Professional Documents
Culture Documents
Tavee2017 PDF
Tavee2017 PDF
Uploaded by
Indah NisaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Tavee2017 PDF
Tavee2017 PDF
Uploaded by
Indah NisaCopyright:
Available Formats
Review Article
Low Back Pain
Address correspondence to
Dr Jinny O. Tavee, Cleveland
Clinic, Department of
Neurology, S-90, 9500 Euclid
Jinny O. Tavee, MD; Kerry H. Levin, MD, FAAN Ave, Cleveland, OH 44195,
taveej2@ccf.org.
Relationship Disclosure:
Dr Tavee has received
ABSTRACT personal compensation for
Purpose of Review: This article provides an overview of evaluating and treating low lectures from Mallinckrodt
Pharmaceuticals and has
back pain in the outpatient setting. received grant/research
Recent Findings: As most cases of acute low back pain have a favorable prognosis, support for work in clinical
current guidelines on imaging studies recommend conservative treatment for 6 weeks trials from Araim
Pharmaceuticals, Inc and
prior to obtaining an MRI if no red flags are present. Of these red flags, a prior history Mallinckrodt Pharmaceuticals.
of cancer is the strongest risk factor for a malignant etiology and requires urgent Dr Levin receives personal
evaluation with MRI. Management of acute low back pain is mainly conservative with compensation for serving as
director of the American
oral non-narcotic analgesics and mobilization as the initial recommendations. For Board of Psychiatry and
patients with radiculopathy, epidural steroids may result in short-term pain relief, but Neurology, serves on the
long-term effects are still unclear. editorial boards of
Continuum and Muscle &
Summary: A systematic, evidence-based approach to the patient with low back pain is Nerve, and receives publishing
key to providing safe and cost-efficient care. royalties from Elsevier and
UpToDate, Inc.
Unlabeled Use of
Continuum (Minneap Minn) 2017;23(2):467–486.
Products/Investigational
Use Disclosure:
Drs Tavee and Levin report
no disclosures.
INTRODUCTION EPIDEMIOLOGY * 2017 American Academy
of Neurology.
Low back pain is the third most common More than 25% of adults in the United
disorder presenting in the neurology States report having experienced low
outpatient clinic (behind peripheral back pain within the preceding 3 months,
neuropathy and migraine, respectively) with a peak prevalence occurring in
and accounts for more than 1 million adults aged 45 to 64 years, and a lifetime
office visits each year.1 While most prevalence of up to 84%.2Y4 Women are
patients initially present to their primary slightly more affected than men and
care physician, early neurologic evalua- also report a higher rate of recurrence.2,3
tion may help guide the patient toward Radicular involvement (reported as sci-
the appropriate level of diagnostic test- atica) is less common, with an estimated
ing and treatment, especially in the prevalence of 1.2% to 43%.5 Risk factors
presence of nerve root involvement. for back pain include obesity, increas-
Low back pain is usually defined as ing age, heavy manual work (twisting,
acute when onset is less than 4 weeks, heavy lifting, vibration), smoking, psy-
subacute if symptoms are present for 4 chosocial factors (depression, stress),
to 12 weeks, and chronic when symp- and deconditioning.6
toms persist for more than 12 weeks. The socioeconomic burden of low
Most cases are localized to the spine back pain is a significant problem
and paraspinal region with no neuro- worldwide. In a recent global survey,
logic symptoms and are considered low back pain was found to be the
musculoskeletal or non-neurologic. In number one cause of disability.7 In the
contrast, neurologic low back pain is United States alone, the direct cost is
accompanied by radicular symptoms, estimated at $34 billion annually, al-
which include leg weakness, radiating though when lost wages and other
pain, or sensory changes that correlate indirect costs are included, this figure
with the affected nerve roots. exceeds $100 billion.2,8
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 467
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
KEY POINTS
h The number one cause PATHOPHYSIOLOGY Neurologic Low Back Pain
of disability worldwide is While musculoskeletal and neurologic In 90% of patients under the age of 65
low back pain. low back pain may share similar contrib- with radicular (neurologic) pain, the
h Disk herniation is the uting factors, the presence (or absence) pain is a result of nerve root compres-
cause of radiculopathy of nerve root involvement results in sion caused by disk herniation.10 The
in 90% of patients two distinct pathophysiologic entities. disk itself has no nociceptive fibers
under the age of 65. and does not result in pain until the
Musculoskeletal Low Back Pain herniated portion comes into contact
The source of musculoskeletal (non- with either the dural lining of the
neurologic) back pain is often non- spinal nerve root sleeve or the poste-
specific and difficult to identify in most rior longitudinal ligament.9 In older
patients. Possible mechanisms include patients, the nerve root is often affected
degenerative spine changes and injury by other age-related degenerative spine
to local spinal structures, which include changes, which include ligamentous hy-
the vertebral column, ligaments, and pertrophy, osteophyte formation, facet
surrounding muscles and soft tissues. joint arthropathy, and neural foraminal
Heavy lifting and other activities that narrowing, although disk herniation
lead to increased tension may result in may also play a role (Figure 6-1). Nerve
muscle fiber or tendon disruption. Re- root compression results in focal ische-
petitive motions or overuse of the para- mia, which may affect axon transport,
spinal muscles, especially those that are and edema.9 Local inflammation may
deconditioned or inactive at baseline, also occur due to an immunogenic
may cause pain and spasms due to response to the exposed contents of
metabolic hyperactivity and production the nucleus pulposus.9 This, in combi-
of lactic acid.9 Arthropathy of the sa- nation with the structural changes
croiliac and facet joints may also con- caused by compression, can result in
tribute to the formation of low back pain. more severe radicular pain.
FIGURE 6-1 Anatomy of degenerative lumbar spine disease. Nerve
root compression may be caused by a number of
degenerative changes that result in neural foraminal
narrowing or direct nerve impingement.
468 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
Lumbar Spinal Stenosis Location h Lumbar spinal stenosis is
In addition to narrowing of the neural Musculoskeletal low back pain is often a slowly progressive
foramina, degenerative spine changes described as a deep ache that is poorly degenerative condition
may result in central canal stenosis and localized, although some patients will that is the most
compression of spinal nerve roots via report that the pain is mainly in the common reason for
direct impingement, CSF flow obstruc- center of the lower back. Radicular spinal surgery in
tion, or vascular compromise.11 A prior disease is a sharp, burning, or needle- older patients.
history of local trauma and surgery are like pain that radiates down into one or h The clinical evaluation
other factors that can contribute to both legs in a dermatomal distribution of low back pain should
spinal stenosis, whereas congenital (Table 6-1). address three main
spine abnormalities are the primary points: (1) pain
etiology in younger patients. Lumbar Severity description (duration,
location, severity,
spinal stenosis is a slowly progressive Pain severity should be routinely asked
triggers, and relieving
degenerative condition that is the most about as part of the history but is widely
factors), (2) neurologic
common reason for spinal surgery in variable depending on psychosocial, involvement, and
older patients.12 cultural, and other factors. (3) identification of
red flags.
CLINICAL HISTORY Triggers/Relieving Factors
h Low back pain that
The clinical evaluation of low back pain Exacerbating and relieving factors, par- persists in all positions
begins with a focused history that ticularly positional changes, are an is concerning for
should address three main points: (1) integral portion of the history. For most malignancy or infection
pain description (duration, location, patients with either musculoskeletal or and should prompt
severity, triggers, and relieving factors), neurologic low back pain, symptoms further diagnostic
(2) determination of neurologic in- are reported to be worse with sitting (es- workup.
volvement, and (3) identification of pecially with prolonged driving or plane
red flags that may indicate the presence travel) and improved when standing for
of serious spinal pathology or systemic a short period of time or lying supine. In
disease requiring urgent intervention. patients with musculoskeletal pain due
to facet joint disease, osteoarthritis, or
Duration muscle strain, the reverse may be true,
Establishing the duration (acute ver- with pain reported as worse with stand-
sus chronic) of pain helps to provide a ing and relieved with sitting.13Y14 Spinal
framework by which further evaluation stenosis is also worse with standing as
and treatment may be determined. Most well as walking. Sacroiliac joint disease
patients with acute musculoskeletal low may be exacerbated by transitioning
back pain will experience spontaneous between sitting and standing.15 Low
improvement within 2 to 4 weeks, back pain that persists in all positions
while symptoms of acute radicular is concerning for malignancy or infec-
pain follow a more protracted course tion and should prompt further diag-
(up to 6 to 8 weeks) but also tend nostic workup. Patients with low back
to be self-limited. Aggressive diagnostic pain due to ankylosing spondylitis may
testing is typically not necessary for also fail to feel improvement while in
either case in the absence of red flags the supine position.
or severe neurologic deficits. Patients
presenting with chronic low back pain Neurologic Involvement
also do not usually require extensive In addition to symptoms of radicular
evaluation but should be questioned pain, patients with neurologic involve-
about any recent symptoms sugges- ment may report weakness of one or
tive of a new, superimposed disorder. both legs described as difficulty with
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 469
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
a
TABLE 6-1 Clinical Presentation in Patients With Lumbar Radiculopathy
Root Dermatomal Sensory
Level Pain Distribution Distribution Weakness Reflex Abnormality
L1 Inguinal region Inguinal region Hip flexion Cremasteric reflex
L2 Inguinal region, Anterior thigh Hip flexion, hip Cremasteric reflex,
anterior thigh adduction thigh adductor reflex
L3 Anterior thigh, knee Distal anteromedial Knee extension, hip Patellar reflex, thigh
thigh including knee flexion, hip adduction adductor reflex
L4 Anterior thigh, Medial leg Knee extension, hip Patellar reflex
medial aspect leg flexion, hip adduction
L5 Posterolateral thigh, Lateral leg, dorsal Foot dorsiflexion, knee Not applicable
lateral leg, medial foot foot, and great toe flexion, hip abduction
S1 Posterior thigh and Posterolateral leg, Foot plantar flexion, knee Achilles reflex
leg, lateral foot lateral aspect of foot, flexion, hip extension
sole of foot
a
Modified with permission from Levin KH, Continuum (Minneap Minn).9 B 2001 American Academy of Neurology. journals.lww.com/
continuum/Citation/2001/07010/LOW_BACK_AND_NECK_PAIN_.2.aspx.
ascending and descending stairs, epi- foramina as well as increased space for
sodes of the leg or legs giving way while the compressed nerve roots. Patients
standing, or slapping of the foot while often report improved pain with bend-
walking, which typically indicates a ing over on the commode or leaning
footdrop and L5 nerve root involvement. forward against a shopping cart, a well-
Sensory changes may be reported as known phenomenon referred to as the
numbness, tingling, cold sensations, grocery cart sign.
electric shocks, or severe burning pains.
Other sensations that may be reported Red Flags
include the feeling of water running Although serious spinal pathology is
down the leg or a “pop” in the lower rare in the primary care setting (less
back at onset followed by the gradual than 1%), the identification of red flags
development of radicular symptoms.13 for disorders such as cauda equina
Radicular pain is usually worsened by compression, cancer, and vertebral in-
factors that increase intrathoracic pres- fection remains key in the evaluation of
sure (eg, coughing, sneezing, or the patients with low back pain (Table 6-2).16
Valsalva maneuver). Neurologic red flags include bowel/
Neurogenic claudication, also known bladder changes and severe or rapidly
as pseudoclaudication, commonly oc- progressive sensory or motor deficits. A
curs in lumbar spinal stenosis and is history of bilateral asymmetric leg
characterized by pain, cramps, or weak- weakness in the presence of urinary
ness that radiates down one or both retention is especially concerning for
lower extremities. Symptoms worsen cauda equina involvement, which re-
with walking or standing and are imme- quires urgent imaging studies and
diately relieved with rest or flexion of surgical evaluation.
the spine forward, which results in Recent systematic reviews found
enlargement of the spinal canal and that a prior history of cancer had the
470 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
all positions, and unexplained weight h A prior history of cancer
TABLE 6-2 Red Flags in the loss. Epidural abscess and other verte- has the highest
Evaluation of Acute bral infections should be suspected in predictive value for
Low Back Pain
the setting of fever, recent infection, detection of malignancy
or IV drug use, although patients who even in the absence of
b Neurologic
are diabetic or otherwise immuno- other red flags.
Red flags for cauda equina compromised may present without h Compression fractures
compression fever. Compression fractures are asso- are associated with
Bowel/bladder disturbances ciated with older age, acute trauma, older age, acute trauma,
Saddle anesthesia
and chronic steroid use. Of note, the and chronic steroid use.
determination to proceed with further
Bilateral asymmetric deficits testing should be based on the pres-
Red flags for severe neurologic ence of a combination of positive red
involvement flags and clinical judgment due to low
Rapidly progressive deficits predictive values of individual risk
factors (with the exception of prior
Multilevel or bilateral
involvement cancer history) (Case 6<1).16,17
A careful history is also important to
Prominent motor weakness
evaluate for an underlying systemic
(eg, footdrop or hip flexion
weakness) disorder that may present with low back
pain. Questions regarding abdominal
b Non-neurologic
and urinary tract symptoms should be
Red flags for cancer posed since intraabdominal/pelvic pa-
Prior history of cancer thology may present with referred pain
to the back. Diffusely reduced mobility
Unexplained weight loss
of the neck and back may be sugges-
Pain in supine position tive of an inflammatory spondylo-
More than 50 years of age arthropathy. Other questions to ask
include whether or not the patient
Pain duration longer than
1 month has a prior history of back pain as this
is the strongest risk factor for an acute
Red flags for spinal fracture
episode.18 Along these lines, infor-
Chronic corticosteroid use mation on previous imaging study
More than 70 years of age findings and treatments tried should
be obtained. A history of more re-
Trauma
mote trauma or recent strenuous
Red flags for spinal infection physical activity may also be impor-
Fever tant. While this may not establish the
specific source of the pain, it may
Recent infection
point toward a mechanical cause
IV drug use rather than an underlying systemic
IV = intravenous. disorder (eg, malignancy), although
some patients will not recall an
inciting event and report that they
highest predictive value for detection simply woke up with the symptoms.
of malignancy even in the absence of Information regarding psychosocial
other red flags.16,17 Other risk factors factors, worker’s compensation claims,
for cancer include failure to improve and substance abuse may also be help-
after 1 month, pain that is present in ful in predicting evolution to chronic
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 471
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
Case 6<1
A 57-year-old woman who was previously healthy presented with a 4-month history of intermittent low
back pain that had become worse over the last 2 weeks. Prior to onset, the patient had carried a suitcase
down the stairs and later that day had developed severe right-sided lower back pain that self-resolved
after 2 weeks. The pain recurred 2 months later after the patient again lifted something heavy, but these
symptoms also improved. Then 2 weeks before presentation, the severe pain returned, accompanied by
new burning paresthesia down the right buttock and posterior thigh as well as progressive difficulty
walking. The pain was much worse than before and
was not relieved by ibuprofen or any positional changes.
In fact, she had been unable to sleep well for the
last 2 weeks because of pain while lying down at night.
She denied any trauma or preceding illnesses.
Examination showed right-sided gastrocnemius
weakness and a reduced right ankle deep tendon reflex.
Lumbar MRI without gadolinium demonstrated
compression fracture deformities of the T12 and L5
vertebral bodies with diffusely abnormal signal
throughout the spine and bilateral sacrum (Figure 6-2).
Further evaluation revealed evidence of multiple
myeloma with a small soft tissue mass extending into
the S1 neural foramina on the right, resulting in nerve
root impingement. The patient underwent extensive
chemotherapy with aggressive pain management and
was in remission 2 years later.
Comment. Although the first two episodes of low
back pain may have been triggered by heavy lifting and
appeared musculoskeletal in nature, the third episode
was radicular and accompanied by red flags that
included pain present in all positions and progressive
neurologic deficits. Furthermore, the neurologic
examination was consistent with a right-sided S1
radiculopathy with significant motor weakness. Early
MRI was thus warranted and revealed changes FIGURE 6-2 Imaging of the patient in Case 6-1.
Sagittal short tau inversion recovery
consistent with malignancy. Disease-appropriate (STIR) MRI demonstrates compression
therapy was initiated with resultant stabilization of fracture deformities of the T12 and L5 vertebral
the patient. bodies (solid arrows) with diffusely abnormal signal
throughout the spinous processes (dashed arrows).
low back pain that may be refractory to dermatome. Similarly, patients may
multiple treatment modalities. demonstrate a myotomal pattern of
weakness, although the motor exami-
PHYSICAL EXAMINATION nation is often confounded by guarding
In conjunction with the history, a or giveway weakness due to pain.
careful neurologic examination can help Despite these limitations, every effort
establish the presence of radicular dis- should be made to test the strength of
ease and localize the lesion (Table 6-1). individual muscles within L2 to S1 myo-
With neurologic involvement, sensory tomes, particularly those innervated
loss or hyperesthesia to pinprick and by the L5 and S1 nerve roots as these
light touch may occur within a specific levels are affected in 95% of lumbar-disk
472 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
herniations.12,19 Strength testing of The neurologic examination may be h Patients with reported
ankle dorsiflexion (L5), great toe exten- further augmented by specific maneu- bowel/bladder
sion (L5 to S1), knee flexion (L5 to S1), vers that can help detect the presence dysfunction should be
hip flexion (L2 to L4), and knee exten- of radicular disease and are easily assessed for rectal tone,
sion (L2 to L4) constitutes a basic motor performed at the bedside. anal wink reflex, and
examination. Evaluation of deep tendon saddle anesthesia to
reflexes, which are unaffected by pain Straight LegYRaising Test evaluate for cauda
and patient effort, is also important as The straight legYraising test is carried equina compression.
the asymmetric absence of a knee (L2 out with the patient in the supine h Patients with lumbar
to L4) or ankle reflex (S1) may serve as position while the examiner raises the spinal stenosis may flex
the only objective neurologic finding on leg on the affected side with the knee forward at the trunk
an otherwise normal examination. extended (Figure 6-3). The test is pos- while walking (grocery
However, deep tendon reflexes may itive and suggestive of L5 or S1 nerve cart sign) to increase the
be absent in patients older than the root compression if radicular symptoms diameter of the spinal
canal and relieve nerve
age of 60 (absent ankle jerks) and in are reproduced or worsened when the
root compression.
patients with prior back surgery or knee leg reaches an angle between 30 de-
replacement. Patients with reported grees and 70 degrees. An increase in
bowel/bladder dysfunction should be symptoms at less than 30 degrees may
assessed for rectal tone, anal wink be nonphysiologic, while pain present
reflex, and saddle anesthesia to evalu- at greater than 70 degrees may occur in
ate for cauda equina dysfunction. normal individuals and is unlikely to be
Valuable information can also be clinically relevant. This test may also be
obtained from the gait examination. As performed with the patient sitting. Pain
described previously, patients with lum- present only when the patient is su-
bar spinal stenosis may demonstrate pine, but not when sitting up (with leg
forward flexion of the trunk while raised), suggests a nonorganic etiology.20
walking (grocery cart sign) to increase
the diameter of the spinal canal and Crossed Straight-Leg Raising Test
relieve compression. A Trendelenburg During the crossed straight-leg raising
gait may be seen in patients with hip test, pain is reproduced when the con-
abduction weakness due to L5 nerve tralateral or unaffected leg is raised with
root compression or primary hip pa- the knee extended. This is a more
thology. Because of the weakened specific test for disk herniation than
pelvic muscles on the affected side, the ipsilateral straight legYraising test,
the patient overcompensates by placing but is not as sensitive.
more weight on the contralateral leg
while taking a step forward with the Bragard Sign
affected one, resulting in a lowered The Bragard sign is another variation of
hip on the unaffected side while the straight legYraising test in which the
walking. Stressed gait testing, in which examiner dorsiflexes the patient’s foot
patients are asked to walk on their at the point when the patient begins
toes and heels, may be more sensitive to experience pain as the leg is being
than direct manual testing of ankle raised (Figure 6-4). This further in-
plantar flexion and dorsiflexion. The creases the nerve root tension and re-
inability to walk on the toes points sults in worsening pain.
toward gastrocnemius (S1) weakness,
whereas difficulty heel walking may Femoral Stretch Test
indicate footdrop and tibialis anterior The femoral stretch test is carried out
(L5) weakness. with the patient in a prone position while
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 473
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
FIGURE 6-3 Straight legYraising test. With the patient in the
supine position, the examiner raises the leg on
the affected side with the knee extended.
The test is positive if radicular symptoms are reproduced or
worsened when the leg reaches an angle between 30 degrees
and 70 degrees.
the affected leg is gently lifted off the [FABER] test) is carried out while the
table and then flexed at the knee patient is supine and the lateral ankle of
(Figure 6-5). Pain in the anterior thigh the affected leg is placed on the contra-
may indicate L2 to L4 root compression. lateral knee. The affected knee is then
slowly brought down to the examina-
Patrick Test tion table (Figure 6-6). Pain during this
The Patrick test (also known as the maneuver is suggestive of pathology in
flexion, abduction, external rotation the hip or sacroiliac joint.
FIGURE 6-4 Bragard sign. The examiner dorsiflexes the
patient’s foot at the point when the patient
begins to experience pain as the leg is being
raised. Worsening pain may indicate increased
nerve root tension.
474 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
FIGURE 6-5 Femoral stretch test. With the patient in a
prone position, the affected leg is gently
lifted off the table and then flexed at
the knee. Pain in the anterior thigh may indicate L2 to
L4 root compression.
General Physical Examination lesions consistent with zoster infection,
A general examination should also be while tufts of hair in the sacral region
performed to look for evidence of a may be indicative of an underlying
systemic etiology or more serious spine vertebral anomaly. Local tenderness
pathology. Tenderness or masses felt over the spine is nonspecific and may
on palpation of the abdomen may occur in numerous disorders, but may
indicate intraabdominal pathology, indicate a vertebral compression frac-
whereas flank tenderness suggests gen- ture in the presence of kyphosis and a
itourinary tract disease. As noted previ- history of sudden back pain with well-
ously, fever may indicate the presence defined onset. A focal muscle mass in
of infection but is often absent in the spinal region may appear to be a
patients with epidural abscess. Inspec- muscle spasm, but it may actually
tion of the skin may reveal herpetic represent local myoedema, as one
FIGURE 6-6 Patrick test (flexion, abduction, external rotation
[FABER] test). While the patient is supine, the
lateral ankle of the affected leg is placed on
the contralateral knee. The affected knee is then slowly brought
down to the examination table. Pain during this maneuver is
suggestive of pathology in the hip or sacroiliac joint.
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 475
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
KEY POINTS
h The presence of multiple study found that the mass is electrically that they may be predictive of treat-
nonphysiologic findings silent with needle EMG examination.9,21 ment outcome in specific settings.23Y26
suggests a nonorganic
etiology that may be Nonphysiologic Back Pain DIAGNOSTIC STUDIES
due to secondary gain, While some degree of pain-related A number of diagnostic tests may be
psychosocial issues, or giveway weakness or exaggerated find- helpful in the evaluation of low back
other factors. ings may be seen in patients with true pain, especially when performed at the
h In the absence of red spine pathology, other more objective appropriate time.
flags, imaging studies signs may sometimes be found on the
should not be obtained examination that do support the pres- Imaging Guidelines
in patients with low ence of a structural and symptomatic According to guidelines set by the
back pain of a duration lesion. However, the presence of mul- American College of Physicians and
of less than 6 weeks. tiple nonphysiologic findings sug- American Academy of Family Physi-
gests a nonorganic etiology that may cians, in the absence of red flags,
be due to secondary gain, psychoso- imaging studies should not be obtained
cial issues, or other factors. In a classic in patients with low back pain of less
but controversial study, Waddell 22 than 6 weeks duration.27,28 Specifically,
established five signs that can be unless there is evidence of progressive
elicited in the office and used as a or severe neurologic deficits, fever,
screening tool to identify patients with acute trauma, sudden back pain with
nonorganic low back pain (Table 6-3). spinal tenderness, or a strong clinical
Of these signs, overreaction was thought suspicion for an underlying systemic
to be most important, although non- disorder, early imaging studies are not
physiologic tenderness over the spine warranted and result in increased costs
was more common in some of the study and possibly unnecessary surgery. These
groups.22 A patient has a positive recommendations are based on system-
screen if three of the five signs are atic reviews and individual studies that
present. Subsequent analyses of the found no significant change in out-
original study have resulted in mixed comes, clinical decision making, or
findings regarding the validity of these patient satisfaction scores when early
signs, although a few studies have shown imaging was performed in patients with
a
TABLE 6-3 Signs Indicating Nonorganic Causes of Low Back Pain
b Overreaction to the examination
b Tenderness to light touch (eg, slight pinch in the lower back)
b Nonlocalizable tenderness that is distributed over a wide area
b Exacerbation of pain with placement of pressure on top of head
b Exacerbation of pain with simulated rotation of spine
b Giveway weakness of multiple muscles
b Nondermatomal sensory changes
b Distraction (pain present with direct straight legYraising test, but not when
leg is raised for plantar reflex evaluation)
a
Data from Waddell G, Spine (Phila Pa 1976).22 journals.lww.com/spinejournal/Abstract/1987/
09000/1987_Volvo_Award_in_Clinical_Sciences__A_New.2.aspx.
476 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINT
low back pain.27,29Y32 Some studies even meningeal disease is suspected. Be- h MRI of the lumbar spine
reported a tendency toward a more cause of the increased resolution, is the study of choice for
favorable outcome at 3 months and however, incidental degenerative spine neurologic back pain
increased sense of well-being for those changes unrelated to the pain are com- because it allows for
who underwent conservative care with- monly seen. In one systematic review, optimal visualization of
out imaging studies compared to those disk degeneration was seen in more than the conus medullaris,
who did have early imaging.27,30,32 one-third of asymptomatic 20-year-old nerve roots, and
Other considerations include the risks individuals with a 12% to 16% increase intervertebral disks.
of radiation exposure that accompany in prevalence per decade up to the age
the use of routine imaging studies. of 50 years; the increase was more
gradual in the older population, reach-
Lumbar Radiography ing 96% in 80-year-old patients.34
Although plain film radiography of the CT may be more sensitive than MRI in
lumbar spine is readily available and detecting bony abnormalities and frac-
cheaper than more advanced imaging tures but is inferior in visualization of the
studies, the information provided is neural structures. CT is usually reserved
limited to the bony spine and its for patients with contraindications for
alignment. In the setting of acute MRI, such as in patients who have im-
trauma, diffuse vertebral disease (eg, planted devices that are MRI incompat-
ankylosing spondylitis), or when risk ible or in those with a history of metallic
factors are present for spinal fracture, hardware from prior spine surgeries
the use of plain films may be warranted. that may result in marked artifact.
However, the sensitivity for malignancy
or infection is low.33 Another drawback Computed Tomography
is that a significant risk of radiation Myelography
exposure exists, particularly in women CT myelography is also not as sensi-
because of the proximity of the repro- tive as MRI for detection of nerve root
ductive organs. It is estimated that the or spinal cord lesions and is a more
radiation exposure to female gonads invasive procedure with significant
from a single plain film of the lumbar risks for complications and radiation
spine is equivalent to that of having a exposure. However, in preparation for
daily chest radiograph for several surgery it may be complementary, espe-
years.27,32 Flexion/extension plain films cially if metallic hardware exists from
may provide additional information on prior surgeries that obscures visualiza-
stability, but these are usually reserved tion of the anatomy on MRI.
for surgical evaluation.
Electromyography
Magnetic Resonance Imaging EMG is a valuable tool in the evaluation
and Computed Tomography of patients with radiculopathy as it can
MRI of the lumbar spine is the study of confirm its presence and help deter-
choice for neurologic back pain be- mine localization, acuity, and severity of
cause it allows for optimal visualiza- the nerve root lesion. The needle ex-
tion of the spinal cord (specifically the amination is the most important part of
conus medullaris), nerve roots, and the study as the demonstration of
intervertebral disks (Figure 6-7). It is fibrillation potentials in a myotomal
also recommended over other studies distribution and paraspinal muscles is
when cancer and infection are sus- the main method of identifying an
pected.32 Gadolinium is typically not active radiculopathy. Of note, however,
necessary unless intradural or lepto- abnormalities isolated to the paraspinal
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 477
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
KEY POINT
h The demonstration of
fibrillation potentials in
a myotomal distribution
on needle EMG is
the main method
of identifying an
active radiculopathy.
FIGURE 6-7 MRI showing spinal canal stenosis. A, Sagittal T2-weighted MRI of the
lumbar spine shows multilevel degenerative changes most severe at
L2–L3 with facet and ligamentous hypertrophy as well as a central disk
herniation resulting in severe central canal narrowing (white arrows). B, This is further
demonstrated on the axial image, which also shows bilateral severe neural foraminal
narrowing (red arrow points to the left foraminal stenosis).
muscles are insufficient for the diag- degenerative spine pathology cannot
nosis of radiculopathy as fibrillation be directly evaluated with routine nerve
potentials can be seen in asymptomatic conduction studies. Also, the needle
individuals (eg, older patients) or those examination should not be performed
with a history of spine surgery given the within 3 to 4 weeks of symptom onset
possibility of local incisional denerva- as this is insufficient time for develop-
tion. Conversely, the absence of fibril- ment of fibrillation potentials. EMG is
lation potentials does not exclude the best used in patients with muscle weak-
possibility of a radiculopathy due to ness, prior surgery, acute on chronic
overlap in innervation, sampling error, disease, multilevel root involvement, or
and reinnervation. Although nerve con- when an alternative or superimposed
duction studies are not as critical as the diagnosis is being considered.
needle examination in a radiculopathy
evaluation, an absent H reflex may help Other Studies
in pointing toward an S1 lesion. For patients with suspected malignancy
EMG can also exclude the possibility or an underlying systemic disorder,
of potential mimics such as a general- erythrocyte sedimentation rate, complete
ized polyneuropathy or focal mononeuro- blood cell count, urinalysis, and other
pathy. However, because of technical disease-appropriate laboratory studies
considerations, a radicular lesion that should be considered. However, these
affects sensory fibers in isolation (eg, tests are not part of the routine evaluation.
sensory radiculopathy) cannot be
detected with this procedure. This is TREATMENT
because the intraspinal canal portion of For patients presenting with acute low
the sensory nerve root that would be back pain with or without radicu-
affected by a disk herniation or other lopathy, the main goals of treatment
478 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
are pain control and preservation of heavy lifting (nothing more than a h In the absence of red
function. In the absence of red flags, gallon of milk) and other exertional flags, conservative
which would require the initiation of activities that can aggravate the pain management for most
urgent disease-appropriate treatment, during the acute pain period. Educa- cases of acute low back
conservative management for most tion and reassurance that up to 70% pain is supported by a
cases of acute low back pain is sup- to 90% of cases do improve with time favorable prognosis
ported by a favorable prognosis regard- are an important part of the initial regardless of pain type.
less of pain type, although recurrence visit as well (Figure 6-8).37,38 h Non-narcotic oral
rates range from 23% to 80%.3,35 Follow-up at 4 weeks with reas- analgesics and a return
sessment for the emergence of red to usual activity are
Musculoskeletal Low Back Pain flags may be done for patients with the primary
Non-narcotic oral analgesics (eg, non- persistent symptoms. If none are iden- recommendations for
steroidal anti-inflammatory drugs tified, continued conservative care early treatment of
[NSAIDs] and muscle relaxants) and with the addition of physical therapy acute musculoskeletal
back pain.
a return to usual activity (mobiliza- that includes back-strengthening exer-
tion) are the primary recommendations cises and spinal manipulation may be
for early treatment of acute musculo- considered. However, a recent study
skeletal back pain (Table 6-4). For found no meaningful benefit when
those with severe pain, short periods physical therapy was performed dur-
of bed rest (1 to 2 hours at a time) ing the acute phase (first 4 weeks)
may be needed but should be mini- compared to usual care.39 Massage
mized, as studies have shown that pa- therapy (short-term benefit) may also
tients who are told to remain active be helpful. If no recovery is seen at 6
report improved pain relief and func- to 8 weeks, the patient should again
tional status compared to those who be reevaluated for red flags with
are recommended bed rest.36 Also, pa- consideration of imaging studies at
tients should be instructed to avoid that time. For symptomatic relief,
TABLE 6-4 Conservative Treatment for Acute Low Back Pain
b Medications (Level of Evidencea)
Nonsteroidal anti-inflammatory drugs (good)
Muscle relaxants (good)
Applied heat (moderate)
Antiepileptic drugsb: gabapentin and topiramate (moderate)
Acetaminophen (limited)
b Self-Care
Return to usual activity/mobilization
Short periods of bed rest (1 to 2 hours maximum) if pain is severe
Avoid heavy lifting (nothing heavier than a gallon of milk)
Lumbar support pillow for travel
a
Rating system based on expert panel review: Good = multiple high-quality studies; moderate =
at least one high-quality study; limited = at least one adequate study.
b
Recommended treatment for radiculopathy.
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 479
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
FIGURE 6-8 Treatment algorithm for acute low back pain.
AEDs = antiepileptic drugs; CT = computed tomography; EMG = electromyography;
MRI = magnetic resonance imaging; NSAIDs = nonsteroidal anti-inflammatory drugs.
480 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
switching to another non-narcotic sults vary depending on approach h Epidural steroids may
analgesic or a combination regimen used, therapeutic intervention chosen provide short-term pain
of medications and physical modali- for comparison, and baseline inclusion relief for radiculopathic
ties (eg, NSAIDs, massage, and yoga) criteria. More recently, epidural ste- pain, especially when
may be helpful. Otherwise, conserva- roid injections have come under close administered by a
tive care is continued. scrutiny because of rising health care transforaminal
costs and the 2012 fungal outbreak approach.
Radiculopathy related to contaminated compounded h Patients with
The natural history of radiculopathy is injectable methylprednisolone, which radiculopathy who fail to
similar to that of musculoskeletal low affected more than 700 patients.47 respond to any treat-
back pain, with a favorable outcome Reports of other serious side effects ment after
reported by 70% to 88% of patients at including paralysis, nerve damage, 6 weeks should be
3 months.40,41 It follows then that for and death have prompted the US reassessed for red flags
patients with radiculopathy who have Food and Drug Administration (FDA) and undergo MRI.
no significant motor weakness or red to add a warning label to epidural
flags, the treatment algorithm for steroid injection products.48 While a
acute musculoskeletal pain may be subset of patients may respond favor-
applied with additional therapeutic ably, given the lack of clear long-term
options such as the use of antiepi- benefit and potential risks of the
leptic medications for neuropathic pain. procedure, the routine use of epidural
Systematic reviews have shown that steroid injections is still considered
both gabapentin and topiramate resulted controversial and is not recommended
in improved pain compared to placebo as a first-line therapy for patients with
and were overall well tolerated.42 radiculopathy.
Systemic steroids may also be con- As in patients with musculoskel-
sidered, but most studies have shown etal low back pain, patients with ra-
no significant benefit in pain or disabil- diculopathy who fail to respond to
ity for patients with radiculopathy or any treatment after 6 weeks should
musculoskeletal low back pain. However, be reassessed for red flags and un-
a recent randomized trial that included dergo imaging studies, preferably MRI
269 patients with acute radiculopathy (Figure 6-8). If nondiagnostic, the
associated with a herniated disk found next step would be EMG. If the EMG
that a 15-day course of oral prednisone demonstrates a well-localized nerve
(60 mg, 40 mg, and 20 mg for 5 days root lesion with evidence of active
each) resulted in improved function at 3 motor axon loss changes, surgical
and 52 weeks, but no significant change evaluation may be considered. How-
in pain or long-term surgery rate.43 ever, if no evidence of correlating
On the other hand, epidural steroid structural pathology exists, then con-
injections have been found to provide tinued conservative management is
short-term pain relief (up to 3 months) recommended unless clinical worsen-
for radicular leg pain with an increased ing or persistence of severe pain and
likelihood of a positive response when sensory symptoms occurs. Clinical and
administered by a transforaminal ap- radiographic improvement is seen in
proach.44,45 Epidural steroid injections most patients with radiculopathy at
may also reduce short-term risk for 6 months to 1 year, with MRI studies
surgery compared to placebo.45,46 demonstrating spontaneous regression
However, interpretation of studies of herniated disk changes in as early
evaluating the benefit of epidural as 2 months.49,50 Of note, patients
steroid injections are difficult as re- with significant motor weakness (eg,
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 481
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
KEY POINTS
h The management of footdrop or hip flexor weakness) ered if a new or emerging pathology is
chronic low back pain should undergo early imaging studies suspected. Oral analgesics found to
should include a careful (at presentation) as surgical interven- be helpful include NSAIDs, antiepi-
review of previous tion may be needed to prevent perma- leptics (gabapentin and topiramate),
treatments and nent deficits. duloxetine, and muscle relaxants.42,53
responses as well as Botulinum toxin may also be an
an evaluation for Lumbar Spinal Stenosis option, as two randomized trials includ-
contributing psychosocial As chronic and progressive degenera- ing 81 patients with chronic low back
factors. tive changes are the main pathophysi- pain found that injection of botulinum
h According to an ology of spinal stenosis, the natural toxin A into the lumbar paraspinal
American Academy of history is somewhat less favorable than muscles resulted in improved pain at 3
Neurology position that seen with musculoskeletal or radic- to 4 weeks and again at 8 weeks com-
statement, the risks of ular back pain, although the severity of pared to normal saline injections.54,55
opioids in treating stenosis seen radiographically often The use of complementary and alter-
noncancerous low back
does not correlate with clinical findings. native medicine practices in chronic
pain outweigh
One study found that 70% of patients low back pain have also been studied
the benefits.
with spinal stenosis reported the same with benefits in pain or disability seen with
degree of symptoms at 4-year follow- yoga, massage, and acupuncture.56Y58
up, 15% clinically worsened, and the Short-term pain reduction has also been
remaining 15% showed improvement.51 seen with herbal preparations, specifi-
Medical management is challenging cally willow bark extract (containing
as most studies show little to no benefit salicin 120 mg/d to 240 mg/d orally)
for therapeutic modalities commonly and devil’s claw (containing harpagoside
used for low back pain. In combination 50 mg/d to 100 mg/d orally).59,60 How-
with other conservative measures, ever, these supplements are not regu-
gabapentin has a small effect on pain lated by the FDA, and their long-term
and on a patient’s ability to walk longer safety has not been established.
distances, and comprehensive physical While some studies have found that
therapy may result in perceived recov- opioids may provide short-term pain
ery, but a recent randomized trial relief for patients with chronic low back
showed no significant benefit with pain, no increased benefit has been
epidural steroid injections over epidural seen when compared to NSAIDs and
lidocaine alone in patients with spinal antidepressants.61 In addition, the po-
stenosis.11,52 Surgical evaluation is of- tential dangers of addiction and over-
ten warranted in patients with progres- dose are major concerns, which
sive or disabling symptoms. resulted in a position article from the
American Academy of Neurology
Chronic Low Back Pain (AAN) stating that the risks of opioids
The management of chronic low back in treating noncancerous low back pain
pain, which by definition persists for outweigh the benefits.62
more than 12 weeks, should include a Insufficient evidence exists to sup-
careful review of previous treatments port the use of radiofrequency ablation,
and responses as well as an evaluation acetaminophen, lidocaine patches, anti-
for contributing psychosocial factors, depressants other than duloxetine,
which may be addressed with referral spinal manipulation, Pilates, and trans-
to psychiatry and counseling. As with cutaneous electrical nerve stimulation
all types of back pain, an evaluation for chronic low back pain. However,
for red flags should also be performed, these therapies are generally safe when
and imaging studies should be consid- used as directed and may be considered
482 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
in refractory cases.53 Optimal treatment CONCLUSION h Current indications for
of chronic back pain consists of a Growing evidence suggests that low early surgery include
multidisciplinary approach that includes back pain in general should be con- cauda equina
an active exercise regimen, psychoso- sidered a chronic condition that is compression and
cial support, and cognitive-behavioral characterized by periodic relapses and radiculopathy with
therapy. A recent systematic review remissions. However, a systematic ap- rapidly progressive or
found that a “biopsychosocial” ap- proach that incorporates a careful his- severe neurologic
proach to the treatment of low back tory and neurologic examination with deficits.
pain, which includes all of these com- evidence-based guidelines can result in h For patients with
ponents, was more effective than stan- optimal care for the patient and a musculoskeletal back
dard exercise therapy, usual care, and positive impact on society. pain associated with
normal activities.63 Risk factors associ- nonspecific degenerative
ated with transformation from acute to changes, response to
REFERENCES surgery has been found
chronic back pain include psychosocial 1. Burke JF, Skolarus LE, Callaghan BC, Kerber to be no different than
factors (anxiety, depression, job dissat- KA. Choosing Wisely: highest-cost tests in
intensive rehabilitation,
isfaction), pending litigation, worker’s outpatient neurology. Ann Neurol
2013;73(5):679Y683. doi:10.1002/ana.23865. but is slightly superior to
compensation claims, tobacco use, and standard care.
prior history of low back pain.64,65 2. National Center for Health Statistics. Health,
United States, 2013: with special feature on
prescription drugs. Hyattsville, MD. 2014.
Surgery cdc.gov/nchs/data/hus/hus13.pdf. Accessed
Current indications for early surgery February 1, 2017.
include cauda equina compression and 3. Hoy D, Bain C, Williams G, et al. A systematic
radiculopathy with rapidly progressive review of the global prevalence of low back
pain. Arthritis Rheum 2012;64(6):2028Y2037.
or severe neurologic deficits. Surgery doi:10.1002/art.34347.
may also be considered in patients with
4. Balagué F, Mannion AF, Pellisé F, Cedraschi C.
spinal stenosis, as systematic reviews Non-specific low back pain. Lancet
suggest that surgical decompression 2012;379(9814):482Y491. doi:10.1016/
results in better outcomes than non- S0140<6736(11)60610<7.
operative management, although re- 5. Konstantinou K, Dunn KM. Sciatica: review
sults are mixed and confounded by of epidemiological studies and prevalence
estimates. Spine (Phila Pa 1976)
marked crossover rates.66,67 Patients 2008;33(22):2464Y2472. doi:10.1097/
with radiculopathy who have milder BRS.0b013e318183a4a2.
deficits associated with a structural 6. Deyo RA, Weinstein JN. Low back pain. N
lesion on MRI or active denervation Engl J Med 2001;344(5):363Y370.
on EMG who fail to respond to doi:10.1056/NEJM200102013440508.
conservative treatment at 4 to 6 weeks 7. Global Burden of Disease Study 2013
Collaborators. Global, regional, and national
may be referred for surgery as well. For
incidence, prevalence, and years lived
patients with musculoskeletal back with disability for 301 acute and chronic
pain associated with nonspecific de- diseases and injuries in 188 countries,
generative changes, response to sur- 1990Y2013: a systematic analysis for the
Global Burden of Disease Study 2013. Lancet
gery has been found to be no different 2015;386(9995):743Y800. doi:10.1016/
than intensive rehabilitation, but is S0140<6736(15)60692<4.
slightly superior to standard care.68 8. Katz JN. Lumbar disc disorders and low-back
Surgical approaches vary depending pain: socioeconomic factors and consequences.
on the pathology and degree of struc- J Bone Joint Surg Am 2006;88(suppl 2):21Y24.
doi:10.2106/JBJS.E.01273.
tural changes, but most patients with
9. Levin KH, Covington EC, Devereaux MW,
spinal stenosis undergo decompressive
et al. Low back and neck pain. Continuum
laminectomy, whereas diskectomy is (Minneap Minn) 2001;7(1 Neck and Back
performed for herniated disks. Pain):7Y43.
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 483
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
10. Koes BW, van Tulder MW, Peul WC. Philadelphia, PA: Lippincott
Diagnosis and treatment of sciatica. BMJ Williams & Wilkins, 2005.
2007;334(7607):1313Y1317. doi:10.1136/
bmj.39223.428495.BE. 21. Johnson EW. The myth of skeletal muscle
spasm. Am J Phys Med Rehab 1989;68(1):1.
11. Genevay S, Atlas SJ. Lumbar spinal stenosis.
Best Pract Res Clin Rheumatol 22. Waddell G. 1987 Volvo award in clinical
2010;24(2):253Y265. doi:10.1016/ sciences. A new clinical model for the
j.berh.2009.11.001. treatment of low-back pain. Spine
(Phila Pa 1976)1987;12(7):632Y644.
12. Deyo RA, Gray DT, Kreuter W, et al. United
States trends in lumbar fusion surgery for 23. Apeldoorn AT, Bosselaar H, Blom-Luberti T,
degenerative conditions. Spine (Phila Pa et al. The reliability of nonorganic
1976) 2005;30(12):1441Y1445. doi:10.1097/ sign-testing and the Waddell score in
01.brs.0000166503.37969.8a. patients with chronic low back pain. Spine
2008;33(7):821Y826. doi:10.1097/
13. Hooten WM, Cohen SP. Evaluation BRS.0b013e318169502a.
and treatment of low back pain: a
clinically focused review for primary 24. Fishbain DA, Cole B, Cutler RB, et al. A
care specialists. Mayo Clin Proc structured evidence-based review on the
2015;90(12):1699Y1718. doi:10.1016/ meaning of nonorganic physical signs:
j.mayocp.2015.10.009. Waddell signs. Pain Med 2003;4(2):141Y181.
doi:10.1046/j.1526<4637.2003.03015.x.
14. Laslett M, McDonald B, Aprill CN, et al.
Clinical predictors of screening lumbar 25. Werneke MW, Harris DE, Lichter RL. Clinical
zygapophyseal joint blocks: development effectiveness of behavioral signs for
of clinical prediction rules. Spine J screening chronic low-back pain patients in
2006;6(4):370Y379. doi:10.1016/ a work-oriented physical rehabilitation
j.spinee.2006.01.004. program. Spine 1993;18(16):2412Y2418.
15. Young S, Aprill C, Laslett M. Correlation of 26. Gaines WG, Hegmann KT. Effectiveness of
clinical examination characteristics with Waddell’s nonorganic signs in predicting a
three sources of chronic low back pain. delayed return to regular work in patients
Spine J 2003;3(6):460Y465. doi:10.1016/ experiencing acute occupational low back
S1529<9430(03)00151<7. pain. Spine (Phila Pa 1976) 1999;24(4):
396Y400. doi:10.1097/00007632<
16. Henschke N, Maher CG, Refshauge KM, et al.
199902150<00021.
Prevalence of and screening for serious
27. Chou R, Qaseem A, Owens DK, et al.
spinal pathology in patients presenting to
Diagnostic imaging for low back pain:
primary care settings with acute low back
advice for high-value health care from the
pain. Arthritis Rheum 2009;60(10):
American College of Physicians. Ann Intern
3072Y3080. doi:10.1002/art.24853.
Med 2011;154(3):181Y189. doi:10.7326/
17. Downie A, Williams CM, Henschke N, et al. 0003<4819<154<3<201102010<00008.
Red flags to screen for malignancy and 28. Choosing wisely. Fifteen things physicians
fracture in patients with low back pain: and patients should question. aafp.org/dam/
systematic review. BMJ 2013;347:f7095. AAFP/documents/about_us/initiatives/
doi:10.1136/bmj.f7095. choosing-wisely-fifteen-questions.pdf.
18. Papageorgiou AC, Croft PR, Thomas E, et al. Accessed February 1, 2017.
Influence of previous pain experience on 29. Modic MT, Obuchowski NA, Ross JS, et al.
the episode incidence of low back pain: Acute low back pain and radiculopathy:
results from the South Manchester Back MR imaging findings and their prognostic
Pain Study. Pain 1996;66(2Y3):181Y185. role and effect on outcome. Radiology
doi:10.1016/0304<3959(96)03022<9. 2005;237(2):597Y604. doi:10.1148/
radiol.2372041509.
19. Deyo RA, Rainville J, Kent DL. What can the
history and physical examination tell us 30. Jarvik JG, Deyo RA. Diagnostic evaluation
about low back pain? JAMA of low back pain with emphasis on imaging.
1992;268(6):760Y765. doi:10.1001/ Ann Intern Med 2002;137(7):586Y597.
jama.1992.03490060092030. doi:10.7326/0003<4819<137<7<200210010<00010.
20. Campbell WW, DeJong RN, 31. Ash LM, Modic MT, Obuchowski NA, et al.
Haerer AF, eds. Incorporating the Effects of diagnostic information, per se, on
fundamentals of neuroanatomy and patient outcomes in acute radiculopathy and
neurophysiology. In: Dejong’s the low back pain. AJNR Am J Neuroradiol
neurologic examination. 6th edition. 2008;29(6):1098Y1103. doi:10.3174/ajnr.A0999.
484 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
32. Chouposition R, Fu R, Carrino JA, Deyo RA. back pain: a review of the evidence for
Imaging strategies for low-back pain: an American Pain Society/American
systematic review and meta-analysis. College of Physicians clinical practice
Lancet 2009;373(9662):463Y472. doi:10.1016/ guideline. Ann Intern Med 2007;147(7):
S0140<6736(09)60172<0. 505Y514. doi:10.7326/0003<4819<147<
33. Deyo RA, Diehl AK. Cancer as a cause of 7<200710020<00008.
back pain: frequency, clinical presentation, 43. Goldberg H, Firtch W, Tyburski M, et al. Oral
and diagnostic strategies. J Gen Intern Med steroids for acute radiculopathy due to a
1988;3(3):230Y238. doi:10.1007/BF02596337. herniated lumbar disk: a randomized clinical
trial. JAMA 2015;313(19):1915Y1923.
34. Brinjikji W, Luetmer PH, Comstock B, et al.
doi:10.1001/jama.2015.4468.
Systematic literature review of imaging
features of spinal degeneration in 44. Cohen SP, Bicket MC, Jamison D, et al.
asymptomatic populations. AJNR Am J Epidural steroids: a comprehensive,
Neuroradiol 2015;36(4):811Y816. evidence-based review. Reg Anesth Pain
doi:10.3174/ajnr.A4173. Med 2013;38(3):175Y200. doi:10.1097/
35. Stanton TR, Henschke N, Maher CG, AAP.0b013e31828ea086.
et al. After an episode of acute 45. Chou R, Hashimoto R, Friedly J, et al.
low back pain, recurrence is unpredictable Epidural corticosteroid injections for
and not as common as previously radiculopathy and spinal stenosis: a
thought. Spine (Phila Pa 1976) systematic review and meta-analysis. Ann
2008;33(26):2923Y2928. doi:10.1097/ Intern Med 2015;163(5):373Y381.
BRS.0b013e31818a3167. doi:10.7326/M15<0934.
36. Dahm KT, Brurberg KG, Jamtvedt G, Hagen
46. Riew KD, Yin Y, Gilula L, et al. The effect of
KB. Advice to rest in bed versus advice to stay
nerve-root injections on the need for opera-
active for acute low-back pain and sciatica.
tive treatment of lumbar radicular pain. A
Cochrane Database Syst Rev 2010;(6):CD007612.
prospective, randomized, controlled,
doi:10.1002/14651858.CD007612.pub2.
double-blind study. J Bone Joint Surg Am
37. Henschke N, Maher CG, Refshauge KM, et al. 2000;82-A(11):1589Y1593.
Prognosis in patients with recent onset low
47. Smith RM, Schaefer MK, Kainer MA, et al.
back pain in Australian primary care:
Fungal infections associated with
inception cohort study. BMJ 2008;337:a171.
contaminated methylprednisolone
doi:10.1136/bmj.a171.
injections. N Engl J Med 2013;369(17):
38. Coste J, Delecoeuillerie G, Cohen de Lara A, et al. 1598Y1609. doi:10.1056/NEJMoa1213978.
Clinical course and prognostic factors in
acute low back pain: an inception cohort 48. Andersson GB. Epidural glucocorticoid
study in primary care practice. BMJ injections in patients with lumbar spinal
1994;308(6928):577Y580. doi:10.1136/ stenosis. N Engl J Med 2014;371(1):75Y76.
bmj.308.6928.577. doi:10.1056/NEJMe1405475.
39. Fritz JM, Magel JS, McFadden M, et al. Early 49. Komori H, Shinomiya K, Nakai O, et al.
physical therapy vs usual care in patients The natural history of herniated nucleus
with recent-onset low back pain: a pulposus with radiculopathy. Spine
randomized clinical trial. JAMA 2015;314(14): (Phila Pa 1976) 1996;21(2):225Y229.
1459Y1467. doi:10.1001/jama.2015.11648. 50. Autio RA, Karppinen J, Niinimäki J, et al.
40. Weber H, Holme I, Amlie E. The natural Determinants of spontaneous resorption of
course of acute sciatica with nerve intervertebral disc herniations. Spine (Phila
root symptoms in a double-blind Pa 1976) 2006;31(11):1247Y1252.
placebo-controlled trial evaluating the
effect of piroxicam. Spine (Phila Pa 1976) 51. Johnsson KE, Rosén I, Udén A. The natural
1993;18(11):1433Y1438. course of lumbar spinal stenosis. Clin Orthop
Relat Res 1992;(279):82Y86.
41. Takada E, Takahashi M, Shimada K.
Natural history of lumbar disc hernia 52. Friedly JL, Comstock BA, Turner JA, et al. A
with radicular leg pain: spontaneous MRI randomized trial of epidural glucocorticoid
changes of the herniated mass and injections for spinal stenosis. N Engl J Med
correlation with clinical outcome. J Orthop 2014;371(1):11Y21. doi:10.1056/
Surg (Hong Kong) 2001;9(1):1Y7. NEJMoa1313265.
42. Chou R, Huffman LH; American Pain 53. Herndon CM, Zoberi KS, Gardner BJ.
Society; American College of Physicians. Common questions about chronic low back
Medications for acute and chronic low pain. Am Fam Physician 2015;91(10):708Y714.
Continuum (Minneap Minn) 2017;23(2):467–486 ContinuumJournal.com 485
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Low Back Pain
54. Foster L, Clapp L, Erickson M, Jabbari B. 61. Chaparro LE, Furlan AD, Deshpande A, et al.
Botulinum toxin A and chronic low back Opioids compared to placebo or other
pain: a randomized, double-blind study. treatments for chronic low-back pain.
Neurology 2001;56(10):1290Y1293. Cochrane Database Syst Rev
doi:10.1212/WNL.56.10.1290. 2013;(8):CD004959. doi:10.1002/
14651858.CD004959.pub4.
55. Jazayeri SM, Ashraf A, Fini HM, et al. Efficacy
of botulinum toxin type a for treating 62. Franklin GM; American Academy of
chronic low back pain. Anesth Pain Med Neurology. Opioids for chronic noncancer
2011;1(2):77Y80. doi:10.5812/ pain: a position paper of the American
kowsar.22287523.1845. Academy of Neurology. Neurology
2014;83(14):1277Y1284. doi:10.1212/
56. Cherkin DC, Eisenberg D, Sherman KJ, et al.
WNL.0000000000000839.
Randomized trial comparing traditional
Chinese medical acupuncture, therapeutic 63. Kamper SJ, Apeldoorn AT, Chiarotto A, et al.
massage, and self-care education for chronic Multidisciplinary biopsychosocial rehabilitation
low back pain. Arch Intern Med for chronic low back pain. Cochrane Database
2001;161(8):1081Y1088. doi:10.1001/ Syst Rev 2014;9:CD000963. doi:10.1002/
archinte.161.8.1081. 14651858.CD000963.pub3.
57. Sherman KJ, Cherkin DC, Erro J, et al. 64. Thomas E, Silman AJ, Croft PR, et al.
Comparing yoga, exercise, and a self-care Predicting who develops chronic low back
book for chronic low back pain: a pain in primary care: a prospective study.
randomized, controlled trial. Ann Intern BMJ 1999;318(7199):1662Y1667. doi:10.1136/
Med 2005;143:849Y856. doi:10.7326/ bmj.318.7199.1662.
0003<4819<143<12<200512200<00003.
65. Pincus T, Burton AK, Vogel S, Field AP. A
58. Chou R, Huffman LH; American Pain Society; systematic review of psychological factors as
American College of Physicians. predictors of chronicity/disability in
Nonpharmacologic therapies for acute and prospective cohorts of low back pain. Spine
chronic low back pain: a review of the (Phila Pa 1976) 2002;27(5):E109YE120.
evidence for an American Pain Society/ 66. Lurie J, Tomkins-Lane C. Management of
American College of Physicians Clinical lumbar spinal stenosis. BMJ 2016;352:h6234.
Practice Guideline. Ann Intern Med doi:10.1136/bmj.h6234.
2007;147(7):492Y504. doi:10.7326/
0003Y4819Y147Y7Y200710020Y00007. 67. Lurie JD, Tosteson TD, Tosteson A, et al.
Long-term outcomes of lumbar spinal
59. Gagnier JJ, van Tulder MW, Berman B, stenosis: eight-year results of the Spine
Bombardier C. Herbal medicine for low back Patient Outcomes Research Trial (SPORT).
pain: a Cochrane review. Spine (Phila Pa Spine (Phila Pa 1976) 2015;40(2):63Y76.
1976) 2007;32(1):82Y92. doi:10.1097/ doi:10.1097/BRS.0000000000000731.
01.brs.0000249525.70011.fe.
68. Chou R, Baisden J, Carragee EJ, et al. Surgery
60. Oltean H, Robbins C, van Tulder MW, et al. for low back pain: a review of the evidence
Herbal medicine for low-back pain.Cochrane for an American Pain Society Clinical Practice
Database Syst Rev 2014;12:CD004504. Guideline. Spine (Phila Pa 1976) 2009;34(10):
doi:10.1002/14651858.CD004504.pub4. 1094Y109. doi:10.1097/BRS.0b013e3181a105fc.
486 ContinuumJournal.com April 2017
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5819)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Test Bank For Bontragers Handbook of Radiographic Positioning and Techniques 9th Edition by Lampignano DownloadDocument15 pagesTest Bank For Bontragers Handbook of Radiographic Positioning and Techniques 9th Edition by Lampignano Downloadstevenstevensjgzaryxbdp100% (26)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Emra Sportsmedicine Splint Guide PDFDocument4 pagesEmra Sportsmedicine Splint Guide PDFDhimas HartantoNo ratings yet
- Small Animal Spinal Disorders (Second Edition)Document369 pagesSmall Animal Spinal Disorders (Second Edition)Aline Constantino100% (3)
- Brachial Plexus InjuriesDocument346 pagesBrachial Plexus InjuriesvinaymanNo ratings yet
- Muscle of Neck (Anatomy) PPT L.PPTX (Priti)Document21 pagesMuscle of Neck (Anatomy) PPT L.PPTX (Priti)Dj Manraj ProductionNo ratings yet
- ACl Surgery Recovery ProtocolDocument10 pagesACl Surgery Recovery ProtocolValentinToderaşcNo ratings yet
- 05.15.17 Bone Pathology (Atkinson) - NotesDocument8 pages05.15.17 Bone Pathology (Atkinson) - NotesDan WuiytNo ratings yet
- Brent D. Et Al - Introduction To Pilates-Based Rehabilitation PDFDocument8 pagesBrent D. Et Al - Introduction To Pilates-Based Rehabilitation PDFJuliana CarraNo ratings yet
- Tentiran Amputee & Prostesa (WawanWN)Document94 pagesTentiran Amputee & Prostesa (WawanWN)CikupaNo ratings yet
- Biomechanics Final ProjectDocument12 pagesBiomechanics Final Projectapi-285913253No ratings yet
- Physiotherapy Rehabilitation Guidelines - Knee ArthrosDocument7 pagesPhysiotherapy Rehabilitation Guidelines - Knee ArthrosmatameaNo ratings yet
- Orthopedic History Taking: DR - Kholoud Al-ZainDocument30 pagesOrthopedic History Taking: DR - Kholoud Al-ZainJim Jose AntonyNo ratings yet
- Article Perfect Posture PuzzleDocument6 pagesArticle Perfect Posture PuzzleMuhammad FahmyNo ratings yet
- Anky SpondyDocument4 pagesAnky Spondyjishu baruaNo ratings yet
- Case Study Lumbar SpineDocument2 pagesCase Study Lumbar SpineMaggie BlackNo ratings yet
- Labeled ItDocument50 pagesLabeled ItKaloy KamaoNo ratings yet
- Talar Fracture Repair and RehabilitationDocument4 pagesTalar Fracture Repair and RehabilitationAlexandra NadinneNo ratings yet
- Ergonomic Awareness: Presented by QBE Loss Control ServicesDocument42 pagesErgonomic Awareness: Presented by QBE Loss Control ServicesirshadnazarNo ratings yet
- Muscle & NMJ: by Adam HollingworthDocument8 pagesMuscle & NMJ: by Adam HollingworthIdrissa ContehNo ratings yet
- Clinical Case Presentation: Khalisshwary 131303130 Batch 33 Group G2Document12 pagesClinical Case Presentation: Khalisshwary 131303130 Batch 33 Group G2Sofea IzyanNo ratings yet
- NCM 116 Skills LabDocument5 pagesNCM 116 Skills LabRoni's Lifestyle LifeNo ratings yet
- Female PelvisDocument39 pagesFemale Pelvisabera100% (1)
- 1.translate Sumber Dan Materi Hafalan (AutoRecovered)Document19 pages1.translate Sumber Dan Materi Hafalan (AutoRecovered)raden chandrajaya listiandokoNo ratings yet
- Skeletal Muscle StructureDocument38 pagesSkeletal Muscle Structuretoyy100% (1)
- 3 at Home Exercises For Cervical SpondylosisDocument1 page3 at Home Exercises For Cervical Spondylosisskhumushi.456No ratings yet
- Dumbell Exercise ProgrammeDocument1 pageDumbell Exercise ProgrammeZakiah Abu KasimNo ratings yet
- 2008-Distal Radius Morphometry in The Malaysian PopulationDocument4 pages2008-Distal Radius Morphometry in The Malaysian PopulationPongnarin JiamwatthanachaiNo ratings yet
- Full Download Ebook PDF Operative Techniques Shoulder and Elbow Surgery 2nd Edition PDFDocument41 pagesFull Download Ebook PDF Operative Techniques Shoulder and Elbow Surgery 2nd Edition PDFmichael.crigler491100% (43)
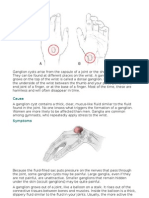
- Ganglion CystsDocument2 pagesGanglion CystsQush AimanNo ratings yet
- MCN Module 3Document9 pagesMCN Module 3Fatrick BernardinoNo ratings yet