Professional Documents
Culture Documents
Pembrolizumab in Microsatellite-Instability-High Advanced Colorectal Cancer JC
Pembrolizumab in Microsatellite-Instability-High Advanced Colorectal Cancer JC
Uploaded by
Yaram0 ratings0% found this document useful (0 votes)
17 views3 pagesThis document summarizes a study examining the use of pembrolizumab as a first-line treatment for microsatellite instability-high (MSI-H) advanced colorectal cancer compared to standard chemotherapy options. The study found that pembrolizumab had a longer progression-free survival of 16.5 months compared to 8.2 months for chemotherapy. Pembrolizumab also had fewer treatment-related adverse effects and better overall response rates than chemotherapy. Based on these results, pembrolizumab demonstrated superior outcomes to standard chemotherapy as a first-line treatment for MSI-H advanced colorectal cancer.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes a study examining the use of pembrolizumab as a first-line treatment for microsatellite instability-high (MSI-H) advanced colorectal cancer compared to standard chemotherapy options. The study found that pembrolizumab had a longer progression-free survival of 16.5 months compared to 8.2 months for chemotherapy. Pembrolizumab also had fewer treatment-related adverse effects and better overall response rates than chemotherapy. Based on these results, pembrolizumab demonstrated superior outcomes to standard chemotherapy as a first-line treatment for MSI-H advanced colorectal cancer.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
17 views3 pagesPembrolizumab in Microsatellite-Instability-High Advanced Colorectal Cancer JC
Pembrolizumab in Microsatellite-Instability-High Advanced Colorectal Cancer JC
Uploaded by
YaramThis document summarizes a study examining the use of pembrolizumab as a first-line treatment for microsatellite instability-high (MSI-H) advanced colorectal cancer compared to standard chemotherapy options. The study found that pembrolizumab had a longer progression-free survival of 16.5 months compared to 8.2 months for chemotherapy. Pembrolizumab also had fewer treatment-related adverse effects and better overall response rates than chemotherapy. Based on these results, pembrolizumab demonstrated superior outcomes to standard chemotherapy as a first-line treatment for MSI-H advanced colorectal cancer.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 3
Pembrolizumab in Microsatellite-Instability-High Advanced Colorectal Cancer Journal Club Summary
● MSI-H/dMMR Colorectal Cancer
○ CRC with presence of mismatch-repair deficiency (dMMR) → decrease response to traditional chemo and
high mutation burden
○ Colorectal cancer (CRC): most common cancer diagnosed in both men and women in the US
■ Lifetime risk for developing CRC ~4.3% and 4.0% for men and women, respectively
○ Risk factors for CRC: FH, sex (males), age, hx IBD, smoking, alcohol use, dietary factors, lack of
physical activity, obesity
● Guideline Recommendations for colorectal cancer (Cetuximab may be substituted for bevacizumab)
○ FOLFOX +/- Bevacizumab
■ Folinic acid
■ 5-fluorouracil
■ oxaliplatin
○ CAPEFOX +/- Bevacizumab
■ Capecitabine
■ Oxaliplatin
○ FOLFIRI +/- Bevacizumab
■ Folinic acid
■ 5-fluorouracil
■ Irinotecan
● Adding folinic acid (Leucovorin) to FOLFOX and FOLFIRI: Can enhance the binding of 5-FU to an enzyme
inside of the cancer cells, enhancing its effect.
● Pembrolizumab (Keytruda)
○ MOA:
■ Highly selective anti-PD1 monoclonal antibody that binds to/blocks PD1 receptor on T
cells
■ Inhibition of PD1 pathway between tumor cells and T-cells reverses T-cell suppression
and induces desired antitumor response
○ FDA Indication (Not currently approved for first line therapy)
■ Tx MSI-H-dMMR colorectal cancer in patients progressed following tx with
fluoropyrimidine, oxaliplatin, and irinotecan
○ Dosing:
■ 200mg IV Q 3 weeks or 400mg IV Q 6 weeks, depending on patient response
○ ADRs:
■ Fatigue, N/D, HA, decreased appetite, skin rash, pruritis, vitiligo, arthralgia, back pain,
hyperglycemia, hypertriglyceridemia, hyponatremia
Journal Club Article:
● Background: programmed death 1 (PD1) blockade has shown benefit in MSI-H or dMMR tumors AFTER
previous therapy, unclear about BEFORE
● Phase 3 randomized, multicenter, international, open-label
● 307 patients
● Tx options: pts randomly entered into these treatment groups
○ Pembrolizumab 200mg every 3 weeks
○ FOLFOX6
○ FOLFOX 6 + bevacizumab
○ FOLFOX + cetuximab
○ FOLFIRI
● Primary endpoints:
○ Progression free survival & overall survival
● Secondary endpoints:
○ Overall response & safety
● Inclusion:
○ >18 yrs old
○ Stage IV
○ ECOG stage 0-1
○ Adequate organ function
○ Prior chemo (completed >6 months prior to randomization)
○ dMMR
○ MSI-H
■ Local PCR analysis of 3-5 tumor analysis
● Study protocol:
○ Pts randomly assigned 1:1 ratio to Pembro or investigator’s choice of chemo
○ Regimens were repeated every 2 weeks (3 weeks for Pembro) up to max 35 treatments with
Pembro* (*or until disease progression, unacceptable tox, decision by physician, pt withdrawal)
○ Follow up: Every 9 weeks
● Statistical Analysis: Kaplan-meier (estimate PFS and duration of response), 2 interim analysis
● Baseline characteristics
○ Medium duration of treatment 11.1 months (Pembro) & 5.7 months (chemo group)
○ 57 pts completed all 35 treatments of Pembro
○ High percentage of pts who did not have prior systemic chemotherapy; point of this study is to look
at best first-line option for chemotherapy
● Endpoints:
○ Looked into if different patients responded better or worse; for most part, most patients responded
similarly
○ Primary endpoint:
■ PFS subgroup analysis: Overall majority of subgroups in pembro was superior to chemo
○ Secondary endpoint: Overall response and safety
■ Complete response:
● Pembro: 11.1% vs 3.9% in chemo
● Those that responded in Pembro group responded better than chemo group
■ Progressive disease:
● Pembro: 29.4% vs 12.3% in chemo
○ Duration of response:
■ Most patients had continued response with Pembro that there was no full data for it (need
to wait until final analysis) but in general, much higher than chemo
○ Safety Endpoints:
■ Grade 3 or higher events: 78% in chemotherapy, 56% in Pembro
■ D/C d/t ADE: Pembro 14%, chemo 12%
■ Infusion rxn: Pembro had higher incidence
● Limitations:
○ 59% either crossed over or recieved anti PD-1 therapy outside of the trial
○ No subgroup analysis of cross-over pts
● Conclusion
○ First-line pembro superior to standard of care
○ SIgnificance to Specialty Pharmacy:
■ Cost of therapy:
● every 3 weeks: $9,869.94
● Every 6 weeks: $19,739.88
■ Optum Specialty Pharmacy does not currently have access to pembrolizumab
■ Access is limited to select specialty pharmacies, infusion centers, cancer tx facilities
■ June 29, 2020 Pembrolizumab granted FDA-approval for first-line treatment of pts with
metastatic MSI-H dMMR CRC
● Clinical significance:
○ Follow up was 32.4 months; PFS was significantly longer with pembrolizumab vs chemotherapy
(16.5 vs 8.2 months)
○ Treatment related AEs significantly lower with pembrolizumab vs chemotherapy
○ Infusion reactions more common with pembrolizumab vs chemotherapy
You might also like
- Miasm AnalysisDocument6 pagesMiasm AnalysisSatyendra Rawat100% (1)
- Top Trials in Gastroenterology & HepatologyFrom EverandTop Trials in Gastroenterology & HepatologyRating: 4.5 out of 5 stars4.5/5 (7)
- Glioblastoma Multiforme (GBM) : Brandon Conley, Michael Dix, Tommy Driscoll, Martin Hoogendijk, Jimmy McmullenDocument34 pagesGlioblastoma Multiforme (GBM) : Brandon Conley, Michael Dix, Tommy Driscoll, Martin Hoogendijk, Jimmy McmullenSerena SpanoNo ratings yet
- ChemotherapyDocument102 pagesChemotherapyJoseph John K Pothanikat100% (1)
- Chemotherapy of Cancer...Document94 pagesChemotherapy of Cancer...Bob MuneneNo ratings yet
- Cardiac DysrhythmiasDocument54 pagesCardiac DysrhythmiasClark LlameraNo ratings yet
- Subinvolution of UterusDocument18 pagesSubinvolution of Uterusaparna100% (2)
- Genetic TestingDocument11 pagesGenetic TestingPriyanka Patel100% (2)
- Short Diagnosis Report: PatientDocument6 pagesShort Diagnosis Report: PatientCarmen JurcoaneNo ratings yet
- Clinical Biochemistry ReviewDocument10 pagesClinical Biochemistry Reviewyaykatai100% (2)
- Dr. Kessler'S Homeopathy Book: Polycrests and Other Remedies Index of DiseasesDocument375 pagesDr. Kessler'S Homeopathy Book: Polycrests and Other Remedies Index of DiseasesVishalNo ratings yet
- 1 Крок 1 ЛС KROK 2007 2017 English BiochemistryDocument480 pages1 Крок 1 ЛС KROK 2007 2017 English BiochemistryAbhani MøhitNo ratings yet
- NCPDocument9 pagesNCPTracy Camille EscobarNo ratings yet
- Tepotinib in Non-Small-Cell Lung Cancer With MET Exon 14 Skipping Mutations JCDocument4 pagesTepotinib in Non-Small-Cell Lung Cancer With MET Exon 14 Skipping Mutations JCYaramNo ratings yet
- Newest - Immunotherapy in Lung CancerDocument31 pagesNewest - Immunotherapy in Lung CancerwisgeorgekwokNo ratings yet
- Onco Remote Consultation Report - Patient Name - Patient ID - GBMDocument20 pagesOnco Remote Consultation Report - Patient Name - Patient ID - GBMSoham DattaNo ratings yet
- Pembrolizumab For EarlyDocument74 pagesPembrolizumab For EarlyKishoreChandraKoradaNo ratings yet
- CancerpainDocument35 pagesCancerpain駱品全No ratings yet
- Journal of Clinical Oncology Volume 32 Number 19 July 2014Document10 pagesJournal of Clinical Oncology Volume 32 Number 19 July 2014ivssonNo ratings yet
- Acetazolamide Journal Club JC 2Document24 pagesAcetazolamide Journal Club JC 2api-740259455No ratings yet
- Breast Cancer FinaleDocument30 pagesBreast Cancer Finaleخايزورا راهيمNo ratings yet
- Case Challenges in The Management of Recurrent or Metastatic Head and Neck Squamous Cell Carcinoma (HNSCC)Document15 pagesCase Challenges in The Management of Recurrent or Metastatic Head and Neck Squamous Cell Carcinoma (HNSCC)Dan NejNo ratings yet
- CINVDocument23 pagesCINVHesham IbrahimNo ratings yet
- Five-Year Outcomes With Pembrolizumab Vs Chemotherapy As First Line in NSCLCDocument7 pagesFive-Year Outcomes With Pembrolizumab Vs Chemotherapy As First Line in NSCLCVu Hong NamNo ratings yet
- Neoblade Trial Slides For NCRI Bladder Cancer MeetingDocument10 pagesNeoblade Trial Slides For NCRI Bladder Cancer MeetingProf_Nick_JamesNo ratings yet
- Europe Balkan Course 2018 Systemic Management of Pancreatic Cancer PopescuDocument64 pagesEurope Balkan Course 2018 Systemic Management of Pancreatic Cancer PopescuCripto MonedeNo ratings yet
- Role of Aprepitant in Chemotherapy Induced Nausea and VomitingDocument13 pagesRole of Aprepitant in Chemotherapy Induced Nausea and Vomitinganon_602767910No ratings yet
- Pembrolizumab Plus Pemetrexedplatinum For Metastatic Nonsquamous NSCLC KEYNOTE 189 Japan StudyDocument11 pagesPembrolizumab Plus Pemetrexedplatinum For Metastatic Nonsquamous NSCLC KEYNOTE 189 Japan StudyasdffdsaNo ratings yet
- Scnausea Protocol 1mar2012Document6 pagesScnausea Protocol 1mar2012Afra FitrianitaNo ratings yet
- GlofitamabDocument12 pagesGlofitamabsuperequsNo ratings yet
- Protocol Update Dec 2019Document13 pagesProtocol Update Dec 2019Aarzu ChoudharyNo ratings yet
- Chemo PT 2 PPT - Lecture 3 For Oncology Nursing CourseDocument36 pagesChemo PT 2 PPT - Lecture 3 For Oncology Nursing CourseOdey GodwinNo ratings yet
- Update in TNBCDocument54 pagesUpdate in TNBCAvinash TaleleNo ratings yet
- Male Breast Carcinoma: Yang Lu MS3 AUC School of MedicineDocument10 pagesMale Breast Carcinoma: Yang Lu MS3 AUC School of MedicineYang JunNo ratings yet
- Case Study PowerpoinrDocument30 pagesCase Study Powerpoinrapi-588508014No ratings yet
- L 105 PembrolizumabDocument5 pagesL 105 PembrolizumabgyulsizNo ratings yet
- Prostate Cancer: Presented To Dr. Fawad Rasool byDocument26 pagesProstate Cancer: Presented To Dr. Fawad Rasool byJunaid MalikNo ratings yet
- Metastatic Breast Disease: Presenter: DR Abdi Osman M. Supervisor: DR D. KiptoonDocument32 pagesMetastatic Breast Disease: Presenter: DR Abdi Osman M. Supervisor: DR D. KiptoonEsq. Nelson OduorNo ratings yet
- Neoadjuvant Chemoradiotherapy in Resectable and Borderline Resectable PDACDocument42 pagesNeoadjuvant Chemoradiotherapy in Resectable and Borderline Resectable PDACAkhil Thomas JacobNo ratings yet
- Five-Year Survival With Combined Nivolumab and Ipilimumab in Advanced MelanomaDocument12 pagesFive-Year Survival With Combined Nivolumab and Ipilimumab in Advanced MelanomaKomarudin JaelNo ratings yet
- Anticancer DrugsDocument57 pagesAnticancer Drugsn4pnjfk6rbNo ratings yet
- Bradley J Monk First Line Pembrolizumab ChemotherapyDocument9 pagesBradley J Monk First Line Pembrolizumab ChemotherapyRaúl DíazNo ratings yet
- Locally Advanced and Metastatic Breast Cancer CasesDocument38 pagesLocally Advanced and Metastatic Breast Cancer Casesnv5yy5ryd5No ratings yet
- Testicular Tumors Part4Document52 pagesTesticular Tumors Part4Ramesh ReddyNo ratings yet
- Erbitux MonotherapyDocument7 pagesErbitux MonotherapyMaulik PatelNo ratings yet
- Bimbingan PPDS Endokrin Prolaktinoma Slide 1-38Document19 pagesBimbingan PPDS Endokrin Prolaktinoma Slide 1-38T. Mirzal Safari Eva SofrizhaNo ratings yet
- TB Se Defiende BiopsiaDocument7 pagesTB Se Defiende Biopsiaouf81No ratings yet
- B7 PDFDocument13 pagesB7 PDFFernanda RibeiroNo ratings yet
- 7902-002 Investigators Meeting Material 08 Feb 2019Document39 pages7902-002 Investigators Meeting Material 08 Feb 2019FERNANDO BUSTAMANTE MORALESNo ratings yet
- Small Lung Cancer Oncological GuidelinesDocument120 pagesSmall Lung Cancer Oncological GuidelinesCharm TanyaNo ratings yet
- Pretomanid National Drug Monograph October 2021: FDA Approval InformationDocument8 pagesPretomanid National Drug Monograph October 2021: FDA Approval InformationAndi SuhriyanaNo ratings yet
- Monday KordeDocument19 pagesMonday KordeNational Press FoundationNo ratings yet
- Pembrolizumab in MSI-H DMMR Advanced Colorectal Cancer A New Standard of CareDocument3 pagesPembrolizumab in MSI-H DMMR Advanced Colorectal Cancer A New Standard of CareasdffdsaNo ratings yet
- Esophageal CancerDocument21 pagesEsophageal CancerYogesh ShindeNo ratings yet
- Webinanar Onko - JoglosemarDocument19 pagesWebinanar Onko - JoglosemarFerdinand SimanjuntakNo ratings yet
- Use of FET-PET in Glioblastoma: Journal Club May 4 2011Document41 pagesUse of FET-PET in Glioblastoma: Journal Club May 4 2011tienloNo ratings yet
- Rancangan Bentuk Sediaan Farmasi Compatibility ModeDocument18 pagesRancangan Bentuk Sediaan Farmasi Compatibility ModeNully Andaretha SugiantoNo ratings yet
- Conquer StudyDocument12 pagesConquer StudyRonald Alonso Méndez Borbón100% (1)
- Anticancer DrugsDocument5 pagesAnticancer DrugsSarithaRajeshNo ratings yet
- Journal Reading: By: Vera Septia Nalurita (2008730129) Preceptor: Dr. Bowo Wahyudi, SPKK Rsud Kota BanjarDocument17 pagesJournal Reading: By: Vera Septia Nalurita (2008730129) Preceptor: Dr. Bowo Wahyudi, SPKK Rsud Kota BanjarVera Septia NaluritaNo ratings yet
- Hypo - RT PC TrialDocument37 pagesHypo - RT PC TrialnitinNo ratings yet
- SiriusDocument10 pagesSiriusJLNo ratings yet
- Pheochromocytoma Towards An Audit of National Surgical PracticeDocument15 pagesPheochromocytoma Towards An Audit of National Surgical PracticedermoNo ratings yet
- Clinical Pharmacology (Clark's Clinical Medicine 9th Ed (2017) - 2)Document38 pagesClinical Pharmacology (Clark's Clinical Medicine 9th Ed (2017) - 2)Rosulescu IonNo ratings yet
- Breast Cancer Notes Part 2Document60 pagesBreast Cancer Notes Part 2Tony YongNo ratings yet
- Itp 2021Document64 pagesItp 2021Victoria MalakNo ratings yet
- Chemotherapy For H&N SCC Past, Present and Future: Charles Gawthrop M.D. Jason Newman M.DDocument71 pagesChemotherapy For H&N SCC Past, Present and Future: Charles Gawthrop M.D. Jason Newman M.DgauravNo ratings yet
- Cancer of The EsophagusDocument6 pagesCancer of The EsophagusDileep SrinivasanNo ratings yet
- A Simple Guide to Pheochromocytoma (Updated), Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Pheochromocytoma (Updated), Diagnosis, Treatment and Related ConditionsNo ratings yet
- Kiniksa Rilonacept In-ServiceDocument2 pagesKiniksa Rilonacept In-ServiceYaramNo ratings yet
- Umbralisib in Patients With CLL Who Are Intolerant To Prior BTK or PI3K-delta Inhibitor TherapyDocument3 pagesUmbralisib in Patients With CLL Who Are Intolerant To Prior BTK or PI3K-delta Inhibitor TherapyYaramNo ratings yet
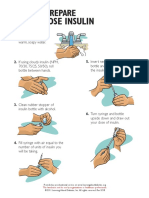
- Mixed Dose Insulin: How To PrepareDocument1 pageMixed Dose Insulin: How To PrepareYaramNo ratings yet
- How To Use: MDI Closed MouthDocument1 pageHow To Use: MDI Closed MouthYaramNo ratings yet
- Single Dose Insulin: How To PrepareDocument1 pageSingle Dose Insulin: How To PrepareYaramNo ratings yet
- Treatments: - No Treatment Has Been Proven To Cure or Delay The Progression of ADDocument6 pagesTreatments: - No Treatment Has Been Proven To Cure or Delay The Progression of ADYaramNo ratings yet
- BloodGlucosMetters ENGLISHDocument1 pageBloodGlucosMetters ENGLISHYaramNo ratings yet
- Questions To Answer: Difference Best Brand To Buy? Is It Worth Taking Any or All of These?Document5 pagesQuestions To Answer: Difference Best Brand To Buy? Is It Worth Taking Any or All of These?YaramNo ratings yet
- Iba Dose Contraints Poster Rev2 0522Document1 pageIba Dose Contraints Poster Rev2 0522Harpreet sainiNo ratings yet
- Encephalopathy - Wikipedia,..Document3 pagesEncephalopathy - Wikipedia,..aristianaNo ratings yet
- BakteriDocument8 pagesBakteriAgus SugiartoNo ratings yet
- Крок 2 англ.Document40 pagesКрок 2 англ.Rahul PatilNo ratings yet
- Reviewer For OediaDocument19 pagesReviewer For Oedias9crhvrymhNo ratings yet
- Warm Sponge and Tepid SpongeDocument1 pageWarm Sponge and Tepid SpongeAulya FahnidaNo ratings yet
- Comparison of Rheumatoid and OsteoarthritisDocument4 pagesComparison of Rheumatoid and OsteoarthritisWaseem Khan AfridiNo ratings yet
- Intrauterine Fetal DemiseDocument7 pagesIntrauterine Fetal DemiseElaisa Mae Delos SantosNo ratings yet
- Mauritius Government GazetteDocument2 pagesMauritius Government GazetteAmrit ChutoorgoonNo ratings yet
- Bullous Disease of The Skin, Acantholytic Bullous Disease (Darier's Disease, Keratosis Follicularis), M 15, Scalp, NeckDocument3 pagesBullous Disease of The Skin, Acantholytic Bullous Disease (Darier's Disease, Keratosis Follicularis), M 15, Scalp, NeckDeba P SarmaNo ratings yet
- Oet Writing Sample 01 EnglishDocument52 pagesOet Writing Sample 01 EnglishMuhammad Ahmad RazaNo ratings yet
- Water RelatedDocument15 pagesWater RelatedMix Content789No ratings yet
- IgG4 Related DiseaseDocument13 pagesIgG4 Related DiseaseLaura Paola Urquizo100% (1)
- HypophysectomyDocument19 pagesHypophysectomyjoel david knda mj100% (1)
- 12 Congenital Lesions of Larynx and Evaluation of StridorDocument77 pages12 Congenital Lesions of Larynx and Evaluation of StridorAbhishek ShahNo ratings yet
- Nursing CS BurnsDocument1 pageNursing CS BurnsBai Jannah Sahida SilonganNo ratings yet
- Intestinal ObstructionDocument6 pagesIntestinal ObstructionCling Cruza0% (1)
- Bird Flu (Avian Influenza)Document6 pagesBird Flu (Avian Influenza)JagadeeshTJNo ratings yet
- Case Presentation Meningitis 1Document17 pagesCase Presentation Meningitis 1chaudharitrushar007No ratings yet
- Determinantes de La Salud La Importancia de Promover Estilos de Vida ActivosDocument10 pagesDeterminantes de La Salud La Importancia de Promover Estilos de Vida ActivosSolange Jessica Perez CastroNo ratings yet
- Scientific Programme 20-1-2021Document15 pagesScientific Programme 20-1-2021Zohra FarooqNo ratings yet