciences, Sapienza, University of Rome, Rome, Italy
Treatment of high-flow arteriovenous malformations (AVMs) of the head and neck with embolization and sur-
gical resection
AIM: Arteriovenous malformations (AVMs) with a high flow of the head and neck are quite rare compared to their low-
flow counterparts, but when they do occur they are often accompanied by massive bleeding or present with significant
esthetic defects. The treatment of these high-flow vascular anomalies is often highly risky. The multidisciplinary approach
required for the assessment and treatment of these lesions should include angioradiology with preoperative superselective
embolization, followed by surgical resection of the lesion within 24 hours and esthetic reconstruction.
MATERIALS OF STUDY: We studied a series of 55 patients with AVMs of the head and neck that were treated surgical-
ly between 1999 and 2009.
RESULTS: Of the 55 patients with AVMs, 7 had hemangiomas and 48 had vascular malformations, of which 28 were
low-flow lesions and 20 were high-flow lesions (AVMs). The high-flow lesions were most commonly located on the lip.
All 48 AVMs underwent surgical resection for concerning symptoms, diagnostic purposes, or esthetic problems. Of the 20
high-flow AVMs, 20% were classified as Schöbinger stage I, 55% as stage II, and 25% as stage III. A combined treat-
ment of embolization and resection was used to resolve 13 of the high-flow AVMs (stages II and III), of which 4
required a flap reconstruction.
CONCLUSION: Recent advances in microsurgery and interventional angioradiology have greatly improved the prognosis for
patients with these malformations. Combined embolization-resection is the treatment of choice for high-flow AVMs, and
esthetic reconstruction with flaps can prevent their recurrence.
KEY WORDS: Arteriovenous malformation, Transcatheteric embolization.
Introduction are currently more than 50 different types. The
International Society of the Study of Vascular Anomalies
A common classification of vascular malformation (ISSVA) classification (ISSVA – 11th Workshop, Rome,
pathologies is required, because in the literature there 1996) is easy to use, particularly for vascular abnormal-
ities of the head and neck. It is based on clinical crite-
ria, evolution, histopathologic and hemodynamic prop-
Pervenuto in Redazione Febbraio 2011. Accettato per la pubblicazione
erties, and comprises two large groups: hemangiomas and
Marzo 2011. vascular malformations 1-2.
Correspondence to: Luciano Bresadola, MD. (e-mail: luciano.bresado- Vascular abnormalities of the head and neck can thus
la@uniroma1.it) be classified as hemangiomas or vascular malformations.
Ann. Ital. Chir., 82, 4, 2011 253
V. Pompa, et al.
Hemangiomas are common in childhood; a conserva- surgical therapy alone often results in a significant reduc-
tive “wait and see” approach is recommended for this tion in most of the clinical features, it is not sufficient
type because most of these lesions regress spontaneously to resolve the problem; a multidisciplinary approach is
3. Histologically, hemangiomas display endothelial considered the treatment of choice 8.
hyperplasia and an increased number of mast cells in Transcatheteric embolization is particularly useful by itself
the proliferative phase 4, and phase involution is char- in children with vascular malformations of the maxilla
acterized by the fibrotic replacement type, reduced cel- or jaw. However, in growing children, surgical removal
lularity, and a normal mast cell count. Conversely, vas- of large segments of bone may lead to impaired facial
cular malformations are labeled “mature” because growth, resulting in an abnormal appearance and dental
although they sometimes occur at birth their incidence occlusion, which itself requires orthodontic-prosthetic
increases with the development and growth of the rehabilitation 9. Surgery in this age group is confined to
body, often manifesting in the adult; they do not “debulking” of the soft tissues of the tumor that is infil-
resolve spontaneously 5. Vascular malformations are not trated by the malformation.
tumors, but rather an accumulation of abnormal ves-
sels with endothelial proliferation and a normal mast
cell count, representing morphogenetic errors with Materials and methods
structural abnormalities but without endothelial cell
proliferation 6. In the 10 years between 1999 and 2009, we treated 55
Vascular malformations can be further classified accord- patients surgically to repair vascular malformations of the
ing to the type of vessel involved, as capillary, venous, head and neck. Data were collected regarding the
lymphatic, and arteriovenous. They are then further patients’ age at the time of surgery, sex, presenting signs
divided into low-flow lesions (capillary, venous, lym- and symptoms, anatomical location of the anomaly, size,
phatic, or combinations thereof ) and high-flow lesions mode of diagnosis, indications for surgery, surgery per-
(blood component, usually arteriovenous) 7. High-flow formed and other treatment modalities, histopathologi-
arteriovenous malformations (AVMs) of the head and cal data, and outcome after treatment. The vascular
neck are particularly problematic with regard to treat- abnormalities were classified based on their histopathol-
ment because of their propensity for rapid growth. While ogy as hemangiomas and AVMs.
TABLE I - Clinical details of 20 patients with oral and maxillofacial high flow malformation.
Case Age Sex Location Symptomatology Istology/ Rx Embolization Type Complications Post Follow Results
Schobinger of surgery surgery up/m
embolization
1 21 M L E T II – EMB Excision 60 VG
2 18 M L E A III – EMB Excision 60 G
3 6 M F S Cg I MR Excision REC EMB 56 S
Excision
Tissue
expansion
scalp
4 8 F C S Cg III MR EMB Excision 48 VG
5 35 M M P A II CT/MR EMB Excision 45 VG
6 42 M N P A II CT/MR EMB Excision 43 G
7 29 F L HT A I – Excision 38 G
8 40 M L S A II – Excision 38 G
9 15 M C S Cg II MR EMB Excision 36 VG
10 23 M C P A II MR EMB Excision 36 VG
11 18 F L S Pub I CT/MR Excision 29 G
12 18 M Na Pa Cg II CT Excision 28 G
13 21 F F S Pub II CT/MR EMB Excision 28 VG
14 36 M C E A I CT/MR Excision REC EMB 24 G
Excision
Free flap
reconstruction
15 10 F F V Cg II MR EMB Excision 24 VG
16 36 M L S A II CT/MR EMB Excision 24 G
17 28 M L P A I – Excision 19 S
18 14 F F S Pub III CT/MR Excision 15 G
19 9 M C S Cg II MR Excision 12 G
20 41 F M S A III CT/MR EMB Excision 6 G
L: lip; F: front; C: cheek; M: mandible; N: neck; Na: nasal dorsum; H: hemorrhage; HT: elevated local temperature; S: swelling; P: pulsatility; Pa: pain;
V: sign of Valsalva; T: traumatic; A: adulthood; Pub: puberty; Cg: congenital; EX: surgical excision; S: sufficient; G: good; VG: very good.
254 Ann. Ital. Chir., 82, 4, 2011
Treatment of high-flow arteriovenous malformations (AVMs) of the head and neck with embolization and surgical resection
Results between high- and low-flow AVMs. The term “high
flow” describes an arteriovenous anomaly comprising
All 55 patients underwent surgical resection of vascular multiple, low-resistance vascular shunts 4. These do not
anomalies of the face or neck with or without the use tend to exhibit expanded cell hyperplasia, but due to
of other modes of treatment. The vascular malforma- hemodynamic mechanisms leading to the formation of
tions of 7 the 55 treated patients were defined as heman- a collateral circulation they deflect the regional blood
giomas, while those of the remaining 48 were AVMs. flow from the periphery. Of crucial importance is that
The series of hemangiomas comprised two males and primary pathological lesions often occur at the arterio-
five females (male:female ratio, 1:2.5) aged 5-42 years le–capillary arteriovenous shunt, large arteries, with dila-
(mean, 22.4 years). The series of AVMs comprised 28 ted draining veins due to recurrences.
low-flow lesions and 20 high-flow lesions. Long-term success can only by guaranteed by complete
Of those with high-flow AVMs, 13 were men and 7 resection of AVMs 3,4,10. Proximal surgical ligation of
were women (Table I) with an age range of 6-42 years arteries without resection is doomed to failure, and must
(mean, 29.2 years). The area most commonly involved be cajoled into what determines the formation of colla-
was the lip (n=7), followed by cheek (n=5), forehead teral circulation to the closure you can not use secon-
(n=4), mandible (n=2), neck (n=1), and nose (n=1). The dary therapeutic embolization. However, esthetic and
lesion size ranged from 5x5x40 mm to 5x5x60 mm. Six functional considerations require minimization of tissue
of these patients submitted to surgery after recurrence removal.
or continuation of a previous treatment for a high-flow The classification of peripheral AVMs proposed by
AVM. The 20 patients in this group presented with a Allison and Kennedy 11 is based on both the clinical
bulge/swelling associated with a progressive enlargement and angiographic characteristics of the flow. It compris-
thereof (n=10), along with an increase in the pulsatility es three groups with the following predominant charac-
index (n=4), bleeding (n=3), pain, and discomfort (n=1), teristics:
a positive Valsalva sign (n=1), and a high local temper- Group 1: arterial and arteriovenous lesions.
ature (n=1). Six patients had a history of congenital dis- Group 2: pathology involving small blood vessels.
ease, while the AVM was observed for the first time dur- Group 3: venous lesions.
ing puberty in three patients, immediately after a trau- More recently, the 11th Workshop of ISSVA presented
ma in one patient, and in adulthood in the remaining a classification that is easy to use and provides for an
ten patients. initial distinction between hemangiomas and vascular
Diagnostic magnetic resonance imaging (MRI) and/or malformations, and a second distinction between AVMs
computed tomography were performed in 15 cases, while into low-flow (capillaries, venous, lymphatic, or combi-
superselective angiography with embolization was con- nations thereof ) and high-flow (arteriovenous) types.
ducted in 11 cases. Surgical excision alone was used in Most of our cases were identified as malformations of
9 patients, while 11 cases (8 Schöbinger stage II or stage the lip (35%), cheeks (25%), and face (20%); there were
III) were treated with superselective embolization 24 no ear malformations. In contrast, Allison and Kennedy
9 and Kohout et al. 12,13 found that the most common
hours after en bloc resection. Two of the patients
required a free flap to be taken from the forearm for locations of 81 AVMs were the cheek (31%) and the
the reconstruction of a radial lip, with debulking in a ear (16%).
second phase. AVMs may progress due to acute stimuli such as trau-
The follow-up period ranged from 6 to 60 months ma, pregnancy, puberty, infection, or iatrogenic injury
(mean 26 months). At follow-up, two of the patients (biopsy, proximal ligation, or subtotal excision) 5,7,12.
who were initially treated by surgical resection only sub- Clinically, the overlying skin may appear normal, as a
sequently underwent preoperative embolization followed pulsatile mass, with redness and increased warmth; oth-
by excision of lesions that required reconstruction of the er clinical features may include pain and excessive
soft tissue using of scalp tissue (after its expansion). All growth, until bleeding heart failure occurs.
of the other lesions were excised with direct closure. Using the classification of Schöbinger, 25% of patients
There were no recurrences in any of the other cases. At were at stage I (skin redness or heat), 55% were at stage
the last follow-up, the results were very good in 7 cases II (visible pulsation or expansion of the lesions), 20%
(35%), good in 11 (55%), and insufficient in 2 cases were at stage III (pain, ulceration, hemorrhage, or infec-
(10%). tion), and none were at stage IV (heart failure). On
MRI, the AVMs were characterized by enlarged blood
vessels with vascular dilation, collateral arteries, and vas-
Discussion cular lesions with considerable drainage (confirming their
high-flow nature). MRI is an essential tool for the ear-
The correct management of vascular anomalies depends ly diagnosis of AVMs that appear as irregular or globu-
upon an accurate diagnosis. It is important to distin- lar masses and which may be located in the brain cor-
guish between hemangiomas and AVMs, and further, tex, in the subcortical gray and white matters. They may
Ann. Ital. Chir., 82, 4, 2011 255
V. Pompa, et al.
be observed as small, round, low-intensity signal spots tion of the involved tissues. The treatment of choice
in or around the mass on T1- or T2-weighted sequences. is the selective embolization of vessels in combination
Low-signal-intensity hemosiderin may also be seen extra- with surgical resection and reconstruction of the soft
cellularly or around the AVMs, indicating symptomatic tissues. The aim of preoperative embolization is main-
or asymptomatic hemorrhage, respectively. Magnetic res- ly to reduce blood loss and facilitate the surgery, and
onance angiography with contrast medium can identify must not be considered a method for reducing the
masses of 1 cm in diameter, but it is not appropriate extent of resection. Surgical resection should not be
for studying the morphology of arteries and veins. delayed beyond 48 hours after embolization because the
Angiography, which was performed in 94.5% (52/55) of resulting inflammation renders the aforementioned
our cases, was necessary to evaluate the anomaly in more hemodynamic benefits useless and the surgery more dif-
detail before excision surgery or embolization 14. This ficult.
revealed a large number of shunts with a high blood An AVM is often not diagnosed until a dramatic bleed-
flow. One case involved the jaw in addition to the main ing event, which may occur following dental treatment,
focus of the hypothalamus and optic nerve, enabling a for example 9. A variety of maneuvers can be used to
diagnosis of Wyburn-Mason syndrome 15. Angiography minimize intraoperative hemorrhage: hypotensive anes-
also revealed involvement of the facial artery and facial thesia 17, a temporary suture around the periphery of
vein in all cases (Table II). the excision margin, and cardiopulmonary bypass with
The treatment of arteriovenous anomalies is difficult and hypodermic circulatory arrest 18.
the results are sometimes disappointing. In 1815, Bell Arterial embolization techniques have improved consid-
16 admitted that an AVM (aneurysm by anastomosis) erably since 1904 when Dawbarn 19 first injected hot
is clearly different from an acquired fistula, and found liquid wax into the external carotid artery of a patient
that long-term success is only possible with total resec- with a craniofacial tumor. Considerable progress has
TABLE II - Detail of embolized oromaxillofacial high flow AVMs.
Case Location Vessels Embolization technique Embolization results
1 L Facial artery PVA 90% reduction of flow
Venous drainage: facial vein
2 L Facial artery PVA
Venous drainage: facial vein and Gelfoam 70% reduction of flow
3 F External carotid artery Coils 40% reduction flow Residual
(internal maxillary and facial arteries) AVM from facial artery
Venous drainage:internal maxillary vein, facial vein
4 C Internal maxillary artery, facial artery PVA 90% reduction of flow
Venous drainage: superficial and deep facial veins
5 M External carotid artery PVA 90% reduction of flow
(facial branches and internal maxillary)
Venous drainage:internal maxillary vein,
facial vein into jugular veins
6 N External carotid artery 70% reduction of flow
9 C Facial artery Coils 90% reduction of flow
Venous drainage: superficial and deep facial veins
10 C Facial artery Coils 90% reduction of flow
Venous drainage: facial vein
13 F External carotid artery PVA 90% reduction of flow
(internal maxillary and facial arteries)
Venous drainage:internal maxillary vein,facial vein
14 C Facial artery PVA 80% reduction of flow
Venous drainage: facial vein and Gelfoam
15 F External carotid artery( internal maxillary) 90% reduction of flow
Venous drainage:internal maxillary vein
16 L Facial artery Coils 80% reduction of flow
Venous drainage: facial vein
20 M External carotid artery PVA 70% reduction of flow
(facial branches and internal maxillary)
Venous drainage:internal maxillary vein,
facial vein into jugular veins
256 Ann. Ital. Chir., 82, 4, 2011
Treatment of high-flow arteriovenous malformations (AVMs) of the head and neck with embolization and surgical resection
been made in the last 10 years, both with respect to of the present cases were due to incomplete and inad-
the improvement in embolic materials (quick-acting N- equate initial surgical resections and subsequent use of
butyl cyanoacrylate glue, polyvinyl alcohol, thrombus- nonoptimal embolization. Appropriate patient selection
inducing coils, and Onyx liquid embolic fluid, or small and use of the right techniques are the main factors
balloons) and in knowledge of the anatomy of the that contribute to successful embolization in the over-
microcirculation. Djindjian and Merland 14 were the all management of extra-axial lesions of the head and
first to use superselective angiography and described in neck.
detail the possible complications of this technique. The The embolic material used is commonly made of
aim of embolization is to block the high-flow shunt polyvinyl alcohol, which is not absorbed and is avail-
between the arterial and venous systems. The reduction able in a series of particle sizes ranging from 0.15 to
or closing of AVMs renders resection and radiosurgery 1.0 mm in diameter. These particles expand by a factor
more accurate, safer, and easier. The potential risks asso- of 10-15 a few seconds after contact with the blood.
ciated with extra-axial embolization include the neuro- The angiographic protocol that we use is as follows.
logical defects caused by the reflux of the material First, diagnostic angiography is performed, followed by
occluding the intra-axial vessels that supply blood to selective embolization. All superselective embolization
the brain and the possible paralysis of cranial nerves procedures are performed within 24 hours before
caused by the closure of the small vessels of the exter- surgery. Access is via the femoral artery up to the
nal carotid artery supplying the cranial peripheral carotid and vertebral vessels; the vessel nearest to the
nerves. However, these complications are rare and are AVM is selected. Pressure measurements are then made
minimized by the experience of the operator 20. It is with a coaxial catheter in order to identify the possi-
essential that these procedures are performed in spe- ble risks of subsequent bleeding. If intracranial involve-
cialized centers, where there are clinicians with specif- ment is expected, temporary anesthesia with sodium
ic appropriate skills. The introduction of the direct- amytal can be applied to the vessels affected by the
flow embolization technique, and a better understand- AVM; this is known as “superselective Wada testing.”
ing of the principles of flow and occlusion have sig- This test provides for the evaluation of particular para-
nificantly lowered complication rates. meters (language, memory, spatial vision, sensitivity
Microshunts may appear after ligation of the main pow- and motor functions) within 5 minutes of general
er supply of the vessels, or due to incomplete emboliza- anesthesia to determine the possible involvement of the
tion, leading to a subtotal resection, after which the intracranial component and functions that arise from
possibility of relapse is often greater than it was for these locations that may in future lead to neurologi-
the primary lesion. The recurrences observed in two cal disorders during embolization or resection.
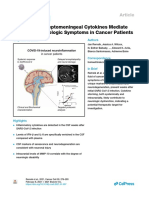
Fig. 1: External Carotid artery and superselective arteriography of inter- Fig. 2: Superselective embolization of maxillary artery with coils.
nal maxillary artery demonstrating high flow AVM interesting maxillary
and facial arteries.
Ann. Ital. Chir., 82, 4, 2011 257
V. Pompa, et al.
Conclusions resezione è il trattamento di scelta per MAV ad alto flus-
so, e la ricostruzione estetica con lembi può prevenire la
A multidisciplinary approach to the treatment of AVMs loro recidiva.
including interventional radiologists, surgeons, plastic
surgeons, anesthetists, and the blood bank has been rec-
ommended by many authors (e.g., 8,21,22). The References
inevitable development of neovascularization, often as a
result of intracranial surgery, may lead to further diffi- 1) Enjolras O: Classification and management of the various super-
culties. Adequate amounts of blood also need to be trans- ficial vascular anomalies: Haemangiomas and vascular malformations.
fused. J Dermatol, 1997; 24:701-10.
The total resection of large AVMs may not be possible, 2) Chang MW: Updated classification of haemangiomas and other
and so it is necessary to inform patients regarding the vascular anomalies. Lymphat Res Biol, 2003;1259-265.
possibility of a second operation. The consensus among 3) McHeik JN, Renauld V, Duport G, Vergnes P, Levard G:
surgeons is that superselective angiography alone is not Surgical treatment of haemangioma in infants. Br J Plast Surg, 2005;
satisfactory as a treatment, unless it is performed with- 58:1067-72.
in 24-48 hours before surgical resection.
4) Mulliken JB, Glowacki J: Haemangiomas and vascular malfor-
We recommend careful evaluation of AVMs and a com-
mations in infants and children: A classification based on endothelial
bined treatment protocol consisting of selective emboliza- characteristics. Plast Reconstr Surg, 1982; 69:412-22.
tion followed by total resection, ideally within 24 hours
7,8. 5) Watzinger F, Gössweiner S, Wagner A, Richling B, Millesi-
Schobel G, Hollmann K: Extensive facial vascular malformations and
haemangiomas: A review of the literature and case reports. J
Craniomaxillofac Surg, 1997; 25:335-43.
Riassunto
6) Leon-Villapalos J, Wolfe K, Kangesu L: GLUT-1: an extra diag-
OBIETTIVO: le malformazioni arterovenose (MAV) ad alto nostic tool to differentiate between haemangiomas and vascular mal-
flusso della testa e del collo sono piuttosto rare rispetto formations. Br J Plast Surg, 2005; 58:348-52.
a quelle a basso flusso, ma quando si verificano sono 7) Jackson IT, Carreño R, Potparic Z, Hussain K: Hemangiomas,
spesso accompagnate da emorragia massiva o si presen- vascular malformations, and lymphovenous malformations: Classification
tano con significativi difetti estetici. Il trattamento di and methods of treatment. Plast Reconstr Surg, 1993; 91:1216-230.
queste malformazioni è ad alto rischio ed è spesso nec- 8) Erdmann MW, Jackson JE, Davies DM, Allison DJ:
essario un approccio multidisciplinare per la valutazione Multidisciplinary approach to the management of head and neck arte-
e il loro trattamento. Tale trattamento dovrebbe includ- riovenous malformations. Ann R Coll Surg Engl, 1995; 77:53-59.
ere l’angioradiologia con l’embolizzazione preoperatoria 9) Rodesch G, Soupre V, Vazquez MP, Alvarez H, Lasjaunias P:
superselettiva, seguita dalla resezione chirurgica della Arteriovenous malformations of the dental arcades. The place of endovas-
lesione nelle seguenti 24 ore e la successiva ricostruzione cular therapy: Results in 12 cases are presented. J Craniomaxillofac Surg,
estetica. 1998; 26:306-13.
MATERIALI DI STUDIO: Abbiamo studiato una serie di 55
10) Coleman CC: Diagnosis and treatment of congenital arteriovenous
pazienti con MAV della testa e del collo che sono stati fistulas of the head and neck. Am J Surg, 1973; 126:557-65.
trattati chirurgicamente tra il 1999 e il 2009.
RISULTATI: Dei 55 pazienti con MAV, 7 avevano eman- 11) Allison DJ, Kennedy A: ABC of vascular diseases. Peripheral arte-
giomi e 48 avevano malformazioni vascolari, di cui 28 riovenous malformations. Br Med J, 1991; 303:1191-194.
sono state le lesioni a basso flusso e 20 sono state le 12) Kohout MP, Hansen M, Pribaz JJ, Mulliken JB: Arteriovenous
lesioni ad alto flusso (MAV). La sede più frequente delle malformations of the head and neck: Natural history and management.
lesioni ad alto flusso sono state le labbra. Tutte le 48 Plast Reconstr Surg, 1998; 102:643-54.
MAV sono state sottoposte a resezione chirurgica legata 13) Wu JK, Bisdorff A, Gelbert F, Enjolras O, Burrows PE,
ai sintomi, a propositi diagnostici, o per problemi esteti- Mulliken JB: Auricular arteriovenous malformation: Evaluation, man-
ci. Delle 20 MAV ad alto flusso, il 20% sono state clas- agement, and outcome. Plast Reconstr Surg, 2005; 115:985-95.
sificate come stadio I di Schobinger, 55% di stadio II, 14) Djindjian R, Merland JJ (eds): Superselective Angiography of the
e il 25% come stadio III. È stato utilizzato un tratta- External Carotid Artery. Berlin: Springer-Verlag, 1978; 76-88.
mento combinato di embolizzazione e resezione chirur-
gica per risolvere 13 del MAV ad alto flusso (fasi II e 15) Wynburn-Mason R: Arteriovenous aneurysm of midbrain and reti-
na, facial nevi and mental changes. Brain, 1943; 66:163-203.
III), di cui 4 hanno richiesto una ricostruzione estetica
con lembo chirurgico. 16) Bell J: The Principles of Surgery. London: Longman, Hurst, Rees,
CONCLUSIONE: I recenti progressi nella microchirurgia e 1815: 456.
nell’angioradiologia interventistica hanno notevolmente 17) Munro IR, Martin RD: The management of gigantic benign cran-
migliorato la prognosi per i pazienti affetti da queste iofacial tumours: The reverse facial osteotomy. Plast Reconstr Surg
malformazioni. Il trattamento combinato embolizzazione- 1980; 65:777-85.
258 Ann. Ital. Chir., 82, 4, 2011
Treatment of high-flow arteriovenous malformations (AVMs) of the head and neck with embolization and surgical resection
18) Mulliken JB, Murray JE, Castaneda AR, Kuban LB: 21) Apfelberg DB, Lane B, Marx MP: Combined (team) approach
Management of a vascular malformation of the face using total circu- to haemangioma management: Arteriography with superselective
latory arrest. J Gynecol Obstet, 1978; 146:168-72. embolization plus YAG laser/sapphire tip resection. Plast Reconstr Surg,
1991; 88:71-82.
19) Dawbarn RHM: The starvation operation for malignancy in the
external carotid area. JAMA, 1904; 17:792-95. 22) Jackson IT, Jack CR, Aycock B, Dubin B, Irons GB: The man-
agement of intraosseous arteriovenous malformations in the head and
20) Riche MC, Merland JJ: Embolization of vascular malformations.
neck areas. Plast Reconstr Surg, 1989; 84:47-54.
In: Mulliken JB, Young AE (eds). Vascular Birthmarks: Hemangiomas
and Malformations. Philadelphia: WB Saunders, 1988; 436-53.
Ann. Ital. Chir., 82, 4, 2011 259
View publication stats
You might also like
- Chen 2015Document6 pagesChen 2015nurminsyahNo ratings yet
- Intra Aortic Balloon Pump (IABP) 2009Document57 pagesIntra Aortic Balloon Pump (IABP) 2009nurminsyahNo ratings yet
- Ferreiro Et Al 2016Document18 pagesFerreiro Et Al 2016nurminsyahNo ratings yet
- Hiponatremia in CHFDocument5 pagesHiponatremia in CHFnurminsyahNo ratings yet
- EF4Document3 pagesEF4FugerMahdeneM'psrNo ratings yet
- Imaging AVMDocument5 pagesImaging AVMnurminsyahNo ratings yet
- Peripheral Vascular ExaminationDocument27 pagesPeripheral Vascular ExaminationnurminsyahNo ratings yet
- EF4Document3 pagesEF4FugerMahdeneM'psrNo ratings yet
- Avm TheraphyDocument11 pagesAvm TheraphynurminsyahNo ratings yet
- Anatomy PDFDocument163 pagesAnatomy PDFnurminsyahNo ratings yet
- Avm TheraphyDocument12 pagesAvm TheraphynurminsyahNo ratings yet
- Cardiology Ultrasound EmergencyDocument92 pagesCardiology Ultrasound Emergencybeeluvit81444No ratings yet
- Imaging AVMDocument5 pagesImaging AVMnurminsyahNo ratings yet
- Radiologi Aneurisma AortaDocument11 pagesRadiologi Aneurisma AortanurminsyahNo ratings yet
- LE Diagnosis and ManagementDocument14 pagesLE Diagnosis and ManagementnurminsyahNo ratings yet
- Avm TheraphyDocument12 pagesAvm TheraphynurminsyahNo ratings yet
- Diagnosisfor PEDocument28 pagesDiagnosisfor PEMohd Syaiful Mohd ArisNo ratings yet
- Cardiology Ultrasound EmergencyDocument92 pagesCardiology Ultrasound Emergencybeeluvit81444No ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Commissioning of A 15T Elekta Unity MR-linac A Sin PDFDocument13 pagesCommissioning of A 15T Elekta Unity MR-linac A Sin PDFMd. Ashikur RahmanNo ratings yet
- Management of Adult Sensorineural Hearing Loss: EtiologiesDocument10 pagesManagement of Adult Sensorineural Hearing Loss: EtiologiesaldimugniNo ratings yet
- A Survey On Brain Tumor Detection-TitlesDocument92 pagesA Survey On Brain Tumor Detection-TitlesDossDossNo ratings yet
- Remsik 2021Document12 pagesRemsik 2021MahmoudNo ratings yet
- Brain Computer InterfaceDocument30 pagesBrain Computer InterfacenehaNo ratings yet
- BioPsych - Reviewer (MIdterm Exam) - Chapter 1Document6 pagesBioPsych - Reviewer (MIdterm Exam) - Chapter 1Francis Xavier AlcazarNo ratings yet
- Dwnload Full Clinical Imaging With Skeletal Chest and Abdominal Pattern Differentials 3rd Edition Marchiori Test Bank PDFDocument36 pagesDwnload Full Clinical Imaging With Skeletal Chest and Abdominal Pattern Differentials 3rd Edition Marchiori Test Bank PDFcharlesdrakejth100% (11)
- DL5 Ifu 2023Document36 pagesDL5 Ifu 2023Prasanna VigneshNo ratings yet
- All About Seizures BrochureDocument13 pagesAll About Seizures BrochureALLIA LOPEZNo ratings yet
- Step 1: Calculate The Total MOH CostsDocument2 pagesStep 1: Calculate The Total MOH CostssmitharsNo ratings yet
- Forensic Radiography White PaperfinDocument38 pagesForensic Radiography White PaperfinMohy AbonohNo ratings yet
- Neuroimaging standards for research into small vessel diseaseDocument17 pagesNeuroimaging standards for research into small vessel diseaseDavid JuanNo ratings yet
- 10.1016/j.jns.2023.121122: Abstracts / Journal of The Neurological Sciences 455 (2023) 121048 38Document1 page10.1016/j.jns.2023.121122: Abstracts / Journal of The Neurological Sciences 455 (2023) 121048 38Amin AminiNo ratings yet
- Diagnostic Imaging of Lower Urinary Tract DiseaseDocument25 pagesDiagnostic Imaging of Lower Urinary Tract DiseaseSoyKlicheRodriguezNo ratings yet
- AIRIS II Standard DetailsDocument20 pagesAIRIS II Standard Detailsiqbal meerNo ratings yet
- Pelvic Bone LesionsDocument23 pagesPelvic Bone LesionsDavidJohnsonNo ratings yet
- MR Physics PrimerDocument98 pagesMR Physics PrimerLaurentiu Radoi100% (1)
- Regional Migratory Osteoporosis of The Knee: A Literature OverviewDocument6 pagesRegional Migratory Osteoporosis of The Knee: A Literature OverviewRobert Partarrieu StegmeierNo ratings yet
- M.tech ProjectDocument5 pagesM.tech ProjectSuresh NallaniNo ratings yet
- Ebook Download LinksDocument13 pagesEbook Download LinksPA201467% (3)
- Fundamentals of StereotaxyDocument45 pagesFundamentals of StereotaxyBenazir BegamNo ratings yet
- JAAOS - Volume 09 - Issue 01 January & February 2001Document70 pagesJAAOS - Volume 09 - Issue 01 January & February 2001kenthepaNo ratings yet
- 2014 @radiologylib William E Morgan Spinal MRI For MusculoskeletalDocument117 pages2014 @radiologylib William E Morgan Spinal MRI For MusculoskeletalkinexNo ratings yet
- Install-Config Guide - SureSigns VS4 Rel A.07Document96 pagesInstall-Config Guide - SureSigns VS4 Rel A.07CHRISTOPHER BURLESON100% (1)
- Lymphatic Drainage of Head and NeckDocument60 pagesLymphatic Drainage of Head and NeckKhadija VasiNo ratings yet
- Management of Sickle Cell Disease in Children: Review ArticleDocument8 pagesManagement of Sickle Cell Disease in Children: Review ArticleH. MD EbrNo ratings yet
- Guidelines For Management of Ischaemic Attack (En)Document51 pagesGuidelines For Management of Ischaemic Attack (En)Богдан ЛажетићNo ratings yet
- Histiocyte Society LCH Treatment GuidelinesDocument21 pagesHistiocyte Society LCH Treatment GuidelinesAshok KumarNo ratings yet
- M. Tech. (BMSP &I) RegulationsDocument24 pagesM. Tech. (BMSP &I) RegulationsarunaNo ratings yet
- High Intensitnd Hifu Can Control Prostate Cancer Fewer Side EffectsDocument9 pagesHigh Intensitnd Hifu Can Control Prostate Cancer Fewer Side EffectsRahul JhaNo ratings yet