Professional Documents
Culture Documents
Skin Manifestations Associated With COVID-19: Current Knowledge and Future Perspectives
Skin Manifestations Associated With COVID-19: Current Knowledge and Future Perspectives
Uploaded by
Kami BOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Skin Manifestations Associated With COVID-19: Current Knowledge and Future Perspectives
Skin Manifestations Associated With COVID-19: Current Knowledge and Future Perspectives
Uploaded by
Kami BCopyright:
Available Formats
Review Article
Dermatology 2021;237:1–12 Received: September 1, 2020
Accepted: November 10, 2020
DOI: 10.1159/000512932 Published online: November 24, 2020
Skin Manifestations Associated with
COVID-19: Current Knowledge and
Future Perspectives
Giovanni Genovese a, b Chiara Moltrasio a, c Emilio Berti a, b
Angelo Valerio Marzano a, b
a Dermatology Unit, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Milan, Italy; b Department of
Pathophysiology and Transplantation, Università degli Studi di Milano, Milan, Italy; c Department of Medical Surgical
and Health Sciences, University of Trieste, Trieste, Italy
Keywords Introduction
COVID-19 · Cutaneous manifestations · SARS-CoV-2
In December 2019, a novel zoonotic RNA virus named
“severe acute respiratory syndrome coronavirus 2” (SARS-
Abstract CoV-2) was isolated in patients with pneumonia in Wuhan,
Background: Coronavirus disease-19 (COVID-19) is an ongo- China. Since then, the disease caused by this virus, called
ing global pandemic caused by the “severe acute respiratory “coronavirus disease-19” (COVID-19), has spread through-
syndrome coronavirus 2” (SARS-CoV-2), which was isolated out the world at a staggering speed becoming a pandemic
for the first time in Wuhan (China) in December 2019. Com- emergency [1]. Although COVID-19 is best known for
mon symptoms include fever, cough, fatigue, dyspnea and causing fever and respiratory symptoms, it has been report-
hypogeusia/hyposmia. Among extrapulmonary signs asso- ed to be associated also with different extrapulmonary
ciated with COVID-19, dermatological manifestations have manifestations, including dermatological signs [2]. Whilst
been increasingly reported in the last few months. Summa- the COVID-19-associated cutaneous manifestations have
ry: The polymorphic nature of COVID-19-associated cutane- been increasingly reported, their exact incidence has yet to
ous manifestations led our group to propose a classification, be estimated, their pathophysiological mechanisms are
which distinguishes the following six main clinical patterns: largely unknown, and the role, direct or indirect, of SARS-
(i) urticarial rash, (ii) confluent erythematous/maculopapu- CoV-2 in their pathogenesis is still debated. Furthermore,
lar/morbilliform rash, (iii) papulovesicular exanthem, (iv) chil- evidence is accumulating that skin manifestations associ-
blain-like acral pattern, (v) livedo reticularis/racemosa-like ated with COVID-19 are extremely polymorphic [3]. In this
pattern, (vi) purpuric “vasculitic” pattern. This review sum- regard, our group proposed the following six main clinical
marizes the current knowledge on COVID-19-associated cu- patterns of COVID-19-associated cutaneous manifesta-
taneous manifestations, focusing on clinical features and tions in a recently published review article: (i) urticarial
therapeutic management of each category and attempting rash, (ii) confluent erythematous/maculopapular/morbil-
to give an overview of the hypothesized pathophysiological liform rash, (iii) papulovesicular exanthem, (iv) chilblain-
mechanisms of these conditions. © 2020 S. Karger AG, Basel like acral pattern, (v) livedo reticularis/racemosa-like pat-
karger@karger.com © 2020 S. Karger AG, Basel Angelo Valerio Marzano
www.karger.com/drm Dermatology Unit
Università degli Studi di Milano
Via Pace 9, IT–20122 Milan (Italy)
angelo.marzano @ unimi.it
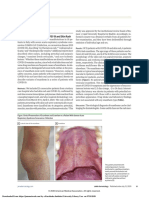
Confluent erythematous/
Livedo reticularis/racemosa-
Urticarial rash maculopapular/morbilliform Papulovesicular exanthem Chilblain-like acral pattern Purpuric “vasculitic” pattern
like pattern
rash
Erythematous- Reticular
Erythematous Erythematous Violaceous papules,
Wheals violaceous macules erythematous-
macules and papules papules and vesicles ulceration
and patches violaceous macules
Predominantly Predominantly Predominantly Predominantly Predominantly Predominantly
involved site: involved site: involved site: involved site: involved site: involved site:
trunk, limbs trunk trunk lower limbs, feet lower limbs lower limbs
Fig. 1. Clinical features of COVID-19-associated cutaneous manifestations.
tern, (vi) purpuric “vasculitic” pattern (shown in Fig. 1) [2]. ia-like eruptions have been subsequently described in
Other authors have attempted to bring clarity in this field, other cohort studies. Galván Casas et al. [4] stated that
suggesting possible classifications of COVID-19-associated urticarial rash occurred in 19% of their cohort, tended to
cutaneous manifestations [4–6]. Finally, distinguishing no- appear simultaneously with systemic symptoms, lasted
sological entities “truly” associated with COVID-19 from approximately 1 week and was associated with medium-
cutaneous drug reactions or exanthems due to viruses oth- high severity of COVID-19. Moreover, itch was almost
er than SARS-CoV-2 remains a frequent open problem. always present [4]. Freeman et al. [10] found a similar
Herein, we have striven to provide a comprehensive prevalence of urticaria (16%) in their series of 716 cases,
overview of the cutaneous manifestations associated with in which urticarial lesions predominantly involved the
COVID-19 subdivided according to the classification by trunk and limbs, relatively sparing the acral sites. As
Marzano et al. [2], focusing on clinical features, histo- shown in Table 1, urticaria-like signs accounted for 11.9%
pathological features, hypothesized pathophysiological of cutaneous manifestations seen in an Italian multicen-
mechanisms and therapeutic management. tric cohort study on 159 patients [unpubl. data]. Urticar-
ial lesions associated with fever were reported to be early
or even prodromal signs of COVID-19, in the absence of
Urticarial Rash respiratory symptoms, in 3 patients [11–13]. Therefore,
the authors of the reports suggested that isolation is need-
Clinical Features and Association with COVID-19 ed for patients developing such skin symptoms if COV-
Severity ID-19 infection is suspected in order to prevent possible
It is well known that urticaria and angioedema can be SARS-CoV-2 transmission [11–13]. COVID-19-related
triggered by viral and bacterial agents, such as cytomega- urticaria occurred also in a familial cluster, involving 2
lovirus, herpesvirus, and Epstein-Barr virus and myco- patients belonging to a Mexican family of 5 people, all in-
plasma. However, establishing a cause-effect relationship fected by SARS-CoV-2 and suffering also from anosmia,
may be difficult in single cases [7, 8]. Urticarial eruptions ageusia, chills and dizziness [14]. Angioedema may ac-
associated with COVID-19 have been first reported by company COVID-19-related urticaria, as evidenced by
Recalcati [9] in his cohort of hospitalized patients, ac- the case published in June 2020 of an elderly man present-
counting for 16.7% of total skin manifestations. Urticar- ing with urticaria, angioedema, general malaise, fatigue,
2 Dermatology 2021;237:1–12 Genovese/Moltrasio/Berti/Marzano
DOI: 10.1159/000512932
Table 1. Prevalence of different clinical patterns in the main studies on COVID-19-associated cutaneous manifestations
First author (total size of study population) Number of patients Number of patients with Number of patients Number of patients Number of patients Number of patients
with urticarial confluent erythematous/ with papulo-vesicular with chilblain-like with livedo reticularis/ with purpuric
rash (%) maculopapular/ exanthem (%) acral pattern (%) racemosa-like “vasculitic”
morbilliform rash (%) pattern (%) pattern (%)
Galván Casas [4] (375) 73 (19) 176 (47) 34 (9) 71 (19) 21 (6)
Freeman [10] (716) 55 (8.1) 115 (16.1) 49 (7.2) 422 (62) 46 (6.4) 51 (7.1)
Askin [29] (52) 7 (13.5) 29 (55.8) 3 (5.8) 1 (1.9) 0 8 (15.4)
De Giorgi [20] (53) 14 (26) 37 (70) 2 (4) 0 0 0
Unpublished data from an Italian
multicentric study (159) 19 (11.9) 48 (30.2) 29 (18.2) 46 (28.9) 4 (2.5) 13 (8.2)
fever and pharyngodynia [15]. Urticarial vasculitis has al. [4], for 44% of the skin manifestations included in the
also been described in association with COVID-19 in 2 study by Freeman et al. [10], who further subdivided this
patients [16]. group of cutaneous lesions into macular erythema (13%),
morbilliform exanthems (22%) and papulosquamous le-
Histopathological Findings sions (9%), and for 30.2% of the cutaneous manifestations
Histopathological studies of urticarial rashes are scant. included in the unpublished Italian multicentric study
In a 60-year-old woman with persistent urticarial erup- shown in Table 1. The prevalence of erythematous rash
tion and interstitial pneumonia who was not under any was higher in other studies, like that published by De
medication, Rodriguez-Jiménez et al. [17] found on his- Giorgi et al. [20] in May 2020, in which erythematous
topathology slight vacuolar interface dermatitis with oc- rashes accounted for 70% of total skin manifestations. In
casional necrotic keratinocytes curiously compatible with the series by Freeman et al. [10], macular erythema, mor-
an erythema multiforme-like pattern. Amatore et al. [18] billiform exanthems and papulosquamous lesions were
documented also the presence of lichenoid and vacuolar predominantly localized on the trunk and limbs, being
interface dermatitis, associated with mild spongiosis, dys- associated with pruritus in most cases. In the same series,
keratotic basal keratinocytes and superficial perivascular these lesions occurred more frequently after COVID-19
lymphocytic infiltrate, in a biopsy of urticarial eruption systemic symptoms’ onset [21]. The clinical picture of the
associated with COVID-19 (Fig. 2). eruptions belonging to this group may range from ery-
thematous confluent rashes to maculopapular eruptions
Therapeutic Options and morbilliform exanthems. Erythematous lesions may
Shanshal [19] suggested low-dose systemic corticoste- show a purpuric evolution [21] or coexist from the begin-
roids as a therapeutic option for COVID-19-associated ning with purpuric lesions [22]. Erythematous papules
urticarial rash. Indeed, the author hypothesized that low- may also be arranged in a morbilliform pattern [23]. In a
dose systemic corticosteroids, combined with nonsedat- subanalysis of the COVID-Piel Study [4] on maculopapu-
ing antihistamines, can help in managing the hyperactiv- lar eruptions including also purpuric, erythema multi-
ity of the immune system in COVID-19, not only to con- forme-like, pityriasis rosea-like, erythema elevatum
trol urticaria, but also to improve possibly the survival diutinum-like and perifollicular eruptions, morbilliform
rate in COVID-19. exanthems were the most frequent maculopapular pat-
tern (n = 80/176, 45.5%) [24]. This study showed that in
most cases lesions were generalized, symmetrical and
Confluent Erythematous/Maculopapular/ started on the trunk with centrifugal progression. In the
Morbilliform Rash same subanalysis, hospital admission due to pneumonia
was very frequent (80%) in patients with a morbilliform
Clinical Features and Association with COVID-19 pattern [24]. In this group, the main differential diagno-
Severity ses are represented by exanthems due to viruses other
Maculopapular eruptions accounted for 47% of all cu- than SARS-CoV-2 and drug-induced cutaneous reac-
taneous manifestations in the cohort of Galván Casas et tions.
COVID-19-Associated Skin Dermatology 2021;237:1–12 3
Manifestations DOI: 10.1159/000512932
a b
c d
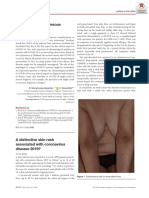
Fig. 2. Histopathological features of the main cutaneous patterns associated with COVID-19. a Urticarial rash.
b Confluent erythematous maculopapular/morbilliform rash. c Chilblain-like acral lesions. d Purpuric “vascu-
litic” pattern.
Histopathological Findings Therapeutic Options
Histopathology of erythematous eruptions was de- The management of confluent erythematous/maculo-
scribed by Gianotti et al. [25], who found vascular dam- papular/morbilliform rash varies according to the sever-
age in all the 3 cases examined. A clinicopathological ity of the clinical picture. Topical corticosteroids can be
characterization of late-onset maculopapular eruptions sufficient in most cases [23], systemic corticosteroids de-
related to COVID-19 was provided also by Reymundo et serving to be administered just in more severe and wide-
al. [26], who observed a mild superficial perivascular lym- spread presentations.
phocytic infiltrate on the histology of 4 patients. In con-
trast, Herrero-Moyano et al. [27] observed dense neutro-
philic infiltrates in 8 patients with late maculopapular Papulovesicular Exanthem
eruptions. The authors of the former study postulated
that this discrepancy could be attributable to the history Clinical Features and Association with COVID-19 Severity
of new drug assumptions in the series of Herrero-Moya- COVID-19-associated papulovesicular exanthem
no et al. [26] (Fig. 2). was first extensively reported in a multicenter Italian
4 Dermatology 2021;237:1–12 Genovese/Moltrasio/Berti/Marzano
DOI: 10.1159/000512932
case series of 22 patients published in April 2020 [28]. nent acantholysis and dyskeratosis associated with the
In this article, it was originally described as “varicella- presence of an unilocular intraepidermal vesicle in a su-
like” due to resemblance of its elementary lesions to prabasal location. Based on these histopathological find-
those of varicella. However, the authors themselves un- ings, the authors refused the term “varicella-like rash”
derlined that the main clinical features of COVID- and proposed a term which was more suitable in their
19-associated papulovesicular exanthem, namely trunk view: “COVID-19-associated acantholytic rash.” Histo-
involvement, scattered distribution and mild/absent pathological findings of another case of papulovesicular
pruritus, differentiated it from “true” varicella. In this eruption revealed extensive epidermal necrosis with ac-
study, skin lesions appeared on average 3 days after sys- antholysis and swelling of keratinocytes, ballooning de-
temic symptoms’ onset and healed after 8 days, without generation of keratinocytes and signs of endotheliitis in
scarring sequelae [28]. The exact prevalence of papulo- the dermal vessels [33]. Acantholysis and ballooned ke-
vesicular exanthems is variable. Indeed, in a cohort of ratinocytes were found also by Fernandez-Nieto et al.
375 patients with COVID-19-associated cutaneous [31] in 2 patients.
manifestations [4], patients with papulovesicular exan- The differential diagnosis with infections caused by
them were 34 (9%), while they were 3 out of 52 (5.8%), members of the Herpesviridae family has been much de-
1 out of 18 (5.5%) and 2 out of 53 (4%) in the cohorts bated. Tammaro et al. [34] described the onset of numer-
published by Askin et al. [29], Recalcati [9] and De ous, isolated vesicles on the back 8 days after COVID-19
Giorgi et al. [20], respectively. In the Italian multicen- diagnosis in a Barcelonan woman and reported on 2 pa-
tric study shown in Table 1, papulovesicular rash ac- tients from Rome presenting with isolated, mildly pru-
counted for 18.2% of skin manifestations. Further- ritic erythematous-vesicular lesions on their trunk, spec-
more, even if papulovesicular exanthem tends to in- ulating that these manifestations might be due to viruses
volve more frequently the adult population, with a belonging to the Herpesviridae family. On the other hand,
median age of 60 years in the study by Marzano et al. classic herpes zoster has been reported to complicate the
[28], also children may be affected [30]. Galván Casas course of COVID-19 [35].
et al. [4] reported that vesicular lesions generally in- The controversy regarding the role of herpesvirus in
volved middle-aged patients, before systemic symp- the etiology of papulovesicular exanthems fuelled an in-
toms’ onset in 15% of cases, and were associated with tense scientific debate. Indeed, some authors raised the
intermediate COVID-19 severity. Fernandez-Nieto et question whether papulovesicular exanthem associated
al. [31] conducted a prospective study on 24 patients with COVID-19 could be diagnosed without ruling out
diagnosed with COVID-19-associated vesicular rash. varicella zoster virus and herpes simplex virus with
In this cohort, the median age (40.5 years) was lower Tzanck smear or polymerase chain reaction (PCR) for the
than that reported by Marzano et al. [28], and COV- Herpesviridae family in the vesicle fluid or on the skin
ID-19 severity was mostly mild or intermediate, with [36, 37]. In our opinion, even if seeking DNA of Herpes-
only 1 patient requiring intensive unit care support. In viridae family members is ideally advisable, clinical diag-
our cohort of 22 patients, a patient was hospitalized in nosis may be reliable in most cases, and the role of herpes
the intensive care unit and 3 patients died [28]. Vesicu- viruses as mere superinfection in patients with dysfunc-
lar rash, which was generally pruritic, appeared after tional immune response associated with COVID-19
COVID-19 diagnosis in most patients (n = 19; 79.2%), needs to be considered [38]. To our knowledge, SARS-
with a median latency time of 14 days [31]. Two differ- CoV-2 has not been hitherto isolated by means of reverse
ent morphological patterns were found: a widespread transcriptase PCR in the vesicle fluid of papulovesicular
polymorphic pattern, more common and consisting of rash [33, 31].
small papules, vesicles and pustules of different sizes,
and a localized pattern, less frequent and consisting of Therapeutic Options
monomorphic lesions, usually involving the mid chest/ No standardized treatments for COVID-19-related
upper abdominal region or the back [31]. papulovesicular exanthem are available, also given that it
is self-healing within a short time frame. Thus, a “wait-
Histopathological Findings and-see” strategy may be recommended.
Mahé et al. [32] reported on 3 patients with typical
COVID-19-associated papulovesicular rash, in which
the histological pattern of skin lesions showed promi-
COVID-19-Associated Skin Dermatology 2021;237:1–12 5
Manifestations DOI: 10.1159/000512932
Chilblain-Like Acral Pattern perivascular and perieccrine sweat gland lymphocytic in-
flammation. Vascular changes such as endotheliitis and mi-
Clinical Features and Association with COVID-19 crothrombi may be found [40, 45, 54, 55] (Fig. 2).
Severity Data on the real association between chilblain-like ac-
COVID-19-related chilblain-like acral lesions have ral lesions and COVID-19 are controversial.
been first described in a 13-year-old boy by Italian au- The first case series failed to perform SARS-CoV-2 test-
thors in early March [39]. Since then, several “outbreaks” ing in all patients, also due to logistic problems and eco-
of chilblain-like acral lesions chiefly involving young nomic restrictions, and diagnosed COVID-19 only in a mi-
adults and children from different countries worldwide nority of patients with chilblain-like acral lesions [40, 44,
have been posted on social media and published in the 47]. Subsequently, some authors systematically sought
scientific literature [40–46]. Caucasians seem to be sig- SARS-CoV-2 with serology and/or nasopharyngeal swab in
nificantly more affected than other ethnic groups [47, 48]. patients with chilblain-like acral lesions. In their cohort of
Chilblain-like acral lesions were the second most fre- 38 children with pseudo-chilblain, Caselli et al. [56] showed
quent cutaneous manifestation (n = 46/159; 28.9%) in the no evidence of SARS-CoV-2 infection by PCR or serology.
multicenter Italian study shown in Table 1. Different Chilblain-like acral lesions appeared not to be directly as-
pathogenetic hypotheses, including increased interferon sociated with COVID-19 also in the case series by Herman
release induced by COVID-19 and consequent cytokine- et al. [57]. These authors failed to detect SARS-CoV-2 in
mediated inflammatory response, have been suggested nasopharyngeal swabs and skin biopsies and demonstrated
[49]. Furthermore, virus-induced endothelial damage as no specific anti-SARS-CoV-2 immunoglobulin IgM or IgG
well as an obliterative microangiopathy and coagulation antibodies in blood samples. Therefore, they concluded
abnormalities could be mechanisms involved in the that lifestyle changes associated with lockdown measures
pathogenesis of these lesions [50]. Chilblain-like acral le- might be a possible explanation for these lesions [57]. Sim-
sions associated with COVID-19 were depicted as ery- ilar results were obtained also by other authors [58–63]
thematous-violaceous patches or plaques predominantly weakening the hypothesis of a direct etiological link be-
involving the feet and, to a lesser extent, hands [40, 51]. tween SARS-CoV-2 and chilblain-like acral lesions.
Rare cases of chilblain-like lesions involving other acral Opposite conclusions have been drawn by Colmenero
sites, such as the auricular region, were also reported [52]. et al. [64], who demonstrated by immunohistochemistry
The occurrence of blistering lesions varied according to and electron microscopy the presence of SARS-CoV-2 in
the case series analyzed; Piccolo et al. [51], indeed, re- endothelial cells of skin biopsies of 7 children with chil-
ported the presence of blistering lesions in 23 out of 54 blain-like acral lesions, suggesting that virus-induced
patients, while other authors did not describe bullous le- vascular damage and secondary ischemia could explain
sions in their series [40, 47]. Dermoscopy of these lesions the pathophysiology of these lesions.
revealed the presence of an indicative pattern represented In the absence of definitive data on chilblain-like acral
by a red background area with purpuric globules [53]. lesions’ pathogenesis, the occurrence of such lesions
Pain/burning sensation as well as pruritus were common- should prompt self-isolation and confirmatory testing for
ly reported symptoms, even if a small proportion of pa- SARS-CoV-2 infection [65].
tients presented with asymptomatic lesions [40, 44, 47].
Unlike other COVID-19-related cutaneous findings, Therapeutic Options
chilblain-like acral lesions tended to mostly involve pa- In the absence of significant therapeutic options for
tients without systemic symptoms. chilblain-like acral lesions associated with COVID-19
The frequent occurrence of chilblain-like lesions in the and given their tendency to spontaneously heal, a “wait-
absence of cold exposure and the involvement of patients and-see” strategy may be suggested.
without evident COVID-19-related symptoms raised the
question whether these manifestations were actually as-
sociated with SARS-CoV-2 infection. Livedo Reticularis/Racemosa-Like Pattern
Histopathological and Pathophysiological Findings Clinical Features and Association with COVID-19
Chilblain-like lesions share many histopathological fea- Severity
tures with idiopathic and autoimmunity-related chilblains, Livedo describes a reticulate pattern of slow blood
including epidermal necrotic keratinocytes, dermal edema, flow, with consequent desaturation of blood and bluish
6 Dermatology 2021;237:1–12 Genovese/Moltrasio/Berti/Marzano
DOI: 10.1159/000512932
cutaneous discoloration. It has been divided into: (i) li- Therapeutic Options
vedo reticularis, which develops as tight, symmetrical, In view of the absence of significant therapeutic op-
lace-like, dusky patches forming complete rings sur- tions for livedo reticularis/racemosa-like lesions associ-
rounding a pale center, generally associated with cold- ated with COVID-19, a “wait-and-see” strategy may be
induced cutaneous vasoconstriction or vascular flow dis- suggested.
turbances such as seen in polycythemia and (ii) livedo
racemosa, characterized by larger, irregular and asym-
metrical rings than seen in livedo reticularis, more fre- Purpuric “Vasculitic” Pattern
quently associated with focal impairment of blood flow,
as it can be seen in Sneddon’s syndrome [66]. Clinical Features and Association with COVID-19
In our classification, the livedo reticularis/racemosa- Severity
like pattern has been distinguished by the purpuric “vas- The first COVID-19-associated cutaneous manifesta-
culitic” pattern because the former likely recognizes a oc- tion with purpuric features was reported by Joob et al.
clusive/microthrombotic vasculopathic etiology, while [76], who described a petechial rash misdiagnosed as den-
the latter can be more likely considered the expression of gue in a COVID-19 patient. Purpuric lesions have been
a “true” vasculitic process [2]. Instead, the classification suggested to occur more frequently in elderly patients
by Galván Casas et al. [4] merged these two patterns into with severe COVID-19, likely representing the cutaneous
the category “livedo/necrosis”. manifestations associated with the highest rate of COV-
In a French study on vascular lesions associated with ID-19-related mortality [4]. This hypothesis is corrobo-
COVID-19, livedo was observed in 1 out of 7 patients rated by the unfavorable prognosis observed in several
[43]. In the large cases series of 716 patients by Freeman cases reported in the literature [77, 78].
et al. [10], livedo reticularis-like lesions, retiform purpura The purpuric pattern reflects the presence of vasculitic
and livedo racemosa-like lesions accounted for 3.5, 2.6 changes probably due to the direct damage of endothelial
and 0.6% of all cutaneous manifestations, respectively. In cells by the virus or dysregulated host inflammatory re-
the multicentric Italian study, livedo reticularis/racemo- sponses induced by COVID-19.
sa-like lesions accounted for 2.5% of cutaneous manifes- These lesions are likely to be very rare, representing
tations (Table 1). 8.2% of skin manifestations included in the Italian multi-
The pathogenic mechanisms at the basis of small blood centric study shown in Table 1. In their case series of 7
vessel occlusion are yet unknown, even if neurogenic, mi- patients with vascular skin lesions related to COVID-19,
crothrombotic or immune complex-mediated etiologies Bouaziz et al. [43] reported 2 patients with purpuric le-
have been postulated [67]. sions with (n = 1) and without (n = 1) necrosis. In the se-
Livedo reticularis-like lesions are frequently mild, ries by Freeman et al. [10], 12/716 (1.8%) and 11/716
transient and not associated with thromboembolic com- (1.6%) cases of patients with palpable purpura and den-
plications [68, 69]. On the contrary, livedo racemosa-like gue-like eruption, respectively, have been reported.
lesions and retiform purpura have often been described Galván Casas et al. [4] reported 21 patients with “livedo/
in patients with severe coagulopathy [60–72]. necrosis,” most of whom presenting cutaneous signs in
concomitance with systemic symptoms’ onset.
Histopathological and Pathophysiological Findings Purpuric lesions may be generalized [79], localized in
The histopathology of livedoid lesions associated with the intertriginous regions [80] or arranged in an acral dis-
COVID-19 has been described by Magro et al. [73], who tribution [81]. Vasculitic lesions may evolve into hemor-
observed in 3 patients pauci-inflammatory microthrom- rhagic blisters [77]. In most severe cases, extensive acute
botic vasculopathy. The same group demonstrated that in necrosis and association with severe coagulopathy may be
the thrombotic retiform purpura of patients with severe seen [78]. Dermoscopy of purpuric lesions revealed the
COVID-19, the vascular thrombosis in the skin and in- presence of papules with incomplete violaceous rim and
ternal organs is associated with a minimal interferon re- a central yellow globule [82].
sponse permitting increased viral replication with release
of viral proteins that localize to the endothelium inducing Histopathological Findings
widespread complement activation [74], which is fre- When performed, histopathology of skin lesions
quent in COVID-19 patients and probably involved in showed leukocytoclastic vasculitis [77, 79], severe neutro-
the pathophysiology of its clinical complications [75]. philic infiltrate within the small vessel walls and in their
COVID-19-Associated Skin Dermatology 2021;237:1–12 7
Manifestations DOI: 10.1159/000512932
Table 2. Summary of clinical features, histopathological findings, severity of COVID-19 systemic symptoms and therapeutic options of
COVID-19-related skin manifestations
Clinical features COVID-19 Histopathological Therapeutic
severity findings options
Urticarial rash Itching urticarial rash predominantly Intermediate Vacuolar interface Low-dose systemic
involving the trunk and limbs; angioedema severity dermatitis associated with corticosteroids
may also rarely occur superficial perivascular combined with
lymphocytic infiltrate nonsedating
antihistamines
Confluent erythematous/ Generalized, symmetrical lesions starting from Intermediate Superficial perivascular Topical
maculopapular/morbilliform the trunk with centrifugal progression; severity lymphocytic and/or corticosteroids for
rash purpuric lesions may coexist from the onset or neutrophilic infiltrate mild cases;
develop during the course of the skin eruption systemic
corticosteroids for
severe cases
Papulovesicular exanthem (i) Widespread polymorphic pattern consisting Intermediate Prominent acantholysis and Wait and see
of small papules, vesicles and pustules of severity dyskeratosis associated with
different sizes; (ii) localized pattern consisting unilocular intraepidermal
of papulovesicular lesions, usually involving vesicles in a suprabasal
the mid chest/upper abdominal region or the location
back
Chilblain-like acral pattern Erythematous-violaceous patches or plaques Asymptomatic Perivascular and Wait and see
predominantly involving the feet or, to a lesser status periadnexal dermal
extent, hands. Pain/burning sensation as well lymphocytic infiltrates
as pruritus were commonly reported
symptoms
Livedo reticularis/ Livedo reticularis-like lesions: mild, transient, Livedo reticularis- Pauci-inflammatory Wait and see
racemosa-like pattern symmetrical, lace-like, dusky patches forming like lesions: microthrombotic
complete rings surrounding a pale center. intermediate vasculopathy
Livedo racemosa-like lesions: large, irregular severity; livedo
and asymmetrical violaceous annular lesions racemosa-like
frequently described in patients with severe lesions: high severity
coagulopathy
Purpuric “vasculitic” pattern Purpuric lesions may be generalized, arranged High severity Leukocytoclastic vasculitis, Topical
in an acral distribution or localized in the severe perivascular corticosteroids for
intertriginous regions. Purpuric elements may neutrophilic and mild cases;
evolve into hemorrhagic blisters, possibly lymphocytic infiltrate, systemic
leading to necrotic-ulcerative lesions presence of fibrin and corticosteroids for
endothelial swelling severe cases
The correlation between severity of COVID-19 systemic symptoms and skin manifestations has been inferred mainly from the study by Freeman et al.
[10].
proximity [77], intense lymphocytic perivascular infil- Other COVID-19-Associated Cutaneous
trates [81], presence of fibrin [79, 81] and endothelial Manifestations
swelling [82] (Fig. 2).
Other peculiar rare COVID-19-related cutaneous
Therapeutic Options manifestations that cannot be pigeonholed in the classifi-
Topical corticosteroids have been successfully used for cation proposed by our group [2] include, among others,
treating mild cases of purpuric lesions [80]. Cases with the erythema multiforme-like eruption [83], pityriasis ro-
necrotic-ulcerative lesions and widespread presentation sea-like rash [84], multi-system inflammatory syndrome
may be treated with systemic corticosteroids. in children [85], anagen effluvium [86] and a pseudoher-
petic variant of Grover disease [87]. However, the spec-
trum of possible COVID-19-associated skin manifesta-
8 Dermatology 2021;237:1–12 Genovese/Moltrasio/Berti/Marzano
DOI: 10.1159/000512932
tions is likely to be still incomplete, and it is expected that Key Message
new entities associated with this infection will be de-
Although COVID-19-associated cutaneous manifestations
scribed. have been increasingly reported, their pathophysiological mecha-
nisms need to be extensively explored. The conditions may be dis-
tinguished in six clinical phenotypes, each showing different his-
Conclusion topathological patterns.
COVID-19-associated cutaneous manifestations have
been increasingly reported in the last few months, garner- Acknowledgment
ing attention both from the international scientific com-
We would like to thank Dr. Cosimo Misciali, Dr. Paolo Sena
munity and from the media. A few months after the out- and Prof. Pietro Quaglino for kindly providing us with histopath-
break of the pandemic, many narrative and systematic ological pictures.
reviews concerning the dermatological manifestations of
COVID-19 have been published [2, 3, 6, 88–91]. A sum-
mary of clinical features, histopathological findings, se- Conflict of Interest Statement
verity of COVID-19 systemic symptoms and therapeutic
options of COVID-19-related skin manifestations has The authors have no conflicts of interest to declare.
been provided in Table 2.
Albeit several hypotheses on pathophysiological
mechanisms at the basis of these skin findings are present Funding Sources
in the literature [50, 92, 93], none of them is substantiated
This paper did not receive any funding.
by strong evidence, and this field needs to be largely elu-
cidated. Moreover, cutaneous eruptions due to viruses
other than SARS-CoV-2 [35, 37] or drugs prescribed for Author Contributions
the management of this infection [94, 95] always need to
be ruled out. Giovanni Genovese wrote the paper with the contribution of
Experimental pathophysiological studies and clinical Chiara Moltrasio. Angelo Valerio Marzano and Emilio Berti su-
data derived from large case series are still needed for pervised the work and revised the paper for critical revision of im-
portant intellectual content.
shedding light onto this novel, underexplored and fasci-
nating topic.
References
1 Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, 5 Potekaev NN, Zhukova OV, Protsenko DN, 9 Recalcati S. Cutaneous manifestations in COV-
et al. Clinical features of patients infected with Demina OM, Khlystova EA, Bogin V. Clinical ID-19: a first perspective. J Eur Acad Derma-
2019 novel coronavirus in Wuhan, China. characteristics of dermatologic manifesta- tol Venereol. 2020 May;34(5):e212–3.
Lancet. 2020 Feb;395(10223):497–506. tions of COVID-19 infection: case series of 15 10 Freeman EE, McMahon DE, Lipoff JB, Rosen-
2 Marzano AV, Cassano N, Genovese G, Mol- patients, review of literature, and proposed bach M, Kovarik C, Desai SR, et al. The spec-
trasio C, Vena GA. Cutaneous manifestations etiological classification. Int J Dermatol. 2020 trum of COVID-19-associated dermatologic
in patients with COVID-19: a preliminary re- Aug;59(8):1000–9. manifestations: an international registry of
view of an emerging issue. Br J Dermatol. 6 Gisondi P, PIaserico S, Bordin C, Alaibac M, 716 patients from 31 countries. J Am Acad
2020 Sep;183(3):431–42. Girolomoni G, Naldi L. Cutaneous manifesta- Dermatol. 2020 Oct;83(4):1118–29.
3 Matar S, Oulès B, Sohier P, Chosidow O, Bey- tions of SARS-CoV-2 infection: a clinical up- 11 van Damme C, Berlingin E, Saussez S, Acca-
lot-Barry M, Dupin N, et al. Cutaneous man- date [online ahead of print]. J Eur Acad Der- puto O. Acute urticaria with pyrexia as the
ifestations in SARS-CoV-2 infection (COV- matol Venereol. 2020 Jun;jdv.16774. first manifestations of a COVID-19 infection.
ID-19): a French experience and a systematic 7 Imbalzano E, Casciaro M, Quartuccio S, Min- J Eur Acad Dermatol Venereol. 2020 Jul;
review of the literature. J Eur Acad Dermatol ciullo PL, Cascio A, Calapai G, et al. Associa- 34(7):e300–1.
Venereol. 2020 Jun;jdv.16775. tion between urticaria and virus infections: A 12 Quintana-Castanedo L, Feito-Rodríguez M,
4 Galván Casas C, Català A, Carretero Hernán- systematic review. Allergy Asthma Proc. 2016 Valero-López I, Chiloeches-Fernández C,
dez G, Rodríguez-Jiménez P, Fernández-Nie- Jan-Feb;37(1):18–22. Sendagorta-Cudós E, Herranz-Pinto P. Urti-
to D, Rodríguez-Villa Lario A, et al. Classifi- 8 Yong SB, Yeh WC, Wu HJ, Chen HH, Huang JY, carial exanthem as early diagnostic clue for
cation of the cutaneous manifestations of Chang TM, et al. Impact of mycoplasma pneu- COVID-19 infection. JAAD Case Rep. 2020
COVID-19: a rapid prospective nationwide monia infection on urticaria: A nationwide, pop- Apr;6(6):498–9.
consensus study in Spain with 375 cases. Br J ulation-based retrospective cohort study in Tai-
Dermatol. 2020 Jul;183(1):71–7. wan. PLoS One. 2019 Dec;14(12):e0226759.
COVID-19-Associated Skin Dermatology 2021;237:1–12 9
Manifestations DOI: 10.1159/000512932
13 Hassan K. Urticaria and angioedema as a pro- ropolitan Area of Milan, Italy. Acta Derm Ve- 37 Llamas-Velasco M, Rodríguez-Jiménez P,
dromal cutaneous manifestation of SARS- nereol. 2020 Apr;100(8):adv00124–2. Chicharro P, De Argila D, Muñoz-Hernández
CoV-2 (COVID-19) infection. BMJ Case Rep. 26 Reymundo A, Fernáldez-Bernáldez A, Reolid P, Daudén E. Reply to “Varicella-like exan-
2020 Jul;13(7):e236981. A, Butrón B, Fernández-Rico P, Muñoz- them as a specific COVID-19-associated skin
14 Cepeda-Valdes R, Carrion-Alvarez D, Trejo- Hernández P, et al. Clinical and histological manifestation: Multicenter case series of 22
Castro A, Hernandez-Torre M, Salas-Alanis J. characterization of late appearance maculo- patients”: To consider varicella-like exan-
Cutaneous manifestations in COVID-19: fa- papular eruptions in association with the them associated with COVID-19, virus vari-
milial cluster of urticarial rash. Clin Exp Der- coronavirus disease 2019. A case series of sev- cella zoster and virus herpes simplex must be
matol. 2020 May;45(7):895–6. en patients. J Eur Acad Dermatol Venereol. ruled out. J Am Acad Dermatol. 2020 Sep;
15 Najafzadeh M, Shahzad F, Ghaderi N, Ansari 2020 Jun;jdv.16707. 83(3):e253–4.
K, Jacob B, Wright A. Urticaria (angioedema) 27 Herrero-Moyano M, Capusan TM, Andreu- 38 Marzano AV, Genovese G. Response to: "Re-
and COVID-19 infection. J Eur Acad Derma- Barasoain M, Alcántara-González J, Ruano- ply to 'Varicella-like exanthem as a specific
tol Venereol. 2020 Oct;34(10):e568–70. Del Salado M, Sánchez-Largo Uceda ME, et COVID-19-associated skin manifestation:
16 de Perosanz-Lobo D, Fernandez-Nieto D, al. A clinicopathological study of eight pa- multicenter case series of 22 patients': To con-
Burgos-Blasco P, Selda-Enriquez G, Carre tients with COVID-19 pneumonia and a late- sider varicella-like exanthem associated with
tero I, Moreno C, et al. Urticarial vasculitis in onset exanthema. J Eur Acad Dermatol Vene- COVID-19, virus varicella zoster and virus
COVID-19 infection: a vasculopathy-related reol. 2020 May;34(9): https://doi.org/10.1111/ herpes simplex must be ruled out." J Am Acad
symptom? J Eur Acad Dermatol Venereol. jdv.16631. Dermatol. 2020 Sep; 83(3):e255–e256.
2020 Oct;34(10):e566–8. 28 Marzano AV, Genovese G, Fabbrocini G, Pi- 39 Mazzotta F, Troccoli T. Acute acro-ischemia
17 Rodríguez-Jiménez P, Chicharro P, De Argila gatto P, Monfrecola G, Piraccini BM, et al. in the child at the time of COVID-19. Eur J
D, Muñoz-Hernández P, Llamas-Velasco M. Varicella-like exanthem as a specific COVID- Pediatr Dermatol. 2020;30(2):71–4.
Urticaria-like lesions in COVID-19 patients 19-associated skin manifestation: multicenter 40 Colonna C, Genovese G, Monzani NA, Picca
are not really urticaria - a case with clinico- case series of 22 patients. J Am Acad Derma- M, Boggio F, Gianotti R, et al. Outbreak of
pathological correlation. J Eur Acad Derma- tol. 2020 Jul;83(1):280–5. chilblain-like acral lesions in children in the
tol Venereol. 2020 May; 34(9): https://doi. 29 Askin O, Altunkalem RN, Altinisik DD, metropolitan area of Milan, Italy, during the
org/10.1111/jdv.16618. Uzuncakmak TK, Tursen U, Kutlubay Z. Cu- COVID-19 pandemic. J Am Acad Dermatol.
18 Amatore F, Macagno N, Mailhe M, Demarez taneous manifestations in hospitalized pa- 2020 Sep;83(3):965–9.
B, Gaudy-Marqueste C, Grob JJ, et al. SARS- tients diagnosed as COVID-19. Dermatol 41 Alramthan A, Aldaraji W. Two cases of
CoV-2 infection presenting as a febrile rash. J Ther (Heidelb). 2020 Jun;24:e13896. COVID-19 presenting with a clinical picture
Eur Acad Dermatol Venereol. 2020 Jul; 30 Genovese G, Colonna C, Marzano AV. Vari- resembling chilblains: first report from the
34(7):e304–6. cella-like exanthem associated with COV- Middle East. Clin Exp Dermatol. 2020 Aug;
19 Shanshal M. Low-dose systemic steroids, an ID-19 in an 8-year-old girl: A diagnostic clue? 45(6):746–8.
emerging therapeutic option for COVID- Pediatr Dermatol. 2020 May;37(3):435–6. 42 Fernandez-Nieto D, Jimenez-Cauhe J, Su-
19-related urticaria. J Dermatolog Treat. 2020 31 Fernandez-Nieto D, Ortega-Quijano D, arez-Valle A, Moreno-Arrones OM, Saceda-
Jul; 16: 1–2. DOI: 10.1080/09546634.2020. Jimenez-Cauhe J, Burgos-Blasco P, de Corralo D, Arana-Raja A, et al. Characteriza-
1795062. Perosanz-Lobo D, Suarez-Valle A, et al. Clin- tion of acute acral skin lesions in nonhospital-
20 De Giorgi V, Recalcati S, Jia Z, Chong W, ical and histological characterization of vesic- ized patients: A case series of 132 patients
Ding R, Deng Y, et al. Cutaneous manifesta- ular COVID-19 rashes: a prospective study in during the COVID-19 outbreak. J Am Acad
tions related to coronavirus disease 2019 a tertiary care hospital. Clin Exp Dermatol. Dermatol. 2020 Jul;83(1):e61–3.
(COVID-19): A prospective study from Chi- 2020 May;45(7):872–5. 43 Bouaziz JD, Duong TA, Jachiet M, Velter C,
na and Italy. J Am Acad Dermatol. 2020 Aug; 32 Mahé A, Birckel E, Merklen C, Lefèbvre P, Lestang P, Cassius C, et al. Vascular skin
83(2):674–5. Hannedouche C, Jost M, et al. Histology of symptoms in COVID-19: a French observa-
21 Rivera-Oyola R, Koschitzky M, Printy R, Liu skin lesions establishes that the vesicular rash tional study. J Eur Acad Dermatol Venereol.
S, Stanger R, Golant AK, et al. Dermatologic associated with COVID-19 is not ‘varicella- 2020 Apr; 34(9): https://doi.org/10.1111/
findings in 2 patients with COVID-19. JAAD like’. J Eur Acad Dermatol Venereol. 2020 jdv.16544.
Case Rep. 2020 Apr;6(6):537–9. Oct;34(10):e559–61. 44 de Masson A, Bouaziz JD, Sulimovic L, Cas-
22 Jimenez-Cauhe J, Ortega-Quijano D, Prieto- 33 Trellu LT, Kaya G, Alberto C, Calame A, sius C, Jachiet M, Ionescu MA, et al.; SNDV
Barrios M, Moreno-Arrones OM, Fernandez- McKee T, Calmy A. Clinicopathologic As- (French National Union of Dermatologists-
Nieto D. Reply to “COVID-19 can present pects of a Papulovesicular Eruption in a Pa- Venereologists). Chilblains is a common cu-
with a rash and be mistaken for dengue”: pe- tient With COVID-19. JAMA Dermatol. 2020 taneous finding during the COVID-19 pan-
techial rash in a patient with COVID-19 in- Aug;156(8):922–4. demic: A retrospective nationwide study from
fection. J Am Acad Dermatol. 2020 Aug; 34 Tammaro A, Adebanjo GA, Parisella FR, Pez- France. J Am Acad Dermatol. 2020 Aug;
83(2):e141–2. zuto A, Rello J. Cutaneous manifestations in 83(2):667–70.
23 Najarian DJ. Morbilliform exanthem associ- COVID-19: the experiences of Barcelona and 45 Cordoro KM, Reynolds SD, Wattier R, Mc-
ated with COVID-19. JAAD Case Rep. 2020 Rome. J Eur Acad Dermatol Venereol. 2020 Calmont TH. Clustered cases of acral pernio-
Apr;6(6):493–4. Jul;34(7):e306–7. sis: clinical features, histopathology, and rela-
24 Català A, Galván-Casas C, Carretero-Hernán- 35 Elsaie ML, Nada HA. Herpes zoster (shingles) tionship to COVID-19. Pediatr Dermatol.
dez G, Rodríguez-Jiménez P, Fernández-Nie- complicating the course of COVID-19 infec- 2020 May;37(3):419–23.
to D, Rodríguez-Villa A, et al. Maculopapular tion. J Dermatolog Treat. DOI: 10.1080/ 46 Fernandez-Nieto D, Ortega-Quijano D, Su-
eruptions associated to COVID-19: A sub- 09546634.2020.1782823. Epub 2020 Oct 12. arez-Valle A, Burgos-Blasco P, Jimenez-
analysis of the COVID-Piel study [Online 36 Lim SY, Tey HL. Response to ‘Classification Cauhe J, Fernandez-Guarino M. Comment
ahead of print]. Dermatol Ther (Heidelb). of the cutaneous manifestations of COV- on: “To consider varicella-like exanthem as-
2020 Aug;e14170. ID-19: a rapid prospective nationwide con- sociated with COVID-19, virus varicella zos-
25 Gianotti R, Veraldi S, Recalcati S, Cusini M, sensus study in Spain with 375 cases’: vesic- ter and virus herpes simplex must be ruled
Ghislanzoni M, Boggio F, et al. Cutaneous ular eruption in COVID-19 - to exclude var- out. Characterization of herpetic lesions in
Clinico-Pathological Findings in three COV- icella. Br J Dermatol. 2020 Oct; 183(4): hospitalized COVID-19 patients”. J Am Acad
ID-19-Positive Patients Observed in the Met- 790–1. Dermatol. 2020 Sep;83(3):e257–9.
10 Dermatology 2021;237:1–12 Genovese/Moltrasio/Berti/Marzano
DOI: 10.1159/000512932
47 Freeman EE, McMahon DE, Lipoff JB, Rosen- 59 Denina M, Pellegrino F, Morotti F, Coppo P, Severe COVID-19. JAMA Dermatol. 2020
bach M, Kovarik C, Takeshita J, et al.; Ameri- Bonsignori IM, Garazzino S, et al. All that glis- Sep;156(9):1–3.
can Academy of Dermatology Ad Hoc Task ters is not COVID: low prevalence of serocon- 72 Bosch-Amate X, Giavedoni P, Podlipnik S,
Force on COVID-19. Pernio-like skin lesions version against SARS-CoV-2 in a pediatric co- Andreu-Febrer C, Sanz-Beltran J, Garcia-
associated with COVID-19: A case series of hort of patients with chilblain-like lesions. J Herrera A, et al. Retiform purpura as a derma-
318 patients from 8 countries. J Am Acad Am Acad Dermatol. 2020 Dec;83(6):1751–53. tological sign of coronavirus disease 2019
Dermatol. 2020 Aug;83(2):486–92. 60 Ko CJ, Harigopal M, Damsky W, Gehlhausen (COVID-19) coagulopathy. J Eur Acad Der-
48 Deutsch A, Blasiak R, Keyes A, Wu J, Marmon JR, Bosenberg M, Patrignelli R, et al. Perniosis matol Venereol. 2020 Oct;34(10):e548–9.
S, Asrani F, et al. Covid toes: phenomenon or during the COVID-19 pandemic: negative 73 Magro C, Mulvey JJ, Berlin D, Nuovo G, Salva-
epiphenomenon? J Am Acad Dermatol. 2020; anti-SARS-CoV-2 immunohistochemistry in tore S, Harp J, et al. Complement associated mi-
83(5):e347–e348. six patients and comparison to perniosis be- crovascular injury and thrombosis in the patho-
49 Zhou Z, Ren L, Zhang L, Zhong J, Xiao Y, Jia fore the emergence of SARS-CoV-2 [Online genesis of severe COVID-19 infection: A report
Z, et al. Overly exuberant innate immune re- ahead of print]. J Cutan Pathol. 2020 Aug; of five cases. Transl Res. 2020 Jun;220:1–13.
sponse to SARS-CoV-2 infection. SSRN Elec- 47(11):997–1002. 74 Magro C, Mulvey JJ, Laurence J, Sanders S,
tronic J. 2020; DOI: 10.2139/ssrn.3551623. 61 Le Cleach L, Dousset L, Assier H, Fourati S, Crowson N, Grossman M, et al. The differing
50 Kaya G, Kaya A, Saurat JH. Clinical and His- Barbarot S, Boulard C, et al.; French Society of pathophysiologies that underlie COVID-19
topathological Features and Potential Patho- Dermatology. Most chilblains observed dur- associated perniosis and thrombotic retiform
logical Mechanisms of Skin Lesions in COV- ing the COVID-19 outbreak occur in patients purpura: a case series. Br J Dermatol. 2020
ID-19: review of the Literature. Dermatopa- who are negative for COVID-19 on poly- Jul;bjd.19415.
thology (Basel). 2020 Jun;7(1):3–16. merase chain reaction and serology testing. Br 75 Cugno M, Meroni PL, Gualtierotti R, Griffini
51 Piccolo V, Neri I, Filippeschi C, Oranges T, J Dermatol. 2020 Nov;183(5):866–74. S, Grovetti E, Torri A, et al. Complement ac-
Argenziano G, Battarra VC, et al. Chilblain- 62 Lesort C, Kanitakis J, Villani A, Ducroux E, tivation in patients with COVID-19: A novel
like lesions during COVID-19 epidemic: a Bouschon P, Fattouh K, et al. COVID-19 and therapeutic target. J Allergy Clin Immunol.
preliminary study on 63 patients. J Eur Acad outbreak of chilblains: are they related? J Eur 2020 Jul;146(1):215–7.
Dermatol Venereol. 2020 Jul;34(7):e291–3. Acad Dermatol Venereol. 2020 Jun;jdv.16779. 76 Joob B, Wiwanitkit V. COVID-19 can present
52 Proietti I, Tolino E, Bernardini N, Mambrin 63 Roca-Ginés J, Torres-Navarro I, Sánchez-Ar- with a rash and be mistaken for dengue. J Am
A, Balduzzi V, Marchesiello A, et al. Auricle ráez J, Abril-Pérez C, Sabalza-Baztán O, Par- Acad Dermatol. 2020 May;82(5):e177.
perniosis as a manifestation of Covid-19 in- do-Granell S, et al. Assessment of Acute Acral 77 Negrini S, Guadagno A, Greco M, Parodi A,
fection. Dermatol Ther (Heidelb). 2020 Lesions in a Case Series of Children and Ado- Burlando M. An unusual case of bullous
Jul;e14089. lescents During the COVID-19 Pandemic. haemorrhagic vasculitis in a COVID-19 pa-
53 Navarro L, Andina D, Noguera-Morel L, JAMA Dermatol. 2020 Sep;156(9):992–7. tient. J Eur Acad Dermatol Venereol. 2020
Hernández-Martín A, Colmenero I, Torrelo 64 Colmenero I, Santonja C, Alonso-Riaño M, Jun;jdv.16760.
A. Dermoscopy features of COVID-19-relat- Noguera-Morel L, Hernández-Martín A, An- 78 Del Giudice P, Boudoumi D, Le Guen B, Re-
ed chilblains in children and adolescents. J dina D, et al. SARS-CoV-2 endothelial infec- verte M, Gutnecht J, Lacour JP, et al. Cata-
Eur Acad Dermatol Venereol. 2020 tion causes COVID-19 chilblains: histopatho- strophic acute bilateral lower limbs necrosis
Jul;jdv.16800. logical, immunohistochemical and ultra- associated with COVID-19 as a likely conse-
54 Kanitakis J, Lesort C, Danset M, Jullien D. structural study of seven paediatric cases. Br J quence of both vasculitis and coagulopathy.
Chilblain-like acral lesions during the COV- Dermatol. 2020 Oct;183(4):729–37. J Eur Acad Dermatol Venereol. 2020
ID-19 pandemic (“COVID toes”): Histologic, 65 Ladha MA, Luca N, Constantinescu C, Naert Jun;jdv.16763.
immunofluorescence, and immunohisto- K, Ramien ML. Approach to chilblains during 79 Caputo V, Schroeder J, Rongioletti F. A gen-
chemical study of 17 cases. J Am Acad Der- the COVID-19 pandemic. J Cutan Med Surg. eralized purpuric eruption with histopatho-
matol. 2020 Sep;83(3):870–5. 2020 Sep/Oct;24(5):504–17. logic features of leucocytoclastic vasculitis in
55 Locatelli AG, Robustelli Test E, Vezzoli P, Ca- 66 Griffiths C, Barker J, Bleiker T, Chalmers R, a patient severely ill with COVID-19. J Eur
rugno A, Moggio E, Consonni L, et al. Histo- Creamer D. Rook’s textbook of dermatology. Acad Dermatol Venereol. 2020 Oct;
logic features of long-lasting chilblain-like le- 9th ed, rev. Hoboken: Wiley-Blackwell; 2016. 34(10):e579–81.
sions in a paediatric COVID-19 patient. J Eur 67 Khalil S, Hinds BR, Manalo IF, Vargas IM, 80 Karaca Z, Yayli S, Çalışkan O. A unilateral
Acad Dermatol Venereol. 2020 Aug; Mallela S, Jacobs R. Livedo reticularis as a pre- purpuric rash in a patient with COVID-19 in-
34(8):e365–8. senting sign of severe acute respiratory syn- fection. Dermatol Ther (Heidelb). 2020 Jul;
56 Caselli D, Chironna M, Loconsole D, Nigri L, drome coronavirus 2 infection. JAAD Case 33(4):e13798.
Mazzotta F, Bonamonte D, et al. No evidence Rep. 2020 Sep;6(9):871–4. 81 García-Gil MF, Monte Serrano J, García Gar-
of SARS-CoV-2 infection by polymerase 68 Manalo IF, Smith MK, Cheeley J, Jacobs R. A cía M, Barra Borao V, Matovelle Ochoa C,
chain reaction or serology in children with dermatologic manifestation of COVID-19: Ramirez-Lluch M, et al. Acral purpuric le-
pseudo-chilblain [Online ahead of print]. Br J transient livedo reticularis. J Am Acad Der- sions associated with coagulation disorders
Dermatol. 2020 Oct;183(4):784–5. matol. 2020 Aug;83(2):700. during the COVID-19 pandemic. Int J Der-
57 Herman A, Peeters C, Verroken A, Tromme 69 Verheyden M, Grosber M, Gutermuth J, matol. 2020 Sep;59(9):1151–2.
I, Tennstedt D, Marot L, et al. Evaluation of Velkeniers B. Relapsing symmetric livedo re- 82 Larrondo J, Cabrera R, Gosch M, Larrondo F,
Chilblains as a Manifestation of the COV- ticularis in a patient with COVID-19 infec- Aylwin M, Castro A. Papular-purpuric exan-
ID-19 Pandemic. JAMA Dermatol. 2020 Sep; tion. J Eur Acad Dermatol Venereol. 2020 them in a COVID-19 patient: clinical and der-
156(9):998–1003. Jun;jdv.16773. moscopic description. J Eur Acad Dermatol
58 Docampo-Simón A, Sánchez-Pujol MJ, Juan- 70 Chibane S, Gibeau G, Poulin F, Tessier P, Venereol. 2020 Oct;34(10):e570–2.
Carpena G, Palazón-Cabanes JC, Vergara-De Goulet M, Carrier M, et al. Hyperacute multi- 83 Jimenez-Cauhe J, Ortega-Quijano D, Carret-
Caso E, Berbegal L, et al. Are chilblain-like ac- organ thromboembolic storm in COVID-19: ero-Barrio I, Suarez-Valle A, Saceda-Corralo
ral skin lesions really indicative of COV- a case report. J Thromb Thrombolysis. 2020 D, Moreno-Garcia Del Real C, et al. Erythema
ID-19? A prospective study and literature re- Jun;6:1–4. multiforme-like eruption in patients with
view. J Eur Acad Dermatol Venereol. 2020 71 Droesch C, Do MH, DeSancho M, Lee EJ, COVID-19 infection: clinical and histological
May; 34(9): https://doi.org/10.1111/jdv. Magro C, Harp J. Livedoid and Purpuric Skin findings. Clin Exp Dermatol. 2020 May;45(7):
16665. Eruptions Associated With Coagulopathy in 892–5.
COVID-19-Associated Skin Dermatology 2021;237:1–12 11
Manifestations DOI: 10.1159/000512932
84 Ehsani AH, Nasimi M, Bigdelo Z. Pityriasis 88 Almutairi A, Alfaleh M, Alasheikh M. Derma- 92 Criado PR, Abdalla BM, de Assis IC, van Blar-
rosea as a cutaneous manifestation of COV- tological Manifestations in Patients With cum de Graaff Mello C, Caputo GC, Vieira IC.
ID-19 infection. J Eur Acad Dermatol Vene- SARS-CoV-2: A Systematic Review. Cureus. Are the cutaneous manifestations during or
reol. 2020 May;34(9): https://doi.org/10.1111/ 2020 Jul;12(7):e9446. due to SARS-CoV-2 infection/COVID-19
jdv.16579. 89 Seirafianpour F, Sodagar S, Pour Mohammad frequent or not? Revision of possible patho-
85 Gupta A, Gill A, Sharma M, Garg M. Multi- A, Panahi P, Mozafarpoor S, Almasi S, et al. physiologic mechanisms. Inflamm Res. 2020
System Inflammatory Syndrome in a Child Cutaneous manifestations and consider- Aug;69(8):745–56.
Mimicking Kawasaki Disease. J Trop Pediatr. ations in COVID-19 pandemic: A systematic 93 Novak N, Peng W, Naegeli MC, Galván C,
2020 Aug;fmaa060. review. Dermatol Ther (Heidelb). 2020 Kolm-Djamei I, Brüggen C, et al. SARS-
86 Shanshal M. COVID-19 related anagen efflu- Jul;e13986. CoV-2, COVID-19, skin and immunology -
vium. J Dermatolog Treat. 2020 Jul; 16: 1–2. 90 Zhao Q, Fang X, Pang Z, Zhang B, Liu H, What do we know so far? Allergy. 2020
DOI: 10.1080/09546634.2020.1792400. Zhang F. COVID-19 and cutaneous manifes- Jul;all.14498.
87 Llamas-Velasco M, Chicharro P, Rodríguez- tations: a systematic review. J Eur Acad Der- 94 Herman A, Matthews M, Mairlot M, Nobile
Jiménez P, Martos-Cabrera L, De Argila D, matol Venereol. DOI: 10.1111/jdv.16778. L, Fameree L, Jacquet LM, et al. Drug reaction
Fernández-Figueras M, et al. Comment on Epub 2020 Jun 28. with eosinophilia and systemic symptoms
‘Clinical and histological characterization of 91 Wang Y, Fang R, Zhang H, Tang K, Sun Q. syndrome in a patient with COVID-19. J Eur
vesicular COVID-19 rashes: a prospective Contributions of dermatologists to COV- Acad Dermatol Venereol. 2020 Jul;jdv.16838.
study in a tertiary care hospital’. Pseudoher- ID-19 research: A brief systematic review. 95 Delaleu J, Deniau B, Battistella M, de Masson
petic Grover disease seems to occur in pa- Dermatol Ther (Heidelb). 2020 Jul; A, Bensaid B, Jachiet M, et al. Acute general-
tients with COVID-19 infection. Clin Exp 33(4):e13713. ized exanthematous pustulosis induced by
Dermatol. 2020 May;45(7):896–8. hydroxychloroquine prescribed for COV-
ID-19. J Allergy Clin Immunol Pract. 2020
Sep;8(8):2777–9.
12 Dermatology 2021;237:1–12 Genovese/Moltrasio/Berti/Marzano
DOI: 10.1159/000512932
You might also like
- Anatomy & Physiology: Essentials ofDocument69 pagesAnatomy & Physiology: Essentials ofclyde i am100% (1)
- Dermatofitosis FitzpatrickDocument28 pagesDermatofitosis FitzpatrickFadli IlhamNo ratings yet
- Autoimmune Pancreatitis: Dr. Arun Gnyawali Resident, General SurgeryDocument27 pagesAutoimmune Pancreatitis: Dr. Arun Gnyawali Resident, General SurgeryArun GnyawaliNo ratings yet
- A Distinctive Skin Rash LTEDocument2 pagesA Distinctive Skin Rash LTEeva yustianaNo ratings yet
- Skin Rashes Guideline in Paediatric Emergency Department (Cross Site)Document33 pagesSkin Rashes Guideline in Paediatric Emergency Department (Cross Site)Eskilda LucildaNo ratings yet
- Digging Up The Bones - MicrobiologyDocument31 pagesDigging Up The Bones - MicrobiologyMossa Di Base100% (1)
- MeningococcemiaDocument5 pagesMeningococcemiazzoOeeNo ratings yet
- Cutaneous Manifestations of COVID-19: Review ArticleDocument9 pagesCutaneous Manifestations of COVID-19: Review ArticleMudassar SattarNo ratings yet
- Skin Lessions Covid-19Document15 pagesSkin Lessions Covid-19JUAN PABLO DE JESUS CASTRO MORANo ratings yet
- Sep2020-Review and ClassificationDocument23 pagesSep2020-Review and ClassificationSAJIN ALEXANDERNo ratings yet
- The Clinical Spectrum of COVID-19eassociated Cutaneous Manifestations: An Italian Multicenter Study of 200 Adult PatientsDocument8 pagesThe Clinical Spectrum of COVID-19eassociated Cutaneous Manifestations: An Italian Multicenter Study of 200 Adult PatientsBotez MartaNo ratings yet
- DTH 34 0Document18 pagesDTH 34 0nadiancupNo ratings yet
- Covid Induced CVDocument23 pagesCovid Induced CVriskiNo ratings yet
- Idcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaDocument3 pagesIdcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaMuhamad ZenNo ratings yet
- Spectrum of Clinicopathologic Findings in COVID-19-induced Skin LesionsDocument9 pagesSpectrum of Clinicopathologic Findings in COVID-19-induced Skin LesionsggenesisNo ratings yet
- Tammaro2020 Covid 19Document7 pagesTammaro2020 Covid 19eva yustianaNo ratings yet
- COVID-19 Fact Sheet ENGDocument38 pagesCOVID-19 Fact Sheet ENGIl Principio CarinoNo ratings yet
- Cutaneous Signs in COVID-19 Patients: A ReviewDocument6 pagesCutaneous Signs in COVID-19 Patients: A Reviewϟ Orbi SinkaNo ratings yet
- Sachdeva 2020Document7 pagesSachdeva 2020CalvinNo ratings yet
- Todj 14 28Document3 pagesTodj 14 28Siva Venkata RamanaNo ratings yet
- Clinical and Histological Characterization of Vesicular COVID-19 Rashes: A Prospective Study in A Tertiary Care HospitalDocument18 pagesClinical and Histological Characterization of Vesicular COVID-19 Rashes: A Prospective Study in A Tertiary Care HospitalANA KARINA ALVARADO OSORIONo ratings yet
- Huynh2022 Article CutaneousManifestationsOfSARSDocument10 pagesHuynh2022 Article CutaneousManifestationsOfSARSgiselaNo ratings yet
- Jurnal Reading Kulit (Jenifer Johana Paath 201383019)Document34 pagesJurnal Reading Kulit (Jenifer Johana Paath 201383019)Mega BagdadNo ratings yet
- COVID-19 Cutaneous Manifestations: Simplifying The ConfusionDocument2 pagesCOVID-19 Cutaneous Manifestations: Simplifying The Confusionanis utamiNo ratings yet
- COVID-19 Fact Sheet ENGDocument32 pagesCOVID-19 Fact Sheet ENGjuancvlNo ratings yet
- Skin Manifestations of COVID-19 in Children Part 1Document7 pagesSkin Manifestations of COVID-19 in Children Part 1Alfi RahmatikaNo ratings yet
- COVID-19 Fact Sheet ENG PDFDocument27 pagesCOVID-19 Fact Sheet ENG PDFLuis Ricardo Soto JimenezNo ratings yet
- Letters: Enanthem in Patients With COVID-19 and Skin RashDocument2 pagesLetters: Enanthem in Patients With COVID-19 and Skin RashDonate 049No ratings yet
- The Role of Emergency Radiology in COVID-19Document13 pagesThe Role of Emergency Radiology in COVID-19ViviApriliaNo ratings yet
- Erythema Multiforme Eruption Due To SARS-COV 2Document3 pagesErythema Multiforme Eruption Due To SARS-COV 2Irzam PratamaNo ratings yet
- Cutaneous and Allergic Reactions Due To COVID-19 Vaccinations: A ReviewDocument9 pagesCutaneous and Allergic Reactions Due To COVID-19 Vaccinations: A ReviewAnis RanisNo ratings yet
- COVID-19 and Dermatology: A Comprehensive Guide For DermatologistsDocument7 pagesCOVID-19 and Dermatology: A Comprehensive Guide For DermatologistsAna Karina Alvarado OsorioNo ratings yet
- Case 3. Dermatomycosis - Scabies For Tutor 2020 - MergedDocument21 pagesCase 3. Dermatomycosis - Scabies For Tutor 2020 - MergedRaihan IsvandiarNo ratings yet
- Dermatopathology For The Surgical Pathologist A Pattern-Based Approach To The Diagnosis of Inflammatory Skin Disorders Part IDocument21 pagesDermatopathology For The Surgical Pathologist A Pattern-Based Approach To The Diagnosis of Inflammatory Skin Disorders Part IkarigargiuloNo ratings yet
- COVID-19 and Cutaneous Manifestations: ReferencesDocument1 pageCOVID-19 and Cutaneous Manifestations: Referenceseva yustianaNo ratings yet
- Cutaneous Manifestation Covid 19Document9 pagesCutaneous Manifestation Covid 19eva yustianaNo ratings yet
- Drug For COVID 19Document12 pagesDrug For COVID 19gygyNo ratings yet
- Oral Manifestations in Covid19Document2 pagesOral Manifestations in Covid19La redazione Tp24No ratings yet
- Ivermectina - Profilaxis Covid-19 - DR HirschDocument8 pagesIvermectina - Profilaxis Covid-19 - DR HirschAlheni Fabiola Miranda GomezNo ratings yet
- Orbital Apex Syndrome - A ReviewDocument15 pagesOrbital Apex Syndrome - A ReviewValeria KuchkaryanNo ratings yet
- Escholarship UC Item 55d3f43cDocument5 pagesEscholarship UC Item 55d3f43cDhessy SusantoNo ratings yet
- Conjunctiva (Hira FJ)Document26 pagesConjunctiva (Hira FJ)Minahil ShahidNo ratings yet
- PIIS1201971221003702Document6 pagesPIIS1201971221003702FlitongNo ratings yet
- MicrofinalDocument7 pagesMicrofinaljwanaNo ratings yet
- Prevalence and Clinical Features of Secondary Skin Lesions in Septic Patients With Bloodstream InfectionsDocument8 pagesPrevalence and Clinical Features of Secondary Skin Lesions in Septic Patients With Bloodstream Infections장민욱No ratings yet
- COVID-19 Outbreak: An Overview: Antimicrobial Section / ReviewDocument9 pagesCOVID-19 Outbreak: An Overview: Antimicrobial Section / ReviewStephanie ChristineNo ratings yet
- Oamjms 10b 1869Document7 pagesOamjms 10b 1869christina kusuma reniNo ratings yet
- Jurnal Ing MK 4Document10 pagesJurnal Ing MK 4Iffah AlhikmahNo ratings yet
- Rashh CovidDocument7 pagesRashh CovidVivi Permana SarieNo ratings yet
- Dermatitis Linearis: Vesicating Dermatosis Caused by Series and ReviewDocument8 pagesDermatitis Linearis: Vesicating Dermatosis Caused by Series and ReviewrositaNo ratings yet
- Tan 2018Document8 pagesTan 2018Bagus Putra KurniawanNo ratings yet
- Dermatology Study Guide 2023-IvDocument7 pagesDermatology Study Guide 2023-IvUnknown ManNo ratings yet
- 2022 Article 2521Document7 pages2022 Article 2521haytham aliNo ratings yet
- Epidemiological Characterization of Dermatomycosis in EthiopiaDocument7 pagesEpidemiological Characterization of Dermatomycosis in EthiopiaMini LaksmiNo ratings yet
- Follow Up of Skin Lesions During The Evolution of COVID 19 A CaseDocument4 pagesFollow Up of Skin Lesions During The Evolution of COVID 19 A CaseZihan ZetiraNo ratings yet
- 2019 MekoguemDocument5 pages2019 MekoguemkropotkineNo ratings yet
- Virales Deramtology EssentialsDocument11 pagesVirales Deramtology EssentialsJuan Pablo LondoñoNo ratings yet
- Cutaneus Manifestation of Coronavirus Disease 2019Document7 pagesCutaneus Manifestation of Coronavirus Disease 2019Maria AgathaNo ratings yet
- KAYE ROJAS Skin Infection BSN 1 Y2 3Document10 pagesKAYE ROJAS Skin Infection BSN 1 Y2 3HERLIN HOBAYANNo ratings yet
- Cutaneous Manifestations and Issues Related To Dermatologic CareDocument10 pagesCutaneous Manifestations and Issues Related To Dermatologic CareCarlos Huaman ZevallosNo ratings yet
- VitiligoFrom EverandVitiligoMauro PicardoNo ratings yet
- Neuroimaging of Covid-19. First Insights based on Clinical CasesFrom EverandNeuroimaging of Covid-19. First Insights based on Clinical CasesSimonetta Gerevini M.D.No ratings yet
- Parasitology Notes - SLU Lictag FrancesDocument49 pagesParasitology Notes - SLU Lictag FrancesJmarc JubiladoNo ratings yet
- Syphilitic Uveitis - EyeWikiDocument5 pagesSyphilitic Uveitis - EyeWikitgrrwccj98No ratings yet
- Bavituximab MOA BrochureDocument3 pagesBavituximab MOA BrochureinternetforumuserNo ratings yet
- Part 2. Causes of DiseasesDocument12 pagesPart 2. Causes of DiseasesKakuru Joseph mNo ratings yet
- Opportunistic Mycoses: Classification Organisms YeastDocument45 pagesOpportunistic Mycoses: Classification Organisms Yeastrevathidadam55555No ratings yet
- Synflorix: What Is in This Leaflet?Document3 pagesSynflorix: What Is in This Leaflet?A Nizar MasbukhinNo ratings yet
- List NajeebDocument22 pagesList NajeebM Marliando Satria PangestuNo ratings yet
- Antiprotozoal and Antihelminthic Drugs - HandoutDocument21 pagesAntiprotozoal and Antihelminthic Drugs - HandoutdonzNo ratings yet
- (Pediaii) - 021 - Disorders of The Respiratory TractDocument17 pages(Pediaii) - 021 - Disorders of The Respiratory TractdoktoraronaNo ratings yet
- KA VaccinationDocument9 pagesKA VaccinationVictor GaborNo ratings yet
- Blood Trasnfusions 1Document7 pagesBlood Trasnfusions 1Silvia RodríguezNo ratings yet
- Unknown - Unknown - Global Vaccine Market Report Overview of MI4A-annotatedDocument14 pagesUnknown - Unknown - Global Vaccine Market Report Overview of MI4A-annotatedAntonio MoncayoNo ratings yet
- MGA VACCINE NA SAKOP NG NIP: BCG Birth Dose, Hepatitis B Birth Dose, OralDocument3 pagesMGA VACCINE NA SAKOP NG NIP: BCG Birth Dose, Hepatitis B Birth Dose, OralVanessa AbboudNo ratings yet
- Daftar Kode Panyakit: Kode Bedah Kode Interna Kode NeuroDocument1 pageDaftar Kode Panyakit: Kode Bedah Kode Interna Kode NeuroMutemjNo ratings yet
- Infection Control Risk Assessment Tool 1208Document7 pagesInfection Control Risk Assessment Tool 1208sostro0% (1)
- Virus Filoviridae PDFDocument11 pagesVirus Filoviridae PDFErika MNo ratings yet
- Isolation and Quarantine Protocol Changes in Jefferson CountyDocument1 pageIsolation and Quarantine Protocol Changes in Jefferson CountyNewzjunkyNo ratings yet
- 220-Management of Genital Herpes in Pregnancy, 2020Document10 pages220-Management of Genital Herpes in Pregnancy, 2020waleedaliNo ratings yet
- Food Allergy NestleDocument11 pagesFood Allergy NestleRositaMagda MataNo ratings yet
- Mtle - Blood Banking (Revised)Document25 pagesMtle - Blood Banking (Revised)docv526No ratings yet
- Communicable DiseaseDocument9 pagesCommunicable DiseaseSusan HepziNo ratings yet
- Immunology Serology in Laboratory Medicine Mary Turgeon Edd Mlsascpcm Full ChapterDocument67 pagesImmunology Serology in Laboratory Medicine Mary Turgeon Edd Mlsascpcm Full Chapterantonio.amos633100% (10)
- Communicable DiseasesDocument7 pagesCommunicable DiseasesRaisa Robelle Quicho100% (1)
- RhinosinusitisDocument8 pagesRhinosinusitisAyuNo ratings yet
- Can Mothers Breastfeed During The COVIDDocument4 pagesCan Mothers Breastfeed During The COVIDAnisa RamdhiniNo ratings yet
- 2022 1 Sim Enem-03-04 Linguag e Cien Humanas Resolvido-3-26Document34 pages2022 1 Sim Enem-03-04 Linguag e Cien Humanas Resolvido-3-26André FilhoNo ratings yet
- Covid 19 AwarenessDocument13 pagesCovid 19 AwarenessAsorihm MhirosaNo ratings yet