Professional Documents
Culture Documents
Behavioral and Psychological Symptoms of Dementia (BPSD) and Their Management
Uploaded by
Kreshnik Idrizaj0 ratings0% found this document useful (0 votes)
43 views33 pages...
Original Title
behavioralandpsychologicalsymptomsofdementia-131210100409-phpapp01
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document...
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
43 views33 pagesBehavioral and Psychological Symptoms of Dementia (BPSD) and Their Management
Uploaded by
Kreshnik Idrizaj...
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 33
Behavioral and psychological
symptoms of dementia(BPSD) and
their management:
Dr.Roopchand.PS
Senior Resident Academic
Department of Neurology
Introduction:
• Behavioral changes, paranoid
delusions, hallucinations and long periods of
screaming were described by Alzheimer in
1907 in his original case description of the
disease.
• An integral part of dementia syndrome.
• BPSD is associated with a more rapid rate of
cognitive decline and greater impairment in
activities of daily living.
• A burden to patients and care givers.
• Costs significantly to overall cost of dementia
care.
• Most of them are treatable.
Prevalence:
• Reported prevalence of BPSD ranges from 50%-
100%.
• BPSD were severe in 36.6% of the
patients, moderate in 49.3%, and mild in 14.1%.
• Depression, apathy and anxiety were the most
common.
• Depending upon cognitive levels, variation in
BPSD frequencies have been reported.
– 92.5% in patients with a MMSE between 11 and 20.
– 84% of the patients with a MMSE between 21 and 30.
FEATURES OF BPSD:
• Myriad manifestations.
• Inappropriate behaviors:
– Physically aggressive behavior : hitting, kicking or
biting
– Physically nonaggressive behavior: pacing or
inappropriately handling objects
– Verbally non aggressive agitation: constant
repetition of sentences or requests.
– Verbal aggression: cursing or screaming
• 24% and 48% of dementia patients have
motor behavioural abnormalities.
• Physical violence and hitting occurs in
approximately 30% in Alzheimer’s dementia
(AD).
• Predictors of aggressive behavior:
– Premorbid history of aggression
– Troubled premorbid relationship between
caregiver and patient
– Multiple problems.
• Wandering:
– Quarter fo AD patients have wandering.
– Elderly wanderers have language impairment,
disorientation and hyperactivity compared to non
wanderers.
– Wanders exhibit better social skills and are less
withdrawn.
• Mood Disturbances:
– Depression is common.
– may not have a typical presentation.
– lack of sad or depressed affect.
• Depressive cognitions, death wishes are
common.
• Anxiety, fear, irritability, anger are also seen.
• Apathy : 70-90% of AD.
• Syndrome of decreased initiation and
motivation, decreased social
engagement, emotional
indifference, diminished reactivity and lack of
persistence.
• Apathy or Depression?
– Dysphoria, hopelessness, guilt, self-criticism,
suicidal ideation, sleep problems and appetite
disturbances are associated with depression.
• Personality change:
– Increasing passivity, coarsening of affect,
decreased spontaneity, inactivity, feelings of
insecurity, less cheerfulness and responsiveness.
– Reduced initiative and drive, grossly insensitive
behavior, lack of restraint, disinhibition, sexual
misadventure, indolence, foolish jokes and pranks
• Psychotic features:
– usually paranoid in nature.
– some one is stealing things, being present in the
room, living inappropriately in the home
(phantom boarder), mishandling personal
finances, planning to harm physically.
– delusions of
infidelity, hypochondriasis, zoopathy, dead
relatives being still alive, erotomania, Capgras
syndrome, believing television images are
real, personal images in a mirror is a different
person, misidentifying own home.
• Other symptoms:
– Screaming is seen in 25%.
– high degree of dependency for ADL.
– Sleep disturbance.
– Dependency for excretory functions and hygiene
maintenance come as a burden to caregivers.
TYPES OF DEMENTIA AND BPSD:
• Some type of BPSD are more common in
certain type dementia.
• AD:
– Aspontaneity and reduced initiative in early
stages.
– Behavioral symptoms occur ad disease progress.
– Aggression, wandering, incontinence, and at least
one symptom of Klüver-Bucy syndrome was found
in 72%.
• DLB:
– Visual hallucinations- more complex, vivid and
rapidly moving.
– Auditory hallucinations, persecutory delusions.
– Fluctuating.
• VaD:
– Judgment and insight is relatively preserved.
– Extreme anxiety and depression.
– Lability and explosive emotional outbursts,
episodes of noisy weeping or laughing
• Pick’s dementia:
– Changes of character and social behavior more.
– Fatuous euphoria or apathy,insensitive behavior, lack
of restraint, and sexual misadventure have been seen.
– Hypermetamorphosis occur early than AD.
• Dementia due to Huntington’s disease:
– Emotional disturbance is a prominent premonitory
feature.
– BPSD are reported for some considerable time before
chorea.
– Paranoid developments may be earliest manifestation.
– Delusions of persecution, religiosity, reference and
grandiosity are common.
– schizophrenic or paraphrenic illness may be present
for years before HD.
• Creutzfeldt-Jakob disease (CJD):
– characterized by neurasthenic symptoms.
– Fatigue, insomnia, anxiety, depression, mental
– slowness and unpredictability of behavior,
auditory hallucinations and delusions are the
usual complaints.
• Alcoholic dementia:
– Profound social disorganization
– Deterioration of personality.
ETIOLOGY OF BPSD:
• Various theoretical models have been
proposed.
• ‘Unmet needs’ model
• A behavioral/learning model
• Environmental vulnerability/reduced stress-
threshold model.
• Premorbid personality has also been linked to
BPSD.
• It has been suggested that some BPSD could
be the consequence of both dementia and an
undiagnosed comorbid bipolar spectrum
disorder or a pre-existing bipolar diathesis
pathoplastically altering the clinical expression
of dementia.
• An imbalance of different neurotransmitters
(acetylcholine, dopamine, noradrenaline, sero
tonin,GABA) has been proposed as the
neurochemical correlate of BPSD.
– increased norepinephrine (NE) activity and/or
hypersensitive adrenoreceptors compensating for
loss of NE neurons – in AD
– Increased activity of dopaminergic
neurotransmission and altered serotonergic
modulation of dopaminergic neurotransmission is
associated with agitated and aggressive behavior
in FTD.
• DAT1 3’-UTR VNTR polymorphism may play a
role in BPSD susceptibility.
ASSESSMENT:
• Depends on history from care giver.
• Specific assessment scales are available.
– Apathy Evaluation Scale (AES)
– Behavioural Rating Scale for Geriatric Patients
– Behaviour Pathology in Alzheimer’s Disease Rating Scale (BEHAVE-
AD)
– Behavioural Rating Scales for Dementia
– Cohen-Mansfield Agitation Inventory (CMAI)
– Cornell Scale for Depression in Dementia (CSDD)
– Frontal Systems Behaviour Inventory (FrSBe)
– Neuropsychiatric Inventory (NPI)
– Neuropsychiatric Inventory– Nursing Home version (NPI-NH)\
– Apathy Inventory (AI)
– Behavioural and Psychological Symptoms Questionnaire (BPSQ).
MANAGEMENT OF BPSD:
• Psychological, behavioral, environmental, and
pharmacological interventions.
• Nonpharmacological intervention is the
preferred initial method of intervention for
BPSD.
Nonpharmacological Intervention
Environmental modifications:
• Environment around the patient can be modified
for a beneficial effect on the BPSD.
• Simulated home environment with appropriate
visual, auditory and olfactory stimuli which may
decrease the chance of trespassing, exit seeking
and other agitation behaviors.
• Reduced stimulation environments.
• Environment can be modified by installing
adequate daytime lighting to improve sleep
patterns in patients with disturbed sleep wake
cycles.
Social interactions:
• One to one interaction for 30 min per day for
10 days has been found to be effective in
decreasing verbally disruptive behavior.
• Regular intensive interaction help in reality
orientation.
• Socialization can be increased by group
activity, conjoint tasks and simple games.
• Displaying photos of near relatives.
• Pet therapy.
Minimize the impact of sensory
deficits:
• Corrective eyeglasses and hearing aids
decrease risk of disorientation.
• Slow and repetitive explanations reduce
confusion and agitation.
Medical and nursing interventions:
• Prompt management of pain is helpful.
• Adequate sleep hygiene – decreases agitation.
• Agitation secondary to fatigue and circadian
rhythm disturbances can be reduced by bright
light therapy.
• Music therapy has been shown to be effective
to reduce BPSD in patients with moderate-
severe dementia.
Behavioral interventions:
• Extinction, differential reinforcement and
stimulus control.
• Reinforcements include social
reinforcements, food, touch, going
outside, etc.
• Consistent daily routines.
• Exercises, removal of restraints, and adequate
rest help in reducing the inappropriate
behavior.
• Spiritual and religious activities.
Pharmacological Intervention:
References:
• Nilamadhab Kar; Behavioral and psychological symptoms of
dementia and their management; Indian J Psychiatry. 2009
January; 51(Suppl1): S77–S86.
• Manjari Tripathi, Deepti Vibha; An approach to and the
rationale for the pharmacological management of behavioral
and psychological symptoms of dementia; IAN 2010; 9
• Franz Müller-Spahn,MD; Behavioral disturbances in
dementia.
• Bradley's Neurology in Clinical Practice, 6th edition
You might also like
- Borderline Personality DisorderDocument128 pagesBorderline Personality Disorderعمر الحدادNo ratings yet
- Psychiatric Disorders in the Elderly: Depression, Anxiety, Dementia, and Sleep IssuesDocument28 pagesPsychiatric Disorders in the Elderly: Depression, Anxiety, Dementia, and Sleep IssuesMienaNo ratings yet
- ALZHEIMERDocument9 pagesALZHEIMERKhem Limoso100% (2)
- Psychiatric Illness: Schizophrenia and Major DepressionDocument23 pagesPsychiatric Illness: Schizophrenia and Major DepressionLealiza B. BruceNo ratings yet
- Sschizophrenia LectureDocument27 pagesSschizophrenia Lectureepic sound everNo ratings yet
- Schizophrenia 2 (Treatment) 2023Document18 pagesSchizophrenia 2 (Treatment) 2023Phoebe LauNo ratings yet
- DEMENTIASDocument33 pagesDEMENTIASchebetnaomi945No ratings yet
- DepressionDocument40 pagesDepressionRubilyn SumayloNo ratings yet
- Dementia: DR Ayunga A.O Physician/lecturer MedicineDocument34 pagesDementia: DR Ayunga A.O Physician/lecturer MedicineMalueth AnguiNo ratings yet
- Antipsychotics For The Treatment of Behavioral and PsychologicalDocument25 pagesAntipsychotics For The Treatment of Behavioral and PsychologicalapaajabolehNo ratings yet
- Understanding Delirium, Dementia and DepressionDocument27 pagesUnderstanding Delirium, Dementia and Depressionadvpracrn1No ratings yet
- Schizophrenia and Other Psychotic Disorders: Southern Philippines Medical CenterDocument44 pagesSchizophrenia and Other Psychotic Disorders: Southern Philippines Medical CenterMaureen JadeNo ratings yet
- Medically Unexplained Symptoms BAHRIDocument58 pagesMedically Unexplained Symptoms BAHRIAhmed AlabwabiNo ratings yet
- 1 - Schizophrenia-PdDocument59 pages1 - Schizophrenia-PdአንዋርጀማልNo ratings yet
- Delirium: Second Year Resident Psychiatry, BMCDocument50 pagesDelirium: Second Year Resident Psychiatry, BMCDr viren SolankiNo ratings yet
- Bule Hora University Institute of health department of psychiatry Schizophrenia and other psychotic disordersDocument56 pagesBule Hora University Institute of health department of psychiatry Schizophrenia and other psychotic disordersErsido SamuelNo ratings yet
- Week 5 - Clinical PsychologyDocument89 pagesWeek 5 - Clinical PsychologyDora SimunovicNo ratings yet
- Somatoform and Sleep DisordersDocument24 pagesSomatoform and Sleep DisordersSegun Dele-davidsNo ratings yet
- SchizophreniaDocument50 pagesSchizophreniaNabina PaneruNo ratings yet
- Organic Brain SyndromeDocument40 pagesOrganic Brain SyndromeShaz ZrinNo ratings yet
- TX BehaviorDocument25 pagesTX BehaviorschenkoNo ratings yet
- Functional Neurological Symptoms in MS: Understanding FNDDocument32 pagesFunctional Neurological Symptoms in MS: Understanding FNDWaqas Ahmed UsmaniNo ratings yet
- Neurocognitive DisordersDocument26 pagesNeurocognitive DisordersGede GiriNo ratings yet
- Rawatan Klien Dua DiagnosisDocument60 pagesRawatan Klien Dua DiagnosisPUSAT LATIHAN AADKNo ratings yet
- SCHIZOPRENIADocument12 pagesSCHIZOPRENIAkalejaiye johnNo ratings yet
- Schizophrenia & Other Psychotic Disorders: Melinda Hermanns, MSN, RN, BCDocument52 pagesSchizophrenia & Other Psychotic Disorders: Melinda Hermanns, MSN, RN, BCrayanhereNo ratings yet
- Psych ReportDocument80 pagesPsych ReportPaul Carlo GonzalesNo ratings yet
- Mental Health - Chapter 10Document4 pagesMental Health - Chapter 10McKinley Anne CarlisleNo ratings yet
- SchizophreniaDocument14 pagesSchizophreniam3230404No ratings yet
- Anxiety Disorders: Types, Symptoms, Causes and TreatmentDocument52 pagesAnxiety Disorders: Types, Symptoms, Causes and TreatmentMuhammad MakkiNo ratings yet
- Mood Disord Ers: DO, RN, MA NDocument39 pagesMood Disord Ers: DO, RN, MA NKrishna BalsarzaNo ratings yet
- Schizophrenia and Psychotic Disorders PPT Chap 21Document46 pagesSchizophrenia and Psychotic Disorders PPT Chap 21Claudia SanchezNo ratings yet
- Psychosis: Fikirte Girma (M.D) Department of Psychiatry AAU November 2014Document42 pagesPsychosis: Fikirte Girma (M.D) Department of Psychiatry AAU November 2014Z26No ratings yet
- Mental Disorders: Sub Ject: Clinical Psychology Presented By: PHD - Mariana CernitanuDocument34 pagesMental Disorders: Sub Ject: Clinical Psychology Presented By: PHD - Mariana CernitanuAlbert PruteanuNo ratings yet
- Psychopathology: Schizophrenia Signs & Symptoms Possible Causes Nursing Diagnoses Treatment & Care Plans Teaching PlansDocument46 pagesPsychopathology: Schizophrenia Signs & Symptoms Possible Causes Nursing Diagnoses Treatment & Care Plans Teaching PlansNadeem IqbalNo ratings yet
- Mood Disorders - ArafatDocument40 pagesMood Disorders - Arafatمرتضى محمد منصورNo ratings yet
- Mood Disorders and SchizophreniaDocument6 pagesMood Disorders and SchizophreniaAdela ChristinaNo ratings yet
- OCD Guide: Understanding Obsessive-Compulsive DisorderDocument22 pagesOCD Guide: Understanding Obsessive-Compulsive DisorderaliNo ratings yet
- SchizophreniaDocument71 pagesSchizophreniaJessamine Rochelle Reyes Esberto100% (3)
- Mental Health Aging Part 1Document16 pagesMental Health Aging Part 1biscotticrcrowderNo ratings yet
- SchizophreniaDocument59 pagesSchizophreniaCrisia GungobNo ratings yet
- HIV and Mental Health: A Biopsychosocial PerspectiveDocument28 pagesHIV and Mental Health: A Biopsychosocial PerspectivePhaimNo ratings yet
- BPD overviewDocument11 pagesBPD overviewNurul Syazwani Ramli100% (1)
- Psyc 311Document20 pagesPsyc 311laralesch2002No ratings yet
- Depressive Disorders Day 1: Diagnosis & PrevalenceDocument20 pagesDepressive Disorders Day 1: Diagnosis & PrevalenceYoussef M.No ratings yet
- Schizophrenia and Other Psychotic DisordersDocument38 pagesSchizophrenia and Other Psychotic DisordersGeorgiana BlagociNo ratings yet
- Aging and Mental HealthDocument77 pagesAging and Mental HealthDarla SaulerNo ratings yet
- Dissociative DisordersDocument25 pagesDissociative DisordersKholoud KholoudNo ratings yet
- Agitation: Brought To You By: Synergy Narasumber: Dr. Irmia Kusumadewi, SPKJ (K)Document39 pagesAgitation: Brought To You By: Synergy Narasumber: Dr. Irmia Kusumadewi, SPKJ (K)Karel RespatiNo ratings yet
- Schizophrenia: 2 Most Frequent Diagnosis of Patients 14-64 Y/o at CRH in 2008Document52 pagesSchizophrenia: 2 Most Frequent Diagnosis of Patients 14-64 Y/o at CRH in 2008michaelNo ratings yet
- Rawatan Klien Dua DiagnosisDocument62 pagesRawatan Klien Dua DiagnosisPUSAT LATIHAN AADKNo ratings yet
- Schizophrenia and Other Psychotic DisordersDocument33 pagesSchizophrenia and Other Psychotic DisordersRey GomezNo ratings yet
- Gangguan Non PsikotikDocument15 pagesGangguan Non PsikotikGusti Zidni FahmiNo ratings yet
- Unit 2 Abnormal PsychologyDocument44 pagesUnit 2 Abnormal PsychologyMohammed SaniNo ratings yet
- Abnormal Behavior and Psychopathology: Clinical PsychologyDocument5 pagesAbnormal Behavior and Psychopathology: Clinical PsychologyJerine Bonus ApostolNo ratings yet
- Borderline Personality Disorder: The ultimate guide to borderline personality disorder including signs and symptoms, diagnosis, treatment, and how to improve and manage it!From EverandBorderline Personality Disorder: The ultimate guide to borderline personality disorder including signs and symptoms, diagnosis, treatment, and how to improve and manage it!No ratings yet
- A Simple Guide to Pick Disease, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Pick Disease, Diagnosis, Treatment and Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Mental Health Guide: For students, teachers, school psychologists, nurses, social workers, counselors and parents.From EverandMental Health Guide: For students, teachers, school psychologists, nurses, social workers, counselors and parents.No ratings yet
- Cognitive Behavioral Therapy (CBT) for Depression, Anxiety, Phobias and Panic AttacksFrom EverandCognitive Behavioral Therapy (CBT) for Depression, Anxiety, Phobias and Panic AttacksNo ratings yet
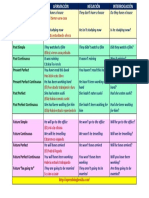
- Learn English verb tenses with examples of affirmation, negation and interrogationDocument1 pageLearn English verb tenses with examples of affirmation, negation and interrogationAnonymous QcXf4QNo ratings yet
- The Cinderella' Gas: Reading Part 4 - Matching Paragraphs To HeadingsDocument1 pageThe Cinderella' Gas: Reading Part 4 - Matching Paragraphs To HeadingscamaleonlanglearNo ratings yet
- Guia Aptis Resumen PDFDocument12 pagesGuia Aptis Resumen PDFJosé Antonio Ochoa GonzálezNo ratings yet
- New Guide To Medicines & Drugs - K TORODocument514 pagesNew Guide To Medicines & Drugs - K TOROKreshnik Idrizaj100% (1)
- Reading Unit 3Document2 pagesReading Unit 3Laura BernabéNo ratings yet
- FCE Reading Practice Test 1 KeyDocument2 pagesFCE Reading Practice Test 1 KeypabloNo ratings yet
- Exercise - Grammar Unit 2 - Comparative and Superlative PDFDocument2 pagesExercise - Grammar Unit 2 - Comparative and Superlative PDFlibbymcardNo ratings yet
- Exercise - Grammar Unit 2 - Adjectives - Ed and - Ing PDFDocument2 pagesExercise - Grammar Unit 2 - Adjectives - Ed and - Ing PDFRosa García RomeroNo ratings yet
- Τεστ ΑγγλικωνDocument0 pagesΤεστ ΑγγλικωνSouzanTheNo ratings yet
- Exercise - Grammar Unit 4 - Past TensesDocument2 pagesExercise - Grammar Unit 4 - Past TensesMaria BNo ratings yet
- APTIS Practice Tests BookDocument5 pagesAPTIS Practice Tests BookNOELIA100% (1)
- SpeakingDocument3 pagesSpeakingLorena Sánchez PérezNo ratings yet
- ZWMGWDPRAITWS - Concise for reading comprehension documentDocument28 pagesZWMGWDPRAITWS - Concise for reading comprehension documentHiếu LươngNo ratings yet
- Aptis Used To and WouldDocument2 pagesAptis Used To and WouldjuliNo ratings yet
- Aptis Grammar and Vocabulary Test - Final Preparation: 1 - Refresh Your MemoryDocument23 pagesAptis Grammar and Vocabulary Test - Final Preparation: 1 - Refresh Your MemoryKreshnik Idrizaj0% (1)
- Aptis Reading PDFDocument6 pagesAptis Reading PDFerikNo ratings yet
- 15ol1jD4SGGz9BAtM0ya - Team Approaches in Psychiatric Disease Roles and Responsibilities - RueggDocument26 pages15ol1jD4SGGz9BAtM0ya - Team Approaches in Psychiatric Disease Roles and Responsibilities - RueggKreshnik IdrizajNo ratings yet
- Aptis Mo CK: October 2015Document4 pagesAptis Mo CK: October 2015Kreshnik IdrizajNo ratings yet
- APTIS Grammar and Vocabulary TestDocument10 pagesAPTIS Grammar and Vocabulary TestQuang KhangNo ratings yet
- Aptis Grammar and Vocabulary Demo Test PDFDocument4 pagesAptis Grammar and Vocabulary Demo Test PDFZhanna50% (4)
- Aptis Practice Materials Reading Mock Test AnswersDocument13 pagesAptis Practice Materials Reading Mock Test Answersisa100% (8)
- Alcohol Use DisorderMay2021Document49 pagesAlcohol Use DisorderMay2021Kreshnik IdrizajNo ratings yet
- SSidhu 2020 Hansen Presentation For AttendeesDocument69 pagesSSidhu 2020 Hansen Presentation For AttendeesKreshnik IdrizajNo ratings yet
- 16 CPG Psychotherapies in CapDocument20 pages16 CPG Psychotherapies in CapKreshnik IdrizajNo ratings yet
- Alcohol and Tolerance - Alcohol Alert 95Document3 pagesAlcohol and Tolerance - Alcohol Alert 95Kreshnik IdrizajNo ratings yet
- 16 June Dementia - Personal Experience Robin ThomsonDocument15 pages16 June Dementia - Personal Experience Robin ThomsonKreshnik IdrizajNo ratings yet
- Activity - Grammar Unit 2 - QuantifiersDocument2 pagesActivity - Grammar Unit 2 - QuantifiersCecilia MuñozNo ratings yet
- Alcohol PresentationDocument12 pagesAlcohol PresentationKreshnik IdrizajNo ratings yet
- ALCOHOL DEPENDENCE: MOA, DIAGNOSIS, TREATMENT, WITHDRAWAL & COMPLICATIONSDocument20 pagesALCOHOL DEPENDENCE: MOA, DIAGNOSIS, TREATMENT, WITHDRAWAL & COMPLICATIONSKreshnik IdrizajNo ratings yet
- PsychiatryDocument52 pagesPsychiatryEma100% (13)
- Surgical Handpiece Maintenance PosterDocument2 pagesSurgical Handpiece Maintenance PosterHayes MaineNo ratings yet
- Report For Missing Sealing PlateDocument9 pagesReport For Missing Sealing PlateFazalmin shahNo ratings yet
- Atty. Carla Santamaria-Seña Wills and Succession ReviewDocument111 pagesAtty. Carla Santamaria-Seña Wills and Succession ReviewvickimabelliNo ratings yet
- Año del Fortalecimiento de la Soberanía NacionalDocument4 pagesAño del Fortalecimiento de la Soberanía NacionalRYAN 28SKNo ratings yet
- Eng Ind CS Bangalore Mall PDFDocument4 pagesEng Ind CS Bangalore Mall PDFJessica SyiemliehNo ratings yet
- Assignment 8 SolutionsDocument7 pagesAssignment 8 SolutionsCarlos Israel Esparza AndradeNo ratings yet
- Articol Final Rev MG-MK LB Engleza - Clinica Virtuala OnlineDocument14 pagesArticol Final Rev MG-MK LB Engleza - Clinica Virtuala Onlineadina1971No ratings yet
- Wisdom Chi KungDocument0 pagesWisdom Chi KungDevlinPyxNo ratings yet
- Multiple Reactions Assignment Problems 2 To 5Document2 pagesMultiple Reactions Assignment Problems 2 To 5DechenPemaNo ratings yet
- C CA AS SC CL Liin Niiq QU UE E // C CA AS SE ER RE EP PO OR RT TDocument7 pagesC CA AS SC CL Liin Niiq QU UE E // C CA AS SE ER RE EP PO OR RT TG Virucha Meivila IINo ratings yet
- Materials Needed For Breast Care:: Repeat This Step Until The Breast Is CleanDocument4 pagesMaterials Needed For Breast Care:: Repeat This Step Until The Breast Is CleanGulayan, Renz Bryelle T.No ratings yet
- The Good NurseDocument2 pagesThe Good NurseKiela Therese LabroNo ratings yet
- 2 Second Grade English Diagnostic Test (Autoguardado)Document5 pages2 Second Grade English Diagnostic Test (Autoguardado)MELISSA KARENTH MONTES PINTONo ratings yet
- Nanostrength Block Copolymers For Epoxy TougheningDocument5 pagesNanostrength Block Copolymers For Epoxy TougheningRonald GeorgeNo ratings yet
- CP107 Vol II-ERT 2B - 12-Dec 2019 (PA) - 3Document209 pagesCP107 Vol II-ERT 2B - 12-Dec 2019 (PA) - 3NghiaNo ratings yet
- 10 DNA Testing Myths Busted, and Other Favorite Posts: by Blaine T. BettingerDocument11 pages10 DNA Testing Myths Busted, and Other Favorite Posts: by Blaine T. BettingerSexy888No ratings yet
- Ethnomusicology in Times of TroubleDocument15 pagesEthnomusicology in Times of TroubleLéo Corrêa BomfimNo ratings yet
- The Maharashtra Shops and Establishments (Regulation of Employment and Conditions of Service) Rules, 2018Document2 pagesThe Maharashtra Shops and Establishments (Regulation of Employment and Conditions of Service) Rules, 2018Gopinath hNo ratings yet
- Removal of A Pinned Spiral by Generating Target Waves With A Localized StimulusDocument5 pagesRemoval of A Pinned Spiral by Generating Target Waves With A Localized StimulusGretymjNo ratings yet
- Business Plan: Prepare by Hau Teen Yee FabriceDocument26 pagesBusiness Plan: Prepare by Hau Teen Yee FabricekarimanrlfNo ratings yet
- The Impact of ProstitutionDocument6 pagesThe Impact of ProstitutionLea TanNo ratings yet
- Quality Management System at Pharmaceutical IndustryDocument85 pagesQuality Management System at Pharmaceutical IndustryTissa Novida Aulia ZahraNo ratings yet
- Organozinc CompoundDocument8 pagesOrganozinc Compoundamanuel tafeseNo ratings yet
- PDFDocument478 pagesPDFPriyaranjan PradhanNo ratings yet
- General Catalogue 2019: UNIOR D.DDocument401 pagesGeneral Catalogue 2019: UNIOR D.DjinpoeNo ratings yet
- Pedest Tbox Toolbox - 4 Sidewalks and Walkways PDFDocument44 pagesPedest Tbox Toolbox - 4 Sidewalks and Walkways PDFbagibagifileNo ratings yet
- KOLHAN UNIVERSITY B.Sc Zoology Semester I Exam 2021 Provisional Marks CardDocument2 pagesKOLHAN UNIVERSITY B.Sc Zoology Semester I Exam 2021 Provisional Marks CardSmritiNo ratings yet
- Adime Malnutrition and OncolgyDocument6 pagesAdime Malnutrition and Oncolgyapi-300587226100% (1)
- Incident Accident FormDocument4 pagesIncident Accident Formsaravanan ssNo ratings yet
- Fuel CellDocument71 pagesFuel CellAhmed Mostafa100% (1)