Professional Documents
Culture Documents
Retinal Occlusion
Retinal Occlusion
Uploaded by
Deni TionCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Retinal Occlusion
Retinal Occlusion
Uploaded by
Deni TionCopyright:
Available Formats
Chapter 10
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
Retinal Vein Occlusions
Jost B. Jonas a · Jordi Monés b · Agnès Glacet-Bernard c · Gabriel Coscas c
a Department of Ophthalmology, Medical Faculty Mannheim, University of Heidelberg, Mannheim, Germany; b Institut de la
Màcula i de la Retina, Barcelona, Spain; c Service Universitaire d’Ophtalmologie, Hôpital Intercommunal de Créteil, Créteil, France
Abstract (vascular endothelial growth factor) drugs (bevacizumab,
Retinal vein occlusions (RVOs) have been defined as reti- ranibizumab, aflibercept) may be intravitreally adminis-
nal vascular disorders characterized by dilatation of reti- tered, avoiding the irreversibly destructive effect of laser
nal veins with retinal and subretinal hemorrhages, macu- coagulation, which previously was applied in a ‘grid’ pat-
lar edema, and a varying degree of retinal ischemia. tern over the extrafoveolar leaking area. The side effects
Retinal angiography, either as fluorescein and indocya- of intraocularly applied steroids in relatively young pa-
nine green (ICG) angiography or in the form of optical tients including cataract formation and ocular hyperten-
coherence tomography (OCT)-based angiography, is es- sion have to be considered. © 2017 S. Karger AG, Basel
sential for the diagnosis and assessment of the prognosis
of RVOs. It allows the differentiation of diverse types of
RVOs, such as perfused or nonperfused, as well as the de- Retinal vein occlusions (RVOs) have been de-
tection of different modalities in the natural history of fined as retinal vascular disorders characterized
RVOs. OCT angiographic imaging in combination with by engorgement and dilatation of the retinal veins
dye angiography (fluorescein or ICG) is the most effective due to increased retinal venous blood pressure,
method to assess the amount and location of cystoid with secondary (mostly) intraretinal hemorrhag-
macular edema and the persistence, regression, and de- es; (mostly) intraretinal (and partially subretinal)
gree of ischemia. OCT can additionally display the pres- edema which can also include the foveal region
ence and integrity of the outer limiting membrane and of and which can lead to hard retinal exudates as de-
the inner and outer segments of the photoreceptors as posits of lipids; and a varying degree of retinal
useful biomarkers for the prognosis and as a guide for the ischemia including cotton wool spots as signs of
treatment of RVO. Due to the relatively often benign and it (Hayreh, 1964; Hayreh, 1965; Coscas et al.,
self-limiting course of nonischemic RVOs, therapy may 1978; Hayreh, 1983; The Central Vein Occlusion
initially be delayed. If macular edema extends into the Study, 1993; The Central Vein Occlusion Study
foveolar region and persists, intravitreal medical therapy Group M report, 1995; The Central Vein Occlu-
including steroids (triamcinolone; fluocinolone or dexa- sion Study Group N report, 1995; Hayreh et al.,
methasone in slow-release devices) and/or anti-VEGF 1990; Coscas et al., 1984)1–9.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Downloaded by:
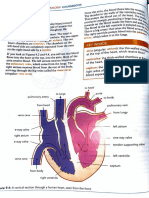
Fig. 1. Fundus photograph showing a CRVO. Fig. 2. Fundus photograph showing a superior temporal
BRVO.
As soon as the foveal region is involved in 1978)1–3. In ischemic RVO, there are well-estab-
macular edema, central visual acuity drops. lished stigmata of inner retinal ischemia, includ-
RVOs are differentiated into: ing marked retinal capillary nonperfusion, cotton
• Central retinal vein occlusion (CRVO), if the wool spots mainly in the acute phase, visual acuity
whole retinal venous retinal system is in- of counting fingers or less, perimetric defects so
volved, and if the presumed site of an in- that only the Goldmann target V4e can be detect-
creased venous outflow resistance is located in ed, a relative afferent pupillary defect of more
the lamina cribrosa and/or posterior to ita than 1.2 logarithmic units, and later, intraocular
(fig. 1) neovascularization. In nonischemic (or perfused)
• Branch retinal vein occlusion (BRVO), if the RVO, there is essentially a relative stasis of retinal
venous engorgement involves only branches venous blood flow and macular edema associated
of the whole retinal venous system; depending with leakage from the altered retinal capillary
on the site where the engorgement starts, one bed.
can further subdivide into BRVOs which orig-
inate in the optic disc and BRVOs which orig-
inate at an arteriovenous crossing (fig. 2) Epidemiology
Based on the seminal works by Hayreh, the de-
gree of ischemia has been used to further classify RVOs are one of the most common causes of a
the RVOs into ischemic and nonischemic types retinal vascular abnormality and a frequent cause
(Hayreh, 1964; Hayreh, 1965; Coscas et al., of visual loss. Being recognized at least as early as
a
If the superior or the inferior hemisphere of the fundus is involved, the presumed site of the occlusion is one of the two trunks
of the intraneural central retinal vein where this congenital abnormality exists. This entity (hemicentral RVO) is considered a vari-
ant of CRVO.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
140 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
1855 (Liebreich, 1855)10, RVOs have been the overlapping confidence intervals suggested that
subject of more than 3,000 publications so far. ethnic differences were not statistically signifi-
Current estimates of the prevalence of RVOs are cant. In the Multiethnic Study of Atherosclerosis
derived from major population-based studies, (Cheung et al., 2008)16, the only study with four
such as the Blue Mountains Eye Study, the Beaver ethnic groups examined in one investigation, the
Dam Eye Study, and a combined analysis of the crude prevalence of any RVO was similar across
Atherosclerosis Risk in Communities and Car- whites, blacks, Chinese, and Hispanics.
diovascular Health Studies (Klein et al., 2000; It is worth noting that in the Multiethnic Study
Mitchell et al., 1996; Wong et al., 2005)11–13. of Atherosclerosis, sample sizes of each ethnic
More recent data have been published from group were relatively small, particularly the Chi-
other ethnic groups: the Beijing Eye Study (Liu et nese subgroup (n = 724), and that all participants
al., 2007; Zhou et al., 2013)14, 15, the Multiethnic were United States residents who were free from
Study of Atherosclerosis (Cheung et al., 2008)16, clinical cardiovascular disease (i.e., generally
the Singapore Malay Eye Study (Lim et al., 2008)17, healthier study participants). Therefore, the Mul-
and the Central India Eye and Medical Study (Jo- tiethnic Study of Atherosclerosis might not be
nas et al., 2013)18. The reported prevalence of sufficiently powered to detect meaningful ethnic
RVOs varied widely across these studies, ranging difference in RVO prevalence, and should not be
from 0.3% (Mitchell et al., 1996)12 to 1.6%. The expected to represent different ethnic groups out-
variability between the prevalence rates among side the US. Other studies of multiple ethnic sam-
the various studies is likely related to the relative- ples as a single study also did not have sufficient
ly small number of RVO patients in any single numbers of RVO cases to examine ethnic differ-
study, differences in the study methodologies ences by RVO subtypes. The higher prevalence of
(e.g., retinal photography), and possible ethnic BRVO in some ethnic groups may reflect different
differences in the distribution of RVO risk fac- population distributions of RVO risk factors. For
tors. As a result of these limitations, estimations example, the prevalence of arterial hypertension
of RVO prevalence are relatively imprecise. and uncontrolled hypertension has been reported
Furthermore, most single studies rarely report to be higher in Asians (Leenen et al., 2008)25 and
on the prevalence of different RVO subtypes, Hispanics (Read et al., 2007)26 than in whites
namely CRVO and BRVO, which are important (Giles et al., 2007; Ostchega et al., 2008)27, 28.
to distinguish as they differ in their risk factors Summarizing all available data on the preva-
(Hayreh et al., 2001; O’Mahoney et al., 2008)19, 20, lence rates of RVOs worldwide, one may estimate
prognosis, and treatment (Hayreh, 2005; McIn- that 14–19 million adults are affected by the dis-
tosh et al., 2006; Mohamed et al., 2006)21–23. ease worldwide. The prevalence of both BRVO
A recent multicenter study pooled individual and CRVO increases significantly with age, but
level data of more than 70,000 adults in 15 studies does not differ by gender. Possible ethnic differ-
around the world (Rogers et al., 2009)24. The ences in the prevalence of RVO may reflect differ-
prevalence rates per 1,000 persons were 4.42 for ences in the prevalence of vascular risk factors,
BRVO and 0.80 for CRVO, with these prevalence particularly arterial hypertension; ethnic-related
rates being age- and gender-standardized to the differences in the prevalence of glaucomatous op-
2008 world population aged 30 years and older. tic neuropathy as the major ocular risk factor; or
The prevalence of RVOs was similar between other unknown factors. Although population-
men and women, and increased with age. Overall, based investigations revealed a significantly high-
the prevalence of BRVO was highest in Asians er prevalence of BRVOs than of CRVOs, CRVOs
and Hispanics and lowest in whites, although the cause considerably more visual burden. Differ-
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 141
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
ences between the results of population-based patients only), and thyroid disorder compared
studies and the findings obtained in hospital- with the US white control population.
based investigations may be due to the fact that A variety of systemic disorders may be present
population-based studies count any RVO includ- in association with different types of RVO and in
ing those RVOs located outside of the fovea and different age groups, and their relative prevalence
without drop in visual acuity, while patients with differs significantly, so that the common practice
extrafoveal RVOs usually do not go to a hospital of generalizing about these disorders for an entire
and are thus not included in the hospital-based group of patients with RVO can be misleading.
investigations. Apart from a routine medical evaluation, an ex-
tensive and expensive workup for systemic dis-
Factors Associated with RVOs eases seems unwarranted in the vast majority of
In probably the largest study on associations be- patients with RVO (Hayreh et al., 2001)19.
tween RVOs and other factors, Hayreh et al. In a second study, the same authors investi-
(2001)19 prospectively investigated 1,090 consec- gated hematological abnormalities associated
utive patients with RVOs, almost all of whom with the various types of RVO (Hayreh et al.,
were Caucasians. They found that there was a sig- 2002)29. A variety of hematological abnormalities
nificantly higher prevalence of arterial hyperten- may be seen in association with different types of
sion in BRVO compared with CRVO and hemi- RVOs, but the routine inexpensive hematological
central RVO. BRVO also had a significantly high- evaluation may usually be sufficient for RVO pa-
er prevalence of peripheral vascular disease, tients. Based on their findings in the study and on
venous disease, peptic ulcer, and other gastroin- a literature review, Hayreh and colleagues addi-
testinal disease compared with CRVO. tionally suggested that treatment with anticoagu-
The proportion of patients with BRVO with lants or platelet antiaggregating agents may ad-
cerebrovascular disease was also significantly versely influence the visual outcome, without any
greater than that of the combined group of pa- evidence of a protective or beneficial effect. Simi-
tients with CRVO and patients with hemicentral lar findings were reported from other hospital-
RVO. There was no significant difference in the based studies (The Eye Disease Case-Control
prevalence of any systemic disease between Study Group, 1993)30, which underlined that
CRVO and hemicentral RVO. A significantly CRVO patients display a cardiovascular risk pro-
greater prevalence of arterial hypertension and file. A decreased risk was observed with increas-
diabetes mellitus was present in the ischemic ing levels of physical activity, increasing levels of
CRVO group compared with the nonischemic alcohol consumption, and in women using post-
CRVO group. Similarly, arterial hypertension menopausal estrogens.
and ischemic heart disease were more prevalent Evidence gathered in population-based stud-
in major BRVO than in macular BRVO. ies on associations between RVO and ocular and
Relative to the US white control population, systemic factors confirms that RVOs are signifi-
the combined group of patients with CRVO and cantly associated with glaucomatous optic neu-
patients with hemicentral RVO had a higher ropathy and arterial hypertension, as shown in
prevalence of arterial hypertension, peptic ulcer, the Blue Mountains Eye Study, the Beaver Dam
diabetes mellitus (in the ischemic type only), and Eye Study, and the Beijing Eye Study, to name
thyroid disorder. The patients with BRVO showed only a few (Klein et al., 2000; Mitchell et al., 1996;
a greater prevalence of arterial hypertension, Liu et al., 2007)11, 12, 14. Corresponding with the
cerebrovascular disease, chronic obstructive pul- association with arterial hypertension, the studies
monary disease, peptic ulcer, diabetes (in young also suggested increased mortality for patients
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
142 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
with RVOs and an age of less than 70 years (Cu- evated arterial pressure during arousal from
gati et al., 2007; Xu et al., 2007)31, 32. sleep, oxidative stress, and a hypercoagulable
Familial clustering of RVOs has been ob- state. The prevalence of OSAS is particularly
served, yet the role of gene mutation in RVO re- high in obese patients. The authors concluded
mains uncertain (Girmens et al., 2008)33. It has that OSAS is largely underdiagnosed and that it
remained unclear whether RVOs are associated may account for the occurrence RVOs in many
with abnormalities of the blood clotting system, patients, particularly since RVOs may develop
such as factor V Leiden, factor XII deficiency, predominantly during sleeping. In clinical prac-
glucose-6-phosphate dehydrogenase deficiency, tice, it appears to be important to take into ac-
decreased plasma homocysteine level, presence count the strong potential association between
of antiphospholipid antibodies, or intake of war- OSAS and RVOs since the treatment of OSAS
farin and aspirin (The Central Vein Occlusion has been demonstrated to reduce the risk of car-
Study Group, 1997; Glacet-Bernard et al., 1994; diovascular and cerebrovascular disorders.
Arsène et al., 2005; Kuhli et al., 2002; Kuhli et al., Interestingly, the amount of macular edema in
2004; Pinna et al., 2007)34–39. In a recent pilot patients with RVOs shows diurnal changes.
project, higher estimated cerebrospinal fluid Paques et al. (2005)46 and Gupta et al. (2009)47
pressure was associated with a higher incidence examined patients with macular edema due to
of RVOs originating at the optic nerve head (i.e., CRVO and observed a significantly thicker macu-
CRVOs, hemicentral RVOs, and BRVOs origi- lar edema at 7:00 am than at 7:00 pm, parallel to
nating at the optic nerve head) in a 10-year fol- changes in visual acuity. In a parallel manner, the
low-up examination of the Beijing Eye Study (Jo- choroid is slightly thicker in the morning than in
nas et al., 2015)40. From a pathogenic point of the afternoon (Usui et al., 2012; Tan et al., 2012)48,
49
view, this association may explain the associa- . Since both the central retinal vein and the vor-
tion between the incidence of RVOs and arterial tex veins with the choroidal blood drain via the
hypertension since arterial blood pressure is cor- superior orbital vein into the brain, the findings
related with cerebrospinal fluid pressure (Ber- of diurnal changes in macular edema in patients
dahl et al., 2012; Ren et al., 2013)41, 42. The asso- with RVO and in choroidal thickness point to a
ciation may also fit with the observation that potential role the cerebrospinal fluid pressure
RVOs are usually noticed by the patients in the may play for RVOs and potentially other condi-
morning after sleeping. During sleeping, cere- tions: due to hydrostatic reasons, the cerebrospi-
brospinal fluid pressure is increased due to hy- nal fluid pressure is higher at night and in the ear-
drostatic reasons. The association also agrees ly morning than during daytime (Jonas et al.,
with the finding that wider retinal vein diameters 2016)50. Correspondingly, also for choroidal
are associated with higher estimated cerebrospi- thickness, a positive association with estimated
nal fluid pressure (Jonas et al., 2014)43. Interest- cerebrospinal fluid pressure has been found (Jo-
ingly, obstructive sleep apnea syndrome (OSAS) nas et al., 2014)51. Interestingly, chronic RVOs
has recently been shown to be associated with were not significantly associated with choroidal
RVOs and also to be an independent risk factor thickness (Du et al., 2013)52, while a study by
of RVO (Glacet-Bernard et al. 2010; Chou et al., Tsuiki et al. (Tsuiki et al., 2013)53 on patients with
2012)44, 45. The local and systemic effects of unilateral CRVO revealed an abnormally thick
OSAS could contribute to the development of subfoveal choroid. Tsuiki et al. additionally de-
RVOs: nocturnal hypoxemia and hypercapnia, tected that after treatment with intravitreal beva-
respiratory efforts, increased intrathoracic, in- cizumab, subfoveal choroidal thickness signifi-
tracranial and cerebral spinal fluid pressure, el- cantly decreased to normal values. Central cor-
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 143
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
neal thickness was not related with the prevalence cularization were low visual acuity and a high
of RVOs (Xu et al., 2010)54, nor was the size of the amount of nonperfusion seen by fluorescein an-
optic nerve head (Xu et al., 2012)55. giography (FA). Of eyes initially categorized as
nonperfused or indeterminate, 35% (61/176) de-
veloped iris or angle neovascularization, com-
Clinical Course pared with 10% (56/538) of eyes initially catego-
rized as perfused. Other risk factors were venous
The natural history and prognosis of RVOs have tortuosity, extensive retinal hemorrhage, and
been examined in only a few prospective studies duration of less than 1 month. Neovascular glau-
(Koizumi et al., 2007)56. The natural history of coma that was unsuccessfully managed with
CRVO has been assessed in the Central Retinal medical treatment developed in only 10 eyes. No
Vein Occlusion Study (The Central Vein Occlu- eye was enucleated. Thus, visual acuity at base-
sion Study Group, 1997)32, a prospective cohort line is a strong predictor of visual acuity at 3
study with randomized clinical trials of specific years for eyes with good baseline vision and eyes
subgroups of patients. It included 725 patients with poor baseline vision, but a poor predictor
with CRVO who were observed for a 3-year fol- for intermediate acuities. Visual acuity is also a
low-up every 4 months. Visual acuity outcome strong predictor for the development of iris and
was largely dependent on initial acuity: angle neovascularization, as is nonperfusion.
• Sixty-five percent of patients with initially During the course of follow-up, one third of the
good visual acuity (20/40 or better) main- eyes with perfusion became ischemic. Some sys-
tained visual acuity in the same range at the temic factors have also been demonstrated to be
end of the study. associated with retinal ischemia, such as an ele-
• Patients with intermediate initial acuity (20/50 vated hematocrit level, elevated fibrinogen, old-
to 20/200) showed a variable outcome: 19% er age, and male gender (Glacet-Bernard et al.,
improved to better than 20/50, 44% stayed in 1996)57. Some patients may present with pro-
the intermediate group, and 37% had final vi- nounced perivenular whitening and abrupt vi-
sual acuity worse than 20/200. sual loss. While the fundus shows minimal signs
• Patients who had poor visual acuity at the of venous obstruction, careful examination can
first visit (<20/200) had an 80% chance of reveal areas of retinal opacification in a perive-
having a visual acuity less than 20/200 at the nous pattern (fig. 3). These patients usually re-
final visit, whether perfused or nonperfused cover, even in cases with severe visual loss at pre-
initially. sentation, often with residual microscotomas
In the first 4 months of follow-up, 81 (15%) (Browning, 2002; Paques et al., 2003)58, 59. In
of the 547 eyes with good perfusion developed these patients the prognostic value of visual acu-
ischemia. During the next 32 months of follow- ity at the initial examination may be question-
up, an additional 19% of eyes were found to have able. Another important aspect is duration of the
developed ischemia, yielding a total of 34% after disease. In some reports on the natural course,
3 years. The development of nonperfusion or 26% of patients had transient macular edema
ischemia was most rapid in the first 4 months with spontaneous resolution (Gutman, 1977)60.
and progressed continuously throughout the en- This finding may explain the relatively good re-
tire duration of follow-up. When iris or angle sults even in the control groups of some studies
neovascularization occurred, it was treated such as GENEVA, BRAVO, and CRUISE, in
promptly with panretinal photocoagulation. which patients with recent-onset macular edema
The strongest predictors of iris or angle neovas- due to RVO were included (Thach et al., 2014;
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
144 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
edema, scattered superficial or deep hemorrhag-
es, cotton wool spots, and venous dilatation. Old
RVOs are characterized by (occluded and)
sheathed retinal veins, venous-venous collaterals,
and intraretinal hard exudates.
The ophthalmoscopic examination allows the
differentiation into CRVO and BRVO, and the
subclassification into BRVO originating in the
optic nerve head and BRVO originating at arte-
riovenous crossings or limited to macular ve-
nules (fig. 1, 2). In addition, the differentiation
into ischemic RVOs (with large deep hemor-
rhage) and nonischemic RVOs (with mainly
flame hemorrhage) is of high clinical impor-
Fig. 3. Blue reflectance photograph of a patient with
CRVO and perivenular whitening. tance, particularly with respect to the prognosis
of the disease.
Slit lamp biomicroscopy of the anterior seg-
Campochiaro et al., 2010; Haller et al., 2010; ment is mandatory for all patients with RVOs to
Haller et al., 2011)61–64. In contrast, chronic detect iris neovascularization as early as possible.
macular edema is associated with poor visual A vascular congestion of iris vessels may be con-
prognosis and needs to be treated. sidered as an early evidence of the presence of va-
sodilator factors released from the retina that pre-
cede in many patients the actual onset of iris neo-
Diagnosis: Imaging and Functional Testing, vascularization (Hayreh et al., 2005; Paques et al.,
Stages, and Classifications 2004)21, 66.
Clinical Signs Fluorescein Angiography
Patients with an RVO usually notice a painless Besides the recently developed OCT-based angi-
loss in vision, which may affect parts of the whole ography FA is the only examination which direct-
visual field, depending on whether it is a BRVO or ly visualizes not only large retinal vessels but also
CRVO. If the drop in vision is experienced shortly the retinal macular capillary bed (Casselholmde
after its development, the majority of the patients Salles et al., 2016; Coscas et al., 2016; Abri Agh-
report they noticed the visual impairment in the dam et al., 2016; Kashani et al., 2015; Suzuki et al.,
morning (Hayreh et al., 1980)65. This may imply 2016)67–71. FA both confirms the slow-down of
that the RVO occurred at night during sleep. retinal blood circulation and evaluates the effects
Increasing pain is rarely the first symptom no- of the vein obstruction on the capillary bed. FA is
ticed by the patient. It can occur if a previously therefore the ‘clue tool’ for the diagnosis and
unnoticed ischemic RVO led to the development prognosis of RVO, permitting the differentiation
of iris neovascularization and neovascular glau- between the nonischemic type and the ischemic
coma. form (Hayreh, 1965; Coscas et al., 1978; Hayreh et
The ophthalmologic diagnosis of RVO is made al., 1990; Glacet-Bernard et al., 1996; Laatikainen
primarily by conventional ophthalmoscopy. et al., 1976)1, 3, 8, 57, 72. FA is essential in diagnosing
Recent RVOs are characterized by the pres- RVO and before choosing the therapeutic option
ence of retinal edema, optic disk hyperemia or (fig. 4).
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 145
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
a b
c d
Fig. 4. Nonischemic CRVO with persistent macular edema (courtesy of Agnes Glacet-Bernard).
a Color photography: well-perfused CRVO with flame-shaped hemorrhages. b FA displaying the
slowdown of retinal blood circulation and dilation of the capillary bed, visible in the macular area.
c On the late frame, fluorescein leakage is collected in pseudocystic cavities. d Peripheral retinal
quadrants remained well-perfused. e SD-OCT: macular thickness was increased to 755 μm.
The confirmation of the RVO diagnosis is than 2–3 s is regarded as ‘normal’ and a longer
mainly related to the increase in the length of the time (more than 5 s) is considered ‘delayed’. Nev-
retinal transit time, defined as the time between ertheless, the quantification of retinal transit time
the first fluorescein appearance in the main reti- by FA is not significantly accurate because it de-
nal arteries and its appearance as a laminar flow pends on the rapidity of the antecubital intrave-
in the main posterior veins. A transit time of less nous injection and on the frequency of the frames.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
146 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
a b
Fig. 5. Nonischemic CRVO with persistent macular edema (courtesy of Agnes Glacet-Bernard). a One
year after the onset, fundus aspect returned grossly to normal. b FA showing persistent dilation of
the capillary bed in the macular area. c SD-OCT (Spectralis): central macular thickness was 601 μm.
d SD-OCT (Cirrus): 1 month after bevacizumab injection, macular edema completely disappeared.
However, video angiography using a scanning Dilatation of retinal veins and capillaries, observed
laser ophthalmoscope showed an improvement in on the early frames of FA, is generally seen in all
the evaluation and the measurement of retinal cir- forms of RVO, with late leakage in the macular area
culation times, which is particularly important for and late staining at the level of the wall of the main
the diagnosis of combined retinal occlusion, such posterior veins. Hyperpermeability can be more
as RVO associated with cilioretinal artery occlu- marked showing early and intense leakage from the
sion or combined retinal artery and vein occlusion. macular capillary bed and collection of the dye on
FA also permits the localization and the qualita- the late frames of FA in radially orientated pseudo-
tive evaluation of retinal capillary bed changes that cystic cavities forming the typical cystoid macular
includes hyperpermeability and/or nonperfusion. edema with a ‘petaloid pattern’ (fig. 4, 5).
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 147
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
a b
Fig. 6. Ischemic CRVO (courtesy of Agnes Glacet-Bernard). a Color photography of a CRVO with
numerous cotton wool spots and deep hemorrhages. b FA displaying the slowdown of retinal
blood circulation and widespread capillary nonperfusion. c OCT: macular thickness was dramati-
cally increased up to more than 1,000 μm; a foveal detachment is visible. d Final OCT (16 months
after the onset of the CRVO and after panretinal photocoagulation): macular atrophy. The photo-
receptor layer is no longer visible. Central retinal thickness was 139 μm.
Capillary nonperfusion is most analyzable on leakage at the level of the wall of the vessels cross-
the early frames of FA, at the arteriovenous time, ing over the ischemic area (Coscas et al., 1978)3.
before leakage. Macular nonperfusion is correlat- When retinal hemorrhages are numerous and
ed with a bad visual prognosis and its diagnosis deep, it can be impossible to assess the integrity of
must be done in the pretherapeutic evaluation of the retinal capillary bed. Extensive hemorrhagic
a macular edema. Peripheral nonperfusion char- RVO usually corresponds to ischemic RVO. The
acterizes the ischemic forms, which are prone to diagnosis of ischemic RVO is confirmed by clini-
ocular neovascularization (fig. 6). Sudden inter- cal data such as severe and sudden loss in visual
ruption of the blood flow can be observed giving acuity, the presence of absolute central scotomas,
the aspect of a dead tree, with late staining and/or and the iris and angle aspect.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
148 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
SCP
DCP SCP DCP
a b c d
Fig. 7. BRVO with cystoid macular edema: comprehensive assessment on OCT angiography (top images: C-Scan – bot-
tom images: B-Scan), including multiple, large, cystoid spaces, deeply ‘black’, without any signal in the superior tem-
poral quadrant (a, b) and the regression of the cysts after 3 anti-VEGF injections, leaving the area as nonperfused and
no change in the retinal capillaries: disorganization with dilation and disruption (c, d).
FA is a relatively easy method to recognize the of the posterior layer corresponding to atrophy or
diverse types of RVO, both perfused and nonper- fibrosis of the retinal pigment epithelium, subret-
fused (and mixed types), as well as to detect the inal accumulation of material (fibrosis), lamellar
different modalities in natural history [regression macular hole, intraretinal lipid exudates, and in-
of the macular edema or progression to ischemic traretinal hemorrhage (fig. 4–6).
type (acutely or slowly)]. Recent studies have suggested that in BRVOs,
FA is an effective method to determine the visual function and recovery of vision is correlat-
presence (or absence) of macular cystoid edema, ed with thickness of the central macula, and that
its extension, persistence, or regression. More- is correlated with the integrity of the inner and
over, in BRVO, FA examination makes it easy to outer segments of the photoreceptors in the fovea
differentiate the cases threatening the macula and (Ota et al., 2008)74.
evaluate the extension of nonperfused capillary Spectral domain OCT (SD-OCT) helps to
bed areas. quantify the amount of cystoid macular edema
and supplies additional information, such as
Optical Coherence Tomography whether the accumulated fluid is located most-
Optical coherence tomography (OCT) examina- ly within the retinal layers or additionally in
tion is widely used to detect changes in the retinal the subretinal space (Shroff et al., 2008)75.
architecture of eyes affected by various macular Thanks to a better definition of the scans, SD-
diseases and to quantitatively measure retinal OCT can display the presence and integrity of
thickness (Catier et al., 2005)73. the outer limiting membrane and of the inner
In RVO, OCT can display intraretinal cystoid and outer segments of the photoreceptors,
spaces responsible for the increase in retinal which provides useful information for progno-
thickness often associated with serous detach- sis (fig. 4–6).
ment of the neurosensory retina. The retinal cys-
toid spaces can be numerous and confluent, OCT-Based Angiography
forming a large central cystoid space. Associated OCT-based angiography, which has recently
findings can be observed such as vitreous macular been introduced into clinical practice, is a very
adherence, epiretinal membrane, hyperreflexivity promising technique to visualize the vascular
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 149
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
a b c
Fig. 8. RVO with cystoid macular edema: comprehensive assessment on OCT angiography, including a C-scan section
taken at the level of the ganglion cell layer (superficial capillary plexus) (a), another one taken at the inner nuclear
layer (deep capillary plexus) (b), and the corresponding B-scan passing through the foveal depression (c). The cystoid
spaces are deeply ‘black’, without any signal. Note the capillary network disorganization with scarcity, dilation, and
disruption. Slides obtained with manual segmentation.
system of the retina and choriocapillaris in differ- mentation, and no risk of an allergy. OCT angi-
ent layers in a noninvasive manner (Wei et al., ography also allows the distinction between the
2013; Wang et al., 2014; Jia et al., 2014; Jia et al., superficial capillary plexus and deep capillary
2015; Yu et al. 2015; Pechauer et al., 2015; Glacet- plexus. OCT angiography may soon be automat-
Bernard et al., 2016; Sellam et al., 2016)76–83. Its ically quantified for a specific analysis of follow-
disadvantage as compared to FA is that OCT an- up (fig. 7, 8).
giography does not show leakage and pooling of OCT angiography is a fast noninvasive exam
fluid, so that a conventional SD-OCT is neces- that allows the imaging of both plexuses in vein
sary to detect macular swelling and edema. The retinal occlusion. The deep capillary plexus is pre-
advantages of OCT angiography are that it is not dominantly affected. Recent studies have demon-
invasive and that it allows the visualization of the strated correlations between vascular densities,
different vascular systems of the retina, optic superficial foveal avascular zone, visual acuity,
nerve head, and choriocapillaris separately in the and FA peripheral ischemia.
different layers of the retina and optic nerve head. The follow-up of macular edema and hypo-
There is also a need to enlarge the field of exami- perfusion and also of peripheral ischemia will be-
nation so that the whole macular region and the come more efficient with OCT angiography,
fundus periphery can be explored (as it is actu- which is undergoing continuous development.
ally possible upon FA). Some preliminary inves-
tigations have suggested that OCT angiography Additional Examinations
may in some clinical situations become a substi- Additional diagnostic clues may be obtained by a
tute for FA in the clinical assessment of macular modified type of ophthalmodynamometry
edema in RVOs. OCT angiography allows the (Hitchings et al., 1976; Jonas, 2003; Jonas, 2003;
specific analysis of both macular edema and the Jonas, 2003; Jonas, 2004)84–88. The Goldmann
macular capillary bed architecture with more contact lens-associated ophthalmodynamomet-
contrast (as compared to FA), more specific seg- ric device provides a direct visualization of the
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
150 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
optic disk when manually asserting pressure of anterior chamber angle neovascularization,
onto the globe, and it allows an assessment of the neovascular glaucoma, retinal and/or optic disk
blood pressure in the central retinal artery and neovascularization, vitreous hemorrhage, or vi-
central retinal vein (Harder et al., 2007; Jonas et sual acuity. The study revealed, however, a statis-
al., 2007)89, 90. In particular, ophthalmodyna- tically significant difference in the incidence of
mometry is helpful in the differentiation between iris neovascularization between the two groups.
the ischemic type of CRVO versus the nonisch- Consequently, the Central Retinal Vein Occlu-
emic type. The central retinal vein pressure was sion Study was conducted in the year 1997 (The
usually higher than the diastolic arterial blood Central Vein Occlusion Study Group, 1997)34.
pressure in eyes with ischemic CRVO, and it was According to the results of the study, attention to
usually lower than the diastolic arterial blood visual acuity is a crucial element of the initial ex-
pressure in eyes with a nonischemic CRVO (Jo- amination because it is an important indicator of
nas et al., 2007)90. Future studies may examine final visual prognosis and neovascularization
whether an increased central retinal vein pres- risk. A visual acuity worse than 20/200 is highly
sure in asymptomatic eyes may indicate an in- correlated with the presence and development of
creased risk for the eventual development of retinal ischemia and neovascularization. The
RVOs. study suggested that at the patient’s initial visit it
would be important to perform a careful slit
lamp examination and gonioscopy to evaluate
Management any iris or anterior chamber angle neovascular-
ization. If true neovascularization is already
Treatment of Associated Conditions present, a panretinal laser photocoagulation
Since the population-based studies mentioned should be considered. (In the rare clinical situa-
above and multicenter prospective studies such as tion of simultaneous bilateral CRVOs, the pos-
the Central Retinal Vein Occlusion Study have sibility of hyperviscosity should be considered
shown associations between RVOs, glaucoma, and diagnostically excluded.) A follow-up sched-
and arterial hypertension (Klein et al., 2000; ule should be established depending on the dura-
Mitchell et al., 1996; Wong et al., 2005)11–13, glau- tion and severity of the occlusion and the pa-
coma and arterial hypertension should be exclud- tient’s circumstances.
ed in patients with RVOs. It has remained unclear • Patients with initial visual acuity less than
so far whether lowering of the intraocular pres- 20/200 may be examined every month for the
sure in glaucoma patients or a better control of initial 6 months.
blood pressure in patients with arterial hyperten- • Prognosis is mixed for patients with visual
sion is beneficial for the final visual outcome after acuity between 20/50 and 20/200; either
RVOs. monthly or bimonthly follow-ups may be in-
stituted initially (and possibly revised) de-
Laser Photocoagulation pending on exactly where on the scale the pa-
Central Retinal Vein Occlusion tient’s visual acuity falls, whether the CRVO is
In 1990, a prospective study of argon laser pan- progressing or improving, and other factors.
retinal photocoagulation performed over a 10- • If visual acuity decreases at any time during fol-
year period in 123 eyes with ischemic CRVO was low-up to less than 20/200, it is likely that exten-
reported (Hayreh et al., 1990)91. Eyes treated by sive nonperfusion has developed in the eye.
laser coagulation as compared with untreated • If visual acuity is 20/40 or better, the patient
eyes did not differ significantly in the incidence may be asked to return every 1–2 months for 6
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 151
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
months, with precise examination of the mac- Branch Vein Occlusion Study Group, 1986)92, 93.
ular area using FA and OCT. With respect to the question whether grid argon
A decrease in visual acuity may also be fre- laser photocoagulation was useful in improving
quently associated with macular edema, persis- visual acuity in eyes with BRVO and macular ede-
tent or recurrent, easily recognized with the help ma and vision reduced to 20/40 or worse, the
of FA and quantified in OCT examinations, dur- study included 139 eyes, which were randomly
ing follow-up. In 1995, The Central Retinal Vein assigned to either a treated group or an untreated
Occlusion Study evaluated the efficacy of grid la- control group with a mean follow-up of 3.1 years
ser treatment on macular edema compared to a for all study eyes. The gain in visual acuity from
control group (The Central Retinal Vein Occlu- baseline maintained for 2 consecutive visits was
sion Study Group, 1995)6. Grid laser treatment significantly greater in the treated eyes (at least 2
clearly reduced the angiographic evidence of Snellen lines). Grid laser photocoagulation was,
macular edema compared to controls but visual therefore, recommended for patients with macu-
acuity was not statistically improved in the treat- lar edema associated with BRVO who met the el-
ed group: after a 3-year follow-up, visual acuity igibility criteria of this study (visual acuity of
improved spontaneously in 24% of the control 20/40 or less, persistent macular edema lasting for
group versus 27% after grid laser treatment. Nev- 4 months or longer, resorption of macular hem-
ertheless, grid laser treatment could be offered to orrhages).
young patients, even if no positive result but only In 1993, another prospective study was report-
a trend is shown in patients less than 60 years of ed on 271 eyes with major BRVO and ischemic
age. hemicentral RVO, which either underwent scat-
In conclusion, the first essential step in the ter argon laser photocoagulation to the involved
management of CRVO is to determine the type of sector (n = 61 eyes) or remained untreated (n =
CRVO since the prognosis, complications, visual 210 eyes) (Hayreh et al., 1993)94. This study con-
outcome, and management of nonischemic and cluded that argon laser photocoagulation treat-
ischemic CRVO are different. Ocular neovascu- ment should be given only when neovasculariza-
larization is a complication of ischemic RVO tion was seen and not otherwise, because in the
only. (It is important to remember that the con- latter case, the detrimental effects of laser coagu-
ventional prevalent use of a 10-disk area of retinal lation might outweigh its beneficial effects. In the
capillary obliteration is not a valid parameter to assessment of published studies on the effect of
differentiate ischemic from non-ischemic RVO, laser treatment on visual outcome of patients
or to predict ocular neovascularization.) The nat- with RVO, every laser coagulation spot in the
ural history of the disease with the possibility of a macular region led to a scotoma in the pericentral
spontaneous improvement particularly in the visual field.
nonischemic group, with macular edema, should Several other investigations were focused on
not be mistaken for a beneficial effect of treat- the laser treatment of RVO (Arnarsson et al.,
ment in studies without a control group. 2000; Maár et al., 2004; Ohashi et al., 2004; Esrick
et al., 2005; Parodi et al., 2006; Hayreh, 2003)95–
100
Branch Retinal Vein Occlusion . Laser photocoagulation in a ‘grid’ pattern
The Branch Vein Occlusion Study’s multicenter over the area, demonstrated as leaking by FA, re-
randomized controlled clinical trial was designed mains to be one of the ‘reference treatments for
to address questions regarding the management macular edema’ due to BRVO. The Pascal® laser
of complications of branch vein occlusion (The is useful for the comfort and safety of the patient,
Branch Vein Occlusion Study Group, 1984; The as it avoids overdosed or confluent impacts.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
152 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
Ophthalmic: Surgical Treatment the peeling of the inner limiting membrane),
Besides retinal laser coagulation, surgical treat- peeling of the inner limiting membrane may be
ment modalities have been reported for RVOs. reserved for clinical situations in which other mo-
For BRVO originating at arteriovenous crossings, dalities of treatment, namely the intravitreal in-
a sheathotomy has been suggested to liberalize the jection of antiedematous (steroids) or anti-VEGF
retinal venule and the retinal arteriole from their drugs, have failed in achieving a satisfactory im-
surrounding adventitious tissue at the crossing provement in vision, and in which the blood per-
site (Opremcak et al., 1999; Shah et al., 2000; Le fusion of the macula physiologically allows an in-
Rouic et al., 2001; Cahill et al., 2003; Fujii et al., crease in visual acuity.
2003; Mason et al., 2004; Charbonnel et al., 2004; The peeling of the inner limiting membrane of
Yamaji et al., 2004; Yamamoto et al., 2004)101–109. the retina is similar to the vitrectomy technique
Randomized trials with an untreated control applied for diffuse diabetic macular edema asso-
group and a clear differentiation between the ciated with taut membranes (Lewis et al., 1992)129.
ischemic type of BRVO and the nonischemic type The decrease in macular edema observed after
of BRVO have been scarce. It may be question- vitrectomy could be the result of an increase in
able, therefore, whether sheathotomy is a recom- oxygen concentration in the macular area. Other
mended therapy for BRVOs originating at the ar- hypotheses have been suggested to explain the
teriovenous crossing site. In most clinical sites, positive effect of vitrectomy, such as a decom-
this surgical technique was not introduced or has pression from tangential tractions, removal of in-
been abandoned. travitreal proinflammatory and proangiogenic
Radial neurotomy has been suggested as ther- factors, collateral development stimulation, or
apy for CRVO (Opremcak et al., 2001; García- specific Müller cell fibrosis (Mandelcorn et al.,
Arumí et al., 2003; Weizer et al., 2003; Spaide et 2004;Stefánsson, 2009)118, 130.
al., 2004; Arevalo et al., 2008)110–114. However, The positive action of vitrectomy seems dura-
randomized prospective trials have not yet shown ble, which differs from intravitreal injection. The
beneficial effects of radial neurotomy for the combination of surgery and intravitreal injection
treatment of CRVO, so it is unclear whether the of steroids could permit a more rapid and lasting
technique should be recommended (Hayreh, action (Nkeme et al., 2006)120. Another surgical
2002)115. Again, in most clinical sites, this surgical technique consists of vitrectomy combined with
technique was not introduced or has been aban- an injection of tissue plasminogen activator into
doned. the retinal vein (Weiss, 1998; Weiss et al., 2001)131,
132
Another surgical technique which has been . This technique, however, has still not achieved
used for the treatment of RVOs is the peeling of wide distribution and application.
the inner limiting membrane off the macula to re-
duce macular edema (Saika et al., 2001; García- Ophthalmic: Intravitreal Drug
Arumí et al., 2004; Mandelcorn et al., 2004; Ra- Intravitreal Steroids (Triamcinolone,
detzky et al., 2004; Nkeme et al., 2006; Kumagai et Fluocinolone, Dexamethasone)
al., 2007; Kumagai et al., 2007; Berker et al., 2008; Intravitreal triamcinolone acetonide has been
Oh et al., 2008; Arai et al., 2009; DeCroos et al., increasingly used in studies for treatment of vari-
2009; Lu et al., 2009; Uemura et al., 2009)116–128. ous intraocular proliferative, edematous, and
In view of the risk of surgical complications (such neovascular diseases, such as diffuse diabetic
as the development of iatrogenic peripheral reti- macular edema, proliferative diabetic retinopa-
nal defects with secondary retinal detachment or thy, neovascular glaucoma, persistent pseudo-
a iatrogenic damage to the paracentral retina by phakic cystoid macular edema, CRVO (Green-
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 153
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
berg et al., 2002; Jonas et al., 2002, 2005; Park et versus Corticosteroid for Retinal Vein Occlusion
al., 2003)133–136, and in other clinical situations. (SCORE) study’s multicenter clinical trial of 411
Systemic and local side effects reported include participants compared the efficacy and safety of
cataract, secondary ocular hypertension leading 1-mg and 4-mg doses of preservative-free intra-
in some patients to secondary chronic open-angle vitreal triamcinolone with standard care (grid
glaucoma, and postinjection infectious endo- photocoagulation in eyes without dense macular
phthalmitis (Wingate et al., 1999; Bakri et al., hemorrhage and deferral of photocoagulation
2003; Benz et al., 2003; Jonas et al., 2003; Jonas et until hemorrhage clears in eyes with dense macu-
al., 2003; Jonas et al., 2004)137–142. lar hemorrhage) for eyes with vision loss associ-
Due to its antiedematous and antiangiogenic ated with macular edema secondary to BRVO.
effects, as shown in experimental investigations The drug used in this trial was prepared as a ster-
and clinical studies (Ishibashi et al., 1985; Wilson ile, preservative-free, single-use, intravitreal in-
et al., 1992; Antoszyk et al., 1993; Penfold et al., jection (Trivaris®; Allergan Inc., Irvine, Calif.,
2001; Penfold et al., 2002)143–147, intravitreal tri- USA) in 1-mg and 4-mg doses, in a volume of 0.05
amcinolone acetonide has additionally been used ml. The main outcome measure was the gain in
in studies on RVOs (Jonas et al., 2002; Bashshur visual acuity letter score of 15 or more from base-
et al., 2004; Ip et al., 2004; Jonas et al., 2004; Kara- line to month 12. Twenty-nine, 26, and 27% of the
corlu et al., 2004; Karacorlu et al., 2005; Cekiç et participants achieved the primary outcome in the
al., 2005; Cekiç et al., 2005; Jonas et al., 2005; Jo- standard care, 1-mg, and 4-mg groups, respec-
nas et al., 2005; Jonas et al., 2005; Lee et al., 2005; tively. None of the pairwise comparisons between
Chen et al., 2006; Goff et al., 2006; Gregori et al., the 3 groups was statistically significant at month
2006; Jonas, 2006; Ramezani et al., 2006; Bhavsar 12. The rates of elevated intraocular pressure and
et al., 2007; Hirano et al., 2007; Jonas et al., 2007; cataract were similar for the standard care and
Karacorlu et al., 2007; Pathai, 2007; Cakir et al., 1-mg groups, but higher in the 4-mg group. The
2008; Chung et al., 2008; Park et al., 2008; Parodi study group concluded that there was no differ-
et al., 2008; Patel et al., 2008; Riese et al., 2008; ence identified in visual acuity at 12 months for
Roth et al., 2008; Cheng et al., 2009; Gewaily and the standard care group compared with the tri-
Greenberg, 2009; McAllister et al., 2009; Scott et amcinolone groups; however, rates of adverse
al., 2009; Wang et al., 2009; Wu et al., 2009)148–182. events (particularly elevated intraocular pressure
Although randomized trials on the intravitreal and cataract) were highest in the 4-mg group. The
use of triamcinolone in particular and of steroids authors inferred that ‘grid photocoagulation as
in general as treatment of RVO have been missing applied in the SCORE study remained the stan-
until recently, the available literature strongly dard care for patients with vision loss associated
suggests an antiedematous effect of intravitreal with macular edema secondary to BRVO who
triamcinolone and an associated improvement in have characteristics similar to participants in the
vision. Due to the limited duration of the intra- SCORE-BRVO trial. Grid photocoagulation
ocular availability of triamcinolone, the visual should remain the benchmark against which oth-
improvement is limited in its duration. It may de- er treatments are compared in clinical trials for
pend on the dosage of triamcinolone used. eyes with vision loss associated with macular ede-
Prospective double-masked randomized trials ma secondary to BRVO.’ One may, however, also
have been published presenting leading knowl- consider the limitation of the study. Central vi-
edge on the intravitreal use of steroids for treat- sual acuity and the paracentral visual field both
ment of RVOs (Scott et al., 2009; Scott et al., 2009; contribute to the quality of vision. Paracentral la-
Scott et al., 2009)180, 183, 184. The Standard Care ser coagulation in contrast to intravitreal triam-
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
154 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
cinolone leads to paracentral visual field defects. tween the 1-mg and 4-mg groups (p = 0.97). The
Since the paracentral visual field or reading abil- rates of elevated intraocular pressure and cataract
ity was not examined, the conclusions of the were similar for the observation and 1-mg groups,
SCORE-BRVO study may be valid for the out- but higher in the 4-mg group.
come parameter of central visual acuity; however, The study group concluded that intravitreal
it may remain questionable whether the results triamcinolone was superior to observation for
also refer to the quality of vision in general. treating vision loss associated with macular ede-
As mentioned in the natural course section, it ma secondary to CRVO in patients who had char-
is important to consider the duration of the ede- acteristics similar to those in the SCORE-CRVO
ma. In the subgroup analysis in the SCORE-BR- trial. The 1-mg dose had a safety profile superior
VO trial, patients with a duration of less than 3 to that of the 4-mg dose. The authors suggested
months showed a trend to have more benefit with that intravitreal triamcinolone in a 1-mg dose,
usual care. However, among those patients that following the retreatment criteria applied in the
had a macular edema of more than 3 months’ du- SCORE study, should be considered for up to 1
ration, 34% in the 4-mg group showed a gain in year and possibly 2 years for patients with charac-
visual acuity letter score of 15 or more, versus teristics similar to those in the SCORE-CRVO tri-
15% in the photocoagulation group. According to al. The formulation used in this study (Trivaris®)
the authors, these numbers were not significant is not currently available.
but show the importance of the duration of the Dexamethasone has been used for a long time
edema at the time of analyzing the results of the as a potent corticosteroid that decreases inflam-
different trials, which may differ in the baseline matory mediators implicated in macular edema.
characteristics. In the SCORE-BRVO trial, more Due to its anti-edematous and antiangiogenic ef-
than 50% of the patients had a macular edema fects, intravitreal dexamethasone has been used
with a duration of less than 3 months. If approxi- in studies on RVOs. Previous data suggest fewer
mately 25% of patients with BRVO have a tran- side effects than for other corticosteroids. Be-
sient edema as a natural course (Gutman, 1977)60, cause of the short half-life of intravitreal injec-
it is possible that in the SCORE-BRVO study ap- tions of dexamethasone, an intravitreal dexa-
proximately 12% of patients had transient macu- methasone implant (Ozurdex) was developed to
lar edema with spontaneous resolution. deliver sustained levels of dexamethasone to the
With respect to CRVO, the results of the back of the eye in a 6-month randomized con-
SCORE-CRVO study differed from the findings trolled clinical trial on macular edema associated
in the SCORE-BRVO study. In the SCORE- with RVO, the GENEVA study. The objective of
CRVO study (Ip et al., 2009)185, 271 participants the GENEVA study was to evaluate an intravit-
with macular edema secondary to perfused real dexamethasone drug delivery system (Ozur-
CRVO were included. Seven, 27, and 26% of the dex®) in patients with vision loss due to macular
participants achieved the primary outcome (i.e., edema associated with RVO. The study design in-
gain in visual acuity letter score of 15 or more cluded two identical, randomized, prospective,
from baseline to month 12) in the observation, multicenter, masked, sham-controlled, parallel
1-mg, and 4-mg groups, respectively. The odds of groups. Phase III clinical trials were conducted in
achieving the primary outcome were 5.0 times 2 periods of 6 months each. In the double-masked,
greater in the 1-mg group than in the observation initial treatment phase, patients were randomly
group (p = 0.001) and 5.0 times greater in the assigned (1: 1:1) to receive either a 350-μg or a
4-mg group than in the observation group (p = 700-μg dexamethasone implant, or to receive
0.001). There was no difference identified be- sham treatment (needleless applicator). In the
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 155
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
open-label phase (2nd injection), patients re- achieving at least a 15-letter or 10-letter improve-
ceived a 700-μg dexamethasone implant. The pri- ment from baseline BCVA was significantly
mary endpoint was the time to achieve a ≥15-let- greater in the dexamethasone 700-μg group than
ter (3 Snellen lines) improvement in best-correct- in the sham group from day 30 through day 90.
ed visual acuity (BCVA), and key secondary The greatest response was seen at day 60:
endpoints included BCVA over the 6-month trial, • 29% of patients in the dexamethasone 700-μg
central retinal thickness measured by OCT, and group achieved at least a 15-letter improve-
safety. To be eligible for the study, the patients ment from baseline as compared with 11% in
had to be >18 years of age, have a >34- and <68-let- the sham group
ter improvement in BCVA (20/200 to 20/50), and • 51% of patients in the dexamethasone 700-μg
a macular edema with the following characteris- group achieved at least a 10-letter improve-
tics: (1) involvement of the fovea, (2) due to either ment from baseline as compared with 26% in
BRVO or CRVO, (3) duration of macular edema the sham group
of 6 weeks to 12 months for BRVO, (4) duration • Statistical differences between the dexametha-
of macular edema of 6 weeks to 9 months for sone groups and the sham group were no lon-
CRVO, (5) visual acuity decrease due to edema, ger seen at day 180 in an analysis of all patients
and (6) retinal thickness of ≥300 μm in the central The difference in mean change in BCVA from
1-mm macula subfield. The percentage of pa- baseline between the dexamethasone 700-μg
tients with BRVO or CRVO was similar in the 3 group and the sham group was statistically sig-
groups with about two thirds of BRVO patients nificant: (1) at all time points for all patients, (2)
(68.1% of BRVO patients for the dexamethasone at all time points for BRVO patients, and (3) at
700-μg group) and one third of CRVO patients in days 30, 60, and 90 for CRVO patients. The main
each group (39.1% of CRVO patients for the difference between the BRVO and CRVO sub-
dexamethasone 700-μg group). The duration of groups was in the sham treatment group. Among
macular edema was similar in each group with patients with BRVO in the sham group, mean
about 15% of the patients having a macular ede- BCVA slowly improved over the course of the
ma of <3 months’ duration, 50% with a macular study. In contrast, mean BCVA slowly declined to
edema duration between 3 and 6 months, and below baseline levels among CRVO patients in
30% with a macular edema duration >6 months the sham group.
(16.4% of the patients <3 months, 51.3% between Mean change from baseline in BCVA was sim-
3 and 6 months, and 32.3% >6 months). Only ilar following a second treatment with dexameth-
1.2% of patients in the dexamethasone 700-μg asone 700 or 350 μg. Patients who had received
group and 1% of patient in the dexamethasone sham treatment in the initial treatment phase
350-μg group discontinued because of an ocular demonstrated a lower mean change from baseline
adverse event. It is noteworthy that only 15% of in BCVA after receiving open-label treatment
the patients had macular edema of less than 3 than patients who had received dexamethasone
months’ duration in comparison to more than 700 or 350 μg during the initial treatment phase.
50% in the SCORE-BRVO trial, 51.5–53.8% in the The percentage of patients in the dexametha-
BRAVO trial, and 51.5–61.5% in the CRUISE tri- sone groups reaching an intraocular pressure of
al. This might affect the results and create difficul- ≥35 mm Hg (about 2–3% of the patients at day
ties when comparing trials, since spontaneous 60), ≥25 mm Hg (about 15% of the patients at day
resolution is higher among those trials in which a 60), and ≥10 mm Hg (about 15% of the patients
large number of patients have a short duration of at day 60) peaked at day 60 and returned to base-
the macular edema. The proportion of patients line by day 180. After 12 months (2 injections of
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
156 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
dexamethasone), only 1.2% of the patients (n = 4) Ranibizumab, Pegaptanib. Related to bevaci-
had an intraocular pressure procedure and 0.9% zumab, the effect of ranibizumab and pegaptanib
of patients (n = 3) a cataract surgery (for the on macular edema in eyes with RVOs has been re-
700-μg/700-μg group, patients injected twice). ported in several studies (Campochiaro et al.,
Adverse events in the initial treatment whose 2008; Pieramici et al., 2008; Spaide et al., 2009;
maximum severity increased during the open-la- Wroblewski et al., 2009)195–198. These studies all
bel extension were reported for 2.6% of the pa- reported on a reduction in macular edema after
tients (700-μg/700-μg group). the intravitreal injection of the anti-VEGF drugs.
In summary, two identical, randomized, pro- The first multicenter, randomized study on the ef-
spective, multicenter, masked, sham-controlled, fect of anti-VEGF therapy in the treatment of RVO
parallel-group, phase III clinical trials showed a was designed to evaluate the efficacy of pegaptanib
statistically significant effect and a rapid action, sodium. The results have been reported at the
with a maximum effect at day 60 and a decrease Congress of the European Vitreo-Retinal Society
of the effect beginning at day 90 but still persistent in 2006. Patients with visual loss due to macular
at day 180. The 2nd injection is effective, with an edema secondary to CRVO were randomly as-
even slightly better effect than after the 1st injec- signed to sham injection, 0.3, or 1 mg of pegap-
tion. No adverse events were related to the injec- tanib sodium. The group treated with 1 mg of
tion, with a low cataract rate and low rates of per- pegaptanib sodium showed a higher rate of visual
sistent intraocular pressure increases. These re- gain superior to 5 letters and a lower rate of loss of
sults suggest that this slow-release device for the 15 letters or more than the control group (p < 0.05
intraocular dexamethasone delivery could be and p < 0.01, respectively). There was a difference
considered as a first-choice therapy in both BRVO of 13 letters in the change in visual acuity between
and CRVO retinal diseases. the control group (sham injections) and the group
treated with 1 mg of pegaptanib sodium.
Intravitreal Anti-VEGF Drugs Several retrospective and prospective case se-
On the basis of the published results of prospec- ries illustrated that intravitreal bevacizumab re-
tive randomized controlled trials, intravitreal an- sulted in improvement in visual acuity, concomi-
ti-VEGF drugs have been developed as front-line tant with a reduction in central macular thickness
therapy for the treatment of ME associated with (Epstein et al., 2012; Epstein et al., 2012; Zhang et
CRVOs42 and BRVOs (Campochiaro et al., 2010; al., 2011; Kriechbaum et al., 2008; Prager et al.,
Ho et al., 2016)62, 186. 2009; Ding et al., 2011)199–204. Epstein and col-
Bevacizumab. Since the landmark study on the leagues reported in a prospective controlled clini-
intravitreal use of bevacizumab for treatment of cal trial the beneficial effect of intravitreal bevaci-
exudative age-related macular degeneration zumab for the treatment of macular edema due to
(Rosenfeld et al., 2005)187, bevacizumab has be- RVOs. These findings were confirmed by a recent
come a medication used worldwide for patients relatively large series with a 2-year follow-up (Hi-
affected by various neovascular intraocular dis- kichi et al., 2014)205. Although bevacizumab has
eases including RVOs (Iturralde et al., 2006; been reported to have a similar effect as ranibi-
Jaissle et al., 2006; Rosenfeld et al., 2006; Spandau zumab in controlling macular edema of CRVO
et al., 2006; Costa et al., 2007; Matsumoto et al., patients in various studies, its use in treating
2007; Rabena et al., 2007)188–194. Most of the stud- RVO-related macular edema is mainly off-label
ies published so far agree that bevacizumab and (Kriechbaum et al., 2008; Costa et al., 2007; Ferr-
ranibizumab appear to have improved vision in ara et al., 2007; Pai et al., 2007; Ehlers et al.,
patients with RVOs. 2011)206–210.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 157
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
Ranibizumab. The Ranibizumab for the Treat- RVOs. Hemodilution is expected to prevent the
ment of Macular Edema after Central Retinal slowdown of blood circulation and its complica-
Vein Occlusion (CRUISE) trials compared the ef- tions by dramatically lowering blood viscosity.
fectiveness of ranibizumab 0.3 or 0.5 mg with Some randomized studies have been published
sham in patients with macular edema secondary on the topic showing a statistically significant dif-
to CRVO. Both 6-month and 12-month results ference between treated and nontreated patients
showed superiority of ranibizumab in terms of (Hansen et al., 1989; Hansen et al., 1989; Wolf et
functional and anatomical improvement (Brown al., 1994; Hattenbach et al., 1999; Glacet-Bernard
et al., 2010; Campochiaro et al., 2011)211, 212. After et al., 2001)217–221. These monocenter studies
the CRUISE trial, the 0.5-mg ranibizumab dose were conducted in the 1980s and 1990s, and used
was marketed for treatment of ME resulting from different treatment protocols. A more recent
CRVO. Long-term treatment outcomes were multicenter controlled randomized study using
provided in the HORIZON cohort and the RE- erythrocyte-apheresis, an automated method of
TAIN study, confirming the results with respect hemodilution, confirmed the beneficial effect of
to functional and anatomical improvement in the isovolumic hemodilution administered early in
ranibizumab study group (Campochiaro et al., the course of the CRVO (Glacet-Bernard et al.,
2014)213. The effects of ranibizumab on CRVO 2011)222. For economic and pharmaceutical rea-
and BRVO patients were further ascertained by a sons, however, this treatment becomes less read-
post hoc analysis study regarding the data ob- ily available.
tained by CRUISE and BRAVO (Thach et al.,
2014)61. The improvement in visual acuity could Prevention
be observed as early as 7 days after the injection Only a few studies have addressed the prevention
and were maintained up to 12 months by the as- of a recurrence of an RVO in the same eye or the
needed doses. development of an RVO in the contralateral eye.
Aflibercept. GALILEO and COPERNICUS So far, none of these studies have shown a release
were two sister, phase III randomized double- device, and intravitreal anti-VEGF drugs (bevaci-
masked multicenter clinical studies, which aimed zumab, ranibizumab, aflibercept, pegaptanib)
to evaluate the intravitreal VEGF aflibercept in may at least temporarily reduce any benefit. In
patients with CRVO-related macular edema particular, thrombocyte aggregation inhibitors
(Boyer et al., 2012; Brown et al., 2013)214, 215. It and anticoagulant drugs were not shown to be of
revealed that the study group with aflibercept benefit (Koizumi et al., 2007; McIntosh et al.,
showed a significantly better functional and mor- 2007)56, 223.
phological outcome as compared to the control
group. It was also concluded that visual acuity Potential Future Developments
gain achieved by intravitreally applied aflibercept Future developments may include new intraocu-
could be maintained with less frequent doses of lar drug delivery systems (comparable to the
aflibercept after a loading period. In the GALI- dexamethasone posterior segment drug delivery
LEO study, significantly more aflibercept-treated system (Ozurdex®) for intraocular delivery of
patients gained >15 letters by week 24 than those steroids (Kuppermann et al., 2007; Williams et al.,
receiving sham injections (Holz et al., 2013)216. 2009)224, 225. Other future developments are com-
bination treatments of steroids with anti-VEGF
Systemic Therapy drugs, other slow-release devices for the intraocu-
Several studies have suggested a beneficial effect lar steroid delivery (Ramchandran et al., 2008)226,
of hemodilution as a therapy of the early phase of and addressing aspects of retinal protection and
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
158 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
reopening of occluded retinal capillaries (Otani et Since most studies, particularly those on the use
al., 2004; Harris et al., 2006; Smith, 2006; Jonas et of retinal laser coagulation, performed so far have
al., 2008; Jonas et al., 2009; Ma et al., 2009)227–232. addressed mainly central visual acuity and have
not taken into account the pericentral visual field,
and since pericentral laser coagulation in contrast
Conclusion to an intravitreal drug therapy deteriorates the
pericentral visual field, the clinical value of a peri-
RVOs belong to the most frequently encountered central laser treatment in comparison with intra-
retinal vascular diseases in all ethnic groups. If the vitreal drug therapy has remained unclear.
macula is involved, central visual acuity drops, A preventive therapy to avoid a recurrence of
depending on the amount of foveal edema and RVOs or the development of an RVO in the con-
macular ischemia. It is essential to differentiate tralateral eye has not yet been shown.
between the nonischemic type, which has a rela-
tively good prognosis without treatment, and the
ischemic type, which has a relatively poor prog- Key Messages
nosis. Known risk factors for RVOs include sys-
temic arterial hypertension and glaucomatous • The diagnosis of macular edema from RVO is
optic neuropathy. facilitated by OCT, which allows retinal thick-
Generally vision can be improved as much as it ness to be quantified, and is a useful tool to
was decreased by macular edema. The amount of evaluate the treatment.
vision loss due to capillary nonperfusion cannot • FA or OCT-based angiography remains essen-
currently be markedly increased. Recent case series tial to differentiate perfused macular edema
studies and prospective randomized trials have from ischemic macular edema.
suggested that intravitreal steroids (triamcinolone, • In CRVO, intravitreal injections of steroids or
fluocinolone, dexamethasone in a slow-release de- antiangiogenic drugs seem to demonstrate a
vice) and intravitreal anti-VEGF drugs (bevaci- benefit compared to the natural course. Ongo-
zumab, ranibizumab, aflibercept, pegaptanib) may ing studies are expected to confirm these pre-
at least temporarily reduce foveal edema and cor- liminary results.
respondingly improve visual function. The dura- • Some patients may have transient macular
tion of edema is also crucial. Some patients may edema with spontaneous visual acuity recov-
have transient macular edema with spontaneous ery, but when macular edema is persistent, the
visual acuity recovery. Alternatively, when macu- earlier the treatment the better the chances of
lar edema is persistent, the earlier the treatment the visual response.
better the chances of visual response.
References
1 Hayreh SS: Occlusion of the central reti- 3 Coscas G, Dhermy P: Occlusions veineu- 5 The Central Vein Occlusion Study. Base-
nal vessels. Br J Ophthalmol 1965;49: ses rétiniennes. Paris, Masson, 1978, pp line and early natural history report.
626–645. 283–346. Arch Ophthalmol 1993;111:1087–1095.
2 Hayreh SS: An experimental study of the 4 Hayreh SS: Classification of central reti- 6 The Central Vein Occlusion Study
central retinal vein occlusion. Trans nal vein occlusion. Ophthalmology Group M report. Evaluation of grid pat-
Ophthalmol Soc UK 1964;84:586–595. 1983;90:458–474. tern photocoagulation for macular ede-
ma in central vein occlusion. Ophthal-
mology 1995;102:1425–1433.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 159
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
7 The Central Vein Occlusion Study 19 Hayreh SS, Zimmerman B, McCarthy 30 Risk factors for branch retinal vein oc-
Group N report. A randomized clinical MJ, Podhajsky P: Systemic diseases as- clusion. The Eye Disease Case-Control
trial of early panretinal photocoagula- sociated with various types of retinal Study Group. Am J Ophthalmol 1993;
tion for ischemic central vein occlusion. vein occlusion. Am J Ophthalmol 2001; 116:286–296.
Ophthalmology 1995;102:1434–1444. 131:61–77. 31 Cugati S, Wang JJ, Knudtson MD,
8 Hayreh SS, Klugman MR, Beri M, Kimu- 20 O’Mahoney PR, Wong DT, Ray JG: Reti- Rochtchina E, Klein R, Klein BE, Wong
ra AE, Podhajsky P: Differentiation of nal vein occlusion and traditional risk TY, Mitchell P: Retinal vein occlusion
ischemic from non-ischemic central factors for atherosclerosis. Arch Oph- and vascular mortality: pooled data
retinal vein occlusion during the early thalmol 2008;126:692–699. analysis of 2 population-based cohorts.
acute phase. Graefes Arch Clin Exp Oph- 21 Hayreh S: Prevalent misconceptions Ophthalmology 2007;114:520–524.
thalmol 1990;228:201–217. about acute retinal vascular occlusive 32 Xu L, Liu W, Wang Y, Yang H, Jonas JB:
9 Coscas G, Gaudric A: Natural course of disorders. Prog Retin Eye Res 2005;24: Retinal vein occlusions and mortality.
nonaphakic cystoid macular edema. 493–519. The Beijing Eye Study. Am J Ophthal-
Surv Ophthalmol 1984;28(sup- 22 McIntosh R, Mohamed Q, Saw S, Wong mol 2007;144:972–973.
pl):471–484. T: Interventions for branch retinal vein 33 Girmens JF, Scheer S, Heron E, Sahel JA,
10 Liebreich R: Ueber die Farbe des Augen- occlusion. Ophthalmology 2006;114: Tournier-Lasserve E, Paques M: Famil-
hintergrundes. Albrecht Von Graefes 835–854. ial central retinal vein occlusion. Eye
Arch Ophthalmol 1855;1:333–358. 23 Mohamed Q, McIntosh R, Saw S, Wong 2008;22:308–310.
11 Klein R, Klein BE, Moss SE, Meuer SM: T: Interventions for central retinal vein 34 Natural history and clinical management
The epidemiology of retinal vein occlu- occlusion: an evidence-based systematic of central retinal vein occlusion. The
sion: the Beaver Dam Eye Study. Trans review. Ophthalmology 2006;114:507– Central Vein Occlusion Study Group.
Am Ophthalmol Soc 2000;98:133–141. 519. Arch Ophthalmol 1997;115:486–491.
12 Mitchell P, Smith W, Chang A: Preva- 24 Rogers S, McIntosh RL, Cheung N, Lim 35 Glacet-Bernard A, Bayani N, Chretien P,
lence and associations of retinal vein L, Wang JJ, Mitchell P, Kowalski JW, Cochard C, Lelong F, Coscas G: An-
occlusion in Australia. The Blue Moun- Nguyen H, Wong TY; International Eye tiphospholipid antibodies in retinal vas-
tains Eye Study. Arch Ophthalmol 1996; Disease Consortium: The prevalence cular occlusions. A prospective study of
114:1243–1247. and number of people with retinal vein 75 patients. Arch Ophthalmol 1994;112:
13 Wong TY, Larsen EK, Klein R, Mitchell occlusion: pooled data from population- 790–795.
P, Couper DJ, Klein BE, Hubbard LD, based studies from the US, Europe, Aus- 36 Arsène S, Delahousse B, Regina S, Le Lez
Siscovick DS, Sharrett AR: Cardiovascu- tralia and Asia. Ophthalmology 2010; ML, Pisella PJ, Gruel Y: Increased preva-
lar risk factors for retinal vein occlusion 117:313–319.e1. lence of factor V Leiden in patients with
and arteriolar emboli: the Atherosclero- 25 Leenen FH, Dumais J, McInnis NH, Tur- retinal vein occlusion and under 60
sis Risk in Communities & Cardiovascu- ton P, Stratychuk L, Nemeth K, Moy years of age. Thromb Haemost 2005;94:
lar Health studies. Ophthalmology 2005; Lum-Kwong M, Fodor G: Results of the 101–106.
112:540–547. Ontario survey on the prevalence and 37 Kuhli C, Scharrer I, Koch F, Ohrloff C,
14 Liu W, Xu L, Jonas JB: Vein occlusion in control of hypertension. CMAJ 2008; Hattenbach LO: Factor XII deficiency: a
Chinese subjects. Ophthalmology 2007; 178:1441–1449. thrombophilic risk factor for retinal vein
114:1795–1796. 26 Read JG, Gorman BK: Racial/ethnic dif- occlusion. Am J Ophthalmol 2004;137:
15 Zhou JQ, Xu L, Wang S, Wang YX, You ferences in hypertension and depression 459–464.
QS, Tu Y, Yang H, Jonas JB: The 10-year among US adult women. Ethn Dis 2007; 38 Kuhli C, Hattenbach LO, Scharrer I,
incidence and risk factors of retinal vein 17:389–396. Koch F, Ohrloff C: High prevalence of
occlusion: the Beijing Eye Study. Oph- 27 Giles T, Aranda JMJ, Suh DC, Choi IS, resistance to APC in young patients with
thalmology 2013;120:803–808. Preblick R, Rocha R, Frech-Tamas F: retinal vein occlusion. Graefes Arch Clin
16 Cheung N, Klein R, Wang JJ, Cotch MF, Ethnic/racial variations in blood pres- Exp Ophthalmol 2002;240:163–168.
Islam AF, Klein BE, Cushman M, Wong sure awareness, treatment, and control. 39 Pinna A, Carru C, Solinas G, Zinellu A,
TY: Traditional and novel cardiovascu- J Clin Hypertens 2007;9:345–354. Carta F: Glucose-6-phosphate dehydro-
lar risk factors for retinal vein occlusion: 28 Ostchega Y, Hughes JP, Wright JD, Mc- genase deficiency in retinal vein occlu-
the multiethnic study of atherosclerosis. Dowell MA, Louis T: Are demographic sion. Invest Ophthalmol Vis Sci 2007;48:
Invest Ophthalmol Vis Sci 2008;49: characteristics, health care access and 2747–2752.
4297–4302. utilization, and comorbid conditions 40 Jonas JB, Wang N, Wang YX, You QS,
17 Lim LL, Cheung N, Wang JJ, Islam FM, associated with hypertension among US Yang D, Xie X, Xu L: Incident retinal vein
Mitchell P, Saw SM, Aung T, Wong TY: adults? Am J Hypertens 2008;21:159– occlusions and estimated cerebrospinal
Prevalence and risk factors of retinal 165. fluid pressure. The Beijing Eye Study.
vein occlusion in an Asian population. 29 Hayreh SS, Zimmerman MB, Podhajsky Acta Ophthalmol 2015;93:e522–e526.
Br J Ophthalmol 2008;92:1316–1319. P: Hematological abnormalities associ- 41 Berdahl JP, Fleischman D, Zaydlarova J,
18 Jonas JB, Nangia V, Khare A, Sinha A, ated with various types of retinal vein Stinnett S, Allingham RR, Fautsch MP:
Lambat S: Prevalence of retinal vein oc- occlusion. Graefes Arch Clin Exp Oph- Body mass index has a linear relation-
clusion. The Central India Eye and Med- thalmol 2002;240:180–196. ship with cerebrospinal fluid pressure.
ical Study. Retina 2013;33:152–159. Invest Ophthalmol Vis Sci 2012;53:
1422–1427.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
160 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
42 Ren R, Wang N, Zhang X, Tian G, Jonas 52 Du KF, Xu L, Shao L, Chen CX, Zhou JQ, 63 Haller JA, Bandello F, Belfort R Jr, Blu-
JB: Cerebrospinal fluid pressure corre- Wang YX, You QS, Jonas JB, Wei WB: menkranz MS, Gillies M, Heier J, Loew-
lated with body mass index. Graefes Subfoveal choroidal thickness in retinal enstein A, Yoon YH, Jacques ML, Jiao J,
Arch Clin Exp Ophthalmol 2013;250: vein occlusion. The Beijing Eye Study Li XY, Whitcup SM; OZURDEX GENE-
445–446. 2011. Ophthalmology 2013;120:2749– VA Study Group: Randomized, sham-
43 Jonas JB, Wang N, Wang S, Wang YX, 2750. controlled trial of dexamethasone intra-
You QS, Yang D, Wei WB, Xu L: Retinal 53 Tsuiki E, Suzuma K, Ueki R, Maekawa vitreal implant in patients with macular
vessel diameter and estimated cerebro- Y, Kitaoka T: Enhanced depth imaging edema due to retinal vein occlusion.
spinal fluid pressure in arterial hyper- optical coherence tomography of the Ophthalmology 2010;117:1134–1146.
tension. The Beijing Eye Study. Am J choroid in central retinal vein occlusion. 64 Haller JA, Bandello F, Belfort R Jr, Blu-
Hypertens 2014;27:1170–1178. Am J Ophthalmol 2013;156:543–547. menkranz MS, Gillies M, Heier J, Loew-
44 Glacet-Bernard A, les Jardins GL, Lasry S, 54 Xu L, You QS, Jonas JB: Central corneal enstein A, Yoon YH, Jiao J, Li XY, Whit-
Coscas G, Soubrane G, Souied E, Housset thickness and retinal vein occlusions: cup SM; Ozurdex GENEVA Study
B: Obstructive sleep apnea among pa- the Beijing Eye Study. Graefes Arch Clin Group, Li J: Dexamethasone intravitreal
tients with retinal vein occlusion. Arch Exp Ophthalmol 2010;248:759–760. implant in patients with macular edema
Ophthalmol 2010;128:1533–1538. 55 Xu L, You QS, Liu W, Jonas JB: Smoking related to branch or central retinal vein
45 Chou K-T, Huang C-C, Tsai DC, Chen and retinal vein occlusions. The Beijing occlusion twelve-month study results.
YM, Perng DW, Shiao GM, Lee YC, Leu Eye Study. Graefes Arch Clin Ophthal- Ophthalmology 2011;118:2453–2460.
HB: Sleep apnea and risk of retinal vein mol 2010;248:1046–1046. 65 Hayreh SS, Hayreh MS: Hemi-central
occlusion: a nationwide population- 56 Koizumi H, Ferrara DC, Bruè C, Spaide retinal vein occlusion. Pathogenesis,
based study of Taiwanese. Am J Oph- RF: Central retinal vein occlusion case- clinical features, and natural history.
thalmol 2012;154:200–205. control study. Am J Ophthalmol 2007; Arch Ophthalmol 1980;98:1600–1609.
46 Paques M, Massin P, Sahel JA, Gaudric 144:858–863. 66 Paques M, Girmens JF, Riviere E, Sahel
A, Bergmann JF, Azancot S, Lévy BI, 57 Glacet-Bernard A, Coscas G, Chabanel J: Dilation of the minor arterial circle of
Vicaut E: Circadian fluctuations of mac- A, Zourdani A, Lelong F, Samama MM: the iris preceding rubeosis iridis during
ular edema in patients with morning Prognostic factors for retinal vein occlu- retinal vein occlusion. Am J Ophthalmol
vision blurring: correlation with arterial sion: prospective study of 175 cases. 2004;138:1083–1086.
pressure and effect of light deprivation. Ophthalmology 1996;103:551–560. 67 Casselholmde Salles M, Kvanta A, Am-
Invest Ophthalmol Vis Sci 2005;46: 58 Browning DJ: Patchy ischemic retinal rén U, Epstein D: Optical coherence to-
4707–4711. whitening in acute central retinal vein mography angiography in central retinal
47 Gupta B, Grewal J, Adewoyin T, Pelosini occlusion. Ophthalmology 2002;109: vein occlusion: correlation between the
L, Williamson TH: Diurnal variation of 2154–2159. foveal avascular zone and visual acuity.
macular oedema in CRVO: prospective 59 Paques M, Gaudric A: Perivenous macu- Invest Ophthalmol Vis Sci 2016;
study. Graefes Arch Clin Exp Ophthal- lar whitening during central retinal vein 57:OCT242–OCT246.
mol 2009;247:593–596. occlusion. Arch Ophthalmol 2003;121: 68 Coscas F, Glacet-Bernard A, Miere A,
48 Usui S, Ikuno Y, Akiba M, Maruko I, 1488–1491. Caillaux V, Uzzan J, Lupidi M, Coscas G,
Sekiryu T, Nishida K, Iida T: Circadian 60 Gutman FA: Macular edema in branch Souied EH: Optical coherence tomogra-
changes in subfoveal choroidal thick- retinal vein occlusion: prognosis and phy angiography in retinal vein occlu-
ness and the relationship with circula- management. Trans Am Acad Ophthal- sion: evaluation of superficial and deep
tory factors in healthy subjects. Invest mol Otolaryngol 1977;83:488–495. capillary plexa. Am J Ophthalmol 2016;
Ophthalmol Vis Sci 2012;53:2300–2307. 61 Thach AB, Yau L, Hoang C, Tuomi L: 161:160–171.
49 Tan CS, Ouyang Y, Ruiz H, Sadda SR: Time to clinically significant visual acu- 69 Abri Aghdam K, Reznicek L, Soltan San-
Diurnal variation of choroidal thickness ity gains after ranibizumab treatment jari M, Framme C, Bajor A, Klingenstein
in normal, healthy subjects measured by for retinal vein occlusion: BRAVO and A, Kernt M, Seidensticker F: Peripheral
spectral domain optical coherence to- CRUISE trials. Ophthalmology 2014; retinal non-perfusion and treatment
mography. Invest Ophthalmol Vis Sci 121:1059–1066. response in branch retinal vein occlu-
2012;53:261–266. 62 Campochiaro PA, Heier JS, Feiner L, sion. Int J Ophthalmol 2016;9:858–862.
50 Jonas JB, Wang N, Yang D, Ritch R, Gray S, Saroj N, Rundle AC, Murahashi 70 Kashani AH, Lee SY, Moshfeghi A,
Panda-Jonas S: Facts and myths of cere- WY, Rubio RG; BRAVO Investigators: Durbin MK, Puliafito CA: Optical coher-
brospinal fluid pressure for the physiol- Ranibizumab for macular edema follow- ence tomography angiography of retinal
ogy of the eye. Prog Retin Eye Res 2015; ing branch retinal vein occlusion: six venous occlusion. Retina 2015;35:2323–
46:67–83. month primary end point results of a 2331.
51 Jonas JB, Wang N, Wang YX, You QS, phase III study. Ophthalmology 2010; 71 Suzuki N, Hirano Y, Yoshida M, Tomi-
Yang D, Xie X, Wei WB, Xu L: Subfoveal 117:1102–1112. yasu T, Uemura A, Yasukawa T, Ogura
choroidal thickness and cerebrospinal Y: Microvascular abnormalities on opti-
fluid pressure. The Beijing Eye Study cal coherence tomography angiography
2011. Invest Ophthalmol Vis Sci 2014; in macular edema associated with
55:1292–1928. branch retinal vein occlusion. Am J
Ophthalmol 2016;161:126–132.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 161
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
72 Laatikainen L, Kohner EM: Fluorescein 82 Glacet-Bernard A, Sellam A, Coscas F, 94 Hayreh SS, Rubenstein L, Podhajsky P:
angiography and its prognostic signifi- Coscas G, Souied EH: Optical coherence Argon laser scatter photocoagulation
cance in central retinal vein occlusion. tomography angiography in retinal vein in treatment of branch retinal vein
Br J Ophthalmol 1976;60:411–418. occlusion treated with dexamethasone occlusion. A prospective clinical trial.
73 Catier A, Tadayoni R, Paques M, Ergin- Implant: a new test for follow-up evalua- Ophthalmologica 1993;206:1–14.
ay A, Haouchine B, Gaudric A, Massin tion. Eur J Ophthalmol 2016;26:460–468. 95 Arnarsson A, Stefánsson E: Laser treat-
P: Characterization of macular edema 83 Sellam A, Glacet-Bernard A, Coscas F, ment and the mechanism of edema
from various etiologies by optical coher- Miere A, Coscas G, Souied E: Qualitative reduction in branch retinal vein occlu-
ence tomography. Am J Ophthalmol and quantitative follow-up using optical sion. Invest Ophthalmol Vis Sci 2000;
2005;140:200–206. coherence tomography angiography of 41:877–879.
74 Ota M, Tsujikawa A, Kita M, Miyamoto retinal vein occlusion treated with anti- 96 Maár N, Luksch A, Graebe A, Ergun E,
K, Sakamoto A, Yamaike N, Kotera Y, VEGF: optical coherence tomography Wimpissinger B, Tittl M, Vécsei P, Stur
Yoshimura N: Integrity of foveal photo- angiography follow-up of retinal vein M, Schmetterer L: Effect of laser pho-
receptor layer in central retinal vein oc- occlusion. Retina 2016, Epub ahead of tocoagulation on the retinal vessel di-
clusion. Retina 2008;28:1502–1508. print. ameter in branch and macular vein
75 Shroff D, Mehta DK, Arora R, Narula R, 84 Hitchings RA, Spaeth GL: Chronic reti- occlusion. Arch Ophthalmol 2004;122:
Chauhan D: Natural history of macular nal vein occlusion in glaucoma. Br J 987–991.
status in recent-onset branch retinal Ophthalmol 1976;60:694–699. 97 Ohashi H, Oh H, Nishiwaki H, Nonaka
vein occlusion: an optical coherence 85 Jonas JB: Reproducibility of ophthalmo- A, Takagi H: Delayed absorption of
tomography study. Int Ophthalmol dynamometric measurements of the cen- macular edema accompanying serous
2008;28:261–268. tral retinal artery and vein collapse pres- retinal detachment after grid laser
76 Wei E, Jia Y, Tan O, Potsaid B, Liu JJ, sure. Br J Ophthalmol 2003;87:577–579. treatment in patients with branch reti-
Choi W, Fujimoto JG, Huang D: Parafo- 86 Jonas JB: Ophthalmodynamometric as- nal vein occlusion. Ophthalmology
veal retinal vascular response to pattern sessment of the central retinal vein col- 2004;111:2050–2056.
visual stimulation assessed with OCT lapse pressure in eyes with retinal vein 98 Esrick E, Subramanian ML, Heier JS,
angiography. PLoS One 2013;8:e81343. stasis or occlusion. Graefes Arch Clin Devaiah AK, Topping TM, Frederick
77 Wang X, Jia Y, Spain R, Potsaid B, Liu JJ, Exp Ophthalmol 2003;241:367–370. AR, Morley MG: Multiple laser treat-
Baumann B, Hornegger J, Fujimoto JG, 87 Jonas JB: Central retinal artery and vein ments for macular edema attributable
Wu Q, Huang D: Optical coherence to- pressure in patients with chronic open- to branch retinal vein occlusion. Am J
mography angiography of optic nerve angle glaucoma. Br J Ophthalmol 2003; Ophthalmol 2005;139:653–657.
head and parafovea in multiple sclerosis. 87:949–951. 99 Parodi MB, Spasse S, Iacono P, Di Ste-
Br J Ophthalmol 2014;98:1368–1373. 88 Jonas JB: Ophthalmodynamometric de- fano G, Canziani T, Ravalico G: Sub-
78 Jia Y, Wei E, Wang X, Zhang X, Morri- termination of the central retinal vessel threshold grid laser treatment of mac-
son JC, Parikh M, Lombardi LH, Gattey collapse pressure correlated with sys- ular edema secondary to branch retinal
DM, Armour RL, Edmunds B, Kraus temic blood pressure. Br J Ophthalmol vein occlusion with micropulse infra-
MF, Fujimoto JG, Huang D: Optical co- 2004;88:501–504. red (810 nanometer) diode laser. Oph-
herence tomography angiography of 89 Harder B, Jonas JB: Frequency of spon- thalmology 2006;113:2237–2242.
optic disc perfusion in glaucoma. Oph- taneous pulsations of the central retinal 100 Hayreh SS: Management of central
thalmology 2014;121:1322–1332. vein in normal eyes. Br J Ophthalmol retinal vein occlusion. Ophthalmologi-
79 Jia Y, Bailey ST, Hwang TS, McClintic 2007;91:401–402. ca 2003;217:167–188.
SM, Gao SS, Pennesi ME, Flaxel CJ, Lau- 90 Jonas JB, Harder B: Ophthalmodynamo- 101 Opremcak EM, Bruce RA: Surgical
er AK, Wilson DJ, Hornegger J, Fujimo- metric differences between ischemic ver- decompression of branch retinal vein
to JG, Huang D: Quantitative optical sus non-ischemic retinal vein occlusion. occlusion via arteriovenous crossing
coherence tomography angiography of Am J Ophthalmol 2007;143:112–116. sheathotomy: a prospective review of
vascular abnormalities in the living hu- 91 Hayreh SS, Klugman MR, Podhajsky P, 15 cases. Retina 1999;19:1–5.
man eye. Proc Natl Acad Sci USA 2015; Servais GE, Perkins ES: Argon laser pan- 102 Shah GK, Sharma S, Fineman MS, Fe-
112:E2395–E2402. retinal photocoagulation in ischemic derman J, Brown MM, Brown GC: Ar-
80 Yu J, Jiang C, Wang X, Zhu L, Gu R, Xu central retinal vein occlusion. A 10-year teriovenous adventitial sheathotomy
H, Jia Y, Huang D, Sun X: Macular per- prospective study. Graefes Arch Clin for the treatment of macular edema
fusion in healthy Chinese: an optical Exp Ophthalmol 1990;228:281–296. associated with branch retinal vein
coherence tomography angiogram 92 Argon laser photocoagulation for macu- occlusion. Am J Ophthalmol 2000;129:
study. Invest Ophthalmol Vis Sci 2015; lar edema in branch vein occlusion. The 104–106.
56:3212–3217. Branch Vein Occlusion Study Group. 103 Le Rouic JF, Bejjani RA, Rumen F,
81 Pechauer AD, Jia Y, Liu L, Gao SS, Jiang Am J Ophthalmol 1984;98:271–282. Caudron C, Bettembourg O, Renard G,
C, Huang D: Optical coherence tomog- 93 Argon laser scatter photocoagulation for Chauvaud D: Adventitial sheathotomy
raphy angiography of peripapillary reti- prevention of neovascularization and for decompression of recent onset
nal blood flow response to hyperoxia. vitreous hemorrhage in branch vein branch retinal vein occlusion. Graefes
Invest Ophthalmol Vis Sci 2015;56: occlusion. A randomized clinical trial. Arch Clin Exp Ophthalmol 2001;239:
3287–3291. Branch Vein Occlusion Study Group. 747–751.
Arch Ophthalmol 1986;104:34–41.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
162 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
104 Cahill MT, Kaiser PK, Sears JE, Fekrat 113 Spaide RF, Klancnik JM Jr, Gross NE: 122 Kumagai K, Furukawa M, Ogino N,
S: The effect of arteriovenous sheathot- Retinal choroidal collateral circulation Larson E, Uemura A: Long-term visual
omy on cystoid macular oedema sec- after radial optic neurotomy correlated outcomes after vitrectomy for macular
ondary to branch retinal vein occlu- with the lessening of macular edema. edema with foveal hemorrhage in
sion. Br J Ophthalmol 2003;87: Retina 2004;243:356–359. branch retinal vein occlusion. Retina
1329–1332. 114 Arevalo JF, Garcia RA, Wu L, Rodri- 2007;27:584–588.
105 Fujii GY, de Juan E Jr, Humayun MS: guez FJ, Dalma-Weiszhausz J, Quiroz- 123 Berker N, Batman C: Surgical treat-
Improvements after sheathotomy for Mercado H, Morales-Canton V, Roca ment of central retinal vein occlusion.
branch retinal vein occlusion docu- JA, Berrocal MH, Graue-Wiechers F, Acta Ophthalmol 2008;86:245–252.
mented by optical coherence tomogra- Robledo V; Pan-American Collabora- 124 Oh IK, Kim S, Oh J, Huh K: Long-term
phy and scanning laser ophthalmo- tive Retina Study Group: Radial optic visual outcome of arteriovenous ad-
scope. Ophthalmic Surg Lasers neurotomy for central retinal vein oc- ventitial sheathotomy on branch reti-
Imaging 2003;34:49–52. clusion: results of the Pan-American nal vein occlusion induced macular
106 Mason J 3rd, Feist R, White M Jr, Collaborative Retina Study Group (PA- edema. Korean J Ophthalmol 2008;22:
Swanner J, McGwin G Jr, Emond T: CORES). Retina 2008;288:1044–1052. 1–5.
Sheathotomy to decompress branch 115 Hayreh SS: Radial optic neurotomy for 125 Arai M, Yamamoto S, Mitamura Y,
retinal vein occlusion: a matched con- central retinal vein occlusion. Retina Sato E, Sugawara T, Mizunoya S: Effi-
trol study. Ophthalmology 2004;111: 2002;226:827. cacy of vitrectomy and internal limit-
540–545. 116 Saika S, Tanaka T, Miyamoto T, Ohni- ing membrane removal for macular
107 Charbonnel J, Glacet-Bernard A, Koro- shi Y: Surgical posterior vitreous de- edema associated with branch retinal
belnik JF, Nyouma-Moune E, Pour- tachment combined with gas/air tam- vein occlusion. Ophthalmologica 2009;
naras CJ, Colin J, Coscas G, Soubrane ponade for treating macular edema 223:172–176.
G: Management of branch retinal vein associated with branch retinal vein 126 DeCroos FC, Shuler RK Jr, Stinnett S,
occlusion with vitrectomy and arterio- occlusion: retinal tomography and vi- Fekrat S: Pars plana vitrectomy, inter-
venous adventitial sheathotomy, the sual outcome. Graefes Arch Clin Exp nal limiting membrane peeling, and
possible role of surgical posterior vitre- Ophthalmol 2001;239:729–732. panretinal endophotocoagulation for
ous detachment. Graefes Arch Clin 117 García-Arumí J, Martinez-Castillo V, macular edema secondary to central
Exp Ophthalmol 2004;242:223–228. Boixadera A, Blasco H, Corcostegui B: retinal vein occlusion. Am J Ophthal-
108 Yamaji H, Shiraga F, Tsuchida Y, Ya- Management of macular edema in mol 2009;147:627–633.e1.
mamoto Y, Ohtsuki H: Evaluation of branch retinal vein occlusion with shea- 127 Lu N, Wang NL, Wang GL, Li XW,
arteriovenous crossing sheathotomy thotomy and recombinant tissue plas- Wang Y: Vitreous surgery with direct
for branch retinal vein occlusion by minogen activator. Retina 2004;24:530– central retinal artery massage for cen-
fluorescein videoangiography and im- 540. tral retinal artery occlusion. Eye 2009;
age analysis. Am J Ophthalmol 2004; 118 Mandelcorn MS, Nrusimhadevara RK: 23:867–872.
137:834–841. Internal limiting membrane peeling 128 Uemura A, Yamamoto S, Sato E, Suga-
109 Yamamoto S, Saito W, Yagi F, Takeu- for decompression of macular edema wara T, Mitamura Y, Mizunoya S: Vit-
chi S, Sato E, Mizunoya S: Vitrectomy in retinal vein occlusion: a report of 14 rectomy alone versus vitrectomy with
with or without arteriovenous adventi- cases. Retina 2004;24:348–355. simultaneous intravitreal injection of
tial sheathotomy for macular edema 119 Radetzky S, Walter P, Fauser S, Koi- triamcinolone for macular edema as-
associated with branch retinal vein zumi K, Kirchhof B, Joussen AM: Vi- sociated with branch retinal vein oc-
occlusion. Am J Ophthalmol 2004;138: sual outcome of patients with macular clusion. Ophthalmic Surg Lasers Imag-
907–914. edema after pars plana vitrectomy and ing 2009;40:6–12.
110 Opremcak EM, Bruce RA, Lomeo MD, indocyanine green-assisted peeling of 129 Lewis H, Abrams GW, Blumenkranz
Ridenour CD, Letson AD, Rehmar AJ: the internal limiting membrane. Grae- MS, Campo RV: Vitrectomy for dia-
Radial optic neurotomy for central fes Arch Clin Exp Ophthalmol 2004; betic macular traction and edema as-
retinal vein occlusion: a retrospective 242:273–278. sociated with posterior hyaloidal trac-
pilot study of 11 consecutive cases. 120 Nkeme J, Glacet-Bernard A, Gnikpingo tion. Ophthalmology 1992;99:753–759.
Retina 2001;215:408–415. K, Zourdani A, Mimoun G, Mahiddine 130 Stefánsson E: Physiology of vitreous
111 García-Arumí J, Boixadera A, Martine- H, Gkoritsa A, Tchamo A, Coscas G, surgery. Graefes Arch Clin Exp Oph-
zCastillo V, Castillo R, Dou A, Corco- Soubrane G: Surgical treatment of per- thalmol 2009;247:147–163.
stegui B: Chorioretinal anastomosis sistent macular edema in retinal vein 131 Weiss JN: Treatment of central retinal
after radial optic neurotomy for central occlusion (in French). J Fr Ophthalmol vein occlusion by injection of tissue
retinal vein occlusion. Arch Ophthal- 2006;29:808–814. plasminogen activator into a retinal
mol 2003;121:1385–1391. 121 Kumagai K, Furukawa M, Ogino N, vein. Am J Ophthalmol 1998;126:142–
112 Weizer JS, Stinnett SS, Fekrat S: Radial Uemura A, Larson E: Long-term out- 144.
optic neurotomy as treatment for cen- comes of vitrectomy with or without 132 Weiss JN, Bynoe LA: Injection of tissue
tral retinal vein occlusion. Am J Oph- arteriovenous sheathotomy in branch plasminogen activator into a branch
thalmol 2003;136:814–819. retinal vein occlusion. Retina 2007;27: retinal vein in eyes with central retinal
49–54. vein occlusion. Ophthalmology 2001;
108:2249–2257.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 163
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
133 Greenberg PB, Martidis A, Rogers AH, 145 Antoszyk AN, Gottlieb JL, Machemer 154 Cekiç O, Chang S, Tseng JJ, Barile GR,
Duker JS, Reichel E: Intravitreal triam- R, Hatchell DL: The effects of intravit- Weissman H, Del Priore LV, Schiff
cinolone acetonide for macular oede- real triamcinolone acetonide on exper- WM, Weiss M, Klancnik JM Jr: Intra-
ma due to central retinal vein occlu- imental pre-retinal neovascularization. vitreal triamcinolone treatment for
sion. Br J Ophthalmol 2002;86: Graefes Arch Clin Exp Ophthalmol macular edema associated with central
247–248. 1993;231:34–40. retinal vein occlusion and hemiretinal
134 Jonas JB, Kreissig I, Degenring RF: 146 Penfold PL, Wong JG, Gyory J, Billson vein occlusion. Retina 2005;25:846–
Intravitreal triamcinolone acetonide as FA: Effects of triamcinolone acetonide 850.
treatment of macular oedema in cen- on microglial morphology and quanti- 155 Cekiç O, Chang S, Tseng JJ, Barile GR,
tral retinal vein occlusion. Graefes tative expression of MHC-II in exuda- Del Priore LV, Weissman H, Schiff
Arch Clin Exp Ophthalmol 2002;240: tive age-related macular degeneration. WM, Ober MD: Intravitreal triamcino-
782–783. Clin Exp Ophthalmol 2001;29:188– lone injection for treatment of macular
135 Park CH, Jaffe GJ, Fekrat S: Intravitreal 192. edema secondary to branch retinal
triamcinolone acetonide in eyes with 147 Penfold PL, Wen L, Madigan MC, King vein occlusion. Retina 2005;25:851–
cystoid macular edema associated with NJ, Provis JM: Modulation of perme- 855.
central retinal vein occlusion. Am J ability and adhesion molecule expres- 156 Jonas JB, Akkoyun I, Kamppeter B, Kre-
Ophthalmol 2003;136:419–425. sion by human choroidal endothelial issig I, Degenring RF: Branch retinal
136 Jonas JB: Intravitreal triamcinolone cells. Invest Ophthalmol Vis Sci 2002; vein occlusion treated by intravitreal
acetonide for treatment of intraocular 43:3125–3130. triamcinolone acetonide. Eye 2005;19:
oedematous and neovascular diseases. 148 Jonas JB, Kreissig I, Degenring RF: 65–71.
Acta Ophthalmol 2005;83:645–663. Intravitreal triamcinolone acetonide as 157 Jonas JB, Akkoyun I, Kamppeter B,
137 Wingate RJ, Beaumont PE: Intravitreal treatment of macular edema in central Kreissig I, Degenring RF: Intravitreal
triamcinolone and elevated intraocular retinal vein occlusion. Graefes Arch triamcinolone acetonide for treatment
pressure. Aust NZ J Ophthalmol 1999; Clin Exp Ophthalmol 2002;240:782– of central retinal vein occlusion. Eur J
27:431–432. 783. Ophthalmol 2005;15:751–758.
138 Bakri SJ, Beer PM: The effect of intra- 149 Bashshur ZF, Ma’luf RN, Allam S, Jur- 158 Jonas JB, Kreissig I, Degenring R: In-
vitreal triamcinolone acetonide on di FA, Haddad RS, Noureddin BN: In- travitreal triamcinolone acetonide for
intraocular pressure. Ophthalmic Surg travitreal triamcinolone for the man- treatment of intraocular proliferative,
Lasers Imaging 2003;34:386–390. agement of macular edema due to exudative, and neovascular diseases.
139 Benz MS, Murray TG, Dubovy SR, Katz nonischemic central retinal vein occlu- Prog Retin Eye Res 2005;24:587–611.
RS, Eifrig CW: Endophthalmitis caused sion. Arch Ophthalmol 2004;122: 159 Lee H, Shah GK: Intravitreal triamcino-
by Mycobacterium chelonae absces- 1137–1140. lone as primary treatment of cystoid
sus after intravitreal injection of triam- 150 Ip MS, Gottlieb JL, Kahana A, Scott IU, macular edema secondary to branch
cinolone. Arch Ophthalmol 2003;121: Altaweel MM, Blodi BA, Gangnon RE, retinal vein occlusion. Retina 2005;25:
271–273. Puliafito CA: Intravitreal triamcino- 551–555.
140 Jonas JB, Kreissig I, Degenring RF: En- lone for the treatment of macular ede- 160 Chen SD, Sundaram V, Lochhead J,
dophthalmitis after intravitreal injec- ma associated with central retinal vein Patel CK: Intravitreal triamcinolone
tion of triamcinolone acetonide. Arch occlusion. Arch Ophthalmol 2004;122: for the treatment of ischemic macular
Ophthalmol 2003;121:1663–1664. 1131–1136. edema associated with branch retinal
141 Jonas JB, Kreissig I, Degenring R: In- 151 Jonas JB, Degenring R, Kamppeter B, vein occlusion. Am J Ophthalmol 2006;
traocular pressure after intravitreal Kreissig I, Akkoyun I: Duration of the 141:876–883.
injection of triamcinolone acetonide. effect of intravitreal triamcinolone 161 Goff MJ, Jumper JM, Yang SS, Fu AD,
Br J Ophthalmol 2003;87:24–27. acetonide as treatment of diffuse dia- Johnson RN, McDonald HR, Ai E: In-
142 Jonas JB, Bleyl U: Morphallaxia-like betic macular edema. Am J Ophthal- travitreal triamcinolone acetonide
ocular histology after intravitreal tri- mol 2004;138:158–160. treatment of macular edema associated
amcinolone acetonide. Br J Ophthal- 152 Karacorlu M, Ozdemir H, Karacorlu S: with central retinal vein occlusion.
mol 2004;88:839–840. Intravitreal triamcinolone acetonide Retina 2006;26:896–901.
143 Ishibashi T, Miki K, Sorgente N, Pat- for the treatment of central retinal vein 162 Gregori NZ, Rosenfeld PJ, Puliafito CA,
terson R, Ryan SJ: Effects of intravit- occlusion in young patients. Retina Flynn HW Jr, Lee JE, Mavrofrides EC,
real administration of steroids on ex- 2004;24:324–327. Smiddy WE, Murray TG, Berrocal AM,
perimental subretinal 153 Karacorlu M, Ozdemir H, Karacorlu Scott IU, Gregori G: One-year safety
neovascularization in the subhuman SA: Resolution of serous macular de- and efficacy of intravitreal triamcino-
primate. Arch Ophthalmol 1985;103: tachment after intravitreal triamcino- lone acetonide for the management of
708–711. lone acetonide treatment of patients macular edema secondary to central
144 Wilson CA, Berkowitz BA, Sato Y, with branch retinal vein occlusion. retinal vein occlusion. Retina 2006;26:
Ando N, Handa JT, de Juan E Jr: Treat- Retina 2005;25:856–860. 889–895.
ment with intravitreal steroid reduces 163 Jonas JB: Intravitreal triamcinolone
blood-retinal barrier breakdown due acetonide: a change in a paradigm.
to retinal photocoagulation. Arch Oph- Ophthalmic Res 2006;38:218–245.
thalmol 1992;110:1155–1159.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
164 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
164 Ramezani A, Entezari M, Moradian S, 173 Parodi MB, Iacono P, Ravalico G: In- 182 Wu WC, Cheng KC, Wu HJ: Intravit-
Tabatabaei H, Kadkhodaei S: Intravit- travitreal triamcinolone acetonide real triamcinolone acetonide vs bevaci-
real triamcinolone for acute central combined with subthreshold grid laser zumab for treatment of macular oede-
retinal vein occlusion; a randomized treatment for macular oedema in ma due to central retinal vein
clinical trial. Graefes Arch Clin Exp branch retinal vein occlusion: a pilot occlusion. Eye (Lond) 2009;23:2215–
Ophthalmol 2006;244:1601–1606. study. Br J Ophthalmol 2008;92:1046– 2222.
165 Bhavsar AR, Ip MS, Glassman AR; DR- 1050. 183 Scott IU, VanVeldhuisen PC, Oden NL,
CRnet and the SCORE Study Groups: 174 Patel PJ, Zaheer I, Karia N: Intravitreal Ip MS, Blodi BA, Jumper JM, Figueroa
The risk of endophthalmitis following triamcinolone acetonide for macular M, SCORE Study Investigator Group:
intravitreal triamcinolone injection in oedema owing to retinal vein occlu- SCORE Study report 1: baseline asso-
the DRCRnet and SCORE clinical tri- sion. Eye 2008;22:60–64. ciations between central retinal thick-
als. Am J Ophthalmol 2007;144:454– 175 Riese J, Loukopoulos V, Meier C, Tim- ness and visual acuity in patients with
456. mermann M, Gerding H: Combined retinal vein occlusion. Ophthalmology
166 Hirano Y, Sakurai E, Yoshida M, Ogura intravitreal triamcinolone injection 2009;116:504–512.
Y: Comparative study on efficacy of a and laser photocoagulation in eyes 184 Scott IU, Blodi BA, Ip MS, Vanveld-
combination therapy of triamcinolone with persistent macular edema after huisen PC, Oden NL, Chan CK, Gonza-
acetonide administration with and branch retinal vein occlusion. Graefes lez V; SCORE Study Investigator
without vitrectomy for macular edema Arch Clin Exp Ophthalmol 2008;246: Group: SCORE Study Report 2: in-
associated with branch retinal vein 1671–1676. terobserver agreement between inves-
occlusion. Ophthalmic Res 2007;39: 176 Roth DB, Cukras C, Radhakrishnan R, tigator and reading center classifica-
207–212. Feuer WJ, Yarian DL, Green SN, tion of retinal vein occlusion type.
167 Jonas JB, Rensch F: Decreased retinal Wheatley HM, Prenner J: Intravitreal Ophthalmology 2009;116:756–761.
vein diameter after intravitreal triam- triamcinolone acetonide injections in 185 Ip MS, Scott IU, VanVeldhuisen PC,
cinolone for retinal vein occlusions. Br the treatment of retinal vein occlu- Oden NL, Blodi BA, Fisher M, Singer-
J Ophthalmol 2007;91:1711–1712. sions. Ophthalmic Surg Lasers Imaging man LJ, Tolentino M, Chan CK, Gon-
168 Karacorlu M, Karacorlu SA, Ozdemir 2008;39:446–454. zalez VH; SCORE Study Research
H, Senturk F: Intravitreal triamcino- 177 Cheng KC, Wu WC, Lin CJ: Intravitreal Group: A randomized trial comparing
lone acetonide for treatment of serous triamcinolone acetonide for patients the efficacy and safety of intravitreal
macular detachment in central retinal with macular oedema due to central triamcinolone with observation to
vein occlusion. Retina 2007;27:1026– retinal vein occlusion in Taiwan. Eye treat vision loss associated with macu-
1030. 2009;23:849–857. lar edema secondary to central retinal
169 Pathai S: Intravitreal triamcinolone 178 Gewaily D, Greenberg PB: Intravitreal vein occlusion: the Standard Care vs
acetonide for treatment of persistent steroids versus observation for macu- Corticosteroid for Retinal Vein Occlu-
macular oedema in branch retinal vein lar edema secondary to central retinal sion (SCORE) study report 5. Arch
occlusion. Eye 2007;21:255–256. vein occlusion. Cochrane Database Ophthalmol 2009;127:1101–1114.
170 Cakir M, Dogan M, Bayraktar Z, Syst Rev 2009;1:CD007324. 186 Ho M, Liu DT, Lam DS, Jonas JB: Reti-
Bayraktar S, Acar N, Altan T, Kapran 179 McAllister IL, Vijayasekaran S, Chen nal vein occlusions, from basics to the
Z, Yilmaz OF: Efficacy of intravitreal SD, Yu DY: Effect of triamcinolone latest treatment. Retina 2016;36:432–
triamcinolone for the treatment of acetonide on vascular endothelial 448.
macular edema secondary to branch growth factor and occludin levels in 187 Rosenfeld PJ, Moshfeghi AA, Puliafito
retinal vein occlusion in eyes with or branch retinal vein occlusion. Am J CA: Optical coherence tomography
without grid laser photocoagulation. Ophthalmol 2009;147:838–846. findings after an intravitreal injection
Retina 2008;28:465–472. 180 Scott IU, Ip MS, VanVeldhuisen PC, of bevacizumab (Avastin) for neovas-
171 Chung EJ, Lee H, Koh HJ: Arteriove- Oden NL, Blodi BA, Fisher M, Chan cular age-related macular degenera-
nous crossing sheathotomy versus in- CK, Gonzalez VH, Singerman LJ, To- tion. Ophthalmic Surg Lasers Imaging
travitreal triamcinolone acetonide in- lentino M; SCORE Study Research 2005;36:331–335.
jection for treatment of macular edema Group: A randomized trial comparing 188 Iturralde D, Spaide RF, Meyrele CB,
associated with branch retinal vein the efficacy and safety of intravitreal Klancnik JM, Yannuzzi LA, Fisher YL,
occlusion. Graefes Arch Clin Exp Oph- triamcinolone with standard care to Sorenson J, Slakter JS, Freund KB,
thalmol 2008;246:967–974. treat vision loss associated with macu- Cooney M, Fine HF: Intravitreal beva-
172 Park SP, Ahn JK: Changes of aqueous lar edema secondary to branch retinal cizumab (Avastin) treatment of macu-
vascular endothelial growth factor and vein occlusion: the Standard Care vs lar edema in central retinal vein occlu-
interleukin-6 after intravitreal triam- Corticosteroid for Retinal Vein Occlu- sion: a short-term study. Retina 2006;
cinolone for branch retinal vein occlu- sion (SCORE) study report 6. Arch 26:279–284.
sion. Clin Exp Ophthalmol 2008;36: Ophthalmol 2009;127:1115–1128.
831–835. 181 Wang L, Song H: Effects of repeated
injection of intravitreal triamcinolone
on macular oedema in central retinal
vein occlusion. Acta Ophthalmol 2009;
87:285–289.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 165
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
189 Jaissle GB, Ziemssen F, Petermeier K, 198 Wroblewski JJ, Wells JA 3rd, Adamis AP, 207 Costa RA, Jorge R, Calucci D, et al: In-
Szurman P, Ladewig M, Gelisken F, Buggage RR, Cunningham ET Jr, Gold- travitreal bevacizumab (avastin) for
Völker M, Holz FG, Bartz-Schmidt KU: baum M, Guyer DR, Katz B, Altaweel central and hemicentral retinal vein
Bevacizumab zur Therapie des MM; Pegaptanib in Central Retinal Vein occlusions: IBeVO study. Retina 2007;
sekundären Makulaödems nach Occlusion Study Group: Pegaptanib so- 27:141–149.
venösen Gefässverschlüssen. Ophthal- dium for macular edema secondary to 208 Ferrara DC, Koizumi H, Spaide RF:
mologe 2006;103:471–475. central retinal vein occlusion. Arch Oph- Early bevacizumab treatment of cen-
190 Rosenfeld PJ, Fung AE, Pulifito CA: thalmol 2009;127:374–380. tral retinal vein occlusion. Am J Oph-
Optical coherence tomography find- 199 Epstein DL, Algvere PV, von Wendt G, thalmol 2007;144:864–871.
ings after an intravitreal injection of Seregard S, Kvanta A: Bevacizumab for 209 Pai SA, Shetty R, Vijayan PB, et al:
bevacizumab (Avastin) for macular macular edema in central retinal vein Clinical, anatomic, and electrophysi-
edema from central retinal vein occlu- occlusion: a prospective, randomized, ologic evaluation following intravitreal
sion. Ophthalmic Surg Lasers Imaging double-masked clinical study. Oph- bevacizumab for macular edema in
2006;36:336–339. thalmology 2012;119:1184–1189. retinal vein occlusion. Am J Ophthal-
191 Spandau UH, Ihloff AK, Jonas JB: In- 200 Epstein DL, Algvere PV, von Wendt G, mol 2007;143:601–606.
travitreal bevacizumab treatment of Seregard S, Kvanta A: Benefit from 210 Ehlers JP, Decroos FC, Fekrat S: Intra-
macular oedema due to central retinal bevacizumab for macular edema in vitreal bevacizumab for macular ede-
vein occlusion. Acta Ophthalmol 2006; central retinal vein occlusion: twelve- ma secondary to branch retinal vein
84:555–556. month results of a prospective, ran- occlusion. Retina 2011;31:1856–1862.
192 Costa RA, Jorge R, Calucci D, Melo LA domized study. Ophthalmology 2012; 211 Brown DM, Campochiaro PA, Singh
Jr, Cardillo JA, Scott IU: Intravitreal 119:2587–2591. RP, Li Z, Gray S, Saroj N, Rundle AC,
bevacizumab (Avastin) for central and 201 Zhang H, Liu ZL, Sun P, Gu F: Intravit- Rubio RG, Murahashi WY; CRUISE
hemicentral retinal vein occlusions: real bevacizumab for treatment of Investigators: Ranibizumab for macu-
IBeVO study. Retina 2007;27:141–149. macular edema secondary to central lar edema following central retinal vein
193 Matsumoto Y, Freund KB, Peiretti E, retinal vein occlusion: eighteen-month occlusion: six-month primary end
Cooney MJ, Ferrara DC, Yannuzzi LA: results of a prospective trial. J Ocul point results of a phase III study. Oph-
Rebound macular edema following Pharmacol Ther 2011;27:615–621. thalmology 2010;117:1124–1133.
bevacizumab (Avastin) therapy for 202 Kriechbaum K, Michels S, Prager F, 212 Campochiaro PA, Brown DM, Awh
retinal venous occlusive disease. Retina Georgopoulos M, Funk M, Geitzenauer CC, Lee SY, Gray S, Saroj N, Murahashi
2007;27:426–431. W, Schmidt-Erfurth U: Intravitreal WY, Rubio RG: Sustained benefits
194 Rabena MD, Pieramici DJ, Castellarin Avastin for macular oedema secondary from ranibizumab for macular edema
AA, Nasir MA, Avery RL: Intravitreal to retinal vein occlusion: a prospective following central retinal vein occlu-
bevacizumab (Avastin) in the treat- study. Br J Ophthalmol 2008;92:518– sion: twelve-month outcomes of a
ment of macular edema secondary to 522. phase III study. Ophthalmology 2011;
branch retinal vein occlusion. Retina 203 Prager F, Michels S, Kriechbaum K, 118:2041–2049.
2007;27:419–425. Georgopoulos M, Funk M, Geitzenauer 213 Campochiaro PA, Sophie R, Pearlman
195 Campochiaro PA, Hafiz G, Shah SM, W, Polak K, Schmidt-Erfurth U: Intra- J, Brown DM, Boyer DS, Heier JS, Mar-
Nguyen QD, Ying H, Do DV, Quinlan vitreal bevacizumab (Avastin) for mac- cus DM, Feiner L, Patel A; RETAIN
E, Zimmer-Galler I, Haller JA, Solo- ular oedema secondary to retinal vein Study Group: Long-term outcomes in
mon SD, Sung JU, Hadi Y, Janjua KA, occlusion: 12-month results of a pro- patients with retinal vein occlusion
Jawed N, Choy DF, Arron JR: Ranibi- spective clinical trial. Br J Ophthalmol treated with ranibizumab: the RETAIN
zumab for macular edema due to reti- 2009;93:452–456. study. Ophthalmology 2014;121:209–
nal vein occlusions: implication of 204 Ding X, Li J, Hu X, Yu S, Pan J, Tang S: 219.
VEGF as a critical stimulator. Mol Prospective study of intravitreal triam- 214 Boyer D, Heier J, Brown DM, Clark
Ther 2008;16:791–799. cinolone acetonide versus bevacizum- WL, Vitti R, Berliner AJ, Groetzbach G,
196 Pieramici DJ, Rabena M, Castellarin ab for macular edema secondary to Zeitz O, Sandbrink R, Zhu X, Beck-
AA, Nasir M, See R, Norton T, Sanchez central retinal vein occlusion. Retina mann K, Haller JA: Vascular endothe-
A, Risard S, Avery RL: Ranibizumab 2011;31:838–845. lial growth factor Trap-Eye for macular
for the treatment of macular edema 205 Hikichi T, Higuchi M, Matsushita T, edema secondary to central retinal
associated with perfused central retinal Kosaka S, Matsushita R, Takami K, Oht- vein occlusion: six-month results of
vein occlusions. Ophthalmology 2008; suka H, Kitamei H, Shioya S: Two-year the phase 3 COPERNICUS study. Oph-
115:e47–e54. outcomes of intravitreal bevacizumab thalmology 2012;119:1024–1032.
197 Spaide RF, Chang LK, Klancnik JM, therapy for macular oedema secondary 215 Brown DM, Heier JS, Clark WL, Boyer
Yannuzzi LA, Sorenson J, Slakter JS, to branch retinal vein occlusion. Br J DS, Vitti R, Berliner AJ, Zeitz O, Sand-
Freund KB, Klein R: Prospective study Ophthalmol 2014;98:195–199. brink R, Zhu X, Haller JA: Intravitreal
of intravitreal ranibizumab as a treat- 206 Kriechbaum K, Michels S, Prager F, et aflibercept injection for macular ede-
ment for decreased visual acuity sec- al: Intravitreal avastin for macular oe- ma secondary to central retinal vein
ondary to central retinal vein occlu- dema secondary to retinal vein occlu- occlusion: 1-year results from the
sion. Am J Ophthalmol 2009;147: sion: a prospective study. Br J Ophthal- phase 3 COPERNICUS study. Am J
298–306. mol 2008;92:518–522. Ophthalmol 2013;155:429–437.
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
166 Jonas · Monés · Glacet-Bernard · Coscas
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
216 Holz FG, Roider J, Ogura Y, Korobel- 221 Glacet-Bernard A, Zourdani A, Mil- 226 Ramchandran RS, Fekrat S, Stinnett
nik JF, Simader C, Groetzbach G, Vitti houb M, Maraqua N, Coscas G, Sou- SS, Jaffe GJ: Fluocinolone acetonide
R, Berliner AJ, Hiemeyer F, Beckmann brane G: Effect of isovolemic hemodi- sustained drug delivery device for
K, Zeitz O, Sandbrink R: VEGF Trap- lution in central retinal vein occlusion. chronic central retinal vein occlusion:
Eye for macular oedema secondary to Graefes Arch Clin Exp Ophthalmol 12-month results. Am J Ophthalmol
central retinal vein occlusion: 6-month 2001;239:909–914. 2008;146:285–291.
results of the phase III GALILEO 222 Glacet-Bernard A, Atassi M, Fardeau 227 Otani A, Dorrell MI, Kinder K, Otero
study. Br J Ophthalmol 2013;97:278– C, Romanet JP, Tonini M, Conrath J, FJ, Schimmel P, Friedlander M: Rescue
284. Denis P, Mauget-Faÿsse M, Coscas G, of retinal degeneration by intravitreal-
217 Hansen LL, Wiek J, Schade M, Müller- Soubrane G, Souied E: Hemodilution ly injected adult bone marrow-derived
Stolzenburg N, Wiederholt M: Effect therapy using automated erythrocy- lineage-negative hematopoietic stem
and compatibility of isovolaemic hae- tapheresis in central retinal vein occlu- cells. J Clin Invest 2004;114:765–774.
modilution in the treatment of isch- sion: results of a multicenter random- 228 Harris JR, Brown GA, Jorgensen M,
aemic and non-ischaemic central reti- ized controlled study. Graefes Arch Kaushal S, Ellis EA, Grant MB, Scott
nal vein occlusion. Ophthalmologica Clin Exp Ophthalmol 2011;249:505– EW: Bone marrow-derived cells home
1989;199:90–99. 512. to and regenerate retinal pigment epi-
218 Hansen LL, Wiek J, Wiederholt M: A 223 McIntosh RL, Mohamed Q, Saw SM, thelium after injury. Invest Ophthal-
randomised prospective study of treat- Wong TY: Interventions for branch mol Vis Sci 2006;47:2108–2113.
ment of non-ischaemic central retinal retinal vein occlusion: an evidence- 229 Smith LE: Bone marrow-derived stem
vein occlusion by isovolaemic haemo- based systematic review. Ophthalmol- cells preserve cone vision in retinitis
dilution. Br J Ophthalmol 1989;73: ogy 2007;114:835–854. pigmentosa. J Clin Invest 2006;114:
895–899. 224 Kuppermann BD, Blumenkranz MS, 755–757.
219 Wolf S, Arend O, Bertram B, Remky A, Haller JA, Williams GA, Weinberg DV, 230 Jonas JB, Witzens-Harig M, Arseniev
Schulte K, Wald KJ, Reim M: Hemodi- Chou C, Whitcup SM; Dexamethasone L, Ho AD: Intravitreal autologous bone
lution therapy in central retinal vein DDS Phase II Study Group: Random- marrow derived mononuclear cell
occlusion. One-year results of a pro- ized controlled study of an intravitre- transplantation: a feasibility report.
spective randomized study. Graefes ous dexamethasone drug delivery sys- Acta Ophthalmol 2008;86:225–226.
Arch Clin Exp Ophthalmol 1994;232: tem in patients with persistent macular 231 Jonas JB, Witzens-Harig M, Arseniev
33–39. edema. Arch Ophthalmol 2007;125: L, Ho AD: Intravitreal autologous bo-
220 Hattenbach LO, Wellermann G, 309–317. nemarrow-derived mononuclear cell
Steinkamp GW, Scharrer I, Koch FH, 225 Williams GA, Haller JA, Kuppermann transplantation. Acta Ophthalmol
Ohrloff C: Visual outcome after treat- BD, Blumenkranz MS, Weinberg DV, 2010;88:e131–e132.
ment with low-dose recombinant tis- Chou C, Whitcup SM; Dexamethasone 232 Ma K, Xu L, Zhang H, Zhang S, Pu M,
sue plasminogen activator or hemodi- DDS Phase II Study Group: Dexameth- Jonas JB: Effect of brimonidine on reti-
lution in ischemic central retinal vein asone posterior-segment drug delivery nal ganglion cell survival in an optic
occlusion. Ophthalmologica 1999; system in the treatment of macular nerve crush model. Am J Ophthalmol
2136:360–366. edema resulting from uveitis or Irvine- 2009;147:326–331.
Gass syndrome. Am J Ophthalmol
2009;1476:1048–1054.
Prof. Jost B. Jonas
Universitäts-Augenklinik
Theodor-Kutzer-Ufer 1–3
DE–68167 Mannheim (Germany)
E-Mail jost.jonas @ medma.uni-heidelberg.de
132.239.1.231 - 3/31/2017 6:24:44 PM
Univ. of California San Diego
Retinal Vein Occlusions 167
Downloaded by:
Coscas G (ed): Macular Edema. 2nd, revised and extended edition.
Dev Ophthalmol. Basel, Karger, 2017, vol 58, pp 139–167 (DOI: 10.1159/000455278)
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5819)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Last Time I Wore A Dress Paper PDFDocument8 pagesThe Last Time I Wore A Dress Paper PDFapi-490648327No ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Real Man EssayDocument14 pagesReal Man EssayAnonymous TaiMB7No ratings yet
- 31chiense Body ClockDocument6 pages31chiense Body ClockDrHitaishi SinghNo ratings yet
- ENT300 - Final Project - Fresh Chicken FarmDocument163 pagesENT300 - Final Project - Fresh Chicken FarmamirhazieqNo ratings yet
- Drug InteractionDocument151 pagesDrug Interactionapi-3724213100% (1)
- Cosmetic Surgery in Manchester by Dr. Deemesh Oudit PDFDocument5 pagesCosmetic Surgery in Manchester by Dr. Deemesh Oudit PDFDeemesh ouditNo ratings yet
- Confidentiality in Pharmacy PracticeDocument20 pagesConfidentiality in Pharmacy PracticeGeorge John AmegashieNo ratings yet
- Janapriyavaidyap PDFDocument127 pagesJanapriyavaidyap PDFBala Kiran GaddamNo ratings yet
- Book 15 Jan 2024Document1 pageBook 15 Jan 2024Karan SinghNo ratings yet
- ILL Livestock VaccinesDocument19 pagesILL Livestock VaccinesKrushna Mohan BeuraNo ratings yet
- FibroadenomaDocument11 pagesFibroadenomaAimanazrul ZainudinNo ratings yet
- Core Exercises 5 Workouts To Tighten Your Abs, Strengthen Your Back, and Improve Balance (Lauren E. Elson MD, Michele Stanten Etc.)Document54 pagesCore Exercises 5 Workouts To Tighten Your Abs, Strengthen Your Back, and Improve Balance (Lauren E. Elson MD, Michele Stanten Etc.)HeyitzmeNo ratings yet
- Mayapada Hospital - Medical Personnel - CS LinDocument76 pagesMayapada Hospital - Medical Personnel - CS Linjansen siahaanNo ratings yet
- Foods To Eat and AvoidDocument1 pageFoods To Eat and AvoidVijay GopalanNo ratings yet
- Nursing Mnemonics: Everything Made EASY Part 2: MemoryDocument5 pagesNursing Mnemonics: Everything Made EASY Part 2: MemoryCrystal Ann Monsale TadiamonNo ratings yet
- Missed Monteggia FXDocument16 pagesMissed Monteggia FXEric RothNo ratings yet
- Lymph Drainage For DetoxificationDocument8 pagesLymph Drainage For DetoxificationJay JonesNo ratings yet
- Nursing Sample Task 03 Peter DunbarDocument2 pagesNursing Sample Task 03 Peter DunbarDiana Hazel Delos ReyesNo ratings yet
- Asthma 4th Ed - T. Clark (Arnold, 2000) WWDocument493 pagesAsthma 4th Ed - T. Clark (Arnold, 2000) WWGeorge DanilaNo ratings yet
- 1 s2.0 S209379112300063X MainDocument8 pages1 s2.0 S209379112300063X Mainshoshanasingh52No ratings yet
- Mitochondrial DisorderDocument55 pagesMitochondrial DisorderRaja DarmawanNo ratings yet
- Community Organizing Participatory Action ResearchDocument29 pagesCommunity Organizing Participatory Action ResearchNoreen PadillaNo ratings yet
- CHOLELITHIASISDocument3 pagesCHOLELITHIASISMontero, Ma. Cecilia - BSN 3-BNo ratings yet
- Scripture Against CancerDocument7 pagesScripture Against CancerENIOLA TOSINNo ratings yet
- Human Performance QuestionaireDocument139 pagesHuman Performance Questionaireचंदन सिन्हा100% (1)
- PLAGUE: Medical Management and Countermeasure Development.Document52 pagesPLAGUE: Medical Management and Countermeasure Development.Dmitri PopovNo ratings yet
- Module 3 ACCTG 1 A & B Partnership & CorporationDocument32 pagesModule 3 ACCTG 1 A & B Partnership & CorporationMary Lynn Dela PeñaNo ratings yet
- Pycnogenol Consumer/Patient Information SheetDocument1 pagePycnogenol Consumer/Patient Information SheetDeboraNainggolanNo ratings yet
- Costochondritis RoleplayDocument2 pagesCostochondritis Roleplayxx leeNo ratings yet
- (Paper) Prevalence of an inflammation & necrosis syndrome in suckling piglets - 2019年Document11 pages(Paper) Prevalence of an inflammation & necrosis syndrome in suckling piglets - 2019年Matthew HsuNo ratings yet