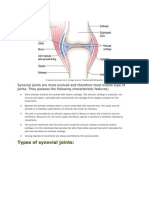
Professional Documents
Culture Documents
Tratamento Estético Das Veias
Tratamento Estético Das Veias
Uploaded by
NatháliaSouzaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Tratamento Estético Das Veias
Tratamento Estético Das Veias
Uploaded by
NatháliaSouzaCopyright:
Available Formats
Featured Operative Technique
Aesthetic Treatment of Leg Veins
Victoria A. Vitale-Lewis, MD
The author’s preferred treatment for spider veins is sclerotherapy, a technique that uses irritants to obliterate
the vessel lumen. She reserves laser treatment for vessels too small to sclerose, matting, and patients who
refuse sclerotherapy. Treatment is initiated only after ruling out reflux in the larger superficial venous systems
or through the perforators. For long lasting and satisfying results, the author recommends multiple treatments,
using the lowest concentration of the most effective sclerosant to achieve vessel obliteration with minimal
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
thrombus formation. She presents a guide to pretreatment evaluation, sclerosing solutions, injection tech-
nique, and posttreatment care. (Aesthetic Surg J 2008;28:573–583.)
T
he key to success in the aesthetic treatment of leg ed vein close to the saphenofemoral junction upon exam-
veins is identification and control of the source of ination of her thigh (Figure 3A). The Doppler probe was
venous reflux. Unsightly cosmetic leg veins or placed just below the saphenofemoral junction and, on
“spider veins,” distinguished from varicose veins on the release of distal compression, augmentation of the
basis of size, include telangiectasias, or fine red spider Doppler signal for longer than 1 second was heard, indi-
veins (<1 mm); venulectasias, or slightly larger, bluish cating reflux. This finding was confirmed by augmenta-
spider veins (<2 mm); and reticular veins (2 to 4 mm; tion of the signal with proximal compression applied by a
Figure 1). The larger leg veins, including the saphenous valsalva maneuver (Figure 3B).
veins and their tributaries, become varicose as the result A physician who is reluctant to use the Doppler ultra-
of significant venous reflux. The treatment of venous sound as a screening tool may simply order a duplex
reflux is considered medically necessary compared with scan to rule out significant venous reflux (in patients in
the treatment of spider veins, which is viewed as purely whom physical examination raises this issue). Duplex
aesthetic. venous imaging provides not only an audio but also a
visual picture of reflux. This software is now available
PREOPERATIVE EVALUATION on a laptop computer and is routinely used by phlebolo-
Reflux in the larger superficial venous systems or gists who treat significant venous reflux.
through the perforators must be ruled out (or treated) A patient with significant venous reflux in the saphe-
before treating spider veins. Usually, reflux can be nous systems, including tributaries or nonsaphenous
assessed by simple circumferential clinical examination varicose veins, is referred to a vascular surgeon for
of the entire leg, ruling out the presence of bulging vari- endovenous ablation with either radiofrequency or laser
cosities, especially along the paths of the long and short or ambulatory phlebectomy. Treatment of significant
saphenous veins, their major tributaries, and the sites of reflux in these larger veins, while providing a cosmetic
the common perforators (Figure 2). Once it is deter- benefit to patients, is considered medically necessary.
mined that the problem is limited to cosmetic spider Once significant reflux is ruled out, treatment of the
veins, no further testing is required.1 cosmetic spider veins—consisting of reticular veins,
If, on physical examination, a question of significant venulectasias, and telangiectasias—is initiated. Treat-
venous reflux arises, noninvasive venous testing is indi- ment depends on the diameter of the vessel; however,
cated. Doppler ultrasound is useful as a screening tool in typically, different diameters of veins occur together in
patients that demonstrate questionable reflux on clinical the same cluster (Figure 4). In fact, this association of
exam. In a study evaluating veins that appeared appro- reticular veins with spider veins has been studied and it
priate for cosmetic treatment, 22% of patients with spi- has been shown that 88% of patients with thigh telang-
der veins were found to have superficial venous iectasias had incompetent reticular veins on Doppler
incompetency, usually in the long saphenous system.2 ultrasound and 89% on duplex scanning.3,4
One such patient complained of a patch of spider
veins on the calf, but was actually found to have a dilat- SCLEROTHERAPY
The goal of the treatment is complete obliteration of
the vessel lumen. My initial approach to treatment is
Dr. Vitale-Lewis is in private practice in Melbourne, FL. sclerotherapy.
Aesthetic Surgery Journal Volume 28 • Number 5 • September/October 2008 • 573
Characteristics of Leg and Thigh Veins
Spider Veins
Telangiectasias < 1 mm - fine and red in color
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
Venulectasias < 2 mm - larger and purple in color
Reticular veins 2-4 mm
Larger Leg Varices
Medical/surgical treatment required
Illustrations by
William M. Winn,
Atlanta, GA
Figure 1. Classification of veins based on size. Spider veins include (A) telangiectasias or fine red spider veins <1 mm; (B) venulectasias slightly
larger, bluish spider veins < 2 mm, and (C) reticular veins 2 to 4 mm. The larger varicose veins (D)—including the saphenous veins and their tribu-
taries, if present—require treatment that is usually considered medically necessary, performed before treatment of the cosmetic spider veins.
Polidocanol United States from compounding pharmacies. BioForm
Choosing a sclerosing agent may be complicated by the Medical (San Mateo, CA) has now licensed United States
fact that these agents tend to enter and leave the market. rights to Aethoxysklerol, a sclerosing agent containing
My favorite sclerosing agent is polidocanol, which is not polidocanol, which is commonly used in Europe. I
approved by the US Food and Drug Administration believe this agent deserves some consideration if it once
(FDA) but could, until recently, be obtained in the again becomes available. It is classified by its mecha-
574 • Volume 28 • Number 5 • September/October 2008 Aesthetic Surgery Journal
A Superficial Superficial
epigastric v. epigastric v.
B Superficial
Superficial Superficial circumflex iliac v.
circumflex external
iliac v. pudental v.
Anteriolateral v.
Long saphenous v.
Anteriolateral v.
Posterior medial v.
Hunter perforator
Boyd perforator Long saphenous v.
Anterior malleolar v.
Anterior malleolar v.
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
Posterior malleolar v.
Cockett’s perforating v.
C
Dorsal venous arch
Connection
to posterio- Saphenopopliteal
medial v. junction
Intrasaphenous v. Short saphenous v.
Paraperoneal perforator
Figure 2. Physical circumferential examination of the entire lower extremity—especially along the paths of the long (A, B) and short (C) saphenous
vein, their major tributaries, and the sites of the common perforators—must be performed to rule out the presence of varicose veins.
nism of action as a detergent and is weaker than the oth- Because of the current unavailability of polidocanol,
er commonly used detergent approved by the FDA, sodi- and based on a study in Europe showing that chromated
um tetradecyl sulfate (STS). glycerin is superior to polidocanol for sclerotherapy of
Basically, all sclerosing agents are irritants that injure leg telangiectasias,7 I have recently begun using glycerin
the endothelial surfaces, resulting in obliteration of the for sclerotherapy of the very small telangiectasias (<1.0
vessel lumen (Figure 5).5 Polidocanol has been widely mm in diameter). Glycerin is available in a 72% concen-
used for sclerotherapy of spider veins in concentrations tration in the United States from compounding pharma-
of 0.25% to 0.75%. The concentration I have most com- cies because glycerin is used in cerebral edema and
monly used is the 0.5% solution (Table 1). If a patient acute glaucoma. It has been shown to be as effective as
has a significant number of larger spider veins, including chromated glycerin, which is more widely used in
reticular veins, then at the first treatment, I may use a Europe.8 I dilute the 72% glycerin 2:1 with 1% xylocaine
0.75% solution in these larger spider veins or increase with epinephrine to decrease its viscosity and pain on
the efficacy of the 0.5% solution by foaming, which I injection (Table 1).
will discuss. The maximum daily dose of polidocanol is
2 mg per kg of body weight. This dose is equivalent to Sodium Tetradecyl Sulfate
28 mL of a 0.5% solution in a 70-kg person, which well STS is approved by the FDA and has been used as a scle-
exceeds the usual amount that would be required in a rosing detergent since the 1940s (except for the period
single treatment session, even in the case of extensive from 2000 to 2002 when its manufacture was discontin-
spider vein involvement.6 ued). However, be mindful that STS is a stronger deter-
Aesthetic Treatment of Leg Veins Volume 28 • Number 5 • September/October 2008 • 575
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
A
Figure 3. A, This patient has clinical findings suggestive of reflux at
the saphenofemoral junction. B, The patient is undergoing Doppler
ultrasound screening for reflux at the saphenofemoral junction. With
the probe placed just below the saphenofemoral junction, a loud sig-
nal, audible for longer than a second on release of distal compres- B
sion, is indicative of reflux.
gent than polidocanol and carries an increased risk of with tiny bubbles (Figure 6). The bubbles of the lipid
adverse sequelae, such as hyperpigmentation and telang- micelles provide a larger surface area of contact with the
iectatic matting.9 STS in concentrations of 0.1% to endothelium, thus increasing the sclerosing efficacy of
0.15% can be used for sclerotherapy of telangiectasias the detergent. Foaming also increases effectiveness by
less than 1 mm in diameter as an alternative to the 72% inducing vasospasm of the injected vessel so that there
glycerin diluted 2:1 (if the use of only one agent is is less backflow of blood and dilution of the agent before
desired). For vessels 1 to 3 mm in size, I recommend it can have its sclerosing effect. Because foaming
0.15% to 0.25% foamed STS solution and 0.25% to increases the effectiveness of the sclerosing agent, it
0.5% foamed solution for 3- to 6-mm veins (Table 1). allows for lower concentrations to be used.
The maximum amount that can be injected at a single
treatment session is 10 mL of a 3% solution which, at Preparation
the low concentrations used for treating spider veins, Patients usually require 3 30-minute sclerotherapy ses-
would rarely be approached in a single session. sions at 4- to 6-week intervals. This time interval
between sessions is optimal for the sclerosant effect to
Foaming With Air accomplish vessel obliteration. The patient is instructed
In patients undergoing sclerotherapy of venulectasias to avoid applying leg creams on the day of the procedure
and reticular veins, the efficacy of the detergent can be and to purchase and bring with them 10 to 20 mm Hg
increased by foaming with air. A 3-mL syringe filled with graduated compression pantyhose. Photographic docu-
0.25 mL of detergent is attached to a second 3-mL mentation of the spider veins is mandatory before treat-
syringe filled with 1.25 mL of air, using a double or 3- ment. It is difficult to standardize photographic views
way stopcock. The amount of air in the syringe is impor- because the number and locations of the spider veins
tant because the ratio of gas to air is ideally 4:1 to 5:1. vary among patients. However, inclusion of a recogniza-
The sclerosant is then pushed between the 2 syringes ble joint, such as a portion of knee or ankle, helps in ori-
several times until the detergent appears as white foam enting the image for later postoperative comparison.
576 • Volume 28 • Number 5 • September/October 2008 Aesthetic Surgery Journal
Telangiectasias
Venulectasias
Reticular vein
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
B C
Figure 4. A, Common arborizing pattern of spider veins with feeding reticular vein and branching
venulectasias and fine telangiectasias. B, Typical lateral thigh cartwheel pattern with feeding reticular
vein. C, Typical cluster of spider veins including telangiectasias, venulectasias, and reticular vein.
Sclerosing agent
Vein wall
Endothelium
Endothelial damage
Endofibrosis with
obliteration of lumen
Figure 5. All sclerosing agents damage the endothelial surfaces, causing fibrosis, which results in the
obliteration of the vessel lumen.
Aesthetic Treatment of Leg Veins Volume 28 • Number 5 • September/October 2008 • 577
Table 1. Most commonly used dilutions for sclerotherapy
solutions
Polidocanol usually diluted for injection in a 30-mL vial of 0.9%
sodium chloride
Preparation 1: 0.5% Polidocanol
5 mL 3% Polidocanol
25 mL 0.9% sodium chloride (for injection)
Preparation 2: 0.75% Polidocanol
7.5 mL 3% Polidocanol
22.5 mL 0.9% sodium chloride (for injection)
72% glycerin (usually diluted for injection in 3-mL syringes)
Diluted 2:1:
1 mL 72% glycerin.
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
0.5 mL 1% xylocaine with epinephrine
Figure 6. The detergent is foamed to increase efficacy. One 3-mL
STS (usually diluted for injection in a 30-mL vial of 0.9% sodium syringe is filled with 0.25 mL of 0.5% polidocanol, and the second 3-
chloride) mL syringe is filled with 1.25 mL of air. Pushing the sclerosant
between the 2 syringes several times foams the detergent with a gas
Preparation 1: 0.15% STS to liquid ratio of 5:1, appearing as white foam with tiny bubbles.
1 mL 3% STS
19 mL 0.9% sodium chloride (for injection)
Preparation 2: 0.25% STS in the deeper reticular veins where the depth is less
2 mL 3% STS obvious than the more superficial spider veins. Using
22 mL 0.9% sodium chloride (for injection) low injection pressure and stopping the injection at a
Preparation 3: 0.5% STS particular site when a 1 to 2 cm area is empty of blood
4 mL 3% STS are recommended techniques. Continuing the injection
20 mL 0.9% sodium chloride (for injection) beyond this point is likely to increase the incidence of
extravasation and telangiectatic matting.10 Injections
STS = sodium tetradecyl sulfate. are limited to 0.5 mL of the sclerosant at any one site
for the same reason.
If a wheal starts to develop at the injection site as
INJECTIONS the sclerosant is injected, indicating extravasation, then
Injections are performed with the patient in the supine I abort the injection at that site and digitally compress
position. The legs are prepped with alcohol, which is the injection site. This will dilute the extravasated scle-
used not only as an antiseptic, but also to improve rosant by diffusion and, hopefully, avert significant
visualization of the veins by changing the index of skin injury to the skin. Only if there is a significant extrava-
refraction. Optimal lighting and magnification are need- sation would I inject a solution of 75 units of
ed. Several different types of transillumination lighting hyaluronidase in 3 mL of saline.11 One of the reasons I
are available to facilitate visualizing the vessels, partic- prefer polidocanol is that the chance of inducing signif-
ularly the reticular veins. icant necrosis on extravasation is minimal when 0.5%
The injections are performed with 30 gauge 0.5-inch to 0.75% concentrations are used. For very tiny telang-
disposable needles and 3-mL syringes. The needle is iectasias, 72% glycerin in a 2:1 dilution with lidocaine
bent to a 30° to 45° angle so that it is parallel to the has become popular because it is even more innocuous
skin upon entry. Also, the bevel of the needle is turned upon extravasation, which is difficult to avoid with
upward so that the needle may sometimes actually be these very tiny vessels.8 In most cases of missing a
seen in the lumen of the spider vein (Figure 7). The 3- lumen on injection, the needle is deep to the vein.
mL syringes are filled with only 1 to 1.5 mL of the scle- Maintaining digital pressure on this failed site, I would
rosant so that the syringe can be held and the plunger select a second injection site into the spider vein, mak-
pushed with the same hand, freeing the opposite hand ing sure that the needle is properly bent and as parallel
for retraction of the skin. The site of entry into the spi- to the skin as possible in order to ensure more superfi-
der vein is at the source of the reflux if identifiable. A cial placement. The procedure can be tedious, but per-
feeding reticular vein, if present, is sclerosed first severance is necessary for a good result.
(Figure 8). Along a reticular vein, 0.5 mL of sclerosant Cotton balls and tape are applied to the injection
is injected at 5.0-cm intervals. The skin is punctured sites as the treatment progresses. This provides com-
approximately 1 mm from the desired location of entry pression and hides the hyperemic reaction in the scle-
into the spider vein. The needle is then guided into the rosed spider vein that develops 30 seconds after the
spider vein with a gentle but bold puncture. It is not sclerotherapy, which can be perceived by the patient as
necessary or productive to obtain a blood return except persistence of the spider vein (Figure 9).
578 • Volume 28 • Number 5 • September/October 2008 Aesthetic Surgery Journal
Digital pressure on pre-
vious injection site
Low injection pressure
30-45 angle
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
Skin
1-2 cm area emptied of blood
Fat
Sclerosing agent
< 0.5mL at each site
30 gauge 1/2⬙ needle, bevel up
(facing toward skin)
Figure 7. A, The injections are performed with 30-gauge half-inch disposable needles and 3-mL syringes filled with only 1 to 1.5 mL of the scle-
rosant. The needle is bent at a 30° to 45° angle, to be parallel to the skin, with the bevel turned upward. Digital pressure is applied at the previ-
ous injection site. B, Using low injection pressure, injecting less than 0.5 mL at each site, and stopping the injection when a 1 to 2 cm area is
empty of blood are recommended techniques to decrease the incidence of extravasation and telangiectatic matting.
1. Proper hand position for traction
2. Inject reticular vein first at 5 cm
intervals
Figure 8. Proper position of the hands, syringe, and needle for injection with optimal retraction. The syringe is half-full, the
needle is bent, and the bevel faces upward. If the reticular vein is present, inject it first at 5.0-cm intervals.
Aesthetic Treatment of Leg Veins Volume 28 • Number 5 • September/October 2008 • 579
A B
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
Figure 9. A, Pretreatment view. B, Posttreatment view about 30 seconds after the initial blanching—as the vein is cleared of blood, an intense
hyperemic reaction develops.
A B C
Figure 10. Evacuation of microthrombi, if present, 1 week following sclerotherapy, is recommended to decrease the incidence of adverse seque-
lae, including hyperpigmentation and telangiectatic matting. Microthrombi appear as ink-like deposits in the vein. A, The skin is punctured over
the microthrombus with a 25-gauge needle. B, The liquefied coagulum is expressed. C, Typical appearance of the removed clot. A few other
thrombi still required declotting.
POSTOPERATIVE MANAGEMENT
is the ideal degree of compression.14,16 I have found my
Compression patients to be noncompliant with this higher degree of
When treatment is completed, 10- to 20-mm Hg graduated graduated compression stockings.
compression stockings are applied before the patient
hangs their legs downward to minimize the backflow of Ambulation
blood. The patient is instructed to wear the support hose The patient is encouraged to walk posttreatment to avoid
for a minimum of 72 hours. There is debate in the litera- deep vein thrombosis which, although exceedingly rare,
ture about the effectiveness of compression and the opti- has been reported in 2 patients following sclerotherapy
mal degree of compression and length of compression of spider veins.17,18
time.12-14 I advise the patient that continuous wear for 3
weeks provides less chance of adverse sequelae than 3 Follow-Up Care
days of wear with even less chance of adverse sequelae if Hyperpigmentation and telangiectatic matting are two of
worn for 6 weeks.15 Based on the 2007 study by Kern,12 the most common adverse sequelae following sclerother-
many practitioners are recommending 20-mm Hg graduat- apy. The goal of the treatment is successful obliteration
ed compression stockings for 3 weeks postsclerotherapy. of the vessel lumen with minimal thrombus formation.
However, other practitioners believe that 30- to 40-mm Hg A higher incidence of the most common adverse seque-
580 • Volume 28 • Number 5 • September/October 2008 Aesthetic Surgery Journal
occur over 24 months.21-23 I recommend a topical agent
for the treatment of hyperpigmentation, Hiruval-35
(Vimex Pharma), which may be effective in decreasing
the hemosiderin deposits that are the primary cause of
postsclerotherapy hyperpigmentation. Minocycline should
be discontinued during the course of sclerotherapy to
avoid minocycline-aggravated postsclerotherapy pigmen-
tation, which may persist for years.24 I have not used the
Q-switched ruby laser or weekly subcutaneous injections
with deferoxamine mesylate, both of which have been
suggested in the literature for treatment of postscle-
rotherapy hyperpigmentation.25,26
If matting occurs, I first check and sclerose any previ-
ously unidentified sources of reflux, such as a feeding
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
reticular vein (Figure 11). Once the source of the reflux
is controlled, the matting usually will fade. The matting
itself may be sclerosed with 0.25% polidocanol or 72%
glycerin diluted 2:1, but it will require many treatments.
If treatment is unsuccessful, I would then resort to laser
treatments with a potassium titanyl phosphate or
pulsed-dye laser.
LASER
I reserve use of the laser for 3 indications: (1) cleanup
after sclerotherapy for vessels too small to sclerose, (2)
matting, and (3) a patient who refuses sclerotherapy.
Patients who fear injection pain need to be told that the
laser is not painless, especially if they have larger blue
spider veins. Although a variety of vascular lasers have
been used in the past, the 1064-nm Nd:YAG laser is
presently the most widely used, especially for vessels
Figure 11. Demonstrates telangiectatic matting around a previously
sclerosed spider vein. It is recommended to look for and sclerose any greater than 1 mm in diameter and depth.27 In general,
previously unidentified sources of reflux, such as a feeding reticular spider veins of less than 1 to 4 mm respond best to spot
vein. Following this, the matting will usually fade. sizes of 2.5 to 6.0 mm with fluences of 100 to 22 J/cm2
and pulse durations of 20 to 60 ms, using larger spot
lae is felt to occur following excess thrombus forma- sizes, lower fluences, and longer pulse durations for the
tion.19,20 I see patients 1 week posttreatment, at which larger vessels; and smaller spot sizes, higher fluences
time any coagulum is liquefied, making evacuation pos- and shorter pulse durations for the smaller vessels. 28 In
sible. Microthrombi appear as ink-like deposits in the some instances 2 passes over the vessel may be needed
vein. If there are any such areas seen, I puncture the for closure. Although some practitioners believe that
skin using a 25-gauge needle and express the clot laser treatment is just as successful as sclerotherapy in
(Figure 10). If hyperpigmentation develops, I reassure the obliteration of spider veins,29 I agree with the major-
the patient that substantial lightening usually occurs in ity of practitioners who have had better clinical success
the first 6 months, although gradual lightening will with sclerotherapy than laser treatments.30, 31
A B C
Figure 12. A, Pretreatment view of a 52-year-old woman. B, Posttreatment view 2.5 years following 3 sclerotherapy treatments with 0.5% sodium
tetradecyl sulfate. C, Posttreatment view after 10 years.
Aesthetic Treatment of Leg Veins Volume 28 • Number 5 • September/October 2008 • 581
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
A B
Figure 13. A, Pretreatment view of a 62-year-old woman. B, Posttreatment view 6 months following 2 sclerotherapy treatments with 0.5%
polidocanol.
A B
Figure 14. A, Pretreatment view of a 46-year-old woman. B, Posttreatment view 1 year following 3 sclerotherapy treatments with 0.5% polidocanol.
582 • Volume 28 • Number 5 • September/October 2008 Aesthetic Surgery Journal
CONCLUSIONS 18. Reid RG, Rothnie MG. Treatment of varicose veins by compression scle-
rotherapy. Br J Surg 1968;55:889–895.
Successful treatment of leg veins, whether by laser or 19. Orbach EJ. Hazards of sclerotherapy of varicose veins—Their preven-
sclerotherapy, requires the identification and treatment tion and treatment of complications. Vasa 1979;8:170–173.
of the highest point of reflux. Multiple treatments using 20. Goldman MP, Bennett RG. Treatment of telangiectasias: A review. J Am
Acad Dermatol 1987;17:167–182.
the lowest concentration of the most effective sclerosant
21. Goldman MP, Kaplan RP, Duffy DM. Post-sclerotherapy hyperpigmenta-
to achieve vessel obliteration with minimal thrombus tion: A histological evaluation. J Dermatol Surg Oncol 1987;13:547–550.
formation will lead to long-lasting and satisfying results 22. Goldman PM. Sclerotherapy of superficial veins and telangiectasias of
(Figures 12 to 14). The current available option of 2 the lower extremities. Dermatol Clin 1987;5:369–379.
treatment modalities, sclerotherapy and laser, or a com- 23. Georgiev M. Post-sclerotherapy hyperpigmentations: A 1-year follow-
up. J Dermatol Surg Oncol 1990;16:608–610.
bination of both, can help to achieve even greater suc-
24. Green D. Persistent post-sclerotherapy pigmentation due to minocy-
cess and satisfy more patients. ◗ cline: Three cases and a review of post-sclerotherapy pigmentation. J
Cosmet Dermatol 2002;1:173–182.
DISCLOSURES 25. Tafazzoli A, Rostan EF, Goldman MP. Q-switched ruby laser treatment
for post- sclerotherapy hyperpigmentation. Dermatol Surg
Downloaded from https://academic.oup.com/asj/article-abstract/28/5/573/203135 by guest on 05 June 2020
The author has no financial interest in and receives no compensa- 2000;26:653–656.
tion from the manufacturers of products mentioned in this article. 26. Lopez L, Dilley RB, Henriquez JA. Cutaneous hyperpigmentation fol-
lowing venous sclerotherapy treated with deferoxamine mesylate.
REFERENCES Dermatol Surg 2001;27:795–798.
1. Goldman MP, Fornek A. Anatomy and pathophysiology of varicose 27. Kauvar A, Khrom T. Laser treatment of leg veins. Semin Cutan Med
veins. J Dermatol Surg Oncol 1989;15:138–145. Surg 2005;24:184–192.
2. Thibault PK, Louis WA. Recurrent varicose veins part I: Evaluation uti- 28. Bäumler W, Ulrich H, Hartl A, Landthaler M, Shafirstein G. Optimal
lizing duplex venous imaging. J Dermatol Surg Oncol 1992;18:618–624. parameters for the treatment of leg veins using Nd:YAG lasers at 1064
3. Weiss RA, Weiss MA. Doppler ultrasound findings in reticular veins of nm. Br J Dermatol 2006;155:364–371.
the thigh subdermic lateral venous system and implications for scle- 29. Levy JL, Elbahr C, Jouve E, Mordon S. Comparison and sequential
rotherapy. J Dermatol Surg Oncol 1993;19:947–951. study of long-pulsed Nd:YAG 1064 nm and sclerotherapy in leg telang-
4. Somjen GM, Ziegenbein R, Johnston AH, Royle JP. Anatomical exami- iectasias treatment. Laser Surg Med 2004;34:273–276.
nation of leg telangiectasias with duplex scanning. J Dermatol Surg 30. Lupton JR, Alster TS, Romero P. Clinical comparison of sclerotherapy
Oncol 1993;19:940–945. versus long-pulsed Nd:YAG laser treatment for lower extremity telang-
5. Ochsner A, Garside E. The intravenous injection of sclerosing sub- iectasias. Dermatol Surg 2002;28:694–697.
stances: Experimental comparative studies of changes in the vessels. 31. Goldman M. Lasers and sclerotherapy of leg veins: My perspective on
Ann Surg 1932;96:691–718. treatment outcomes. Dermatol Surg 2002;28:969.
6. Vitale-Lewis V. Sclerosing agents. In: Vitale-Lewis V, ed. Sclerotherapy
Accepted for publication June 19, 2008.
of Spider Veins. 1st ed. Newton, MA: Butterworth Heinemann; 1995:68.
7. Kern P, Ramelet A, Wütschert R, Bounameaux H, Hayoz D. Single- Reprint requests: Victoria A. Vitale-Lewis, MD, 1513 S. Harbor City Blvd.,
blind, randomized study comparing chromated glycerin, polidocanol Melbourne, FL 32901. E-mail: vvl@drvitalelewis.com.
solution, and polidocanol foam for treatment of telangiectatic leg veins. Copyright © 2008 by The American Society for Aesthetic Plastic Surgery, Inc.
Dermatol Surg 2004;30:367–372. 1090-820X/$34.00
8. Leach BC, Goldman MP. Comparative trial between sodium tetradecyl doi:10.1016/j.asj.2008.06.006
sulfate and glycerin in the treatment of telangiectatic leg veins.
Dermatol Surg 2003;29:612–614.
9. Goldman MP. Treatment of varicose and telangiectatic leg veins:
Double-blind prospective comparative trial between aethoxysklerol and
sotradecol. Dermatol Surg 2002;28:52–55.
10. Ouvry PA. Telangiectasia and sclerotherapy. J Dermatol Surg Oncol
1989;15:177–181.
11. Zimmet SE. Hyaluronidase in the prevention of sclerotherapy-induced
extravasation necrosis: A dose-response study. Dermatol Surg
1996;22:73–76.
12. Kern P, Ramelet AA, Wütschert R, Hayoz D. Compression after scle-
rotherapy for telangiectasias and reticular leg veins: A randomized con-
trolled study. J Vasc Surg 2007;45:1212–1226.
13. Fraser IA, Perry EP, Hatton M, Watkin DFL. Prolonged bandaging is not
required following sclerotherapy of varicose veins. Br J Surg
1985;72:488–490.
14. Goldman MP, Beaudoing D, Marley W, Lopez L, Butie A. Compression
in the treatment of leg telangiectasia: A preliminary report. J Dermatol
Surg Oncol 1990;16:322–325.
15. Weiss RA, Sadick NS, Goldman MP, Weiss MA. Post-sclerotherapy com-
pression: Controlled comparative study of duration of compression and
its effects on clinical outcome. Dermatol Surg 1999;25:105–108.
16. Goldman MP. How to utilize compression after sclerotherapy. Dermatol
Surg 2002;28:860–862.
17. Beresford SA, Chant AD, Jones HO, Piachaud D, Weddell JM. Varicose
veins: A comparison of surgery and injection/compression sclerothera-
py. Lancet 1978;1:921–924.
Aesthetic Treatment of Leg Veins Volume 28 • Number 5 • September/October 2008 • 583
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5819)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Quarter 1 - Module 1: Cookery 10Document21 pagesQuarter 1 - Module 1: Cookery 10Lany T. Catamin90% (62)
- Meridianpa46 ChecklistDocument6 pagesMeridianpa46 ChecklistArmandoanayaNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- S4965V2166 FS Preliminary PDFDocument20 pagesS4965V2166 FS Preliminary PDFmartinuruguayNo ratings yet
- Bio-Medical Waste ManagementDocument38 pagesBio-Medical Waste Managementabhishek80% (5)
- CoatDocument16 pagesCoatbalasubramanyam kotaNo ratings yet
- SCOPE of Plant AuditDocument2 pagesSCOPE of Plant AuditaroontpeNo ratings yet
- A Typical Synovial JointDocument8 pagesA Typical Synovial JointSheena Mae AtienzaNo ratings yet
- Request Letter StgoDocument3 pagesRequest Letter StgoJohn Paul De VeraNo ratings yet
- HRM Bpoland.Document9 pagesHRM Bpoland.SIDDHARTH PALNo ratings yet
- Are U Trying To Switch JobDocument5 pagesAre U Trying To Switch JobJesseNo ratings yet
- Samuel, Bucher & Suzuki - CAP 5, The Cambridge Handbook of Research Methods in Clinical PsychologyDocument9 pagesSamuel, Bucher & Suzuki - CAP 5, The Cambridge Handbook of Research Methods in Clinical PsychologyCarla AbarcaNo ratings yet
- Forest Fire Detection Using Image ProcessingDocument16 pagesForest Fire Detection Using Image ProcessingChilupuri Sreeya100% (1)
- PM GB GearmotorDocument10 pagesPM GB GearmotorMulugeta Kiros GebeyehuNo ratings yet
- FXSQ - PAVE FCU-Daikin-VRV-CutsheetDocument1 pageFXSQ - PAVE FCU-Daikin-VRV-Cutsheetsergio.anacletoNo ratings yet
- Corrected Map by IkbalDocument4 pagesCorrected Map by IkbalDrManoj Kumar SharmaNo ratings yet
- Ginger Beer - The Old Fashioned WayDocument5 pagesGinger Beer - The Old Fashioned WaySidnei Palatnik100% (1)
- 2 - States of Matter PDFDocument26 pages2 - States of Matter PDFRisialyn ManalangNo ratings yet
- Time Book PayrollDocument1 pageTime Book PayrollDarlyn Bagnol100% (2)
- Sensus Sonix - 12 - 16 - 25 Ultrasonic Meters LG-1021 PDFDocument2 pagesSensus Sonix - 12 - 16 - 25 Ultrasonic Meters LG-1021 PDFPaolita Auza BalderramaNo ratings yet
- A WolfdogDocument11 pagesA Wolfdogvolcom111No ratings yet
- Organizational Development Case Analysis-The Old Family BankDocument3 pagesOrganizational Development Case Analysis-The Old Family BankFabian HartmannNo ratings yet
- Safety Stock (Service Level) SQ Root of (Lead Time/Demand Period) Mean Absolute Value (MAD) MAD - Is Mean Average DeviationDocument1 pageSafety Stock (Service Level) SQ Root of (Lead Time/Demand Period) Mean Absolute Value (MAD) MAD - Is Mean Average DeviationNiraj KumarNo ratings yet
- Drugs in Pregnancy and LactationDocument7 pagesDrugs in Pregnancy and LactationAdria DiamanteNo ratings yet
- High Pressure UCV Catalog 2020Document10 pagesHigh Pressure UCV Catalog 2020МаксимNo ratings yet
- Saxena 2017Document13 pagesSaxena 2017Bimmo Dwi HartonoNo ratings yet
- ASME17-1 - Wire Rope Replacement CriteriaDocument2 pagesASME17-1 - Wire Rope Replacement Criteriaegyinspectoryahoo100% (1)
- Pump Curve and DefinitionDocument8 pagesPump Curve and DefinitionAleidinNo ratings yet
- Abortion Op EdDocument3 pagesAbortion Op EdMadeline GlotfeltyNo ratings yet
- General Biology 1 Final Exam 2nd QuarterDocument9 pagesGeneral Biology 1 Final Exam 2nd Quarterjoei Arquero100% (1)
- TEAS - Design Criteria - Final - EngDocument19 pagesTEAS - Design Criteria - Final - EngJan BakosNo ratings yet