Professional Documents
Culture Documents
Hold The Smartphone! Tele-Epilepsy in A Post eCOVID-19 World
Uploaded by
HusniatulFitriahOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Hold The Smartphone! Tele-Epilepsy in A Post eCOVID-19 World
Uploaded by
HusniatulFitriahCopyright:
Available Formats
EDITORIAL
Hold the Smartphone! Tele-epilepsy in a
PosteCOVID-19 World
See also page 29
E
pilepsy is the third leading contributor increase health literacy, and to widen sup-
to the global burden of disease for port networks for PWE.
neurologic disorders, affecting 65 An increasing number of patients seeking
million people worldwide.1 Besides the care and a shortage of neurologists have
direct impact of seizures, people with epi- limited access to neurologic care. This is
lepsy (PWE) face problems including especially true in epilepsy care, for which a
disruption to work and education, psycho- significant shortage of specialists exists. This
logical stress, and social stigma. PWE also burden has become even larger with the
require regular outpatient visits for optimi- COVID-19 pandemic because of the self-
zation of antiseizure medication (ASM) isolation and strict lockdowns.2 Fortu-
therapy, management of epilepsy-related nately, access to smartphones and high-
psychological problems, and counseling on speed Internet has now become ubiquitous
family planning. Unfortunately, PWE often in both developed and many developing
have restricted driving privileges that can countries.3 These advances have made tele-
hinder traveling for these visits. The epilepsy a “new normal.” Ample evidence
containment measures established to face supports the successful use of tele-epilepsy
the coronavirus disease 2019 (COVID-19) for the diagnosis and follow-up of PWE.6 A
pandemic have further compounded this tele-epilepsy initial visit can help diagnose
problem.2 Luckily, the rapid emergence of patients living in areas remote from centers
telemedicine, catalyzed by the COVID-19 with epilepsy expertise. It can also facilitate
pandemic, using smartphone applications early identification and referral for an epi-
(apps) offers unique opportunities to address lepsy surgery evaluation. Follow-up outpa-
these.3 The integration of telemedicine in the tient visits for PWE that focus on seizure
health care systems has been accelerated by control, ASM adherence, ASM adverse
the increase in smartphone users, with the effects, and counseling can also be easily
latest figures estimating more than 3.5 performed using this platform. Besides, tele-
billion users worldwide.4 epilepsy enables direct communication with
In this issue of Mayo Clinic Proceedings, community providers and allows patients to
Tatum and Acton5 discuss the clinical utility stay with their local providers while
of smartphones for PWE in the poste improving consultation and access to higher
COVID-19 world. The authors highlighted level epilepsy care when it is needed.6
the massive potential of smartphone-based Differentiating an epileptic seizure from
telehealth in epilepsy care, including the a psychogenic nonepileptic seizure (PNES)
diagnostic value of smartphone videos remains a clinical art, one that is supported
(Figure). The technology can also facilitate by video encephalography (EEG). The wide
remote management of the adverse conse- availability of smartphones incorporating a
quences of recurrent seizures in PWE. Be- camera makes it possible to obtain a video
sides, smartphone-based seizure diaries and recording of the ictal event. Examining these
other apps can help track and document videos can help improve the diagnostic ac-
seizure frequency, ASM use, and nondrug curacy of PNES, especially when motor signs
therapy administration. Furthermore, are present. A recent multicenter trial found
smartphone-accessible online communities that a physician review of a high-quality
can be used to improve patient education, to smartphone seizure video resulted in the
4 Mayo Clin Proc. n January 2021;96(1):4-6 n https://doi.org/10.1016/j.mayocp.2020.11.010
www.mayoclinicproceedings.org n ª 2020 Mayo Foundation for Medical Education and Research
EDITORIAL
diagnostic accuracy of epilepsy and PNES
>95% of the time.7 Clinicians also had more
confidence in a diagnosis when it included a
smartphone video. The ability to identify
patients without epilepsy just by reviewing a
smartphone video could help realign health
care resources to patients for whom the need
is highest.7 During the peak of COVID-19,
most medical centers had closed their epi-
lepsy monitoring units either to free beds for
patients with COVID-19 or as part of
temporarily stopping elective procedures.
The diagnosis of PNES by review of smart-
phone videos certainly can eliminate un-
necessary epilepsy monitoring unit
admissions in the posteCOVID-19 world.
Current methods for assessing treatment
outcomes in epilepsy focus on reducing
seizure activity; however, self-reported seizure
occurrence can be unreliable. This along with
the need to prevent seizure-related injuries
has fostered the development of wearable de-
vices, paired with smartphones, to detect sei-
zures in real-time continuously.8 Seizure
detection devices use single modalities or
combinations of EEG, video, accelerometry, FIGURE. Smartphone-assisted tele-epilepsy in a posteCOVID-19 world.
electromyography, electrocardiography, pho-
toplethysmography, and electrodermal activ-
ity.8 Almost all smartphones have built-in Smartphones also have the potential to
global positioning system receivers, sensing change the dynamics of epilepsy self-
capabilities, and motion detectors or acceler- management. For example, smartphone
ometers, enabling clinicians to “close the medication apps can help detect potential
loop” by timely detecting seizures. Seizure medication interactions and remind patients
alarms and safety devices are particularly to take their medication on time.10 The latter
crucial for those with ASM-resistant epilepsy increases medication compliance, one of the
who are at risk of prolonged convulsive sei- most significant issues in PWE. On the other
zures; left unattended, this could lead to hand, seizure diary apps allow patients to re-
sudden unexpected death in epilepsy. Along cord information that may give insight into a
the same lines, the development of patient’s seizure triggers.10 Information in the
smartphone-compatible electrode caps offers form of a medication and seizure diary also
an opportunity for complete EEG systems makes it possible for neurologists to tailor the
(“tele-EEG”) that are portable and user- treatment plan. Besides, online epilepsy self-
friendly.9 Continuous tele-EEG monitoring management programs such as Internet-
could detect spikes that typically precede sei- based psychosocial interventions can be easily
zures and alert patients in advance (ie, seizure integrated using smartphone apps. Further-
forecasting). Tele-EEG also has the potential more, smartphone apps, including music and
to increase access to EEG services in remote therapeutic video games, present new op-
and resource-limited settings.9 Certainly, portunities to incorporate nonpharmacologic
there is a need for remote monitoring capa- interventions.10 In addition, smartphone-
bilities to manage PWE in the posteCOVID- accessible online communities provide self-
19 world. learning by providing relevant educational
Mayo Clin Proc. n January 2021;96(1):4-6 n https://doi.org/10.1016/j.mayocp.2020.11.010 5
www.mayoclinicproceedings.org
MAYO CLINIC PROCEEDINGS
content and expand support networks in the indeed become the “new normal” for PWE’s
posteCOVID-19 world. long-term management in the posteCOVID-
The authors acknowledged that although 19 world. However, the platform requires
the possibilities of smartphone-assisted tele- regulation and standardization to ensure
epilepsy care are endless, ethical and legal is- consistency and quality in its application to
sues remain a concern. When the pandemic the care of PWE and to safeguard issues
begins to resolve, due diligence is required to pertaining to privacy and security.
ensure that privacy is addressed appropri-
ately. Gaps in Internet and smartphone ac- Anteneh M. Feyissa, MD, MSc
cess, confidentiality, medical errors, and Department of Neurology
Mayo Clinic
malpractice potential also require attention. Jacksonville, FL
Smartphone apps may share sensitive data
with advertisers and other third parties in Potential Competing Interests: The author reports no
competing interests.
ways not anticipated by users. Besides, devices
and sensors designed to detect seizures may Correspondence: Address to Anteneh M. Feyissa, MD, MSc,
collect information on the household’s activ- Department of Neurology, Mayo Clinic, 4500 San Pablo Rd,
Jacksonville, FL 32224 (Feyissa.Anteneh@mayo.edu).
ities that a patient wishes to keep private.
From a diagnostic standpoint, smartphone
REFERENCES
videos may not capture the entire ictal period
1. Ngugi AK, Bottomley C, Kleinschmidt I, Sander JW,
or may capture only the postictal period, Newton CR. Estimation of the burden of active and life-time
potentially misguiding the correct diagnosis.7 epilepsy: a meta-analytic approach. Epilepsia. 2010;51(5):883-
890.
Importantly, although the technology is wide- 2. Fesler JR, Stanton S, Merner K, et al. Bridging the gap in epilepsy
reaching, it cannot replace face-to-face visits care: a single-center experience of 3700 outpatient tele-
(“doctor’s touch”) in some circumstances. epilepsy visits. Epilepsia. 2020 [Online ahead of print].
3. Lopez-Jimenez F, Attia Z, Arruda-Olson AM, et al. Artificial in-
Smartphone technology, combined with telligence in cardiology: present and future. Mayo Clin Proc.
artificial intelligence, is advancing rapidly.3 2020;95(5):1015-1039.
4. Statista. Number of smartphone users worldwide from 2016 to
Integrating this technology with tele- 2021. https://www.statista.com/statistics/330695/number-of-
epilepsy care will increase health care ac- smartphone-users-worldwide/. Accessed October 21, 2020.
cess for the underserved and rural patients 5. Tatum WO, Acton EK. Smartphones in epilepsy: the new age
of Aquarius. Mayo Clin Proc. 2021;96(1):29-31.
and improves comanagement between local 6. Hatcher-Martin JM, Adams JL, Anderson ER, et al. Telemed-
neurologists and epilepsy providers. In the icine in neurology: Telemedicine Work Group of the Amer-
ican Academy of Neurology update. Neurology. 2020;94(1):
era of increasing medical costs, tele-epilepsy 30-38.
has the potential to reduce health care sys- 7. Tatum WO, Hirsch LJ, Gelfand MA, et al. Assessment of
tem costs. Besides, smartphone apps allow the predictive value of outpatient smartphone videos for
diagnosis of epileptic seizures. JAMA Neurol. 2020;77(5):
continuous monitoring of PWE and use of 593-600.
this information to inform management de- 8. Bruno E, Viana PF, Sperling MR, Richardson MP. Seizure detec-
tion at home: do devices on the market match the needs of
cisions. Smartphone-assisted seizure detec-
people living with epilepsy and their caregivers? Epilepsia.
tion devices have also opened new avenues 2020 [Online ahead of print].
to improve both the safety and treatment of 9. McKenzie ED, Lim AS, Leung EC, et al. Validation of a
smartphone-based EEG among people with epilepsy: a pro-
PWE. Furthermore, smartphone-assisted spective study. Sci Rep. 2017;7:45567.
tele-EEG will undoubtedly increase access 10. Afra P, Bruggers CS, Sweney M, et al. Mobile Software as a
to EEG services to remote and resource- medical device (SaMD) for the treatment of epilepsy: develop-
ment of digital therapeutics comprising behavioral and music-
limited populations. Practical tele-epilepsy based interventions for neurological disorders. Front Hum Neu-
tools, supported by smartphones, will rosci. 2018;12:171.
n n
6 Mayo Clin Proc. January 2021;96(1):4-6 https://doi.org/10.1016/j.mayocp.2020.11.010
www.mayoclinicproceedings.org
You might also like
- Echography and Doppler of the BrainFrom EverandEchography and Doppler of the BrainChiara RobbaNo ratings yet
- Remote and Longterm Selfmonitoring of Electroencephalographic and Noninvasive Measurable Variables at Home in Patients With Epilepsy EEGHOME Protocol For An Observational studyJMIR Research ProtocolsDocument12 pagesRemote and Longterm Selfmonitoring of Electroencephalographic and Noninvasive Measurable Variables at Home in Patients With Epilepsy EEGHOME Protocol For An Observational studyJMIR Research ProtocolsMiguel PalacioNo ratings yet
- JPD - 2021 - 11 s1 - JPD 11 s1 jpd202398 - JPD 11 jpd202398Document9 pagesJPD - 2021 - 11 s1 - JPD 11 s1 jpd202398 - JPD 11 jpd202398OKCTMVNo ratings yet
- Parlar Et Al. - 2020 - "You Can't Touch This" Delivery of Inpatient Neur PDFDocument17 pagesParlar Et Al. - 2020 - "You Can't Touch This" Delivery of Inpatient Neur PDFMaría VélezNo ratings yet
- Artificial Intelligence Deployment in Diabetic Retinopathy - The Last Step of The Translation ContinuumDocument2 pagesArtificial Intelligence Deployment in Diabetic Retinopathy - The Last Step of The Translation ContinuumDr. Abhishek OnkarNo ratings yet
- Comment: Telemedicine - Maintaining Quality During Times of TransitionDocument2 pagesComment: Telemedicine - Maintaining Quality During Times of Transitiontresy kalawaNo ratings yet
- Epilepsi Jurnal PhoneDocument10 pagesEpilepsi Jurnal PhoneRio HardiatmaNo ratings yet
- Comment: Published July 10, 2020 S2589-7500 (20) 30162-XDocument2 pagesComment: Published July 10, 2020 S2589-7500 (20) 30162-XJeff HambreNo ratings yet
- 2020karoly SeizurediaryforecastingDocument11 pages2020karoly SeizurediaryforecastingLevin KuhlmannNo ratings yet
- Advances in Telemedicine in OphthalmologyDocument11 pagesAdvances in Telemedicine in OphthalmologyMoneer Ali tahaNo ratings yet
- 1 s2.0 S1059131120303162 MainDocument9 pages1 s2.0 S1059131120303162 MainInes Arias PazNo ratings yet
- Accelerating Telemedicine For Cerebral Palsy During The COVID-19 Pandemic and BeyondDocument7 pagesAccelerating Telemedicine For Cerebral Palsy During The COVID-19 Pandemic and BeyondDjNo ratings yet
- On The Internet of Medical ThingsDocument1 pageOn The Internet of Medical ThingsdrhipoNo ratings yet
- Medication Management Needs ICT-based Approaches IDocument8 pagesMedication Management Needs ICT-based Approaches IAnkit ChandraNo ratings yet
- Comparison Study of Funduscopic Examination Using A Smartphone-Based Digital Ophthalmoscope and The Direct OphthalmoscopeDocument6 pagesComparison Study of Funduscopic Examination Using A Smartphone-Based Digital Ophthalmoscope and The Direct OphthalmoscopeWalisson BarbosaNo ratings yet
- Telefarmacia in Covid-19Document9 pagesTelefarmacia in Covid-19George ComonitaNo ratings yet
- 10 1093@ije@dyx058Document5 pages10 1093@ije@dyx058SakinaNo ratings yet
- Health Informatics SupportDocument7 pagesHealth Informatics SupportNada courseNo ratings yet
- Diagnóstico CIDPDocument7 pagesDiagnóstico CIDPMarysol UlloaNo ratings yet
- Global Poliomyelitis Eradication Status and ImplicationsDocument2 pagesGlobal Poliomyelitis Eradication Status and Implicationsxiongmao2389No ratings yet
- Using ICT in SchoolDocument5 pagesUsing ICT in Schoolsiti syuhada binti zainalNo ratings yet
- OBEDOZA, Franco Obedoza II CDocument1 pageOBEDOZA, Franco Obedoza II CFranco ObedozaNo ratings yet
- Keywords:-Adherence Problematic Adopting Electronic: Alarm Reminder Viral Load Value IntroducedDocument7 pagesKeywords:-Adherence Problematic Adopting Electronic: Alarm Reminder Viral Load Value IntroducedInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Telepathology in The Philippines: A Review and Future ProspectsDocument5 pagesTelepathology in The Philippines: A Review and Future ProspectsAr-jay PorrasNo ratings yet
- EHealth and COVIDDocument10 pagesEHealth and COVIDWalter ReyesNo ratings yet
- Big Jurnal RevDocument2 pagesBig Jurnal RevMuhamad Farrel RizqullahNo ratings yet
- Opportunities From The Coronavirus Disease 2019 Pandemic For Transforming Psychiatric Care With TelehealthDocument2 pagesOpportunities From The Coronavirus Disease 2019 Pandemic For Transforming Psychiatric Care With TelehealthmarieNo ratings yet
- Kenya National Manual For The Management of HIV Related OIsDocument162 pagesKenya National Manual For The Management of HIV Related OIsKknow DdrugNo ratings yet
- Cost Minimization of A Telehomecare Prog PDFDocument10 pagesCost Minimization of A Telehomecare Prog PDFRirin AptNo ratings yet
- Comparative Analysis of Deep Learning Convolutional Neural Networks Based On Transfer Learning For Pneumonia DetectionDocument12 pagesComparative Analysis of Deep Learning Convolutional Neural Networks Based On Transfer Learning For Pneumonia DetectionIJRASETPublicationsNo ratings yet
- WSN ExperentialDocument12 pagesWSN ExperentialGayatri BarnwalNo ratings yet
- Benefits and Drawbacks of Tele MedicineDocument11 pagesBenefits and Drawbacks of Tele MedicinessriraghavNo ratings yet
- Telehealth Home Support During COVID-19 Confinement ForDocument13 pagesTelehealth Home Support During COVID-19 Confinement ForPaulina TNo ratings yet
- 415 2020 Article 9898Document2 pages415 2020 Article 9898gevowo3277No ratings yet
- Ebola Detection SystemDocument4 pagesEbola Detection Systemlaura robertNo ratings yet
- Jurnal Telenursing Athiqah Syukri 2BDocument2 pagesJurnal Telenursing Athiqah Syukri 2BAthiqah SyukriNo ratings yet
- PAHOIMSEIHCOVID-19200029A EngDocument4 pagesPAHOIMSEIHCOVID-19200029A Engfisioterapi 2019No ratings yet
- Telemedicine For Epilepsy Support in Resource-Poor Settings: Public HealthDocument4 pagesTelemedicine For Epilepsy Support in Resource-Poor Settings: Public HealthHusniatulFitriahNo ratings yet
- Autoimmune Encephalitis in The Philippines A Scoping ReviewDocument10 pagesAutoimmune Encephalitis in The Philippines A Scoping ReviewGerald PagalingNo ratings yet
- Telehealth in Urology: A Systematic Review of The Literature. How Much Can Telemedicine Be Useful During and After The COVID-19 Pandemic?Document26 pagesTelehealth in Urology: A Systematic Review of The Literature. How Much Can Telemedicine Be Useful During and After The COVID-19 Pandemic?bintag mahaputraNo ratings yet
- PARANEOPLASTICDocument8 pagesPARANEOPLASTICMuhammad Imran MirzaNo ratings yet
- Applsci 13 03211Document14 pagesApplsci 13 03211Kovid AggarwalNo ratings yet
- 10 1001@jama 2020 2342Document2 pages10 1001@jama 2020 2342mostafa shahrabiNo ratings yet
- An Intelligent Telecardiology System Using A Wearable and Wireless ECG To Detect Atrial FibrillationDocument8 pagesAn Intelligent Telecardiology System Using A Wearable and Wireless ECG To Detect Atrial FibrillationAlexandru SerbNo ratings yet
- Acm Publish Ahead of Print 10.1097.acm.0000000000003711Document6 pagesAcm Publish Ahead of Print 10.1097.acm.0000000000003711gracia garciaNo ratings yet
- 1 s2.0 S003962571630090X MainDocument14 pages1 s2.0 S003962571630090X MainBenjamin NgNo ratings yet
- Epilepsia Open - 2021 - Bonilla - Biodegradable Nanoparticles For The Treatment of Epilepsy From Current Advances ToDocument12 pagesEpilepsia Open - 2021 - Bonilla - Biodegradable Nanoparticles For The Treatment of Epilepsy From Current Advances ToAlhara YuwandaNo ratings yet
- SLIDE DECK - Capacity Building For NGAs.Document40 pagesSLIDE DECK - Capacity Building For NGAs.hanniemaelimonNo ratings yet
- Sleep TelemedicineDocument11 pagesSleep Telemedicinesavvy_as_98-1No ratings yet
- Epilepsy Surgery in The Philippines: Annabell CHUADocument3 pagesEpilepsy Surgery in The Philippines: Annabell CHUAGlaiza BartolomeNo ratings yet
- Research PaperDocument78 pagesResearch PaperLester Paul SivilaNo ratings yet
- Comparison of Neuropsychological Assessment by Videoconference and Face To FaceDocument11 pagesComparison of Neuropsychological Assessment by Videoconference and Face To FaceGundisalvus FragaNo ratings yet
- Due To The InfectionDocument3 pagesDue To The InfectionSabariah Mohd DaudNo ratings yet
- Jpeck,+june2021 Telemetry Monitoring SpreadDocument2 pagesJpeck,+june2021 Telemetry Monitoring Spreadtublight sNo ratings yet
- Wearable Sensors For COVID-19Document8 pagesWearable Sensors For COVID-19Jemimah Aniel ClimacoNo ratings yet
- DON Guidelines On The Use of Tele-Neuropsychology (April 2020)Document8 pagesDON Guidelines On The Use of Tele-Neuropsychology (April 2020)Marina DrakeNo ratings yet
- Nursing Informatics-Innovative Technology in HealthDocument2 pagesNursing Informatics-Innovative Technology in HealthAnonymous izrFWiQ100% (1)
- 2023 - Pitfalls in Scalp EEG - Current Obstacles and Future Directions - SandorDocument21 pages2023 - Pitfalls in Scalp EEG - Current Obstacles and Future Directions - SandorJose Carlos Licea BlancoNo ratings yet
- Minimizing Artifact Induced False Alarms For Seizure Detection in Wearable EEG Devices With Gradient Boosted Tree ClassifiersDocument16 pagesMinimizing Artifact Induced False Alarms For Seizure Detection in Wearable EEG Devices With Gradient Boosted Tree ClassifiersG GggNo ratings yet
- The Diagnosis of Scabies by Non-Expert Examiners: A Study of Diagnostic AccuracyDocument13 pagesThe Diagnosis of Scabies by Non-Expert Examiners: A Study of Diagnostic AccuracyAnisa Rifkia ZSNo ratings yet
- August 2009 Go Guide Newsletter The MountaineersDocument20 pagesAugust 2009 Go Guide Newsletter The MountaineersMountaineersNo ratings yet
- 3rd Quarterly Exam in Mathematics 4Document9 pages3rd Quarterly Exam in Mathematics 4Jaycer De MesaNo ratings yet
- Critical Issue Leisha CavallaroDocument8 pagesCritical Issue Leisha Cavallaroapi-216287146No ratings yet
- IDOC As Web ServiceDocument40 pagesIDOC As Web ServiceUmesh Nanjaiah100% (2)
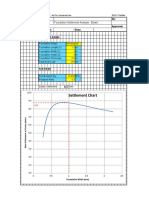
- Settlement Chart: Foundation Settlement Analysis - ElasticDocument2 pagesSettlement Chart: Foundation Settlement Analysis - ElasticCSEC Uganda Ltd.No ratings yet
- List of Dealers Selected From Cuttack I Range For Tax Audit During 2011-12Document24 pagesList of Dealers Selected From Cuttack I Range For Tax Audit During 2011-12rchowdhury_10No ratings yet
- Corporation: Pre-Trimmed IC Voltage Controlled AmplifiersDocument8 pagesCorporation: Pre-Trimmed IC Voltage Controlled AmplifiersBrandon ParsonsNo ratings yet
- OTPBank Securities SI 20210217Document6 pagesOTPBank Securities SI 20210217bdsourav0No ratings yet
- PA SystemDocument1 pagePA SystemSherif SalamaNo ratings yet
- Star Trek The Next Generation RPG Last Unicorn Games PDFDocument320 pagesStar Trek The Next Generation RPG Last Unicorn Games PDFNicolas Morin50% (2)
- Inventory Management System VB6Document7 pagesInventory Management System VB6PureNo ratings yet
- Pedagogy MCQsDocument85 pagesPedagogy MCQsPrasanna KumarNo ratings yet
- Sibunag River Development Project: Industry Sector: Business Type: Location TypeDocument4 pagesSibunag River Development Project: Industry Sector: Business Type: Location Typeemma gallosNo ratings yet
- Federico Giusfredi - Syntax of The Luwian LanguageDocument229 pagesFederico Giusfredi - Syntax of The Luwian LanguageLucySky7No ratings yet
- Bayer Clinitek-500-Operator-Manual PDFDocument77 pagesBayer Clinitek-500-Operator-Manual PDFSergio Iván CasillasNo ratings yet
- Appraisal of DSE & CSEDocument31 pagesAppraisal of DSE & CSEMohammad Shaniaz IslamNo ratings yet
- Marketing Plan Rental LaptopDocument15 pagesMarketing Plan Rental LaptopDany AkbarNo ratings yet
- Ψηφιακός Γραμματισμός ΣταΟπτικοακουστικά Μέσα Σε Διαδικτυακά Περιβάλλοντα ΜάθησηςDocument19 pagesΨηφιακός Γραμματισμός ΣταΟπτικοακουστικά Μέσα Σε Διαδικτυακά Περιβάλλοντα ΜάθησηςSofos LoisosNo ratings yet
- How Is The Working Principle of Load Shedding in Power Plants, and What Are The Terms of The InstallationDocument6 pagesHow Is The Working Principle of Load Shedding in Power Plants, and What Are The Terms of The InstallationAbdulyunus AmirNo ratings yet
- Basic Electronics New - 3110016Document4 pagesBasic Electronics New - 3110016Sneha PandyaNo ratings yet
- Union Feb. 10, 2016Document16 pagesUnion Feb. 10, 2016Your News. When You Want It.No ratings yet
- Abs TechnologyDocument14 pagesAbs Technologyanime landNo ratings yet
- Learning Objectives: Plumbing SystemsDocument25 pagesLearning Objectives: Plumbing Systemsanil horrisonNo ratings yet
- 12th Commerce Study Material English MediumDocument97 pages12th Commerce Study Material English MediumDeepak ajar100% (1)
- Sky Trak MANUAL PDFDocument906 pagesSky Trak MANUAL PDFCris Lozoya100% (1)
- 2018 2019UndergraduateEnglishTaughtCoursesDocument40 pages2018 2019UndergraduateEnglishTaughtCoursesmalu accountNo ratings yet
- Midview of 2Document4 pagesMidview of 2api-285760777No ratings yet
- Kode BajaDocument11 pagesKode BajaUriyanaNo ratings yet
- Revealed Comparative AdvantageDocument5 pagesRevealed Comparative AdvantageiamrahulkumarNo ratings yet
- 2) QuestionsDocument95 pages2) Questionsgita safiraNo ratings yet