Professional Documents
Culture Documents
Thyroid Malignancy/ Papillary Thyroid Carcinoma
Uploaded by
Maryam FadahOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Thyroid Malignancy/ Papillary Thyroid Carcinoma
Uploaded by
Maryam FadahCopyright:
Available Formats
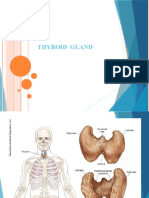
Thyroid malignancy/ Papillary thyroid carcinoma
Epidemiology
Most common type of thyroid malignancy 70-80%
Mean age: 30-50 years
Female to male ratio: 2.5:1
Risk factors: childhood radiation, first degree-relatives thyroid carcinoma, familial
syndromes: werner, cowden, carney complex, familial polyposis
Pathological classification
PTC gross morphology: Hard, whitish, flat
Histological morphology: microscopic calcification, necrosis, and cystic changes.
Papillary projection, psammoma bodies (microcalcification lumps of cells, caused by
sloughed papillary projections). Cuboidal cells with pale, abundant cytoplasm,
crowded nuclei that may demonstrate grooving and internuclear cytoplasmic inclusion
– Orphan Annie nuclei -
Diagnosis is made by characteristic nuclear cellular feature.
Made by FNA cytology
- Classical papillary carcinoma
- Encapsulated follicular variant (10% of PTC) has excellent prognosis, why count
it as PTC variant? Cause it behave like PTC
- Columnar
- Hobnail
- Tall cell carcinoma
Clinical Features
Slow growing painless mass
Dysphagia
Dyspnea
Dysphonia
Localized:
Palpable thyroid nodule
Metastatic:
Painless lateral neck mass (detected before the primary lesion) – Lateral aberrant thyroid -
PTC with no metastasis - Prognosis is 10 years survival (for all stages) greater than 95%
Factors affecting the prognosis:
Age (most important prognostic factor)
Tumor size
Tumor extension
PTC metastasis site:
PTC with Lung metastasis – Prognosis 50% at 10 years
PTC with Brain metastasis – Prognosis median 1-year survival
The most common site for metastasis is the lung then bone then liver then brain.
Lymph node does not effect the prognosis unless the patient has lymph metastasis and he is
older than 45 (increases risk of death by 46%)
Lymph node metastasis is very common – most commonly cervical lymph node
Multifocality is associated with increase of risk of cervical nodal metastasis
Invasion of adjacent structure: esophagus, trachea, recurrent laryngeal nerve (RLN)
You might also like
- 2022ABFM ITEMultChoiceDocument71 pages2022ABFM ITEMultChoiceMaryam FadahNo ratings yet
- 2022ABFM ITEMultChoiceDocument71 pages2022ABFM ITEMultChoiceMaryam FadahNo ratings yet
- $12. Urinary Tract Infections 2015Document39 pages$12. Urinary Tract Infections 2015Sindhu BabuNo ratings yet
- Thyroid Neoplasms: Kelompok 3 Dr. Reza Maulana Dr. Intan E. Napitupulu Drg. Andi Arfandi ArifuddinDocument41 pagesThyroid Neoplasms: Kelompok 3 Dr. Reza Maulana Dr. Intan E. Napitupulu Drg. Andi Arfandi ArifuddinIntan Eklesiana NapitupuluNo ratings yet
- Epk FDocument73 pagesEpk FBryan FjbNo ratings yet
- Ovarian Tumours PresentationDocument49 pagesOvarian Tumours PresentationChoden JamyangNo ratings yet
- Oncology TOLo Week 3Document8 pagesOncology TOLo Week 3CarolineJiaNo ratings yet
- Thyroid Neoplasms: Muhammad Haris Aslam Janjua Resident, Surgical Unit I SIMS/Services Hospital, LahoreDocument116 pagesThyroid Neoplasms: Muhammad Haris Aslam Janjua Resident, Surgical Unit I SIMS/Services Hospital, LahoreHajra IsrarNo ratings yet
- Papillary Thyroid CarcinomaDocument9 pagesPapillary Thyroid CarcinomaELinkTulusNo ratings yet
- Tumors of Nervous SystemDocument50 pagesTumors of Nervous SystemNininghrNo ratings yet
- Genitourinary Tract Tumors Including Renal Tumors: Pre-ReadingDocument31 pagesGenitourinary Tract Tumors Including Renal Tumors: Pre-Readingmus zaharaNo ratings yet
- Testicular Tumor - Dr. FaizDocument54 pagesTesticular Tumor - Dr. FaizFemale calmNo ratings yet
- Update of Thyroid NoduleDocument40 pagesUpdate of Thyroid NoduleAsif JIELANINo ratings yet
- Mediastinal Tumors: by Temesgen G/MariamDocument51 pagesMediastinal Tumors: by Temesgen G/MariamVincent SerNo ratings yet
- Neoplasms of Testis NishDocument54 pagesNeoplasms of Testis NishRamesh ReddyNo ratings yet
- Thyroid NeoplasmsDocument62 pagesThyroid Neoplasmshemanarasimha gandikotaNo ratings yet
- TJW Bladder CancerDocument35 pagesTJW Bladder CancerShariq ShaNo ratings yet
- Thyroid Cancer PDFDocument67 pagesThyroid Cancer PDFJaredNo ratings yet
- Thyroid Carcinoma: DR Suleman Mumtaz PG 2 Ward 2Document81 pagesThyroid Carcinoma: DR Suleman Mumtaz PG 2 Ward 2suleman2009No ratings yet
- I. Primary 1. Epithelial 2. Non-EpithelialDocument25 pagesI. Primary 1. Epithelial 2. Non-EpithelialSifu Perniagaan MayaNo ratings yet
- Neoplasms Thyroid N ParathyroidsDocument88 pagesNeoplasms Thyroid N ParathyroidsBkas GrgNo ratings yet
- Assessment and Diagnosis of Abdominal Masses in Children: Resident Education Lecture SeriesDocument45 pagesAssessment and Diagnosis of Abdominal Masses in Children: Resident Education Lecture SeriesboubiyouNo ratings yet
- Tumor IntraabdomenDocument30 pagesTumor IntraabdomenBedahanakugmNo ratings yet
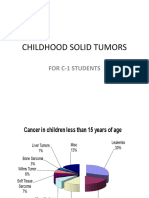
- Childhood Solid Tumors: For C-1 StudentsDocument72 pagesChildhood Solid Tumors: For C-1 StudentsYemata HailuNo ratings yet
- DR 180114164748Document43 pagesDR 180114164748Hasnain ToheedNo ratings yet
- CBL Thyroid Pgy3Document48 pagesCBL Thyroid Pgy3imad mokalledNo ratings yet
- Testicular Tumours 2020Document55 pagesTesticular Tumours 2020Ramesh ReddyNo ratings yet
- What Do You Need To Know About Breast Cancer: DR / Mokhtar Gusmallah Clinical OncologistDocument26 pagesWhat Do You Need To Know About Breast Cancer: DR / Mokhtar Gusmallah Clinical OncologistjehemirNo ratings yet
- Tumor Pada AnakDocument65 pagesTumor Pada Anakdr.cintaNo ratings yet
- ThyroidDocument43 pagesThyroidchowhan04No ratings yet
- Dept Patologi Anatomi FK UmiDocument41 pagesDept Patologi Anatomi FK UmiWulan NoviantiNo ratings yet
- Thyroid Neoplasm: Dr. M. Abrar BarakzaiDocument38 pagesThyroid Neoplasm: Dr. M. Abrar Barakzaimohammed alrubaiaanNo ratings yet
- I. Primary 1. Epithelial 2. Non-EpithelialDocument25 pagesI. Primary 1. Epithelial 2. Non-EpithelialSifu Perniagaan MayaNo ratings yet
- Neuroblastoma My Lecture 2011Document153 pagesNeuroblastoma My Lecture 2011Wael ElsawyNo ratings yet
- Approach To A Patient With "Solitary Thyroid Nodule" (STN)Document6 pagesApproach To A Patient With "Solitary Thyroid Nodule" (STN)Jacob Alexander MarpaungNo ratings yet
- Reproduction Pathology ReviewDocument9 pagesReproduction Pathology ReviewkishorechandraNo ratings yet
- Surgical Management of Malignant TumorsDocument129 pagesSurgical Management of Malignant TumorsAshish JainNo ratings yet
- Carcinoma of Penis: DR Hitesh Patel Associate Professor Surgery Department GMERS Medical College, GotriDocument55 pagesCarcinoma of Penis: DR Hitesh Patel Associate Professor Surgery Department GMERS Medical College, Gotrihitesh3150% (1)
- Colon CancerDocument64 pagesColon CancerAjay BhagatNo ratings yet
- Null - PDF 3Document24 pagesNull - PDF 3مهند حسام محمد سعيد عبدNo ratings yet
- ARROCase SalivaryGlandTumorsDocument61 pagesARROCase SalivaryGlandTumorssnolinNo ratings yet
- A.K12 - FINAL Management Brain Tumors Dr. Dr. Rr. Suzy Indharty, M. Kes, SP - BsDocument42 pagesA.K12 - FINAL Management Brain Tumors Dr. Dr. Rr. Suzy Indharty, M. Kes, SP - BsandrianyNo ratings yet
- The Evaluation and Management of Neck Masses of Unknown EtiologyDocument38 pagesThe Evaluation and Management of Neck Masses of Unknown EtiologyShaxawan Mahmood AliNo ratings yet
- Common Childhood Solid Tumors (Part 2)Document56 pagesCommon Childhood Solid Tumors (Part 2)Princess Aira Bucag CarbonelNo ratings yet
- Brain Tumors in Pediatrics: Resident Education Lecture SeriesDocument28 pagesBrain Tumors in Pediatrics: Resident Education Lecture SeriesCandy crushNo ratings yet
- Neoplasia: Dr. Phoo Pwint Maw KhineDocument28 pagesNeoplasia: Dr. Phoo Pwint Maw KhineThinagari JevataranNo ratings yet
- Pediatric Abdominal TumorsDocument27 pagesPediatric Abdominal TumorsDlman JamalNo ratings yet
- I. Primary 1. Epithelial 2. Non-EpithelialDocument25 pagesI. Primary 1. Epithelial 2. Non-EpithelialSifu Perniagaan MayaNo ratings yet
- Acc 59 s1 66Document7 pagesAcc 59 s1 66luzvi1708No ratings yet
- ThyroidDocument102 pagesThyroidfadoNo ratings yet
- CBL Thyroid FinalDocument48 pagesCBL Thyroid Finalimad mokalledNo ratings yet
- All You Have Ever Wanted To Know About Mucoepidermoid CarcinomaDocument63 pagesAll You Have Ever Wanted To Know About Mucoepidermoid CarcinomaNeeraj TekariaNo ratings yet
- Endometrial Cancer: DR P Mukonoweshuro Consultant Pathologist RUH BathDocument59 pagesEndometrial Cancer: DR P Mukonoweshuro Consultant Pathologist RUH BathmesNo ratings yet
- Brain Tumors in Pediatrics: Resident Education Lecture SeriesDocument28 pagesBrain Tumors in Pediatrics: Resident Education Lecture SeriesFetinuhan97No ratings yet
- Eau Guidelines On Penile Cancer: Introduction and EpidemiologyDocument15 pagesEau Guidelines On Penile Cancer: Introduction and Epidemiologyhypebeast dopeNo ratings yet
- Medullary CancerDocument32 pagesMedullary CancerLily DenekeNo ratings yet
- Malignant Disorders of The OvariesDocument15 pagesMalignant Disorders of The OvarieskenyakisumuNo ratings yet
- Neoplasms of Infancy and ChildhoodDocument29 pagesNeoplasms of Infancy and ChildhoodtheintrovNo ratings yet
- Breast Cancer (Aka BR CA) : - Routine Screening For Genetic Abnormalities of A Strong Family HX of BR CA Is NOT NeededDocument6 pagesBreast Cancer (Aka BR CA) : - Routine Screening For Genetic Abnormalities of A Strong Family HX of BR CA Is NOT NeededChanthorn SokNo ratings yet
- Neuroendocrine Tumors: Surgical Evaluation and ManagementFrom EverandNeuroendocrine Tumors: Surgical Evaluation and ManagementJordan M. CloydNo ratings yet
- Infectious Causes of Cancer: A Guide for Nurses and Healthcare ProfessionalsFrom EverandInfectious Causes of Cancer: A Guide for Nurses and Healthcare ProfessionalsNo ratings yet
- Iron Defeciency AnemiaDocument7 pagesIron Defeciency AnemiaMaryam FadahNo ratings yet
- Acute Exacerbation of Chronic Obstructive Pulmonary DiseaseDocument108 pagesAcute Exacerbation of Chronic Obstructive Pulmonary DiseaseMaryam FadahNo ratings yet
- Obesity in Adults AafpDocument2 pagesObesity in Adults AafpMaryam FadahNo ratings yet
- Vitamin D DefeciencyDocument6 pagesVitamin D DefeciencyMaryam FadahNo ratings yet
- Vitamin D ScreeningDocument7 pagesVitamin D ScreeningMaryam FadahNo ratings yet
- AAFP Cushing's Disease - Clinical Manifestations and Diagnostic Evaluation - American Family PhysicianDocument9 pagesAAFP Cushing's Disease - Clinical Manifestations and Diagnostic Evaluation - American Family PhysicianMaryam FadahNo ratings yet
- Cardiac Arrest VF/Pulseless VT Learning Station ChecklistDocument5 pagesCardiac Arrest VF/Pulseless VT Learning Station ChecklistMaryam FadahNo ratings yet
- Family Medicine Presentation - DysuriaDocument17 pagesFamily Medicine Presentation - DysuriaMaryam FadahNo ratings yet
- Efast: Name Position Normal US Pic Abnormal US Pic SubcostalDocument4 pagesEfast: Name Position Normal US Pic Abnormal US Pic SubcostalMaryam FadahNo ratings yet
- Addison Disease Early Detection and TreatmentDocument6 pagesAddison Disease Early Detection and TreatmentNajib Al FatinNo ratings yet
- E FastDocument4 pagesE FastMaryam FadahNo ratings yet
- Ugib Esophagitis: Candida, Herpes Simplex Virus, Cytomegalovirus, and Human ImmunodeficiencyDocument1 pageUgib Esophagitis: Candida, Herpes Simplex Virus, Cytomegalovirus, and Human ImmunodeficiencyMaryam FadahNo ratings yet
- Stimulating NeurotransmittersDocument1 pageStimulating NeurotransmittersMaryam FadahNo ratings yet
- Centriacinar Panacinar Paraseptal Irregular Emphysema Bullous EmphysemaDocument1 pageCentriacinar Panacinar Paraseptal Irregular Emphysema Bullous EmphysemaMaryam FadahNo ratings yet
- The Right Clinical Information, Right Where It's Needed: Last Updated: Sep 12, 2019Document92 pagesThe Right Clinical Information, Right Where It's Needed: Last Updated: Sep 12, 2019Maryam FadahNo ratings yet
- ND NDDocument1 pageND NDMaryam FadahNo ratings yet
- Acute COPD ExacerbationDocument65 pagesAcute COPD ExacerbationMaryam FadahNo ratings yet
- Chronic DiarrheaDocument1 pageChronic DiarrheaMaryam FadahNo ratings yet
- Intrahepatic Biliary Tract DiseaseDocument1 pageIntrahepatic Biliary Tract DiseaseMaryam FadahNo ratings yet
- Vasculitis SummaryDocument1 pageVasculitis SummaryMaryam FadahNo ratings yet
- Primary Cardiac Tumors SummaryDocument2 pagesPrimary Cardiac Tumors SummaryMaryam FadahNo ratings yet
- Hypotension DrugsDocument1 pageHypotension DrugsMaryam FadahNo ratings yet
- Red Vascular: Polygonal Cells Growing in Nests or Cords Lamellae of Dense CollagenDocument3 pagesRed Vascular: Polygonal Cells Growing in Nests or Cords Lamellae of Dense CollagenMaryam FadahNo ratings yet
- Demand Ischemia: Not A Total Occlusion, So If YouDocument1 pageDemand Ischemia: Not A Total Occlusion, So If YouMaryam FadahNo ratings yet
- Stimulating NeurotransmittersDocument1 pageStimulating NeurotransmittersMaryam FadahNo ratings yet
- Release Is Stimulated Whenever Nutrients Reach Down Into The Distal BowelDocument1 pageRelease Is Stimulated Whenever Nutrients Reach Down Into The Distal BowelMaryam FadahNo ratings yet
- Stanolol From The Name Stanly (Male)Document2 pagesStanolol From The Name Stanly (Male)Maryam FadahNo ratings yet