Professional Documents
Culture Documents
4AR. Proposal For A Protocolo Frenillo Alterado
Uploaded by
Andrea Díaz RodríguezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
4AR. Proposal For A Protocolo Frenillo Alterado
Uploaded by
Andrea Díaz RodríguezCopyright:
Available Formats
Proposal for a
myofunctional therapy S. Saccomanno*, A. Di Tullio***,
protocol in case of
L. D’Alatri**, C. Grippaudo*
Fondazione Policlinico Universitario A. Gemelli IRCCS,
Roma, Università Cattolica del Sacro Cuore, Rome, italy
altered lingual frenulum.
*Dental Institute, Head and Neck Department
**Otorhinolaryngology, Head and Neck Department,
***ENT, Università Cattolica del Sacro Cuore
A pilot study
e-mail: sabinasaccomanno@hotmail.it
DOI 10.23804/ejpd.2019.20.01.13
Abstract Introduction
The lingual frenulum is a fibromucosal tissue extending
In this article, the authors propose a specific
from the floor of the mouth to the midline of the ventral
Myofunctional Therapy Protocol for patients with
surface of the tongue. The primary function of the frenulum
altered lingual frenulum. In such cases tongue
muscles are hypofunctioning and their range is to keep a balance between the growing bones, the
of motion is reduced. To compensate for this tongue and the lip muscles during fetal development, and
limitation, dysfunctional lingual motor patterns to limit the movement of the muscular tissues like lips,
are established, such as the use of some muscles tongue and cheeks [Srinivasan and Chitharanjan, 2013]. The
at the expense of others; this negatively affects the alteration of the lingual frenulum is a congenital anomaly
development and functions of the stomatognathic that limits tongue mobility and has a series of implications
system. The Myofunctional Therapy Protocol for the stomatognathic system, resulting in a critical impact
presented in this pilot study was developed with the on the oral functions and therefore on the growth and
aim of making the muscles of the tongue, the floor development of the orofacial complex. The onset of this
of the mouth and the soft palate more coordinated, congenital anomaly shows a greater impact in males rather
and increasing muscle contraction strength, in order than females, with a ratio of 3:1 and with a 5% incidence
to produce improvements on the muscle tone, on reported at birth [Huang et al., 2015]. The main impairments
orofacial and nasal functions and a better wound
concern breastfeeding [Bhattad et al., 2013; Pompéiaa et al.,
healing and functional recovery in the case of
surgical therapy (frenulotomy).
2017; Yoon et al., 2017a], craniofacial growth [Pompéiaa et
al., 2017; Srinivasan et al., 2013; Yoon et al., 2017b], dental
occlusion [Bhattad et al., 2013; Vaz and Bai, 2015; Yoon et
al., 2017a], breathing [Bhattad et al., 2013; Pompéiaa et al.,
2017; Yoon et al., 2017a], swallowing [Bhattad et al., 2013;
Pompéiaa et al., 2017; Yoon et al., 2017a], verbal articulation
[Pompéiaa et al., 2017; Suzart and de Carvalho, 2016], social
and relational aspects [Bhattad et al., 2013]; it is also related
to the syndrome of obstructive sleep apnea [Guilleminault et
al., 2016; Huang et al., 2015]. Myofunctional rehabilitation
aims to increase awareness of correct postures, optimisation
of amplitude, accuracy, coordination of tongue movements,
strengthening muscular and functional capacities and optimal
participation of the tongue in all other lingual functions such
as swallowing, chewing, and non-verbal functions. Above all,
it is important to make these processes automatic through
repetition, for the principle of neuroplasticity and cortical
reorganisation during the motor rehabilitation process. It is
this automatism that is the most difficult target to achieve,
so it is important to provide a maintenance protocol to keep
stability over time. In this article it is presented a Myofunctional
KEYWORD Altered lingual frenulum, Deviate Therapy Protocol, simple to perform for patients and which is
swallowing, Myofunctional therapy, Short lingual useful for enhancing orofacial and nasal functions in cases of
frenulum, Tongue-tie. altered lingual frenulum.
European Journal of Paediatric Dentistry vol. 20/1-2019 67
SACCOMANNO S. E.T AL
100% 8 7
Tongue strength Lip strength
50
83
6
47
75% 5 5
4
4 4 5 40 38
50% 40
2
25%
17 0 30 27
0% D.V. D.T. MI. MA. B.B. F.P. 26
23 23
Male Female Sample 19
20
13 15
FIG. 1 Male prevalence of the sample. FIG. 2 Respiratory type. 11 10
10
Materials and methods 0
D.V. D.T. MI. MA. B.B. F.P. D.V. D.T. MI. MA. B.B. F.P.
The sample comprised 6 children (5 males and 1 female), aged
Sample
between 4.5 and 11.7 years (mean age of 7.7 years). The inclusion
criterion was the presence of an altered lingual frenulum; the FIG. 3 IOPI – Measure of strength in kPA.
exclusion criteria were: the presence of genetic syndromes,
malformations, auditory, cognitive and motor abnormalities.
The sample underwent a dental and orthodontic examination
and no cavities were found in any subject. Parents were asked Tongue endurance Lip endurance
to fill out a questionnaire on eating habits, oral hygiene habits, 35
fluoride prophylaxis and family history of caries [Paglia et al., 30
2016]. To estimate the risk of malocclusion, the ROMA index 30
(Risk Of Malocclusion Assessment) [Grippaudo et al., 2008] 24
25
was applied in 5 patients in mixed dentition and the Baby- 22
ROMA index [Grippaudo et al., 2014] for the patient in primary 20
dentition. The 5 patients in mixed dentition obtained Grade 3
of the ROMA index and were classified as "moderate risk", due 15
to the presence of moderate changes in dental and/or skeletal 12 10
relationships, but tending to persist and worsen over time. The 10 10 9 9
7
patient in primary dentition was classified as having Grade 1 5 5 6
of the Baby-ROMA index for which the risk of malocclusion 5
is considered mild and routine checks are recommended to
0
monitor the occlusion. Early treatment of orthodontic problems D.V. D.T. MI. MA. B.B. F.P. D.V. D.T. MI. MA. B.B. F.P.
can be useful in preventing the worsening of the condition in
permanent dentition [Grippaudo et al., 2013a]. Sample
The sample was submitted to myofunctional evaluation at
the Orthodontics department of the Gemelli University Hospital FIG. 4 IOPI – Measure of endurance in seconds.
in Rome. All evaluations were conducted by the same speech
therapist, to minimise variability. This one-on-one 60 min tongue tip to maxillary Incisive papillae at roof of mouth
individual assessment was carried out in a single session. The (MIOTTIP) to maximal interincisal mouth opening (MIO) and
assessment method included a functional analysis through it identifies functional ankyloglossia [Yoon et al., 2017a],
standardised and non-standardised tools, such as: reporting a degree 3 of tongue mobility, which is significantly
• The Lingual Frenulum Protocol [Marchesan, 2012]; below average, in 5 out of 6 cases (Fig. 5). The analysis of the
• Iowa Oral Performance Instrument (IOPI Pro), evaluation of respiratory type shows that with a score of 4/13, 2 children have
the tongue and lips strength and endurance [Adams et al., a nasal breathing, while 4 children with a score between 5-7/13,
2013; Clark et al., 2009]; have slight oro-nasal breathing (Fig. 2).
• Assessment of the airway and expiratory permeability test Following the baseline evaluation, the study sample was
with the adapted oronasal plaque, from the Protocol for trained by the same speech therapist to correctly execute the
the Phonoaudiological Assessment of Breathing with Scores exercises of the Myofunctional Therapy Protocol. Later, the
(ProPABS) [Susanibar and Dacillo, 2015]; sample was randomly divided into 3 groups.
• Clinical examination of the swallowing of saliva, water and The first group included 2 patients studied as a control, to
biscuit (Kinder Cards, Ferrero); whom no therapy was prescribed.
• Video and photographic documentation. The second group included 2 patients who were prescribed
In the enrolled sample a positive correlation between the the home exercises according to the Myofunctional Therapy
predominance of short lingual frenulum [Huang et al., 2015] in Protocol, to be performed daily without the supervision of the
males is reported (Fig. 1). From the myofunctional evaluation speech therapist.
of the sample, data can be traced back to a prominent The third group included 2 patients treated by the same
hypofunction of the tongue muscles and of the orbicularis oris speech therapist for 3 weeks, with a frequency of 3 office visits
(Fig. 3, 4). The tongue range of motion ratio (TRMR) is a ratio of per week, which was associated with the assignment of home
mouth opening with exercises of the proposed Protocol.
68 European Journal of Paediatric Dentistry vol. 20/1-2019
PAEDIATRIC ORAL PATHOLOGY
MIO MIOTTIP TRMR %
80
60
59
46,3 46,1 46
33,7 39
40 34
31,6
27,2 27
23
18 18 17
20
8,8 11
6,1 6,7
0
D.V. D.T. MI. MA. B.B. F.P. D.V. D.T. MI. MA. B.B. F.P. D.V. D.T. MI. MA. B.B. F.P.
Sample
FIG. 5 Restriction of tongue mobility in mm and percentage report.
Tongue strength Lip strength Tongue strength Lip strength
60 50
47 51 40 40
50
40
40
30
26
30 23
20 19 19
15 18
20 11 11 13 13
14
10 10
10
0 0
F.P. F.P. B.B. B.B. F.P. F.P. B.B. B.B. D.V. D.V. D.T. D.T. D.V. D.V. D.T. D.T.
after after after after after after after after
3 3 3 3 3 3 3 3
weeks weeks weeks weeks weeks weeks weeks weeks
FIG. 6 IOPI – Measure of strength in kPA, pre- and post-TMF. FIG. 7 IOPI – Measure of strength in kPA, Control group.
The treatment practice developed for this pilot study included to help the patient become aware of the morphology of the
the Myofunctional Therapy Protocol, which was complemented oral cavity and in particular of the tongue and the palate, as a
by the Therapy Diary for conducting home exercises. The prerequisite to restore functional neuromuscular patterns.
Protocol consisted of 8 exercises, divided according to the Proposed exercises
functional goals to be pursued. Each goal included 2 exercises, 1. Raise the tip of the tongue on the maxillary incisive papillae
for each of which there were 15 repetitions. To make therapy and then exercise a light suction. Hold this position for 10
more motivating and increase the compliance of patients in seconds.
the developmental age, the exercises have been proposed 2. Place the tip of the tongue on the maxillary incisive papillae,
in a playful formulation. In the same way, the Therapy Diary then slide the tongue backwards over the palate in the
was created, containing a personal data sheet, practical and direction of the uvula, then forward again, repositioning it
explanatory advices for the exercises, schedules for the planning on the papillae.
of the therapy program. Furthermore, the diary was a useful
aid to the speech therapist to monitor the regularity with which Second goal
the exercises were performed at home. Patients who were Increase mouth opening and optimise the elevation of the
prescribed this Protocol at home, had to repeat the exercises tongue; stimulate the coordination of the orbicularis oris and
following the directions of the Therapy Diary. Each exercise had optimise lip competence.
to be repeated 15 times, for 3 sessions a day in front of the Proposed exercises
mirror, since visual feedback reduces variability in performance; 3. Slowly open the mouth, touch the maxillary incisive papillae
in this way, every day the children performed at least 30 minutes with the tip of the tongue, then open the mouth to the
of myofunctional home therapy. maximum.
4. Place the tip of the tongue on the maxillary incisive papillae;
First goal keeping this position, open and close the mouth, without
Establish tongue rest posture and increase oral proprioception pushing the tongue against the teeth.
European Journal of Paediatric Dentistry vol. 20/1-2019 69
SACCOMANNO S. E.T AL
Tongue endurance Lip endurance
70 Tongue endurance Lip endurance
25 22 22
60 60
20
50
40 15
30 9 9
30 24 10
20 5 5 5 5
12 5
6 6 10 7
10
0
0 D.V. D.V. D.T. D.T. D.V. D.V. D.T. D.T.
F.P. F.P. B.B. B.B. F.P. F.P. B.B. B.B. after after after after
after after after after 3 3 3 3
3 3 3 3 weeks weeks weeks weeks
weeks weeks weeks weeks
FIG. 8 IOPI – Measure of endurance in seconds, pre- and post-TMF. FIG. 9 IOPI – Measure of endurance in seconds, Control group.
MIO MIOTTIP TRMR% MIO MIOTTIP TRMR%
54 40
48 35 33,7 33,7 31,6 31,6
25 39 46
44,1 30 27 27
20 34 32,5
25
18 18
15 20
10 19,2 18 21,2 17,6 15
10 8,8 8,8
6,7 6,1 6,1
5 5
0 0
F.P. F.P. B.B. B.B. F.P. F.P. B.B. B.B. F.P. F.P. B.B. B.B. D.V. D.V. D.T. D.T. D.V. D.V. D.T. D.T. D.V. D.V. D.T. D.T.
after after after after after after after after after after after after
3 3 3 3 3 3 3 3 3 3 3 3
weeks weeks weeks weeks weeks weeks weeks weeks weeks weeks weeks weeks
FIG. 10 Restriction of lingual mobility in mm, pre- and post-TMF. FIG. 11 Restriction of lingual mobility in mm, Control group.
Third goal quantitative data emerged from the evaluations are shown in
To tone up the muscles of the tongue and the floor of the Figures 7-11.
mouth, to increase muscle contraction strength and endurance
and to enhance the pharyngeal phase of swallowing.
Proposed exercises Results
5. Protrude the tongue, first making it look wide-shaped, then
making it pointed-shaped. From the analysis of the results, we observe the differences
6. Lift the tip of the tongue just behind the retroincisal papilla. between the 3 groups studied.
Attach the posterior part of the tongue to the palate. In the first group, studied as a control, to which no therapy
Breathe in air between the tongue and the palate to create was prescribed, no results were observed.
a vacuum. Slowly open the mouth. Hold this position for 5 In the second group, which has been prescribed the home
seconds, then detach the tongue from the palate, producing exercises of the proposed Protocol without the supervision of
an explosive sound similar to a "CHUCK" ['tƒ ak]. the speech therapist, no results have been highlighted.
In the third group, treated with the Myofunctional Therapy
Fourth goal with the control of the same speech therapist and with the
To improve tongue and soft palate mobility, strengthening their prescription of the home exercises, positive results were obtained
muscles and in particular the genioglossus and the palatoglossus that confirm the achievement of the 4 goals set.
muscles, to enhance nasal breathing [Paskay, 2016].
Proposed exercises First goal
7. Make circular movements with the tongue on the outer Both treated patients of the third group showed that they
surface of the teeth. acquired the rest position of the tongue by visual assessment,
8. Move the tip of the tongue upwards, as close as possible to and had a better awareness of their oral cavity.
the nose, then downwards towards the chin; then sideways
towards the labial commissures. Second goal
In both patients there was a significant increase in the
After 3 weeks, the same speech therapist re-performed maximum interincisal opening (MIO) and the maximum
the myofunctional assessment, in the same way, to the group interincisal opening with the tip of the tongue in contact with
of cases treated by the therapist and the control group. The the maxillary incisive papillae (MIOTTIP). As a result, an increase
70 European Journal of Paediatric Dentistry vol. 20/1-2019
PAEDIATRIC ORAL PATHOLOGY
A B C D
FIG. 12 Touching the labial commissures with the tip of the tongue. A-B Baseline evaluation. C-D Post-TMF.
A B C D
FIG. 13 Protrusion of the tongue. A-B Baseline evaluation. C-D Post-TMF.
in the TRMR was obtained, that is the ratio between MIO and on the upper lip (Fig. 14) and a better adherence and pressure
MIOTTIP, which determines a change in the restrictions of tongue exerted in the palate suction test.
mobility [Yoon et al., 2017a] (Fig. 10). The other general tests of Although it was not a therapeutic target, qualitative
the Lingual Frenulum Protocol [Marchesan, 2012] which describe improvements were noted for speech and articulation. In
the morphological characteristics of the lingual frenulum were particular, a reduction of articulatory distortions is appreciated,
unchanged, due to the histological structure typical of the above all for phonemes / t /, / d /, / l /, / n /, / s / and for the
lingual frenulum [Martinelli et al., 2014]. The reinforcement of consonant groups. Lip involvement and mandibular lateralisation
lip competence has been objectively detected through the IOPI. during the verbal articulation were reduced, compared to the
In both treated groups there was an increase in the orbicularis early assessment.
oris strength (Fig. 6), measured in kiloPascal [Adams et al., 2013; The sample enrolled for this study had a positive correlation
Clark et al., 2009]. The lip endurance was increased only in one with the predominantly male onset of the short lingual frenulum
of the two cases (Fig. 8). [Huang et al., 2015].
Although the sample was very small, the results obtained
Third goal by applying the Myofunctional Therapy Protocol as proposed
The IOPI documented an objective increase in the tongue were encouraging and many aspects emerged to guide future
strength (Fig. 6), measured in kilopascal. The tongue endurance therapy sessions. No results were found in the functional
was increased only in one of the two cases (Fig. 8). On clinical performance of the patients who performed the home therapy
examination, swallowing was more functional, as there was without the control of the speech therapist, mostly due to the
minimal effort of the orofacial muscles, better mandibular discontinuity in therapy, as the exercises were not performed
stabilisation and the absence of recruitment of the head and daily because the patients experienced difficulties in performing
shoulder muscles. the protocol systematically. The supervision of the speech
therapist is essential in determining the success of the therapy,
Fourth goal within the time allotted for the therapy cycle, as patients need
The breathing function presented qualitative improvements. modeling, correcting, providing instructions and supervising the
According to the breathing protocol (ProPABS) [Susanibar implementation of the home assignments.
and Dacillo, 2015] in the semi-subjective examination of the
respiratory type, an increase in the patency of the nasal cavities Discussion
was visible (Fig. 15), while the markings of the nasal condensation
remained minimally asymmetric and the scores of the functional This pilot study is particularly important if we consider the
breathing evaluation remained unchanged. This result was due paucity of references concerning the application of myofunctional
to the muscular strengthening of the tongue and soft palate, in therapy in patients with altered lingual frenulum. Even in this
particular of the genioglossus and the palatoglossus muscles, small sample, the Myofunctional Therapy Protocol has produced
which had important repercussions on the breathing function, multiple results, improving orofacial and nasal functions.
and on the maintenance of the patency of the upper airways Improvement of the muscle tone and of the contraction strength
[Paskay, 2016]. The functional tests of the Lingual Frenulum of the tongue and the lips and the increase of tongue mobility
Protocol [Marchesan, 2012], showed qualitative improvements obtained have brought about subsequent improvements on the
of tongue mobility, observable in the lateralisation movements stomatognatic functions. This Protocol can be associated with
of the tongue in the direction of the labial commissures (Fig. 12), surgical frenulum release, to ensure the achievement of better
protrusion of the tongue (Fig. 13A-B), elevation of the tongue results and a more rapid and effective functional recovery, in
European Journal of Paediatric Dentistry vol. 20/1-2019 71
SACCOMANNO S. E.T AL
A B C D
FIG. 14 Touch the upper lip with the tip of the tongue. A Baseline FIG. 15 Nasal condensation marking. A Baseline evaluation, B Post-
evaluation, B Post-TMF. TMF.
order to avoid the risk of formation of postoperative scars that References
would limit tongue mobility, requiring surgical revision. The
application of this Myofunctional Therapy Protocol ensures the › Adams V, Mathisen B, Baines S, Lazarus C, Callister R. A Systematic review and meta-analysis of
measurements of tongue and hand strength and endurance using the Iowa Oral Performance Instrument
success of the treatment, as it helps to optimise the suprahyoid
(IOPI). Dysphagia 2013 Sep;28(3):350-69. Epub 2013 Mar 7.
muscles, recover the compromised oral functions and prevent › Bhattad M, Baliga MS, Kriplani R. Clinical Guidelines and management of ankyloglossia with 1-year
the tissues from re-connecting after surgery, causing relapse followup: report of 3 cases. Case Rep Dent 2013;2013:185803. Epub 2013 Jan 29.
[Moeller, 2012]. After the surgical release of the lingual frenulum › Clark HM, O’Brien K, Calleja A, Corrie SN. Effects of directional exercise on lingual strength. Journal of
[Junqueira et al., 2014], it is necessary to respect the times and Speech, Language, and Hearing Research 2009; 52: 1034-1047.
› Grippaudo C, Paolantonio EG, Deli R, La Torre G. Orthodontic treatment need in the Italian child population.
phases of the wound healing process. In the first three post-
Eur J Paediatr Dent 2008 Jun;9(2):71-5.
operative days, during the phases of haemostasis, inflammation › Grippaudo C, Pantanali F, Paolantonio EG, Saulle R, La Torre G, Deli R. Orthodontic treatment timing in
and proliferation, the patient must abstain from myofunctional growing patients. Eur J Paediatr Dent 2013a Sep;14(3):231-6.
therapy exercises. The patient is encouraged to speak, to gently › Grippaudo C, Pantanali F, Paolantonio EG, Grecolini ME, Saulle R, La Torre G, Deli R. Prevalence of
move the tongue and to rinse the wound with saline. After malocclusion in Italian schoolchildren and orthodontic treatment need. Eur J Paediatr Dent 2013b
the third post-operative day, the speech therapist observes the Dec;14(4):314-8.
› Grippaudo C, Paolantonio EG, Pantanali F, Antonini G, Deli R. Early orthodontic treatment: a new index to
patient to determine the state of wound inflammation, ensuring assess the risk of malocclusion in primary dentition. Eur J Paediatr Dent 2014 Dec;15(4):401-6.
that there is no excessive pain, bleeding, heat or drainage from › Guilleminault C, Huseni S, Lo L. A frequent phenotype for paediatric sleep apnoea: short lingual frenulum.
the wound. It is necessary to schedule a follow-up appointment ERJ Open Res 2016 Jul 29;2(3). pii: 00043-2016. eCollection 2016 Jul.
with the speech therapist for the following week, during the › Huang YS, Quo S, Berkowski JA, Guilleminault C. Short lingual frenulum and obstructive sleep apnea in
maturation and remodeling of the wound: during this phase children. Int J Pediatr Res 2015; 1:003.
› Junqueira MA, Cunha N, Costa e Silva LL, Araújo LB, Moretti AB, Couto Filho CE, Sakai VT. Surgical
the Myofunctional Therapy Protocol will be administered for an techniques for the treatment of ankyloglossia in children: a case series. J Appl Oral Sci 2014 Jun;22(3):241-
effective and stable post-surgical treatment over time. 8.
› Marchesan IQ. Lingual Frenulum Protocol. Int J Orofacial Myology 2012 Nov;38:89-103.
Conclusions › Martinelli R, Martinelli G, Berretin-Felix G, Marchesan I. et al. Histological characteristics of altered human
lingual frenulum. Int J Pediatrics Child Health 2014;2: 5-9.
› Moeller JL. Orofacial myofunctional therapy: why not? Cranio 2012 Oct;30(4):235-6.
Myofunctional therapy is an essential support for the
› Paglia L, Scaglioni S, Torchia V, De Cosmi V, Moretti M, Marzo G, Giuca MR. Familial and dietary risk factors
development of the cranio-mandibular-occlusal complex, in Early Childhood Caries. Eur J Paediatr Dent 2016 Jun;17(2):93-9.
as the posture of the tongue, its mobility and its orofacial › Paskay LC. Multitasking properties of some orofacial muscles. IJOM 2016 Nov;42.
functions play a significant role in facial skeletal development › Pompéiaa L, Ilinsky RS, Ortolani C, Faltin K. Ankyloglossia and its influence on growth and development of
[Saccomanno et al., 2014]. In the scientific literature there the stomatognathic system. Rev Paul Pediatr 2017 Apr-Jun;35(2):216-221.
› Saccomanno S, Antonini G, D'Alatri L, D'Angelantonio M, Fiorita A, Deli R. Patients treated with
are very few studies that document myofunctional therapy
orthodontic-myofunctional therapeutic protocol. Eur J Paediat Dent 2012;13 (3): 241-3.
protocols for cases of altered lingual frenulum. The protocol › Saccomanno S, Antonini G, D'Alatri L, D'Angelantonio M, Fiorita A, Deli R. Causal relationship between
presented in this pilot study produces objectively quantifiable malocclusion and oral muscles dysfunction: a model of approach. Eur J Paediat Dent 2012; 13 (4): 321-3.
results, suggesting to be effective in reinforcing the intrinsic and › Saccomanno S, Deli R. Terapia miofunzionale e ortognatodonzia. Milano: Edi-ermes; 2014.
extrinsic tongue muscles, the orbicularis oris, the floor of the › Saccomanno S, Martini C, D’Alatri L, Farina S, Grippaudo C. Validity of a specific myofunctional therapy
protocol in children with Down Syndrome. Eur J Paediatr Dent 2018 Sep;19(3):243-246.
mouth and the soft palate, improving oral proprioception and
› Saccomanno S, Paskay LC, New trends in myo functional therapy - occlusion, muscles and posture. Edi-
qualitatively enhancing oral functions in cases of altered lingual Ermes; 2019 in press.
frenulum. It is proposed to apply the Myofunctional Therapy › Ito Y, Shimizu T, Nakamura T, Takatama C. Effectiveness of tongue-tie division for speech disorder in
Protocol to a larger study sample to standardise it and make children. Pediatr Int 2015 Apr;57(2):222-6.
it usable for functional improvement of borderline cases, pre- › Srinivasan B, Chitharanjan AB. Skeletal and dental characteristics in subjects with ankyloglossia. Prog
Orthod 2013 Nov 7;14:44.
surgery preparation and for rehabilitation post frenectomy-
› Susanibar F, Dacillo C. Protocollo di valutazione logopedica della respirazione con punteggi. ProVaLoRe.
frenotomy. In case of alteration of the lingual frenulum, the early Ediz. Multilingue. LCF Edizioni; 2015.
diagnosis, the multidisciplinary management and the adoption › Suzart DD, de Carvalho AR. Speech disorders related to alterations of the lingual frenulum in schoolchildren.
of a systematic Myofunctional Therapy Protocol are the key Rev CEFAC São Paulo 2016 Nov-Dec;18(6).
to success for an effective and decisive procedure, in order to › Vaz AC, Bai PM. Lingual frenulum and malocclusion: An overlooked tissue or a minor issue. Indian J Dent
Res 2015;26:488-92.
prevent the occurrence of structural and functional alterations
› Yoon A, Zaghi S, Weitzman R, Ha S, Law CS, Guilleminault C, Liu SYC. Toward a functional definition of
and guarantee an improvement in the quality of life of these ankyloglossia: validating current grading scales for lingual frenulum length and tongue mobility in 1052
patients. subjects. Sleep Breath 2017a Sep;21(3):767-775.
› Yoon AJ, Ha S, Law CS, Guilleminault C, Liu SY. Ankyloglossia as a risk factor for maxillary hypoplasia and
Acknowledgments soft palate elongation: A functional – morphological study. Orthod Craniofac Res 2017b Nov;20(4):237-
244.
We would like to thank Licia Coceani Paskay, MS, CCC-SLP,
Los Angeles, CA, USA, for her expert advice and contribution.
72 European Journal of Paediatric Dentistry vol. 20/1-2019
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Toe To Head Boston-2Document61 pagesToe To Head Boston-2Máté Boa100% (1)
- PasTest MCQs With Answers PDFDocument317 pagesPasTest MCQs With Answers PDFHayan Falhout67% (3)
- ArticulationDocument9 pagesArticulationMohan KalawateNo ratings yet
- MR Bean Dentist Present SimpleDocument1 pageMR Bean Dentist Present SimpleRosanna BellaubiNo ratings yet
- Feeding and Esating in Early Intervention. A Trust Based ApproachDocument24 pagesFeeding and Esating in Early Intervention. A Trust Based ApproachAndrea Díaz Rodríguez100% (1)
- Dentsply Sirona Universal Stains Glaze Dfu PDFDocument12 pagesDentsply Sirona Universal Stains Glaze Dfu PDFslim wali0% (1)
- EAT UP Family Centered Feeding InterventDocument15 pagesEAT UP Family Centered Feeding InterventAndrea Díaz RodríguezNo ratings yet
- The Embodied Mind Cognitive Science and Human ExpeDocument5 pagesThe Embodied Mind Cognitive Science and Human ExpeAndrea Díaz RodríguezNo ratings yet
- HOME PROGRAM - Stuttering Modification Strategy/Fluency-Enhancing Technique Definition/Practice TasksDocument26 pagesHOME PROGRAM - Stuttering Modification Strategy/Fluency-Enhancing Technique Definition/Practice TasksAndrea Díaz RodríguezNo ratings yet
- Building Mealtime Environments and RelationshipsDocument28 pagesBuilding Mealtime Environments and RelationshipsAndrea Díaz RodríguezNo ratings yet
- Kumari (2019) Prediction of Nutritive Sucking in PretermDocument7 pagesKumari (2019) Prediction of Nutritive Sucking in PretermAndrea Díaz RodríguezNo ratings yet
- Speechkids Oral Motor / Feeding Questionnaire: BreakfastDocument4 pagesSpeechkids Oral Motor / Feeding Questionnaire: BreakfastAndrea Díaz RodríguezNo ratings yet
- Pacifier UseDocument7 pagesPacifier UseAndrea Díaz RodríguezNo ratings yet
- Impact of Breast Milk On Intelligence Quotient, Brain Size, andDocument6 pagesImpact of Breast Milk On Intelligence Quotient, Brain Size, andAndrea Díaz RodríguezNo ratings yet
- Pang2020 Article NutrientsOrNursingUnderstandinDocument11 pagesPang2020 Article NutrientsOrNursingUnderstandinAndrea Díaz RodríguezNo ratings yet
- Bmjopen 2018 026449Document13 pagesBmjopen 2018 026449Andrea Díaz RodríguezNo ratings yet
- Pacifiers Thumb Sucking Breastfeeding andDocument9 pagesPacifiers Thumb Sucking Breastfeeding andLaura Ortiz BermudezNo ratings yet
- An Investigation of The Flow Rates of Disposable Bottle Teats Used To Feed Preterm and Medically Fragile Infants in Neon 2019Document28 pagesAn Investigation of The Flow Rates of Disposable Bottle Teats Used To Feed Preterm and Medically Fragile Infants in Neon 2019Andrea Díaz RodríguezNo ratings yet
- Determinants of Milk Flow Through Nipple UnitsDocument3 pagesDeterminants of Milk Flow Through Nipple UnitsAndrea Díaz RodríguezNo ratings yet
- Myofungtional Chuang 2016Document6 pagesMyofungtional Chuang 2016Priska AngeliaNo ratings yet
- 1AR. Evidence of Orofacial Myofunctional Therapy Asma y RinitisDocument6 pages1AR. Evidence of Orofacial Myofunctional Therapy Asma y RinitisAndrea Díaz RodríguezNo ratings yet
- Articulo 1 PDFDocument9 pagesArticulo 1 PDFPayito AltamiranoNo ratings yet
- Revision Sistemica Uso de Copa Versus Otros Metodos de SuplementacionDocument43 pagesRevision Sistemica Uso de Copa Versus Otros Metodos de SuplementacionAndrea Díaz RodríguezNo ratings yet
- Counselling On BFDocument7 pagesCounselling On BFAndrea Díaz RodríguezNo ratings yet
- Bmjopen 2017 016739Document5 pagesBmjopen 2017 016739ayuNo ratings yet
- Zimmerman 2015Document5 pagesZimmerman 2015Muhammad SidiqNo ratings yet
- Determinants of Milk Flow Through Nipple UnitsDocument3 pagesDeterminants of Milk Flow Through Nipple UnitsAndrea Díaz RodríguezNo ratings yet
- Appendix - C Nipple Flow RatesDocument1 pageAppendix - C Nipple Flow RatesAndrea Díaz RodríguezNo ratings yet
- Counselling On BFDocument7 pagesCounselling On BFAndrea Díaz RodríguezNo ratings yet
- dgb10.1136 - Bmjopen 2017 018621 PDFDocument6 pagesdgb10.1136 - Bmjopen 2017 018621 PDFAndrea Díaz RodríguezNo ratings yet
- An Investigation of The Flow Rates of Disposable Bottle Teats Used To Feed Preterm and Medically Fragile Infants in Neon 2019Document28 pagesAn Investigation of The Flow Rates of Disposable Bottle Teats Used To Feed Preterm and Medically Fragile Infants in Neon 2019Andrea Díaz RodríguezNo ratings yet
- Lingual Frenulum Protocol With Scores For Infants IJOM 2012Document10 pagesLingual Frenulum Protocol With Scores For Infants IJOM 2012Omar DSNo ratings yet
- dgb10.1136 - Bmjopen 2017 018621 PDFDocument6 pagesdgb10.1136 - Bmjopen 2017 018621 PDFAndrea Díaz RodríguezNo ratings yet
- Lactation Suppression: Forgotten Aspect of Care For The Mother of A Dying ChildDocument5 pagesLactation Suppression: Forgotten Aspect of Care For The Mother of A Dying ChildAndrea Díaz RodríguezNo ratings yet
- Karishma AzizDocument6 pagesKarishma AzizHafsa MalikNo ratings yet
- SD RPD DiscussionDocument4 pagesSD RPD DiscussionRona TabingNo ratings yet
- MLV136 REV C Locator PresentationDocument58 pagesMLV136 REV C Locator PresentationS. BenzaquenNo ratings yet
- Bone ReactionDocument9 pagesBone ReactionFourthMolar.comNo ratings yet
- Sentence Stalking GuideDocument14 pagesSentence Stalking GuideSamarth AroraNo ratings yet
- Mclaurin 2020Document9 pagesMclaurin 2020magus davilaNo ratings yet
- Gingival RetractionDocument106 pagesGingival RetractionManishaNo ratings yet
- Incidence of Dry Socket After Third Molar ExtractionDocument2 pagesIncidence of Dry Socket After Third Molar ExtractionI Gusti Ayu WulanNo ratings yet
- Cranial Base Angle in Relation To MalocclusionDocument50 pagesCranial Base Angle in Relation To Malocclusionheycoolalex100% (1)
- Homeopathic RemediesDocument15 pagesHomeopathic Remediessaeedchaand100% (1)
- The Permanent Mandibular IncisorsDocument23 pagesThe Permanent Mandibular IncisorsDina YasserNo ratings yet
- Kya Apke Toothpaste Mein Namak Zaroori Hai?Document5 pagesKya Apke Toothpaste Mein Namak Zaroori Hai?Md Faisal Alam XI-CNo ratings yet
- Lecture 5 Laser in Operative DentistryDocument7 pagesLecture 5 Laser in Operative DentistryDt omarNo ratings yet
- Prosthesis 03 00032 v2Document9 pagesProsthesis 03 00032 v2Carmen FierascuNo ratings yet
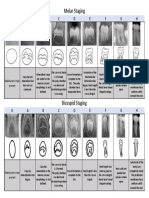
- Demirjian Staging Molar Bicuspid FinalDocument1 pageDemirjian Staging Molar Bicuspid FinalfernandoNo ratings yet
- PaedsDocument17 pagesPaedsmierahNo ratings yet
- Introduction To Dentistry 1 Year Lect. 1Document44 pagesIntroduction To Dentistry 1 Year Lect. 1abdulrazaqNo ratings yet
- Lecture 8, Pulpal Considerations (Liners & Bases)Document10 pagesLecture 8, Pulpal Considerations (Liners & Bases)JustDen09No ratings yet
- Textbook&Jurnal IPMDocument39 pagesTextbook&Jurnal IPMyesicadeaNo ratings yet
- The Role of Intercondylar Distance in The Posterior Teeth ArrangementDocument5 pagesThe Role of Intercondylar Distance in The Posterior Teeth ArrangementBharath KondaveetiNo ratings yet
- Role of PeriodontistDocument5 pagesRole of PeriodontistNeetha ShenoyNo ratings yet
- Requirement and Responsibility MFPDocument4 pagesRequirement and Responsibility MFPAlexandru Codrin-IonutNo ratings yet
- Hospital ListDocument3 pagesHospital ListShoaib MalikNo ratings yet
- Efectos AdversosDocument10 pagesEfectos Adversosjeimmy dulceyNo ratings yet
- Modern Endodontic Principes IrrigationDocument10 pagesModern Endodontic Principes IrrigationDulgheru StefanNo ratings yet