Professional Documents
Culture Documents
Procrsmed00155 0018
Procrsmed00155 0018
Uploaded by
Tharun kumar0 ratings0% found this document useful (0 votes)
9 views2 pagescauses for proptosis
Original Title
procrsmed00155-0018
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentcauses for proptosis
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views2 pagesProcrsmed00155 0018
Procrsmed00155 0018
Uploaded by
Tharun kumarcauses for proptosis
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 2
544 Proc. roy. Soc. Med.
Volume 61 June 1968 20
with bilateral open angle glaucoma but unilateral this it is not difficult to make a diagnosis
pseudo-exfoliation, and showed that the eye with of renal retinopathy and the patient is referred
pseudo-exfoliation fared worse. to the appropriate medical team. The team may,
however, have difficult questions to put to the
Pigmentary glaucoma: One subject, the mother of ophthalmologist. For example: What is the
the index patient, was examined; both had myopic visual prognosis for this patient? In view of his
right eyes with tension consistently higher than occupation is it reasonable to dialyse the patient
in the emmetropic left eyes. The mother's tensions in the acute phase of the illness? Alternatively, is
were borderline in the left eye and PO/C ratios it justifiable for him to take up a place in the
were 200 in the right eye and 114 in the left. There chronic dialysis unit, or to have a mini-kidney
were slight pigment deposits in the angles. After that he can work himself at home, or should he
treatment of the left eye with dexamethasone be considered for a cadaver graft?
0-1 % eyedrops twice daily for three weeks there The following cases illustrate these problems:
was a rise in pressure of 12 mm. The discs were
suspicious but there were no definite field defects. Case 1 Mr H, aged 32. Lorry driver
Open angle glaucoma was suspected. First seen by an ophthalmologist on a domiciliary
Becker & Podos (1966) record instances of visit. Vision in both eyes limited to counting fingers;
open angle glaucoma, pigmentary glaucoma, lower fundi showed gross renal retinopathy with bilateral
Krukenberg's spindles and glaucoma suspects serous detachments of the retine.
On admission: Blood urea 300 mg/100 ml; blood
occurring in the same family. pressure 230/135.
18.10.66: Transferred to King's College Hospital for
Conclusions dialysis.
Evidence is presented showing a connexion Investigations: Blood urea 640 mg/100 ml; blood
between: (1) Open-angle glaucoma and low- pressure: 140/100; Hb 46%.
tension glaucoma. (2) Glaucoma capsulare and Peritoneal dialysis was started and his blood urea
pigmentary glaucoma. (3) Pigmentary glaucoma came down to 130 mg/100 ml. He was difficult to
and open-angle glaucoma. An explanation for stabilize on dialysis. 27.10.66: Renal biopsy sbowed a
these connexions would be a genetically deter- sclerosis. completely nonfunctioning kidney due to hypertensive
mined tendency to glaucoma common to all the Three weeks after admission he had recovered to an
conditions mentioned above. extent where he could walk round the ward, being
maintained on peritoneal dialysis each night. During
Acknowledgment: I am grateful to Professor E S this time there was an increase in the size and number
Perkins and Dr J Gloster for their help in the of himorrhages in his fundi, and a very guarded
preparation of this paper. prognosis about his future visual function, which at
this time was N. 48, was given. Six weeks after
REFERENCES admission his fundi showed no decrease in the soft
Becker B, Kolker A E & Roth F D white exudates and an increase in hemorrhages, and
(1960) Amer. J. Ophthal. 50, 557 two weeks after this he died in (left-sided) cardiac
Becker B & Podos S M (1966) Arch. Ophthal. 76, 635
Miller S J U& Paterson G D (1962) Brit. J. Ophthal. 46, 513 failure.
Tarkkanen A
(1962) Acta ophthal. (Kbh.) Suppl. 71, pp 61, 62
(1965) Acta ophthal. (Kbh.) 43, 514 Case 2 MrAK, aged 28
Waardenburg P J, Franceschetti A & Klein D A known case of Marfan's syndrome with severe
(1961) Genetics and Ophthalmology. Assen; 1, 625
hypertension due to renal damage. His fundi were
similar to those of Case 1. He also had large lower
serous detachments and very cedematous fundi with
soft exudates but no himorrhages.
On admission: Blood pressure 220/140; blood urea
530 mg/100 ml.
Visual Prognosis in Renal Failure Treatment: Peritoneal dialysis was commenced and
blood urea rapidly returned to normal; blood pressure
by C C Cory MB was controlled on methyldopa. Renal biopsy showed
(King's College Hospital, London) chronic glomerulonephritis with what was assumed to
be nonfunctioning kidneys. He was considered un-
With the introduction of the artificial kidney, suitable for sending to a chronic dialysis centre in
peritoneal dialysis and transplantation of the view of the scarcity of places available and his known
disabilities.
kidney, a new problem, the visual prognosis in On Christmas Eve dialysis was discontinued but by
renal failure, faces the ophthalmologist. New Year's Eve he was producing considerable
When seen in the acute stage of renal failure, quantities of urine. Blood urea was reduced to
the first symptom reported by the patient is 34 mg/100 ml and the appearances of his fundi had
sometimes a deterioration of vision. From improved.
21 Section of Ophthalmology 545
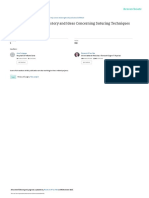
Ellis & Fonken (1966) found that fundus Case 1 Man, aged 38 (Fig 1)
changes resolve if the graft is successful although Presented with left-sided proptosis of 3 mm in upward
they comment that after severe cedema they may and inward direction. A mass was just palpable in the
have some macular scarring which may lead to a lower quadrant of the orbit. An encapsulated tumour,
deterioration of vision. This improvement is which proved to be a neurilemmoma, was removed
similar to that of a gross hypertensive retinopathy via an anterior orbitotomy. He has since remained
symptom-free.
due to a pheochromocytoma. When the tumour
is removed and the blood pressure returns to
normal the fundus reverts to a normal appear- Case 2 Man, aged 36
ance. In toxaemia of pregnancy the same Presented with left frontal headache and diplopia in
the straight-ahead position for three weeks. Twelve
improvement may occur. years previously he had sustained a fracture of the
The answer, therefore, that we should give to orbital plate of the left frontal bone involving the
the renal team is: 'You resolve the renal function sinus. An irreducible left-sided proptosis of 6 mm was
and the eyes will resolve themselves.' present, the greatest displacement being downwards
and laterally. A mass was palpable in the upper inner
REFERENCE angle of the orbit. Compression lines were noted at
Ellis P P & Fonken H A (1966) Arch. Ophthal. 75, 36
the posterior pole on fundus examination. Skull
X-ray showed a defect of the upper inner angle of the
orbit. Mucocele arising from the left frontal sinus was
diagnosed. Following orbital exploration by a neuro-
surgeon a fronto-ethmoidal mucocele was removed.
Three months later, after an upper respiratory tract
infection, proptosis recurred and subsided after a few
days without treatment. Since then there have been
Unilateral Proptosis several recurrences associated with nasal congestion
and subsiding with the use of nasal decongestants. He
by Surgeon Lt-Commander now shows restriction of dextro-elevation of the left
A J Rintoul MB DO eye possibly due to tethering of the left superior
(Royal Naval Hospital, Haslar) oblique muscle by scar tissue.
Nine cases of unilateral proptosis have been Case 3 Man, aged 33
seen in the Eye Department of the Royal Naval Presented with right-sided proptosis of two weeks'
Hospital at Haslar during a period of eighteen duration with forward, downward and outward dis-
months. These have been diagnosed as 5 cases placement of 3 mm. No localized mass was palpable
of dysthyroid eye disease, 1 pseudotumour, 1 but a leash of dilated conjunctival blood vessels was
tumour, 1 mucocele and 1 inflammatory. The seen at the outer canthus and restricted elevation was
place of dysthyroid eye disease at the head of the present. Lid lag and lid retraction were noted in the
list is the same as in the series published by left eye.
Clinical investigations, including thyroid function
Drescher & Benedict (1950), Schultz et al. (1961), studies, orbital phlebogram and carotid angiogram,
Reese (1964) and Catalino et al. (1964). were normal. It was then thought that the proptosis
Four of the cases at Haslar were treated by might be of endocrine origin and, in the absence of
surgical intervention but in only one of these has visual loss, a period of observation seemed reasonable
there been an absence of sequelh. In this case the before exposing him to intra-orbital surgery. For four
approach was an anterior one through the orbital months his condition remained unchanged; then the
septum. The other 3 cases illustrate the difficulties forward proptosis increased to 6 mm and vision
in the management of intra-orbital disease. dropped to 6/12. By this time fundus examination
showed venous congestion and papilleedema and it
was felt that surgical decompression was indicated.
_
::
-
-
'
::
.er
e
!:
:i
.:
:i
.
::
i .
!:'
-
!
;:::
:::
::
::::
::::
.:::
Operation was performed by a neurosurgeon via the
.@ioaZ'°-E§°~~~~~~~~~~~~~~~~.
transfrontal approach and an attempt was made to
, ^
remove an infiltrating retro-orbital mass. This left him
with a blind eye, a fixed dilated pupil and optic
atrophy. Expert opinion on histological appearance
is divided between inflammatory pseudotumour and
lymphosarcoma. A course of radiotherapy has been
given and he has since remained well.
Case 4 Man, aged 21 (Fig 2)
Presented with a right proptosis of ten days' duration,
coincident diplopia and a blocked right nostril. The
Fig 1 Case 1, left proptosis Mass in lower temporal left eye showed lid lag and lid retraction. Two years
quadrant previously he had had subtotal thyroidectomy for
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5811)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Navy Seal DisciplineDocument46 pagesNavy Seal DisciplineEddy Muñoz93% (15)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Attitude PPT 1Document16 pagesAttitude PPT 1CANAN HART REGO SDM COLLEGE OF BUSINESS MANAGEMENT POST GRADUATE CENTRE50% (2)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Chicken's MoltingDocument11 pagesChicken's MoltingKhaira Fani100% (1)
- Bhavabhuti - Rama's Last Act (Clay Sanskrit Library) (2007) PDFDocument458 pagesBhavabhuti - Rama's Last Act (Clay Sanskrit Library) (2007) PDFTharun kumar100% (1)
- Griffith Theory of Brittle Fracture, Modifiction of Griffith Theory and FractographyDocument16 pagesGriffith Theory of Brittle Fracture, Modifiction of Griffith Theory and Fractographyyuvi yuviNo ratings yet
- Jikiden7 3Document9 pagesJikiden7 3Manojkumar NairNo ratings yet
- An Ideal Christian HomeDocument5 pagesAn Ideal Christian HomeJane AgantemNo ratings yet
- Factors Affecting Quality of Nursing CareDocument16 pagesFactors Affecting Quality of Nursing CareSathish Rajamani75% (12)
- Auma Control Valve ManualDocument20 pagesAuma Control Valve ManualAnto ThoppilNo ratings yet
- DNA BarcodingDocument29 pagesDNA Barcodingmcdonald212No ratings yet
- The Medical Detectives PDFDocument3 pagesThe Medical Detectives PDFTharun kumarNo ratings yet
- Motorcycle DiariesDocument5 pagesMotorcycle DiariesTharun kumarNo ratings yet
- From Ants To Staples: History and Ideas Concerning Suturing TechniquesDocument9 pagesFrom Ants To Staples: History and Ideas Concerning Suturing TechniquesTharun kumarNo ratings yet
- Atalan1999 ADocument4 pagesAtalan1999 AMario NúñezNo ratings yet
- Writing 3 EssayDocument2 pagesWriting 3 EssayKarinaNo ratings yet
- T-Rex ST50-11&ST125-11Document40 pagesT-Rex ST50-11&ST125-11autopart39No ratings yet
- Chapter 6 AggregatesDocument10 pagesChapter 6 AggregatesShinwari SabNo ratings yet
- U.S. Supreme Court Draft Opinion Overturning Roe v. WadeDocument98 pagesU.S. Supreme Court Draft Opinion Overturning Roe v. WadeMichael_Roberts2019No ratings yet
- Risk Assessment and Disaster Management Plan in Chasnala Coal MineDocument6 pagesRisk Assessment and Disaster Management Plan in Chasnala Coal MineIJSTENo ratings yet
- BDRMMC2021-2023 (AutoRecovered)Document16 pagesBDRMMC2021-2023 (AutoRecovered)Marra cielo OcayNo ratings yet
- Comparison Table For Tubes, Line Pipes and FittingDocument2 pagesComparison Table For Tubes, Line Pipes and FittingNamye Yelus100% (1)
- Paes 141 - Weeder - SpecsDocument11 pagesPaes 141 - Weeder - SpecsAlgin Real MagmanlacNo ratings yet
- 3D BioprintingDocument8 pages3D BioprintingCarooNo ratings yet
- Chapter 9 Section 1 SciDocument3 pagesChapter 9 Section 1 SciThere is only 2 Genders100% (1)
- CalisthenicsDocument3 pagesCalisthenicsoikNo ratings yet
- Operation Manual: Beveling and Deburring Device B5Document13 pagesOperation Manual: Beveling and Deburring Device B5bulentNo ratings yet
- The Pittston Dispatch 05-08-2011Document80 pagesThe Pittston Dispatch 05-08-2011The Times LeaderNo ratings yet
- The Physical Self: I. The Self As Impacted by The BodyDocument2 pagesThe Physical Self: I. The Self As Impacted by The BodyJoanne LazaNo ratings yet
- GS80 Parts ManualDocument248 pagesGS80 Parts ManualUbaldo Enrique Caraballo EstradaNo ratings yet
- SDC ManualDocument7 pagesSDC ManualfjserranogNo ratings yet
- Technical Sheet (Model YAF-14S)Document1 pageTechnical Sheet (Model YAF-14S)Zainab Abizer MerchantNo ratings yet
- Chapter 4: Functional Anatomy of Prokaryotic and Eukaryotic CellsDocument94 pagesChapter 4: Functional Anatomy of Prokaryotic and Eukaryotic CellsTrevannie EdwardsNo ratings yet
- Skills in Clinical Nursing 8Th Edition Berman Test Bank Full Chapter PDFDocument17 pagesSkills in Clinical Nursing 8Th Edition Berman Test Bank Full Chapter PDFcarolyn.mullen927100% (16)