Professional Documents
Culture Documents
Effective Protocol For Daily High-Quality Direct Posterior Composite Restorations. The Interdental Anatomy of The Class-2 Composite Restoration
Effective Protocol For Daily High-Quality Direct Posterior Composite Restorations. The Interdental Anatomy of The Class-2 Composite Restoration
Uploaded by
Kothiwal DentalOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Effective Protocol For Daily High-Quality Direct Posterior Composite Restorations. The Interdental Anatomy of The Class-2 Composite Restoration
Effective Protocol For Daily High-Quality Direct Posterior Composite Restorations. The Interdental Anatomy of The Class-2 Composite Restoration
Uploaded by
Kothiwal DentalCopyright:
Available Formats
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.
2021
Copyright 2021, Quintessenz Verlags-GmbH
Effective Protocol for Daily High-quality Direct Posterior
Composite Restorations. The Interdental Anatomy of the
Class-2 Composite Restoration
Marleen Peumansa / Pasquale Venutib / Gianfranco Politanoc / Bart Van Meerbeekd
Abstract: The importance of the interdental anatomy of a class-2 direct composite restoration is one of the most
underestimated topics in direct posterior composite restorations. The proximal emergence profile of the restoration
and the contact area should be designed to maximize arch continuity and to minimize food impaction. Other re-
storative criteria that must be fulfilled are marginal adaptation compatible with the dental and periodontal integrity,
and geometry of the marginal ridge compatible with the mechanical integrity of the restoration under load. Short-
comings will result in masticatory discomfort, caries, periodontal problems and undesired movement of teeth. In
vitro and in vivo studies showed that the use a contoured sectional metal matrix band with a separation clamp re-
sults in the tightest contact point. However, this matrix system also has shortcomings and does not give the ex-
pected result in all class-2 cavities. The variation in depth, width of the box, distance between the cervical cavity
margin and the adjacent tooth requires customization of the interproximal space. In order to realize this, sectional
matrix bands with several profiles of curvature, variation of wedges and separation clamps, and the use of teflon
tape are required. In addition, dentists should follow a protocol allowing them to build a proximal composite sur- r
face that fulfills the required restorative criteria. Pre-wedging, space evaluation, interproximal clearance, correct se-
lection, positioning and stabilization of the matrix band are important steps in this protocol.
Keywords: class-2, composite resin restoration, matrix system, proximal contact point, proximal emergence profile.
J Adhes Dent 2021; 23: 21–34. Submitted for publication: 20.07.20; accepted for publication: 18.08.20
doi: 10.3290/j.jad.b916819
S atisfactory rehabilitation of a proximal surface when res-
toring a class-2 cavity with a direct composite restor-
ation requires fulfillment of several criteria, including attain-
the interproximal area can lead to masticatory discomfort,
recurrent caries, and periodontal disease. In addition, an
inadequate contact may cause tooth movement and instabil-
ment of an anatomically correct contour and tight contact ity of the dental arch.2,7,13,15,39 One of the issues of masti-
area, adequate marginal adaptation and accurate marginal catory discomfort is “neurological switching”. The patient
ridge placement. Shortcomings in this regard have impor- starts to chew exclusively on the other side of the mouth in
tant implications for the adjacent tissues. Food impaction in order to avoid discomfort, unbalancing the system.37
To achieve adequate proximal geometry, the proximal
contour of the class-2 composite restoration should ideally
resemble that of an intact natural tooth (Fig 1). In the natu-
ral dentition, the interproximal contact is suggested to be
a Associate Professor, KU Leuven (University of Leuven), Department of Oral an area of 1.5-2 mm rather than a point (2) (Fig 2a). The
Health Sciences, BIOMAT & UZ Leuven (University Hospitals Leuven), Dentistry,
Leuven, Belgium. Wrote the manuscript, constructed the figures. contact area is located at the transition between the middle
b Dentist in Private Practice, Mirabella Eclano, Avellino, Italy. Developed the and occlusal third of the proximal plane in a cervico-occlu-
concept, constructed the figures, proofread the manuscript. sal direction, and at the transition between the middle and
c Dentist in Private Practice, Rome, Italy. Developed the concept, constructed buccal third in a bucco-lingual direction (3) (Figs 2b and 2c).
the figures, proofread the manuscript. In addition, the contour of the proximal surface in both di-
d Full Professor, KU Leuven (University of Leuven), Department of Oral Health Sci-i rections should be copied, respecting the natural buccal,
ences, BIOMAT & UZ Leuven (University Hospitals Leuven), Dentistry, Leuven,
Belgium. Proofread the manuscript. lingual, occlusal and gingival embrasure.
It is difficult to define optimal adequate proximal contact
Correspondence: Professor Marleen Peumans, KU Leuven (University of Leuven), tightness, as there is large intra- and interindividual varia-
Department of Oral Health Sciences, BIOMAT & UZ Leuven (University Hospitals
Leuven), Dentistry, Kapucijnenvoer 7, B-3000, Leuven, Belgium. tion.9,20,25,41 The proximal contact tightness in vivo can be
Tel: +32-16-332744; e-mail: marleen.peumans@kuleuven.be significantly influenced by location, tooth type, chewing,
Vol 23, No 1, 2021 21
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
Fig 1 In a natural dentition with normal tooth position, the contact areas in the premolar/ Fig 3 Radiograph taken after placement
molar region are located at the transition middle-buccal third in a bucco-lingual direction, and of several large MOD direct composite res-
at the transition middle-occlusal third in a cervico-occlusal direction (white rings). torations with a straight circular matrix
band. Notice narrow contact areas occluso-
gingivally (white arrows). The height of con-
tour of the restorations is right at the
occluso-proximal line angle. The patient
complained of food impaction in the large
interproximal areas.
time of day, the periodontal condition of the tooth and inter-
and intra-arch integrity.9
The reconstruction of a satisfactory anatomically con-
toured proximal surface in class-2 direct composite restora-
tions remains an issue for most dental practitioners. This is
partly inherent to polymerization shrinkage and the lack of
condensability of the resin composite materials,10,33 the
a use of rubber-dam,8,34 and the thickness and elastic dis-
placement of the matrix band.17,19
Traditional circumferential straight metal matrix bands,
used for placement of amalgam restorations, showed many
shortcomings in the formation of tight proximal contacts in
class-2 composite restorations. The contacts produced with
these matrix bands are often occluso-gingivally narrow, and
the height of restoration’s contour is often right at the oc-
b cluso-proximal line angle (Fig 3).5,26,33 Consequently, the
contact area is easily lost when the marginal ridge area is
smoothed. In addition, the thinner marginal ridge formed
with a straight matrix band is less fracture-resistant than a
more voluminous marginal ridge created with a contoured
matrix band.26
Several techniques and instruments have been proposed
to obtain tight proximal contacts: pre-wedging,9,11,24 the
c use of condensable composites,36 and proximal box-forming
Fig 2 (a) In the natural dentition the interproximal contact is sug- tools, among others.5,20,22,24,33,36 However, none of these
gested to be an area of 1.5-2 mm (blue circle). (b) Occlusal view: attempts proved adequate to create a tight contact area.
A correct contour of the proximal surface in a bucco-lingual direction According to several in vitro and in vivo studies, the
results in a contact area that is located at the transition between strongest proximal contact area in class-2 composite resto-
the middle and the buccal third. The buccal and lingual embrasure rations is obtained using a sectional metal matrix system in
are indicated by the red lines. (c) Buccal view: The proximal contact
combination with a separation ring.20,24,25,33,36,41
area is positioned at the maximum contour of the proximal surface.
This is located at the transition between the middle-occlusal third in
Nevertheless, some shortcomings have been described
a cervico-occlusal direction (blue circle). A correct proximal emer-
r using these modern metal sectional matrix systems in com-
gence profile and well-positioned contact area results in the forma- bination with a separation clamp. When the cavity is wide
tion of an occlusal and gingival embrasure (red lines). open in a bucco-lingual direction, the matrix will be dished-in
22 The Journal of Adhesive Dentistry
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
in the cavity by placement of the separation clamp. Chuang
et al5 observed that the contacts constructed using a dead
soft metal sectional matrix and separation clamp exhibited
good contact tightness, but showed a concave area in the
middle of the contact surface and overextension of compos-
ite at the buccal and lingual side. Another in vitro study
a b c
compared different circumferential matrices with a dead
soft metal sectional matrix band with separation ring.16 The
sectional matrix reproduced the tightest contact area. How-
ever, no system was able to reproduce proximal morphology
similar to that of an intact tooth. In these in vitro studies,
the use of an easily deformable dead soft metal matrix in
combination with a separation clamp were probably respon-
sible for the not smoothly formed and over-contoured proxi- d e
mal surface with tight contact. A strong metal matrix that
does not deform plastically (permanently) is required to
overcome this problem.
Another limitation of the commonly used sectional metal
matrix bands is that all these matrices have approximately
the same curvature or maximum contour. Nevertheless, a
large variation in width/depth of the box, in interproximal f g
distance between the cervical cavity margin and the adja- Fig 4 (a–c) Three interdental separation techniques demonstrated
cent tooth, is observed in class-2 cavities in daily clinical on a manikin model: (a) using a wooden wedge, (b) a separation
practice. Consequently, the interdental area needs to be clamp and (c) an interdental separator (Elliot separator, Carl Martin;
customized. This implies that the armamentarium for cor- r Solingen, Germany). The tips of the separator are covered with blue
rect build-up of a proximal box should be extended with sec- plastic rings in order to have better grip. (d) The Elliot Separator
(Carl Martin) without plastic tips. (e) Clinical situation with use of
tional matrix bands with a more pronounced curvature. In
the Elliot separator to obtain interdental separation before place-
addition, the dentist has to be aware of several tips and ment of a DO composite restoration on the 2nd premolar. Next to
tricks in order to correctly position and stabilize the matrix the separation function, the tips stabilize the matrix band. (f–g) After
band to achieve a tight adaptation between matrix band placement of the restoration and removal of the matrix band, a well-
and cavity margins. In this article, a protocol is presented formed proximal surface and tight contact area can be observed:
that allows the dentist to have control over creating a cor- r (f) buccal view, (g) lateral view.
rectly formed proximal surface with tight contact area in
class-2 composite restorations. This protocol, based on ex-
tensive clinical experience of one of the authors (PV), will
be documented by means of several clinical cases.
PROTOCOL FOR PLACING CLASS-2 COMPOSITE
RESTORATIONS WITH AN ADEQUATE INTER-
DENTAL ANATOMY
The protocol consists of 8 different steps, which will be y Selection of the matrix band
described consecutively in detail. y Positioning of matrix band: control position in a cervico-
y Rubber-dam isolation occlusal and bucco-lingual direction
y Pre-wedging y Stabilization of the matrix band, interdental separation,
y Space evaluation evaluation of contact area and fit to the cavity margins
y Interproximal clearance y Composite layering
Fig 5 Pre-wedging with an anatomical hard
wooden wedge before the start of the cavity
preparation creates interdental separation and
helps to compensate for the thickness of the
matrix band. In addition, it protects the gingiva
and the adjacent tooth during prepping and
finishing of the proximal cavity margins.
Vol 23, No 1, 2021 23
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
Fig 6 (a) Initial situation: a 30-year old female patient requested replacement of the
existing amalgam restorations. (b) Rubber-dam isolation and cavity preparation. The area
of hypomineralized enamel at the mesio-palatal cusp of the 1st molar was not included in
the preparation. One can also notice erosive cupping on the cusps. (c) Placement of a
soft stainless-steel matrix in combination with a separation clamp with prongs with
V-shaped end (Palodent Plus, Denstply Sirona; Konstanz, Germany). The matrix was
a adapted to the cavity margins using teflon tape. The matrix was too wide open in the
occlusal third, resulting in proximal over-contour in this area. A slight plastic deformation
of the matrix is noticed. This is caused by pushing the teflon tape in between matrix
band and separation clamp. (d) The MO cavity on the molar was filled with composite and
the matrix band removed. An over-contoured proximal surface can be noticed. This should
be corrected in order to obtain a correct proximal contour of the DO restoration on the
b premolar. (e) In the middle and occlusal third, the proximal contour of the adjacent tooth
can be adjusted using abrasive discs (Soflex 2382 C+M, 3M Oral Care; St Paul, MN,
USA). (f and g) Diamond-coated files with different grit sizes connected on a reciprocating
handpiece (Komet, Brasseler; Lemgo, Germany) are used to recontour the cervical and
occlusal third. (h) The mesial surface of the 1st molar was recontoured resulting in volu-
metric harmony of the interproximal area. Notice the interproximal clearance of the DO
cavity on the premolar. (i) Evaluation of the mesial contour of the 1st molar from the
c palatal side. (j) Interproximal clearance results in accessible restoration margins at the
buccal and lingual side. The excess of adhesive and flowable/composite (white arrows)
can easily be removed with a composite finishing disc (Soflex 2382 C+M, 3M Oral Care).
(k) Final class-2 composite restorations showing an anatomical proximal contour and
a tight contact area. The form of the natural buccal and lingual embrasure has been
respected. (l) Palatal view of the final restorations.
d
It is clear from the literature that interdental separation is the key factor to
e f g produce a tight proximal contact during placement of Class-2 composite res-
torations. Interdental separation can be obtained in several ways: pre-wedg-
ing, use of a separation clamp, and use of an interdental separator device
(Fig 4).5,6,16,18,30,33,35,36
Rubber-dam Isolation
h Rubber-dam isolation is a requirement for successful placement of a direct
composite restoration.32 To facilitate the clinical protocol for placement of a
composite restoration, the teeth should be isolated under rubber-dam before
cavity preparation. The dentist has to be aware that rubber-dam placement
significantly increases the proximal contact strength.9,34 In an in vivo study by
Dörfer et al,8 the reduction in contact strength was significantly higher be-
i
tween 1st molar and 2nd premolar, compared to canine/1st premolar and
1st/2nd premolar. The additional space lost due to rubber-dam placement
should be taken into account and requires a strong interdental separation
during cavity preparation and placement of the composite restoration.
j Pre-wedging
Pre-wedging consists of a wooden wedge pressed firmly into the interdental
space before cavity preparation and kept in place during preparation.1,6,11,40
This can result in separation of the teeth of up to 100-200 μm.4,14 The addi-
tional space created can compensate for the thickness of the matrix band,
the polymerization shrinkage of the composite, and the negative effect of
k rubber-dam placement.
Anatomical hard wooden wedges are preferred as they have the most pro-
nounced separation effect (Fig 5). The wooden wedge absorbs water during
the restorative procedure, resulting in expansion (swelling) of the wedge. A
soft wooden wedge will become weaker and more flexible, causing the separa-
tion effect to decrease. In a clinical trial, Loomans et al21 observed that pre-
l wedging with a wooden wedge resulted in a significantly lower separation ef- f
24 The Journal of Adhesive Dentistry
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
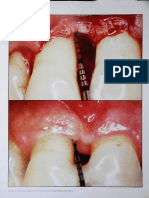
Fig 7 (a) The absence of interproximal clearance at the buccal
side interferes with passive positioning of the matrix. (b) The matrix
is forced interproximally resulting in deformation of the matrix and
inversion of the emergence profile. (c) Interproximal clearance is
created.
a b c
Fig 8 (a) Hard steel sectional matrix bands (TORVM; Moscow,
Russia) with a thickness of 50 μm. The matrix bands are available
in different heights and with subgingival extension. This matrix band
shows a slight curvature. (b) Hard steel (50 μm thick) perforated
metal matrices (TORVM). These matrices are available in 5 sizes.
They can be used in combination with a matrix tightener. These
matrix bands have a more pronounced curvature compared to the
traditional sectional matrix bands. The curvature starts more cervi- a
cally, making this matrix band useful to restore a box with a deeper
cervical cavity margin. (c) Hard steel (50 μm thick) saddle matrix
(TORVM). These matrices are available in 3 sizes. They can be used
in combination with a matrix tightener. The curvature of this matrix
is quite similar to that of the perforated metal matrix. (d) BioFit
matrix bands (Bioclear Matrix Systems) are transparent and available
in two thicknesses (BioFit Blue matrix: 50 μm and BioFit HD matrix:
76 μm) and 3 different heights (4.5, 5.5, 6.5 mm). The colorless
transparent BioFit HD matrices are more rigid, which allows them to
be placed as metal matrices. The blue transparant BiofFit Blue ma- b
trix is more flexible. These matrices have a more pronounced curva-
ture and larger bucco-lingual wrap. In addition, the occlusal
embrasure is included in the matrix band. These matrix bands are
part of the Bioclear Posterior matrix system (Bioclear Matrix Sys-
tems), including separation rings (Twinring) and diamond wedges
(cfr. Infra).
Fig 9 Schematic presentation of the maximum curvature of the
sectional matrix (TORVM), the saddle matrix (TORVM), the perfo-
rated contoured matrix (TORVM) and the BioFit HD matrix (Bioclear
Matrix Systems). Matrix bands of 6.5 mm height were used.
fect than placement of a separation clamp (with or without Next to the separation effect, the wedge protects the
a wedge). However, it should be noted that the separation rubber-dam and interdental papilla, and prevents the bur
was maintained for only 5 min. This is much shorter than from damaging the adjacent tooth while prepping the cervi-
the clinical time needed to prepare a class-2 cavity and cal cavity margin and creating interproximal clearance in the
place a composite restoration. cervical area.
Vol 23, No 1, 2021 25
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
a a b
b
c
c
d
Fig 10 (a) A hard steel (50 μm thick) sectional matrix band does Fig 11 (a-b) A saddle matrix (TORVM) or perforated contoured ma-
not deform permanently during placement and positioning of the sep- trix (TORVM) (pink dotted line) is selected in class-2 cavities where
aration clamp compared with (b) a soft stainless steel matrix band. the distance between the cervical cavity margin and the adjacent
After burnishing, the matrix band is deformed in the center. This will tooth is ±0.7 mm (pink double arrow). (a) This is possible when the
result in an irregularity in the proximal composite surface at the level teeth are positioned a bit further from each other, or when the
of the contact area). (c) A sectional matrix (red dotted line) is se- tooth is tilted. (b) The most common situation is when the cavity
lected in class-2 cavities where the distance between the cervical margin becomes deeper. This kind of situations requires a more
cavity margin and the adjacent tooth is ±0.5 mm (red double arrow). pronounced curvature of the matrix band. (c) The saddle matrix
(TORVM) is mainly used in medium deep class-2 cavities. (d) A
perforated contoured matrix band (TORVM) is used to restore a
MO cavity with a deep cervical cavity margin. The matrix band is
tightened in between the two molars using a matrix tightener.
Teflon tape is pushed in between the matrix band and rubber-dam
to adapt the matrix band to the cavity margins. No wedge is used.
The distal surface of the second premolar was damaged by the
previous operator.
Space Evaluation the one hand, interproximal clearance allows passive posi-
Volumetric harmony of the interproximal area is essential for tioning of the matrix. Forcing the matrix band in an inter- r
a functional and esthetic class-2 composite restoration. proximal space without interproximal clearance can result in
Therefore, the interproximal space available should be evalu- deformation of the matrix, invagination of the matrix, and in-
ated prior to placement of the matrix band. An over-contoured version of the emergence profile (Fig 7). On the other hand,
proximal surface of the adjacent tooth should be corrected, accessible and visible margins facilitate finishing, polishing,
as this can result in inverted anatomy and the formation of a and re-polishing of the restoration margins (Figs 6j to 6l).
deficient contact area (dimension, position) (Fig 6).
If needed, the proximal contour of the adjacent tooth can Selection of the Matrix Band
be adjusted using abrasive disks in the middle and occlusal Contoured sectional metal matrices are widely considered
third (Fig 6e). In the cervical third, a reciprocating hand- to be the most effective matrices for placement of direct
piece with diamond-coated files can be used, and/or abra- composite restorations involving the proximal surface. For
sive strips (Figs 6f and 6g). the restoration of a single box, only one thickness of the
metal material is encountered instead of two, making con-
Evaluation of Interproximal Clearance tact generation easier.41 Circumferentially contoured matri-
Interproximal clearance means that the buccal and lingual ces, especially when used without a separation ring, hinder
margins of the box are accessible (Figs 6h, 6i, and 7). On the construction of a tight proximal contact point. In addi-
26 The Journal of Adhesive Dentistry
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
a a b
c d
b c
d e e f
Fig 12 (a) BioFit matrix (Bioclear Matrix Systems) (green dotted Fig 14 (a) Initial situation: caries lesions are present at the distal
line) is selected in class-2 cavities where the distance between the side of the 1st molar and the mesial side of 2nd molar. (b) After open-
cervical cavity margin and the adjacent tooth is ±0.9 mm (green ing the distal marginal ridge of the 1st molar a deep caries lesion, ex-x
double arrow). The most common situation is when the cavity mar- r tending below the cemento-enamel junction, is observed. Electrosurgery
gin becomes deeper. (b) The large distance between the cervical of the interdental papil takes place to visualize the cervical cavity mar-
r
cavity margin of the 1st molar and 2nd premolar requires the use of gin and facilitate rubber-dam isolation (c) The teeth are isolated under
a BioFit matrix (Bioclear Matrix Systems) to restore the mesial side rubber-dam and the cavity preparations on both molars are finished. A
of the molar. (c) The matrix band is positioned and stabilized with a BioFit Blue matrix (Bioclear Matrix Systems) is selected to restore the
Diamond Wedge (Bioclear Matrix Systems). Additional stabilization deep Class-2 cavity on tooth 46. The matrix band is positioned. A
is obtained with block-out resin placed in between the matrix band Sabre Wedge (predecessor of the diamond wedge, BioClear Matrix Sys-
and the adjacent tooth. (d-e) After placing the composite restoration tems) is used to stabilize the matrix band and to obtain a good adapta-
on the 1st molar, the mesial surface shows an adequate contour. tion to the deep cervical cavity margin. Additional stabilization of the
This allows the dentist to obtain a correct contour at the distal side matrix band towards the buccal and lingual surface is realized with
of the 2nd premolar; (d) occlusal view, (e) buccal view. block-out resin. (d) After placement of the composite restorations on
both molars, the restored proximal surfaces show an adequate emer- r
gence profile and contact area. (e) Radiograph of the initial situation
showing the deep caries lesion on tooth 46, (f) Radiograph after place-
ment of the composite restorations. One can notice a good adaptation
of the composite to the deep cervical cavity margin on the 1st molar.
Fig 13 The distance between the cervical cavity margin and the Fig 15 Selection of the matrix band with the correct height. The
adjacent tooth largely determines the selection of the matrix band. matrix band should be positioned ±0.5 mm above the marginal
When the space is ±0.5 mm a sectional matrix band (TORVM) is ridge of the adjacent tooth. This is necessary to give the proximal
selected. When the space is around ±0.7 mm a saddle matrix surface a correct contour in a cervico-occlusal direction.
(TORVM) or a perforated matrix (TORVM) is selected. These 3 types
of hard steel metal matrix bands can be used in 90% of the class-2
restorations. A BioFit matrix (Bioclear Matrix Systems) is selected
when the interdental distance is ±0.9 mm.
Vol 23, No 1, 2021 27
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
Table 1 List of several commercially available sectional metal matrix bands
Material Sizes Thickness
Palodent Plus Soft stainless steel 3.5, 4.5, 5.5, 6.5, 7.5 mm 38 μm
(Dentsply Sirona; Konstanz, Germany)
Garrison Sectional Matrices Soft stainless steel 3.2, 3.8, 4.6, 5.5, 6.4 mm 38-40 μm
(Garrison Dental Solution; Übach Palenberg, Germany) 3.2, 3.8, 6.0, 6.4, 8.7 mm with ledge
TorVM Hard stainless steel Small, medium, large 35-50 μm
(TorVM; Moscow, Russia) Soft stainless steel small, medium, large with ledge
Quickmat Sectional Matrix Soft stainless steel 5, 6.4 mm 25-40 μm
(Polydentia; Mezzovico-Vira, Switzerland) 6.4 mm with ledge
Contact Matrix Stiff flex 5.5, 6.5 mm 60 μm
(Danville Materials; San Ramon, CA, USA) Dead soft 8.75 mm with ledge 40 μm
a b
Fig 17 Different wedges available on the dental market including
plastic V-shaped wedges, hard and soft anatomical wooden wedges,
silicone wedges and hard plastic wedges.
c d
a b
e
Fig 16 (a) A BioFit Blue Matrix is placed interproximally and fixed Fig 18 (a) When a tall wooden wedge is required for fixation and
with a diamond wedge (Bioclear Matrix systems). Occlusal view: adaptation of the matrix band, the wedge often reaches above the
The diamond wedge adapt the matrix band well to the cavity margins. cervical cavity margin. The wedge pushes the matrix band into the
(b). Buccal view: one can easily control the height of the matrix band cavity (white arrow). This results in the formation of a large
as the occlusal embrasure is included in the matrix band. A well- interdental area with increased food impaction. (b) After corrective
positioned contact area (white circle) is noticed. (c and d) Place- trimming of the wooden wedge (= customization of the wedge)
ment of the separation ring of the Bioclear matrix system (Twinring; (yellow arrow), the matrix band can keep its normal contour.
Bioclear Matrix Systems) is required to compensate for the thick-
ness of the matrix band. The adaptation of the ring prongs towards
the matrix band is not optimal in the occlusal part. This can be im-
proved by pushing teflon tape in between clamp and matrix band
(white arrows). (e) A sectional metal matrix band is centered bucco-
lingually, so that the contact area is in a correct position.
28 The Journal of Adhesive Dentistry
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
a b
Fig 20 A variety of separation clamps is available on the dental
market.
c d
tion, circular matrix bands produce more capillarity, in many
cases negating the efforts to obtain optimal isolation.
The sectional matrix should have a correct curved profile,
making it possible to create a correct emergence profile in
e f a cervico-occlusal direction. To select the correct matrix
band, one must be aware of its maximum curvature. Figures
8 and 9 show different matrix bands (used by the authors)
with their maximum curvature.
As mentioned above, it is important that the matrix band
is strong and does not deform plastically under the typical
stress applied during handling by the dentist. A 50-μm hard
steel matrix band can keep its ideal proximal contour more
easily during placement of the wedge, separation clamp,
and teflon tape, compared with a dead metal or soft steel
g metal matrix (Figs 10a and 10b). TORVM (Moscow, Russia)
delivers 50-μm-thick hard steel contoured sectional matrix
Fig 19 (a) Diamond wedges belonging to the Bioclear matrix system bands (Table 1). The matrix bands are available in different
(Bioclear Matrix Systems), available in different sizes (S, M, L, XL).
heights, with and without subgingival extension (Fig 8a). A
(b) Diamond cut-out (yellow arrow) allows for the tip of the wedge to
collapse during placement, facilitating insertion of the wedge. Once
6.5-mm-high sectional matrix band has a maximum curva-
placed, the tips burst open to create a gingival seal. The wedges ture of ±0.5 mm (Figs 9 and 10c). An increased proximal
show a low profile. The largest wedge (green), the so-called deep curvature (cervico-incisally) of the matrix band is required
caries wedge, has a furcal flare (white arrow) which allows the when the distance between the cervical cavity margin and
wedge to adapt better to deep caries and root furcations. (c) A large the adjacent tooth increases. This is observed when the
distance between the cervical cavity margin and the premolar cervical cavity margin is located in a more apical position.
requires the use of a BioFit matrix (Bioclear Matrix Systems) with Hard stainless steel sectional saddle matrices (TORVM)
a pronounced curvature. (d) The green diamond wedge is and the perforated metal matrices (TORVM) (6.5 mm
positioned interproximally and stabilizes the matrix band. By push-
height) have a maximum curvature of ±0.7 mm (Figs 8b, 8c,
ing the wedge interproximally a tight adaptation between matrix
band and cavity margins can be obtained. (e) Proximal view after
9, 11). The maximum curvature starts more cervically, mak-
positioning of the matrix band. The contact area is in a correct ing it easier to reach deeper margins. Here too, 50-μm thick
position. (f) After placing the composite restoration, the teeth show matrix bands are preferred.
anatomically contoured proximal surfaces and a well-positioned BioFit Matrix bands (Bioclear Matrix Systems; Tacoma,
contact area. (g) Occlusal view of the restored molar and premolar. WA, USA) have the highest maximum curvature (±0.9 mm)
A tight contact area is obtained. The form of the buccal and lingual (Figs 8d, 9, 12). These matrix bands are contoured plastic
embrasure has been respected. (Mylar) sectional matrices, available in two thicknesses
(BioFit Blue Matrix: 50 μm and BioFit HD matrix: 76 μm)
and 3 different heights (4.5, 5.5, 6.5 mm). Transparent
matrices may allow better light transmission and allegedly
more effective polymerization of the underlying resin com-
posite. The BioFit matrix bands have a larger bucco-lingual
Vol 23, No 1, 2021 29
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
a b
a b
c d
Fig 21 (a) Placement of a sectional matrix band fixed with a
wedge. The matrix band is in a correct position and shows an ideal c d
curvature. (b) After placement of the separation clamp, the matrix
band straightens in the occlusal third (white circle). This will result Fig 22 (a) Several class-2 cavities need to be restored. It is best
in the formation of a closed occlusal embrasure and a less con- to start with the cavities at the mesial side of the 1st molar and dis-
toured marginal ridge. Chipping will occur more easily during occlusal tal side of the 1st premolar. Because the distance between the cer- r
loading. The marginal ridge and occlusal embrasure can be con- vical cavity margins is small, a sectional hard steel matrix (TORVM)
toured after placement of the restoration with a Soflex disk (3M Oral is used. (b) The matrix band is fixed with a wedge. The matrix band
Care). However, this requires additional time for the operator. (c) A adapts well at the cervical cavity margin, but is a slightly open at
sectional metal matrix band is positioned interproximally. (d) After the occlusal part of the 1st premolar. (c) The matrix bands are relo-
placement of a wedge and separation clamp the matrix opens cated by putting teflon tape in the proximal cavity of the adjacent
slightly in the cervical area. This gap can be closed by pushing tooth. Additional stabilization of the matrix bands is obtained by
teflon tape in between wedge and matrix band. placing flowable between matrix band and adjacent tooth. (d) After
restoring the cavities and removal of the matrix band, an adequate
proximal contour is obtained. No additional contouring is required.
wrap, and can be used in cavities that are more open in a give the proximal surface a correct contour in a cervico-
bucco-lingual direction. In addition, the matrix features a occlusal direction. If the matrix band is too high, there is a
curved occlusal embrasure, which, if the matrix is well-posi- risk that the marginal ridge and the occlusal surface will be
tioned, shortens the finishing time of the occlusal embra- modelled too high. Consequently, considerable time will be
sure with burs or disks. needed to grind in the occlusion. If the matrix band is too
To conclude, the selection of the matrix band will largely be short, there is a risk that the marginal ridge will overlap the
determined by the distance between the cervical cavity margin marginal ridge of the adjacent tooth, or even worse, will
and the adjacent tooth. Guidelines regarding selection of the bond to an existing composite restoration of the adjacent
matrix band are presented in Fig 13. In line with the extensive tooth.
clinical experience of one of the authors (PV), a hard steel In case a BioFit matrix (Bioclear Matrix Systems) is used,
metal contoured sectional matrix (sectional [TORVM], saddle the occlusal embrasure is included in the matrix band. If
matrix [TORVM], perforated metal matrix [TOVM]) are advised the correct height of the matrix band is selected, the den-
in 90% of the clinical cases, while a BioFit matrix (Bioclear tist has good control, provided the occlusal embrasure is in
Matrix Systems) is advisable in 10% of the cases. a correct position (Figs 16a to 16d).
It is beyond the scope of this article to discuss the treat- In addition, the matrix band should be centered bucco-
ment of extreme situations with deep cervical cavity mar- r lingually so that the contact area will be in the correct posi-
gins (Figs 11d and 14). This was described in detail by tion in a bucco-lingual direction (Figs 16c to 16e).
Venuti in 2018.38
Stabilization of the Matrix Band, Interdental
Positioning of the Matrix Band: Control Position in a Separation, Evaluation of Contact Area and Fit to the
Cervico-occlusal and Bucco-lingual Direction Cavity Margins
The matrix band should be inserted into the interproximal Stabilization of the matrix band can be obtained using a
space without any friction (with free axis of insertion) and wedge, a separation ring, teflon tape, and a flowable block-
should have the correct height. This is ±0.5 mm above the out resin. The different possibilities and indications are dis-
marginal ridge of the adjacent tooth (Fig 15), in order to cussed below.
30 The Journal of Adhesive Dentistry
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
Fig 23 (a) Initial situation. Proximal caries lesions were present
on the 1st (distal side) and 2nd premolar (mesial and distal side).
(b) Rubber-dam isolation and final class-2 cavity preparations with
interproximal clearance. (c) The large distance between the distal
cervical cavity margin of the 2nd premolar and 1st molar requires
the use of a more curved matrix band. (d) A BioFit HD matrix band a b
(Bioclear Matrix Systems) was selected and positioned. (e). Buccal
view of the cavity preparations. (f) After positioning of the matrix
band, one can notice that the contact area and the marginal ridge
are in the correct position. (g) Palatal view after placement of the
matrix band. (h) Positioning of the separation clamp (Twinring) and
placement of a Diamond wedge (Bioclear Matrix Systems). At the
mesial side a sectional matrix band (TORVM) was positioned and
fixed with a wooded wedge. The matrix band was relocated with teflon
tape in the mesial cavity of the 1st premolar. A separation clamp is c d
not needed at the mesial side. (i) The composite restoration on the
2nd premolar was placed and the matrix bands were removed-occlusal
view. (j) Buccal view- both proximal surfaces show an adequate
proximal contour. A well-positioned contact area can be noticed
between 1st molar and 2nd premolar. (k) After restoring both pre-
molars an adequate interdental anatomy is observed-occlusal view.
(l) Buccal view.
e f
g h
Wedge
The wedge has a double function. First, separation is real-
ized between the teeth, which compensates for the matrix
thickness and enables establishing a strong interproximal
i j
contact. Second, the wedge needs to adapt the matrix
accurately to the contour of the tooth all around the cavity
floor. The wedge can be inserted from either the lingual or
buccal side or even from both, provided that the matrix
remains closely adapted to the cavity floor. The wedge is
most commonly inserted from the lingual side, as the lin-
gual triangular embrasure is wider than the buccal one.
A large variety of wedges is available on the dental market
(Fig 17). k l
Wooden wedges
Anatomical hard wooden wedges are preferred as they have
a larger separation effect than soft wooden wedges.
If the upper part of the wedge is higher than the cavity Plastic and silicone wedges
floor, it will cause a convexity of the matrix towards the in- Plastic V-shaped wedges and their proprietary sectional ma-
terior of the cavity. In this situation, the wedge must be trix system are availbe from several manufacturers. These
customized (Fig 18). wedges are open at the gingival side, so that they do not
The wedge also needs customization in situations where interfere with the interdental papilla and do not displace the
concavities are present in the proximal cervical area, such rubber-dam. This allows them to be pushed further into the
as the mesial side of the upper 1st premolar and lower 1st interdental area and results in a good fixation of the matrix
molar, as well as the distal side of upper 1st molar.30 band. Their flexibility allows them to adapt the matrix band
Vol 23, No 1, 2021 31
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
Fig 24 (a) Cavity preparation. (b) Place-
ment of the sectional matrix band fixed with
a hard wooden wedge (also used for pre-
wedging). A contact area between matrix
band and adjacent tooth can be noticed. In
this situation, a separation clamp is not re-
quired. (c) Final restoration after removal of
rubber-dam, showing a tight and well-con-
a b c toured proximal surface and marginal ridge.
Fig 25 a) Layering of the box starts with application of the adhe-
sive, followed by (b) placement of a 1.5-2 mm layer of highly filled
flowable composite in the cervical part of the box, in order to im-
a b prove the internal and marginal adaptation in this critical area of the
box.31 (c) Further build-up of the proximal enamel wall with a con-
ventional small particle hybrid composite, in order to have the best
physico-mechanical properties in the area of the marginal ridge. (d)
In the occlusal cavity, the dentin part is replaced with a highly filled
flowable composite. Enamel replacement is performed with a small
particle hybrid composite following the successive cusp build-up
technique.31 (e) After contouring and finishing the interdental anat-
c d e omy is restored.
more easily to the cervical cavity margin. Their separation sulting in more even tension, and better adaptation of the
effect is less effective than wooden wedges. matrix band to the buccal and lingual surface of the tooth,
Diamond wedges (Bioclear Matrix Systems) are used in and will reduce proximal overhangs.23
combination with the transparent BioFit matrices (Fig 19). Placement of a separation clamp also has drawbacks.
They are available in different sizes (S, M, L, XL). In addi- On the one hand, straightening of the matrix band in the
tion, a deep caries/fluting model (the green-coded color) is occlusal third is often noticed (Figs 21a and 21b). This
available, which is able to adapt the matrix well to deep strongly reduces the presence of a natural occlusal embra-
cavity margins (Figs 19b to 19e). The diamond cutout allows sure. Contouring the marginal ridge after removal of the ma-
the wedge to pass through the narrow part of the embrasure trix band increases the finishing time. On the other hand,
and then opens to stay locked in place and apply pressure the sectional metal matrix band sometimes opens in the
evenly to avoid line-angle overhangs. The wedges show a cervical area after placement of the wedge and positioning
low profile in order not to push the matrix inside the cavity. of the separation clamp (Figs 21c and 21d). It can be diffi-
cult and quite time consuming to close this gap at the cervi-
Separation clamp cal cavity margin by pushing teflon tape in between the
Next to the use of a wedge, a separation clamp will create wedge and the matrix band.
interdental separation and stabilize the matrix band. A large Because of these shortcomings, the following strategy is
variety of separation clamps is available on the dental mar-r presented regarding use of a separation clamp.
ket (Fig 20). The rings of the clamp are made out of stain- When two opposite class-2 cavities need to be restored,
less steel or Ni-titanium. In general, stainless steel rings it is preferred not to use a separation clamp when restoring
have a weaker separation effect compared to Ni-titanium the first box. When the matrix band has an ideal contour
rings, and they lose their separation effect more easily. after positioning, it will only be stabilized by the wedge. Tef-
f
Most rings are angled to allow stackability in any combina- lon tape can be placed in the opposite cavity to stabilize or
tion for MOD and multiple-tooth restorations. The ring relocate the matrix (Fig 22). Some flowable composite or
prongs can be made out of stainless steel, Ni-titanium, block-out resin can be used to increase stabilization of the
glass fiber-reinforced plastic or soft silicone. The prongs matrix band. Contouring of the proximal surface after re-
can be straight or have a V-shaped end. Ring prongs with a moval of the matrix band will be strongly reduced or even
V-shaped end can be placed in a more stable position re- superfluous (Fig 22d).
32 The Journal of Adhesive Dentistry
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
To restore a single box in a quadrant using a BioFit Ma- Several in vitro and in vivo studies have shown that de-
trix (BioClear Matrix systems), a separation clamp is re- spite all efforts to prevent interproximal overhang, complete
quired in order to obtain a strong contact area. The V- prevention of overhang in the cervical third of the box is al-
shaped separation ring of the Bioclear matrix system most impossible.12,22,23,27,29 However, in none of these
(Twinring, Bioclear Matrix Systems) creates a strong separa- studies was teflon tape used to improve the adaptation be-
tion force. After positioning of clamp and wedge, one can tween matrix band and cavity margins. Nevertheless, it re-
control the location of the contact area (Fig 23). mains a difficult task to have complete control over mar-
For the restoration of a single box in a quadrant and use ginal adaptation in the cervical area in the different clinical
of a sectional metal matrix, there are two options. situations. If the marginal overhang is adhesively attached,
If, after positioning of the matrix band fixed with a and is smooth and continuous, the effect on the periodon-
wooden wedge, the matrix band has an adequate contour tal condition can be expected to be negligble.
and contacts the adjacent tooth, placement of the separa-
tion clamp is not needed (Fig 24). The interdental separa- Flowable or block-out resin
tion created by the wedge (on the condition that pre-wedg- Block-out or flowable resin can be applied between matrix
ing was also carried out) will be strong enough to finally band and adjacent tooth in order to help in stabilize the
obtain a tight contact area. matrix band, especially in these situations where a separa-
If the matrix band does not make contact with the adja- tion clamp is not used. (Figs 12c, 22c).
cent tooth after fixation with the wedge, a separation clamp
is required in order to obtain a strong contact area. Recre- Composite Layering
ation of a naturally contoured occlusal embrasure with com- After correct positioning and stabilization of the matrix
posite finishing disks may be required. band, the adhesive is applied and composite layering is
For the restoration of a MOD cavity, it is preferable to performed (Fig 25).31
apply the matrix and ring at one location and the matrix at
the other contact area, then restore the first contact area, It is the aim of the protocol presented in this article to pro-
remove the first ring and afterwards apply the second ring. vide the general dentist with guidelines, tips, and tricks to
Placement of the two rings simultaneously both mesially obtain adequate interdental anatomy and marginal adapta-
and distally results in a separation effect in the opposite tion in class-2 composite restorations. The protocol is
direction and therefore diminishes their effect at the ap- based on extensive clinical experience of one of the au-
plied contact area.24 thors. A possible point of critique is that the protocol is
In two clinical trials, the contact tightness of proximal not completely evidence based. The only evidence found
boxes restored by using a metal sectional matrix band and in the literature is that using a sectional matrix band in
separation clamp was stronger than before treatment. How- combination with a separation clamp showed the best re-
ever, none of the patients participating in these studies re- sults in creating a tight contact point. In the authors’ opin-
ported any discomfort when such a tight contact area was ion, it is quite impossible to have a completely evidence-
constructed.25,41 In a 6-month follow-up, Loomans et al25 based protocol, as the large variation in clinical situations
reported that tighter contacts tend to loosen and weaker requires customization of the interdental area.
contacts remain almost unchanged. From these results, one
may conclude that achieving a tight contact is preferred.
CONCLUSION
Teflon tape
Teflon is a polymer of tetrafluoroethylene. It is a plastic, To obtain a tight, well-positioned contact area and ana-
non-sticky material resistant to high temperatures. Teflon is tomically contoured proximal surface in class-2 direct com-
commonly used in several fields of industry, from aero- posite restorations, the following steps in the clinical pro-
space and computer applications to frying pans. During the tocol are important: rubber-dam isolation, pre-wedging,
last decade, the classic plumber’s teflon tape has also space evaluation, interproximal clearance, selection, posi-
been used in the dental office. tioning and stabilization of the matrix band. In order to
Teflon tape can be used to relocate the matrix when two customize the interdental area, sectional contoured matrix
class-2 cavities next to each other have to be restored in bands with different curvatures are required. The curvature
order to correctly position the matrix band (Figs 22c, 23h). of the matrix band is largely determined by the distance
For restoration of the proximal box of a class-2 cavity, between the cervical cavity margin of the class-2 cavity
teflon can be used to push the matrix towards the tooth to and the adjacent tooth. The matrix band should be strong
optimize the adaptation of matrix to the cavity margins (buc- and not deform plastically. A separation clamp should be
cal, lingual and cervical) (Figs 6c, 11d). This results in a used depending on the clinical situation. Finally, it is im-
slight excess of composite at the cavity margins and re- portant to obtain a tight adaptation between matrix band
duces the finishing time of the restoration. A tight fit should and cavity margins before applying the composite.
most certainly be obtained in the cervical area, where ac-
cess with finishing instruments is difficult and can endan-
ger the integrity of the teeth and the periodontium.
Vol 23, No 1, 2021 33
Personal PDF for Authors (Specimen copy), Account ID 916717, created at 03.02.2021
Copyright 2021, Quintessenz Verlags-GmbH
Peumans et al
ACKNOWLEDGMENTS 24. Loomans BA, Opdam NJ, Roeters JF, Bronkhorst EM, Plasschaert AJ. In-
fluence of composite resin consistency and placement technique on prox-
The authors thank Dr. Javier Tapia Guadix (restorative dentist, Spain) imal contact tightness of Class II restorations. J Adhes Dent 2006;8:
305–310.
for kindly providing the pictures of the clinical case presented in Fig 6.
25. Loomans BAC, Opdam NJM, Roeters FJM, Bronkhorst EM, Plasschaert
AJM. The long-term effect of a composite resin on proximal contact tight-
ness. J Dent 2007;35:104–108.
REFERENCES 26. Loomans BAC, Roeters FJM, Opdam NJM, Kuijs RH. The effect of proxi-
mal contour on marginal ridge fracture of Class II composite resin resto-
1. Albers HF. Posterior resins: Class II preparations. In: Albers HF (ed). rations. J Dent 2008;36:828–832.
Tooth Colored Restoratives, ed 9. London: BC Decker, 2001:219–233. 27. Müllejans R, Badawi MOF, Raab WHM, Lang H. An in vitro comparison of
2. Ash MM. Wheeler’s dental anatomy, physiology and occlusion, ed 7. Phil- metal and transparent matrices used for bonded Class II resin composite
adelphia: W.B. Saunders, 1993:102–307. restorations. Oper Dent 2003;28:122–126.
3. Brand R, Isselhard DE. Fundamental and preventive curvatures. Proximal 28. Nash RW, Lowe RA, Leinfelder K. Using packable composite for direct
alignment of the teeth and protection of the periodontium. In: Brand R, posterior placement. J Am Dent Assoc 2001;132:1099–1104.
Isselhard DE (eds). Chapter 3: Anatomy of orofacial structures – A com- 29. Opdam NJM, Roeters FJM, Feilzer AJ, Smale I. A radiographic and scan-
prehensive approach, enhanced 7th ed. St Louis: Mosby, 2014:28–36. ning electron microscopic study of approximal overhangs of Class II resin
4. Clark D. The seven deadly sins of traditional Class II restorations. Dent composite restorations placed in vivo. J Dent 1998;26:319–327.
Today 2017;36:119–121. 30. Patras M, Doukoudakis S. Class II composite restorations and proximal
5. Chuang SF, Su KS, Wang CH, Chang CH. Morphological analysis of proxi- concavities: clinical implications and management. Oper Dent 2013;38:
mal contacts in Class II direct restorations with 3D image reconstruction. 119–124
J Dent 2011;39:448–456. 31. Peumans M, Politano G, Bazos P, Severino D, Van Meerbeek B. Effective
6. de la Peña VA, Garcia RP, Garcia RP. Sectional matrix: step-by-step direc- and simplified protocol for daily high-quality direct posterior composite res-
tions for their clinical use. Br Dent J 2016;220:11–14. torations. ‘The simplified layering and finishing protocol’. J Adhes Dent
7. Dörfer CE. Der Approximalraum. Dtsch Zahnartzl Z 1997;52:151–167. 2020;22:581–596.
8. Dörfer CE, Schriever A, Heidemann D, Staehle HJ, Pioch T. Influence of 32. Peumans M. Politano G, Van Meerbeek B. Effective and simplified proto-
rubber-dam on the reconstruction of proximal contacts with adhesive col for daily high-quality direct posterior composite restorations: Cavity
tooth-colored restorations. J Adhes Dent 2001;3:169–175. preparation and design; the ‘hidden quality’ of the posterior composite
restoration. J Adhes Dent 2020;22:597–614.
9. Dörfer CE, von Bethlenfalvy ER, Staelhe HJ, Pioch T. Factors influencing
proximal dental contact strengths. Eur J Oral Sci 2000;108:368–377. 33. Peumans M, Van Meerbeek B, Asscherickx K, Simon S, Abe Y, Lambrechts
P, Vanherle G. Do condensable composites help to achieve better proximal
10. El-Shamy H, Saber MH, Dörfer CE, El-Badrawy W, Loomans BAC. Influ-
contacts? Dent Mater 2001;17:533–541.
ence of volumetric shrinkage and curing light intensity on proximal con-
tact tightness of Class II resin composite restorations: in vitro study. 34. Rau PJ, Pioch T, Staehle HJ, Dörfer CE. Influence of the rubber-dam on
Oper Dent 2012;37:205–210. proximal contact strengths. Oper Dent 2006;31:171–175.
11. Eli I, Weiss E, Kozlovsky A, Levi N. Wedges in restorative dentistry: princi- 35. Saber MH, El-Badrawy W, Loomans BAC, Ahmend DR, Dörfer CE, El Zohairy
ples and applications. J Oral Rehabil 1991;18:257–264. A. Creating tight proximal contacts for MOD resin composite restorations.
Oper Dent 2011;36:304–310.
12. Frankenberger R, Krämer N, Pelka M, Petschelt A. Internal adaptation
and overhang formation of direct Class II composite restorations. Clin 36. Saber MH, Loomans BAC, El Zohairy A, Dörfer CE, El-Badrawy W. Evaluation
Oral Investig 1999;3:208–215. of proximal contact tightness of Class II resin composite restorations.
Oper Dent 2010;35:37–43.
13. Hancock EB, Mayo CV, Schwab RR, Wirthlin MR. Influence of interdental
contacts on periodontal status. J Periodontol 1980;51:445–449. 37. Santana-Mora U, López-Cedrún J, Mora MJ, Otero XL, Santana-Penín U.
Temporomandibular disorders: the habitual chewing side syndrome. PLoS
14. Hellie CM, Charbeneau GT, Craig RG, Brandau HE. Quantitative evalua-
One 2013;8:e59980
tion of proximal tooth movement effected by wedging: a pilot study. J
Prosthet Dent 1985;53:335–341. 38. Venuti P. Rethinking deep marginal extension (DME). IJCD 2018;7:26–32.
15. Jernberg GR, Bakdash MB, Keenan KM. Relationship between proximal 39. Von Bethlenfalvy ER, Staelhe HJ, Dörfer CE. Einfluss marginal parodontitis
tooth open contacts and periodontal disease. J Periodontol 1983;54: auf die approximale kontaktstärke. Dtsch Zahnartzl Z 2000;55:411–416.
529–533. 40. Wang JC, Charbeneau GT, Gregory WA, Dennison JB. Quantitative evalua-
16. Kampouropoulos D, Paximada C, Loukidis M, Kakaboura A. The influence tion of proximal contacts in class 2 composite resin restorations: a clini-
of matrix type on the proximal contact in Class II resin composite restora- cal study. Oper Dent 1989;14:193–202.
tions. Oper Dent 2010;35:454–462. 41. Wirshing E, Loomans BAC, Klaiber B, Dörfer CE. Influence of matrix sys-
17. Keogh TP, Bertolotty RI. Creating tight, anatomically correct interproximal tems on proximal contact tightness of 2- and 3- posterior composite res-
contacts. Dent Clin North Am 2001;45:83–102. torations in vivo. J Dent 2011;39:386–390.
18. Loomans B, Hilton T. Extended resin composite restorations: techniques
and procedures. Oper Dent 2016;(suppl 7):S58–S67.
19. Loomans B, Opdam NJM, Roeters FJM, Bronkhorst EM, Burgersdijk RCW.
Comparison of proximal contacts of Class II resin composite restorations
in vitro. Oper Dent 2006;31:688–693.
20. Loomans BAC, Opdam NJM, Roeters FJM, Bronkhorst EM, Burgersdijk
RCW, Dörfer CE. A randomized clinical trial on proximal contacts on pos-
terior composites. J Dent 2006;34:292–297. Clinical relevance: Placement of a Class-2 composite
21. Loomans BAC, Opdam NJM, Bronkhorst EM, Roeters FJM, Dörfer CE. A restoration with correct interdental anatomy and strong
clinical study on interdental separation techniques. Oper Dent 2007;32: contact area requires the use of a contoured sectional
207–211.
matrix band. The matrix band must be strong and not
22. Loomans BAC, Opdam NJM, Roeters FJM, Bronkhorst EM, Huysmans
NCDNJM. Restoration techniques and marginal overhang in Class II com- deform plastically. The maximum contour of the matrix
posite resin restorations. J Dent 2009;37:712–717. band is largely determined by the distance between the
23. Loomans BAC, Opdam NJM, Roeters JM, Huysmans MCDNJM. Proximal cervical cavity margin and the adjacent tooth.
marginal overhang of composite restorations in relation to placement
technique of separation rings. Oper Dent 2012;37:21–27.
34 The Journal of Adhesive Dentistry
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5813)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Dsce High YieldDocument29 pagesDsce High YieldLorenzini Grant50% (2)
- Ceu Revalida Word97 2003docDocument874 pagesCeu Revalida Word97 2003docChelo Jan Geronimo82% (11)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Schoenbaum Implant Prosthetics in The Aesthetic Zone Science Protocol TechniquesDocument24 pagesSchoenbaum Implant Prosthetics in The Aesthetic Zone Science Protocol TechniquesЮля КолмаковаNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Toxic Tooth Root Canal Mercola InterviewDocument13 pagesToxic Tooth Root Canal Mercola InterviewAntonio PitaguariNo ratings yet
- UnknownDocument370 pagesUnknownTrương Văn ĐôngNo ratings yet
- Breed Predispositions To Dental and Oral Disease in Dogs 1St Edition Brook Niemiec Full ChapterDocument33 pagesBreed Predispositions To Dental and Oral Disease in Dogs 1St Edition Brook Niemiec Full Chaptermartha.wallace593100% (10)
- Orthodontic Management of A Horizontally Impacted Maxillary Incisor in An Adolescent PatientDocument11 pagesOrthodontic Management of A Horizontally Impacted Maxillary Incisor in An Adolescent PatientMarcos Gómez SosaNo ratings yet
- Teacher'S Health Card: SHD Form 4Document3 pagesTeacher'S Health Card: SHD Form 4Chonie VillanuevaNo ratings yet
- Al-Harbi - 2018 - A Guide To Minimally Invasive Crown Lengthening and Tooth Preparation For Rehabilitating Pink and White AeDocument7 pagesAl-Harbi - 2018 - A Guide To Minimally Invasive Crown Lengthening and Tooth Preparation For Rehabilitating Pink and White AefishribbonNo ratings yet
- 21 Principles of Smile DesignDocument44 pages21 Principles of Smile DesignOT100% (2)
- Prometric 2015 DR - Kadeeb Vol1.0. Jan2015 SolvedDocument54 pagesPrometric 2015 DR - Kadeeb Vol1.0. Jan2015 SolvedSubhajit Saha0% (1)
- Facial Aesthetics: International Journal of Current Research June 2015Document7 pagesFacial Aesthetics: International Journal of Current Research June 2015SUMEET SODHINo ratings yet
- Simplified Papila Cortellini 1999Document13 pagesSimplified Papila Cortellini 1999Razvan SalageanNo ratings yet
- Assessment Mouth and Oropharynx LipsDocument8 pagesAssessment Mouth and Oropharynx LipsQuinmarc LimNo ratings yet
- Pre Treatment Assesment of ImplantDocument19 pagesPre Treatment Assesment of Implantdrgayen6042No ratings yet
- ADocument8 pagesARaghava DasariNo ratings yet
- Alginate Impression MaterialDocument92 pagesAlginate Impression MaterialrusschallengerNo ratings yet
- Porcelain Fused To Metal (PFM) Crowns and Caries in Adjacent TeetDocument5 pagesPorcelain Fused To Metal (PFM) Crowns and Caries in Adjacent Teetbaiq rengganis dewiNo ratings yet
- Jurnal NUPDocument10 pagesJurnal NUPsusi apriliantyNo ratings yet
- SPEAR Biologic Width EbookDocument33 pagesSPEAR Biologic Width EbookalyssaNo ratings yet
- Maxillary Injection TechniquesDocument127 pagesMaxillary Injection TechniquesD YasIr MussaNo ratings yet
- Caries Case StudyDocument19 pagesCaries Case Studyapi-279025476No ratings yet
- 5phase II Periodontal TherapyDocument54 pages5phase II Periodontal TherapyKaraz StudiosNo ratings yet
- Very Good Guide For Fixed ProsthoDocument71 pagesVery Good Guide For Fixed ProsthoKaty Svensson100% (2)
- 10 Tips About Aesthetic ImplantologyDocument16 pages10 Tips About Aesthetic ImplantologyMario Troncoso Andersenn0% (1)
- A Review of The Functional and Esthetic RequirementDocument9 pagesA Review of The Functional and Esthetic RequirementAna Massiel NarváezNo ratings yet
- Surgical Crown LengtheningDocument96 pagesSurgical Crown LengtheningJevin Stivie Cialy100% (2)
- Paper Getis IDocument3 pagesPaper Getis IAlaghen VespanathanNo ratings yet
- Krok 2 Stomatology: Test Items For Licensing ExaminationDocument28 pagesKrok 2 Stomatology: Test Items For Licensing ExaminationjimmyNo ratings yet
- Peri ImplantitisDocument12 pagesPeri ImplantitisbobNo ratings yet