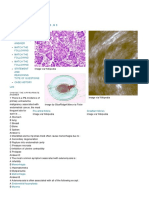
Professional Documents
Culture Documents
Wound Healing Problems in The Mouth: Frontiers in Physiology November 2016
Uploaded by
rozh rasulOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Wound Healing Problems in The Mouth: Frontiers in Physiology November 2016
Uploaded by
rozh rasulCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/309610101
Wound Healing Problems in the Mouth
Article in Frontiers in Physiology · November 2016
DOI: 10.3389/fphys.2016.00507
CITATIONS READS
47 3,373
4 authors, including:
Constantinus Politis Reinhilde Jacobs
Universitair Ziekenhuis Leuven KU Leuven
453 PUBLICATIONS 2,751 CITATIONS 622 PUBLICATIONS 17,785 CITATIONS
SEE PROFILE SEE PROFILE
Jimoh Olubanwo Agbaje
KU Leuven
76 PUBLICATIONS 689 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
Comparison between MRI and arthroscopy of the TMJ View project
Osteodent - assessment of bone loss using panoramic dental radiographs View project
All content following this page was uploaded by Jimoh Olubanwo Agbaje on 02 November 2016.
The user has requested enhancement of the downloaded file.
REVIEW
published: 02 November 2016
doi: 10.3389/fphys.2016.00507
Wound Healing Problems in the
Mouth
Constantinus Politis 1, 2*, Joseph Schoenaers 2 , Reinhilde Jacobs 1 and Jimoh O. Agbaje 1, 2
1
OMFS-IMPATH Research Group, Department of Imaging and Pathology, Katholieke Universiteit Leuven, Leuven, Belgium,
2
Oral and Maxillofacial Surgery, Leuven University Hospitals, Leuven, Belgium
Wound healing is a primary survival mechanism that is largely taken for granted. The
literature includes relatively little information about disturbed wound healing, and there is
no acceptable classification describing wound healing process in the oral region. Wound
healing comprises a sequence of complex biological processes. All tissues follow an
essentially identical pattern to complete the healing process with minimal scar formation.
The oral cavity is a remarkable environment in which wound healing occurs in warm oral
fluid containing millions of microorganisms. The present review provides a basic overview
of the wound healing process and with a discussion of the local and general factors that
play roles in achieving efficient would healing. Results of oral cavity wound healing can
vary from a clinically healed wound without scar formation and with histologically normal
Edited by:
connective tissue under epithelial cells to extreme forms of trismus caused by fibrosis.
Gianpaolo Papaccio, Many local and general factors affect oral wound healing, and an improved understanding
Seconda Università degli Studi di of these factors will help to address issues that lead to poor oral wound healing.
Napoli, Italy
Reviewed by: Keywords: oral, wound healing, dental implant, nerve damage, local and general factors, inflammation, granulation
Keiji Moriyama, tissue
Tokyo Medical and Dental University,
Japan
Marianna Bei, INTRODUCTION
Harvard Medical School, USA
*Correspondence:
In Greek mythology, the Rod of Asclepius is a serpent-entwined rod wielded by the Greek god
Constantinus Politis Asclepius. Wounded patients could be healed if they were brought to the temple and the serpent
constantinus.politis@uzleuven.be licked their wounds during the night (Gardner, 1925). The Rod of Asclepius is still used as a symbol
associated with modern medicine and health care. Wound healing is a primary survival mechanism
Specialty section: that is largely taken for granted. Although, wound healing has long been considered a primary
This article was submitted to aspect of medical practice, disturbed wound healing is infrequently discussed in the literature, and
Craniofacial Biology and Dental there is no acceptable classification to describe wound healing processes in the oral region.
Research, Wound healing entails a sequence of complex biological processes (Bielefeld et al., 2013). All
a section of the journal
tissues follow an essentially identical pattern to promote healing with minimal scar formation. One
Frontiers in Physiology
fundamental difference between would healing and regeneration is that all tissues are capable of
Received: 29 August 2016 renewal, but healed tissue does not always possess the same functionality or morphology as the
Accepted: 14 October 2016
lost tissue (Takeo et al., 2015). Moreover, wound healing is a protective function of the body that
Published: 02 November 2016
focuses on quick recovery (Wong et al., 2013), whereas the process of regeneration in an hostile
Citation:
environment takes more time. In particular, the oral cavity is a remarkable environment in which
Politis C, Schoenaers J, Jacobs R and
Agbaje JO (2016) Wound Healing
wound healing occurs in warm oral fluid that contains millions of microorganisms.
Problems in the Mouth. The present review provides a basic overview of wound healing, focusing on specific
Front. Physiol. 7:507. characteristics of the process of wound healing in the oral cavity. We also discuss local and general
doi: 10.3389/fphys.2016.00507 factors that play roles in achieving efficient wound healing.
Frontiers in Physiology | www.frontiersin.org 1 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
NORMAL WOUND HEALING PROCESS 1992; Mutschler, 2012). Macrophages also play major roles in
initiating collagen synthesis, and in the formation of endothelial
Wound healing requires multiple finely tuned processes that cells and fibroblasts. Overall, macrophages act as the engine
occur in a specific sequence (Bielefeld et al., 2013; Eming of the wound healing process (Cohen et al., 1992; Mutschler,
et al., 2014). Intact hemostatic and inflammatory mechanisms 2012). Granulocytes and macrophages both exhibit an anaerobic
are needed, and mesenchymal cells must migrate to the metabolism, produce collagenase, feed on bacterial debris, and
wounded area and proliferate at site of injury. To maintain produce lactate, which decreases the tissue pH (Cohen et al.,
organization and give rise to newly formed tissue, angiogenesis 1992; Velnar et al., 2009). Like hemostasis, this process also must
and epithelialization occur, together with collagen synthesis, be regulated. Acceleration, amplification, and downregulation
binding, and alignment which causing open wounds to contract are important mechanisms in the normal wound healing
(Bielefeld et al., 2013; Eming et al., 2014; Takeo et al., 2015). process. Prostaglandins and leukotrienes are pro-inflammatory
Further wound healing involves regeneration (the substitution mediators, while inflammatory reactions are suppressed by
of damaged tissues with the same cell type) and fibrosis substances such as lipoxins, resolvins, and protectins (Cohen
(replacement of damaged tissues with connective tissue). These et al., 1992; Gharaee-Kermani and Phan, 2001; Velnar et al., 2009;
processes involve three types of cells. First, epithelial cells are Ozturk and Ermertcan, 2011).
required, which can continuously regenerate. For the secondary This inflammatory phase is followed by granulation tissue
stage of organization, there is also a need for cells that replicate on formation, re-epithelialization, and formation of a connective
a lower level but that can replicate at a high rate in the presence tissue matrix (Broughton et al., 2006; Rodriguez-Merchan,
of a stimuli to recover the original tissue—for example, fibroblasts 2012). Granulation tissue comprises a dense population of
and vascular endothelial cells. Finally, cells that lack the ability to macrophages, fibroblasts, capillary networks, fibronectin,
divide are required, such as cells of the peripheral nerve system hyaluronic acid and endothelial cells (Rodriguez-Merchan, 2012;
and odontoblasts (Mahdavian et al., 2011; Reinke and Sorg, 2012; Discepoli et al., 2013). Macrophages, fibroblasts, and endothelial
Bielefeld et al., 2013; Wong et al., 2013). cells are interdependent during granulation tissue formation
(Rodriguez-Merchan, 2012; Discepoli et al., 2013). Hypoxia is
WOUND HEALING PROCESS SEQUENCE an important trigger for neovascularization during this phase
(Schreml et al., 2010; Larjava, 2012). Fluid continues to leak
Wound healing is initiated by the formation of a blood from the wound until basal membrane formation (Kirsner and
clot that closes the wound. Vasoconstriction occurs to stop Eaglstein, 1993; Broughton et al., 2006). At this time, fibroblasts
the bleeding, followed by platelet activation (Cooper, 1999; are recruited from the wound edges, and circulating fibrocytes
Broughton et al., 2006). Platelets play several important roles and mesenchymal progenitor cells migrate to the immature
within a wound, including regulating primary hemostasis during connective tissue matrix (Kirsner and Eaglstein, 1993; Cooper,
the aggregation phase and secondary hemostasis during the 1999; Broughton et al., 2006).
coagulation phase. Platelets produce biologically active products, Re-epithelialization starts from the wound edge, where
including vasoactive mediators and chemotactic factors, such epithelial cells lose their hemi-desmosomal connections and
as proteases, cytokines, and growth factors (Broughton et al., migrate through the provisional fibrin–fibronectin matrix
2006; Cooper, 1999). Cytokines send out chemotactic signals through the wound until they encounter identical cells (Kirsner
to inflammatory cells and local cell populations. The fibrin– and Eaglstein, 1993; Cooper, 1999; Broughton et al., 2006; Li
fibronectin clot formed during secondary hemostasis serves as et al., 2007). Targeted migration and proliferation through a
a temporary matrix to allow epithelial cells and fibroblasts to loose underlying network requires an efficient, balanced, and
migrate into the wound. Upon clot formation, thrombin is enzymatically supported procedure of “cutting and pasting”
activated to prevent excessive blood clotting (Cooper, 1999; (Hunt et al., 2000; Broughton et al., 2006; Li et al., 2007;
Diegelmann and Evans, 2004; Broughton et al., 2006). During Ozturk and Ermertcan, 2011). The process through which the
the tertiary hemostatic phase, fibrinolytic system activation leads epithelial cells of two wound edges make direct contact is called
to fibrin degradation. The peptides released during this process healing by primary intention (Cohen et al., 1992; Vanwijck, 2001;
provoke chemotaxis and increase capillary permeability (Cooper, Broughton et al., 2006). On the other hand, healing by secondary
1999; Diegelmann and Evans, 2004; Broughton et al., 2006). intention occurs when migrating cells make a connection after
Cytokines initiate an inflammatory reaction that serves to a certain time, through granulation tissue or not (Cohen et al.,
remove debris, damaged or necrotic tissues, and microorganisms 1992; Vanwijck, 2001; Broughton et al., 2006). The healing
(Gharaee-Kermani and Phan, 2001; Li et al., 2007). Blood process is slower in open wounds due to delayed epithelial
vessels situated near the wound show dilatation, increased closure and a higher rate of granulation tissue formation (Cohen
capillary permeability with plasma exudation, and decreased et al., 1992; Vanwijck, 2001; Sorensen, 2012; Glim et al., 2013;
blood flow (Cohen et al., 1992; Li et al., 2007). Leucocytes Karamanos et al., 2015). The fibronectin connective tissue
are attracted to the center of the wound, which quickly form is initially loose, with gradual replacement by bigger and
becomes saturated with granulocytes and macrophages. In the stronger collagen bundles. This protects wound against damage
early stage, primary neutrophilic granulocytes are involved from traction and pressure. Extracellular matrix formation is
in protecting against bacterial invasion, while macrophages initiated at the wound edge, and gradually progresses to the
become the dominant cells after a few days (Cohen et al., center/core of the wound. This process is similar to the matrix
Frontiers in Physiology | www.frontiersin.org 2 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
maturation, as both are initiated at the edge and gradually Periodontal Healing
continue toward the wound center. During this maturation Healing after a tooth extraction follows the same pattern, with
process, new blood vessel formation decreases (Cohen et al., 1992; the inclusion of a bone healing process (Larjava, 2012; Discepoli
Broughton et al., 2006; Velnar et al., 2009; Ozturk and Ermertcan, et al., 2013). Minutes after the tooth is extracted, the alveoli
2011). are closed via blood clotting. Re-epithelialization starts 24 h
The final stage of the wound healing process is called the post-extraction. After 1 week, the blood clot is replaced with
contraction phase, which begins following sufficient collagen granulation tissue. After 8 weeks, the extraction cavity is filled
formation in the granular tissue. In the contraction phase, the with bone (Larjava, 2012; Discepoli et al., 2013). The bone
distance between wound edges is closed, reducing the wound remodeling process continues for 6 months after the extraction,
surface, and fastening the wound closure. This last process and is accompanied by a loss of alveolar width and length
occurs due to differentiation of fibroblasts and other progenitor due to resorption and remodeling (Discepoli et al., 2013). The
cells into myofibroblasts. Myofibroblasts with an actin-enriched amount of bone loss varies among individuals, and depends
cytoskeleton provide matrix constriction. Wound contraction on the location, the presence of adjacent teeth, the treatment
is followed by the remodeling process, in which matrix protocol, smoking behavior, and the use of membranes and
production stops, fibroblasts are degraded, and myofibroblasts bone substitutes (Trombelli et al., 2008). A review of the
enter apoptosis (Cohen et al., 1992; Broughton et al., 2006; Velnar effects of plasma concentrates showed reduced post-surgical pain
et al., 2009; Ozturk and Ermertcan, 2011). The final result of and burden, but no improvement or increase of hard tissue
wound healing can range from a clinically healed wound with no regeneration (Moraschini and Barboza, 2015).
scar formation and with histologically normal connective tissue Wound healing after periodontal surgery carries a notable risk
under epithelial cells to extreme forms of trismus caused by of degradation of the interdental papilla, with the occurrence
fibrosis. of black triangles. Specific incisions and flaps are important to
ensure minimum retraction, and good oral hygiene is critical to
avoid inflammation (Larjava, 2012; Discepoli et al., 2013; Glim
Timing of Wound Healing Phases et al., 2013; Lindhe et al., 2015).
Within the wound healing process, the inflammatory phase
involves homeostasis and inflammation, which start at the Healing at Dental Implant Interfaces
moment of injury and continue for up to 4 to 6 days. A specific form of wound healing occurs around dental implants.
The proliferation phase involves epithelialization, angiogenesis, In biphasic dental implant procedures, the implant is placed
granulation tissue formation, and collagen deposition, and takes directly under or at the same level as the bone surface. The cover
place from day 4 to day 14 after injury. Epithelial cell migration screw is overlaid with soft tissues that heal without substantial
starts after 24 h. The maturation and remodeling phase starts granulation tissue formation. Healing in the bone occurs between
from day 8 after injury and proceeds for about a year (Kirsner the edge surface of the implant and the prepared osteotomy edge
and Eaglstein, 1993; Ennis and Meneses, 2000; Hunt et al., 2000; (Larjava, 2012; Lindhe et al., 2015). Blood clots form mainly at
Broughton et al., 2006; Larjava, 2012). the inner side of the implant grooves, and are then infiltrated
by granulocytes and macrophages. Fibroblastic progenitor cells
migrate into the provisional matrix, enabling formation of
SPECIFIC CHARACTERISTICS OF THE granulation tissue, which is then vascularized by endothelial
ORAL CAVITY WOUND HEALING cell migration. Finally, the cells in the granulation tissue
PROCESS differentiate into osteoblasts, creating bone. This bone formation
starts 4 days after placement of dental implants, achieving
Healing of the Palate maximum bone–implant contact after 3 months (Larjava, 2012).
Wound healing in the oral cavity is typically characterized by Depending on the mechanical stress caused by occlusal forces,
healing of the palate and gingival tissue in the presence of bone remodeling around the dental implant persists for at least
healthy underlying bones and without scar tissue formation 1 year.
(Glim et al., 2013). This is due to early onset of the inflammatory
phase, decreased levels of immunity mediators, fewer blood Dental Pulp Healing
vessels, more cells originating from the bone marrow, rapid re- Dental pulp healing mainly relies on preservation of the
epithelialization, and rapid fibroblast proliferation (Funato et al., apical blood supply and survival of the damaged odontoblast
1999; Glim et al., 2013). In fetal wound healing, the inflammatory layer (Goldberg, 2011; Dimitrova-Nakov et al., 2014). If the
phase is absent (Larson et al., 2010). odontoblast layer is sufficiently intact, the odontoblasts and
Wound healing in the palate is more difficult in the absence of Hoehl’s cells can influence the formation of tubular or atubular
healthy underlying bone. In such cases, wound healing might be reactionary (tertiary) dentin (Goldberg, 2011; Dimitrova-Nakov
accompanied by perforation to the nose and antrum or by serious et al., 2014). Additionally, an opening of the pulp that causes only
scarring. This can lead to narrowing of the transversal width of superficial dental pulp necrosis can provoke an inflammatory
the maxilla if the patient is in their growing phase, as is observed reaction that attracts pulpal stem cells or progenitor cells to
in cleft patients who have surgery of the palate (Broughton et al., the wound edge, where they differentiate into odontoblast-like
2006; Larjava, 2012). cells that produce reparative dentin or osteodentin. However,
Frontiers in Physiology | www.frontiersin.org 3 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
persistent inflammation in the dental pulp can lead to pulp The indirect bone healing sequence can be summarized as
necrosis (Goldberg, 2011). follows: (1) inflammation and hematoma formation, (2) fragment
stabilization by periosteal and endosteal callus formation, (3)
Bone Healing continuity restoration by membranous and endochondral bone
Jawbone fractures can heal by primary or secondary intention. formation, and (4) formation of osteons and Haversian canals,
Bone healing by primary intention (also termed direct bone and functional adaptation (Junqueira and Carneiro, 2007).
healing) occurs without callus formation, given the presence After blood clot formation, osteocytes die on both sides of
of a good blood supply and an existing stable fixation without the fracture and the bone matrix degrades. This is followed
mobility of the bone fragments—which must be in direct contact by the recovery phase in which dead cells, the thrombus,
with each other with a fracture gap of up to 1 mm (Adell et al., and the degraded bone matrix are cleaned up (Adell et al.,
1987; Discepoli et al., 2013). Under these conditions, osteoblasts 1987; Broughton et al., 2006; Discepoli et al., 2013). The
are activated within 1 to 3 days, and osteoid is established within surrounding tissue prompts revascularization and angiogenesis,
a week. Bridging the gap with primary bone can take 4 to 6 weeks together with strong cell proliferation. The nature of the
depending on the gap distance. This primary bone contains large formed tissue is associated with the fracture stability and
numbers of osteocytes and collagen fibers intertwined (woven the tissue vascularization. In cases of less stable fracture or
bone) to create a spatial braid or plexus (Adell et al., 1987; poor vascularization, a cartilaginous callus forms first, which
Broughton et al., 2006). This bone is subsequently replaced by is then converted to endochondral bone, followed by further
mature secondary bone that is characterized by a parallel collagen transformation into woven bone, and finally by conversion
fiber arrangement. The concentric lamellae (lamellar bone) are to secondary (lamellar) bone as the stabilization improves.
better calcified, making secondary bone stronger than primary When bone fragments show high mobility or a large gap,
bone (Hom et al., 2009). and in cases of periosteum damage, a connective tissue-like
Bone healing by secondary intention (also termed indirect callus is formed that clinically appears as a pseudarthrosis in
bone healing) is characterized by callus formation, and is by which the bone fragments opposite each other remain mobile
far the most important form of bone healing in maxillo- (Broughton et al., 2006; Guo and Dipietro, 2010; Discepoli et al.,
facial surgery (Adell et al., 1987; Broughton et al., 2006). 2013).
FIGURE 1 | (A) Granuloma formation after reconstruction surgery through a bone from the anterior iliac crest in region 12. (B) Panoramic radiography indicates a
vertical bone deficit in region 12. (C) Exploration of a wound from which the residue of a non-healed bone graft was removed. A large part of the originally implanted
bone graft has already disappeared due to necrosis and/or resorption. (D) The necrotic bone graft with an osteosynthesis screw.
Frontiers in Physiology | www.frontiersin.org 4 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
Healing of Facial Burns as well as preprosthetic reconstructive surgery (Hollander and
Burns on the face or in the mouth often exhibit compromised Singer, 1999; Guo and Dipietro, 2010; Dunda et al., 2015;
wound healing with pronounced scarring (Guo and Dipietro, Karamanos et al., 2015). Substantial morbidity in mouth, head,
2010; Glim et al., 2013). The extent of thermal damage depends and neck surgery is influenced by many factors, including
on the temperature, contact time, skin or mucosa thickness, and existing scars, large defect size, non-vascularized autologous bone
degree of vascularization within the injured area. Due to vascular grafts or free bone grafts, poor oral hygiene, difficult wound
and inflammatory reactions, burns continue to damage deeper closure, and pre-existing or postoperative infections (Guo and
structures for 48–72 h following the initial insult (Larjava, 2012). Dipietro, 2010; Dunda et al., 2015; Karamanos et al., 2015).
Healing of Large Defects
Wound healing problems are also commonly associated with CLINICAL MANIFESTATIONS OF
reconstructive surgery of congenital defects, trauma, or tumors, DISTURBED WOUND HEALING IN THE
MOUTH
Disturbed wound healing has many manifestations, with the
potential for wound healing disturbance at every phase.
Clinical manifestations can include excessive bleeding or
absence of blood clot formation as seen in alveolitis sicca.
Other manifestations can include the granuloma formation
(Figures 1A–D), sinus polyps (Figures 2A–C), fistulas, wound
dehiscence, ulcers, perforations, wound necrosis, flap necrosis
(Figure 3), pus formation, chronic infections with or without
granulation tissue formation (Figure 4), keloid formation
(Figures 5A,B), fibrosis, and trismus (Adell et al., 1987; Guo
and Dipietro, 2010; Glim et al., 2013; Roy et al., 2013;
Karamanos et al., 2015). Hom et al. (2009) states that the
following clinical signs indicate poor wound healing: persistent
inflammation for longer than 7 days, malodorous wound,
increased exudate, delayed epithelization, maceration of the
surrounding skin, wound dehiscence, and necrotic tissue. A
traumatic eosinophil granuloma of the tongue can also be
considered a manifestation of poor healing progress. Pro-
inflammatory mediators continue to dominate during chronic
infections (Hunt et al., 2000).
FIGURE 2 | (A) A sinus polyp is a manifestation of a poorly healing antrum
perforation that does not spontaneously close. This can lead to the bony Cases of nerve damage in the trigeminus area exhibit a special
height of the rest alveolus being too small following tooth extraction, and the form of tissue damage due to disturbed wound healing. Damage
connection between the mouth and antrum being too wide. (B) Panoramic to the branches of the nervus trigeminus due to nerve crushing
radiography shows loss of bone height separating the antrum of the oral cavity or pressure can cause dysfunction in the form of neuropathic
in region 26. (C) Brightening of the wound edges reveals the dimension of the
connection between the antrum and oral cavity.
pain with or without hypoesthesia of the innervation area (Politis
et al., 2014). Although, the mechanisms have not yet been
FIGURE 3 | (A) Progressive necrosis of a double free flap (fibula + anterolateral femur flap) due to a combination of factors, leading to complete ischemia and death of
the free flap. (B) The necrotic flap was removed and temporally replaced with a wick.
Frontiers in Physiology | www.frontiersin.org 5 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
TABLE 1 | Local and general factors that contribute to disturbed wound
healing.
Local factors General factors
– Wound size – Hereditary defects of wound healing
– Wound localization – Nutritional deficiency
– Postoperative bleeding – HIV
– Thermal damage – Cancer
– Perforation to the sinus maxillary – Old age
– Sharp bone edges – Diabetes
– Local anesthesia – Jaundice
– Infection – Alcoholism
– Hypo-perfusion – Uremia
– Ischemia – Immunosuppressives
– Foreign body – Corticosteroids
– Smoking – Chemotherapeutics
FIGURE 4 | A poorly healing wound after extraction of 48. Eight weeks – Venous insufficiency – Antiresorptive medication
after extraction, the patient continued to complain of pain, and granulation
– Mechanical trauma – Other medication
tissue was found in the wound. Wound exploration revealed a pathological
fracture together with necrotic bone tissue and bone sequesters. – Local toxins – Vitamin A
– Head or neck irradiation – Hypothyroidism
– Cancer of the mouth – Hyperbaric oxygen
– Presence of necrotic tissue – Anemia
– Local stem cell injections
– Underlying pathological fractures
– Injudicious flap design in surgeries
– Edema
– Pathological mobility
– Tooth in the line of a jaw fracture
– Traumatic occlusion
FIGURE 5 | An 11-year-old boy presented with keloid formation on the
upper lip (A) and the thorax (B) after a traffic accident with bicycle.
Hypertrophic scarring and keloid formation indicate abnormal wound healing. bleeding tendencies only give rise to disturbed wound healing in
the presence of pathological bleeding (Rodriguez-Merchan, 2012;
Figures 6A,B).
elucidated, it is hypothesized that this effect occurs when the
nerve and its surrounding environment (vasa nervosum, bone, Hypoxia and Oxygen Tension
and adipose tissue) do not sufficiently recover during wound Wounds must have a minimum oxygen tension of 30 mmHg
healing. for normal cell division, and a minimum of 15 mmHg
A typical form of disturbed wound healing involves the for fibroblast proliferation (Schreml et al., 2010). Bacterial
root resorption of an element following tooth trauma, tooth destruction by phagocytosis relies on a high partial oxygen
transplantation, or reimplantation of an element. Severe damage pressure in the tissues. Sufficient oxygenation is also required
to the periodontal ligament and cementum transcends the for cell proliferation, angiogenesis, collagen synthesis and re-
healing capacity, giving rise to tooth ankyloses and replacement epithelization. The role of oxygen has mainly been investigated
resorption (Goldberg, 2011; Dimitrova-Nakov et al., 2014). through in vitro or animal experiments, and there is not yet
sufficient in vivo data from humans to truly understand the role
of oxygen in wound healing (Yip, 2015). However, it is clear that
LOCAL FACTORS INFLUENCING WOUND hypoxia is associated with disturbed wound healing and with
HEALING IN THE MOUTH bacterial colonization in chronic wounds (Schreml et al., 2010).
It is clinically useful to be aware of the local and general factors Ischemia
that are associated with disturbances of normal wound healing Following dental trauma (avulsion, extrusive luxation, or lateral
processes (Table 1). luxation) or tooth transplantation, a special form of local
ischemia can arise in which neovascularization occurs through
Postoperative Bleeding an open apex, and is followed by osteodentin deposition with
Postoperative bleeding disturbs granulation tissue formation and a small central pulpal channel that contains a blood supply—
slow the healing process (Larjava, 2012). Hereditary and acquired termed root canal obliteration. This predominantly occurs in
Frontiers in Physiology | www.frontiersin.org 6 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
FIGURE 6 | (A) A 62-year-old woman presented with repeated postoperative bleeding after extraction of 36. The pictures shows a coagulum. The patient had a
history of Crohn’s disease for which she took infliximab, and a history of atrial fibrillation for which she used anticoagulants. She also took flecainide and bisoprolol
fumarate due to arrhythmias. (B) The wound heal after 6 weeks. Wound healing was likely delayed due to the postoperative bleeding, but possibly also due to the use
of Infliximab, which is a TNF-α inhibitor.
connection following closure with a Rehrmann flap (Guo and
Dipietro, 2010).
Thermal Damage
Excessive monopolar electrocoagulation of the bone, or drilling
without cooling, can lead to bone necrosis and the formation
of bone sequesters (Guo and Dipietro, 2010; Karamanos et al.,
2015).
Edema
Wound edema restricts the oxygen and nutrient supply to the
wound by enlarging the diffusion distance.
Injudicious Flap Design in Surgeries
FIGURE 7 | Buccosinusal connection after apex resection of 16, in To avoid flap necrosis and loss of wound covering in periodontal
which the incision was incorrectly performed on the opening to the surgery (Lindhe et al., 2015) and in stomatology (Stoelinga
sinus rather than on the healthy bone edges. A broad trapezium-shaped et al., 2009), one must follow the basic principles of surgery.
incision would have been desirable.
This includes ensuring that the flap base is sufficiently wide,
limiting the use of monopolar electrocoagulation, ensuring that
the wound edges are on healthy bone, and creating no excessive
teeth with an open apex, within the first year after trauma. The tension on a wound edge. Moreover, Incisions should not be
role of odontoblasts in this process remains unclear (Goldberg, made on an open junction to the maxillary sinus, but rather on
2011). healthy bone edges (Figure 7).
Antrum Perforation Corpus Alienum (Foreign Body)
Antrum perforation can lead to bad wound healing following Common corpora aliena in the mouth can vary from a piece
extraction of a molar or premolar in the upper jaw. of gutta percha or root canal cement to inserted hydroxyapatite
granules or osteosynthesis screws. Residual tooth elements, a
Local Infection radix relicta, residual pieces of crown, and bone sequesters can
Infection keeps a wound in an inflammatory state. Such also act as corpora aliena and lead to chronic wound infections.
infections are not necessarily prominently visible. A chronic Remaining wicks and compresses can also lead to poor wound
maxillary sinusitis can lead to recurrence of a buccosinusal healing and latent infections (Figure 8).
Frontiers in Physiology | www.frontiersin.org 7 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
FIGURE 8 | (A) A 16-year-old patient was referred due to persisting pain and pus in the extraction cavity of 48. Radiography shows incomplete bone healing in loco
48. (B) Wound exploration reveals gauze that remained unnoticed in the wound.
FIGURE 9 | (A) 67-year-old patient presented with Kelly syndrome, maxilla atrophy, 20-year history of smoking, and 9-year use of corticosteroids and methotrexate.
Maxilla reconstruction was performed through cranial bone. (B) Status before reconstruction. (C) Wound dehiscence with exposed bone. (D) Healing by second
intention after removal of the necrotic bone fragment and wound debris.
Following removal of the wisdom teeth in the mandible, fixation. This is also possible in the mandible after a mandibular
wound healing can be delayed by ischemic necrosis of the buccal fracture or osteotomy of the mandible (Adell et al., 1987).
edge of the alveolus (Stoelinga et al., 2009). On some occasions,
dental implants can act as a corpus alienum and cause severe Tooth Element in the Line of a Jaw Fracture
wound healing problems, such that removal is the only option. A non-union can be caused by a tooth element in the line of a
Although, a corpus alienum is often visible on radiography, this mandibular fracture, especially when the tooth exhibits a root
is not always the case—amalgam tattoos, crown cement around fracture.
an abutment, and small residues of broken reamers and files can
be easily overlooked and cause chronic problems. Traumatic Occlusion
As opposed to in a toothless maxilla, the presence of natural
Pathological Mobility dentition can threaten a reconstruction when the elements bite
Following a Le Fort I fracture or a Le Fort I osteotomy, a pseudo on the thin mucosa. Exposure of a bone fragment shortly after
arthrosis can develop due to either bruxism or insufficient rigid reconstruction can threaten the integration (Figures 9A–D). A
Frontiers in Physiology | www.frontiersin.org 8 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
FIGURE 10 | A 59-year-old male presented with wound healing
problems 2 months after placement of four implants in the mandibula.
The patient had been using systemic corticosteroids for the past 15 years due
to lung sarcoidosis, and had stopped smoking years ago. Despite excessive
alcohol use, neuropathy based on thiamin deficiency, and abnormal liver tests,
the patient was able to maintain professional activity and a good social
integration.
patient will often present not one but multiple simultaneous
contributory factors. Clinical situations that carry higher risk FIGURE 11 | A 58-year-old female presented with chronic infection,
include Kelly syndrome and an egression of the lateral parts of with pus and fistula formation in the neck. The patient had a history of
mouth floor carcinoma, alcoholism, depression, axonal polyneuropathy,
the maxilla with an edentate antagonistic jawbone.
Crohn’s disease, and nephrotic syndrome. Inadequate oral intake due to pain,
with secondary hypoalbuminemia and ion disorders, contributed to poor
Sutures wound healing and low resistance to infections.
Intraoral wounds are usually sutured with resorbable suture.
With regards to resorbable sutures, the tissue reactivity ranges
from polydioxanone (PDS) and polyglyconate (Maxon) being the
least reactive, to polyglycolic acid (PGA) and polyglactin acid literature does not include data supporting this association with
(Vicryl) showing mid-level reactivity, to chromic catgut as the regards to oral wounds.
most reactive with tissues (Hollander and Singer, 1999).
Local Anesthesia Hereditary Factors
In cell cultures and laboratory animals, local anesthetics exhibit In the literature, Ehlers-Danlos syndrome and Marfan syndrome
an inhibitory effect on wound healing, which is mainly reflected are stated to be associated with bad wound healing (Cohen et al.,
in the inflammatory and proliferation phase of wound healing 1992). However, at our tertiary center, we have not noted any
(Brower and Johnson, 2003). The use of epinephrine underlines problems with wound healing in the mouth among these patients
this effect (Dogan et al., 2003). Significant clinical effects have not over the last 30 years. Wound healing in the mouth is problematic
been proven in humans. However, it is recommended to not use among patients with osteogenesis imperfecta or epidermolysis
large volumes of local anesthetics (tumescent infiltration) in close bullosa.
proximity to surgical incisions in the gingiva.
Vitamin A
GENERAL FACTORS INFLUENCING THE Macrophage numbers increase with vitamin A intake. A lack of
WOUND HEALING IN THE MOUTH macrophages leads to reduced collagen synthesis and inhibits
wound healing.
Age
Although, age has been proposed to be a cause of bad wound
healing, this is not supported by evidence (Karamanos et al., Corticosteroids
2015). Corticosteroids have an inhibitory effect on macrophages,
leading to a decline in collagen synthesis. Acute administration
Obesity of high doses of corticosteroids should not impair wound healing,
Obesity is considered to be a general factor contributing to as opposed to chronic corticosteroid administration (Wang et al.,
disturbed wound healing (Guo and Dipietro, 2010). However, the 2013; Figure 10).
Frontiers in Physiology | www.frontiersin.org 9 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
FIGURE 12 | (A) A 51-year-old woman presented with peri-implantitis. She was a smoker with unstable diabetes mellitus. Her tooth implants (Nobel Biocare Mk III Ti
Unite) had been placed too close to each other, and the central implant in loco 12 had not been used. (B) An attempt was made to remove the infectious tissue
without removing the implant, and to substitute through artificial bone (BioOss® ) and L-PFR membranes. (C) LPRF membranes (D) End result after recovery attempt,
which did not account for numerous factors that impede wound healing.
Nutrition
Several epidemiological studies report that conditions related to
chronic inflammation can be improved by a diet rich in bioactive
fat mediators—as present in fish oil, e.g., poly unsaturated fatty
acids, eicosapentaenoic acid and docosahexaenoic acid—together
with low-dose aspirin (McDaniel et al., 2011). A diet rich in
omega-3 fatty acids can be recommended for treatment of
chronic inflammatory processes (Simopoulos, 2011; Roy et al.,
2013).
Undernutrition is a problem in wound healing, as is
established in daily practice among some patients with mouth
cancer combined with ethanol abuse (Figure 11), and in
depressed elderly patients who are socially isolated. Protein and
FIGURE 13 | A 50-year-old patient presented with a neck dissection at
vitamin deficiencies particularly influence wound healing (Shafer
the left side. She was known to abuse ethanol, to suffer from undernutrition,
et al., 1983). and to have a T4N0M0 spinocellular carcinoma of the left alveolar processes.
She was referred due to wound healing problems and recurrent necrosis of the
reconstruction through free flaps. Both a fibula flap and a lateral radialis flap
Diabetes Mellitus had failed. The wound in the neck exhibits inflammation, pus formation, and
Diabetes mellitus can severely disturb wound healing, likely due maceration of the wound edges.
to toxic sorbitol accumulation in tissues, pericapillary albumin
deposition that hampers nutrient and oxygen diffusion, and
disturbed collagen synthesis and collagen maturation (Broughton Smoking
et al., 2006). Patients with diabetes also exhibit macrophage Smoking has severe negative effects on all phases of wound
dysfunction that causes the inflammatory phase to last longer healing (Sorensen, 2012). Quitting smoking 4 weeks before
(Roy et al., 2013; Figures 12A–D). surgery has positive effects on the inflammatory phase, but
the proliferation phase remains disturbed. Administration of
vitamins C and E can decrease the damage in smokers,
Ethanol Abuse particularly related to collagen synthesis (Sorensen, 2012).
Alcohol metabolism leads to formation of acetaldehyde, reactive
oxygen radicals, and other molecules that damage healthy tissue. Medication
Almost all phases of wound healing are adversely affected by Bisphosphates, denosumab, and biologicals can cause severe
ethanol consumption (Jung et al., 2011; Figure 13). wound healing problems, with clinical manifestations including
Frontiers in Physiology | www.frontiersin.org 10 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
after extractions in patients with a history of chemotherapy
(Dietrich and Antoniades, 2012). Blood platelets and white
blood cells are highly important in wound healing; therefore,
wound healing complications are observed during active
immunosuppression or chemotherapy (Dunda et al., 2015).
However, this disadvantageous effect on wound healing is not
permanent.
Radiotherapy
Patients who undergo radiation therapy due to cancer of the
mouth of more than 50 Gy have much greater risk of problems
with wound healing after tooth extraction, particularly in the
molar region of the mandible (Sulaiman et al., 2003). Extractions
in these patients increase the risk of osteoradionecrosis of the
jaws when the radiation dose exceeds 50 Gy (Lee et al., 2009;
Tsai et al., 2013) more so when other risk factors are present
simultaneous (Nabil and Samman, 2012; Nadella et al., 2015).
Preoperative radiotherapy due to oral cancer is associated with
higher complication than postoperative radiotherapy (Momeni
et al., 2011; Mucke et al., 2012). The effects of radiation on the
FIGURE 14 | A 25-year-old female with progressive necrosis of the wound healing after surgery are dose - and fraction dependent
maxilla, showing loss of all molars in the right maxilla and the alveolar and are based primarily on a chronic vascular injury. This also
bone, with the emergence of a buccosinusal connection that occurred applies to transfer tissue that undergoes postoperative irradiation
after ustekinumab use for Crohn’s disease treatment. (A) A panoramic in the mouth. Jacobsen et al (Jacobsen et al., 2014) recorded an
radiography from the first consult, where the complaint of loose teeth was
formulated. (B) Three months after the radiography in panel A, we see the loss
Implant survival rates of 86% in non-irradiated grafted fibular
of elements 18, 17, 16, and 15. (Photo left). Two months later, an antrum bone, and 38% in irradiated grafted fibular bone.
perforation spontaneously occurred. Fibrosis, atrophy, contraction of oral mucosa, fistula
formation, wound dehiscence, skin flap reconstructive failure,
non-healing wound and skin necrosis are documented side
ulcers, wound dehiscence, bone necrosis, fistulas, and antrum effects of radiation therapy (Dormand et al., 2005; Gieringer
perforations (Figures 14A,B). et al., 2011; Haubner et al., 2012).
Hyperbaric Oxygen Anemia
Hyperbaric oxygen therapy is not used for normal wound In maxillo-facial reconstructions using free flaps, low
healing, but is indicated in complex compromised acute hemoglobin levels should be avoided, especially when the
injuries with tissue crushing, as well as in necrotic infections, flap exhibits characteristics of ischemia (Xie et al., 2015).
osteomyelitis, chronic ulcers, and late complications of
radiotherapy (Dauwe et al., 2014).
CONCLUSION
HIV
HIV-positive patients do not seem to have more complications Wound healing in the mouth occurs in the presence of many
following tooth extraction (Dodson, 1997), but do show more challenges, including a high bacterial and viral load, and
complication after mandibular fracture treatment (Schmidt et al., usually proceeds undisturbed and with preserved oral function.
1995). The risk for complications significantly increases when the When a facial or intra-oral wound presents a disturbed healing
number of CD4 T-lymphocytes is less than 400 per microliter process, it is recommended to conduct a thorough and judicious
(Dodson, 1997). examination to eliminate or correct underlying local or general
factors.
Chemotherapy—Immunosuppression
Chemotherapy for mouth cancer can result in oral mucositis AUTHOR CONTRIBUTIONS
during the active treatment phase, and in vitro studies indicate
disturbed wound healing during chemotherapy. However, CP, Initiated the review and assist in writing and review. JA, Write
disturbed wound healing is not a clinically significant finding the review. RJ and JS, Reviewed the manuscript.
REFERENCES Bielefeld, K. A., Amini-Nik, S., and Alman, B. A. (2013). Cutaneous wound healing:
recruiting developmental pathways for regeneration. Cell. Mol. Life Sci. 70,
Adell, R., Eriksson, B., Nylén, O., and Ridell, A. (1987). Delayed 2059–2081. doi: 10.1007/s00018-012-1152-9
healing of fractures of the mandibular body. Int. J. Oral Broughton, G. II, Janis, J. E., and Attinger, C. E. (2006). Wound
Maxillofac. Surg. 16, 15–24. doi: 10.1016/S0901-5027(87) healing: an overview. Plast Reconstr. Surg. 117, 1e–32e. doi:
80026-7 10.1097/01.prs.0000222562.60260.f9
Frontiers in Physiology | www.frontiersin.org 11 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
Brower, M. C., and Johnson, M. E. (2003). Adverse effects of local anesthetic Jacobsen, C., Kruse, A., Lübbers, H. T., Zwahlen, R., Studer, S., Zemann, W., et al.
infiltration on wound healing. Reg. Anesth. Pain Med. 28, 233–240. doi: (2014). Is mandibular reconstruction using vascularized fibula flaps and dental
10.1097/00115550-200305000-00011 implants a reasonable treatment? Clin. Implant. Dent. Relat. Res. 16, 419–428.
Cohen, I. K., Diegelmann, R. F., and Lindblad, W. J. (eds.). (1992). Wound Healing: doi: 10.1111/cid.12004
Biochemical and Clinical Aspects. Philadelphia: WB. Saunders Company; Jung, M. K., Callaci, J. J., Lauing, K. L., Otis, J. S., Radek, K. A., Jones, M. K., et al.
Harcourt Brace Jovanovich, Inc. (2011). Alcohol exposure and mechanisms of tissue injury and repair. Alcohol.
Cooper, D. M. (1999). Wound healing: new understandings. Nurse Pract. Forum Clin. Exp. Res. 35, 392–399. doi: 10.1111/j.1530-0277.2010.01356.x
10, 74–86. Junqueira, L. C., and Carneiro, J. (2007). Functionele Histologie. Maarssen: Elsevier
Dauwe, P. B., Pulikkottil, B. J., Lavery, L., Stuzin, J. M., and Rohrich, R. J. Gezondheidszorg.
(2014). Does hyperbaric oxygen therapy work in facilitating acute wound Karamanos, E., Osgood, G., Siddiqui, A., and Rubinfeld, I. (2015). Wound
healing: a systematic review. Plast. Reconstr. Surg. 133, 208e–215e. doi: healing in plastic surgery: does age matter? An American college of surgeons
10.1097/01.prs.0000436849.79161.a4 national surgical quality improvement program study. Plast. Reconstr. Surg.
Diegelmann, R. F., and Evans, M. C. (2004). Wound healing: an overview of acute, 135, 876–881. doi: 10.1097/PRS.0000000000000974
fibrotic and delayed healing. Front. Biosci. 9, 283–289. Kirsner, R. S., and Eaglstein, W. H. (1993). The wound healing process. Dermatol.
Dietrich, E., and Antoniades, K. (2012). Molecularly targeted drugs for the Clin. 11, 629–640.
treatment of cancer: oral complications and pathophysiology. Hippokratia 16, Larjava, H. (2012). Oral Wound Healing: Cell Biology and Clinical Management.
196–199. West Sussex: John Wiley & Sons, Inc.
Dimitrova-Nakov, S., Baudry, A., Harichane, Y., Kellermann, O., and Goldberg, M. Larson, B. J., Longaker, M. T., and Lorenz, H. P. (2010). Scarless fetal wound
(2014). Pulp stem cells: implication in reparative dentin formation. J. Endod. 40, healing: a basic science review. Plast. Reconstr. Surg. 126, 1172–1180. doi:
S13–S18. doi: 10.1016/j.joen.2014.01.011 10.1097/PRS.0b013e3181eae781
Discepoli, N., Vignoletti, F., Laino, L., de Sanctis, M., Muñoz, F., and Sanz, Lee, I. J., Koom, W. S., Lee, C. G., Kim, Y. B., Yoo, S. W., Keum, K. C., et al. (2009).
M. (2013). Early healing of the alveolar process after tooth extraction: an Risk factors and dose-effect relationship for mandibular osteoradionecrosis in
experimental study in the beagle dog. J. Clin. Periodontol. 40, 638–644. doi: oral and oropharyngeal cancer patients. Int. J. Radiat. Oncol. Biol. Phys. 75,
10.1111/jcpe.12074 1084–1091. doi: 10.1016/j.ijrobp.2008.12.052
Dodson, T. B. (1997). HIV status and the risk of post-extraction complications. J. Li, J., Chen, J., and Kirsner, R. (2007). Pathophysiology of acute wound healing.
Dent. Res. 76, 1644–1652. doi: 10.1177/00220345970760100501 Clin. Dermatol. 25, 9–18. doi: 10.1016/j.clindermatol.2006.09.007
Dogan, N., Uçok, C., Korkmaz, C., Ucok, O., and Karasu, H. A. (2003). The effects Lindhe, J., Karring, T., and Lang, N. P. (eds.). (2015). Clinical Periodontology and
of articaine hydrochloride on wound healing: an experimental study. J. Oral Implant Dentistry, 4th Edn. Blackwell; Munksgaard.
Maxillofac. Surg. 61, 1467–1470. doi: 10.1016/j.joms.2003.05.002 Mahdavian, D. B., van der Veer, W. M., van Egmond, M., Niessen, F. B., and
Dormand, E. L., Banwell, P. E., and Goodacre, T. E. (2005). Radiotherapy Beelen, R. H. (2011). Macrophages in skin injury and repair. Immunobiology
and wound healing. Int. Wound J. 2, 112–127. doi: 10.1111/j.1742- 216, 753–762. doi: 10.1016/j.imbio.2011.01.001
4801.2005.00079.x McDaniel, J. C., Massey, K., and Nicolaou, A. (2011). Fish oil supplementation
Dunda, S. E., Bozkurt, A., Pallua, N., and Krapohl, B. D. (2015). Reconstructive alters levels of lipid mediators of inflammation in microenvironment of
surgery in immunocompromised patients: evaluation and therapy. GMS acute human wounds. Wound Repair Regen. 19, 189–200. doi: 10.1111/j.1524-
Interdiscip. Plast. Reconstr. Surg. DGPW 4:Doc18. doi: 10.3205/iprs000077 475X.2010.00659.x
Eming, S. A., Martin, P., and Tomic-Canic, M. (2014). Wound repair and Momeni, A., Kim, R. Y., Kattan, A., Tennefoss, J., Lee, T. H., and Lee, G. K.
regeneration: mechanisms, signaling, and translation. Sci. Transl. Med. 6, (2011). The effect of preoperative radiotherapy on complication rate after
265sr6. doi: 10.1126/scitranslmed.3009337 microsurgical head and neck reconstruction. J. Plast. Reconstr. Aesthet. Surg.
Ennis, W. J., and Meneses, P. (2000). Wound healing at the local level: the stunned 64, 1454–1459. doi: 10.1016/j.bjps.2011.06.043
wound. Ostomy Wound Manage 46, 39S–48S. Moraschini, V., and Barboza, E. S. (2015). Effect of autologous platelet concentrates
Funato, N., Moriyama, K., Baba, Y., and Kuroda, T. (1999). Evidence for apoptosis for alveolar socket preservation: a systematic review. Int. J. Oral Maxillofac.
induction in myofibroblasts during palatal mucoperiosteal repair. J. Dent. Res. Surg. 44, 632–641. doi: 10.1016/j.ijom.2014.12.010
78, 1511–1517. doi: 10.1177/00220345990780090501 Mücke, T., Rau, A., Weitz, J., Ljubic, A., Rohleder, N., Wolff, K. D.,
Gardner E. A. (1925). An address on the cures of æsculapius. The Lancet 206, et al. (2012). Influence of irradiation and oncologic surgery on head
688–691. and neck microsurgical reconstructions. Oral Oncol. 48, 367–371. doi:
Gharaee-Kermani, M., and Phan, S. H. (2001). Role of cytokines and cytokine 10.1016/j.oraloncology.2011.11.013
therapy in wound healing and fibrotic diseases. Curr. Pharm. Des. 7, 1083–1103. Mutschler, W. (2012). [Physiology and pathophysiology of wound healing
doi: 10.2174/1381612013397573 of wound defects]. Unfallchirurg 115, 767–773. doi: 10.1007/s00113-012-
Gieringer, M., Gosepath, J., and Naim, R. (2011). Radiotherapy and wound healing: 2208-x
principles, management and prospects (review). Oncol. Rep. 26, 299–307. doi: Nabil, S., and Samman, N. (2012). Risk factors for osteoradionecrosis after head
10.3892/or.2011.1319 and neck radiation: a systematic review. Oral Surg. Oral Med. Oral Pathol. Oral
Glim, J. E., van Egmond, M., Niessen, F. B., Everts, V., and Beelen, R. H. (2013). Radiol. 113, 54–69. doi: 10.1016/j.tripleo.2011.07.042
Detrimental dermal wound healing: what can we learn from the oral mucosa? Nadella, K. R., Kodali, R. M., Guttikonda, L. K., and Jonnalagadda, A. (2015).
Wound Repair Regen. 21, 648–660. doi: 10.1111/wrr.12072 Osteoradionecrosis of the Jaws: clinico-therapeutic management: a literature
Goldberg, M. (2011). Pulp healing and regeneration: more questions than answers. review and update. J. Maxillofac. Oral Surg. 14, 891–901. doi: 10.1007/s12663-
Adv. Dent. Res. 23, 270–274. doi: 10.1177/0022034511405385 015-0762-9
Guo, S., and Dipietro, L. A. (2010). Factors affecting wound healing. J. Dent. Res. Öztürk, F., and Ermertcan, A. T. (2011). Wound healing: a new approach
89, 219–229. doi: 10.1177/0022034509359125 to the topical wound care. Cutan. Ocul. Toxicol. 30, 92–99. doi:
Haubner, F., Ohmann, E., Pohl, F., Strutz, J., and Gassner, H. G. (2012). Wound 10.3109/15569527.2010.539586
healing after radiation therapy: review of the literature. Radiat. Oncol. 7, 162. Politis, C., Lambrichts, I., and Agbaje, J. O. (2014). Neuropathic pain after
doi: 10.1186/1748-717X-7-162 orthognathic surgery. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 117,
Hollander, J. E., and Singer, A. J. (1999). Laceration management. Ann. Emerg. e102–e107. doi: 10.1016/j.oooo.2013.08.001
Med. 34, 356–367. doi: 10.1016/S0196-0644(99)70131-9 Reinke, J. M., and Sorg, H. (2012). Wound repair and regeneration. Eur. Surg. Res.
Hom, D. B., Hebda, P. A., Gosain, A. K., and Friedman, C. D. (eds.). (2009). 49, 35–43. doi: 10.1159/000339613
Essential Tissue Healing of the Face and Neck. Shelton, CT: BC Decker Inc., Rodriguez-Merchan, E. C. (2012). Surgical wound healing in bleeding disorders.
People’s Medical Publishing. Haemophilia 18, 487–490. doi: 10.1111/j.1365-2516.2012.02760.x
Hunt, T. K., Hopf, H., and Hussain, Z. (2000). Physiology of wound healing. Adv. Roy, S., Das, A., and Sen, C. K. (2013). “Disorder of localized inflammation in
Skin Wound Care 13, 6–11. wound healing: a systems perspective,” in Complex Systems and Computational
Frontiers in Physiology | www.frontiersin.org 12 November 2016 | Volume 7 | Article 507
Politis et al. Wound Healing Problems in the Mouth
Biology Approaches to Acute Inflammation, eds Y. Vodovotz and G. An (New with oropharyngeal cancer. Int. J. Radiat. Oncol. Biol. Phys. 85, 415–420. doi:
York, NY: Springer), 173–183. 10.1016/j.ijrobp.2012.05.032
Schmidt, B., Kearns, G., Perrott, D., and Kaban, L. B. (1995). Infection Vanwijck, R. (2001). [Surgical biology of wound healing]. Bull. Mem. Acad. R. Med.
following treatment of mandibular fractures in human immunodeficiency Belg. 156, 175–184.
virus seropositive patients. J. Oral Maxillofac. Surg. 53, 1134–1139. doi: Velnar, T., Bailey, T., and Smrkolj, V. (2009). The wound healing process: an
10.1016/0278-2391(95)90618-5 overview of the cellular and molecular mechanisms. J. Int. Med. Res. 37,
Schreml, S., Szeimies, R. M., Prantl, L., Karrer, S., Landthaler, M., and Babilas, 1528–1542. doi: 10.1177/147323000903700531
P. (2010). Oxygen in acute and chronic wound healing. Br. J. Dermatol. 163, Wang, A. S., Armstrong, E. J., and Armstrong, A. W. (2013). Corticosteroids and
257–268. doi: 10.1111/j.1365-2133.2010.09804.x wound healing: clinical considerations in the perioperative period. Am. J. Surg.
Shafer, W. G., Hine, M. K., Levy, B. M., and Tomich, C. E. (1983). Textbook of Oral 206, 410–417. doi: 10.1016/j.amjsurg.2012.11.018
Pathology, 4th Edn. Philadelphia: WB Saunders Company. Wong, V. W., Gurtner, G. C., and Longaker, M. T. (2013). Wound healing:
Simopoulos, A. P. (2011). Evolutionary aspects of diet: the omega-6/omega-3 ratio a paradigm for regeneration. Mayo Clin. Proc. 88, 1022–1031. doi:
and the brain. Mol. Neurobiol. 44, 203–215. doi: 10.1007/s12035-010-8162-0 10.1016/j.mayocp.2013.04.012
Sørensen, L. T. (2012). Wound healing and infection in surgery: the Xie, P., Jia, S., Tye, R., Chavez-Munoz, C., Vracar-Grabar, M., Hong,
pathophysiological impact of smoking, smoking cessation, and nicotine S. J., et al. (2015). Systemic administration of hemoglobin improves
replacement therapy: a systematic review. Ann. Surg. 255, 1069–1079. doi: ischemic wound healing. J. Surg. Res. 194, 696–705. doi: 10.1016/j.jss.2014.
10.1097/SLA.0b013e31824f632d 10.050
Stoelinga, P. J. W., Brouns, J. J. A., and Merkx, M. A. W. (2009). Mondchirurgie Yip, W. L. (2015). Influence of oxygen on wound healing. Int. Wound J. 12,
voor tandartsen. Houten: Bohn Stafleu van Loghum. 620–624. doi: 10.1111/iwj.12324
Sulaiman, F., Huryn, J. M., and Zlotolow, I. M. (2003). Dental extractions in the
irradiated head and neck patient: a retrospective analysis of Memorial Sloan- Conflict of Interest Statement: The authors declare that the research was
Kettering Cancer Center protocols, criteria, and end results. J. Oral Maxillofac. conducted in the absence of any commercial or financial relationships that could
Surg. 61, 1123–1131. doi: 10.1016/S0278-2391(03)00669-4 be construed as a potential conflict of interest.
Takeo, M., Lee, W., and Ito, M. (2015). Wound healing and skin regeneration. Cold
Spring Harb. Perspect. Med. 5:a023267. doi: 10.1101/cshperspect.a023267 Copyright © 2016 Politis, Schoenaers, Jacobs and Agbaje. This is an open-access
Trombelli, L., Farina, R., Marzola, A., Bozzi, L., Liljenberg, B., and Lindhe, J. (2008). article distributed under the terms of the Creative Commons Attribution License (CC
Modeling and remodeling of human extraction sockets. J. Clin. Periodontol. 35, BY). The use, distribution or reproduction in other forums is permitted, provided the
630–639. doi: 10.1111/j.1600-051X.2008.01246.x original author(s) or licensor are credited and that the original publication in this
Tsai, C. J., Hofstede, T. M., Sturgis, E. M., Garden, A. S., Lindberg, M. E., Wei, Q., journal is cited, in accordance with accepted academic practice. No use, distribution
et al. (2013). Osteoradionecrosis and radiation dose to the mandible in patients or reproduction is permitted which does not comply with these terms.
Frontiers in Physiology | www.frontiersin.org 13 November 2016 | Volume 7 | Article 507
View publication stats
You might also like
- Case Presentation - Malignant Pleural Effusion EditedDocument117 pagesCase Presentation - Malignant Pleural Effusion EditedChristian Gallardo, MD100% (1)
- A Homeopathic Practice R Hughes 1Document52 pagesA Homeopathic Practice R Hughes 1goharNo ratings yet
- Red Flag: MSK Services Pathway - Shoulder PathologyDocument11 pagesRed Flag: MSK Services Pathway - Shoulder PathologyMuhammed ElgasimNo ratings yet
- MCQs Gynaec 2 - ObGynDocument10 pagesMCQs Gynaec 2 - ObGynbmhsh100% (3)
- Wound Healing Concepts in Clinical Practice of OMFDocument23 pagesWound Healing Concepts in Clinical Practice of OMFrozh rasulNo ratings yet
- Woundhealingseminar 150216070848 Conversion Gate02Document103 pagesWoundhealingseminar 150216070848 Conversion Gate02mohan100% (1)
- Stem Cells in OrthodonticsDocument4 pagesStem Cells in OrthodonticsInternational Journal of Innovative Science and Research Technology100% (1)
- Regenerative EndodonticsDocument13 pagesRegenerative EndodonticsIJAR JOURNAL100% (1)
- Biologic Interfaces in Esthetic Dentistry. Part I: The Perio/restorative InterfaceDocument21 pagesBiologic Interfaces in Esthetic Dentistry. Part I: The Perio/restorative InterfaceRoopa BabannavarNo ratings yet
- Ped A Internship 1517300917 PDF 2Document13 pagesPed A Internship 1517300917 PDF 2dariasuslowaNo ratings yet
- Berglundh Et Al-2018-Journal of Clinical PeriodontologyDocument6 pagesBerglundh Et Al-2018-Journal of Clinical PeriodontologyCristian CulcitchiNo ratings yet
- Wound Healing Problems in The Mouth: Constantinus Politis, Joseph Schoenaers, Reinhilde Jacobs and Jimoh O. AgbajeDocument13 pagesWound Healing Problems in The Mouth: Constantinus Politis, Joseph Schoenaers, Reinhilde Jacobs and Jimoh O. AgbajeankitaNo ratings yet
- Cicatrización ImplanteDocument18 pagesCicatrización Implantejorge sepulvedaNo ratings yet
- Soft Tissue Wound Healing Around Teeth and Dental ImplantsDocument17 pagesSoft Tissue Wound Healing Around Teeth and Dental ImplantsDavid CastañedaNo ratings yet
- Jcpe 12206 PDFDocument17 pagesJcpe 12206 PDFrozh rasulNo ratings yet
- Jcpe 12206 PDFDocument17 pagesJcpe 12206 PDFrozh rasulNo ratings yet
- Jcpe 12206 PDFDocument17 pagesJcpe 12206 PDFrozh rasulNo ratings yet
- Aps 2019 00913Document5 pagesAps 2019 00913lsintaningtyasNo ratings yet
- Occlusal Disharmony and Chronic Oro-Facial PainDocument9 pagesOcclusal Disharmony and Chronic Oro-Facial PaindepttofprosthodonticsNo ratings yet
- Modified classification guides treatment of altered passive and active eruptionDocument7 pagesModified classification guides treatment of altered passive and active eruptionMara CondorNo ratings yet
- Anterior Open Bite in The Mixed Dentition: European Journal of Paediatric Dentistry March 2019Document4 pagesAnterior Open Bite in The Mixed Dentition: European Journal of Paediatric Dentistry March 2019TIFFANINo ratings yet
- Amat P. 2008Document26 pagesAmat P. 2008AndreaVanoyMartinNo ratings yet
- Artigo Efficacyof OraldiclofenacDocument8 pagesArtigo Efficacyof OraldiclofenacHarold CamargoNo ratings yet
- Gingival Biotype Determines Periodontal Disease and Treatment OutcomesDocument6 pagesGingival Biotype Determines Periodontal Disease and Treatment Outcomesilich sevillaNo ratings yet
- Review of New Trends in Myofunctional Therapy OcclDocument4 pagesReview of New Trends in Myofunctional Therapy Occl이창엽No ratings yet
- s41121 016 0003 9 PDFDocument9 pagess41121 016 0003 9 PDFXray PolyclinicNo ratings yet
- Buchbender 2017Document20 pagesBuchbender 2017dreneanastriNo ratings yet
- Anterior Open Bite in The Mixed Dentition: European Journal of Paediatric Dentistry March 2019Document4 pagesAnterior Open Bite in The Mixed Dentition: European Journal of Paediatric Dentistry March 2019Mirza GlusacNo ratings yet
- Int Endodontic J - 2022 - Segura Egea - Impact of Systemic Health On Treatment Outcomes in Endodontics-1Document17 pagesInt Endodontic J - 2022 - Segura Egea - Impact of Systemic Health On Treatment Outcomes in Endodontics-1Nishant ChauhanNo ratings yet
- Histologia MeniniDocument10 pagesHistologia Meninijuanita enriquezNo ratings yet
- Occlusion, Orthodontics and Posture: Are There Evidences? The Example of ScoliosisDocument10 pagesOcclusion, Orthodontics and Posture: Are There Evidences? The Example of ScoliosisAndreaVanoyMartinNo ratings yet
- Odontoblast Control of Dental Pulp in Ammation Triggered by Cariogenic BacteriaDocument4 pagesOdontoblast Control of Dental Pulp in Ammation Triggered by Cariogenic BacteriaJavier Farias VeraNo ratings yet
- The Viazis Classification of Malocclusion: Journal of Dental Health Oral Disorders & TherapyDocument9 pagesThe Viazis Classification of Malocclusion: Journal of Dental Health Oral Disorders & TherapyWilmer Yanquen VillarrealNo ratings yet
- A Review of The Crown Lengthening Surgery The BasiDocument8 pagesA Review of The Crown Lengthening Surgery The BasiPaTt Tyy RodríguezNo ratings yet
- Hydrogel Vs DycalDocument10 pagesHydrogel Vs DycalConsultorio Odontologico Dra Yoli PerdomoNo ratings yet
- Sellke1998 PDFDocument9 pagesSellke1998 PDFHARITHA H.PNo ratings yet
- Jurnal PBL 1Document6 pagesJurnal PBL 1Sundae McdNo ratings yet
- Intravenous Zoledronic Acid in Postmenopausal Women With Low Bone Mineral DensityDocument9 pagesIntravenous Zoledronic Acid in Postmenopausal Women With Low Bone Mineral DensityCalvin AffendyNo ratings yet
- Re MineralizationDocument16 pagesRe MineralizationAnindyaNoviaPutriNo ratings yet
- IEJ - Revitalization in EndodonticsDocument7 pagesIEJ - Revitalization in Endodonticssoho1303No ratings yet
- Bergenholtz Spangberg 2004 Controversies in EndodonticsDocument16 pagesBergenholtz Spangberg 2004 Controversies in Endodontics筒井絢子No ratings yet
- Effect of Low Power Laser On Postoperative Pain in Endodontic Treatment: Literature ReviewDocument5 pagesEffect of Low Power Laser On Postoperative Pain in Endodontic Treatment: Literature ReviewIJAERS JOURNALNo ratings yet
- Orthodontic Trainee Gains Award To Research Cleft Palate MorphogenesisDocument1 pageOrthodontic Trainee Gains Award To Research Cleft Palate MorphogenesisClaudia BarbosaNo ratings yet
- CJR General Chemist Group TwoDocument15 pagesCJR General Chemist Group TwoGresia FalentinaNo ratings yet
- Sri Dwi Mutiara - Jurnal Maloklusi 1Document8 pagesSri Dwi Mutiara - Jurnal Maloklusi 1sri dwi mutiaraNo ratings yet
- Application of Ozonized Oils in Human Body and Oral Cavity Systems Aplicação Dos Óleos Ozonizados Nos Sistemas Do Corpo Humano e Cavidade OralDocument11 pagesApplication of Ozonized Oils in Human Body and Oral Cavity Systems Aplicação Dos Óleos Ozonizados Nos Sistemas Do Corpo Humano e Cavidade OralTiago Oliveira ImperiortoNo ratings yet
- 2011 SOSORT Guidelines: Orthopaedic and Rehabilitation Treatment of Idiopathic Scoliosis During GrowthDocument36 pages2011 SOSORT Guidelines: Orthopaedic and Rehabilitation Treatment of Idiopathic Scoliosis During GrowthAnindira RustandiNo ratings yet
- Ozone Therapy For Low Back Pain A Systematic RevieDocument11 pagesOzone Therapy For Low Back Pain A Systematic Revieluis buenaventuraNo ratings yet
- 4th Article PDFDocument10 pages4th Article PDFSafu SalehNo ratings yet
- qi_Soldatos_37133Document18 pagesqi_Soldatos_37133Juliana Gomes BarretoNo ratings yet
- Scope of Endodontics: Regenerative Endodontics: AAE Position StatementDocument3 pagesScope of Endodontics: Regenerative Endodontics: AAE Position StatementPuneet ChahalNo ratings yet
- JIntOralHealth 2021 13 5 441 3278672Document10 pagesJIntOralHealth 2021 13 5 441 3278672IgnasNo ratings yet
- The Functional Appliance Debate The Choice Is YourDocument2 pagesThe Functional Appliance Debate The Choice Is YourAriana AmarilesNo ratings yet
- Vallejo Rosero2019Document21 pagesVallejo Rosero2019sdadNo ratings yet
- Voice Rest Versus Exercise: A Review of The Literature: Madison, WisconsinDocument9 pagesVoice Rest Versus Exercise: A Review of The Literature: Madison, WisconsinJaime Crisosto AlarcónNo ratings yet
- Irrigation Solutions in Open Fractures of The Lower Extremities: Evaluation of Isotonic Saline and Distilled WaterDocument6 pagesIrrigation Solutions in Open Fractures of The Lower Extremities: Evaluation of Isotonic Saline and Distilled WaterDita Putri DamayantiNo ratings yet
- Ι Mplant-Supported Overdentures: Clinical Review: · September 2017Document10 pagesΙ Mplant-Supported Overdentures: Clinical Review: · September 2017ankitaNo ratings yet
- Jcraniofac - Surg Quessaaccepted Jul.22Document4 pagesJcraniofac - Surg Quessaaccepted Jul.22Julio SantanaNo ratings yet
- Effectiveness of Myofunctional Therapy in Ankyloglossia: A Systematic ReviewDocument18 pagesEffectiveness of Myofunctional Therapy in Ankyloglossia: A Systematic Reviewmistic0No ratings yet
- Int Endodontic J - 2022 - Fransson - Tooth Survival After Endodontic TreatmentDocument14 pagesInt Endodontic J - 2022 - Fransson - Tooth Survival After Endodontic TreatmentkecasweatNo ratings yet
- Chenetal 2009aJOMIDocument33 pagesChenetal 2009aJOMI63127No ratings yet
- Dedication: "Give Me A Place To Stand On, and I Will Move The Earth."Document304 pagesDedication: "Give Me A Place To Stand On, and I Will Move The Earth."Amiana Joy SaguidNo ratings yet
- Tooth Movement (Frontiers of Oral Biology)Document92 pagesTooth Movement (Frontiers of Oral Biology)GABRIELA NIETO GONZALEZNo ratings yet
- How Does The Timing of Implant Placement To Extraction Affect Outcome?Document24 pagesHow Does The Timing of Implant Placement To Extraction Affect Outcome?Narissaporn ChaiprakitNo ratings yet
- Nihms 222369 PDFDocument18 pagesNihms 222369 PDFmariasoledaNo ratings yet
- 51.1artigos Blog Microbotox Lift SupercíloDocument6 pages51.1artigos Blog Microbotox Lift SupercíloAlberto EliasNo ratings yet
- Joint Function Preservation: A Focus on the Osteochondral UnitFrom EverandJoint Function Preservation: A Focus on the Osteochondral UnitNo ratings yet
- Wound Healing in Oral Mucosa Results in PDFDocument13 pagesWound Healing in Oral Mucosa Results in PDFrozh rasulNo ratings yet
- Harrsion 1991 PDFDocument8 pagesHarrsion 1991 PDFrozh rasulNo ratings yet
- Wound Healing in Oral Mucosa Results in PDFDocument13 pagesWound Healing in Oral Mucosa Results in PDFrozh rasulNo ratings yet
- Harrsion 1991 PDFDocument8 pagesHarrsion 1991 PDFrozh rasulNo ratings yet
- Saliva and Wound Healing: Henk S. Brand, Enno C.I. VeermanDocument6 pagesSaliva and Wound Healing: Henk S. Brand, Enno C.I. Veermanrozh rasulNo ratings yet
- Harrsion 1991 PDFDocument8 pagesHarrsion 1991 PDFrozh rasulNo ratings yet
- Jcpe 12206 PDFDocument17 pagesJcpe 12206 PDFrozh rasulNo ratings yet
- Jcpe 12206 PDFDocument17 pagesJcpe 12206 PDFrozh rasulNo ratings yet
- Platelet Rich Plasma: New Insights For Cutaneous Wound Healing ManagementDocument20 pagesPlatelet Rich Plasma: New Insights For Cutaneous Wound Healing Managementrozh rasulNo ratings yet
- Recent Trends On Wound Management: New Therapeutic Choices Based On Polymeric CarriersDocument24 pagesRecent Trends On Wound Management: New Therapeutic Choices Based On Polymeric Carriersrozh rasulNo ratings yet
- Scarlet Fever - Background, Pathophysiology, EtiologyDocument8 pagesScarlet Fever - Background, Pathophysiology, EtiologyPaskalia ChristinNo ratings yet
- Mapeh Week 4-5 Q3Document16 pagesMapeh Week 4-5 Q3Jinky PinedaNo ratings yet
- Davao Doctors College General Malvar ST., Davao City Nursing ProgramDocument12 pagesDavao Doctors College General Malvar ST., Davao City Nursing ProgramJerremy LuqueNo ratings yet
- Acetyl Cy Stein Epk CatsDocument5 pagesAcetyl Cy Stein Epk CatsOchima Walichi PrameswariNo ratings yet
- Kartu Soal Bahasa Inggris XIIDocument7 pagesKartu Soal Bahasa Inggris XIICut FitriasariNo ratings yet
- Effectiveness of BNT162b2 Vaccine Against Omicron Variant in South AfricaDocument3 pagesEffectiveness of BNT162b2 Vaccine Against Omicron Variant in South AfricaDaniel A. SaldanaNo ratings yet
- Research Menopause DepressionDocument5 pagesResearch Menopause DepressionVinitha JobyNo ratings yet
- Annals of Medicine and Surgery: Sara Bouabdella, Soraya Aouali, Hanan Ragragui, Nada Zizi, Siham DikhayeDocument3 pagesAnnals of Medicine and Surgery: Sara Bouabdella, Soraya Aouali, Hanan Ragragui, Nada Zizi, Siham DikhayeGeysel SuarezNo ratings yet
- Oral Health in Persons With Down Syndrome A Literature ReviewDocument9 pagesOral Health in Persons With Down Syndrome A Literature ReviewRisana RahoofNo ratings yet
- Art - 2386Document37 pagesArt - 2386Kumar palNo ratings yet
- "A Day in My Life During Covid-19" The Entrepreneurial MindDocument7 pages"A Day in My Life During Covid-19" The Entrepreneurial MindG & E ApparelNo ratings yet
- Epstein-Barr Virus (Infectious Mononucleosis)Document3 pagesEpstein-Barr Virus (Infectious Mononucleosis)KanayaNo ratings yet
- Material HandlingDocument51 pagesMaterial HandlingRaeedi PullaraoNo ratings yet
- Classroom Activity HLTWHS002Document6 pagesClassroom Activity HLTWHS002Sonam Gurung100% (1)
- Pengaruh Varietas Dan Umur Tanaman Berbeda Terhadap Jumlah Populasi Dan Tingkat Serangan Hama Dan Penyakit Pisang (Musa SP.) Di Kabupaten SukabumiDocument8 pagesPengaruh Varietas Dan Umur Tanaman Berbeda Terhadap Jumlah Populasi Dan Tingkat Serangan Hama Dan Penyakit Pisang (Musa SP.) Di Kabupaten SukabumiAdil NugrohoNo ratings yet
- DMJ 2020 0258Document17 pagesDMJ 2020 0258Elena Borş MorariNo ratings yet
- The Incidence of Venous Thromboembolism in Commercial Airline Pilots. A Cohort Study of 2630 PilotsDocument6 pagesThe Incidence of Venous Thromboembolism in Commercial Airline Pilots. A Cohort Study of 2630 Pilotsluis11256No ratings yet
- Dalal & MishraDocument491 pagesDalal & MishraKarthika M TharakanNo ratings yet
- 1-Aarogyam B + Covid Ab IgG - PO3827226873-180Document16 pages1-Aarogyam B + Covid Ab IgG - PO3827226873-180Rohit PandeyNo ratings yet
- 10 Health Benefits of Scent Leaf (Efinrin) for Oral Hygiene, Malaria, Pain ReliefDocument3 pages10 Health Benefits of Scent Leaf (Efinrin) for Oral Hygiene, Malaria, Pain ReliefAishaNo ratings yet
- Quiz Critical CareDocument15 pagesQuiz Critical CareSuma AhmadNo ratings yet
- Modified Thayer Martin Medium Base (W/o Supplement) : CompositionDocument3 pagesModified Thayer Martin Medium Base (W/o Supplement) : CompositionAbid SiddiquiNo ratings yet
- Dengue AwarenessDocument25 pagesDengue AwarenessAsorihm MhirosaNo ratings yet
- Pericarditis NCLEX Review: Serous Fluid Is Between The Parietal and Visceral LayerDocument3 pagesPericarditis NCLEX Review: Serous Fluid Is Between The Parietal and Visceral LayerJustine Dinice MunozNo ratings yet
- 001 Diagnosis of Neurological DiseaseDocument7 pages001 Diagnosis of Neurological DiseasemgvbNo ratings yet