Professional Documents
Culture Documents
Title: Oral Vesiculobullous Lesions Associated With Sars-Cov-2 Infection
Uploaded by
coral coralOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Title: Oral Vesiculobullous Lesions Associated With Sars-Cov-2 Infection
Uploaded by
coral coralCopyright:
Available Formats
Accepted Article
DR CARMEN MARTIN CARRERAS-PRESAS (Orcid ID : 0000-0002-0937-0994)
Article type : Short Communication
TITLE: Oral vesiculobullous lesions associated with SARS-CoV-2 infection
RUNNING TITLE: Oral manifestations in COVID-19 patients
KEYWORDS: COVID-19, oral mucosal lesions, mucocutaneous viral lesions.
AUTHORS:
Martín Carreras-Presas, Carmen
Adult´s Dentistry Department. Oral Medicine. Universidad Europea de Madrid. Madrid. Spain
ORCID ID: 0000-0002-0937-0994
carmen.martin2@universidadeuropea.es
Amaro Sánchez, Juan
Master in Periodontics. Universidad Rey Juan Carlos. Madrid. Spain
coeamaro@gmail.com
López-Sánchez, Antonio Francisco
Head of Master in Periodontics. Universidad Rey Juan Carlos. Madrid. Spain
antonio.lopez@urjc.es
Jané-Salas, Enric
Dentistry Department. Universidad de Barcelona. Cataluña. España
ORCID ID:0000-0002-3574-4603
enricjanesalas@ub.edu
Somacarrera Pérez, Maria Luisa
This article has been accepted for publication and undergone full peer review but has not been
through the copyediting, typesetting, pagination and proofreading process, which may lead to
differences between this version and the Version of Record. Please cite this article as doi:
10.1111/ODI.13382
This article is protected by copyright. All rights reserved
Adult´s Dentistry Department. Oral Medicine. Universidad Europea de Madrid. Madrid. Spain
Accepted Article
mluisa.somacarrera@universidadeuropea.es
Corresponding author:
Martín Carreras-Presas, Carmen
Address: Valle de Cachemira St. 46, 2º 2. Zipcode: 28039. Madrid. Spain
Email address: carmen.martin2@universidadeuropea.es
Date of submission: 04/20/2020
ABSTRACT
The coronavirus pandemic that began in China at the end of last year, claimed its first confirmed
death in Spain at the end of January 2020, where to date, 200,000 infections and 20,852 deaths
have been recorded. In addition to the manifestations of SARS-CoV-2 infection described in the
literature (fever, dry cough, diarrhea, and respiratory involvement) recently, skin exanthematic
lesions have been described.
We present three cases (two suspected and one confirmed) of patients presenting ulcers in the oral
cavity. Oral manifestations developed during the lock-down period between the last week of
March and the first week of April 2020, and consisted of pain, desquamative gingivitis, ulcers and
blisters. To the best of our knowledge, this is the first case report describing of a COVID-19
patient with oral manifestations. Intraoral examinations should be carried out in patients affected
by SARS-CoV-2, always when having the recommended protection measures available to a better
understanding of the disease.
TEXT
Humans infected with SARS-CoV-2 are at risk of developing serious and life-threatening
conditions, such as severe acute respiratory syndrome.
Recent data suggest the more common signs and symptoms of SARS-CoV-2 infection to be
headache, sore throat, hyposmia, hypogeusia, diarrhea, dyspnea, and in severe cases pneumonia.
This article is protected by copyright. All rights reserved
(Wang et al., 2020)
Accepted Article
Some authors in Italy reported cases of dermatologic implication in patients affected by SARS-
CoV-2 infection (Recalcati, 2020). Since then, we have seen more reports describing dermatologic
involvement, including lesions that range from affectation of hands and feet in teenagers to
vasculitis, rash, urticaria and varicella-like lesions. (Estebanez et al., 2020)
Spain has been severely affected by the COVID-19 outbreak (Bonanad et al., 2020). The majority
of dental clinics and university clinics are closed, only treating emergencies if the entity has the
protective measures necessary. There is a nationwide lack of serological tests available, both for
patients and for healthcare providers.
We here present three cases associated to this virus. Two where there is a suspicion of COVID-19,
and one case of confirmed infection. All cases presented ulcers or blisters in the oral cavity,
appearing and developing during the isolation period between the last week of March and the first
week of April 2020. We were not able to examine them in our clinic due to the state of alarm
declared from the 14th of March, but offered the possibility of video consultations.
Patient 1
A 56-year-old healthy male patient without any relevant medical history was isolated with
suspected infection of SARS-CoV-2. He presented asthenia and fever for 2 days, reporting
hyposmia, dysgeusia and enlargement of lymph nodes in the neck. Testing for COVID-19 was not
performed in the hospital due to the non-severity of his case. He was sent home by his general
practitioner. He complained of pain in his palate and sore throat. We asked him to send us a photo
(Figure 1). The lesions resembled a herpetic recurrent stomatitis, however, it was the first time the
patient had them. We prescribed Valaciclovir 500 mg every 8 hours for 10 days, and topical
antiseptics with chlorhexidine and hyaluronic acid. After 10 days there was a full recovery of the
oral lesions. The patient is currently waiting for serological testing to confirm whether or not he
had a non-severe COVID-19 disease.
Patient 2
A 58-year-old male with diabetes and hypertension reported pain on his palate. He assumed it was
a bacterial infection of a tooth and reached out to us for an appointment. His wife had been
This article is protected by copyright. All rights reserved
diagnosed with COVID-19 and they were both isolated in their home. We asked for a photo and
Accepted Article
we could see multiple small ulcers on his palate with unilateral affection. (Figure 2). The patient
did not have any previous history of herpetic infection.
The lesions were painful and solved within 1 week using topical antiseptic mouthwash.
Patient 3:
A 65-year-old female patient developed high fever, diarrhea and pain on her tongue, on the 12th of
March 2020. She suffered from obesity and hypertension controlled by diuretics and an ACE
inhibitor. A week after developing symptoms she fainted at home and was taken to the hospital
where she was diagnosed with bilateral pneumonia due to SARS CoV-2 infection. She was given
antibiotics, corticosteroids and antiviral drugs (Lopinavir 200 mg, Ritonavir 50 mg,
Hidroxychloroquine 200 mg). On the 30th of March she was discharged. On the 4th of April she
developed a rash under her breasts and other parts of the skin, including her back and genital area.
She had complained of pain on her tongue from the beginning, but she told us she had not been
given an intraoral examination yet. She was taken back to the hospital where the dermatologist
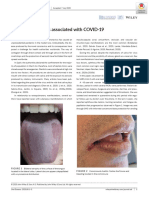
performed a biopsy and prescribed antifungals. A week later she developed blisters in her internal
lip mucosa as well as a desquamative gingivitis (Figure 3). We prescribed hyaluronic acid and
chlorhexidine mouthwash. Her general practitioner prescribed prednisolone 30 mg per day. Her
lesions improved within 3 days and she is now recovering in isolation at home. The result of the
biopsy revealed non-specific morphological findings with some criteria suggestive of viral
exanthema or urticariform dermatitis with discrete blood extravasation.
In our opinion, it makes good sense that this virus provokes exanthematic lesions that may
resemble other viral processes we are used to diagnosing in the dental clinic.
The patients presented ulcers or blisters, which are common elementary lesions observed in other
viral processes, such as aphthous fever, hand, foot and mouth disease and herpetic
gingivostomatitis, as described by Scully and Samaranayake in 2016 (Scully & Samaranayake,
2016)
In the first 2 cases, lesions were affecting keratinized tissue, as seen in herpes simplex lesions.
(Scully & Samaranayake, 2016) In the last case, oral lesions affected both keratinized and non-
This article is protected by copyright. All rights reserved
keratinized tissue and were more compatible with an erythema multiforme. (Trayes, Love, &
Accepted Article
Studdiford, 2019)(Schwartz & Janniger, 2020)
As we were not able to perform biopsies, further studies need to be carried out in order to
determine whether oral manifestations are common in patients affected by SARS-CoV-2 infection
or if the emotional distress of the situation itself could trigger such lesions. (Jon B. Suzich, 2018)
(Chida & Mao, 2009)
It is important to mention that the 3 cases all reported having had pain, oral ulcers or blisters
before seeking medical advice. We suspect that intraoral lesions often are misdiagnosed due to the
lack of intraoral examinations, considering the severity of other pathological processes that might
concur with this viral infection. To the best of our knowledge, this is the first case report of a
COVID-19 patient presenting intraoral manifestations.
We encourage all medical doctors, dentists and dermatologists to perform intraoral examinations
in patients suspected or affected by SARS-CoV-2, always when having the recommended
protection measures available.
This article is protected by copyright. All rights reserved
AUTHOR CONTRIBUTION
Accepted Article
Carmen Martin and Juan Amaro evaluated the case reports and wrote the original draft. Antonio
Lopez edited the original draft and Enric Jané was responsible for resources. Maria Luisa
Somacarrera supervised the final manuscript.
CONFLICTS OF INTEREST
None to declare
ACKNOWLEDGEMENTS
We would like to thank Dr. Diego Fernández-Nieto, dermatologist at Ramón y Cajal Hospital
(Madrid) for sharing with us the anatomopathological result of the skin biopsy of patient number
3, Fuensanta Martín and Dr. Helene Alseth-Alvarado for their reviews and comments.
REFERENCES
Bonanad, C., Garcia-Blas, S., Tarazona-Santabalbina, F. J., Diez-Villanueva, P., Ayesta, A.,
Fores, J. S., … Martinez-Selles, M. (2020). [Coronavirus: the geriatric emergency of 2020.
Joint document of the Geriatric Cardiology Section of the Spanish Society of Cardiology and
the Spanish Society of Geriatrics and Gerontology]. Revista espanola de cardiologia.
https://doi.org/10.1016/j.recesp.2020.03.027
Chida, Y., & Mao, X. (2009). Does psychosocial stress predict symptomatic herpes simplex virus
recurrence? A meta-analytic investigation on prospective studies. Brain, Behavior, and
Immunity, 23(7), 917–925. https://doi.org/10.1016/j.bbi.2009.04.009
Estebanez, A., Perez-Santiago, L., Silva, E., Guillen-Climent, S., Garcia-Vazquez, A., & Ramon,
M. D. (2020). Cutaneous manifestations in COVID-19: a new contribution. Journal of the
European Academy of Dermatology and Venereology : JEADV.
https://doi.org/10.1111/jdv.16474
Jon B. Suzich, A. R. C. (2018). Strength in Diversity: Understanding the Pathways of HSV-1
reactivation. Virology, 522, 81–91. https://doi.org/10.1016/j.virol.2018.07.011.Strength
This article is protected by copyright. All rights reserved
Recalcati, S. (2020, March). Cutaneous manifestations in COVID-19: a first perspective. Journal
Accepted Article
of the European Academy of Dermatology and Venereology : JEADV.
https://doi.org/10.1111/jdv.16387
Schwartz, R. A., & Janniger, C. K. (2020). Generalized Pustular Figurate Erythema A Newly
Delineated Severe Cutaneous Drug Reaction Linked with Hydroxychloroquine.
Dermatologic Therapy, n/a(n/a PG-), 2–4. https://doi.org/10.1111/dth.13380
Scully, C., & Samaranayake, L. P. (2016). Emerging and changing viral diseases in the new
millennium. Oral Diseases, 22(3), 171–179. https://doi.org/10.1111/odi.12356
Trayes, K. P., Love, G., & Studdiford, J. S. (2019). Erythema Multiforme: Recognition and
Management. American Family Physician, 100(2), 82–88.
Wang, D., Hu, B., Hu, C., Zhu, F., Liu, X., Zhang, J., … Peng, Z. (2020). Clinical Characteristics
of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan,
China. JAMA. https://doi.org/10.1001/jama.2020.1585
FIGURE LEGENDS
Figure 1: Multiple orange-colored ulcers with an erythematous halo and symmetric distribution on
the right hard palate of the patient
Figure 2. Multiple pinpoint yellowish ulcers with an erythematous halo on the left hard palate of
the patient.
Figure 3. a) The aspect of the back of the patient the day the biopsy was performed at the hospital.
The patient reported that the lesions were more pruritic than painful. b) The patient presented 3
blisters on the inner lip mucosa. The blister located closer to her right commissure was intact and
tense. The bulla located on the left appeared to be broken. The lesions were affecting both intra-
and extraoral mucosa, and the patient developed crusts on the external lip mucosa 3 days after this
photo was taken.
This article is protected by copyright. All rights reserved
Accepted Article
odi_13382_f1.jpg
This article is protected by copyright. All rights reserved
Accepted Article
odi_13382_f2.jpg
This article is protected by copyright. All rights reserved
Accepted Article
odi_13382_f3.jpg
This article is protected by copyright. All rights reserved
You might also like
- Coronavirus Disease COVID-19Document953 pagesCoronavirus Disease COVID-19Claudio GodoyNo ratings yet
- Radiation TherapyDocument2 pagesRadiation TherapyAngel Joy CatalanNo ratings yet
- Wound Healing: Second EditionDocument115 pagesWound Healing: Second EditionLody100% (1)
- Tissue Salt Primer SchuesslerDocument36 pagesTissue Salt Primer SchuesslerYanka IlarionovaNo ratings yet
- ABC of Wound Healing WWW - Dof3tna - Net WWW - Egydr.com Drhamdy2009Document49 pagesABC of Wound Healing WWW - Dof3tna - Net WWW - Egydr.com Drhamdy2009steadiNo ratings yet
- Examination of An UlcerDocument65 pagesExamination of An UlcerDrAmrit Veer100% (3)
- Oral Manifestations of Systemic DiseasesDocument148 pagesOral Manifestations of Systemic DiseasesGaurav Gupta100% (1)
- Atlas of Common Oral Mucosal Lesions (Final) AIN SHAMS UNIVERSITY IN EgyptDocument92 pagesAtlas of Common Oral Mucosal Lesions (Final) AIN SHAMS UNIVERSITY IN EgyptAbdEl-latifM.Al-smaryNo ratings yet
- Mouth Ulcer and Diseases of The Tongue - Cause and CureDocument4 pagesMouth Ulcer and Diseases of The Tongue - Cause and CureJago BharathNo ratings yet
- Diagnosis and Protection of COVID-19 in StomatologyDocument5 pagesDiagnosis and Protection of COVID-19 in StomatologyBOHR International Journal of Current research in Dentistry (BIJCRID)No ratings yet
- Evidence Based Oral MedicineDocument13 pagesEvidence Based Oral MedicineShantanu DixitNo ratings yet
- Allergic Manifestation in Oral Cavity. Exudative Polymorphic Erythema. Chronic Recurrent Aphthous Stomatitis.Document38 pagesAllergic Manifestation in Oral Cavity. Exudative Polymorphic Erythema. Chronic Recurrent Aphthous Stomatitis.Alex DaniciNo ratings yet
- Odi 13382Document3 pagesOdi 13382Winda KhosasiNo ratings yet
- Necrotizing Periodontal Disease: Oral Manifestation of COVID-19Document5 pagesNecrotizing Periodontal Disease: Oral Manifestation of COVID-19cabarcaxNo ratings yet
- PIIS1201971220304471Document3 pagesPIIS1201971220304471Enggiana RenawatiNo ratings yet
- Tammaro2020 Covid 19Document7 pagesTammaro2020 Covid 19eva yustianaNo ratings yet
- Necrotizing Periodontal Disease: Oral Manifestation of COVID-19Document2 pagesNecrotizing Periodontal Disease: Oral Manifestation of COVID-19meliantha 102012472No ratings yet
- 1708 1732Document25 pages1708 1732gwodentaleducationNo ratings yet
- 2020-dr Palma CovidDocument8 pages2020-dr Palma CovidmelissaNo ratings yet
- Pi Is 1201971220307001Document4 pagesPi Is 1201971220307001Ara EzenNo ratings yet
- Dental JournalDocument7 pagesDental Journaliqbal faturahmanNo ratings yet
- COVID-19 Dentistry-Related Aspects: A Literature: Concise ReviewDocument6 pagesCOVID-19 Dentistry-Related Aspects: A Literature: Concise ReviewSofiaNo ratings yet
- Articulo 3-EritemaDocument4 pagesArticulo 3-EritemaMariuxi CastroNo ratings yet
- Medoral 25 E563Document2 pagesMedoral 25 E563dentist studentNo ratings yet
- IPArchCytolHistopatholRes 6-2-135 139Document5 pagesIPArchCytolHistopatholRes 6-2-135 139FeliciaDewiNo ratings yet
- JCM 10 00757 v2Document10 pagesJCM 10 00757 v2Feby Kuntum Mayang SariNo ratings yet
- Absence of Specific Cutaneous Manifestations of SeDocument1 pageAbsence of Specific Cutaneous Manifestations of Senadya aliviaNo ratings yet
- Follow Up of Skin Lesions During The Evolution of COVID 19 A CaseDocument4 pagesFollow Up of Skin Lesions During The Evolution of COVID 19 A CaseZihan ZetiraNo ratings yet
- Doaa A. Yousef, Reda S. Sabra: Oral Ulceration in Patient With SAR-COV2 Infection. A Case ReportDocument7 pagesDoaa A. Yousef, Reda S. Sabra: Oral Ulceration in Patient With SAR-COV2 Infection. A Case ReportFeby Kuntum Mayang SariNo ratings yet
- 0718 381X Ijodontos 16 01 112Document8 pages0718 381X Ijodontos 16 01 112Sozin DamarkNo ratings yet
- Jurnal Gingivitis Vivian 190631174Document5 pagesJurnal Gingivitis Vivian 190631174VivianNo ratings yet
- Ever Since The Emergence of COVIDDocument5 pagesEver Since The Emergence of COVIDMehrnaz MoradiNo ratings yet
- 1 PBDocument4 pages1 PBFan AccountNo ratings yet
- Coronavirus Disease 19 (COVID-19) : Implications For Clinical Dental CareDocument21 pagesCoronavirus Disease 19 (COVID-19) : Implications For Clinical Dental CareSergio Losada AmayaNo ratings yet
- Biological and Social Aspects of Coronavirus Disease 2019 (COVID-19) Related To Oral HealthDocument11 pagesBiological and Social Aspects of Coronavirus Disease 2019 (COVID-19) Related To Oral HealthXimena amayaNo ratings yet
- Conjunctivitis Can Be The Only Presenting Sign and PDFDocument7 pagesConjunctivitis Can Be The Only Presenting Sign and PDFkhairaniNo ratings yet
- 2nd Activity 2Document10 pages2nd Activity 2Vinayaka cable and Internet ProvidersNo ratings yet
- Peds 2020-1711 Full PDFDocument7 pagesPeds 2020-1711 Full PDF12va Promocion Pediatria PUCENo ratings yet
- COVID-19: Present and Future Challenges For Dental Practice: Environmental Research and Public HealthDocument10 pagesCOVID-19: Present and Future Challenges For Dental Practice: Environmental Research and Public HealthFirda IzzatiNo ratings yet
- Version of Record Doi: 10.1111/ODI.13463Document3 pagesVersion of Record Doi: 10.1111/ODI.13463cabarcaxNo ratings yet
- How Has Covid 19 Affected The Sector and Dental Health?Document5 pagesHow Has Covid 19 Affected The Sector and Dental Health?api-643791617No ratings yet
- Redefining Dental Practice During and Post-COVID-19 Era: A ReviewDocument9 pagesRedefining Dental Practice During and Post-COVID-19 Era: A Reviewapridey parinding08No ratings yet
- COVID-19 and Dentistry: Prevention in Dental Practice, A Literature ReviewDocument12 pagesCOVID-19 and Dentistry: Prevention in Dental Practice, A Literature ReviewrosminiNo ratings yet
- Cutaneous Manifestations in COVID 19 A First PerspectivDocument2 pagesCutaneous Manifestations in COVID 19 A First PerspectivZihan ZetiraNo ratings yet
- IFEA IES Endodontic and Dental Practice During COVID-19Document24 pagesIFEA IES Endodontic and Dental Practice During COVID-19Mohammed TarekNo ratings yet
- Chapter25 2021 Book CoronavirusDisease COVID 19Document954 pagesChapter25 2021 Book CoronavirusDisease COVID 19Tep B 21083 Luki LoviandiNo ratings yet
- Acute Acro-Ischemia in The Child at The Time of Covid-19Document3 pagesAcute Acro-Ischemia in The Child at The Time of Covid-19Manuel AcuñaNo ratings yet
- 1807 3107 Bor 34 E048Document7 pages1807 3107 Bor 34 E048Luis GómezNo ratings yet
- Dental Considerations After The Outbreak of 2019 Novel Coronavirus Disease: A Review of LiteratureDocument7 pagesDental Considerations After The Outbreak of 2019 Novel Coronavirus Disease: A Review of Literatureharshita parasharNo ratings yet
- Idcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaDocument3 pagesIdcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaMuhamad ZenNo ratings yet
- Oral Manifestations in Covid19Document2 pagesOral Manifestations in Covid19La redazione Tp24No ratings yet
- AGAS - EPID - Section 18Document3 pagesAGAS - EPID - Section 18Maxine AgasNo ratings yet
- The Novel Coronavirus Pandemic: Challenges & Coping Strategies For Dental PractitionersDocument13 pagesThe Novel Coronavirus Pandemic: Challenges & Coping Strategies For Dental PractitionersHindol DasNo ratings yet
- Coronavirus (COVID-19) Outbreak: What The Department of Endoscopy Should KnowDocument6 pagesCoronavirus (COVID-19) Outbreak: What The Department of Endoscopy Should KnowswabrijNo ratings yet
- Oral Manifestations Associated With COVID-19: Letter To The EditorDocument3 pagesOral Manifestations Associated With COVID-19: Letter To The EditorSandra DelgadoNo ratings yet
- Chen-2020-Preventive and Control Measures ForDocument6 pagesChen-2020-Preventive and Control Measures ForJaime GonzalezNo ratings yet
- Oral Manifestations Associated To Covid 19Document4 pagesOral Manifestations Associated To Covid 19Enggiana RenawatiNo ratings yet
- Oral Manifestations in Hospitalized COVID PatientsDocument7 pagesOral Manifestations in Hospitalized COVID PatientsEdoardo BiancoNo ratings yet
- Science Repository: An Interim Report On The Dental Practice Management: COVID-19Document4 pagesScience Repository: An Interim Report On The Dental Practice Management: COVID-19Amadea EmanuelaNo ratings yet
- Oral Lesions Diagnosis Associated With HIV.Document6 pagesOral Lesions Diagnosis Associated With HIV.Saira BasurtoNo ratings yet
- Lesiones Orales Covid19Document7 pagesLesiones Orales Covid19Diana PerezNo ratings yet
- Article On Covid 19 and OrthodonticsDocument20 pagesArticle On Covid 19 and OrthodonticsBenet BabuNo ratings yet
- Impacts of The COVID 19Document4 pagesImpacts of The COVID 19Athenaeum Scientific PublishersNo ratings yet
- Manifestasi Oral Infeksi COVID-19: Yobel R. Woran, Lydia E. N. Tendean, Christy N. MintjelunganDocument5 pagesManifestasi Oral Infeksi COVID-19: Yobel R. Woran, Lydia E. N. Tendean, Christy N. MintjelunganAra EzenNo ratings yet
- Urticarial Exanthem As Early Diagnostic Clue For COVID-19 InfectionDocument2 pagesUrticarial Exanthem As Early Diagnostic Clue For COVID-19 Infectionandini senjaNo ratings yet
- Methods of Dental Examination of Patients With Covid 19Document6 pagesMethods of Dental Examination of Patients With Covid 19Central Asian StudiesNo ratings yet
- Jerônimo Et Al., 2021Document6 pagesJerônimo Et Al., 2021Claudia BrilhanteNo ratings yet
- Jocd 14066Document5 pagesJocd 14066IqusmnNo ratings yet
- Lesi Rongga Mulut Diagnosis Dan Penanganannya PDFDocument35 pagesLesi Rongga Mulut Diagnosis Dan Penanganannya PDFFhaNo ratings yet
- Oral Pathology Clinical Pathologic Correlations 6th Edition Regezi Test BankDocument31 pagesOral Pathology Clinical Pathologic Correlations 6th Edition Regezi Test Bankmatte.caudalebvf100% (22)
- Ipmtl 1 - Annissaqiella - Acute Traumatic Ulcer RevDocument15 pagesIpmtl 1 - Annissaqiella - Acute Traumatic Ulcer RevAnnissaqiellaMaharaniNo ratings yet
- Epidemiology of Oral CancerDocument12 pagesEpidemiology of Oral Cancerعدي عبدالالهNo ratings yet
- StomatitisDocument3 pagesStomatitiswidya RDNo ratings yet
- Oral Path 2 - Lecture 2 DFBDocument7 pagesOral Path 2 - Lecture 2 DFBJana Louise DesamitoNo ratings yet
- Pemphigus VulgarisDocument3 pagesPemphigus VulgarisAdib MuntasirNo ratings yet
- Oral Manifestations of Systemic DiseasesDocument18 pagesOral Manifestations of Systemic DiseasesYashpreetsingh BhatiaNo ratings yet
- Non-Plaque Induced Gingival Diseases: Palle Holmstrup - Jacqueline Plemons - Joerg MeyleDocument16 pagesNon-Plaque Induced Gingival Diseases: Palle Holmstrup - Jacqueline Plemons - Joerg MeyleAnniJassoNo ratings yet
- Lec 8 Ulcerative Vesicular & Bullous LesionsDocument6 pagesLec 8 Ulcerative Vesicular & Bullous LesionsAbd 9961No ratings yet
- Oral Medicine Imp QuestionsDocument8 pagesOral Medicine Imp QuestionssabreennafiyaNo ratings yet
- Crohn's DiseaseDocument1 pageCrohn's DiseaseibrahimNo ratings yet
- NCP EbuenDocument3 pagesNCP EbuenNocReyesNo ratings yet
- Pemeriksaan Fisik THTDocument83 pagesPemeriksaan Fisik THTClara ReginaNo ratings yet
- IyotDocument7 pagesIyotMonaimLaraMacabangonIVNo ratings yet
- Daids Ae Grading Table v2 Nov2014Document33 pagesDaids Ae Grading Table v2 Nov2014Dinu Diana ArdeleanuNo ratings yet
- Gizzard Erosion and Ulceration Syndrome in Chickens and Turkeys A Review of Causal or Predisposing FactorsDocument8 pagesGizzard Erosion and Ulceration Syndrome in Chickens and Turkeys A Review of Causal or Predisposing FactorsgorrikNo ratings yet
- Diabetes y Periodontitis PDFDocument8 pagesDiabetes y Periodontitis PDFKty SinistNo ratings yet
- JR IPM - Comprehensive Management of Oral Frailty in Multiple Systemic Disease Geriatric Patient (Case Report)Document30 pagesJR IPM - Comprehensive Management of Oral Frailty in Multiple Systemic Disease Geriatric Patient (Case Report)NUR HAYUNINGTYASNo ratings yet
- Mucosal LesionsDocument36 pagesMucosal LesionsGaurav PuriNo ratings yet