Professional Documents
Culture Documents
Ild 150019
Ild 150019
Uploaded by
Vikas PunamiyaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ild 150019
Ild 150019
Uploaded by
Vikas PunamiyaCopyright:
Available Formats
Letters
RESEARCH LETTER gectomy, abdominal hysterectomy, radical prostatectomy,
nephrectomy, or cystectomy from April 1, 2003, through
Trends in Pulmonary Function Testing March 31, 2013.
Before Noncardiothoracic Surgery The outcome of interest was preoperative PFT, defined as
Preoperative pulmonary function tests (PFTs) assess the physician claims for simple spirometry, flow-volume loop, lung
severity of known pulmonary disease, diagnose causes of compliance, carbon monoxide diffusion capacity, or bron-
respiratory symptoms, and may help identify patients who chial provocative studies within 60 days before surgery. For
are at risk for postoperative comparison, we identified nonoperative PFTs, defined as tests
pulmonary complications. conducted from 181 through 365 days before surgery.
Invited Commentary
While useful in selected After dividing the study into 3-month intervals,3 rates of
page 1359
patients, unnecessary test- preoperative and nonoperative PFTs were measured for each
ing is costly.1 Few guidelines interval. Temporal trends in PFT rates were plotted and visu-
Related articles pages 1272 for the appropriate use of ally inspected to assess for time points when they changed sub-
and 1352
preoperative PFTs exist, stantially. We tested for the effect of guidelines on trends using
with the most recent being segmented linear regression models.4 These analyses were then
the April 2006 American College of Physicians guidelines2 repeated within subgroups that were stratified by periopera-
on risk assessment and prevention of postoperative pulmo- tive pulmonary risk based on the presence or absence of asthma
nary complications. We conducted a population-based or chronic obstructive pulmonary disease.
study in Ontario, Canada, to describe temporal trends in
preoperative PFTs and to assess whether the guidelines Results | Of 511 625 individuals in the cohort, 3.6% under-
influenced these trends. went preoperative PFTs while 3.3% had nonoperative PFTs.
Among high-risk individuals with asthma or chronic
Methods | Following research ethics approval from Sunny- obstructive pulmonary disease, the proportions who under-
brook Health Sciences Centre, we conducted a retrospective went preoperative and nonoperative testing were similar at
c o h o r t s t u d y u s i ng d e i d e nt i f i e d d a t a f r o m l i n ke d 8.3%. Conversely, among individuals without these condi-
population-based administrative databases. The cohort tions, 2.0% had preoperative testing while 1.6% had nonop-
included individuals who were 40 years or older who under- erative testing.
went elective abdominal aortic aneurysm repair, carotid Plotted trends showed that preoperative PFT rates de-
endarterectomy, peripheral arterial bypass, hip replace- creased during the study while nonoperative rates remained
ment, knee replacement, large-bowel resection, partial liver stable (Figure 1). Trends in preoperative PFT rates appeared
resection, pancreatoduodenectomy, gastrectomy, esopha- to decrease following the American College of Physicians guide-
Figure 1. Trends in PFTs Before Elective Noncardiothoracic Surgery From April 1, 2003, Through March 31, 2013
60
55 Preoperative
50 Nonoperative
45
PFTs, No. per 1000 Procedures
40
35
30
25 Rates of pulmonary function tests
(PFTs) in Ontario, Canada. The
20 vertical dotted line represents the
15
publication of the American College
of Physicians guidelines regarding
10 risk assessment for perioperative
pulmonary complications. In
5
segmented regression modeling,
0 trends in preoperative testing
2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 2013 2014 deceased significantly (P = .006)
Year of Hospital Admission following publication of these
guidelines.
1410 JAMA Internal Medicine August 2015 Volume 175, Number 8 (Reprinted) jamainternalmedicine.com
Copyright 2015 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 09/02/2019
Letters
Figure 2. Trends in Preoperative and Nonoperative PFTs From April 1, 2003, Through March 31, 2013, in Subgroups
Stratified by Perioperative Pulmonary Risk
140
COPD/asthma (preoperative PFT)
COPD/asthma (nonoperative PFT)
No asthma/COPD (preoperative PFT)
120
No asthma/COPD (nonoperative PFT)
PFTs, No. per 1000 Procedures
100
80
60
40
20
0
2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 2013 2014
Year of Hospital Admission
Rates of pulmonary function tests (PFTs) among patients with and without chronic obstructive pulmonary disease (COPD) or asthma. The vertical dotted line
represents the publication of the American College of Physicians guidelines regarding risk assessment for perioperative pulmonary complications. In segmented
regression modeling, trends in preoperative testing decreased significantly after publication of these guidelines in both the high-risk (P < .001) and
low-risk (P = .01) subgroups.
lines; this trend was confirmed using segmented regression nonoperative setting. These findings indicate the need for more
modeling (P = .006). Qualitatively similar patterns were ob- research to identify which surgical patients most benefit from
served in subgroups with and without risk factors for postop- preoperative PFTs.
erative pulmonary complications (Figure 2).
Louise Y. Sun, MD, SM, FRCPC
Discussion | Preoperative PFT rates in Ontario, Canada, were low, Andrea S. Gershon, MD, MSc, FRCPC
decreasing from 1 of 23 procedures in 2003 to 1 of 38 proce- Dennis T. Ko, MD, MSc, FRCPC
dures in 2013. These trends were qualitatively similar in sub- Stephan R. Thilen, MD, MS
groups stratified by risk for postoperative pulmonary compli- Lingsong Yun, MSc
cations. Notably, these decreasing preoperative PFT rates W. Scott Beattie, MD, PhD, FRCPC
contrast starkly with concurrent increases in rates of other peri- Duminda N. Wijeysundera, MD, PhD, FRCPC
operative interventions, such as preoperative anesthesia Author Affiliations: Department of Anesthesia, Toronto General Hospital,
consultations5 and stress testing.6 While the April 2006 pub- Toronto, Ontario, Canada (Sun, Beattie, Wijeysundera); Department of
lication of the updated American College of Physicians guide- Anesthesia, University of Toronto, Toronto, Ontario, Canada (Sun, Beattie,
Wijeysundera); Division of Cardiac Anesthesiology, University of Ottawa Heart
lines was followed by substantial decreases in preoperative PFT Institute, Ottawa, Ontario, Canada (Sun); Lung Health Program, Institute for
rates, these guidelines were unlikely to have been the sole rea- Clinical Evaluative Sciences, Toronto, Ontario, Canada (Gershon); Cardiovascular
son for this trend. Specifically, they were not associated with Research Program, Institute for Clinical Evaluative Sciences, Toronto, Ontario,
Canada (Ko, Yun, Wijeysundera); Department of Medicine, Sunnybrook Health
any large-scale promotion projects or changes in provincial
Sciences Centre, Toronto, Ontario, Canada (Gershon); Division of Cardiology,
health insurance payment schedules. The decline in preop- Schulich Heart Centre, Sunnybrook Health Sciences Centre, Toronto, Ontario,
erative PFT rates may, in part, be explained by increased use Canada (Gershon, Ko); Division of Cardiology, University of Toronto, Toronto,
of bedside spirometry and other alternative pulmonary tests, Ontario, Canada (Gershon, Ko); Department of Anesthesiology and Pain
Medicine, University of Washington, Seattle (Thilen); Li Ka Shing Knowledge
which are not captured by provincial administrative data-
Institute, St Michael’s Hospital, Toronto, Ontario, Canada (Wijeysundera).
bases. While less costly and possibly more accessible at some
Corresponding Author: Louise Y. Sun, MD, SM, FRCPC, Division of Cardiac
hospitals, these alternative tests have limitations, such as mea- Anesthesiology, University of Ottawa Heart Institute, 40 Ruskin St, Room
surement error.7 H2410, Ottawa, ON K1Y 4W7, Canada (lsun@ottawaheart.ca).
Given the low overall rate of preoperative PFTs, large- Published Online: June 8, 2015. doi:10.1001/jamainternmed.2015.2087.
scale efforts to reduce this testing are likely unnecessary. By Author Contributions: Drs Sun and Wijeysundera had full access to all the data
2013, preoperative PFTs were performed in less than 8% of On- in the study and take responsibility for the integrity of the data and the accuracy
of the data analysis.
tario patients with risk factors for pulmonary complications
Study concept and design: Sun, Beattie, Wijeysundera.
while preoperative testing rates among individuals without Acquisition, analysis, or interpretation of data: Sun, Gershon, Ko, Thilen, Yun,
known respiratory disease had approached rates seen in the Wijeysundera.
jamainternalmedicine.com (Reprinted) JAMA Internal Medicine August 2015 Volume 175, Number 8 1411
Copyright 2015 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 09/02/2019
Letters
Drafting of the manuscript: Sun, Beattie, Wijeysundera. Methods | The NHANES was designed to provide cross-
Critical revision of the manuscript for important intellectual content: Sun, sectional estimates of the prevalence of major diseases, nu-
Gershon, Ko, Thilen, Yun, Wijeysundera.
Statistical analysis: Sun, Yun, Wijeysundera. tritional disorders, and potential risk factors among the US
Obtained funding: Wijeysundera. population. 3 We aggregated data from 2007-2008, 2009-
Administrative, technical, or material support: Beattie, Wijeysundera. 2010, and 2011-2012 and included only adults who were 25 years
Study supervision: Beattie, Wijeysundera.
or older (n = 15 208), excluding those who were pregnant at the
Conflict of Interest Disclosures: Dr Gershon reports receiving support through
time of examination (n = 125) or provided insufficient data re-
a Physicians’ Services Incorporated Foundation Fellowship in Translational
Health Research; Dr Ko, through a Clinician-Scientist Award from the Heart and garding weight and height (n = 827). The NHANES obtained ap-
Stroke Foundation; Drs Beattie and Wijeysundera, through Merit Awards from proval from the National Center for Health Statistics Re-
the University of Toronto Department of Anesthesia; and Dr Wijeysundera, search Ethics Review Board and participants provided written
through a Clinician-Scientist Award from the Canadian Institutes of Health
consent.
Research. Dr Beattie reports being the R. Fraser Elliot Chair of Cardiac
Anesthesia at the University Health Network. No other disclosures were Weight and height were measured during the physical ex-
reported. amination using standard procedures. Patients’ BMIs (calcu-
Funding/Support: This study was supported in part by the Institute for Clinical lated as weight in kilograms divided by height in meters
Evaluative Sciences, which is supported in part by the Ontario Ministry of Health squared) were classified according to the following catego-
and Long-Term Care.
ries: underweight (<18.5), normal weight (18.5-24.9), over-
Role of the Funder/Sponsor: The funding sources had no role in the design and
weight (25.0-29.9), obesity class 1 (30.0-34.9), obesity class 2
conduct of the study; collection, management, analysis, and interpretation of
the data; preparation, review, or approval of the manuscript; and decision to (35.0-39.9), and obesity class 3 (≥40).2
submit the manuscript for publication. Data regarding patients’ age, sex, and race/ethnicity were
Disclaimer: The opinions, results, and conclusions are those of the authors, and collected. Age was classified as 25 to 54 years or 55 or more
no endorsement by the Ontario Ministry of Health and Long-Term Care or the years. Self-reported race/ethnicity were categorized as Mexi-
Institute for Clinical Evaluative Sciences is intended or should be inferred.
can American, non-Hispanic black, non-Hispanic white, or
1. De Nino LA, Lawrence VA, Averyt EC, Hilsenbeck SG, Dhanda R, Page CP.
other.
Preoperative spirometry and laparotomy: blowing away dollars. Chest. 1997;111
(6):1536-1541. We stratified the analyses by sex and calculated the
2. Qaseem A, Snow V, Fitterman N, et al; Clinical Efficacy Assessment weighted proportion estimates in each BMI category by race
Subcommittee of the American College of Physicians. Risk assessment for and or ethnic group and age group. All statistical analyses were con-
strategies to reduce perioperative pulmonary complications for patients ducted in Stata, version 12.0 (StataCorp LP), using survey analy-
undergoing noncardiothoracic surgery: a guideline from the American College
of Physicians. Ann Intern Med. 2006;144(8):575-580.
sis procedures to account for the complex sampling design.
3. Wijeysundera DN, Mamdani M, Laupacis A, et al. Clinical evidence, practice
guidelines, and β-blocker utilization before major noncardiac surgery. Circ Results | Of the sample population, 39.96% (weighted n =
Cardiovasc Qual Outcomes. 2012;5(4):558-565. 36 325 297) of men and 29.74% (weighted n = 28 894 630) of
4. Wagner AK, Soumerai SB, Zhang F, Ross-Degnan D. Segmented regression women were overweight and 35.04% (weighted n = 31 847 198)
analysis of interrupted time series studies in medication use research. J Clin of men and 36.84% (weighted n = 35 792 733) of women were
Pharm Ther. 2002;27(4):299-309.
obese. The weight status distribution was similar for both sexes
5. Wijeysundera DN, Austin PC, Beattie WS, Hux JE, Laupacis A.
across racial groups (Table), except for the proportion of non-
A population-based study of anesthesia consultation before major noncardiac
surgery. Arch Intern Med. 2009;169(6):595-602. Hispanic white women, which was higher in the normal-
6. Sheffield KM, McAdams PS, Benarroch-Gampel J, et al. Overuse of weight than the overweight category. Compared with 20 years
preoperative cardiac stress testing in Medicare patients undergoing elective ago, the greatest increase in the proportion of patients in the
noncardiac surgery. Ann Surg. 2013;257(1):73-80. obesity class 3 category was among non-Hispanic black women.
7. Stoller JK, Orens DK, Hoisington E, McCarthy K. Bedside spirometry in a
tertiary care hospital: the Cleveland Clinic experience. Respir Care. 2002;47(5):
Discussion | Compared with 1988-1994,2 the distribution of the
578-582.
population’s weight status has increased in the past 20 years.
The rising trends in overweight and obesity warrant timely at-
Prevalence of Overweight and Obesity tention from health-policy and health care–system decision
in the United States, 2007-2012 makers. Clinical practice for the prevention and treatment of
Overweight and obesity are associated with various chronic chronic conditions has mainly focused on screening high-
conditions.1 These conditions are considerable health care and risk populations. As a result, people in higher-weight catego-
societal burdens, yet could potentially be averted by prevent- ries are more likely to be diagnosed with the chronic diseases
ing weight gain and obesity. In a prior analysis, now almost 20 associated with excess weight2 because of more frequent mea-
years old, Must et al2 used a nationally representative data set surements, compared with people in the normal-weight cat-
from 1988 through 1994 and reported the US chronic disease egory. This approach may ignore individuals with normal
burden associated with body mass index (BMI), thus inform- weight and their weight gain, which puts them at risk.
ing clinical practice and the priorities for cost-effective pre- Population-based strategies helping to reduce modifi-
vention strategies. Using the most recent data in the National able risk factors such as physical environment interventions,
Health and Nutrition Examination Survey (NHANES, 2007- enhancing primary care efforts to prevent and treat obesity,
2012), we updated the prevalence of overweight and obesity and altering societal norms of behavior are required.4 In 2012,
by sex, age, and race/ethnicity and compared the values with the Institute of Medicine identified population-based obesity-
those of the earlier study.2 prevention strategies that target physical activity, healthy diet,
1412 JAMA Internal Medicine August 2015 Volume 175, Number 8 (Reprinted) jamainternalmedicine.com
Copyright 2015 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ on 09/02/2019
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5819)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- Dr. Amy's Simplified Road Map To HealthDocument15 pagesDr. Amy's Simplified Road Map To HealthDr. Amy Yasko100% (46)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Asthma in Children PPT 1Document30 pagesAsthma in Children PPT 1Rinto Nugroho100% (1)
- CH3 - Case 3 Deciding Who Receives The Swine Flu Vaccine (Chapter 3, Page 178)Document3 pagesCH3 - Case 3 Deciding Who Receives The Swine Flu Vaccine (Chapter 3, Page 178)zoehyhNo ratings yet
- Chapter I.ii - IIIDocument24 pagesChapter I.ii - IIIaureateiNo ratings yet
- Surgery TacticsDocument154 pagesSurgery TacticsAiman Arifin50% (2)
- Direction: Read The Question Carefully and Choose The Letter of The Correct Answer. Encircle The Letter ofDocument5 pagesDirection: Read The Question Carefully and Choose The Letter of The Correct Answer. Encircle The Letter ofSarah Jane PescadorNo ratings yet
- Benign Prostatic HyperplasiaDocument28 pagesBenign Prostatic HyperplasiaFedrick MasatuNo ratings yet
- Copy of Integumentary Student Resources 1Document12 pagesCopy of Integumentary Student Resources 1Alondra Hernandez ReyesNo ratings yet
- FU-M3-CU11 Respiratory Function and Nursing CareDocument17 pagesFU-M3-CU11 Respiratory Function and Nursing CareHERLIN HOBAYANNo ratings yet
- Jacobson v. Massachusetts, 197 U.S. 11 (1905)Document17 pagesJacobson v. Massachusetts, 197 U.S. 11 (1905)Scribd Government Docs100% (1)
- 0312 Antibody IdDocument18 pages0312 Antibody IdKen WayNo ratings yet
- G9, Practice Test No. 2: Part Ii. ReadingDocument14 pagesG9, Practice Test No. 2: Part Ii. ReadingngoetNo ratings yet
- Klasifikasi Prosedur ICD9CMDocument258 pagesKlasifikasi Prosedur ICD9CMJivitaBasarahNo ratings yet
- Cardiopulmonary: Basic Life SupportDocument10 pagesCardiopulmonary: Basic Life SupportSteven GrosserNo ratings yet
- Reproductive Organs of Farm AnimalsDocument54 pagesReproductive Organs of Farm AnimalsJanice LiNo ratings yet
- MCQ Part 1 (First Term)Document15 pagesMCQ Part 1 (First Term)Mahmoud RagabNo ratings yet
- Online Learner Permit ApplicationDocument2 pagesOnline Learner Permit ApplicationCalvin MaiNo ratings yet
- Health Problems and RemediesDocument2 pagesHealth Problems and RemediesAdrienn Kolonicsné KocsisNo ratings yet
- MAH Final Report 5Document60 pagesMAH Final Report 5sandip1936No ratings yet
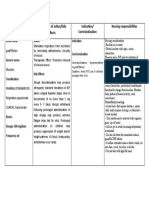
- Drug Mechanism of Action/side Effects Indication/ Contraindication Nursing ResponsibilitiesDocument1 pageDrug Mechanism of Action/side Effects Indication/ Contraindication Nursing ResponsibilitiesSheryhan Tahir BayleNo ratings yet
- Dawa Administration: Environmental and Social Impacts of Stone Quarrying: in DireDocument15 pagesDawa Administration: Environmental and Social Impacts of Stone Quarrying: in DireOmar Abdel Aziz IbrahimNo ratings yet
- MAPEH (AutoRecovered)Document12 pagesMAPEH (AutoRecovered)Mark Jerome MontañoNo ratings yet
- Excel de ConsultasDocument232 pagesExcel de Consultaslaura sanchezNo ratings yet
- Soft Tissue SarcomasDocument37 pagesSoft Tissue SarcomasHealth Education Library for People100% (1)
- Group 3-Kaposi SarcomaDocument25 pagesGroup 3-Kaposi SarcomaShiangNo ratings yet
- T1 Surgery Aseptic & Antiseptics in SurgeryDocument20 pagesT1 Surgery Aseptic & Antiseptics in SurgeryRishik RanaNo ratings yet
- Pharmacy - Aegrotat Supplementary - Biochemistry Microbiology Immunology - PC 221 - Feb 2022Document4 pagesPharmacy - Aegrotat Supplementary - Biochemistry Microbiology Immunology - PC 221 - Feb 2022THE MASUVHELELE POSTNo ratings yet
- ACF MAINS 2021 403 (Animal Husbandry and Verterinary Science) 20032021104724Document2 pagesACF MAINS 2021 403 (Animal Husbandry and Verterinary Science) 20032021104724rainbowNo ratings yet
- Chapter 1 by GroupDocument23 pagesChapter 1 by GroupNizel BaesNo ratings yet
- DR Mercola - FDA Says Misinformation Is A Top KillerDocument7 pagesDR Mercola - FDA Says Misinformation Is A Top Killerguy777No ratings yet