Professional Documents
Culture Documents
Lazarine Leprosy: A Unique Phenomenon of Leprosy: Case Report
Uploaded by
irwan junOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Lazarine Leprosy: A Unique Phenomenon of Leprosy: Case Report
Uploaded by
irwan junCopyright:
Available Formats
[Downloaded free from http://www.ijmyco.org on Sunday, February 14, 2021, IP: 180.242.51.
124]
Case Report
Lazarine Leprosy: A Unique Phenomenon of Leprosy
Vaishali Wankhade1, Vrutika Shah2, Rajesh P. Singh1, Dharitri Bhat3
Departments of Dermatology, Venereology and Leprosy and 3Pathology, Government Medical College, Nagpur, 2Department of Dermatology, Venereology and
1
Leprosy, Seth GS Medical College and KEM Hospital, Mumbai, Maharashtra, India
Abstract
Leprosy, a chronic granulomatous disease, has been known since ages but even today continues to baffle the clinicians with a wide spectrum
of clinical, histopathological, and immunological characteristics. Leprosy reactions are mainly of two types, namely, Type 1 and Type 2. In
Type 1 leprosy reaction, the preexisting lesions become erythematous, edematous, and rarely ulcerate. Ulcerating Type 1 reaction is called
lazarine leprosy. Ulcerations may occur in borderline tuberculoid (BT) pole or borderline lepromatous pole but more common in BT pole.
In this postelimination era of leprosy, we report an interesting case report of BT Hansen’s disease with Type 1 lepra reaction with ulceration,
namely, lazarine leprosy.
Keywords: Lazarine, lepra reaction, tuberculoid, ulceration
Submitted: 01-Jun-2020 Revised: 01-Jul-2020 Accepted: 07-Jul-2020 Published: 28‑Aug‑2020
Introduction loss of hair over the lesions. On motor examination, book test,
card test, and Froment’s sign were positive on the right hand,
Lazarine leprosy, namely, ulcerating Type 1 reaction, was first
indicating the involvement of the deep branch of the ulnar
described in 1852 by Raphael Lucio and Ignacio Alvarado.[1]
nerve. Peripheral nerve examination is tabulated in Table 1.
Type 1 lepra reaction is a cell‑mediated immune reaction seen
The slit‑skin smear (SSS) performed from the right earlobe, left
in borderline forms of leprosy; the preexisting lesions become
eyebrow, and the plaque over the chest was positive for acid‑fast
erythematous, edematous, and rarely ulcerate. In 1930, in the
bacilli. Morphological index (MI) showed all fragmented
Fifth International Congress of Leprosy, it was concluded
bacilli, and bacteriological index (BI) was 1+. Histopathology
that lazarine leprosy can occur in tuberculoid pole because of
from the periphery of the plaques over the left thigh and chest
high inflammation and in lepromatous pole because of high
showed peri‑adnexal dense infiltrate with superficial and deep
bacillary load.[2]
dermal granulomas consisting of predominantly epithelioid
Case Report cells, lymphocytes, few neutrophils, and macrophages, with
A 69‑year‑old male presented to our outpatient department eosinophilic cytoplasm suggestive of borderline tuberculoid (BT)
(OPD) with multiple, asymptomatic, reddish, raised lesions Hansen’s disease. Based on the above findings, the patient was
all over the body for 4 months. No history of fever, tingling diagnosed as a case of BT Hansen’s disease and was started
numbness of hands and feet, weakness of hands and feet, on multibacillary multidrug therapy (MBMDT). Four weeks
epistaxis, or redness of the eyes was present. A history of
irregular treatment taken in the form of white‑ and red‑colored Address for correspondence:
blister packets for 2–3 months was present. General examination Dr. Vrutika Shah,
was within normal limits. The body mass index of the patient was B/1103, Apollo Pride Enclave Complex, Opp. Thane Bharat Sahakari Bank,
23.3 kg/m2. On cutaneous examination, multiple, erythematous, Vishnunagar, Thane-West, Maharashtra, India.
dry, scaly, annular plaques with well‑defined, inner borders E-mail: vrutikashah25@gmail.com
and sloping outer border giving an inverted saucer‑shaped ORCID:
appearance were seen over the chest, back, bilateral upper and https://orcid.org/0000‑0001‑6543‑7244
lower limbs, and soles. There were sensory impairment and
This is an open access journal, and articles are distributed under the terms of the Creative
Access this article online Commons Attribution‑NonCommercial‑ShareAlike 4.0 License, which allows others to
Quick Response Code: remix, tweak, and build upon the work non‑commercially, as long as appropriate credit
Website: is given and the new creations are licensed under the identical terms.
www.ijmyco.org For reprints contact: WKHLRPMedknow_reprints@wolterskluwer.com
DOI: How to cite this article: Wankhade V, Shah V, Singh RP, Bhat D.
10.4103/ijmy.ijmy_104_20 Lazarine leprosy: A unique phenomenon of leprosy. Int J Mycobacteriol
2020;9:329-31.
© 2020 International Journal of Mycobacteriology | Published by Wolters Kluwer - Medknow 329
[Downloaded free from http://www.ijmyco.org on Sunday, February 14, 2021, IP: 180.242.51.124]
Wankhade, et al.: Lazarine leprosy
after taking MBMDT, the patient presented to our OPD with presentations in leprosy are often seen due to partial and
spontaneous ulcerations over the preexisting lesions. No history delayed treatment. These lead to high morbidity among the
of any new lesions was present. Constitutional symptoms patients and a major risk for transmission and disabilities.
were absent. Cutaneous examination revealed nontender Two types of ulcers are seen in Hansen’s disease, namely,
ulcers with well‑defined margins and a clear base appearing leprous ulcers and trophic ulcers.[3] Trophic ulcers are seen
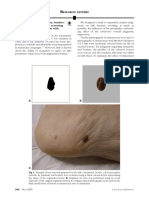
on the preexisting plaques over the chest [Figure 1a] and due to sensory impairment, whereas leprous ulcers are seen
back [Figure 1b]. The floor was covered with reddish granulation
tissue, and the surrounding skin was hyperpigmented. The
ulnar nerves and common peroneal nerves were bilaterally
thickened (Grade 1) and nontender, with the right more
thickened than the left. Hematological investigations revealed
low hemoglobin (Hb – 8.8 g/dL) and low hematocrit (26%).
The mean corpuscular volume (90.7 fL), mean corpuscular
hemoglobin (MCH) (30.6 pg), MCH concentration (33.8 g/dL),
and red cell distribution width (14.1%) were within normal
limits. Serum reticulocyte count was 1%. Peripheral blood smear
showed mild hypochromasia and microcytosis with rest of the
picture being normal. Due to financial constraints, investigations
a b
such as serum iron studies could not be performed. Based on
the above blood picture, a diagnosis of iron deficiency anemia Figure 1: (a and b) Multiple, nontender ulcers with well‑defined margins
was made by the physician. Other investigations such as fasting and a clear base appearing over the preexisting plaques over the
chest (black arrow) and back (red arrow)
and postprandial blood glucose levels, liver function test (total
protein level was 6.3 g/dL and serum albumin level was 4.5
g/dL), renal function test, and urine routine microscopy were
within normal limits. Venereal Disease Research Laboratory and
HIV ELISA tests were nonreactive. Pus culture revealed growth
of Staphylococcus aureus. Blood culture grew no organism.
SSS performed from the right earlobe, left eyebrow, and the
papule over the back was positive. MI showed all fragmented
bacilli, and BI was 1+. Histopathology from the periphery of the
ulcerated plaque of the chest and upper back [Figure 2] showed
mild hyperkeratosis, focal parakeratosis, and focally thinned‑out
epidermis with normal rete ridges. The subepidermal zone was
variably infiltrated. Reticular dermis showed multiple discrete Figure 2: Granulomas composed of epithelioid histiocytes, lymphocytes,
and mostly coalesced epithelioid cell granulomas composed multiple foreign body and Langhans (black arrow) giant cells, with few
of epithelioid histiocytes; lymphocytes; and multiple, large, neutrophils present (H and E, ×10 and ×40)
multinucleated (Langhans and foreign‑body type) giant cells.
Few foci showed neutrophils. Similar infiltrate was seen to
extend to the deep dermis and subcutaneous tissue. There was no
evidence of any vessel wall damage or macrophages or collagen
disruption. Similar histopathology findings were observed from
biopsy of the periphery of the plaque over the right sole. On
clinicopathological correlation, a diagnosis of BT Hansen’s
disease with ulcerative Type 1 lepra reaction, i.e., lazarine
leprosy, was made. The patient was started on oral prednisolone
40 mg once daily in the morning after breakfast and tapered
after every 2 weeks to 30 mg, 20 mg, 15 mg, 10 mg, and 5 mg
and then discontinued. Oral amoxicillin/clavulanic acid 625 mg
three times a day was given for 10 days and then discontinued.
After 3 weeks of treatment, the ulcers healed with hypochromic
atrophic scars with a hyperpigmented border [Figure 3].
Discussion Figure 3: Pre‑ and post‑treatment photographs of the ulcers healing
The term “lazarine leprosy” designates a severe, widespread, with hypochromic atrophic scars and hyperpigmented borders over the
ulcerative phenomenon in patients with leprosy.[3] Atypical chest (red arrows) and back (black arrows)
330 International Journal of Mycobacteriology ¦ Volume 9 ¦ Issue 3 ¦ July-September 2020
[Downloaded free from http://www.ijmyco.org on Sunday, February 14, 2021, IP: 180.242.51.124]
Wankhade, et al.: Lazarine leprosy
and circulatory signs; very prominent varicose veins; absence
Table 1: Peripheral nerve examination
of eye lesions; and an absolute absence of nodules.[1,8] Our
Nerve Thickening Tender patient had tingling of hands and feet. Polymerase chain
Supraorbital nerve Not thickened Nontender reaction can help in identifying leprosy diagnosis in
Supratrochlear nerve Not thickened Nontender suspected patients with clinically atypical lesions, presenting
Infraorbital nerve Not thickened Nontender with negative baciloscopy and indecisive histopathology.[9]
Great auricular nerve Not thickened Nontender Diagnosis at an early stage is absolutely essential for earlier
Radial nerve Not thickened Nontender treatment to prevent leprosy‑related disabilities and its benefit
Ulnar nerve Grade 1 thickened Nontender for termination or control of infection transmission.[10]
Radiocutaneous nerve Not thickened Nontender
Median nerve Not thickened Nontender
Anterior cutaneous nerves of thigh Not thickened Nontender Conclusion
Common peroneal nerve Grade 1 thickened Nontender Thus, even today as we are trying hard to eradicate leprosy,
Anterior tibial nerve Not thickened Nontender newer forms of presentation continue to crop. In an
Posterior tibial nerve Not thickened Nontender endemic country like India, we still need to have an open
eye to recognize the varied manifestations of leprosy so
due to alteration in the immune status of these patients or the as to ensure prompt diagnosis and treatment, which can
excessive load of bacilli in these tissues. In tuberculoid pole, reduce the morbidity in potentially treatable patients. We
the major cause of lesional ulceration is Type 1 lepra reaction, present this case of lazarine leprosy on account of its rare
i.e., lazarine leprosy due to alteration in the immune status of occurrence and its association with anemia and superadded
the patient. In lepromatous pole, lesional ulceration is seen in infection along with the involvement of torso which is rare
lesions of erythema nodosum leprosum necroticans (Type 2 in lazarine leprosy.
lepra reaction) or rarely lazarine leprosy due to high bacillary Declaration of patient consent
load in the lesions. The authors certify that they have obtained all appropriate
Type 1 reaction is a delayed‑type of hypersensitivity, where patient consent forms. In the form, the patient has given his
the preexisting lesions become erythematous, edematous, and consent for his images and other clinical information to be
rarely ulcerate. This rare ulcerating type of Type 1 reaction reported in the journal. The patient understands that his name
is called lazarine leprosy. The exact pathogenic mechanism and initial will not be published, and due efforts will be made
of lazarine leprosy is unknown, but various factors have to conceal his identity, but anonymity cannot be guaranteed.
been implicated such as breakdown of local immunity, Financial support and sponsorship
increased proliferation of bacilli, and severe tissue edema.[4] Nil.
Protein malnutrition has been suggested to play a main role
in the pathogenesis of ulceration. [3] Protein malnutrition Conflicts of interest
leads to an enhanced susceptibility to secondary pathogens, There are no conflicts of interest.
such as streptococci and staphylococci, which results from
concomitant debilitation of humoral antibody mechanisms.[5] In References
few cases, lazarine leprosy has also been seen in BT Hansen’s 1. Lucio R, Alvarado I. Opusculo Sobre el Mal de San Lazaro o
disease without any malnutrition or immunosuppression.[6] Elephantiasis de Los Griegos. México: Murguía e Cia; 1852. p. 53.
In our patient, there was evidence of superadded bacterial 2. Pardo‑Castello V, Caballero GM. Lazarine leprosy: A peculiar
infection along with anemia but no other evidence of protein monosymptomatic form of leprosy. Arch Derm Syph 1931;23:1‑11.
3. Nanda S, Bansal S, Grover C, Garg V, Reddy BS. Lazarine
malnutrition or immunosuppression. leprosy‑revisited? Indian J Lepr 2004;76:351‑4.
In this form of leprosy, there are no localized skin infiltrations.[1] 4. Sunandini PA, Prasad PG, Chalam KV, Padmasri Y. Type 1 Lepra
Reaction With Ulceration (Lazarine Leprosy) Two interesting case
Frequent reaction episodes take place with scarlet spots which reports. IOSR‑JDMS 2015;14:22‑5.
later darken and ulcerate and usually heal with atrophic and 5. Skinsnes LK, Higa LH. The role of protein malnutrition in the
hypochromic scars with a thin hyperpigmented border as pathogenesis of ulcerative “Lazarine” leprosy. Int J Lepr Other
was seen in our patient.[7] The lesions spread in an upward Mycobact Dis 1976;44:346‑58.
6. Salafia A. Lazarine leprosy–revisited. Indian J Lepr 2005;77:182‑3.
direction, frequently involve extensor aspects of the feet, legs, 7. Letícia F, Macedo de SE, Letícia CM, Ferreira VP. Vasculonecrotic
hands, forearms, arms, and rarely on the face and torso.[8] In reactions in leprosy. Braz J Infect Dis 2007;11:378‑82.
our patient, however, the trunk was also involved. Tingling 8. Saúl A, Novales J. Lucio‑Latapí leprosy and the Lucio phenomenon.
of hands and feet, hypo‑ or anhidrosis, alopecia of eyelashes Acta Leprol 1983;1:115‑32.
9. Naaz F, Mohanty PS, Bansal AK, Kumar D, Gupta UD. Challenges
and eyebrows, smooth and rosy skin are also reported in these beyond elimination in leprosy. Int J Mycobacteriol 2017;6:222‑8.
patients.[1] Other clinical and systemic manifestations include 10. Govindharaj P, Srinivasan S, Darlong J. Perception toward the disease
saddle‑nose deformity; rhinitis; gastrointestinal, respiratory, of the people affected by leprosy. Int J Mycobacteriol 2018;7:247‑50.
International Journal of Mycobacteriology ¦ Volume 9 ¦ Issue 3 ¦ July-September 2020 331
You might also like
- Bon Ami Bakery CNY 2022Document27 pagesBon Ami Bakery CNY 2022irwan junNo ratings yet
- REJURANDocument13 pagesREJURANirwan junNo ratings yet
- Acne Fulminans Successfully Treated With CyclosporDocument3 pagesAcne Fulminans Successfully Treated With Cyclosporirwan junNo ratings yet
- Skin Immunity To Dermatophytes: From Experimental Infection Models To Human DiseaseDocument16 pagesSkin Immunity To Dermatophytes: From Experimental Infection Models To Human Diseaseirwan junNo ratings yet
- Acne Fulminans Successfully Treated With CyclosporDocument3 pagesAcne Fulminans Successfully Treated With Cyclosporirwan junNo ratings yet
- Reactive Perforating Leprosy: A Rare Case Report of Type 2 Leprosy ReactionDocument3 pagesReactive Perforating Leprosy: A Rare Case Report of Type 2 Leprosy Reactionirwan junNo ratings yet
- Pajk 20211117Document4 pagesPajk 20211117irwan junNo ratings yet
- Dermatologica Sinica: Pa-Fan Hsiao, Yang-Chih Lin, Cheng-Chieh Huang, Yu-Hung WuDocument5 pagesDermatologica Sinica: Pa-Fan Hsiao, Yang-Chih Lin, Cheng-Chieh Huang, Yu-Hung Wuirwan junNo ratings yet
- Crown Vessels and Shiny White Structures in Dermoscopy of HistoidDocument3 pagesCrown Vessels and Shiny White Structures in Dermoscopy of Histoidirwan junNo ratings yet
- Acne Fulminans Successfully Treated With CyclosporDocument3 pagesAcne Fulminans Successfully Treated With Cyclosporirwan junNo ratings yet
- Are We Witnessing A Paradigm Shift in Leprosy Two Atypical Presentations of HistoidDocument4 pagesAre We Witnessing A Paradigm Shift in Leprosy Two Atypical Presentations of Histoidirwan junNo ratings yet
- Hepatitis C Dan LucioDocument4 pagesHepatitis C Dan Lucioirwan junNo ratings yet
- Role of Peeling in HPIDocument8 pagesRole of Peeling in HPIirwan junNo ratings yet
- Acne Fulminans Successfully Treated With CyclosporDocument3 pagesAcne Fulminans Successfully Treated With Cyclosporirwan junNo ratings yet
- Late Leprosy Reaction Presenting As Erythema Multiforme Like ENLDocument3 pagesLate Leprosy Reaction Presenting As Erythema Multiforme Like ENLirwan junNo ratings yet
- Fractional CO2 Laser ComplicationsDocument6 pagesFractional CO2 Laser Complicationsirwan junNo ratings yet
- Probiotic CreamDocument8 pagesProbiotic Creamirwan junNo ratings yet
- A Practical Approach To Chemical PeelsDocument8 pagesA Practical Approach To Chemical Peelsleenatalia93100% (2)
- Topical Corticosteroid Effects on the Skin's Barrier FunctionDocument8 pagesTopical Corticosteroid Effects on the Skin's Barrier Functionirwan junNo ratings yet
- Morphea-Like Lesions After Botulinum Toxin A Injections: Ase SeriesDocument3 pagesMorphea-Like Lesions After Botulinum Toxin A Injections: Ase Seriesirwan junNo ratings yet
- Psoriasis TopicalDocument8 pagesPsoriasis Topicalirwan junNo ratings yet
- Update On Non-Melanoma PDFDocument18 pagesUpdate On Non-Melanoma PDFirwan junNo ratings yet
- Dyer - Postoperative Regimen - 1995Document6 pagesDyer - Postoperative Regimen - 1995irwan junNo ratings yet
- Morphea-Like Lesions After Botulinum Toxin A Injections: Ase SeriesDocument3 pagesMorphea-Like Lesions After Botulinum Toxin A Injections: Ase Seriesirwan junNo ratings yet
- BlefaroplastiDocument65 pagesBlefaroplastiirwan jun100% (1)
- Helicobacter in EczemaDocument8 pagesHelicobacter in Eczemairwan junNo ratings yet
- Esearch Letters: AY M CAD ErmatolDocument3 pagesEsearch Letters: AY M CAD Ermatolirwan junNo ratings yet
- Integrated Management of Childhood IllnessDocument23 pagesIntegrated Management of Childhood Illnessirwan junNo ratings yet
- HyaluronidaseDocument2 pagesHyaluronidaseirwan junNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- 2022 - Epidemiologia - Sifilis VIH en Homosexuales HombresDocument25 pages2022 - Epidemiologia - Sifilis VIH en Homosexuales HombresEduardo RodriguezNo ratings yet
- Hypotheses and Variables in Research StudiesDocument8 pagesHypotheses and Variables in Research StudiesvaninagarajanNo ratings yet
- Bagan KejangDocument10 pagesBagan KejangNie' MKNo ratings yet
- Entendimiento de Los Datos DisponiblesDocument10 pagesEntendimiento de Los Datos DisponiblesJose Miguel González PeraltaNo ratings yet
- Course Details - CHC32015 Certificate III in Community Services - Mark Oliphant CollegeDocument1 pageCourse Details - CHC32015 Certificate III in Community Services - Mark Oliphant CollegeSaroja ChhetriNo ratings yet
- MSQH 5th Editon Standards - 02 Final GS 17apr 2019Document99 pagesMSQH 5th Editon Standards - 02 Final GS 17apr 2019Aku NieNo ratings yet
- Epidemiological Characterization of Tibial Plateau FracturesDocument7 pagesEpidemiological Characterization of Tibial Plateau FracturesArmando RodriguezNo ratings yet
- Penitenciaria Estatal Oso Blanco Contaminacion 2013-29Document2 pagesPenitenciaria Estatal Oso Blanco Contaminacion 2013-29Emily RamosNo ratings yet
- Functions of A Student Head NurseDocument6 pagesFunctions of A Student Head NurseJan Ayenlieh Balandra Bertumen100% (1)
- Mitral Valve ProlapseDocument2 pagesMitral Valve ProlapseLena MarieNo ratings yet
- SWINE PROUCTION Lab Manual 4 5Document6 pagesSWINE PROUCTION Lab Manual 4 5Sasheen Ulgasan DulosNo ratings yet
- Kirk D. Strosahl, Patricia J. Robinson, Thomas Gustavsson Brief Interventions For Radical Change Principles and Practice of Focused Acceptance and Commitment Therapy PDFDocument297 pagesKirk D. Strosahl, Patricia J. Robinson, Thomas Gustavsson Brief Interventions For Radical Change Principles and Practice of Focused Acceptance and Commitment Therapy PDFebiznes100% (18)
- Quality Certificate CHEPDocument2 pagesQuality Certificate CHEPKumar RajadhyakshNo ratings yet
- Diagnosing and Classifying Vocal FaultsDocument27 pagesDiagnosing and Classifying Vocal FaultsSean Gabel82% (17)
- Febuxostat EMEADocument51 pagesFebuxostat EMEAIndra PaqotzNo ratings yet
- Violent Video GamesDocument7 pagesViolent Video Gamesapi-356126032No ratings yet
- Ely Mae Abunin Family Nursing Care Plan Poor Environmental SanitationDocument1 pageEly Mae Abunin Family Nursing Care Plan Poor Environmental SanitationJamie HaravataNo ratings yet
- Fact Sheet 11 - DebriefingDocument3 pagesFact Sheet 11 - Debriefingkhushi.avatharaNo ratings yet
- SurgiVet Advisor Tech Vital Signs MonitorDocument6 pagesSurgiVet Advisor Tech Vital Signs MonitorKihanNo ratings yet
- Social SkillsDocument55 pagesSocial SkillshandpamNo ratings yet
- ECG HISTORYDocument3 pagesECG HISTORYJanine Alicia VargasNo ratings yet
- ArticleDocument2 pagesArticleFemale Ruler Blue LoverNo ratings yet
- Botox QuotationDocument4 pagesBotox QuotationCatherine ZamudioNo ratings yet
- October 23, 2015 Strathmore TimesDocument28 pagesOctober 23, 2015 Strathmore TimesStrathmore TimesNo ratings yet
- Beatriz Echeverri ResumeDocument1 pageBeatriz Echeverri Resumeapi-436063355No ratings yet
- The Benefits of Water TherapyDocument5 pagesThe Benefits of Water TherapyJohn Paul CordovaNo ratings yet
- NEW ISLAMABAD INTERNATIONAL AIRPORT CHILLED WATER SYSTEM FLUSHINGDocument9 pagesNEW ISLAMABAD INTERNATIONAL AIRPORT CHILLED WATER SYSTEM FLUSHINGArslan ButtNo ratings yet
- Ati RN 2016 Mental HealthDocument6 pagesAti RN 2016 Mental HealthStan Tan0% (1)
- Preston Smith: EducationDocument1 pagePreston Smith: Educationapi-437394219No ratings yet
- Public Health Nutrition Career OptionsDocument2 pagesPublic Health Nutrition Career OptionsZaka RehmanNo ratings yet