Professional Documents
Culture Documents
86bf PDF
Uploaded by
CentanarianOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
86bf PDF
Uploaded by
CentanarianCopyright:
Available Formats
Int J Pharm Bio Sci 2014 Oct; 5(4): (B) 196 - 200
Research Article Biochemistry
International Journal of Pharma and Bio Sciences ISSN
0975-6299
SERUM URIC ACID - PHOSPHATE RATIO AS A DIFFERENTIAL
DIAGNOSTIC MARKER OF PROSTATE DISORDERS
SUDHA K, RESHMA K* AND AKSHATHA L N
Department of Biochemistry, Kasturba Medical College,
Mangalore, Manipal University Manipal ,India
ABSTRACT
Prostate cancer (PC), benign prostatic hyperplasia (BPH) and prostatitis are the most
common disorders of the prostate gland. Prostate specific antigen (PSA), the marker of
prostate cancer has shown reasonable sensitivity but has limited specificity for
distinguishing PC from BPH.This study attempts to evaluate the use of uric acid
phosphate ratio as a tool in differential diagnosis of prostate disorders. PSA, uric acid
and phosphate were estimated in serum of 75 patients with prostate disorders .PSA
levels were significantly high in PC compared to other disorders. Phosphate levels were
significantly lower in prostatitis patients, and an apparent increase in uric acid levels in
BPH patients. Serum uric acid phosphate ratio was markedly high in prostatitis followed
by BPH patients and least in PC establishing the role of the ratio in the differential
diagnosis of prostate disorders.
KEY WORDS: Prostate cancer, Prostatitis, Benign prostatic hyperplasia, Uric acid/phosphate
ratio
RESHMA K
Associate Professor Department of Biochemistry, Kasturba Medical College,
Mangalore, Manipal University Manipal ,India
This article can be downloaded from www.ijpbs.net
B - 196
Int J Pharm Bio Sci 2014 Oct; 5(4): (B) 196 - 200
INTRODUCTION
Prostate cancer is one of the most common MATERIALS AND METHODS
malignancies in old aged men in India.The
second most important prostate disorder of
75 patients with prostate disorders aged
the prostate includes benign prostatic
between 40-60 years and with serum PSA
hyperplasia (BPH) where accumulation of
levels greater than10 ng/ml were considered
dihydrotestosterone with aging leads to
for the study.25 patients had prostate cancer,
enlargement of prostate1.Bacterial prostatitis
25 had benign prostatic hyperplasia and 25
both acute and chronic are characterized by
had prostatitis. The study was approved by
inflammation due to urogenic infections of
Institutional ethics committee and informed
prostate gland2.Whether there is an
consent was taken from all the subjects.
association between the development of BPH
Prostate cancer was confirmed by biopsy
and PC is controversial 3.Prostate specific
report. Patients with acute urinary tract
antigen ( PSA) is the most common serum
infection, smokers, alcoholics and diabetics
marker of prostate cancer. PSA has shown
were excluded from the study. Fasting blood
reasonable sensitivity for detection of incipient
sample was collected in plain vacutainer and
cancer and can predict response to treatment
serum was used for estimations. Prostate
but in the critical diagnostic range of 4-
specific antigen was estimated by ECLIA in
10ng/ml it has limited specificityfor
4 Cobas e 41110. Serum uric acid was estimated
distinguishing PC from BPH . A mounting
by uricase -peroxidase method and phosphate
body of evidence suggests that increased
was estimated by ammonium
production of reactive oxygen species(ROS) is
phosphomolybdate end point method
linked to inflammatory diseases, aging
spectrophotometrically11.Statistical analysis
processes and to etiopathogenesis of age
was done using ANOVA to compare the data
related diseases like PC and BPH
5 between the three diseases. Correlation study
.Association of uric acid an extracellular
was done by Kruskalwalis test12.
antioxidant with inflammation is an established
fact. Hyperuricemia in cancer patients is
thought to result from increased nucleic acid RESULTS
turnover in rapidly proliferating tissue 6. The
complexity of acute and chronic inflammatory The present study clearly indicates that
process may either lead to prostate prostate cancer is more prevalent in men who
hyperplasia and / or prostate cancer. Prostate are in age group of more than 65 years.
cells are activated by chemokines and trigger Followed by BPH which is more common in
processes like angiogenesis, cellular growth men above 55 years of age .Prostatitis is
and extravasation as well as neoplasia7. found to be highly prevalent in younger age
Experimental and clinical data implicate group. PSA levels were significantly higher in
calcium as the risk factor in development of serum of men with prostate cancer (p<0.000)
prostate cancer8, Serum levels of calcium compared to BPH and prostatitis. Post hoc
correlated with PSA which supported the test revealed that the difference was more
hypothesis that hypercalcemia may stimulate significant between prostate cancer and
prostate cancer9, however data on relation BPH(p<0.002) and slightly less significant
between phosphate ions and PC or BPH is between PC and prostatitis (p<0.01). Serum
sparse. Hence, the present study aims at phosphate level was significantly lower in
evaluating uric acid and phosphate in the prostatitis compared to the other two groups
serum of patients with prostatic disorders and (p<0.008). The difference was much more
then exploring the possibility of using the ratio significant between BPH and prostatitis
in differential diagnosis. (p<0.006).There was an apparent increase in
serum uric acid in BPH than prostatitis and
PC. Though the mean uric acid showed
considerable variations across the groups,
post hoc test did not show any significance
This article can be downloaded from www.ijpbs.net
B - 197
Int J Pharm Bio Sci 2014 Oct; 5(4): (B) 196 - 200
between the groups. Uric acid phosphate ratio was statistically significant in BPH (r =0. 344,
was also markedly high in prostatitis, followed p < 0.05) (Table 2). There was a negative
by BPH and cancer. However, the values correlation between PSA and uric acid
were statistically insignificant. (Table 1) There phosphate ratio in all the three disorders (r=-
was a positive correlation between PSA and 0.619), though it was statistically significant
age in all the three prostate disorders which only for PC. (Table 3)
Table 1
Comparisons of PSA , Uric acid, Phosphate and Uric acid/Phosphate ratio in
PC, Prostatitis and BPH ( Mean +SD)
Prostate cancer BPH Prostatitis
(n=25) (n=25) (n=25)
AGE 73.62+9.34 67.70+8.28 61.28+15.67
a c
PSA(ng/mL) 118.27+77.7*** 9.42+6.98 14.22+7.38
URIC ACID (UA) 6.6+3.83 13.18+9.27 9.44+3.84
(mg/dL)
b
PHOSPHATE(P) 4.4+1.49 4.82+1.54 3.25+0.93*
(mg/dL)
UA/P 1.64+0.79 2.7+1.68 3.02+1.34
***p<0.000 significantly different from BPH &Prostatitis
*p=0.008 statistically different from BPH &PC
a; p=0.002, c ; p<0.01significantly different from PC
b ;p=0.006significantly different from Prostatitis
Table 2
Correlation of PSA with Age in prostate disorders
r p
Prostatitis -0.327 0.326
BPH 0.530 0.05*
Prostate Cancer 0.569 0.05*
*Statistically significant
Table 3
Correlation of PSA with uric acid phosphate ratio in prostate disorders
r p
Prostatitis -0.173 0.612
BPH -0.113 0.53
Prostate Cancer -0.619 0.05*
*Statistically significant
DISCUSSION
PSA an androgen regulated protease and prostatitis. However PSA level has low
produced by prostate epithelial cell and specificity as BPH and prostatitis could not be
prostate cancer cells increase in prostatitis, differentiated further in this study. PSA level
BPH,prostate cancer, acute urinary retention were higher in prostatitis compared to BPH.
and renal failure13.Though PSA had a limited Earlier studies on PSA indicate that in the
capacity in distinguishing prostate cancer and critical diagnostic range of 4 to 20 ng per ml
BPH due to considerable overlap,in the PSA had limited capacity for distinguishing
present study PSA level were significantly early prostate cancer and BPH. In cancer and
higher in cancer patients compared to BPH inflammatory disorders, oxidative stress, an
This article can be downloaded from www.ijpbs.net
B - 198
Int J Pharm Bio Sci 2014 Oct; 5(4): (B) 196 - 200
innate key event characterized by supra level was slightly lowered in patients with
physiological reactive oxygen species has prostate cancer compared to that of BPH.
been identified as one of the hall mark of Supporting the above data a case study
disease progression14.One of the studies showing hypophosphatemia and hyper
showed that various inflammatory processes phosphaturia in a 65 year old man with
and cell biological cascades are involved in prostate cancer has been reported24.Prostate
the etiopathogenesis of either Prostatitis, BPH cancer induced oncogenic
or prostate cancer15.. In the present study uric hypophosphatemicosteomalacia. Calcitriol
acid level were markedly high in BPH slows the rate of PSA secretion into serum
compared to the other two groups clearly providing indirect evidence for a protective
suggesting the role of uric acid as a novel influence of high vitamin D3 on prostate
growth factor .Supporting our findings cancer23. Thus it can be argued that low
16
Hammarstemet.al also observed serum phosphate level in prostatitis is
hyperuricemia in patients with BPH, advantageous in preventing development of
underlining the hypothesis of an association of cancer. Hypophosphatemia stimulates
hyperuricemia in development of BPH. In one activation of vitamin D3 and increases
of the earlier studies patients with prostate circulating calcitriol25. In this study uric acid
cancer and chronic prostatitis presented with phosphate ratio was markedly high in BPH
decreased antioxidant capacity5.Lopez compared to prostate cancer. Mean U/P ratio
Lauret.al 18 also did not support the theory of in BPH was double that of PC indicating the
protective role of uric acid against PC fact that the ratio can be used as a marker
occurrence. Further hypouricemia in cancer that can differentiate between BPH and
patient is thought to reflect increased renal prostate cancer,The ratio higher in prostatitis
secretion as a result of tubular damage or compared to BPH also suggests the
tumour related humoral factor19.However, importance of U/P ratio in differential
Hammarsten et al 20considered hyperuricemia diagnosis of prostate disorder.
as a risk factor in development of prostate
cancer. Low uric acid level in prostate cancer CONCLUSION
and prostatitis observed in the present study is
well supported by an earlier study which
PSA had low specificity and additional
shows significantly low uric acid and depletion
biomarker was needed to differentiate
of antioxidant in prostate cancer patients with
between prostate cancer and BPH. In this
high PSA level 21, although it is not in
article we evaluated a novel approach to find a
agreement with one of the earlier studies22 In
diagnostic marker for prostate disorders. The
the present study patients with prostatitis have
study supports the utility of UA/P ratio as a
significantly lower inorganic phosphate level in
diagnostic marker for BPH and offers an
serum compared to patients with prostate
alternative sensitive unique marker in
cancer and BPH. Hypophosphatemia
differentiating BPH and PC.
stimulate active vitamin D3 production which
has anti tumour effect in prostate23,phosphate
REFERENCES
1. Isaacs JT, Coffey DS. Etiology and Hyperplasia--a risk factor for developing
disease process of benign prostatic clinical prostate cancer. Scand J Urol
Hyperplasia. Prostate Suppl, 2:33-50, Nephrol, 36(5):330-8,(2002).
(1989). 4. Balk SP, Ko YJ, Bubley GJ. Biology of
2. Habermacher GM, Chason JT, Schaeffer prostate-specific antigen.J ClinOncol.,
AJ. Prostatitis/chronic pelvic pain 21(2):383-91,(2003).
Syndrome.Annu Rev Med, 57:195- 5. PaschosA, PandyaR, DuivenvoordenW C
206,(2006). M and J H Pinthus.Oxidative stress in
3. Hammarsten J, Högstedt B. Calculated prostate cancer: changing research
fast-growing benign prostatic concepts towards a novel paradigm for
This article can be downloaded from www.ijpbs.net
B - 199
Int J Pharm Bio Sci 2014 Oct; 5(4): (B) 196 - 200
prevention and therapeutics.Prostate Biomedical Research, 23(2): 227-
Cancer and Prostatic Diseases, 16:217- 230,(2012).
225,(2013). 17. Hammarsten J, Högstedt B. Calculated
6. Khaja, Hajera. Uric acid as a growth fast-growing benign prostatic
factor for activated B cells. Medical Hyperplasia--a risk factor for eveloping
biophysics, 2:101, (2009). clinical prostate cancer. Scand J
7. König JE, Senge T, Allhoff EP, König W. UrolNephrol., 36(5):330-8, (2002).
Analysis of the inflammatory network In 18. LópezLaur JD, Abud M, López Fontana
benign prostate hyperplasia and prostate C, Silva J, Cisella Y, Pérez Elizalde R,
cancer. Prostate. 58(2):121-9,(2004). Ortiz A. Antioxidant power and cellular
8. Edward Giovannucci, Yen Liu, Meir JS, damage in prostate cancer. Arch EspUrol,
Walter CW Cancer. A prospective study 61(5):563-9, (2008).
of calcium intake and incident and fatal 19. Kolonel LN, Yoshizawa C, Nomura AM,
prostate cancer. Epidemiol Biomarkers Stemmermann GN. Relationship of serum
Prev, 15(2):203-10,(2006). uric acid to cancer occurrence in a
9. Balk SP,Ko YJ, BubleyCJ.Biology of prospective male cohort. Cancer
prostate specific antigen.J.Clin Epidemiol Biomarkers Prev., 3(3):225-8,
Oncol,21(2):383- 91, (2003). (1994).
10. Roddam AW, Rimmer J, Nickerson C, 20. Hammarsten J, Högstedt B. Clinical,
Ward AM. Prostate-specific antigen: bias haemodynamic, anthropometric,
and molarity of commercial assays for metabolic and insulin profile of men with
PSA in use in England. Ann Clin high-stage and high-grade clinical
Biochem, 43:35-48,(2006). prostate cancer. Blood Press,13(1):47-
11. Newmann DJ, Price CP. Renal function 55,(2004).
and nitrogen metabolites.In:Burtis CA 21. Akinloye O, Adaramoye O, Kareem O.
Ashwood ER,editors.Teitz text book of Changes in antioxidant status and lipid
Clinical Chemistry.3rded.Philadelphia:WB peroxidation in Nigerian patients with
Saunders Company,1204-70:(1999). prostate carcinoma. Pol Arch Med Wewn,
12. Daly JA and Ertingshausen G. Direct 119(9):526-32,(2009).
method for determining inorganic 22. Bhagyalakshmi A, Sampath Kumar V,
phosphate in serum with the “centrifi Rama Devi, Rama Rao J, Harini.
chem”.Clin.Chem,18:263-265,(1972). Comparative study of biochemical
13. Jan Hammarsten & Ralph markers in prostatitis,BPH & carcinoma of
Peeker .Urological aspects of the prostate with and without
metabolic syndrome.Nature Reviews metastasis.IJPBS,2(2):117-122,(2012).
Urology, 8:483-494,(2011). 23. Edward G, Eric B, Alicja W, AlbertsA ,
14. AdedapoKS, ArinolaOG, ShittuOB, Meir JS, Graham AC, Walter CW
KareemOI, OkoloCA, NwobiLN. .Calcium and fructose intake in relation to
Diagnostic value of lipids, total risk of prostate cancer. Cancer Research.
antioxidants, and trace metals in benign 58: 442-447, (1998).
prostate hyperplasia and prostate cancer. 24. Nakahama H, Nakanishi T, Uno H,
Niger J ClinPract, 15(3):293-297, (2012). Takaoka T,Taji N,Uyama O,Kitada O,
15. Shapiro E, Becich MU, Hartanto V, Lepor Sugita M, Miyauchi A,Sugishita T, Fujita
H. The relative proportion of stromal and T.Prostate Cancer-Induced Oncogenic
epithelial hyperplasia is related to the Hypophosphatemic OsteomalaciaUrol
development of symptomatic benign Int,55:38–40,(1995).
prostate hyperplasia. The Jr of Urology, 25. Jennifer W, Gary GS, David CS, Robert
147(5): 1293-1297, (1992). B. Phase trial of oral 1,25 dihydroxy
16. Vinod Chandran, Anitha M, Avinash SS, vitamin D (calcitriol) in hormone refractory
Gayathri M Rao, Beena V Shetty, SudhaK prostate cancer .N Engl J Med, 351:1513-
. Protein oxidation: A potential cause of 1520,(2004).
hypoalbuminemia in oral cancer.
This article can be downloaded from www.ijpbs.net
B - 200
You might also like
- McGill Pain QuestionnaireDocument6 pagesMcGill Pain Questionnairejimitkapadia100% (1)
- CASE STUDY ON ACUTE Renal FailureDocument38 pagesCASE STUDY ON ACUTE Renal FailureOdey Godwin100% (1)
- Prostate CancerDocument4 pagesProstate CancerNadia SalwaniNo ratings yet
- Genetic Disorders: A Look at Von Willebrand Disease, Cystic Fibrosis, Huntington's Disease and MoreDocument18 pagesGenetic Disorders: A Look at Von Willebrand Disease, Cystic Fibrosis, Huntington's Disease and MoreDiya 2787% (69)
- Malawi 2014 Malawi Obstetric and Gynaecology Protocols GuidelinesDocument105 pagesMalawi 2014 Malawi Obstetric and Gynaecology Protocols GuidelinesHải Ly Đào100% (1)
- PediatricsDocument87 pagesPediatricsCarlos HernándezNo ratings yet
- Delivery Room Drug StudyDocument9 pagesDelivery Room Drug Studymacel sibayan100% (9)
- Biliary Tract Surgery in Dogs and CatsDocument5 pagesBiliary Tract Surgery in Dogs and CatsEsther ArifinNo ratings yet
- Test Bank For Medical Surgical Nursing Concept & Practices 2nd Edition, DeWitDocument24 pagesTest Bank For Medical Surgical Nursing Concept & Practices 2nd Edition, DeWitILL10167% (3)
- STREPTOMYCINDocument3 pagesSTREPTOMYCINChad InongNo ratings yet
- 86bf PDFDocument5 pages86bf PDFCentanarianNo ratings yet
- Benign Prostatic Hyperplasia: Does Prostate Size Matter?: N P BPHDocument6 pagesBenign Prostatic Hyperplasia: Does Prostate Size Matter?: N P BPHganangahimsaNo ratings yet
- 119 Iajps119122017Document5 pages119 Iajps119122017Baru Chandrasekhar RaoNo ratings yet
- Advances in Prostatic Diagnostics in Dogs 2018Document4 pagesAdvances in Prostatic Diagnostics in Dogs 2018Orlando Karim Shiro Jr.No ratings yet
- Comparison of Serum Microseminoprotein-Beta (MSMB) With Total Prostate Specific Antigen (TPSA) in The Diagnosis of Prostate Cancer in African MenDocument7 pagesComparison of Serum Microseminoprotein-Beta (MSMB) With Total Prostate Specific Antigen (TPSA) in The Diagnosis of Prostate Cancer in African MenInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- TheprostatepaperDocument12 pagesTheprostatepapermarlonkoesenNo ratings yet
- 5ARI e PSA: Questioni Aperte: Original ArticleDocument5 pages5ARI e PSA: Questioni Aperte: Original ArticleCentanarianNo ratings yet
- JR BPHDocument29 pagesJR BPHHandre PutraNo ratings yet
- Incidentally Diagnosed Adenocarcinoma Prostate After Surgery For Clinically Benign Prostatomegaly A 2 Years Retrospective StudyDocument6 pagesIncidentally Diagnosed Adenocarcinoma Prostate After Surgery For Clinically Benign Prostatomegaly A 2 Years Retrospective StudyIJAR JOURNALNo ratings yet
- Hubungan Usia Dengan Kadar Prostate SpecDocument5 pagesHubungan Usia Dengan Kadar Prostate SpecSuyat SuyatmiNo ratings yet
- Urologi 2018Document10 pagesUrologi 2018Albarr YusufNo ratings yet
- Jurnal B.inggris Kanker Prostat PDFDocument17 pagesJurnal B.inggris Kanker Prostat PDFBoni Mohammad SalehNo ratings yet
- LATIL - PERMIN - The Prostate - 2015Document11 pagesLATIL - PERMIN - The Prostate - 2015Mavos OdinNo ratings yet
- Assessment of Factors Associated With PSA Level in Prostate Cancer Cases and Controls From Three Geographical RegionsDocument16 pagesAssessment of Factors Associated With PSA Level in Prostate Cancer Cases and Controls From Three Geographical RegionsAbdikarim MohamedNo ratings yet
- Metabolics SyndromeDocument10 pagesMetabolics SyndromeWerry 21No ratings yet
- Jolly 2015Document13 pagesJolly 2015BalkisBenHassineNo ratings yet
- Journal of Photochemistry & Photobiology, B: BiologyDocument6 pagesJournal of Photochemistry & Photobiology, B: BiologyGabriel ŞarguNo ratings yet
- Diagnostic Utility of Protein To Creatinine RatioDocument21 pagesDiagnostic Utility of Protein To Creatinine RatioDinda YenviartiNo ratings yet
- NIH Public Access: Opposing Roles of Folate in Prostate CancerDocument12 pagesNIH Public Access: Opposing Roles of Folate in Prostate Cancermumu4loveNo ratings yet
- 3567 FullDocument4 pages3567 FullRyuuParisudhaNo ratings yet
- Low Serum Testosterone Is A Predictor of High-Grade Disease in Patients With Prostate CancerDocument7 pagesLow Serum Testosterone Is A Predictor of High-Grade Disease in Patients With Prostate CancerJuninho BatistaNo ratings yet
- Useful For: Alpha-Fetoprotein (AFP) Tumor Marker, SerumDocument3 pagesUseful For: Alpha-Fetoprotein (AFP) Tumor Marker, SerumGeralden Vinluan PingolNo ratings yet
- BPH and Prostate Cancer RiskDocument9 pagesBPH and Prostate Cancer RiskEvita LarasNo ratings yet
- Aur v2 Id1016Document5 pagesAur v2 Id1016weisiNo ratings yet
- NIH Public Access: Cholesterol and Benign Prostate DiseaseDocument20 pagesNIH Public Access: Cholesterol and Benign Prostate DiseasejojdoNo ratings yet
- PIIS097368831830032XDocument5 pagesPIIS097368831830032Xella faotNo ratings yet
- NIH Public Access: Author ManuscriptDocument21 pagesNIH Public Access: Author ManuscriptgiannidietNo ratings yet
- 10.1515@cclm-2019-0693 GGGDocument14 pages10.1515@cclm-2019-0693 GGGGrace Pinto AlvarezNo ratings yet
- Articulo - PsaDocument9 pagesArticulo - PsaGrace Pinto AlvarezNo ratings yet
- My Final SeminarDocument40 pagesMy Final SeminartimiiniyiiNo ratings yet
- Study of Heart Rate Variability in Benign Prostatic Hyperplasia - A Hospital-Based StudyDocument3 pagesStudy of Heart Rate Variability in Benign Prostatic Hyperplasia - A Hospital-Based Studydwi-148502No ratings yet
- 10 1177@1535370217693117 PDFDocument27 pages10 1177@1535370217693117 PDFsafrinaNo ratings yet
- Etiology, Epidemiology, and Natural History HBPDocument13 pagesEtiology, Epidemiology, and Natural History HBPuricoletNo ratings yet
- Benign Prostatic Hyperplasia A ReviewDocument3 pagesBenign Prostatic Hyperplasia A ReviewKIU PUBLICATION AND EXTENSIONNo ratings yet
- Assesmentof Fibro Q Test, AAR & APRI Indices As Markers of Fibrosis in Chronic Liver DiseaseDocument5 pagesAssesmentof Fibro Q Test, AAR & APRI Indices As Markers of Fibrosis in Chronic Liver Diseaseferdinan goutamaNo ratings yet
- Serum PSA Concentration Is Powerfull Predictor of Acute Urinary Retension and Need For Surgery in Men With BPHDocument8 pagesSerum PSA Concentration Is Powerfull Predictor of Acute Urinary Retension and Need For Surgery in Men With BPHArga Putra PradanaNo ratings yet
- Non invasve marksers of iver fibrosis in nafldDocument3 pagesNon invasve marksers of iver fibrosis in nafldSvt Mscofficial2No ratings yet
- Clinical Nutrition: Emma Louise Metcalfe, Alison Avenell, Andrew FraserDocument8 pagesClinical Nutrition: Emma Louise Metcalfe, Alison Avenell, Andrew FraserHadi KuriryNo ratings yet
- Brain, Behavior, and Immunity: Chamindie PunyadeeraDocument2 pagesBrain, Behavior, and Immunity: Chamindie PunyadeeraSabiran GibranNo ratings yet
- Bioscientific Review (BSR) : The Correlation Between Alpha-Fetoprotein and Liver Function TestsDocument10 pagesBioscientific Review (BSR) : The Correlation Between Alpha-Fetoprotein and Liver Function TestsUMT JournalsNo ratings yet
- Imaging in BPHDocument6 pagesImaging in BPHadityaNo ratings yet
- To Estimate The Uric Acid Levels in Patients With Polycystic Ovarian Syndrome (Pcos)Document5 pagesTo Estimate The Uric Acid Levels in Patients With Polycystic Ovarian Syndrome (Pcos)IJAR JOURNALNo ratings yet
- Pa Tho PhysiologyDocument9 pagesPa Tho PhysiologyMabz Posadas BisnarNo ratings yet
- Hepatits PatientsDocument5 pagesHepatits PatientsCharles RajNo ratings yet
- Patofisiologi BPHDocument7 pagesPatofisiologi BPHAghfira Putri AnderiNo ratings yet
- Chronic Prostatitis A Possible Cause of HematospermiaDocument6 pagesChronic Prostatitis A Possible Cause of HematospermiaZlatan ZvizdicNo ratings yet
- Correlation of Serum Alanine Aminotransferase and Aspartate Aminotransferase Levels To Liver Histology in Chronic Hepatitis CDocument5 pagesCorrelation of Serum Alanine Aminotransferase and Aspartate Aminotransferase Levels To Liver Histology in Chronic Hepatitis CSaba KhanNo ratings yet
- ProCaSS Intervention Tool (Final 23-07)Document47 pagesProCaSS Intervention Tool (Final 23-07)Lim ZXNo ratings yet
- Ceju 66 00246Document4 pagesCeju 66 00246Àlex MataNo ratings yet
- The Research of The Application of A New Urinary BDocument7 pagesThe Research of The Application of A New Urinary BNealNo ratings yet
- Babaian 2001Document4 pagesBabaian 2001Benny KurniawanNo ratings yet
- The Threshold of Alpha-Fetoprotein (AFP) For The Diagnosis of Hepatocellular Carcinoma: A Systematic Review and Meta-AnalysisDocument21 pagesThe Threshold of Alpha-Fetoprotein (AFP) For The Diagnosis of Hepatocellular Carcinoma: A Systematic Review and Meta-AnalysisMariskaNo ratings yet
- Arc BPH Chapter1Document8 pagesArc BPH Chapter1Civa NuhaNo ratings yet
- PsakineticsDocument6 pagesPsakineticsRicardo Alfredo Valderrama GómezNo ratings yet
- Rev. SystDocument9 pagesRev. Systdr.israquiNo ratings yet
- Diet and Lifestyle Recommendations for Prostate Cancer PatientsDocument24 pagesDiet and Lifestyle Recommendations for Prostate Cancer PatientsLuis C Ribon VNo ratings yet
- 10 1 1 915 1495 PDFDocument8 pages10 1 1 915 1495 PDFWahyonoNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 17: OncologyFrom EverandComplementary and Alternative Medical Lab Testing Part 17: OncologyNo ratings yet
- 5ARI e PSA: Evidenze: Giuseppe Morgia, Daniele Urzì, Giorgio Ivan RussoDocument8 pages5ARI e PSA: Evidenze: Giuseppe Morgia, Daniele Urzì, Giorgio Ivan RussoCentanarianNo ratings yet
- 5ARI e PSA: Questioni Aperte: Original ArticleDocument5 pages5ARI e PSA: Questioni Aperte: Original ArticleCentanarianNo ratings yet
- Inventions.: Generally ExperiencedDocument1 pageInventions.: Generally ExperiencedCentanarianNo ratings yet
- Ijcmr 1579 v1Document5 pagesIjcmr 1579 v1YaserNo ratings yet
- The Caliber and Length of The Urethra in Asymptomatic Taiwanese Adult FemalesDocument3 pagesThe Caliber and Length of The Urethra in Asymptomatic Taiwanese Adult FemalesCentanarianNo ratings yet
- Ecr2012 C-1412Document10 pagesEcr2012 C-1412CentanarianNo ratings yet
- Acr-Spr Practice Parameter For The Performance of Fluoroscopic and Sonographic Voiding Cystourethrography in ChildrenDocument11 pagesAcr-Spr Practice Parameter For The Performance of Fluoroscopic and Sonographic Voiding Cystourethrography in ChildrenCentanarianNo ratings yet
- Micturating CystourethrogramDocument3 pagesMicturating CystourethrogramCentanarianNo ratings yet
- Micturating CystourethrogramDocument3 pagesMicturating CystourethrogramCentanarianNo ratings yet
- Journal of Indian Association of Pediatric SurgeonsDocument23 pagesJournal of Indian Association of Pediatric SurgeonsCentanarianNo ratings yet
- Voiding Cystourethrogram - VCUGDocument3 pagesVoiding Cystourethrogram - VCUGCentanarianNo ratings yet
- Urethral Stricture Disease: Evaluation of The Male UrethraDocument5 pagesUrethral Stricture Disease: Evaluation of The Male UrethraCentanarianNo ratings yet
- Urethral Stricture Disease: Evaluation of The Male UrethraDocument5 pagesUrethral Stricture Disease: Evaluation of The Male UrethraCentanarianNo ratings yet
- Acta Med Iran 2012 50 7 468 472 4Document5 pagesActa Med Iran 2012 50 7 468 472 4CentanarianNo ratings yet
- Diameter UretraDocument5 pagesDiameter Uretraduo_ngoNo ratings yet
- Voiding Cystourethrogram - VCUGDocument3 pagesVoiding Cystourethrogram - VCUGCentanarianNo ratings yet
- c1Document5 pagesc1CentanarianNo ratings yet
- Ureteroscopy Techniques and Outcomes for Treating Kidney Stones and CancerDocument66 pagesUreteroscopy Techniques and Outcomes for Treating Kidney Stones and CancerCentanarianNo ratings yet
- Northwestern Medicine Cystoscopy NMHDocument3 pagesNorthwestern Medicine Cystoscopy NMHCentanarianNo ratings yet
- Agenda Per 041016 Kanoppi End of Project ReviewDocument2 pagesAgenda Per 041016 Kanoppi End of Project ReviewCentanarianNo ratings yet
- 04A Appendix4APLATAManuscript SFMGPQ v10 25FEB2013Document7 pages04A Appendix4APLATAManuscript SFMGPQ v10 25FEB2013bagusNo ratings yet
- Adelia Permatasari Wolfram Medical ReportDocument5 pagesAdelia Permatasari Wolfram Medical ReportCentanarianNo ratings yet
- Pain Impact and Emotional Distress QuestionnaireDocument1 pagePain Impact and Emotional Distress QuestionnaireCentanarianNo ratings yet
- c1Document19 pagesc1CentanarianNo ratings yet
- c1Document19 pagesc1CentanarianNo ratings yet
- 04A Appendix4APLATAManuscript SFMGPQ v10 25FEB2013Document7 pages04A Appendix4APLATAManuscript SFMGPQ v10 25FEB2013bagusNo ratings yet
- Iief PDFDocument3 pagesIief PDFCentanarianNo ratings yet
- Cognitive Psychology DefinitionDocument30 pagesCognitive Psychology DefinitionJuvy IringanNo ratings yet
- Blood Brain Barrier PDFDocument5 pagesBlood Brain Barrier PDFRoxanA BocaNo ratings yet
- HIV-Associated Dementia GuideDocument3 pagesHIV-Associated Dementia GuideintanpalupiNo ratings yet
- Poultry Necropsy BasicsDocument25 pagesPoultry Necropsy BasicsDr.Kedar Karki ,M.V.Sc.Preventive Vet.Medicine CLSU Philippines100% (4)
- (THT) Allergic Rhinitis For Medical StudentDocument40 pages(THT) Allergic Rhinitis For Medical StudentTheresia Radinda FelimNo ratings yet
- Seminar Post Test I - FeedbackDocument2 pagesSeminar Post Test I - FeedbackNICOLE ANNE MAE PASCUALNo ratings yet
- OSCE Chart Cough (KK)Document4 pagesOSCE Chart Cough (KK)api-26938624No ratings yet
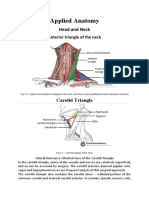
- Applied Anatomy of the Head and NeckDocument9 pagesApplied Anatomy of the Head and NeckdivinaNo ratings yet
- FUO-6th Year MedicineDocument25 pagesFUO-6th Year MedicineananNo ratings yet
- Pathophysiology of Type 1 DiabetesDocument14 pagesPathophysiology of Type 1 DiabetesBoNo ratings yet
- BilirubinDocument3 pagesBilirubinIkhza LastPandawaNo ratings yet
- DermatologyDocument120 pagesDermatologyMustafa Thaier Al-KaraghouliNo ratings yet
- Assessment of Chest PainDocument59 pagesAssessment of Chest PainMaria GarabajiuNo ratings yet
- Raktapitta With Reference To Thrombocytopenia A Conceptual StudyDocument4 pagesRaktapitta With Reference To Thrombocytopenia A Conceptual StudyEditor IJTSRDNo ratings yet
- Pathophysiology of Diabetes MellitusDocument3 pagesPathophysiology of Diabetes MellitusFc ßobby HechanovaNo ratings yet
- Case Study: International Journal of Current ResearchDocument2 pagesCase Study: International Journal of Current ResearchUtami MayasariNo ratings yet
- Anesthesia Lecture 1Document16 pagesAnesthesia Lecture 1drhiwaomer100% (9)
- Vitamin D DeficiencyDocument8 pagesVitamin D DeficiencyAyeza DuaNo ratings yet
- WSCProceedings2008 2009Document315 pagesWSCProceedings2008 2009Anbu AzhaganNo ratings yet
- Case 3-2020: A 44-Year-Old Man With Weight Loss, Diarrhea, and Abdominal PainDocument10 pagesCase 3-2020: A 44-Year-Old Man With Weight Loss, Diarrhea, and Abdominal PainAlvaro Andres Flores JimenezNo ratings yet
- Chromosome MappingDocument4 pagesChromosome MappingJonelle U. BaloloyNo ratings yet