Professional Documents
Culture Documents
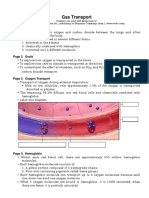
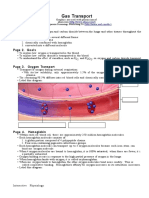
Transport of Gases
Uploaded by
Arvinth Guna Segaran0 ratings0% found this document useful (0 votes)
25 views2 pagesits an explanation of how gases exchange
Original Title
transport of gases
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentits an explanation of how gases exchange
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
25 views2 pagesTransport of Gases
Uploaded by
Arvinth Guna Segaranits an explanation of how gases exchange
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 2
AS DISSOLVED FORM Hydrogen ions dissociated from carbonic acid are
buffered by hemoglobin inside the cell.
Carbon dioxide diffuses into blood and dissolves in
the fluid of plasma forming a simple solution. Reverse chloride shift is the process by which
Only about 3 mL/100 mL of plasma of carbon chloride ions are moved back into plasma from
dioxide is transported as dissolved state. RBC shift. It occurs in lungs.
It is about 7% of total carbon dioxide in the blood. It helps in elimination of carbon dioxide from the
blood.
AS CARBONIC ACID
Bicarbonate is converted back into carbon dioxide,
which has to be expelled out.
Part of dissolved carbon dioxide in plasma
combines with the water to form carbonic acid. It takes place by the following mechanism:
Transport ofcarbon dioxide in this form is When blood reaches the alveoli, sodium
negligible. bicarbonate in plasma dissociates into sodium and
bicarbonate
AS BICARBONATE ions.
Bicarbonate ion moves into the RBC.
About 63% of carbon dioxide is transported as It makes chloride ion to move out of the RBC into
bicarbonate. the plasma, where it combines with sodium and
From plasma, carbon dioxide enters theRBCs. forms sodium chloride.
In the RBCs, carbon dioxide combines with water Bicarbonate ion inside the RBC combines with
to form carbonic acid. hydrogen ion forms carbonic acid, which
The reaction inside RBCs is very rapid because of dissociates into water and carbon dioxide.
the presence of carbonic anhydrase. Carbon dioxide is then expelled out
This enzyme accelerates the reaction.
Carbonic anhydrase is present only inside the RBCs AS CARBAMINO COMPOUNDS
and not in plasma.
That is why carbonic acid formation is at least 200 About 30% of carbon dioxide is transported as
to 300 times more in RBCs than in plasma. carbamino compounds.
Carbonic acid is very unstable. Carbon dioxide is transported in blood in
Almost all carbonic acid (99.9%) formed in red combination with hemoglobin and plasma
blood corpuscles, dissociates into bicarbonate and proteins.
hydrogen ions. Carbon dioxide combines with hemoglobin to form
Concentration of bicarbonate ions in the cell carbamino hemoglobin or carbahemoglobin.
increases more and more And it combines with plasma proteins to form
Due to high concentration, bicarbonate ions carbamino proteins.
diffuse through the cell membrane into plasma. Carbamino hemoglobin and carbamino proteins
are together called carbamino compounds.
Chloride shift occurs when carbon dioxide enters Carbon dioxide combines with proteins or
the blood from tissues. hemoglobin with a loose bond so that, carbon
In plasma, plenty of sodium chloride is present. dioxide is easily released into alveoli, where the
It dissociates into sodium and chloride ions partial pressure of carbon dioxide is low.
When the negatively charged bicarbonate ions Thus, the combination of carbon dioxide with
move out of RBC into the plasma, the negatively proteins and hemoglobin is a reversible one.
charged chloride ions move into the RBC in order Amount of carbon dioxide transported in
to maintain the electrolyte equilibrium (ionic combination with plasma proteins is very less
balance). compared to the amount transported in
Anion exchanger 1 (band 3 protein), which acts combination with hemoglobin.
like antiport pump in RBC membrane is It is because the quantity of proteins in plasma is
responsible for the exchange of bicarbonate ions only half of the quantity of hemoglobin.
and chloride ions.
Bicarbonate ions combine with sodium ions in the
plasma and form sodium bicarbonate.
In this form, it is transported in the blood.
AS SIMPLE SOLUTION
Oxygen dissolves in water of plasma and is
transported
in this physical form.
Amount of oxygen transported in this way is very
negligible. It is only 0.3 mL/100 mL of plasma. It
forms only about 3% of total oxygen in blood.
It is because of poor solubility of oxygen in water
content of plasma.
Still, transport of oxygen in this form becomes
important during the conditions like muscular
exercise to meet the excess demand of oxygen by
the tissues.
IN COMBINATION WITH HEMOGLOBIN
Oxygen combines with hemoglobin in blood and is
transported as oxyhemoglobin.
Transport of oxygen in this form is important
because, maximum amount (97%) of oxygen is
transported by this method.
BASIS FOR OXYGEN TRANSPORT
At high PO2, Oxygen binds with Hb
At low PO2, Oxygen released from Hb.
Oxygenation of Hemoglobin
Oxygen combines with hemoglobin only as a
physical combination.
It is only oxygenation and not oxidation.
This type of combination of oxygen with
hemoglobin has got some advantages.
Oxygen can be readily released from hemoglobin
when it is needed.
Hemoglobin accepts oxygen readily whenever the
partial pressure of oxygen in the blood is more.
Hemoglobin gives out oxygen whenever the partial
pressure of oxygen in the blood is less.
Oxygen combines with the iron in heme part of
hemoglobin.
Each molecule of hemoglobin contains 4 atoms of
iron.
Iron of the hemoglobin is present in ferrous form.
Each iron atom combines with one molecule of
oxygen.
After combination, iron remains in ferrous form
only.
That is why the combination of oxygen with
hemoglobin is called oxygenation and not
oxidation.
You might also like
- Eczema and DermatitisDocument43 pagesEczema and DermatitisArvinth Guna SegaranNo ratings yet
- Disorders of Red Blood CellsDocument3 pagesDisorders of Red Blood CellsArvinth Guna SegaranNo ratings yet
- Dengue Malaria Group3Document135 pagesDengue Malaria Group3Arvinth Guna SegaranNo ratings yet
- Renal Pathology GuideDocument3 pagesRenal Pathology GuideArvinth Guna SegaranNo ratings yet
- Dengue Malaria Group2Document100 pagesDengue Malaria Group2Arvinth Guna SegaranNo ratings yet
- Lung MCQDocument7 pagesLung MCQArvinth Guna Segaran100% (2)
- Review The Causes of Decreased Breath SoundsDocument1 pageReview The Causes of Decreased Breath SoundsArvinth Guna SegaranNo ratings yet
- Dengue Malaria Group1 EditedDocument120 pagesDengue Malaria Group1 EditedArvinth Guna SegaranNo ratings yet
- Breathing: Joshua, Youssef, and ApolloDocument28 pagesBreathing: Joshua, Youssef, and ApolloArvinth Guna SegaranNo ratings yet
- Forensic Medicine Mcqs by Sir NiazDocument13 pagesForensic Medicine Mcqs by Sir NiazYasaan ChaudharyNo ratings yet
- Anatomy of SkinDocument26 pagesAnatomy of SkinArvinth Guna SegaranNo ratings yet
- Wiki Resp Mcqs ExplainedDocument7 pagesWiki Resp Mcqs ExplainedArvinth Guna SegaranNo ratings yet
- Idc4u May12Document18 pagesIdc4u May12Arvinth Guna SegaranNo ratings yet
- SteDis - HospWMDocument68 pagesSteDis - HospWMArvinth Guna SegaranNo ratings yet
- Study+guide++community+medicine+2010 2011 PDFDocument55 pagesStudy+guide++community+medicine+2010 2011 PDFArvinth Guna SegaranNo ratings yet
- Foremed - DEC 2010 PDFDocument4 pagesForemed - DEC 2010 PDFArvinth Guna SegaranNo ratings yet
- Anatomy of SkinDocument26 pagesAnatomy of SkinArvinth Guna SegaranNo ratings yet
- Breath Sounds - CSC Respiratory System: Type of Sound Normal Abnormal Continuous Discontinuo US OthersDocument2 pagesBreath Sounds - CSC Respiratory System: Type of Sound Normal Abnormal Continuous Discontinuo US OthersArvinth Guna SegaranNo ratings yet
- Anticoagulatns, Antiplatelets, Fibrinolytics, AntifibrinolyticsDocument2 pagesAnticoagulatns, Antiplatelets, Fibrinolytics, AntifibrinolyticsArvinth Guna SegaranNo ratings yet
- MuetDocument20 pagesMuetArvinth Guna SegaranNo ratings yet
- Lung MCQDocument7 pagesLung MCQArvinth Guna Segaran100% (2)
- Principles of Treatment of IhdDocument3 pagesPrinciples of Treatment of IhdArvinth Guna SegaranNo ratings yet
- Physio Rs QuizDocument2 pagesPhysio Rs QuizArvinth Guna SegaranNo ratings yet
- Vision PhysioDocument1 pageVision PhysioArvinth Guna SegaranNo ratings yet
- Breath Sounds - CSC Respiratory System: Type of Sound Normal Abnormal Continuous Discontinuo US OthersDocument2 pagesBreath Sounds - CSC Respiratory System: Type of Sound Normal Abnormal Continuous Discontinuo US OthersArvinth Guna SegaranNo ratings yet
- Sputum Analysis and Clinical Course of TBDocument3 pagesSputum Analysis and Clinical Course of TBArvinth Guna SegaranNo ratings yet
- Gender Roles Affecting Health and IllnessDocument3 pagesGender Roles Affecting Health and IllnessArvinth Guna SegaranNo ratings yet
- Educational Blog on Bilirubin Conjugation and Calcitriol SynthesisDocument3 pagesEducational Blog on Bilirubin Conjugation and Calcitriol SynthesisArvinth Guna Segaran0% (1)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Periyar Institute of Distance Education (Pride)Document206 pagesPeriyar Institute of Distance Education (Pride)Anistus Rok BranishNo ratings yet
- Chapter 15 Respiratory SystemDocument29 pagesChapter 15 Respiratory SystemMacthalas QuiazonNo ratings yet
- 17 CRISP PhysiologyDocument5 pages17 CRISP PhysiologySyed Aijaz44% (9)
- Trasport of Respiratory GasesDocument35 pagesTrasport of Respiratory GasesDJ PNo ratings yet
- Eathing and Exchange of GasesDocument15 pagesEathing and Exchange of Gasesg1307No ratings yet
- Transport of Oxygen and CarbondioxideDocument27 pagesTransport of Oxygen and CarbondioxideDhanush SatheeshNo ratings yet
- Haemoglobin and O2 CO2 TransportDocument33 pagesHaemoglobin and O2 CO2 TransportRenad AlharbiNo ratings yet
- Transport of Carbon Dioxide in the BodyDocument9 pagesTransport of Carbon Dioxide in the BodyBarkat ShazliNo ratings yet
- Gas Transport in the BloodDocument19 pagesGas Transport in the BloodMarilia BonorinoNo ratings yet
- Rabbit RespirationDocument5 pagesRabbit RespirationshajehanNo ratings yet
- Physical Principles of Gas ExchangeDocument12 pagesPhysical Principles of Gas ExchangeKo HakuNo ratings yet
- Gas TransportDocument19 pagesGas TransportJesus GutierrezNo ratings yet
- CAIE Biology A-level Transport in Mammals FlashcardsDocument77 pagesCAIE Biology A-level Transport in Mammals FlashcardsElisaNo ratings yet
- RespirationDocument10 pagesRespirationADWAIT LALUNo ratings yet
- Ujian Pengesahan P2 2019Document6 pagesUjian Pengesahan P2 2019Then MoliNo ratings yet
- 1-The Bicarbonate Buffer System-2022Document41 pages1-The Bicarbonate Buffer System-2022Keerthi Chowdary AmaraneniNo ratings yet
- Co2 PDFDocument4 pagesCo2 PDFSITI SARAH BTE NOOR MEAHNo ratings yet
- Chloride Shift Mechanism ScriptDocument3 pagesChloride Shift Mechanism ScriptdavenNo ratings yet
- Ransport Of: Dr. Roopa Kotha Dr. Shaji MathewDocument36 pagesRansport Of: Dr. Roopa Kotha Dr. Shaji MathewRenganathan SockalingamNo ratings yet