Professional Documents
Culture Documents
Pathology 5.04 Male Genitalia - Dr. Villamayor
Uploaded by
Shaira Aquino VerzosaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pathology 5.04 Male Genitalia - Dr. Villamayor
Uploaded by
Shaira Aquino VerzosaCopyright:
Available Formats
Subject:
Pathology Second Semester A.Y. 2013-‐2014
Topic: Male Genital Tract Diseases
Lecturer: Dr. Carina P. Villamayor
Date: January 8, 2015
OUTLINE o Interferes with cleanliness and permits accumulation of
I. Penis secretion and detritus under the prepuce →Prone to
A. Congenital repeated infection (deposition of smegma: desquamated
B. Inflammation epithelial cells, sweat, debris) and carcinoma
C. Tumors
o May result from anomalous development or from repeated
II. Testis/Epididymis
A. Congenital
attacks of infection causing scaring of the preputal ring.
B. Regressive
C. Inflammation
D. Vascular diseases
E. Tumors
III. Prostate
A. Inflammation
B. Benign Enlargement
C. Malignancy
PENIS
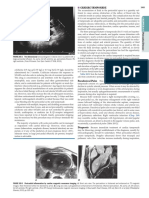
A. CONGENITAL Figure 3. Phimosis
PARAPHIMOSIS
• Malformations of the penis
o Phimotic prepuce is forcibly retracted over the glans penis
o Abnormal location of the urethral orifice along the penile
o Extremely painful
shaft
o Cause urethral constriction and serious acute urinary
o Malformation of the urethral groove and urethral canal
retention
creating abnormal openings on the penis
o May be associated with failure of normal descent of the
B. INFLAMMATION
testes and with malformation of the urinary tract
• Invariably involves the glans and prepuce and include a variety
o Abnormal opening is usually constricted and may result in
of specific infection ( sexually transmitted disease) and
urinary obstruction and increase in risk of ascending urinary
nonspecific infection
tract infection
o Normal ejaculation and insemination may be hampered or
BALANOSPOSTHITIS
blocked → result in sterility
• Infection of the glans and prepuce caused by a variety of
HYPOSPADIAS (Ventral Aspect) organisms:
-‐ More common (1/300 live male births) o Candida albicans
EPISPADIAS (Dorsal Aspect) o Anaerobes
o Gardnerella
o Pyogenic
• Occurs as a consequence of poor local hygiene in uncircumcised
males, causing the accumulation of smegma beneath the
prepuce.
Figure
1.
Hypospadias
Figure
4.
Balanosposthitis
C. TUMORS
(NEOPLASIA)
I. BENIGN
CONDYLOMA
ACUMINATA
“Venereal
or
Genital
warts”
o Benign
sexually
transmitted
tumor
caused
by
HPV
types
6
and
11
Figure
2.
Epispadias
o Exactly
the
same
appearance
and
etiology
as
on
the
female
external
genitalia
PHIMOSIS
o May
occur
on
any
moist
mucocutaneous
surface
of
the
o Abnormal
small
opening
which
prevents
normal
retraction
of
External
genitalia
and/or
perineum
the
prepuce
o Recur,
rarely
progress
to
carcinoma
Trans Group: Sadaya, Saligan, Salindong, Salise Page 1 of 11
Edited By:
Gross
o Occurs in the external genitalia and perineum, often on the
coronal sulcus and inner surface of the prepuce
o Single or multiple sessile or pednculated, red papillary
exrescence that vary from 1mm to several mm in diameter
Figure
7.
Bowen
Disease(Gross
and
Histology).
Right:
note
“loss
of
maturation
pattern”
where
surface
cells
not
much
different
from
base
cells,
quite
typical
of
squamous
CJS
everywhere
Figure
5.
Condyloma
Acuminatum:
multiple
pedunculated
red
papillary
excrescence
BOWENOID
PAPULOSIS
Histology
o Sexually
active
adults;
younger
patients
o Branching,
villous
papillary
CT
stroma
that
may
have
o Presence
of
multiple
pigmented
reddish-‐
papular
lesions
superficial
hyperkeratosis
and
acanthosis
(
thickening
of
o Never
develops
to
invasive
CA,
can
spontaneously
regress
underlying
epidermis)
Table
1.
Bowen’s
Disease
vs.
Bowenoid
Papulosis
o Koilocytosis:
perinuclear
cytoplasmic
vacuolization
of
the
Bowen’s
Disease
Bowenoid
Papulosis
squamous
cells,
classical
for
HPV
Associated
with
HPV
16
o May
have
a
viral
atypia
but
true
dysplasia
is
rare
History
of
promiscuous
sexual
activity
o Intact
basement
membrane
Solitary
lesions
Multiple
lesions
Older
patients
Younger
patients
Usually
progress
to
SCCA
in
10
%
of
Never
develops
into
invasive
CA
cases
(high
grade
CIS)
B. INVASIVE
SQUAMOUS
CELL
CARCINOMA
o Infiltrating
or
invasive
o US:
Uncommon
(<1%
CA
in
male)
o Asia,
Africa,
S.
America:
10-‐20%
of
male
malignancies
o Usually
this
is
present
in
patients
with
poor
local
hygiene
Figure
6.Condylomata
Acuminata
(histo):
Left:
Papillary
(villous)
architecture
o Ages
40-‐70
years
old
and
thickening
of
epidermis.
Right:
Koilocytosis;
nuclei
appear
raisin-‐like.
o Circumcision
confers
protection
o Association
with
genital
hygiene
and
HPV
16
and
18
II. MALIGNANT
o HPV
16
most
frequent
culprit
and
HPV
DNA
can
be
detected
A. In-‐situ
o Cigarette
smoking
increases
risk
of
developing
CA
of
the
penis
BOWEN
DISEASE
o Bowen
disease
may
transform
into
SCCA
in
10%
of
patients
o Squamous
cell
carcinoma-‐in-‐situ
of
the
skin
of
the
shaft
of
the
penis
and
scrotum
Gross
o Occurs
in
the
genital
region
of
both
men
and
women,
usually
o Papillary
lesion
stimulate
condyloma
acuminata
producing
a
over
35
years
old
verrucous
cauliflower-‐like
fungating
masses
Gross
o Flat
lesions
appear
as
areas
of
epithelial
thickening
o Solitary,
thickened
gray-‐white,
shiny,
opaque,
and
velvety
accompanied
by
graying
and
fissuring
of
the
mucosal
surface
plaque
with
shallow
ulceration
and
crusting
o Progress
to
ulcerated
papule
o Single
or
multiple
shiny
red
velvety
plaques
on
the
glans
and
prepuce
–
Erythroplasia
of
Queyrat
Histology
o
Epidermal
proliferation
with
numerous
mitosis,
dysplastic
cells
with
lack
of
orderly
maturation
and
large
hyperchromatic
nuclei
o Dermal-‐epidermal
border
is
markedly
delineated
by
intact
Basement
Membrane
o Over
the
span
of
years,
10%
may
develop
infiltrating
squamous
carcinoma
and
visceral
cancer
Figure
8.
Squamous
Cell
Carcinoma
of
the
Penis
Histology
o Differentiation
and
can
have
connection
or
no
connection
to
the
epidermis.
Page 2 of 11
2. Endocrine factors, or
3. Mechanical factors that prevent passage of the fetal
testis thru the inguinal canal
o Epidemiology:
§ 1% of all births
§ Unilateral >> bilateral (25% cases)
§ Associated with significantly increased incidence of germ
cell tumors (recall that major lesions in the testis are
tumors)
o Clinical significance: (from Essentials of Rubin’s Pathology)
Figure 9. Note the presence of keratin pearls and large cells with pleomorphic § Related to an increased incidence of infertility and germ
nuclei and prominent nucleoli. Intercellular bridging: even if it is neoplastic
cell neoplasia
you could still see the distinct demarcation of the cells from each other. There
§ Bilateral cryptorchidism à azoospermia (infertile)
is presence of abundant pink cytoplasm.
§ Unilateral cryptorchidism à oligospermia (sperm count
<20 million.mL) in 40% of cases
o Characterized by an arrest in the development of germ cells
associated with marked hyalinization and thickening of the
basement membrane of the spermatic tubules
Figure
10.
Slowly
growing,
locally
invasive.
Lesions
are
non-‐painful
until
ulceration
and
infection
develop.
Presence
of
atypia
or
angry
looking
nucleus
with
coarse
chromatin.
Metastasis
to
inguinal
and
iliac
nodes.
VERRUCOUS
CARCINOMA
(Giant
Condyloma
or
Bushke-‐Lowenstein
tumor)
o Uncommon,
exophytic
well
differentiated
variant
with
low
Figure
11.
(L)
Normal
testis
shows
tubules
with
active
spermatogenesis.
(R)
malignant
potential;
locally
invasive
but
rarely
metastasize.
Testicular
atrophy
in
cryptorchidism.
The
tubules
show
Sertoli
cells
but
no
o Believed
to
be
caused
by
HPV
16
due
to
koilocytic
changes
spermatogenesis.
There
is
thickening
of
basement
membranes
and
an
apparent
increase
in
interstitial
Leydig
cells.
insuperficial
layer;
papillary
appearance
like
condyloma
acuminatum.
o No
spermatogenic
activity
o Asymptomatic
but
undescended
testes
are
palpable
in
the
II.
TESTIS/EPIDIDYMIS
inguinal
canal
• Epididymis:
mostly
inflammatory
diseases
o Requires
surgical
correction
(orchiopexy)
• Testis:
mostly
tumors
OTHER
CONGENITAL
ANOMALIES:
A.
Congenital
Anomalies
o absence
of
one
or
more
testes
CRYPTORCHIDISM
o fusion
of
the
testes
(synorchism)
o Complete
or
incomplete
failure
of
the
intra-‐intra-‐abdominal
testes
to
descend
into
the
scrotal
sac
NOTE
Congenital
anomalies
are
extremely
rare,
EXCEPT
for
RECALL
cryptorchidism.
Testicular
descent
occurs
in
2
phases:
1. Transabdominal
phase
B.
Regressive
Changes
• the
testis
comes
to
lie
within
the
lower
TESTICULAR
ATROPHY
abdomen
or
brim
of
pelvis
o regressive
change
that
affects
the
testis
• controlled
by
müllerian-‐inhibiting
substance
o Can
have
several
causes,
including:
2. Inguinoscrotal
phase
1. atherosclerotic
narrowing
of
the
blood
supply
in
old
age
• testes
descend
thru
the
inguinal
canal
into
2. end
stage
of
an
inflammatory
orchitis,
whatever
the
the
scrotal
sac
etiologic
agent
• controlled
by
androgen
3. Cryptorchidism
(undescended
testes
are
sterile)
• more
commonly
affected
in
cryptorchidism
4. hypopituitarism
5. generalized
malnutrition
or
cachexia
6. irradiation
o Pathogenesis:
(from
Essentials
of
Rubin’s
Pathology)
7. prolonged
administration
of
female
sex
hormones,
§ The
causes
of
testicular
maldescent
are
usually
unknown,
(treatment
of
patients
with
carcinoma
of
the
prostate
but
theoretically
the
condition
could
be
related
to:
and
cirrhosis)
1. Developmental
disorders
of
the
gonad,
8. exhaustion
atrophy
(produce
high
levels
of
follicle-‐
Page 3 of 11
stimulating pituitary syndrome) o Clinical significance:
o Atrophy occasionally occurs as a primary failure of genetic § Such inflammatory involvement of the epididymis and
origin, such as in Klinefelter syndrome. testis is often followed by fibrous scarring, which in many
o An end-‐stage pattern of testicular injury, i.e. it occurs after cases leads to sterility.
several other patterns associated with decreased fertility (such § However, usually the interstitial cells of Leydig are not
as hypospadias, maturation arrest, vas deferens obstruction) totally destroyed, so sexual activity is not disturbed.
have been manifested o Epididymitis
o In some cases, if a specific cause for testicular injury can be § Acute or chronic inflammation of the epididymis usually
found and removed before development of atrophy, then test caused by bacteria
function can be restored. § Cause varies with patient’s age:
Childhood (uncommon) congenital genitourinary
abnormality and infection
with Gram (-‐) rods
sexually active <35 y/o Chlamydia trachomatis,
Neisseria gonorrhoeae
(STD pathogens)
>35 y/o E. coli, Pseudomonas
(UTI pathogens)
o Orchitis
§ Acute of chronic inflammation of the testis
§ May occur as part of epididymo-‐orchitis or be an isolated
testicular inflammation
§ Often secondary of UTI; typically associated with
Figure 12. Testicular atrophy, classical pattern, showing ghosting or fibrosis of epididymis.
tubules (arrow), NO spermatogenesis, INCREASED interstitial cells of Leydig.
SPECIFIC INFLAMMATIONS
C. Inflammatory Lesions of the Testis o Three major specific inflammatory states that affect the
• Inflammations are more common in the epididymis than in the testis/epididymis:
testis 1. Gonorrhea – arises in epididymis
• Inflammatory lesions of the testis usually involve the epididymis 2. Tuberculosis – arises in epididymis
first. These include: 3. Syphilis – arises in testis
o Sexually transmitted diseases e.g. syphilis o Mumps
o Nonspecific epididymitis and orchitis § A systemic viral disease of the parotid glands that most
o Mumps commonly affects school children. But at this age group,
o Tuberculosis testicular involvement is uncommon.
o Autoimmune granulomatous orchitis § Only 20% of adult males present with mumps
• 20-‐30% of these postpubertal males may develop
associated orchitis
§ Morphology:
• Edema and congestion
• Chronic inflammatory infiltrate
• May cause atrophy and sterility
o Tuberculosis
§ TB begins in the epididymis and may spread to the testis
§ Infection invokes the characteristic granulomatous
inflammation and caseous necrosis
Figure
13.
(L)
Scrotal
swelling.
(R)
Huge
collection
of
neutrophils.
NONSPECIFIC
EPIDIDYMITIS
AND
ORCHITIS
o Epididymitis
and
possible
subsequent
orchitis
are
commonly
related
to
UTIs
(cystitis,
urethritis,
prostatitis)
§ Infections
in
the
urinary
tract
may
reach
the
epididymis
and
testis
thru
either:
(1)
vas
deference
or
(2)
lymphatics
of
the
spermatic
cord.
o Pathogenesis:
§ Bacterial
invasion
à
nonspecific
acute
inflammation
(congestion,
edema,
and
infiltration
by
neutrophils,
Figure
14.
Tuberculous
orchitis,
showing
granulomatous
cheesy
material.
macrophages,
and
lymphocytes)
§ Infection
spreads
from
interstitial
connective
tissue
à
tubules
à
frank
abscess
formation
or
complete
suppurative
necrosis
of
entire
epididymis
à
testis
Page 4 of 11
o Either in utero or shortly after birth
o Lacks any associated anatomic defect that allows
excessive mobility of testis
2. Adult Torsion
o Typically seen in adolescence
o Presents as sudden onset of testicular pain
o Often occurs without any inciting injury
o May even occur during sleep
o Results from a bilateral anatomic defect where the testis
has increased mobility (bell-‐clapped abnormality—i.e.
the testis is free to swing, much like the gong/clapper
inside a bell)
Figure 15. (L) Areas of necrosis. (R) Presence of Langans giant cells. o If one testis becomes twisted, the unaffected one can be
saved from subsequent twisting by surgically fixing it to
AUTOIMMUNE GRANULOMATOUS ORCHITIS the scrotum (orchiopexy)
o Rare finding in middle aged men
o Presents in middle age as a moderately tender testicular mass E. Testicular Neoplasms
of sudden onset sometimes associated with fever • Epidemiology:
o Distinguished by granulomas restricted to spermatic tubules o Most important cause of painless enlargement of testis (since
o Although an autoimmune basis is suspected, the cause of painless, patients usually present with the later stage of the
these lesions remains unknown disease)
o 2/100,000 males, whites > blacks (US)
NOTES o Increased frequency in siblings
• Often, Inflammations in the testicle ALSO involve the o Peak incidence 15-‐34 yrs
epididymis, and vice versa. Commonly, urinary tract o Most are malignant
gram negatives infect BOTH o Associated with germ cell maldevelopment
• However, § Cryptorchidism (most important risk factor)
1. Mumps and TB are the most common agents of § Testicular dysgenesis(XXY) syndrome
primarily orchitis, and • Pathogenesis:
2. CHLAMYDIA and TORSION are the most common o 95% arise from germ cells
causes of primarily epididymitis. § Isochromosome 12, i(12p), is a common finding
§ Intratubular germ cell neoplasms
D. Vascular Disorders § Most germ cell tumors are aggressive cancers capable of
TORSION OF THE TESTIS rapid, wide dissemination, although with current therapy
o Twisting of the spermatic cord cuts off venous drainage to the most can be cured.
testis; thick-‐walled arteries remain patent, allowing vascular o Rarely arise from Sertoli cells or Leydig cells
engorgement followed by hemorrhagic infarction. § These are often benign
o Lymphoma – 5% of testicular neoplasms are secondary to
aggressive Non-‐Hodgkin’s lymphoma
§ Most common testicular neoplasm in men > 60 y/o
• Try to rule out lymphoma first before considering other
testicular neoplasms for patients in this age
§ Diffuse large cell lymphoma
• most common testicular neoplasm in men, regardless
of age
• WHO Classification of Testicular Tumors:
o One histologic pattern (40%) – pure forms
§ Seminomas (30%) – best prognosis because it is extremely
Figure 16. Infarcted, purple testicle & epididymis due to torsion; with
radiosensitive; one of the most common testicular
hemorrhagic infarction.
neoplasms
§ Embryonal carcinoma
o If complete torsion, severe pain and infarction of testicular
§ Yolk sac tumor
germ cells occur within a few hours
§ Choriocarcinoma
o Often presents after vigorous physical activity
§ Teratoma
o May be associated with a congenital abnormality that allows
o Multiple histologic patterns (60%) – combination of different
excess mobility of the testis
forms
o Reduction of torsion within 6 hours can lead to complete
§ Embryonal CA + teratoma
recovery; delay by 12-‐24 hours may cause severe or total loss
§ Choriocarcinoma + other
of testicular viability.
§ Other combinations
o Torsion is one of the few urologic emergencies
2 Types of Testicular Torsion
1. Neonatal Torsion
Page 5 of 11
Figure 18. Seminoma of the Testis appears as a fairly well circumscribed pale,
fleshy, homogenous mass
Histology
o Clear seminoma cells, delicate septa, lymphocytic infiltrate
Figure 17. Histogenesis of Testicular Neoplasms. See text below for
explanation. o The classic seminoma cell is large and round to polyhedral and
has a distinct cell membrane; a clear or watery-‐appearing
• Histogenesis of Testicular Neoplasms: cytoplasm; and a large, central nucleus with one or two
1. Neoplasms arising from germ cell precursors are divided into prominent nucleoli.
either the seminomatous or nonseminomatous group: o Approximately 15% of seminomas contains synctiotrophoblasts
a. If the neoplasm undergoes gonadal differentiation resulting in elevated levels of human chorionic gonadotropin
(seminomatous group): (HCG) though not to the extent of those with choriocarcinoma
§ it is a seminoma, which is usually found in 40-‐ o May also be accompanied by ill-‐defined granulomatous
50 year olds. reaction (in contrast to well-‐formed discrete granulomas seen
§ Another example of gonadal differentiation is in TB)
spermatocytic seminoma which is very rare. o Anaplastic Seminoma is used to indicate greater cellular and
b. When the neoplasm undergoes totipotential nuclear irregularity with more frequent tumor giant cells and
differentiation, it is nonseminomatous. many mitoses but is not associated with worse prognosis
2. Nonseminomas are called embryonal CA.
a. If embryonal neoplasms undergo trophoblastic
differentiation, it is called choriocharcinoma.
§ Choriocarcinoma is heralded by an increase in
beta-‐hCG, which can also be found in females.
b. If it undergoes yolk sac differentiation, it is called a
yolk sac tumor.
§ This is the most common tumor in infants and
children less than 3 years old.
§ It is usually alpha-‐feto-‐protein (AFP) positive.
c. For somatic differentiation, there is the teratoma
which affects all ages.
§ Teratomas can either be mature, immature or
Figure 19. Seminoma Left: Low magnifiation shows clear seminoma cells
have malignant differentiation. divided into poorly demarcated lobules by delicate septa. Right: Microscopic
examination reveals large cells with distinct cell borders, pale nuclei,
NOTES prominent nucleoli, and a sparse lymphocytic infiltrate. The larger cells are
• Females also have choriocarcinoma, yolk sac tumors, GERM cells and they often do look like spermatocytes from normal histology.
and teratoma. The smaller cells look like typical lymphocytes because they are typical
lymphocytes. Usually, there are good numbers of BOTH kinds of cells
• Seminomas in females are called dysgerminoma (they
have the same histologic picture)
EMBRYONAL CARCINOMA
o Keywords: Hemorrhagic mass, alveolar/tubular patterns, AFP
SEMINOMA
elevated
o Keywords: Clear seminoma cells, delicate septa, lymphocytic
o These cells are usually described as “primitive,” but usually
infiltrates
show kind of a GLANDULAR pattern, which is why in the old days
o Most common type of germ cell tumor (50%)
they were often called adenocarcinomas. But remember they
o Peak incidence at third decade and almost never in infants
are GERM cells, NOT glandular epithelial cells
o Identical tumor in ovary: dysgerminoma
o Occurs mostly in 20 to 30-‐year age group
o Seminomas produce bulky masses, sometimes 10 times the
o More aggressive than seminomas
size of the normal testis
Gross
Gross
o Typical seminoma has a homogenous, gray-‐white, lobulated cut
o Tumor is smaller than seminoma and usually does not replace
surface, usually devoid of hemorrhage or necrosis
entire testis
o Tunica albuginea is not penetrated but occasionally extension
o Variegated, poorly demarcated on margins, punctuated by foci
to epididymis, spermatic cord, or scrotal sac occurs
of hemorrhage or necrosis
Page 6 of 11
Figure 20. Embryonal carcinoma: Hemorrhagic mass.
Histology Figure 22. Choriocarcinoma
o Cells grow in alveolar or tubular patterns, sometimes with YOLK SAC TUMOR
papillary convolutions o AKA endodermal sinus tumor
o Lack well-‐formed glands with basally-‐situated nuclei and apical o Most common testicular tumor in infants and children up to 3yo
cytoplasm seen in teratomas (good prognosis in this age group)
o More differentiated lesions may display sheets of cells
o Epithelial appearance: large, anaplastic, and have hyperchromatic Gross
nuclei with prominent nucleoli o Tumor is nonencapsulated
o In contrast to seminoma: indistinct cell borders and there is o Cross section: homogenous, yellow white, mucinous appearance
considerable variation in cell and nuclear size and shape
o Mitotic figures and tumor giant cells frequently seen Histology
o Lacelike (reticular) network of medium-‐sized cuboidal or
flattened cells
o Papillary structures, solid cords of cells may be seen
o In approximately 50%, structures resembling endodermal sinus,
SCHILLER-‐DUVAL BODIES, may be seen; these consist of
mesodermal core with a central capillary and a visceral and
parietal layer of cells resembling primitive glomeruli
o Present within and outside cytoplasm are eosinophilic, hyaline
like globules in which alpha-‐fetoprotein (AFP) and alpha1-‐
antitrypsin can be demonstrated by immunocytochemical
staining
o AFP in tumor cells is highly characteristic and it underscores
Figure 21. Embryonal carcinoma shows sheets of undifferentiated cells as well their differentiation into yolk sac cells.
as primitive glandular differentiation. The nuclei are large and
hyperchromatic.
CHORIOCARCINOMA
o Keywords: trophoblastic differentiation, HCG, hemorrhage and
necrosis
o Highly malignant form of testicular cancer (ST and CT cells)
o In its “pure” form it is rare, <1% of all germ cell tumors
Gross
o They cause no testicular enlargement and are detected only as a
small palpable nodule Figure 23. Schiller-‐Duval bodies
o Tumors are small and rarely larger than 5cm in diameter
o Hemorrhage and necrosis extremely common
Histology
o Two cell types:
• Syncytiotrophoblastic cells – large and have many lobular
or hyperchromatic nuclei and an abundant eosinophilic
vacuolated cytoplasm. HCG readily demonstrated in the
cytoplasm
• Cytotrophoblastic cells – more regular and tend to be
polygonal, with distinct borders and clear cytoplasm. They
grow in cords or masses and have a singly, fairly uniform
nucleus
Figure 24. Yolk sac tumor with lacelike reticular network
TERATOMA, MALIGNANT TERATOMA, TERATOCARCINOMA
o Conglomeration of tissue arising from ectoderm, mesoderm, and
endoderm (more than one germ layer)
Page 7 of 11
o Most testicular teratomas are malignant. Most ovarian teratomas
are benign (e.g. dermoid cyst)
o In post-‐pubertal males, teratomas are usually malignant whether
immature or mature (bad prognosis)
o Clusters of squamous epithelium, hair, skin glands (most common
thing that is found in teratoma) composed of a heterogenous,
helter-‐skelter collection of differentiated cells
• Neural tissue, retina, muscle bundles, islands of cartilage,
structures reminiscent of thyroid gland, bronchial or
bronchiolar epithelium, bits of intestinal wall or brain
substance
Figure
27.
HYPERPLASIAS:
TZ;
CARCINOMAS:
PZ.
Carcinomas/neoplasias
(e.g.
prostate
cancer):
usually
in
peripheral
zone.
Hyperplasia
(e.g.
BPH):
usually
in
transitional
zone.
Usual
screening
for
prostate
cancer:
Digital
Rectal
Examination
(DRE)
is
used;
posterior
part
of
peripheral
zone
of
prostate
is
usually
affected.
A. INFLAMMATION
(Not
extensively
discussed
by
the
lecturer.
Info
lifted
from
Robbins)
Figure
25
.
Teratoma
of
the
testis
(Immature
teratoma)
-‐
the
variegated
cut
surfaces
with
cysts
reflects
the
multiplicity
of
tissue
found
histologically.
PROSTATITIS
Heterogenous,
with
solid,
sometimes
cartilaginous
and
cystic
areas.
I.
ACUTE
BACTERIAL
PROSTATITIS
o Usually
same
as
Urinary
Tract
Pathogens
o Most
common
are
various
strains:
E.coli,
Gram(-‐)
rods,
enterococci
and
staphylococci
o Become
implanted
by
intraprostatic
reflux
of
urine
from
the
posterior
urethra
or
from
the
urinary
bladder
OR
seed
the
prostate
by
lymphohematogenous
routes
from
distant
foci
of
infection
o May
usually
follow
a
surgical
manipulation
of
urethra
or
prostate
gland
itself.
(e.g.
catheterization)
o DRE:
tender
and
boggy
o Clinical
manifestations:
fevers,
chills
and
dysuria
o Diagnosis:
urine
culture
and
clinical
features
Figure
26.
Teratoma
of
the
Testis-‐
consisting
of
a
disogranized
collection
of
glands,
cartilage,
smooth
muscle,
and
immature
stroma
Morphology
PROSTATE
o Minute,
disseminated
abscesses
o Large,
coalescent
focal
areas
of
necrosis
• Normal
adult
prostate
weighs
20gm;
has
a
chestnut
structure
o Diffuse
edema,
congestion
and
boggy
suppuration
of
entire
• Retroperitoneal
organ
encircling
the
neck
of
the
bladder
and
gland.
urethra,
and
is
devoid
of
a
distinct
capsule
• Enlargement
of
the
prostate
will
constrict
the
urethra.
Most
patients
will
complain
of
urinary
incontinence
and
present
with
a
distended
bladder.
Just
insert
a
catheter
to
relieve
it.
• Some
patients
will
have
no
idea
that
their
prostate
is
enlarged
unless
they
already
present
urinary
problems.
• 3
pathologic
processes:
inflammation,
benign
nodular
enlargement
(most
common),
tumors
• The
normal
prostate
has
several
different
zones
o Central
Zone
(CZ)
–
nearest
the
urethra
o Peripheral
Zone
(PZ)
–
nearest
the
capsule
o Transitional
Zone
(TZ)
–
between
the
two
o Periurethral
zone
Figure
28.
Acute
Prostatitis.
With
a
lot
of
Neutrophils.
Page 8 of 11
II. CHRONIC PROSTATITIS leads to urethral obstruction.
o Usually abacterial but also often are recurrent or persistent from • Hypertrophy = enlargement of the prostate
acute; most common form • Hyperplasia = increase in the number of glands and increased
prostatic stroma
• Secondary to the hypertrophy and hyperplasia, they can form
nodules which can be palpated during DRE
• Associated with old age (Common disorder in men over age 50
years)
• Associated with urinary obstruction, frequency, bladder
hypertrophy and bladder trabeculations
• Not considered to be a premalignant lesion
Morphology
• Prostate weighs between 60-‐100gm
Figure 29. Chronic Prostatitis; due to Lymphocytes seen. • Hyperplasia originates in the transition zone
• The hallmark of BPH is nodularity due to glandular proliferation
1. CHRONIC BACTERIAL PROSTATITIS or dilation and to fibrous or muscular proliferation of the stroma
o Difficult to diagnose and treat • Common location of BPH: Median lobe (median lobe
o Clinical symptoms: Low back pain, dysuria and perineal and hypertrophy) and lateral lobes
suprapubic discomfort • Androgen-‐related (DHT produced by the stromal cells)
o Usually present with recurrent urinary tract infections (cystitis,
and urethritis) caused by the same organism → continuation of Clinical Features
infection
• Increased gland size and smoothe ms-‐mediated contraction of
the prostate leading to obstruction, increased resistance to
o Diagnosis:
urinary outflow, inability to fully empty bladder creating a
o Leukocytosis in the expressed prostatic secretions
possible site of infection, increased urinary frequency, nocturia,
o Positive bacterial culture
difficulty in starting and stopping the stream of urine, overflow
dribbling, dysuria.
2. CHRONIC ABACTERIAL PROSTATITIS
o Most common form of prostatitis
o Indistinguishable from the bacterial type.
o No history of recurrent urinary tract infection
o Expressed prostatic secretions: >10 leukocytes/HPF
o Bacterial cultures (-‐)
III. GRANULOMATOUS PROSTATITIS
o Tuberculosis or non-‐tuberculosis
o May be specific or non-‐specific
o Fungal prostatitis is seen in immunocompromised patients
o Nonspecific granulomatous prostatitis is relatively common;
presents secretions from ruptured prostatic ducts and acini;
o (-‐) Bacteria Figure 31. Left: Cross Section of prostate: blue arrows: nodules, can weigh as
much as 100gm; due to increased number of epithelial cells and stromal
components in the periurethral area of the prostate. Right: Prostate chips.
Figure
30.
Granulomatous
Prostatitis.
Figure
32.
Nodular
hyperplasia.
Forms
nodules
or
trabeculations.
Normal
gland
has
a
basal
cell
layer
made
up
of
columnar
cells;
double
layer;
can
be
B. BENIGN
ENLARGEMENT
columnar
or
cuboidal.
Has
increased
number
of
glands.
The
glands
are
lined
by
• BPH
(H
=
Hypertrophy)
or
BPH
(
H
=
Hyperplasia)
a
two
cell
layer:
Basal
and
Columnar
layers.
• Glandular
and
Stromal
Hyperplasia
• “Nodular”
Hyperplasia
–
aka
Benign
Prostatic
Hyperplasia,
where
nodules
compress
and
narrow
the
urethral
canal
which
Page 9 of 11
CLINICAL COURSE
o Often clinically silent
o Earliest symptom: change in urinary frequency
o Monitoring through Digital Rectal Exam (DRE)
o Prostate Specific Antigen (PSA) – most important test used in the
diagnosis and management of prostate CA; organ-‐specififc, not
cancer-‐specific
o 4 ng/ml in peripheral blood
o Free PSA < 25% (<10% in Robbins)
o Transrectal ultrasound-‐ determine the size
o Needle Biopsy – required to confirm the diagnosis
o Prostatism – presents like BPH ie. Urinary incontinence
o Osteoblastic metastases – presents with bone pain
o Usually in the vertebra (lumbar spine > proximal femur > pelvis >
Figure 33. BPH. Dilatation and proliferation of the acini, hyperplasia of the thoracic spine > ribs)
acini. Glandular hyperplasia, note ABSENCE of nucleoli. Also note nuclei are
where they should be, i.e., basal. Also note glands are NOT back to back, but MORPHOLOGY
each one is separated by thin fibrous tissue. • In approx. 70% of cases, carcinoma of the prostate arises in the
peripheral zone.
• THREE conditions favor a BENIGN process: • On cross section, neoplastic tissue is gritty and firm, but when
o Glandular hyperplasia, note ABSENCE of nucleoli. embedded within prostatic substance it may be difficult to
o Also note nuclei are where they should be, i.e., basal. visualize and be more readily apparent on palpation.
o Also note glands are NOT back to back, but each one is • May commonly involve periprostatic tissue, seminal vesicles,
separated by thin fibrous tissue. and base of the urinary bladder.
• Histologically, most lesions are adenoCAs that produce well-‐
C. MALIGNANCY defined gland patterns. The glands are typically smaller than
ADENOCARCINOMA benign glands and are lined by a single uniform layer of cuboidal
EPIDEMIOLOGY or low columnar epith.
o Most common cancer in men • The outer basal cell layer is absent.
o About 70/100,00 men in US; about 29% of cancer in the US
(2007) TREATMENT: Surgery, radiation, hormones, chemotherapy
o 200,000 new cases/year in US
o 20% are lethal
Note: Prostate CA: AdenoCA
o Second most common cause of cancer death in men
Penis CA: Squamous Cell CA
o Peak incidence of clinical cancer is 65-‐75 yo
o Latent CA is even more prevalent; latency is due to its
asymptomatic presentation
o >50% in men > 80 yo
o 20% in men in their 50s; 70% in men 70-‐80 y/o
o Uncommon in Asians; frequent in blacks
PATHOGENESIS
• Hormonal Factors
o Androgens – Bind with androgen receptor in the neoplastic
cell and induce the expression of pro-‐growth and pro-‐
survival gene factors in the neoplastic cells
o Does not occur in eunuchs (castrated)
o Orchiectomy and/or estrogen treatment inhibits growth of
the cancer
• Genetic Factors
Figure 34. (Left) Local extension to periprostatic tissue Metastases spread via
o Increased risk in first order relatives
lymphatics first: obturator and para-‐aortic nodes. Hematogenous: bones.
o Blacks > Whites (but symptomatic CA) (Right) Glands are smaller than benign glands and are lined by cuboidal or low
• Environmental Factors columnar; outer basal cell layer is absent; fused glands, no more septa
o Geographic differences in incidence of clinical cancer (not separating them. Note the various sized glands with almost no stroma in
of latent CA) between.
o Change in incidence with migration
• Diet and lifestyle
o More westernized (increased consumption of fats), increase
in incidence of prostate cancer. Dietary products that
inhibit, prevent, delay progression of prostate cancer
include lycopenes, vitamin A, Vitamin E, selenium and soy
products
Page 10 of 11
Figure 38. Gleason Score. Grade 1 -‐ most well-‐differentiated tumors in which
the neoplastic glands are uniform and round in appearance and are packed
into well-‐circumscribed nodules. Grade 5 -‐ no glandular differentiation, tumor
cells infiltrate the stroma in the form of cords, sheets and nests
• A Gleason’s final SCORE is the SUM of the predominant pattern
Figure 35. NUCLEOLI separate benign from malignant prostate glands!!! Of
(1-‐5) and the secondary pattern (1-‐5).
course there are other differentiating features, but this is the MOST RELIABLE
one. The presence of NUCLEOLI in most of these cells almost nails the • So a Gleason GRADE ranges from 1-‐5, and a Gleason SCORE
diagnosis of malignancy. ranges from 2-‐10.
• Grading is of particular importance in prostatic cancer because
grade and stage are the best prognostic predictors.
STAGING
• Staging of prostatic cancer is important in the selection of
appropriate form of therapy
o A(T1) MICROSCOPIC ONLY
o B(T2) MACROSCOPIC (PALPABLE)
o C(T3 &T4) EXTRACAPSULAR
o D(N1-‐3,M1) METASTATIC
• Prognosis dependent on stage and histologic grade
o 90% 10 YR survival for A AND B
o 10-‐40% 10 YR survival for C AND D
Figure 36. Perineural Invasion. Even if, theoretically, the prostate gland cells Table 2. Staging of Prostate CA using the TNM System
look 100%, if they surround nerve spaces, they are malignant
TNM
ANATOMIC FINDINGS
DESIGNATION
Extent of primary Tumor (T)
T1 CLINICALLY INAPPARENT LESION (BY
PALPATION/IMAGING STUDIES)
T1a Involvement of ≤5% of resected tissue
T1b Involvement of >5% of resected tissue
T1c Carcinoma present on needle biopsy (following
elevated PSA)
T2 PALPABLE/VISIBLE CANCER CONFINED TO
PROSTATE
T2a Involvement of ≤5% of one lobe
T2b Involvement of >5% of one lobe, but unilateral
Figure 37. TIP: Multiple bone metastases in males is usually carcinoma of the
prostate. (Commonly affects lumbar spine>femur>pelvis>thoracic spine>ribs) T2c Involvement of both lobes
T3 LOCAL EXTRAPROSTATIC EXTENSION
GRADING (GLEASON SYSTEM) T3a Extracapsular extension
• Gleason Score: Predominant pattern (1-‐5) + Secondary pattern T3b Seminal vesical invasion
(1-‐5) T4 INVASION OF CONTIGUOUS ORGANS AND/OR
o Grades 2-‐4: well-‐differentiated SUPPORTING STRUCTURES INC BLADDER NECK,
o Grades 5-‐6: intermediate grade RECTUM, EXTERNAL SPHINCTER, LEVATOR MS,
o Grade 7: moderate to poorly differentiated CA OR PELVIC FLOOR
o Grades 8-‐10: high grade tumor Status of Regional Lymph Nodes (N)
• BEST Score = 2; WORST SCORE = 10 N0 NO REGIONAL NODAL METASTASES
• Prostate CA are stratified into 5 grades based on glandular N1 METASTASIS IN REGIONAL LYMPH NODES
patterns of differentiation. Distant Metastases (M)
• Most tumors form more than 1 pattern. One assigns a primary M0 NO DISTANT METASTASES
grade to the dominant pattern and a secondary grade to the M1 DISTANT METASTASES PRESENT
second most frequent pattern. The two numeric grades are then M1a Metastases to distant lymph nodes
added to obtain a combined Gleason score. M1b Bone metastases
• Exception to the rule: If three patterns are present on biopsy, M1c Other distant sites
the most common and highest grades are added together.
Page 11 of 11
You might also like
- Gross B 2.25. EarDocument4 pagesGross B 2.25. EarShaira Aquino VerzosaNo ratings yet
- Gross B 2.27. Correlative Anatomy of The Special SensesDocument7 pagesGross B 2.27. Correlative Anatomy of The Special SensesShaira Aquino VerzosaNo ratings yet
- Gross B 2.20. Superficial Structures and Posterior Triangle of The NeckDocument6 pagesGross B 2.20. Superficial Structures and Posterior Triangle of The NeckShaira Aquino VerzosaNo ratings yet
- Pathology 5.01.1 Kidney I - Dr. MesinaDocument14 pagesPathology 5.01.1 Kidney I - Dr. MesinaShaira Aquino VerzosaNo ratings yet
- Cardiac TamponadeDocument3 pagesCardiac TamponadeShaira Aquino VerzosaNo ratings yet
- Approach and ECGDocument35 pagesApproach and ECGShaira Aquino VerzosaNo ratings yet
- Agents Causing Coma or SeizuresDocument3 pagesAgents Causing Coma or SeizuresShaira Aquino VerzosaNo ratings yet
- Basic Science Questions: ND RD TH THDocument42 pagesBasic Science Questions: ND RD TH THShaira Aquino VerzosaNo ratings yet
- Diseases of Peripheral NervesDocument111 pagesDiseases of Peripheral NervesShaira Aquino VerzosaNo ratings yet
- Pediatric Cervical LymphadenopathyDocument13 pagesPediatric Cervical LymphadenopathyShaira Aquino VerzosaNo ratings yet
- Medical Neurosciences NotesDocument43 pagesMedical Neurosciences NotesShaira Aquino VerzosaNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Micro TeachingDocument3 pagesMicro Teachingapi-273530753No ratings yet
- Notice: Grant and Cooperative Agreement Awards: Public Housing Neighborhood Networks ProgramDocument3 pagesNotice: Grant and Cooperative Agreement Awards: Public Housing Neighborhood Networks ProgramJustia.comNo ratings yet
- Photo Essay (Lyka)Document2 pagesPhoto Essay (Lyka)Lyka LadonNo ratings yet
- 2 Lista Total de Soportados 14-12-2022Document758 pages2 Lista Total de Soportados 14-12-2022Emanuel EspindolaNo ratings yet
- Queen of Hearts Rules - FinalDocument3 pagesQueen of Hearts Rules - FinalAudrey ErwinNo ratings yet
- Improving Downstream Processes To Recover Tartaric AcidDocument10 pagesImproving Downstream Processes To Recover Tartaric AcidFabio CastellanosNo ratings yet
- 401 Lourdes School Quezon City Inc. v. GarciaDocument2 pages401 Lourdes School Quezon City Inc. v. GarciaIldefonso HernaezNo ratings yet
- HDFC Bank-Centurion Bank of Punjab: Presented By: Sachi Bani Perhar Mba-Ib 2010-2012Document40 pagesHDFC Bank-Centurion Bank of Punjab: Presented By: Sachi Bani Perhar Mba-Ib 2010-2012Sumit MalikNo ratings yet
- FCAPSDocument5 pagesFCAPSPablo ParreñoNo ratings yet
- Applications of Tensor Functions in Solid MechanicsDocument303 pagesApplications of Tensor Functions in Solid Mechanicsking sunNo ratings yet
- Cryptography Practical 1Document41 pagesCryptography Practical 1Harsha GangwaniNo ratings yet
- Science Technology and SocietyDocument46 pagesScience Technology and SocietyCharles Elquime GalaponNo ratings yet
- Contract of Lease (711) - AguilarDocument7 pagesContract of Lease (711) - AguilarCoy Resurreccion Camarse100% (2)
- (IME) (Starfinder) (Acc) Wildstorm IndustriesDocument51 pages(IME) (Starfinder) (Acc) Wildstorm IndustriesFilipe Galiza79% (14)
- Duterte Vs SandiganbayanDocument17 pagesDuterte Vs SandiganbayanAnonymous KvztB3No ratings yet
- CPGDocument9 pagesCPGEra ParkNo ratings yet
- What Is An Ethical Dilemma?: Decision-Making ProcessDocument7 pagesWhat Is An Ethical Dilemma?: Decision-Making ProcessGauravsNo ratings yet
- Diva Arbitrage Fund PresentationDocument65 pagesDiva Arbitrage Fund Presentationchuff6675No ratings yet
- Reflection On An American ElegyDocument2 pagesReflection On An American ElegyacmyslNo ratings yet
- Task 1: MonologueDocument4 pagesTask 1: MonologueLaura Cánovas CabanesNo ratings yet
- Chapter 6 Bone Tissue 2304Document37 pagesChapter 6 Bone Tissue 2304Sav Oli100% (1)
- PUERPERAL SEPSIS CoverDocument9 pagesPUERPERAL SEPSIS CoverKerpersky LogNo ratings yet
- Fix Problems in Windows SearchDocument2 pagesFix Problems in Windows SearchSabah SalihNo ratings yet
- ANI Network - Quick Bill Pay PDFDocument2 pagesANI Network - Quick Bill Pay PDFSandeep DwivediNo ratings yet
- A List of Run Commands For Wind - Sem AutorDocument6 pagesA List of Run Commands For Wind - Sem AutorJoão José SantosNo ratings yet
- PsychometricsDocument4 pagesPsychometricsCor Villanueva33% (3)
- VIII and IXDocument56 pagesVIII and IXTinn ApNo ratings yet
- Cabot - Conductive Carbon Black For Use in Acrylic and Epoxy CoatingsDocument2 pagesCabot - Conductive Carbon Black For Use in Acrylic and Epoxy CoatingsLin Niu0% (1)
- The Skylane Pilot's CompanionDocument221 pagesThe Skylane Pilot's CompanionItayefrat100% (6)
- 5f Time of Legends Joan of Arc RulebookDocument36 pages5f Time of Legends Joan of Arc Rulebookpierre borget100% (1)