Professional Documents
Culture Documents
Respiratory Physiology Lab
Uploaded by
SLU MED 1-cCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Respiratory Physiology Lab
Uploaded by
SLU MED 1-cCopyright:
Available Formats
Saint Louis University
School of Medicine PHYSIOLOGY LAB
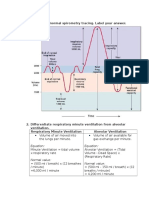
3. What happens to FRC, ERV, IRV, and VC when a person lies
F.01 Respiratory Physiology supine from a standing position? Why?
Expiratory Reserve Decrease
OUTLINE Volume
I. Spirometry: Lung capacities and volumes
Functional Residual Decrease
II. Respiratory Calculations: Lung volumes, dead
Capacity
space and alveolar ventilation
III. Measurement of Peak Expiratory Flow Rate
IV. Examination of Chest and Lungs Inspiratory Reserve Increase
V. Case 1 Volume
VI. Case 2
VII. Case 3 Vital Capacity Decrease
Total Lung Capacity Decrease
I. SPIROMETRY: LUNG CAPACITIES AND VOLUMES Functional residual capacity decreases as a result of a decrease in the
expiratory reserve volume, compared to an erect position. However,
Spirometry is a basic pulmonary function test which measures the
the decrease in the functional residual capacity results in an increase in
amount of air inspired and expired.
the inspiratory reserve volume. Since the venous return to the thorax
● Detecting lung diseases
increases in supine position, the vital capacity and the total lung
● Determining the degree of impairment
capacity may decrease.
● Monitoring the effects of environmental and occupational
exposure II. RESPIRATORY CALCULATIONS: LUNG VOLUMES,
● Determining the effects of medication DEAD SPACE AND ALVEOLAR VENTILATION
1. Diagram the pulmonary volumes and capacities and label
the following: RV, IRV, TLC, TV, ERV, FRC, VC and IC. 1. Using the information provided in figure 1-1, what are the
values for the tidal volume, inspiratory capacity, expiratory
reserve volume, functional residual capacity, vital capacity,
and total lung capacity?
2. Draw the flow volume loop of the following: Tidal Volume 500ml
Inspiratory Capacity 3500ml
Expiratory Reserve Volume 1000ml
Functional Residual 2500ml
Capacity
Vital Capacity 4500ml
Total Lung Capacity 6000ml
2. What is the name of the volume remaining in the lungs
after maximal expiration that is not measurable by
spirometry? What other lung volumes or capacities are not
measurable by spirometry?
The volume that remains in the lungs after maximal expiration and
Obstructive Respiratory Defect - sigmoid curve (hard expiration)
cannot be measured by spirometry is residual volume (RV). The
Restrictive Respiratory Defects - similar as normal but small flow
other lung volumes that are not measurable by spirometry are
volume loop (minimal inhalation)
PHYSIOLOGY LABORATORY 1 of 6 [Block B]
Saint Louis University
School of Medicine PHYSIOLOGY LAB
Functional residual capacity (FRC) and total lung capacity
(TLC) because they already contain residual volume. b. Crackles: is also known as “rales” or “crepitation” and is more
commonly heard on inspiration rather than on exhalation. Crackles is
3. Define and differentiate anatomic dead space, alveolar dead the snapping, rattling or clicking sound heard on auscultation as a
space and physiologic dead space? result of fluid build-up in the interstitium or the pleura of the lungs.
Disease states such as congestive heart failure, pleural effusion and
Alveolar dead space is sum of the volumes of those alveoli which emphysema are the common conditions wherein crackles are heard.
have little or no blood flowing through their adjacent pulmonary
capillaries. An example is an alveolus that is ventilated but not 3. What is egophony?
perfused, as a result, no gas exchange can occur. Alveolar dead space Egophony is a transmitted voice sound generated by the larynx that
is negligible in healthy individuals but can increase dramatically in causes modification of the voice resembling the “bleating of a goat”
some lung diseases due to ventilation perfusion mismatch. that is heard upon auscultation. Egophony is commonly heard with
patients having pleurisy with effusion.
Anatomical dead space is the volume of the conducting airways Clinicians usually elicit the finding by having the patient vocalize the
(150-250mL). It is the portion of the airways which conducts gas to long vowel “EE” and then listening for the abnormal transformation of
alveoli. No gas exchange is possible in the spaces. In healthy lungs the sound into a loud nasal “AH” (the “AH” sound ranges from the “a”
where the alveolar dead space is small, anatomical dead space is of the word hat to the “a” of the word cart; this finding is sometimes
constant regardless of circulation. called E-to-A change). Although all vowel sounds are altered by the
lung (even healthy lung), what makes egophony distinctive is the
Physiological dead space is the part of the tidal volume which does intensity of the change and the suddenness with which it appears over
not participate in gas exchange. a small area on one side of the chest. Therefore, before concluding a
III. MEASUREMENT OF PEAK EXPIRATORY FLOW patient has egophony, the clinician should confirm that a similar
change of sound is absent over the identical location of the opposite
RATE
chest.
1. What is peak expiratory flow rate?
Peak expiratory flow rate or PEFR is greatest flow rate achieved V. CASE 1
during the expiratory maneuver. This is among the three main
Nene is a 37-year-old call center agent. She is a known asthmatic
pulmonary function tests in creating a flow-volume loop; the other two
since childhood. She is married to Noynoy who is a heavy smoker with
includes the FVC and expiratory flow rates.
whom she has 3 children aged 4, 7 and 10. Her maintenance
medications are Salmeterol Fluticasone (Seretide) and Salbutamol MDI
2. Discuss the advantage of PEFR monitoring and mention
as needed. However, Nene's compliance to Seretide is poor and she
clinical conditions where it is useful?
relies only on her Salbutamol inhaler for exacerbations. 3 days ago,
Measuring the maximum speed expiration of the patient is important
she developed low grade fever, colds and general body malaise. This
for the physician to monitor and determine the functionality of the
was followed by dyspnea and nocturnal wheezing. Patient did not seek
lungs, severity of asthma symptoms. This can also be used for creating
consult but instead self-medicated with salbutamol nebulization. The
asthma management plans. This is used to distinguish the condition of
condition worsened now with noted chest tightness and dyspnea even
the patient based on the result; if the peak flow is high the patient is
at rest. She was rushed to the emergency room. Initial physical
well on the other hand when the patient has low reading it is indicated
examination revealed BP 140/90, CR 114/min, RR 32/min with noted
that his airways are constricted.
use of accessory muscles of inspiration. Chest and Lung examination
According to the American Lung Association, peak flow readings are
revealed intercostals and subcostal retractions with diffuse wheeze and
classified into 3 zones. The green zone indicates respiratory is under
tight air entry. ABG revealed the following results: pH of 7.48, pCO2 35
good control, yellow zone indicates the respiratory airways are
mmHg, HCO3 22, paO2 52mmHg, FiO2 0.21.
narrowing and additional medication may be required, red zone
indicates medical emergency, severe airway narrowing and involves
Questions:
contacting a doctor.
1. What is the expected spirometry result for Bronchial
IV. EXAMINATION OF CHEST AND LUNGS Asthma? Based on the patient's spirometry results, what
parameters denote presence of obstructive airway disease?
1. What happens to the vibration, percussion note, and breath What parameters denote reversibility? Explain
sounds if there were: a) What is the expected spirometry result for Bronchial Asthma
• < 70% FEV₁/FVC
Percussion Breath • Reversible
Vibration
note sounds • FEV₁ increased by 12% and 200 ml (after nebulization)
A. Air in the b) Based on the patient's spirometry results, what parameters denote
Hyperresonance Hyperresonance Diminished
pleural cavity presence of obstructive airway disease?
• < 70% FEV₁/FVC
B. Fluid in • Irreversible: permanent destruction
Decreased Dullness Diminished
pleural cavity • FEV₁ does NOT improve by 12% and 200 ml (after
nebulization)
C. • No period of normalcy
Solidification • Destruction of airways due to cigarettes and exposure
Increased Dullness Diminished to biomass fuels
of lung
segment
c) What parameters denote reversibility?
2. When do you hear the following adventitious sounds? A significant rise in FEV1 is diagnostic for asthma, which is reversible,
a. Wheeze: wheezing denotes airway obstruction such that there is after the intake of bronchodilator like Salbutamol. If FEV1 has not risen
narrowed passage for air and so on exhalation, a sound is produced. significantly after the intake of the bronchodilator, the obstruction is
Airway obstruction diseases such as bronchial asthma, chronic likely to be irreversible and caused by abnormality (like COPD) and
obstructive pulmonary disease, pertussis, aspiration and laryngeal or other tests will be necessary to make a definite diagnosis.
tracheal tumors are the most common causes of wheezing.
PHYSIOLOGY LABORATORY 2 of 6 [Block B]
Saint Louis University
School of Medicine PHYSIOLOGY LAB
4. Interpret initial ABG results. Explain the reason behind the
2. What lung volumes and capacities are affected in bronchial abnormality. What abnormality should be the foremost
asthma? Compare these changes to normal PFT consideration in making corrections?
In bronchial asthma, the airways become narrowed and results
in difficulty in inspiration and expiration. Since the negative PARAMETER ABG RESULTS NORMAL INTERPRETATION
intrathoracic pressure during inspiration aids to maintain the airways VALUES
open during inspiration, the impact of the disease is greater during
expiration than during inspiration. This causes trapping of air inside pH 7.48 7.35-7.45 High
the lungs causing the residual volume and hence the functional
residual capacity to be increased. The inspiratory reserve volume is
pCO2 35 mmHg 35-45 Normal
relatively constant, but the expiratory reserve volume tends to
decrease. mmHg
Residual Volume Increase paO2 52 mmHg 80-100 Low
mmHg
Functional Increase
Residual Capacity HCO3 22 meq/L 22-26 meq/L Normal
Inspiratory Relatively Constant
Reserve Volume
The result of the patient’s ABG would conclude respiratory alkalosis,
Expiratory Decrease uncompensated with hypoxemia.
Reserve Volume
Bronchoconstriction caused by the bronchial asthma of the patient
limits the oxygen levels in the blood thus also limiting the oxygen
3. Define “work of breathing”. What are the factors that affect supply to the tissues. This would result to the compensatory response
work of breathing? List and explain all the clinical which is to increase the respiratory rate so as to increase also the
manifestations of Nene that shows alteration of the work of oxygen supply. However, hyperventilation would increase the excretion
breathing. of CO2 thus decreasing the pCO2 levels of the patient and eventually
leading to increased pH due to decreased carbonic acid generation and
Work of breathing is the defined as the work required to overcome relatively increased bicarbonate levels.
the inherent mechanical properties of the lungs, such as elastic and
force-resistive forces, and to move both the lungs and the thoracic The decreased pCO2 should be addressed first so at to bring back the
wall. other values to normal which is necessary for optimum oxygenation.
Breathing into a paper bag during acute attacks limits the escape of
● Factors affecting the work of breathing include: CO2 and allows re-inhalation of it back to the lungs. Returning the
pCO2 back to its normal value would then allow carbonic acid
1. Compliance: the ability of the lungs to distend during respiration is generation through the enzyme carbonic anhydrase found in the lungs
one of the major contributing factors to the work of breathing such thus decreasing the pH back to its normal value.
that decreased compliance, in instances such as in fibrosis and
decreased surfactant levels in the lungs, there is increased work of
breathing. VI. CASE 2
1.What is the most likely predisposing factor to Noynoy’s
2. Resistance from other tissues, such as in the case of increased condition? Explain how this leads to his present illness.
pulmonary venous pressure due to drowning, increases the work of
breathing. Noynoy has been a smoker since he was 15 years old, thus we can
identify smoking as the major predisposing factor in his condition. The
3. In disease states, such as bronchial asthma and chronic accumulation of the components of a cigarette, specifically nicotine
obstructive pulmonary disease where there is increased oxygen and carbon dioxide, in the respiratory epithelium adversely affects the
demand but decreased oxygen supply, the work of breathing increases sweeping (of foreign particles) function of the epithelium that serves to
so as to compensate for the low oxygen levels in the blood and in the clear and protect the airways. This will then cause irritation and will
tissues. manifest as cough. In cases of chronic irritation the respiratory
epithelium is converted into a stratified squamous epithelium through
● Manifestations of the patient: the process of metastatic metaplasia. The dyspnea experienced by
Noynoy can be attributed to the large air pockets (bullae) formed
1. Nocturnal wheezing: bronchoconstriction brought about by her
due to the severe destruction of small airways. These bullae replace
bronchial asthma, decreases the diameter of the passageway for air
the lung tissues. The breakdown of the lung tissue (emphysema)
flow thus creating a sound upon exhalation.
results to a poor airflow and small airway disease known as
2. Tachypnea: increase in the respiratory rate is the body’s response obstructive bronchiolitis, causing his inability to breathe out air
to decreased oxygen levels in the body such that the lungs fully. His lethargy and drowsiness may be attributed to the
compensate by increasing the frequency of respiration so as to meet resulting little amount of oxygen and high amount of carbon
the oxygen demand. dioxide that entered his brain.
3. Dyspnea and chest pain: the primary muscles of respiration 2. Interpret the spirometry results of Noynoy. What are the
would be overused and therefore exhaust causing pain and difficulty of criteria for diagnosing his disease? Differentiate this from a
breathing. This would then trigger the body to recruit accessory spirometry of a bronchial asthma patient like Nene.
muscles of respiration so as to help in the ventilation.
PHYSIOLOGY LABORATORY 3 of 6 [Block B]
Saint Louis University
School of Medicine PHYSIOLOGY LAB
The spirometry results of Noynoy are noted to be significantly respiratory rate during exercise, result in a progressive increase in
diminished. The diminished FEV1 indicates that there is an increased FRC. This phenomenon is called dynamic hyperinflation and is largely
airway resistance to expiratory flow. The low FVC, on the other hand, responsible for exercise limitation in COPD.
denotes that there is a premature closure of airway during expiration. B. PURSED LIP BREATHING
The following are the criteria for diagnosing his disease: Ventilatory muscle dysfunction A number of factors contribute to
ventilatory muscle dysfunction in COPD. A major factor is a
● FORCED VITAL CAPACITY (FVC)- The most basic maneuver in consequence of hyperinflation, which limits force generation and
spirometry; volume of air that can forcibly be blown out after full endurance, and places the inspiratory muscles at a mechanical
inspiration. disadvantage. Other factors include nutritional alterations, a sustained
● FORCED EXPIRATORY VOLUME IN 1 SECOND (FEV1) - The inflammatory response that affects the contractile apparatus, tissue
volume of air that can forcibly be blown out in one second, after full hypoxia, and loss of muscle mass.These factors also affect other
inspiration. skeletal muscles, which may further contribute to exercise limitation
● FEV1/FVC ratio (FEV1%)- The ratio of FEV1 to FVC. C. NECK VEIN ENGORGEMENT AND BIPEDAL EDEMA
○ Healthy adults: approximately 70–85% (declining with age) Cardiovascular disturbances Cardiovascular disturbances are
○ In obstructive diseases (asthma, COPD, chronic bronchitis, common in COPD and may represent a complication of COPD itself or
emphysema): may be triggered by the same factor, that is, smoking. Recently it has
■ FEV1 (<80%, often ~45%) diminished because of been proposed that lung inflammation may directly affect
increased airway resistance to expiratory flow. atherogenesis by driving systemic inflammation. Pulmonary
■ FVC may be decreased as well, due to the premature hypertension is a late complication of COPD and independently
closure of airway in expiration, just not as diminished as FEV1. This worsens its prognosis. A major factor is chronic hypoxia, which can
generates a reduced value (<80%, often ~45%). result in pulmonary vasoconstriction. Right ventricular dysfunction and
○ In restrictive diseases (such as pulmonary fibrosis): FEV1 and failure (cor pulmonale) may eventually develop and add to the
FVC both reduced proportionally, and the value may be normal or morbidity and mortality of this disease. This phenomenon will lead to
even increased as a result of decreased lung compliance. the increase volume in venous system resulting to neck vein
● TIDAL VOLUME (TV) - The amount of air normally inhaled or engorgement and bipedal edema.
exhaled at rest (normal quiet respiration).
● TOTAL LUNG CAPACITY (TLC) - The maximum volume of air
present in the lungs after maximal inspiration.
● Asthma is restrictive while COPD is obstructive, however, both
will have low FEV1/FVC which is <70%.
3. Draw the MEF of a COPD patient alongside a normal MEF.
Which of the lung volumes and capacities change in COPD
patients?
The respiratory volume of the expiratory flow and total lung
capacity decrease in patients with COPD.
4. Explain the physiologic basis for the following clinical
manifestations of Noynoy .
A. CHRONIC COUGH, PROGRESSIVE DYSPNEA AND
WHEEZING
Airflow limitation and hyperinflation Expiratory airflow
limitation is the principal physiological defect in COPD. Intrinsic airway
factors relate to bronchial wall inflammation and include mucosal
inflammation/edema, bronchial wall remodeling/fibrosis, and increased
mucosal secretions. Extrinsic factors involve the loss of elastic tissue
support for small airways and the dynamic expiratory compression of
these airways. Other factors such as respiratory muscle dysfunction
can further limit airflow in some patients. Hyperinflation can also occur 5. Interpret the ABGs of Noynoy. Explain the decrease in pO2
in COPD, leading to an increase in functional residual capacity (FRC)— and the increase in pCO2. What could have caused his
the amount of air that remains in the lungs at the end of tidal deterioration? Why was there a change in Noynoy’s
exhalation. This can lead to gas trapping and an increase in residual sensorium? How will the abnormality in the blood gas alter
volume (RV). As a consequence, there is an augmentation of the the delivery of O2 to the tissue?
inspiratory work of breathing, which is an important factor in
producing dyspnea. As the expiratory time is essential for lung
Noynoy’s ABG Result
emptying, factors that decrease this time, such as an increasing
PHYSIOLOGY LABORATORY 4 of 6 [Block B]
Saint Louis University
School of Medicine PHYSIOLOGY LAB
constantly on the other hand Noynoy differs as it became high after 2-
On 2 hours 12 hours after 12 hours of admission. Nini’s fiO2 is normal throughout the test while
Admission after Noynoy became high 2-12 hours after admission.
pH 7.32 7.28 7.10 2. What is the expected PFT result for Nini? Draw the MEF of a
patient with pulmonary fibrosis compared to normal and
pCO2 48 mmHg 54 mmHg 68 mmHg COPD patient. What other lung function tests may be used to
confirm the diagnosis? Explain the mechanism behind the
HCO3 26 28 30 examination.
Nini has both obstructive and restrictive pulmonary disorder
pO2 56 mmHg 92 mmHg 81 mmHg
Other lung function tests are lung volume determination,
FiO2 21% 40% 40% pulse oximetry, PEFR, Diffusing capacity of lung for Carbon
monoxide, assessment of respiratory muscle strength.
The patient is in respiratory acidosis. There is gradual increase in
pCO2 and decrease in pO2 levels. An increase in pCOs is an The lung tests would request the patient to facilitate maneuvers like
indication that it is “respiratory” instead of “metabolic”. Due to the inhaling, forceful inhaling and remaining lung volume after exhaling
destruction of bronchial walls or accumulation of sputum, there is can be performed by the patient to evaluate the condition and function
insufficient oxygenation process, increasing the CO2 accumulation and of the lungs.
decreasing the O2 supply. Increase CO2 results to hypercapnia and
hypoxemia, resulting to decrease delivery of O2 to the tissues. Acidic
blood decreases the affinity of O2 to blood.
Mechanisms of hypoventilation in COPD:
● Decreased responsiveness to hypoxia and hypercapnia
● Increased ventilation-perfusion mismatch leading to increased dead
space ventilation
● Decreased diaphragmatic function due to fatigue and hyperinflation
VII. CASE 3
1. What are the factors that predisposed to Nini’s condition?
Explain the mechanism behind its occurrence
Nini most likely developed her condition from inhaling asbestos
while washing the clothes of someone who works with asbestos.
Mesothelioma is a type of cancer that develops from the thin layer of
tissue that covers many internal organs. The predisposing factor to
mesothelioma is asbestos, as 80% of the patients have known
exposure to it works with places that contains asbestos, so those who
are working with asbestos is at risk. Other contributing factors for CHECKPOINT!
mesothelioma include inhalation of talc, restrictive lung disease,
excessive sedation, chronic obstructive pulmonary disease, 1. a basic pulmonary function test which measures the amount of
genetics and infection with the simian virus. air inspired and expired
2. Normal physiologic pH
2. Why is the dyspnea worse during exertion? What factors 3. A type of cancer that develops from thin layer of tissue that
are affected that caused the increase in the work of covers many internal organs and can be caused by inhaling
breathing? asbestos
The dyspnea is worse during exertion because of asbestos 4. a space that is the part of the tidal volume which does not
in which 80% of the cause of mesothelioma, is pleural thickening, participate in gas exchange.
often manifested as discrete pleural plaques, Visceral pleural 5. Shape of flow volume loop of patients with obstructive lung
thickening often includes blunting of the costophrenic angle and disease
extends diffusely up the chest wall, if advanced, visceral pleural 6. What happens to FRC and ERV when a person lies supine from
thickening is associated with dyspnea. a standing position?
7. the volume remaining in the lungs after maximal expiration
3. Interpret the ABG results. Explain the difference in finding 8. volumes that are not measurable by spirometry
pre and post exercise. How does her ABG results differ from 9. a transmitted voice sound generated by the larynx that causes
that of Noynoy? modification of the voice resembling the “bleating of a goat”
10. Expected spirometry result for Bronchial Asthma
Nini has a difficulty breathing as interpreted in her ABG result due to T/F
her mesothelioma, rare aggreasive form of cancer in the lining if the 11. In bronchial asthma, the airways become narrowed and results
lungs and abdomen or heart and interstitial pulmonary fibrosis. in difficulty in inspiration but not in expiration.
Her ABG results are: 12. Alveolar dead space is the volume of the conducting airways.
a. pH = 7.46-7.60 which is above normal that is 7.4 thus she is It is the portion of the airways which conducts gas to alveoli.
experiencing alkalemia 13. Restrictive Respiratory Defects results in flow volume loop is
b. pCO2 = 32-28 which is very low from the normal that is 40 similar as normal but small flow volume loop due to minimal
c. fiO2 = are within the normal range inhalation.
d. HCO3 = 13-17 which is going high to compensate the low amount Interpret:
of CO2 14. pH=7.48 pCO2=35 mmHg paO2=52 mmHg HCO3=22 meQ/L
Nini and Noynoy differs in their pH, pCO2, HCO3 and fiO2. Nini has
high (alkalosis) while Noynoy has low (Acidosis). Nini’s pCO2 is low
while Noynoy has high. Their HCO3 differs in that Nini has low
PHYSIOLOGY LABORATORY 5 of 6 [Block B]
Saint Louis University
School of Medicine PHYSIOLOGY LAB
1. Spirometry
2. 7.4
3. mesothelioma
4. Physiologic dead space
5. sigmoid curve
6. decrease, decrease
7. residual volume
8. TLC, FRC
9. egophony
10. < 70% FEV₁/FVC, Reversible, FEV₁ increased by 12% and 200
ml (after nebulization)
11. F (difficulty in inspiration and expiration)
12. F (Anatomic dead space)
13. T
14. Respiratory alkalosis, uncompensated with hypoxemia
PHYSIOLOGY LABORATORY 6 of 6 [Block B]
You might also like
- Spirometry E-Guide 2013Document28 pagesSpirometry E-Guide 2013Vidal Odon Ramos MermaNo ratings yet
- Dr. Ali’s Uworld Notes For Step 2 CK ElectrolytesDocument15 pagesDr. Ali’s Uworld Notes For Step 2 CK ElectrolytesBoogy WoogyNo ratings yet
- Spirometry: Dr. Dora FlorianDocument15 pagesSpirometry: Dr. Dora FlorianDoraNo ratings yet
- Clinical Examination of Respiratory SystemDocument37 pagesClinical Examination of Respiratory SystemDipienshu BhatNo ratings yet
- Symptom Flow Chart (Difficulty Breathing)Document2 pagesSymptom Flow Chart (Difficulty Breathing)Jeff ZhouNo ratings yet
- Lung Mechanics and Ventilation-Lecture NotesDocument16 pagesLung Mechanics and Ventilation-Lecture NotesCarlos Eduardo LinaresNo ratings yet
- 4 - Pulmonary PathophysiologyDocument56 pages4 - Pulmonary PathophysiologyReynandriel100% (1)
- Asthma and CopdDocument44 pagesAsthma and CopdBeer Dilacshe100% (1)
- Pulmonary Physiology NotesDocument18 pagesPulmonary Physiology Noteslezibells100% (2)
- Final PhysioDocument1,111 pagesFinal PhysioSana Savana Aman R100% (1)
- Electrolyte DisordersDocument10 pagesElectrolyte DisordersSlavicaNo ratings yet
- Acute Respiratory Distress SyndromeDocument30 pagesAcute Respiratory Distress SyndromeNikhil GhubadeNo ratings yet
- How To Take A Set of Arterial Blood Gases (Abgs) : Think Lemon Juice in A Salted Paper Cut ..It Does Smart A Little!Document48 pagesHow To Take A Set of Arterial Blood Gases (Abgs) : Think Lemon Juice in A Salted Paper Cut ..It Does Smart A Little!shiv dattaNo ratings yet
- NAFLD—Where We Stand TodayDocument32 pagesNAFLD—Where We Stand TodaySaad MotawéaNo ratings yet
- Simple Office SpirometryDocument42 pagesSimple Office SpirometryRoberto Merza III100% (4)
- Body Plethysmography AvneetDocument54 pagesBody Plethysmography Avneetsalimtajamul100% (3)
- The Coronary CirculationDocument12 pagesThe Coronary CirculationJulia PutnikNo ratings yet
- Cardiovascular Pathology 1:: Blood VesselsDocument48 pagesCardiovascular Pathology 1:: Blood VesselsRaiver CadenNo ratings yet
- Pericardial EffusionDocument3 pagesPericardial EffusionNita Hurek100% (1)
- Approach To Ventricular ArrhythmiasDocument18 pagesApproach To Ventricular ArrhythmiasDavid CruzNo ratings yet
- Lung Sounds: An Assessment of The Patient in Respiratory DistressDocument40 pagesLung Sounds: An Assessment of The Patient in Respiratory DistressJoseph Rodney de LeonNo ratings yet
- Normal Spirometry Tracing and Clinical ApplicationsDocument2 pagesNormal Spirometry Tracing and Clinical ApplicationsAlyssa LeonesNo ratings yet
- Pulmonary: Ftplectures Pulmonary System Lecture NotesDocument34 pagesPulmonary: Ftplectures Pulmonary System Lecture NotesArif Setyawan100% (1)
- Arterial Blood GasDocument48 pagesArterial Blood GaslovianettesherryNo ratings yet
- Arterial Blood Gas InterpretationDocument65 pagesArterial Blood Gas InterpretationDaniel AryanNo ratings yet
- Respiratory PhysiologyDocument38 pagesRespiratory Physiologyramadan100% (3)
- Chest X-ray Interpretation GuideDocument104 pagesChest X-ray Interpretation GuideIbra Geeky100% (1)
- Spirometry Interpretation: Lung VolumesDocument4 pagesSpirometry Interpretation: Lung VolumesBobet ReñaNo ratings yet
- PFT Interpretation AlgorithmDocument4 pagesPFT Interpretation AlgorithmJason Steel50% (2)
- COPD Acute Management ABCDEDocument11 pagesCOPD Acute Management ABCDESSNo ratings yet
- Surface Tension Lab - Advanced VersionDocument6 pagesSurface Tension Lab - Advanced VersionTeachLABScINo ratings yet
- Respiratory failure and ARDS: causes, symptoms, treatmentDocument52 pagesRespiratory failure and ARDS: causes, symptoms, treatmentAlex ChiuNo ratings yet
- Anaesthesia and Atrial FibrillationDocument15 pagesAnaesthesia and Atrial FibrillationNaresh Dhawan100% (1)
- Signs of Respiratory Distress in Your Child: Signs To Look ForDocument2 pagesSigns of Respiratory Distress in Your Child: Signs To Look ForMa GynNo ratings yet
- Platelet DisordersDocument12 pagesPlatelet Disordersopi nean100% (1)
- AARC Clinical Practice Guideline Blood Gas Analysis and Hemoximetry: 2013Document10 pagesAARC Clinical Practice Guideline Blood Gas Analysis and Hemoximetry: 2013jvalenciagNo ratings yet
- ABGS Arterial Blood GasesDocument27 pagesABGS Arterial Blood GasesMuhammad asif samiNo ratings yet
- BARORECEPTORS AND CHEMORECEPTORS: REGULATION OF CARDIAC PRESSURESDocument4 pagesBARORECEPTORS AND CHEMORECEPTORS: REGULATION OF CARDIAC PRESSURESDrbee10No ratings yet
- UAW Respiratory Final Study Guide YupDocument116 pagesUAW Respiratory Final Study Guide YupNabeel Shahzad100% (1)
- Asthma Lancet 23febDocument18 pagesAsthma Lancet 23febMr. LNo ratings yet
- Left Ventricular Non-CompactionDocument20 pagesLeft Ventricular Non-CompactionlawlietNo ratings yet
- Pulmonary EmbolismDocument2 pagesPulmonary EmbolismArijit ChakravortyNo ratings yet
- My Cardiac and Chest SymptomsDocument58 pagesMy Cardiac and Chest SymptomsDhamirah SakinahNo ratings yet
- Respiratory EmergenciesDocument34 pagesRespiratory EmergenciesRoshana MallawaarachchiNo ratings yet
- Tachyarrhythmias When Should I Refer?Document25 pagesTachyarrhythmias When Should I Refer?Cindy Seow Sieng TengNo ratings yet
- EKG InterpretationDocument63 pagesEKG InterpretationMiriam Cindy MathullaNo ratings yet
- Physiology Acid QuizDocument5 pagesPhysiology Acid QuizRavi AminNo ratings yet
- Arterial Blood Gases: A Step by Step GuideDocument19 pagesArterial Blood Gases: A Step by Step GuideKathleen Ann50% (2)
- Updated: Dec 07, 2016 Author: Justina Gamache, MD Chief Editor: Guy W Soo Hoo, MD, MPHDocument42 pagesUpdated: Dec 07, 2016 Author: Justina Gamache, MD Chief Editor: Guy W Soo Hoo, MD, MPHgita suci arianiNo ratings yet
- Pulmonary Function TestDocument77 pagesPulmonary Function TestMohammed Saad NabhanNo ratings yet
- 3rd Edition Self-Assessment in Respiratory MedicineDocument267 pages3rd Edition Self-Assessment in Respiratory MedicineamjadsabahNo ratings yet
- Aortic StenosisDocument3 pagesAortic StenosisMaxine BaraquiaNo ratings yet
- National Asthma - Bronchiolitis - COPD GuidelinesDocument84 pagesNational Asthma - Bronchiolitis - COPD GuidelinesFaisol Kabir86% (7)
- Register for Pediatric Asthma WorkshopDocument2 pagesRegister for Pediatric Asthma WorkshopAntonio TayaoNo ratings yet
- Captopril Renography - Detect Renal Artery StenosisDocument3 pagesCaptopril Renography - Detect Renal Artery StenosisSri HariNo ratings yet
- X Thorax BeoordelenDocument135 pagesX Thorax BeoordelenmtescasuraNo ratings yet
- Basics of Ventilatory SupportDocument43 pagesBasics of Ventilatory SupportAdhithya BhatNo ratings yet
- Respiratory System - History & Physical Examination: Mohan KumarDocument35 pagesRespiratory System - History & Physical Examination: Mohan KumaraagarwalmdNo ratings yet
- Intermittent Positive Pressure BreathingDocument12 pagesIntermittent Positive Pressure BreathingHitesh RohitNo ratings yet
- BengzonDocument5 pagesBengzonmceline19No ratings yet
- Academic Writing in English: Carolyn Brimley Norris, Ph.D. Language Services University of Helsinki 2015Document86 pagesAcademic Writing in English: Carolyn Brimley Norris, Ph.D. Language Services University of Helsinki 2015nasralaNo ratings yet
- Automatic Analysis of Annual Financial Reports: A Case StudyDocument11 pagesAutomatic Analysis of Annual Financial Reports: A Case StudyYuliana MargarettaNo ratings yet
- Indesign: A How-To Guide For Creating A Professional Resumé Using IndesignDocument14 pagesIndesign: A How-To Guide For Creating A Professional Resumé Using IndesignmadpancakesNo ratings yet
- Cover Letter and Thank You Letter ExamplesDocument7 pagesCover Letter and Thank You Letter Examplesf675ztsf100% (2)
- BioassayDocument38 pagesBioassayMuhammad Masoom AkhtarNo ratings yet
- Highway Construction Production Rates and Estimated Contracct TimesDocument95 pagesHighway Construction Production Rates and Estimated Contracct TimesLTE002No ratings yet
- Kinematics of MachineDocument4 pagesKinematics of MachineSumit KambleNo ratings yet
- Racionalidad Acotada 1Document4 pagesRacionalidad Acotada 1Hector J. RubiniNo ratings yet
- FSLDMDocument5 pagesFSLDMaiabbasi9615No ratings yet
- Earned Value Management Systems ANSI/EIA-748-C Intent GuideDocument59 pagesEarned Value Management Systems ANSI/EIA-748-C Intent Guidekarditobambang23No ratings yet
- Hospital Ship Feasibility StudyDocument10 pagesHospital Ship Feasibility StudyRhona JhoyNo ratings yet
- The Authors Guild vs. Google, Inc. Facts: Plaintiffs, Who Are Authors of Published Books UnderDocument15 pagesThe Authors Guild vs. Google, Inc. Facts: Plaintiffs, Who Are Authors of Published Books UnderElead Gaddiel S. AlbueroNo ratings yet
- Organization and Operation of Partnerships and LLPsDocument50 pagesOrganization and Operation of Partnerships and LLPsAliaa Hosam100% (1)
- Mid-Semester Exam ED2 2020Document11 pagesMid-Semester Exam ED2 2020Subhabrata MajumdarNo ratings yet
- Cyber Security Module 1Document4 pagesCyber Security Module 1silentnightNo ratings yet
- Charatible Trust FINAL BOOKDocument80 pagesCharatible Trust FINAL BOOKAmitNo ratings yet
- NATO Intelligence Exploitation of The InternetDocument104 pagesNATO Intelligence Exploitation of The Internetmauro.pennacchietti100% (1)
- Lightning Attachment Models and Maximum Shielding Failure Current: Application To Transmission LinesDocument9 pagesLightning Attachment Models and Maximum Shielding Failure Current: Application To Transmission LinespedramNo ratings yet
- The Nazi Master PlanDocument28 pagesThe Nazi Master PlanFolad109No ratings yet
- Newton's Third Law and Vectors TutorialDocument9 pagesNewton's Third Law and Vectors TutorialpalparasNo ratings yet
- Kudippaka" - in Kannur Politics An Investigation?Document8 pagesKudippaka" - in Kannur Politics An Investigation?Anonymous CwJeBCAXpNo ratings yet
- Ch1 - Part I - Meaning of ResearchDocument36 pagesCh1 - Part I - Meaning of ResearchKirubel MulugetaNo ratings yet
- Personal Development PlanDocument10 pagesPersonal Development PlanNg Thị Kh ThiệnNo ratings yet
- Pride and Prejudice Plot StructureDocument3 pagesPride and Prejudice Plot StructureGeetanjali Joshi100% (2)
- Jurnal Kebidanan KomunitasDocument5 pagesJurnal Kebidanan KomunitasdeffiNo ratings yet
- Arvydas Sliogeris The Thing and Art Two Essays On The Ontotopy of The Work of Art 1Document168 pagesArvydas Sliogeris The Thing and Art Two Essays On The Ontotopy of The Work of Art 1Richard OhNo ratings yet
- Background Surya NepalDocument11 pagesBackground Surya NepalUjibpradhan67% (3)
- ReportDocument3 pagesReportPrecious Anne MacalinoNo ratings yet
- Subcontractor Agreement TemplateDocument20 pagesSubcontractor Agreement TemplateJoseph Rod Allan Alano90% (10)
- Functional Training and Beyond: Building the Ultimate Superfunctional Body and MindFrom EverandFunctional Training and Beyond: Building the Ultimate Superfunctional Body and MindRating: 4.5 out of 5 stars4.5/5 (1)
- Aging Backwards: Reverse the Aging Process and Look 10 Years Younger in 30 Minutes a DayFrom EverandAging Backwards: Reverse the Aging Process and Look 10 Years Younger in 30 Minutes a DayNo ratings yet
- Chair Yoga: Sit, Stretch, and Strengthen Your Way to a Happier, Healthier YouFrom EverandChair Yoga: Sit, Stretch, and Strengthen Your Way to a Happier, Healthier YouRating: 3.5 out of 5 stars3.5/5 (5)
- Whole Body Barefoot: Transitioning Well to Minimal FootwearFrom EverandWhole Body Barefoot: Transitioning Well to Minimal FootwearRating: 4 out of 5 stars4/5 (16)
- Strong Is the New Beautiful: Embrace Your Natural Beauty, Eat Clean, and Harness Your PowerFrom EverandStrong Is the New Beautiful: Embrace Your Natural Beauty, Eat Clean, and Harness Your PowerRating: 4 out of 5 stars4/5 (5)
- Body by Science: A Research Based Program for Strength Training, Body building, and Complete Fitness in 12 Minutes a WeekFrom EverandBody by Science: A Research Based Program for Strength Training, Body building, and Complete Fitness in 12 Minutes a WeekRating: 4.5 out of 5 stars4.5/5 (84)
- Music For Healing: With Nature Sounds For Natural Healing Powers: Sounds Of Nature, Deep Sleep Music, Meditation, Relaxation, Healing MusicFrom EverandMusic For Healing: With Nature Sounds For Natural Healing Powers: Sounds Of Nature, Deep Sleep Music, Meditation, Relaxation, Healing MusicRating: 5 out of 5 stars5/5 (1)
- Power of 10: The Once-A-Week Slow Motion Fitness RevolutionFrom EverandPower of 10: The Once-A-Week Slow Motion Fitness RevolutionRating: 3.5 out of 5 stars3.5/5 (11)
- Peak: The New Science of Athletic Performance That is Revolutionizing SportsFrom EverandPeak: The New Science of Athletic Performance That is Revolutionizing SportsRating: 5 out of 5 stars5/5 (95)
- Boundless: Upgrade Your Brain, Optimize Your Body & Defy AgingFrom EverandBoundless: Upgrade Your Brain, Optimize Your Body & Defy AgingRating: 4.5 out of 5 stars4.5/5 (66)
- Endure: Mind, Body, and the Curiously Elastic Limits of Human PerformanceFrom EverandEndure: Mind, Body, and the Curiously Elastic Limits of Human PerformanceRating: 4.5 out of 5 stars4.5/5 (237)
- The Seven Spiritual Laws of Yoga: A Practical Guide to Healing Body, Mind, and SpiritFrom EverandThe Seven Spiritual Laws of Yoga: A Practical Guide to Healing Body, Mind, and SpiritRating: 4.5 out of 5 stars4.5/5 (73)
- Weight Lifting Is a Waste of Time: So Is Cardio, and There’s a Better Way to Have the Body You WantFrom EverandWeight Lifting Is a Waste of Time: So Is Cardio, and There’s a Better Way to Have the Body You WantRating: 4.5 out of 5 stars4.5/5 (38)
- Relentless: From Good to Great to UnstoppableFrom EverandRelentless: From Good to Great to UnstoppableRating: 5 out of 5 stars5/5 (783)
- Muscle for Life: Get Lean, Strong, and Healthy at Any Age!From EverandMuscle for Life: Get Lean, Strong, and Healthy at Any Age!Rating: 4.5 out of 5 stars4.5/5 (22)
- Not a Diet Book: Take Control. Gain Confidence. Change Your Life.From EverandNot a Diet Book: Take Control. Gain Confidence. Change Your Life.Rating: 4.5 out of 5 stars4.5/5 (124)
- Yamas & Niyamas: Exploring Yoga's Ethical PracticeFrom EverandYamas & Niyamas: Exploring Yoga's Ethical PracticeRating: 4.5 out of 5 stars4.5/5 (110)
- Roxane Gay & Everand Originals: Built for This: The Quiet Strength of PowerliftingFrom EverandRoxane Gay & Everand Originals: Built for This: The Quiet Strength of PowerliftingRating: 4.5 out of 5 stars4.5/5 (132)
- You: Breathing Easy: Meditation and Breathing Techniques to Relax, Refresh and RevitalizeFrom EverandYou: Breathing Easy: Meditation and Breathing Techniques to Relax, Refresh and RevitalizeRating: 3 out of 5 stars3/5 (5)
- SAS Training Manual: How to get fit enough to pass a special forces selection courseFrom EverandSAS Training Manual: How to get fit enough to pass a special forces selection courseRating: 4 out of 5 stars4/5 (3)
- The Yogi Code: Seven Universal Laws of Infinite SuccessFrom EverandThe Yogi Code: Seven Universal Laws of Infinite SuccessRating: 4.5 out of 5 stars4.5/5 (104)
- Body by Science: A Research Based Program to Get the Results You Want in 12 Minutes a WeekFrom EverandBody by Science: A Research Based Program to Get the Results You Want in 12 Minutes a WeekRating: 4 out of 5 stars4/5 (38)
- Buteyko Breathing Course Manual: For use with the Advanced Buteyko CourseFrom EverandButeyko Breathing Course Manual: For use with the Advanced Buteyko CourseRating: 5 out of 5 stars5/5 (1)
- Wall Pilates: Quick-and-Simple to Lose Weight and Stay Healthy. A 30-Day Journey with + 100 ExercisesFrom EverandWall Pilates: Quick-and-Simple to Lose Weight and Stay Healthy. A 30-Day Journey with + 100 ExercisesNo ratings yet
- The Yamas & Niyamas: Exploring Yoga's Ethical PracticeFrom EverandThe Yamas & Niyamas: Exploring Yoga's Ethical PracticeRating: 4.5 out of 5 stars4.5/5 (19)
- The Calisthenics Codex: Fifty Exercises for Functional FitnessFrom EverandThe Calisthenics Codex: Fifty Exercises for Functional FitnessRating: 4 out of 5 stars4/5 (9)
- 7 Weeks to 10 Pounds of Muscle: The Complete Day-by-Day Program to Pack on Lean, Healthy Muscle MassFrom Everand7 Weeks to 10 Pounds of Muscle: The Complete Day-by-Day Program to Pack on Lean, Healthy Muscle MassRating: 4 out of 5 stars4/5 (2)