Professional Documents
Culture Documents
HISTOMOROFOME
Uploaded by
Mayra PereiraCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
HISTOMOROFOME
Uploaded by
Mayra PereiraCopyright:
Available Formats
AJCP / Original Article
Placental Histomorphometry in Gestational Diabetes
Mellitus
The Relationship Between Subsequent Type 2 Diabetes Mellitus
and Race/Ethnicity
Rhonda Bentley-Lewis, MD,1 Deanna L. Dawson,1 Julia B. Wenger, MPH,2 Ravi I. Thadhani,
MD,2 and Drucilla J. Roberts, MD3
Downloaded from https://academic.oup.com/ajcp/article-abstract/141/4/587/1761455 by guest on 25 April 2020
CME/SAM
From the 1Medicine/Diabetes Unit, Massachusetts General Hospital, Boston, MA; 2Medicine/Division of Nephrology, Massachusetts General Hospital,
Boston, MA; and 3Pathology, Massachusetts General Hospital, Boston, MA.
Key Words: Placental histomorphometry; Gestational diabetes mellitus; Type 2 diabetes mellitus; Race/ethnicity
DOI: 10.1309/AJCPX81AUNFPOTLL
ABSTRACT Upon completion of this activity you will be able to:
• define gestational diabetes mellitus (GDM).
Objectives: We examined placental histomorphometry in • describe placental histomorphometry associated with a
gestational diabetes mellitus (GDM) for factors associated normotensive pregnancy complicated by GDM.
• describe racial differences in placental histomorphometry
with race/ethnicity and subsequent type 2 diabetes mellitus associated with GDM.
(T2DM).
The ASCP is accredited by the Accreditation Council for Continuing
Medical Education to provide continuing medical education for physicians.
Methods: We identified 124 placentas from singleton, full- The ASCP designates this journal-based CME activity for a maximum of
term live births whose mothers had clinically defined GDM 1 AMA PRA Category 1 Credit ™ per article. Physicians should claim only
and self-reported race/ethnicity. Clinical and placental the credit commensurate with the extent of their participation in the activ-
ity. This activity qualifies as an American Board of Pathology Maintenance
diagnoses were abstracted from medical records. of Certification Part II Self-Assessment Module.
The authors of this article and the planning committee members and staff
Results: Forty-eight white and 76 nonwhite women were have no relevant financial relationships with commercial interests to disclose.
Questions appear on p 607. Exam is located at www.ascp.org/ajcpcme.
followed for 4.1 years (median, range 0.0-8.9 years). White
women developed less T2DM (12.5% vs 35.5%; P = .005)
but had higher systolic (mean ± SD, 116 ± 13 vs 109 ± 11
mm Hg; P < .001) and diastolic (71 ± 9 vs 68 ± 7 mm Hg;
P = .02) blood pressure, more smoking (35.4% vs 10.5%; Gestational diabetes mellitus (GDM) affects approxi-
P = .004), and more chorangiosis (52.1% vs 30.3%; P = .02) mately 7% of all pregnancies in the United States, but
than nonwhite women. prevalence estimates are as high as 18% among women of
nonwhite race/ethnicity.1 GDM increases the risk for type
Conclusions: Although more nonwhite women developed 2 diabetes mellitus (T2DM) and cardiovascular disease
T2DM, more white women had chorangiosis, possibly subsequent to pregnancy2; therefore, early risk stratifica-
secondary to the higher percentage of smokers among them. tion of women with GDM is critical to the development of
Further study is necessary to elucidate the relationship appropriate primary prevention strategies. Although several
among chorangiosis, subsequent maternal T2DM, and race. risk factors have been identified as associated with progres-
sion to T2DM in women with GDM, including higher body
mass index, older age, and higher frequency of GDM in past
pregnancies,3 these factors incompletely identify the risk.
Because the placenta reflects the maternal metabolic milieu
during pregnancy, the use of placenta-derived data for sub-
sequent maternal disease is another opportunity to inform
risk stratification in this population.
© American Society for Clinical Pathology Am J Clin Pathol 2014;141:587-592 587
587 DOI: 10.1309/AJCPX81AUNFPOTLL 587
Bentley-Lewis et al / Placental Histomorphometry in GDM
The placenta is the critical organ responsible for fetal venous plasma glucose values greater than or equal to the
growth and development, as well as the transfer of blood, oxy- defined threshold levels (fasting, ≥95 mg/dL; 1 hour, ≥180
gen, nutrients, and waste between the mother and the fetus.4 mg/dL; 2 hours, ≥155 mg/dL; and 3 hours, ≥140 mg/dL) on
Normal placental anatomy comprises the lacuna, floating a 100-g oral glucose tolerance test. Among the women who
and anchoring villi, villous and extravillous cytotrophoblasts, met the GDM criteria (n = 157), only those who delivered full-
syncytiotrophoblasts, uterine blood vessels, and uterine con- term, singleton live births were selected for the study (n = 129).
nective tissue.5 Pathologic changes in placental structure Race and ethnicity were self-reported, and the women
and function have been observed in type 1 diabetes mellitus identified themselves as black, white, Asian, Hispanic, or
(T1DM)6 and T2DM.7 In addition, placental abnormalities in “other.” Those who did not self-identify race/ethnicity were
GDM have been reported8 and have paralleled those associat- categorized as “unknown” (n = 5) and were not included in the
ed with pregestational diabetes, including increased fetal and population of women examined by race/ethnicity (n = 124). All
Downloaded from https://academic.oup.com/ajcp/article-abstract/141/4/587/1761455 by guest on 25 April 2020
placental weight, diameter, and thickness9; cytotrophoblastic participants completed informed written consent to encompass
hyperplasia; villous edema and fibrin deposits; and choran- this study, and the study protocol was approved by the Partners
giosis.8 However, placental abnormalities in GDM have not Human Research Committee Institutional Review Board.
been associated with subsequent maternal risk for T2DM. In
addition, the role of race/ethnicity in GDM placental pathol- Placenta Specimen Examination
ogy has not been fully elucidated. The pathologic specimens previously had been processed
Therefore, we sought to compare placental histomor- by gross and histologic examinations. A standard gross tem-
phometry from pregnancies complicated by GDM and exam- plate was followed, and at least three sections of placenta were
ine factors that distinguished women from racially/ethnically sampled for histology (cord, membranes, and parenchyma).
diverse populations compared with white populations. We One of four perinatal pathology experts rotating on service
hypothesized that the placentas of women from racially/ethni- (including D.J.R.) performed the initial diagnostic examina-
cally diverse populations would have a higher prevalence of tion and reported the findings. All placental specimens select-
vascular abnormalities given the higher prevalence of GDM ed for our database were reexamined by two authors (D.J.R.
and concomitant cardiovascular disease risk among these and D.L.D.), who were both blinded to clinical history.
populations.2 Second, because women with GDM have simi- The gross parameters examined included placental
lar placental pathology as women with T1DM and T2DM, we weight, cord weight, cord length, and cord insertion site.
hypothesized that placental pathology would provide insight Samples were also coded for villous maturation, categorized
regarding the risk of subsequent T2DM postpartum. as mature, slightly immature, or immature. Mature villi had
at least a minimum of one vasculosyncytial membrane and
one syncytiotrophoblastic knot per two terminal villi. Slightly
immature villi were coded for villi bordering the two other
Materials and Methods
classifications but not meeting criteria for villous maturational
arrest.12 Immature villi were coded when the villi were large
Population Selection without vasculosyncytial membranes and with a prominent
Participants for this study were selected from placental cytotrophoblastic layer.
pathology specimens received in the Massachusetts General On histologic examination, we scored and diagnosed vil-
Hospital (MGH) Pathology Department between January 1, lous maturational arrest; dysmorphic villi, defined as villi with
2001, and December 31, 2009 (n = 765). We then cross-ref- prominent trophoblastic layers without knots, irregular villous
erenced this population with a population of women who pre- contours, open villous stroma, and hypovascularization; and
sented for prenatal care to the MGH Obstetrical Department chorangiosis, defined as 20 or more capillaries in a cluster of
between September 1998 and January 2007 and were par- villi in three ×40 fields.13 We captured maternal inflamma-
ticipants in the MGH Obstetric Maternal Study (MOMS).10 tion as an aggregate of the measures of villitis of unclear or
These women, initially followed during pregnancy for the unknown etiology14; interface inflammation, confluent basal
development of preeclampsia, were subsequently observed plate chronic villitis with deciduitis, and/or confluent chronic
for a median of 11.1 years postpartum and had data on the inflammation on the fetal side of the chorionic plate; and
development of T2DM subsequent to pregnancy. plasma cell deciduitis. Maternal and fetal evidence of acute
Of the population of women with pathology specimens chorioamnionitis was classified using the Redline nosology.15
who also had longitudinal clinical data from the MOMS Measures of fetal stress identified included the presence of
data set (n = 178), we selected those categorized as having a an increased number of circulating fetal nucleated RBCs
clinically confirmed diagnosis of GDM by Carpenter-Coustan and multifocal or diffuse acute villous edema. Measures of
criteria.11 Women were diagnosed if they had two or more placental perfusion pathologies included placental infarcts,
588 Am J Clin Pathol 2014;141:587-592 © American Society for Clinical Pathology
588 DOI: 10.1309/AJCPX81AUNFPOTLL
AJCP / Original Article
distal villous hypoplasia, and fetal thrombotic vasculopa- nonwhite population to the white population. The statistical
thy.16 Decidual vasculopathy was characterized by fibrinoid analyses were performed using the SAS for Windows version
necrosis with or without atherosis in the decidua capsularis, 9.1 statistical software package (SAS Institute, Cary, NC). A
decidual necrosis with atherosis in the decidua basalis, or P value less than .05 was considered statistically significant.
the presence of small muscularized arterioles in the decidua
basalis. Meconium, fibrin deposition, intervillous thrombi,
and calcification were also evaluated. Results
Statistical Analysis Clinical Findings
The placental pathologic and clinical parameters were From the initial 765 specimens available, we identified
compared and used to evaluate the differences in placental the 129 women with biochemically defined GDM who had
Downloaded from https://academic.oup.com/ajcp/article-abstract/141/4/587/1761455 by guest on 25 April 2020
pathology and vasculature between the two populations. full-term, singleton live births. Among these 129 women, 5
Continuous variables were summarized using means and women did not identify their race/ethnicity and were excluded
standard deviations, while frequency distributions account- from the analysis population (n = 124). Maternal and neonatal
ing for missing values were used for categorical variables. baseline characteristics for the study population are listed
Summary characteristics of white vs nonwhite subjects were in ❚Table 1❚. Of the 124 women who provided information
compared using Mann-Whitney tests and c2 tests where regarding their race, 48 were white, four were black, 14 were
appropriate. To complete our analysis of the placenta, clinical Asian, 51 were Hispanic, one was Native American, and six
and pathologic data were analyzed and compared to examine were “other” nonwhite but unspecified race/ethnicity. The
the differences in placental vasculature in women from the women were followed for a median of 4.1 (range, 0.0-8.9)
❚Table 1❚
Clinical Characteristics of the Study Population With Gestational Diabetes Mellitusa
Characteristic All White Nonwhiteb P Value
No. of patients 129 48 76
Age, y 32.4 ± 5.8 32.7 ± 5.6 32.0 ± 6.0 .71
Body mass index, kg/m 2 30.0 ± 6.7 30.5 ± 7.2 29.8 ± 6.4 .71
Systolic blood pressure, mm Hg 112 ± 12 116 ± 13 109 ± 11 .001c
Diastolic blood pressure, mm Hg 69 ± 8 71 ± 9 68 ± 7 .02c
Total cholesterol, mg/dL 195 ± 38 189 ± 41 199 ± 37 .52
High-density lipoprotein, mg/dL 53 ± 13 55 ± 14 51 ± 13 .44
Low-density lipoprotein, mg/dL 114 ± 28 109 ± 28 116 ± 29 .49
Triglycerides, mg/dL 172 ± 128 188 ± 174 163 ± 90 .75
Gestational age at prenatal visit, wk 12.1 ± 6.0 11.5 ± 5.2 12.2 ± 6.3 .88
No. of total pregnancies 2.7 ± 1.7 2.4 ± 1.4 2.7 ± 1.6 .44
No. of live births 1.0 ± 1.3 0.7 ± 0.8 1.1 ± 1.3 .19
Weight gain, lb 21.3 ± 12.7 21.9 ± 13.8 20.7 ± 12.1 .85
Preeclampsia 2 (1.6) 1 (2.1) 1 (1.3) .74
Gestational age at delivery, wk 39.5 ± 1.1 39.4 ± 1.1 39.4 ± 3.3 .53
Baby weight, g 3,670 ± 618 3,667 ± 505 3,676 ± 699 .66
Birth weight for gestational age percentile, % 62.9 ± 30.0 64.2 ± 29.0 61.7 ± 31.3 .64
Time from MGH delivery to follow-up, median (range), y 4.1 (0-8.9) 3.7 (0-8.5) 4.1 (0-8.9) .96
d
Essential hypertension 17 (13.2) 6 (12.5) 11 (14.5) .53
Diabetes mellitusd 34 (26.4) 6 (12.5) 27 (35.5) .005c
Smoking status .004c
Never 56 (43.4) 18 (37.5) 36 (47.4)
Past 18 (14.0) 17 (35.4)e 8 (10.5)e
Current 8 (6.2)
Race
White 48 (37.2)
Black 4 (3.1)
Asian 14 (10.9)
Hispanic 51 (39.5)
Native American 1 (0.8)
Other nonwhite 6 (4.7)
Unknown 5 (3.9)
MGH, Massachusetts General Hospital.
a Values are presented as mean ± SD or number (%) unless otherwise indicated. Percentages that do not add up to 100% denote missing or unknown data.
b Nonwhite group includes all categories except white and “unknown.”
c Significant at P < .05.
d Percentage denotes development of disease following delivery.
e Numbers include past and current smokers.
© American Society for Clinical Pathology Am J Clin Pathol 2014;141:587-592 589
589 DOI: 10.1309/AJCPX81AUNFPOTLL 589
Bentley-Lewis et al / Placental Histomorphometry in GDM
years from delivery to last MGH encounter, and we observed Pathologic Findings
that the development of T2DM after pregnancy among the Gross and histomorphometric examinations were per-
nonwhite population was nearly three times more frequent formed on all 129 placentas in the study cohort, and the
compared with the white population (35.5% vs 12.5%; P = findings are listed in ❚Table 2❚. Placental weight (mean ± SD,
.005). White women also had higher systolic (mean ± SD, 116 532 ± 108 vs 540 ± 148 g; P = .88) and gestational age at
± 13 vs 109 ± 11 mm Hg; P < .001) and diastolic (71 ± 9 vs delivery (39.4 ± 1.1 vs 39.4 ± 3.3 weeks; P = .53) were similar
68 ± 7 mm Hg; P = .02) blood pressure compared with non- between the white and nonwhite populations. We observed
white women. Notably, the number of past or current smokers a larger number of slightly immature placentas in the white
was significantly higher among the white compared with the population compared with the nonwhite population (91.7% vs
nonwhite women (35.4% vs 10.5%; P = .004). Otherwise, 89.5%), but this difference did not achieve statistical signifi-
both the white and nonwhite populations had similar clinical, cance in the overall maturation category. Chorangiosis was
Downloaded from https://academic.oup.com/ajcp/article-abstract/141/4/587/1761455 by guest on 25 April 2020
prenatal, and perinatal parameters. significantly higher in placentas from the white population
compared with the nonwhite population (52.1% vs 30.3%, P =
.02) ❚Image 1❚. Excluding chorangiosis, the placental pathol-
❚Table 2❚ ogy parameters were not statistically significantly different
Placental Pathology Characteristics in the Study Population between the white and nonwhite populations (Table 2).
With Gestational Diabetes Mellitusa
Characteristic All White Nonwhiteb P Value
Discussion
Placental weight, g 536 ± 132 532 ± 108 540 ± 148 .88 In our study, we analyzed the placental histomorphom-
Placental weight .95
percentile etry of GDM among women from white and nonwhite
<10 24 (18.6) 9 (18.8) 14 (18.4) populations. To our knowledge, this is the first study that has
10-90 72 (55.8) 27 (56.3) 41 (54.0)
>90 33 (25.6) 12 (25.0) 21 (27.6) examined racial/ethnic differences in the placental pathology
Cord length, cm 36.1 ± 13.8 33.7 ± 14.8 37.2 ± 13.2 .19 of women with GDM with a consideration of the clinical
Cord insertion 5.0 ± 2.4 4.7 ± 2.5 5.2 ± 2.3 .25
Cord insertion location .26 implications during and subsequent to pregnancy. Clinically,
Membranous 2 (1.6) 0 2 (2.6) we observed that white women had higher blood pressure,
Maturation .92
Mature 9 (7.0) 3 (6.3) 6 (7.9)
were more likely to be smokers, and were less likely to
Slightly immature 117 (90.7) 44 (91.7) 68 (89.5) develop subsequent T2DM than the nonwhite women. From
Immature 3 (2.3) 1 (2.1) 2 (2.6) a pathology perspective, we observed that placental pathology
Chorangiosis 49 (38.0) 25 (52.1) 23 (30.3) .02c
Chorangiosis— 7 (5.4) 4 (8.3) 3 (4.0) .30 was largely similar between the white and nonwhite popula-
focal diffuse tions. However, we did observe that white women with GDM
Dysmorphic 16 (12.4) 5 (10.4) 11 (14.5) .51
Maturation arrest 0 0 0 NA had a greater percentage of chorangiosis than was evident
Inflammation 51 (39.5) 19 (39.6) 30 (39.5) .99 among nonwhite women with GDM, a finding worthy of
Acute chorioamnionitis 22 (17.1) 6 (12.5) 14 (18.4) .38
Villitis of unclear/ 26 (20.2) 11 (22.9) 14 (18.4) .54 further consideration.
unknown etiology Chorangiosis refers to the presence of excess blood ves-
Interface inflammation 4 (3.1) 2 (4.2) 2 (2.6) .64
Deciduitis 2 (1.6) 2 (4.2) 0 .07
sels in the placental villi. Ogino and Redline13 observed that
Fetal acute 2 (1.6) 1 (2.1) 1 (1.3) .74 chorangiosis is significantly associated with having enlarged
chorioamnionitis placenta, immature villi, and maternal diabetes. In addi-
Vasculitis 6 (4.7) 2 (4.2) 3 (4.0) .74
Nucleated RBCs 6 (4.7) 3 (6.3) 3 (4.0) .54 tion, they observed in the literature that chorangiosis is also
Acute villous edema 14 (10.9) 5 (10.4) 9 (11.8) .81 associated with maternal anemia, smoking, twin gestations,
Placental infarcts 20 (15.5) 8 (16.7) 12 (15.8) .90
Intervillous thrombi 26 (20.2) 9 (18.8) 16 (21.1) .76 and delivery at high altitudes. In our study, all women were
Fetal thrombotic 9 (7.0) 1 (2.1) 8 (10.5) .07 healthy, and none were reported to have anemia or cardiovas-
vasculopathy
Avascular villi 5 (3.9) 1 (2.1) 4 (5.3) .38 cular disease. In addition, all pregnancies in our study cohort
Edema 1 (0.8) 1 (2.1) 0 .21 were singleton and delivered at MGH, so ambient altitude
Meconium 39 (30.2) 11 (22.9) 27 (35.5) .14
Extensive meconium 2 (1.6) 0 2 (2.6) .26
was not a factor. However, a significantly greater number,
Decidual vasculopathy 2 (1.6) 1 (2.1) 1 (1.3) NA 35.4%, of the white women identified as past or current
Calcification 14 (10.9) 4 (8.3) 9 (11.8) .53 smokers compared with 10.5% of the nonwhite population
Fibrin 11 (8.5) 2 (4.2) 8 (10.5) .21
Atherosis 1 (0.8) 0 1 (1.3) .42 (P = .004). Therefore, it is possible that the relatively high
proportion of past or current smokers in the white population
NA, not applicable.
a Values are presented as mean ± SD or number (%). Percentages that do not add up contributed to the greater degree of chorangiosis in that popu-
to 100% denote missing or unknown data. lation, although both populations’ insulin dependence during
b Nonwhite group includes all categories except white and “unknown.”
c Significant at P < .05.
pregnancy should also be considered.
590 Am J Clin Pathol 2014;141:587-592 © American Society for Clinical Pathology
590 DOI: 10.1309/AJCPX81AUNFPOTLL
AJCP / Original Article
A B
Downloaded from https://academic.oup.com/ajcp/article-abstract/141/4/587/1761455 by guest on 25 April 2020
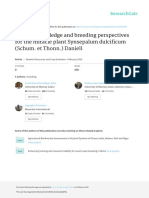
❚Image 1❚ Mature placentas at ×20. A, Chorangiosis. Multiple capillaries are in all villi with villous expansion (H&E). B, Normal
nonchorangiotic placenta showing normal number of capillaries in villi (H&E).
Several studies have considered glycemic control during of chorangiosis in our population. In addition, to elucidate the
pregnancy when investigating placental pathology associated observed racial difference in the degree of chorangiosis, it
with diabetes. Calderon et al17 found that abnormal glycemic would be beneficial to examine a population of white women
levels could contribute to morphometric abnormalities observed without GDM to distinguish this association with chorangio-
in the GDM placenta. Gauster et al8 supported these findings, sis as race mediated or GDM associated. Furthermore, we had
concluding that poorly controlled GDM could result in villous limited racial/ethnic diversity within our nonwhite population.
edema and increased fibrin in the placenta. While GDM has This could have limited the differences between the white and
numerous implications for the vasculature and gross charac- nonwhite populations.
teristics of the placenta, it has also been shown to contribute In summary, we identified that chorangiosis was more
to impaired placental function, including reduced glucose prevalent among white compared with nonwhite women with
metabolism and the ability to metabolize other substrates.18,19 GDM. Excluding chorangiosis, we found that the placental
Alternatively, good glycemic control during pregnancy pathology of the white and nonwhite women did not differ
reduces adverse clinical pregnancy outcomes associated with significantly. This finding is clinically relevant for at least two
GDM,20 but normoglycemia does not mediate all the patho- reasons. First, the placentas of women with GDM may not
logic characteristics associated with GDM.21-23 In our popula- undergo routine pathologic examination depending on institu-
tion, the only pathologic difference was that chorangiosis was tional practice. However, our findings suggest that placental
significantly more prevalent among the white compared with pathologic examination may demonstrate changes with impli-
the nonwhite women with GDM. Because we do not know the cations for maternal postpartum cardiometabolic disease risk
degree of insulin use or glycemic control of these women, we surveillance. Second, the identification of placental pathology
do not know if the greater incidence of chorangiosis among may serve as an indicator of underlying maternal disease. For
white women resulted from greater intrapartum insulin use, example, in our study, we identified a racial/ethnic differ-
presumably leading to improved intrapartum glycemic control ence in the presence of chorangiosis, which has been directly
and consequently less T2DM development subsequent to preg- linked to clinical parameters such as maternal dysglycemia
nancy. Conversely, more intrapartum insulin use among non- and anemia.13 Consequently, this may be correlated with the
white women with GDM would be consistent with data sug- prenatal measurements of these parameters and potentially
gesting an increased rate of subsequent development of T2DM lead to the consideration of additional prenatal intervention in
in this setting.24 Nonetheless, we require the data regarding certain populations.
insulin use and glycemic control to clarify this relationship. Further study is warranted to determine the cause of
Accordingly, one limitation of our study is the lack of greater chorangiosis in our white population and examine
information on glucose control or insulin use during pregnan- whether this observation is related to smoking, insulin use,
cy. These data would facilitate the elucidation of the etiology glycemic control, or specifically race. We also found that
© American Society for Clinical Pathology Am J Clin Pathol 2014;141:587-592 591
591 DOI: 10.1309/AJCPX81AUNFPOTLL 591
Bentley-Lewis et al / Placental Histomorphometry in GDM
more nonwhite women developed T2DM after pregnancy 8. Gauster M, Desoye G, Totsch M, et al. The placenta and
than white women in our GDM population. However, fur- gestational diabetes mellitus. Curr Diabetes Rep. 2012;12:16-
23.
ther research is necessary to determine if the higher rate of
9. Ashfaq M, Janjua MZ, Channa MA. Effect of gestational
subsequent T2DM in nonwhite populations is associated with diabetes and maternal hypertension on gross morphology
differences in placental pathology. This may provide another of placenta. J Ayub Med Coll. 2005;17:44-47.
opportunity for risk stratification in GDM populations to 10. Wolf M, Sandler L, Muñoz K, et al. First trimester insulin
inform evidence-based interventions to alleviate racial/ethnic resistance and subsequent preeclampsia: a prospective study.
J Clin Endocrinol Metab. 2002;87:1563-1568.
disparities in GDM and T2DM.
11. Carpenter MW, Coustan DR. Criteria for screening tests for
gestational diabetes. Am J Obstet Gynecol. 1982;144:768-773.
Address reprint requests to Dr Bentley-Lewis, Massachusetts
12. Stallmach T, Hebisch G, Meier K, et al. Rescue by birth:
General Hospital, 55 Fruit St, Bulfinch 4-415, Boston, MA 02114; defective placental maturation and late fetal mortality. Obstet
e-mail: Bentley-Lewis.Rhonda@mgh.harvard.edu.
Downloaded from https://academic.oup.com/ajcp/article-abstract/141/4/587/1761455 by guest on 25 April 2020
Gynecol. 2001;97:505-509.
13. Ogino S, Redline RW. Villous capillary lesions of the
This study was supported by grant 1R03DK096152 from placenta: distinctions between chorangioma, chorangioma-
the National Institutes of Health (NIH) and the Robert Wood tosis, and chorangiosis. Hum Pathol. 2000;31:945-954.
Johnson Foundation Harold Amos Medical Faculty Development
14. Redline RW. Villitis of unknown etiology: noninfectious
Program (R.B.-L.); Harvard Catalyst Summer Clinical and chronic villitis in the placenta. Hum Pathol. 2007;38:1439-
Translational Research Program (D.L.D.); K24 DK094872 from 1446.
the NIH (R.I.T.); and the Massachusetts General Hospital (MGH) 15. Redline RW, Faye-Petersen O, Heller D, et al. Amniotic
Pathology Department (D.J.R.). infection syndrome: nosology and reproducibility of placental
These data were presented in part as an abstract poster reaction patterns. Pediatr Dev Pathol. 2003;6:435-448.
presentation at the Endocrine Society’s 95th Annual Meeting; 16. Redline RW, Ariel I, Baergen RN, et al. Fetal vascular
June 15, 2013; San Francisco, CA. obstructive lesions: nosology and reproducibility of placental
Acknowledgments: We thank Kaitlyn Barnes, Stella St. reaction patterns. Pediatr Dev Pathol. 2004;7:443-452.
Hubert, Grace Xiong, Melissa Ong, Annie Yang, and Jennifer 17. Calderon IM, Damasceno DC, Amorin RL, et al.
Huynh of the MGH Diabetes Research Center for their assistance Morphometric study of placental villi and vessels in women
with data compilation and manuscript preparation. with mild hyperglycemia or gestational or overt diabetes.
Diabetes Res Clin Pract. 2007;78:65-71.
18. Osmond DT, Nolan CJ, King RG, et al. Effects of gestational
References diabetes on human placental glucose uptake, transfer, and
utilisation. Diabetologia. 2000;43:576-582.
1. Coustan DR, Lowe LP, Metzger BE, et al. The Hyperglycemia
and Adverse Pregnancy Outcome (HAPO) study: paving 19. Sobrevia L, Abarzua F, Nien JK, et al. Review: differential
the way for new diagnostic criteria for gestational diabetes placental macrovascular and microvascular endothelial
mellitus. Am J Obstet Gynecol. 2010;202:654.e1-6. dysfunction in gestational diabetes. Placenta. 2011;32(suppl
2):S159-S164.
2. Bentley-Lewis R. Late cardiovascular consequences
of gestational diabetes mellitus. Semin Reprod Med. 20. Langer O, Rodriguez DA, Xenakis EM, et al. Intensified
2009;27:322-329. versus conventional management of gestational diabetes.
Am J Obstet Gynecol. 1994;170:1036-1046.
3. Winhofer Y, Tura A, Prikoszovich T, et al. The impact of
recurrent gestational diabetes on maternal metabolic and 21. Gheorman L, Plesea IE, Gheorman V. Histopathological
cardiovascular risk factors. Eur J Clin Invest. 2013;43:190- considerations of placenta in pregnancy with diabetes.
197. Romanian J Morphol Embryol. 2012;53:329-336.
4. Wang Y, Zhao S. Placental blood circulation. In: Vascular 22. Jones CJ, Fox H. Placental changes in gestational diabetes:
Biology of the Placenta. San Rafael, CA: Morgan & Claypool an ultrastructural study. Obstet Gynecol. 1976;48:274-280.
Life Sciences; 2010:3-12. 23. al-Okail MS, al-Attas OS. Histological changes in placental
5. Regnault TR, Galan HL, Parker TA, et al. Placental syncytiotrophoblasts of poorly controlled gestational diabetic
development in normal and compromised pregnancies— patients. Endocrine J. 1994;41:355-360.
a review. Placenta. 2002;23(suppl A):S119-S129. 24. Lee AJ, Hiscock RJ, Wein P, et al. Gestational diabetes
6. Jauniaux E, Burton GJ. Villous histomorphometry and mellitus: clinical predictors and long-term risk of developing
placental bed biopsy investigation in type I diabetic type 2 diabetes: a retrospective cohort study using survival
pregnancies. Placenta. 2006;27:468-474. analysis. Diabetes Care. 2007;30:878-883.
7. Beauharnais CC, Roberts DJ, Wexler DJ. High rate of
placental infarcts in type 2 compared with type 1 diabetes.
J Clin Endocrinol Metab. 2012;97:E1160-E1164.
592 Am J Clin Pathol 2014;141:587-592 © American Society for Clinical Pathology
592 DOI: 10.1309/AJCPX81AUNFPOTLL
You might also like
- Management of Hereditary Colorectal Cancer: A Multidisciplinary ApproachFrom EverandManagement of Hereditary Colorectal Cancer: A Multidisciplinary ApproachJose G. GuillemNo ratings yet
- Breast Disease: Diagnosis and Pathology, Volume 1From EverandBreast Disease: Diagnosis and Pathology, Volume 1Adnan AydinerNo ratings yet
- NIH Public Access: Placental Histomorphometry in Gestational Diabetes MellitusDocument13 pagesNIH Public Access: Placental Histomorphometry in Gestational Diabetes MellitusMayra PereiraNo ratings yet
- Disbetes Obs PDFDocument18 pagesDisbetes Obs PDFdhruvNo ratings yet
- Prevalence of Diabetes Mellitus Amongst Antenatal Clinic Attendees at Booking in A Teaching Hospital in Rivers State, NigeriaDocument3 pagesPrevalence of Diabetes Mellitus Amongst Antenatal Clinic Attendees at Booking in A Teaching Hospital in Rivers State, NigeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Gestational Diabetes Risk Factors and Long-Term Consequences For Both Mother and Offspring: A Literature ReviewDocument27 pagesGestational Diabetes Risk Factors and Long-Term Consequences For Both Mother and Offspring: A Literature ReviewBala ChandiranNo ratings yet
- Pre-Existing Diabetes Mellitus and Adverse PDFDocument5 pagesPre-Existing Diabetes Mellitus and Adverse PDFMetebNo ratings yet
- Ni Hms 713785Document16 pagesNi Hms 713785mnn164No ratings yet
- A Prospective Study of Gestational DMDocument6 pagesA Prospective Study of Gestational DMOdilia Rondang Mauli SimarmataNo ratings yet
- Gestational Diabetes Mellitus Acog CopDocument8 pagesGestational Diabetes Mellitus Acog CopAndrea Sandoval OteroNo ratings yet
- Ref 3Document10 pagesRef 3asshagab04No ratings yet
- Articulo de InvestigacionDocument8 pagesArticulo de Investigacionjai_santiago_rojasNo ratings yet
- ACOG Practice Bulletin No137 PDFDocument11 pagesACOG Practice Bulletin No137 PDFRodrigo Pérez CuelloNo ratings yet
- PIIS0002937821019992Document2 pagesPIIS0002937821019992made dharmaNo ratings yet
- Ensemble1-2022-Analysis and Prediction of Gestational Diabetes MellitusDocument20 pagesEnsemble1-2022-Analysis and Prediction of Gestational Diabetes MellitusMeriam Jemel HachichaNo ratings yet
- Overweight and The Metabolic Syndrome in Adult Offspring of Women With Diet-Treated Gestational Diabetes Mellitus or Type 1 DiabetesDocument7 pagesOverweight and The Metabolic Syndrome in Adult Offspring of Women With Diet-Treated Gestational Diabetes Mellitus or Type 1 DiabetesMyoman FernandaNo ratings yet
- VHRM 5 085Document4 pagesVHRM 5 085Agus WijayaNo ratings yet
- By Guest On 26 April 2018Document8 pagesBy Guest On 26 April 2018silvanaNo ratings yet
- Diabetes Mellitus and Pregnancy: Chapter OutlineDocument21 pagesDiabetes Mellitus and Pregnancy: Chapter OutlineqalbiNo ratings yet
- Diabetes GAM 2015Document7 pagesDiabetes GAM 2015Anonymous qsegfnnOdNo ratings yet
- Jurnal Na 2Document7 pagesJurnal Na 2Febri AkneldoNo ratings yet
- Gdiabetes GENESDocument7 pagesGdiabetes GENESsalman672003No ratings yet
- Video 12 PDFDocument5 pagesVideo 12 PDFAndreas NatanNo ratings yet
- Biomarkers Predictive of Gestational Diabetes Mellitus Appearing Before Impaired Glucose ToleranceDocument9 pagesBiomarkers Predictive of Gestational Diabetes Mellitus Appearing Before Impaired Glucose ToleranceTomNo ratings yet
- Advances in Prenatal Screening For Down Syndrome - General Principles and Second Trimester TestingDocument16 pagesAdvances in Prenatal Screening For Down Syndrome - General Principles and Second Trimester TestingMáthé AdriennNo ratings yet
- Maternal and Perinatal Outcomes in PGDM vs GDMDocument6 pagesMaternal and Perinatal Outcomes in PGDM vs GDMrischaNo ratings yet
- Preterm Parturition and Pre-Eclampsia: The Confluence of Two Great Gestational SyndromesDocument7 pagesPreterm Parturition and Pre-Eclampsia: The Confluence of Two Great Gestational SyndromesmarinanananaNo ratings yet
- 176S Tuesday Posters Obstetrics & GynecologyDocument1 page176S Tuesday Posters Obstetrics & GynecologyJoseph BennettNo ratings yet
- Local Versus International Criteria in Predicting Gestational Diabetes Mellitus Related Pregnancy OutcomesDocument10 pagesLocal Versus International Criteria in Predicting Gestational Diabetes Mellitus Related Pregnancy OutcomesCj CCNo ratings yet
- Diabetes EmbarazoDocument18 pagesDiabetes EmbarazoLorain CossioNo ratings yet
- HHS Public Access: Gestational Diabetes MellitusDocument19 pagesHHS Public Access: Gestational Diabetes MellitusAnne MarieNo ratings yet
- Febriyanti M. AdamDocument23 pagesFebriyanti M. AdamRinda UnoNo ratings yet
- Adolescent Dairy Product Consumption and Risk of Type 2 Diabetes in Middle-Aged WomenDocument8 pagesAdolescent Dairy Product Consumption and Risk of Type 2 Diabetes in Middle-Aged WomenWoodyNo ratings yet
- Gestational Diabetes Literature ReviewDocument12 pagesGestational Diabetes Literature Reviewc5rfkq8n100% (1)
- CDC 84627 DS1Document15 pagesCDC 84627 DS1Thu HoaiNo ratings yet
- DM Gestacional 2014Document6 pagesDM Gestacional 2014mariajuliabechepecheNo ratings yet
- First-Trimester Biomarker Panel May Predict Gestational DiabetesDocument6 pagesFirst-Trimester Biomarker Panel May Predict Gestational DiabetesDevianti TandialloNo ratings yet
- Syphilis in PregnancyDocument17 pagesSyphilis in PregnancyKevin Stanley HalimNo ratings yet
- Thomas 2017Document21 pagesThomas 2017TarNo ratings yet
- Diabetes Gestacional 2022 NejmDocument12 pagesDiabetes Gestacional 2022 NejmGabrielaNo ratings yet
- Medical Record Validation of Maternally Reported History of PreeclampsiDocument7 pagesMedical Record Validation of Maternally Reported History of PreeclampsiezaNo ratings yet
- Gestational Diabetes - On Broadening The DiagnosisDocument2 pagesGestational Diabetes - On Broadening The DiagnosisWillians ReyesNo ratings yet
- Original Articles: Reproductive Endocrinology: A A B C D e e ADocument11 pagesOriginal Articles: Reproductive Endocrinology: A A B C D e e ACoco MelonNo ratings yet
- The obstetrician's role in preventing long-term cardiometabolic diseaseDocument8 pagesThe obstetrician's role in preventing long-term cardiometabolic diseaseKeeranmayeeishraNo ratings yet
- ÓbitoDocument111 pagesÓbitoDamián López RangelNo ratings yet
- DownloadDocument6 pagesDownloadKai GgNo ratings yet
- Gestational Diabetes Mellitus Update and Review of Literature 2161 038X.S2 008 PDFDocument6 pagesGestational Diabetes Mellitus Update and Review of Literature 2161 038X.S2 008 PDFBuluan Mps McadNo ratings yet
- A Case Analysis OnDocument27 pagesA Case Analysis Onbunso padillaNo ratings yet
- Cohort Profile: NICHD Fetal Growth Studies - Singletons and TwinsDocument13 pagesCohort Profile: NICHD Fetal Growth Studies - Singletons and Twinselin luhulimaNo ratings yet
- ACOG Management of Stillbirth PDFDocument14 pagesACOG Management of Stillbirth PDFLêMinhĐứcNo ratings yet
- Literature Review On Prevalence of Gestational DiabetesDocument8 pagesLiterature Review On Prevalence of Gestational DiabetesafdtrajxqNo ratings yet
- Jurnal PerinaDocument7 pagesJurnal PerinaBhismo PasetyoNo ratings yet
- 3 IncidenceDocument13 pages3 IncidenceRonald Ivan WijayaNo ratings yet
- Gestational Diabetes Mellitus ThesisDocument4 pagesGestational Diabetes Mellitus Thesisbseb81xq100% (2)
- Pregnancy and Child Health Outcomes in Pediatric and Young Adult Leukemia and Lymphoma Survivors: A Systematic ReviewDocument25 pagesPregnancy and Child Health Outcomes in Pediatric and Young Adult Leukemia and Lymphoma Survivors: A Systematic ReviewAbdurrahman HasanuddinNo ratings yet
- Metabolic Syndrome in Childhood: Association With Birth Weight, Maternal Obesity, and Gestational Diabetes MellitusDocument9 pagesMetabolic Syndrome in Childhood: Association With Birth Weight, Maternal Obesity, and Gestational Diabetes MellitusAnnisa FujiantiNo ratings yet
- Genetics of childhood obesity and high-throughput DNA sequencingDocument45 pagesGenetics of childhood obesity and high-throughput DNA sequencingvisiniNo ratings yet
- Analysis of Patterns of Patient Compliance After An Abnormal Pap Smear Result The Influence of Demographic Characteristics On Patient ComplianceDocument5 pagesAnalysis of Patterns of Patient Compliance After An Abnormal Pap Smear Result The Influence of Demographic Characteristics On Patient Compliancevyvie89No ratings yet
- Complementary and Alternative Medical Lab Testing Part 10: ObstetricsFrom EverandComplementary and Alternative Medical Lab Testing Part 10: ObstetricsNo ratings yet
- Diagnosis and Management of Hereditary Cancer: Tabular-Based Clinical and Genetic AspectsFrom EverandDiagnosis and Management of Hereditary Cancer: Tabular-Based Clinical and Genetic AspectsNo ratings yet
- Demir 2007Document9 pagesDemir 2007Mayra PereiraNo ratings yet
- Modelo DMGDocument5 pagesModelo DMGMayra PereiraNo ratings yet
- Review Article: Streptozotocin-Induced Diabetes Models: Pathophysiological Mechanisms and Fetal OutcomesDocument12 pagesReview Article: Streptozotocin-Induced Diabetes Models: Pathophysiological Mechanisms and Fetal OutcomesMayra PereiraNo ratings yet
- Ijcep0008 5196Document7 pagesIjcep0008 5196Mayra PereiraNo ratings yet
- AerobicDocument7 pagesAerobicMayra PereiraNo ratings yet
- Physiology and Pathophysiology of Steroid Biosynthesis, Transport and Metabolism in The Human PlacentaDocument29 pagesPhysiology and Pathophysiology of Steroid Biosynthesis, Transport and Metabolism in The Human PlacentaMayra PereiraNo ratings yet
- Maternal Exercise Alters Placental mTOR and Nutrient TransportDocument14 pagesMaternal Exercise Alters Placental mTOR and Nutrient TransportMayra PereiraNo ratings yet
- Placenta: SciencedirectDocument8 pagesPlacenta: SciencedirectMayra PereiraNo ratings yet
- Endocrinology & Metabolic SyndromeDocument13 pagesEndocrinology & Metabolic SyndromeMayra PereiraNo ratings yet
- Holmes PDFDocument6 pagesHolmes PDFMayra PereiraNo ratings yet
- Placenta Changes in Pregnancy With Gestational Diabetes: R I G I N A L A P E RDocument6 pagesPlacenta Changes in Pregnancy With Gestational Diabetes: R I G I N A L A P E RMayra PereiraNo ratings yet
- A Study of Placental Histological Changes in Gestational - Mulheres PDFDocument4 pagesA Study of Placental Histological Changes in Gestational - Mulheres PDFMayra PereiraNo ratings yet
- Who PDFDocument23 pagesWho PDFMayra PereiraNo ratings yet
- Shafiullah PDFDocument12 pagesShafiullah PDFMayra PereiraNo ratings yet
- Exercise and Skeletal Muscle Glucose Transporter 4 Expression: Molecular MechanismsDocument5 pagesExercise and Skeletal Muscle Glucose Transporter 4 Expression: Molecular MechanismsMayra PereiraNo ratings yet
- Who Klasifikasi 2019Document40 pagesWho Klasifikasi 2019Amel fNo ratings yet
- Gestational Diabetes: Key PointsDocument5 pagesGestational Diabetes: Key PointsMayra PereiraNo ratings yet
- Exercise and Skeletal Muscle Glucose Transporter 4 Expression: Molecular MechanismsDocument5 pagesExercise and Skeletal Muscle Glucose Transporter 4 Expression: Molecular MechanismsMayra PereiraNo ratings yet
- Vargas Terrones2018 2Document6 pagesVargas Terrones2018 2alvaro alarconNo ratings yet
- Who Klasifikasi 2019Document40 pagesWho Klasifikasi 2019Amel fNo ratings yet
- Who PDFDocument23 pagesWho PDFMayra PereiraNo ratings yet
- Da Silva PDFDocument5 pagesDa Silva PDFMayra PereiraNo ratings yet
- Vargas Terrones2018 2Document6 pagesVargas Terrones2018 2alvaro alarconNo ratings yet
- Gestational Diabetes: Key PointsDocument5 pagesGestational Diabetes: Key PointsMayra PereiraNo ratings yet
- Holmes PDFDocument6 pagesHolmes PDFMayra PereiraNo ratings yet
- Shafiullah PDFDocument12 pagesShafiullah PDFMayra PereiraNo ratings yet
- Da Silva PDFDocument5 pagesDa Silva PDFMayra PereiraNo ratings yet
- 2000 - Maximal Lactate-Steady-State Independent of Performance (Med. Sci. Sports Exerc.) PDFDocument5 pages2000 - Maximal Lactate-Steady-State Independent of Performance (Med. Sci. Sports Exerc.) PDFMayra PereiraNo ratings yet
- WJD 2 196 PDFDocument8 pagesWJD 2 196 PDFMayra PereiraNo ratings yet
- International Journal of Cardiology May 2021 Issue 1Document275 pagesInternational Journal of Cardiology May 2021 Issue 1Fareesha KhanNo ratings yet
- Bible Aromatherapy 2022Document39 pagesBible Aromatherapy 2022johanjacobvelosagomezNo ratings yet
- Session 10. Review of Centric Records RECORDSDocument25 pagesSession 10. Review of Centric Records RECORDSbaraa.abdulrahman.23No ratings yet
- Anaesthesia For Adenotonsillectomy An UpdateDocument7 pagesAnaesthesia For Adenotonsillectomy An UpdateSrihari JanakiNo ratings yet
- Misconceptions About The Use of Genetic Tests in PopulationsDocument4 pagesMisconceptions About The Use of Genetic Tests in PopulationsAneeshNo ratings yet
- Vaccine Excipient & Media Summary: Excipients Included in U.S. Vaccines, by VaccineDocument4 pagesVaccine Excipient & Media Summary: Excipients Included in U.S. Vaccines, by VaccineZeljko RasoNo ratings yet
- Anti - HyperlipidemiaDocument18 pagesAnti - HyperlipidemiaZakarie Abdullahi Hussein100% (1)
- Manual For Dental TechniciansDocument186 pagesManual For Dental Techniciansstabik96% (23)
- Nursing Care Plan For GlaucomaDocument3 pagesNursing Care Plan For Glaucomaderic79% (28)
- Genetic Disorders: Chromosomal Abnormalities and Down SyndromeDocument27 pagesGenetic Disorders: Chromosomal Abnormalities and Down SyndromeMerwan KemalNo ratings yet
- Case Presentation - Group 9 - B - Medix Medical HospitalDocument31 pagesCase Presentation - Group 9 - B - Medix Medical HospitalChantemayne VillanuevaNo ratings yet
- Drug Metabolism-LectDocument35 pagesDrug Metabolism-LectFiona OyatsiNo ratings yet
- List of International Days and WeeksDocument10 pagesList of International Days and WeeksSatram RoopaniNo ratings yet
- Clinical Efficiency of Three Caries Removal Systems: Rotary Excavation, Carisolv, and PapacarieDocument8 pagesClinical Efficiency of Three Caries Removal Systems: Rotary Excavation, Carisolv, and PapacarieVianney Guadalupe González ElizaldeNo ratings yet
- Effect of Deep Breathing on Blood Pressure in Hypertensive PatientsDocument10 pagesEffect of Deep Breathing on Blood Pressure in Hypertensive PatientssendyNo ratings yet
- Introduction to Radiotherapy: Blackboard AssignmentDocument2 pagesIntroduction to Radiotherapy: Blackboard AssignmentRafaNo ratings yet
- Community Question Bank (N.a)Document41 pagesCommunity Question Bank (N.a)Sumaya AfifyNo ratings yet
- DVLA Null NewDocument1 pageDVLA Null NewTaniaNo ratings yet
- Epidemiologi DialipidemiaDocument5 pagesEpidemiologi DialipidemianurfitrizuhurhurNo ratings yet
- Guidelines For Case Classification For The National Birth Defects Prevention StudyDocument9 pagesGuidelines For Case Classification For The National Birth Defects Prevention Studyjorge davidNo ratings yet
- Risk factors of diabetic retinopathy and vision threatening diabetic retinopathy and vision threatening diabetic retinopaty based on diabetic retinopathy screening program in greater bandung, west java.astriDocument14 pagesRisk factors of diabetic retinopathy and vision threatening diabetic retinopathy and vision threatening diabetic retinopaty based on diabetic retinopathy screening program in greater bandung, west java.astriSi PuputNo ratings yet
- Khatib2017 PDFDocument14 pagesKhatib2017 PDFluxmansrikanthaNo ratings yet
- NCP For Older Adults With Sleep DisturbanceDocument17 pagesNCP For Older Adults With Sleep DisturbanceAlienda Puspita PutriNo ratings yet
- Cadorna, Chesca L. - NCPDocument2 pagesCadorna, Chesca L. - NCPCadorna Chesca LoboNo ratings yet
- Prenatal Development and Birth: The Developing Person Through The Life Span Kathleen Stassen Berger - Tenth EditionDocument42 pagesPrenatal Development and Birth: The Developing Person Through The Life Span Kathleen Stassen Berger - Tenth EditionJoel PayneNo ratings yet
- Achigan-DakoTchokponhoueNDanikouetal 2015Document13 pagesAchigan-DakoTchokponhoueNDanikouetal 2015Juan Pablo Hernandez PaezNo ratings yet
- Podcast Script "Hustle Culture" OPENING: Haiii I'am Hidayah Malika and Welcome To Speak Up' PodcastDocument3 pagesPodcast Script "Hustle Culture" OPENING: Haiii I'am Hidayah Malika and Welcome To Speak Up' PodcastMas'adatul HidayahNo ratings yet
- 13 AntibioticsAntiRetroviralsAIDS PDFDocument90 pages13 AntibioticsAntiRetroviralsAIDS PDFjenniferluzonNo ratings yet
- Physical Fitness Physical FitnessDocument18 pagesPhysical Fitness Physical FitnessCharmaine JanorasNo ratings yet
- Heavenly Spa MenuDocument2 pagesHeavenly Spa MenuDeTaaliNo ratings yet