Professional Documents
Culture Documents
2017 Pneumonia Irrational Use of Antibiotics
2017 Pneumonia Irrational Use of Antibiotics
Uploaded by
Reka Vikaria AnggreliaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2017 Pneumonia Irrational Use of Antibiotics
2017 Pneumonia Irrational Use of Antibiotics
Uploaded by
Reka Vikaria AnggreliaCopyright:
Available Formats
Paediatrica Indonesiana
p-ISSN 0030-9311; e-ISSN 2338-476X; Vol.57, No.4(2017). p. 211-5 ; doi: http://dx.doi.org/10.14238/pi57.4.2017.211-5
Original Article
Irrational use of antibiotics and clinical outcomes in
children with pneumonia
Yusuf, Indah Kartika Murni, Amalia Setyati
B
Abstract acterial pneumonia is the main cause of
Background Pneumonia is a major cause of morbidity and morbidity and mortality in children below 5
mortality in children under five. Antibiotic treatment must be years of age. The incidence and its mortality
started immediately in children with pneumonia. The irrational
use of antibiotics may increase morbidity and mortality in children
are higher in developing countries. The
with pneumonia. incidence of bacterial pneumonia in children below 5
Obejctive To determine the prevalence of the irrational use of years of age was estimated to be 0.29 episodes each year
antibiotics and clinical outcomes in children with pneumonia. for children in developing countries, and 0.05 episodes
Methods We conducted a cross-sectional study in children with
pneumonia who were admitted to the Pediatric Ward or PICU for children in developed countries.1 In 2013, there
at Dr. Sardjito Hospital, Yogyakarta, from December 2010 to were 156 million new episodes for the year worldwide,
February 2013. Data were obtained from subjects’ medical records. with as many as 151 million in developing countries.
Children with malnutrition, congenital heart defects, sepsis, Most cases were found in India (43 million), China (21
shock, central nervous system disorders, syndromes, or other
concomitant infections were excluded. million), Pakistan (10 million), as well as Bangladesh,
Results Of 46 children who fulfilled the inclusion criteria, 13 Indonesia, and Nigeria (6 million each).2
(28.3%) used antibiotics irrationally and 7 (15.2%) died. Most Antibiotic therapy must be started immediately
subjects were aged less than 1 year (25 subjects, 54.3%) and in children with suspected community-acquired
1 - < 5 years (18 subjects, 39.1%). The female to male ratio was
1:1. Most cases were referred from other hospitals (23 subjects, pneumonia (CAP) caused by bacteria.3 Inappropriate
50%). Twenty-eight (60.9%) subjects stayed in hospital > 7 days. antibiotic treatment may lead to greater expense, toxic
Ampicillin was the most common first-line, empirical antibiotic side effects, antibiotic resistance, and superinfections
used (32 subjects, 69.6%). Blood cultures were obtained in 20 that are difficult to treat. Thus, antibiotics should be
(43.5%) patients, yielding no growth in 16 subjects, coagulase-
negative staphylococci (CONS) in 3 subjects, and Pseudomonas
aeruginosa in 1 subject. The irrational use of antibiotics was
significantly associated with mortality in a univariate analysis [PR
6.35; (95%CI 1.40 to 28.69); P=0.006]. From the Department of Child Health, Gadjah Mada University Medical
Conclusion The irrational use of antibiotics is common among School/Dr. Sardjito Hospital, Yogyakarta, Central Java, Indonesia.
children with pneumonia and is significantly associated with
mortality. [Paediatr Indones. 2017;57:211-5 ; doi: http://dx.doi. Reprint requests to: Yusuf, Department of Child Health, Gadjah Mada
org/10.14238/pi57.4.2017.211-5 ]. University Medical School/Dr. Sardjito General Hospital, Yogyakarta.
Jalan Kesehatan No. 1 Sekip Yogyakarta 55284, Indonesia. Telp.
+62-813-11387443, +62-274-561616; Fax. +62-274-583745; Email:
yusuf_balfast@yahoo.co.id.
Keywords: antibiotic; irrational; pneumonia
Paediatr Indones, Vol. 57, No. 4, July 2017 • 211
Yusuf et al: Irrational use of antibiotics and clinical outcomes in children with pneumonia
used rationally for the treatment of pneumonia.4,5 of admission to the time of discharge, regardless of
Irrational use of antibiotics significantly increased primary outcome and classified into two categories:
morbidity and mortality in children with infections, 0-7 days or > 7 days. Type of case was classified
including pneumonia.6 Although antibiotics have an as community, if patients had come directly to the
important role in reducing mortality of pneumonia, hospital, referral, if patients were referred by another
research has been limited. We aimed to evaluate the hospital, or transfer, if patients were initially treated
irrational use of antibiotics and outcomes in children in the PICU.
with pneumonia at Sardjito Hospital. Data was described and analyzed with P values,
prevalence ratio (PR), 95% confidence intervals.
Bivariate analysis was done with Chi-square and
Methods Fisher’s tests. Statistical analysis was performed with
SPSS software. This study was approved by the Ethics
This cross-sectional study was conducted in the Committee for Medical Research, Gadjah Mada
Pediatric Ward and PICU of Sardjito Hospital, University Medical School.
Yogyakarta, Central Java, in November 2016. Subjects
were children with pneumonia treated according to
standard medical procedures of Sardjito Hospital, Results
aged 1 month - < 18 years, and hospitalized between
December 2010 and February 2013. Data were Fourty six children were fulfilled the inclusion
obtained from patients’ medical records. The exclusion criteria, of whom 13 (28.3%) received irrational use
criteria were children with malnutrition, congenital of antibiotics and 7 (15.2%) died. The characteristics
heart defects, sepsis, shock, central nervous system of subjects are shown in Table 1.
disorders, disease syndromes, or other concomitant
infections. The minimum required number of subjects Table 1. Characteristics of subjects
was calculated to be 46, with 0.05 confidence level Characteristics N=46
and 80% power. Gender, n(%)
The subjects’ basic characteristics were age, sex, Male 23 (50.0)
and case classification. The outcomes were classified Female 23 (50.0)
into primary (survived/died) and secondary (length Age, n(%)
< 1 year 25 (54.3)
of hospital stay, rational/irrational use of antibiotics, 1 - < 5 years 18 (39.1)
type of antibiotics used, first-line antibiotics, 5 - < 10 years 1 (2.2)
combination antibiotics, blood cultures, and types ≥ 10 years 2 (4.3)
of microorganisms). The independent variable was Type of case, n(%)
Community 21 (45.7)
the irrational use of antibiotics, while the dependent Referral 23 (50.0)
variables were primary outcomes (survived or died) PICU transfer 2 (4.3)
and the secondary outcomes of hospital length of stay
of 0-7 days or > 7 days.
Pneumonia was a diagnosis made by treating Data on primary outcomes, rationality of
clinicians and was written in medical records as a antibiotics, type of irrational use, length of stay, blood
final diagnosis based on ICD 10 of pneumonia which culture results, types of microorganisms, and empirical
was J18. The diagnosis of pneumonia in Dr. Sardjito therapy are shown in Table 2.
Hospital was made by clinical and radiological Univariate analysis of primary outcomes and
findings. The type of the pneumonia in this study was rationality of antibiotic use is shown in Table 3.
CAP. The irrational use of antibiotics was defined as Univariate analysis of length of stay and rationality
antibiotic use that was not in accordance with that of antibiotic use is shown in Table 4.
recommended for particular indications, dose, and/
or length of treatment. Length of stay was defined to
be the number of days hospitalization from the time
212 • Paediatr Indones, Vol. 57, No. 4, July 017
Yusuf et al: Irrational use of antibiotics and clinical outcomes in children with pneumonia
Table 2. Clinical outcomes Discussion
Outcomes N=46
Primary outcomes, n(%) Of 46 children with pneumonia, 7 (15.2%) died,
Survived 39 (84.8)
similar to that reported by Latumahina et al. (15%).1
Died 7 (15.2)
Thirteen of our subjects (28.3%) received irrational
Rationality of antibiotic use, n(%)
Irrational 13 (28.3) antibiotic treatment for pneumonia. A previous study
Spectrum/indication 12 (92.3) reported a similar 24% in Sardjito Hospital, although
Length of treatment 1 (7.0) higher percentages were reported in Mongolia (56.6%),
Dose 0
Rational 33 (7.17) Turkey (56.5%), and India (56%). These differences
Length of stay, n(%) may have been due to studying only children below 5
0-7 days 18 (39.1) years of age or including adults.4,7,8,9
> 7 days 28 (60.9) Most of our subjects were < 1 year of age (25;
Blood culture, n(%) 54.3%) or 1 - < 5 years old (18; 39.1%), with a 1:1
Culture 20 (43.5)
No growth 16
ratio of males to females. Pneumonia was found to be
Coagulase-negative staphylococcus 3 the main cause of morbidity and mortality in children
(CONS) 1 below 5 years by Latumahina et al. and the Indonesian
Pseudomonas aeruginosa 26 (56.5)
No culture
Ministry of Health.1,10
Most pneumonia was caused by infectious
First-line antibiotics, n(%)
Ampicillin 32 (69.6) agents, although non-infectious causes included food
Ceftriaxone 5 (10.9) or gastric acid aspiration, foreign bodies, hydrocarbon
Cefotaxime 8 (17.4) and lipoid agents, hypersensitivity reactions, drugs,
Imipenem 1 (2.2)
and radiation pneumonitis. Most of the time it was
Antibiotics combination, n(%)
Cefotaxime 1 (3.3) hard to find the cause of pneumonia, because invasive
Ceftazidime 1 (3.3) specimen collection was rarely, if ever, performed.
Cefixime 1 (3.3) Specimens from the upper respiratory tract or sputum
Chloramphenicol 14 (46.7)
Amikacin 2 (6.7)
are usually not accurate for determining the cause of
Gentamicin 11 (36.7) lower respiratory tract disease.11
Note: Antibiotics combination were given in 30 patients Treatment of pneumonia is based on the
causative agent and clinical findings,12 although,
Table 3. Univariate analysis of primary outcomes and generally, clinical signs do not help to differentiate
rationality of antibiotic use etiologies of pneumonia. Early identification of
Antibiotic Primary outcomes PR P etiology is also difficult, so antibiotics are usually
use Died Survived (95%CI) value chosen by an empirical approach. All patients in
Irrational 5 8 6.35 0.006 this study received empirical antibiotic treatment.
Rational 2 31 (1.40 to 28.69) Ampicillin was the most common first-line, empirical
antibiotic used (32; 69.6%), while the most common
combination antibiotics used were chloramphenicol
(14; 46.7%) and gentamicin (11; 36.7%). These
Table 4. Univariate analysis of length of stay and rationality
of antibiotic use
findings were in agreement with the World Health
Organization (WHO) and the Indonesian Pediatrics
Antibiotic Length of stay PR
use (95%CI) P Society (IPS) recommendations that children with
More than 0-7 days
7 days
value severe and very severe pneumonia be hospitalized,
receive ampicillin as the first-line treatment, and
Irrational 10 3 1.41 0.161
(0.92 to 2.17) be observed for next 24 to 72 hours. If the patient
Rational 2 31
has a good response, treatment must be continue
for 5 days. But if the patient becomes worse within
48 hours or experiences severe clinical conditions
(unable to eat/drink, vomiting at all feedings, seizure,
Paediatr Indones, Vol. 57, No. 4, July 2017 • 213
Yusuf et al: Irrational use of antibiotics and clinical outcomes in children with pneumonia
lethargy, unconsciousness, or cyanosis with respiratory aeruginosa. This result differed from the reported
distress), chloramphenicol must be added. Patients pneumonia etiologies in children of Streptococcus
with severe clinical conditions should directly be pneumoniae, Haemophilus influenza, and respiratory
given a combination of ampicillin-chloramphenicol or syncytial virus.16,17 Blood cultures in PICU patients
ampicillin-gentamicin. If the patient is unresponsive at Cipto Mangunkusumo Hospital (CMH), Jakarta,
to the above antibiotics, amikacin or cephalosporin were similar to our findings at Sardjito Hospital,
could be used.13 as those CMH patients had mostly Pseudomonas
We noted that empirical therapy was not always (33.1%), coagulase-negative staphylococcus (19.5%),
given according to the recommended protocol, and Klebsiella pneumoniae (13.3%).11 The most
such as with the use of cefotaxime, imipenem, and commonly found species in this study was coagulase-
ceftazidime. This finding may have been due to most negative staphylococcus (15%), but blood culture
cases (23; 50%) being referred from other hospitals or was performed in only 20 patients, 4 of which grew
directly treated in the PICU (2; 4.3%). The antibiotics bacteria. As such, these findings are too weak to be
used in other hospitals also might have influenced the basis of microorganism sensitivity data.
the sensitivity of microorganisms to antibiotics, as It has been shown that adequate antibiotic
increased antibiotic resistance among respiratory treatment shortens the length of stay and decreases
infectious agents might affect the choice of empirical mortality. The dilemma is that decreased antibiotic
treatment.14 usage decreases resistance, but delayed or inadequate
From 13 subjects who used antibiotics irrationally, treatment increases the mortality and morbidity of
almost all were considered irrational based on pneumonia, especially that caused by Gram-negative
spectrum of disease (12; 92.3%), while only 1 (7.7%) bacteria.18 We also found a significant association
was based on duration. There was no irrational use between irrational use of antibiotics and death (PR
based on dosage. However, these results were not 6.35; 95%CI 1.40 to 28.69; P=0.006).
subjected to a qualitative antibiotic evaluation using Antibiotic resistance and death outcome could
Gyssens pathway, that classifies antibiotic use into not be analyzed because only 20 subjects underwent
six categories: I. incorrect usage, IIa. incorrect dose, blood cultures. Those patients were the severe or very
IIb. incorrect intervals, IIc. incorrect route, IIIa. severe cases, so they did not reflect the general study
incorrect due to long duration, IIIb. incorrect due to population.
short duration, IVa. incorrect due to a more effective Athale et al. reported that inadequate empirical
antibiotic, IVb. incorrect due to a closer spectrum, V. antibiotics for 30 days length of stay resulted in higher
no indication for antibiotics, and VI. medical records mortality (11.1%) than did a 7-day length of stay
not complete enough to evaluate. The antibiotic is (3.7%). For delayed empirical therapy, there was no
correct if the evaluation matches with category I, but significant difference in mortality between 7 days or
incorrect if it is IIa, IIb, IIc, IIIa, IIIb, IVa, IVb, IVc, 30 days length of stay.19
IVd, V (II,III,IV,V).15 We used a 7-day limit for the length of stay
In developing countries, hospital microbiology outcome based on the standard duration of pneumonia
data of that could be used to guide patient management treatment of 5-7 days.13 Eighteen subjects (39.1%) had
is rare to non-existent. Specimen collection from the a 0-7-day length of stay; 28 subjects (60.9%) had a
lungs to assess the pneumonia etiology is not possible, > 7 day length of stay. No significant association
so specimens were taken from tracheal aspiration of was observed between irrational use of antibiotics
intubated patients. This specimen is not sensitive and length of stay, indicating that the severity of the
enough to define the pneumonia etiology. 11 In disease could influence the length of stay.
addition, blood cultures from pneumonia patients This study has several limitations. First, we
are not routinely performed, except in cases of very used retrospective data, so risk factors and outcome
severe pneumonia. In our study, 20 subjects had were taken from one point of time. Second, there
cultures started on the day of admission, but only was no precise data on the severity of pneumonia or
4/20 had positive findings: 3/20 coagulase-negative previous history of hospitalization, such as length of
staphylococcus (CONS) and 1/20 Pseudomonas stay or previous antibiotics used. Third, a qualitative
214 • Paediatr Indones, Vol. 57, No. 4, July 017
Yusuf et al: Irrational use of antibiotics and clinical outcomes in children with pneumonia
evaluation of antibiotic treatment was done with only Arch Dis Child. 2015;100:454-9.
3 parameters: incorrect spectrum/indication, dose, and 8. Dorj G, Hendrie D, Parsons R, Sunderland B. An evaluation
length of treatment, so the classification of irrational of prescribing practices for community-acquired pneumonia
antibiotic use was weak. (CAP) in Mongolia. BMC Health Serv Res. 2013;13:379.
In conclusion, irrational use of antibiotics in 9. Sachdev HP, Mahajan SC, Garg A. Improving antibiotic
children with pneumonia at Dr. Sardjito Hospital and bronchodilator prescription in children presenting with
is significantly associated with death, but we find difficult breathing: experience form an urban hospital in
no such relationship with length of stay. Irrational India. Indian Pediatr. 2001;38:827-38.
use of antibiotics was defined by simple clinical and 10. Kementerian Kesehatan. Data dan informasi tahun 2014
laboratory data that were used to diagnose pneumonia. (Profil Kesehatan Indonesia), Jakarta: Kementerian
Further study using Gyssens pathway, the degree of Kesehatan Republik Indonesia; 2015.
pneumonia severity, previous hospitalization history 11. Setyati A, Murni IK. Pola kuman pasien pneumonia di
(length of stay and antibiotic use), blood cultures for instalasi rawat intensif anak (IRIA) RSUP Dr. Sardjito. M
all subjects, and better study methods are needed. Med Indones. 2012;46:195-200.
12. Sectish TC, Charles GP. Pneumonia. In: Behrman RE, editor.
Nelson’s textbook of pediatrics. 18th ed. New York: WB
Conflict of Interest Saunders; 2007. p. 1795-9.
13. Kementerian Kesehatan RI/World Health Organization.
None declared. Pelayanan kesehatan anak di rumah sakit: Pedoman bagi
rumah sakit rujukan tingkat pertama di kabupaten /kota.
Jakarta: Kemenkes RI/WHO; 2009. p.86-93.
References 14. Widyaningsih R, Buntaran L. Pola kuman penyebab ventilator
associated pneumonia (VAP) dan sensitivitas terhadap
1. Latumahina ASN, Triasih R, Hermawan K. Pengembangan antibiotik di RSAB Harapan Kita. Sari Pediatri. 2012;13:384-
dan validasi skor prediksi kematian pada anak dengan 90.
pneumonia. [thesis]. [Yogyakarta]: Universitas Gadjah Mada; 15. Gyssens IC. Audits for monitoring the quality of antimicrobial
2016. prescription. In: Van der Meer JW, Gould IM, editors.
2. Walker CL, Rudan I, Liu L, Nair H, Theodoratou E, Bhutta Antibiotic policies theory and practice. New York: Kluwer
ZA, et al. Global burden of childhood pneumonia and Academic; 2005. p. 197-226.
diarrhoea. Lancet. 2013;381:1405–16. 16. Watt JP, Wolfson LJ, O’Brien KL, Henkle E, Deloria-Knoll M,
3. Ostapchuk M, Roberts DM, Haddy R. Community-acquired McCall N, et al. Burden of disease caused by Haemophilus
pneumonia in infants and children. Am Fam Physician. influenzae type b in children younger than 5 years: global
2004;70:899–908. estimates. Lancet. 2009;374:903–11.
4. Ceyhan M, Yildirim I, Ecevit C, Aydogan A, Ornek A, Salman 17. Nair H, Nokes DJ, Gessner BD, Dherani M, Madhi SA,
N, et al. Inappropriate antimicrobial use in Turkish pediatric Singleton RJ, et al. Global burden of acute lower respiratory
hospitals: a multicenter point prevalence survey. Int J Infect infections due to respiratory syncytial virus in young
Dis. 2010;14:e55–61. children: a systematic review and meta-analysis. Lancet.
5. Gerber JS, Newland JG, Coffin SE, Hall M, Thurm C, Prasad 2010;375:1545–55.
PA, et al. Variability in antibiotic use at children’s hospitals. 18. Adisasmito AW, Hadinegoro SRS. Infeksi gram negatif di ICU
Pediatrics. 2010;126:1067–73. anak: epidemiologi, manajemen antibiotik dan pencegahan.
6. Marquet K, Liesenborgs A, Bergs J, Vleugels A, Claes N. Sari Pediatri. 2004;6:32-9.
Incidence and outcome of inappropriate in-hospital empiric 19. Athale UH, Brown RC, Furman WL. Immunomodulation.
antibiotics for severe infection: a systematic review and meta- In: Patrick CC, editor. Clinical management of infections
analysis. Crit Care. 2015;19:63. in immunocompromized infants and children. 1 st ed.
7. Murni IK, Duke T, Kinney S, Daley AJ, Soenarto Y. Reducing Philadelphia: Lippincott Williams & Wilkins; 2001. p. 584-
hospital-acquired infections and improving the rational use 615.
of antibiotics in a developing country: an effectiveness study.
Paediatr Indones, Vol. 57, No. 4, July 2017 • 215
You might also like
- Update On Congenital Hypothyroidism: ReviewDocument7 pagesUpdate On Congenital Hypothyroidism: ReviewReka Vikaria AnggreliaNo ratings yet
- Current Antibiotic Use in The Treatment of EntericDocument26 pagesCurrent Antibiotic Use in The Treatment of EntericReka Vikaria AnggreliaNo ratings yet
- 2015 Myopia A Growing Global Problem WithDocument1 page2015 Myopia A Growing Global Problem WithReka Vikaria AnggreliaNo ratings yet
- Commissioned Article Computer Vision Syndrome: A Review: Jatinder Bali, Naveen Neeraj, Renu Thakur BaliDocument8 pagesCommissioned Article Computer Vision Syndrome: A Review: Jatinder Bali, Naveen Neeraj, Renu Thakur BaliReka Vikaria AnggreliaNo ratings yet
- Computer Vision Syndrome (CVS)Document9 pagesComputer Vision Syndrome (CVS)Reka Vikaria AnggreliaNo ratings yet
- Tumbling e ChartDocument21 pagesTumbling e ChartReka Vikaria AnggreliaNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (843)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5810)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (346)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Paitent Infromation On SulfasalazineDocument4 pagesPaitent Infromation On SulfasalazineDuyenNo ratings yet
- CDC COVID ScreeningDocument4 pagesCDC COVID ScreeningDaniel KrugNo ratings yet
- European Patent Specification: Anti-Il-33 Antibodies and Uses ThereofDocument129 pagesEuropean Patent Specification: Anti-Il-33 Antibodies and Uses ThereofavalosheNo ratings yet
- Akizawa 2009Document9 pagesAkizawa 2009PROF. ERWIN M. GLOBIO, MSITNo ratings yet
- Handbook of Epigenetics The New Molecular and Medical Genetics 3Rd Edition Trygve O Tollefsbol Full ChapterDocument67 pagesHandbook of Epigenetics The New Molecular and Medical Genetics 3Rd Edition Trygve O Tollefsbol Full Chapterdarrell.sesler392100% (2)
- Health Policy and Planning in IndiaDocument10 pagesHealth Policy and Planning in IndiaShubhaDavalgiNo ratings yet
- Presented By, Alana Joy Roll No: 3 3 Yr Pharm DDocument29 pagesPresented By, Alana Joy Roll No: 3 3 Yr Pharm DREETHUNo ratings yet
- Drug StudyDocument7 pagesDrug StudyMan GatuankoNo ratings yet
- Coronavirus Disease 2019 (COVID-19) in The EU/EEA and The UK - Ninth UpdateDocument50 pagesCoronavirus Disease 2019 (COVID-19) in The EU/EEA and The UK - Ninth UpdateCadjosse LtaNo ratings yet
- NCP Hep2Document3 pagesNCP Hep2Jordz PlaciNo ratings yet
- Vacuna Moderna Updated CDC September 11, 2023 Clinical Review - SPIKEVAXDocument156 pagesVacuna Moderna Updated CDC September 11, 2023 Clinical Review - SPIKEVAX9jz5dzj5gwNo ratings yet
- Registration Form For Use of Swimming PoolDocument2 pagesRegistration Form For Use of Swimming PoolSwati SinghNo ratings yet
- Tobacco Regulation Act of 2003Document2 pagesTobacco Regulation Act of 2003Jarvin SantosNo ratings yet
- BIO100 Exam 3 Review SheetDocument8 pagesBIO100 Exam 3 Review SheetSeanNo ratings yet
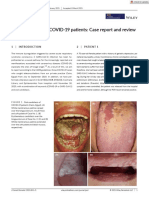
- Oral Candidiasis of COVID-19 Patients Case Report and ReviewDocument5 pagesOral Candidiasis of COVID-19 Patients Case Report and ReviewElizabeth SihiteNo ratings yet
- Factors Modifying Drug EffectsDocument47 pagesFactors Modifying Drug EffectsRiddhi Jain100% (1)
- Post Operative Care (P.o.c) : It Is The Care The Patient Is Received After The SurgeryDocument8 pagesPost Operative Care (P.o.c) : It Is The Care The Patient Is Received After The SurgeryJana AliNo ratings yet
- Lecture 24-25 - Antihypertensive AgentsDocument30 pagesLecture 24-25 - Antihypertensive AgentsJedoNo ratings yet
- Transes 1 (PEDIATRICS-LAB)Document2 pagesTranses 1 (PEDIATRICS-LAB)Ashley Judd EmpaynadoNo ratings yet
- NHS FPX6004 BorovacSarah Assessment3 1Document7 pagesNHS FPX6004 BorovacSarah Assessment3 1sara walterNo ratings yet
- Creative Homeopathy Excerpt ANTONIE PEPPLERDocument13 pagesCreative Homeopathy Excerpt ANTONIE PEPPLERshanti08No ratings yet
- ALL Clinicals of ThoraxDocument26 pagesALL Clinicals of Thoraxnaranjanlal01No ratings yet
- Lipoma of The Oral and Maxillofacial RegionDocument10 pagesLipoma of The Oral and Maxillofacial RegionLaila FortunatoNo ratings yet
- Learning Contract EndocrinologyDocument6 pagesLearning Contract EndocrinologyGerald AndersonNo ratings yet
- Report Health Records Kuinet Dispensary EdnahDocument27 pagesReport Health Records Kuinet Dispensary EdnahsamuelNo ratings yet
- Vsim Nursing Assignment #1: Toua Xiong 501 Pathophysiology and Pharmacology Gelsey Jian University of Maryland School of Nursing 9/14/18Document7 pagesVsim Nursing Assignment #1: Toua Xiong 501 Pathophysiology and Pharmacology Gelsey Jian University of Maryland School of Nursing 9/14/18Gelsey Gelsinator JianNo ratings yet
- NiacinDocument2 pagesNiacinΚωνσταντίνος ΓκάργκαςNo ratings yet
- AnkleDocument13 pagesAnklesadiaNo ratings yet
- Nursing Health HistoryDocument9 pagesNursing Health HistoryJajangNo ratings yet
- Final Exam With MCQ AnswersDocument18 pagesFinal Exam With MCQ AnswersRoyal GautamNo ratings yet